Abstract
Background:
A relationship has been reported between blood concentrations of coagulation factor VII (FVII) and obesity. In addition to its role in coagulation, FVII has been shown to inhibit insulin signals in adipocytes. However, the production of FVII by adipocytes remains unclear.
Objective:
We herein investigated the production and secretion of FVII by adipocytes, especially in relation to obesity-related conditions including adipose inflammation and sympathetic nerve activation.
Methods:
C57Bl/6J mice were fed a low- or high-fat diet and the expression of FVII messenger RNA (mRNA) was then examined in adipose tissue. 3T3-L1 cells were used as an adipocyte model for in vitro experiments in which these cells were treated with tumor necrosis factor-α (TNF-α) or isoproterenol. The expression and secretion of FVII were assessed by quantitative real-time PCR, Western blotting and enzyme-linked immunosorbent assays.
Results:
The expression of FVII mRNA in the adipose tissue of mice fed with high-fat diet was significantly higher than that in mice fed with low-fat diet. Expression of the FVII gene and protein was induced during adipogenesis and maintained in mature adipocytes. The expression and secretion of FVII mRNA were increased in the culture medium of 3T3-L1 adipocytes treated with TNF-α, and these effects were blocked when these cells were exposed to inhibitors of mitogen-activated kinases or NF-κB activation. The β-adrenoceptor agonist isoproterenol stimulated the secretion of FVII from mature adipocytes via the cyclic AMP/protein kinase A pathway. Blockade of secreted FVII with the anti-FVII antibody did not affect the phosphorylation of Akt in the isoproterenol-stimulated adipocytes.
Conclusion:
Obese adipose tissue produced FVII. The production and secretion of FVII by adipocytes was enhanced by TNF-α or isoproterenol via different mechanisms. These results indicate that FVII is an adipokine that plays an important role in the pathogenesis of obesity.
Similar content being viewed by others
Introduction
Obesity is characterized by the excessive accumulation of fat. Recent studies reported that obesity was associated with a dysregulation in adipokines and the infiltration of inflammatory cells, which has been linked to the upregulation of tumor necrosis factor-α (TNF-α). Furthermore, the neural networks of multiple organs including sympathetic nerve activation have been shown to contribute to the pathogenesis of obesity.1, 2, 3 The incidence of many cardiovascular risk factors such as lipid abnormalities, hypertension and diabetes is higher in obese patients.4 In addition to these risk factors, a previous study demonstrated that hemostatic and fibrinolytic disturbances had a role in the pathogenesis of cardiovascular diseases as a consequence of obesity and its related complications.5 Plasma concentrations of fibrinogen, factor VII, factor VIII, von Willebrand factor and plasminogen activator inhibitor-1 (PAI-1) were shown to be significantly higher in obese subjects than in non-obese subjects.6
Coagulation factor VII (FVII) is a vitamin K-dependent glycoprotein that is mainly produced by the liver. FVII is crucially involved in the extrinsic pathway of blood coagulation.7 It is present in the circulation primarily as an inactive zymogen. When vascular wall injuries occur, FVII forms a complex with its cell surface receptor and cofactor, tissue factor (TF). Once in a complex with TF, FVII is rapidly cleaved to its active form (FVIIa), which subsequently converts zymogen factor IX and factor X into active enzymes. Activated factor X accelerates the formation of thrombin, which, in turn, mediates the formation of fibrin to produce blood clots. Thus, FVII has a pivotal role in initiating the TF-induced coagulation pathway. In addition to this crucial role of FVII in blood coagulation, Badeanlou et al.8 recently reported that FVII has other roles in metabolism by inhibiting insulin signals via the TF-protease activating receptor 2 pathway in adipocytes.8 These aforementioned roles implicate FVII as a multi-functional molecule in vivo.
Evidence is accumulating to show that FVII is related to obesity and its associated conditions. Body mass index and the waist-to-hip ratio are independently associated with circulating levels of fibrinogen and FVII as well as those of anti-fibrinolytic proteins including PAI-1.9 FVII levels were also found to be higher in subjects with metabolic syndrome than in healthy subjects.10 High-fat meals induce the postprandial activation of plasma FVII.11 Elevated values of plasma FVII due to obesity were decreased by weight reductions in both humans12, 13, 14 and mice.15 These lines of evidence indicated that FVII has a pivotal role in obesity. Plasma FVII levels have been closely associated with serum triglyceride levels, and were attenuated by interventions with anti-dyslipidemic agents,16 which may be explained by FVII partly binding to very low-density lipoproteins in plasma.17 Moreover, increased plasma FVII levels have been reported in patients with diabetes and have been associated with an increase in systemic blood coagulation activity.18, 19, 20 A glucose clump study revealed that the mechanism by which FVII levels were modulated in diabetes was mediated, at least in part, by hyperglycemia, not hyperinsulinemia.21 FVII activity has been proposed as an independent cardiovascular risk factor, was shown to be higher in various atherosclerotic diseases.22 Overall, FVII has been associated with the pathophysiology of obesity, dyslipidemia and diabetes.
FVII is mainly produced by the liver and is secreted into the blood.7 However, several studies described the extra-hepatic production of FVII.23, 24 Mihara et al.25 showed that the expression of FVII messenger RNA (mRNA) in the adipose tissue of db/db mice was higher than that in control mice. db/db mice are leptin receptor-deficient mutant mice that spontaneously become obese.26 The cell components of adipose tissue include pre-adipocytes, fibroblasts, endothelial cells and immune cells in addition to adipocytes. However, it currently remains unclear whether FVII gene expression is higher in the adipose tissue of obese wild-type mice and also which kinds of cells in adipose tissue produce FVII.
