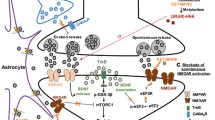
Abstract
Low doses of ketamine trigger rapid and lasting antidepressant effects after one injection in treatment-resistant patients with major depressive disorder. Modulation of AMPA receptors (AMPARs) in the hippocampus and prefrontal cortex is suggested to mediate the antidepressant action of ketamine and of one of its metabolites (2R,6R)-hydroxynorketamine ((2R,6R)-HNK). We have examined whether ketamine and (2R,6R)-HNK affect glutamatergic transmission and plasticity in the mesolimbic system, brain regions known to have key roles in reward-motivated behaviors, mood and hedonic drive. We found that one day after the injection of a low dose of ketamine, long-term potentiation (LTP) in the nucleus accumbens (NAc) was impaired. Loss of LTP was maintained for 7 days and was not associated with an altered basal synaptic transmission mediated by AMPARs and N-methyl-D-aspartate receptors (NMDARs). Inhibition of mammalian target of rapamycin signaling with rapamycin did not prevent the ketamine-induced loss of LTP but inhibited LTP in saline-treated mice. However, ketamine blunted the increase in the phosphorylation of the GluA1 subunit of AMPARs at a calcium/calmodulin-dependent protein kinase II/protein kinase C site induced by an LTP induction protocol. Moreover, ketamine caused a persistent increased phosphorylation of GluA1 at a protein kinase A site. (2R,6R)-HNK also impaired LTP in the NAc. In dopaminergic neurons of the ventral tegmental area from ketamine- or (2R,6R)-HNK-treated mice, AMPAR-mediated responses were depressed, while those mediated by NMDARs were unaltered, which resulted in a reduced AMPA/NMDA ratio, a measure of long-term synaptic depression. These results demonstrate that a single injection of ketamine or (2R,6R)-HNK induces enduring alterations in the function of AMPARs and synaptic plasticity in brain regions involved in reward-related behaviors.
Similar content being viewed by others
Introduction
A low dose of ketamine, given to treatment-resistant depressed patients, causes rapid antidepressant responses, which can last 3–14 days. Unfortunately, the usefulness of ketamine for the treatment of depression is limited because of the dissociative, psychotic and abuse properties of this drug.1,2,3,4 The antidepressant mechanism of action of ketamine has been proposed to be mediated through non-competitive antagonism at N-methyl-D-aspartate receptors (NMDARs) and subsequent activation of AMPA receptors (AMPARs).5 Furthermore, a recent study demonstrated antidepressant efficacy, with reduced side effects, of a metabolite of ketamine, (2R,6R)-hydroxynorketamine ((2R,6R)-HNK), through stimulation of AMPARs, independently of NMDAR antagonism.6 These data, along with data on the antidepressant effects of AMPAkines, implicate AMPARs as potent pharmacological targets for the development of effective treatment of depression.7 However, it should be noted that a recent study could not demonstrate antidepressant action of (2R,6R)-HNK in two mouse models of depression although ketamine was potent in alleviating depression-like symptoms in these models.8 Further research on the ability of ketamine and its metabolites to modulate AMPARs as a mechanism of rapid and lasting antidepressant actions is warranted. Several lines of evidence suggest that depression is associated with altered synaptic plasticity of excitatory synapses and that ketamine promotes AMPAR function and synaptogenesis.9,10,11,12,13 Thus, modulation of glutamatergic neurotransmission and plasticity in the hippocampus and medial prefrontal cortex is suggested to mediate the antidepressant action of ketamine.9,10,11,12,13 Both AMPARs and NMDARs are critical elements of forms of long-term synaptic plasticity such as long-term potentiation (LTP), a potential neurophysiological correlate of learning and memory.14,15 Whether ketamine induces lasting alterations of LTP and how these possible alterations occur are still unresolved questions. Furthermore, in addition to the hippocampus and prefrontal cortex, depression involves the mesolimbic dopamine system, brain regions critically implicated in reward-motivated behaviors, mood and hedonic drive.10,16 In particular, the glutamatergic inputs from the hippocampus and cortex to the nucleus accumbens (NAc) and dopaminergic (DA) innervation of the NAc from the ventral tegmental area (VTA) have key roles in these motivational behaviors. Recent structural studies using magnetic resonance imaging have reported enlarged NAc in patients with major depressive disorder which was normalized by ketamine in patients who responded to this antidepressant treatment.17 The antidepressant action of ketamine might involve lasting neuroadaptations in the NAc and VTA, but the underlying mechanisms have not been extensively investigated.
Our aims were to examine whether a single injection of a low dose of ketamine produces lasting changes in glutamatergic synaptic transmission or in synaptic plasticity in the NAc and VTA-DA neurons. We also examined whether ketamine alters the function of AMPARs and NMDARs in these brain regions. Our results demonstrate a lack of lasting effects of ketamine on NMDAR function in the NAc and VTA-DA neurons. Ketamine, however, induces lasting alterations in synaptic plasticity through modulation of AMPAR signaling and function in these brain regions, suggesting a potential role for AMPARs in the mesolimbic circuit in the prolonged antidepressant action of a single dose of ketamine.
Materials and methods
Experiments were approved by our local ethical committee (The Stockholm’s North Animal Experimentation Ethics Committee). All efforts were made to minimize animal suffering. Male C57BL6 mice aged 5–13 weeks received a single intraperitoneal injection of either vehicle (saline), (R,S)-ketamine (3 or 10 mg kg−1), (2R,6R)-HNK (10 mg kg−1) or pentobarbital (5 mg kg−1). Animals were randomly injected with either saline, ketamine, (2R,6R)-HNK or pentobarbital, and the experimenters were not blinded to the treatment administered to the mice. The behavioral effects of ketamine in rodents have been examined by several groups6,18,19,20,21 and therefore will not be investigated in this study. The doses of ketamine and (2R,6R)-HNK used in the present study were based on previous work demonstrating antidepressant actions of these compounds in animal models.6,18,19,20,21 (S)-ketamine has a stronger affinity for NMDARs than (R)-ketamine and has been tested in clinical trials for treatment-resistant depression.22 We have used (R,S)-ketamine, because the antidepressant action of ketamine may not be directly related to its ability to block NMDARs6 and because antidepressant actions have been described for both (R) and (S) enantiomers in models of depression.8,19 Twenty-four hours or 7 days following the injection, mice were killed for brain slice electrophysiology, western blotting or immunohistochemistry as described previously.23,24,25,26 Briefly, extracellular field potentials were recorded using a glass micropipette filled with extracellular solution positioned in the Core region of the NAc (Supplementary Figure 1). These synaptic responses, or field excitatory postsynaptic potentials/population spikes (fEPSP/PSs), were evoked by stimulation pulses applied to the brain slice through a concentric bipolar stimulating electrode placed near the recording electrode (Supplementary Figure 1). Whole-cell patch-clamp recordings of visually identified medium spiny projection neurons in the NAc and DA neurons in the VTA were made with patch electrodes filled with a cesium-based or potassium gluconate-based intracellular solution. The pipette tip was filled with 0.2% neurobiotin for post-recording identification of the cells in the VTA. AMPAR-mediated excitatory postsynaptic currents (EPSCs) were measured in the presence of gabazine (SR-95531, 10 μM) to block GABAA receptors at a holding membrane potential of −80 mV. NMDAR-mediated EPSCs were measured at a holding membrane potential of +40 mV in the presence of gabazine (SR-95531, 10 μM) and DNQX (10 μM) to block AMPARs. EPSCs were evoked by electrical stimulation through a patch pipette filled with extracellular solution placed near the recorded neuron. The AMPA/NMDA ratio was calculated by dividing the amplitude of the EPSC measured at −80 mV (AMPA-EPSC) with the amplitude of the EPSC measured at +40 mV in the presence of DNQX (NMDA-EPSC). Data are expressed as mean±s.e.m. with n indicating the number of slices, neurons or mice tested (for exact numbers of slices, neurons and mice examined, see Results section). No statistical methods were used to estimate sample size and outliers were not excluded from the analyses. Statistical significance of the results was assessed by using the Student’s t-test for paired and unpaired observations, Mann–Whitney test, one-way analysis of variance followed by Dunnett’s multiple comparison test or Fisher’s exact test. For details on Materials and Methods, see Supplementary Information.
