Abstract
The Questionnaire of Cognitive Schema Activation in Sexual Context (QCSASC) is a validated and widespread used measure to assess the self-schemas elicited during sexual negative events in both men and women. The current study aimed to test the psychometric characteristics of the Italian version of the QCSASC in both heterosexual men and women. After linguistic translation, the psychometric properties (internal consistency, construct and discriminant validity) were evaluated in 1038 participants (435 men and 603 women, 767 healthy and 271 clinicals complaining of sexual problems). Confirmatory factor analyses showed a not satisfactory fit of the original factor structure of the QCSASC versions. Principal component analyses were performed highlighting two new factorial structures, further validated with CFAs (“Helpless” and “Unlovable”). Cronbach’s alpha, composite reliability and average variance extracted were used as internal consistency measures. Moreover, the QCSASC showed a strong association with emotional response and sexual functioning, being able to differentiate between sexually clinical and control group. Current findings support the validity and the internal consistency of the QCSASC Italian version and allows to assess dysfunctional cognitive schemas activated when facing sexual problematic situations for both clinical and research purposes.
Similar content being viewed by others
Introduction
Schemas are described as core structures of the cognitive system [1]. They represent patterns of internal experience (including memories, beliefs, emotions, thoughts, scripts and stereotypes) developed during childhood and further elaborated throughout the lifetime [2]. Schemas organize incoming information giving significance to what it is perceived, and they consequently guide emotional and behavioral responses to stimuli [1]. The organization of new perceptions into schemas is fast, to better evaluate and react reaching an aim or protecting from danger (real or perceived). Experience and environment select and reinforce the more adaptive schemas in specific circumstances [3]. They can be both functional or dysfunctional, depending on the content, the rigidity and the emotional/behavioral response associated [4]. Usually, schemas are stable and difficult to modify. Part of the cognitive therapy approach is focused on dealing with rigid schemas to reach a wider cognitive flexibility. As a matter of fact, rigid dysfunctional schemas are involved in the onset of many psychopathologies such as depression (mainly characterized by negative self-schemas) and anxiety (in which the “self” is perceived as inadequate or mistreated by the others) [5].
Although a growing body of literature underlines the importance of cognitions in sexual functioning [6,7,8,9,10,11,12,13], the specific cognitive-affective mechanisms involved in the activation and regulation of subjective and genital response are still not completely understood. When people become aware of being aroused, they cognitively elaborate the sexual stimuli and maintain the attention to them. When this process results in a positive evaluation, feelings of sexual desire and arousal can be experienced [14, 15]. According to Barlow’s model of sexual functioning (1986), during a sexual stimulation sexually healthy men and women tend to respond with positive affect and focus on sexual cues, whereas people with sexual problems usually focus their attention to non-relevant non-sexual stimuli and are more likely to experience negative affect [13, 16,17,18]. Cognitions (e.g., performance anxiety and attitude toward sex) were also included in the Basson’s circular model [19], stating that the cognitive appraisal of sexual stimuli influences women’s experience of subjective sexual arousal. Positive attitudes toward sex and low levels of performance anxiety may facilitate a pleasurable experience of sex and higher levels of sexual motivation in both men and women [20,21,22,23]. An inappropriate attentional focus that involves attending to negative consequences of not performing or some other issues, can inhibit the arousal through the mechanism of cognitive interference, distraction or spectatoring [24,25,26]. Thus, sexually functional and dysfunctional subjects react very differently to a variety of cognitive sets related to sex [26].
Cognitive schemas role in onset and maintenance of sexual complaints has been emphasized in the last years [27,28,29,30,31,32,33,34,35,36]. Starting from the notion of “sexual scripts” (cognitive framework responsible for planning, coordinating and expressing social conduct including sexual behavior) conceptualized by Gagnon and Simon [37], and the pioneering research of Andersen et al. [38, 39] on the “sexual self-schema”, cognitive schemas have been under active research in matter of relational issues and sexual dysfunctions [40,41,42,43,44,45,46,47]. Several studies have shown that cognitive factors (such as distraction, efficacy expectancies, causal attributions, schemas, sexual beliefs and automatic thoughts) play a significant role in determining sexual response [43].
