Abstract
Study Design
Clinically related experimental study.
Objective
Evaluation of strain in posterior low lumbar and spinopelvic instrumentation for multilevel fusion resulting from the impact of such mechanical factors as physiologic motion, different combinations of posterior and anterior instrumentation, and different techniques of interbody device implantation.
Summary of Background Data
Currently different combinations of posterior and anterior instrumentation as well as surgical techniques are used for multilevel lumbar fusion. Their impact on risk of device failure has not been well studied. Strain is a well-known predictor of metal fatigue and breakage measurable in experimental conditions.
Methods
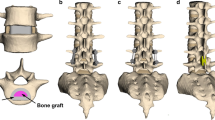
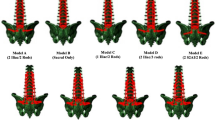
Twelve human lumbar spine cadaveric specimens were tested. Following surgical methods of lumbar pedicle screw fixation (L2–S1) with and without spinopelvic fixation by iliac bolt (SFIB) were experimentally modeled: posterior (PLF); transforaminal (TLIF); and a combination of posterior and anterior interbody instrumentation (ALIF+PLF) with and without anterior supplemental fixation by anterior plate or diverging screws through an integrated plate. Strain was defined at the S1 screws, L5–S1 segment of posterior rods, and iliac bolt connectors; measurement was performed during flexion, extension, and axial rotation in physiological range of motion and applied force.
Results
The highest strain was observed in the S1 screws and iliac bolt connectors specifically during rotation. The S1 screw strain was lower in ALIF+PLF during sagittal motion but not rotation. Supplemental anterior fixation in ALIF+PLF diminished the S1 strain during extension. Strain in the posterior rods was higher after TLIF and PLF and was increased by SFIB; this strain was lowest after ALIF+PLF, as supplemental anterior fixation diminished the strain during extension, in particular, cages with anterior screws more than anterior plate. Strain in the iliac bolt connectors was mainly determined by direction of motion.
Conclusions
Different devices modify strain in low posterior instrumentation, which is higher after transforaminal and posterior techniques, specifically with spinopelvic fixation.
Level of Evidence
N/A.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Burger E, Noshchenko A, Barton C, et al. Sagittal plane correction is correlated with quality of life at early followup in adult deformity patients. In: SICOT, editor. International Society of Orthopaedic Surgery and Traumatology (SICOT), 36th World Congress, Guangzhou, China, September 17–19 2015.
Smith JS, Shaffrey CI, Lafage V, et al. Comparison of best versus worst clinical outcomes for adult spinal deformity surgery: a retrospective review of a prospectively collected, multicenter database with 2-year follow-up. J Neurosurg Spine 2015;23:349–59.
Smith JS, Singh M, Klineberg E, et al. Surgical treatment of pathological loss of lumbar lordosis (flatback) in patients with normal sagittal vertical axis achieves similar clinical improvement as surgical treatment of elevated sagittal vertical axis: clinical article. J Neurosurg Spine 2014;21:160–70.
Kebaish KM. Sacropelvic fixation: techniques and complications. Spine (Phila Pa 1976) 2010;35:2245–51.
Edwards 2nd CC, Bridwell KH, Patel A, et al. Long adult deformity fusions to L5 and the sacrum. A matched cohort analysis. Spine (Phila Pa 1976) 2004;29:1996–2005.
Shen FH, Mason JR, Shimer AL, et al. Pelvic fixation for adult scoliosis. Eur Spine J 2013;22(suppl 2):S265–75.
Bydon M, Macki M, Abt NB, et al. The cost-effectiveness of interbody fusions versus posterolateral fusions in 137 patients with lumbar spondylolisthesis. Spine J 2015;15:492–8.
McLnnis MM, Olchanski N, Kemner JE, et al. Budget impact of new rhbmp-2 formulation in patients undergoing posterolateral spinal fusion procedures for degenerative disc disease in randomized controlled trial (RCT). Value Health 2010;13:A305.
Carreon LY, Glassman SD, Djurasovic M, et al. RhBMP-2 versus iliac crest bone graft for lumbar spine fusion in patients over 60 years of age: a cost-utility study. Spine 2009;34:238–43.
Alvin MD, Lubelski D, Abdullah KG, et al. Cost-utility analysis of instrumented fusion versus decompression alone for grade I L4-L5 spondylolisthesis at 1-year follow-up: a pilot study. Clin Spine Surg 2016;29:E80–6.
