Abstract
This is the first of two papers outlining the orthodontic management of patients with cleft lip and palate. This paper will review orthodontic input into children with cleft lip and palate from birth to the late mixed dentition before definitive orthodontics. It will emphasise the importance of timing in alveolar bone grafting, the role of the general dental practitioner and the impact of timing on definitive orthodontic outcome.
Key points
To understand the orthodontic management of patients with cleft lip and palate.
To understand the importance of the multidisciplinary team within decision-making.
Dental health is imperative for good orthodontic outcomes.
Similar content being viewed by others
Introduction
The orthodontist is recognised as one of the key members of the team as part of the multidisciplinary approach to cleft care.1 They are often involved in several episodes of orthodontic intervention within a child's life and as with all specialities, it is incumbent upon them to evaluate outcomes of their interventions continually, longitudinally and those of other members of the team.
The purpose of this article is to review the orthodontic interventions required and the interactions with other members of the cleft team and the general dental practitioner. As previously mentioned, children with cleft palate and those with a cleft lip are completely different entities. Children with cleft palate have a higher incidence of dental anomalies than the general population2 and often present with crowding in both upper and lower arches. For the purposes of this and the second orthodontic article, we will focus on children with clefting involving the lip, alveolus and palate, as these children present with greatest variability of dental anomalies and most significant malocclusion and therefore require the greatest orthodontic input and challenges.3
Multiple courses of orthodontic intervention place a significant burden of care on patients and families. Semb et al.4 in their longitudinal cohort study looking at the duration of treatment for children with cleft lip and palate born between 1976 and 1979 found the overall length of orthodontic treatment ranged from 3-8.5 years with 49-94 visits for the centres studied. This has led more recently to progressively simplified orthodontic protocols within the UK, although a recent retrospective study from one centre found a mean duration of 3.4 years and on average, 44 appointments for all cleft types, with the longest duration for children with bilateral cleft lip and palate. Clearly, this represents a significantly longer duration and visit expectation compared to a non-cleft population, where 18 visits and 1.6 years' duration would be considered the norm.5 Reducing the orthodontic burden of care for these children and young adults will be a common theme throughout the article.
The orthodontic intervention will be divided into two papers based on chronology. Paper one will consider interventions from birth to the late mixed dentition, whereas paper two will concentrate on the adult dentition and the adult returner patient.
For the purposes of this article, we will concentrate on two areas:
Pre-surgical orthopaedics
Alveolar bone grafting.
Pre-surgical orthopaedics
Although when present, a cleft through the alveolus appears to produce an apparent defect when measuring the alveolar volume, a deficiency hardly exists when compared to non-cleft children.6 The apparent defect is caused by the displacement of the alveolar shelves (Fig. 1). Pre-surgical orthopaedics plates frequently used in conjunction with lip strapping/taping aim to normalise soft tissue and alveolar tissues. Lip taping or strapping produces tension across the cleft site to approximate the soft tissues and to some extent, retract the anterior alveolar segment which may be flared labially (Fig. 2).
Traditional pre-surgical or pre-operative orthopaedic appliances have been advocated for many years 7 but have fallen out of favour in most teams in the UK. There are, however, teams around the world where they are utilised.8,9 The appliances are acrylic plates that are used to obturate the cleft and passively or actively encourage closer approximation of the alveolar shelves before lip and palate closure. The plates are held in place by taping to the child's face and require frequent visits for adjustment and grinding (Fig. 3).
Perceived benefits of these plates include facilitation of feeding, guidance of maxillary segment growth and development, normalisation of tongue function, facilitation of surgery, better speech, and positive psychological benefit for the patients.6 The Dutchcleft Study, a randomised clinical trial, comparing passive plates with controls in children with unilateral cleft lip and palate, did not support these benefits up to the age of six and was shown to be not cost-effective.10,11 Later follow-up to the children at 12 years further supported the lack of benefit for transverse dimension.12 A similar conclusion for dental arch relationships has been found when utilised in children with bilateral cleft lip and palate. Bartzela et al.13 found in their retrospective longitudinal inter-centre outcome study that any small benefit obtained by infant orthopaedics in the short-term was not maintained at age nine.