In order to assess the influence of some dysfunctional cognitive self-schemas in heterosexual oriented sexual problematic situations, Nobre and Pinto-Gouveia created [9] and validated [43] the Questionnaire of Cognitive Schema Activation in Sexual Context (QCSASC). The questionnaire is based on Beck’s theory [48, 49] in which two principal categories of negative schemas are generally related to psychopathological symptomatology: “Helpless” schema is referred to the idea of feeling personally powerless, weak, vulnerable, incompetent, inferior and without hope; “Unlovable” schema is related to the feeling of not deserving to be loved, accepted, appreciated or desired by the others. The QCSASC items are inferred from Beck taxonomy [48], counting for 28 core beliefs (14 for “Helpless” and 14 for “Unlovable”). Clinical evidences suggested that men are more used to report Helpless schemas in association with sexual dysfunctions compared with women, because they usually interpret sexual dysfunctions as a sign of personal weakness and incompetence [50,51,52]. Women are more used to respond with Unlovable schemas, supported by the idea that mainly social/interpersonal issues are involved in female sexual dysfunctions [53, 54]. Nobre and Pinto-Gouveia [43] confirmed only partially the two factors structure, identifying other three domains (incompetence, self-depreciation and difference/loneliness). About genders, Nobre and Pinto-Gouveia [44] found that incompetence-related attribution to sexual failures play a significant role in both men and women. QCSASC was shown as a good measure of dysfunctional cognitive schemas compared with others available (e.g., “Schema Questionnaire” by Young and Brown [55] “Sexual Self-Schema” by Andersen and Cyranowski [38] and Andersen et al. [39], also able to distinguish between sexually clinical and healthy people. Specifically, data indicated that QCSASC total score was significantly higher (F(1,227) = 14.63; p < 0.001) for the clinical sample (M = 46.76) compared with controls (M = 35.81) [43]. Moreover, they found a strong association between the identification with unsuccessful sexual episodes (sexual problems events) and higher negative self-schemas [43, 44]. A detailed description of the questionnaire is reported in “Measures”.
The QCSASC was assessed in many researches [7, 10, 41, 45, 46, 56,57,58,59,60,61,62,63,64,65]. Exploring male sexual response, Quinta-Gomes and Nobre [63, 66] found that men with lower sexual functioning scores showed a significantly higher frequency of dysfunctional schemas such as “Difference/Loneliness”, “Self-Depreciation”, “Incompetence” and “Undesirability/Rejection” in unsuccessful sexual situations. On sexual desire, Nimbi et al. [7, 56, 57] did not find any direct effect of the QCSASC domains on the levels of sexual desire in men. Regarding to females [10, 45], most of the women with sexual dysfunctions reported the activation of “Incompetence” schemas when facing unsuccessful sexual situations. For example, Viozzi et al. [64, 65] showed significant higher scores in “Incompetence”, “Helpless” and “Difference/Loneliness” subscales in a group of women claiming for sexual pain compared with healthy women. Regarding to different sexual orientations, similar pathways were observed in gay men and lesbian women using a QCSASC adapted form for homosexual orientation [46]. A moderation role of dysfunctional sexual beliefs was shown in the association between the frequency of negative sexual episodes and incompetence schemas in homosexual and heterosexual men and women [60,61,62].
Therefore, the assessment of dysfunctional cognitive schemas could be an important domain to be considered in the evaluation and treatment of sexual problems, and, as a result, the spreading of tools such as the QCSASC could facilitate multicultural research and increase the adoption of holistic care taking for patients. Apart from the utility to have a language translation of a questionnaire, testing the validity of a psycho-sociological measure every 10–15 years is strongly recommended in psychometry. The following study will also show data on the use of cognitive schemas in sexual context in the Italian population. Schemas are also culture dependent and related to general messages about sex and genders. We expect to confirm the difference between men and women on the activation of different schemas (incompetence for man and unlovable/rejection for women) and the association between the presence of sexual dysfunctions and negative schemas.
Aims
The current study aimed to explore the internal reliability, construct and discriminant validity of the QCSASC Italian versions for heterosexual men and women. The discriminant validity was tested comparing the scores of sexually clinical and healthy groups. Clinical implications are discussed.
Methods
Participants and procedures
A total of 1038 volunteers (435 males and 603 females) from the general population participated in the study. People were recruited with a snowball technique from the Department of Dynamic and Clinical Psychology, “Sapienza” University of Rome and by advertisements on website (www.sessuologiaclinicaroma.it) and social networks (Facebook and LinkedIn). Participants were given a personal ID code to access a web-survey (available on “Google.docs” platform) to restrict one response per person. Data were collected online, protected by private ID and encrypted password, and then downloaded and locked up in an external hard disk at the Institute of Clinical Sexology. About 13.2% of the people willing to be involved did not complete the online survey. Non-responses where allowed in the survey, but incomplete questionnaires (4.2%) where excluded from the current analyses. Participants completed an informed consent. The questionnaire administered was anonymous and no remuneration was provided. Including criteria were being Italian citizens, at least 18 years old, being predominantly heterosexual (we considered the first two points measured by the seven-points Kinsey scale because the QCSASC items are heterosexually oriented) and sexually active (at least one sexual intercourse) in the last 6 months. Exclusion criteria were the presence of clinical psychopathological levels measured by SCL-90-R (Global Score Index < 1) or previous hospitalization for psychiatric diseases. For the discriminant analyses, participants were split into four subgroups (sexually healthy and clinical men and women) based on the self-declaration at four items: “During the last 6 months, did you have any sexual problem?”, “If Yes, please describe your sexual difficulty”, “How long have you been claiming this sexual problem?”, and “Did you report a significant personal distress about this problem?”. Only people declaring having at least a distressing sexual problem for 6 months or more were put in the “clinical group”. The institutional ethics committee of the *** expressed the consent to conduct the study on 21 January 2015. Data were collected from June 2015 to December 2016.
Measures
Sociodemographic questionnaire
Participants answered a brief sociodemographic form to collect general information such as age, sexual orientation (seven-points Kinsey scale), relationship and marital status, educational level, work status, children and sexual difficulties.
