Abstract
Genetic abnormalities are a hallmark of cancer. Hereby, cytogenetic aberrations and small-scale abnormalities, such as single-nucleotide variations and insertion/deletion mutations, have emerged as two alternative modes of genetic diversification. Both mechanisms are at work in acute myeloid leukemia (AML), in which conventional karyotyping and molecular studies demonstrate that gene mutations occur predominantly in cytogenetically normal AML, whereas chromosomal changes are a driving force of development and progression of disease in aberrant karyotype AML. All steps of disease evolution in AML, ranging from the transformation of preleukemic clones into overt leukemia to the expansion and recurrence of malignant clones, are paralleled by clonal evolution at either the gene mutation or chromosome aberration level. Preleukemic conditions, such as Fanconi anemia and Bloom syndrome, demonstrate that the acquisition of chromosomal aberrations can contribute to leukemic transformation. Similar to what has been shown at the mutational level, expansion and recurrence of AML clones goes along with increasing genetic diversification. Hereby, cytogenetically more evolved subclones are at a proliferative advantage and outgrow ancestor clones or have evolved toward a more aggressive behavior with additional newly acquired aberrations as compared with the initial leukemic clone, respectively.
Similar content being viewed by others
Introduction
First reports of increased aneuploidy with aging in lymphocytes from healthy individuals were published in the early 1960s.1, 2 Chromosomes lost most frequently were identified as the X chromosome in females and the Y chromosome in males.3 Loss of the Y chromosome was subsequently commonly observed in bone marrow cells of elderly men without hematologic disorders as well as in different types of myeloid and lymphoid malignancies.4, 5, 6 Long thought to be an irrelevant byproduct of aging, age-dependent post-zygotic Y chromosome loss has most recently been shown to be associated with an increased risk of both hematologic and non-hematologic malignancies.7 Similarly, the incidence of clonal chromosomal mosaicism, as detected by single-nucleotide polymorphism profiling in peripheral blood cells of large cohorts of healthy individuals, rapidly increases in the elderly and is associated with a 10-fold risk to develop acute myeloid leukemia (AML) or other hematologic cancers.8, 9 Moreover, many of the mosaic chromosomal anomalies found are identical to those detectable in hematologic cancers. These findings clearly indicate that the age-associated emergence of small clones of white blood cells harboring chromosomal aberrations predisposes elderly individuals to hematologic malignancies and point to the importance of cytogenetic aberrations as leukemogenic drivers.
Types of genetic alterations in human cancer
The majority of human malignancies are characterized by large-scale chromosomal abnormalities, such as DNA copy-number variations (CNVs).10 Likewise, submicroscopic genetic alterations, such as single-nucleotide variations and insertion/deletion mutations, are present in a plethora of genes in almost all cancer types. In a seminal paper that appeared almost 20 years ago, Lengauer and Vogelstein were the first to demonstrate that chromosome-level aberrations and small-scale mutations occurred strictly alternatively to each other in colorectal cancer cell lines, a finding that later evolved into the categorization of colorectal cancer cases into two groups designated as chromosomal instability (CIN) and microsatellite instability types.11 Of note, large meta-analyses have meanwhile shown that CIN is associated with a worse prognosis in colorectal cancers.12
Recent advances in high-throughput techniques have allowed to sequence the complete genomes of multiple tumor types, thereby reshaping the understanding of cancer genomes and their complexity.13 One fundamental insight that has emerged from the analysis of >3000 tumors, representing 12 different cancer types, was a striking inverse relationship between recurrent CNVs and somatic single-nucleotide variations/insertion/deletion mutations, reminiscent of what has been found by Lengauer and Vogelstein in colorectal cancers earlier. On the basis of this observation, tumors can now be subdivided—independent of their tissue of origin—into two major classes, one primarily with small-scale mutations (M class) and the other primarily with CNVs (C class).14 Each tumor entity is composed of tumors belonging to the M and C classes in different proportions (Figure 1). For example, almost all clear-cell kidney carcinomas and glioblastomas belong to the M class, whereas most ovarian and breast carcinomas are included into the C class. In addition, it has been proposed that CNVs and aneuploidy can cause a modest mutator phenotype by enhancing genetic recombination and defective DNA damage repair, thereby providing a possible mechanistic link between aneuploidy and mutational instability in some types of cancer.15, 16, 17 Vice versa, mutations in genes that cause CIN are still searched for, with TP53 and cohesion complex components being possible candidates as further discussed below.
Both large-scale chromosomal aberrations as well as gene mutations contribute to malignant transformation and cancer progression, and seem to occur complementary to each other in many cancer types. On the other hand, both phenomena might well be interconnected, as CNVs and aneuploidy have been found to increase the frequency of gene mutations.
The analysis of mutational data from >8200 sporadic cancers revealed that, on average, tumors contain only 1 oncogene and 3 tumor suppressor gene mutations, but 3 chromosome arm gains, 5 chromosome arm losses, 2 whole-chromosome gains, 2 whole-chromosome losses, 12 focal deletions and 11 focal amplifications.18 The same work has shown that the spatial distribution of oncogenes and tumor suppressor genes on chromosomes can predict the complex but non-random patterns of aneuploidy observed in cancer genomes. These data reveal that somatic DNA copy-number alterations comprise a large proportion of cancer-driving events and illustrate the close link between chromosome aberrations on the one hand and oncogene/tumor suppressor gene alterations on the other.
The inverse correlation between CNVs and single-nucleotide variations/insertion/deletion mutations also supports the concept that these alterations reflect distinct oncogenic processes that drive cancer development and progression. In AML ~75% of cases belong to the M class and ~25% to the C class with multiple chromosomal gains and losses, the latter closely matching the percentage of cases with unfavorable cytogenetics and displaying a suspicious lack of mutations in genes typically mutated in AML.14, 19 In this article, we will focus on the contributions of DNA copy-number alterations and CIN to essential features of AML pathogenesis. Specifically, we will discuss the role of the different mutation types in clonal heterogeneity (that is, the number and diversity of subclones within an individual cancer) and clonal progression (that is, the increase in ‘fitness’ of a particular clone). These issues are not only relevant to the understanding of AML biology but also have clinical implications, as integrative analyses of the genetic features and clonal structures of AML cases have provided important insights into the cellular basis of leukemia initiation, treatment response and relapse, which may lead to new diagnostic and therapeutic strategies.