In the early 1990s, Greyson and his colleagues modified the infant orthopaedic plate combining the traditional plate with nasal stents: the procedure they now term nasal alveolar moulding (NAM). The aim of NAM was to not only provide the 'benefit' of the plate but also manipulate the nasal cartilages to improve their anatomical form and aesthetics post lip closure.14
NAM comes with a significant burden of care than even compared to traditional infant orthopaedics when evaluating the number of visits required for fabrication and days worn.15 Systematic reviews and meta-analysis suggest that it may offer some aesthetic and symmetry advantages. However, no obvious dental arch development and midface growth benefits children with unilateral cleft lip and palate in the short-term.16,17 Studies evaluating NAM in the longer-term show limited impact over untreated controls in internal nasal form, including septal deviation.18 All reports however cite a lack of quality of evidence in their conclusions.
Alveolar bone grafting
Prior to the advent of alveolar bone grafting, children with a cleft involving the dental alveolus often had residual oronasal fistulae, nasal reflux, food impaction and chronic periodontal disease within the region which could ultimately lead to tooth loss. Because of the associated bony defect, orthodontics to align displaced teeth within the regions was limited and prosthetic options to replace the teeth that were absent were significantly hindered.
In the early 1970s, Boyne and Sands published reports on a new technique to repair an alveolar cleft utilising cancellous bone.19,20 They suggested the procedure should be undertaken in the mixed dentition before canine eruption (approximate age: 9-10 years). Modern optimisation of this treatment allows dental eruption within the region producing a continuous dental arch and has transformed the dental management and rehabilitation of children with cleft lip and palate.21
Timing
Timing of bone graft procedures can be broadly classified into two ranges: primary (<2 years of age) and secondary (5-11 years). Primary grafting has largely been discounted as a suitable timing in most centres around the world due to its impact of mid-facial growth.
Within the secondary grafting range, timing options advocated are 5-8 years before incisor eruption22,23 and 9-11 years before cleft-associated canine eruption.21,24,25
Irrespective of which age range for secondary grafting, the principle is to graft to the alveolus allowing permanent tooth eruption into the graft, which is critical for tooth periodontal health and graft survival.26,27,28
In the UK, the grafts are mostly carried out between the ages of 9-11 years. Proponents of grafting slightly earlier, at age 6-8 years, suggest better periodontal outcome for the central incisor adjacent to the cleft,22 without compromising facial growth29 or the quality of bone radiographically when compared to those grafted in the later mixed dentition.30 However, this is weighed against the maturity of the child and their ability to cope with orthodontic intervention when necessary. A recent systematic review, however, concluded it could be acceptable to graft slightly earlier, but the evidence was limited to change from the conventional gold standard of 9-11 years.31 Grafting at 9-11 years aims to provide adequate bone for eruption of the canine tooth associated with the cleft. When a suitable lateral incisor tooth, usually on the mesial side of the cleft, is present, a slightly earlier graft prior eruption is considered.21 This timing appears to minimally impact facial growth32,33,34 and radiographic success rates within the UK and centres around the world are excellent.30,35,36,37,38
Assessment
In order to facilitate pre-surgical dental/orthodontic intervention, bone graft assessment usually takes place between 7-8 years. This timing allows early enough evaluation should a viable lateral incisor, usually on the mesial to cleft, be present. If present, slightly earlier grafting is undertaken to encourage its eruption through the graft (Fig. 4). However, in most cases, timing is determined by the cleft-associated canine. This timing is critical to the outcome of the graft procedure, with a high success rate for those performed before canine eruption.24,32,39,40,41,42,43,44
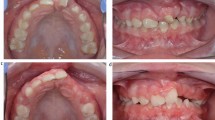
a) Orthopantomogram radiograph of a child with a unilateral cleft lip showing a well-formed lateral incisor on the mesial side of the cleft, offering the possibility of early bone graft. b) Intra-oral upper occlusal image of the child of the child showing a defect in the alveolus and a deciduous lateral incisor erupting on the mesial side of the defect. c) Intra-oral frontal image of the child of the child showing a defect in the alveolus and a deciduous lateral incisor erupting on the mesial side of the defect. d) Intra-oral upper occlusal image of the child of post bone-graft in the adult dentition showing eruption through the graft of the upper left lateral incisor. e) Intra-oral frontal image of the child of post bone-graft in the adult dentition showing eruption through the graft of the upper left lateral incisor
An orthopantomogram radiograph is usually taken for assessment and the teeth associated with the cleft site are evaluated for morphology, root development and proximity of the crown to the cleft region. Root formation of approximately ¼ to ½45 and close approximation to the cleft and imminent eruption26 are considered optimal for tooth eruption through the graft (Fig. 5). The advent of cone beam computed tomography (CT) allows a much greater visualisation of the cleft area. In practical terms, however, it offers little benefit to the surgeon, except where multiple teeth in the cleft site require locating prior removal, or where the extent of a partial cleft needs assessment and the two-dimensional plain radiograph will not provide this. Where a partial cleft exists, clinical signs can often give clues as to the extent of the cleft. Distal inclination and rotation of the incisor associated with the cleft, a notch on the palatal aspect and lack of support for the alar base on the cleft side are often tell-tale signs of a significant cleft existing (Fig. 6).
