Abstract
Most mental disorders, when examined independently, are associated with an elevated risk for suicide attempt. However, mental disorders often co-occur, and that co-occurrence is well explained by models where specific mental disorders are understood as manifestations of latent dimensions of psychopathology. To date, it remains unclear whether the risk of suicide attempt is due to specific mental disorders, to specific dimensions of psychopathology (that is, internalizing and externalizing dimensions), to a general psychopathology factor or to a combination of these explanations. In a large nationally representative prospective survey, the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC), we used structural equation modeling to examine the shared and specific effects of Axis I and Axis II disorders on the occurrence of suicide attempts in the general population and among individuals with a lifetime history of suicidal ideation. Effects of mental disorders on the risk of suicide attempt were exerted almost exclusively through a general psychopathology factor representing the shared effect across all mental disorders. Effects of remitted psychiatric disorders on the risk of suicide attempt were fully mediated by current mental disorders. Similar patterns of associations were found in individuals with suicidal ideation. These results held when using different approaches to modeling psychiatric comorbidity. Our findings underscore the importance of adopting dimensional approaches to comorbidity in the study of suicidal behavior. Because mental disorders increase the risk of suicide attempt through a general psychopathology liability, this dimension should be considered as an important therapeutic target to substantially advance suicide prevention.
Similar content being viewed by others
Introduction
Despite considerable advances in our understanding of its neurobiology, suicide continues to be among the leading causes of death worldwide.1, 2 Epidemiological studies in the West suggest that a vast majority of suicide attempters have a diagnosable psychiatric disorder, supporting the notion that mental disorders are among the strongest predictors of suicide attempt.3, 4, 5
Most mental disorders, when examined independently, are associated with greater risk for suicide attempt.3, 5, 6, 7, 8, 9, 10, 11, 12 However, mental disorders often co-occur,13 and that co-occurrence is well explained by models where specific disorders are understood as manifestations of latent correlated liability factors (for example, internalizing and externalizing dimensions).14, 15 Two previous studies16, 17 have suggested that transdiagnostic factors may account for links between individual disorders and suicide-related outcomes. However, their models focused on a limited number of psychiatric disorders (that is, Axis I internalizing disorders). The predictive utility of these transdiagnostic factors has never been examined while adjusting for potential confounders, such as prior suicide attempts and sociodemographic characteristics. In addition, as dimensions underlying psychopathology are positively correlated,18 the risk of suicide attempt might be increased mostly by a general psychopathology factor (representing the shared effect across all mental disorders) rather than by specific dimensions of psychopathology.17 Therefore, to date, it remains unclear whether the risk of suicide attempt is due to specific Axis I or Axis II disorders, to specific dimensions of psychopathology (for example, externalizing dimension), to a general psychopathology factor or to a combination of these explanations.16, 17 This question is crucial because if suicide attempt risk is disorder-specific, disorder-specific interventions may be needed for risk reduction. By contrast, if the risk is mostly mediated through transdiagnostic factors, interventions that address these factors may have greater impact on suicide risk reduction.
A second unanswered question is whether remitted psychiatric disorders increase the risk of suicide attempt exclusively through the greater risk for current disorders or whether they have other sustained, specific effects independent of current disorders. In addition to advancing the understanding of the mechanisms through which mental disorders lead to suicide attempts, this question has also important implications for suicide prevention by allowing better identification of those at greater risk for suicide attempt among individuals with a history of mental disorders.
Last, recent epidemiological studies have suggested that mental disorders may have weaker effects on predicting suicide attempts among individuals with suicidal ideation5, 10 and that instead, suicide attempts in those individuals are better explained by a distinct genetic component.19, 20, 21 However, no study has examined this issue by taking into account the presence of comorbid mental disorders among those with suicidal ideation.5
This prospective study examined the shared and specific effects of a wide range of DSM-IV Axis I and Axis II disorders on the 3-year risk for suicide attempt. As dimensions underlying psychopathology are correlated,18 we used a bifactor latent variable approach to disentangle the effects shared by all mental disorders (that is, general psychopathology), those specific to dimensions of psychopathology (for example, internalizing dimension) and those specific to mental disorders per se (for example, major depressive episode). We repeated these analyses in the subsample of individuals with a lifetime history of suicidal ideation at Wave 1 to examine whether the effects of mental disorders on the risk of suicide attempt are similar in this group.
Materials and methods
Sample
Data were drawn from the Wave 1 and Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions (NESARC), a nationally representative face-to-face survey of the US adult population, conducted in 2001–2002 (Wave 1) and 2004–2005 (Wave 2) by the National Institute on Alcoholism and Alcohol Abuse (NIAAA) and described in detail elsewhere.22 The target population included the civilian noninstitutionalized population, aged 18 years and older, residing in the United States. The cumulative response rate at Wave 2 was 70.2%, resulting in 34 653 Wave 2 interviews.22 The Wave 2 NESARC data were weighted to be representative of the US civilian population based on the 2000 census.22 The research protocol, including written informed consent procedures, received full human subjects review and approval from the US Census bureau and the Office of Management and Budget. The present analysis includes the 20 089 female and 14 564 male participants who completed interviews at both waves.