Questionnaire of Cognitive Schema Activation in Sexual Context
QCSASC [43] is a 28-item instrument able to assesses cognitive self-schemas activated when facing sexual problematic situations. The first part of the test consists of the presentation of four sexual common episodes related to the most known sexual dysfunctions: hypoactive sexual desire disorder (HSDD), erectile disorder (ED), premature (PE) and delayed ejaculation (DE) in the male version, and HSDD, subjective arousal difficulties (SAD), anorgasmia (AO) and vaginismus (VA) in the female one. Participants are asked to indicate the frequency of these events from 1 (never happened) to 5 (happened often). Bearing in mind the most recurrent situation (if any) among these mentioned above, participants are asked to indicate the feelings usually associated to the situation from a list of 10 emotions: worry, sadness, disillusion, fear, guilt, shame, anger, hurt, pleasure and satisfaction. Still focusing on the most recurrent sexual episode endorsed, participants are asked to rate on a five-point Likert scale (“1 – completely false” to “5 – completely true”), the degree of agreement with 28 self-statements reproducing the self-schemas presented by Beck [48]. Five domains were identified in the original Portuguese version:
-
1.
“Undesirability/Rejection” – domain reflecting self-beliefs related to social undesirability and rejection (e.g., “I’m defective”, “I’m bound to be rejected” or “I’m unwanted”);
-
2.
“Incompetence” – dimension characterized by self-beliefs of failure, incompetence, and powerlessness (e.g., “I’m incompetent” and “I’m powerless”);
-
3.
“Self-Depreciation” – factor represented by beliefs related to the self-worthiness and self-defective ideas (e.g., “I’m bad” and “I’m unlikable”);
-
4.
“Difference/Loneliness” – dimension characterized by a belief of being different and lonely (e.g., “I’m different” and “I’m bound to be alone”);
-
5.
“Helpless” – domain represented by beliefs of being helpless and needy (e.g., “I’m needy” and “I’m helpless”).
Specific indexes for the five domains and for the total scale can be calculated through the sum of schema items (higher scores reflecting higher negative schema activation). The five-factor structure found by Nobre and Pinto-Gouveia [43] was different from the two-factor model (Helpless and Unlovable) proposed by Beck [48]. Anyhow, Factor 1 (Undesirability/Rejection) and Factor 2 (Incompetence) represent the two broad domains of unlovability and helplessness [43]. The original measure presented good reliability and validity, and can discriminate between sexually clinical and healthy participants.
International index of erectile function (IIEF)
IIEF [67] is a widely used, multidimensional 15-item instrument for the evaluation of male sexual function. A general index of sexual function and five specific dimensions can be calculated: erectile function, orgasmic function, sexual desire, satisfaction with intercourse and overall satisfaction. Higher scores indicate better sexual functioning. Psychometric studies reported good reliability, validity and the ability to discriminate between sexually clinical and healthy people. The Cronbach’s alpha values for this measure in the current study ranged from 0.87 (sexual desire) to 0.91 (overall satisfaction).
Female sexual function index (FSFI)
FSFI [68] is a well-known 19-item instrument providing detailed information on the general sexual functioning and six specific dimensions: sexual desire, sexual arousal, lubrication, orgasm, sexual satisfaction and sexual pain. Higher scores indicate better sexual functioning. The measure presents acceptable test–retest reliability, internal consistency, validity and the ability to discriminate between sexually clinical and healthy people. The Cronbach’s alpha values for this measure in the current study ranged from 0.82 (sexual arousal) to 0.90 (sexual pain).
Linguistic validation
The two original versions of QCSASC were translated into Italian by the authors. The translation was controlled by a professional supervisor and then translated back into English by a mother-tongue language expert with a specific scientific expertise. The English version was checked with the original questionnaire to avoid main significance bias and tested in a small group of 20 men and 20 women to identify comprehension problems. Questionnaires and scoring are reported in (Appendix A, B and C (Table 9)).
Statistical analysis
The psychometric properties of the Italian version of the QCSASC were assessed by several statistical tests following the guidelines of Sakaluk and Short [69]. Construct validity was estimated at item level with Principal Component Analysis (PCA) to find the underling constructs of the questionnaires. In this phase, a direct oblimin rotation was used. After reaching two satisfying models, they were organized as Path Diagrams and tested with Confirmatory Factor Analysis (CFA). Composite reliability (CR) and average variance extracted (AVE) values were examined. Internal consistency was assessed using Cronbach’s alpha. Pearson correlations, one-way Multivariate Analyses of Covariance (MANCOVAs) and Mann–Whitney U-test were used to analyze associations with affective response and differences between clinical and sexually healthy men and women. Age and educational level were controlled considering them as covariates in the MANCOVAs because of their well-established direct association with sexual problems (higher in older people) and dysfunctional schema activation (higher in lower education). Two-tailed results were considered. PCAs, Cronbach’s alphas, Pearson correlations and MANCOVAs and Mann-Whitney U-test were performed using IBM SPSS v. 23.0; CFAs were tested with IBM SPSS Amos v.22 (SPSS Inc., Chicago, IL, USA).
Results
Participants mean age was 30.02 ± 9.42 (range 18–76) and sociodemographic characteristics of male and female groups are reported in Table 1.