Pre-graft preparation
Dental health and tooth removal
A recent dental review should be completed before a bone graft assessment appointment. Oral health is considered critical for bone graft success and children should have no active dental disease before grafting.46 Poor oral hygiene is an important factor and graft infection leads to a greater incidence of graft failure.41 Issues should be dealt with pre-operatively through liaison with the local general dental practitioner and cleft dental team, including the specialist paediatric dentist where necessary.
Cleft involving the alveolus are associated with several dental anomalies, particularly hypoplasia of the adjacent central incisor (Fig. 7), which is in turn associated with dental caries and increased gingivitis.47,48 This again should be dealt with before graft placement.49
Deciduous teeth associated with the cleft site are, in many teams' protocols, removed pre-operatively to increase the amount of attached mucosa for flap construction during the procedure. This may also aid access to the cleft site, with or without orthodontic intervention at the time of grafting. Although these teeth can be removed at the time of the grafting procedure, there is a suggestion that this may lead to poorer bone graft radiological result.41 As well as deciduous tooth removal, the procedure may be combined under a short anaesthetic with supernumerary removal on the distal side of the cleft, which have been shown when present to be related to increased canine impaction.50 Where teeth are to be removed, particularly those closely associated with the cleft canine, this should be carried out approximately 3-6 months before the graft to encourage time for healing but not so distant as to encourage early canine eruption.
Pre-graft orthodontics
Although several authors suggest the indications of orthodontics pre-graft is to correct posterior crossbites,51,52,53 this is only appropriate where the skeletal pattern allows and requires long-term retention to maintain it increasing the burden of care for the patient.51
Rather than crossbite correction per se being the main indicator for orthodontic intervention, the primary reason should be to aid surgical access to the cleft site. Although some have suggested orthodontic intervention leads to better outcomes,54,55 it is not always essential to aid surgical access, particularly where deciduous teeth associated with the cleft have been removed. Therefore, where unnecessary to aid access, orthodontic intervention should be balanced against benefit for the patient.
Where orthodontics is necessary, many protocols involve an appliance to increase the maxillary arch in a transverse direction, for example a tri- or quad-helix. This has the impact where the segments are adjusted of increasing the size of the cleft pre-surgically which has been shown to negatively impact outcomes.30,56
Liao and Huang 54 suggest orthodontic input would be better focused on incisors impinging on the cleft site or expansion on a more anterior-posterior direction by proclining retroclined incisors (Fig. 8). The type of appliances used to produce this movement can be removable appliances, which can be removed post-operatively; sectional fixed appliances also don't impinge on the bone graft recipient site at the time of surgery.
a) Intra-oral maxillary occlusal image of a child with a unilateral cleft lip and palate at the time of bone graft assessment. b) Intra-oral right lateral image of a child with a unilateral cleft lip and palate at the time of bone graft assessment showing both central incisors in crossbite and a unilateral crossbite. c) aIntra-oral frontal image of a child with a unilateral cleft lip and palate at the time of bone graft assessment showing both central incisors in crossbite and a unilateral crossbite. d) Intra-oral right lateral image of a child with a unilateral cleft lip and palate after pre bone graft orthodontic input to procline the upper central incisors and extraction of the upper right deciduous canine. e) Intra-oral right lateral image of a child with a unilateral cleft lip and palate after pre bone graft orthodontic input to procline the upper central incisors and extraction of the upper right deciduous canine. f) Intra-oral frontal image of a child with a unilateral cleft lip and palate after pre bone graft orthodontic input to procline the upper central incisors and extraction of the upper right deciduous canine. g) Intra-oral maxillary occlusal image of a child with a unilateral cleft lip and palate post bone graft with eruption of the upper right canine through the graft. h) Intra-oral right lateral image of a child with a unilateral cleft lip and palate post bone graft with eruption of the upper right canine through the graft. i) Intra-oral frontal image of a child with a unilateral cleft lip and palate post bone graft with eruption of the upper right canine through the graft. j) Intra-oral maxillary occlusal image of a child with a unilateral cleft lip and palate orthodontic treatment with space closure and correction of the unilateral crossbite. k) Intra-oral right lateral image of a child with a unilateral cleft lip and palate orthodontic treatment with space closure and correction of the unilateral crossbite. l) Intra-oral frontal image of a child with a unilateral cleft lip and palate orthodontic treatment with space closure and correction of the unilateral crossbite
Although not always necessary for a unilateral cleft, there is less debate over whether orthodontics is necessary for a bilateral cleft. This is because, not only do the tooth positions impinge on good access to the cleft site for the surgeons, but the premaxilla carrying the central incisor teeth is often mobile, requiring stabilisation in the post-operative period. From an orthodontic perspective, the premaxilla itself can be frequently displaced, creating a significant centreline shift, which can be extremely challenging to correct post bone graft if it is not corrected pre-graft (Fig. 9).