Measures
Assessments of DSM-IV Axis I and Axis II disorders
Mental disorders were assessed using the Alcohol Use Disorder and Associated Disabilities Interview Schedule, DSM-IV version (AUDADIS-IV), a structured diagnostic instrument administered by trained lay interviewers.22 Axis I diagnoses included substance use disorders (alcohol use disorder, drug use disorder and nicotine dependence), mood disorders (major depressive disorder, dysthymic disorder and bipolar disorder), anxiety disorders (panic disorder, social anxiety disorder, specific phobia and generalized anxiety disorder) and pathological gambling. For all Axis I disorders, diagnoses were made in the past 12 months prior to Wave 1. Axis II disorders (including avoidant, dependent, obsessive-compulsive, histrionic, paranoid, schizoid and antisocial personality disorders) were assessed on a lifetime basis.22 The test-retest reliability and validity of AUDADIS-IV measures of DSM-IV mental disorders is good to excellent for substance use disorders and fair to good for other disorders.23, 24, 25, 26, 27
Assessment of lifetime suicidal ideation and suicide attempts
To assess lifetime history of suicidal ideation and suicide attempt at baseline, individuals with a lifetime history of 2-week episode of depressed mood and/or anhedonia were asked in Wave 1 whether they had ever felt like they wanted to die or ever thought a lot about their own death or committing suicide, and whether they had ever attempted suicide. To assess for incident cases of suicide attempt, all Wave 2 respondents were asked: ‘Since last interview, did you ever attempt suicide?’
Statistical analysis
Because previous work has shown that internalizing disorders are more prevalent among women and externalizing disorders are more prevalent among men,28 all analyses were stratified by gender. Weighted percentages and their corresponding standard errors were calculated to provide descriptive information about the relationships of past-year Axis I disorders and lifetime Axis II disorders assessed at Wave 1 with suicide attempt occurrence between the two Waves. Odds ratios, population attributable fractions (PAFs) and their 95% confidence intervals were calculated to provide information on future suicide attempts within each subpopulation with each mental disorder.
Next, we used confirmatory factor analysis (CFA) to identify the latent structure underlying individual mental disorders assessed at Wave 1. Building upon the CFA model fit by Blanco et al.18, 29 on these data, which generated three dimensions (‘internalizing I’, ‘internalizing II’ and ‘externalizing’), we performed a bifactor CFA model to determine whether a general psychopathology factor measured by all mental disorders in addition to disorder-specific factors30, 31, 32 fit the underlying structure of mental disorders. We also tested an alternative approach to modeling mental disorder comorbidity and built upon the distress-fear-externalizing CFA model15, 28, 33, 34 and performed a bifactor CFA model. We examined measures of goodness-of-fit, including the comparative fit index (CFI), the Tucker–Lewis index (TLI) and the root mean squared error of approximation (RMSEA). CFI and TLI values greater than 0.95 and values of RMSEA less than 0.06 are commonly used to indicate good model fit and were used as cutoffs.35
Finally, after confirming that the measurement parameters of the bifactor models were sex invariant, we used a multiple-group structural equation model stratified by sex to assess shared and specific effects of the different mental disorders at Wave 1 on the risk of suicide attempt, while adjusting for prior suicide attempt and sociodemographic characteristics, that is, age, race/ethnicity (White versus non-White), marital status (married versus non-married) and household income. Specifically, we examined three sets of relationships: (i) the effect of the general psychopathology liability factor (representing the effects shared across all mental disorders) on the risk of suicide attempt, (ii) the effects of each of the dimensions of psychopathology on the risk of suicide attempt beyond the effect of the general psychopathology factor and (iii) the effects of mental disorders per se on the risk of suicide attempt above and beyond the shared effects of mental disorders through the latent factors. These analyses were conducted in both the full sample and the subpopulation of subjects with a lifetime history of suicidal ideation at the time of Wave 1 interview.
