Abstract
Podocyte lipotoxicity mediated by impaired cellular cholesterol efflux plays a crucial role in the development of diabetic kidney disease (DKD), and the identification of potential therapeutic targets that regulate podocyte cholesterol homeostasis has clinical significance. Coiled-coil domain containing 92 (CCDC92) is a novel molecule related to metabolic disorders and insulin resistance. However, whether the expression level of CCDC92 is changed in kidney parenchymal cells and the role of CCDC92 in podocytes remain unclear. In this study, we found that Ccdc92 was significantly induced in glomeruli from type 2 diabetic mice, especially in podocytes. Importantly, upregulation of Ccdc92 in glomeruli was positively correlated with an increased urine albumin-to-creatinine ratio (UACR) and podocyte loss. Functionally, podocyte-specific deletion of Ccdc92 attenuated proteinuria, glomerular expansion and podocyte injury in mice with DKD. We further demonstrated that Ccdc92 contributed to lipid accumulation by inhibiting cholesterol efflux, finally promoting podocyte injury. Mechanistically, Ccdc92 promoted the degradation of ABCA1 by regulating PA28α-mediated proteasome activity and then reduced cholesterol efflux. Thus, our studies indicate that Ccdc92 contributes to podocyte injury by regulating the PA28α/ABCA1/cholesterol efflux axis in DKD.
Similar content being viewed by others
Introduction
Diabetic kidney disease (DKD), a major complication of diabetes, has been considered as the leading cause of end-stage renal disease (ESRD) [1]. An increasing number of studies have suggested that dysregulation of lipid metabolism in the kidney is a major determinant of DKD [2]. Although accumulation of lipids occurs in podocytes, mesangial cells and proximal tubule epithelial cells, different renal parenchymal cells show different sensitivities to lipid accumulation in DKD [3]. Notably, podocytes are especially sensitive to lipotoxic injury, causing insulin resistance and cell death [3]. Lipid metabolism in podocytes is a dynamic process, including lipid synthesis, uptake, oxidation, lipolysis and efflux [4, 5]. Recent studies indicate that impaired cellular cholesterol efflux plays a crucial role in the pathogenesis of podocytes [6,7,8]. Improving cholesterol efflux attenuates podocyte injury in glomerular disease [6]. Therefore, the identification of potential therapeutic targets that alter podocyte cholesterol efflux is of importance in DKD.
Coiled-coil domain containing 92 (CCDC92), also known as Limkain Beta 2 and FLJ22471, has been reported to be associated with obesity, type 2 diabetes (T2D), and coronary artery disease [9,10,11,12]. A very recent study demonstrated that Ccdc92 knockout reduced obesity and increased insulin sensitivity under high-fat diet (HFD) conditions. Through the generation of Ccdc92 knockout mice, the researchers mainly addressed the importance of CCDC92 in adipocyte differentiation and inflammation-mediated insulin resistance [13], and their results suggested that CCDC92 may be a key factor in metabolic disorders. However, the roles and exact mechanisms of CCDC92 in lipid metabolism and related diseases, especially diabetic kidney disease, are still unclear.
In this study, we found that CCDC92 was induced in podocytes from type 2 diabetic mice. Ccdc92 deficiency in podocytes reduced lipid accumulation by increasing cholesterol efflux. Mechanistically, Ccdc92 promoted the degradation of ATP-binding cassette transporter 1 (ABCA1) by regulating PA28α-mediated proteasome activity, finally leading to the inhibition of cholesterol efflux in podocytes. Our findings suggest that Ccdc92 contributes to podocyte injury by regulating the PA28α/ABCA1/cholesterol efflux axis in DKD.
Materials and methods
Details of the methods are provided in the supplementary complete materials and methods section.
Establishment of podocyte-specific Ccdc92 knockout mice
Ccdc92flox/+ (Ccdc92fl/+) mice (C57BL/6 J) were provided by Shanghai Model Organisms Center, Inc. (Shanghai, China) and were crossed with mice expressing Cre recombinase (Cre) under the control of the podocin promoter (B6.Cg-Tg[NPHS2-cre]295Lbh/J; The Jackson Laboratory) to generate mice with podocyte-specific Ccdc92 knockout mice (Podocin-Cre/Ccdc92fl/fl; Cre+/Ccdc92fl/fl).
Spontaneous type 2 diabetic db/db (BKS) mice
Heterozygous BKS db/m mice (BKS.Cg-Dock7m +/+Leprdb/J, Stock No. 000642) and homozygous BKS db/db mice (B6.BKS(D)-Leprdb/J, Stock No.000697) were purchased from The Jackson Laboratory.
Generation of podocyte-specific Ccdc92 knockout mice with spontaneous type 2 diabetes
Mice with podocyte-specific Ccdc92 deletion mice (Cre+/Ccdc92fl/fl) were crossed with db/+ mice to generate db/+//Cre+/Ccdc92fl/+ mice, which were crossed with db/+//Cre-/Ccdc92fl/+ mice to obtain db/+//Cre+/Ccdc92fl/fl and db/+//Cre-/Ccdc92fl/fl mice. Then, db/+//Cre+/Ccdc92fl/fl mice were crossed with db/+//Cre-/Ccdc92fl/fl mice to generate podocyte-specific Ccdc92 knockout mice with spontaneous type 2 diabetes (db/db//Cre+/Ccdc92fl/fl). In addition, db/db//Cre-/Ccdc92fl/fl mice were used as controls.
Establishment of HFD-induced DKD in mice
Six-week-old male Cre+/Ccdc92fl/fl mice and their littermate Cre-/Ccdc92fl/fl mice were fed either a high-fat diet (HFD; 60 kcal% from fat, Research Diets, D12492) or a control diet (Research Diets, D12450J) for 32 weeks.
Statistical analysis
Data are expressed as mean ± SEM. Statistical analyses were performed with GraphPad Prism (version 8.0, GraphPad Software, San Diego, CA). Details of the statistical analyses can be found in the supplementary complete materials and methods section.