CIN as a driver of clonal heterogeneity and progression
Clonal heterogeneity and progression are fueled by genomic instability, which comes in two flavors—mutational/microsatellite instability and CIN. To accumulate large numbers of mutations, which allow for selection, adaptation and evolution of individual clones within a tumor, it has long been proposed that, in contrast to normal cells, cancer cells possess a mutator phenotype resulting from disruption of genes that maintain genetic stability, as normal mutation rates cannot account for the number of mutations found in human cancers.20, 21 With regard to AML, however, newer data argue that the spontaneous mutation rate in normal hematopoietic cells is low.22 Also, a hypermutator phenotype seems to be absent in most AML cases.23
Similar to the mutator phenotype underlying small-scale mutations, CIN is thought to be increased in certain tumors by defective microtubule-kinetochore interactions, faulty sister chromatid cohesion, telomere dysfunction, aberrant spindle checkpoint signaling or supernumerary centrosomes, which cause merotelic microtubule-kinetochore attachents by clustering of multiple spindle poles into a bipolar mitotic spindle array (Figure 2).24 Most of these mechanisms converge to produce lagging chromosomes during anaphase, ultimately leading to increased whole-chromosome missegregation rates as well as structural chromosome aberrations by damage to lagging chromosomes during cytokinesis.25 In addition to the above evidence for persistent chromosome missegregation in CIN-positive colorectal cancer cell lines, further support for a role of CIN in malignant transformation comes from a rare hereditary disorder called mosaic variegated aneuploidy. This condition is caused by mutations in the spindle checkpoint gene BUBR1 and leads to CIN with consecutive constitutional mosaicism for chromosomal gains and losses and subsequent predisposition to several types of cancer, including AML.26, 27, 28, 29
Mechanisms of chromosomal instability (CIN). (a) Mitotic cell (DNA stained in blue, α-tubulin in red, γ-tubulin, which labels centrosomes, in green) harboring supernumerary centrosomes that are clustered into two spindle poles, thereby allowing for the formation of a pseudo-bipolar spindle array. Centrosomal clustering, however, occurs through the formation of a multipolar intermediate that causes merotelic microtubule-kinetochore attachents (b), which subsequently produce lagging chromosomes during anaphase, ultimately leading to increased whole-chromosome missegregation (c, d). (c) DNA is stained in blue, α-tubulin in red and CREST, which labels kinetochores, in greens. (d) Only the CREST staining is displayed. Adopted from Anderhub et al.114
From a mechanistic point of view, it is interesting to note that recent cancer genome analyses have discovered a high frequency of mutations in genes encoding cohesin complex subunits in a variety of human malignancies, including AML. Cohesin is a multi-protein complex composed of four core subunits (SMC1A, SMC3, RAD21, STAG1 or STAG2), which is responsible for sister chromatid cohesion until its cleavage during mitosis, thereby enabling faithful segregation of sister chromatids into two daughter cells.30 In addition, cohesin has been reported to be involved in mother–daughter centriole engagement, mitotic licensing of centriole duplication by separase-dependent cohesin cleavage and coordinated separation of centrioles and chromatids.31, 32 In 2011, recurrent inactivating mutations in the cohesin subunit STAG2 were reported in several types of human cancer.15 In this study, truncating mutations or deletions of STAG2, which localizes to the X chromosome, were associated with complete loss of STAG2 expression. Whereas knockout of STAG2 in near-diploid HCT-116 cells led to precocious sister chromatid separation and aneuploidy induction, replacement of mutant STAG2 by the wild-type gene led to restoration of sister chromatid cohesion and correction of abnormal mitotic figures and CIN in two glioblastoma cell lines with mutated STAG2. These data suggested that mutational inactivation of the cohesin complex represents a major genetic mechanism underlying the occurrence of CIN and aneuploidy in human cancers. Subsequently, several studies have identified mutually exclusive, recurrent mutations in the cohesin components SMC1A, SMC3, STAG2 and RAD21 in myelodysplastic syndrome (MDS) and AML at frequencies between 6 and 13%.19, 33, 34, 35, 36, 37, 38 As most of the AML cases with cohesin mutations identified in these studies harbored normal or near-normal karyotypes, it was speculated that the loss of other functions of the cohesin complex, such as regulation of gene transcription, and not its canonical role in sister chromatid cohesion might be involved in leukemogenesis. In a recent analysis of 1060 patients with myeloid malignancies, somatic cohesion mutations were detected in 12% of cases, which were mutually exclusive and mostly resulted in predicted loss of function.39 Interestingly, deep sequencing revealed that the majority of these mutations represented secondary events in clonal hierarchy and were most prevalent in high-risk MDS and secondary AML, where they appeared to be associated with a poor prognosis. In addition, an association with trisomy 8 was found, again arguing for a possible link between cohesin mutations and karyotype aberrations. Continued investigations will be necessary to define the mechanism(s) by which cohesin mutations contribute to malignant transformation and understand their contribution, if any, to CIN.
CIN in myeloid malignancies
Aneuploidy, defined as a state of abnormal chromosome number and a consequence of CIN, has been implicated in tumorigenesis for many decades and constitutes an important prognostic marker in many types of malignancies. For example, AML with complex karyotype, defined as three or more clonal chromosome aberrations in the absence of one of the WHO-designated balanced rearrangements t(8;21)(q22;q22), inv(16)(p13q22)/ (16;16)(p13;q22), t(15;17)(q22;q21), t(9;11)(p22;q23), t(v;11)(v;q23), t(6;9)(p23;q34) and inv(3)(q21q26)/t(3;3)(q21;q26), is associated with an exceptionally poor prognosis.40, 41, 42 In contrast, data on the presence and prognostic relevance of a potentially underlying CIN have only recently begun to accumulate, as it is technically challenging to directly measure chromosome missegregation rates. As a consequence, aneuploidy has frequently but mistakenly been used as a surrogate marker of CIN, rather than directly measuring the cell-to-cell variability of chromosome copy numbers or the frequency of lagging chromosomes as more accurate reflections of CIN.24, 43 Although the presence and prognostic relevance of CIN have been established in colorectal cancers as described above, only little data on the role of CIN, as evidenced by gross aneuploidy and pronounced cell-to-cell variability, are available for hematologic malignancies. As one example, a higher degree of cell-to-cell variability of chromosome copy numbers determined by interphase fluorescence in situ hybridization with centromeric probes was shown to portend a poor prognosis in MDS.43
Emergence of malignant AML clones
Preleukemic conditions provide important insights into the emergence of malignant clones with cytogenetic aberrations as well as into the contribution of CIN to MDS/AML development. Fanconi anemia, which is characterized by CIN as a consequence of defective DNA damage response and mitotic chromosome segregation,44, 45 is one example. Affected patients are at high risk for developing different types of neoplasms. The most frequent malignancies in Fanconi anemia are MDS and AML, with a cumulative incidence approaching 33% by 40 years of age.46, 47 In MDS or AML secondary to Fanconi anemia, gains of chromosome 3q, which lead to overexpression of the EVI1 oncogene, and monosomy 7/del(7q) were detectable in 12/29 and 5/29 patients, respectively.48 Remarkably, these cytogenetic aberrations were exclusively found in patients with MDS and AML, but not in patients with untransformed Fanconi anemia, implying a contribution to leukemic transformation. In contrast, gains of chromosome 1q were found at all stages of Fanconi anemia bone marrow evolution, including cases with isolated hypoplastic or aplastic anemia. Another study showed that although chromosome 3 and 7 aberrations were present in some Fanconi anemia patients prior to leukemic transformation, virtually all individuals with these chromosomal abnormalities subsequently developed MDS/AML.49
Similar to Fanconi anemia, individuals affected by Bloom syndrome, a genetic disorder caused by mutations in the BLM RecQ helicase, are predisposed to a wide variety of neoplasms, including hematologic malignancies. Intriguingly, analogous to Fanconi anemia, a preferential occurrence of monosomy 7 or deletions of the long arm of chromosome 7 was found in bone marrow cells from Bloom syndrome patients with MDS or AML.50
Progression of aplastic anemia to MDS and AML is also frequently associated with the appearance of cytogenetic aberrations.51 Hematopoiesis in aplastic anemia is regarded as oligoclonal, and the depletion of healthy clones by autoimmunity predisposes to the expansion of cytogenetically aberrant clones.52 The most prevalent cytogenetic aberration in aplastic anemia is monosomy 7, which heralds a poor prognosis and progression to MDS/AML, similar to the situation in Fanconi anemia described above; the second most prevalent is trisomy 8, which is prognostically more favorable.53, 54
Do functional differences between mutational and chromosomal evolution exist and, if so, what are the respective contributions of mutational versus chromosomal evolution to the emergence of malignant clones and clonal heterogeneity in myeloid malignancies? It has previously been reported that a low mean telomere length of leukocytes at the time of diagnosis of aplastic anemia is associated with increased risk of relapse, clonal evolution with progression to MDS/AML and decreased overall survival.55 New data from the same group now revealed that while cells from aplastic anemia patients with clonal evolution showed marked progressive telomere attrition during the period preceding development of monosomy 7, only two out of 13 patients acquired mutations in myeloid cells, as determined by targeted sequencing of 125 candidate genes recurrently mutated in AML and MDS.56 These findings led to the conclusion that in aplastic anemia, telomere shortening, rather than accumulation of point mutations in hematopoietic cells, precedes aneuploidy and malignant transformation at an early stage of leukemogenesis. Therefore, at least in the context of MDS/AML secondary to aplastic anemia, telomere shortening and subsequent CIN rather than the accrual of oncogenic mutations seem to pave the way toward malignancy. Similarly, data describing average and individual telomere lengths in MDS and AML showed that the transition from MDS to AML is characterized by increased telomere shortening and chromosomal abnormalities.57 Also, in AML, particularly in abnormal karyotype AML, TERT mutations involving the telomere repair complex have been described.58 Biologically, it has been suggested that dysfunctional telomeres limit the stem cell pool, which favors the selection of stem cells with deficient DNA damage response prone to CIN. Furthermore, critically short telomeres can fuse with other ‘free ends’ and thus promote further genomic instability.59, 60
Together, these data clearly argue for the acquisition of cytogenetic aberrations as one step toward the evolution of the malignant phenotype in MDS/AML, which is in tune with the retrospective detection of the t(8;21)(q22;q22) on Guthrie cards of newborns who developed AML later in life, indicating the need for further genetic ‘hits’ to trigger the leukemic phenotype.61 In a report by Stark et al.62 two monozygotic twins, who were both diagnosed with AML M7 at the age of 22 months, displayed trisomy 21 in their leukemic blasts, suggestive of a common intrauterine origin of the leukemia. Remarkably, one of the twins harbored an additional del(20q), whereas the other had acquired additional trisomy 8, both of which have to be considered as secondary events indicative of clonal evolution. This case is highly reminiscent of the twin studies by the Greaves group in pediatric acute lymphoblastic leukemia,63 which typically observed an early—likely initiating—preleukemic mutation, which was acquired prenatally and was detectable on neonatal blood spots of both twins, and subsequent—likely progression-related—genetic hits in the leukemic cells of the diseased twin.