As internalization and externalization dimensions are positively correlated,18 an advantage of modeling a bifactor model is that a general psychopathology factor accounts for a good deal of this correlation, is orthogonal to these dimensions and saturates each mental disorder diagnosis directly.30, 31, 32 The bifactor model allows to disambiguate from each other effects shared by all mental disorders (represented by the general psychopathology factor), those shared by disorders within each dimension of psychopathology (for example, externalizing dimension) and the specific effect of each mental disorder per se.36
The relationship between the general psychopathology factor and the risk for attempting suicide is interpreted as the effect of the overall shared mental disorder liability predictors on the risk for attempting suicide. By contrast, the relationships examined between the specific dimensions of psychopathology or specific individual disorders and the risk of suicide attempt are interpreted as the direct effects, because they indicate effects that are not mediated through the general psychopathology factor. Standardized estimates of the relationship between suicide attempt and each latent factor indicate how many standard deviations higher (or lower) the mean of the latent variable underlying the binary outcome are expected to be for each increase in an additional unit of that latent factor while adjusting for the other factors and covariates. To determine whether a particular type of mental disorder predicts suicide attempt above and beyond the association attributable to the latent variables, modification indices (that is, chi-square tests with 1 degree of freedom) were examined to test whether any residuals associated with individual mental disorders are correlated with the risk of suicide attempt. To avoid including direct effects that could be significant because of multiple testing and because of the large sample size,29, 37 we considered significant direct effects of items with modification index greater or equal to 10.
To examine whether remitted disorders had an additional effect on the risk of suicide attempt, we repeated analyses including lifetime, remitted psychiatric disorders at Wave 1. Were lifetime remitted disorders to exert independent effects, the model would show direct effects from those disorders on suicide attempt. If remitted disorders only predict current disorders, it would indicate that their association with suicide attempts was fully mediated by current disorders.
We decided a priori to evaluate statistical significance using a two-sided design with alpha set at 0.005 in the analysis for the full population and at 0.05 in the analysis for the subpopulation with suicidal ideation.38, 39
PAFs were computed using the Punaf program40 for STATA software (Svy routines in Stata, version 11.0; StataCorp, College Station, TX, USA).40, 41 The program implements the method for estimating PAFs as recommended by Greenland and Drescher42 for cohort studies. All other analyses were conducted in Mplus Version 7.3.37 The default estimator for the analysis was the variance-adjusted weighted least squares (WLSMV), a robust estimator appropriate for ordered categorical and dichotomous observed variables such as the ones used in this study.37 All analyses accounted for the NESARC’s complex sampling design.
Complementary analyses
To examine the robustness of our findings, we also performed a second-order model with the three dimensions of psychopathology for the internalizing I-internalizing II-externalizing CFA model and the internalizing and externalizing dimensions for the distress-fear-externalizing CFA model loading on a general psychopathology factor.18, 29
Results
Associations of mental disorders with future suicide attempt
The prevalence rates of suicide attempt during the 3-year follow-up period were 0.5% in men (s.e.=0.01, N=75) and 0.9% in women (s.e.=0.01, N=178) in the full sample, and 2.1% in men (s.e.=0.5, N=37) and 3.3% in women (s.e.=0.4, N=106) in the subpopulation of individuals with a lifetime history of suicidal ideation.
A majority of male (75.3%) and female (66.9%) participants in the full sample who attempted suicide between Waves 1 and 2 had a past-year DSM-IV Axis I disorder or a lifetime Axis II disorder at Wave 1. These rates were even higher among subjects with a history of suicidal ideation at Wave 1 (90.4% in men and 85.6% in women, respectively). In the full sample, PAFs of mental disorders in predicting suicide attempt were significant for 16 disorders in women and 9 disorders in men, with PAFs ranging from 12.8% (avoidant personality disorder) to 30% (nicotine dependence) in men and from 5.8% (dependent personality disorder) to 35.2% (major depressive episode) in women. In the subpopulation of individuals with a history of suicidal ideation, PAFs were significant for 10 disorders in women and 3 disorders in men, and ranged from 26.5% (panic disorder) to 38% (alcohol use disorder) in men and from 8.2% (drug use disorder) to 41.7% (major depressive episode) in women (Table 1).
Structure of current mental disorders
The multiple-group bifactor three-dimension CFA model with a general psychopathology factor measured by all mental disorders in addition to disorder-specific dimensions provided an excellent fit to the data (CFI=0.979, TLI=0.977, RMSEA=0.011). In the subsample of participants with lifetime history of suicidal ideation in Wave 1, fit indices were also good (CFI=0.964, TLI=0.960 and RMSEA=0.018) (see Supplementary Tables 1 and 2). The fit indices for the bifactor model of the distress-fear-externalizing structure were excellent in the full population (CFI=0.985, TLI=0.979 and RMSEA=0.012) and good in the subpopulation of individuals with suicidal ideation (CFI=0.964, TLI=0.950 and RMSEA=0.023) (see Supplementary Tables 3 and 4).
Effects of transdiagnostic factors on the risk of suicide attempt
After adjusting for age, race/ethnicity, household income, marital status and prior suicide attempt, the general psychopathology factor representing the shared effect of all mental disorders increased the risk of suicide attempt in both genders (Figures 1 and 2). In addition, having a household income lower than $20 000 increased the risk of suicide attempt in men only. Prior suicide attempt increased the risk of suicide attempt in both genders. There were no direct effects from any dimension of psychopathology or disorder on suicide attempt in both genders. The bifactor model of the distress-fear-externalizing structure provided the same pattern of associations between mental disorders and suicide attempt both in the full population and in the subpopulation of individuals with suicidal ideation, except for a small variation: in these models, based exclusively on Axis I disorders and antisocial personality disorder, there was a positive direct effect of the distress factor on suicide attempt in women only, probably because of the absence of other personality disorders in the structure of these models (Figures 3 and 4).
