Abstract
The HERG ion channel belongs to the voltage-gated potassium (Kv) channel family and is involved in potassium efflux during cellular repolarization. Mutations in HERG have been linked to long QT syndrome, which is associated with elevated secretion of glucagon-like peptide-1 (GLP-1). However, the precise contribution of HERG to GLP-1 secretion remains unclear. In this study, we demonstrate the expression of HERG in GLP-1-producing L-cells within the intestinal epithelium of rodents. Using a mouse L-cell model (GLUTag cell line), we observed that downregulation of HERG led to a significant prolongation of action potential duration, an increase in intracellular calcium concentration, and a stimulation of GLP-1 secretion following exposure to nutrients. These findings provide evidence that HERG plays a direct role in regulating GLP-1 secretion in the intestine and may hold promise as a potential target for the treatment of diabetes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Background
The human ether-a-go-go-related gene (HERG) encodes the HERG ion channel, which is a member of the voltage-dependent potassium channel (Kv) family. Mutations in HERG result in reduced potassium efflux during repolarization, leading to prolonged QT interval, polymorphic ventricular tachycardia, cardiac syncope, and sudden death (Sanguinetti et al. 1995; Hylten-Cavallius et al. 2017). This condition is referred to as Long QT Syndrome (LQTS) (Curran et al. 1995) Within the broader Kv channel family (Shi et al. 1997), the HERG ion channels are expressed in the human pancreas and have been found to negatively regulate insulin secretion while positively regulating glucagon secretion (Hardy et al. 2009). Studies have shown that individuals with LQTS caused by loss-of-function mutations in HERG exhibit elevated secretion of glucagon-like peptide-1 (GLP-1) following an oral glucose tolerance test (OGTT) (Hylten-Cavallius et al. 2017). However, the specific role of HERG in L-cells remains unexplored.
Repolarizing potassium channels play a critical role in hormone secretion within endocrine cells (Hardy et al. 2009). In pancreatic beta cells, the conversion of glucose to ATP leads to the closure of KATP channels and subsequent depolarization of the cell membrane (Rorsman et al. 1994; Rajan et al. 1990). This depolarization triggers calcium influx, stimulating insulin exocytosis (Hardy et al. 2009; Sher et al. 2003). Simultaneously, the membrane depolarization initiates the opening of repolarizing (voltage-gated) Kv channels, facilitating the repolarization of the action potential. Our previous research has revealed that insulin secretion in pancreatic islet beta cells is regulated by the interplay between depolarized KATP channels and repolarized Kv channels during glucose stimulation (Yang et al. 2018). Inhibition of Kv channel repolarization has been shown to enhance insulin secretion in beta cells (MacDonald et al. 2002; MacDonald and Wheeler 2003).
GLP-1 is a hormone secreted by intestinal L-cells that stimulates insulin release in response to food intake. The glucose-sensing mechanism in L-cells resembles that of pancreatic cells (Reimann and Gribble 2002). Glucose uptake in intestinal epithelial cells is facilitated by brush-edge sodium-glucose co-transporters, allowing glucose to enter the intestinal L-cells through the apical membrane. Subsequently, intracellular ATP generation leads to the closure of ATP-dependent potassium ion channels, resulting in cell membrane depolarization and calcium influx, ultimately triggering the release of GLP-1 (Gribble and Reimann 2019; Sun et al. 2017). Given the recent success of GLP-1 mimetics and inhibitors of GLP-1 degradation in the treatment of type 2 diabetes (Drucker and Nauck 2006), there is growing interest in targeting L-cells to enhance GLP-1 secretion (Holst 2007; Gribble 2008). Therefore, understanding the sensory and secretory pathways of L-cells is crucial for the success of this therapeutic approach.
In this study, we investigated the involvement of HERG in L-cells using the murine GLUTag cell line. Our results demonstrated high expression levels of HERG channels in GLUTag cells. Upon knockdown of HERG, we observed a significant reduction in Kv currents and an extension of the action potential duration. Additionally, downregulation of HERG expression resulted in an increase in intracellular calcium concentration ([Ca2+]i) and a potentiation of GLP-1 secretion from GLUTag cells following nutrient stimulation. These findings provide evidence that the HERG channel plays a regulatory role in the secretion of GLP-1 in murine L-cells.
