Abstract
One of the newest areas of research in the biomedical field is the investigation of innovative medication drug delivery methods through nanofibers. Electrospinning has emerged as the most feasible method for producing the nanofibers with a variety of advantageous properties that are critical in a variety of applications spanning from the environment to medicine. Electrospinning is a potential technology for generating a nanofibrous materials because it allows pharmaceuticals to be inserted in the nanofibers and delivered over a specific time. The amazing properties of nanofibers are due to their tiny pore size and high surface area, particularly like polymer-based nanofibers. Ultra-fine fibers made from a variety of polymers, including synthetic, natural, and hybrid materials, have been studied effectively. Because of their potential uses in drug delivery systems, nanofibers with good drug-loading capabilities, regulated release, and great stability have piqued the interest of researchers. The manufacture of fibers at nanoscale for diverse medical applications is ensured by the multidisciplinary science of nanotechnology which is rapidly growing which needs focused review in the current results. Recent studies have discussed some aspect of the use of the electrospinning method to create fibers for the effective delivery of drugs. Electrospun fibers, on the other hand, are confined to tissue scaffolding applications needs to be reviewed. This review describes an overview of the electrospinning techniques and applications in drug delivery and the current developments in the nanomaterial-based drug delivery systems particularly by employing nanofibers produced by the electrospinning methods.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Electrospinning, Nanofibers, and Advantages
Nanofibers are the excellent candidates for sustained drug delivery methods so the electrospinning attracts the researchers to create novel nanofibers. Nanofibers with high capacity for medication loading and gradual drug release have kindled the interest in the delivery of drugs for current researchers [1]. Electrospinning is one of the strong method for creating nanofibrous material from diverse polymers using an electric current [2]. Multi-axial electrospinning, which employs several concentric spinnerets, has transformed the application possibilities of electrospinning in the recent decade [3]. Polymers with the core and shell structures are important in the aspect of drug delivery [4]. Electrospinning has proven to be a simple and beneficial method used to produce, from the micrometer to nanoscale, fiber materials for drug carriers. Nanofibers may be used to produce instantaneous and controlled medication release in a variety of situations. The primary characteristics that form nanofibers and make them attractive candidates for achieving immediate drug release are their high specific surface area ratio, which constitute a significant area of contact for dissolution their high porosity and their ability to convert crystalline drugs to an amorphous form. The polymer is usually fabricated using volatile solvents, which has led to the development of fibers with a high surface area and porous structure. If fewer non-volatile solvents are used they may lead to the development of fibers having lower surface area and increasing pore size [5]. To deliver medications locally to a specified place, the use of nanofibrous membranes filled with therapeutic substances is a promising strategy [5, 6]. For a range of drug delivery applications, the fibers made using standard electrospinning methods have previously been reported [7]. Majority of the organic solvents are used to make polymer solutions for the electrospinning; however, these are not compatible with several medicines and biomolecules [8] such as the lacuna. For this, core sheath-constructed triaxial fibers can help to alleviate some of the problems. Furthermore, triaxial electrospinning can help to solve many other concerns in this area, such as improving the ability of poorly soluble medicines to dissolve, facilitating drug to a long-time release, and achieving good kinetic release [9]. A quick release from the outside shell for quick impact and a delayed release for the long-term therapeutic release from the core can be facilitated by the triaxial fiber-based drug delivery systems [10]. It is difficult to deliver poor water-soluble medicines such as anti-retroviral and chemotherapeutic medications [11, 12] that can be overcome using these mentioned nanofibers. Electrospinning is a simple technology for manufacturing ultrafine fibers with diameters ranging from micrometers to nanometers and with controllable properties. By applying a high electric field to a polymer or melt, ultrathin fibers are produced. Long years ago, electrostatic forces were used to create ultrafine fibers [13] which is taken as a note. Now this technology is known as electrospinning and is gaining popularity due to its extraordinary simplicity, adaptability, and prospective applications in a variety of industries [14].
Uses of Electrospun Nanofiber in Medical Field
One of the most promising applications of the electrospun nanofibers among the many possibilities is the medication delivery. The large impact strength, high entrapment efficiency, simultaneous administration of various medicines, ease of operation, and cost-effectiveness of electrospinning in drug delivery are all the appealing qualities [15, 16]. The usage of electrospun fibers as drug carriers in current biomedical applications, particularly after local chemotherapy, will be a promising approach for the future [17, 18]. Several controlled drug-release characteristics, including rapid, calm, pulsatile, postponed, and biphasic releases, have been successfully achieved using the electrospun nanofibers [19, 20]. To boost the therapeutic efficacy of medications and vaccines, delivery systems for drugs are used to transport them to a specific location inside the body with a regulated release. Increasing the medicinal drugs solubility and chemical stability is the initial step toward achieving these objectives. By first increasing the level of therapeutic medicines at the desired location and secondly improving their pharmacological effectiveness, minimizing side effects, and then supplying and maintaining the concentration of those medicines there. Due to their distinctive qualities, such as biological properties, biodegradability, as well as surface functionalization, micro-biodegradable polymer-based systems and nanometer range (colloidal, particles, cannulas, and fibers) have lot of attention in the field of drug delivery devices. Moreover, they can achieve controlled drug release or active targeted drug delivery and enhance medication stability and bioavailability [21]. Oil in water nanoemulsions has become increasingly popular for encapsulating lipophilic compounds and for improving well the encapsulation of lipophilic compounds and the improvement of medication stability and administration, while micro-scale fluids are widely used methods for the oral and molecules distribution via oral and injectable routes [22]. Furthermore, because of their inexpensive manufacturing techniques, polymeric micro/nanoparticles are promising solutions for industrial scale-up and the realization of the controlled medication release [23]. Specifically, by varying the monomer composition, crystallinity, glass transition temperature (Tg), porosity, and intrinsic viscosity, a regulated medication may be achieved. The non-toxic metabolites that can be easily removed by the kidney or liver in the use of alginate polymers have been studied recently [24, 25]. When in contact with the human body, polymers show excellent biocompatibility and can be frequently utilized in the desired medical applications to prevent antibody responses and even to increase inflammation [26,27,28]. Cellulose, chitosan, gelatin, and silk proteins are examples of the natural polymer that can be used to form fibers [29]. Poly(vinyl alcohol), poly(lactic-co-glycolic acid), and polycaprolactone are examples of synthetic polymers that can be used to create fibers [30, 31]. Natural polymers are considered as a reasonably safe, biocompatible, and biodegradable material in biomedical applications [32]. The most common researchers use cellulose, a linear polysaccharide that makes up the majority of the cell wall structures [33]. Synthetic polymers have their own benefits over natural polymers in terms of stability and improved mechanical qualities. Polycaprolactone is an aliphatic semicrystalline polymer derived by osteolysis that contains hexanoic acid [34] and makes a non-toxic and well-liked fibers are reported, such as medicine administration, wound plug dressings, and stents, because it can be eliminated through the digestive system. Janmohammadi et al. provided extensive information on the usage of this PCL scaffolds for tissue engineering applications [35].
Processing Techniques Used to Prepare Nanofiber-Based Composites
This class of nanomaterial comprises nanotubes and nanorods as well as nanofibers, which can be taken as nanostructures. Moreover, nanoparticles can be anchored in nanofiber bulk or on their surface, resulting in nano-fiber-based composite materials. Nowadays, popular techniques used to create polymeric nanostructures or fibers focus mostly on electrospinning, self-assembly, phase separation, drawing, and template synthesis procedures [36,37,38,39,40]. Batteries made of sodium -ion and lithium -ion use the reported nanofibers [41]. Manufacture of nanofibers, nanotubes made of polymer, metal, and metal oxide material components [42,43,44,45,46,47,48,49,50,51,52].
Polymer-Based Nanofibers
Manufacture of nanofibers employing a broad variety of polymer solutions, including both synthetic and natural recyclable and non-biodegradable, has become possible by the electrospinning techniques [53,54,55,56]. Owing to a variety of environmental problems, a recent study is concentrating on the use of biodegradable polymers in the creation of different biomedical applications with an environmental protection components in it [57,58,59,60,61,62,63,64,65]. Nanofibers are commonly made from polymers and copolymers [66,67,68,69,70,71,72,73]. Synthetic polymers, as opposed to natural polymers, often offer greater versatility in terms of production, processing, and alteration as well as being more cost-effective than natural polymers. It is also important to note that mechanical characteristic may be modified efficiently and selectively. Synthetic polymer, however, have poor bioactivity and hence need more alterations than natural polymers. Natural polymers, in contrast, are intrinsically bioactive, exhibiting cell-interactive domains on their backbones, and scaffolds created from them promote greater cell attachment, multiplication, and differentiation than scaffolds generated from synthetic polymers. The benefits of both synthetic and natural polymers researchers have developed include hybrid nanofiber that have physical qualities and strong bioactivity making them particularly well suited for wound regeneration [73]. Many experiments have been undertaken to control the biological activity utilizing biomaterials that have a specific structure and produce cell informative signals comparable to the cellular matrix (CM) [74,75,76] is the new finding. Throughout the last decade, there has been a rise in global research and reports related to electrospinning. The overall number of publications in electrospinning has increased significantly over the last 20 years. These data were acquired from Scopus [77,78,79,80] and processing parameters for electrospinning [81, 82] and electrospun characterization for a wide range of applications [83,84,85,86]. Nanofibers are fibers that range in diameter from 1 to 100 nm. Since they have a significant promise for a wide range of applications and can achieve certain advantages of nanostructured materials, furthermore, the topic of nanofibers has caught the interest particularly in the nanotechnology and nanomedicine and made tremendous development in the recent past. Nanoparticles have been investigated for various biomedical applications for over a decade. In general, the use of nano-sized particles offers several advantages over other drug delivery systems. They are used to (1) enhance the solubility of highly hydrophobic drugs, (2) provide sustained and controlled release of encapsulated drugs, (3) increase the stability of therapeutic agents by chemical or physical means, (4) deliver higher concentrations of drugs to target areas due to an Enhanced Permeation and Retention effect, and (5) provide targeted treatments when modified with cell-specific ligands. Drug-loaded nanoparticles often accumulate in hair follicles and therefore facilitate the penetration of drug molecules through the superficial layers of the SC, followed by drug release into the deeper layers of the skin. The most commonly used nanoparticles for topical and/or transdermal drug delivery are polymeric nanoparticles, nanoemulsions, lipid-based nanoparticles (liposomes and solid–lipid nanoparticles), metal nanoparticles, and dendrimers [14, 18, 21]. The idea will be implemented and further elaborated in our future work that is in progress. Nanofiber offers advantageous qualities, such as a high surface area-to-mass ratio, customizable size and shape, and the ability to build a porous mesh, which creates a good (3D) network, which results in their increased applications [87]. Nutrient infusion and cell penetration within the fiber-deepening structure are the further recent advantages of 3D electrospun scaffolds [88]. Substantial technical advances in electrospinning technology have enabled the invention and manufacture of desirable attributes of new polymer-based material, with the ability to change conductivity, wettability, and antimicrobial properties [89].