Results
Ketamine induces lasting impairment of LTP in the NAc
We have examined whether a low dose of ketamine impacts the induction of LTP, an NMDAR-dependent lasting increase in glutamatergic synaptic strength, in the NAc.27,28 Mice received a single intraperitoneal injection of either saline or ketamine (3 or 10 mg kg−1) 1 day or 7 days before the electrophysiological experiments were performed. These time points were chosen, because we wanted to address the lasting effect of ketamine beyond the acute blockade of NMDARs by ketamine, which would inhibit LTP. Furthermore, the antidepressant response seen in patients and preclinical studies is observed within hours after the injection and maintained for at least 1 week.11 Examination of the effects of ketamine and (2R,6R)-HNK administered at shorter time points would most likely have resulted in inhibition of LTP induction due to blockade of NMDARs. Indeed, ketamine and its metabolites, in particular (2R,6R)-HNK, are still present in plasma and brain 30–60 min after their injection.29 We did not examine the effect of chronic administration of ketamine or (2R,6R)-HNK, because antidepressant actions are observed following a single injection and chronic ketamine treatment has no effect on depression-like behavior.30 We measured fEPSP/PSs mediated by AMPARs in the core region of the NAc in brain slices as described previously28 (Supplementary Figure 1). When a stable baseline fEPSP/PS amplitude was obtained, we applied a high-frequency stimulation (HFS) consisting of three trains (1 s duration) at 100 Hz with a 10 s inter-train interval. Single stimulation was thereafter resumed. In mice that received an injection of saline 24 h or 7 days before the recordings were made, HFS induced a long-lasting potentiation of the fEPSP/PS amplitude or LTP (% of baseline 55–60 min after HFS, 24 h: 133.6±7.4; n=12; P<0.01, paired Student’s t-test; Figure 1a and e; 7 days: 133.3±11.2; n=13; P<0.05, paired Student’s t-test; Figure 2a and d). In the NAc of ketamine-treated mice the magnitude of LTP was significantly decreased. One day after the injection of 3 mg kg−1 ketamine, the amplitude of the fEPSP/PS measured 55–60 min after HFS was 118.4±8.7% of baseline (n=9; P>0.05, paired Student’s t-test; Figure 1b and e). There was a tendency for a reduced inhibition of LTP 7 days after the injection of 3 mg kg−1 ketamine (% of baseline: 116.7±6.9; n=13; P<0.05, paired Student’s t-test; Figure 2b and d). A dose of 10 mg kg−1 induced a stronger and longer-lasting inhibition of LTP (% of baseline, 24 h: 109.9±6.7; n=15; P>0.05, paired Student’s t-test; Figure 1c and e; 7 days: 103.8±4.7; n=12; P>0.05, paired Student’s t-test; Figure 2c and d). (2R,6R)-HNK (10 mg kg−1) injected 1 day before the electrophysiological experiments were performed also inhibited LTP induction in the NAc (% of baseline: 103.6±6.9, n=10, P>0.05, paired Student’s t-test; Figure 1d and e). In addition, ketamine and (2R,6R)-HNK decreased not only the magnitude of LTP but also the number of slices that showed LTP (Figures 1f and 2e). These results demonstrate that ketamine impairs LTP induction in the NAc in a dose- and time-dependent manner. Indeed, the reduction in the magnitude of LTP is maintained seven days after a single injection of ketamine. Our results also show that a metabolite of ketamine impairs LTP in the NAc. Impairment of LTP is not due to the anesthetic properties of ketamine because a single injection of another anesthetic drug, pentobarbital (5 mg kg−1), did not inhibit LTP (Supplementary Figure 1).
Long-term potentiation (LTP) in the nucleus accumbens (NAc) is impaired 1 day after injection of ketamine and (2R,6R)-hydroxynorketamine ((2R,6R)-HNK). (a–d) Graphs show the mean±s.e.m. amplitude of the field excitatory postsynaptic potentials/population spikes (fEPSP/PSs) measured in the NAc, expressed as a percentage of baseline, before and after high-frequency stimulation (HFS), applied at the time indicated by the arrow. LTP was induced in mice treated with a single injection of saline (a, n=12), but was reduced in mice treated with ketamine 3 mg kg-1 (b, n=9), ketamine 10 mg kg−1 (c, n=15) or (2R,6R)-HNK (d, n=10) one day after the injection. Representative records of fEPSP/PSs measured in four slices at the time points indicated on the graphs are shown above the graphs. (e) Average effect of ketamine and (2R,6R)-HNK on the magnitude of LTP in the slices presented in (a–d). # P<0.05 one-way analysis of variance (ANOVA), Dunnett’s multiple comparison test. **P<0.01 paired Student’s t-test. (f) Percentage of slices that showed LTP or no LTP in saline-, ketamine- and (2R,6R)-HNK-treated mice. ## P<0.01, Fisher’s exact test.
Lasting inhibition of long-term potentiation (LTP) induction in the nucleus accumbens (NAc) 7 days after the administration of ketamine. (a–c) Mean±s.e.m. amplitude of the field excitatory postsynaptic potentials/population spikes (fEPSP/PSs), expressed as a percentage of baseline, before and after high-frequency stimulation (HFS) in mice treated with a single injection of saline (a, n=13), ketamine 3 mg kg−1 (b, n=13) or 10 mg kg-1 (c, n=12) 7 days after the injection. (d) Average effect of ketamine on the magnitude of LTP in the slices presented in (a–c). # P <0.05 one-way analysis of variance (ANOVA), Dunnett’s multiple comparison test. *P<0.05 paired Student’s t-test. (e) Percentage of slices that demonstrated LTP or no LTP in saline- and ketamine-treated mice. # P<0.05, Fisher’s exact test.
Ketamine does not alter basal glutamatergic synaptic transmission in the NAc
We then investigated potential mechanisms underlying the impairment of LTP induced by ketamine. We first examined whether ketamine altered the basic properties of glutamatergic synaptic transmission. We found that input/output curves of fEPSP/PSs amplitude were similar in mice treated with either saline, ketamine or (2R,6R)-HNK 1 day or 7 days following the injection (Supplementary Figure 1). The paired-pulse ratio of two successive fEPSP/PSs, a measure of presynaptic modulation of glutamate release, was not affected by ketamine either (Supplementary Figure 1). We further examined a potential effect of ketamine on glutamatergic synaptic transmission by performing whole-cell patch clamp recordings of individual projection neurons in the NAc 1 day after injection of either saline or ketamine (10 mg kg−1). Spontaneous AMPAR-mediated EPSCs (sEPSCs) were measured in cells voltage-clamped at −80 mV. The frequency and amplitude of sEPSCs were similar in saline- and ketamine-treated mice (frequency (Hz): saline 1.36±0.26; n=15; ketamine 1.09±0.22; n=14. P>0.05, Mann–Whitney test; amplitude (pA): saline 16.7±0.8; n=15; ketamine 17.7±1.3; n=14; P>0.05, Mann–Whitney test; Figure 3a). We also measured AMPAR-mediated EPSCs evoked by electrical stimulation of the slice in individual projection neurons in the NAc voltage-clamped at −80 mV. Ketamine did not alter the paired-pulse ratio of two consecutive EPSCs (saline: 1.4±0.1; n=11; ketamine: 1.6±0.1; n=16: P>0.05, Mann–Whitney test; Figure 3b).
Ketamine does not alter basal glutamatergic synaptic transmission in the nucleus accumbens (NAc). (a) The frequency and amplitude of spontaneous excitatory postsynaptic currents (EPSCs) measured with whole-cell patch clamp recording in individual projection neurons in the NAc were similar in saline- and ketamine-treated mice (saline: n=15; ketamine 10 mg kg−1 1 day: n=14). Representative recordings of spontaneous EPSCs (sEPSCs) in two neurons are shown on the left. (b) The paired-pulse ratio of two successive evoked EPSCs was not altered by ketamine (saline: n=11; ketamine: n=16). (c) The ratio between AMPA receptor (AMPAR)- and N-methyl-D-aspartate receptor (NMDAR)-EPSCs was unchanged (saline: n=9; ketamine: n=9). (d) Ketamine did not alter the contribution of GluN2B to synaptic NMDARs as shown by a similar inhibition of the NMDAR-EPSC induced by the GluN2B antagonist Ro 25–6981 (saline: n=7; ketamine: n=10). (e) Ketamine did not alter the protein amounts of GluN1 and GluN2B in the NAc (n=13 and 15 mice). (f) Immunofluorescence of GluN2B was similar in the NAc of saline- and ketamine-treated mice.