We herein investigated whether the upregulated expression of FVII in the adipose tissue of wild-type obese mice was also present in mutant db/db mice. We then focused on adipocytes, which comprise the vast majority of cells in adipose tissue, to examine the production and secretion of FVII. We determined whether and how adipocytes produced and secreted FVII, especially in two obesity-related conditions: adipose inflammation and sympathetic nerve activation.
Materials and methods
Chemicals
Mouse recombinant TNF-α, interleukin-1β (IL-1β), IL-6, isoproterenol, sodium salicylate, isobutyl-methyl-xanthine, 8-bromo-cyclic AMP (8-bromo-cAMP) and H-89 (N-[2-(p-bromocinnamylamino)ethyl]-5-isoquinoline-sulfonamide) were purchased from Sigma (St Louis, MO, USA). U0126 was purchased from Cayman Chemical (Ann Arbor, MI, USA), and SB202190, SP600125 and 6-amino-4-(4-phenoxyphenylethylamino) quinazoline were from ENZO Life Sciences (Farmingdale, NY, USA).
Animals
Male C57BL/6J mice (Charles River Japan, Tokyo, Japan) were maintained in a temperature- and light-controlled room. After a 2-week acclimation period, mice were fed with a low-fat (LF; D12450B, Research Diets, New Brunswick, NJ, USA) or high-fat diet (HF; D12492, Research Diets) for 10 weeks. Epididymal adipose tissue was removed and frozen at −80 °C for further analysis. All animal interventions were performed in accordance with the Animal Care and Use Committee of Asahikawa Medical University.
Cell culture and adipocyte differentiation
3T3-L1 fibroblasts were purchased from the American Type Culture Collection (Manassas, VA, USA). In each experiment, cells were seeded into six-well culture plates. The cells were induced to differentiate into adipocytes according to the standard protocol using isobutyl-methyl-xanthine, dexamethasone and insulin (MDI) as described previously.27 Fully differentiated adipocytes were used 12–14 days after the induction of differentiation.
Cell treatment
Messenger RNA and intracellular protein were extracted at each time point as indicated in the figure legends and then used in the experiments.27 Fully differentiated 3T3-L1 adipocytes were treated with TNF-α, IL-1β or IL-6 at a dose of 20 ng ml–1 for 24 h, and total RNA was then extracted for the expression analysis of FVII. The effects of TNF-α on FVII expression were investigated using multiple concentrations (0–20 ng ml–1) of TNF-α for 36 h or at different time points (0–36 h) at a dose of 20 ng ml–1. Cells were treated with a mitogen-activated protein kinase (MAPK) inhibitor, U0126 (10 μM), SB202190 (10 μM) or SP600125 (20 μM) 0.5 h before the treatment with TNF-α. Cells were also treated with a NF-κB inhibitor, sodium salicylate or quinazoline 0.5 h before the treatment with TNF-α. After cells were treated with these inhibitors, TNF-α at a dose of 20 ng ml–1 was added to the medium, and the cells were then incubated for an additional 36 h. Sodium salicylate was dissolved in water, whereas the MAPK inhibitors and quinazoline were dissolved in dimethyl sulfoxide. The experiments with inhibitors were performed with an adjustment to a final concentration of 0.1% dimethyl sulfoxide in the medium.
Isoproterenol was dissolved in endotoxin-free sterile water (Sigma) to make a stock solution. Cells were treated with isoproterenol at different doses or at serial time points as indicated in the figure legends. Cell culture media were saved and used for further analysis using Western blotting and enzyme-linked immunosorbent assay (ELISA). Intracellular protein and total RNA were extracted for further analyses. 3T3-L1 adipocytes were treated with several combinations of isoproterenol (3 μM) and isobutyl-methyl-xanthine (0–100 μM) for 2 h. 3T3-L1 adipocytes were also treated with 8-bromo-cAMP for 2 h. The cells were treated with H-89, a specific inhibitor of cAMP-dependent protein kinase A (PKA) activation 0.5 h before the treatment with isoproterenol at a dose of 10 μM for 2 h. Cells were cultured in the presence of the anti-FVII antibody (1 μg ml–1) for 0.5 h before isoproterenol (3 μM, 24 h) was added. At the end of the treatment, insulin (5 nM) was added for 10 min. In these experiments, the culture medium was saved and intracellular protein was extracted for further analyses.
Quantitative real-time PCR analysis
RNA extraction and complementary DNA synthesis were performed as described previously.27 Briefly, quantitative real-time PCR analysis were performed with an Applied Biosystems 7500 Sequence Detection System using the TaqMan Gene Expression master mix, according to the manufacturer's instructions (Applied Biosystems, Foster City, CA, USA). Validated TaqMan Gene Expression Assays containing gene-specific TaqMan probes and primers (Applied Biosystems) for mouse coagulation factor VII (Mm00487333_m1) were used for assay-on-demand gene expression products. Amplification was determined using the comparative threshold cycle (Ct) method and Sequence Detection Software version 1.4 (Applied Biosystems). The 2–ddCt method was used to calculate the relative expression of mRNA.27 18S ribosomal RNA was used as the endogenous reference gene because its expression did not significantly change between samples. Results were normalized by the expression levels of the eukaryotic 18S ribosomal RNA gene (Hs99999901_s1) and were then calculated as fold changes relative to the vehicle control. All experiments were performed at least in triplicate.
