Abstract
The importance of secretory IgA in controlling the microbiota is well known, yet how the antibody affects the perception of the commensals by the local immune system is still poorly defined. We have previously shown that the transport of secretory IgA in complex with bacteria across intestinal microfold cells results in an association with dendritic cells in Peyer’s patches. However, the consequences of such an interaction on dendritic cell conditioning have not been elucidated. In this study, we analyzed the impact of the commensal Lactobacillus rhamnosus, alone or associated with secretory IgA, on the responsiveness of dendritic cells freshly recovered from mouse Peyer’s patches, mesenteric lymph nodes, and spleen. Lactobacillus rhamnosus-conditioned mucosal dendritic cells are characterized by increased expression of Toll-like receptor regulatory proteins [including single immunoglobulin interleukin-1 receptor-related molecule, suppressor of cytokine signaling 1, and Toll-interacting molecule] and retinaldehyde dehydrogenase 2, low surface expression of co-stimulatory markers, high anti- versus pro-inflammatory cytokine production ratios, and induction of T regulatory cells with suppressive function. Association with secretory IgA enhanced the anti-inflammatory/regulatory Lactobacillus rhamnosus-induced conditioning of mucosal dendritic cells, particularly in Peyer’s patches. At the systemic level, activation of splenic dendritic cells exposed to Lactobacillus rhamnosus was partially dampened upon association with secretory IgA. These data suggest that secretory IgA, through coating of commensal bacteria, contributes to the conditioning of mucosal dendritic cells toward tolerogenic profiles essential for the maintenance of intestinal homeostasis.
Similar content being viewed by others
Introduction
The mucosal surface of the gastrointestinal tract is in constant interaction with the luminal microenvironment, which contains ever-changing commensal microbiota, as well as a variety of bacterial, viral and protozoan pathogens. In this highly anti-genic environment, the mucosal immune system must remain hyporesponsive (tolerant) to food antigens, self-antigens and commensal bacteria, while initiating protective responses to pathogens to prevent periodic host infection. In contrast to the systemic compartment, which needs to remain sterile, mucosal surfaces are capable of coping with various challenges while preserving homeostasis. Symbiotic control of the microbiota by the intestinal immune system relies on the modulation of dendritic cells (DCs) and T cells by intrinsic characteristics associated with microbial-associated molecular patterns.1, 2, 3, 4 Moreover, beyond contributing to host defense against intestinal pathogens, secretory IgA (SIgA) governs the quantitative and qualitative control of the commensal microbiota composition and prevents systemic dissemination.5, 6, 7, 8
SIgA is the most abundant antibody molecule on the mucosal surfaces of humans and most other mammals.9, 10 While other isotypes are rapidly degraded, intact SIgA molecules have been regularly demonstrated in samples from mucosal surfaces, even in the presence oflarge numbers ofmicroorganisms. The stabilityof SIgA depends largely on its secretory component, which is covalently bonded to Fcα and masks potential proteolytic cleavage sites in this region.11 These properties make SIgA particularly well suited to operate with preserved functionality in the enzymatically hostile environment that prevails on gut mucosal surfaces. Furthermore, the presence of SIgA at mucosal surfaces requires that pro-inflammatory processes are kept under control, a feature that is essential to the maintenance of the integrity and functionality of the epithelial barrier.10, 12, 13
We have previously demonstrated that commensal or pathogenic bacteria in complex with SIgA in the lumen are targeted to underlying DCs in the subepithelial dome region of Peyer’s patches (PP),14 but do not interact with lamina propria DCs. This result most likely indicates that this pathway is important to ensure appropriate communication between the luminal contents and the associated immune system. The transport of SIgA-based immune complexes across microfold (M) cells in PPs and capture by local CD11c+CD11b+MHCII+DCs in the subepithelial dome region15, 16 suggests that this process is the primary pathway by which commensal bacteria are exposed to these antigen-presenting cells. DCs in the intestinal lamina propria and MLNs exhibit tightly regulated expression of surface markers that contribute to the induction of Foxp3+T regulatory (Treg) cells17, 18 and the production of IL-10 and TGF-β under the influence of constitutive environmental signals,19 including interaction with commensal bacteria.20 The association of SIgA with bacteria may therefore have an impact on the conditioning of PP and MLN DCs, but this has, to our knowledge, never been investigated.
To examine this hypothesis, we exposed DCs freshly isolated from mouse mucosal PPs and MLNs, or from the spleen, to the commensal-representative bacterium Lactobacillus rhamnosus (LPR), alone or in complex with SIgA (SIgA-LPR). Comparison of DC responsiveness with respect to several immunologic markers relevant to the mechanistic dissection ofDC conditioning toward a tolerogenic profile was investigated. The results support the concept that the tissue from which DCs are isolated is important in the regulation of immune patterns involved in commensal bacteria sensing, and also reveal the so far unknown contribution of SIgA to the process of DC conditioning at both the mucosal and systemic level.
Materials and methods
Mice
Female BALB/c mice (Jackson Laboratory)with conventional microbiota were purchased from Charles River France (L’Arbresle, France). DO11.10 TCR transgenic mice21 were used as a source of naïve OVA-specific T cells. Female C57BL/ 6 mice (Jackson Laboratory) were used as a source of splenocytes for a mixed lymphocyte reaction assay. Mice were housed in the animal facility of the Centre Hospitalier Universitaire Vaudois under conventional conditions prior to use at the age of 6-8 weeks. All experiments were performed upon approval of the State of Vaud Veterinary Office.