Glutamatergic synapses in the NAc have functional NMDARs, which contribute to synaptic transmission and LTP.27,31 In order to assess whether these synaptic NMDARs were affected by ketamine, we measured EPSCs mediated by NMDARs in neurons voltage-clamped at +40 mV. The ratio between AMPAR-EPSC and NMDAR-EPSC, a measure of long-term synaptic plasticity, was unaltered by ketamine (saline: 2.5±0.3; n=9; ketamine 10 mg kg-1: 2.0±0.3; n=9; P>0.05, Mann–Whitney test; Figure 3c). The pharmacological and biophysical properties of NMDARs are critically determined by the GluN2 subunits they contain.32,33 The GluN2B subunit is the predominant GluN2 subunit in the NAc and forms functional NMDARs at glutamatergic synapses.31,34 In addition, antagonism of NMDARs that contain the GluN2B subunit were suggested to have beneficial antidepressant actions.3,11 Therefore, we examined whether ketamine altered the contribution of GluN2B to functional NMDARs in the NAc. The GluN2B-containing NMDAR antagonist Ro 25–6981 (1 μM) applied in the perfusion solution reduced the amplitude of NMDAR-EPSCs to 36.2±6.5% of baseline in saline-treated mice (n=7) and to 34.9±3.7% of baseline in mice treated with ketamine 10 mg kg−1 (n=10; P>0.05. compared with saline, Mann–Whitney test, Figure 3d). Thus, ketamine does not affect the contribution of GluN2B to synaptic NMDARs in the NAc. Using western blotting, we examined the protein levels of GluN2B and of the obligatory subunit GluN1. We found that the amounts of these two subunits in the NAc were not altered by ketamine (Figure 3e). Using immunohistochemistry, we found that the distribution of cells that contained GluN2B in the core region of the NAc was similar in saline- and ketamine-treated mice both 1 day (Figure 3f) and 7 days (Supplementary Figure 2) after the injection. In order to further substantiate our findings, we have examined the contribution of GluN2A, the other GluN2 subunit present in projection neurons in the NAc.31 There was no significant difference in the ability of the GluN2A antagonist TCN-201 (10 μM) to reduce the amplitude of the NMDAR-EPSC in saline- and in ketamine-treated mice, but there was a small population of neurons which were not sensitive to TCN-201 in ketamine-treated mice (Supplementary Figure 3). Together, these results show that the basic properties of synaptic transmission in the NAc, that is, glutamate release and synaptic responses mediated by AMPARs or NMDARs, are unaffected following ketamine administration.
Mechanisms that mediate the blockade of LTP induction by ketamine
Ketamine has been shown to increase protein levels of brain-derived neurotrophic factor (BDNF) in the hippocampus.20 This increase is transient and the levels of BDNF return to control values after 24 h. We found that one day after the injection of ketamine (10 mg kg−1), the levels of BDNF were not altered in the NAc as compared with saline-treated mice (Supplementary Figure 4). Ketamine activates mammalian target of rapamycin (mTOR) signaling.35,36,37,38 We therefore examined the possibility that inhibition of mTOR with rapamycin could prevent ketamine-induced impairment of LTP. We found that in the presence of rapamycin in the perfusion solution, LTP remained impaired in the NAc of ketamine-treated mice (10 mg kg−1 1 day; without rapamycin: 109.9±6.7; n=15; with rapamycin: 200 nM: 109.5±9.1; n=9; with rapamycin: 1 μM: 95.1±9.4; n=5; P>0.05, one-way analysis of variance, Dunnett’s multiple comparison test; Figure 4a). mTOR regulates protein synthesis and plasticity changes that might contribute to learning and memory.39,40,41 Thus, mTOR is also likely to have a role in the maintenance of LTP. In line with this possibility, rapamycin was shown to block early-phase LTP and late-phase LTP in the hippocampus39,42,43 and in the medial prefrontal cortex.41 We therefore examined the contribution of mTOR in the induction of LTP in the NAc of saline-treated mice. We found that rapamycin applied in the perfusion solution dose-dependently inhibited LTP induction (without rapamycin: 133.6±7.4; n=12; with rapamycin: 200 nM: 110.8±7.6; n=14; with rapamycin: 1 μM: 104.9±5.7; n=8; P<0.05, one-way analysis of variance, Dunnett’s multiple comparison test; Figure 4b). These results suggest that activation of mTOR contributes to LTP induction in the NAc. As both ketamine and HFS activate mTOR, ketamine might occlude further synaptic potentiation of glutamatergic transmission induced by HFS. Given that synaptic transmission is not affected by ketamine, a mechanism other than occlusion is likely to be involved in the ketamine-induced impairment of LTP.
Involvement of mammalian target of rapamycin (mTOR) and phosphorylation of GluA1 in long-term potentiation (LTP) induction and its impairment by ketamine. (a and b) Mean±s.e.m. amplitude of the field excitatory postsynaptic potentials/population spikes (fEPSP/PSs) before and after high-frequency stimulation (HFS) in the presence of the mTOR inhibitor rapamycin (200 nM and 1 μM) applied in the perfusion solution as indicated by the horizontal bars. Mice received a single injection of ketamine 10 mg kg−1 (a) or saline (b) 1 day before the recordings were performed. Bar graphs show the average effect of rapamycin on LTP in ketamine-treated mice (a, control slices: n=15, rapamycin 200 nM: n=9; rapamycin 1 μM: n=5) and in saline-treated mice (b, control slices: n=12, rapamycin 200 nM: n=14; rapamycin 1 μM: n=8). #P<0.05 one-way analysis of variance (ANOVA), Dunnett’s multiple comparison test. **P<0.01, paired Student’s t-test. (c) Upper graphs show the average amounts of total GluA1, phospho-Ser831-GluA1 and phospho-Ser845-GluA1 in control slices (which did not receive HFS) normalized to the values in saline-treated mice (n=9–11 mice). Lower graphs show the amounts of total GluA1, phospho-Ser831-GluA1 and phospho-Ser845-GluA1 in slices that received HFS, normalized to the values in control slices. #P<0.05 unpaired Student’s t-test. *P<0.05 paired Student’s t-test. Examples of western blottings are shown on the right.
Long-term synaptic plasticity has been associated with changes in the phosphorylation of the GluA1 subunit of AMPARs at two residues: Ser831 which is phosphorylated by calcium/calmodulin-dependent protein kinase II (CaMKII) or protein kinase C (PKC), and Ser845, which is phosphorylated by cyclic-AMP-dependent protein kinase A. Phosphorylation of GluA1 was shown to target AMPAR at the synapse, to increase channel conductance and to modulate LTP induction.44,45,46 Interestingly, chronic stress and administration of ketamine were found to modulate the phosphorylation of GluA1 in the hippocampus5,38 and amygdala.47 We therefore examined the possibility that a potential mechanism for LTP induction by HFS and inhibition by ketamine involved an altered phosphorylation of GluA1 in the NAc. We performed western blotting experiments with slices from which the NAc was dissected and frozen, and we found that ketamine did not affect the total levels of GluA1 or Ser831-GluA1 phosphorylation. However, HFS increased the amount of Ser831-GluA1 phosphorylation in saline-treated mice but not in ketamine-treated mice (Figure 4c). We also found that ketamine increased Ser845-GluA1 phosphorylation in the NAc as compared to saline-treated mice. HFS did not modify Ser845-GluA1 phosphorylation in saline- or ketamine-treated mice (Figure 4c). These results demonstrate that LTP is associated with an increase in the phosphorylation of Ser831-GluA1, but not Ser845-GluA1, in saline-treated mice. Ketamine impairs HFS-induced phosphorylation of Ser831-GluA1 but promotes the phosphorylation of Ser845-GluA1.
Ketamine reduces AMPAR-mediated transmission in VTA-DA neurons and does not affect NMDARs
Given that VTA-DA neurons are involved in reward-related behaviors, we examined whether ketamine alters glutamatergic transmission in these neurons by performing whole-cell patch-clamp recordings in the VTA. We confirmed that the recorded neurons in the VTA were DA, and not non-DA, neurons by applying neurobiotin through diffusion from the intracellular solution in the recording pipette. Using immunohistochemistry, we found that the recorded neurons contained both neurobiotin and tyrosine hydroxylase, the rate-limiting enzyme in the synthesis of dopamine (Figure 5a and Supplementary Figure 5). Neurons were also identified based on their well-described membrane characteristics and action potential firing (Supplementary Figures 5 and 6). Previous studies have reported that the electrophysiological membrane properties of VTA neurons and the location of these neurons within the VTA differed between those projecting to the NAc and those projecting to the prefrontal cortex.48,49,50 Moreover, the VTA contains few glutamatergic neurons which are located more medially in the VTA.51,52 On the basis of the location of the recorded neurons in the VTA (mostly lateral and not medial), their spontaneous firing and membrane properties (for example, large I h, afterhyperpolarization and excitability profile, see Supplementary Figures 5 and 6), it is likely that DA neurons, and not glutamatergic neurons, in the VTA that project to the NAc, and not to the cortex, were examined in the present study.