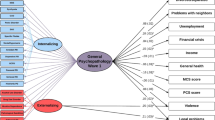
Bifactor model of the internalizing I–internalizing II–externalizing structure testing the shared and specific effects of mental disorders on the occurrence of suicide attempt in a general population sample of men (n=14 564) during a 3-year follow-up period. Ellipses are used to denote latent constructs, rectangles are used to denote the observed variables measuring or impacting on these constructs. The bifactor model parses disorder variance into general variance (i.e., variance of the general psychopathology factor), variance of dimensions of psychopathology (e.g., variance of the externalizing dimension) and unique variance (variance of each mental disorder per se). Regression coefficients shown are standardized. Values in brackets indicate their standard errors. Only significant effects (two-sided P<0.005) are represented in the model. There is no specific dimension of psychopathology or disorder with modification index greater or equal to 10 to predict suicide attempt in addition. Reference groups used for covariates are individuals with a household income equal or higher than $70 000, aged 18–29 years, non-White, not married and not living with someone as if married, and without a lifetime history of suicide attempt at Wave 1. GAD, generalized anxiety disorder; MDE, major depressive episode; OCPD, obsessive-compulsive personality disorder; PD, personality disorder; SAD, social anxiety disorder.
Bifactor model of the internalizing I–internalizing II–externalizing structure testing the shared and specific effects of mental disorders on the occurrence of suicide attempt in a general population sample of women (n=20 089) during a 3-year follow-up period. Ellipses are used to denote latent constructs, rectangles are used to denote the observed variables measuring or impacting on these constructs. The bifactor model parses disorder variance into general variance (i.e., variance of the general psychopathology factor), variance of dimensions of psychopathology (e.g., variance of the externalizing dimension) and unique variance (variance of each mental disorder per se). Regression coefficients shown are standardized. Values in brackets indicate their standard errors. Only significant effects (two-sided P<0.005) are represented in the model. There is no specific dimension of psychopathology or disorder with modification index greater or equal to 10 to predict suicide attempt in addition. Reference groups used for covariates are individuals with a household income equal or higher than $70 000, aged 18–29 years, non-White, not married and not living with someone as if married, and without a lifetime history of suicide attempt at Wave 1. GAD, generalized anxiety disorder; MDE, major depressive episode; OCPD, obsessive-compulsive personality disorder; PD, personality disorder; SAD, social anxiety disorder.
Bifactor model of the distress-fear-externalizing structure testing the shared and specific effects of mental disorders on the occurrence of suicide attempt in a general population sample of men (n=14 564) during a 3-year follow-up period. Ellipses are used to denote latent constructs, rectangles are used to denote the observed variables measuring or impacting on these constructs. The bifactor model parses disorder variance into general variance (i.e., variance of the general psychopathology factor), variance of dimensions of psychopathology (e.g., variance of the externalizing dimension) and unique variance (variance of each mental disorder per se). Regression coefficients shown are standardized. Values in brackets indicate their standard errors. Only significant effects (two-sided P<0.005) are represented in the model. There is no specific dimension of psychopathology or disorder with modification index greater or equal to 10 to predict suicide attempt in addition. Reference groups used for covariates are individuals with a household income equal or higher than $70 000, aged 18–29 years, non-White, not married and not living with someone as if married, and without a lifetime history of suicide attempt at Wave 1. GAD, generalized anxiety disorder; MDE, major depressive episode; PD, personality disorder; SAD, social anxiety disorder.
Bifactor model of the distress-fear-externalizing structure testing the shared and specific effects of mental disorders on the occurrence of suicide attempt in a general population sample of women (n=20 089) during a 3-year follow-up period. Ellipses are used to denote latent constructs, rectangles are used to denote the observed variables measuring or impacting on these constructs. The bifactor model parses disorder variance into general variance (i.e., variance of the general psychopathology factor), variance of dimensions of psychopathology (e.g., variance of the externalizing dimension) and unique variance (variance of each mental disorder per se). Regression coefficients shown are standardized. Values in brackets indicate their standard errors. Only significant effects (two-sided P<0.005) are represented in the model. Dotted arrow indicates direct effect beyond effect of the general psychopathology factor. There is no other specific dimension of psychopathology or disorder with modification index greater or equal to 10 to predict suicide attempt in addition. Reference groups used for covariates are individuals with a household income equal or higher than $70 000, aged 18–29 years, non-White, not married and not living with someone as if married, and without a lifetime history of suicide attempt at Wave 1. GAD, generalized anxiety disorder; MDE, major depressive episode; PD, personality disorder; SAD, social anxiety disorder.