Results
Ccdc92 was involved in podocyte injury under diabetic conditions
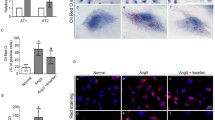
In this study, we found that Ccdc92 was significantly upregulated in the kidneys of db/db mice and high-fat diet (HFD)-induced diabetic mice (Fig. 1a, b). Importantly, the expression of Ccdc92 in glomeruli was positively correlated with the urine albumin-to-creatinine ratio (UACR) (Fig. 1c), suggesting that CCDC92 might be related to glomerular injury in DKD. Immunofluorescence (IF) staining further showed that Ccdc92 was expressed in glomerular cells and significantly upregulated in podocytes from diabetic mice (Fig. 1d, Supplementary Fig. S1a), but there was no obvious change of Ccdc92 expression in endothelial cells or mesangial cells from db/db mice (Supplementary Fig. S1b). Moreover, the expression of Ccdc92 in glomeruli was negatively correlated with the podocyte number in diabetic mice (Fig. 1e, f). In vitro, Ccdc92 was significantly induced in mouse podocytes exposed to high glucose (HG; Fig. 1g), advanced glycation end products (AGE; Fig. 1h), or cholesterol (Fig. 1i), but there were no obvious changes of Ccdc92 expression in HG-treated mouse glomerular endothelial cells (MGECs) or mouse mesangial cells (SV40 MES 13) (Fig. 1j, k). Moreover, we further confirmed the upregulation of Ccdc92 in glomeruli, especially in podocytes, from DKD patients (Fig. 1l, Supplementary Table S1).
a Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in the cortex of kidney from db/db mice (n = 8 for each group). ***P < 0.001 vs. control mice. b Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in the cortex of kidney from HFD-induced diabetic mice (n = 8 for each group). ***P < 0.001 vs. control mice. c Correlation between glomerular Ccdc92 expression and urine albumin to creatinine ratio (UACR) in all subjects (n = 16). d Statistical analyses of Ccdc92 in glomeruli from db/db and HFD induced diabetic mice detected by IHC (n = 8 for each group). ***P < 0.001 vs. control mice. e Photomicrographs and quantifications showing the staining of Wilms’ Tumer 1 (WT1, used as a podocyte marker) in the kidney from db/db or HFD induced diabetic mice (n = 8 for each group). ***P < 0.001 vs. control mice. f Correlation between glomerular Ccdc92 expression and WT-1 in all animals (n = 16). g Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in mouse podocytes treated with high glucose (HG, 15 or 30 mmol/L) for 24 h (n = 6 for each group). Mannitol was used as the osmotic pressure control for HG. ***P < 0.001 vs. control. h Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in podocytes treated with advanced glycation end-product (AGE, 50-200 μg/mL) for 24 h (n = 6 for each group). ***P < 0.001 vs. control. i Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in podocytes treated with cholesterol (100-400 μg/mL) for 24 h (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. control. j Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in mouse glomerular endothelial cells (MGEC) treated with high glucose (HG, 15 or 30 mmol/L) for 24 h (n = 6 for each group). Mannitol was used as the osmotic pressure control for HG. k Representative Western blot gel documents and summarized data showing the relative protein levels of Ccdc92 in mouse mesangial cells (SV40 MES 13) treated with high glucose (HG, 15 or 30 mmol/L) for 24 h (n = 6 for each group). Mannitol was used as the osmotic pressure control for HG. l Representative immunohistochemistry (IHC) and immunofluorescence (IF) images and quantification of glomerular Ccdc92 expression (based on IHC) from normal subjects (n = 12) and patients with DKD (n = 8). Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-tailed Student’s unpaired t test analysis (a, b, d–e), one-way ANOVA followed by Tukey’s post-test (g–k), Spearman’s correlations (c, f), Kruskal-Wallis test followed by Dunn’s post-test (l).
Ccdc92 deficiency attenuated podocyte injury in DKD
To better elucidate the role of Ccdc92 in podocyte injury, mice with podocyte-specific deletion of Ccdc92 (Podocin-Cre Ccdc92fl/fl; Cre+/Ccdc92fl/fl) were generated by the Cre-Loxp recombination system (Supplementary Fig. S2a), which were confirmed by tail genotyping (Supplementary Fig. S2b), immunofluorescent staining (Supplementary Fig. S2c) and reduction of Ccdc92 in isolated glomeruli (Supplementary Fig. S2d). All mice were viable and fertile. To establish diabetic mice, Cre+/Ccdc92fl/fl mice were crossed with db/+ mice, and the resulting db/db/Cre+/Ccdc92fl/fl mice and the corresponding control mice were used in this study (Supplementary Fig. S2e). db/+/Cre+/Ccdc92fl/fl mice did not show any physiological changes, including changes in body weight, kidney weight, heart rate, blood pressure, and glucose level (Supplementary Table S2). However, our results showed that 20-week-old db/db/Cre-/Ccdc92fl/fl mice exhibited a significant increase in urinary albumin excretion (Fig. 2a), glomerular expansion (Fig. 2b) and podocyte injury (Fig. 2c), as evidenced by glomerular basement membrane (GBM) thickening and podocyte foot process broadening and effacement, which were reversed by podocyte-specific deletion of Ccdc92 (db/db/Cre+/Ccdc92fl/fl). We further demonstrated that Ccdc92 deficiency attenuated podocyte injury in db/db mice, based on the upregulation of key podocyte differentiation markers, such as nephrin and podocin (Fig. 2d). Notably, conditional knockout of Ccdc92 in podocytes significantly reduced podocyte loss in db/db mice (Fig. 2e). In addition, we confirmed the detrimental role of Ccdc92 in HFD-induced diabetic mice and found that podocyte-specific deletion of Ccdc92 alleviated albuminuria, glomerulosclerosis and podocyte injury (Supplementary Fig. S3a-e, Supplementary Table S2).
a Urinary albumin creatinine ratio in different groups of mice at 20-week ages (n = 8 for each group). **P < 0.01, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. b Morphological examinations of glomerular changes by periodic acid–schiff (PAS) analyses in mice (n = 8 for each group). ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. c Morphological examinations of glomerular changes by transmission electron microscopy (TEM) analysis in mice (n = 8 for each group). **P < 0.01, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. d Representative immunofluorescence (IF) images showing the expressions of nephrin and podocin in glomeruli from mice (n = 8 for each group). *P < 0.05, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. e Representative IF imaging and quantifications of Wilms’ Tumer 1 (WT-1) (green) per glomerulus in the kidney (n = 8 for each group). *P < 0.05, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ##P < 0.01 vs. db/db//Cre-/Ccdc92fl/fl mice. Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-way ANOVA followed by Tukey’s post-test (a–e).