Source of SIgA
Culture supernatants of the mouse hybridoma cell clone IgAC5, specific for Shigella flexneri serotype 5a LPS, grown at 37 °C in RPMI-1640 medium complemented with 10% fetal calf serum were used as a source of IgA.22 To reconstitute SIgA, equimolar amounts of purified polymeric IgAC5 mAb and recombinant mouse secretory component were combined as described.22
Bacteria
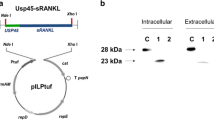
The commensal strain Lactobacillus rhamnosus (LPR) CGMCC 1.3724 was cultured according to a previously published protocol.23 Washed bacteria were resuspended at a concentration of 1 × 108 CFU/ml. Pure bacterial cultures or bacterial cultures associated with 0.5 μg of reconstituted SIgA at room temperature for 1 h16 were then incubated with DCs isolated from various tissues. For SIgA-LPR complex observations (Figure 1a), SIgA were labeled with indocyanin-3 as previously reported,15 and the formation of complex between LPR and SIgA-Cy3 was verified using a Zeiss LSM 710 Meta confocal microscope (Carl Zeiss, Jena, Germany). Images were captured with a 63X objective and processed using ZEN 2009 light edition (Zeiss).
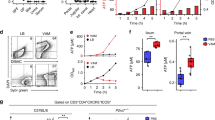
Visualization of SIgA-LPR complexes and DC gating strategy. (a) Observation of association of LPR with SIgAC5-Cy3 by laser-scanning confocal microscopy (see Materials and Methods); bacteria are visualized by differential interference contrast or by co-localization with SIgAC5-Cy3 as a merged picture. Bars: 5 μm. (b) DC phenotyping (see Materials and Methods). Gating strategy used for the identification of the CD11c+CD11b+MHCII+ F4/80−CD8− DC subtype used in the study. DCs were detected following the exclusion of dead cells, selection for F4/ 80-negative and CD8-negative cells, and then positively selected for CD11b, CD11c and MHCII surface markers. Plots are from one experiment and are representative of at least four independent experiments.
MACS isolation of PP, MLN and splenic DCs and naïve CD4+CD62L+CD25− T cells
For preparation of tissue-derived DCs, the procedure of Kadaoui and Corthésy15 was followed. The resulting purity of CD11c+ DCs (referred to as totDCs hereafter) was 90–95%.
Naïve CD4+CD62L+CD25− T cells from DO11.10 mice were isolated from spleen (processed as above) using a CD4+CD62L+ T cell isolation kit II (Miltenyi Biote) supplemented with biotinylated anti-CD25 mAb; a purity of 90–95% was achieved.24
Conditioning of totDCs from PPs, MLNs and the spleen
DCs isolated by magnetic cell sorting from various tissues were cultured in plain medium serving as a control or conditioned ex vivo with LPR alone (ratio of 2 bacteria per DC, based on titration experiments25), LPR in complex with SIgA, SIgA alone, or challenged with 2 μg ml−1 E. coli LPS (E. coli, 055: B5; Calbiochem) overnight in 100 μl of DMEM complemented with 5% fetal calf serum, 50 μM β-mercaptoethanol, 1 mM Na-pyruvate, 10 mM Hepes (pH 7.3) at 37 °C in a humidified 5% CO2 atmosphere.
Phenotyping of conditioned DCs
Overnight conditioned DCs were washed twice in PBS containing 1% fetal calfserum and incubated in the same solution with blocking rat anti-mouse CD16/32 mAbs (BD Biosciences) for 20 min at 4 °C. DCs were then labeled with appropriate combinations of mAbs specific for CD11c (APC-conjugated), CD11b (PE-Cy7-conjugated), MHC-II (PE-conjugated), F4/80 (PerCP-Cy5.5-conjugated), CD8 (Pacific Blue-conjugated), CD40 (FITC-conjugated), CD80 (FITC-conjugated), CD86 (FITC)-conjugated), or isotype controls (BD Biosciences, Allschwil, Switzerland) for 30 min at 4 °C. Cells were washed and re-suspended in PBS-1% FCS prior to analysis using a LSR II flow cytometer (BD Biosciences) and FlowJo software (Tree Star, Ashland, OR, USA). After initial gating on side and forward scatters, dead cells (propidium iodide staining), F4/80-positive and CD8-positive cells were excluded. Positive selection for CD11c, CD11b and MHCII was then carried, resulting in the isolation of CD11c+CD11b+MHCII+F4/80−CD8− DCs (Figure 1b). An analysis of CD40, CD80 and CD86 surface markers was performed on this particular phenotype with relative changes in expression displayed as the ratio between experimental levels and DCs kept in plain medium (CTRL in figures).
Real time RT-PCR
PPs, MLNs and splenic (plain or conditioned) CD11c+ CD11b+MHCII+F4/80−CD8−DCs were sorted using a FACS Aria II cell sorter (BD Biosciences), following the gating strategy given above. Total RNA was isolated using a Qiagen RNeasy Mini Kit and cDNA was generated with the Superscript First-Strand Synthesis System for RT-PCR and random hexamer primers (Invitrogen) according to the manufacturer’s protocols. Two microliters of the reverse transcription reaction containing cDNA was used as a template for quantitative real-time PCR using SYBR Green Master Mix (Roche Applied Science), and gene-specific primers. Sequences of the sense and anti-sense primers were as follows: retinaldehyde dehydrogenase 1 (Aldh1a1), 5′ -ATGGTTTAGCAGCAGGACTCTTC-3′ and 5′-CCAGACATCTTGAATCCACCGAA-3′26; retinaldehyde dehydrogenase 2 (Aldh1a2), 5′-GACTTGTAGCAGCTG TCTTCACT-3′ and 5′ -CACCCATTTCTCTCCCATTTCC-3′ 26; single immunoglobulin interleukin-1 receptor-related molecule (Sigirr), 5′-GTGGCTGAAAGATGGTCTGGCAT TG-3′ and 5′-CA GGTGAAGGTTCCATAGTCCTCTGC-3′ 27; suppressor of cytokine signaling 1 (Socs1), 5′-CTGCGGCTTCTATTGGGGAC-3′ and 5′ -AAAAGGCAGTCGAAGGTCTCG-3′28; Toll-interacting molecule (Tollip), 5′-TTGGCTATGTGCCCATTGC-3′ and 5′-AG CTTTGAGGTCCTCTTCATTACAG-3 ′29; glyceraldehyde-3-phosphate dehydrogenase (Gapdh), 5′-CCAGGTTGTCTCCTGCGAC-3′ and 5′-CCTGTTGCTGTAGCCGTATTCA-3′. PCRs and analyses were performed using a ABI Prism sequence detection system 7500 (PE Applied Biosystems). PCR conditions were as follows. Tdenaturation: 95 °C, 15 s; Tannealing and extension: 60 °C, 1 min; 40 cycles. Gene expression was calculated relative to Gapdh. The comparative CT method (ΔCT,30), where CT represents the cycle number where the SYBR green fluorescence crossed the threshold value set at 0.2, was used to assess relative changes in mRNA levels between samples.