The effects of remitted psychiatric disorders on the risk of suicide attempt were fully mediated by current mental disorders in both genders (data available on request).
The patterns of association found in the full population held among individuals with a lifetime history of suicidal ideation in Wave 1 (see Supplementary Figures 1 to 4). No sociodemographic characteristics had direct effects on the risk of suicide attempt in this subpopulation in either gender.
Complementary analyses
The fit indices for the second-order model with the three dimensions of psychopathology for the internalizing I-internalizing II-externalizing CFA model and the internalizing and externalizing dimensions for the distress-fear-externalizing CFA model loading on a general psychopathology factor were CFI⩾0.949, TLI⩾0.944 and RMSEA⩽0.023 (see Supplementary Tables 5 to 8). The second-order model showed very similar results to the bifactor model both in the full population and in the subpopulation of individuals with a history of suicidal ideation (see Supplementary Figures 5 to 12).
Discussion
In a large, longitudinal, nationally representative sample of US adults, mental disorders were strongly associated with the risk of suicide attempt during the 3-year follow-up, and their effect on this risk occurred in both genders almost exclusively through a general psychopathology dimension representing the shared effects across all mental disorders, independently of sociodemographic characteristics and history of prior suicide attempts. Furthermore, the effect of remitted psychopathology on the risk of suicide attempt was fully mediated by current mental disorders. Similar patterns of associations between mental disorders and suicide attempts were also found in the subsample of individuals with suicidal ideation at Wave 1. These results held when using different approaches to modeling psychiatric comorbidity. These findings advance our understanding of suicide attempt in several important ways.
Although previous studies have consistently demonstrated that psychiatric disorders increase the risk for suicide attempts,3, 5, 6, 7, 8, 9, 10, 11 our results show that this risk is not uniquely associated with any single disorder, but rather mediated by an overall latent liability (that is, predisposition) to psychopathology. Increased psychopathological load, as measured by higher scores on the general psychopathology latent variable, is associated with a greater risk for suicide attempt. Our results help reconcile and summarize findings that both internalizing (for example, major depressive episode) and externalizing disorders (for example, substance use disorders), as well as comorbidity5, 11 and severity of disorders,43 increase the risk of suicide attempt. They also suggest that although interventions on individual disorders are likely to decrease this risk, interventions directed at broader, more global psychopathological processes are likely to have greater effect. As mental disorders can be understood as manifestations of latent correlated liability factors (for example, internalization and externalization dimensions),14 remission of one specific disorder (for example, major depressive episode) may be insufficient to reduce the risk of suicide attempt if the psychopathological load of the general psychopathology dimension remains as indicated by all other disorders loading on this dimension. At a more general level, our findings are consistent with current dimensional conceptualizations of psychopathology33, 34, 44, 45, 46, 47, 48, 49 and call for identification of psychological and biological processes underlying these broad psychopathological dimensions. There is already evidence that the brain circuitry and neurochemistry abnormalities related to psychiatric disorders tend to overlap within the same liability dimension50, 51, 52 and across dimensions.53 Our findings held for both genders suggesting that, although levels of liabilities for internalizing and externalizing disorders may vary by gender,28, 54 the effects of those liabilities on the risk of suicide attempt are similar across genders.
A second important finding of the present study was that remitted psychiatric disorders exerted their effects on the risk of suicide attempt through current disorders. From an etiological perspective, these results suggest that prior and current psychiatric disorders are manifestations of more general overarching liabilities that mediate the associations between mental disorders and suicide attempts. From a clinical point of view, our results suggest that assessment of current disorders may provide most of the information necessary to assess the risk of suicide attempt associated with psychiatric disorders.55 However, structured interviews tend to underestimate the prevalence of remitted psychiatric disorders,56 and current disorders can also decrease the likelihood of recalling past disorders.57 Therefore, it is possible that this result may be partly biased by an underestimation of remitted psychiatric disorders. Nevertheless, structured interviews mimic clinical interviews, in which recall bias can also occur. Therefore, our results suggest that patient report on past disorders adds little to the prediction of future suicide attempts.
Last, in contrast to some prior cross-sectional studies,5, 58 we found that patterns of associations of mental disorders with increased risk of suicide attempt also held in the subpopulation of participants with suicidal ideation in both genders, suggesting that underlying mechanisms may be similar in this population and in the general population. The difference between our findings and those of previous studies may be due to the inclusion of Axis II disorders in our analyses and our approach to modeling comorbidity. Our findings underscore the importance of carefully modeling comorbidity to advance our understanding of suicidal behavior.