2 Methods
2.1 Animal care and cell culture
C57BL/6J mice were obtained from Jiangsu Gempharmatech Laboratories (Jiangsu, Nanjing, China) and housed under controlled conditions, including a constant temperature and humidity, a 12-h light–dark cycle, and ad libitum access to a regular diet. Only male mice were used for our experiments. All animal procedures were conducted in accordance with the guidelines and regulations of the Animal Care and Experimentation Committee at Capital Medical University. The murine L-cell line GLUTag cells have been extensively validated as models for studying GLP-1 secretion by intestinal L-cells (Reimann and Gribble 2002; Gagnon et al. 2015). GLUTag cells, originally provided by Prof. D.J. Drucker at the University of Toronto, Canada(Drucker et al. 1994)), were cultured in high-glucose Dulbecco's modified Eagle medium (DMEM) with a glucose concentration of 25 mmol/L and supplemented with 10% fetal bovine serum (FBS). The cells were maintained in a humidified incubator at 37°C with 95% air and 5% CO2.
2.2 Immunoblotting analysis
Tissues and cells were lysed in a lysis buffer containing 20 mmol/L Tris–HCl pH 7.5, 150 mmol/L NaCl, 1 mmol/L MgCl2, 1% Triton X-100, 1 mmol/L PMSF, and a complete protease inhibitor cocktail (Roche). After centrifugation at 14,000 r/min for 10 min at 4°C, the supernatants were collected as protein samples. Western blot experiments were performed as previously described (Wang et al. 2020). Immunoreactive signals were detected using ECL Prime (GE Healthcare Biosciences) and an ImageQuant 500 chemiluminescence detection system (GE Healthcare Bioscience).
2.3 Immunofluorescence staining
Frozen sections from C57BL/6J mice were fixed with 3% paraformaldehyde in phosphate-buffered saline (PBS) for 30 min and permeabilized with 0.1% Triton X-100 in PBS for 30 min. The cells were then blocked with PBS containing 1% bovine serum albumin (BSA) for 15 min. Coverslips were incubated with primary antibodies overnight, followed by incubation with Alexa Fluor 488- or 568-conjugated secondary antibodies (Invitrogen; 1:500 dilution) for 60 min at room temperature. Microscopic images were acquired using a 3D Histech Digital Pathology System and CaseViewer software.
2.4 RNA isolation and gene expression analysis
RNA was extracted using Trizol Reagent (Invitrogen) following the manufacturer's instructions. Total RNA (1 μg) was reverse transcribed using oligo-(dT)12–18 primer and Superscript III (Invitrogen). Quantitative PCR was performed on a LightCycler 480 Real-Time PCR System (Roche, Basel, Switzerland) using SYBR Green I Master Mix reagent (Roche) and specific primers. All reactions were performed in triplicate. The relative mRNA expression level was calculated and normalized against Rplp0/36B4 mRNA expression. The primer sequences for mouse genes are listed in Table 1.
2.5 siRNA transfection
GLUTag cells were seeded in 24-well plates and transfected at 80% confluence with 100 nmol/L scramble siRNAs or siRNAs targeting mouse HERG (sc-42498, Santa Cruz) using Lipofectamine RNAiMAX (Invitrogen) according to the manufacturer's instructions. After 48 h of transfection, cells were used for RNA isolation followed by real-time PCR or reseeded on coverslips for voltage clamp measurements.