Cytokine/chemokine secretion by DCs from PPs, MLNs and the spleen
Isolated PP-, MLN- or spleen-derived CD11c+ DCs (1 × 105 cells) were conditioned or stimulated as indicated above in a final volume of 200 μl. Insufficient DCs from the CD11c+ CD11b+MHCII+F4/80−CD8−subset could be sorted from PPs for this particular analysis, so we had to compare total MACS-isolated CD11c+ DCs (referred to as totDCs) from each tissue. Production of IL-12p70, KC, TNF-α, IL-6, and IL-10 by conditioned/activated totDCs was measured in supernatants collected after overnight incubation using Multiplex array technology according to the manufacturer's instructions (Life Technologies, Zug, Switzerland) in a BioPlex 200 instrument (Bio-Rad Laboratories, Reinach, Switzerland). Due to particular sample preparation prior to analysis, TGF-β was measured by a sandwich ELISA following the procedure provided by the supplier (R&D Systems, Abingdon, UK). Cytokine and chemokine levels are expressed as pg/ml (Table 1).
Stimulation of T lymphocytes
Following overnight conditioning with LPR alone, SIgA-LPR or LPS, sorted PP and MLN, and splenic CD11c+CD11b+ MHCII+F4/80−CD8−DCs (2.5 × 104) were loaded with the OVA 323-339 peptide (2 μg ml−1), followed by incubation with freshly isolated naïve CD4+CD62L+CD25− T cells (2.5 × 105) from transgenic DO11.10 mice for 72 h. No other stimulus was provided to the co-cultures. 3H-thymidine (0.5 μCi) was added to each culture for the last 18 h of the incubation period. The cells were then harvested on glass fiber filters on a PHD cell harvester (Cambridge Technology, Watertown, MA) and proliferation was assessed as the amount of the incorporation of 3H-thymidine into cell DNA, as measured by β-scintillation counting of the harvested samples. Stimulation indices were measured relative to the CTRL set arbitrarily at 1.0. Conversion of naïve CD4+CD62L+CD25− T cells into Treg cells was assessed after 72 h of incubation: cells were stained with anti-CD25 and -CD4 mAbs (BD Biosciences), whereas intracellular Foxp3 expression was evaluated by using an anti-mouse Foxp3 staining kit (eBioscience, San Diego, CA). The percentages of converted CD4+ CD25+ Foxp3+ Tregs were determined on an identical number (25 000) of CD4+ T cells for each experimental condition. In neutralizing experiments, mAbs against mouse IL-10 (JESS-16E3, BD Biosciences) or TGF-β (1D11.16.8, BioXcell, West Lebanon, NH) or IgG isotype controls were added to the DC-T cell cultures at a final concentration of 5 μg ml−1.
Suppression assay
The suppressive capacity of converted Tregs was assessed with a mixed lymphocyte reaction (MLR) assay. Spleens were harvested from BALB/c or C57Bl/6 mice and a single-cell suspension was prepared. After lysis of red blood cells with 155 mM NH4Cl-10 mM KHCO3 lysis buffer (Sigma-Aldrich), cells were washed with PBS, re-suspended in complete medium and tested for viability. Then, 1 × 105 responder cells from BALB/c mice were co-cultured with 1 × 105 irradiated (3000 rads) stimulator cells from C57BL/6 mice in a 96-well round-bottom plate together with different numbers of sorted CD4+CD25+ T cells from DC cultures previously incubated with SIgA-LPR or LPR in a total volume of 200 μl well−1. Expression of Foxp3 by DC-converted CD4+ CD25+ Treg cells was confirmed by flow cytometry. After 3 days of culture, cells were pulsed with 1 μCi of 3H-thymidine for 18 h. Cells were harvested and 3H-thymidine incorporation was measured by β-scintillation counting.
Statistical analysis
The significance of the data were evaluated by nonparametric one-way ANOVA with Bonferroni's multiple comparison test or a paired t-test. The results are depicted as the mean±s.d. of n determinations. Differences were considered to be significant when P values<0.05. Graph generation and statistical analyses were performed using GraphPad Prism software version 6.
Results
Pattern of expression of TLR regulatory proteins in mucosal and splenic conditioned DCs
In steady-state, although intestinal DCs express less TLR2 and TLR4 than their splenic counterparts,31, 32 this expression pattern does not satisfactorily explain how the gut mucosal surface discriminates between symbiotic and pathogenic bacteria.33 We hypothesized that differential expression of TLR regulatory proteins (SIGIRR, Tollip and SOCS1) in mucosal and splenic CD11c+CD11b+MHCII+F4/80−CD8− DCs (Figure 1b) following conditioning with LPR or SIgA-LPR may serve as a mechanism to restrict intestinal DC overreaction. SIGIRR, a protein located at the plasma membrane of immature DCs, sequesters adaptor proteins and prevents signaling via TLR4.34 Tollip is an adaptor molecule that binds TLR2 and TLR4 to inhibit MyD88-mediated activation and blocks IL-1 receptor associated kinases (IRAKs) function in the TLR pathway.35 Finally, SOCS1 acts by suppressing cytokine signaling and serves as a negative regulator ofTLR4 and 9 signaling upon targeting of IRAK1.36 As examined by qRT-PCR in sorted CD11c+CD11b+MHCII+F4/80−CD8− DCs, incubation with LPR alone significantly upregulated mRNA expression in DCs isolated from PPs and MLNs, but no effect could be detected on splenic DCs (Figures 2a and c). Because the commensal bacterium LPR in complex with SIgA was shown to associate in vivo with the CD11c+ CD11b+ MHCII+ DC subtype in PPs,16 we sought to examine whether such an interaction can further modulate the expression of TLR regulatory proteins in DCs isolated from PPs, MLNs and spleen. The association of SIgA with LPR did increase the expression of the three tested genes in a statistically significant manner only in PPs. SIgA per se, or LPS serving as an indicator of cell fitness and responsiveness post-isolation, had no significant effect. These results indicate that conditioning of mucosal DCs with LPR, and as identified here with SIgA-LPR complexes in PPs, upregulates the expression of molecules that dampen TLR signaling.
