Abstract
Carcinogenic tobacco-specific nitrosamines (TSNAs) such as 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK) are found only in tobacco and derived products. Food and Drug Administration of the United States (US FDA) lists NNK as one of the 93 harmful and potentially harmful constituents (HPHCs) found in tobacco products and tobacco smoke. The aim of this study was to use the urinary concentration of 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol (NNAL), a major metabolite of NNK, to quantitatively estimate exposure to NNK in the US general population. In 2011–2012, the Centers for Disease Control and Prevention’s National Health and Nutrition Examination Survey (NHANES) collected urine and serum samples from a representative sample of US residents. We used a serum cotinine cutoff of 10 ng/ml with combination of questionnaire data to select non-users from cigarette users and used self-reported data to determine different tobacco product user groups. We estimated the absorbed total daily dose of NNK using a probabilistic method based on a two-compartment model. The geometric mean (GM) for the daily dose of NNK among smokers aged 12–16 years was significantly higher than that for non-users at the same age stage exposed to second-hand smoke (SHS) (P<0.001). Among those exposed to SHS, the GM for daily dose of NNK in young children (6–11 years) was nearly three times of those for adults in the age range 21–59 years. Among cigarette users, non-Hispanic Whites had the highest NNK daily dose and Mexican Americans had the lowest levels. Exclusive snuff or chewing product users had significantly higher daily dose of NNK than did cigarette smokers. Our study found that the maximum daily dose of NNK for children aged from 6 to 11 years and that for a significant percentage of cigarette users, chewing product and snuff users were higher than an estimated provisional “reference” risk level.
Similar content being viewed by others
INTRODUCTION
4-(Methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK) is one of the tobacco-specific nitrosamines (TSNA) that is found only in tobacco and tobacco-derived products.1, 2 The toxicity of NNK was evaluated in mammals and consistent carcinogenic effects have been observed.3, 4, 5, 6, 7 Recently, NNK was listed as one of the 93 harmful and potentially harmful constituents (HPHCs) in tobacco products and tobacco smoke by the Food and Drug Administration of the United States.8 Therefore, information on the body burden of NNK is crucial for assessing health effects associated with tobacco exposure in the general population.
NNK is formed mainly by nitrosation of nicotine and related tobacco alkaloids during tobacco manufacturing procedures, for example, aging, curing and fermentation. In particular, the application of different manufacturing procedures and conditions often leads to varied NNK amounts in various tobacco products.9, 10 NNK levels among different tobacco products could also vary when factors, that is, soil conditions, agricultural practices and use of fertilizer, change. In addition, NNK can also be formed during the storage and use of tobacco products.9, 11 Generally, higher levels of NNK have been observed in smokeless tobacco than in cigarettes.12
NNK is absorbed mainly through direct inhalation of the mainstream smoke (MS) by cigarette smokers13 and through oral absorption by those using smokeless tobacco products, such as oral snuff and chewing tobacco. Non-smokers absorb it by inhaling second-hand smoke (SHS), resulting from exhaled mainstream smoke and sidestream smoke.14, 15 People can be exposed to NNK by routes other than inhalation. NNK can be absorbed dermally when NNK on contaminated surfaces touches the skin. In addition, people can be exposed through oral ingestion of dusts containing NNK. NNK absorbed in mammals is metabolized to 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol (NNAL), with an urinary excretion half-life of 10–45 days.16, 17, 18 Nearly half of the total NNAL can be further metabolized to 4-hydroxy-4-(3-pyridyl)butanoic acid and NNAL-N-oxide. However, these latter metabolites are not specific to NNK; they can also be produced during the metabolism of nicotine and perhaps other TSNAs.2, 19, 20, 21 For these reasons NNAL in human urine is recognized as the preferred biomarker of NNK exposure from tobacco.2, 22, 23
Since 2007, the US Centers for Disease Control and Prevention (CDC) has been monitoring the total urinary NNAL in representative samples of the US population through the National Health and Nutrition Examination Survey (NHANES). Xia et al.24 and Bernert et al.25 reported urinary levels of NNAL in smokers and non-smokers participated in NHANES during 2007–2008, respectively. The major objective of this study was to assess exposure to NNK in the US general population by estimating the total absorbed daily dose of NNK based on total NNAL concentrations measured in urine collected from participants in NHANES conducted during 2011–2012. The results presented in this study provide an effective assessment of the country’s NNK exposure, and this assessment can serve as a means of making informed judgments about the need for health protection of the general population, including determining the efficacy of regulation of tobacco products and the best means of preventing cancer.
MATERIALS AND METHODS
Study Population
NHANES is a recurring cross sectional survey conducted by the National Center for Health Statistics (NCHS) of US CDC. NHANES seeks to measure the health and nutrition status of the US general population by use of a representative sample of the civilian non-institutionalized US population. NHANES makes use of household interviews, standardized physical examinations and the collection of medical histories and biological specimens.26 NHANES 2011–2012 was conducted in 30 locations throughout the United States. Our study includes urinary total NNAL and the serum cotinine from the 2-year survey cycle, including a total of 6705 participants aged ≥6 years with valid measurements of these two biomarkers. NHANES was reviewed and approved by the CDC Ethical Review Board and complied with all national and international guidelines on research involving human subjects.