Protein extraction and Western blotting
Protein extraction and Western blotting were performed as described previously.27 Briefly, to analyze the culture medium, 10 μl out of 1 ml of culture medium (cell culture area of 10 cm2 per well) was subjected to SDS–polyacrylamide gel electrophoresis (SDS–PAGE). To analyze cell lysates, equal amounts of extracted protein (20 μg per lane) were resolved on SDS–PAGE. Western blotting was performed using an antibody against FVII (Novus Biologicals, Littleton, CO, USA), PPAR-γ, C/EBP-α, p-PKAα/β/γ catalytic subunits (Thr 198), β-actin (Santa Cruz Biotechnology, Santa Cruz, CA, USA), phospho-Akt (Ser 473) or Akt (Cell Signaling Technology, Danvers, MA, USA). Immunoreactive bands were visualized with enhanced chemiluminescence (GE Health Care, Tokyo, Japan) using a Light Capture II system (ATTO Co., Tokyo, Japan).
Mouse FVII ELISA
3T3-L1 adipocytes were cultured in six-well culture plates and treated as described in each experiment. A 100 μl aliquot of the culture medium (1.0-ml per well) was applied to the Mouse Coagulation Factor FVII ELISA Set (SEK50034, Sino Biological, Beijing, China) using a 96-well ELISA plate (MS-8796F, Sumitomo Bakelite Co. Ltd., Tokyo, Japan), according to the manufacturer's instructions with slight modifications. Color development was performed using 3,3′,5,5′-tetramethylbenzidine (Sigma). The absorbance of each well was read at a wavelength of 450 nm with a microplate reader (MTP-120, Corona Electric, Hitachinaka, Japan). The concentration of FVII was calculated from the standard curve in each experiment.
Statistical analysis
The results are expressed as means±s.e. Two-tailed unpaired Student’s t-tests were used for comparison of the two groups. To compare more than two groups, analysis of variance was performed followed by Turkey’s multiple comparison tests using GraphPad PRISM software version 5 (GraphPad Software Inc., San Diego, CA, USA). P<0.05 was considered significant.
Results
FVII expression was increased in the adipose tissue of obese wild-type mice fed with HF diet
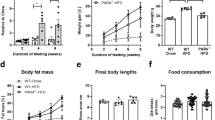
Male C57BL/6J mice were fed a LF or HF diet for 10 weeks. At the end of the experiment, mice fed with HF diet became obese; the body weights of mice fed with HF diet were higher than those fed with LF diet (n=4, 39.4 vs 28.4 g, P<0.05). Gene expression levels of FVII in epididymal adipose tissue were significantly higher (55-fold) in HF diet mice than in LF diet mice, as analyzed by quantitative real-time PCR (Figure 1a).
Factor VII expression in the adipose tissue of mice and during adipogenesis in 3T3-L1 cells. (a) Male C57BL/6J mice were fed a low-fat (LF) or high-fat (HF) diet for 10 weeks (n=4). Total RNA was extracted from epididymal fat tissue and FVII mRNA expression levels were measured using quantitative real-time PCR. Expression values were normalized to 18S ribosomal RNA (rRNA) and fold changes were expressed relative to LF. Data are represented as mean±s.e. *P<0.05 significantly different from LF. (b, c) 3T3-L1 cells were induced to differentiate, as described in the Materials and methods section. MDI represents the duration of differentiation induction. The gene (b) and protein (c) expression of FVII was determined at various time points during adipogenesis by quantitative real-time PCR and immunoblotting. (b) FVII gene expression levels were normalized with the expression levels of 18S rRNA. Results were calculated as fold changes relative to the values on day –2 and expressed as mean±s.e. (n=3). *P<0.05 significantly different from day –2. (c) FVII protein expression in cell lysates [FVII (lys)] during the course of adipocyte differentiation (n=3) was visualized. Representative blots are shown. PPAR-γ and C/EBP-α protein expression was used as markers of adipocyte differentiation. β-actin was used as an internal loading control.
3T3-L1 adipocytes expressed FVII
In addition to adipocytes, adipose tissue consists of endothelial cells, smooth muscle cells and circulating blood cells. We next attempted to investigate whether adipocytes expressed FVII. We examined the expression of FVII during adipocyte differentiation in 3T3-L1 cells. The expression of FVII mRNA was rapidly and significantly induced during the treatment with a differentiation cocktail (MDI) and was ~100-fold higher than that before the induction (day –2; Figure 1b). FVII mRNA levels had decreased on day 2, but were maintained at higher levels in mature adipocytes up to day 20. The protein expression of FVII in cell lysates was also detected in mature adipocytes by immunoblotting (Figure 1c). The differentiation of adipocytes was assessed based on the expression of the adipocyte markers, PPAR-γ and CEBP-α.28 These results indicated that adipocytes expressed FVII.
FVII expression was increased by TNF-α at the gene level in 3T3-L1 adipocytes
Fully differentiated adipocytes were exposed to various cytokines related to the pathogenesis of obesity, such as TNF-α, IL-1β and IL-6. As shown in Figure 2a, TNF-α significantly increased FVII gene expression levels (P<0.05), while IL-1β and IL-6 did not. The increase observed in the expression of FVII mRNA was both dose and time dependent (Figures 2b and c). The secretion of FVII in conditioned medium was also increased, as confirmed by immunoblotting (Figures 2d and e) and ELISA (Figures 2f and g). These results demonstrated that TNF-α increased the expression and secretion of FVII in 3T3-L1 adipocytes.