Analysis by real-time RT-PCR of the expression of TLR regulatory proteins Sigirr (a), Tollip (b), Socs1 (c), and of the vitamin A metabolizing enzymes Raldh2 (d) and Raldh1 (e) by conditioned, FACS-sorted PP-, MLN- and spleen-derived CD11c+CD11b+MHCII + F4/80−CD8− DCs. All RNA samples were isolated from two independent groups of four animals and analyzed in triplicates. For all gene products tested, the relative expression level was normalized to Gapdh RNA with the control (CTRL) set at 1. Data pooled from the two groups are shown as the mean±s.d. The significance of the data were evaluated by nonparametric one-way ANOVA with Bonferroni's multiple comparison test (a) or paired t-test (b). ''a'' indicates comparison with CTRL and ''b'' indicates comparison between LPR-conditioned DCs and SIgA-LPR-conditioned DCs *, P values < 0.01; **, P values < 0.005.
Pattern of expression of vitamin A metabolizing enzymes in mucosal and splenic conditioned DCs
The differential expression of RALDH enzymes by mucosal tissues compared with spleen and peripheral lymph nodes suggests that these enzymes are important for the topical production of retinoic acid and the induction of DCs with a tolerogenic phenotype.37 We therefore examined whether cellular proteins known to intervene in the differentiation of mucosal tolerogenic DCs could be regulated via exposure to LPR or SIgA-LPR complexes. Incubation with LPR induced higher expression of Raldh2 mRNA in PPs than in splenic DCs (Figure 2d). Consistent with the presence of commensal-SIgA immune complexes in PPs, SIgA bound to LPR further promoted the expression of Raldh2 mRNA in DCs isolated from this tissue but not in DCs recovered from draining MLNs or spleen. No change in the level of expression of Raldh1 mRNA was observed in either mucosa-derived or in splenic DCs (Figure 2e), arguing for a specific effect observed in the induction of the Raldh2 gene. In comparison with the control, stimulation with LPS did not change the level of RNA expression for the two forms of RALDH tested (Figures 2d and e). This leads us to conclude that the sensing of the SIgA-LPR complex by PP DCs increases the expression of an enzyme instrumental to the production of retinoic acid involved in local immune regulation, particularly at the mucosal level.
Pattern of surface activation markers on mucosal and splenic conditioned DCs
Given the observation that TLR regulatory proteins and RALDH2 are upregulated in mucosal D11c+CD11b+MHCII+ F4/80−CD8− DCs, we next sought to determine whether conditioning with LPR- and SIgA-LPR modulates surface expression of the activation markers CD40, CD80 and CD86, the basal level of expression of which is depicted in Figure 3, upper left panel. In comparison with co-incubation with LPS, which induced strong co-stimulatory marker upregulation, no increase in the surface expression of either marker was detected in PP and MLN DCs exposed to LPR, SIgA-LPR or SIgA (Figure 3), which is indicative of a tolerogenic phenotype.38 By contrast, incubation of LPR alone with spleen-derived DCs showed an increased expression of CD40, CD80 and CD86 compared with control cells, although to a lower extent than that induced by LPS. This result indicates that tissue origin leads to a different degree of DC activation with respect to commensal bacteria, with modulation by SIgA occurring for splenic DCs only.
Expression of surface activation markers of conditioned, gated CD11c+CD11b+MHCII+ F4/80−CD8−DCs from mouse PPs, MLNs and the spleen. Upper left panel shows background level of expression of CD40, CD80 and CD86. Panels CD40, CD80 and CD86 show changes in expression of the three activation markers post-DC conditioning calculated as a function of the control (CTRL) arbitrarily fixed at 1 and plotted as fold increases. All DC samples were isolated from 3 independent groups of 4 animals and analyzed in triplicate. Data pooled from the three groups are depicted as the mean±s.d. The significance of the data were evaluated by nonparametric one-way ANOVA with Bonferroni's multiple comparison test compared with CTRL.*, P values < 0.05; **, P values < 0.01.
Pattern of cytokine/chemokine secretion by conditioned mucosal and splenic DCs
We then sought to examine how the incubation of LPR alone or in complex with SIgA, or controls, with DCs, affected their release of pro-inflammatory (IL12p70, KC, TNF-α, IL-6) and anti-inflammatory (IL-10, and TGF-β) cytokines. Because an insufficient quantity of DCs from the CD11c+CD11b+MHCII+F4/80−CD8−subset were sorted from PPs to then allow measurable amounts of cytokines post-incubation with diverse stimuli, we had to rely on cytokine production from the conditioning of total MACS-isolated CD11c+ DCs (referred to as totDCs in the next two paragraphs) from each tissue. LPR had no significant effect on IL-12p70, KC and TNF-α production by PP and MLN totDCs (Table 1), whereas LPR stimulated secretion by spleen totDCs (P=0.01). Association with SIgA significantly decreased LPR-induced production of the three cytokines in splenic totDCs only (P=0.008). Exposure of PP, MLN and splenic totDCs to LPR moderately increased IL-6 production (0.02⩽P⩽0.006). A down-regulating effect mediated by SIgA was observed in splenic totDCs only (P=0.01). Overall, these results show that the pattern of secretion of the pro-inflammatory cytokines IL-12p70, KC, TNF-α, but not IL-6, is associated with a poor responsive state of mucosal DCs to LPR and SIgA-LPR. By contrast, SIgA dampens the effect of bacterial exposure in the case of splenic DCs, as was observed for activation markers (Figure 3). Consistent with its activating properties, SIgA elevated a response to LPS that could be observed in totDCs recovered from all the tissues (0.008⩽P⩽0.001).
