Abstract
Tumour-induced dysfunction of cytotoxic T cells in patients with multiple myeloma (MM) may contribute to immune escape and be responsible for the lack of therapeutic efficacy of immune checkpoint blockade. We therefore investigated dysfunctional clonal T cells in MM and demonstrated immunosenescence but not exhaustion as a predominant feature. T-cell clones were detected in 75% of MM patients and their prognostic significance was revalidated in a new post-immunomodulatory drug cohort. The cells exhibited a senescent secretory effector phenotype: KLRG-1+/CD57+/CD160+/CD28−. Normal-for-age telomere lengths indicate that senescence is telomere independent and potentially reversible. p38-mitogen-activated protein kinase, p16 and p21 signalling pathways known to induce senescence were not elevated. Telomerase activity was found to be elevated and this may explain how normal telomere lengths are maintained in senescent cells. T-cell receptor signalling checkpoints were normal but elevated SMAD levels associated with T-cell inactivation were detected and may provide a potential target for the reversal of clonal T-cell dysfunction in MM. Low programmed death 1 and cytotoxic T-lymphocyte-associated antigen 4 expression detected on T-cell clones infers that these cells are not exhausted but suggests that there would be a suboptimal response to immune checkpoint blockade in MM. Our data suggest that other immunostimulatory strategies are required in MM.
Similar content being viewed by others
Introduction
The failure of immune surveillance in human cancer can be attributed to tumour-induced molecular and cellular mechanisms that incapacitate immune cells and effector responses, including tumour-specific cytotoxic T cells, which allows for tumour progression. Immune cells introduced as adoptive cellular immunotherapy can also be suppressed.1, 2 Thus overcoming tumour-induced T-cell hypo-responsiveness is an important consideration for immune therapies. However, the underlying mechanisms of dysfunction must first be characterised.
Immune dysfunction in patients with multiple myeloma (MM) is multifactorial and includes transforming growth factor-β (TGF-β)-induced dendritic cell dysfunction,3 regulatory T-cell/T helper type 17 cell imbalance,4, 5 generation of acquired regulatory T cells by trogocytosis6 and increased myeloid-derived suppressor cells.7 Tumour-induced immune dysfunction is also greater in patients with MM than other B-cell malignancies.5, 6, 7, 8, 9 T-cell dysfunction appears to be restricted to those cells affected by the MM cancer cells as patients with MM do not exhibit the classical pattern of infections associated with a T-cell immunodeficiency state, such as fungal and mycobacterial infections.
Dysfunctional T cells observed in cancer can be classified as anergic, exhausted or senescent according to phenotypic characteristics (Figure 1 and Table 1).10 Anergic T cells are hypo-responsive owing to inadequate T-cell receptor (TCR) co-stimulation through CD28 signaling or in the presence of high co-inhibitory signalling such as cytotoxic T-lymphocyte-associated antigen 4 (CTLA-4)11 and the cells fail to produce IL-2.12 T-cell exhaustion occurs after chronic antigen overstimulation and results in the upregulation of 64 multiple inhibitory receptors, including programmed death 1 (PD-1), CTLA-4, CD160, T-cell immunoglobulin and mucin protein-3 (Tim-3) and lymphocyte activation gene-3 (LAG-3), and an inability to express interferon-γ.13−15 Senescent T cells are late differentiated memory T cells generally associated with aging. They lack CD28, express regulatory receptors, are in cell-cycle arrest and have enhanced secretion of inflammatory cytokines.16 There are two types: telomere-dependent senescence (replicative senescence), which results from telomere attrition triggered by DNA damage, p53 protein or cyclin-dependent kinase inhibitor (CDKI) p21CIP1/WAF1 (p21) pathways;17 and telomere-independent senescence, which is induced by stress and an altered signal transduction pathway generally involving the CDKI p16INK4a (p16) and the retinoblastoma tumour-suppressor (pRb).18 Nuclear factor (NF)-κB signaling has also been implicated in the induction of a phenomenon known as senescence-associated secretory phenotype (SASP). These cells are senescent but retain their ability to secrete pro-inflammatory factors.19
Different types of dysfunctional T cells in cancer. Dysfunctional T cells can be classified as anergic, exhausted or senescent based on different phenotypic markers or activated signalling pathways. Anergic T cells are induced when there is incomplete co-stimulation provided by CD28 during TCR ligation or in the presence of high co-inhibitory signalling by CTLA-4. Exhausted T cells result from chronic overstimulation and results in the overexpression of multiple inhibitory markers, such as PD-1, CTLA-4, CD160, Tim-3 and LAG-3. Senescent T cells are associated with aging and the natural lifespan of cells and express markers CD57, CD160 and KLRG-1 and lack CD28. Telomere-dependent senescent cells are characterised by shortened telomeres and cell-cycle arrest and upregulated p16 and p21 pathways (replicative senescence). Telomere-independent senescent cells have normal telomeres, possibly maintained with upregulated telomerase activity, and senescence can be induced by an upregulated p38-MAPK pathway (Adapted from Crespo et al.10).
Cytotoxic T cells are the predominant effector cell involved in cancer immune destruction, and expanded clones of cytotoxic T cells exist in patients with MM,20, 21, 22 chronic myeloid leukemia,23, 24 Waldenström’s macroglobulinemia (WM)25 and myelodysplastic syndromes.26, 27 The T-cell clones in MM patients can constitute up to 50% of all blood lymphocytes and are hypo-responsive in vitro,4, 25 but despite this, their presence is related to better survival.20, 21, 22, 28, 29 Overcoming the hypo-responsiveness of these cells, regardless of their specificity, could provide a novel cell therapy based on the restoration of the host’s immune response.
In this study, a large cohort of MM patients was tested to verify the prognostic advantage of expanded T-cell clones in patients receiving current therapy including novel agents. We identified MM T-cell clones as telomere-independent senescent cells and attempted to identify agents that were responsible for inducing senescence. We also demonstrated normal TCR signalling and low PD-1 and CTLA-4 expression. This suggests that the response to immune checkpoint blockade therapy would be suboptimal in MM. In addition, we have identified abnormalities in p-SMAD levels in the TGF-β pathway that could be responsible for dysfunction in these cells and suggest that this may provide a novel target for immune recovery therapy.