2.6 Electrophysiology experiment
The GLUTag cells were transfected with siRNA and cultured in 35 mm dishes for 48 h before the experiments. Patch-clamp recordings were performed on single cells using an EPC-10 amplifier and PULSE software (HEKA Electronik, Lambrecht, Germany). Kv currents were recorded from a holding potential of -70 mV to various depolarizing pulses (-70 to + 70 mV) in 10 mV increments for 2 s in GLUTag cells. The extracellular solution contained (in mmol/L): 10 KCl, 125 NaCl, 2 CaCl2, 2 MgCl2, 1 glucose, and 10 HEPES (pH adjusted to 7.4). The intracellular solution contained (in mmol/L): 130 KCl, 10 NaCl, 2 CaCl2, 10 EGTA, 10 HEPES, 2 MgCl2, and 1 MgATP (pH adjusted to 7.4). Action potentials were elicited by a 0.5 nA current injection for 50 ms in GLUTag cells. The electrode solutions for recording action potentials contained (in mmol/L): 76 K2SO4, 10 KCl, 10 NaCl, 55 sucrose, 1 MgCl2, and 10 HEPES (pH adjusted to 7.2) and, while the extracellular solution contained (in mmol/L): 5.6 KCl, 138 NaCl, 2.6 CaCl2, 1.2 MgCl2, 1 glucose, and 10 HEPES (pH adjusted to 7.4). Data were recorded using pCLAMP software (Axon Instruments) with a 16-bit digital model converter and analyzed with ClampFit software. Experiments were performed at a temperature of 22–24°C.
2.7 GLP-1 secretion assay
GLUTag cells were seeded in 24-well plates at a density of 200,000 cells per well in 1 mL of culture medium. Forty-eight hours after plating, cells were rinsed with HBSS and then incubated in Krebs–Ringer bicarbonate buffer (KRBB; 120 mmol/L NaCl, 5 mmol/L KCl, 24 mmol/L NaHCO3, 1 mmol/L MgCl2, 2 mmol/L CaCl2, 15 mmol/L HEPES pH 7.4, 0.1% BSA) for 30 min, followed by incubation in the same buffer or a high-glucose buffer containing 10 mmol/L glucose for an additional 2 h. Some GLUTag cells were treated with 10 mmol/L glucose KRBB containing 10 μmol/L Forskolin (Sigma) plus 10 μmol/L IBMX (Sigma) or 2 μmol/L OEA (MCE) or 10 mmol/L glutamine (Gibco). After the 2-h incubation, media were collected, and cells were lysed in lysis buffer. The level of GLP-1 was measured using a total GLP-1 ELISA kit (Millipore) and an Infinite 200 Pro Reader (TECAN, Switzerland).
2.8 Measurement of intracellular calcium concentration ([Ca2+]i)
Cells were plated on glass coverslips and incubated in a humidified incubator for 24 h. Before the imaging experiment, cells were loaded with 2 μmol/L Fura-4 AM (Dojindo, Japan) in KRBB (0 mmol/L glucose) at 37°C for 30 min with 0 mmol/L glucose KRBB to remove excess Fluo-4 AM. Subsequently, cells were pre-incubated in 0 mmol/L glucose KRBB for an additional 30 min before being stimulated with 10 mmol/L high-glucose KRBB. Imaging experiments were performed using a DeltaVision Ultra High-Resolution Microscope (GE, USA) with a 60 × objective. Fluo-4 AM was excited at 488 nm, and emission was collected at 525 nm. Sequential confocal images of cells were recorded starting from 60 s before stimulation at 5-s intervals and analyzed using ImageJ software. The ratio of fluorescence change (F/F0) was used to reflect changes in intracellular Ca2+ levels, where F is the observed fluorescence density, and F0 is the average baseline fluorescence density during the first 30 s before stimulation.
2.9 Statistical analysis
All data are presented as mean ± SEM and were compared using a Student's t-test or one-way ANOVA with a Tukey's test for multiple comparisons. A P-value of less than 0.05 was considered statistically significant.
3 Results
3.1 Expression analysis of HERG in murine intestinal L-cells
To assess the expression level of HERG in murine intestinal L-cells, we performed mRNA analysis using reverse transcription PCR (RT-PCR) in the ileum, colon, and GLUTag cells (Fig. 1a). The results revealed significant expression of HERG mRNA in these tissues. To confirm HERG protein expression, we conducted western blot analysis, comparing the expression levels in GLUTag cells and murine brain (used as a positive control) (Fig. 1b). Interestingly, HERG protein exhibited high expression in GLUTag cells, surpassing even the expression observed in murine brain.