We observed that IL-10 production was upregulated by LPR in totDCs from PPs (P=0.01), MLNs (P=0.008) and spleen (P=0.03; Table 1). The association of LPR with SIgA increased IL-10 production in PP totDCs only (P=0.01). Incubation with LPS triggered IL-10 production in all three tissues (P=0.03). TGF-β production in PP totDCs was stimulated in the presence of LPR (P=0.03) and further increased upon association with SIgA (P=0.02). No enhancement of TGF-β production upon incubation with LPR alone was observed in MLN and splenic totDCs, whereas association with SIgA had a positive effect in PPs and MLN (P=0.03; Table 1, sixth column). TGF-β was diminished in comparison with the control in all tissues after exposure to LPS (P⩽0.01). Differential fine-tuning of the cytokine profile supports the notion that SIgA in association with LPR acts as a partner to further modulate DCs toward a more anti-inflammatory pattern.
Capacity of mucosal and splenic conditioned DCs to induce T cell proliferation and Treg development
Based on the above observation that mucosal and splenic DCs exposed to various stimuli display different properties (Figure 2, Figure 3 and Table 1), we next investigated whether this translated into different functional features. We first analyzed the ability of conditioned and sorted CD11c+CD11b+ MHCII+F4/80−CD8− DCs recovered from mucosal PPs and MLN, as well as from the spleen for the systemic environment, to induce the proliferation of isolated naïve antigen-specific CD4+CD62L+CD25− T cells using the OVA-specific DO11.10 system. LPS-primed OVA peptide-loaded DCs isolated from mucosal tissues and spleen strongly induced the proliferation of DO11.10 CD4+CD62L+CD25−T cells, whereas conditioning of the OVA peptide-loaded PP and MLN DCs with LPR or SIgA-LPR not only failed to stimulate such cells but also triggered hyporesponsiveness of T cells compared with the control (Figures 4a and b). Consistent with the pattern of surface markers and secreted cytokines (Figure 3 and Table 1), splenic DCs moderately activated T cells after conditioning with LPR. T cell activation was significantly reduced when in complex with SIgA (Figure 4c).
Proliferative responses of purified naïve DO11.10 CD4+CD62L+CD25− T cells incubated in the presence of conditioned, FACS-sorted CD11c+CD11b+MHCII+ F4/80−CD8−DCs pulsed with the OVA 323-339 peptide. DCs were isolated from PPs (a), from MLNs (b) and from the spleen (c). The results are presented as stimulation indices, with control (CTRL) serving as the reference and show means±s.d. of one representative experiment performed 2-3 times with cells isolated from 4 animals. The significance of the data were evaluated by nonparametric one-way ANOVA with Bonferroni's multiple comparison test compared with CTRL. *P values < 0.05; **P values < 0.01.
Development of Treg cells post-incubation with conditioned DCs for 72 h was examined next. A marked conversion of naïve DO11.10 CD4+CD62L+CD25−T cells into CD4+CD25+ Foxp3+Treg cells was observed upon analysis of an equal amount of CD4+T cells following incubation with PP- and MLN-derived LPR-conditioned CD11c+CD11b+MHCII+ F4/80−CD8−DCs compared with control (Figures 5a and b). SIgA in association with LPR further increased this differentiation into Treg cells. LPS-treated DCs yielded lower Treg cell conversion compared with control (Figures 5a and b). Incubation of DCs and T cells in the presence of neutralizing mAbs specific for TGF-β or IL-10 led to a statistically significant reduction in the expansion of Treg cells, which is in agreement with the role of these cytokines in the generation of Treg cells.19 At the systemic level, no Treg cells were generated above background when spleen-derived DCs were conditioned by LPR or SIgA-LPR (Figure 5c), reflecting the more pro-inflammatory cytokine pattern displayed by such DCs, which is presumably not counteracted by IL-10 and TGF-β. Finally, we confirmed the actual regulatory function of Treg lymphocytes by assessing their ability to suppress the proliferation of effector cells using the MLR assay. The addition of mucosal DC-converted Tregs in increasing amounts to a constant amount of responder cells yielded a progressive reduction in proliferation, as reflected by lower 3H-thymidine incorporation (Figure 5d). The sum of these data shows, at the functional level, that in addition to differences linked to tissue origin, the presence of SIgA is essential in driving the homeostatic perception of commensal bacteria by DCs, as exemplified by their differential capacity to affect antigen-specific T cell proliferation and to generate antigen-specific Treg cells with suppressive function.
Generation of functional CD4+CD25+Foxp3+Treg cells after co-culture of purified naïve DO11.10 CD4+CD62L+CD25− T cells with conditioned, FACS-sorted, CD11c+CD11b+MHCII+ F4/80−CD8−DCs pulsed with the OVA 323-339 peptide. Conversion of naïve DO11.10 CD4+CD62L+CD25− T cells into Treg cells after incubation in the presence of PP-derived DCs (a) as such and in the presence of TGF-β or IL-10 neutralizing mAbs. (b) Same experiment as in (a), with co-cultures performed in the presence of conditioned, FACS-sorted DCs from MLN. (c) No conversion into Treg is observed with conditioned and sorted DCs from splenic origin. (d) Treg obtained as in (a) and (b) were sorted by FACS and added at different ratios (Treg: spleen cells) to a mixed lymphocyte reaction (MLR) assay (1 × 105 responder cells: 1 × 105 stimulator cells). Proliferation was evaluated by 3H-thymidine incorporation. The results show mean±s.d. and are representative of 2-3 independent experiments (DCs from 4 animals for each) performed in triplicate. c.p.m., counts per minute. The significance of the data were evaluated by nonparametric one-way ANOVA with Bonferroni's multiple comparison test (a) or paired t-test (b). In (a) and (b), ‘a’ indicates comparison with control (CTRL) and ‘b’ indicates comparison between LPR-conditioned DCs and SIgA-LPR-conditioned DCs. In panel D, ‘a’ indicates comparison with No Treg and “b” indicates comparison between LPR-conditioned DCs and SIgA-LPR-conditioned DCs.*, P values<0.05; **, P values<0.005.