In vitro, genetic silencing of Ccdc92 (Fig. 3a) attenuated actin cytoskeleton disorganization (Fig. 3b) and apoptosis (Fig. 3c, d) and upregulated nephrin and podocin expression (Fig. 3e, f) in podocytes exposed to HG.
a Representative Western blot gel documents and summarized data showing the gene silencing efficiency of Ccdc92 by a Ccdc92-siRNA transfection in podocytes (n = 6 for each group). ***P < 0.001 vs. scramble (si-NC). b Representative immunofluorescence (IF) images of F-actin by phalloidine staining (n = 6 for each group) in podocytes with different treatments. **P < 0.01, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. c Flow cytometry analysis to evaluate the role of Ccdc92 on the regulation of apoptosis (n = 6 for each group). **P < 0.01, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. d Representative Western blot gel documents and summarized data showing the relative protein levels of cleaved-poly-ADP-ribose polymerase1 (PARP1) in podocytes with different treatments (n = 6 for each group). ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. e Representative Western blot gel documents and summarized data showing the relative protein levels of nephrin in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. f Representative Western blot gel documents and summarized data showing the relative protein levels of podocin in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. g Photomicrographs and quantifications showing Nile Red staining in podocytes from different groups (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. h Representative images and quantifications showing lipid deposition by immunofluorescence staining of adipophilin (green) and synaptopodin (red) in kidney from mice (n = 8 for each group). **P < 0.01, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-tailed Student’s unpaired t test analysis (a), Two-way ANOVA followed by Tukey’s post-test (b–h).
Ccdc92 contributed to podocyte lipotoxicity by inhibiting ABCA1-mediated cholesterol efflux
Lipid accumulation was increased in podocytes exposed to HG, based on Nile red staining (Fig. 3g), which was reversed by Ccdc92 knockdown. In vivo, podocyte-specific deletion of Ccdc92 reduced the expression of adipophilin, a lipid droplet-specific marker [14], in podocytes from both db/db mice (Fig. 3h) and HFD-induced diabetic mice (Supplementary Fig. S3f), suggesting that Ccdc92 is involved in lipid metabolism of podocyte under DKD.
To explore the role of CCDC92 in lipid metabolism of podocyte, we performed lipidomic analysis and found that CCDC92 was mainly involved in cholesterol metabolism pathways in podocytes, according to Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment analysis of the differentially abundant metabolites (Fig. 4a). We further demonstrated that Ccdc92 knockdown significantly increased the cholesterol efflux capacity (Fig. 4b) but had no obvious effect on cholesterol uptake (Fig. 4c), finally leading to the reduction of total intracellular cholesterol content (Fig. 4d) in podocytes exposed to HG. Consistent with this finding, there was less cholesterol accumulation, as determined by filipin staining, in podocytes labeled with synaptopodin from db/db/Cre+/Ccdc92fl/fl mice compared to db/db/Cre-/Ccdc92fl/fl mice (Fig. 4e). Moreover, we measured the expression of ATP-binding cassette transporter A1 (ABCA1) and ATP-binding cassette protein G1 (ABCG1), which are the two key factors regulating cholesterol efflux, in podocytes [15]. Our results showed that HG treatment significantly decreased the protein levels of ABCA1 and ABCG1, but genetic silencing of Ccdc92 preferentially increased the ABCA1 protein level (Fig. 4f). Moreover, podocyte-specific knockout of Ccdc92 increased the protein level of ABCA1 in isolated glomeruli from db/db mice (Fig. 4g). Notably, there was no obvious change of ABCA1 mRNA level in HG-treated podocytes and isolated glomeruli from diabetic Cre+/Ccdc92fl/fl mice (Fig. 4h, i), suggesting that a posttranscriptional regulation pathway may be involved in Ccdc92-mediated ABCA1 downregulation. In addition, genetic silencing of ABCA1 (Fig. 4j) counteracted the protective role of Ccdc92 knockdown in podocytes exposed to HG, as evidenced by the increased actin cytoskeleton disorganization (Fig. 4k) and accumulation of total cholesterol (Fig. 4l), indicating that ABCA1 is involved in CCDC92-mediated cholesterol homeostasis in podocytes.
a Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment based on the UPLC-MS/MS analysis of podocytes in different groups. Rich factor refers to the ratio of the number of differentially expressed metabolites in the corresponding pathway to the total number of metabolites detected and annotated by the pathway. The size of dots represents the number of differentially significant metabolites enriched in the corresponding pathway. b Cholesterol efflux capacity in podocytes with different treatments (n = 6 for each group). ***P < 0.001 vs. scramble (si-NC) control, ##P < 0.01 vs. scramble of HG treatment. c Cholesterol uptake in podocytes with different treatments (n = 6 for each group). ***P < 0.001 vs. scramble (si-NC) control. d Levels of total cholesterol in podocytes with different treatments (n = 6 for each group). ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. e Representative images showing cholesterol deposition by immunofluorescence staining of Filipin (blue) and synaptopodin (red) in kidney from mice. f Representative Western blot gel documents and summarized data showing the relative protein levels of ABCA1 and ABCG1 in podocytes with different treatments (n = 6 for each group). *P < 0.05, **P < 0.01, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. g Representative Western blot gel documents and summarized data showing the relative protein levels of ABCA1 in isolated glomeruli from different groups of mice (n = 8 for each group). **P < 0.01, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. h Summarized data showing the effect of Ccdc92 on the mRNA levels of Abca1 in podocytes treated with HG (n = 6 for each group). Levels of the housekeeping gene β-actin were used as an internal control for the normalization of RNA quantity among the samples. ***P < 0.001 vs. scramble (si-NC) control. i Summarized data showing the effect of CCDC92 on the mRNA levels of Abca1 in isolated glomeruli from different groups of mice (n = 6 for each group). Levels of the housekeeping gene β-actin were used as an internal control for the normalization of RNA quantity among the samples. ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice. j Representative Western blot gel documents and summarized data showing the gene silencing efficiency of Abca1 by a Abca1-siRNA transfection in podocytes (n = 6 for each group). ***P < 0.001 vs. scramble (si-NC). k Representative immunofluorescence images of F-actin by phalloidine staining (n = 6 for each group) in mouse podocytes with different treatments. **P < 0.01, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment, +++P < 0.001 vs. si-Ccdc92 podocytes (si-Ccdc92) with HG. l The levels of total cholesterol in podocytes with different treatments (n = 6 for each group). **P < 0.01, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment, +++P < 0.001 vs. si-Ccdc92 podocytes (si-Ccdc92) with HG. Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-tailed Student’s unpaired t test analysis (j), Two-way ANOVA followed by Tukey’s post-test (b–d, f–l).