Gene expression and secretion of FVII induced by TNF-α in 3T3-L1 adipocytes. (a) Fully differentiated 3T3-L1 adipocytes were treated with either TNF-α, interleukin (IL)-1β, IL-6 or vehicle (Veh) for 24 h (n=3). (b, d and f) 3T3-L1 adipocytes were treated with different concentrations of TNF-α at doses of 0, 2 and 20 ng ml–1 for 36 h (n=3). (c, e and g) 3T3-L1 adipocytes were treated with 20 ng ml–1 of TNF-α for 12, 24 and 36 h (n=3). (h) Fully differentiated 3T3-L1 adipocytes were cultured in the presence of U0126 (10 μM), SB202190 (SB, 10 μM) or SP600125 (SP, 20 μM) for 0.5 h before the addition of TNF-α (20 ng ml–1, 36 h; n=3). (i) Cells were also cultured in the presence of salicylate (Sal, 10 mM) or quinazoline (QNZ, 20 nM) for 0.5 h before the addition of TNF-α (20 ng ml–1, 36 h; n=4). Dimethyl sulfoxide (DMSO) was used as a vehicle control. FVII gene expression (a–c, h and i) was analyzed by quantitative PCR and normalized to the expression of 18S ribosomal RNA. The secretion of FVII into the medium [FVII (m)] was analyzed by immunoblotting (d, e) and ELISA (f, g). Representative blots are shown. Data were calculated by fold changes vs vehicle control (a, b and f), time 0 (c, g) or control without TNF-α (h, i) and expressed as the mean±s.e. *P<0.05 vs control.
MAPK and NF-κB signaling may be involved in the TNF-α-induced expression of FVII in 3T3-L1 adipocytes
To investigate the mechanism by which TNF-α increased the expression of FVII, we examined the possible involvement of MAPK and NF-κB signaling. MAPKs are a family of three distinct protein kinases called MEK-ERK1/2, p38 and c-Jun N-terminal kinase (JNK), and are involved in the intracellular signaling of TNF-α.29 To clarify whether each MAPK was involved in the increased expression of FVII mRNA by TNF-α, we examined the effects of each kinase inhibitor for MEK (U0126), p38 (SB202190) or JNK (SP600125) on the mRNA expression of FVII by TNF-α in 3T3-L1 adipocytes. As shown in Figure 2h, all three MAPK inhibitors blocked the induction of FVII mRNA by TNF-α. We next employed two kinds of inhibitors of NF-κB activation, sodium salicylate and quinazoline. Pretreatment with these inhibitors canceled the induction of FVII expression induced by TNF-α (Figure 2i). These results indicated that the TNF-α-induced expression of FVII may be mediated by MAPK and NF-κB signaling.
Isoproterenol-induced FVII secretion in 3T3-L1 adipocytes
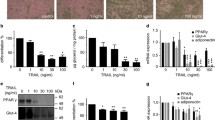
Sympathetic nerve activation is a feature in the pathogenesis of obesity.1, 2, 3 We attempted to stimulate 3T3-L1 adipocytes by isoproterenol, an agonist of the β-adrenergic receptor. As shown in Figure 3a, isoproterenol dose dependently increased the secretion of FVII in the medium. Time-course analysis revealed that isoproterenol significantly increased the secretion of FVII after 60 min, as confirmed by immunoblotting and ELISA (Figures 3b and c). The treatment with isoproterenol did not appear to affect the secretion of FVII in cell lysates. Isoproterenol did not alter the mRNA expression levels of FVII (Figure 3d). These results indicated that isoproterenol stimulated the secretion of FVII in 3T3-L1 adipocytes.
Isoproterenol-induced secretion of FVII by 3T3-L1 adipocytes via the cAMP–PKA pathway. (a) Fully differentiated 3T3-L1 adipocytes were treated with isoproterenol at a dose of 0, 1, 3 or 10 μM for 24 h. (b–d) 3T3-L1 adipocytes were treated with 3 μM of isoproterenol at different time points, and the culture medium was then collected. Total intracellular protein and total RNA were then extracted. (e) Fully differentiated 3T3-L1 adipocytes were treated with a combination of isoproterenol (Isop, 3 μM) and isobutyl-methyl-xanthine (IBMX, 0–100 μM) as indicated for 2 h. (f) 3T3-L1 adipocytes were treated with 8-bromo-cAMP (8BrcAMP) for 2 h. (g) 3T3-L1 adipocytes were pretreated with the cAMP-dependent PKA inhibitor H-89 for 0.5 h and were then treated with isoproterenol (Isop, 10 μM) for 2 h. An equal volume (10 μl) of the culture medium (1 ml per well) was analyzed by immunoblotting. The protein expression of FVII in the medium (a, b, e, f and g) and cells (b) was visualized using Western blotting. Phosphorylated PKA (p-PKA) was used as a positive control, and β-actin was used as a loading control. Representative blots of secreted FVII in the medium [FVII (m)] and cellular FVII [FVII (lys)] are shown. (c) Secreted FVII in the culture medium were evaluated using murine FVII ELISA (n=3). *P<0.05 significantly different from time 0. (d) FVII mRNA expression was analyzed at different time points after the treatment with isoproterenol by quantitative real-time PCR (n=3). No significant difference was observed in FVII mRNA levels between the time points examined.