a) Intra-oral maxillary occlusal image of a child with a bilateral cleft lip and palate at the time of bone graft assessment. There is displacement of the premaxillary segment to the patients left. b) Intra-oral frontal image of a child with a bilateral cleft lip and palate at the time of bone graft assessment. There is displacement of the premaxillary segment to the patients left. c) Intra-oral maxillary occlusal image of a child with a bilateral cleft lip and palate after orthodontic intervention. A fixed appliance including Glasgow Anterior Stabilisation (GAS) (two orthodontic bands in both central incisors, connected together and a self-ligating orthodontic tube soldered to the connector, to allow archwire engagement) on the pre-maxillary segment has been utilised to stabilise the premaxilla and correct the premaxillary displacement. Deciduous teeth around the cleft site have been extracted. d) Intra-oral frontal image of a child with a bilateral cleft lip and palate after orthodontic intervention. A fixed appliance including GAS on the premaxillary segment has been utilised to stabilise the premaxilla and correct the premaxillary displacement. Deciduous teeth around the cleft site have been extracted. e) Intra-oral maxillary occlusal image of a child with bilateral cleft lip and palate post bone graft and removal of the fixed appliance. f) Intra-oral frontal image of a child with bilateral cleft lip and palate post bone graft and removal of the fixed appliance. g) Intra-oral maxillary occlusal image of a child with bilateral cleft lip and palate post-bone graft and eruption of both maxillary canines through the bone graft site. h) Intra-oral maxillary occlusal image of a child with bilateral cleft lip and palate post bone graft and eruption of both maxillary canines through the bone graft site
When the premaxilla is mobile and displaced it can be stabilised by utilising fixed appliances. Care must be taken particularly on the anterior teeth when placing the appliances, as little bone often exists on the distal side of the central incisors, meaning any adverse distal movement of the roots of the incisor teeth can result in fenestration, resorption, and in some cases, loss of vitality. To reduce this occurrence, the brackets on the incisor teeth are placed in such a way to prevent this. Alternatively, some have advocated other anterior appliances that avoid tooth movement all together and simply link the anterior teeth together in their pre-surgical positions57 (Fig. 9).
For relatively young children, any form of fixed appliance can be challenging, and it is the orthodontist's responsibility to limit this intervention to a minimum while also being mindful of the ideal timing for the graft. To this effect, these appliances are often started a year or so before the optimal timing for grafting. To stabilise the graft, there is often a thick stabilising wire running across the site and therefore, there is a need for liaison within the team between surgeon and orthodontist to make sure this is removed at the time of surgery and replaced immediately post-op to allow the stabilisation during the healing phase while still allowing access to the cleft site for the surgeon.
The appliance is often maintained for a number of months post-surgery to allow bony healing. However, this should be balanced against its impact on oral hygiene, maintenance and orthodontic treatment burden when further definitive orthodontic care will be required a few years later.