Applications of Nanofibers in Drug Delivery
To provide the necessary therapeutic impact and guarantee its particular drug-release profile, a pharmaceutical needs a competent drug delivery system. The disposition, timing, and rate of release of a pharmaceutical must be customized as closely as practical to the medication’s therapeutic objective. Due to the clear distinguishing characteristics of nanofibers, it is frequently used in health care to manage pharmaceutical delivery from hydrophilic and biodegradable polymers. Nanofiber-based system offer several distinct advantages for application in wound dressing. The highly porous nature of nanofibers helps cellular respiration and creates ideal surroundings to aid in wound healing. The moisture under the occlusive dressing helps in healing and it provides optimum barrier to wound exudate which may enclose cytokines and proteins supportive in injury. The water vapor transmission rate through a wound is an important parameter for selecting materials for wound dressing. Thus, the selection of polymer for fabrication of nanofiber for wound dressing is extremely essential. For this purpose, nanofibers embedded with growth factors have shown promising results with fast recovery. Nanofiber-based wound dressing have also been explored for healing of chronic wounds. Recently, nanofibers have been used for detection of hormones that created polyvinylpyrrolidone/chitosan/reduced graphene oxide electrospun nanofibers functionalized with Laccase enzyme to identify 17a-ethinylestradiol (EE2), a female synthetic hormone which alters endocrine system causing health problems. The nanofiber mat was placed in fluorine-doped tin oxide that together caused a synergistic effect. The results showed a good reproducibility and a limit detection of 0.15 pmol L−1. The device potential as a biosensor is further confirmed by its performance in synthetic and human urine. A novel platform used the fluorescent sensing to identify nucleic acids, proteins, and cancer cells. The design of the mat consisted in a NF-capture/target/reporter-G3SG sandwich type to find a b-thalassemia gene fragment. This fiber had the advantage of strong emission of G3SG and the area–volume ratio. This proved the highly sensitive detection not only on targets, HeLa cells were able to be captured [15]. Nanofibers should be used to dispense a wide range of pharmaceuticals, including bioactive proteins, DNA, and medications, that are weakly or completely soluble in water as well as water-insoluble medications [90]. A composite substance is composed of two or more materials, each of which has unique properties. When two materials are composed, they make a harder or lighter material. Thus, the combination can improve strength and stiffness. Fiber-reinforced composite fibers have several advantages in the biomedical area, including biocompatibility, biodegradability, high specific modulus, and durability [91]. To produce synergistic mechanical properties, a polymer composite is mixed with reinforcing fillers in a polymer matrix [92]. Much research has been undertaken looking at the use of this nanofiber composite scaffolds in bone regeneration, soft tissue reconstruction, diabetic wound healing, antimicrobial application, blood vessel grafting, and nerve tissue engineering [93,94,95,96,97,98,99,100]. Electrospinning is an important scaffold fabrication technique employed in regenerative tissue engineering. Synthetic and polymer-based ESM support cell proliferation and attachment. Various types of stem cell attachment and differentiation into specific lineage also evidenced that the electrospun fibers are favorable cell supporting scaffolds. Electrospun fibers are also acting as a cell carrier to recruit the cells at the therapeutic site, acting as a stem cell niche and biomolecule carrier. Electrospun topography, mechanical properties, surface chemistry, and alignment are tenable which are crucial for cell proliferation and differentiation. It could guide as well the neurite extension. Mimicking ECM structure and ECM chemical composition is the major advantage of electrospinning. Hence, electrospun fibers fabricated using polymers are promising biocompatible material in regenerative tissue engineering application. Tissue engineering is one main area focusing on regenerative medicine, which uses these nanofibrous scaffolds for replacement of blood vessels, nerve, skin, muscle, bone, and cartilage. Several reports are there for using the scaffolds for delivery of drug and other bioactive molecules. In addition to the experimental components, mathematical models for optimizing and tuning in vitro and in vivo drug release have been established [101]. The number of tests is reduced by in silico models, which will be used to understand the physical and chemical causes of the drug release [101,102,103]. Electrospun fiber networks can be transformed directly into hydrogels based on the type of polymer or polymers used, but also fiber networks can be combined with hydrogels, as in a composite, to design new functional biomedical materials. In fact, hydrogel electrospun fiber composites fortified with cells appear to be quite promising candidates for cartilage repair. In rabbit cartridge damage is shown to be repaired very effectively using a hydrogel nanofiber composite. Specifically, the nanofiber hydrogel was used to deliver chondrocytes to promote the cartilage repair. Self-assembled nanofiber hydrogels are considered to be utilized with collagen-like functions toward, for instance, cardiomyocyte culture in 2D and 3D. Recent works showed that hydrophilic self-assembling nanofiber hydrogels can support the culture of both rat cardiomyocytes and human embryonic stem-cell-derived cardiomyocytes, which could lead to promising applications in cardiac tissue engineering. Hydrogels were also fabricated from silk nanofibers by combining β-sheet-rich silk nanofibers with amorphous silk nanofibers. The composite nanofiber networks were transformed into hydrogels by horseradish peroxidase cross-linking in an electric field. Such nanofiber hydrogels demonstrated osteogenic differentiation and the aligned aggregation of stem cells in vitro, while also exhibiting osteo-inductive capacity in vivo. Such improved tissue performance with nanofiber hydrogels supports encouraging applications in bone tissue engineering [97, 104, 105]. Nanofiber hydrogels also can be constructed from special blends of polymers that are usually immiscible with very diverse physical and chemical properties. Therein, polyimide and polyvinyl alcohol polymers were blended in solution and electrospun into hydrogels that demonstrate unique mechanical properties, particularly stretching ability suitable for abiotic soft tissue applications. Direct hydrogel electrospinning is still quite challenging to be adapted to any hydrogel material system. However, several promising works have been reported, and this specific technology should be furthered possibly by utilizing the concepts of reactive electrospinning. Very recent studies showed that co-electrospinning of biopolymers with gels or hydrogels is also possible and that such products could be designed specifically for drug delivery. For instance, polycaprolactone nanofibers were produced by co-electrospinning with vancomycin hydrochloride and simvastatin drugs that were already in gel form. The resultant hydrogel/polymer nanofiber composite could sustain drug release for as long as 14 days. Another notable work demonstrated synthesis of reactive macromers that contained protease-cleavable and fluorescent peptides that could form electrospun fibrous hydrogels through a photoinitiated polymerization. These nanofiber hydrogels could release hyaluronic acid for a period of 24 days near protease implants, ensuring effective implant–tissue interaction. The technology and applications of encapsulated electrospun nanofibers in hydrogel matrices included the formation of coatings from such composites. Impressive sustained drug-release profiles (40 days) were reported from ultraviolet light-assisted electrospinning of core–shell fully crosslinked poly(N-isopropylacrylamide-co-N-isopropylmethacrylamide) hydrogel-based nanofibers for thermally induced drug delivery fabricated poly(l-lactide)-Rhodamine B-loaded nanofibrous material, which encapsulated poly(N-isopropylacrylamide-co-N-isopropylmethacrylamide) hydrogel containing gold nanorods that the authors indicated had resembled natural structures, such as jellyfish or hydra. This nanofiber hydrogel could regulate drug release when subjected to near-infrared light stimulation. Remarkable sustained drug-release profiles were obtained extending into 75 days. Furthermore, a key review article discussed diverse fabrication methods and extensive biomedical applications of nanofiber-based hydrogels ranging from bone tissue generation [77, 106].
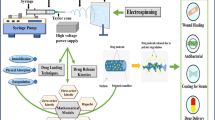
Nanofiber materials might be employed as gene and medication delivery carriers and scaffolds for tissue engineering, cartilage, cardio, dermatology, and bone regeneration. Figure 1 depicts the common applications of nanofibers/fiber composites.
A strong knowledge of the process on electrospinning will enhance control of the electrospun products, making this technique more viable. It mainly focuses on approaches for improving drug solubility, producing biomolecules, and managing drug release. Moreover, innovative approaches to manipulating the characteristics of nanofibers in the context of drug administration with support from the most recent literature will be useful to the researchers in this field. This study also provides a detailed analysis of the research and development of electrospinned polymer nanofibers utilized in the medication delivery. The aim of this review is to offer an overview of the various electrospinning methodologies for drug delivery methods by providing insight into the various techniques and recent application applications.
Electrospinning as a Method of Producing Nanofibers
Figure 2 shows a schematic design of typical electrospinning equipment. In this setup, a stainless-steel capillary syringe that has a blunt end is used to hold the polymer liquid solution. The syringe is inserted into a syringe pump, which allows the solution’s flow rate modified and precisely controlled. The syringe can be oriented horizontally. Pumping of the polymer via a capillary tube that is coupled to a controlled high-voltage source that delivers voltages depending on the experimental demand typically ranges from a few to tens of kilovolts. As a final component, the experimental system incorporates a ground collector. Because there is a capillary situated at a particular length from the ground collector enables the generation of a strong electric field so as to enable a fiber production process to take place. The present level of achieving this condition is quite low, seldom. The electrospinning method is carried out using various capillary systems often known as spinnerets. The three spinneret types that are most often utilized are coaxial, single jet, and multi-jet. Many types of collectors may also be classified. Flat plates, meshes, rings, disks, drums, and multiple parallel; plates are an example of illustrative collector layouts [106]. When a strong electric field is formed with a high potential applied to the capillary polymer solution, because of the liquid surface tension, polymer at the capillary changes to a drop. The surface of the droplets is stable in the absence of a field of electricity (Fig. 2A). When an electric field is applied, electrical currents accumulate on the polymer solution’s surface, resulting in the development of large electrostatic forces which are repulsive forces (Fig. 2B). These pressures cause distortion, resulting in the Taylor cone, a conical droplet form. When the electric field surpasses a particular value, the solution surface forces are crossed and a charged jet of polymer solution is expelled from the cone’s tip (Fig. 2C). The electric field effect caused this jet to flow in the direction of a ground collector. The non-uniform distribution of charges within the polymer jet causes rotating movements that alter the jet’s structure. The jet’s polymer chains tend to stretch and align themselves due to the strong evaporation. In the form of a pure polymer nanofiber, the jet of polymer is subsequently deposited on the collector. Depending on the characteristics of the solution, the deposition of the polymer nanofibers are started in the collector.