Laboratory Methods
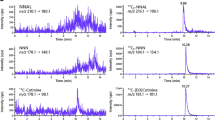
The urine samples were shipped on dry ice to the National Center for Environmental Health at CDC. There, the samples were stored at under−60 °C until analyzed. The analytical method for measuring urinary total NNAL with a limit of detection (LOD) of 0.6 pg/ml has been described in previous studies.22, 27 Briefly, the analytical approach involved enzymatic hydrolysis of the conjugated species of NNAL with β-glucuronidase in 5 ml urine spiked with 13C6-labeled NNAL internal standard, followed by online solid-phase extraction, separation with high-performance liquid chromatography, and detection by isotope-dilution positive ion electrospray ionization tandem mass spectrometry (HPLC-API MS/MS). Thus, “total” NNAL is the sum of free and conjugated forms of NNAL.
Serum cotinine was measured by using a validated HPLC-API-MS/MS method for all NHANES participants. This method used a LOD of 0.015 ng/ml.28, 29 Briefly, serum samples were first equilibrated with trideuterated cotinine internal standard and then extracted using ChemElute columns (Varian, CA, USA), followed by evaporative concentration, and analysis by HPLC-API-MS/MS. Urinary creatinine concentration was measured using an automated colorimetric method on a Beckman Coulter UniCel DxC800 Synchron clinical analyzer (Beckman Instruments, Brea, CA, USA). Calibration standards, quality control samples and laboratory blanks were included in each analytical batch, along with the study samples. Instruments were regularly evaluated to maintain the high sensitivity. All reported biomarker results met the accuracy and precision specifications of the rigorous quality control/quality assurance program of the Division of Laboratory Sciences, National Center for Environmental Health, CDC.30
Computational Method
Estimation of the daily absorption of NNK using total urinary NNAL concentration
We used a two-compartment computational method to estimate daily NNK dose based on the assumptions that NNK metabolites are eliminated from the human body following a linear two-compartment pattern and that the urinary excretion of these metabolites follows first-order kinetics. No large-scale study has yet been reported in the peer-reviewed literature estimating the daily dose of NNK from tobacco use. Conveniently, a deterministic method based on the same principle was used to study the exposure to phthalate esters by David31 and Kohn et al.32 Because NNAL has a relatively long excretion half-life (estimates ranging from 10 to 45 days),16, 17, 18 a similar method can be used to estimate the NNK dose by assuming that the daily absorption of NNK and metabolic clearance of NNAL could reach a steady state.
Daily dose of NNK was estimated by use of a probabilistic computational approach. To perform the probabilistic computation, we used a Monte Carlo (MC) simulation by sampling the input values from the statistical distributions of involved variables. The principle equation used for calculation was:

where Daily dosei is the ith total daily uptake of NNK (ng/kg-BW/day), UCi is the sampled ith creatinine-corrected urinary NNAL concentration (ng/mg), CEi is the sampled ith creatinine excretion rate normalized by body weight (mg/kg/day) calculated by multiplying creatinine concentration by urine flow rate and dividing by bodyweight, fi is the sampled ith fraction of NNAL excreted through urine (Supplementary Figure S1), and MWNNK and MWNNAL are the molecular weights of NNK and NNAL, respectively. Twenty-four-hour rate of creatinine excretion was assumed to be the same as for the time integrated by the spot urine. Distributions of those parameters used in MC simulation for different subgroups are listed in Supplementary Tables S1 and S2 (Supplementary Materials).
MC simulation
We performed MC simulations to provide the distributions of parameters involved in the computation (Supplementary Tables S1 and S2). For each sub-group in the population, we simulated 50,000 iterations. Within each iteration, a value of each parameter was randomly selected from its generated distribution. In order to avoid physiologically implausible values for the parameters involved in the simulation, we truncated the upper and lower bounds of each distribution at 1.96 times the SD above and below the mean, a method that includes 95% of the total distribution, following the methods used by Wei et al.33 The minimum, maximum, weighted means and variances for the measured urinary NNAL for each group were directly inputted into the MC simulations to obtain the distributions of daily absorption of NNK.
Tobacco use Status and Demographic Categories
Participants were categorized as cigarette smokers if their serum cotinine concentrations were >10 ng/ml.34, 35 Cigarette users who also self-reported use of any other tobacco products within the past 5 days were excluded at the time of the survey, including those using cigar, pipe and snuff, chewing tobacco, patch and gum. Non-users were selected if their serum cotinine concentrations were ≤10 ng/ml and those self-reported use of any tobacco products within the past 5 days of the survey were excluded. On the basis of self-reported data, we categorized race/ethnicity into four groups: non-Hispanic white, non-Hispanic black, Mexican American, and other race/ethnicity. Age, reported in years at the last birthday, was categorized in four groups: 6–11 (kids), 12–19 (adolescents), 20–59 (adults), and ≥60 (elderly) years.