Ccdc92 deficiency increased the protein level of ABCA1 through the proteasome pathway
By analysis based on the Search Tool for the Retrieval of Interacting Genes (STRING), we found that Ccdc92 interacted with various protease regulatory subunits (Fig. 5a). Moreover, Gene Ontology (GO) analysis (Fig. 5b) in Tandem Mass Tags (TMT) proteomics analysis indicated that Ccdc92 was related to the regulation of proteasome activity. Therefore, we further assessed the relationship between Ccdc92 and proteasome activity in podocytes under HG conditions. Our results showed that Ccdc92 knockdown reduced HG-induced proteasome activity determined by chymotrypsin like activity, which was reversed by overexpression of Ccdc92 in podocytes (Fig. 5c, Supplementary Fig. S4a). Moreover, podocyte-specific deletion of Ccdc92 reduced the expression of β5i, an immunoproteasome subunit indicating the activation of the ubiquitin‒proteasome system (UPS) [16], in isolated glomeruli and podocytes from db/db mice (Fig. 5d, e). Furthermore, treatment with MG132, a proteasome inhibitor [17], reduced proteasome activity (Fig. 5f) and increased the protein level of ABCA1 (Fig. 5g), abrogating the effect of Ccdc92 overexpression on the protein level of ABCA1 in podocytes exposed to HG treatment. Additionally, Ccdc92 deficiency increased the total level of ubiquitin in HG-treated podocytes and in glomeruli and podocytes from db/db mice (Fig. 5h-j). However, genetic silencing of Ccdc92 did not increase the total level of ubiquitin in MG132-treated podocytes (Supplementary Fig. S4b), suggesting that CCDC92 might regulate the level of ABCA1 through proteasome activity independent of ubiquitination stage.
a Protein–protein interaction (PPI) networks based on Search Tool for the Retrieval of Interacting Genes (STRING) database. The line segment indicates both functional and physical protein associations. b Gene Ontology (GO) function analysis in podocytes with or without Ccdc92 overexpression by Tandem Mass Tags (TMT) proteomics analysis. All differentially expressed proteins are compared with all proteins of the reference species with the annotation results of GO functions, and the significance of the difference between the two is obtained by Fisher’s Exact Test. The top abscissa represents the GO secondary functional annotation information, while the bottom represents the statistical results of differential proteins under each GO functional classification. The ordinate represents the percentage of the number of differentially expressed proteins under each functional classification to the total number of differentially expressed proteins. The color represents the significance of the enriched GO functional classification. c Proteasome activity represented by the chymotrypsin-like activity in podocytes with different treatments (n = 6 for each group). *P < 0.05, **P < 0.01, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment, +++P < 0.001 vs. Ccdc92 knockdown (si-Ccdc92) podocytes with HG treatment. d Representative Western blot gel documents and summarized data showing the relative protein levels of β5i in isolated glomeruli from different groups of mice (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, ###P < 0.001 vs. db/db//Cre-/Ccdc92fl/fl mice. e Representative immunofluorescence images of β5i (green) and synaptopodin (red) in glomeruli from different groups of mice. f Proteasome activity represented by the chymotrypsin-like activity in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. g Representative Western blot gel documents and summarized data showing the relative protein levels of ABCA1 in podocytes with different treatments (n = 6 for each group). ***P < 0.001 vs. scramble (OE-NC) control, ##P < 0.01 vs. scramble of HG treatment, +++P < 0.001 vs. Ccdc92-overexpression (OE-Ccdc92) podocytes with HG treatment. h Representative Western blot gel documents showing the relative levels of Ubiquitin in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. i Representative Western blot gel documents showing the relative levels of Ubiquitin in isolated glomeruli from different groups of mice (n = 6 for each group). ***P < 0.001 vs. db/+//Cre-/Ccdc92fl/fl mice, #P < 0.05 vs. db/db//Cre-/Ccdc92fl/fl mice. j Representative immunofluorescence images showing the expression of Ubiquitin in podocytes from different groups of mice. Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-way ANOVA followed by Tukey’s post-test (c, d, f–i).
Ccdc92 promoted HG-induced proteasome activity in podocytes by binding to PA28α
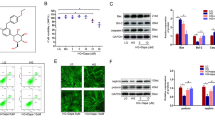
PA28α, a well-known and important proteasome activator subunit, plays a crucial role in regulating proteasome activity [18]. Given the properties of the coiled-coil structure of CCDC92 and the results of STRING and TMT proteomic analyses indicating that the molecular functions of CCDC92 are highly related to “binding” and “catalytic activity” (Fig. 6a), we investigated the interaction between CCDC92 and PA28α. The results of IF (Fig. 6b) and coimmunoprecipitation (Co-IP) (Fig. 6c) assays confirmed that Ccdc92 bound to PA28α and that the binding activity was enhanced under HG conditions (Fig. 6c). It is known that proteasomal degradation is critically dependent on proteasome activators, such as PA28, which bind to the end of the 20 S core particle for reposition of its gating residues and allow access to doomed substrates [19]. Then, we demonstrated by a Co-IP assay that Ccdc92 deficiency reduced the HG-induced binding between PA28α and the 20 S core subunit α4 (Fig. 6d). Furthermore, genetic silencing of PA28α in podocytes (Supplementary Fig. S5a) counteracted the effects of Ccdc92 on proteasome activation (Fig. 6e), the protein level of ABCA1 (Fig. 6f), the cholesterol efflux capacity (Fig. 6g) and lipid accumulation (Fig. 6h, i). Overexpression of Ccdc92 aggravated actin cytoskeleton disorganization in podocytes exposed to HG, which was partially reversed by genetic silencing of PA28α (Supplementary Fig. S5b).