The Utilization of Nanofibers Composites as a Medication Delivery System
An increasing interest in the physiochemical properties of composite nanofibers created from biodegradable and biocompatible polymers such as their large area of surface, tiny diameter, as well as high aspect ratio [107,108,109,110] is to be considered. A drug carrier that fits all of these parameters is interestingly an electrospun nanofiber. Composite nanofibers are multiphase fibers in which at least single phase having a nanoscale dimension is also be considered. Mechanical properties, such as heat resistance, are the most important criteria in terms of the stability of the carriers. In many domains, the chemical endurance, optical and surface characteristics, molecular permeability, and electrical conductivity of the composite nanofibers exceeded those of the individual material components. Rezk et al. reported that beta-tricalcium phosphate incorporates cellulose acetate and polycaprolactone as a composite mat to imitate to stimulate the biomineralization process that demonstrated the potential of electrospun nanofibers [111]. There are a number of challenges that must be surmounted: 1. Electrospun fibers necessitate the use of organic solvents in their fabrication. Organic solvent residues make the composites less biocompatible. The green chemistry of preparation should be considered. 2. The large-scale preparation of fibers remains a challenge in the face of industrialization needs. Multi-needle collaborative electrospinning has issues with jet interactions, needle clogging, and cleaning difficulties. Needle-free electrospinning method initially allows the production of large quantities of nanofibers, but they are exceedingly in homogeneously dispersed. 3. Nanoparticles are sporadically arranged in nanofibers, and NNHs have weak mechanical properties. This makes them more fragile as tissue scaffolds for tissue engineering applications. It is vital to investigate the “bridge” that improves the interaction of NPs with the substrate. 4. Precisely controlling nanoparticle alignment in fibers is a huge difficulty. This has the potential to have a significant impact on the electron transport efficiency of in electrically sensitive drug release. This has a detrimental impact on the biosensor as well. (5) The studies on drug release were carried out in a more ideal environment. When confronted with the organism’s complicated physiological environment, more research is needed to determine how to precisely control the drug’s initial burst release and duration of activity. Drug loading using ionized drug molecules results in higher conductivity and, thus, a higher charge density of the jet during fiber formation. The diameter of the electrospun fibers decreases, leading to more rapid drug release, at higher drug-loading levels because of the salt effect. The incorporation of water-soluble acetaminophen also increases the release rate of polylactic acid nanofibers because the dissolution of the drug generates pores. An increased drug content leads to increased burst release, whereas a lower content leads to the creation of a less porous structure upon initial diffusion. Among all the approaches for drug loading into nanofiber, blending of the drug with polymeric solution to generate nanofibers through a single-phase electrospinning technique is of utmost importance, the physiochemical properties compatibility must be considered to attain favorable drug encapsulation, distribution, and desired release kinetics, and lipophilic drugs are loaded in lipophilic polymers, while hydrophilic polymer solutions drug release can be modified using a blend of hydrophilic polymers. Several studies have indicated that addition of hydrophilic polymers reduces burst release and improves the drug-loading efficiency [9, 33]. They also used controlled drug release by loading a multi-membrane of polyvinyl acetate and poly(vinyl alcohol) to stimulate the release [111]. Li et al. effectively created a compound nanofiber for prolonged drug release composed of flexible inorganic composites with carboxy modification. That study discovered that when additionally carboxy radicals were used to treat these nanofibers, they gained a greater capacity for drug loading and a sustained rate of drug release [112]. The fundamental mechanism of an enhanced drug loading was established as an ionic interaction between daunorubicin molecules and the carboxyl group [112]. Coaxial electrospinning to create nanofiber in the core–shell forming an N-carboxymethyl chitosan/PVA/PCL composite loaded with the cancer medication doxorubicin was reported. After incorporating N-carboxymethyl chitosan into the polyvinyl alcohol solution, it was electrospun separately with polycaprolactone using the coaxial electrospinning apparatus, as illustrated in Fig. 3 [113]. In the physiological pH, carboxylic and amine groups of N-carboxymethyl chitosan were shown to be weak that shows higher swelling and faster doxorubicin release from the nanofibers at an acidic pH [113]. Doxorubicin is more readily separated from the nanofiber at this acidic pH. As a result, the composite nanofibers made from the core–shell matrix are excellent candidates for using as the pH-sensitive drug carrier for doxorubicin. Zhao et al. used electrospinning to create a medication delivery system from a composite nanofiber consisting of carboxymethylation integrated polyethylene oxide. According to their finding, the inclusion of carboxymethylation in polyethylene oxide can boost the conductivity of the spinning solution due to the increased ionization characteristics. When the carboxymethylation concentration in the nanofibers was raised, the elongation of the nanofibers decreased significantly. This existence of hydrogen bond interactions between carboxymethylation curdlan and polyethylene oxide in the nanofibers resulted in a significant improvement in tensile strength and Young’s modulus [114].
Increased humidity causes an increase in fiber porosity. Higher temperature accelerates solvent volatilization and decreases polymer solution viscosity, resulting in a much smaller fiber diameter [115]. The results to be mentioned are (1) coupling of positively charged chitosan with negatively charged groups on the outer surface of the bacterium, which attack the permeability of the cell wall; (2) the interaction of dispersed hydrolysis products with DNA, which hinders mRNA and protein synthesis; (3) the chelation of nutrients important metals; and (4) the formation of a chitosan membrane on the cell surface that blocks nutrients from entering the cell or function as an oxalate barrier. Chitosan is soluble in organic acids, such as an aqueous solution of lactic, acetic, and formic acids, as was previously reported. Chitosan may be made soluble in solutions of water, ethanol, methanol, and acetone by adding a little quantity of acid. It is a positively charged polyelectrolyte with a pH of 2 to 6, resulting in very viscous solutions [71]. Moreover, powerful hydrogen bonds generate a network as three-dimensional that prevents polymer chains from moving when subjected to an electric field [116]. But electrospinning of chitosan is often regarded as a difficult method [117]. The recent trends in chitosan electrospinning for antibacterial applications were reported. Furthermore, the aspect impacting chitosan's antibacterial characteristics and the issues related to this polymer’s electrospinning method were explored. There were two key elements of chitosan utilization for electrospinning nanofibers that were highlighted. Moreover, the polymers molecular weight must reflect the considerable role played by the number of polymer chain entanglements in the solution. Polymers with a high molecular weight yield higher and less molecular weight resulting in spheres rather than fibers [118]. Because of the various sources of raw materials used in their synthesis and their adaptability in the terms of chemical alterations, electrospun fibers based on antibacterial polymers appear to receive increasing attention. The incorporation of biocide into the fibers is a common method used in the creation of antimicrobial nanofibers. This can be accomplished by mixing each active molecule in the polymer solution before electrospinning, entrapping the active agent in the fiber cores by coaxial electrospinning, carrying the active agent in nanostructures before dispersing site in the electrospinning solution, or attaching the active agent to the surface of the fiber. Biocides, antibiotics, metal oxide nanoparticles, metallic nanoparticles, and bioactive natural chemicals have all been employed in the past. For enriching antibiotics with polymer, the medication was usually dispersed in the same solvent and then the polymer is slowly mixed with stirring to form a homogeneous solution for electrospinning. Many hydrophobic and hydrophilic antibiotics (ciprofloxacin gentamycin, ampicillin, mupirocin, cefoxitin, tetracycline, and others) have been employed in this aspect with different polymer nanofibers (coPLA, PLGA, PCL/PLA, PLA, and others) throughout the last decade utilizing this straightforward approach [119, 120]. By changing initial concentration of the drug in the electrospinning fluid, this approach may accept a wide variety of antibiotics integrated into the nanofibers. Antibiotics incorporated in the polymer solution may influence the electrospinning of the polymer and the shape of the nanofibers via the changes in the solutions conductivity, surface tension, and viscosity. Kim et al. [121] demonstrated that adding sodium cefoxitin to the PLA/PLGA/PLA-b-PEG solution enhanced the conductivity and electrospinnability, permitting the creation of more uniform nanofibers, and lowered the fiber diameter [121]. Several biocides, including, triclosan, chlorhexidine, and PHMB, have antibacterial activity against both gram-positive and gram-negative bacteria. Considering these qualities, it was found that they may also be integrated to nanofibers. These less molecular weight structures have traditionally been electrospinned after being mixed in polymer solutions. These cationic chemicals reduce the resistance of the electrospinning solutions and produced a 20% drop in fiber diameter, but had no effect on the crystallinity of the generated fibers [122]. It should be emphasized that in aqueous solutions, such mixing nearly invariably leads to the quick active release of the drug from the nanofibers. But, some of the biocides (e.g., chlorhexidine) have functional groups that might be employed to the fiber surface and slow down the release process [123]. The multiple benefits of the electrospinning approach have resulted in the creation of nanofibers employing a diverse spectrum of polymeric solutions [53,54,55,56]. So, the current research is concentrating on the use of biodegradable polymers in the development of different biomedical applications [57,58,59,60,61,62,63,64,65]. Biodegradable and biocompatible polymers that are often used to create nanofibers today [66,67,68,69,70,71,72,73]. Using water as a medium and then solidifying electrospun materials to increase their stability in bodily fluids is an alternative to using harmful solvents. Because of this, non-toxic solvents are frequently utilized in cell-electrospinning and bio-electrospraying techniques to fabricate biological structures utilizing natural polymers [124]. The bioactive compound is surface immobilized in drug delivery devices following electrospinning. By avoiding the direct interaction of the key molecule with the nonaqueous solvent, unintended molecular degradation can be prevented [125]. In the current years, it has been proven that nanometer electrospun fiber could be efficient antimicrobial fiber since their physical and chemical characteristics can be tuned to numerous applications needing essential and biological activity [78]. Because it has non-toxicity, non-mutagenicity, and non-immunogenicity, electrospun materials polymers are being extensively used. One of the most well-known natural polysaccharides is chitosan, a partly N-deacetylated chitin derivative. It is the only positively charged natural alkaline polysaccharide that has been reported and is made up of random combinations of d-glucosamine and N-acetyl-d-glucosamine connected by a (1–4) bond in the polymer backbone [126]. An amino group is located at the C-6 position of this polymer, while primary and secondary hydroxyl groups are located at the C-6 and C-3 locations, respectively. It can transform glucosamine molecules into the soluble form of R-NH3 [127]. A detailed examination of the available literature data revealed that the most prevalent antimicrobial nanofibers based on chitosan incorporated antibacterial agents such as metal/metal nanoparticles, antibiotics, or biologically active particles [128]. With the inclusion of AgNPs, researchers were able to create nanofibrous chitosan/polyvinyl alcohol (PVOH) fibers. The antibacterial test revealed that these fibers had adequate resistance to E. coli, and bacterial mortality was observed to be lowered with increasing chitosan concentration (above 20%) in the system. Some years back, there were results of easy biomedical devices with two layers, the first of electrospun chitosan/TiO2 fibers and the second of adipose tissue extracellular matrix [129]. It has been demonstrated that adding metallic ZnO to chitosan-based fibers considerably improves their antibacterial properties. Chitosan fibers were shown to have minimum inhibitory concentrations (MIC) of 130 and 190 m/ml for E. coli and Candida albicans, respectively. For E. coli and Candida albicans, the composite fibers had reduced MIC values (110 and 160 m/ml, respectively). Moreover, chitosan has been suggested as a matrix for garcinia extract electrospinning. This material was put onto an electrospun fiber of chitosan/EDTA/PVA and the bactericidal action against S. aureus and E. coli was well documented [130, 131]. Mixing antibiotics to a polymer solution before electrospinning is a straight way to load large doses of pharmaceuticals onto any polymer nanofiber, but this procedure has a significant downside. Several studies have demonstrated that nanofiber antibiotics leach fast in aqueous solutions, a process known as burst release. To give a more prolonged release, many ways have been employed. The coaxial electrospinning method, the one solution includes a polymer and the other solution contains an antibiotic, is one preferred way. Another method for achieving prolonged release is to encapsulate or adsorb the medication into a nanomaterial before dissolving in the polymer solution. Taking these qualities into consideration, it was discovered that they may also be integrated into nanofibers [122, 132]. Table 1 highlights the new recent improvements in the novel nanofibers in terms of various types of polymers employed and applications addressed.
Types of Nanofibers Composite Reported in Medication Delivery
Nanocomposite materials consist of anisotropic and inhomogeneous materials in nature. A composite material is formed by combining at least two synthetic or natural components, often with opposing chemical or physical properties, to form a stronger new material [133]. Nonetheless, the material does not completely mix or lose their distinct nature, rather, they integrate and contribute their most advantageous features to improve the result or final product. Composite materials are classified based on their composition, which is separated into two types, base raw and filler material [134]. In general, the base material that interacts or holds the filler material together is called as a matrix or a binder, while the filler materials can be known in the presence of natural and synthetic materials in the form of fibers, filaments, particles, sheets, or fragments [134]. As shown in Fig. 4, fiber is an excellent example of a filler that has been incorporated with a base material to create fiber-reinforced materials. According to the matrix component, composite nanofibers may be categorized into three categories: polymer matrix composites such as PVA/CNT nanofibers [135], composite ceramic matrix materials, for example, collagen/nanohydroxyapatite nanofibers [136], as well as metal matrix composites, such as ZnO/PAN nanofibers [137]. Polymer matrix composites are made up of an organic polymer continuous phase and a reinforced fiber dispersion phase [138]. The spontaneous phase functions as a matrix, keeping the fibers intact and enabling good weight transmission [139, 140]. In the case of ceramic fibers, fibers are placed in a ceramic matrix to create ceramic matrix composites to design non-rigid ceramics [141]. Metal matrix composites are also materials made by adding reinforcement to an alloy or metal matrix in the form of particles, fibers, whiskers, or even sheet metal [142]. Metal-loaded matrix composites provide a wide range of features that surpass rigid initial materials, including strong mechanical forces, resistance to wear, and also well as corrosion [142]. A good composite is chosen based on the applications used. So, polymer-based ceramic nanofiber composites might be a great option for medical applications where organic and inorganic components offer an important contribute in bone tissue construction. For example, polycaprolactone/hydroxyapatite nanofibers have been employed as a medication carrier for rifampicin for the treat infections of associated with ortho implants [143]. Hydroxyapatite is used because it is a biocompatible ceramic that has been found to improve the bioactivity [143]. Additionally, polymer–polymer nanofiber composites might be useful in soft tissue engineering, for example, created with a hydrophilic intermediate layer comprised a mix of polyvinyl alcohol and silk fibroin, while the top and bottom layers were created separately from polylactic acid and polycaprolactone [144]. As a result, the material selection was exclusively decided by the functional characteristics required for the specific application.