Ketamine induces a form of long-term depression in ventral tegmental area (VTA)-dopaminergic (DA) neurons. (a) Confocal images showing double immunofluorescence for tyrosine hydroxylase (TH) (red) and neurobiotin (green), demonstrating that the recorded neuron in the VTA was DA. (b) The frequency and amplitude of spontaneous excitatory postsynaptic currents (EPSCs) measured with whole-cell patch clamp recordings of individual VTA-DA neurons were decreased in ketamine-treated mice (saline: n=15; ketamine 10 mg kg-1 one day: n=21). *P<0.05, **P<0.01, Mann–Whitney test. (c) The paired-pulse ratio of two successive evoked EPSCs (inter-stimulus interval: 30 ms) was not altered by ketamine (saline: n=21; ketamine: n=13). (d) The AMPA/N-methyl-D-aspartate (NMDA) ratio was decreased in ketamine-treated mice (saline: n=26; ketamine: n=13). **P<0.01, Mann–Whitney test. (e) The amounts of GluA1, phospho-Ser831-GluA1 and phospho-Ser845-GluA1 were unaltered by ketamine (n=9–11 mice). (f) Ketamine did not alter the contribution of GluN2B to synaptic NMDA receptors (NMDARs) (saline: n=14; ketamine: n=9). (g) The amounts of GluN1 and GluN2B were not altered by ketamine (n=9–11 mice). (h) Localization of GluN2B in VTA-DA neurons was similar in saline- and ketamine-treated mice.
The membrane properties of VTA-DA neurons were similar in mice treated with saline, ketamine or (2R,6R)-HNK (Supplementary Figures 5 and 6). In VTA-DA neurons recorded from mice treated with ketamine (10 mg kg−1) or (2R,6R)-HNK (10 mg kg−1), the spontaneous action potential firing, measured in cell-attached mode, the I h current and afterhyperpolarization were not significantly different from those measured in neurons from saline-treated mice 1 day after the injection (Supplementary Figures 5 and 6). Pentobarbital (5 mg kg−1) did not affect the membrane properties and firing of VTA-DA neurons one day after the injection (Supplementary Figure 5).
We measured glutamatergic synaptic transmission in VTA-DA neurons 1 day after intraperitoneal injection of saline, ketamine or (2R,6R)-HNK. We found that ketamine 3 mg kg−1 did not modify AMPAR-mediated glutamatergic synaptic transmission (Supplementary Figure 7). However, ketamine 10 mg kg−1 depressed both the frequency (0.47±0.07 Hz) and the amplitude (22.88±1.89 pA; n=21) of sEPSCs as compared with saline-treated mice (frequency: 0.98±0.19 Hz; n=15; P<0.01, Mann–Whitney test; amplitude: 30.87±2.67 pA; n=15; P<0.05, Mann–Whitney test; Figure 5b). (2R,6R)-HNK (10 mg kg−1) also reduced the frequency and the amplitude of sEPSCs as compared with saline-treated mice (Supplementary Figure 7). The amplitude, but not frequency, of miniature EPSCs measured in the presence of tetrodotoxin (0.5 μM) was decreased in ketamine-treated mice as compared with saline-treated mice (Supplementary Figure 7). We measured evoked EPSCs mediated by AMPARs and NMDARs. Ketamine did not alter the ratio between the amplitude of two consecutive AMPAR-EPSCs (saline: 0.78±0.04; n=21; ketamine; 0.88±0.04; n=13; P>0.05, Mann–Whitney test; Figure 5c). In addition, the ratio between AMPAR-EPSCs and NMDAR-EPSCs was decreased in ketamine-treated mice as compared with saline-treated mice (saline: 2.89±0.25; n=26; ketamine: 1.68±0.25; n= 13; P<0.01, Mann–Whitney test; Figure 5d). (2R,6R)-HNK (10 mg kg−1) also reduced the AMPA/NMDA ratio as compared with saline-treated mice (Supplementary Figure 7). The decrease in the frequency of sEPSCs suggests a possible presynaptic action of ketamine, but might also be due to the decrease in the amplitude of individual events. Indeed, the decrease in the amplitude of sEPSCs and miniature EPSCs, the lack of effect of ketamine on the paired-pulse ratio and the decrease in the AMPA/NMDA ratio all suggest a postsynaptic action of ketamine. The total amounts of GluA1, phospho-Ser831-GluA1 and phospho-Ser845-GluA1 were unaffected by ketamine administration (Figure 5e). The levels of BDNF were not altered in the VTA as compared with saline-treated mice (Supplementary Figure 4). Thus, ketamine induces a form of long-term synaptic depression of AMPAR-mediated synaptic responses in VTA-DA neurons, which does not involve a decrease in the amounts, or phosphorylation, of GluA1.
We found that the contribution of GluN2B to synaptic NMDARs in VTA-DA neurons was similar in saline- and ketamine-treated mice. Indeed, Ro 25–6981 (1 μM) decreased the amplitude of NMDAR-EPSCs to 36.4±3.6% of baseline in saline-treated mice (n=6) and to 45.7±4.4% of baseline in ketamine-treated mice (n=7; P>0.05, Mann–Whitney test; Figure 5f). Ketamine did not alter the total amounts of GluN1 and GluN2B or the expression of GluN2B in VTA-DA neurons (Figure 5g, h and Supplementary Figure 2). The contribution of GluN2D to synaptic NMDARs in VTA-DA neurons was similar in ketamine- and saline-treated mice (Supplementary Figure 3). These results demonstrate that ketamine does not alter the functional properties of NMDARs in VTA-DA neurons.
Discussion
The principal aim of our study was to determine if a single, low dose of ketamine induces lasting modulation of the function of AMPARs and NMDARs in the NAc and VTA, two brain regions involved in reward-related behaviors, mood and hedonic drive. Our study demonstrates that ketamine inhibits the function of AMPARs, but not NMDARs, in the mesolimbic DA circuit. Although ketamine does not affect basal glutamatergic synaptic transmission in the NAc, this compound induces lasting inhibition of LTP. Ketamine may blunt increases in glutamatergic synaptic transmission in the NAc under situations of intense activity in glutamatergic inputs, and may promote other forms of synaptic plasticity. Ketamine also induces a form of long-term depression (LTD) in VTA-DA neurons that might lead to decreased activity in these neurons and decreased DA modulation of the NAc. Our results also demonstrate that the metabolite of ketamine, (2R,6R)-HNK, mimics the effects of ketamine on AMPAR function in the NAc and VTA-DA neurons.
Long-term changes in glutamatergic synaptic strength such as LTP are potential candidates for cellular mechanisms of learning and memory. These forms of synaptic plasticity might be impaired in disease states and modulated by various pharmacological treatments. Our results demonstrate that an induction protocol that induces LTP in the NAc of saline-treated mice fails to induce LTP in mice treated with a single, low dose of ketamine. This impairment is observed one day post injection and is maintained after seven days. Recent observations demonstrate that a metabolite of ketamine, (2R,6R)-HNK, affects AMPAR function through a mechanism independent of NMDAR inhibition, suggesting that the initial antagonism of NMDARs by ketamine is not an obligatory step in the antidepressant action of this compound.6 Our results demonstrate that, like ketamine, (2R,6R)-HNK impairs LTP induction in the NAc. Ketamine and (2R,6R)-HNK may inhibit LTP induction in an NMDAR-independent manner, or through a mechanism downstream of NMDAR blockade. These potential mechanisms remain to be identified. Importantly, our present results indicate that this effect of ketamine does not involve an altered function of NMDARs, significant factors in LTP induction. Indeed, the amount and expression of the main subunits that compose functional NMDARs in projection neurons of the NAc, that is, GluN1 and GluN2B, are unchanged by ketamine as shown immunohistochemically, with western blot experiments and with electrophysiological analysis of NMDAR-mediated EPSCs. We found that GluN2A did not contribute to synaptic NMDAR-EPSCs in a small population of NAc neurons in ketamine-treated mice. This might be due to a specific effect of ketamine in this neuronal population, which remains to be identified. Another probable explanation is the exclusive contribution of GluN2B to synaptic NMDARs, as shown by the large inhibitory action of the GluN2B antagonist in a small number of neurons. Nevertheless, our results suggest that a low dose of ketamine does not alter the molecular identity of NMDARs in most NAc neurons.