Other studies on adult AML with t(8;21)(q22;q22) showed detectable levels of the resulting RUNX1-RUNX1T1 fusion transcript in normal myeloid cells as well as in highly purified hematopoietic stem cells from patients in long-term remission.64, 65, 66 Similarly, other cytogenetic abnormalities, including inv(16)(p13q22), t(6;9)(p23;q34), t(17;20) and add(2)(q37) have been found in hematopoietic stem and progenitor populations of patients with AML in complete remission.67 In addition, recent work has identified, aside from mutations in DNMT3A, IDH2, ASXL1 and IKZF1, the inv(16)(p13q22) to occur in preleukemic hematopoietic stem cells.68 These findings illustrate that chromosomal aberrations can contribute to the earliest events in the transformation process, and that the stepwise acquisition of karyotypic aberrations contributes to the development of MDS/AML similar to what has been well established at the mutational level for acute lymphoblastic leukemia and MDS/AML.69, 70, 71
As opposed to the concept of tumorigenesis as a stepwise evolutionary process, a phenomenon called chromothripsis has recently been introduced as an additional mechanism of karyotype evolution.72 In chromothripsis, a chromosome is shattered into multiple pieces during a single catastrophic event. Typically, numerous genomic rearrangements cluster to one or few chromosomes or even a single chromosome arm. This phenomenon, which might be responsible for structural chromosome aberrations especially in AML with complex karyotype abnormalities, has been detected in cases of TP53-mutated AML by single-nucleotide polymorphism arrays and was suggested to be of independent prognostic significance.73 However, its frequency as well as its contribution to chromosomal aberrations and prognosis of AML have yet to be determined.
Progression of malignant AML clones
The contribution of chromosomal aberrations to clonal progression is well established in MDS. In a study addressing cytogenetic evolution in MDS, 40/153 (26.1%) patients acquired secondary cytogenetic abnormalities even prior to transformation to AML with a median follow-up of 45.2 months.74 Interestingly, acquisition of del(5q) was typically detected in early MDS, whereas monosomy 7, del(7q) and del(17p) were frequently seen in patients with advanced MDS. Results were similar in another cohort with 18/85 (21.2%) patients experiencing cytogenetic evolution, particularly those with an elevated blast percentage and a higher International Prognostic Scoring System risk score.75 In both studies, cytogenetic evolution was shown to increase the risk of clinical progression and death.
Along the same lines, recent work has shed light on the role and the consequences of evolution of monosomy 7 in myeloid malignancies. Monosomy 7 and del(7q) are among the most common chromosomal abnormalities in patients with AML and MDS. In contrast to several other monosomies, where large parts of the respective chromosome are not actually lost but can be found in marker and/or ring chromosomes by Spectral Karyotyping and Multiplex-fluorescence in situ hybridization, monosomy 7 is associated with loss of the chromosomal material in most cases. For this reason, the negative prognostic impact of isolated del(7q) may be less pronounced as compared with monosomy 7.76, 77 A recent study now suggests that complete monosomy 7 represents the terminal stage of karyotype evolution during MDS progression with del(7q) and subsequent formation of a ring chromosome 7 being intermediate stages, which would also explain their better prognosis.78 In this scenario, ring chromosome 7 formation seems to result from telomere erosion in del(7q) cells. Ring chromosomes themselves are known to be unstable and prone to become lost during cell division.79
Core-binding factor (CBF) AMLs are cytogenetically defined by the presence of a t(8;21)(q22;q22) or an inv(16)(p13q22)/t(16;16)(p13;q22) and associated with favorable outcome.80 Although two large studies by the British Medical Research Council and the Cancer and Leukemia Group B concluded that additional chromosomal aberrations do not impact on prognosis in CBF AML,80, 81, 82 newer results suggest that loss of the Y chromosome is associated with shorter overall survival in t(8;21)(q22;q22) patients, whereas trisomy 22 prolonged relapse-free survival in inv(16)(p13q22) AML.83
As mentioned above, AML with complex karyotype is associated with extremely poor outcome. Similarly, monosomal karyotypes, defined by the presence of one single autosomal monosomy in association with at least one additional autosomal monosomy or one structural chromosomal abnormality excluding marker and ring chromosomes, are associated with a dismal prognosis and seem to add prognostic information, even in complex karyotype AML.84 One important peculiarity of C class malignancies is their strong association with TP53 mutations, consistent with TP53 deficiency causing CIN.14 Alternatively, 17p13, the chromosomal region where TP53 is located, might constitute one of the non-random but common targets of chromosomal aberrations, as recently suggested.18 In any case, it has been shown by several groups that TP53, which is otherwise only rarely affected in AML, is the most frequently altered gene in complex as well as monosomal karyotype AML. TP53 aberrant cases display a higher degree of karyotypic complexity and an exceptionally dismal outcome.85, 86 As among 234 complex karyotype AML cases analyzed, TP53 mutations as determined by DNA sequencing were more frequent (141/234 cases (60%)) than TP53 losses as determined by array-CGH analysis (94/234 cases (40%)),85 it might be concluded that TP53 loss of function indeed causes CIN, with subsequent development of complex karyotype alterations, rather than being a consequence of it.
Additional evidence supporting a prognostic role of CIN in clonal evolution in myeloid malignancies comes from interphase fluorescence in situ hybridization data on CD34-positive bone marrow cells from patients with MDS (Figure 3). Although only a comparatively small cohort of patients has been analyzed, elevated CIN levels, as determined as fractions of cells with numbers of individual chromosomes deviating from the normal diploid status, were associated with both poor prognosis and AML evolution, with high-level CIN being detectable antecedent to clinical deterioration.43 In conclusion, CIN is a driving force of MDS progression.
Chromosomal instability (CIN) in CD34-positive cells of an MDS patient in longitudinal follow-up. CIN is measured by hybridization with centromeric interphase FISH probes for chromosomes 6 and 7 stained in red and green, respectively. Though time points are only 1 month apart, CIN has markedly increased from (a) to (b), moving chromosome numbers from a diploid status in (a) to mono-, tri- and tetrasomies in (b). Interestingly, in this case increasing CIN preceded transformation into AML by 4 months, indicating that CIN is a driving force of clonal evolution and leukemia progression. Adopted from Heilig et al.43
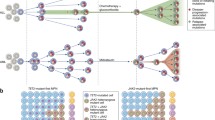
Recent work has evaluated clonal heterogeneity of primary AML cells using conventional karyotyping of metaphases to detect cytogenetic subclones.87 This analysis of subclonal architecture offers insights into cytogenetic evolution. Assessing the cytogenetic data from two large randomized clinical trials, subclone formation was detectable in 33% of aberrant karyotypes at first diagnosis. Though this phenomenon was detectable in all cytogenetic categories, it was particularly frequent in patients with high-risk karyotype aberrations including complex aberrant, monosomal or del(17p) karyotypes, where subclone frequencies of 69%, 67% and 65% were observed, respectively. For karyotypes with defined subclones, oncogenetic ancestral trees were developed in analogy to studies in acute lymphoblastic leukemia. For AML patients with two subclones, a ‘mother–daughter’ pattern was by far the most prevalent, where the daughter subclone harbored an extra cytogenetic aberration in addition to those present in the mother clone. Also, in some cases with two defined subclones, sister clones of common genetic origin were observed, though the presumed common ancestor clone was no longer detectable and appeared to have been outgrown. If three or more subclones were detectable, they typically aligned themselves into a branched rather than a linearly successive ancestral tree pattern. The striking similarity of these oncogenetic tree models in AML with those established in ALL69, 70 emphasizes that the concept of clonal evolution by genetic diversification and subsequent selection of subclones is similar in acute lymphoblastic leukemia and AML. In conclusion, these subclone patterns suggest that leukemogenesis in AML is a stepwise process. Typically, daughter subclones carry additional cytogenetic aberrations, which confer a more aggressive phenotype and a selection advantage, permitting the cytogenetically more evolved daughter subclone to outgrow the mother clone. This concept is illustrated in CBF leukemias, where t(8;21)(q22;q22) and inv(16)(p13q22) can be regarded as the primary cytogenetic events at the root of the ancestral tree owing to their universal presence in all subclones, and where additional cytogenetic aberrations detected in some of the subclones are well-known secondary abnormalities, such as trisomy 22 in inv(16)-positive AML (Figure 4). No longitudinal studies assessing subclone architecture over time as proof of this evolutionary concept have been reported yet, though the clinical case of a cytogenetically more evolved minor daughter subclone outgrowing the mother clone within 3 months has been reported for a pediatric AML patient with Down syndrome.88 The authors interpret this case as an example of rapid clonal evolution and the transitory nature of clonal chromosomal aberrations.