Interest in creating nanofibers using electrospinning techniques for tissue engineering applications (shown Fig. 5) is growing tremendously. These electrospun nanofibers resemble the native materials with nanoscale characteristics. Specific responses for tissue regeneration are offered by extra cellular matrix. Moreover, they show a high surface area-to-volume ratio due to their high porosity and interconnecting fibers, which change the chemical and physical characteristics of the polymer composite. Moreover, the scaffolds’ three-dimensional structure offers a transitional support for cell migration, proliferation, and adhesion in addition to having favorable mechanical qualities for medical applications. The inclusion of additional materials to the scaffolds in tissue engineering applications enables the development of hybrid composite nanofibers with desired qualities. When polymer-based nanofibers are combined with biocompatible, natural materials, the resulting architecture creates scaffolds with great mechanical strength and that also biomimetic and have bio functional properties that may mirror those of genuine bone. The recent discovery of bone tissue engineering as a new medical preliminary strategy to treat tissue repair by encouraging the formation and proliferation of bone cells while providing a unique substrate for tissue repair at the facture site (Shrestha et al. 2016b) [145].
Drug delivery is employed electrospun materials to achieve controlled drug release. Using electrospun fibers for drug delivery applications has some unique advantages, including efficient drug loading and encapsulation, diversity of material selection to be compatible with various drugs, simple modulation of the release rate, and simple processability. Specific attention is given to common mechanisms of sustaining the release of drugs loaded in the fiber-based formulations. The release mechanism is simply defined as “the way in which drug molecules are transported or released.” Understanding the release mechanisms is a key step to developing the DDS dosage form. Regardless of the dosage forms, different release mechanisms or rate controlling processes in the polymeric DDSs have been reported in the literature, mainly including dissolution of the drug, diffusion through water-filled pores, diffusion through the polymer matrix, degradation, erosion, swelling, and osmotic pumping. However, the three main release mechanisms associated with drug release from common dosage forms are diffusion (through water-filled pores or the polymer bulk), degradation/erosion, and osmotic pumping. Among these mechanisms, the degradation/erosion does not require drug transport within the polymeric matrix, whereas in the other ones, the drug molecule transport is to be released. In diffusion-controlled rate systems, the drug molecules randomly move out of the device through a difference of chemical potential as a driving force. The diffusion can occur within a polymer matrix or across a polymeric membrane, which surrounds a drug reservoir core [125, 146].
The primary account of functionalization that offers good benefits in incorporating the hydrophobic and hydrophilic drugs, particularly in the fast dissolving drug delivery materials, is the incorporation of different active agents through direct mixing with the electrospun solution. To this aim, responsible efforts are being made to create electrospun nanofiber-based rapid dissolving drug delivery systems based on different hydrophilic polymers and drug molecules for a range of medical uses. Early work in this area addressed the construction of rapid delivery of drugs systems for poorly soluble pharmaceuticals using electrospinned blend solution of ibuprofen and polyvinylpyrrolidone (K30) polymer as model drug carriers. Solution of electrospinning was made by dissolving polyvinylpyrrolidone K30 and ibuprofen in ethanol and setting the concentration of polymer at 30% (w/v), and the concentration of drug was 7.5% (w/v), which was utilized in the electrospinning process. From the insight into the thermal degradation, morphology, and crystalline nature of the drug, the interaction of drug molecule with polymer was characterized using a polarized optical microscope, scanning electron microscope (SEM), differential scanning calorimetry (DSC), and Fourier transform infrared (FT-IR) spectroscopy. Additionally, the wetting and dissolution behavior of the nanofibers encapsulated has been researched to better understand their rapid dissolving property and the related results indicated the nanofibers were enclosed tightly. Additional drug release was determined to be 84.9% and 58.7%, respectively, within the first 20 s, with total dissolution reached in 40 and 60 s [147]. Electrospinning is an excellent method for encapsulating several drugs in to their fibers for various medical purposes. An effort has been made to show the encapsulation of paracetamol and caffeine in polyvinylpyrrolidone fibers through electrospinning and their potential in oral rapid dissolving films [148]. PVA nanofibers encapsulated with riboflavin and caffeine as model medicines for oral rapid dissolving delivery systems with dissolution and wetting times of roughly 1.5 and 4.5 s, respectively [149], was proposed. Natural biopolymers have recently received a lot of attention as a drug carrier compared to the synthetic or semisynthetic polymers. The encapsulation of medication in pullulan/chitosan composite nanofiber through electrospinning is a unique model in the production of oral fast dissolving films [150]. Recognizing the various advantages of electrospinning technology that offers promise in several applications, considerable interest is continuously seen in the modification of conventional electrospinning setups. Coaxial electrospinning is a cutting-edge technique that involves the continuous flow of various solutions through distinct coaxial capillaries, resulting in the physical separation of core/shell fibers. Many processing factors impact coaxial electrospinning in the same way as they do ordinary electrospinning. The creation of core/shell fibers has broad implications for the development of drug delivery systems with a burst or sustained release characteristics. Furthermore, with the help of spinning shell polymer, active substances that do not develop fibrous nature can be contained in the core of the fiber additionally, the method has the advantage of encapsulating two or more drug molecules with varying solubilization and biological activity into a single delivery system. As a result, given all of the merits of coaxial electrospinning, the technique has been widely adopted in the formation of drug delivery systems [151, 152]. As a result, rapid dissolving medication delivery devices have been developed utilizing this method. In this context, a specific demonstration employed a coaxial electrospinning method to construct a rapid dissolving system encapsulated with the weakly water-soluble medicinal quercetin [153] was reported. Emulsion electrospinning gives a possible alternative, enabling the formation of core–shell nanofibers by encapsulation of the drug inside micelles. Usually, the formation of drug-containing micelles occurs by addition of a supernatant to a water solution of the drug itself. Vigorous mixing of the so-formed micelles with an oil solution of the polymer forms a stable emulsion suitable for electrospinning. The advantages are mainly two: the first is a minimized contact of the bioactive molecule and the organic solvent, allowing the use of various combinations of hydrophilic drugs and hydrophobic polymers and the second advantage is due to the easy formation of uniform core–shell structure without the use of specific coaxial apparatus. Another approach for drug loading involves surface immobilization of the bioactive molecule after the electrospinning process. Thus, it is possible to avoid every contact between the active molecule and the organic solvent, preventing any undesired degradation. Another advantage is the preservation of the original degradation and mechanical proprieties of the polymeric matrix. However, achieving a longer release over time requires strong non-covalent bonding between the polymer and the drug and usually a cross-linking process. Another strategy adopted for the fabrication of fast dissolving oral involves the supramolecular complexation of drugs before the spinning process. The use of cyclodextrin allowed the formation of a complex with hydrocortisone, before the direct spinning of the solution. The so-formed cyclodextrin-hydrocortisone fibers proved to be a very promising material for oral delivery application due to the increase in solubility and fast dissolution [4]. Table 2 summarizes the wound dressing, tissue engineering, and bone regeneration in applications of various polymer-based electrospun nanofibers and fiber mats utilized as topical drug delivery. Despite their various shortcomings in manufacturing, biopolymer nanoparticles can transport bioactive chemicals to target tissues and cells. Drug-loading capacity and wide size dispersion are the advantages. Furthermore, because biopolymer-based nanoparticles can be tailored to certain sizes, they may be sustained for an extended length of time, making them an appealing therapeutic agent for drug delivery. Figure 6 depicts a schematic representation of drug loading in nanocomposites and the drug delivery mechanism. Plant-derived polysaccharides and animal-derived proteins make biopolymers. Silk, gelatin, collagen, and albumin are the most common proteins used in the drug delivery.
In Vitro Studies on Drug Release
The practical applications of drug release have been reported in the literature to help readers to identify such uses some case studies have been given here. To fully understand the ciprofloxacin release, two sets of in vitro drug-release experiments were performed [154]. First, a modified paddle technique for single-medium dissolution (pH 7.4 PBS) was used to measure the drug release from NF6 nanofibers containing ciprofloxacin comparable to with its corresponding physical combination and a raw ciprofloxacin powder. At 37 °C, PBS medium was used for the release studies. At 100 rpm, the paddle was rotating. The buffer solution was then manually sampled at intervals of 5, 10, 15, 30, 60, and 90 min, after sampling, new PBS was added to the volume and followed by a UV–Vis spectrophotometer with a maximum wavelength of 275 nm. The calibration curve of ciprofloxacin in pH 7.4 PBS was used to compute the cumulative ciprofloxacin release of 25 to 100%. The average results and standard deviations for each experiment were carried out in triplicate and the average values are reported [154]. In addition, the aforementioned Hanson dissolution tester explored a two-stage release test as a biorelevant gastrointestinal transfer methodology to better replicate the in vivo circumstances. As the nanofibers included 1w/w% ciprofloxacin, a part of 25-mg ciprofloxacin powder was compared to a mass of NF6 electrospun sample that was 100 times bigger. Following the addition of the samples to 25 ml of FaSSGF, 2-ml aliquots were obtained at the following time intervals 1, 3, 5, 10, 15 and 30 min. Twenty-five milliliters of FaSSIF concentrate was swiftly injected into the stomach media as a bolus just after the previous sample. The buffer strength and surfactant concentration of the FaSSIF concentrate are twice as strong as those of the normal FaSSIF. In this manner, the final dissolving medium will be the standard FaSSIF after adding 25 ml of FaSSIF concentrate to 25 ml of FaSSGF. J.Mann et al. have reported the process and preparation of the FaSSIF concentrate. After the medium change, 2-ml aliquots were sampled at 1, 3, 5, 10, 15, 30, and 60 min. Fresh FaSSIF media was used to replace each volume that was taken. During the experiment, the temperature in the dissolving containers was thermostatic at 37 °C and the paddle speed was set at 100 rpm. Similar to the previous release research, the absorbance values obtained by UV–Vis spectrophotometry at a maximum of 277 nm and 272 nm in the case of the FaSSGF and FaSSIF medium, respectively, were used to determine the cumulative drug release (25 to100%). The results and standard deviations for each experiment were carried out in triplicate are presented [154]. In vitro diffusion investigation was made by the use of the Franz diffusion cell. The receptor compartment was held at 370 °C and filled with 20 ml of acetate buffer at a pH of 5.5. An improved nanofiber sample was kept in the donor compartment over a dialysis membrane. The 1-ml aliquot was taken out and replaced after a reasonably long period of time with a fresh buffer solution held at the same temperature. The substance was tested in triplicate at 336 nm with a UV spectrophotometer [155].
Utilizing a diffusion method at a pH of 5.5 piroxicam-loaded nanofiber patches were subjected to in vitro drug-release tests. Based on the results, it was discovered that the pH 5.5 was used to control the in vitro drug release. Drug release from PRX 1, PRX2, PRX3, PRX4, and PRX5 formulations in an acetic buffer with a pH of 5.5 was 84.65%, 86.78%, 91.96%, 94.86%, and 87.88%, respectively. Researchers observed the release of piroxicam from nanofiber patches during a 12-h period in a pH 5.5. The formulation PRX4 showed a greater release rate than the other formulations evaluated between PRX1 and PRX5 [156].