Ketamine was shown to activate the mTOR signaling pathway and to facilitate new protein synthesis. This may contribute to increased glutamatergic transmission by insertion of AMPARs at synapses in the hippocampus and medial prefrontal cortex.3,11,38 In the NAc, we found that LTP in saline-treated mice is blocked by an mTOR inhibitor, rapamycin, suggesting a role for mTOR in this form of synaptic plasticity. In line with this possibility, an LTP induction protocol was shown to increase mTOR phosphorylation in the medial prefrontal cortex.41 The observation that rapamycin does not prevent impairment of LTP in ketamine-treated mice, suggests that the lasting blockade of LTP by ketamine does not involve a lasting inhibition of mTOR or that mechanisms downstream of mTOR activation mediate the blockade of LTP by ketamine. Alternatively, rapamycin and ketamine might impair LTP through distinct pathways. In addition, (2R,6R)-HNK was shown to modulate AMPAR function in the hippocampus without enhancing mTOR phosphorylation.6 Whether ketamine and (2R,6R)-HNK impair LTP induction in the NAc through mTOR signaling pathway remains to be determined. The actions of ketamine and HFS are not occlusive because we did not observe any potentiation of AMPAR-mediated responses with single-cell recordings or with field recordings in the NAc. Thus, ketamine does not modify basal glutamatergic synaptic transmission and does not seem to promote targeting of AMPARs to the synapse under normal conditions (that is, with no intense activity in glutamatergic fibers). Hebbian modifications of synaptic transmission such as LTP, well described in the hippocampus and cortex, involve the activation of NMDARs and subsequent phosphorylation of AMPARs by CaMKII/PKC.14,15,44,46 In the NAc, we previously found that LTP is dependent on NMDARs27 and we now demonstrate that LTP induction involves the activation of CaMKII/PKC as well as mTOR. Indeed, in saline-treated mice, LTP is inhibited by rapamycin and is associated with an increase in the phosphorylation of GluA1 at a CaMKII/PKC site (Ser831). Interestingly, we found that this phosphorylation and the induction of LTP are blunted in ketamine-treated mice. These results demonstrate that ketamine inhibits Hebbian modifications in the NAc through an intracellular mechanism that leads to a site-specific impairment of CaMKII/PKC activation and phosphorylation of the GluA1 subunit of AMPARs. Interestingly, ketamine does not affect the basal phosphorylation of Ser831-GluA1, suggesting that different signaling pathways are involved under normal activity as compared with that under intense activity. Future experiments with mice bearing a targeted alanine substitution of Ser831-GluA1, to prevent phosphorylation of this residue, in the NAc, will provide further evidence for the involvement of the CaMKII/PKC pathway in the antidepressant action of ketamine. In addition, several signal transduction pathways, which remain to be identified, are likely involved in mediating the action of ketamine and in stress- and depression-induced alterations of synaptic plasticity.53 Our results also show that ketamine increases the phosphorylation of GluA1 at a protein kinase A site (Ser845). Although phosphorylation of Ser845-GluA1 has a role in increasing channel conductance and insertion of AMPARs at the synapse,44,45 we did not find a change in the basal properties of synaptic transmission in ketamine-treated mice. Several reports have demonstrated that ketamine, and also (2R,6R)-HNK, applied in the perfusion solution enhance AMPAR-mediated synaptic transmission in the hippocampus.6,20,38,54,55,56,57,58 Other reports demonstrate a lack of effect of this treatment in the same brain region59 and suggest that the acute effect of ketamine is dependent on the concentration of this compound used and the location of the recording within the hippocampus (somatic vs dendritic recordings).58 The ketamine-induced increase in hippocampal synaptic transmission is mimicked or blocked by NMDAR antagonists55,57,58 and requires presynaptic NMDARs.54 Furthermore, the increased glutamatergic transmission is not long-lasting, because the EPSP returns to baseline 2–3 h after ketamine perfusion.54 Zhang et al. 26,38,54 further demonstrated that ketamine applied in the perfusion solution or administered intraperitoneally increases the phosphorylation of Ser845-GluA1 and the expression of total GluA1 in the hippocampus. Our observations in the NAc were made using an experimental paradigm different from the studies in the hippocampus. Together, these different studies demonstrate that the effect of ketamine is time-dependent and region-specific. The fact that we did not observe an increased glutamatergic transmission in the NAc one day after the injection of ketamine, although the phosphorylation of Ser845-GluA1 is increased, indicates that the ketamine-induced alterations in the phosphorylation of GluA1 are critical, lasting effects, which warrant further investigation. An alternate explanation is the possibility that increased phosphorylation of Ser845-GluA1 primes glutamatergic synapses for another form of LTP.60 For example, acute administration of ketamine is suggested to increase dopamine levels in NAc,61,62 which in turn could stimulate D1 receptors resulting in increased phosphorylation of Ser845-GluA1. Other mechanisms such as homeostatic plasticity might also contribute to the action of ketamine.11,63 An alternative explanation is that the ketamine-induced increase in protein kinase A-mediated Ser845-GluA1 phosphorylation might allow for an amplified LTD through dephosphorylation of Ser845-GluA1 by protein phosphatases.46 Consistent with this hypothesis, we found that ketamine potentiates LTD in the NAc (unpublished observations). Moreover, in chronic stress models of depression, LTD in the NAc is disrupted in susceptible mice64 and induction of LTD in the afferents to the NAc from the ventral hippocampus has a pro-resilient effect.65 Taken together, the aforementioned results and our findings support the possibility that ketamine prevents potentiation of glutamatergic synapses in conditions of intense activation of glutamatergic inputs and oppose a loss of synaptic depression induced by, for example, chronic stress.
We also observed that ketamine and (2R,6R)-HNK depress glutamatergic synaptic transmission onto VTA-DA neurons. Thus, ketamine and (2R,6R)-HNK induce a form of LTD, which does not seem to involve a change in the composition and function of NMDARs in VTA-DA neurons. The mechanism by which ketamine and (2R,6R)-HNK induce LTD involves a postsynaptic locus of action and AMPARs. Although we did not find that ketamine modified the amounts or phosphorylation of GluA1, it is likely to be that internalization of AMPARs or a change in their molecular identity mediate ketamine-induced LTD. In fact, a form of NMDAR-independent LTD has been demonstrated in VTA-DA neurons that is induced by the activation of group I metabotropic glutamate receptors (mGluRs), a switch in the subunit composition of AMPARs and a redistribution of AMPARs from synaptic to extrasynaptic or intracellular locations.66,67 Interestingly, group I mGluRs, in particular mGluR5, are potential targets for the development of antidepressants.68 Both NMDARs and AMPARs are regulated by mGluR5 through intracellular mechanisms,69 and mGluR5 deletion induces anti-depressive-like behavior in young mice.70 The function of ketamine-induced LTD in VTA-DA neurons might be to protect neurons against excessive firing activity. In a social defeat stress model of depression, the firing and excitability of VTA-DA neurons were shown to be increased in susceptible mice but unaltered or decreased in resilient mice.50,71 Phasic activation of VTA-DA neurons that project to the NAc is also pro-susceptible while inhibition of this pathway is pro-resilient in a social-defeat-stress model of depression.72 Our results are in favor of decreased glutamatergic input in VTA-DA neurons as a potential antidepressant mechanism of action of ketamine. Earlier electrophysiological studies in the anesthetized rat have shown that ketamine restores the decreased population activity of VTA-DA neurons in helpless rats, in a region- and time-dependent manner.61 Acute administration of ketamine increased the number of spontaneously active neurons in the VTA through AMPARs.62 These observations are not inconsistent with our results because we examined the effect of ketamine one day after its injection. The lasting effect of ketamine on population activity in all parts of the VTA and the involvement of AMPARs remain to be determined.
The finding that ketamine and (2R,6R)-HNK induce lasting changes in basal glutamatergic synaptic transmission in the VTA but not in the NAc suggest a synapse-specific action of these compounds. Indeed, glutamatergic inputs to these two nuclei arise from several different brain regions, that is, prefrontal cortex, amygdala, thalamus and hippocampus for the NAc, and medial prefrontal cortex, pedunculopontine tegmentum, lateral habenula, hypothalamus, bed nucleus of the stria terminalis, laterodorsal tegmental area and dorsal raphe for the VTA.73,74,75,76 Ketamine might specifically alter one or several of these excitatory inputs to the VTA but not the excitatory inputs to the NAc. In addition, trafficking of AMPARs, in particular those containing or lacking the GluA2 subunit, at specific glutamatergic synapses might underlie the modulatory action of ketamine specifically in the VTA.77
The doses (3 and 10 mg kg −1) of ketamine and (2R,6R)-HNK used in the present study were based on previous work demonstrating antidepressant actions of these compounds in animal models.6,18,19 Sub-anesthetic doses of ketamine administered to healthy volunteers induce cognitive effects and psychosis, which last during the duration of ketamine infusion and up to 2 h.78,79 Ketamine exacerbates psychotic symptoms in patients with schizophrenia and the duration of this effect is short-lasting.80,81,82 Higher doses of ketamine are usually required to induce locomotor stimulation in rodent models of psychosis.83 Interestingly, lasting changes in synaptic plasticity have been observed in the hippocampus following administration of a single dose of NMDAR antagonists, in particular MK801, in animal models of acute psychosis.84 Therefore, we cannot totally rule out the possibility that the synaptic changes observed in our study do not relate to the dissociative, psychotic and/or abuse properties of ketamine. We cannot be certain that the alterations in synaptic plasticity induced by ketamine reported here underlie antidepressant action of this drug. Indeed, in this study, we did not correlate our electrophysiological observations with behavioral alterations induced by ketamine or (2R,6R)-HNK, because the latter have been described in several other published studies and the doses used are well described for producing antidepressant actions in rodent models.6,19,85
The role of ionotropic glutamate receptors in the NAc and VTA, and the involvement of these brain regions in mediating the effects of ketamine have not been extensively examined. To better disentangle the role of the AMPARs and NMDARs in the VTA-NAc circuit in the therapeutic versus side effects of ketamine, future electrophysiological and behavioral studies with, for example, conditional mice with ablation of specific AMPAR or NMDAR subunits in the VTA and NAc are needed. To our knowledge, such studies have not been performed, but the impact of deletion of AMPAR and NMDAR subunits in other neuronal circuitries on behavior and synaptic transmission have been performed. For example, deletion of GluN2B in principal cortical neurons mimics and occludes the actions of ketamine on behavior, glutamatergic synaptic transmission and protein synthesis.86 Knockdown of GluN2B in the bed nucleus of the stria terminalis also mimics the affective effect of ketamine87 and deletion of GluA1 in glutamatergic neurons during adolescence induces behavioral alterations that resemble schizophrenia-like abnormalities but not depression- or anxiety-like alterations.88,89 Knock-in mice in which Ser845-GluA1 is replaced by alanine demonstrate loss of ketamine-induced synaptic potentiation in the hippocampus and impaired behavioral improvement induced by ketamine.54 Future studies examining the effect of ketamine on behavior and LTP induction in the NAc of mice with a targeted alanine substitution of Ser831-GluA1 might reveal the role of this phosphorylation residue in mediating the antidepressant action of ketamine. Furthermore, the use of optogenetic tools, for example, will allow identifying the neurophysiological and behavioral consequences of an altered synaptic plasticity and function of AMPARs induced by ketamine in the NAc-VTA circuitry and in the different neuronal populations that compose these nuclei.