a The molecular functions (MF) analysis in podocytes with or without Ccdc92 overexpression by Tandem Mass Tags (TMT) proteomics analysis. The vertical axis in the figure represents the Gene Ontology (GO) secondary functional annotation information (GO Terms name), and the horizontal axis represents the number of differentially expressed proteins under this functional classification. b Representative immunofluorescence images of Ccdc92 (green) and PA28α (red) staining in podocytes showing the co-localization. c Representative Western blot gel documents and summarized data showing the levels of PA28α in podocytes with different treatments (n = 6 for each group). Ccdc92 was immunoprecipitated with rabbit antibody to Ccdc92 and the presence of PA28α in the immune-complex was assessed by Western blot with the antibody to PA28α. Negative control using isotype matched normal IgG (rabbit) was done to check for antibody specificity. ***P < 0.001 vs. control. d Representative Western blot gel documents and summarized data showing the levels of PA28α in podocytes with different treatments (n = 6 for each group). The 20 S proteasome α4 was immunoprecipitated with rabbit antibody to 20 S proteasome α4 and the presence of PA28α in the immune-complex was assessed by Western blot with the antibody to PA28α. Negative control using isotype matched normal IgG (rabbit) was done to check for antibody specificity. ***P < 0.001 vs. scramble (si-NC) control, ###P < 0.001 vs. scramble of HG treatment. e. Proteasome activity represented by the chymotrypsin-like activity in podocytes with different treatments (n = 6 for each group). **P < 0.01, ***P < 0.001 vs. scramble (OE-NC) control, ###P < 0.001 vs. scramble of HG treatment, +++P < 0.001 vs. Ccdc92-overexpression (OE-Ccdc92) podocytes with HG treatment. f Representative Western blot gel documents and summarized data showing the relative protein levels of ABCA1 in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (OE-NC) control, #P < 0.05 vs. scramble of HG treatment, +++P < 0.001 vs. Ccdc92-overexpression (OE-Ccdc92) podocytes with HG treatment. g The cholesterol efflux capacity in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. scramble (OE-NC) control, ##P < 0.01 vs. scramble of HG treatment, +++P < 0.001 vs. Ccdc92-overexpression (OE-Ccdc92) podocytes with HG treatment. h Photomicrographs and quantifications showing Oil Red O staining in podocytes from different groups (n = 6 for each group). ***P < 0.001 vs. scramble (OE-NC) control, #P < 0.05 vs. scramble of HG treatment, ++P < 0.01 vs. Ccdc92-overexpression (OE-Ccdc92) podocytes with HG treatment. i Photomicrographs and quantifications showing Nile Red staining in podocytes from different groups (n = 6 for each group). ***P < 0.001 vs. scramble (OE-NC) control, ###P < 0.001 vs. scramble of HG treatment, +++P < 0.001 vs. Ccdc92-overexpression (OE-Ccdc92) podocytes with HG treatment. Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-tailed Student’s unpaired t test analysis (c), Two-way ANOVA followed by Tukey’s post-test (d–i).
The Ccdc92 ∆aa59–113 mutation counteracted the effects of Ccdc92 on podocyte lipotoxicity
Finally, to identify the binding region of CCDC92 to PA28α, we generated four Ccdc92 deletion mutants, including two of them lacking aa 1-27 (FLAG-Ccdc92 ∆1-27) and aa 59-113 (FLAG-Ccdc92 ∆59-113) in the coiled-coil domain predicted by Jpred4 and other two lacking other domains containing aa 153-193 and aa 251-314 (FLAG-Ccdc92 ∆153-193, FLAG-Ccdc92 ∆251-314) based on the UniProt database (Fig. 7a). It was found that the Ccdc92 deletion mutant lacking the aa 59–113 in the coiled-coil domain (FLAG-Ccdc92 ∆59-113) could not bind to PA28α, while there were no significant differences in the binding of wild-type (WT) Ccdc92 and the other three mutants to PA28α (Fig. 7b). Importantly, our results further confirmed that deletion of aa59–113 of Ccdc92 in podocytes abolished the effects of Ccdc92 on proteasome activation (Fig. 7c), the protein level of ABCA1 (Fig. 7d), the cholesterol efflux capacity (Fig. 7e), lipid accumulation (Fig. 7f, g) and podocyte injury (Supplementary Fig. S6a, b).
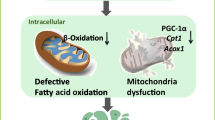
a Four different Ccdc92 deletion mutants were constructed, each lacking one of the coiled-coil or other domains predicted by Jpred4 and Uniprot database. b Representative Western blot gel documents and summarized data showing the levels of PA28α in podocytes with different treatments. Ccdc92 was immunoprecipitated with the rabbit antibody to FLAG and the presence of PA28α in the immune-complex was assessed by Western blot with the antibody to PA28α. Negative control using isotype matched normal IgG (rabbit) was done to check for antibody specificity. c Proteasome activity represented by the chymotrypsin-like activity in podocytes with different treatments (n = 6 for each group). *P < 0.05, **P < 0.01, ***P < 0.001 vs. control (pCMV6-Entry), ##P < 0.01 vs. pCMV6-Entry with high glucose (HG) treatment, ++P < 0.01 vs. Ccdc92-overexpression podocytes (pCMV6-Ccdc92) with HG treatment. d Representative Western blot gel documents and summarized data showing the relative protein levels of ABCA1 in podocytes with different treatments (n = 6 for each group). *P < 0.05, ***P < 0.001 vs. pCMV6-Entry, ###P < 0.001 vs. pCMV6-Entry with HG treatment, +++P < 0.001 vs. pCMV6-Ccdc92 with HG treatment. e The cholesterol efflux capacity in podocytes with different treatments (n = 6 for each group). **P < 0.01, ***P < 0.001 vs. pCMV6-Entry, ##P < 0.01 vs. pCMV6-Entry with HG treatment, ++P < 0.01 vs. pCMV6-Ccdc92 with HG treatment. f Photomicrographs and quantifications showing Nile Red staining in podocytes from different groups (n = 6 for each group). ***P < 0.001 vs. pCMV6-Entry, ###P < 0.001 vs. pCMV6-Entry with HG treatment, +++P < 0.001 vs. pCMV6-Ccdc92 with HG treatment. g Photomicrographs and quantifications showing cholesterol deposition by immunofluorescence staining of Filipin (green) and Wilms tumor type1 (WT1, red) of podocytes in different groups (n = 6 for each group). ***P < 0.001 vs. pCMV6-Entry, ###P < 0.001 vs. pCMV6-Entry with HG treatment, +++P < 0.001 vs. pCMV6-Ccdc92 with HG treatment. h Schematic depicting CCDC92 promotes podocyte injury by regulating PA28α/ABCA1/cholesterol efflux axis in diabetic kidney disease. Data are expressed as mean ± SEM and n indicates the number of biologically independent experiments. Two-way ANOVA followed by Tukey’s post-test (c–g).