The cAMP/PKA signaling pathway was involved in the isoproterenol-induced secretion of FVII by 3T3-L1 adipocytes
We next investigated the involvement of the cAMP/PKA signaling pathway in the isoproterenol-induced secretion of FVII by adipocytes. Fully differentiated 3T3-L1 adipocytes were treated with a combination of isoproterenol and an inhibitor of cyclic guanosine monophosphate phosphodiesterase isobutyl-methyl-xanthine, thereby enhancing the concentration of endogenous cytosolic cAMP. As demonstrated in Figure 3e, isobutyl-methyl-xanthine amplified the isoproterenol-induced secretion of FVII by 3T3-L1 adipocytes. A treatment with an analog of cAMP, 8-bromo-cAMP stimulated the secretion of FVII by 3T3-L1 adipocytes in parallel with the increased phosphorylation of PKA (Figure 3f). A treatment with the cAMP-dependent PKA inhibitor H-89 canceled the isoproterenol-induced increase in the secretion of FVII (Figure 3g). Collectively, these results showed that the isoproterenol-induced secretion of FVII was mediated by the cAMP/PKA signaling pathway.
Effect of blocking secreted FVII induced by isoproterenol using the anti-FVII antibody on insulin signaling.
We investigated whether secreted FVII by the stimulation with isoproterenol affected insulin signaling in cells. Isoproterenol attenuated the insulin-stimulated phosphorylation of Akt (Figure 4). The phosphorylation of Akt was not increased by the blockade of secreted FVII with the anti-FVII antibody.
Effect of blocking the secretion of FVII induced by isoproterenol using an anti-FVII antibody on insulin signaling. Fully differentiated 3T3-L1 adipocytes were cultured in the presence of an anti-FVII antibody (1 μg ml–1) for 0.5 h before the addition of isoproterenol (Isop, 3 μM, 24 h; n=3). At the end of the treatment, insulin (5 nM) was added for 10 min. The protein expression of phospho-Akt (Ser 473) by cells was visualized using Western blotting. Total Akt was used as a loading control. Representative blots are shown.
Discussion
In the present study, we first showed that the mRNA expression levels of FVII in the adipose tissue of diet-induced obese mice were higher than those of lean control mice. Taken together with the findings of a previous study using obese db/db mutant mice,25 our results using wild-type mice reinforced FVII gene expression being increased in obese adipose tissue. We next determined whether adipocytes, which account for the vast majority of cells in adipose tissue secreted FVII using 3T3-L1 cells and demonstrated that adipocytes produces and secretes blood coagulation FVII. We further confirmed that the gene expression of FVII was induced in the early stage of adipocyte differentiation and this increase in expression was maintained to a late stage in mature adipocytes, which suggested that FVII may be an adipokine.
Adipose tissue is an active endocrine and paracrine organ that releases a large number of cytokines and bioactive mediators such as leptin, adiponectin, IL-6 and TNF-α, which influence not only body weight homeostasis, but also insulin resistance, diabetes, lipid levels, blood pressure, coagulation, fibrinolysis, inflammation and atherosclerosis.30 Obesity is associated with metabolically unfavorable changes in the expression of these adipokines: increased levels of TNF-α, IL-6, resistin, PAI-1 and leptin, and reduced levels of adiponectin. One important reason for the altered profiles of adipokines is adipose inflammation, which is characterized by the infiltration of immune cells into obese adipose tissue. Although adipocytes secrete TNF-α, infiltrated macrophages predominantly secrete TNF-α, thereby worsening adipose inflammation. Thus, TNF-α has been identified as a key cytokine that alters the metabolic function of adipocytes. For example, TNF-α was shown to reduce the production of adiponectin, but increased PAI-1 levels in adipocytes.29 Therefore, we speculated that TNF-α may have a role in the increased expression of FVII in adipose tissue. We herein demonstrated that TNF-α increased the expression of FVII in adipocytes through the MAPK–NF-κB pathway, which suggested that chronic inflammation may promote the secretion of FVII from adipocytes. Since plasma levels of FVII have been positively associated with obesity,5 adipose FVII may contribute, at least in part, to the increased levels of FVII observed with obesity. The degree to which adipocyte-derived FVII contributes to the systemic concentration of FVII needs to be validated.
In our study, obese adipose tissue expressed 55-fold higher levels of FVII mRNA than non-obese adipose tissue. Even though TNF-α is also known to stimulate an increase in the expression of FVII mRNA by 3T3-L1 adipocytes, our results revealed only a several-fold increase in the expression of FVII mRNA. One possibility is that infiltrated macrophages may also synthesize FVII because macrophages in atheroma have been shown to produce FVII.23 Another possibility is that the production of FVII in response to inflammatory stimuli may be higher in the isolated adipocytes of adipose tissue from obese mice or in vivo than in the cultured cell line used in the present study. Most of our studies have relied on cultured murine adipocytes; therefore, further investigations with other cell lines or in vivo studies are warranted.