Study of the Kinetics and Mechanism of Drug Release
The dissolving kinetics of the ciprofloxacin powder were compared to the release kinetics of ciprofloxacin from the electrospun nanofiber and the physical mixture. The acquired cumulative drug release and time curves were fitted with five different mathematical models: (1) zero-order, (2) first-order, (3) Hixson–Crowell, (4) Higuchi, and (5) Korsmeyer–Peppas model to characterize the kinetics. The regression coefficient (R2) value was calculated and compared in order to assess which model was used [121].
In Vitro Diffusion Study
An essential approach for foretelling how a medicine would act in vivo is in vitro diffusion profiling. The outcomes of the in vitro skin permeation tests of the curcumin from nanofiber transdermal patches at 24 h was done. The total quantity of drug diffusion from the 17.5 weight percentage cellulose acetate phthalate formulation was 309.02 µg/cm2. Mixed zero-order/ first-order kinetics were used to determine the cumulative quantity of medication that permeated through the pig skin per square centimeter of patch over time. The in vitro diffusion profiles for the formulations did not fit closely with either zero-order (r2 = 0.8962) or first-order kinetics (r2 = 0.973), which indicates that drug permeation from the patch is governed by a diffusion mechanism. As many diffusion processes can be represented by coupling of a Fickian and non-Fickian mechanism, to describe the controlled diffusion of drugs from polymer matrices, Ritger and Peppa introduced the power law equation Mt/M∞) = Ktn, where Mt is the amount of drug released at time t, M∞ is the nominal total amount of drug released at K the kinetic constant, and n is the diffusion exponent that is used to characterize the release mechanism. The value of n can be calculated from the slope of ln(Mt/M∞) versus lnt and can indicate the operating diffusion mechanism. The Fickian mechanism predominated in all formulated nanofibers, according to the n value (0.504) determined using this equation. In this situation, the Fickian mechanisms findings confirm those of Higuchis equation. As a result, the patches show a drug delivery mechanism that is dominated by diffusion [156].
Theoretical Studies on Polymer-Based Nanofiber
Complexes made of ampicillin and starch in various combinations are reported. This system has been successfully tested with the B3LYP basis set calculations. There was no fictitious frequency in this case. They calculated three typical configurations of complexes formed from ampicillin and starch. The total energies for configurations was − 4003.999471, − 4003.999251, and − 4003.986094 a.u. The complexes with the selective configurations appear to be more stable than the complex with the other configuration. In addition, hydrogen bonding interactions can be attributed to the OH bond lengths vary from 1.8 to 2.9 Å. Between starch and ampicillin, there are 9, 9, and 3 hydrogen bonds, respectively. To sum up the oxygen atoms in carbonyl, the oxygen atoms and hydrogen atoms in carboxyl and the hydrogen atoms in the benzene ring are the active sites for ampicillin molecules. The hydrogen atoms and oxygen atoms in starch molecules act as also active sites [157].
The models from hydrophilic peptide show an indirect relationship between biological activity and the molecular properties of the octanol–water partition coefficient (logP), the ΔGAP energy (ΔGapE) and therefore the potential of ionization.
However, the HOMO orbital energy (EHOMO), total absolute charge, and Ghose–Crippen molar refractivity (AMR) are terms that have been specifically linked to the activity and affinity. Biological activity is described by ADME model. The thermodynamic and transport properties of the molecular system, topological, and molecular descriptors that were employed in the simulation algorithm analysis. The thermodynamic and transport characteristics of a chemical system are influenced by the Van der Waals interactions, also known as London scattering attractions, which connect the molecule electronic polarizability and molar refractivity. AMR is a constitutive additive characteristic that may be calculated to take into account atom-level contributions, connectivity, and several other corrective factors. AMR has historically made major contributions to the study of electron binding in organic molecules, making it a vital physical–chemical parameter can be effectively used to predict the binding and delivery of the drug with nanofibers in future [158].
Future Outlooks
The negative problems relating to the electrospun nanofibers could be solved using a thorough and organized theoretical methodology. In future, medical treatment may find useful to treat patients using the tailored scaffolds with combined tissue engineering and precise medication release using nanofibrous materials. Customized nanofiber with distinctive qualities and simplicity of application might become more significant in personalized treatment very soon. The development of several platforms for drug delivery technologies has advanced significantly as a result of the introduction of diverse nanofiber manufacturing processes. Although these technologies have advanced significantly recently, still certain restrictions are there. Leading research in solution blowing, electrospinning, centrifugal spinning making its way to large-scale manufacturing and certain systems are already in the pipeline. Even though these cutting-edge approaches have demonstrated considerable potential in generating uniform and continuous fibers, the intricate, multifarious working solution parameters and associated elements affect fiber manufacturing should be addressed. As a result of these factors, the uses of nanofibers through preclinical and clinical examination to aid the process to the medical treatment is warranted.
Conclusion
In conclusion, the review gives a general overview of electrospun nanofiber-based drug delivery systems, focusing on their distinguishing characteristics, such as their large surface area, high porosity, excellent drug encapsulation characteristics through various methods, and controlled release. Also, this study summarized recent developments in the creation and use of hydrogel-based biomedical nanofiber, with a particular focus on drug-release functionality. The electrospun composite biomaterials for regenerative medicine, medication delivery, tissue engineering, and other uses are discussed in various aspects. For example, the application stars from wound healing. The review also looked at the list of synthetic polymers, natural polymers, and polymer-free nanofibers used in the creation of the drug delivery systems, by acknowledging their hydrophilic nature and capacity to form a hydrogen bond with encapsulated drugs that attempt to achieve uniform drug distribution and release of drugs which results in enhanced therapeutic effectiveness. It has become quite common to use electrospun biodegradable polymer networks embedded in hydrogels made of polysaccharides is also discussed. The nanofibrous created by conventional electrospinning may deliver drugs with targeted drug delivery in response to pH conditions and can give quick and prolonged drug release is noted. Coaxial electrospinning can create materials with several uses is highlighted. Creating intelligent and regulated medication delivery systems is simple and convenient using electrospinning method is explored. Electrospinning potential uses virtually endless and serve as a great foundation for the creation of novel drug delivery systems that maximize therapeutic benefit while reducing negative effects are the points highlighted in the various sections of this review. A drug-loaded electrospun fiber patches may be a practical place to begin exploring for a novel platform that is optimized for drug delivery and compatibility with transdermal enhancers. Additionally, it exhibits improved diffusion, lowers the dosage frequency and improves patient compliance, and produces powerful controlled release patches when applied topically. So, the kinetics of drug delivery is discussed in a variety of situations, chemical reactivity has been effectively justified and explained using quantum reactivity. As a result, these zones show a positive area that electrophile groups can assault. The release mechanism characteristics of polymer-based drug delivery systems have been extensively studied using DFT. It is anticipated that increased multidisciplinary efforts for the future of nanomedicine from the atomic perspective at a low cost with accurate and reliable quantum mechanics calculations will be stimulated by the logic of rational drug delivery systems and the continuous improvement in computing power of DFT is taken into account finally. Thus, this review offers the guide to the researchers in biomedical materials and drug delivery systems.
Data availability
Manuscript has no associated data.
References
S. Eskitoros-Togay, Y. Melda, E. Bulbul, S. Tort, F.D. Korkmaz, F. Acartürk, N. Dilsiz, Fabrication of doxycycline-loaded electrospun PCL/PEO membranes for a potential drug delivery system, Int. J. Pharm. 565, 83–94 (2019). https://doi.org/10.1016/j.ijpharm.2019.04.073
K. Ghosal, C. Agatemor, Z. Špitálsky, S. Thomas, E. Kny, Electrospinning tissue engineering and wound dressing scaffolds from polymertitanium dioxide nanocomposites. Chem. Eng. J. 358, 1262–1278 (2019). https://doi.org/10.1016/j.cej.2018.10.117
A. Khalf, S.V. Madihally, Recent advances in multiaxial electrospinning for drug delivery. Eur. J. Pharm. Biopharm. 112, 1–17 (2017). https://doi.org/10.1016/j.ejpb.2016.11.010
H. Chen, N. Wang, J. Di, Y. Zhao, Y. Song, L. Jiang, Nanowire-in-microtube structured core/shell fibers via multifluidic coaxial electrospinning, Langmuir 26(13), 11291–11296 (2010). https://doi.org/10.1021/la100611f
A.J. Meinel, O. Germershaus, T. Luhmann, H.P. Merkle, L. Meinel, Electrospun matrices for localized drug delivery: current technologies and selected biomedical applications. Eur. J. Pharm. Biopharm. 81(1), 1–13 (2012)