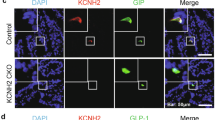
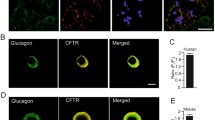
Expression and localization of HERG in GLUTag cells and murine L-cells. a Quantitative PCR analysis showing the mRNA expression of HERG in murine ileum, colon, and GLUTag cells. b Western blot analysis demonstrating the protein expression of HERG in murine ileum, colon, brain, and GLUTag cells. c Relative mRNA expression of Kv channels in GLUTag cells compared to Kir6.2 (KATP channels) after normalization with an internal control. d Immunofluorescence analysis showing the localization of HERG channel (red) in murine ileum with GLP-1 (green) as a marker of L-cells. Nuclei (blue) were stained with DAPI. Scale bar: 50 μm. e Immunofluorescence analysis depicting the localization of HERG channel (red) in GLUTag cells. Scale bar: 10 μm. Each experiment was repeated at least three times
To investigate the expression of Kv channels in GLUTag cells, we performed quantitative PCR (qPCR) profiling (Fig. 1c). The results demonstrated substantial expression of Kv2.1, Kv4.1, Kv5.1, Kv6.2, Kv9.3, and Kv11.1, with Kv11.1 (encoded by the HERG gene) exhibiting the second highest expression level among the detected Kv channels.
To determine the cellular localization of HERG, immunofluorescence staining was performed on frozen sections of murine ileum tissue. The results showed colocalization of HERG with GLP-1 in the intestinal L-cells (Fig. 1d). Furthermore, we examined the localization of HERG protein in GLUTag cells and observed its presence in both the plasma membrane and cytosol of murine L-cells (Fig. 1e).
3.2 The impact of HERG on Kv current and action potential in GLUTag cells
To investigate the role of HERG in GLUTag cells, we employed siRNA-mediated knockdown of HERG expression. qPCR and western blot analysis confirmed a significant decrease in HERG expression in HERG siRNA-treated GLUTag cells compared to control cells transfected with scramble siRNA (Fig. 2a and b). To evaluate the effect of HERG knockdown on whole-cell Kv currents, we performed patch-clamp recordings as described in the Methods section (Fig. 2c). The analysis revealed a substantial reduction in Kv currents in HERG siRNA-treated GLUTag cells compared to control cells (Fig. 2d). Kv channels play a critical role in the repolarization of action potentials, and their inhibition leads to an extended action potential duration (APD). To assess the impact of HERG on action potential repolarization, we evoked electrical action potentials in current-clamp mode and measured the APD in GLUTag cells. The results demonstrated that HERG siRNA-treated cells exhibited a prolonged repolarization phase compared to control cells (Fig. 2e). These findings provide compelling evidence that the HERG channel regulates Kv currents involved in action potential repolarization in GLUTag cells. The reduction of HERG channel expression leads to a prolonged APD, indicating the crucial role of HERG in modulating the electrophysiological properties of GLUTag cells.