Bone graft outcome assessment
Traditionally, outcomes for alveolar bone grafting are assessed through plain radiographic examination. Studies comparing outcomes where bone grafting is performed can be subdivided into those that look at approximately six months post graft42,58 and those that look following tooth eruption through the graft.24,32,46,59,60 In both time periods, the outcomes for graft bone height/cleft bone infiltration are superior when grafting occurs before canine eruption.61
Three-dimensional radiographic assessment using CT suggests that the bone grafts are almost completely lost in the short- to mid-term unless the canine or lateral incisor tooth, if present, erupts through the graft or is moved orthodontically into the graft to close the space anteriorly (Fig. 8).27,61 This requirement for graft survival is also found at ten years62,63 and 20 years post graft.64
The primary objective of grafting is to allow tooth eruption, most notably, the cleft canine and definitive orthodontic intervention.21 Although short-term (six month) radiographic follow-up and outcome is important, it doesn't appear to necessarily relate to the cleft canine tooth eruption. The canine tooth associated with the alveolar cleft has a delayed root formation compared to the general population,65,66 although grafting before its eruption has been found to accelerate root development.66 Despite this, the cleft canine still has a delayed eruption compared to the population norm.66,67
The cleft canine also has an increased incidence of impaction,21,68,69 particularly in unilateral rather than bilateral clefts.43,45 As with any canine impaction, the tooth may require further surgery to expose it, prolong orthodontic treatment and add to the overall orthodontic burden of care. This will be discussed in part two of this paper which will review the orthodontic and retention challenges following development of the adult dentition. It will also discuss orthodontics for the returning adult and orthodontics for orthognathic surgery.
Conclusion
This paper (part one of two) has highlighted the orthodontic input into a child with cleft lip and palate from birth to the late mixed dentition. It has emphasised the importance of timing and planning in relation to alveolar bone grafting and its ultimate impact on definitive orthodontic outcome.
References
Shaw W C, Williams A C, Sandy J R, Devlin H B. Minimum standards for the management of cleft lip and palate: efforts to close the audit loop. Royal College of Surgeons of England. Ann R Coll Surg Engl 1996; 78: 110-114.
Ranta R. A review of tooth formation in children with cleft lip/palate. Am J Orthod Dentofacial Orthop 1986; 90: 11-18.
Baek S-H, Moon H-S, Yang W-S. Cleft type and Angle's classification of malocclusion in Korean cleft patients. Eur J Orthod 2002; 24: 647-653.
Semb G, Brattström V, Mølsted K, Prahl-Andersen B, Shaw W C. The Eurocleft study: intercenter study of treatment outcome in patients with complete cleft lip and palate. Part 1: introduction and treatment experience. Cleft Palate Craniofac J 2005; 42: 64-68.
Tsichlaki A, Chin S Y, Pandis N, Fleming P S. How long does treatment with fixed orthodontic appliances last? A systematic review. Am J Orthod Dentofacial Orthop 2016; 149: 308-318.
Prahl-Andersen B. Dental treatment of predental and infant patients with clefts and craniofacial anomalies Cleft Palate Craniofac J 2000; 37: 528-532.
McNeil C K. Congenital cleft palate; a case of congenital cleft palate that required the fitting of a special appliance. Br Dent J 1948; 84: 137-141.
Bongaarts C A, Kuijpers-Jagtman A M, van't Hof M A, Prahl-Andersen B. The effect of infant orthopedics on the occlusion of the deciduous dentition in children with complete unilateral cleft lip and palate (Dutchcleft). Cleft Palate Craniofac J 2004; 41: 633-641.
Meazzini M C, Capasso E, Morabito A, Garattini G, Brusati R. Comparison of growth results in patients with unilateral cleft lip and palate after early secondary gingivoalveoloplasty and secondary bone grafting: 20 years follow up. Scand J Plast Reconstr Surg Hand Surg 2008; 42: 290-295.
Bongaarts C A, van't Hof M A, Prahl-Andersen B, Dirks I V, Kuijpers-Jagtman A M. Infant orthopedics has no effect on maxillary arch dimensions in the deciduous dentition of children with complete unilateral cleft lip and palate (Dutchcleft) Cleft Palate Craniofac J 2006; 43: 665-672.
Bongaarts C A, Prahl-Andersen B, Bronkhorst E M et al. Infant orthopedics and facial growth in complete unilateral cleft lip and palate until six years of age (Dutchcleft). Cleft Palate Craniofac J 2009; 46: 654-663.
Noverraz R L, Disse M A, Ongkosuwito E M, Kuijpers-Jagtman A M, Prahl C. Transverse dental arch relationship at 9 and 12 years in children with unilateral cleft lip and palate treated with infant orthopedics: a randomized clinical trial (DUTCHCLEFT). Clin Oral Investig 2015; 19: 2255-2265.