S.M. Shahriar, J. Mondal, M.N. Hasan, V. Revuri, D.Y. Lee, Y.-K. Lee, Electrospinning nanofibers for therapeutics delivery. Nanomaterials 9(4), 532 (2019)
Y. Ding, W. Li, F. Zhang, Z. Liu, N.Z. Ezazi, D. Liu, H.A. Santos, Electrospun fibrous architectures for drug delivery, tissue engineering and cancer therapy, Adv. Funct. Mater. 29(2), 1802852, https://doi.org/10.1002/adfm.201802852 (2019)
R. Augustine, A.A. Zahid, A. Hasan, M. Wang, T.J. Webster, CTGF loaded electrospun dual porous core-shell membrane for diabetic wound healing, Int. J. Nanomed. 14, 8573 (2019). https://doi.org/10.2147/IJN.S224047
E.J. Torres-Martínez, J.M.C. Bravo, A.S. Medina, G.L.P. González, L.J.V. Gómez, A summary of electrospun nanofibers as drug delivery system: drugs loaded and biopolymers used as matrices. Curr. Drug Deliv. 15 (10), 1360–1374 (2018)
D. Han, A.J. Steckl, Triaxial electrospun nanofiber membranes for controlled dual release of functional molecules. ACS Appl. Mater. Interfaces 5(16), 8241–8245 (2013). https://doi.org/10.1021/am402376c
Alejandro Sosnik, Robin Augustine, Challenges in oral drug delivery of antiretrovirals and the innovative strategies to overcome them, Adv. Drug Deliv. Rev. 103 105–120, https://doi.org/10.1016/j.addr.2015.12.022 (2016)
K. Ghosal, S. Adak, C. Agatemor, G. Praveen, N. Kalarikkal, S. Thomas, Novel interpenetrating polymeric network-based microbeads for delivery of poorly water-soluble drug, J. Polym. Res. 27(4), 1–11 (2020). https://doi.org/10.1007/s10965-020-02077-6
A. Furmhals, US Patent 1,975,504 (1934)
Z.M. Huang, Y.Z. Zhang, M. Kotaki, S. Ramakrishna, A review on polymer nanofibers by electrospinning and their applications in nanocomposites. Compos. Sci. Technol. 63, 2223–2253 (2003)
B. Wang, Y. Wang, T. Yin, Q. Yu, Applications of electrospinning technique in drug delivery. Chem. Eng. Commun. 197, 1315–1338 (2010)
S. Chakraborty, I.C. Liao, A. Adler, K.W. Leong, Electrohydrodynamics: a facile technique to fabricate drug delivery systems. Adv. Drug Deliv. Rev. 61, 1043–1054 (2009)
S. Liu, G. Zhou, D. Liu, Z. Xie, Y. Huang, X. Wang, W. Wu, X. Jing, Inhibition of orthotopic secondary hepatic carcinoma in mice by doxorubicin-loaded electrospun polylactide nanofibers. J. Mater. Chem. B. 1, 101–109 (2013)
M. Zamani, M.P. Prabhakaran, S. Ramakrishna, Advances in drug delivery via electrospun and electrosprayed nanomaterials. Int. J. Nanomed. 8, 2997–3017 (2013)
M. Prabaharan, R. Jayakumar, S.V. Nair, Electrospun nanofibrous scaffolds—current status and prospects in drug delivery. Adv. Polym. Sci. 246, 241–262 (2012)
Y.Z. Zhang, C.T. Lim, S. Ramakrishna, Z.M. Huang, Recent development of polymer nanofibers for biomedical and biotechnological applications. J. Mater. Sci. Mater. Mech. 16, 933–946 (2005)
N. Hasirci, Micro and nano systems in biomedicine and drug delivery, in Nanomaterials and Nanosystems for Biomedical Applications, ed. by Mozafari, M.R. (Springer, Dordrecht, 2007), pp. 1–26
R. Vecchione, V. Quagliariello, P. Giustetto, D. Calabria, A. Sathya, R. Marotta, M. Profeta, S. Nitti, N. Silvestri, T. Pellegrino et al., Oil/water nano-emulsion loaded with cobalt ferrite oxide nanocubes for photo-acoustic and magnetic resonance dual imaging in cancer: in vitro and preclinical studies. Nanomed. Nanotechnol. Biol. Med. 13, 275–286 (2017)
E. Lagreca, V. Onesto, C. Di Natale, S. La Manna, P.A. Netti, R. Vecchione, Recent advances in the formulation of PLGA microparticles for controlled drug delivery. Prog. Biomater. 9, 153–174 (2020)
C. Di Natale, E. Lagreca, V. Panzetta, M. Gallo, F. Passannanti, M. Vitale, S. Fusco, R. Vecchione, R. Nigro, P. Netti, Morphological and rheological guided design for the microencapsulation process of Lactobacillus paracasei CBA L74 in calcium alginate microspheres. Front. Bioeng. Biotechnol. 9, 660691 (2021)
S.A. Strobel, K. Hudnall, B. Arbaugh, J.C. Cunniffe, H.B. Scher, T. Jeoh, Stability of fish oil in calcium alginate microcapsules cross-linked by in situ internal gelation during spray drying. Food Bioprocess Technol. 13, 275–287 (2020)
M.T. Safian, K. Umar, T. Parveen, A.A. Yaqoob, M.N.M. Ibrahim, Eight-biomedical applications of smart polymer composites, in Smart Polymer Nanocomposites: Biomedical and Environmental Applications (Elsevier, Cambridge, 2021), pp. 183–204
P. Chakraborty, H. Oved, D. Bychenko, Y. Yao, Y. Tang, S. Zilberzwige-Tal, G. Wei, T. Dvir, E. Gazit, Nanoengineered peptide-based antimicrobial conductive supramolecular biomaterial for cardiac tissue engineering. Adv. Mater. 33, 2008715 (2021)
S. Kang, S. Hou, X. Chen, D.G. Yu, L. Wang, X. Li, G.R.R. Williams, Energy-saving electrospinning with a concentric Teflon-core rod spinneret to create medicated nanofibers. Polymers 12, 2421 (2020)
A. Sionkowska, Collagen blended with natural polymers: recent advances and trends. Prog. Polym. Sci. 122, 101452 (2021)
A.A. Yaqoob, M.T. Safian, M. Rashid, T. Parveen, K. Umar, M.N.M. Ibrahim, Introduction of smart polymer nanocomposites, in Smart Polymer Nanocomposites: Biomedical and Environmental Applications (Elsevier, Cambridge, 2021), pp. 1–25
K. Jung, N. Corrigan, E.H.H. Wong, C. Boyer, Bioactive synthetic polymers. Adv. Mater. 34, 2105063 (2021)
K. Joyce, G.T. Fabra, Y. Bozkurt, A. Pandit, Bioactive Potential of natural biomaterials: identification, retention and assessment of biological properties. Signal Transduc. Target. Ther. 6, 1–28 (2021)
T. Rosén, B.S. Hsiao, L.D. Söderberg, Elucidating the opportunities and challenges for nanocellulose spinning. Adv. Mater. 33, 2001238 (2021)
M. Dziadek, K. Dziadek, K. Checinska, B. Zagrajczuk, M. Golda-Cepa, M. Brzychczy-Wloch, E. Menaszek, A. Kopec, K. Cholewa-Kowalska, PCL and PCL/bioactive glass biomaterials as carriers for biologically active polyphenolic compounds: comprehensive physicochemical and biological evaluation. Bioact. Mater. 6, 1811–1826 (2021)
M. Janmohammadi, M.S. Nourbakhsh, Electrospun polycaprolactone scaffolds for tissue engineering: a review. Int. J. Polym. Mater. Polym. Biomater. 68, 527–539 (2019)
N. Bu, Y. Huang, X. Wang, Z. Yin, Continuously tunable and oriented nanofiber direct-written by mechano-electrospinning. Mater. Manuf. Process. 27, 1318–1323 (2012)
S.L. Tao, T.A. Desai, Aligned arrays of biodegradable poly(ε-caprolactone) nanowires and nanofibers by template synthesis. Nano Lett. 7, 1463–1468 (2007)
H.S. Liao, J. Lin, Y. Liu, P. Huang, A. Jin, X. Chen, Self-assembly mechanisms of nanofibers from peptide amphiphiles in solution and on substrate surfaces. Nanoscale 8, 14814–14820 (2016)
L. Li, J. Ge, L. Wang, B. Guo, P.X. Ma, Electroactive nanofibrous biomimetic scaffolds by thermally induced phase separation. J. Mater. Chem. B 2, 6119–6130 (2014)
C. Zhang, Y. Li, P. Wang, H. Zhang, Electrospinning of nanofibers: potentials and perspectives for active food packaging. Compr. Rev. Food Sci. Food Saf. 19, 479–502 (2020)
J. Jin, Z.Q. Shi, C.Y. Wang, Electrochemical performance of electrospun carbon nanofibers as free-standing and binder-free anodes for sodium-ion and lithium-ion batteries. Electrochim. Acta 141, 302–310 (2014)
M. Bognitzki, H. Hou, M. Ishaque, T. Frese, M. Hellwig, C. Schwarte, A. Schaper, J.H. Wendorff, A. Greiner, Polymer, metal, and hybrid nano- and mesotubes by coating degradable polymer template fibers (TUFT process). Adv. Mater. 12, 637–640 (2000)
W. Liu, M. Graham, E.A. Evans, D.H. Reneker, Poly (meta-phenylene isophthalamide) nanofibers: coating and post processing. J. Mater. Res. 17, 3206–3212 (2002)
H. Hou, Z. Jun, A. Reuning, A. Schaper, J.H. Wendorff, A. Greiner, Poly(p-xylylene) nanotubes by coating and removal of ultrathin polymer template fibers. Macromolecules 35, 2429–2431 (2002)
J. Song, Q. Deng, M. Huang, Z. Kong, Carbon nanotube enhanced membrane distillation for salty and dyeing wastewater treatment by electrospinning technology. Environ. Res. 204, 111892 (2022)
D. Xu, Y. Chen, T. Qiu, S. Qi, L. Zhang, M. Yin, K. Ge, X. Wei, X. Tian, P. Wang et al., Hierarchical mesoporous SnO2 nanotube templated by Staphylococcus aureus through electrospinning for highly sensitive detection of triethylamine. Mater. Sci. Semicond. Process. 136, 106129 (2021)
A. Ahmad, M.A. Khan, A. Nazir, S.N. Arshad, M.B. Qadir, Z. Khaliq, Z.S. Khan, A.N. Satti, B. Mushtaq, A. Shahzad, Triaxial electrospun mixed-phased TiO2 nanofiber-in-nanotube structure with enhanced photocatalytic activity. Microporous Mesoporous Mater. 320, 111104 (2021)
C. Chang, V.H. Tran, J. Wang, Y.-K. Fuh, L. Lin, Direct-write piezoelectric polymeric nanogenerator with high energy conversion efficiency. Nano Lett. 10, 15 (2010)
S. Mansouri, T.F. Sheikholeslami, A. Behzadmehr, Investigation on the electrospun PVDF/NP-ZnO nanofibers for application in environmental energy harvesting. J. Mater. Res. Technol. 8, 1608–1615 (2019)
A.G. MacDiarmid, W.E. Jones, I.D. Norris, J. Gao, A.T. Johnson, N.J. Pinto, J. Hone, B. Han, F.K. Ko, H. Okuzaki et al., Electrostatically-generated nanofibers of electronic polymers. Synth. Met. 119, 27–30 (2001)
D. Gandavadi, S. Sundarrajan, S. Ramakrishna, Bio-based nanofibers involved in wastewater treatment. Macromol. Mater. Eng. 304, 1–15 (2019)
A.R. Wassel, M.E. El-Naggar, K. Shoueir, Recent advances in polymer/metal/metal oxide hybrid nanostructures for catalytic applications: a review. J. Environ. Chem. Eng. 8, 104175 (2020)
D. Sharma, B.K. Satapathy, Optimization and physical performance evaluation of electrospun nanofibrous mats of PLA, PCL and their blends. J. Ind. Text (2020). https://doi.org/10.1177/1528083720944502
B.J. Kim, H. Cheong, E.S. Choi, S.H. Yun, B.H. Choi, K.S. Park, I.S. Kim, D.H. Park, H.J. Cha, Accelerated skin wound healing using electrospun nanofibrous mats blended with mussel adhesive protein and polycaprolactone. J. Biomed. Mater. Res. Part A 105, 218–225 (2017)
L.D. De Carvalho, B.U. Peres, H. Maezono, Y. Shen, M. Haapasalo, J. Jackson, R.M. Carvalho, A.P. Manso, Doxycycline release and antibacterial activity from PMMA/PEO electrospun fiber mats. J. Appl. Oral Sci. 27, 1–10 (2019)