Our results should be interpreted in the light of several limitations. First, despite its prospective design, our study cannot establish a causal relationship between mental disorders and the occurrence of suicide attempt.59 Second, although Wave 1 of the NESARC examined a wide range of Axis I and Axis II mental disorders, several disorders, including psychotic disorders and borderline personality disorder, known to be linked to suicide attempts, were not included. For example, because borderline personality disorder was assessed in Wave 2, we decided not to include this disorder in our study to preserve its prospective design. However, the structure of psychiatric disorders seems to be robust to the inclusion of a broad range of disorders as indicators and the inclusion of borderline personality disorder in additional analyses did not modify the statistical significance of the effect of the general psychopathology factor on the risk of suicide in any gender. Third, our study examined the occurrence of suicide attempts in a 3-year period and the pattern of associations may differ for longer or shorter periods of time.
Despite these limitations, our findings underscore the importance of adopting dimensional approaches to comorbidity in the study of suicidal behavior, which may help disentangle biological and psychological mechanisms underlying the associations of these psychopathological dimensions with suicide attempt. Because mental disorders increase the risk of suicide attempt through a broad general psychopathological liability, this dimension should be considered as an important potential therapeutic target to substantially progress in suicide prevention.
References
Rockett IRH, Regier MD, Kapusta ND, Coben JH, Miller TR, Hanzlick RL et al. Leading causes of unintentional and intentional injury mortality: united states, 2000–2009. Am J Public Health 2012; 102: e84–e92.
Nock MK, Borges G, Bromet EJ, Cha CB, Kessler RC, Lee S . Suicide and suicidal behavior. Epidemiol Rev 2008; 30: 133–154.
Harris EC, Barraclough B . Suicide as an outcome for mental disorders. A meta-analysis. Br J Psychiatry 1997; 170: 205–228.
Pokorny AD . Prediction of suicide in psychiatric patients. Report of a prospective study. Arch Gen Psychiatry 1983; 40: 249–257.
Nock MK, Hwang I, Sampson NA, Kessler RC . Mental disorders, comorbidity and suicidal behavior: results from the National Comorbidity Survey Replication. Mol Psychiatry 2010; 15: 868–876.
Weissman MM, Klerman GL, Markowitz JS, Ouellette R . Suicidal ideation and suicide attempts in panic disorder and attacks. N Engl J Med 1989; 321: 1209–1214.
Bostwick JM, Pankratz VS . Affective disorders and suicide risk: a reexamination. Am J Psychiatry 2000; 157: 1925–1932.
Phillips MR, Yang G, Li S, Li Y . Suicide and the unique prevalence pattern of schizophrenia in mainland China: a retrospective observational study. Lancet 2004; 364: 1062–1068.
Kessler RC, Berglund P, Borges G, Nock M, Wang PS . Trends in suicide ideation, plans, gestures, and attempts in the United States, 1990-1992 to 2001-2003. JAMA 2005; 293: 2487–2495.
Nock MK, Borges G, Bromet EJ, Alonso J, Angermeyer M, Beautrais A et al. Cross-national prevalence and risk factors for suicidal ideation, plans and attempts. Br J Psychiatry 2008; 192: 98–105.
Kessler RC, Borges G, Walters EE . Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry 1999; 56: 617–626.
Hoertel N, Le Strat Y, Lavaud P, Dubertret C, Limosin F . Generalizability of clinical trial results for bipolar disorder to community samples: findings from the national epidemiologic survey on alcohol and related conditions. J Clin Psychiatry 2013; 74: 265–270.
Kessler RC, Chiu WT, Demler O, Merikangas KR, Walters EE . Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 2005; 62: 617–627.
Krueger RF, Markon KE . Reinterpreting comorbidity: a model-based approach to understanding and classifying psychopathology. Annu Rev Clin Psychol 2006; 2: 111–133.
Slade T, Watson D . The structure of common DSM-IV and ICD-10 mental disorders in the Australian general population. Psychol Med 2006; 36: 1593–1600.
Eaton NR, Krueger RF, Markon KE, Keyes KM, Skodol AE, Wall M et al. The structure and predictive validity of the internalizing disorders. J Abnorm Psychol 2013; 122: 86–92.
Watson D, Naragon-Gainey K . Personality, emotions, and the emotional disorders. Clin Psychol Sci 2014; 2: 422–442.
Blanco C, Krueger RF, Hasin DS, Liu SM, Wang S, Kerridge BT et al. Mapping common psychiatric disorders: structure and predictive validity in the National Epidemiologic Survey on Alcohol and Related Conditions. JAMA Psychiatry 2013; 70: 199–208.
Bondy B, Buettner A, Zill P . Genetics of suicide. Mol Psychiatry 2006; 11: 336–351.
Brent DA, Mann JJ . Family genetic studies, suicide, and suicidal behavior. Am J Med Genet C Semin Med Genet 2005; 133C: 13–24.
Brent DA, Mann JJ . Familial pathways to suicidal behavior—understanding and preventing suicide among adolescents. N Engl J Med 2006; 355: 2719–2721.