Methods
Patients
Peripheral blood (PB) and bone marrow (BM) samples were collected from 103 MM patients attending our clinic. Sample collection and clinical record review from patients and aged-matched normal controls were performed after patient informed consent and approval by the institutional Human Ethics Review Committee (X12-0205) in accordance with the Declaration of Helsinki. The clinical characteristics of the different patient cohorts are shown in Supplementary Table S1.
Flow cytometric analysis
Peripheral blood mononuclear cells (PBMC) were obtained by Ficoll Paque (GE Healthcare, Uppsala, Sweden). Flow cytometric analysis was performed on a BD FACS Canto II (BD Biosciences, San Jose, CA, USA) and flow sorting was performed on a BD FACS ARIA II (BD Biosciences). Clonal T cells were classified as CD3+/CD8+/TCR-Vβ+/CD57+ (hereafter clones) and were compared with the internal biological control: non-clonal T cells, which were CD3+/CD8+/TCR-Vβ−/CD57+ (hereafter non-clonal or Vβ-57+). Two other CD8+ subsets: Vβ+CD57− and Vβ-CD57−, were also included.
TCR-Vβ repertoire analysis
Patients were screened for clonal T-cell expansions by analysis of the TCR-Vβ (hereafter Vβ) repertoire (Supplementary Figure S1) using an IOTest Beta Mark TCR-Vβ Repertoire Kit (Beckman Coulter, Brea, CA, USA) as previously described.4, 25, 29 Vβ+ clones were identified by the overexpression of a Vβ family defined as greater than the mean+3 s.d. after Vβ analysis of 42 age-matched controls for each Vβ family.
CFSE (carboxyfluorescein succinimidyl ester) proliferation assay
CFSE-labelled clonal and non-clonal T cells were stimulated with anti-CD3/CD28 MACS iBeads (Miltenyi Biotec, Bergisch Gladbach, Germany) at a 1:1 ratio and 0.1 μg/ml interleukin (IL)-2 (R&D Systems, Minneapolis, MN, USA) for 4 days, as previously described.4 The effect of 0.1 μg/ml IL-12 (R&D Systems), 20 ng/ml IL-15 (R&D Systems), 50 ng/ml IL-21 (Invitrogen Corporation, Camarillo, CA, USA), 50 ng/ml anti-CD137 (BD Biosciences), 50 ng/ml anti-CD134 (BD Biosciences) and 5 μm lenalidomide (Celgene Corporation, San Diego, CA, USA) on T-cell proliferation was also tested.
14-Day ex vivo expansions
Purified T-cell clones from MM patients were expanded using the Miltenyi T-cell Activation/Expansion Kit according to the manufacturer’s protocol. In brief, T cells were stimulated at a ratio of 1:1 with anti-CD3/28 beads and cultured in RPMI supplemented with 10% AB serum and 20 units IL-2/ml (R&D) in a 96-well U-bottommed plate (BD Biosciences) for 14 days.
Phospho-flow analysis of signalling pathways
For phospho-flow cytometry (PFC) analysis of phosphorylated (p) proteins: p-SMAD2 (pS465/pS467)/ p-SMAD3 (pS423/pS425) (pSMAD), p-SHP-2 (pY542), p-p38-MAPK (mitogen-activated protein kinase) (pT180/pY182) (BD Biosciences), PBMC were labelled with anti-CD8 PE-Cy7 and phycoerythrin (PE)- or fluorescein isothiocyanate (FITC)-conjugated anti-Vβ. Cells were fixed with BD Cytofix buffer (BD Biosciences) at 37 °C and then permeabilised with ice-cold BD Perm III Buffer (BD Biosciences). Cells were labelled with anti-CD57 efluor-450 (BioLegend, San Diego, CA, USA), CD3 PerCP-Cy5.5 (BD Biosciences) and anti-phospho-antibody.
For p-ZAP-70 (pY142), CD3-ζ, p16 (BD Biosciences), p21 (Genesearch, Arundel, QLD, Australia) and Bcl-xL (Abcam, Cambridge, UK), cells were stained with surface markers to identify clonal T cells and then fixed and permeabilised with BD Cytofix/Cytoperm (BD Biosciences) on ice. Cells were washed twice with BD Perm/Wash buffer before incubation with intracellular antibody. Phospho-extracellular signal–regulated kinase (p-ERK; BD Biosciences) was studied using the Beckman Coulter Perfix-P Kit (Beckman Coulter) according to the manufacturer’s instructions. Fluorescence minus one controls were used to establish positive expression limits and determine constitutive phosphorylated protein expression.
Phenotypic analysis of T-cell clones
The surface phenotype was studied using flow cytometry (FC) to classify the T-cell clones as either anergic, exhausted or senescent.10 Three antibody panels were used: all with anti-CD3 V500, anti-CD8 APC-H7, anti-CD57 V450 (BD Biosciences) and anti-Vβ PE/FITC (Beckman Coulter) for the identification of T-cell clones and then (1) anti-PD1 PE-Cy7 and anti-PD-L1 FITC/PE (BD Biosciences); (2) anti-LAG-3 APC (R&D Systems) and anti-TIM-3 PE-Cy7 (BioLegend) or (3) CD27 FITC/PE and CD28 PerCP-Cy5.5 (BD Biosciences). The senescent phenotype was studied by flow detection of KLRG-1 (Biolegend) and intracellular p16, p21 and p38-MAPK (BD Biosciences) and measurement of telomere length (TL) by quantitative PCR (qPCR) and flow–fluorescence in situ hybridization (flow-FISH).
Telomere assessment by qPCR
DNA was extracted using the Maxwell 16-Cell Low Elution Volume DNA Purification Kit (Promega, Madison, WI, USA) and cryopreserved for PCR. Assessment of TL was performed according to previous methods.30, 31 All PCR reactions were performed in triplicate on the Rotorgene Q (Qiagen, Hilden, Germany). Relative TL was calculated by dividing the telomeric DNA quantity by the single copy gene DNA quantity (T/S). T/S of MM patient T-cell clones were compared with an age-matched normal range established by Dr P Barbaro, Children’s Medical Research Institute, Westmead, NSW, Australia.