Discussion
The novelty of our data resides in the observation that SIgA plays an important role in the sensing of the microbiota by further promoting the tolerogenic conditioning of mucosal DCs. At the mechanistic level, our results show SIgA-mediated potentiation of the expression of the TLR regulatory proteins SIGIRR, Tollip and SOCS1, and the vitamin A metabolizing enzyme RALDH2 in PP DCs conditioned by LPR. At the func-tionallevel, thistranslatesinbasicallyunchanged DCactivation markers, the production of IL-10 and TGF-β by mucosal DCs, into a reduction of antigen-specific T cell proliferation and differentiation into functional Tregs. These findings provide a link between the need for SIgA to control the expansion39 and character40 of the intestinal microbiota, the bacterial sensing by PPs,16 and the development of a tolerogenic phenotype of local DCs that is important for intestinal homeostasis.41
The default response of the intestinal immune system to most antigens is the induction of immunological tolerance, which is difficult to reconcile with the constant exposure to ligands for TLR and other pattern recognition receptors.42 Our work provides insights into this paradox by showing that contrary to splenic DCs, PP and MLN DCs have increased expression of proteins involved in the negative regulation of TLR-mediated responses (SIGIRR, Tollip, SOCS1) following conditioning with LPR. The presence of SIgA further supported the expression ofsuchproteins in PP DCs only, i.e., cells undergoing massive exposure to environmental antigens. Such differences may thus represent one of the mechanisms by which DCs residing in different tissues are likely to have a different reaction to their surrounding environment.43 This result adds to the complexity of research examining how the regulation of TLR signaling by commensals may contribute to the quenching of immune responses induced by pathogenic bacteria that express TLR ligands. Noteworthy, mice lacking either SIGIRR or SOCS1 have increased susceptibility to inflammatory intestinal diseases.44
In comparison with the control, enhanced production of IL-10 and TGF-β and to a lesser extent IL-6 by DCs isolated from the PPs and MLNs is worth noting, as these three cyto-kines have crucial homeostatic functions in the intestinal environment41 and participate in the isotypic switch leading to production of local IgA.1, 45 The unchanged pattern of pro-inflammatory cytokines resulting from incubation with LPR and SIgA-LPR undergoes drastic modifications after incubation with LPS, strongly suggesting that PP and MLN DCs have the intrinsic capacity to discriminate between harmless and harmful signals. In comparison to the mucosal environment, DCs isolated from the spleen secrete more pro-inflammatory and less anti-inflammatory cytokines when exposed to LPR, yet this is no longer true when associated with SIgA, showing similarity to the in vivo situation.12 The highest reactivity of spleen-derived DCs exposed to LPR is most likely required to rapidly detect and eliminate commensal bacteria that have gained access to this normally sterile compartment.46
The positive effect of SIgA is marked as a function of the parameters examined in DC responsiveness. Such differences may be explained by the presence of endogenous SIgA bound to DCs isolated from the MLNs and PPs (J. Mikulic, unpublished data). Our approach of using tissue-derived DCs has, however, allowed us to unravel the contribution of SIgA in this process. In the absence of the prototype IgA receptor CD89 in mice, an anticipated development will be to identify the receptor(s) for SIgA on mucosal DCs and to determine how crosslinking alters DC signaling and responsiveness. A clue could come from the observation that the specific ICAM-3 grabbing nonintegrin receptor 1 (SIGNR1) has been shown to bind SIgA on the surface of bone marrow-derived DCs and can induce signaling favoring non-inflammatory responses.38 Collectively, these data extend, at the functional level, our previous observations made in mice that show that immune complexes consisting of commensal bacteria and SIgA specifically target PPs CD11c+ CD11b+MHCII+ DCs.16
Although a convenient source of cells, the use of in vitro generated monocyte-derived DCs does not truly reflect the intrinsic nature of DCs and their in situ activities. This is particularly true when testing interactions with antibody ligands15 or the effects of bacteria on gut-associated DCs.47 The different responsiveness of DCs incubated with LPR or LPS used as a surrogate of pathogen-like signal suggests that DCs from mucosal and systemic tissues have intrinsic properties making them capable of discriminating between stimuli of different natures. It is noteworthy that incubation with dead commensal bacteria led to different results,47, 48 an observation that can be explained by the recent finding that the signature of microbial viability plays a role in alerting the immune system.49
We found that in contrast to splenic DCs, PP- and MLN-derived DCs conditioned by LPR or SIgA-LPR develop characteristics of tolerogenic/homeostatic cells unable to stimulate naïve T cells, yet promote differentiation into Treg cells. The suppressive function of Treg cells converted by conditioned DCs from either the PPs or MLNs was confirmed by the MLR assay. In the physiological context of newborns, it is plausible that, right after birth, the combination of newly colonizing bacteria and maternal SIgA from breast milk contributes to actively establish a state of tolerance toward gut microbiota important for the proper development of the immunomodulatory function of the gut.6 Such a hypothesis may provide an explanation for the finding that an exquisite specificity exists in the TCRs of Treg cells from the mouse colon compared with Treg cells from other organs.50
In conclusion, SIgA appears to play an important role in the facilitation of communication in the mucosal environment between DCs and commensal bacteria as illustrated with LPR in this study. Although the anti-inflammatory properties of SIgA toward mucosal pathogens have been documented in many instances, these data underscore its role in contributing to the tolerogenic outcome of the interaction between mucosal DCs and commensal bacteria. Our work brings the first pieces of evidence toward deciphering the pathways through which SIgA, in complex with commensal bacteria, may contribute to educate mucosal DCs, especially in PPs, to promote local homeostasis.