Validity and reliability of the male QCSASC
First, CFA was assessed to verify the consistency of the original structure of the QCSASC (5 factors, 28 items) [43]. Maximum likelihood (ML) estimation method was used following Tabachnick and Fidell [70]. CFA reported non-satisfactory model fit, comparison and parsimony results (χ2 = 2825.41, df = 292, root mean square error of approximation (RMSEA) = 0.108, goodness of fit index (GFI) = 0.75, normed fit index (NFI) = 0.82, comparative fit index (CFI) = 0.85). Moreover, data showed very high correlations between some of the factors (r > 0.90). For these reasons, PCAs were conducted on the 28 items of the Italian version to explore the most representative factorial structure using a direct oblimin rotation. Kaiser-Meyer-Olkin (KMO) value of 0.96 supported the adequacy of the sample. The significance of Bartlett’s test of sphericity (χ2 = 10,573.02; p < 0.001) meant that correlations between items were largely enough to conduct a PCA. PCAs were run following the Monte Carlo parallel analysis. This procedure identified two components accounting for 61.42% of total variance. Item selection was based on loadings higher than 0.4 on the respective factors. Table 2 shows the component loadings after rotation (pattern matrix) for each item included. Intercorrelation between factors was statistically significant (r = 0.76; p < 0.001).
CFA was conducted on the two-factor solution (28 items) measuring indices of model fit, comparison and parsimony. ML estimation method was used following Tabachnick and Fidell [70]. To increase the model fit, pathways between error variance for items inside the same factor were inserted. Chi-square for the model (Fig. 1) was significant (χ2 = 572.66; df = 253; p < 0.001). RMSEA with 90% confidence intervals was 0.054 (CI = 0.048–0.060). Other fit indices evaluated included GFI = 0.92, NFI = 0.95 and CFI = 0.97. Acceptable fit was reached in all measures except for chi-square because of its sensitivity to sample size [71, 72]. Regression coefficients for this model ranged from 0.51 to 0.85 and were all statistically significant (p < 0.001).
Internal consistency was assessed using Cronbach’s alpha for each factor and total score. The Cronbach’s alpha coefficients were satisfactory (Helpless = 0.95; Unlovable = 0.95; QCSASC Total Score = 0.97). The CR for each construct is above the expected thresholds of 0.70 (Helpless = 0.93; Unlovable = 0.95; Total Score = 0.94). The AVE for each construct is above the expected thresholds of 0.50 (Helpless = 0.51; Unlovable = 0.56; Total Score = 0.53).
Validity and reliability of the female QCSASC
CFA was assessed to verify the consistency of the original structure of the QCSASC (5 factors, 28 items) [43]. ML estimation method was used following Tabachnick and Fidell [70]. CFA reported non-satisfactory model fit, comparison and parsimony results (χ2 = 2894.31, df = 292, RMSEA = 0.121, GFI = 0.71, NFI = 0.80, CFI = 0.81). Moreover, data showed very high correlations between some of the factors (r > 0.90). For these reasons, PCAs were conducted on the 28 items of the Italian version using a direct oblimin rotation. KMO value of 0.95 supported the adequacy of the sample and the significance of Bartlett’s test of sphericity (χ2 = 15,170.75; p < 0.001) validated the PCA results. PCAs were run following the Monte Carlo parallel analysis. The most suitable and interpretable PCA was identified in two components, which accounted for 60.55% of total variance. Item selection was based on loadings higher than 0.4 on the respective factors. Table 3 shows the component loadings after rotation (pattern matrix) for each item included. Intercorrelation between factors was significant (r = 0.78; p < 0.001).
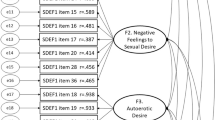
CFA was conducted on the two-factor solution (28 items) measuring indices of model fit, comparison and parsimony. ML estimation method was used following Tabachnick and Fidell [70]. To increase the model fit, pathways between error variance for items inside the same factor were inserted. Chi-square for the model (Fig. 2) was significant (χ2 = 696.35; df = 228; p < 0.001). RMSEA with 90% confidence intervals was 0.058 (CI = 0.053–0.063). Other fit indices evaluated were GFI = 0.93, NFI = 0.96 and CFI = 0.97. Acceptable fit was reached in all measures except for chi-square because of its sensitivity to sample size [71, 72]. Regression coefficients for this model ranged from 0.52 to 0.89 and were all statistically significant (p < 0.001).
Internal consistency was assessed using Cronbach’s alpha for both factors and total score. The Cronbach’s alpha coefficients were satisfactory (Helpless = 0.94; Unlovable = 0.95; QCSASC Total Score = 0.97). The CR for each construct is above the expected thresholds of 0.70 (Helpless = 0.94; Unlovable = 0.95; Total Score = 0.95). The AVE for each construct is above the expected thresholds of 0.50 (Helpless = 0.52; Unlovable = 0.57; Total Score = 0.55).