Most previous studies examining the molecular antidepressant mechanisms of ketamine have investigated actions in cortical regions, in particular prefrontal cortex, or hippocampus and have reported that ketamine promotes AMPAR function and synaptogenesis.9,10,11,12,13,90 A possible change in AMPAR and NMDAR functions in mediating the antidepressant effect of ketamine is supported by a study using magnetic resonance spectroscopy in healthy human controls showing an increased glutamine/glutamate ratio induced by ketamine after 24 h, reflecting increased synaptic glutamate neurotransmission, specifically in frontal cortical regions with high density of AMPARs.91 Our present data, which demonstrate a reduced synaptic potentiation and AMPAR function in VTA-NAc circuit, may therefore appear contradictory. However, several previous studies have shown opposite changes in depressed states and antidepressant responses on neuroplasticity in NAc when compared with prefrontal cortex and hippocampus.16 For example, it has been reported that stress-induced depression increases BDNF in the NAc,92,93 but decreases this neurotrophic factor in the hippocampus.94 Ketamine was shown to increase BDNF in the hippocampus but this effect was not sustained after 24 h.20 Our results do not allow us to determine if ketamine alters the levels of BDNF in the NAc and VTA, because the levels of this growth factor were unaltered 24 h after the injection, which might indicate that BDNF levels have already returned to baseline levels both in the NAc and VTA. Enhanced AMPAR function, as demonstrated by, for example, enhanced AMPA/NMDA ratio, increased glutamatergic synaptic transmission or increased phosphorylation of GluA1,5,7,38,86,95 was suggested to mediate synaptic plasticity underlying the antidepressant effects of ketamine and (2R,6R)-HNK. These observations were made in the hippocampus or prefrontal cortex. Our data demonstrate decreased ability to strengthen glutamatergic synapses in the NAc and decreased AMPAR function in the VTA, following ketamine administration. Together, these studies and our results suggest that ketamine mediates opposite synaptic changes and ionotropic glutamate receptor modulation in cortical regions and hippocampus versus deep brain nuclei of the mesolimbic system.
Conclusions
In several recent clinical trials, ketamine was found to exert a rapid antidepressant effect in formerly treatment resistant patients after one intravenous treatment. Our findings demonstrate that ketamine and (2R,6R)-HNK induce a lasting modulation of AMPAR function and synaptic plasticity at glutamatergic synapses in the NAc and VTA. Ketamine and (2R,6R)-HNK seem to prevent potentiation and induce depression of glutamatergic synapses in the NAc and VTA-DA neurons. This study provides new insights into the role of AMPARs in the brain reward circuit in mediating the effects of ketamine and might be useful for the development of pharmacological tools that could be of therapeutic benefit in the treatment of depression.
References
Zarate CA Jr., Singh JB, Carlson PJ, Brutsche NE, Ameli R, Luckenbaugh DA et al. A randomized trial of an N-methyl-D-aspartate antagonist in treatment-resistant major depression. Arch Gen Psychiatry 2006; 63: 856–864.
Berman RM, Cappiello A, Anand A, Oren DA, Heninger GR, Charney DS et al. Antidepressant effects of ketamine in depressed patients. Biol Psychiatry 2000; 47: 351–354.
Zarate CA Jr., Machado-Vieira R. Ketamine: translating mechanistic discoveries into the next generation of glutamate modulators for mood disorders. Mol Psychiatry 2017; 22: 324–327.
Scheuing L, Chiu CT, Liao HM, Chuang DM. Antidepressant mechanism of ketamine: perspective from preclinical studies. Front Neurosci 2015; 9: 249.
Maeng S, Zarate CA Jr., Du J, Schloesser RJ, McCammon J, Chen G et al. Cellular mechanisms underlying the antidepressant effects of ketamine: role of alpha-amino-3-hydroxy-5-methylisoxazole-4-propionic acid receptors. Biol Psychiatry 2008; 63: 349–352.
Zanos P, Moaddel R, Morris PJ, Georgiou P, Fischell J, Elmer GI et al. NMDAR inhibition-independent antidepressant actions of ketamine metabolites. Nature 2016; 533: 481–486.
Freudenberg F, Celikel T, Reif A. The role of alpha-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid (AMPA) receptors in depression: central mediators of pathophysiology and antidepressant activity? Neurosci Biobehav Rev 2015; 52: 193–206.
Yang C, Qu Y, Abe M, Nozawa D, Chaki S, Hashimoto K. R)-Ketamine shows greater potency and longer lasting antidepressant effects than its metabolite (2R,6R)-hydroxynorketamine. Biol Psychiatry 2017; 82: e43–e44.
Thompson SM, Kallarackal AJ, Kvarta MD, Van Dyke AM, LeGates TA, Cai X. An excitatory synapse hypothesis of depression. Trends Neurosci 2015; 38: 279–294.
Kavalali ET, Monteggia LM. How does ketamine elicit a rapid antidepressant response? Curr Opin Pharmacol 2015; 20: 35–39.
Abdallah CG, Adams TG, Kelmendi B, Esterlis I, Sanacora G, Krystal JH. Ketamine’s mechanism of action: a path to rapid-acting antidepressants. Depress Anxiety 2016; 33: 689–697.
Carreno FR, Donegan JJ, Boley AM, Shah A, DeGuzman M, Frazer A et al. Activation of a ventral hippocampus-medial prefrontal cortex pathway is both necessary and sufficient for an antidepressant response to ketamine. Mol Psychiatry 2016; 21: 1298–1308.
Musazzi L, Treccani G, Mallei A, Popoli M. The action of antidepressants on the glutamate system: regulation of glutamate release and glutamate receptors. Biol Psychiatry 2013; 73: 1180–1188.
Malenka RC, Bear MF. LTP. and LTD: an embarrassment of riches. Neuron 2004; 44: 5–21.
Bear MF. Bidirectional synaptic plasticity: from theory to reality. Phil Trans R Soc Lond B Biol Sci 2003; 358: 649–655.
Russo SJ, Nestler EJ. The brain reward circuitry in mood disorders. Nat Rev Neurosci 2013; 14: 609–625.
Abdallah CG, Jackowski A, Salas R, Gupta S, Sato JR, Mao X et al. The nucleus accumbens and ketamine treatment in major depressive disorder. Neuropsychopharmacology 2017; 42: 1739–1746.
Zhang JC, Li SX, Hashimoto KR. -)-ketamine shows greater potency and longer lasting antidepressant effects than S (+)-ketamine. Pharmacol Biochem Behav 2014; 116: 137–141.
Yang C, Shirayama Y, Zhang JC, Ren Q, Yao W, Ma M et al. R-ketamine: a rapid-onset and sustained antidepressant without psychotomimetic side effects. Transl Psychiatry 2015; 5: e632.
Autry AE, Adachi M, Nosyreva E, Na ES, Los MF, Cheng PF et al. NMDA receptor blockade at rest triggers rapid behavioural antidepressant responses. Nature 2011; 475: 91–U109.
Browne CA, Lucki I. Antidepressant effects of ketamine: mechanisms underlying fast-acting novel antidepressants. Front Pharmacol 2013; 4: 161.
Singh JB, Fedgchin M, Daly E, Xi L, Melman C, De Bruecker G et al. Intravenous esketamine in adult treatment-resistant depression: a double-blind, double-randomization, placebo-controlled study. Biol Psychiatry 2016; 80: 424–431.