Discussion
Although intensive glycemic control or targeting of the renin–angiotensin–aldosterone system (RAAS) with angiotensin-converting enzyme inhibitors (ACEi) and angiotensin receptor blockers (ARBs) can provide beneficial effects to patients with DKD [20], there is no specific treatment to fully prevent the development of DKD, suggesting that factors other than impaired glucose metabolism and altered hemodynamics can promote DKD. Recently, an increasing number of studies have revealed that ectopic lipid accumulation, termed lipotoxicity, has been recognized to play a role in the pathogenesis of DKD [2, 21,22,23]. Among glomerular cells, podocytes are particularly sensitive to lipotoxic injury [3]. It was reported that the accumulation of both cholesterol ester and fatty acid metabolites in podocytes was involved in the pathogenesis of glomerular dysfunction in DKD [24]. Notably, cholesterol accumulates in the cytoplasm of podocytes from patients and mice with DKD. Excessive cholesterol accumulation can perturb the slit diaphragm, adversely affect podocyte function and even induce proteinuric kidney diseases [6,7,8, 25]. However, pharmacological induction of cholesterol efflux with cyclodextrin alleviates podocyte injury in DKD [26], indicating that enhanced cholesterol efflux protects against podocyte injury through reprogramming of cholesterol homeostasis. In this study, we found that upregulation of Ccdc92 in glomeruli was positively correlated with an increased UACR and podocyte loss in mice with DKD and that Ccdc92 knockdown significantly increased the cholesterol efflux capacity but had no obvious effect on cholesterol uptake, thereby reducing the total intracellular cholesterol content and attenuating podocyte injury, indicating that CCDC92 might contribute to podocyte lipotoxicity by decreasing cholesterol efflux.
Cholesterol efflux is a sophisticated and dynamic process involving multiple subprocesses and related factors. Among the related factors, ABCA1 and ABCG1 are recognized as the two key factors regulating cholesterol efflux in the context of podocyte injury [7, 8, 27]. In this study, we found that Ccdc92 preferentially decreased the protein level of ABCA1, which is a transmembrane protein that regulates the efflux of cholesterol and phospholipids in an ATP-dependent manner [28, 29]. ABCA1 expression is positively correlated with the estimated glomerular filtration rate (GFR) [7]. Moreover, podocyte ABCA1 deficiency is sufficient to confer susceptibility to injury in the context of DKD [8], and activation of ABCA1 by its overexpression or by treatment with A30, a pharmacological inducer, ameliorates podocyte injury [8]. In this study, we demonstrated that Ccdc92 negatively regulated the expression of ABCA1 and that genetic silencing of ABCA1 increased the intracellular cholesterol content in Ccdc92-knockdown podocytes exposed to HG, suggesting that CCDC92 might inhibit cholesterol efflux by regulating ABCA1.
Interestingly, we found that Ccdc92 regulated the protein level rather than the mRNA level of ABCA1 under diabetic conditions, suggesting that this regulation might occur at the posttranscriptional level. The ubiquitin‒proteasome system (UPS), one of the major intracellular protein degradation pathways, is important for maintaining cell homeostasis [30]. During this process, upregulation of proteasome activity specifically occurs in patients with membranous nephropathy (MN), focal segmental glomerulosclerosis (FSGS) and DKD, which is considered as a sign of persistent podocyte injury [31, 32]. Meanwhile, the role of UPS is highlighted in the pathogenesis and progression of various diseases including secondary complications of diabetes, suggesting that targeting the UPS might be a novel strategy to prevent DKD [33]. Importantly, the UPS can also serve as an important determinant for cellular cholesterol homeostasis through the regulation of cholesterol metabolism [34]. Furthermore, proteasomal inhibition can induce the expression of ABCA1 and cholesterol efflux in macrophages [35], suggesting that proteasome regulates cholesterol efflux by mediating ABCA1 expression. The results from our bioinformatics analysis strongly suggested that Ccdc92 interacted with the proteasome. We further demonstrated that Ccdc92 regulated the level of ABCA1 via UPS-mediated degradation, consistent with previous studies showing that the ubiquitination degradation pathway contributed to the reduced level of ABCA1 in the context of cell injury [34, 35]. Interestingly, our results showed that genetic silencing of Ccdc92 did not increase the total level of ubiquitin in MG132-treated podocytes, indicating that CCDC92 might regulate the level of ABCA1 through proteasome activity, independent of ubiquitination stage.
Mechanistically, CCDC92 participates in a variety of biological processes by binding to other proteins [36, 37]. Our proteomic analysis strongly suggested that CCDC92 might interact with some protease subunits with catalytic activity. PA28α, a well-known and important proteasome activator subunit, is recognized as a key factor in regulating proteasome activity [18]. Moreover, previous studies have reported that the PA28 proteasome and the immunoproteasome are involved in the development of DKD [31]. PA28α/PA28β double knockout in mice attenuates albuminuria in the context of DKD [38], suggesting that PA28-mediated alteration of proteasome activity contributes to DKD. Our results demonstrated that Ccdc92 can bind to PA28α, consequently enhancing the interaction of PA28α with the core subunit of the proteasome, in turn promoting proteasome activity and accelerating ABCA1 degradation, finally leading to the disruption of cholesterol homeostasis in podocytes. More accurately, we further found that the aa 59–113 in the coiled-coil domain of Ccdc92 was necessary for the binding of PA28α. Moreover, we provided direct evidence for the effects of Ccdc92 aa59–113 on lipid metabolism and podocyte injury, suggesting that the aa 59–113 in the coiled-coil domain of CCDC92 is vital for regulating the PA28α/ABCA1/cholesterol efflux axis.