Telomere assessment by flow-FISH
TL was also measured using the DAKO Telomere PNA Kit/FITC (Elitech, Braeside, VIC, Australia) according to the manufacturer’s protocol. Relative TL was calculated by comparing the TL of patient cells to a control cell line with long telomeres (CCRF-CEM; kindly provided by Dr Tatjana Kilo).
Measurement of telomerase by FC
Human telomerase reverse transcriptase (hTERT), the catalytic subunit of human telomerase was measured by FC. PBMC were fixed and permeabilised using the Leucoperm Kit (AbD Serotec, Oxford, UK), labelled with purified anti-hTERT (1:200; Clone 2C4, Thermo Scientific, Scoresby, VIC, Australia) or purified mouse anti-IgM κ isotype control (1:100, BD Biosciences). Cells were washed, labelled with secondary goat anti-mouse Ig-APC (1:100, BD Biosciences) and then washed twice before labelling with clonal T-cell surface antibodies.
Statistical analysis
Statistical analysis using Student's t-test, Mann–Whitney test and Kaplan–Meier survival curves were performed using Prism (Version 6, GraphPad Software, La Jolla, CA, USA).
Results
Expanded T-cell clones in patients with MM are associated with an improved survival and have an increased incidence post-immunomodulatory drug (post-IMiD) therapy
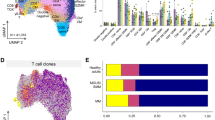
Clonal T-cell expansions were detected in 75% of MM patients and >90% were CD8+. Of the patients who had received therapy, 70% had received IMiDs. The presence of T-cell clones at any stage of disease was associated with an improved survival (χ2=21.01; P<0.0001; Figure 2a). There was no correlation between the presence of T-cell clones and disease status, as was shown previously,20, 28 nor with International Staging System stage, previous treatment or current treatment (Supplementary Table S2). Exposure to thalidomide induces additional T-cell clones in patients, raising their frequency from approximately 50% to 76%,28 which was similar to the incidence of 75% identified in this study (Table 2). There was no prognostic advantage for patients with a large clone size (>20% of CD3+ cells) compared with a moderate clone size (<20% of CD3 cells) (χ2=0.11; P=not significant (NS); Figure 2b). There was also no preferential usage of any one TCR-Vβ family (Figure 2c).
Prognostic significance of T-cell clones in MM. (a) Overall survival of 103 MM patients in this cohort according to the presence of T-cell clones (χ2=21.01; P<0.0001). (b) Overall survival of patients with large clone size (>20% of all CD3+ cells) and moderate clone size (<20% but >3 s.d. of age-matched mean; χ2=0.11; P=NS). (c) Incidence of the TCR-Vβ families among the T-cell expansions.
Clonal T cells in MM are hypo-responsive and fail to respond to a panel of immune modulators
T-cell clones from MM patients (n=15) failed to proliferate when stimulated with anti-CD3/28 beads, whereas non-clonal T cells showed active proliferation in 4-day cultures (P<0.0001; Figure 3b). The addition of potential immune modulators as well as anti-CD2/3/28 beads and IL-2 failed to increase the proliferation of the T-cell clones in vitro (Figure 3c). We previously reported that MM patients surviving >10 years invariably demonstrate clonal expansions that have proliferative capacity.4 This was re-examined using an expanded 10-year MM survivor group and the same correlation was found (n=32; Figure 3b). The lack of response of clonal and non-clonal T cells from a representative 10-year MM survivor to a variety of immune modulators is also shown in Supplementary Figure S2. In 14-day ex vivo expansions, flow-sorted clonal T cells from six of the eight 10-year MM survivors could be expanded, whereas six of the seven non-10-year survivors did not expand (Figure 3d).
Proliferation of T-cell clones in MM. T-cell clones were stimulated with anti-CD3/28 beads for 4 days and proliferation was tracked with CFSE. Proliferation was measured as the percentage of cells that had undergone >1 cell division. (a) Representative histogram measuring CD8+ T-cell proliferation using CFSE. (shaded: unstimulated; unshaded: stimulated). (b) Proliferation of clonal and non-clonal T cells from 10-year survivor and non-10-year survivor MM patients. (t=6.675; P<0.0001). (c) Effect of different immune modulators on clonal T-cell proliferation as compared with cells stimulated with anti-CD3/28 beads and IL-2 only. (d) Fourteen-day ex vivo expansions of clonal T cells from 10-year survivor (mean fold expansion: 19.5) and non-10-year survivor (mean fold expansion=1.0) MM patients.
MM T-cell clones have normal TCR signalling
Components of the TCR-signalling pathway (Supplementary Figure S3) were assessed by PFC. Following TCR engagement, the tyrosine kinase ZAP-70 is required for activation of downstream signalling pathways.32 Both constitutive and stimulated p-ZAP-70 expression was present at similar levels in MM T-cell clones compared with non-clonal T cells (n=18). SHP-2 is a tyrosine phosphatase that dephosphorylates signalling molecules and dampens T-cell signalling.33 There was a trend for both constitutive and stimulated p-SHP-2 levels to be higher in the T-cell clones compared with non-clones, but this was not statistically significant (n=12). CD3-ζ, a TCR component,34 was present at significantly higher levels on clonal T cells compared with non-clonal T cells (n=19; P<0.02) suggesting that signal transduction was not impaired (Supplementary Figure S4).
MM T-cell clones have a defective p-SMAD pathway that blocks cell-cycle progression
We previously identified several dysfunctional pathways in expanded T-cell clones in WM by bioinformatic analysis of microarray expression data.25 We selected key protein targets from these pathways (Supplementary Figure S3) and examined the expression levels by PFC in clonal and non-clonal T cells from 10-year and non-10-year survivors of MM.