K. Kurpinski, S. Patel, Dura mater regeneration with a novel synthetic, bilayered nanofibrous dural substitute: an experimental study. Nanomedicine 6, 325–337 (2011)
K. Shoueir, S. Kandil, H. El-hosainy, M. El-Kemary, Tailoring the surface reactivity of plasmonic Au@TiO2 photocatalyst bio-based chitosan fiber towards cleaner of harmful water pollutants under visible-light irradiation. J. Clean. Prod. 230, 383–393 (2019)
Z.A. Al-Ahmed, B.A. Al Jahdaly, H.A. Radwan, A.A. Hassana, A. Almahri, M.K. Ahmed, M.M. Taher, Electrospun nanofibrous scaffolds of ε-polycaprolactone containing graphene oxide and encapsulated with magnetite nanoparticles for wound healing utilizations. Mater. Res. Express 8, 025013 (2021)
A. Farboudi, K. Mahboobnia, F. Chogan, M. Karimi, A. Askari, S. Banihashem, S. Davaran, M. Irani, UiO-66 metal organic framework nanoparticles loaded carboxymethyl chitosan/poly ethylene oxide/polyurethane core-shell nanofibers for controlled release of doxorubicin and folic acid. Int. J. Biol. Macromol. 150, 178–188 (2020)
H.S. Sofi, T. Akram, A.H. Tamboli, A. Majeed, N. Shabir, F.A. Sheikh, Novel lavender oil and silver nanoparticles simultaneously loaded onto polyurethane nanofibers for wound-healing applications. Int. J. Pharm. 569, 118590 (2019)
A. Ullah, S. Ullah, M.Q. Khan, M. Hashmi, P.D. Nam, Y. Kato, Y. Tamada, I.S. Kim, Manuka honey incorporated cellulose acetate nanofibrous mats: fabrication and in vitro evaluation as a potential wound dressing. Int. J. Biol. Macromol. 155, 479–489 (2020)
C.H. Lee, K.S. Liu, C.W. Cheng, E.C. Chan, K.C. Hung, M.J. Hsieh, S.H. Chang, X. Fu, J.H. Juang, I.C. Hsieh et al., Codelivery of sustainable antimicrobial agents and platelet-derived growth factor via biodegradable nanofibers for repair of diabetic infectious wounds. ACS Infect. Dis. 6, 2688–2697 (2020)
K. Kalantari, A.M. Afifi, H. Jahangirian, T.J. Webster, Biomedical applications of chitosan electrospun nanofibers as a green polymer—review. Carbohydr. Polym. 207, 588–600 (2019)
A. Cordoba, C. Saldias, M. Urz, M. Montalti, M. Guernelli, M.L. Focarete, A. Leiva, On the versatile role of electrospun polymer nanofibers as photocatalytic hybrid materials applied to contaminated water remediation: a brief review. Nanomaterials 12, 756 (2022)
A. Greiner, J.H. Wendorff, Electrospinning: a fascinating method for the preparation of ultrathin fibers. Angew. Chem. Int. Ed. 46, 5670–5703 (2007)
T. Cheng, R.D. Hund, D. Aibibu, J. Horakova, C. Cherif, Pure chitosan and chitsoan/chitosan lactate blended nanofibres made by single step electrospinning. Autex Res. J. 13, 128–133 (2013)
I. Steyaert, L. Van Der Schueren, H. Rahier, K. De Clerck, An alternative solvent system for blend electrospinning of polycaprolactone/chitosan nanofibres. Macromol. Symp. 321–322, 71–75 (2012)
J. Xu, J. Zhang, W. Gao, H. Liang, H. Wang, J. Li, Preparation of chitosan/PLA blend micro/nanofibers by electrospinning. Mater. Lett. 63, 658–660 (2009)
M. Pakravan, M.C. Heuzey, A. Ajji, A fundamental study of chitosan/PEO electrospinning. Polymer 52, 4813–4824 (2011)
Z. Chen, X. Mo, F. Qing, Electrospinning of collagen–chitosan complex. Mater. Lett. 61, 3490–3494 (2007)
H. Homayoni, S.A.H. Ravandi, M. Valizadeh, Electrospinning of chitosan nanofibers: processing optimization. Carbohydr. Polym. 77, 656–661 (2009)
M. Peesan, R. Rujiravanit, P. Supaphol, Electrospinning of hexanoyl chitosan/polylactide blends. J. Biomater. Sci. Polym. Ed. 17, 547–565 (2006)
C. Kriegel, A. Arrechi, K. Kit, D.J. Mcclements, J. Weiss, Fabrication, functionalization, and application of electrospun biopolymer nanofibers. Crit. Rev. Food Sci. Nutr. 48, 775–797 (2008)
A.K. Azad, S.M.A. Al-Mahmood, J.F. Kennedy, B. Chatterjee, H. Bera, Electro-hydrodynamic assisted synthesis of lecithinstabilized peppermint oil-loaded alginate microbeads for intestinal drug delivery. Int. J Biol. Macromol 185, 861–875 (2021)
M. Licciardello, C. Tonda-Turo, A. Gallina, G. Ciofani, G. Ciardelli, Fabrication of extracellular matrix-like membranes for loading piezoelectric nanoparticles. J Phys. Mater. 3, 034004 (2020)
C.M. Kelleher, J.P. Vacanti, Engineering extracellular matrix through nanotechnology. J. R. Soc. Interface 7, S717–S729 (2010)
A.A. El-Shanshory, M.M. Agwa, A.I. Abd-Elhamid, H.M.A. Soliman, X. Mo, E.R. Kenawy, Metronidazole topically immobilized electrospun nanofibrous scaffold: novel secondary intention wound healing accelerator. Polymers 14, 454 (2022)
N. Hamdan, A. Yamin, S.A. Hamid, W.K.W.A. Khodir, V. Guarino, Functionalized antimicrobial nanofibers: design criteria and recent advances. J. Funct. Biomater. 12, 59 (2021)
Y. Huo, Y. Tan, K. Zhao, Z. Lu, L. Zhong, Y. Tang, Enhanced electromagnetic wave absorption properties of Ni magnetic coating-functionalized SiC/C nanofibers synthesized by electrospinning and magnetron sputtering technology. Chem. Phys. Lett. 763, 138230 (2021)
Y. Wang, Y. Jiang, Y. Zhang, S. Wen, Y. Wang, H. Zhang, Dual functional electrospun core-shell nanofibers for anti-infective guided bone regeneration membranes. Mater. Sci. Eng. C 98, 134–139 (2019)
A. Kopp, R. Smeets, M. Gosau, N. Kröger, S. Fuest, M. Köpf, M. Kruse, J. Krieger, R. Rutkowski, A. Henningsen et al., Effect of process parameters on additive-free electrospinning of regenerated silk fibroin nonwovens. Bioact. Mater. 5, 241–252 (2020)
M.V. Someswararao, R.S. Dubey, P.S.V. Subbarao, S. Singh, Electrospinning process parameters dependent investigation of TiO2 nanofibers. Results Phys. 11, 223–231 (2018)
C. Xue, L.D. Wilson, Preparation and characterization of salicylic acid grafted chitosan electrospun fibers. Carbohydr. Polym. 275, 118751 (2022)
C. Voniatis, D. Barczikai, G. Gyulai, A. Jedlovszky-Hajdu, Fabrication and characterisation of electrospun polycaprolactone/polysuccinimide composite meshes. J. Mol. Liq. 323, 115094 (2021)
Q. Jin, Y. Fu, G. Zhang, L. Xu, G. Jin, L. Tang, J. Ju, W. Zhao, R. Hou, Nanofiber electrospinning combined with rotary bioprinting for fabricating small-diameter vessels with endothelium and smooth muscle. Composites Part B Eng. 234, 109691 (2022)
B.V.D. Voorde, B. Sensu, L.D. Vos, R. Colenbier, H. Baskan, J. Geltmeyer, L. Parmentier, L.V. Daele, R.I. Dmitriev, L. Pyl et al., Electrospinning of poly (decamethylene terephthalate) to support vascular graft applications. Eur. Polym. J. 165, 111003 (2022)
A. Barhoum, K. Pal, H. Rahier, H. Uludag, I.S. Kim, M. Bechelany, Nanofibers as new-generation materials: from spinning and nano-spinning fabrication techniques to emerging applications. Appl. Mater. Today 17, 1–35 (2019)
G. Zhao, X. Zhang, T.J. Lu, F. Xu, Recent advances in electrospun nanofibrous scaffolds for cardiac tissue engineering. Adv. Funct. Mater. 25, 5726–5738 (2015)
Z. Zhang, X.J. Wang, Current progresses of 3D bioprinting based tissue engineering. Quant. Biol. 5, 136–142 (2017)
F. Mohammadian, A. Eatemadi, Drug loading and delivery using nanofibers scaffolds. Artif. Cells Nanomed. Biotechnol. 45, 881–888 (2017)
N. Anup, T. Chavan, S. Chavan, S. Polaka, D. Kalyane, S.N. Abed, K.N. Venugopala, K. Kalia, R.K. Tekade, Reinforced electrospun nanofiber composites for drug delivery applications. J. Biomed. Mater. Res. Part A 109, 2036–2064 (2021)
G. Wang, D. Yu, A.D. Kelkar, L. Zhang, Electrospun nanofiber: emerging reinforcing filler in polymer matrix composite materials. Prog. Polym. Sci. 75, 73–107 (2017)
M. Nune, S. Manchineella, T. Govindaraju, K.S. Narayan, Melanin incorporated electroactive and antioxidant silk fibroin nanofibrous scaffolds for nerve tissue engineering. Mater. Sci. Eng. C 94, 17–25 (2019)
A.W. Jatoi, H. Ogasawara, I.S. Kim, Q.Q. Ni, Cellulose acetate/multi-wall carbon nanotube/Ag nanofiber composite for antibacterial applications. Mater. Sci. Eng. C 110, 110679 (2020)
H. Kuang, Y. Wang, Y. Shi, W. Yao, X. He, X. Liu, X. Mo, S. Lu, P. Zhang, Construction and performance evaluation of Hep/silk-PLCL composite nanofiber small-caliber artificial blood vessel graft. Biomaterials 259, 120288 (2020)
F. Serio, A.F. Cruz, A. Chandra, C. Nobile, G.R. Rossi, E. D’Amone, G. Gigli, L.L.D. Mercato, C.C.D. Oliveira, Electrospun polyvinyl-alcohol/gum arabic nanofibers: biomimetic platform for in vitro cell growth and cancer nanomedicine delivery. Int. J. Biol. Macromol. 188, 764–773 (2021)
X. Li, B. Cho, R. Martin, M. Seu, C. Zhang, Z. Zhou, J.S. Choi, X. Jiang, L. Chen, G. Walia et al., Nanofiber-hydrogel composite-mediated angiogenesis for soft tissue reconstruction. Sci. Transl. Med. 11, eaau6210 (2019)
Z. Zheng, Y. Liu, W. Huang, Y. Mo, Y. Lan, R. Guo, B. Cheng, Neurotensin-loaded PLGA/CNC composite nanofiber membranes accelerate diabetic wound healing. Artif. Cells Nanomed. Biotechnol. 46, 493–501 (2018)
M. Harjo, M. Järvekülg, T. Tamm, T.F. Otero, R. Kiefer, Concept of an artificial muscle design on polypyrrole nanofiber scaffolds. PLoS ONE 15, e0232851 (2020)
S.H. Jegal, J.H. Park, J.H. Kim, T.H. Kim, U.S. Shin, T.I. Kim, H.W. Kim, Functional composite nanofibers of poly (lactideco-caprolactone) containing gelatin-apatite bone mimetic precipitate for bone regeneration. Acta Biomater. 7, 1609–1617 (2011)
C. Di Natale, V. Onesto, E. Lagreca, R. Vecchione, P.A. Netti, Tunable release of curcumin with an in silico-supported approach from mixtures of highly porous PLGA microparticles. Materials 13, 1807 (2020)
J. Siepmann, F. Siepmann, Modeling of diffusion-controlled drug delivery. J. Control. Release 161, 351–362 (2012)
N. Malekjani, S.M. Jafari, Modeling the release of food bioactive ingredients from carriers/nanocarriers by the empirical, semiempirical, and mechanistic models. Compr. Rev. Food Sci. Food Saf. 20, 3–47 (2021)
N.B. Shelke, P. Lee, M. Anderson, N. Mistry, R.K. Nagarale, X.-M. Ma, X. Yu, S.G. Kumbar, Neural tissue engineering: nanofiber-hydrogel based composite scaffolds. Polym. Adv. Technol. 27, 42–51 (2016)
J.D. Tang, C. Mura, K.J. Lampe, Stimuli-responsive, pentapeptide, nanofiber hydrogel for tissue engineering. J. Am. Chem. Soc. 141, 4886–4899 (2019)
D. Sharma, S. Saha, B.K. Satapathy, Recent advances in polymer scaffolds for biomedical applications. J. Biomater. Sci. Polym. Ed. 33, 342–408 (2022)