Discriminant validity
In order to analyze discriminant validity, we used one-way MANCOVAs (controlling for age and educational level) between the clinical (participants declaring having sexual problems in the last 6 months) and the control group (sexually healthy participants) (Table 4). We expected that the clinical group would present higher scores on both male and female QCSASC scales, supporting the hypothesis that the questionnaires evaluate clusters of thoughts, which are conceptualized as vulnerability factors for the development or maintenance of sexual dysfunctions. The models were significant for both males (λ = 0.83; p < 0.001) and females (λ = 0.88; p < 0.001). Results showed that the clinical group presented higher significant scores on all domains of the QCSASC compared with controls in both men and women.
As the QCSASC subscales were not normally distributed, we also tested for clinical and control differences employing nonparametric statistical analyses. In particular, men and women distributions were compared using the Mann–Whitney U-test. As reported in Table 5, results confirmed that control and clinical participants were significantly different in each domain, with clinical groups reporting higher dysfunctional schema activation scores.
Associations between sexual situations, emotions and cognitive schemas
The most reported sexual complaints in the sexually healthy group were PE (27.4%) and DE (26.4%) for man and AO (27.1%) and HSDD (16.7%) for women. In the clinical group, the most reported complaints were ED (48.4%) and PE (41.9%) for males and VA (50.3%) and SAD (47.6%) for females. Correlations between sexual situations and emotions are showed in Table 6. For men, the identification with sexual dysfunctions was more often associated with the endorsement of sadness, disillusion, fear, guilt, pleasure and satisfaction. Women more often reported the association with worry, sadness, disillusion, fear and shame. When facing sexual problems, both men and women were characterized by negative emotional response: in particular men reported less positive feelings (e.g., pleasure and satisfaction) and women endorsed more negative emotions (e.g., disillusion and sadness).
With regard to the associations between sexual situations and cognitive schemas (Table 7), the analysis showed significant correlations in all domains for both genders, in particular for arousal and orgasm complaints.
Associations between cognitive schemas and sexual function
It was also verified if the scores of the Italian QCSASC were directly correlated to sexual function. All statistically significant results (Table 8) were found, showing that a major endorsement of Helpless and Unlovable self-schemas is associated with worse sexual functioning in all areas for both genders.
Discussion
The main purpose of the current study was to investigate the psychometric properties of the Italian version of the QCSASC. After linguistic translation, CFAs were run, failing to confirm the original questionnaire structure in both males and females [43]. The unsatisfactory model fit suggested that a new structure was needed to better explain data. For this reason, PCAs were necessary to find a new structure for both genders. To be more accurate, the Monte Carlo parallel analyses was performed. The best structures were identified in two components, identical for males and females. Factors found reflected the original structure suggested by Beck [48]: “Helpless” (characterized by the idea of one self as weak and hopeless) and “Unlovable” (referred to beliefs like being undesirable and unworthy). CFAs confirmed the good fit of the new versions: even if chi-square was significant, other indices reported (RMSEA, GFI, NFI and CFI) were satisfying on both versions. The final versions counted 28 items for both genders, explaining 61.42 and 60.55% of variance for males and females, respectively. Moreover, internal consistency showed good results reporting satisfactory Cronbach’s alpha, CR and AVE values. Overall, the Italian version of QCSASC demonstrated good psychometric properties.
The differences with the original version need to be further discussed. The original solution was not supported [43] and two new structures consistent with Beck’s dysfunctional schemas theory [48, 49] were reported. “Helpless” and “Unlovable” factors describe two of the main sexual self-schemas, which clinicians could to observe and face in sexual therapy. Part of integrated sexual approach is focused on replacing rigid schemas with more flexible cognitions about sexuality, allowing the patient to have a more functional reaction to adverse sexual events [42, 47, 73].
The modification of item/factor structure is common in PCAs and it could depend on both statistical and cultural reasons. Statistically, in the validation study on a different sample, some minor fluctuations and intersections between similar factors are possible. This happens more frequently when the subscales are closely connected (as in this case) or when the sample size is small. Culturally, the background in which the original QCSASC has been validated should be considered: some minor cultural differences could be identified within Italy and Portugal (both referring to the “Mediterranean – Catholic background”) [74]. Time could be an important variable in play: in fact, the original questionnaire was developed in 2000 and validated in 2009 [9, 43]. Psychometry is strongly recommended to update the validation studies of a psychosociological measure every 10–15 years: the behavior and the beliefs about sexuality may change a lot, and probably repeating the psychometric study in Portugal today could show a new QCSASC structure, closer to the one presented in this paper.
The findings for cognitive schemas, emotions and sexual functioning seem to support the biopsychosocial model, which is focused on the integration of different aspects of sexuality for a holistic understanding [73]. Self-schemas elicited in sexual problematic situations were associated with more negative emotions in women and fewer positive emotions in men. Women and men reported to use both Helpless and Unlovable self-schemas facing negative sexual situations. Contrary to the literature supporting a gender difference in sexual schema activation [50,51,52,53,54], similar scores on schemas referring to feeling Helpless and Unlovable in men and women were also noticed by Nobre and Pinto-Gouveia [43]. These authors suggested that the traditional “double standard” (in which men’s sexuality is mostly performance related if compared with women, characterized by love and commitment) seems not to influence directly the self-schemas activation. Another possible explanation is that women nowadays could be more focused on performance and men on relationship than before. Moreover, the use of schemas presented was correlated with lower sexual functioning in both genders. This is consistent with previous studies [10, 41, 43,44,45,46, 58,59,60,61,62,63,64,65] and could suggest that the QCSASC may detect two variables that have a role on the development and maintenance of sexual dysfunctions. Its use could be useful to facilitate the assessment and evaluate the psychological treatment.