In the TOB pathway, TGF-β stimulates p-SMAD, which can interact with Tob to maintain T-cell inactivation. Tob can also interact with CDKI p27kip1 causing cell-cycle arrest.35 Expression of p-SMAD did not differ between the different CD8+ T-cell subsets studied when all MM patients were analysed together (n=11; Supplementary Figure S5B). However, significantly higher levels of this phosphorylated protein were found in non-proliferative T-cell clones of non-10-year survivors compared with proliferative T-cell clones of 10-year MM survivors (U=5.0; P=0.01; Supplementary Figure S5C). Treatment and disease status did not impact these findings (Supplementary Table S1).
No significant differences were found between different CD8+ T-cell subsets studied or between T-cell clones of 10-year and non-10-year survivors for p-ERK (related to proliferation36) or Bcl-xL (antiapoptotic protein37) (Supplementary Figure S5).
Low PD-1 and CTLA-4 expression suggests that immune checkpoints are not responsible for hypo-responsiveness and may not be appropriate therapeutic targets in patients with MM
For immune checkpoint blockade to be successful in MM, it is essential that antigen-specific effector CD8+ T cells are present and that these cells can recognise myeloma-specific targets. As clonal T cells in MM are possibly tumour-specific T cells, we examined CTLA-4 and PD-1 expression on PB and BM T cells from MM patients and age-matched controls. The T-cell clones expressed significantly lower levels of PD-1 than the non-clonal T cells in both PB (n=12; P=0.0005; Figure 4b) and BM (n=11; P=0.02; Figure 4c) and also in comparison to CD8+ CD57+ T cells from age-matched normal controls (U=11; P=0.01). Similarly, CTLA-4 expression was significantly lower on T-cell clones found in the PB compared with non-clonal cells (n=19; P=0.005; Figure 4e) but this was not significantly different in the BM (n=4; Figure 4f).
Immune checkpoints on MM T-cell clones. Representative histograms measuring (a) PD-1 and (d) CTLA-4 on PB clonal T cells from an MM patient. PD-1 expression on clonal and non-clonal T cells in both (b) PB (P=0.0005) and (c) BM (P=0.02) of MM patients. CTLA-4 expression on clonal and non-clonal T cells in both (e) PB (P=0.005) and (f) BM (P=NS) of MM patients.
MM T-cell clones have a phenotype that suggests a state of telomere-independent senescence rather than anergy or exhaustion
MM T-cell clones expressed low levels of LAG-3, TIM-3 (n=9; Figures 5b and c), PD-1 and CTLA-4 (Figures 4b and e) and did not express CD28 (Figure 5e). The expression of these molecules did not differ from non-clonal T cells. Based on the exclusion of these phenotypic markers, T-cell clones are not anergic or exhausted. T-cell clones in MM patients are CD57+, express CD160 (n=9; Figure 5d) and are of the late differentiated phenotype as demonstrated by the lack of CD27 and CD28. KLRG-1 was expressed at significantly higher levels on T-cell clones than on non-clonal T cells (n=8; t=4.60; P<0.003; Figure 5f). Based on these phenotypic markers, T-cell clones are senescent.
Expression of anergic/exhausted/senescent phenotypic markers and TL measurement of MM T-cell clones. (a) Representative histograms of phenotypic markers (LAG-3, TIM-3, CD160, KLRG1) and the expression of CD27 and CD28 on MM T-cell clones for the classification of T-cell clones as anergic, exhausted or senescent. (b) LAG-3 expression on clonal T cells as compared with non-clonal T cells (P=NS). (c) TIM-3 expression on clonal T cells as compared with non-clonal T cells (P=NS). (d) CD160 expression on MM CD8+ T cells. (e) Classification of T-cell clones into late-stage phenotype (CD27−CD28−) or intermediate (int) stage phenotype (CD27+CD28−) (f) KLRG-1 expression on clonal T cells as compared with non-clonal T cells (t=4.60; P<0.003). (g) TL measurement by qPCR (T/S: telomere:single copy gene ratio) of clonal and non-clonal T cells (P=NS). (h) Representative analysis of TL by flow-FISH in a MM patient according to fluorescence of fluorescein-conjugated telomeric probes. (i) TL measurement (relative telomere length: RTL) by flow-FISH of clonal T cells and non-clonal T cells and CD8+CD57+ T cells from age-matched normal controls (P=NS).
TL measurement by qPCR demonstrated that clonal T cells did not have shortened telomeres compared with non-clonal T cells (n=4; Figure 5g) and an age-matched normal range (data not shown). Likewise, the TL of clonal T cells as measured by flow-FISH (Figure 5h) was not significantly different from non-clonal T cells or age-matched normal controls (n=5; Figure 5i). Telomerase activity (hTERT levels) was significantly higher in T-cell clones than in non-clonal cells (data not shown; t=2.35; P<0.04).
Table 1 summarises the phenotype of T-cell clones from MM patients and compares this with the phenotype of anergic, exhausted and senescent T cells. The results suggest that the T-cell clones of patients with MM are telomere-independent senescent cells. Treatment and disease status did not impact these findings (Supplementary Table S1).
Telomere-independent senescence cannot be attributed to involvement of p38-MAPK signalling or elevated p16 or p21 pathways
Blockade of p38-MAPK signalling has reversed telomere-independent senescence in CD4+CD45RA+CD27− T cells38 and in CD8+ effector memory T cells that re-express CD45RA (EMRA) T cells.39, 40 We studied the p38 signalling pathway in T-cell clones by PFC to determine whether elevated p-p38-MAPK signalling was responsible for inducing senescence. Constitutive p-p38 expression in T-cell clones did not differ from other T-cell subsets (n=7) and phorbol myristate acetate (PMA) stimulation did not augment p38 levels (n=6; Supplementary Figure S6), indicating that this pathway was not responsible for inducing senescence.
The p16 and p21 proteins can maintain Rb in a hypo-phosphorylated, active state to initiate and sustain cell-cycle arrest;18 however, the levels of these proteins were not elevated in T-cell clones, compared with the other CD8 T-cell subsets (n=13; n=12; Supplementary Figure S7). Thus the telomere-independent senescence of the MM T-cell clones appears to relate to other mechanisms.