Prolongation of action potential duration in GLUTag cells upon HERG channel knockdown. a, b GLUTag cells were transfected with either 100 nmol/L scramble siRNA (siRNA-NC) or siRNA against HERG (siRNA-HERG) for 48 h, and the expression of HERG mRNA (a) and protein (b) was assessed using qPCR and western blot analysis (n = 3). c Representative whole-cell recordings of Kv currents from GLUTag cells treated with siRNA-NC or siRNA-HERG. d Current–voltage relationship curves for Kv currents determined by normalizing the data to the maximum current (siRNA-NC, n = 10; siRNA-HERG, n = 10). e Bar graphs representing the Kv current at a potential of 70 mV. f Representative action potentials recorded from GLUTag cells in current-clamp mode. g Bar graphs showing the action potential duration (siRNA-NC, n = 10; siRNA-HERG, n = 10). Statistical significance was assessed using a Student's t-test. *P < 0.05, ***P < 0.001
3.3 The impact of HERG on calcium concentration ([Ca2+]i) in GLUTag cells
To gain further insights into the involvement of HERG channels in calcium homeostasis, we examined the impact of HERG on [Ca2+]i in GLUTag cells. By utilizing siRNA-mediated knockdown, we successfully reduced HERG expression in GLUTag cells and subsequently measured the [Ca2+]i response to 10 mM glucose stimulation. Our findings revealed a significant increase in [Ca2+]i upon HERG reduction (Fig. 3a), exhibiting a 1.44-fold elevation compared to control cells (Fig. 3b). These results indicate that the downregulation of HERG amplifies the [Ca2+]i response following glucose stimulation in GLUTag cells.
Effect of HERG knockdown on intracellular calcium concentration ([Ca2+]i) in GLUTag cells. Intracellular calcium concentration ([Ca2+]i) was measured using 2 μmol/L Fluo 4-AM and a DeltaVision Ultra High-Resolution Microscope equipped with a 60 × objective at 37 °C. Readings were taken every 5 s for a total of 31 min, with 1 min recorded before and 30 min following glucose stimulation (10 mmol/L). a The fluorescence change ratio (F/F0) was recorded for GLUTag cells treated with scramble siRNA (n = 23 cells) and HERG siRNA (n = 23 cells). b The average area under the curve (AUC) of the HERG siRNA group was significantly higher compared to the control group (P < 0.01). Statistical significance was determined using a Student's t-test. **P < 0.01
3.4 The impact of HERG on GLP-1 secretion in GLUTag cells
Given that HERG reduction increased intracellular [Ca2+], we investigated whether it would also enhance GLP-1 secretion in GLUTag cells. Firstly, we assessed the total amount of GLP-1 in siRNA-treated GLUTag cells and found no significant change, indicating that HERG inhibition did not affect the expression of GLP-1 in L cells (Fig. 4a). Subsequently, we evaluated GLP-1 secretion under various stimulation conditions. We found that while HERG reduction had no impact on GLP-1 secretion under basal conditions (0 mmol/L glucose), it significantly increased GLP-1 secretion upon 10 mmol/L glucose stimulation (Fig. 4b) (Reimann et al. 2008). To further examine the effect of other stimulators, we stimulated GLUTag cells with 10 mmol/L glutamine to mimic amino acid stimulation (Tolhurst et al. 2011), 2 μmol/L GPR119 agonist 2-oleoylglycerol (OEA) to mimic fatty acid stimulation (Lauffer et al. 2009; Hodge et al. 2016), and 10 μmol/L forskolin plus 10 μmol/L 3-isobutyl-1-methylxanthine (IBMX) to mimic cAMP stimulation (Simpson et al. 2007). Our findings revealed that glutamine and cAMP stimulation significantly enhanced GLP-1 secretion in HERG reduction cells (Fig. 4c and e), whereas OEA stimulation resulted in only a slight increase in GLP-1 secretion (Fig. 4d). Lastly, we examined the protein expression of HERG in GLUTag cells treated with different nutrients and found no significant changes compared to untreated cells, suggesting that nutrients did not regulate HERG expression in L cells (Fig. 4f and g). Collectively, these findings suggest that HERG reduction enhances GLP-1 secretion in GLUTag cells.