The research presented has some limitations. First, participants were selected with a “snowball” technique and therefore is not possible to generalize the results for the Italian population. Second, test–retest reliability, convergent, divergent, concurrent or discriminant validity were not assessed in this study. For these reasons, further studies should be conducted to replicate current findings and extend the psychometric understanding of the QCSASC. Moreover, next studies should also consider extending the evaluation of the schemas activated in other sexual contexts: the QCSASC reports only some of the main negative events that can occur in heterosexual sexual situations, but the variability of cases of sexual problems is much wider (e.g., pain during intercourses, hypersexuality, persistent genital arousal, different sexual orientations, etc.). Multicultural studies about the interaction between cognition, affection and sexual response to explore differences and similarities between countries are also needed. In general, our results seem to validate the idea that cognitive schemas activated in sexual negative events could have a role on the onset and on the maintenance of sexual dysfunctions.
Conclusions
The present study tries to extend the psychometric knowledge of the QCSASC on an Italian group. Results seem to be premising, but they should be deepened by further studies. The use of the QCSASC could be recommended in both clinical and research field. The benefits for a clinician, as well as for a researcher, may be diverse: firstly, this psychometric tool may help to better explain the nature of the sexual dysfunctions etiology (onset and maintenance); second, it may give important cues to the clinician to cope with for the resolution of a sexual symptom and it may help to verify the efficacy of a sexual therapy. Therapists should deal with the negative cognitive schemas activated when facing unsuccessful sexual episodes and give the possibility to the patient to understand and to break the cycle (negative thoughts, anxiety response, symptom and distress).
References
Beck AT. Depression: clinical, experimental, and theoretical aspects. Philadelphia: University of Pennsylvania Press; 1967.
Dozois DJ, Beck AT. Cognitive schemas, beliefs and assumptions. Risk Factors Depress. 2008;1:121–43.
Nadkarni S, Narayanan VK. Strategic schemas, strategic flexibility, and firm performance: the moderating role of industry clockspeed. Strateg Manag J. 2007;28:243–70.
Young JE. Schema-focused cognitive therapy and the case of Ms. S. J Psychother Integr. 2005;15:115.
Alford BA, Beck AT. The integrative power of cognitive therapy. Guilford Press; 1998.
Janssen E, Everaerd W, Spiering M, Janssen J. Automatic processes and the appraisal of sexual stimuli: towards an information processing model of sexual arousal. J Sex Res. 2000;37:8–23.
Nimbi FM, Tripodi F, Rossi R, Simonelli C. Expanding the analysis of psychosocial factors of sexual desire in men. J Sex Med. 2018;15:230–44.
Nobre PJ, Pinto-Gouveia J. Emotions during sexual activity: differences between sexually functional and dysfunctional men and women. Arch Sex Behav. 2006;35:491–9.
Nobre PJ, Pinto-Gouveia J. Questionnaire of Cognitive Schema Activation in Sexual Context (QCASC). Unpublished manuscript, Faculty of Psychology and Educational Science, University of Coimbra, Portugal, 2000.
Nobre PJ, Pinto-Gouveia J. Cognitive and emotional predictors of female sexual dysfunctions: preliminary findings. J Sex Marital Ther. 2008;34:325–42.
Nobre PJ, Pinto-Gouveia J. Sexual modes questionnaire: measure to assess the interaction among cognitions, emotions, and sexual response. J Sex Res. 2003;40:368–82.
Peterson ZD, Janssen E. Ambivalent affect and sexual response: the impact of co-occurring positive and negative emotions on subjective and physiological responses to erotic stimuli. Arch Sex Behav. 2007;36:793–807.
Vilarinho S, Laja P, Carvalho J, Quinta-Gomes AL, Oliveira C, Janssen E et al. Affective and cognitive determinants of women’s sexual response to erotica. J Sex Med. 2014;11:2671–8.
Dewitte M. Different perspectives on the sex-attachment link: towards an emotion-motivational account. J Sex Res. 2012;49:105–24.
Dewitte M. Gender differences in liking and wanting sex: examining the role of motivational context and implicit versus explicit processing. Arch Sex Behav. 2015;44:1663–74.
Laan E, Everaerd W, Van Aanhold M, Rebel M. Performance demand and sexual arousal in women. Behav Res Ther. 1993;31:25–35.
Meston C, Gorzalka B. Differential effects of sympathetic activation on sexual arousal in sexually dysfunctional and functional women. J Abnorm Psychol. 1996;105:582–91.
Palace EM, Gorzalka BB. The enhancing effects of anxiety on arousal in sexually dysfunctional and functional women. J Abnorm Psychol. 1990;99:403–11.
Basson R. Human sex-response cycles. J Sex Marital Ther. 2001;27:33–43.