Schotanus SM, Fredholm BB, Chergui K. NMDA depresses glutamatergic synaptic transmission in the striatum through the activation of adenosine A1 receptors: evidence from knockout mice. Neuropharmacology 2006; 51: 272–282.
Zhang X, Feng ZJ, Chergui K. Allosteric modulation of GluN2C/GluN2D-containing NMDA receptors bidirectionally modulates dopamine release: implication for Parkinson’s disease. Br J Pharmacol 2014; 171: 3938–3945.
Zhang X, Chergui K. Dopamine depletion of the striatum causes a cell-type specific reorganization of GluN2B- and GluN2D-containing NMDA receptors. Neuropharmacology 2015; 92: 108–115.
Zhang X, Yao N, Chergui K. The GABAA receptor agonist muscimol induces an age- and region-dependent form of long-term depression in the mouse striatum. Learn Mem 2016; 23: 479–485.
Schotanus SM, Chergui K. Long-term potentiation in the nucleus accumbens requires both NR2A- and NR2B-containing N-methyl-D-aspartate receptors. Eur J Neurosci 2008; 27: 1957–1964.
Schotanus SM, Chergui K. Dopamine D1 receptors and group I metabotropic glutamate receptors contribute to the induction of long-term potentiation in the nucleus accumbens. Neuropharmacology 2008; 54: 837–844.
Can A, Zanos P, Moaddel R, Kang HJ, Dossou KS, Wainer IW et al. Effects of ketamine and ketamine metabolites on evoked striatal dopamine release, dopamine receptors, and monoamine transporters. J Pharmacol Exp Ther 2016; 359: 159–170.
Kara NZ, Agam G, Anderson GW, Zitron N, Einat H. Lack of effect of chronic ketamine administration on depression-like behavior and frontal cortex autophagy in female and male ICR mice. Behav Brain Res 2017; 317: 576–580.
Chergui K. Dopamine induces a GluN2A-dependent form of long-term depression of NMDA synaptic responses in the nucleus accumbens. Neuropharmacology 2011; 60: 975–981.
Kohr G. NMDA receptor function: subunit composition versus spatial distribution. Cell Tissue Res 2006; 326: 439–446.
Paoletti P, Bellone C, Zhou Q. NMDA receptor subunit diversity: impact on receptor properties, synaptic plasticity and disease. Nat Rev Neurosci 2013; 14: 383–400.
Landwehrmeyer GB, Standaert DG, Testa CM, Penney JB Jr., Young AB. NMDA receptor subunit mRNA expression by projection neurons and interneurons in rat striatum. J Neurosci 1995; 15: 5297–5307.
Li N, Lee B, Liu RJ, Banasr M, Dwyer JM, Iwata M et al. mTOR-dependent synapse formation underlies the rapid antidepressant effects of NMDA antagonists. Science 2010; 329: 959–964.
Duman RS, Li N, Liu RJ, Duric V, Aghajanian G. Signaling pathways underlying the rapid antidepressant actions of ketamine. Neuropharmacology 2012; 62: 35–41.
Paul RK, Singh NS, Khadeer M, Moaddel R, Sanghvi M, Green CE et al. (R,S)-Ketamine metabolites (R,S)-norketamine and (2S,6S)-hydroxynorketamine increase the mammalian target of rapamycin function. Anesthesiology 2014; 121: 149–159.
Zhang K, Yamaki VN, Wei Z, Zheng Y, Cai X. Differential regulation of GluA1 expression by ketamine and memantine. Behav Brain Res 2017; 316: 152–159.
Stoica L, Zhu PJ, Huang W, Zhou H, Kozma SC, Costa-Mattioli M. Selective pharmacogenetic inhibition of mammalian target of Rapamycin complex I (mTORC1) blocks long-term synaptic plasticity and memory storage. Proc Natl Acad Sci USA 2011; 108: 3791–3796.
Graber TE, McCamphill PK, Sossin WS. A recollection of mTOR signaling in learning and memory. Learn Mem 2013; 20: 518–530.
Sui L, Wang J, Li BM. Role of the phosphoinositide 3-kinase-Akt-mammalian target of the rapamycin signaling pathway in long-term potentiation and trace fear conditioning memory in rat medial prefrontal cortex. Learn Mem 2008; 15: 762–776.
Tsokas P, Grace EA, Chan P, Ma T, Sealfon SC, Iyengar R et al. Local protein synthesis mediates a rapid increase in dendritic elongation factor 1 A after induction of late long-term potentiation. J Neurosci 2005; 25: 5833–5843.
Kelly MT, Crary JF, Sacktor TC. Regulation of protein kinase Mzeta synthesis by multiple kinases in long-term potentiation. J Neurosci 2007; 27: 3439–3444.
Huganir RL, Nicoll RA. AMPARs and synaptic plasticity: the last 25 years. Neuron 2013; 80: 704–717.
Diering GH, Heo S, Hussain NK, Liu B, Huganir RL. Extensive phosphorylation of AMPA receptors in neurons. Proc Natl Acad Sci USA 2016; 113: E4920–E4927.
Lee HK, Barbarosie M, Kameyama K, Bear MF, Huganir RL. Regulation of distinct AMPA receptor phosphorylation sites during bidirectional synaptic plasticity. Nature 2000; 405: 955–959.
Chandran A, Iyo AH, Jernigan CS, Legutko B, Austin MC, Karolewicz B. Reduced phosphorylation of the mTOR signaling pathway components in the amygdala of rats exposed to chronic stress. Prog Neuropsychopharmacol Biol Psychiatry 2013; 40: 240–245.
Lammel S, Ion DI, Roeper J, Malenka RC. Projection-specific modulation of dopamine neuron synapses by aversive and rewarding stimuli. Neuron 2011; 70: 855–862.
Lammel S, Hetzel A, Hackel O, Jones I, Liss B, Roeper J. Unique properties of mesoprefrontal neurons within a dual mesocorticolimbic dopamine system. Neuron 2008; 57: 760–773.
Friedman AK, Walsh JJ, Juarez B, Ku SM, Chaudhury D, Wang J et al. Enhancing depression mechanisms in midbrain dopamine neurons achieves homeostatic resilience. Science 2014; 344: 313–319.
Hnasko TS, Hjelmstad GO, Fields HL, Edwards RH. Ventral tegmental area glutamate neurons: electrophysiological properties and projections. J Neurosci 2012; 32: 15076–15085.
Yamaguchi T, Qi J, Wang HL, Zhang S, Morales M. Glutamatergic and dopaminergic neurons in the mouse ventral tegmental area. Eur J Neurosci 2015; 41: 760–772.
Marsden WN. Synaptic plasticity in depression: molecular, cellular and functional correlates. Prog Neuropsychopharmacol Biol Psychiatry 2013; 43: 168–184.
Zhang K, Xu T, Yuan Z, Wei Z, Yamaki VN, Huang M et al. Essential roles of AMPA receptor GluA1 phosphorylation and presynaptic HCN channels in fast-acting antidepressant responses of ketamine. Sci Signal 2016; 9: ra123.
Narimatsu E, Kawamata Y, Kawamata M, Fujimura N, Namiki A. NMDA receptor-mediated mechanism of ketamine-induced facilitation of glutamatergic excitatory synaptic transmission. Brain Res 2002; 953: 272–275.
Southan AP, Wann KT. In vitro actions of ketamine and methohexitone in the rat hippocampus. Br J Anaesth 1989; 63: 574–580.
Nosyreva E, Szabla K, Autry AE, Ryazanov AG, Monteggia LM, Kavalali ET. Acute suppression of spontaneous neurotransmission drives synaptic potentiation. J Neurosci 2013; 33: 6990–7002.
Izumi Y, Zorumski CF. Metaplastic effects of subanesthetic ketamine on CA1 hippocampal function. Neuropharmacology 2014; 86: 273–281.
Ribeiro PO, Tome AR, Silva HB, Cunha RA, Antunes LM. Clinically relevant concentrations of ketamine mainly affect long-term potentiation rather than basal excitatory synaptic transmission and do not change paired-pulse facilitation in mouse hippocampal slices. Brain Res 2014; 1560: 10–17.
Oh MC, Derkach VA, Guire ES, Soderling TR. Extrasynaptic membrane trafficking regulated by GluR1 serine 845 phosphorylation primes AMPA receptors for long-term potentiation. J Biol Chem 2006; 281: 752–758.
Belujon P, Grace AA. Restoring mood balance in depression: ketamine reverses deficit in dopamine-dependent synaptic plasticity. Biol Psychiatry 2014; 76: 927–936.
Witkin JM, Monn JA, Schoepp DD, Li X, Overshiner C, Mitchell SN et al. The rapidly acting antidepressant ketamine and the mGlu2/3 receptor antagonist LY341495 rapidly engage dopaminergic mood circuits. J Pharmacol Exp Ther 2016; 358: 71–82.