Stepwise clonal evolution by sublcone formation in CBF AML. The mother clone (a) harbors the CBF translocation—in this case t(8;21)(q22;q22)—as the initiating event. Then a daughter subclone with an additional aberration arises (b)—in this schematic case del(9q)—, and by proliferative advantage begins to outgrow (c) and replace (d) the mother clone. Thus, this model considers subclone formation (b, c) as a transitory step toward a more evolved clone carrying an additional aberration (d). This concept is implied by the finding that the additional aberrations that set apart the subclones in CBF leukemias (b, c) are the same aberrations known to occur as concomitant full clone aberrations (d): loss of a gonosome, del(9q) and del(7q) in t(8;21)(q22;q22) AML; and trisomy 22, trisomy 8 and del(7q) in inv(16)(p13q22) AML.87
Remarkably, detection of cytogenetic subclones was predictive of a poor prognosis in non-CBF leukemias, particularly in karyotypes classified as composite karyotypes owing to their pronounced clonal heterogeneity.87 From a biological point of view, subclone formation may increase the risk for the emergence of chemotherapy-resistant subclones.89 This might explain why AML patients with cytogenetic subclones benefit in particular from allogeneic transplantation, an immune-based treatment approach thought to be less amenable to drug-resistance development by clonal evolution.
According to the European LeukemiaNet definition, ~20% of patients with t(8;21)(q22;q22) and about 10% of patients with inv(16)(p13q22)/t(16;16)(p13;q22) or t(15;17)(q22;q21) would be considered to have a complex karyotype because they harbor two or more secondary aberrations in addition to their respective primary translocation or inversion. However, as discussed above, with the exception of the loss of the Y chromosome in t(8;21)(q22;q22) patients and trisomy 22 in inv(16)(p13q22) AML, several studies have documented that in these cytogenetic subgroups increased karyotypic complexity does not affect clinical outcome comparable to other patients with three or more chromosomal aberrations.80, 82, 83, 90 Interestingly, the above-mentioned work87 has shown that in AML, cytogenetic subclone formation as a measure of clonal heterogeneity is particularly frequent and pronounced in adverse-risk patients with complex aberrant, monosomal and abnl(17p) karyotypes.81, 84, 86, 91 In contrast, in CBF leukemias, subclone formation was less frequent with composite karyotypes as an indicator of high-level CIN being virtually absent. From these data it may be concluded that, at least in part, complex karyotype AMLs carry a poor prognosis not because they harbor a fixed number of chromosomal abnormalities but rather because they are highly chromosomally unstable, thereby allowing for selection, adaptation and evolution via clonal heterogeneity.
The role of cytogenetic subclone formation was also analyzed in a recent study on MDS and AML patients with del(5q).92 Cytogenetic subclones were detectable in 233/573 (40.7%) of MDS and 345/627 (55.0%) of AML patients harboring del(5q). Notably, subclone formation was more frequent in patients with unbalanced rearrangements of 5q than in patients with interstitial del(5q), reflecting increased genetic instability in the former group. Similar to the findings by Bochtler et al.87 in this analysis, subclone formation in MDS—though not in AML—conferred an inferior prognosis.
Recurrence of malignant AML clones
Molecular diagnostic tools have yielded much insight into the mechanisms underlying disease relapse in AML. In their pioneering work, Ding et al.33 suggested two patterns of relapse: either the founding clone at first diagnosis recurred after acquiring additional aberrations, or a subclone of the founding clone gave rise to relapse after overcoming chemotherapy by gaining additional mutations. Accordingly, this study established clonal diversification as one mechanism for disease recurrence. The following rules appear to apply to the relapse clone: (i) AML at relapse is clonally related to the primary AML at first diagnosis. Relapse clones share genetic features already present initially. The emergence of genetically truly unrelated clones is considered exceptional. If a genetically unrelated clone is found, a second independent disease, especially therapy-related MDS or AML, should be considered rather than relapse of the primary disorder. (ii) Typically, AML is genetically more evolved at relapse than at first diagnosis with higher genetic complexity at relapse being observed both at the molecular and cytogenetic level.33, 93 For example, in a study by Krönke et al.94 the mean number of CNVs and uniparental disomies per case significantly increased from 0.28 at first diagnosis to 1.06 at relapse. This is in tune with older cytogenetic data, which had demonstrated a karyotype change from first diagnosis to relapse in 39–68% of patients with the acquisition of additional cytogenetic aberrations (53–70%) as the prevailing pattern.95, 96, 97 On the contrary, clonal de-evolution with loss of cytogenetic aberrations (13–17%) or both phenomena combined (14–33%) was less frequent. (iii) It is not necessarily the most expanded subclone that evolves into the relapse clone; initially minor subclones can give rise to relapse as well.33 (iv) In this model, mutations first noticed at relapse might be true de novo aberrations. Alternatively, they could have been present in a minor subclone at first diagnosis that escaped detection but has expanded at relapse.98 (v) In some cases, relapse can be traced back to a clone ancestral to the initial leukemic clone, meaning that relapses can arise from an initially coexisting preleukemic clone as well.68, 94, 99 Of note, these principles of clonal evolution and relapse are reminiscent of the patterns described in ALL by the pioneering work of the Greaves and Mullighan groups,69, 70, 100 suggesting that they are not specific for AML, but apply to acute leukemias in general.
Numerous studies in AML have juxtaposed cytogenetic and molecular markers at first diagnosis versus relapse to align them on a trajectory from early, disease-initiating events to late, cooperating events leading to disease progression and relapse. The underlying hypothesis is that stable markers present at first diagnosis and relapse are early, initiating events, whereas markers gained at relapse are regarded as late and progression- related. The scenario of a marker lost at relapse would suggest its appearance shortly before leukemia outbreak at first diagnosis and would put it in a middle position of the leukemia trajectory.
Several recent molecular studies have illustrated the succession of molecular markers along the evolution path of AML. In this chronological hierarchy, DNMT3A mutations are an archetypical early event at the very root of leukemogenesis. It can be reliably detected in initial and relapse sample pairs. In a study by Krönke et al.,94 DNMT3A mutations were the most stable marker retained in 97% of relapse cases. Interestingly, DNMT3A mutations are also detectable in remission samples with mutated allele frequencies similar to or even higher than at first diagnosis. In addition, as stated before, mutations in DNMT3A have recently been directly shown to occur in preleukemic hematopoietic stem cells.68, 101 This suggests that these mutations are acquired early as preleukemic events in hematopoietic stem cells or myeloid precursors and form a reservoir for disease recurrence.