Brotto LA, Basson R, Luria MA. Mindfulness-based group psychoeducational intervention targeting sexual arousal disorder in women. J Sex Med. 2008;5:1646–59.
Giles KP, McCabe MP. Conceptualizing women’s sexual function: linear vs. circular models of sexual response. J Sex Med. 2009;6:2761–71.
McCabe M. The role of performance anxiety in the development and maintenance of sexual dysfunction in men and women. Int J Stress Manag. 2005;12:379–88.
McCabe M, Cobain MJ. The impact of individual and relationship factors on sexual dysfunction in males and females. J Sex Marital Ther. 1998;13:131–43.
Kaplan HS. The new sex therapy. New York: Brunner/Mazel; 1974
Masters W, Johnson, V. Human sexual inadequacy. Boston: Little, Brown; 1970.
Barlow DH. Causes of sexual dysfunction: the role of anxiety and cognitive interference. J Consult Clin Psychol. 1986;54:140–8.
Carpenter KM, Andersen BL, Fowler JM, Maxwell GL. Sexual self schema as a moderator of sexual and psychological outcomes for gynecologic cancer survivors. Arch Sex Behav. 2009;38:828–41.
Cyranowski JM, Andersen BL. Schemas, sexuality, and romantic attachment. J Personal Social Psychol. 1998;74:1364–79.
Cyranowski JM, Andersen BL. Evidence of self-schematic cognitive processing in women with differing sexual self-views. J Social Clin Psychol. 2000;19:519–43.
Géonet M, De Sutter P, Zech E. Cognitive factors in women hypoactive sexual desire disorder. Sexologies. 2013;22:e9–e15.
Kuffel SW, Heiman JR. Effects of depressive symptoms and experimentally adopted schemas on sexual arousal and affect in sexually healthy women. Arch Sex Behav. 2006;35:160–74.
Meston CM, Rellini AH, Heiman JR. Women’s history of sexual abuse, their sexuality, and sexual self-schemas. J Consult Clin Psychol. 2006;74:229–40.
Reissing ED, Laliberté GM, Davis HJ. Young women’s sexual adjustment: the role of sexual self-schema, sexual self-efficacy, sexual aversion and body attitudes. Can J Human Sex. 2005;14:77–89.
Sigre-Leirós V, Carvalho J, Nobre P. Preliminary findings on men’s sexual self-schema and sexual offending: differences between subtypes of offenders. J Sex Res. 2016;53:204–13.
Stanton AM, Meston CM, Boyd RL. Sexual self-schemas in the real world: investigating the ecological validity of language-based markers of childhood sexual abuse. Cyber Behav Social Netw. 2017;20:382–8.
Ziaee P, Mashhadi A. The effectiveness of sexual education focused on cognitive schemas, on the improvement of sexual functioning among female married students. Evid Based Care. 2014;4:73–82.
Gagnon JH, Simon W. Sexual conduct: the social origins of human sexuality. Chicago: Aldine; 1973.
Andersen BL, Cyranowski JM. Women’s sexual self-schema. J Personal Social Psychol. 1994;67:1079.
Andersen BL, Cyranowski JM, Espindle D. Men’s sexual self-schema. J Personal Social Psychol. 1999;76:645–53.
Gagnon JH, Rosen RC, Leiblum SR. Cognitive and social aspects of sexual dysfunction: sexual scripts in sex therapy. J Sex & Marital Ther. 1982;8:44–56.
Gomes ALQ, Nobre P. Early maladaptive schemas and sexual dysfunction in men. Arch Sex Behav. 2012;41:311–20.
Kirana PS, Tripodi F, Reisman Y, Porst H. The EFS and ESSM syllabus of clinical sexology. Amsterdam: Medix; 2013.
Nobre PJ, Pinto-Gouveia J. Questionnaire of cognitive schema activation in sexual context: a measure to assess cognitive schemas activated in unsuccessful sexual situations. J Sex Res. 2009a;46:425–37.
Nobre PJ, Pinto-Gouveia J. Cognitive schemas associated with negative sexual events: a comparison of men and women with and without sexual dysfunction. Arch Sex Behav. 2009b;38:842–51.
Oliveira C, Nobre PJ. Cognitive structures in women with sexual dysfunction: the role of early maladaptive schemas. J Sex Med. 2013;10:1755–63.
Peixoto MM, Nobre P. Cognitive schemas activated in sexual context: a comparative study with homosexual and heterosexual men and women, with and without sexual problems. Cogn Ther Res. 2015;39:390–402.
Reisman Y, Porst H, Lowenstein L, Tripodi F, Kirana, SP. The ESSM manual of sexual medicine. Amsterdam: Medix; 2015.
Beck J. Cognitive therapy: basics and beyond. New York: Guilford; 1995.
Beck AT. Beyond belief: a theory of modes, personality, and psychopathology. In: Salkovskis P, editor. Frontiers of cognitive therapy. New York: Guilford; 1996. p. 1–25.
Carey MP, Wincze JP, Meisler AW. Sexual dysfunction: male erectile disorder. In: Barlow DH, editor. Clinical handbook of psychological disorders: a step by step treatment manual. 2nd ed. New York: Guilford Press; 1993; p. 442–80.