Turrigiano G. Homeostatic synaptic plasticity: local and global mechanisms for stabilizing neuronal function. Cold Spring Harb Perspect Biol 2012; 4: a005736.
Jiang B, Wang W, Wang F, Hu ZL, Xiao JL, Yang S et al. The stability of NR2B in the nucleus accumbens controls behavioral and synaptic adaptations to chronic stress. Biol Psychiatry 2013; 74: 145–155.
Bagot RC, Parise EM, Peña CJ, Zhang H-X, Maze I, Chaudhury D et al. Ventral hippocampal afferents to the nucleus accumbens regulate susceptibility to depression. Nat Commun 2015; 6: 7062.
Bellone C, Luscher C. mGluRs induce a long-term depression in the ventral tegmental area that involves a switch of the subunit composition of AMPA receptors. Eur J Neurosci 2005; 21: 1280–1288.
Polter AM, Stress KauerJA. and VTA synapses: implications for addiction and depression. Eur J Neurosci 2014; 39: 1179–1188.
Chaki S, Ago Y, Palucha-Paniewiera A, Matrisciano F, Pilc A. mGlu2/3 and mGlu5 receptors: potential targets for novel antidepressants. Neuropharmacology 2013; 66: 40–52.
Park M, Niciu MJ, Zarate CA Jr.. Novel glutamatergic treatments for severe mood disorders. Curr Behav Neurosci Rep 2015; 2: 198–208.
Inta D, Vogt MA, Luoni A, Filipovic D, Lima-Ojeda JM, Pfeiffer N et al. Significant increase in anxiety during aging in mGlu5 receptor knockout mice. Behav Brain Res 2013; 241: 27–31.
Krishnan V, Han MH, Graham DL, Berton O, Renthal W, Russo SJ et al. Molecular adaptations underlying susceptibility and resistance to social defeat in brain reward regions. Cell 2007; 131: 391–404.
Chaudhury D, Walsh JJ, Friedman AK, Juarez B, Ku SM, Koo JW et al. Rapid regulation of depression-related behaviours by control of midbrain dopamine neurons. Nature 2013; 493: 532–536.
Groenewegen HJ, Wright CI, Beijer AV, Voorn P. Convergence and segregation of ventral striatal inputs and outputs. Ann N Y Acad Sci 1999; 877: 49–63.
Meredith GE. The synaptic framework for chemical signaling in nucleus accumbens. Ann N Y Acad Sci 1999; 877: 140–156.
Sesack SR, Carr DB, Omelchenko N, Pinto A. Anatomical substrates for glutamate-dopamine interactions: evidence for specificity of connections and extrasynaptic actions. Ann N Y Acad Sci 2003; 1003: 36–52.
Morales M, Margolis EB. Ventral tegmental area: cellular heterogeneity, connectivity and behaviour. Nat Rev Neurosci 2017; 18: 73–85.
van Huijstee AN, Mansvelder HD. Glutamatergic synaptic plasticity in the mesocorticolimbic system in addiction. Front Cell Neurosci 2014; 8: 466.
Krystal JH, Karper LP, Seibyl JP, Freeman GK, Delaney R, Bremner JD et al. Subanesthetic effects of the noncompetitive NMDA antagonist, ketamine, in humans. Psychotomimetic, perceptual, cognitive, and neuroendocrine responses. Arch Gen Psychiatry 1994; 51: 199–214.
Malhotra AK, Pinals DA, Weingartner H, Sirocco K, Missar CD, Pickar D et al. NMDA receptor function and human cognition: the effects of ketamine in healthy volunteers. Neuropsychopharmacology 1996; 14: 301–307.
Malhotra AK, Pinals DA, Adler CM, Elman I, Clifton A, Pickar D et al. Ketamine-induced exacerbation of psychotic symptoms and cognitive impairment in neuroleptic-free schizophrenics. Neuropsychopharmacology 1997; 17: 141–150.
Pennybaker SJ, Luckenbaugh DA, Park LT, Marquardt CA, Zarate CA Jr.. Ketamine and psychosis history: antidepressant efficacy and psychotomimetic effects postinfusion. Biol Psychiatry 2017; 82: e35–e36.
Lahti AC, Koffel B, LaPorte D, Tamminga CA. Subanesthetic doses of ketamine stimulate psychosis in schizophrenia. Neuropsychopharmacology 1995; 13: 9–19.
Trujillo KA, Smith ML, Sullivan B, Heller CY, Garcia C, Bates M. The neurobehavioral pharmacology of ketamine: implications for drug abuse, addiction, and psychiatric disorders. ILAR J 2011; 52: 366–378.
Wiescholleck V, Manahan-Vaughan D. Long-lasting changes in hippocampal synaptic plasticity and cognition in an animal model of NMDA receptor dysfunction in psychosis. Neuropharmacology 2013; 74: 48–58.
Yang B, Zhang JC, Han M, Yao W, Yang C, Ren Q et al. Comparison of R-ketamine and rapastinel antidepressant effects in the social defeat stress model of depression. Psychopharmacology (Berl) 2016; 233: 3647–3657.
Miller OH, Yang L, Wang C-C, Hargroder EA, Zhang Y, Delpire E et al. GluN2B-containing NMDA receptors regulate depression-like behavior and are critical for the rapid antidepressant actions of ketamine. Elife 2014; 3: e0358.
Louderback KM, Wills TA, Muglia LJ, Winder DG. Knockdown of BNST GluN2B-containing NMDA receptors mimics the actions of ketamine on novelty-induced hypophagia. Transl Psychiatry 2013; 3: e331.
Inta D, Vogt MA, Elkin H, Weber T, Lima-Ojeda JM, Schneider M et al. Phenotype of mice with inducible ablation of GluA1 AMPA receptors during late adolescence: relevance for mental disorders. Hippocampus 2014; 24: 424–435.
Vogt MA, Elkin H, Pfeiffer N, Sprengel R, Gass P, Inta D. Impact of adolescent GluA1 AMPA receptor ablation in forebrain excitatory neurons on behavioural correlates of mood disorders. Eur Arch Psychiatry Clin Neurosci 2014; 264: 625–629.
Zunszain PA, Horowitz MA, Cattaneo A, Lupi MM, Pariante CM. Ketamine: synaptogenesis, immunomodulation and glycogen synthase kinase-3 as underlying mechanisms of its antidepressant properties. Mol Psychiatry 2013; 18: 1236–1241.
Li M, Demenescu LR, Colic L, Metzger CD, Heinze HJ, Steiner J et al. Temporal dynamics of antidepressant ketamine effects on glutamine cycling follow regional fingerprints of AMPA and NMDA receptor densities. Neuropsychopharmacology 2017; 42: 1201–1209.
Berton O, McClung CA, Dileone RJ, Krishnan V, Renthal W, Russo SJ et al. Essential role of BDNF in the mesolimbic dopamine pathway in social defeat stress. Science 2006; 311: 864–868.
Wook Koo J, Labonte B, Engmann O, Calipari ES, Juarez B, Lorsch Z et al. Essential role of mesolimbic brain-derived neurotrophic factor in chronic social stress-induced depressive behaviors. Biol Psychiatry 2016; 80: 469–478.
Tsankova NM, Berton O, Renthal W, Kumar A, Neve RL, Nestler EJ. Sustained hippocampal chromatin regulation in a mouse model of depression and antidepressant action. Nat Neurosci 2006; 9: 519–525.
Zarate CA Jr., Machado-Vieira R. GSK-3: a key regulatory target for ketamine's rapid antidepressant effects mediated by enhanced AMPA to NMDA throughput. Bipolar Disord 2016; 18: 702–705.
Acknowledgments
We thank Dr Holly Green for her comments on the manuscript. This work was supported by the Swedish Research Council (grant 2014-3254) and The Swedish foundation for International Cooperation in Research and Higher Education (STINT).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Yao, N., Skiteva, O., Zhang, X. et al. Ketamine and its metabolite (2R,6R)-hydroxynorketamine induce lasting alterations in glutamatergic synaptic plasticity in the mesolimbic circuit. Mol Psychiatry 23, 2066–2077 (2018). https://doi.org/10.1038/mp.2017.239
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2017.239
- Springer Nature Limited
This article is cited by
-
New perspective on sustained antidepressant effect: focus on neurexins regulating synaptic plasticity
Cell Death Discovery (2024)
-
Targeting metaplasticity mechanisms to promote sustained antidepressant actions
Molecular Psychiatry (2024)
-
Ketamine Improves the Glymphatic Pathway by Reducing the Pyroptosis of Hippocampal Astrocytes in the Chronic Unpredictable Mild Stress Model
Molecular Neurobiology (2024)
-
Aberrant somatic calcium channel function in cNurr1 and LRRK2-G2019S mice
npj Parkinson's Disease (2023)
-
A case series of group-based ketamine-assisted psychotherapy for patients in residential treatment for eating disorders with comorbid depression and anxiety disorders
Journal of Eating Disorders (2022)