Software and Statistical Analysis
The geometric means (GM) and the percentiles were calculated using SAS (release 9.3; SAS Institute, Cary, NC, USA) and SUDAAN (release 11.0) after incorporating the sample population weights, which account for unequal selection probabilities, cluster design and planned oversampling of certain subgroups resulting from the complex multistage probability design of NHANES. Statistics were also performed for creatinine-corrected urinary NNAL concentrations to correct for variable urine dilutions in the “spot” samples. Parametric statistics were performed only on categories with sufficient frequency of detection (> 60%) to avoid undue influence on the estimates caused by imputed values in the analyses. For concentrations below the LOD, the value of the LOD divided by the square root of two was substituted.36, 37 We considered differences between two groups to be statistically significant when P<0.05. The MC simulation was performed by use of Matlab software (R2013a, Mathworks).
RESULTS
In NHANES 2011–2012, we identified 4831 participants as non-tobacco users who had serum cotinine levels ⩽10 ng/ml38 and did not use any tobacco products at the time when samples were collected. Urinary total NNAL was detected in 62.2% of non-tobacco users (Table 1 and Figure 1). We also identified 961 participants as active cigarette smokers with serum cotinine >10 ng/ml. Participants without valid measurements for body weights (kg), urine flow (ml/min) and urinary creatinine concentration (mg/dl) were not included in this study even when their urinary NNAL and serum cotinine concentrations were available, because all these measurements were involved in the MC simulation.
Among all non-tobacco users, significantly higher geometric means and 95th percentiles of urinary total NNAL were observed among children aged from 6 to 19 years than those for adults aged >20 years. Creatinine-adjusted concentrations of NNAL were nearly twice as high in children (ages 6–11 years) as those in adolescents (ages 12–19 years) (Table 2).
Sixty-six subjects aged 12–19 years were identified as active under-age cigarette users in NHANES 2011–2012. Estimated total daily dose of NNK among these cigarette smokers were >30 times higher than those among non-smokers at the same ages (Table 3). Both the total daily absorbed NNK and urinary NNAL among these underage smokers were significantly lower than for adult smokers (Table 4).
Geometric mean and the 95th percentile for both volume-based and creatinine-adjusted urinary total NNAL, categorized in race/ethnicity groups, are also given in Tables 2 and 4. Non-Hispanic Blacks had the highest levels at all percentiles for both volume-based and creatinine-corrected NNAL concentrations in the non-smoker group, while in the cigarette smoker group, non-Hispanic Whites had the highest urinary NNAL concentrations (both volume based and creatinine adjusted). Mexican Americans in both the non-smoker and cigarette smoker groups had consistently lower creatinine-adjusted levels at all percentiles than other race/ethnicities.
One hundred and sixty-one participants reported using other tobacco products, including pipes, cigars, snuff, chewing tobacco, patch, gum and so on. Ninety-four participants used either pipes or cigars, and 55 subjects used either snuff or chewing tobacco products (Table 5). Those subjects using nicotine replacement therapy (e.g., patch, gum and so on.) were not listed owing to either small sample size or inappropriateness to combine with other groups. Total urinary NNAL was nearly detected in all those subjects. The creatinine-adjusted geometric mean for pipe or cigar users (36.7 pg/mg creatinine) is less than one-fourth of that for the cigarette users (216 pg/mg creatinine).
DISCUSSION
This study used a MC approach to calculate total daily absorbed dose of NNK. This approach allows for the use of distributions of urinary NNAL concentrations and incorporates variations and uncertainties from factors such as metabolism at a population scale. Take the urinary excretion fraction of NNAL, for example, large variations were observed in metabolism studies, including primates and human. Hecht et al.39 reported that total NNAL glucuronides accounted for 15–25 % of the urinary metabolites of NNK at all doses examined in patas monkey. Meger et al.40 reported the urinary excretion of total NNAL was in the range from 25% in 24-h urine to 58% in 10-day urine in rhesus monkey. Instead of the deterministic method in which usually a single value was used for each parameter, the MC approach can generate more realistic distributions of those parameter involved in the simulation (i.e., 15–58% was used for the fraction of NNAL excreted through urine) by propagating the parameter variability into the model, and thus the model output reflects the probabilities that those values could occur. Therefore, the Montel Carlo approach can provide better estimations of the daily absorbed NNK doses.
The higher daily dose of NNK among children aged 6–11 years old than those for adults likely reflects the differences in the time activities, the number of smokers in the home, and perhaps the metabolism and so on of children and adults. A previous study found that children living in apartments had higher mean cotinine levels than children in detached houses41. In fact, it is very likely that the characteristics of homes can be another important influence in SHS exposure and thus in NNK dose for non-users. Young children may be more vulnerable to household SHS because they may spend more of their time in homes where SHS exists as a result of cigarette use by the smokers in their home; alternatively, SHS could emanate from a smoker’s residence in multi-unit housing to expose non-users living in other units. A previous study by Matt et al.42 suggests that a smoker who smoked outside the home reduced, but not completely eliminated, the exposure of the family to SHS. The reason postulated was that the outside tobacco smoke could penetrate the windows, walls and doors of the indoor environment.
