Abstract
Chronic inflammation is associated with a variety of pathological conditions in epithelial tissues, including cancer, metaplasia and aberrant wound healing. In relation to this, a significant body of evidence suggests that aberration of epithelial stem and progenitor cell function is a contributing factor in inflammation-related disease, although the underlying cellular and molecular mechanisms remain to be fully elucidated. In this study, we have delineated the effect of chronic inflammation on epithelial stem/progenitor cells using the corneal epithelium as a model tissue. Using a combination of mouse genetics, pharmacological approaches and in vitro assays, we demonstrate that chronic inflammation elicits aberrant mechanotransduction in the regenerating corneal epithelium. As a consequence, a YAP–TAZ/β-catenin cascade is triggered, resulting in the induction of epidermal differentiation on the ocular surface. Collectively, the results of this study demonstrate that chronic inflammation and mechanotransduction are linked and act to elicit pathological responses in regenerating epithelia.








Similar content being viewed by others
References
Arwert, E. N., Hoste, E. & Watt, F. M. Epithelial stem cells, wound healing and cancer. Nat. Rev. Cancer 12, 170–180 (2012).
Grivennikov, S. I., Greten, F. R. & Karin, M. Immunity, inflammation, and cancer. Cell 140, 883–899 (2010).
Herfs, M., Hubert, P. & Delvenne, P. Epithelial metaplasia: adult stem cell reprogramming and (pre)neoplastic transformation mediated by inflammation? Trends Mol. Med. 15, 245–253 (2009).
Karin, M. Nuclear factor-κB in cancer development and progression. Nature 441, 431–436 (2006).
Tu, S. et al. Overexpression of interleukin-1β induces gastric inflammation and cancer and mobilizes myeloid-derived suppressor cells in mice. Cancer Cell 14, 408–419 (2008).
Wu, S. et al. A human colonic commensal promotes colon tumorigenesis via activation of T helper type 17 T cell responses. Nat. Med. 15, 1016–1022 (2009).
Quante, M. et al. Bile acid and inflammation activate gastric cardia stem cells in a mouse model of Barrett-like metaplasia. Cancer Cell 21, 36–51 (2012).
Barker, N. et al. Crypt stem cells as the cells-of-origin of intestinal cancer. Nature 457, 608–611 (2009).
Driessens, G., Beck, B., Caauwe, A., Simons, B. D. & Blanpain, C. Defining the mode of tumour growth by clonal analysis. Nature 488, 527–530 (2012).
Shenoy, A. K. et al. Transition from colitis to cancer: high Wnt activity sustains the tumor-initiating potential of colon cancer stem cell precursors. Cancer Res. 72, 5091–5100 (2012).
Boulter, L. et al. Macrophage-derived Wnt opposes Notch signaling to specify hepatic progenitor cell fate in chronic liver disease. Nat. Med. 18, 572–579 (2012).
Taniguchi, K. et al. A gp130-Src-YAP module links inflammation to epithelial regeneration. Nature 519, 57–62 (2015).
Di Piazza, M., Nowell, C. S., Koch, U., Durham, A. D. & Radtke, F. Loss of cutaneous TSLP-dependent immune responses skews the balance of inflammation from tumor protective to tumor promoting. Cancer Cell 22, 479–493 (2012).
Aragona, M. et al. A mechanical checkpoint controls multicellular growth through YAP/TAZ regulation by actin-processing factors. Cell 154, 1047–1059 (2013).
Samuel, M. S. & Olson, M. F. Actomyosin contractililty: force power drives tumor growth. Cell Cycle 10, 3409–3410 (2011).
Humphrey, J. D., Dufresne, E. R. & Schwartz, M. A. Mechanotransduction and extracellular matrix homeostasis. Nat. Rev. Mol. Cell Biol. 15, 802–812 (2014).
Paszek, M. J. et al. Tensional homeostasis and the malignant phenotype. Cancer Cell 8, 241–254 (2005).