Discussion
Expanded CD8+ T-cell clones present in the blood of patients with MM have previously been shown to be associated with a good prognosis.20, 28 Using a new cohort of patients, we have validated the association between the presence of T-cell clones, at all stages of the disease, with a favourable prognosis and shown an increased incidence of T-cell clones after IMiD therapy. However, these cells are hypo-responsive and fail to proliferate in vitro. Whether these potentially protective cytotoxic T cells are anergic, exhausted or senescent could help determine whether their hypo-responsiveness is reversible, regardless of their specificity. We have made the important new observation that the T-cell clones displayed features of senescent T cells: that is, KLRG-1+, CD57+, CD160+, and CD28− cell surface phenotype. A key finding of this study is that these clonal cells have TLs that are identical to the non-clonal T cells of age-matched controls, which suggests that their senescence is telomere independent and potentially reversible.
A plausible explanation for the presence of senescent T cells that do not have shortened telomeres is the upregulation of telomerase to maintain TL during long-term persistence. T-cell clones had significantly higher levels of hTERT than non-clonal T cells. The T-cell clones in MM are highly differentiated EMRA and studies have shown that, while EMRA T cells do have shorter telomeres than naive CD8 T cells, they have longer telomeres than effector memory T cells that express CD45RO (EM).39
Immune dysfunction in cancer may be mediated by the downregulated expression of TCR-related signalling proteins.41 An earlier study of MM patients revealed slightly lower levels of CD3-ζ chain and ZAP-70 expression in resting CD4+ and CD8+ T cells when compared with healthy controls, and after in vitro activation with super antigen staphylococcal enterotoxin B, both proteins were significantly downregulated. This was more pronounced in patients with stage III MM.42 In contrast, we found that these two TCR-signalling proteins were not significantly downregulated in T-cell clones when compared with non-clonal T cells or healthy controls (data not shown). This difference may be explained by the fact that we measured the more functionally relevant ZAP-70 in the phosphorylated state (pY292), whereas the previous MM study measured total ZAP-70 protein.42 We also measured pZAP-70 after hydrogen peroxide stimulation but no significant difference between clonal and non-clonal T cells was found. The TCR-signalling pathway can also be inhibited by PD-1-mediated recruitment of SHP-2 to inactivate T cells. It has been demonstrated that, with aging T cells associated with replicative senescence, there may be an imbalance of positive and negative TCR signalling, with increased inhibitory signalling through SHP1/2.43 However, after TCR ligation with anti-CD3/28 beads, both constitutive and stimulated pSHP-2 levels did not differ between clonal and non-clonal T cells, suggesting that SHP-2 does not have an inhibitory effect on T-cell signalling. Furthermore, we have shown that PD-1 expression is low on these T-cell clones, implying minimal SHP-2 recruitment. These data suggest that there is no abnormality in the TCR signalling in the MM T-cell clones.
TGF-β-dependent p-SMAD activation has been shown to inhibit CD3/28-mediated T-cell proliferation in mouse models.44 We detected significantly higher levels of this protein in the T-cell clones of non-10-year survivors, which are non-proliferative after CD3/28 activation, suggesting that this is a possible molecular target to reverse hypo-responsiveness.
To characterise the mechanism of senescence induction in T-cell clones, we examined pathways that are associated with telomere-dependent and -independent senescence. Telomere-independent senescence is induced in response to cellular stress or disruptions to normal cell signalling, such as upregulation of p16 and Rb, leading to an antiproliferative state.45 Senescence triggered by shortened telomeres (telomere-dependent senescence) is regulated by signalling through ATM to p53, leading to the upregulation of p21 and therefore cell-cycle arrest.17 Elevated levels of p16 were not detected in the T-cell clones of MM patients and they were not different from non-clonal T cells, indicating that the p16 pathway is not responsible for inducing clonal T-cell senescence. Our data correlate with a study which also showed that senescent cells with average TL had low levels of p16.46 Cells with low levels of p16 at senescence are able to proliferate again after p53 inactivation, whereas cells with high p16 are unable to proliferate after p53 inactivation,45 suggesting that it may be possible to reactivate the MM T-cell clones. MM T-cell clones did not have upregulated p21 expression and therefore do not have telomere-dependent senescence.
The p38-MAPK pathway has been implicated in senescence and blocking of this pathway has successfully reversed senescence in CD4+ CD27−CD28− T cells38 and CD8+ EMRA T cells.39, 40 T cells had either high constitutive p38-MAPK expression or, upon PMA activation, were unable to upregulate p38-MAPK expression to the levels of non-senescent T cells. Our data indicate that constitutive p38-MAPK levels are not elevated in clonal T cells, and upon PMA activation, there was no impairment of p38-MAPK upregulation when compared with non-clonal T cells. These results suggest that this pathway does not have a role in inducing senescence in MM T-cell clones.
Other cell signalling molecules may be responsible for inducing senescence in MM T-cell clones. NF-κβ signalling is required for the maintenance of SASP19 and inhibition of this pathway can bypass growth arrest and reverse senescence.47 IL-6, a cytokine present at high levels in the MM microenvironment, has been described as a key player in oncogene-induced senescence48 and can upregulate NF-κβ signalling, while preventing apoptosis to maintain cell senescence.19 MM T-cell clones retain their ability to produce interferon-γ4 and display the characteristics of SASP, so the NF-κβ pathway should be investigated. Overexpression of c-myc can also cause cell senescence as part of a cancer defence mechanism.49 Microarray data from WM T-cell clones indicated that c-myc and NF-κβ were upregulated in T-cell clones,25 and the relationship between these proteins and clonal T-cell responses need to be explored in the MM setting. In mouse models, KLRG-1+/CD8+ T-cell senescence was related to p15 INK4b expression. The human equivalent of this protein is P14 ARF.50 Further investigation of the levels of these other cell-cycle regulatory proteins is required to elucidate the mechanism of senescence induction.