References
Cong Y, Feng T, Fujihashi K, Schoeb TR, Elsona CO . A dominant, coordinated T regulatory cell-IgA response to the intestinal microbiota. Proc Natl Acad Sci USA 2009; 106: 19256–19261.
Atarashi K, Tanoue T, Oshima K et al. Treg induction by a rationally selected mixture of Clostridia strains from the human microbiota. Nature 2013; 500: 232–236.
Brandtzaeg P . Gate-keeper function of the intestinal epithelium. Benef Microbes 2013; 4: 67–82.
Probst HC, Muth S, Schild H . Regulation of the tolerogenic function of steady-state DCs. Eur J Immunol 2014; 44: 927–933.
Pabst O . New concepts in the generation and functions of IgA. Nat Rev Immunol 2012; 12: 821–832.
Rogier EW, Frantz AL, Bruno ME et al. Secretory antibodies in breast milk promote long-term intestinal homeostasis by regulating the gut microbiota and host gene expression. Proc Natl Acad Sci USA 2014; 111: 3074–3079.
Mathias A, Pais B, Favre L, Benyacoub J, Corthesy B . Role of secretory IgA in the mucosal sensing of commensal bacteria. Gut Microbes 2014; 5: 688–695.
Peterson DA, Planer JD, Guruge JL et al. Characterizing the interactions between a naturally primed immunoglobulin A and its conserved Bacteroides thetaiotaomicron species-specific epitope in gnotobiotic mice. J Biol Chem 2015; 290: 12630–12649.
Cerutti A, Chen K, Chorny A . Immunoglobulin responses at the mucosal interface. Annu Rev Immunol 2011; 29: 273–293.
Corthésy B . Multi-faceted functions of secretory IgA at mucosal surfaces. Front Immunol 2013; 4: 185.
Crottet P, Corthésy B . Secretory component delays the conversion of secretory IgA into antigen binding competent F(ab)’2: a possible implication for mucosal defense. J Immunol 1998; 161: 5445–5453.
Boullier S, Tanguy M, Kadaoui KA et al. Secretory IgA-mediated neutralization of Shigellaflexneri prevents tissue destruction by down-regulating inflammatory circuits. J. Immunol 2009; 183: 5879–5885.
Slack E, Balmer ML, Macpherson AJ . B cells as a critical node in the microbiota-host immune system network. Immunol Rev 2014; 260: 50–66.
Rey J, Garin N, Spertini F, Corthesy B . Targeting of secretory IgA to Peyer's patch dendritic and T cells after transport by intestinal M cells. J Immunol 2004; 172: 3026–3033.
Kadaoui KA, Corthésy B . Secretory IgA mediates bacterial translocation to dendritic cells in mouse Peyer's patches with restriction to mucosal compartment. J Immunol 2007; 179: 7751–7757.
Rol N, Favre L, Benyacoub J, Corthésy B . The role of secretory immunoglobulin A in the natural sensing of commensal bacteria by mouse Peyer'spatch dendritic cells. J Biol Chem 2012; 287: 40074–40082.
Zheng SG, Wang JH, Stohl W et al. TGF-beta requires CTLA-4 early after T cell activation to induce FoxP3 and generate adaptive CD4+CD25+ regulatory cells. J Immunol 2006; 176: 3321–3329.
Sun CM, Hall JA, Blank RB et al. Small intestine lamina propria dendritic cells promote de novo generation of Foxp3 T reg cells via retinoic acid. J Exp Med 2007; 204: 1775–1785.
Coombes JL, Powrie F . Dendritic cells in intestinal immune regulation. Nat Rev Immunol 2008; 8: 435–446.
Chieppa M, Rescigno M, Huang AY, Germain RN . Dynamic imaging of dendritic cell extension into the small bowel lumen in response to epithelial cell TLR engagement. J Exp Med 2006; 203: 2841–2852.
Murphy KM, Heimberger AB, Loh DY . Induction by antigen of intrathymic apoptosis of CD4+CD8+TCRlo thymocytes in vivo. Science 1990; 250: 1720–1723.
Phalipon A, Cardona A, Kraehenbuhl JP, Edelman L, Sansonetti PJ, Corthésy B . Secretory component: a new role in secretory IgA-mediated immune exclusion in vivo. Immunity 2002; 17: 107–115.
Mathias A, Corthésy B . Recognition of gram-positive intestinal bacteria by hybridoma- and colostrum-derived secretory immunoglobulin A is mediated by carbohydrates. JBiolChem 2011; 286: 17239–17247.
Atarashi K, Nishimura J, Shima T et al. ATP drives lamina propria Th17 cell differentation. Nature 2008; 455: 808–812.
Mathias A, Duc M, Favre L, Benyacoub J, Blum S, Cortheesy B . Potentiation of polarized intestinal Caco-2 cell responsiveness to probiotic complexed with secretory IgA. J Biol Chem 2010; 285: 33906–33913.
Manicassamy S, Ravindran R, Deng J et al. TLR2 dependent induction of vitamin A metabolizing enzymes in dendritic cells promotes T regulatory responses and inhibits TH-17 mediated autoimmunity. NatMed 2009; 15: 401–409.
Jiang X, McClellan SA, Barrett RP, Zhang Y, Hazlett LD . Vasoactive intestinal peptide down regulates proinflammatory TLRs while upregulating anti-inflammatory TLRs in the infected cornea. J Immunol 2012; 189: 269–278.
Wang P, Hou J, Lin L et al. Inducible microRNA-155 feedback promotes type I IFN signaling in antiviral innate immunity by targeting suppressor of cytokine signaling 1. J Immunol 2010; 185: 6626–6233.
Oshima N, Ishihara S, Rumi MA et al. A20 is an early responding negative regulator of Toll-like receptor 5 signalling in intestinal epithelial cells during inflammation. Clin Exp Immunol 2009; 159: 185–198.