Levental, K. R. et al. Matrix crosslinking forces tumor progression by enhancing integrin signaling. Cell 139, 891–906 (2009).
Bonnans, C., Chou, J. & Werb, Z. Remodelling the extracellular matrix in development and disease. Nat. Rev. Mol. Cell Biol. 15, 786–801 (2014).
McHedlidze, T. et al. Interleukin-33-dependent innate lymphoid cells mediate hepatic fibrosis. Immunity 39, 357–371 (2013).
Aceves, S. S. & Ackerman, S. J. Relationships between eosinophilic inflammation, tissue remodeling, and fibrosis in eosinophilic esophagitis. Immunol. Allergy Clin. North Am. 29, 197–211 (2009).
Zhu, Z. et al. Pulmonary expression of interleukin-13 causes inflammation, mucus hypersecretion, subepithelial fibrosis, physiologic abnormalities, and eotaxin production. J. Clin. Invest. 103, 779–788 (1999).
Daniels, J. T., Dart, J. K., Tuft, S. J. & Khaw, P. T. Corneal stem cells in review. Wound Repair Regen. 9, 483–494 (2001).
Daniels, J. T. et al. Limbal epithelial stem cell therapy. Expert Opin. Biol. Ther. 7, 1–3 (2007).
Majo, F., Rochat, A., Nicolas, M., Jaoude, G. A. & Barrandon, Y. Oligopotent stem cells are distributed throughout the mammalian ocular surface. Nature 456, 250–254 (2008).
Liang, L., Sheha, H., Li, J. & Tseng, S. C. Limbal stem cell transplantation: new progresses and challenges. Eye 23, 1946–1953 (2009).
Samson, C. M., Nduaguba, C., Baltatzis, S. & Foster, C. S. Limbal stem cell transplantation in chronic inflammatory eye disease. Ophthalmology 109, 862–868 (2002).
McNamara, N. A., Gallup, M. & Porco, T. C. Establishing PAX6 as a biomarker to detect early loss of ocular phenotype in human patients with Sjogren’s syndrome. Invest. Ophthalmol. Vis. Sci. 55, 7079–7084 (2014).
Chen, Y. T. et al. Immune profile of squamous metaplasia development in autoimmune regulator-deficient dry eye. Mol. Vis. 15, 563–576 (2009).
Chen, Y. T. et al. Interleukin-1 receptor mediates the interplay between CD4+ T cells and ocular resident cells to promote keratinizing squamous metaplasia in Sjogren’s syndrome. Lab. Invest. 92, 556–570 (2012).
Vauclair, S. et al. Corneal epithelial cell fate is maintained during repair by Notch1 signaling via the regulation of vitamin A metabolism. Dev. Cell 13, 242–253 (2007).
Demehri, S. et al. Notch-deficient skin induces a lethal systemic B-lymphoproliferative disorder by secreting TSLP, a sentinel for epidermal integrity. PLoS Biol. 6, e123 (2008).
Dumortier, A. et al. Atopic dermatitis-like disease and associated lethal myeloproliferative disorder arise from loss of Notch signaling in the murine skin. PLoS ONE 5, e9258 (2010).
Guinea-Viniegra, J. et al. Differentiation-induced skin cancer suppression by FOS, p53, and TACE/ADAM17. J. Clin. Invest. 122, 2898–2910 (2012).
Murthy, A. et al. Notch activation by the metalloproteinase ADAM17 regulates myeloproliferation and atopic barrier immunity by suppressing epithelial cytokine synthesis. Immunity 36, 105–119 (2012).
Schonthaler, H. B., Guinea-Viniegra, J. & Wagner, E. F. Targeting inflammation by modulating the Jun/AP-1 pathway. Ann. Rheum. Dis. 70, i109–i112 (2011).