The finding that these MM T-cell clones are senescent rather than anergic or exhausted is significant. T cells in the cancer setting are usually considered to be exhausted, similar to the T cells observed in patients with chronic viral infection owing to the constant exposure to high levels of tumour antigens and an immunosuppressive microenvironment.51 Exhausted T cells commonly express the inhibitory receptors PD-1, LAG-3, TIM-3 and CTLA-4 and have dysregulated signalling pathways.14, 52 The MM T-cell clones expressed low levels of these inhibitory receptors. They are also unlike the exhausted T cells found in melanoma patients, a highly antigenic tumour, which have high levels of PD-1 and therefore are susceptible to PD-1 blockade. Anergic T cells are induced during inadequate TCR co-stimulation or in the presence of high inhibitory signalling, which may be present in the cancer microenvironment. The hypo-responsiveness of the MM T-cell clones, however, cannot be reversed with endogenous IL-2 and inhibitory receptors such as CTLA-4 and PD-1 are not highly expressed. MM T-cell clones are also unlike an aged T-cell (replicative senescence) as they do not have shortened telomeres exhibited by T cells that have gone through multiple rounds of proliferation. The MM T-cell clones are held in a suspended non-proliferative state and persist for long periods of time owing to inhibition of apoptosis. T-cell clones in MM are also not expansions of large granular lymphocytes. They exhibit the same phenotype (CD3+CD8+CD57+) but do not have increased signal transducer and activator of transcription factor 3 expression (data not shown) that is associated with large granular lymphocytic leukaemia.53 As MM T-cell clone immunosenescence is not related to shortened telomeres, we believe that it is potentially reversible if the mechanisms of senescence induction can be elucidated. If it is related to dysfunctional signalling pathways, it may be possible to remodulate the pathways with small-molecule inhibitors or drugs, such as IMiDs or histone deacetylase inhibitors.
We have highlighted the low expression of immune checkpoint target PD-1 on T-cell clones found in the BM in a previous report.54 This study extends that observation, documenting low levels of PD-1 and CTLA-4 detected on T-cell clones that may explain why Phase 1 studies of PD-1 inhibitor Nivolumab failed to provide a meaningful clinical response in 100% of MM patients.55 It may be worthwhile to continue investigation of immune checkpoint blockade as part of combination therapy in MM. It has recently been demonstrated that lenalidomide can enhance immune checkpoint blockade-induced immune responses in myeloma.56 The reason for downregulated PD-1 expression in T-cell clones in MM is unknown and transcription factors that regulate PD-1 expression, including T-bet or Blimp-1,57, 58 are under investigation. Interestingly, it has also been reported that T-bet controls cytotoxic and cytokine secretory functions of CD8+ effector T cells and also the sensitivity of cells to senescence.59
In conclusion, the T-cell clones in MM have a distinct molecular signature of telomere-independent senescence rather than anergy or exhaustion. An improved understanding of the mechanisms involved in the induction of these senescent clonal T cells and how their cellular functions are affected has provided potential targets to restore clonal T-cell function, including pSMAD. This may present a unique opportunity to enhance tumour immunity in MM.
References
Kofler DM, Chmielewski M, Rappl G, Hombach A, Riet T, Schmidt A et al. CD28 costimulation impairs the efficacy of a redirected T-cell antitumor attack in the presence of regulatory T cells which can be overcome by preventing Lck activation. Mol Ther 2011; 19: 760–767.
Motz GT, Coukos G . Deciphering and reversing tumor immune suppression. Immunity 2013; 39: 61–73.
Brown R, Pope B, Murray A, Esdale W, Sze DM, Gibson J et al. Dendritic cells from patients with myeloma are numerically normal but functionally defective as they fail to up-regulate CD80 (B7-1) expression after huCD40LT stimulation because of inhibition by transforming growth factor-beta1 and interleukin-10. Blood 2001; 98: 2992–2998.
Bryant C, Suen H, Brown R, Yang S, Favaloro J, Aklilu E et al. Long-term survival in multiple myeloma is associated with a distinct immunological profile, which includes proliferative cytotoxic T-cell clones and a favourable Treg/Th17 balance. Blood Cancer J 2013; 3: e148.
Favaloro J, Brown R, Aklilu E, Yang S, Suen H, Hart D et al. Myeloma skews regulatory T and pro-inflammatory T helper 17 cell balance in favor of a suppressive state. Leuk Lymphoma 2014; 55: 1090–1098.
Brown R, Kabani K, Favaloro J, Yang S, Ho PJ, Gibson J et al. CD86+ or HLA-G+ can be transferred via trogocytosis from myeloma cells to T cells and are associated with poor prognosis. Blood 2012; 120: 2055–2063.
Favaloro J, Liyadipitiya T, Brown R, Yang S, Suen H, Woodland N et al. Myeloid derived suppressor cells are numerically, functionally and phenotypically different in patients with multiple myeloma. Leuk Lymphoma 2014; 55: 2893–2900.
Brown R, Suen H, Favaloro J, Yang S, Ho PJ, Gibson J et al. Trogocytosis generates acquired regulatory T cells adding further complexity to the dysfunctional immune response in multiple myeloma. Oncoimmunology 2012; 1: 1658–1660.
Brown RD, Joshua DE . T-cell responses in myeloma. In: Munshi N, Anderson K (eds). Advances in Biology and Therapy of Multiple Myeloma vol. 2. Springer: New York, NY, USA, 2013, pp 3–24.
Crespo J, Sun H, Welling TH, Tian Z, Zou W . T-cell anergy, exhaustion, senescence, and stemness in the tumor microenvironment. Curr Opin Immunol 2013; 25: 214–221.
Choi S, Schwartz RH . Molecular mechanisms for adaptive tolerance and other T-cell anergy models. Semin Immunol 2007; 19: 140–152.
Schwartz RH . T-cell anergy. Annu Rev Immunol 2003; 21: 305–334.
Blackburn SD, Shin H, Haining WN, Zou T, Workman CJ, Polley A et al. Coregulation of CD8+ T-cell exhaustion by multiple inhibitory receptors during chronic viral infection. Nat Immunol 2009; 10: 29–37.