Sympathetic nerve system (SNS) activation is a feature in the pathogenesis of obesity.1, 2, 3 Compared with subcutaneous fat, abdominal visceral fat is a prime adipose tissue depot that links obesity with elevated sympathetic nerve activity.31, 32 Anatomically, sympathetic nerves innervate adipose tissue.33, 34 Therefore, the increased activation of sympathetic nerves via β-adrenoceptors in adipocytes is critical for the regulation of lipid mobilization.35 Previous studies with sympathetic nerve denervation revealed that SNS regulated cell proliferation in adipocytes.36 Moreover, the chronic activation of β3-adrenoceptors was associated with the transformation of white fat to brown fat.37, 38 Thus, SNS has pivotal roles in adipocyte physiology. Therefore, we explored the effects of SNS activation on the secretion of FVII by adipocytes. In the present study, we showed that stimulating 3T3-L1 adipocytes with isoproterenol, an agonist of β-adrenergic receptor, increased the secretion of FVII. The activation of β-adrenergic receptors generally triggers adenylyl cyclase to release cAMP, as in adipocytes. The release of cAMP activates PKA, which, in turn, phosphorylates triglyceride lipase, hormone-sensitive lipase and perilipins in adipose tissue, ultimately resulting in the lipolysis of stored triglycerides. Our results indicate that the mechanism by which isoproterenol increases the secretion of FVII in adipocytes was mediated by the cAMP–PKA pathway, similar to the pathway for lipolysis.
When we compared the stimulations used on 3T3-L1 adipocytes, the mechanism underlying the secretion of FVII mediated by β-adrenergic receptor activation was found to be distinct from that by TNF-α. Moreover, the time-course and magnitude of the secretion were different between both stimulations; the secretion of FVII by the activation of β-adrenergic receptors was greater and faster than that by TNF-α. Regarding differences in the regulatory mechanisms of FVII, several studies indicated that the production of FVII was regulated by multiple mechanisms. For example, insulin has been shown to reduce the expression and secretion of FVII mRNA by hepatocytes through the transcription factor, C/EBP-β.39 Glucose deprivation in the culture medium results in an increase in the expression of FVII in hepatocytes by activating transcription factor 4.40 The extra-hepatic expression of FVII has been reported in addition to that in the liver. For example, some mammary cancer cell lines express FVII.24 FVII mRNA and protein were also detected in the macrophages and aortic smooth muscle cells of advanced atherosclerotic lesions.23 Collectively, these findings indicate that the expression of FVII may not be restricted to hepatocytes, it may also occur in extra-hepatic cells including adipocytes, and is regulated by multiple mechanisms.
Adipose tissue has been implicated in hemostasis, coagulation and fibrinolysis.41 Adipose tissue induces platelet activation through the secretion of adipokines such as leptin and adiponectin, and may contribute to hypercoagulation through the production of TF. The hypertrophic adipocytes observed in obesity produce and secrete PAI-1, which is the most important endogenous inhibitor of tissue plasminogen activator and urokinase-type plasminogen activator.42 PAI-1 inhibits fibrinolysis, thereby promoting blood coagulation. Our results suggest that adipocytes similarly increasing FVII and PAI-1 levels to facilitate blood coagulation. However, the activation of β-adrenergic receptors and other cAMP-elevating agents has been shown to suppress the production of PAI-1 in adipose tissue,43, 44 in contrast to the production of FVII. Thus, the effects of catecholamines on the secretion of PAI-1 may be incompatible with that of FVII.
FVII was previously shown to inhibit insulin signals in adipocytes,8 indicating that FVII secreted from adipocytes may exacerbate local insulin resistance in an autocrine manner. Therefore, we tested the direct effects of secreted FVII on insulin signaling in our adipocyte model by evaluating the phosphorylation of Akt when FVII secretion was blocked using an anti-FVII antibody. The results obtained showed that the inactivation of secreted FVII did not affect the phosphorylation of Akt. Isoproterenol apparently inhibited basal levels of phosphorylation; therefore, suppressive effect may have canceled the blocking effect of FVII. Badeanlou et al.8 demonstrated that exogenous FVIIa inhibited the phosphorylation of Akt in 3T3-L1 adipocytes at a concentration of 25 nM. In our experiments, the maximum concentration of secreted FVII was ~800 pg ml–1, which corresponded to 0.015 nM, suggesting that the concentration of secreted FVII in our model was too low to affect insulin signaling. Therefore, we cannot confirm the definite effects of FVII on local insulin resistance at this stage. In the future, the pathophysiological significance of adipocyte-derived FVII will be revealed by using other models, for example, adipocyte-specific FVII knock-out mice.
In summary, the results presented herein substantiate the expression of FVII being induced during adipocyte differentiation and maintained in mature adipocytes. The secretion of FVII from adipocytes was stimulated by either TNF-α or isoproterenol, which suggested that FVII in adipocytes could have a pivotal role in obesity (Figure 5). A clearer understanding of the mechanism underlying the production of FVII by adipocytes may lead to the amelioration of the deleterious aspects of obesity. Taken together, the present study provides the first evidence that FVII is an adipokine associated with coagulation, inflammation and obesity.
Schematic illustration of the expression and secretion of FVII in adipocytes. The expression of FVII is programmed during the differentiation of 3T3-L1 cells from fibroblasts to adipocytes. The expression of FVII is maintained in mature adipocytes. In obesity, infiltrated inflammatory cells such as macrophages (Mφ) predominantly secrete TNF-α. The results of the present study indicated that TNF-α induced the expression and secretion of FVII from adipocytes by affecting gene expression levels presumably via the MAPK and NF-κB pathways. On the other hand, the stimulation of β-adrenoceptors using isoproterenol rapidly induced the secretion of FVII via the cAMP–PKA pathway without affecting gene expression levels. FVII secreted by adipocytes may influence the pathogenesis of obesity because FVII acts locally to inhibit insulin signaling. Thus, FVII secreted by adipocytes may contribute to the higher concentrations of FVII observed with obesity.