Inhalation exposure in the population exposed to tobacco smoke accounts for a predominant portion of NNK daily uptake for cigarette users, while oral ingestion could be the major NNK exposure source for oral tobacco product users (Figure 2). Regardless of the tobacco use condition, dermal exposure and oral ingestion cannot be ruled out as exposure contributors to non-tobacco product users. A recent study by Sleiman et al.43 found that NNK can be produced whenever residual nicotine from tobacco smoke that has sorbed to indoor surfaces, including clothing and human skin, reacts with ambient nitrous acid. This source of NNK has been termed third-hand smoke. According to a series of studies by the US Environmental Protection Agency,44 young children have higher frequencies of hand-to-mouth and object-to-mouth behaviors than do adults. If we assume that children have been exposed to the same levels of NNK in ambient and indoor air as adults, the daily intake from dermal and oral exposures could be higher for children because of the higher frequencies of children’s surface/object-hand-mouth behaviors. Additionally, children are sometimes unaware of the risks of SHS exposure and thus do not distance themselves from adults smoking in their vicinity. These factors may also contribute to the higher NNK dose estimated for children; additional work is needed to characterize the potential health risks associated with these tobacco-related exposures. Higher NNK dose for children also suggests efforts are needed to encourage restrictions on smoking at the locations when children are present.35
The lower levels in under-age smokers could be explained mainly by the differences in their smoking characteristics—for example, under-age smokers usually consume fewer cigarettes per day (CPD) than do adults for various reasons, including the lower frequency of children’s addiction and the greater difficulty of obtaining cigarettes. Although the daily absorbed dose of NNK in adolescent smokers (ages 12–19 years) was significantly lower than those of adult smokers (P<0.05), these adolescent smokers had NNK doses 30 times higher than adolescents exposed to SHS only.
Estimated total daily dose of NNK show similar variation patterns to the total urinary NNAL among the race/ethnicity groups. These results are consistent with those found in previous studies.45, 46, 47 Racial/ethnic differences could exist in the entire process, from the absorption to the final excretion of NNK in human bodies. Other plausible factors explaining the differences might be socioeconomic status, smoking behavior and time activity.
We observed that both volume-based and creatinine-adjusted GMs of total urinary NNAL for snuff or chewing tobacco users are >50% higher than those for all cigarette users. Our finding in NHANES 2011–2012 is similar to those previous pilot studies.48, 49 Correspondingly, the total NNK daily dose in smokeless tobacco users (snuff and chewing tobacco) are significantly higher than those for cigarette smokers and other tobacco users (Table 3), suggesting smokeless tobacco is not a safe substitute for smoking. Oral tobacco may result in higher NNK exposure because of potentially higher levels of NNK forming in smokeless products.
No minimal risk level or reference dose has been published as a comparison value for the estimated daily dose of NNK in this study. However, toxicological studies have observed prevalent cancer tumors at low doses of NNK administered to laboratory animals. Several studies on rats found a sharp increase in tumor induction occurs between total equivalent subcutaneous doses of approximately 0.3–1.0 mg/kg/day.3, 50, 51 Belinsky et al.52 reported that a 10% tumor incidence was induced at an NNK dose of 0.1 mg/kg in a group of rats treated three times a week for 20 weeks. By including a standard 10-fold inter-species and 10-fold intra-species uncertainty factors, along with a 10-fold chronic uncertainty factor, we derived a provisional “reference” level of 100 ng/kg-bw/day. The estimate daily doses of NNK at higher percentiles among both cigarette and oral tobacco product users are all significantly >100 ng/kg-bw/day (Table 5). Among non-tobacco users, the highest percentile for kids also exceeds the level of 100 ng/kg-bw/day. This provisional “reference” level of 100 ng/kg-bw/day was estimated based on limited available studies; additional studies are needed to better characterize the lower end of the dose/response curve. Once these additional studies have been completed, the estimated provisional “reference” level could be <100 ng/kg-bw/day.
NNK is only one of many carcinogenic compounds in tobacco smoke; adverse health outcomes result from the combined effects of chronic exposure to these harmful chemicals. Thus there is no safe level of exposure to tobacco smoke.53, 54, 55, 56 However, it is still important to conduct an exposure assessment to characterize exposure from multiple sources, including assessing the contribution of a single constituent in tobacco smoke, such as NNK. Such a contribution assessment can establish the exposure–response relationships in human populations. Establishing NNK uptake and urinary excretion in people exposed to tobacco products, for example, can help an investigator make informed judgments about the best means to protect people’s health, including determining the efficacy of regulation of tobacco products and the best means of preventing cancer.