Deyo RA, Martin BI, Kreuter W, et al. Revision surgery following operations for lumbar stenosis. J Bone Joint Surg Am 2011;93:1979–86.
Marchi L, Oliveira L, Coutinho E. Results and complications after 2-level axial lumbar interbody fusion with a minimum 2-year follow-up. J Neurosurg Spine 2012;17:187–92.
Barton C, Noshchenko A, Patel V, et al. Risk factors associated with rod fracture after osteotomy for adult spine deformity. In: Internation Society of Orthopaedic Surgery and Traumatology (SICOT) 36th World Congress, Guangzhou, China, September 17–19 2015.
Cho W, Mason JR, Smith JS, et al. Failure of lumbopelvic fixation after long construct fusions in patients with adult spinal deformity: clinical and radiographic risk factors: clinical article. J Neurosurg Spine 2013;19:445–53.
Fleischer GD, Kim YJ, Ferrara LA, et al. Biomechanical analysis of sacral screw strain and range of motion in long posterior spinal fixation constructs: effects of lumbosacral fixation strategies in reducing sacral screw strains. Spine (Phila Pa 1976) 2012;37:E163–9.
Rousseau MA, Lazennec JY, Saillant G. Circumferential arthrodesis using PEEK cages at the lumbar spine. J Spinal Disord Tech 2007;20:278–81.
Noshchenko A, Plaseied A, Patel VV, et al. Correlation of vertebral strength topography with 3-dimensional computed tomographic structure. Spine (Phila Pa 1976) 2013;38:339–49.
Harris BM, Hilibrand AS, Savas PE, et al. Transforaminal lumbar interbody fusion: the effect of various instrumentation techniques on the flexibility of the lumbar spine. Spine (Phila Pa 1976) 2004;29:E65–70.
Roessle ML, Fatemi A. Strain-controlled fatigue properties of steels and some simple approximations. Int J Fatigue 2000;22:495–511.
Glantz SA. Primer of Biostatistics. 6th ed. New York: McGraw-Hill Medical; 2005.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author disclosures
CJK (reports grants from DePuy/Synthes Inc, during the conduct of the study; grants from Medtronic Sofamor-Danek, grants from Aesculap, grants from SI Bone, grants from Vertiflex, grants and personal fees from Medicrea, grants from Orthofix, grants from Integra Life Sciences Corporation, grants from Pfizer, grants from Spinal Kinetics, grants from MTF, grants from National Institutes of Health, grants from Globus, outside the submitted work); DI (reports grants from DePuy/Synthes Inc, during the conduct of the study); EML (reports grants from DePuy/Synthes Inc, during the conduct of the study; grants from Medtronic, grants from SI Bone, outside the submitted work); AN (reports grants from Synthes, during the conduct of the study); VVP (reports grants from Synthes, during the conduct of the study; grants from Aesculap, grants from Stryker, grants from SI Bone, grants from National Institutes of Health, grants from Medtronic, grants from Musculoskeletal Transplant Foundation, outside the submitted work); CB (reports grants from DePuy/Synthes Inc, during the conduct of the study); TB (reports grants from DePuy/Synthes Inc, during the conduct of the study; grants from Stryker Endoscopy, SMV Scientific, and Acumed outside the submitted work); CMJC (reports grants from DePuy/Synthes Inc, during the conduct of the study; personal fees from DePuy/Synthes Inc, grants from Medtronic, grants from Aesculap, grants from Medicrea, grants from Vertiflex, grants from AOSpine, outside the submitted work); ELB (reports grants from Synthes, during the conduct of the study; grants from Medtronic, grants from Aesculap, grants from SI Bone, grants from Vertiflex, grants from Medicrea, grants from Synthes, grants from Orthofix, grants from Integra LifeSciences, grants from Anschutz Foundation, grants from OREF, grants from OMeGA, from null, from null, outside the submitted work).
The authors give permission to reproduce copyrighted materials or signed patient consent forms.
Research grant funding and instrumentation were provided by DePuy/Synthes.
Supplementary data
Rights and permissions
About this article
Cite this article
Kleck, C.J., Illing, D., Lindley, E.M. et al. Strain in Posterior Instrumentation Resulted by Different Combinations of Posterior and Anterior Devices for Long Spine Fusion Constructs. Spine Deform 5, 27–36 (2017). https://doi.org/10.1016/j.jspd.2016.09.045
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2016.09.045