Some limitations of this study should be noted. Although we demonstrated that Ccdc92 regulated ABCA1 via the proteasome pathway, we cannot exclude the possibility that other targets of Ccdc92 may also be involved in this process. It is known that the UPS can control all aspects of cholesterol metabolism, including synthesis, uptake and efflux, by regulating specific key molecules, such as ABCG5, ABCG8, liver X receptors (LXRs) α and β, and sterol regulatory element binding proteins (SREBPs) 1 and 2, the master transcriptional regulators of cholesterol metabolism [34], suggesting that the PA28-mediated proteasome system might regulate several molecules related to cholesterol metabolism to promote cholesterol deposition in podocytes. In addition, although recent studies have indicated that Ccdc92 is involved in obesity, T2D and insulin sensitivity [13], few studies have focused on the mechanisms of Ccdc92 in obesity and insulin resistance. In this study, we found that Ccdc92 inhibited cholesterol efflux in podocytes by promoting the degradation of ABCA1, which is also a key factor in regulating adipose tissue lipid content and insulin sensitivity [39]. Therefore, we speculate that similar mechanisms might be involved in these effects of Ccdc92. Further studies are needed to address this possibility.
In conclusion, we demonstrated that Ccdc92 was upregulated in podocytes and promoted lipid accumulation by inhibiting cholesterol efflux. Mechanistically, we found that Ccdc92 promoted the degradation of ABCA1 by regulating PA28α-mediated proteasome activity (Fig. 7h). Our findings suggest that targeting CCDC92-mediated cholesterol metabolism may constitute a new therapeutic strategy for diabetic kidney disease.
Data availability
The proteomics data presented in this study are openly available in ProteomeXchange with identifier PXD036050. Other data that support the findings of this study are available from the corresponding author upon reasonable request.
References
John S. Complication in diabetic nephropathy. Diabetes Metab Syndr. 2016;10:247–9.
Fu Y, Sun Y, Wang M, Hou Y, Huang W, Zhou D, et al. Elevation of JAML promotes diabetic kidney disease by modulating podocyte lipid metabolism. Cell Metab. 2020;32:1052–62.e8.
DeFronzo RA, Reeves WB, Awad AS. Pathophysiology of diabetic kidney disease: impact of SGLT2 inhibitors. Nat Rev Nephrol. 2021;17:319–34.
Wahl P, Ducasa GM, Fornoni A. Systemic and renal lipids in kidney disease development and progression. Am J Physiol Ren Physiol. 2016;310:F433–45.
Brinkkoetter PT, Bork T, Salou S, Liang W, Mizi A, Ozel C, et al. Anaerobic glycolysis maintains the glomerular filtration barrier independent of mitochondrial metabolism and dynamics. Cell Rep. 2019;27:1551–66.e5.
Pedigo CE, Ducasa GM, Leclercq F, Sloan A, Mitrofanova A, Hashmi T, et al. Local TNF causes NFATc1-dependent cholesterol-mediated podocyte injury. J Clin Invest. 2016;126:3336–50.
Herman-Edelstein M, Scherzer P, Tobar A, Levi M, Gafter U. Altered renal lipid metabolism and renal lipid accumulation in human diabetic nephropathy. J Lipid Res. 2014;55:561–72.
Ducasa GM, Mitrofanova A, Mallela SK, Liu X, Molina J, Sloan A, et al. ATP-binding cassette A1 deficiency causes cardiolipin-driven mitochondrial dysfunction in podocytes. J Clin Invest. 2019;129:3387–400.
Huang LO, Rauch A, Mazzaferro E, Preuss M, Carobbio S, Bayrak CS, et al. Genome-wide discovery of genetic loci that uncouple excess adiposity from its comorbidities. Nat Metab. 2021;3:228–43.
Vujkovic M, Keaton JM, Lynch JA, Miller DR, Zhou J, Tcheandjieu C, et al. Discovery of 318 new risk loci for type 2 diabetes and related vascular outcomes among 1.4 million participants in a multi-ancestry meta-analysis. Nat Genet. 2020;52:680–91.
Zhao W, Rasheed A, Tikkanen E, Lee JJ, Butterworth AS, Howson JMM, et al. Identification of new susceptibility loci for type 2 diabetes and shared etiological pathways with coronary heart disease. Nat Genet. 2017;49:1450–7.
Klarin D, Zhu QM, Emdin CA, Chaffin M, Horner S, McMillan BJ, et al. Genetic analysis in UK Biobank links insulin resistance and transendothelial migration pathways to coronary artery disease. Nat Genet. 2017;49:1392–7.
Ren L, Du W, Song D, Lu H, Hamblin MH, Wang C, et al. Genetic ablation of diabetes-associated gene Ccdc92 reduces obesity and insulin resistance in mice. iScience. 2023;26:105769.
Wang Z, Jiang T, Li J, Proctor G, McManaman JL, Lucia S, et al. Regulation of renal lipid metabolism, lipid accumulation, and glomerulosclerosis in FVBdb/db mice with type 2 diabetes. Diabetes. 2005;54:2328–35.
Fornoni A, Merscher S, Kopp JB. Lipid biology of the podocyte—new perspectives offer new opportunities. Nat Rev Nephrol. 2014;10:379–88.
Nijholt DA, de Graaf TR, van Haastert ES, Oliveira AO, Berkers CR, Zwart R, et al. Endoplasmic reticulum stress activates autophagy but not the proteasome in neuronal cells: implications for Alzheimer’s disease. Cell Death Differ. 2011;18:1071–81.
Lee DH, Goldberg AL. Proteasome inhibitors: valuable new tools for cell biologists. Trends Cell Biol. 1998;8:397–403.