Enhancement of GLP-1 secretion in GLUTag cells upon HERG knockdown. GLUTag cells were transfected with either 100 nmol/L scramble siRNA (siRNA-NC) or siRNA against HERG (siRNA-HERG) for 48 h. a Total GLP-1 levels in treated cells were evaluated. GLUTag cells were stimulated individually with 10 mmol/L glucose (b), 10 mM glutamine (c), 2 μmol/L OEA (d), and 10 μmol/L forskolin plus 10 μmol/L IBMX (e), and the levels of GLP-1 were detected using ELISA analysis. Protein levels of HERG from control GLUTag cells with or without stimulation were evaluated using western blot analysis. n = 4 for (a), (b), (c), (d), and (e); n = 3 for (f). Statistical significance was assessed using a Student's t-test for (a), (b), (c), (d), and (e), and One-way ANOVA with a Tukey's test for g. *P < 0.05, n.s. indicates not significant
4 Discussion
In this study, we investigated the expression and functional role of HERG potassium channels in GLUTag cells. Our results demonstrated that downregulation of HERG led to a prolongation of action potential duration and an increase in intracellular calcium concentration. Additionally, we observed that the deficiency of HERG enhanced the secretion of GLP-1 in response to glucose and amino acid stimulation. These findings suggest that HERG is involved in the release of GLP-1 from intestinal L-cells.
The nutrient-stimulated secretory pathways in L-cells and β cells have been reported to share a common glucose sensing mechanism. Upon nutrient intake, such as glucose and amino acids, there is an increase in ATP production, leading to the closure of KATP channels and plasma membrane depolarization. This depolarization results in the opening of voltage-gated calcium channels and subsequent calcium influx, which triggers hormone exocytosis during action potential firing (Reimann and Gribble 2002; Reimann et al. 2008). Kv channels, including HERG, play a crucial role in regulating hormone secretion (MacDonald and Wheeler 2003) by repolarizing the action potential. GLP-1 is secreted by intestinal L-cells in response to dietary components, including carbohydrates, amino acids, and fats (Elliott et al. 1993; Herrmann et al. 1995). These cells are distributed throughout the gut, with higher abundance in the ileum and colon (Eissele et al. 1992; Larsson et al. 1975). Positioned with their apical protrusions facing the gut lumen, L-cells directly sense the concentration of fats and carbohydrates. The glucose sensing mechanism in L-cells shares similarities with pancreatic β cells. Our quantitative polymerase chain reaction screening for Kv channel isoforms revealed that HERG channels were the second-highest expressed in the murine L-cell line, suggesting a potential role of HERG potassium channels in regulating GLP-1 secretion from L-cells.
Mutations in HERG can lead to reduced potassium efflux during repolarization, resulting in prolonged QT interval and long QT syndrome (LQTS) (Babcock and Li 2013). In patients with LQTS-2, HERG mutations have been reported to increase GLP-1 and insulin secretion by over 50% and cause defects in glucagon secretion. This can lead to an increased risk of low blood sugar levels and symptomatic hypoglycemia following glucose ingestion. Dofetilide, a HERG receptor blocker, exhibits a similar effect by inhibiting HERG in both β and L cells, leading to increased insulin and GLP-1 secretion (Hylten-Cavallius et al. 2017).
L-cells are open enteroendocrine cells with apical protrusions facing the intestinal lumen, believed to play a role in nutrient sensing. They respond to various luminal components, particularly the products of carbohydrate, fat, and protein digestion (Elliott et al. 1993; Herrmann et al. 1995). It is proposed that the electrical uptake of glucose or amino acids triggers membrane depolarization, electrical activity, calcium influx via voltage-gated calcium channels, and GLP-1 secretion in L-cells (Gribble 2008; Gribble et al. 2003; Reimann et al. 2005; Reimann et al. 2004).
Our study employed patch-clamp electrophysiology and HERG gene silencing in GLUTag cells, revealing a reduction in HERG channels, which prolonged action potential durations and resulted in increased calcium influx. Calcium imaging further confirmed the elevation of intracellular calcium [Ca2+]i following glucose stimulation in HERG downregulated GLUTag cells. Moreover, we observed that downregulation of HERG enhanced GLP-1 secretion in response to nutrient stimulation in GLUTag cells. These findings support the role of HERG channels in repolarizing intestinal L-cells and highlight the critical involvement of HERG potassium channel activity in regulating GLP-1 secretion. Further studies using HERG-specific knockout mice in L-cells will provide additional insights into the in vivo function of HERG in GLP-1 secretion.