By comparison, NPM1—though regarded as a stable founder mutation and accordingly recognized as provisional entity in the WHO classification—was only retained in 91% of relapse samples.94 In this study, mutant NPM1 was lost in five patients, typically with late relapses and a poor response to salvage chemotherapy. Interestingly, the relapse clones in these five patients had consistently retained their DNMT3A mutations. Therefore and although the sequence of mutation acquisition is not uniform for all patients, NPM1 mutations appear to evolve later in the ancestral tree than DNMT3A mutations. In the chronological succession of molecular markers, TET2 mutations rank next behind NPM1, since at first diagnosis they are frequently detectable only in subclones, and at relapse their allele frequency was shown to decrease.102
At the other end of the spectrum, FLT3 internal tandem duplication (FLT3-ITD) mutations are late cooperating events, as they are absent from preleukemic clones99 and frequently lost or newly gained at relapse.103 In the concept of cooperating, proliferation-enhancing class I and differentiation-abrogating class II mutations in AML pathogenesis104, 105, 106 FLT3-ITD mutations fall into the former category, implying that proliferation-enhancing mutations are typically late events in leukemogenesis heralding progression.107
In a study by Parkin et al.,108 28 AML sample pairs from patients who achieved remission and subsequently relapsed were analyzed for a comprehensive set of mutations. Mutations in DNMT3A, NPM1, IDH1 and 2, ASXL1, TET2 and MLL partial tandem duplications were grouped as stable and thus presumably initiating events, whereas FLT3-ITD mutations and alterations of RUNX1, CEBPA, KRAS and BCORL1 were classified as late cooperating events. The categorization of markers into early and late events by the assessment of relapse clones is very consistent with results from a study by Welch et al.35 who overlaid the genotype of AML M3 with its PML-RARA fusion as prototypical initiating event for comparison with sequencing data from the AML M1 subtype. Mutations exclusively detectable in AML M1 genomes, such as NPM1, DNMT3A, IDH1/2, TET2 and ASXL1, were classified as initiating events, whereas mutations detectable in both the AML M1 and M3 subtypes, such as FLT3-ITD and WT1 mutations, were regarded as late cooperating events.
Remarkably, the stepwise acquisition of mutations follows a non-random pattern, not only with regard to the chronology of their acquisition but also regarding the type of mutations. For example, DNMT3A, NPM1 and FLT3-ITD mutations frequently co-occur and also cluster in RNA expression and DNA methylation screens,109 whereas others, such as NPM1 and CEBPA mutations, are almost mutually exclusive.19 As recently reviewed by Grove and Vassiliou, the initiating mutation thus determines the probability and type of secondary mutations on the path to overt leukemia and relapse.107
Similar data for cytogenetic aberrations are scarce, owing to considerably less sensitive detection methods. Cytogenetic aberrations present at first diagnosis have been shown to be reliably preserved at relapse, strengthening their role as truly initiating events.108 As reviewed above, acquisition of further cytogenetic aberrations is a common phenomenon at AML relapse. However, the precise role of individual chromosomal aberrations is less clear than that of individual gene mutations. In a study by Schmidt-Hieber et al.,97 additional chromosomal aberrations at relapse frequently involved chromosomes 1, 3 and 4, whereas Garson et al.96 frequently observed trisomies 8 and 21. Bacher et al.95 reported on trisomy 8 as well, and in addition found gains of 11q, 15q or 17q and losses of 5q and 9q. Regarding prognosis, karyotype changes per se appeared to have no impact on overall survival after relapse in these studies, with the exception of acquisition of additional structural chromosome 1 abnormalities, which seemed to confer a poor prognosis.97 In a more recent study, aberrations newly acquired at relapse recurrently involved tumor suppressor genes at 12p13 (ETV6), 11p13 (WT1), 17p (TP53) and a gain of 11q23 (MLL).94
Among MDS patients with del(5q) treated with lenalidomide, 29% and 42% progressed to overt AML 3 and 5 years after the start of therapy, respectively.110 In these patients, cytogenetic clonal evolution seems to have at least contributed to leukemic transformation, as 13 of 15 patients displayed additional cytogenetic aberrations at progression to AML, among them nine with a complex karyotype. The prevailing additional aberrations were del(17p) as well as trisomies of chromosomes 8 and 21. The conclusion of the authors that inactivation of TP53 on chromosome 17p is a critical early event in del(5q) MDS clonal evolution is also corroborated by another recent study showing that small subclones with TP53 mutations are present already at initial diagnosis of del(5q) MDS and markedly expand following lenalidomide treatment.111 Thus, lenalidomide treatment appears to drive the selection of TP53 mutant subclones and their relative expansion versus other clones.
Whereas the studies above focused on relapse samples, the study by Parkin et al.108 also investigated primary refractory AML cases by single-nucleotide polymorphism array-based genomic profiling and sequencing of recurrently mutated genes. Here, two scenarios were observed: in some patients, the genetic repertoire of persistent blasts was identical compared with initial diagnosis, with the predominating clone having remained unaltered; in other patients, genetic aberrations were lost, suggesting a coexistence of chemosensitive and chemoresistant subclones.108 Notably, no evolution toward a genetically more advanced clone was observed in these primary refractory cases.
Emergence of therapy-related secondary AML clones
As mentioned above, TP53 mutations are intimately linked to the development of CIN. It has been long known that in therapy-related AML, which is associated with an increased incidence of chromosomal aberrations and poor prognosis, TP53 mutations are far more frequent than in de novo AML.112 Excitingly, it has now been reported that in therapy-related AML patients, hematopoietic progenitor cells harboring TP53 mutations seem to be present prior to chemotherapy exposure, with heterozygous loss of TP53 providing a competitive selection advantage to TP53 wild-type hematopoietic cells after chemotherapy.113 These findings have been revealed by next-generation sequencing of bone marrow specimens and leukapheresis products harvested before or at the time of treatment of the primary cancer and many years before the advent of therapy-related AML. It can be concluded that TP53 mutations are early events in the evolution of therapy-related AML that precede and likely contribute to the high incidence of cytogenetic abnormalites found in this disorder, as discussed above for de novo AML with complex/monosomal karyotypes.
Conclusions
In MDS/AML, the concept of genetic clonal evolution has strong clinical implications. First, the cytogenetic and molecular markers acquired on the path to leukemia yield prognostic information and have become the basis of risk stratification-based therapies. As reviewed above, risk stratification can be further refined by accounting for clonal diversity. Second, aberrations acquired at clonal progression like FLT3-ITD or c-KIT mutations offer the prospect of targeted therapy. Third, the model of clonal evolution has shaped our understanding of treatment strategies and is currently translated into the development of novel therapeutic concepts. For example, the detection of tumor heterogeneity has given insights into mechanisms of treatment resistance with selection of resistant subclones. This has provided a rationale for ‘hitting hard and early’ combination treatment approaches, which aim at eliminating the malignant clone before further genetic diversification sets in. Also, this concept lends strong support to the idea of developing treatment strategies that target early driver lesions present in all tumor cells and might explain the sobering results currently obtained with FLT3 inhibitors. Likewise, it has inspired the development of immune-based therapies, which are presumed to be less susceptible to resistance owing to genetic diversification. The evolution toward a genetically more complex clone at relapse also mirrors the clinical experience that treatment at relapse is less promising, also arguing in favor of aggressive first-line treatment to forestall relapses. In conclusion, in AML the concept of genetic clonal evolution is closely intertwined with diagnostic algorithms, risk stratification and treatment strategies. This has made AML a model disease to study genetic clonal diversity and progression.
References
Jacobs PA, Court Brown WM, Doll R . Distribution of human chromosome counts in relation to age. Nature 1961; 191: 1178–1180.
Jacobs PA, Brunton M, Court Brown WM, Doll R, Goldstein H . Change of human chromosome count distribution with age: evidence for a sex differences. Nature 1963; 197: 1080–1081.
Galloway SM, Buckton KE . Aneuploidy and ageing: chromosome studies on a random sample of the population using G-banding. Cytogenet Cell Genet 1978; 20: 78–95.
Pierre RV, Hoagland HC . Age-associated aneuploidy: loss of Y chromosome from human bone marrow cells with aging. Cancer 1972; 30: 889–894.
Wiktor A, Rybicki BA, Piao ZS, Shurafa M, Barthel B, Maeda K et al. Clinical significance of Y chromosome loss in hematologic disease. Genes Chromosomes Cancer 2000; 27: 11–16.
Loss of the Y chromosome from normal and neoplastic bone marrows. United Kingdom Cancer Cytogenetics Group (UKCCG). Genes Chromosomes Cancer 1992; 5: 83–88.
Forsberg LA, Rasi C, Malmqvist N, Davies H, Pasupulati S, Pakalapati G et al. Mosaic loss of chromosome Y in peripheral blood is associated with shorter survival and higher risk of cancer. Nat Genet 2014; 46: 624–628.
Laurie CC, Laurie CA, Rice K, Doheny KF, Zelnick LR, McHugh CP et al. Detectable clonal mosaicism from birth to old age and its relationship to cancer. Nat Genet 2012; 44: 642–650.
Jacobs KB, Yeager M, Zhou W, Wacholder S, Wang Z, Rodriguez-Santiago B et al. Detectable clonal mosaicism and its relationship to aging and cancer. Nat Genet 2012; 44: 651–658.