Bartzela T, Katsaros C, Shaw W C et al. A longitudinal three-centre study of dental arch relationship in patients with bilateral cleft lip and palate. Cleft Palate Craniofac J 2010; 47: 167-174.
Greyson B H, Cutting C, Wood R. Preoperative columella lengthening in bilateral cleft lip and palate. Plast Reconstr Surg 1993; 92: 1422-1423.
Singer E, Daskalogiannakis J, Russell K A et al. Burden of Care of Various Infant Orthopedic Protocols for Improvement of Nasolabial Esthetics in Patients With CUCLP. Cleft Palate Craniofac J 2018; 55: 1236-1243.
Van der Heijden P, Dijkstra P U, Stellingsma C, van der Laan B F, Korsten-Meijer A G, Goorhuis-Brouwer S M. Limited evidence for the effect of presurgical nasoalveolar molding in unilateral cleft on nasal symmetry: a call for unified research. Plast Reconstr Surg 2013; 131: 62-71.
Padovano W M, Skolnick G B, Naidoo S D, Snyder-Warwick A K, Patel K B. Long-Term Effects of Nasoalveolar Molding in Patients With Unilateral Cleft Lip and Palate: A Systematic Review and Meta-Analysis. Cleft Palate Craniofac J 2022; 59: 462-474.
Massie J P, Bruckman K, Rifkin W J et al. The Effect of Nasoalveolar Molding on Nasal Airway Anatomy: A 9-Year Follow-up of Patients with Unilateral Cleft Lip and Palate. Cleft Palate Craniofac J 2018; 55: 596-601.
Boyne P J, Sands N R. Secondary bone grafting of residual alveolar and palatal clefts. J Oral Surg 1972; 30: 87-92.
Boyne P J, Sands N R. Combined orthodontic-surgical management of residual palato-alveolar cleft defects. Am J Orthod 1976; 70: 20-37.
Semb G. Alveolar bone grafting. Front Oral Biol 2012; 16: 124-136.
Precious D S. A new reliable method for alveolar bone grafting at about 6 years of age. J Oral Maxillofac Surg 2009; 67: 2045-2053.
Mundra L S, Lowe K M, Khechoyan D Y. Alveolar Bone Graft Timing in Patients With Cleft Lip & Palate. J Craniofac Surg 2022; 33: 206-210.
Bergland O, Semb G, Abyholm F E. Elimination of the residual alveolar cleft by secondary bone grafting and subsequent orthodontic treatment. Cleft Palate J 1986; 23: 175-205.
Schultze-Mosgau S, Nkenke E, Schlegel A K, Hirschfelder U, Wiltfang J. Analysis of bone resorption after secondary alveolar cleft bone grafts before and after canine eruption in connection with orthodontic gap closure or prosthodontic treatment. J Oral Maxillofac Surg 2003; 61: 1245-1248.
Ozawa T, Omura S, Fukuyama E, Matsui Y, Torikai K, Fujita K. Factors influencing secondary alveolar bone grafting in cleft lip and palate patients: prospective analysis using CT image analyzer. Cleft Palate Craniofac J 2007; 44: 286-291.
Feichtinger M, Mossböck R, Kärcher H. Assessment of bone resorption after secondary alveolar bone grafting using three-dimensional computed tomography: a three-year study. Cleft Palate Craniofac J 2007; 44: 142-148.
Dissaux C, Bodin F, Grollemund B et al. Evaluation of success of alveolar cleft bone graft performed at 5 years versus 10 years of age. J Craniomaxillofac Surg 2016; 44: 21-26.
Doucet J-C, Russell K A, Daskalogiannakis J et al. Facial Growth of Patients With Complete Unilateral Cleft Lip and Palate Treated With Alveolar Bone Grafting at 6 Years. Cleft Palate Craniofac J 2019; 56: 619-627.
Ruppel J K, Long R E Jr, Oliver D R et al. The Americleft Project: A Comparison of Short- and Longer-Term Secondary Alveolar Bone Graft Outcomes in Two Centres Using the Standardized Way to Assess Grafts Scale. Cleft Palate Craniofac J 2016; 53: 508-515.
Pinheiro F H, Drummond R J, Frota C M, Bartzela T N, Dos Santos P B. Comparison of early and conventional autogenous secondary alveolar bone graft in children with cleft lip and palate: A systematic review. Orthod Craniofac Res 2020; 23: 385-397.