Eckert, R. L. et al. AP1 transcription factors in epidermal differentiation and skin cancer. J. Skin Cancer 2013, 537028 (2013).
Wurm, S. et al. Terminal epidermal differentiation is regulated by the interaction of Fra-2/AP-1 with Ezh2 and ERK1/2. Genes Dev. 29, 144–156 (2015).
Chappaz, S., Flueck, L., Farr, A. G., Rolink, A. G. & Finke, D. Increased TSLP availability restores T- and B-cell compartments in adult IL-7 deficient mice. Blood 110, 3862–3870 (2007).
Omori-Miyake, M. & Ziegler, S. F. Mouse models of allergic diseases: TSLP and its functional roles. Allergol. Int. 61, 27–34 (2012).
Kuraguchi, M. et al. Adenomatous polyposis coli (APC) is required for normal development of skin and thymus. PLoS Genet. 2, e146 (2006).
Miyoshi, K. et al. Activation of β-catenin signaling in differentiated mammary secretory cells induces transdifferentiation into epidermis and squamous metaplasias. Proc. Natl Acad. Sci. USA 99, 219–224 (2002).
Mukhopadhyay, M. et al. Dkk2 plays an essential role in the corneal fate of the ocular surface epithelium. Development 133, 2149–2154 (2006).
Harada, N. et al. Intestinal polyposis in mice with a dominant stable mutation of the β-catenin gene. EMBO J. 18, 5931–5942 (1999).
Dupont, S. et al. Role of YAP/TAZ in mechanotransduction. Nature 474, 179–183 (2011).
Azzolin, L. et al. YAP/TAZ incorporation in the β-catenin destruction complex orchestrates the Wnt response. Cell 158, 157–170 (2014).
Iredale, J. P. Models of liver fibrosis: exploring the dynamic nature of inflammation and repair in a solid organ. J. Clin. Invest. 117, 539–548 (2007).
Carey, W. A., Taylor, G. D., Dean, W. B. & Bristow, J. D. Tenascin-C deficiency attenuates TGF-ss-mediated fibrosis following murine lung injury. Am. J. Physiol. Lung. Cell Mol. Physiol. 299, L785–L793 (2010).
Naik, P. K. et al. Periostin promotes fibrosis and predicts progression in patients with idiopathic pulmonary fibrosis. Am. J. Physiol. Lung. Cell Mol. Physiol. 303, L1046–L1056 (2012).
Lawrance, I. C. et al. Cellular and molecular mediators of intestinal fibrosis. J. Crohn’s Colitis (2015)10.1016/j.crohns.2014.09.008.
Sziksz, E. et al. Fibrosis related inflammatory mediators: role of the IL-10 cytokine family. Mediat. Inflamm. 2015, 764641 (2015).
Kullberg, M. C. et al. TGF-β1 production by CD4+ CD25+ regulatory T cells is not essential for suppression of intestinal inflammation. Eur. J. Immunol. 35, 2886–2895 (2005).
Kenyon, N. J., Ward, R. W., McGrew, G. & Last, J. A. TGF-β1 causes airway fibrosis and increased collagen I and III mRNA in mice. Thorax 58, 772–777 (2003).
Wang, B. et al. Suppression of microRNA-29 expression by TGF-β1 promotes collagen expression and renal fibrosis. J. Am. Soc. Nephrol. 23, 252–265 (2012).
Fulkerson, P. C., Fischetti, C. A. & Rothenberg, M. E. Eosinophils and CCR3 regulate interleukin-13 transgene-induced pulmonary remodeling. Am. J. Pathol. 169, 2117–2126 (2006).
Eyden, B. The myofibroblast: phenotypic characterization as a prerequisite to understanding its functions in translational medicine. J. Cell Mol. Med. 12, 22–37 (2008).
De Wever, O., Demetter, P., Mareel, M. & Bracke, M. Stromal myofibroblasts are drivers of invasive cancer growth. Int. J. Cancer 123, 2229–2238 (2008).
