Abstract
Study
Design: Diagnostic studies—concordance between diagnostic tests.
Objectives
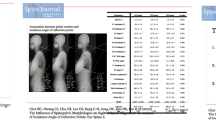
The purpose of this study was to develop a novel spinopelvic parameter (Berbeo-Sardi angle [BSA], the angle formed at the intersection of a line that connects the inferior margin of the sacroiliac joint to the midpoint of a horizontal line joining both femoral heads) measurable in anteroposterior radiographs that indirectly estimates pelvic retroversion and correlates with traditional measurements like pelvic tilt (PT).
Summary
Sagittal balance appraisal and surgical planning rely on the interpretation of spinopelvic parameters. An increased PT reflects pelvic retroversion as a compensatory mechanism to limit sagittal imbalance and correlates with increased pain and disability. However, poor imaging techniques and incorrect patient positioning frequently hamper landmark identification in lateral radiographs, and with no measurable angles in anteroposterior radiographs, it is often impossible to determine PT and pelvic retroversion.
Methods
Whole-spine radiographs from 105 consecutive patients were used to retrospectively measure conventional spinopelvic parameters and the BSA. Intraclass correlation coefficient was used to assess a quantitative correlation between the PT and BSA as indirect measures of pelvic retroversion.
Results
Average values for pelvic incidence, lumbar lordosis, sacral slope, PT, and BSA were 46.5° (±10.23), 48.56° (±12.30), 29.97° (±9.77), 16.94° (±8.03), and 54.47° (±4.05), respectively. We encountered a moderately strong correlation (r = −0.66) between PT and BSA. Receiver operating characteristic plot analysis revealed that a BSA threshold of 46° has a sensitivity of 90% to identify pathologic PT values (>20°), whereas a BSA ≥60° has a specificity of 90% to rule out pelvic retroversion using anteroposterior radiographs.
Conclusions
There is a moderately strong correlation between the BSA, an innovative spinopelvic parameter measurable in anteroposterior radiographs, and PT. BSA seems to show great promise in simplifying spinopelvic appraisal by easily estimating pelvic retroversion associated with sagittal imbalance, while avoiding image-quality issues often encountered in lateral radiographs.
Level of Evidence
Level III.
Article PDF
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
References
Ryan D, Protopsaltis T, Ames C, et al. T1 pelvic angle (TPA) effectively evaluates sagittal deformity and assesses radiographical surgical outcomes longitudinally. Spine 2014;39:1203–10.
Schwab F, Blondel B, Bess S, et al. Radiographic spinopelvic parameters and disability in the setting of adult spinal deformity: a prospective multicenter analysis. Spine 2013;38:E803–12.
Glassman S, Bridwell K, Dimar J, et al. The impact of positive sagittal balance in adult spinal deformity. Spine 2005;30:2024–9.
Klineberg E, Schwab F, Smith J, et al. Sagittal spinal pelvic alignment. Neurosurg Clin N Am 2013;24:157–62.
Lafage V, Schwab F, Patel A, et al. Pelvic tilt and truncal inclination: two key radiographic parameters in the setting of adults with spinal deformity. Spine 2009;34:E599.
Duval-Beaupere G, Schmidt C, Cosson P. A barycentremetric study of the sagittal shape of spine and pelvis: the conditions required for an economic standing position. Ann Biomed Eng 1992;20:451–62.
Dubousset J. Three-dimensional analysis of the scoliotic deformity. In: Weinstein S, editor. The pediatric spine: principles and practice. New York: Raven Press; 1994. p. 479–96.
Lafage V, Blondel B, Smith J, et al. Preoperative planning for pedicle subtraction osteotomy: does pelvic tilt matter? Spine Deform 2014;2:358–66.
Le Huec J, Saddiki R, Franke J, et al. Equilibrium of the human body and the gravity line: the basics. Eur Spine J 2011;20(Suppl 5):558.
Mac-Thiong J, Berthonnaud E, Dimar J, et al. Sagittal alignment of the spine and pelvis during growth. Spine 2004;29:1642–7.
Ames C, Smith J, Scheer J, et al. Impact of spinopelvic alignment on decision making in deformity surgery in adults: a review. J Neurosurg Spine 2012;16:547–64.
Bhalla A, Fayssoux R, Radcliff K. Adult spinal deformity: radiographic parameters. Semin Spine Surg 2015;27:155–8.
Barrey C, Roussouly P, Perrin G, et al. Sagittal balance disorders in severe degenerative spine: can we identify the compensatory mechanisms? Eur Spine J 2011;20(Suppl 5):626.
Obeid I, Hauger O, Aunoble S, et al. Global analysis of sagittal spinal alignment in major deformities: correlation between lack of lumbar lordosis and flexion of the knee. Eur Spine J 2011;20(Suppl 5):681.
Smith J, Klineberg E, Schwab F, et al. Change in classification grade by the SRS-Schwab adult spinal deformity classification predicts impact on health-related quality of life measures: prospective analysis of operative and non-operative treatment. Spine 2013;38:1663–71.
Blondel B, Schwab F, Ungar B, et al. Impact of magnitude and percentage of global sagittal plane correction on health-related quality of life at 2-years follow-up. Neurosurgery 2012;71:341–8.
Schwab F, Lafage V, Patel A, et al. Sagittal plane considerations and the pelvis in the adult patient. Spine 2009;34:1828–33.