In this study, we provide novel estimates of the total daily dose of NNK based on population-representative sampling as part of NHANES 2011–2012. To date, NNK daily dose has not been calculated before for a representative sample of the US population; thus no data are available with which the findings of this study can be compared. Urinary NNAL levels in tobacco users are highly affected by the tobacco consumption24 and those in second-hand smokers could be significantly associated with the smoking prevalence. Both tobacco consumption and smoking prevalence differ across global countries as a result of different tobacco control policies,57 which will largely affect the exposure to tobacco smoke in general population. Thus caution should be taken when comparing the results in this study with those observed in other countries. For example, in 2012, estimated smoking prevalence of daily smoking men aged ≥15 years ranged from >50% in approximately seven countries (i.e., Armenia, Indonesia, Kiribati and so on) to <10% in about nine countries (i.e., Antigua and Barbuda, Dominica, Ethiopia and so on). Sub-Saharan Africa and some developed countries had <20% smoking prevalence.57
The estimation of NNK daily dose based on biomarker data is likely more accurate and precise compared with estimates derived from external information, such as NNK concentrations in air, NNK concentrations in mainstream cigarette smoke, CPD and absorption rates. One main strength is that biomarkers integrate contributions from all potential exposure sources (e.g., air inhalation, oral ingestion and dermal exposure), and therefore provide a total exposure estimate. The use of external information for such an estimate, on the other hand, usually renders it difficult to illustrate all exposure scenarios for dose calculation. Such use of external factors could either underestimate the daily intake, if potential exposure routes are not identified and included in the model, or it could overestimate the value because it requires more parameters that introduce more uncertainties and variations into the model. On the downside, the biomarker approach applied in this study only included three major parameters, and the variations and uncertainties associated to the absorption, distribution, metabolism and excretion of NNK may not be thoroughly incorporated into the calculation. For example, in this study, we used the same distributions of the urinary total NNAL excretion fractions for second-hand smokers and combustion tobacco users (i.e., cigarette and cigar users). As a matter of factor, the parameter values could differ across different demographic groups (i.e., gender, race and age) in the population.24, 58, 59, 60, 61, 62, 63 Besides, parameters, such as excretion fraction, could be dose dependent64 and could be different among those smokers consuming different numbers of cigarettes daily. Due to the limited information available for the excretion fraction at different CPD levels, we were unable to account dose-dependent variations into the model outputs. Finally, it is not currently feasible to differentiate different tobacco exposure scenarios from each other (i.e., homes, workplaces, social settings, public areas and so on) using biomarker concentrations. Therefore biomarker approach does not differentiate the exposure sources and routes that could affect the absorption, distribution, metabolism and excretion mechanisms of NNK. Other computational methods have been widely developed to address such issues—for example, physiologically based pharmacokinetic modeling combined with external exposure scenarios.33 Further investigation is needed to characterize the dose variations and contributions of different tobacco exposure sources in population.
References
Hecht SS, Carmella SG, Stepanov I, Jensen J, Anderson A, Hatsukami DK . Metabolism of the tobacco-specific carcinogen 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone to its biomarker total nnal in smokeless tobacco users. Cancer Epidemiol Biomarkers Rev 2008; 17: 732–735.
Hecht SS . Biochemistry, biology, and carcinogenicity of tobacco-specific N-nitrosamines. Chem Res Toxicol 1998; 11: 559–603.
Hecht SS, Trushin N, Rigotty J, Carmella SG, Borukhova A, Akerkar S, Rivenson A . Complete inhibition of 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone-induced rat lung tumorigenesis and favorable modification of biomarkers by phenethyl isothiocyanate. Cancer Epidemiol Biomarkers Rev 1996; 5: 645–652.
Hoffmann D, Rivenson A, Amin S, Hecht SS . A study of tobacco carcinogenesis .27. Dose-response study of the carcinogenicity of tobacco-specific N-nitrosamines in F344 rats. J Cancer Res Clin 1984; 108: 81–86.
Derby KS, Cuthrell K, Caberto C, Carmella S, Murphy SE, Hecht SS,. Exposure to the carcinogen 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK) in smokers from 3 populations with different risks of lung cancer. Int J Cancer 2009; 125: 2418–2424.
Benowitz NL, Renner CC, Lanier AP, Tyndale RF, Hatsukami DK, Lindgren B et al. Exposure to nicotine and carcinogens among Southwestern Alaskan native cigarette smokers and smokeless tobacco users. Cancer Epidemiol Biomarkers Rev 2012; 21: 934–942.
E.P.A., U.S. US Environmental Protection Agency. Respiratory Health Effects of Passive Smoking: Lung Cancer and Other Disorders 1992. Available from Website: http://cfpub2.epa.gov/ncea/cfm/recordisplay.cfm?deid=2835 (accessed 15 December 2014).
US-FDA. Harmful and Potentially Harmful Constituents in Tobacco Products and Tobacco Smoke: Established List 2012. Available from: http://www.fda.gov/TobaccoProducts/GuidanceComplianceRegulatoryInformation/ucm297786.htm (accessed 11 June 2014).
Hoffmann D, Rivenson A, Wynder EL, Hecht SS . Formation of tobacco-specific nitrosamines—carcinogenicity and role of dietary-fat in their carcinogenicity. Nitrosamines Related N-Nitroso Compounds 1994; 553: 267–278.
Hecht SS, Chen CB, Hirota N, Ornaf RM, Tso TC, Hoffmann D . Tobacco-specific nitrosamines: formation from nicotine in vitro and during tobacco curing and carcinogenicity in strain A mice. J Natl Cancer Inst 1978; 60: 819–824.