Lin, S. L., Kisseleva, T., Brenner, D. A. & Duffield, J. S. Pericytes and perivascular fibroblasts are the primary source of collagen-producing cells in obstructive fibrosis of the kidney. Am. J. Pathol. 173, 1617–1627 (2008).
Huelsken, J., Vogel, R., Erdmann, B., Cotsarelis, G. & Birchmeier, W. β-catenin controls hair follicle morphogenesis and stem cell differentiation in the skin. Cell 105, 533–545 (2001).
Indra, A. K. et al. Temporally-controlled site-specific mutagenesis in the basal layer of the epidermis: comparison of the recombinase activity of the tamoxifen-inducible Cre-ER(T) and Cre-ER(T2) recombinases. Nucleic Acids Res. 27, 4324–4327 (1999).
Radtke, F. et al. Deficient T cell fate specification in mice with an induced inactivation of Notch1. Immunity 10, 547–558 (1999).
Behrens, A. et al. Impaired postnatal hepatocyte proliferation and liver regeneration in mice lacking c-jun in the liver. EMBO J. 21, 1782–1790 (2002).
Oshima, H., Rochat, A., Kedzia, C., Kobayashi, K. & Barrandon, Y. Morphogenesis and renewal of hair follicles from adult multipotent stem cells. Cell 104, 233–245 (2001).
Hutter, J. L. & Bechhoefer, J. Calibration of atomic-force microscope tips. Rev. Sci. Instrum. 64, 1868–1873 (1993).
Hertz, H. Ueber die Berührung fester elastischer Körper. J. für die reine und angewandte Math. 92, 156–171 (1881).
Acknowledgements
This work was supported in part by OptiStem, the Swiss National Science Foundation, the Swiss Cancer League, the Marie Curie Foundation and EuroSystem. P.D.O. and G.E.F. acknowledge financial support from the Swiss National Science Foundation under award number 205321_134786 and 205320_152675 and European Union FP7/2007-2013 ERC under Grant Agreement No. 307338-NaMic. Work performed in the laboratory of S.P. was supported by grants from AIRC (5x1000 and PI) and the ERC. We thank R. Kemler (Max Planck Institute of Immunobiology and Epigenetics, Freiburg, Germany) for providing the conditional β-catenin mice, M. Taketo (Centre for Frontier Medicine, Kyoto University, Japan) for the Ctnnb1ΔEx3 mice and P. Chambon and D. Metzger (Institute of Genetics and Molecular and Cellular Biology, Strasbourg, France) for the K5CreERT and K14CreERT2 mice. We thank J. Huelsken (Swiss Institute for Experimental Cancer Research, EPFL, Lausanne, Switzerland) for providing the TCF–luciferase reporter cells and the anti-periostin antibody. We would like to thank A. Radenovic, J. Artacho, J. Sordet-Dessimoz and M. Garcia for technical assistance with microscopy, histology and flow cytometry. We would like to thank G. Ferrand for guidance and advice concerning animal experiments.
Author information
Authors and Affiliations
Contributions
C.S.N. designed and performed experiments, analysed data and wrote the manuscript. P.D.O. performed nanomechanical measurement experiments and analysed data. L.A. performed experiments and analysed data. S.H. performed experiments and analysed data. E.F.W., G.E.F., M.P.L., Y.B. and S.P. analysed data and provided conceptual and experimental guidance throughout the study. F.R. conceived the study and analysed data.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Inflammation in Notch1Δ mice following corneal injury.