Blanke K, Timothy R, Kuklo T, et al. Clinical photographs and radiographic methodology to evaluate spinal deformity. In: Blanke K, Timothy R, Kuklo T, et al., editors. Spinal deformity study group. Radiographic measurement manual. Memphis, TN: Medtronic Sofamor Danek; 2008. p. 11–30.
Horton W, Brown C, Bridwell K. The effect of arm position on sagittal plane alignment. Spine 2005;30:427–33.
Bonett D. Sample size requirements for estimating intraclass correlations with desired precision. Stat Med 2002;21:1331–5.
StataCorp. Stata Statistical Software: Release 13. College Station, TX: StataCorp LP; 2013.
Chan Y. Correlational analysis (biostatistics 104). Singapore Med J 2003;44:9.
Berjano P, Damilano M, Bozzaro M, et al. Standing lateral lumbar spine and pelvis (SLLP) radiograph: a screening, reduced radiation method, for sagittal imbalance. Eur Spine J 2013;22(Suppl 6):842–6.
Dimar J, Carreon L, Labelle H, et al. Intra- and inter-observer reliability of determining radiographic sagittal parameters of the spine and pelvis using a manual and a computer-assisted methods. Eur Spine J 2008;17:1373–9.
Tannast M, Murphy S, Langlotz F, et al. Estimation of pelvic tilt on anteroposterior x-rays—a comparison of six parameters. Skelet Radiol 2006;35:149–55.
Greko P, Thayer J. Evaluation of quality of lateral full spine radiographs: a statistical study. J Manipulative Physiol Ther 1992;15:217–23.
Morvan G, Mathieu P, Vuillemin V, et al. Standardized way for imaging of the sagittal spinal balance. Eur Spine J 2011;20(Suppl 5):602–8.
Kitajima M, Mawatari M, Aita K, et al. A simple method to determine the pelvic inclination angle based on anteroposterior radiographs. J Orthop Sci 2006;11:342–6.
Konishi N, Mieno T. Determination of acetabular coverage of the femoral head with use of a single anteroposterior radiograph: a new computerized technique. J Bone Joint Surg Am 1993;75:1318–33.
Thoren B, Sahlstedt B. Influence of pelvic position on radiographic measurements of the prosthetic acetabular component. Acta Radiol 1990;31:133–6.
Siebenrock K, Kalbermatten D, Ganz R. Effect of pelvic inclination on determination of acetabular retroversion. A study on cadaver pelves. Clin Orthop Relat Res 2003;407:241–8.
Nishihara S, Sugano N, Nishii T. Measurements of pelvic flexion angle using three-dimensional computed tomography. Clin Orthop Relat Res 2003;411:140–51.
Kojima A, Nakagawa T, Tohkura A. Simulation of acetabular coverage of femoral head using anteroposterior pelvic radiographs. Arch Orthop Trauma Surg 1998;117:330–6.
Jackson R, Peterson M, McManus A, et al. Compensatory spinopelvic balance over the hip axis and better reliability in measuring lordosis to the pelvic radius on standing lateral radiographs of adult volunteers and patients. Spine 1998;23:1750–967.
Blondel B, Schwab F, Patel A, et al. Sacro-femoral-pubic angle: a coronal parameter to estimate pelvic tilt. Eur Spine J 2012;21:719–24.
Ragsdale M, Wong F, Boutin R, et al. Pelvic tilt evaluation from frontal radiographs: the validity, interobserver reliability and intraobserver reproducibility of the sacro-femoral-pubic parameter. J Arthroplasty 2017;32:1665–9.
Ghandhari H, Fouladi D, Safari M, et al. Correlation between pelvic tilt and the sacro-femoral-pubic angle in patients with adolescent idiopathic scoliosis, patients with congenital scoliosis, and healthy individuals. Eur Spine J 2016;25:394–400.
You J, Le P, Cho W. Is sacro-femoral-pubic angle a good indicator of pelvic tilt? Global Spine J 2017;6. s-0036-1582850-s-0036-1582850.
Goldstein J, Macenski M, Griffith S, et al. Lumbar sagittal alignment after fusion with a threaded interbody cage. Spine 2001;26:1137–42.
Lazennec J, Ramare S, Arafati N, et al. Sagittal alignment in lumbosacral fusion: relations between radiological parameters and pain. Eur Spine J 2000;9:47–55.
Le Huec J, Faundez A, Dominguez D, et al. Evidence showing the relationship between sagittal balance and clinical outcomes in surgical treatment of degenerative spinal diseases: a literature review. Int Orthop 2015;39:87–95.
Schwab F, Patel A, Ungar B, et al. Adult spinal deformitypostoperative standing imbalance: How much can you tolerate? an overview of key parameters in assessing alignment and planning corrective surgery. Spine (Phila Pa 1976) 2010;35:2224–31.
Carman D, Browne R, Birch J. Measurement of scoliosis and kyphosis radiographs: Intraobserver and interobserver variation. J Bone Joint Surg Am 1990;72:328–33.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sardi, J.P., Camacho, J.E., Diaz, R.C. et al. The Berbeo-Sardi Angle (BSA): An Innovative Method to Effectively Estimate Pelvic Retroversion in Anteroposterior Radiographs—A Correlation With Traditional Parameters. Spine Deform 6, 105–111 (2018). https://doi.org/10.1016/j.jspd.2017.08.011
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2017.08.011