Wu W, Zhang L, Jain RB, Ashley DL, Watson CH . Determination of carcinogenic tobacco-specific nitrosamines in mainstream smoke from US-brand and non-US-brand cigarettes from 14 countries. Nicotine Tob Res 2005; 7: 443–451.
IARCInternational Agency for Research on Cancer. Smokeless tobacco and some tobacco-specific N-nitrosamines. IARC monographs on the evaluation of carcinogenic risks to humans. Available from: http://monographs.iarc.fr/ENG/Monographs/vol89/index.php (accessed 15 December 2014), 2007.
Hecht SS, Carmella SG, Ye M, Le KA, Jensen JA, Zimmerman CL et al. Quantitation of metabolites of 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone after cessation of smokeless tobacco use. Cancer Res 2002; 62: 129–134.
Helen G, Bernert JT, Hall DB, Sosnoff CS, Xia Y, Balmes JR et al. Exposure to secondhand smoke outside of a bar and a restaurant and tobacco exposure biomarkers in nonsmokers. Environ Health Perspect 2012; 120: 1010–1016.
Vardavas CI, Fthenou E, Patelarou E, Bagkeris E, Murphy S, Hecht SS et al. Exposure to different sources of second-hand smoke during pregnancy and its effect on urinary cotinine and tobacco-specific nitrosamine (NNAL) concentrations. Tob Control. 2012; 22: 194–200.
Hecht SS, Carmella SG, Chen M, Dor Koch JF, Miller AT, Murphy SE et al. Quantitation of urinary metabolites of a tobacco-specific lung carcinogen after smoking cessation. Cancer Res 1999; 59: 590–596.
Jacob P, Havel C, Lee DH, Yu L, Eisner MD, Benowitz NL . Subpicogram per milliliter determination of the tobacco-specific carcinogen metabolite 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol in human urine using liquid chromatography-tandem mass spectrometry. Anal Chem 2008; 80: 8115–8121.
Goniewicz ML, Havel CM, Peng MW, Jacob P, 3rd, Dempsey D, Yu L et al. Elimination kinetics of the tobacco-specific biomarker and lung carcinogen 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol. Cancer Epidemiol Biomarkers Rev 2009; 18: 3421–3425.
Hukkanen J, Jacob P, Benowitz NL . Metabolism and disposition kinetics of nicotine. Pharmacol Rev 2005; 57: 79–115.
McGuffey JE, Wei B, Bernert JT, Morrow JC, Xia B, Wang L et al. Validation of a lc-ms/ms method for quantifying urinary nicotine, six nicotine metabolites and the minor alkaloids—anatabine and anabasine—in smokers’ urine. PLoS One 2014; 9 (7): e101816.
Wei B, Feng J, Rehmani IJ, Miller S, McGuffey JE, Blount BC et al. A high-throughput robotic sample preparation system and HPLC-MS/MS for measuring urinary anatabine, anabasine, nicotine and major nicotine metabolites. Clin Chim Acta 2014; 436 (25): 290–297.
Xia Y, McGuffey JE, Bhattacharyya S, Sellergren B, Yilmaz E, Wang L et al. Analysis of the tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol in urine by extraction on a molecularly imprinted polymer column and liquid chromatography/atmospheric pressure ionization tandem mass spectrometry. Anal Chem 2005; 77: 7639–7645.
Carmella SG, Le KA, Upadhyaya P, Hecht SS . Analysis of N- and O-glucuronides of 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol (NNAL) in human urine. Chem Res Toxicol 2002; 15: 545–550.
Xia Y, Bernert JT, Jain RB, Ashley DL, Pirkle JL . Tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol (NNAL) in smokers in the United States: NHANES 2007-2008. Biomarkers 2011; 16: 112–119.
Bernert JT, Pirkle JL, Xia Y, Jain RB, Ashley DL, Sampson EJ . Urine concentrations of a tobacco-specific nitrosamine carcinogen in the US population from secondhand smoke exposure. Cancer Epidemiol Biomarkers Rev 2010; 19: 2969–2977.
US-CDC. National Health and Nutrition Examination Survey. National Center for Health Statistics. Centers for Disease Control and Prevention. Available from: http://www.cdc.gov/nchs/nhanes.htm (accessed 24 September 2014), 2014.
Xia Y, Bernert JT . Stability of the tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol in urine samples stored at various temperatures. J Anal Toxicol 2010; 34: 411–415.
Bernert JT, Turner WE, Pirkle JL, Sosnoff CS, Akins JR, Waldrep MK et al. Development and validation of sensitive method for determination of serum cotinine in smokers and nonsmokers by liquid chromatography atmospheric pressure ionization tandem mass spectrometry. Clin Chem 1997; 43: 2281–2291.
Bernert JT, McGuffey JE, Morrison MA, Pirkle JL . Comparison of serum and salivary cotinine measurements by a sensitive high-performance liquid chromatography-tandem mass spectrometry method as an indicator of exposure to tobacco smoke among smokers and nonsmokers. J Anal Toxicol 2000; 24: 333–339.