(a) Immunofluorescent staining for K12, K1 and CD45 in unwounded WT (Notch1lox/lox) and Notch1Δ corneas. Data are representative of 6 corneas over three independent experiments. (b) Flow cytometric analysis showing the proportion of total CD45+ cells (upper plots) and CD45+CD11b+Gr1+ cells (lower plots) in WT (Notch1lox/lox) and Notch1Δ cornea 21 days after the repeated injury procedure (see Fig. 1a). Data are representative of 6 individual analyses performed on cells pooled from 4 corneas of each genotype over three independent experiments. (c) Flow cytometric analysis showing proportion of total CD45+ cells (upper plots) and CD45+CD11b+Gr1+ cells (lower plots) in WT (Notch1lox/lox) and Notch1Δ cornea 24 h after a single injury. Data are representative of 6 individual analyses performed on cells pooled from 4 corneas of each genotype over three independent experiments. Scale bars represent 500 μm.
Supplementary Figure 2 Chronic inflammation is associated with CSCM in Notch1Δ mice.
(a) Immunohistochemistry for pS73cjun following repeated corneal injury. (b) QRT-PCR analysis for the indicated cytokines in WT (Notch1lox/lox:cjunlox/lox), Notch1Δ and Notch1Δ:cjunΔ corneal epithelial cells 24 h after a single corneal injury (n = 6 biological replicates for each genotype over three independent experiments. Each replicate consists of corneal epithelial tissue pooled from 6 corneas isolated from 3 mice of each genotype). Data are expressed relative to the expression in WT unwounded corneal epithelial cells. (c,d) Quantification of the proportion of CD45+ cells in WT (Notch1lox/lox:cjunlox/lox), Notch1Δ and Notch1Δ:cjunΔ cornea 21 days after repeated corneal injury (c) or 24 h after a single corneal injury (d). Proportions were measured by performing flow cytometry on dissociated corneas. (n = 6 biological replicates for each genotype over three independent experiments. Each replicate consists of cells pooled from 4 corneas isolated from 2 mice of each genotype). (e) QRT-PCR analysis of Notch1 in the corneal epithelium of WT (Notch1lox/lox:cjunlox/lox), Notch1Δ:cjunΔ and Notch1Δ mice following repeated injury (n = 6 biological replicates for each genotype over three independent experiments. Each replicate consists of corneal epithelial tissue pooled from 6 corneas isolated from 3 mice of each genotype). (f) Representative immunofluorescent staining for K12, K1 and CD45 in Notch1Δ:cjunΔ and Notch1Δ corneas following repeated corneal injury. Large panels are low magnification tiled images. White outlined insets show high magnification images of the indicated regions. (g) Proportion of WT (Notch1lox/lox:cjunlox/lox) (n = 10 corneas), Notch1Δ (n = 20 corneas) and Notch1Δ:cjunΔ (n = 16 corneas) corneal tissue exhibiting corneal or epidermal identity after repeated corneal injury. (h) Immunfluorescent staining for K12, K1, cjun (pS73) and CD45 on corneal tissue isolated from WT (Notch1lox/lox:cjunlox/lox), Notch1Δ:cjunΔ and Notch1Δ mice after repeated corneal injury. Data are representative of 16 corneas. (i) QRT-PCR analysis of Notch1 in the corneal epithelium of WT (Notch1lox/lox) and Notch1Δ mice treated with ophthalmic lubricating gel or Tobradex following repeated injury (n = 6 biological replicates for each treatment over three independent experiments. Each replicate consists of corneal epithelial tissue isolated during corneal wounding of a single eye). Scale bars represent 500 μm on tiled images and 5 μm on all other images. St – Stroma. ∗P < 0.01, ∗∗P < 0.05 (unpaired, two tailed t-tests). Error bars represent standard deviation.
Supplementary Figure 3 Spatial and temporal kinetics of CSCM.