Rosen RC, Leiblum SR, Spector I. Psychologically based treatment for male erectile disorder: a cognitive-interpersonal model. J Sex Marital Ther. 1994;20:67–85.
Sbrocco T, Barlow DH. Conceptualizing the cognitive component of sexual arousal: implications for sexuality research and treatment. In: Salkovskis PM, editor. Frontiers of cognitive therapy. New York: Guilford Press; 1996; p. 419–49.
Leiblum SR. Commentary: critical overview of the new consensus-based definition and classification on female sexual dysfunction. J Sex Marital Ther. 2001;27:159–68.
Basson R. Women’s sexual dysfunction: revised and expanded definitions. Can Med Assoc J. 2005;172:1327–33.
Young JE, Brown G. Young schema questionnaire. Cognitive therapy for personality disorders: A schema-focused approach, 63–76, 1994.
Nimbi FM, Tripodi F, Rossi R, Simonelli C. Biopsychosocial predictors of sexual desire level in men. J Sex Med. 2017a;14:e277.
Nimbi FM, Tripodi F, Rossi R, Simonelli C. PS-01-012 Which biopsychosocial variables affect more level of sexual desire in men? J Sex Med. 2017b;14:e109.
Nobre PJ. Determinants of sexual desire problems in women: testing a cognitive–emotional model. J Sex & Marital Ther. 2009;35:360–77.
Nobre PJ. Psychological determinants of erectile dysfunction: testing a cognitive–emotional model. J Sex Med. 2010;7(4pt1):1429–37.
Peixoto MM, Nobre P. “Macho” beliefs moderate the association between negative sexual episodes and activation of incompetence schemas in sexual context, in gay and heterosexual men. J Sex Med. 2017a;14:518–25.
Peixoto MM, Nobre P. The activation of incompetence schemas in response to negative sexual events in heterosexual and lesbian women: the moderator role of personality traits and dysfunctional sexual beliefs. J Sex Res. 2017b;9:1188–96.
Peixoto MM, Nobre P. Incompetence schemas and sexual functioning in heterosexual and lesbian women: the mediator role of automatic thoughts and affective states during sexual activity. Cogn Ther Res. 2017c;41:304–12.
Quinta-Gomes AL, Nobre P. Psychological variables in male sexual dysfunction: cognitive schemas and personality. Sexologies. 2008;17:124–38.
Viozzi E, Rossi V, Tripodi F, Fabrizi A, Nimbi FM, Simonelli C. Sex life in women with sexual pain: a preliminary study. J Sex Med. 2017a;14:e261.
Viozzi E, Rossi V, Tripodi F, Nimbi FM, Simonelli C. PS-03-001 female sexual pain and quality of sex life: preliminary results of the Italian protocol “sexuality and well-being”. J Sex Med. 2017b;14:e114.
Quinta-Gomes AL, Nobre P. Early maladaptive chemas and sexual dysfunction in men. Arch Sex Behav. 2012;41:311–20.
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A. The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology. 1997;49:822–30.
Rosen C, Brown J, Heiman S, Leiblum C, Meston R, Shabsigh D et al. The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex & Marital Ther. 2000;26:191–208.
Sakaluk JK, Short SD. A methodological review of exploratory factor analysis in sexuality research: used practices, best practices, and data analysis resources. J Sex Res. 2017;54:1–9.
Tabachnick BG, Fidell LS. Using multivariate statistics. 5th ed. New York: Allyn and Bacon; 2007.
Byrne BM. Structural equation modeling with LISREL, PRELIS, and SIMPLIS: basic concepts, applications, and programming. New York: Psychology Press; 2013.
Miles J, Shevlin M. A time and a place for incremental fit indices. Personal Individ Differ. 2007;42:869–74.
Simonelli C, Fabrizi A, Rossi R, Silvaggi C, Tripodi F, Michetti PM. Clinical sexology: an integrated approach between the psychosomatic and the somatopsychic. Sexologies. 2010;19:3–7.
Nimbi FM, Tripodi F, Simonelli C, Nobre P. Sexual Modes Questionnaire (SMQ): translation and psychometric properties of the Italian version of the automatic thought scale. J Sex Med. 2018;15:396–409.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Appendices
Appendix A. Male version Italian Questionnaire of Cognitive Schema Activation in Sexual Context (QCSASC)
▓

Appendix B. Female version Italian Questionnaire of Cognitive Schema Activation in Sexual Context (QCSASC)
▓

Appendix C
Table 9
Rights and permissions
About this article
Cite this article
Nimbi, F.M., Tripodi, F., Simonelli, C. et al. Questionnaire of Cognitive Schema Activation in Sexual Context: translation and psychometric properties of the Italian version. Int J Impot Res 30, 253–264 (2018). https://doi.org/10.1038/s41443-018-0055-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-018-0055-1
- Springer Nature Limited
This article is cited by
-
Sexuality in breast cancer survivors: sexual experiences, emotions, and cognitions in a group of women under hormonal therapy
Breast Cancer (2022)
-
Which psychosocial variables affect drive the most? Analysis of sexual desire in a group of Italian men
International Journal of Impotence Research (2019)