Heid CA, Stevens J, Livak KJ, Williams PM . Real time quantitative PCR. Genome Res 1996; 6: 986–994.
Cerovic V, Jenkins CD, Barnes AG, Milling SW, MacPherson GG, Klavinskis LS . Hyporesponsiveness of intestinal dendritic cells to TLR stimulation is limited to TLR4. J Immunol 2009; 182: 2405–2415.
Davies JM, MacSharry J, Shanahan F . Differential regulation of Toll-like receptor signaling in spleen and Peyer's patch dendritic cells. Immunology 2010; 131: 438–448.
Sansonetti P . To be or not to be a pathogen: that is the mucosally relevant question. Mucosal Immunol 2011; 4: 8–14.
Qin J, Qian Y, Yao J, Grace C, Li X . SIGIRR inhibits interleukin-1 receptor- and toll-like receptor 4-mediated signaling through different mechanisms. J Biol Chem 2005; 280: 25233–25241.
Zhang G, Ghosh S . Negative regulation of toll-like receptor-mediated signaling by Tollip. J Biol Chem 2002; 277: 7059–7065.
Kinjyo I, Hanada T, Inagaki-Ohara K et al. SOCS1/JAB is a negative regulator of LPS-induced macrophage activation. Immunity 2002; 17: 583–591.
Molenaar R, Knippenberg M, Goverse G et al. Expression of retinialdehyde dehydrogenase enzymes in mucosal dendritic cells and gut-draining lymph node stromal cells is controlled by dietary vitamin A. J Immunol 2012; 186: 1934–1942.
Diana J, Moura IC, Vaugier C et al. Secretory IgA induces tolerogenic dendritic cells through SIGNR1 dampening autoimmunity in mice. J Immunol 2013; 191: 2335–2343.
Fagarasan S, Muramatsu M, Suzuki K, Nagaoka H, Hiai H, Honjo T . Critical roles of activation-induced cytidinedeaminase in the homeostasis of gut flora. Science 2002; 298: 1424–1427.
Peterson DA, McNulty NP, Guruge JL, Gordon JI . IgA response to symbiotic bacteria as a mediator of gut homeostasis. Cell Host Microbe 2007; 2: 328–339.
Mowat AM . Anatomical basis of tolerance and immunity to intestinal antigens. Nat Rev Immunol 2003; 3: 331–341.
Shibolet O, Podolsky DK . TLRs in the gut. IV. Negative regulation of Toll-like receptors and intestinal homeostasis: addition by substraction. Am J Physiol Gastroenterol Liver Physiol 2007; 292: G1469–G1473.
Chinen T, Komai K, Muto G et al. Prostaglandin E2 and SOCS1 have a role in intestinal immune tolerance. NatCommun 2011; 2: 190.
Liew FY, Xu D, Brint EK, O'Neill LA . Negative regulation of Toll-like receptor-mediated immune responses. Nat Rev Immunol 2005; 5: 446–458.
Sato A, Hashiguchi M, Toda E, Iwasaki A, Hachimura S, Kaminogawa S . CD11b+Peyer’s patch dendritic cells secrete IL-6 and induce IgA secretion from naive B cells. J Immunol 2003; 171: 3684–3690.
Macpherson AJ, Geuking MB, Slack E, Hapfelmeier S, McCoy KD . The habitat, double life, citizenship, and forgetfulness of IgA. Immunol Rev 2012; 245: 132–146.
Fink LN, Frøkiaer H . Dendritic cells from Peyer's patches and mesenteric lymph nodes differ from spleen dendritic cells in their response to commensal gut bacteria. Scand J Immunol 2008; 68: 270–279.
Christensen HR, Frøkiaer H, Petska JJ . Lactobacilli differentially modulate expression of cytokines and maturation surface markers in murine dendritic cells. J Immunol 2002; 168: 171–178.
Sander LE, Davis MJ, Boekschoten MV et al. Detection of prokaryotic mRNA signifies viability and promotes immunity. Nature 2011; 474: 385–389.
Lathrop SK, Bloom SM, Rao SM et al. Peripheral education of the immune system by colonic commensal microbiota. Nature 2011; 478: 250–254.
Acknowledgements
We acknowledge support from the Swiss Science Research Foundation (grants Nos. 3100-138422 and 3100-156806 to B.C.). The commensal bacterial strain LPR was kindly provided by Nestlé Research Center, Vers-chez-les-Blanc, Switzerland. We thank Dr Gilles Bioley for critical reading of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mikulic, J., Longet, S., Favre, L. et al. Secretory IgA in complex with Lactobacillus rhamnosus potentiates mucosal dendritic cell-mediated Treg cell differentiation via TLR regulatory proteins, RALDH2 and secretion of IL-10 and TGF-β. Cell Mol Immunol 14, 546–556 (2017). https://doi.org/10.1038/cmi.2015.110
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cmi.2015.110
- Springer Nature Limited
Keywords
This article is cited by
-
A new generation of mesenchymal stromal/stem cells differentially trained by immunoregulatory probiotics in a lupus microenvironment
Stem Cell Research & Therapy (2023)
-
The panda-derived Lactiplantibacillus plantarum BSG201683 improves LPS-induced intestinal inflammation and epithelial barrier disruption in vitro
BMC Microbiology (2023)
-
Enhanced IgA coating of bacteria in women with Lactobacillus crispatus-dominated vaginal microbiota
Microbiome (2022)
-
IL-10 and TGF-ß1 Cytokines Stimulated by Ascaris lumbricoides Body Fluid Are Associated with Secretory IgA Levels Against Other Intestinal Pathogens Attenuating Diarrheal Symptoms
Indian Journal of Pediatrics (2021)
-
Selective involution of thymic medulla by cyclosporine A with a decrease of mature thymic epithelia, XCR1+ dendritic cells, and epithelium-free areas containing Foxp3+ thymic regulatory T cells
Histochemistry and Cell Biology (2021)