Understanding the mechanisms underlying GLP-1 secretion is of great interest due to its therapeutic potential for the treatment of metabolic disorders, including type 2 diabetes and obesity. The modulation of HERG channel activity may present a promising avenue for the development of targeted interventions aimed at enhancing GLP-1 secretion and improving glycemic control.
In summary, our study highlights the role of HERG potassium channels in regulating GLP-1 secretion from intestinal L-cells. The downregulation of HERG leads to alterations in action potential duration, intracellular calcium levels, and GLP-1 secretion. These findings contribute to our understanding of the complex mechanisms underlying GLP-1 release and provide a basis for further exploration of HERG channels as potential therapeutic targets for metabolic disorders.
Availability of data and materials
Jin-Kui Yang is the guarantor of this work and, as such, the data that support the findings of this study are available from him upon reasonable request.
Change history
21 February 2024
A Correction to this paper has been published: https://doi.org/10.1007/s44194-024-00029-6
References
Babcock JJ, Li M. HERG channel function: beyond long QT. Acta Pharmacol Sin. 2013;34(3):329–35.
Curran ME, et al. A molecular basis for cardiac arrhythmia: HERG mutations cause long QT syndrome. Cell. 1995;80(5):795–803.
Drucker DJ, et al. Activation of proglucagon gene transcription by protein kinase-A in a novel mouse enteroendocrine cell line. Mol Endocrinol. 1994;8(12):1646–55.
Drucker DJ, Nauck MA. The incretin system: glucagon-like peptide-1 receptor agonists and dipeptidyl peptidase-4 inhibitors in type 2 diabetes. Lancet. 2006;368(9548):1696–705.
Eissele R, et al. Glucagon-like peptide-1 cells in the gastrointestinal tract and pancreas of rat, pig and man. Eur J Clin Invest. 1992;22(4):283–91.
Elliott RM, et al. Glucagon-like peptide-1 (7–36)amide and glucose-dependent insulinotropic polypeptide secretion in response to nutrient ingestion in man: acute post-prandial and 24-h secretion patterns. J Endocrinol. 1993;138(1):159–66.
Gagnon J, et al. Ghrelin is a novel regulator of GLP-1 secretion. Diabetes. 2015;64(5):1513–21.
Gribble FM, et al. A novel glucose-sensing mechanism contributing to glucagon-like peptide-1 secretion from the GLUTag cell line. Diabetes. 2003;52(5):1147–54.
Gribble FM. RD lawrence lecture 2008: targeting GLP-1 release as a potential strategy for the therapy of Type 2 diabetes. Diabet Med. 2008;25(8):889–94.
Gribble FM, Reimann F. Function and mechanisms of enteroendocrine cells and gut hormones in metabolism. Nat Rev Endocrinol. 2019;15(4):226–37.
Hardy AB, et al. Characterization of Erg K+ channels in alpha- and beta-cells of mouse and human islets. J Biol Chem. 2009;284(44):30441–52.
Herrmann C, et al. Glucagon-like peptide-1 and glucose-dependent insulin-releasing polypeptide plasma levels in response to nutrients. Digestion. 1995;56(2):117–26.
Hodge D, et al. Lipid derivatives activate GPR119 and trigger GLP-1 secretion in primary murine L-cells. Peptides. 2016;77:16–20.
Holst JJ. The physiology of glucagon-like peptide 1. Physiol Rev. 2007;87(4):1409–39.
Hylten-Cavallius L, et al. Patients with Long-QT syndrome caused by impaired HERG-encoded Kv11.1 potassium channel have exaggerated endocrine pancreatic and incretin function associated with reactive hypoglycemia. Circulation. 2017;135(18):1705–19.
Larsson LI, et al. Distribution and properties of glucagon immunoreactivity in the digestive tract of various mammals: an immunohistochemical and immunochemical study. Histochemistry. 1975;44(4):281–90.
Lauffer LM, Iakoubov R, Brubaker PL. GPR119 is essential for oleoylethanolamide-induced glucagon-like peptide-1 secretion from the intestinal enteroendocrine L-cell. Diabetes. 2009;58(5):1058–66.