Frohling S, Dohner H . Chromosomal abnormalities in cancer. N Engl J Med 2008; 359: 722–734.
Lengauer C, Kinzler KW, Vogelstein B . Genetic instability in colorectal cancers. Nature 1997; 386: 623–627.
Walther A, Houlston R, Tomlinson I . Association between chromosomal instability and prognosis in colorectal cancer: a meta-analysis. Gut 2008; 57: 941–950.
White BS, DiPersio JF . Genomic tools in acute myeloid leukemia: From the bench to the bedside. Cancer 2014; 120: 1134–1144.
Ciriello G, Miller ML, Aksoy BA, Senbabaoglu Y, Schultz N, Sander C . Emerging landscape of oncogenic signatures across human cancers. Nat Genet 2013; 45: 1127–1133.
Solomon DA, Kim T, Diaz-Martinez LA, Fair J, Elkahloun AG, Harris BT et al. Mutational inactivation of STAG2 causes aneuploidy in human cancer. Science 2011; 333: 1039–1043.
Sheltzer JM, Blank HM, Pfau SJ, Tange Y, George BM, Humpton TJ et al. Aneuploidy drives genomic instability in yeast. Science 2011; 333: 1026–1030.
Kolodner RD, Cleveland DW, Putnam CD . Cancer. Aneuploidy drives a mutator phenotype in cancer. Science 2011; 333: 942–943.
Davoli T, Xu AW, Mengwasser KE, Sack LM, Yoon JC, Park PJ et al. Cumulative haploinsufficiency and triplosensitivity drive aneuploidy patterns and shape the cancer genome. Cell 2013; 155: 948–962.
Cancer Genome Atlas Research N. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N Engl J Med 2013; 368: 2059–2074.
Loeb LA, Springgate CF, Battula N . Errors in DNA replication as a basis of malignant changes. Cancer Res 1974; 34: 2311–2321.
Loeb LA . Mutator phenotype may be required for multistage carcinogenesis. Cancer Res 1991; 51: 3075–3079.
Araten DJ, Golde DW, Zhang RH, Thaler HT, Gargiulo L, Notaro R et al. A quantitative measurement of the human somatic mutation rate. Cancer Res 2005; 65: 8111–8117.
Alexandrov LB, Nik-Zainal S, Wedge DC, Aparicio SA, Behjati S, Biankin AV et al. Signatures of mutational processes in human cancer. Nature 2013; 500: 415–421.
Bakhoum SF, Compton DA . Chromosomal instability and cancer: a complex relationship with therapeutic potential. J Clin Invest 2012; 122: 1138–1143.
Janssen A, van der Burg M, Szuhai K, Kops GJ, Medema RH . Chromosome segregation errors as a cause of DNA damage and structural chromosome aberrations. Science 2011; 333: 1895–1898.
Hunter A . High risk of malignancy in mosaic variegated aneuploidy syndrome. Am J Med Genet A 2003; 117A: 199.
Jacquemont S, Boceno M, Rival JM, Mechinaud F, David A . High risk of malignancy in mosaic variegated aneuploidy syndrome. Am J Med Genet 2002; 109: 17–21, discussion 16.
Hanks S, Coleman K, Reid S, Plaja A, Firth H, Fitzpatrick D et al. Constitutional aneuploidy and cancer predisposition caused by biallelic mutations in BUB1B. Nat Genet 2004; 36: 1159–1161.
Rio Frio T, Lavoie J, Hamel N, Geyer FC, Kushner YB, Novak DJ et al. Homozygous BUB1B mutation and susceptibility to gastrointestinal neoplasia. N Engl J Med 2010; 363: 2628–2637.
Nasmyth K . Segregating sister genomes: the molecular biology of chromosome separation. Science 2002; 297: 559–565.
Schockel L, Mockel M, Mayer B, Boos D, Stemmann O . Cleavage of cohesin rings coordinates the separation of centrioles and chromatids. Nat Cell Biol 2011; 13: 966–972.
Tsou MF, Wang WJ, George KA, Uryu K, Stearns T, Jallepalli PV . Polo kinase and separase regulate the mitotic licensing of centriole duplication in human cells. Dev Cell 2009; 17: 344–354.
Ding L, Ley TJ, Larson DE, Miller CA, Koboldt DC, Welch JS et al. Clonal evolution in relapsed acute myeloid leukaemia revealed by whole-genome sequencing. Nature 2012; 481: 506–510.
Walter MJ, Shen D, Ding L, Shao J, Koboldt DC, Chen K et al. Clonal architecture of secondary acute myeloid leukemia. N Engl J Med 2012; 366: 1090–1098.
Welch JS, Ley TJ, Link DC, Miller CA, Larson DE, Koboldt DC et al. The origin and evolution of mutations in acute myeloid leukemia. Cell 2012; 150: 264–278.
Kon A, Shih LY, Minamino M, Sanada M, Shiraishi Y, Nagata Y et al. Recurrent mutations in multiple components of the cohesin complex in myeloid neoplasms. Nat Genet 2013; 45: 1232–1237.
Thol F, Bollin R, Gehlhaar M, Walter C, Dugas M, Suchanek KJ et al. Mutations in the cohesin complex in acute myeloid leukemia: clinical and prognostic implications. Blood 2014; 123: 914–920.
Yoshida K, Toki T, Okuno Y, Kanezaki R, Shiraishi Y, Sato-Otsubo A et al. The landscape of somatic mutations in Down syndrome-related myeloid disorders. Nat Genet 2013; 45: 1293–1299.
Thota S, Viny AD, Makishima H, Spitzer B, Radivoyevitch T, Przychodzen B et al. Genetic alterations of the cohesin complex genes in myeloid malignancies. Blood 2014; 124: 1790–1798.
Dohner H, Estey EH, Amadori S, Appelbaum FR, Buchner T, Burnett AK et al. Diagnosis and management of acute myeloid leukemia in adults: recommendations from an international expert panel, on behalf of the European LeukemiaNet. Blood 2010; 115: 453–474.
Vardiman JW, Thiele J, Arber DA, Brunning RD, Borowitz MJ, Porwit A et al. The 2008 revision of the World Health Organization (WHO) classification of myeloid neoplasms and acute leukemia: rationale and important changes. Blood 2009; 114: 937–951.
Mrozek K . Cytogenetic, molecular genetic, and clinical characteristics of acute myeloid leukemia with a complex karyotype. Semin Oncol 2008; 35: 365–377.
Heilig CE, Loffler H, Mahlknecht U, Janssen JW, Ho AD, Jauch A et al. Chromosomal instability correlates with poor outcome in patients with myelodysplastic syndromes irrespectively of the cytogenetic risk group. J Cell Mol Med 2010; 14: 895–902.
D'Andrea AD, Grompe M . The Fanconi anaemia/BRCA pathway. Nat Rev Cancer 2003; 3: 23–34.
Naim V, Rosselli F . The FANC pathway and BLM collaborate during mitosis to prevent micro-nucleation and chromosome abnormalities. Nat Cell Biol 2009; 11: 761–768.
Meyer S, Neitzel H, Tonnies H . Chromosomal aberrations associated with clonal evolution and leukemic transformation in fanconi anemia: clinical and biological implications. Anemia 2012; 2012: 349837.
Rosenberg PS, Greene MH, Alter BP . Cancer incidence in persons with Fanconi anemia. Blood 2003; 101: 822–826.
Quentin S, Cuccuini W, Ceccaldi R, Nibourel O, Pondarre C, Pages MP et al. Myelodysplasia and leukemia of Fanconi anemia are associated with a specific pattern of genomic abnormalities that includes cryptic RUNX1/AML1 lesions. Blood 2011; 117: e161–e170.
Mehta PA, Harris RE, Davies SM, Kim MO, Mueller R, Lampkin B et al. Numerical chromosomal changes and risk of development of myelodysplastic syndrome—acute myeloid leukemia in patients with Fanconi anemia. Cancer Genet Cytogenet 2010; 203: 180–186.
Poppe B, Van Limbergen H, Van Roy N, Vandecruys E, De Paepe A, Benoit Y et al. Chromosomal aberrations in Bloom syndrome patients with myeloid malignancies. Cancer Genet Cytogenet 2001; 128: 39–42.