Collins GA, Goldberg AL. The logic of the 26 S proteasome. Cell. 2017;169:792–806.
Lesne J, Locard-Paulet M, Parra J, Zivkovic D, Menneteau T, Bousquet MP, et al. Conformational maps of human 20 S proteasomes reveal PA28- and immuno-dependent inter-ring crosstalks. Nat Commun. 2020;11:6140.
Vartak T, Godson C, Brennan E. Therapeutic potential of pro-resolving mediators in diabetic kidney disease. Adv Drug Deliv Rev. 2021;178:113965.
Kim Y, Lim JH, Kim MY, Kim EN, Yoon HE, Shin SJ, et al. The adiponectin receptor agonist adiporon ameliorates diabetic nephropathy in a model of type 2 diabetes. J Am Soc Nephrol. 2018;29:1108–27.
Patel M, Wang XX, Magomedova L, John R, Rasheed A, Santamaria H, et al. Liver X receptors preserve renal glomerular integrity under normoglycaemia and in diabetes in mice. Diabetologia. 2014;57:435–46.
Kang HM, Ahn SH, Choi P, Ko YA, Han SH, Chinga F, et al. Defective fatty acid oxidation in renal tubular epithelial cells has a key role in kidney fibrosis development. Nat Med. 2015;21:37–46.
Schelling JR. The contribution of lipotoxicity to diabetic kidney disease. Cells. 2022;11:3236.
Song Y, Liu J, Zhao K, Gao L, Zhao J. Cholesterol-induced toxicity: An integrated view of the role of cholesterol in multiple diseases. Cell Metab. 2021;33:1911–25.
Merscher-Gomez S, Guzman J, Pedigo CE, Lehto M, Aguillon-Prada R, Mendez A, et al. Cyclodextrin protects podocytes in diabetic kidney disease. Diabetes. 2013;62:3817–27.
Yang Q, Hu J, Yang Y, Chen Z, Feng J, Zhu Z, et al. Sirt6 deficiency aggravates angiotensin II-induced cholesterol accumulation and injury in podocytes. Theranostics. 2020;10:7465–79.
Wang N, Silver DL, Thiele C, Tall AR. ATP-binding cassette transporter A1 (ABCA1) functions as a cholesterol efflux regulatory protein. J Biol Chem. 2001;276:23742–7.
Oram JF, Lawn RM. ABCA1. The gatekeeper for eliminating excess tissue cholesterol. J Lipid Res. 2001;42:1173–9.
Pohl C, Dikic I. Cellular quality control by the ubiquitin-proteasome system and autophagy. Science. 2019;366:818–22.
Meyer-Schwesinger C. The ubiquitin-proteasome system in kidney physiology and disease. Nat Rev Nephrol. 2019;15:393–411.
Beeken M, Lindenmeyer MT, Blattner SM, Radon V, Oh J, Meyer TN, et al. Alterations in the ubiquitin proteasome system in persistent but not reversible proteinuric diseases. J Am Soc Nephrol. 2014;25:2511–25.
Goru SK, Kadakol A, Gaikwad AB. Hidden targets of ubiquitin proteasome system: to prevent diabetic nephropathy. Pharmacol Res. 2017;120:170–9.
Sharpe LJ, Cook EC, Zelcer N, Brown AJ. The UPS and downs of cholesterol homeostasis. Trends Biochem Sci. 2014;39:527–35.
Ogura M, Ayaori M, Terao Y, Hisada T, Iizuka M, Takiguchi S, et al. Proteasomal inhibition promotes ATP-binding cassette transporter A1 (ABCA1) and ABCG1 expression and cholesterol efflux from macrophages in vitro and in vivo. Arterioscler Thromb Vasc Biol. 2011;31:1980–7.
Chaki M, Airik R, Ghosh AK, Giles RH, Chen R, Slaats GG, et al. Exome capture reveals ZNF423 and CEP164 mutations, linking renal ciliopathies to DNA damage response signaling. Cell. 2012;150:533–48.
Bernatik O, Pejskova P, Vyslouzil D, Hanakova K, Zdrahal Z, Cajanek L. Phosphorylation of multiple proteins involved in ciliogenesis by Tau Tubulin kinase 2. Mol Biol Cell. 2020;31:1032–46.
Yadranji Aghdam S, Mahmoudpour A. Proteasome activators, PA28alpha and PA28beta, govern development of microvascular injury in diabetic nephropathy and retinopathy. Int J Nephrol. 2016;2016:3846573.
de Haan W, Bhattacharjee A, Ruddle P, Kang MH, Hayden MR. ABCA1 in adipocytes regulates adipose tissue lipid content, glucose tolerance, and insulin sensitivity. J Lipid Res. 2014;55:516–23.
Acknowledgements
This study was supported by the National Natural Science Foundation of China (T2321004, 91949202, 82090024, 81873614, 82090021, 81900621, 81970580, 82070753, 82170734, 81800645, 81800643, 22107058); Shandong Provincial Natural Science Foundation, China (ZR2019ZD40, ZR2019MH041, 2023HWYQ-020); The Taishan Scholars Program of Shandong Province, China (tsqn202306074) and Cutting Edge Development Fund of Advanced Medical Research Institute (GYY2023QY01).
Author information
Authors and Affiliations
Contributions
FWZ. conducted the in vivo and in vitro experiments, performed data analysis, and helped write the manuscript. ZYL, MWW, JYD, PZD and HRZ. contributed to the experimental design and performed the in vitro experiments. XJW performed the in vivo animal studies. YS and YZ helped design the experiments. JCW performed confocal microscopy. WT and YSX analyzed the data. FY, ZYW, and ML designed the experiments, interpreted the data, wrote the manuscript, and approved the final version of the manuscript for publication.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zuo, Fw., Liu, Zy., Wang, Mw. et al. CCDC92 promotes podocyte injury by regulating PA28α/ABCA1/cholesterol efflux axis in type 2 diabetic mice. Acta Pharmacol Sin 45, 1019–1031 (2024). https://doi.org/10.1038/s41401-023-01213-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-023-01213-4
- Springer Nature Singapore Pte Ltd.