MacDonald PE, et al. Inhibition of Kv2.1 voltage-dependent K+ channels in pancreatic beta-cells enhances glucose-dependent insulin secretion. J Biol Chem. 2002;277(47):44938–45.
MacDonald PE, Wheeler MB. Voltage-dependent K(+) channels in pancreatic beta cells: role, regulation and potential as therapeutic targets. Diabetologia. 2003;46(8):1046–62.
Rajan AS, et al. Ion channels and insulin secretion. Diabetes Care. 1990;13(3):340–63.
Reimann F, et al. Glutamine potently stimulates glucagon-like peptide-1 secretion from GLUTag cells. Diabetologia. 2004;47(9):1592–601.
Reimann F, et al. Characterization and functional role of voltage gated cation conductances in the glucagon-like peptide-1 secreting GLUTag cell line. J Physiol. 2005;563(Pt 1):161–75.
Reimann F, et al. Glucose sensing in L cells: a primary cell study. Cell Metab. 2008;8(6):532–9.
Reimann F, Gribble FM. Glucose-sensing in glucagon-like peptide-1-secreting cells. Diabetes. 2002;51(9):2757–63.
Rorsman P, et al. Ion channels, electrical activity and insulin secretion. Diabete Metab. 1994;20(2):138–45.
Sanguinetti MC, et al. A mechanistic link between an inherited and an acquired cardiac arrhythmia: HERG encodes the IKr potassium channel. Cell. 1995;81(2):299–307.
Sher E, et al. Voltage-operated calcium channel heterogeneity in pancreatic beta cells: physiopathological implications. J Bioenerg Biomembr. 2003;35(6):687–96.
Shi W, et al. Identification of two nervous system-specific members of the erg potassium channel gene family. J Neurosci. 1997;17(24):9423–32.
Simpson AK, et al. Cyclic AMP triggers glucagon-like peptide-1 secretion from the GLUTag enteroendocrine cell line. Diabetologia. 2007;50(10):2181–9.
Sun EW, et al. Mechanisms controlling glucose-induced GLP-1 secretion in human small intestine. Diabetes. 2017;66(8):2144–9.
Tolhurst G, et al. Glutamine triggers and potentiates glucagon-like peptide-1 secretion by raising cytosolic Ca2+ and cAMP. Endocrinology. 2011;152(2):405–13.
Wang H, et al. Melanophilin accelerates insulin granule fusion without predocking to the plasma membrane. Diabetes. 2020;69(12):2655–66.
Yang JK, et al. From hyper- to hypoinsulinemia and diabetes: effect of KCNH6 on insulin secretion. Cell Rep. 2018;25(13):3800–3810 e6.
Funding
This work was supported by grants from the National Natural Science Foundation of China (82170809) to Hao Wang, National Natural Science Foundation of China (81930019) to Jin-Kui Yang and the Beijing Science & Technology Development (JJ-2020–25) to Lin Zhang. It was also supported by the Top Talent Program of Tongren Hospital to Chang Liu and Outstanding Youth Program of Tongren Hospital to Hao Wang.
Author information
Authors and Affiliations
Contributions
J.K.Y. conceived the idea for the study. C.L., Y.C.Y., R.R.X. and H.W. performed the experiments and processed statistical data. C.L., H.W. drafted the manuscript. J.K.Y. and H.W. were responsible for supporting the study, designing the experiments, and summarizing all research data.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
All animal protocols were approved by the Ethical Review Committee at the Institute of Zoology, Capital Medical University, China.
Consent for publication
Not applicable.
Competing interests
All authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The order of the first author and second author has been exchanged.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yuan, YC., Liu, C., Xie, RR. et al. The role of the HERG channel in the secretion of glucagon-like peptide-1 (GLP-1) from murine intestinal L-cells. Curr Med 2, 5 (2023). https://doi.org/10.1007/s44194-023-00022-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44194-023-00022-5