Grant BF, Goldstein RB, Chou SP, Huang B, Stinson FS, Dawson DA et al. Sociodemographic and psychopathologic predictors of first incidence of DSM-IV substance use, mood and anxiety disorders: results from the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions. Mol Psychiatry 2009; 14: 1051–1066.
Grant BF, Dawson DA, Stinson FS, Chou PS, Kay W, Pickering RP . The Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV (AUDADIS-IV): reliability of alcohol consumption, tobacco use, family history of depression and psychiatric diagnostic modules in a general population sample. Drug Alcohol Depend 2003; 71: 7–16.
Grant BF, Harford TC, Dawson DA, Chou PS, Pickering RP . The Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): reliability of alcohol and drug modules in a general population sample. Drug Alcohol Depend 1995; 39: 37–44.
Hasin D, Carpenter KM, McCloud S, Smith M, Grant BF . The Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): reliability of alcohol and drug modules in a clinical sample. Drug Alcohol Depend 1997; 44: 133–141.
Chatterji S, Saunders JB, Vrasti R, Grant BF, Hasin D, Mager D . Reliability of the alcohol and drug modules of the Alcohol Use Disorder and Associated Disabilities Interview Schedule—Alcohol/Drug-Revised (AUDADIS-ADR): an international comparison. Drug Alcohol Depend 1997; 47: 171–185.
Canino G, Bravo M, Ramírez R, Febo VE, Rubio-Stipec M, Fernández RL et al. The Spanish Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): reliability and concordance with clinical diagnoses in a Hispanic population. J Stud Alcohol Drugs 1999; 60: 790–799.
Eaton NR, Keyes KM, Krueger RF, Balsis S, Skodol AE, Markon KE et al. An invariant dimensional liability model of gender differences in mental disorder prevalence: Evidence from a national sample. J Abnorm Psychol 2012; 121: 282–288.
Magidson JF, Blashill AJ, Wall MM, Balan IC, Wang S, Lejuez CW et al. Relationship between psychiatric disorders and sexually transmitted diseases in a nationally representative sample. J Psychosom Res 2014; 76: 322–328.
Reise SP, Morizot J, Hays RD . The role of the bifactor model in resolving dimensionality issues in health outcomes measures. Qual Life Res 2007; 16 (Suppl 1): 19–31.
Tackett JL, Lahey BB, van Hulle C, Waldman I, Krueger RF, Rathouz PJ . Common genetic influences on negative emotionality and a general psychopathology factor in childhood and adolescence. J Abnorm Psychol 2013; 122: 1142–1153.
Caspi A, Houts RM, Belsky DW, Goldman-Mellor SJ, Harrington H, Israel S et al. The p Factor One General Psychopathology Factor in the Structure of Psychiatric Disorders? Clin Psychol Sci 2014; 2: 119–137.
Krueger RF . The structure of common mental disorders. Arch Gen Psychiatry 1999; 56: 921–926.
Vollebergh WA, Iedema J, Bijl RV, De Graaf R, Smit F, Ormel J . The structure and stability of common mental disorders: the NEMESIS study. Arch Gen Psychiatry 2001; 58: 597–603.
Hu L, Bentler PM . Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Modeling 1999; 6: 1–55.
Wall MM, Li R . Comparison of multiple regression to two latent variable techniques for estimation and prediction. Stat Med 2003; 22: 3671–3685.
Muthén LK, Muthén BO . Mplus User’s Guide Los Angeles, 1998-2006.
Godfrey K . Statistics in practice. Comparing the means of several groups. N Engl J Med 1985; 313: 1450–1456.
Hoertel N, Le Strat Y, Angst J, Dubertret C . Subthreshold bipolar disorder in a U.S. national representative sample: prevalence, correlates and perspectives for psychiatric nosography. J Affect Disord 2013; 146: 338–347.
Newson R PUNAF: Stata module to compute population attributable fractions for cohort studies http://ideas.repec.org/c/boc/bocode/s457193.html. Published October 15, 2010. Accessed November 10 2014.
Crum RM, Mojtabai R, Lazareck S, Bolton JM, Robinson J, Sareen J et al. A prospective assessment of reports of drinking to self-medicate mood symptoms with the incidence and persistence of alcohol dependence. JAMA Psychiatry 2013; 70: 718–726.
Greenland S, Drescher K . Maximum likelihood estimation of the attributable fraction from logistic models. Biometrics 1993; 49: 865–872.
Oquendo MA, Galfalvy H, Russo S, Ellis SP, Grunebaum MF, Burke A et al. Prospective study of clinical predictors of suicidal acts after a major depressive episode in patients with major depressive disorder or bipolar disorder. Am J Psychiatry 2004; 161: 1433–1441.
Kotov R, Ruggero CJ, Krueger RF, Watson D, Yuan Q, Zimmerman M . New dimensions in the quantitative classification of mental illness. Arch Gen Psychiatry 2011; 68: 1003–1011.