Caudill SP, Schleicher RL, Pirkle JL . Multi-rule quality control for the age-related eye disease study. Stat Med 2008; 27: 4094–4106.
David RM . Exposure to phthalate esters. Environ Health Perspect 2000; 108: A440–A440.
Kohn MC, Parham F, Masten SA, Portier CJ, Shelby MD, Brock JW et al. Human exposure estimates for phthalates. Environ Health Perspect 2000; 108: A440–A442.
Wei B, Isukapalli SS, Weisel CP . Studying permethrin exposure in flight attendants using a physiologically based pharmacokinetic model. J Expo Sci Environ Epidemiol 2013; 23: 416–427.
Pirkle JL, Flegal KM, Bernert JT, Brody DJ, Etzel RA, Maurer KR . Exposure of the US population to environmental tobacco smoke. JAMA 1996; 275: 1233–1240.
Pirkle JL, Bernert JT, Caudill SA, Sosnoff CS, Pechacek TF . Trends in the exposure of nonsmokers in the US population to secondhand smoke: 1988-2002. Environ Health Perspect 2006; 114: 853–858.
Hornung RW, Reed LD . Estimation of average concentration in the presence of nondetectable values. Appl Occup Environ Hygiene 1990; 5: 46–51.
Wei BN, Mohan KR, Weisel CP . Exposure of flight attendants to pyrethroid insecticides on commercial flights: Urinary metabolite levels and implications. Int J Hygiene Environ Health 2012; 215: 465–473.
Pirkle JL, Flegal KM, Bernert JT, Brody DJ, Etzel RA, Maurer KR . Exposure of the US population to environmental tobacco smoke—The Third National Health and Nutrition Examination Survey, 1988 to 1991. JAMA 1996; 275: 1233–1240.
Hecht SS, Trushin N, Reid-Quinn CA, Burak ES, Jones AB, Southers JL et al. Metabolism of the tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone in the patas monkey: pharmacokinetics and characterization of glucuronide metabolites. Carcinogenesis 1993; 14: 229–236.
Meger M, Richter E, Zwickenpflug W, Oehlmann C, Hargaden MB, A-Rahim YI et al. Metabolism and disposition of 4-(methylnitrosamino)-1-(3-pyridyl)-1- butanone (NNK) in rhesus monkeys. Drug Metab Dispos 1999; 27: 471–478.
Wilson KM, Klein JD, Blumkin AK, Gottlieb M, Winickoff JP . Tobacco-smoke exposure in children who live in multiunit housing. Pediatrics 2011; 127: 85–92.
Matt GE, Quintana PJ, Zakarian JM, Fortmann AL, Chatfield DA, Hoh E et al. When smokers move out and non-smokers move in: residential thirdhand smoke pollution and exposure. Tob Control 2011; 20: e1.
Sleiman M, Gundel LA, Pankow JF, Jacob P, 3rd, Singer BC, Destaillats H . Formation of carcinogens indoors by surface-mediated reactions of nicotine with nitrous acid, leading to potential thirdhand smoke hazards. Proc Natl Acad Sci USA 2010; 107: 6576–6581.
US-EPA. US Environmental Protection Agency Exposure Factors Handbook 2011 Edition. (Final): Chapter 4—Non-Dietary Ingestion Factors 2011.
Caraballo RS, Giovino GA, Pechacek TF, Mowery PD, Richter PA, Strauss WJ et al. Racial and ethnic differences in serum cotinine levels of cigarette smokers. JAMA 1998; 280: 135–139.
Haiman CA, Stram DO, Wilkens LR, Pike MC, Kolonel LN, Henderson BE et al. Ethnic and racial differences in the smoking-related risk of lung cancer. N Engl J Med 2006; 354: 333–342.
Benowitz NL, Dains KM, Dempsey D, Wilson M, Jacob P . Racial differences in the relationship between number of cigarettes smoked and nicotine and carcinogen exposure. Nicotine Tob Res 2011; 13: 772–783.
Kresty LA, Carmella SG, Borukhova A, Akerkar SA, Gopalakrishnan R, Harris RE et al. Metabolites of a tobacco-specific nitrosamine, 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK), in the urine of smokeless tobacco users: relationship between urinary biomarkers and oral leukoplakia. Cancer Epidemiol Biomarkers Rev 1996; 5: 521–525.
Stepanov I, Hecht SS . Tobacco-specific nitrosamines and their pyridine-N-glucuronides in the urine of smokers and smokeless tobacco users. Cancer Epidemiol Biomarkers Rev 2005; 14: 885–891.
Rivenson A, Hoffmann D, Prokopczyk B, Amin S, Hecht SS . Induction of lung and exocrine pancreas tumors in F344 rats by tobacco-specific and Areca-derived N-nitrosamines. Cancer Res 1988; 48: 6912–6917.
Hoffmann D, Rivenson A, Abbi R, Wynder EL . A study of tobacco carcinogenesis: effect of the fat content of the diet on the carcinogenic activity of 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone in F344 rats. Cancer Res 1993; 53: 2758–2761.