Fourcade J, Sun Z, Pagliano O, Guillaume P, Luescher IF, Sander C et al. CD8(+) T cells specific for tumor antigens can be rendered dysfunctional by the tumor microenvironment through upregulation of the inhibitory receptors BTLA and PD-1. Cancer Res 2012; 72: 887–896.
Woo S-R, Turnis ME, Goldberg MV, Bankoti J, Selby M, Nirschl CJ et al. Immune inhibitory molecules LAG-3 and PD-1 synergistically regulate T-cell function to promote tumoral immune escape. Cancer Res 2012; 72: 917–927.
Dock JN, Effros RB . Role of CD8 T-cell replicative senescence in human aging and in HIV-mediated immunosenescence. Aging Dis 2011; 2: 382–397.
Herbig U, Jobling WA, Chen BPC, Chen DJ, Sedivy JM . Telomere shortening triggers senescence of human cells through a pathway involving ATM, p53, and p21CIP1, but not p16INK4a. Mol Cell 2004; 14: 501–513.
Campisi J, d'Adda di Fagagna F . Cellular senescence: when bad things happen to good cells. Nat Rev Mol Cell Biol 2007; 8: 729–740.
Salminen A, Kauppinen A, Kaarniranta K . Emerging role of NF-κB signaling in the induction of senescence-associated secretory phenotype (SASP). Cell Signal 2012; 24: 835–845.
Brown R, Yuen E, Nelson M, Gibson J, Joshua D . The prognostic significance of T-cell receptor beta gene rearrangements and idiotype-reactive T cells in multiple myeloma. Leukemia 1997; 11: 1312–1317.
Raitakari M, Brown RD, Gibson J, Joshua DE . T cells in myeloma. Hematol Oncol 2003; 21: 33–42.
Joshua D, Brown R, Sze DM, Raitakari M, Gibson J, Ho PJ et al. The role of T cells in myeloma. Hematol J 2003; 4: S26–S28.
Li Y, Yang LJ, Chen SH, Zhang YP, Zhang XL, Luo GX . T-cell receptor Vbeta repertoire usage and clonal expansion of T cells in chronic myelogenous leukemia. Chin Med J 2004; 117: 840–843.
Mustjoki S, Ekblom M, Arstila TP, Dybedal I, Epling-Burnette PK, Guilhot F et al. Clonal expansion of T/NK-cells during tyrosine kinase inhibitor dasatinib therapy. Leukemia 2009; 23: 1398–1405.
Li J, DM-Y Sze, Brown RD, Cowley MJ, Kaplan W, Mo S-L et al. Clonal expansions of cytotoxic T cells exist in the blood of patients with Waldenström macroglobulinemia but exhibit anergic properties and are eliminated by nucleoside analogue therapy. Blood 2010; 115: 3580–3588.
Epling-Burnette P, Painter JS, Rollison DE, Ku E, Vendron D, Widen R et al. Prevalence and clinical association of clonal T-cell expansions in myelodysplastic syndrome. Leukemia 2007; 21: 659–667.
Vries Ad, Langerak AW, Verhaaf B, Niemeyer CM, Stary J, Schmiegelow K et al. T-cell receptor Vbeta CDR3 oligoclonality frequently occurs in childhood refractory cytopenia (MDS-RC) and severe aplastic anemia. Leukemia 2008; 22: 1170–1174.
Brown R, Spencer A, Ho PJ, Kennedy N, Kabani K, Yang S et al. Prognostically significant cytotoxic T-cell clones are stimulated after thalidomide therapy in patients with multiple myeloma. Leuk Lymphoma 2009; 50: 1860–1864.
Sze D, Giesajtis G, Brown RD, Raitakari M, Gibson J, Ho J et al. Clonal cytotoxic T cells are expanded in myeloma and reside in the CD8(+)CD57(+)CD28(-) compartment. Blood 2001; 98: 2817–2827.
Aviv A, Hunt SC, Lin J, Cao X, Kimura M, Blackburn E . Impartial comparative analysis of measurement of leukocyte telomere length/DNA content by Southern blots and qPCR. Nucleic Acids Res 2011; 39: e134.
Cawthon RM . Telomere measurement by quantitative PCR. Nucleic Acids Res 2002; 30: e47.
Au-Yeung BB, Deindl S, Hsu L-Y, Palacios EH, Levin SE, Kuriyan J et al. The structure, regulation, and function of ZAP-70. Immunol Rev 2009; 228: 41–57.
Qu CK . The SHP-2 tyrosine phosphatase: signaling mechanisms and biological functions. Cell Res 2000; 10: 279–288.
Guy CS, Vignali DA . Organization of proximal signal initiation at the TCR:CD3 complex. Immunol Rev 2009; 232: 7–21.
Tzachanis D, Freeman GJ, Hirano N, van Puijenbroek AA, Delfs MW, Berezovskaya A et al. Tob is a negative regulator of activation that is expressed in anergic and quiescent T cells. Nat Immunol 2001; 2: 1174–1182.
Pettiford SM, Herbst R . The protein tyrosine phosphatase HePTP regulates nuclear translocation of ERK2 and can modulate megakaryocytic differentiation of K562 cells. Leukemia 2003; 17: 366–378.
Boise LH, González-García M, Postema CE, Ding L, Lindsten T, Turka LA et al. bcl-x, a bcl-2-related gene that functions as a dominant regulator of apoptotic cell death. Cell 1993; 74: 597–608.
Di Mitri D, Azevedo RI, Henson SM, Libri V, Riddell NE, Macaulay R et al. Reversible senescence in human CD4+CD45RA+CD27− memory T cells. J Immunol 2011; 187: 2093–2100.
Henson SM, Lanna A, Riddell NE, Franzese O, Macaulay R, Griffiths SJ et al. p38 signaling inhibits mTORC1-independent autophagy in senescent human CD8(+) T cells. J Clin Invest 2014; 124: 4004–4016.