Enemark H, Sindet-Paedersen S, Bundgaard M. Long-term results after secondary bone grafting of alveolar clefts. J Oral Maxillofac Surg 1987; 45: 913-919.
Semb G. Effect of alveolar bone grafting on maxillary growth in unilateral cleft lip and palate patients. Cleft Palate J 1988; 25: 288-295.
Levitt T, Long R E Jr, Trotman C A. Maxillary growth in patients with clefts following secondary alveolar bone grafting. Cleft Palate Craniofac J 1999; 36: 398-406.
Shaw W C, Semb G, Nelson P et al. The Eurocleft project 1996-2000: overview. J Craniomaxillofac Surg 2001; 29: 131-142.
Murthy A S, Lehman J A. Evaluation of alveolar bone grafting: a survey of ACPA teams. Cleft Palate Craniofac J 2005; 42: 99-101.
Revington P J, McNamara C, Mukarram S, Perera E, Shah H V, Deacon S A. Alveolar bone grafting: results of a national outcome study. Ann R Coll Surg Engl 2010; 92: 643-646.
Paterson M, Rae J, Paterson P, Gilgrass T, Devlin M, McIntyre G. Secondary Alveolar Bone Grafting (CLEFTSiS) 2007-2010. Cleft Palate Craniofac J 2016; 53: 141-146.
Abyholm F E, Bergland O, Semb G. Secondary bone grafting of alveolar clefts. A surgical/orthodontic treatment enabling a non-prosthodontic rehabilitation in cleft lip and palate patients. Scand J Plast Reconstr Surg 1981; 15: 127-140.
Turvey T A, Vig K, Moriarty J, Hoke J. Delayed bone grafting in the cleft maxilla and palate: a retrospective multidisciplinary analysis. Am J Orthod 1984; 86: 244-256.
Lilja J, Möller M, Friede H, Lauritzen C, Petterson L E, Johanson B. Bone grafting at the stage of mixed dentition in cleft lip and palate patients. Scand J Plast Reconstr Surg Hand Surg 1987; 21: 73-79.
Paulin G, Astrand P, Rosenquist J B, Bartholdson L. Intermediate bone grafting of alveolar clefts. J Craniomaxillofac Surg 1988; 16: 2-7.
Enemark H, Jensen J, Bosch C. Mandibular bone graft material for reconstruction of alveolar cleft defects: long-term results. Cleft Palate Craniofac J 2001; 38: 155-163.
Trindade I K, Mazzottini R, Silva Filho O G, Trindade I E, Deboni M C. Long-term radiographic assessment of secondary alveolar bone grafting outcomes in patients with alveolar clefts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005; 100: 271-277.
El Deeb M, Messer L B, Lehnert M W, Hebda T W, Waite D E. Canine eruption into grafted bone in maxillary alveolar cleft defects. Cleft Palate J 1982; 19: 9-16.
Jia Y L, Fu M K, Ma L. Long-term outcome of secondary alveolar bone grafting in patients with various types of cleft. Br J Oral Maxillofac Surg 2006; 44: 308-312.
Ellwood R P, O'Mullane D M. Association between dental enamel opacities and dental caries in a north Wales population. Caries Res 1994; 28: 383-387.
Malanczuk T, Opitz C, Retzlaff R. Structural changes of dental enamel in both dentitions of cleft lip and palate patients. J Orofac Orthop 1999; 60: 259-268.
Samman N, Cheung L K, Tideman H. A comparison of alveolar bone grafting with and without simultaneous maxillary osteotomies in cleft palate patients. Int J Oral Maxillofac Surg 1994; 23: 65-70.
Vellone V, Cirignaco G, Cavarretta B, Cascone P. Canine Eruption After Secondary Alveolar Bone Graft in Unilateral Cleft Lip and Palate Patients. J Craniofac Surg 2017; 28: 1206-1210.
Freitas J A, Garib D G, Oliveira M et al. Rehabilitative treatment of cleft lip and palate: experience of the Hospital for Rehabilitation of Craniofacial Anomalies-USP (HRAC-USP)-part 2: paediatric dentistry and orthodontics. J Appl Oral Sci 2012; 20: 268-281.
Allareddy V, Bruun R, MacLaine J, Markiewicz M R, Ruiz R, Miller M A. Orthodontic Preparation for Secondary Alveolar Bone Grafting in Patients with Complete Cleft Lip and Palate. Oral Maxillofac Surg Clin North Am 2020; 32: 205-217.