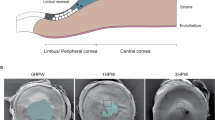
(a) Representative immunofluorescent staining for K12 and K1 on wholemount corneal epithelial tissue isolated from WT and Notch1Δ corneas. Upper panels show unwounded corneas, middle panels show corneal epithelial tissue 24 h after the first injury, lower panels show corneal epithelial tissue 24 h after the second injury. Data are representative of 6 corneal wholemounts over three independent experiments. (b) XY scatter plots showing K12 and K1 expression in limbus, peripheral cornea and central cornea in unwounded corneas and in corneas isolated 24 h after the second corneal injury. Each data point represents mean fluorescence intensity measured from an individual cornea. Grey boxes = WT (Notch1lox/lox), black boxes = Notch1Δ (n = 6 corneas for each genotype over three independent experiments). (c) Immunofluorescent staining for Ki67 on WT and Notch1Δ corneas. Data are representative of 6 corneas. Upper panels show unwounded corneas, middle panels show corneal tissue 24 h after the first injury, lower panels show corneal tissue 24 h after the second injury. Large panels are low magnification tiled images. Insets outlined in green, red and yellow show high magnification images of the limbus, peripheral cornea and central cornea respectively. (d) Quantification of the proportion of Ki67+ cells in the limbus, peripheral cornea and central cornea in unwounded corneas (upper panels), corneas 24 h after the first injury (middle panels) and corneas 24 h after the second injury (lower panels). Black boxes = WT (Notch1lox/lox), grey boxes = Notch1Δ (n = 6 corneas for each genotype over three independent experiments). Scale bars represent 500 μm on tiled images and 5 μm on all other images. St – Stroma, Limb – limbus, Per – Periphery, Cen – Centre. Error bars represent standard deviation.
Supplementary Figure 4 Elevated β-catenin is necessary and sufficient to induce CSCM.
(a–b) Quantification of relative β-catenin expression in limbus, peripheral cornea and central cornea in unwounded eyes (a) and 24 h after the first injury (b). Black bars = WT (Notch1lox/lox), grey bars = Notch1Δ (n = 6 corneas for each genotype over three independent experiments). Values for expression levels are relative values normalised to the expression level in the conjunctiva of each sample, determined by mean fluorescence intensity. (c) Immunofluorescent staining for β-catenin, K12 and K1 on Notch1Δ and Notch1Δ:Ctnnb1Δ corneas after repeated injury. Data are representative of 8 corneas for each genotype over 3 independent experiments. (d) Immunofluorescent staining for β-catenin, K12 and K1 on WT (Ctnnb1lox(Ex3)/lox(Ex3)) and Ctnnb1ΔEx3 corneas 7 days after a single injury. Data are representative of 8 WT corneas and 10 Ctnnb1ΔEx3 corneas over 4 independent experiments. (e) Immunofluorescent staining for K12 and K1 on wholemount corneal epithelial tissue isolated from or WT (Ctnnb1lox(ex3)/lox(ex3)) or Ctnnb1ΔEx3 corneas 7 days after a single corneal injury. Data are representative of 6 WT and 8 Ctnnb1ΔEx3 corneas over 3 independent experiments. Scale bars represent 500 μm on tiled wholemount images and 5 μm on all other images. Error bars represent standard deviation.
Supplementary Figure 5 Inflammation induced CSCM is associated with increased ECM deposition in the corneal stroma.
(a) QRT-PCR analysis of Wnt ligands that exhibit expression in corneal tissue after repeated injury. Analysis was performed on whole corneal tissue isolated from WT (Notch1lox/lox) and Notch1Δ mice 21 days after the 3rd corneal injury (n = 5 biological replicates for each genotype over four independent experiments. Each replicate consists of corneal epithelial tissue pooled from 4 corneas isolated from 2 mice of each genotype). Data are expressed relative to the expression in whole corneal tissue isolated from unwounded mice. Error bars represent standard deviation. (b) Immunofluorescence for Periostin, CD45 and DAPI on chronically inflamed Notch1Δ corneal tissue after repeated injury. Single fluorescent images and merges are shown as indicated. Data are representative of 4 corneas analysed over two independent experiments. Scale bars represent 5 μm. (c) Immunofluorescent staining for K14 and Tenascin C (upper panels) or K14 and Periostin (lower panels) in Notch1Δ mice treated with either ophthalmic gel (control) or Tobradex during the repeated injury procedure. Data are representative of 6 corneas analysed over three independent experiments. Scale bars represent 500 μm.