Li Y, Li X, Ge M, Shi J, Qian L, Zheng Y et al. Long-term follow-up of clonal evolutions in 802 aplastic anemia patients: a single-center experience. Ann Hematol 2011; 90: 529–537.
Afable MG 2nd, Tiu RV, Maciejewski JP . Clonal evolution in aplastic anemia. Hematology Am Soc Hematol Educ Program 2011; 2011: 90–95.
Maciejewski JP, Risitano A, Sloand EM, Nunez O, Young NS . Distinct clinical outcomes for cytogenetic abnormalities evolving from aplastic anemia. Blood 2002; 99: 3129–3135.
Ohara A, Kojima S, Hamajima N, Tsuchida M, Imashuku S, Ohta S et al. Myelodysplastic syndrome and acute myelogenous leukemia as a late clonal complication in children with acquired aplastic anemia. Blood 1997; 90: 1009–1013.
Scheinberg P, Cooper JN, Sloand EM, Wu CO, Calado RT, Young NS . Association of telomere length of peripheral blood leukocytes with hematopoietic relapse, malignant transformation, and survival in severe aplastic anemia. JAMA 2010; 304: 1358–1364.
Dumitriu B, Feng X, Ueda Y, Kajigaya S, Townsley D, Zsu J et al. Clonal Evolution In Aplastic Anemia Is Driven By Chromosomal Instability Rather Than Mutations In Myeloid Malignancy Candidate Gene. 55th ASH Annual Meeting and Exposition, plenary session 2013.
Lange K, Holm L, Vang Nielsen K, Hahn A, Hofmann W, Kreipe H et al. Telomere shortening and chromosomal instability in myelodysplastic syndromes. Genes Chromosomes Cancer 2010; 49: 260–269.
Calado RT, Regal JA, Hills M, Yewdell WT, Dalmazzo LF, Zago MA et al. Constitutional hypomorphic telomerase mutations in patients with acute myeloid leukemia. Proc Natl Acad Sci USA 2009; 106: 1187–1192.
McClintock B . The Stability of Broken Ends of Chromosomes in Zea Mays. Genetics 1941; 26: 234–282.
DePinho RA . The age of cancer. Nature 2000; 408: 248–254.
Wiemels JL, Xiao Z, Buffler PA, Maia AT, Ma X, Dicks BM et al. In utero origin of t(8;21) AML1-ETO translocations in childhood acute myeloid leukemia. Blood 2002; 99: 3801–3805.
Stark B, Jeison M, Preudhomme C, Fenaux P, Ash S, Korek Y et al. Acquired trisomy 21 and distinct clonal evolution in acute megakaryoblastic leukaemia in young monozygotic twins. Br J Haematol 2002; 118: 1082–1086.
Bateman CM, Colman SM, Chaplin T, Young BD, Eden TO, Bhakta M et al. Acquisition of genome-wide copy number alterations in monozygotic twins with acute lymphoblastic leukemia. Blood 2010; 115: 3553–3558.
Kwong YL, Wong KF, Chan V, Chan CH . Persistence of AML1 rearrangement in peripheral blood cells in t(8;21). Cancer Genet Cytogenet 1996; 88: 151–154.
Miyamoto T, Nagafuji K, Akashi K, Harada M, Kyo T, Akashi T et al. Persistence of multipotent progenitors expressing AML1/ETO transcripts in long-term remission patients with t(8;21) acute myelogenous leukemia. Blood 1996; 87: 4789–4796.
Miyamoto T, Weissman IL, Akashi K . AML1/ETO-expressing nonleukemic stem cells in acute myelogenous leukemia with 8;21 chromosomal translocation. Proc Natl Acad Sci USA 2000; 97: 7521–7526.
Feuring-Buske M, Haase D, Buske C, Hiddemann W, Wormann B . Clonal chromosomal abnormalities in the stem cell compartment of patients with acute myeloid leukemia in morphological complete remission. Leukemia 1999; 13: 386–392.
Corces-Zimmerman MR, Hong WJ, Weissman IL, Medeiros BC, Majeti R . Preleukemic mutations in human acute myeloid leukemia affect epigenetic regulators and persist in remission. Proc Natl Acad Sci USA 2014; 111: 2548–2553.
Greaves M . Darwin and evolutionary tales in leukemia. The Ham-Wasserman Lecture. Hematology Am Soc Hematol Educ Program 2009, 3–12.
Anderson K, Lutz C, van Delft FW, Bateman CM, Guo Y, Colman SM et al. Genetic variegation of clonal architecture and propagating cells in leukaemia. Nature 2011; 469: 356–361.
Greaves M, Maley CC . Clonal evolution in cancer. Nature 2012; 481: 306–313.
Stephens PJ, Greenman CD, Fu B, Yang F, Bignell GR, Mudie LJ et al. Massive genomic rearrangement acquired in a single catastrophic event during cancer development. Cell 2011; 144: 27–40.
Rausch T, Jones DT, Zapatka M, Stutz AM, Zichner T, Weischenfeldt J et al. Genome sequencing of pediatric medulloblastoma links catastrophic DNA rearrangements with TP53 mutations. Cell 2012; 148: 59–71.
Bernasconi P, Klersy C, Boni M, Cavigliano PM, Giardini I, Rocca B et al. Does cytogenetic evolution have any prognostic relevance in myelodysplastic syndromes? A study on 153 patients from a single institution. Ann Hematol 2010; 89: 545–551.
Wang H, Wang XQ, Xu XP, Lin GW . Cytogenetic evolution correlates with poor prognosis in myelodysplastic syndrome. Cancer Genet Cytogenet 2010; 196: 159–166.
Cordoba I, Gonzalez-Porras JR, Nomdedeu B, Luno E, de Paz R, Such E et al. Better prognosis for patients with del(7q) than for patients with monosomy 7 in myelodysplastic syndrome. Cancer 2012; 118: 127–133.
Schanz J, Tuchler H, Sole F, Mallo M, Luno E, Cervera J et al. New comprehensive cytogenetic scoring system for primary myelodysplastic syndromes (MDS) and oligoblastic acute myeloid leukemia after MDS derived from an international database merge. J Clin Oncol 2012; 30: 820–829.
Shirneshan K, Platzbecker U, Nolte F, Giagounidis A, Götze K, Schlenk RF et al. Monitoring By Chromosome Banding Analysis (CBA) and FISH Of Circulating CD34+ Cells In Low-Risk MDS Patients Treated In The Le-Mon-5 Study With Lenalidomide Monotherapy Reveals 82% Cytogenetic Responders With Different Response –, Evolutionary -, and Remission Patterns and No Increased Karyotype Evolution (KE). 55th ASH Annual Meeting and Exposition, plenary session 2013.
Bershteyn M, Hayashi Y, Desachy G, Hsiao EC, Sami S, Tsang KM et al. Cell-autonomous correction of ring chromosomes in human induced pluripotent stem cells. Nature 2014; 507: 99–103.
Grimwade D, Walker H, Oliver F, Wheatley K, Harrison C, Harrison G et al. The importance of diagnostic cytogenetics on outcome in AML: analysis of 1,612 patients entered into the MRC AML 10 trial. The Medical Research Council Adult and Children's Leukaemia Working Parties. Blood 1998; 92: 2322–2333.
Grimwade D, Hills RK, Moorman AV, Walker H, Chatters S, Goldstone AH et al. Refinement of cytogenetic classification in acute myeloid leukemia: determination of prognostic significance of rare recurring chromosomal abnormalities among 5876 younger adult patients treated in the United Kingdom Medical Research Council trials. Blood 2010; 116: 354–365.
Byrd JC, Mrozek K, Dodge RK, Carroll AJ, Edwards CG, Arthur DC et al. Pretreatment cytogenetic abnormalities are predictive of induction success, cumulative incidence of relapse, and overall survival in adult patients with de novo acute myeloid leukemia: results from Cancer and Leukemia Group B (CALGB 8461). Blood 2002; 100: 4325–4336.
Schlenk RF, Benner A, Krauter J, Buchner T, Sauerland C, Ehninger G et al. Individual patient data-based meta-analysis of patients aged 16 to 60 years with core binding factor acute myeloid leukemia: a survey of the German Acute Myeloid Leukemia Intergroup. J Clin Oncol 2004; 22: 3741–3750.
Breems DA, Van Putten WL, De Greef GE, Van Zelderen-Bhola SL, Gerssen-Schoorl KB, Mellink CH et al. Monosomal karyotype in acute myeloid leukemia: a better indicator of poor prognosis than a complex karyotype. J Clin Oncol 2008; 26: 4791–4797.