Belinsky SA, Foley JF, White CM, Anderson MW, Maronpot RR . Dose-response relationship between O6-methylguanine formation in Clara cells and induction of pulmonary neoplasia in the rat by 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone. Cancer Res 1990; 50: 3772–3780.
Winickoff JP, Friebely J, Tanski SE, Sherrod C, Matt GE, Hovell MF et al. Beliefs about the health effects of “thirdhand” smoke and home smoking bans. Pediatrics 2009; 123: e74–e79.
Eisner MD, Balmes J, Katz PP, Trupin L, Yelin EH, Blanc PD . Lifetime environmental tobacco smoke exposure and the risk of chronic obstructive pulmonary disease. Environ Health 2005; 4: 7.
Johansson A, Hermansson G, Ludvigsson J . How should parents protect their children from environmental tobacco-smoke exposure in the home? Pediatrics 2004; 113: e291–e295.
Yolton K, Dietrich K, Auinger P, Lanphear BP, Hornung R . Exposure to environmental tobacco smoke and cognitive abilities among US children and adolescents. Environ Health Perspect 2005; 113: 98.
Ng M, Freeman MK, Fleming TD, Robinson M, Dwyer-Lindgren L, Thomson B et al. Smoking prevalence and cigarette consumption in 187 countries, 1980-2012. JAMA 2014; 311: 183–192.
Melikian AA, Djordjevic MV, Hosey J, Zhang J, Chen S, Zang E et al. Gender differences relative to smoking behavior and emissions of toxins from mainstream cigarette smoke. Nicotine Tob Res 2007; 9: 377–387.
Bernert JT, Pirkle JL, Xia Y, Jain RB, Ashley DL, Sampson EJ . Urine concentrations of a tobacco-specific nitrosamine carcinogen in the U.S. population from secondhand smoke exposure. Cancer Epidemiol Biomarkers Rev 2010; 19: 2969–2977.
Ter-Minassian M, Asomaning K, Zhao Y, Chen F, Su L, Carmella SG et al. Genetic variability in the metabolism of the tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK) to 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol (NNAL). Int J Cancer 2012; 130: 1338–1346.
Richie JP, Carmella SG, Muscat JE, Scott DG, Akerkar SA, Hecht SS . Differences in the urinary metabolites of the tobacco-specific lung carcinogen 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone in black and white smokers. Cancer Epidemiol Biomarkers Rev 1997; 6: 783–790.
Muscat JE, Djordjevic MV, Colosimo S, Stellman SD, Richie JP . Racial differences in exposure and glucuronidation of the tobacco‐specific carcinogen 4‐(methylnitrosamino)‐1‐(3‐pyridyl)‐1‐butanone (NNK). Cancer 2005; 103: 1420–1426.
Carmella SG, Akerkar SA, Richie J, Hecht SS . Intraindividual and interindividual differences in metabolites of the tobacco-specific lung carcinogen 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK) in smokers' urine. Cancer Epidemiol Biomarkers Rev 1995; 4: 635–642.
Morse MA, Eklind KI, Toussaint M, Amin SG, Chung F-L . Characterization of a glucuronide metabolite of 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK) and its dose-dependent excretion in the urine of mice and rats. Carcinogenesis 1990; 11: 1819–1823.
Acknowledgements
We thank Yang Xia and Connie S. Sosnoff for measuring urinary total NNAL and serum cotinine, respectively. We also thank Ernest L. Martin, Patricia Ruiz and Rey Decastro at CDC for their valuable comments. The findings and conclusions in this presentation are those of the authors and do not necessarily represent the views of the Centers for Disease Control and Prevention (CDC). Use of trade names and commercial sources is for identification only, and such use does not constitute endorsement by the US Department of Health and Human Services or the Centers for Disease Control and Prevention.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Journal of Exposure Science and Environmental Epidemiology website
Supplementary information
Rights and permissions
About this article
Cite this article
Wei, B., Blount, B., Xia, B. et al. Assessing exposure to tobacco-specific carcinogen NNK using its urinary metabolite NNAL measured in US population: 2011–2012. J Expo Sci Environ Epidemiol 26, 249–256 (2016). https://doi.org/10.1038/jes.2014.88
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jes.2014.88
- Springer Nature America, Inc.
Keywords
This article is cited by
-
Carcinogenic and tobacco smoke-derived particulate matter biomarker uptake and associated healthcare patterns among children
Pediatric Research (2023)
-
Association between DNA methylation variability and self-reported exposure to heavy metals
Scientific Reports (2022)
-
LKB1 phosphorylation and deactivation in lung cancer by NNAL, a metabolite of tobacco-specific carcinogen, in an isomer-dependent manner
Oncogene (2022)
-
Association between Urinary Metabolite Levels of Organophosphorus Flame Retardants and Serum Sex Hormone Levels Measured in a Reference Sample of the US General Population
Exposure and Health (2020)
-
Dietary phytochemicals as the potential protectors against carcinogenesis and their role in cancer chemoprevention
Clinical and Experimental Medicine (2020)