Insel TR, Cuthbert BN, Garvey MA, Heinssen RK, Pine DS, Quinn KJ et al. Research domain criteria (RDoC): toward a new classification framework for research on mental disorders. Am J Psychiatry 2010; 167: 748–751.
Krueger RF, Caspi A, Moffitt TE, Silva PA . The structure and stability of common mental disorders (DSM-III-R): a longitudinal-epidemiological study. J Abnorm Psychol 1998; 107: 216–227.
Krueger RF, Chentsova-Dutton YE, Markon KE, Goldberg D, Ormel J . A cross-cultural study of the structure of comorbidity among common psychopathological syndromes in the general health care setting. J Abnorm Psychol 2003; 112: 437–447.
Kendler KS, Prescott CA, Myers J, Neale MC . The structure of genetic and environmental risk factors for common psychiatric and substance use disorders in men and women. Arch Gen Psychiatry 2003; 60: 929–937.
Kessler RC, Ormel J, Petukhova M, McLaughlin KA, Green JG, Russo LJ et al. Development of lifetime comorbidity in the World Health Organization world mental health surveys. Arch Gen Psychiatry 2011; 68: 90–100.
Etkin A, Schatzberg AF . Common abnormalities and disorder-specific compensation during implicit regulation of emotional processing in generalized anxiety and major depressive disorders. Am J Psychiatry 2011; 168: 968–978.
Goldstein RZ, Volkow ND . Dysfunction of the prefrontal cortex in addiction: neuroimaging findings and clinical implications. Nature Rev Neurosci 2011; 12: 652–669.
Volkow ND, Wang GJ, Tomasi D, Baler RD . Unbalanced neuronal circuits in addiction. Curr Opin Neurobiol 2013; 23: 639–648.
Mann JJ . Neurobiology of suicidal behaviour. Nature Rev Neurosci 2003; 4: 819–828.
Kramer MD, Krueger RF, Hicks BM . The role of internalizing and externalizing liability factors in accounting for gender differences in the prevalence of common psychopathological syndromes. Psychol Med 2008; 38: 51–61.
Beck AT . Beyond belief: a theory of modes, personality, and psychopathology, in Frontiers of Cognitive Therapy, Edited by Salkovskis PM. Guilford: New York, 1996.
Takayanagi Y, Spira AP, Roth KB, Gallo JJ, Eaton WW, Mojtabai R . Accuracy of reports of lifetime mental and physical disorders: results from the Baltimore Epidemiological Catchment Area study. JAMA Psychiatry 2014; 71: 273–280.
Moffitt TE, Caspi A, Taylor A, Kokaua J, Milne BJ, Polanczyk G et al. How common are common mental disorders? Evidence that lifetime prevalence rates are doubled by prospective versus retrospective ascertainment. Psychol Med 2010; 40: 899–909.
Nock MK, Hwang I, Sampson N, Kessler RC, Angermeyer M, Beautrais A et al. Cross-national analysis of the associations among mental disorders and suicidal behavior: findings from the WHO World Mental Health Surveys. PLoS Med 2009; 6: e1000123.
Le Strat Y, Hoertel N . Correlation is no causation: gymnasium proliferation and the risk of obesity. Addiction 2011; 106: 1871–1872.
Acknowledgements
This study was supported by NIH grants DA019606, MH076051 and MH082773 and the New York State Psychiatric Institute (Drs Blanco, Oquendo and Wall), NIDA grant 1F32DA036431 (Dr Kerridge), and a fellowship grant from Public Health Expertise (Dr Hoertel). The sponsors had no additional role in the design and conduct of the study; collection, management, analysis and interpretation of the data; and preparation, review or approval of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Dr Oquendo receives royalties for the commercial use of the C-SSRS and her family owns stock in Bristol Myers Squibb. Dr Limosin is a member of the speakers/advisory boards for Janssen, Euthérapie, Lundbeck and Roche. Other authors report no conflicts of interest.
Additional information
Supplementary Information accompanies the paper on the Molecular Psychiatry website
Supplementary information
Rights and permissions
About this article
Cite this article
Hoertel, N., Franco, S., Wall, M. et al. Mental disorders and risk of suicide attempt: a national prospective study. Mol Psychiatry 20, 718–726 (2015). https://doi.org/10.1038/mp.2015.19
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2015.19
- Springer Nature Limited
This article is cited by
-
A Developmentally Informed Systematic Review and Meta-Analysis of the Strength of General Psychopathology in Childhood and Adolescence
Clinical Child and Family Psychology Review (2024)
-
Application of a Biofeedback Method in the Treatment of Depression
Neuroscience and Behavioral Physiology (2024)
-
A critical evaluation of the p-factor literature
Nature Reviews Psychology (2023)
-
Digital footprints as a new translational approach for mental health care: a commentary
Discover Mental Health (2023)
-
The effect of employment status on people with a mental disability and on daily life satisfaction: The mediating effect of acceptance of disability
Current Psychology (2022)