Rucker FG, Schlenk RF, Bullinger L, Kayser S, Teleanu V, Kett H et al. TP53 alterations in acute myeloid leukemia with complex karyotype correlate with specific copy number alterations, monosomal karyotype, and dismal outcome. Blood 2012; 119: 2114–2121.
Middeke JM, Fang M, Cornelissen JJ, Mohr B, Appelbaum FR, Stadler M et al. Outcome of patients with abnl(17p) acute myeloid leukemia after allogeneic hematopoietic stem cell transplantation. Blood 2014; 123: 2960–2967.
Bochtler T, Stolzel F, Heilig CE, Kunz C, Mohr B, Jauch A et al. Clonal heterogeneity as detected by metaphase karyotyping is an indicator of poor prognosis in acute myeloid leukemia. J Clin Oncol 2013; 31: 3898–3905.
Sawyer JR, Roloson GJ, Head DR, Becton D . Karyotype evolution in a patient with Down syndrome and acute leukemia following a congenital leukemoid reaction. Med Pediatr Oncol 1994; 22: 404–409.
Landau DA, Carter SL, Getz G, Wu CJ . Clonal evolution in hematological malignancies and therapeutic implications. Leukemia 2014; 28: 34–43.
Delaunay J, Vey N, Leblanc T, Fenaux P, Rigal-Huguet F, Witz F et al. Prognosis of inv(16)/t(16;16) acute myeloid leukemia (AML): a survey of 110 cases from the French AML Intergroup. Blood 2003; 102: 462–469.
Perrot A, Luquet I, Pigneux A, Mugneret F, Delaunay J, Harousseau JL et al. Dismal prognostic value of monosomal karyotype in elderly patients with acute myeloid leukemia: a GOELAMS study of 186 patients with unfavorable cytogenetic abnormalities. Blood 2011; 118: 679–685.
Volkert S, Kohlmann A, Schnittger S, Kern W, Haferlach T, Haferlach C . Association of the type of 5q loss with complex karyotype, clonal evolution, TP53 mutation status, and prognosis in acute myeloid leukemia and myelodysplastic syndrome. Genes Chromosomes Cancer 2014; 53: 402–410.
Paulsson K . Genomic heterogeneity in acute leukemia. Cytogenet Genome Res 2013; 139: 174–180.
Kronke J, Bullinger L, Teleanu V, Tschurtz F, Gaidzik VI, Kuhn MW et al. Clonal evolution in relapsed NPM1-mutated acute myeloid leukemia. Blood 2013; 122: 100–108.
Bacher U, Haferlach T, Alpermann T, Zenger M, Kroger N, Beelen DW et al. Comparison of cytogenetic clonal evolution patterns following allogeneic hematopoietic transplantation versus conventional treatment in patients at relapse of AML. Biol Blood Marrow Transplant 2010; 16: 1649–1657.
Garson OM, Hagemeijer A, Sakurai M, Reeves BR, Swansbury GJ, Williams GJ et al. Cytogenetic studies of 103 patients with acute myelogenous leukemia in relapse. Cancer Genet Cytogenet 1989; 40: 187–202.
Schmidt-Hieber M, Blau IW, Richter G, Turkmen S, Bommer C, Thiel G et al. Cytogenetic studies in acute leukemia patients relapsing after allogeneic stem cell transplantation. Cancer Genet Cytogenet 2010; 198: 135–143.
Ottone T, Zaza S, Divona M, Hasan SK, Lavorgna S, Laterza S et al. Identification of emerging FLT3 ITD-positive clones during clinical remission and kinetics of disease relapse in acute myeloid leukaemia with mutated nucleophosmin. Br J Haematol 2013; 161: 533–540.
Jan M, Snyder TM, Corces-Zimmerman MR, Vyas P, Weissman IL, Quake SR et al. Clonal evolution of preleukemic hematopoietic stem cells precedes human acute myeloid leukemia. Sci Transl Med 2012; 4: 149ra18.
Mullighan CG, Phillips LA, Su X, Ma J, Miller CB, Shurtleff SA et al. Genomic analysis of the clonal origins of relapsed acute lymphoblastic leukemia. Science 2008; 322: 1377–1380.
Shlush LI, Zandi S, Mitchell A, Chen WC, Brandwein JM, Gupta V et al. Identification of pre-leukaemic haematopoietic stem cells in acute leukaemia. Nature 2014; 506: 328–333.
Damm F, Markus B, Thol F, Morgan M, Gohring G, Schlegelberger B et al. TET2 mutations in cytogenetically normal acute myeloid leukemia: Clinical implications and evolutionary patterns. Genes Chromosomes Cancer 2014; 53: 824–832.
Nazha A, Cortes J, Faderl S, Pierce S, Daver N, Kadia T et al. Activating internal tandem duplication mutations of the fms-like tyrosine kinase-3 (FLT3-ITD) at complete response and relapse in patients with acute myeloid leukemia. Haematologica 2012; 97: 1242–1245.
Gilliland DG . Molecular genetics of human leukemias: new insights into therapy. Semin Hematol 2002; 39 (4 Suppl 3): 6–11.
Frohling S, Scholl C, Gilliland DG, Levine RL . Genetics of myeloid malignancies: pathogenetic and clinical implications. J Clin Oncol 2005; 23: 6285–6295.
Scholl C, Gilliland DG, Frohling S . Deregulation of signaling pathways in acute myeloid leukemia. Semin Oncol 2008; 35: 336–345.
Grove CS, Vassiliou GS . Acute myeloid leukaemia: a paradigm for the clonal evolution of cancer? Dis Model Mech 2014; 7: 941–951.
Parkin B, Ouillette P, Li Y, Keller J, Lam C, Roulston D et al. Clonal evolution and devolution after chemotherapy in adult acute myelogenous leukemia. Blood 2013; 121: 369–377.
Chen SJ, Shen Y, Chen Z . A panoramic view of acute myeloid leukemia. Nat Genet 2013; 45: 586–587.
Gohring G, Giagounidis A, Busche G, Kreipe HH, Zimmermann M, Hellstrom-Lindberg E et al. Patients with del(5q) MDS who fail to achieve sustained erythroid or cytogenetic remission after treatment with lenalidomide have an increased risk for clonal evolution and AML progression. Ann Hematol 2010; 89: 365–374.
Jadersten M, Saft L, Smith A, Kulasekararaj A, Pomplun S, Gohring G et al. TP53 mutations in low-risk myelodysplastic syndromes with del(5q) predict disease progression. J Clin Oncol 2011; 29: 1971–1979.
Christiansen DH, Andersen MK, Pedersen-Bjergaard J . Mutations with loss of heterozygosity of p53 are common in therapy-related myelodysplasia and acute myeloid leukemia after exposure to alkylating agents and significantly associated with deletion or loss of 5q, a complex karyotype, and a poor prognosis. J Clin Oncol 2001; 19: 1405–1413.
Wong TN, Ramsingh G, Young A, Shen D, Miller C, Lamprecht T et al. The role of early TP53 mutations on the evolution of therapy-related AML. 55th ASH Annual Meeting and Exposition, plenary session 2013.
Anderhub SJ, Kramer A, Maier B . Centrosome amplification in tumorigenesis. Cancer Lett 2012; 322: 8–17.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Bochtler, T., Fröhling, S. & Krämer, A. Role of chromosomal aberrations in clonal diversity and progression of acute myeloid leukemia. Leukemia 29, 1243–1252 (2015). https://doi.org/10.1038/leu.2015.32
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2015.32
- Springer Nature Limited
This article is cited by
-
Prognostic impact of chromosomal changes at relapse after allogeneic hematopoietic cell transplantation for acute myeloid leukemia or myelodysplastic syndrome
Bone Marrow Transplantation (2022)
-
ARID1A has prognostic value in acute myeloid leukemia and promotes cell proliferation via TGF-β1/SMAD3 signaling
Clinical and Experimental Medicine (2022)
-
Nonclonal chromosomal alterations and poor survival in cytopenic patients without hematological malignancies
Molecular Cytogenetics (2019)
-
SMC3 protein levels impact on karyotype and outcome in acute myeloid leukemia
Leukemia (2019)
-
The genetics of myelodysplastic syndrome: from clonal haematopoiesis to secondary leukaemia
Nature Reviews Cancer (2017)