Henson SM, Macaulay R, Riddell NE, Nunn CJ, Akbar AN . Blockade of PD-1 or p38 MAP kinase signaling enhances senescent human CD8(+) T-cell proliferation by distinct pathways. Eur J Immunol 2015; 45: 1441–1451.
Mizoguchi H, O'Shea JJ, Longo DL, Loeffler CM, McVicar DW, Ochoa AC . Alterations in signal transduction molecules in T lymphocytes from tumor-bearing mice. Science 1992; 258: 1795–1798.
Mozaffari F, Hansson L, Kiaii S, Ju X, Rossmann ED, Rabbani H et al. Signalling molecules and cytokine production in T cells of multiple myeloma-increased abnormalities with advancing stage. Br J Haematol 2004; 124: 315–324.
Moro-Garcia MA, Alonso-Arias R, Lopez-Larrea C . Molecular mechanisms involved in the aging of the T-cell immune response. Curr Genomics 2012; 13: 589–602.
McKarns SC, Schwartz RH, Kaminski NE . Smad3 is essential for TGF-β1 to suppress IL-2 production and TCR-induced proliferation, but not IL-2-induced proliferation. J Immunol 2004; 172: 4275–4284.
Beausejour CM, Krtolica A, Galimi F, Narita M, Lowe SW, Yaswen P et al. Reversal of human cellular senescence: roles of the p53 and p16 pathways. EMBO J 2003; 22: 4212–4222.
Migliaccio M, Raj K, Menzel O, Rufer N . Mechanisms that limit the in vitro proliferative potential of human CD8+ T lymphocytes. J Immunol 2005; 174: 3335–3343.
Rovillain E, Mansfield L, Caetano C, Alvarez-Fernandez M, Caballero OL, Medema RH et al. Activation of nuclear factor-kappa B signalling promotes cellular senescence. Oncogene 2011; 30: 2356–2366.
Kuilman T, Michaloglou C, Vredeveld LC, Douma S, van Doorn R, Desmet CJ et al. Oncogene-induced senescence relayed by an interleukin-dependent inflammatory network. Cell 2008; 133: 1019–1031.
Grandori C, Wu KJ, Fernandez P, Ngouenet C, Grim J, Clurman BE et al. Werner syndrome protein limits MYC-induced cellular senescence. Genes Dev 2003; 17: 1569–1574.
Grange M, Giordano M, Mas A, Roncagalli R, Firaguay G, Nunes JA et al. Control of CD8 T-cell proliferation and terminal differentiation by active STAT5 and CDKN2A/CDKN2B. Immunology 2015; 145: 543–557.
Schietinger A, Greenberg PD . Tolerance and exhaustion: defining mechanisms of T-cell dysfunction. Trends Immunol 2014; 35: 51–60.
Woo SR, Turnis ME, Goldberg MV, Bankoti J, Selby M, Nirschl CJ et al. Immune inhibitory molecules LAG-3 and PD-1 synergistically regulate T-cell function to promote tumoral immune escape. Cancer Res 2012; 72: 917–927.
Teramo A, Gattazzo C, Passeri F, Lico A, Tasca G, Cabrelle A et al. Intrinsic and extrinsic mechanisms contribute to maintain the JAK/STAT pathway aberrantly activated in T-type large granular lymphocyte leukemia. Blood 2013; 121: 3843–3854.
Suen H, Brown R, Yang S, Ho PJ, Gibson J, Joshua D . The failure of immune checkpoint blockade in multiple myeloma with PD-1 inhibitors in a phase 1 study. Leukemia 2015; 29: 1621–1622.
Lesokhin AM, Ansell SM, Armand P, Scott EC, Halwani A, Gutierrez M et al. Preliminary results of a phase I study of nivolumab (BMS-936558) in patients with relapsed or refractory lymphoid malignancies. Blood 2014; 124: 291–291.
Gorgun G, Samur MK, Cowens KB, Paula S, Bianchi G, Anderson JE et al. Lenalidomide enhances immune checkpoint blockade-induced immune response in multiple myeloma. Clin Cancer Res 2015; 21: 4607–4618.
Kao C, Oestreich KJ, Paley MA, Crawford A, Angelosanto JM, Ali MA et al. Transcription factor T-bet represses expression of the inhibitory receptor PD-1 and sustains virus-specific CD8+ T-cell responses during chronic infection. Nat Immunol 2011; 12: 663–671.
Lu P, Youngblood BA, Austin JW, Rasheed Mohammed AU, Butler R, Ahmed R et al. Blimp-1 represses CD8 T-cell expression of PD-1 using a feed-forward transcriptional circuit during acute viral infection. J Exp Med 2014; 211: 515–527.
Intlekofer AM, Takemoto N, Kao C, Banerjee A, Schambach F, Northrop JK et al. Requirement for T-bet in the aberrant differentiation of unhelped memory CD8+ T cells. J Exp Med 2007; 204: 2015–2021.
Acknowledgements
The work was supported by Sydney Foundation for Medical Research and the Cancer Institute of New South Wales.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Supplementary information
Rights and permissions
About this article
Cite this article
Suen, H., Brown, R., Yang, S. et al. Multiple myeloma causes clonal T-cell immunosenescence: identification of potential novel targets for promoting tumour immunity and implications for checkpoint blockade. Leukemia 30, 1716–1724 (2016). https://doi.org/10.1038/leu.2016.84
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2016.84
- Springer Nature Limited
This article is cited by
-
The roles of bone remodeling in normal hematopoiesis and age-related hematological malignancies
Bone Research (2023)
-
The immunome of mobilized peripheral blood stem cells is predictive of long-term outcomes and therapy-related myeloid neoplasms in patients with multiple myeloma undergoing autologous stem cell transplant
Blood Cancer Journal (2023)
-
Deciphering mechanisms of immune escape to inform immunotherapeutic strategies in multiple myeloma
Journal of Hematology & Oncology (2022)
-
T-cell counts in peripheral blood at leukapheresis predict responses to subsequent CAR-T cell therapy
Scientific Reports (2022)
-
Immune senescence in multiple myeloma—a role for mitochondrial dysfunction?
Leukemia (2022)