Parsaei Y, Uribe F, Steinbacher D. Orthodontics for Unilateral and Bilateral Cleft Deformities. Oral Maxillofac Surg Clin North Am 2020; 32: 297-307.
Liao Y-F, Huang C-S. Presurgical and postsurgical orthodontics are associated with superior secondary alveolar bone grafting outcomes. J Craniomaxillofac Surg 2015; 43: 717-723.
Chang L, Wang Y, Liu H. Evaluation of the timing of orthodontic arch expansion and graft in cleft lip and palate. Hua Xi Kou Qiang Yi Xue Za Zhi 2016; 34: 205-209.
Long R E Jr, Spangler B E, Yow M. Cleft width and secondary alveolar bone graft success. Cleft Palate Craniofac J 1995; 32: 420-427.
Vuity D, Biddlestone J, Paterson P, Russell C, Devlin M, Gillgrass T. The Glasgow Anterior Stabilisation (GAS) appliance: A novel orthodontic appliance for pre-maxillary stabilisation in bilateral cleft lip and palate. J Plast Reconstr Aesthet Surg 2017; 70: 540-542.
Sindet-Paedersen S, Enemark H. Reconstruction of alveolar clefts with mandibular or iliac crest bone grafts: a comparative study. J Oral Maxillofac Surg 1990; 48: 554-560.
Amanat N, Langdon J D. Secondary alveolar bone grafting in clefts of the lip and palate. J Craniomaxillofac Surg 1991; 19: 7-14.
Kalaaji A, Lilja J, Friede H, Elander A. Bone grafting in the mixed and permanent dentition in cleft lip and palatepatients: long-term results and the role of the surgeon's experience. J Craniomaxillofac Surg 1996; 24: 29-35.
Dado D V, Rosenstein S W, Alder M E, Kernahan D A. Long-term assessment of early alveolar bone grafts using three-dimensional computer-assisted tomography: a pilot study. Plast Reconstr Surg 1997; 99: 1840-1845.
Jabbari F, Skoog V, Reiser E, Hakelius M, Nowinski D. Optimization of dental status improves long-term outcome after alveolar bone grafting in unilateral cleft lip and palate. Cleft Palate Craniofac J 2015; 52: 210-218.
Meyer S, Mølsted K. Long-term outcome of secondary alveolar bone grafting in cleft lip and palate patients: a 10-year follow-up cohort study. J Plast Surg Hand Surg 2013; 47: 503-508.
Jabbari F, Wiklander L, Reiser E, Thor A, Hakelius M, Nowinski D. Secondary Alveolar Bone Grafting in Patients Born With Unilateral Cleft Lip and Palate: A 20-Year Follow-up. Cleft Palate Craniofac J 2018; 55: 173-179.
Park H-M, Han D-H, Baek S-H. Comparison of tooth development stage of the maxillary anterior teeth before and after secondary alveolar bone graft: Unilateral cleft lip and alveolus vs unilateral cleft lip and palate. Angle Orthod 2014; 84: 989-994.
Vandersluis Y R, Fisher D M, Stevens K, Tompson B D, Lou W, Suri S. Comparison of dental outcomes in patients with nonsyndromic complete unilateral cleft lip and palate who receive secondary alveolar bone grafting before or after emergence of the permanent maxillary canine. Am J Orthod Dentofacial Orthop 2020; 157: 668-679.
Solis A, Figueroa A A, Cohen M, Polley J W, Evans C A. Maxillary dental development in complete unilateral alveolar clefts. Cleft Palate Craniofac J 1998; 35: 320-328.
Russell K A, McLeod C E. Canine eruption in patients with complete cleft lip and palate. Cleft Palate Craniofac J 2008; 45: 73-80.
Tortora C, Meazzini M C, Garattini G, Brusati R. Prevalence of abnormalities in dental structure, position, and eruption pattern in a population of unilateral and bilateral cleft lip and palate patients. Cleft Palate Craniofac J 2008; 45: 154-162.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The author declares no conflicts of interest.
Written consent to publish has been obtained for Figures 1 and 2.
Rights and permissions
About this article
Cite this article
Gillgrass, T. The orthodontic management of patients with cleft lip and palate: from birth to the late mixed dentition. Br Dent J 234, 873–880 (2023). https://doi.org/10.1038/s41415-023-5955-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41415-023-5955-x
- Springer Nature Limited
This article is cited by
-
NAM in cleft care - boon or bane
British Dental Journal (2023)