References
Tentolouris N, Liatis S, Katsilambros N . Sympathetic system activity in obesity and metabolic syndrome. Ann NY Acad Sci 2006; 1083: 129–152.
Lambert GW, Straznicky NE, Lambert EA, Dixon JB, Schlaich MP . Sympathetic nervous activation in obesity and the metabolic syndrome—causes, consequences and therapeutic implications. Pharmacol Ther 2010; 126: 159–172.
Canale MP, Manca di Villahermosa S, Martino G, Rovella V, Noce A, De Lorenzo A et al. Obesity-related metabolic syndrome: mechanisms of sympathetic overactivity. Int J Endocrinol 2013; 2013: 865965.
Van Gaal LF, Mertens IL, De Block CE . Mechanisms linking obesity with cardiovascular disease. Nature 2006; 444: 875–880.
Mertens I, Van Gaal LF . Obesity, haemostasis and the fibrinolytic system. Obes Rev 2002; 3: 85–101.
Lorenzet R, Napoleone E, Cutrone A, Donati MB . Thrombosis and obesity: cellular bases. Thromb Res 2012; 129: 285–289.
Monroe DM, Key NS . The tissue factor-factor VIIa complex: procoagulant activity, regulation, and multitasking. J Thromb Haemost 2007; 5: 1097–1105.
Badeanlou L, Furlan-Freguia C, Yang G, Ruf W, Samad F . Tissue factor-protease-activated receptor 2 signaling promotes diet-induced obesity and adipose inflammation. Nat Med 2011; 17: 1490–1497.
Rosito GA, D'Agostino RB, Massaro J, Lipinska I, Mittleman MA, Sutherland P et al. Association between obesity and a prothrombotic state: the Framingham Offspring Study. Thromb Haemost 2004; 91: 683–689.
Godsland IF, Crook D, Proudler AJ, Stevenson JC . Hemostatic risk factors and insulin sensitivity, regional body fat distribution, and the metabolic syndrome. J Clin Endocrinol Metab 2005; 90: 190–197.
Marckmann P, Bladbjerg EM, Jespersen J . Diet and blood coagulation factor VII—a key protein in arterial thrombosis. Eur J Clin Nutr 1998; 52: 75–84.
Connelly JB, Roderick PJ, Cooper JA, Meade TW, Miller GJ . Positive association between self-reported fatty food consumption and factor VII coagulant activity, a risk factor for coronary heart disease, in 4246 middle-aged men. Thromb Haemost 1993; 70: 250–252.
Folsom AR, Qamhieh HT, Wing RR, Jeffery RW, Stinson VL, Kuller LH et al. Impact of weight loss on plasminogen activator inhibitor (PAI-1), factor VII, and other hemostatic factors in moderately overweight adults. Arterioscler Thromb Vasc Biol 1993; 13: 162–169.
Kopp CW, Kopp HP, Steiner S, Kriwanek S, Krzyzanowska K, Bartok A et al. Weight loss reduces tissue factor in morbidly obese patients. Obes Res 2003; 11: 950–956.
Lijnen HR, Van Hul M, Hemmeryckx B . Caloric restriction improves coagulation and inflammation profile in obese mice. Thromb Res 2012; 129: 74–79.
Krysiak R, Gdula-Dymek A, Bachowski R, Okopien B . Pleiotropic effects of atorvastatin and fenofibrate in metabolic syndrome and different types of pre-diabetes. Diabetes Care 2010; 33: 2266–2270.
Dalaker K, Skartlien AH, Prydz H . A new form of coagulation factor VII in plasma. Scand J Haematol 1986; 36: 430–438.
Ceriello A . The post-prandial state and cardiovascular disease: relevance to diabetes mellitus. Diabetes Metab Res Rev 2000; 16: 125–132.
Carr ME . Diabetes mellitus: a hypercoagulable state. J Diabetes Complications 2001; 15: 44–54.
Boden G, Vaidyula VR, Homko C, Cheung P, Rao AK . Circulating tissue factor procoagulant activity and thrombin generation in patients with type 2 diabetes: effects of insulin and glucose. J Clin Endocrinol Metab 2007; 92: 4352–4358.
Rao AK, Chouhan V, Chen X, Sun L, Boden G . Activation of the tissue factor pathway of blood coagulation during prolonged hyperglycemia in young healthy men. Diabetes 1999; 48: 1156–1161.
Kario K, Miyata T, Sakata T, Matsuo T, Kato H . Fluorogenic assay of activated factor VII. Plasma factor VIIa levels in relation to arterial cardiovascular diseases in Japanese. Arterioscler Thromb Vasc Biol 1994; 14: 265–274.
Wilcox JN . Extrahepatic synthesis of factorhuman atherosclerotic vessels VII in human atherosclerotic vessels. Arterioscler Thromb Vasc Biol 2002; 23: 136–141.
Koizume S, Yokota N, Miyagi E, Hirahara F, Nakamura Y, Sakuma Y et al. Hepatocyte nuclear factor-4-independent synthesis of coagulation factor VII in breast cancer cells and its inhibition by targeting selective histone acetyltransferases. Mol Cancer Res 2009; 7: 1928–1936.