Supplementary Figure 6 CSCM is associated with mechanotransduction.
(a,b) Quantification of FAK phosphorylation (upper panels) and nuclear:cytoplasmic ratio of ROCK2 (middle panels) and YAP/TAZ (lower panels) in the limbus, peripheral cornea and central cornea isolated from unwounded eyes (a) or eyes isolated 24 h after the first corneal injury (b). Values for expression levels are relative values normalised to the expression level in the conjunctiva of each sample, determined by mean fluorescence intensity. Black bars = WT (Notch1lox/lox), grey bars = Notch1Δ (n = 6 corneas for each genotype over three independent experiments). Error bars represent standard deviation. (c) Immunofluorescence for pFAK, ROCK2 and YAP/TAZ on corneal tissue isolated from Notch1Δ mice treated with ophthalmic gel (control) or Tobradex during the repeated injury procedure. Data are representative of 6 corneas for each treatment analysed over three independent experiments. Scale bars represent 5 μm.
Supplementary Figure 7 Manipulation of mechanotransduction affects β-catenin expression in corneal epithelial cells.
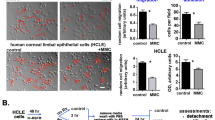
(a,b) Immunofluorescence for β-catenin, K12 and K1 (a) or YAP/TAZ, K12 and K1 (b) on PCESCs cultured on stiff (glass– >2 GPa) substrates and maintained in vehicle (PBS—upper panels) or 10 μM Y27632 (lower panels). Data are representative of 8 individual cultures for each condition. (c–e) Quantification of β-catenin expression (c), YAP/TAZ nuclear:cytoplasmic ratio (d) and the proportion of K12+K1− and K12−K1+ cells (e) in PCESCs maintained in vehicle (PBS) or 10 μM Y27632 (n = 8 individual cultures over four independent experiments). For (c) β-catenin expression is determined by mean fluorescence intensity. (f) Schematic depicting the transfection of TCF-Luc 293 T cells with pR2KD or pEGFP. (g) Western blot performed on TCF-Luc 293T cells 48 h after transfection with pR2KD or pEGFP. (h) Relative luciferase activity in TCF-Luc 293 T cells 48 hours after transfection (n = 6 individual transfections over three independent experiments). ∗P < 0.01, ∗∗P < 0.05, (unpaired, two tailed t-tests). Error bars represent standard deviation. Scale bars represent 20 μm.
Supplementary information
Supplementary Information
Supplementary Information (PDF 1350 kb)
Rights and permissions
About this article
Cite this article
Nowell, C., Odermatt, P., Azzolin, L. et al. Chronic inflammation imposes aberrant cell fate in regenerating epithelia through mechanotransduction. Nat Cell Biol 18, 168–180 (2016). https://doi.org/10.1038/ncb3290
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncb3290
- Springer Nature Limited
This article is cited by
-
Extracellular matrix stiffness mediates uterine repair via the Rap1a/ARHGAP35/RhoA/F-actin/YAP axis
Cell Communication and Signaling (2023)
-
Understanding Ocular Surface Inflammation in Tears Before and After Autologous Cultivated Limbal Epithelial Stem Cell Transplantation
Ophthalmology and Therapy (2023)
-
Collagen type I-mediated mechanotransduction controls epithelial cell fate conversion during intestinal inflammation
Inflammation and Regeneration (2022)
-
An overview of the crosstalk between YAP and cGAS-STING signaling in non-small cell lung cancer: it takes two to tango
Clinical and Translational Oncology (2022)
-
The common YAP activation mediates corneal epithelial regeneration and repair with different-sized wounds
npj Regenerative Medicine (2021)