Mihara M, Aihara K, Ikeda Y, Yoshida S, Kinouchi M, Kurahashi K et al. Inhibition of thrombin action ameliorates insulin resistance in type 2 diabetic db/db mice. Endocrinology 2010; 151: 513–519.
Chen H, Charlat O, Tartaglia LA, Woolf EA, Weng X, Ellis SJ et al. Evidence that the diabetes gene encodes the leptin receptor: identification of a mutation in the leptin receptor gene in db/db mice. Cell 1996; 84: 491–495.
Takahashi N, Yoshizaki T, Hiranaka N, Suzuki T, Yui T, Akanuma M et al. Suppression of lipin-1 expression increases monocyte chemoattractant protein-1 expression in 3T3-L1 adipocytes. Biochem Biophys Res Commun 2011; 415: 200–205.
Lefterova MI, Lazar MA . New developments in adipogenesis. Trends Endocrinol Metab 2009; 20: 107–114.
Cawthorn WP, Sethi JK . TNF-alpha and adipocyte biology. FEBS Lett 2008; 582: 117–131.
Lau DC, Dhillon B, Yan H, Szmitko PE, Verma S . Adipokines: molecular links between obesity and atheroslcerosis. Am J Physiol Heart Circ Physiol 2005; 288: H2031–H2041.
Alvarez GE . Sympathetic neural activation in visceral obesity. Circulation 2002; 106: 2533–2536.
Grassi G, Dell’Oro R, Facchini A, Quarti Trevano F, Bolla GB, Mancia G . Effect of central and peripheral body fat distribution on sympathetic and baroreflex function in obese normotensives. J Hypertens 2004; 22: 2363–2369.
Youngstrom TG, Bartness TJ . Catecholaminergic innervation of white adipose tissue in Siberian hamsters. Am J Physiol 1995; 268: R744–R751.
Bartness TJ, Song CK . Thematic review series: adipocyte biology. Sympathetic and sensory innervation of white adipose tissue. J Lipid Res 2007; 48: 1655–1672.
Bartness TJ, Shrestha YB, Vaughan CH, Schwartz GJ, Song CK . Sensory and sympathetic nervous system control of white adipose tissue lipolysis. Mol Cell Endocrinol 2010; 318: 34–43.
Foster MT, Bartness TJ . Sympathetic but not sensory denervation stimulates white adipocyte proliferation. Am J Physiol Regul Integr Comp Physiol 2006; 291: R1630–R1637.
Himms-Hagen J, Melnyk A, Zingaretti MC, Ceresi E, Barbatelli G, Cinti S . Multilocular fat cells in WAT of CL-316243-treated rats derive directly from white adipocytes. Am J Physiol Cell Physiol 2000; 279: C670–C681.
Jimenez M, Barbatelli G, Allevi R, Cinti S, Seydoux J, Giacobino J-P et al. β3-Adrenoceptor knockout in C57BL/6J mice depresses the occurrence of brown adipocytes in white fat. Eur J Biochem 2003; 270: 699–705.
Jackson AA, Cronin KR, Zachariah R, Carew JA . CCAAT/enhancer-binding protein-beta participates in insulin-responsive expression of the factor VII gene. J Biol Chem 2007; 282: 31156–31165.
Cronin KR, Mangan TP, Carew JA . Upregulation of the coagulation factor VII gene during glucose deprivation is mediated by activating transcription factor 4. PLoS One 2012; 7: e40994.
Faber DR, de Groot PG, Visseren FL . Role of adipose tissue in haemostasis, coagulation and fibrinolysis. Obes Rev 2009; 10: 554–563.
Skurk T, Hauner H . Obesity and impaired fibrinolysis: role of adipose production of plasminogen activator inhibitor-1. Int J Obes Relat Metab Disord 2004; 28: 1357–1364.
Halleux CM, Declerck PJ, Tran SL, Detry R, Brichard SM . Hormonal control of plasminogen activator inhibitor-1 gene expression and production in human adipose tissue: stimulation by glucocorticoids and inhibition by catecholamines. J Clin Endocrinol Metab 1999; 84: 4097–4105.
Gottschling-Zeller H, Aprath I, Skurk T, Hauner H . Beta-Adrenoceptor agonists and other cAMP elevating agents suppress PAI-1 production of human adipocytes in primary culture. Horm Metab Res 2000; 32: 509–514.
Acknowledgements
We thank the members of the Department of Biochemistry, School of Dentistry, Health Sciences University of Hokkaido for the use of laboratory equipment. This work was supported in part by JSPS KAKENHI Grant Numbers 25460696, 23590684 (to NT and MI).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
OK and TS are employees in Sysmex Corporation.
Rights and permissions
About this article
Cite this article
Takahashi, N., Yoshizaki, T., Hiranaka, N. et al. The production of coagulation factor VII by adipocytes is enhanced by tumor necrosis factor-α or isoproterenol. Int J Obes 39, 747–754 (2015). https://doi.org/10.1038/ijo.2014.208
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2014.208
- Springer Nature Limited
This article is cited by
-
Generation of fully functional hepatocyte-like organoids from human induced pluripotent stem cells mixed with Endothelial Cells
Scientific Reports (2019)
-
Sarcolipin expression is repressed by endoplasmic reticulum stress in C2C12 myotubes
Journal of Physiology and Biochemistry (2017)
-
Plasma markers of inflammation and hemostatic and endothelial activity in naturally overweight and obese dogs
BMC Veterinary Research (2016)