F. Davani, M. Alishahi, M. Sabzi, M. Khorram, A. Arastehfar, K. Zomorodian, Dual drug delivery of vancomycin and imipenem/cilastatin by coaxial nanofibers for treatment of diabetic foot ulcer infections. Mater. Sci. Eng. C 123, 111975 (2021)
L.M. Guerrini, M.P. Oliveira, C.C. Stapait, M. Maric, A.M. Santos, N.R. Demarquette, Evaluation of different solvents and solubility parameters on the morphology and diameter of electrospun pullulan nanofibers for curcumin entrapment. Carbohydr. Polym. 251, 117127 (2021)
C. Wang, J. Wang, L. Zeng, Z. Qiao, X. Liu, H. Liu, J. Zhang, J. Ding, Fabrication of electrospun polymer nanofibers with diverse morphologies. Molecules 24, 834 (2019)
E. Mohamed, L.A. Coupland, P.J. Crispin, A. Fitzgerald, D.R. Nisbet, T. Tsuzuki, Non-oxidized cellulose nanofibers as a topical hemostat: in vitro thromboelastometry studies of structure vs function. Carbohydr. Polym. 265, 118043 (2021)
M. Karthega, M. Pranesh, C. Poongothai, N. Srinivasan, Poly caprolactone/titanium dioxide nanofiber coating on AM50 alloy for biomedical application. J. Magnes. Alloys 9, 532–547 (2021)
M.K. Ahmed, S.F. Mansour, R. Al-Wafi, E. Abdel-Fattah, Nanofibers scaffolds of co-doped Bi/Sr-hydroxyapatite encapsulated into polycaprolactone for biomedical applications. J. Mater. Res. Technol. 13, 2297–2309 (2021)
A.I. Rezk, T.I. Hwang, J.Y. Kim, J.Y. Lee, C.H. Park, C.S. Kim, Functional composite nanofibers loaded with β-TCP and SIM as a control drug delivery system. Mater. Lett. 240, 25–29 (2019)
S. Li, J. Zhang, D.D. Ju, X. Li, J.C. Zhang, X. Yan, H.D. Zhang, F. Song, Y.Z. Long, Flexible inorganic composite nanofibers with carboxyl modification for controllable drug delivery and enhanced optical monitoring functionality. Chem. Eng. J. 350, 645–652 (2018)
Z. Chan, Z. Chen, A. Zhang, J. Hu, X. Wang, Z. Yang, Electrospun nanofibers for cancer diagnosis and therapy. Biomater. Sci. 4, 922–932 (2016)
A. Neamnark, R. Rujiravanit, P. Supaphol, Electrospinning of hexanoyl chitosan. Carbohydr. Polym. 66, 298–305 (2006)
E. Antaby, K. Klinkhammer, L. Sabantina, Electrospinning of chitosan for antibacterial applications—current trends. Appl. Sci. 11, 11937 (2021)
C. Burger, B.S. Hsiao, B. Chu, Nanofibrous materials and their applications. Annu. Rev. Mater. Res. 36, 333–368 (2006)
W. Abdul Khodir, A. Abdul Razak, M. Ng, V. Guarino, D. Susanti, Encapsulation and characterization of gentamicin sulfate in the collagen added electrospun nanofibers for skin regeneration. J. Funct. Biomater. 9, 36 (2018)
S. Thenmozhi, N. Dharmaraj, K. Kadirvelu, H.Y. Kim, Electrospun nanofibers: new generation materials for advanced applications. Mater. Sci. Eng. B Solid State Mater. Adv. Technol. 17, 36–48 (2017)
K. Kim, Y.K. Luu, C. Chang, D. Fang, B.S. Hsiao, B. Chu, M. Hadjiargyrou, Incorporation and controlled release of a hydrophilic antibiotic using poly(lactide-co-glycolide)-based electrospun nanofibrous scaffolds. J. Control. Release 98, 47–56 (2004)
L.J. Del Valle, L. Franco, R. Katsarava, J. Puiggalí, Electrospun biodegradable polymers loaded with bactericide agents. AIMS Mol. Sci. 3, 52–87 (2016)
L. Chen, L. Bromberg, T.A. Hatton, G.C. Rutledge, Electrospun cellulose acetate fibers containing chlorhexidine as a bactericide. Polymer 49, 1266–1275 (2008)
M. Puertas-Bartolomé, A. Mora-Boza, L. García-Fernández, Emerging biofabrication techniques: a review on natural polymers for biomedical applications. Polymers 13, 1209 (2021)
A. Luraghi, F. Peri, L. Moroni, Electrospinning for drug delivery applications: a review. J. Control. Release 334, 463–484 (2021)
P. Sorlier, A. Denuzière, C. Viton, A. Domard, Relation between the degree of acetylation and the electrostatic properties of chitin and chitosan. Biomacromolecules 2, 765–772 (2001)
E.I. Rabea, M.E.T. Badawy, C.V. Stevens, G. Smagghe, W. Steurbaut, Chitosan as antimicrobial agent: applications and mode of action. Biomacromolecules 4, 1457–1465 (2003)
A.M. Abdelgawad, S.M. Hudson, O.J. Rojas, Antimicrobial wound dressing nanofiber mats from multicomponent (chitosan/silver-NPs/polyvinyl alcohol) systems. Carbohydr. Polym. 100, 166–178 (2014)
M. Abrigo, S.L. McArthur, P. Kingshott, Electrospun nanofibers as dressings for chronic wound care: advances, challenges, and future prospects. Macromol. Biosci. 14, 772–792 (2014)
Y. Wang, Q. Zhang, C.L. Zhang, P. Li, Characterisation and cooperative antimicrobial properties of chitosan/nano–ZnO composite nanofibrous membranes. Food Chem. 132, 419–427 (2012)
O. Suwantong, P. Pankongadisak, S. Deachathai, P. Supaphol, Electrospun poly (l-lactic acid) fiber mats containing crude Garcinia mangostana extracts for use as wound dressings. Polym. Bull. 71, 925–949 (2014)
S. Bhattacharjee, Understanding the burst release phenomenon: toward designing effective nanoparticulate drug-delivery systems. Ther. Deliv. 12, 21–36 (2021)
G. Guidotti, M. Soccio, E. Bondi, T. Posati, G. Sotgiu, R. Zamboni, A. Torreggiani, F. Corticelli, N. Lotti, A. Aluigi, Effects of the blending ratio on the design of keratin/poly (butylene succinate) nanofibers for drug delivery applications. Biomolecules 11, 1194 (2021)
Y. Su, A. McCarthy, S.L. Wong, R.R. Hollins, G. Wang, J. Xie, Simultaneous delivery of multiple antimicrobial agents by biphasic scaffolds for effective treatment of wound biofilms. Adv. Healthc. Mater. 10, 2100135 (2021)
F. Rahmani, H. Ziyadi, M. Baghali, H. Luo, S. Ramakrishna, Electrospun pvp/pva nanofiber mat as a novel potential transdermal drug-delivery system for buprenorphine: a solution needed for pain management. Appl. Sci. 11, 2779 (2021)
X. Zheng, S. Kang, K. Wang, Y. Yang, D.G. Yu, F. Wan, G.R. Williams, S.W.A. Bligh, Combination of structure-performance and shape-performance relationships for better biphasic release in electrospun Janus fibers. Int. J. Pharm. 596, 120203 (2021)
S.M.M. Amir, M.T.H. Sultan, M. Jawaid, A.H. Ariffin, S. Mohd, K.A.M. Salleh, M.R. Ishak, A.U.M. Shah, Non-destructive testing method for Kevlar and natural fiber and their hybrid composites, in Durability and Life Prediction in Biocomposites, Fibre-Reinforced Composites and Hybrid Composites, ed. by Jawaid, M., Thariq, M., Saba, N. (Woodhead Publishing: Duxford, 2018), pp. 367–388
D.K. Rajak, D.D. Pagar, P.L. Menezes, E. Linul, Fiber-reinforced polymer composites: manufacturing, properties, and applications. Polymers 11, 1667 (2019)
S. Mombini, J. Mohammadnejad, B. Bakhshandeh, A. Narmani, J. Nourmohammadi, S. Vahdat, S. Zirak, Chitosan-PVA-CNT nanofibers as electrically conductive scaffolds for cardiovascular tissue engineering. Int. J. Biol. Macromol. 140, 278–287 (2019)
T. Bian, H. Zhang, H. Xing, Preparation and biological properties of collagen/nano-hydroxyapatite composite nanofibers based on ordered nano-hydroxyapatite ceramic fibers. Colloids Surf. A Physicochem. Eng. Asp. 602, 124802 (2020)
D.N. Phan, R.A. Rebia, Y. Saito, D. Kharaghani, M. Khatri, T. Tanaka, H. Lee, I.S. Kim, Zinc oxide nanoparticles attached to polyacrylonitrile nanofibers with hinokitiol as gluing agent for synergistic antibacterial activities and effective dye removal. J. Ind. Eng. Chem. 85, 258–268 (2020)
K.B. Liew, C.F. Goh, S. Asghar, H.K. Syed, Overview of mechanical and physicochemical properties of polymer matrix composites, in Encyclopedia of Materials: Composites, vol. 1, ed. by Brabazon, D. (Elsevier, Amsterdam, 2021), pp. 565–576 (2021)
R.R. Naslain, Ceramic matrix composites: matrices and processing, in Encyclopedia of Materials: Science and Technology, 2nd ed., ed. by Buschow, K.H.J., Cahn, R.W., Flemings, M.C., Ilschner, B., Kramer, E.J., Mahajan, S., Veyssière., P. (Elsevier, Amsterdam, 2001), pp. 1060–1066
V.K.B. Raja, M. Gupta, Joining of metal matrix composites, in Encyclopedia of Materials: Composites, vol. 1, ed. by Brabazon, D. (Elsevier, Amsterdam, 2021), pp. 502–511
K. Kalantari, A.M. Afifi, H. Jahangirian, T.J. Webster, Biomedical applications of chitosan electrospun nanofibers as a green polymer. Carbohydr. Polym. 207, 588–600 (2019)
J. Wang, M. Windbergs, Controlled dual drug release by coaxial electrospun fibers—impact of the core fluid on drug encapsulation and release. Int. J. Pharm. 556, 363–371 (2019)
D.G. Yu, X.X. Shen, C. Branford-White, K. White, L.M. Zhu, S.W.A. Bligh, Oral fastdissolving drug delivery membranes prepared from electrospun polyvinylpyrrolidone ultrafine fibers. Nanotechnology 20, 055104 (2009)
U.E. Illangakoon, H. Gill, G.C. Shearman, M. Parhizkar, S. Mahalingam, N.P. Chatterton, G.R. Williams, Fast dissolving paracetamol/caffeine nanofibers prepared by electrospinning. Int. J. Pharm. 477, 369–379 (2014)
X. Li, M.A. Kanjwal, L. Lin, I.S. Chronakis, Electrospun polyvinyl-alcohol nanofibers as oral fast-dissolving delivery system of caffeine and riboflavin. Colloids Surf. B Biointerfaces 103, 182–188 (2013)
Z. Qin, X.W. Jia, Q. Liu, B. Kong, H. Wang, Fast dissolving oral films for drug delivery prepared from chitosan/pullulan electrospinning nanofibers. Int. J. Biol. Macromol. 137, 224–231 (2019)
Y. Lu, J. Huang, G. Yu, R. Cardenas, S. Wei, E.K. Wujcik, Z. Guo, Coaxial electrospun fibers: applications in drug delivery and tissue engineering. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnol. 8, 654–677 (2016)
B. Pant, M. Park, S.J. Park, Drug delivery applications of core-sheath nanofibers prepared by coaxial electrospinning: a review. Pharmaceutics 11, 305 (2019)
X.Y. Li, Y.C. Li, D.G. Yu, Y.Z. Liao, X. Wang, Fast disintegrating quercetin-loaded drug delivery systems fabricated using coaxial electrospinning. Int. J. Mol. Sci. 14, 21647–21659 (2013)
L.É. Uhljar, S.Y. Kan, N. Radacsi, V. Koutsos, P. Szabó-Révész, R. Ambrus, In vitro drug release, permeability, and structural test of ciprofloxacin-loaded nanofibers. Pharmaceutics 13, 556–557 (2021). https://doi.org/10.3390/pharmaceutics13040556
R. Ravikumar, M. Ganesh, U. Ubaidulla, E. Young Choi, H. Tae Jang, Preparation, characterization, and in vitro diffusion study of nonwoven electrospun nanofiber of curcumin-loaded cellulose acetate phthalate polymer. Saudi Pharm. J. 25(6), 921–926 (2017). https://doi.org/10.1016/j.jsps.2017.02.004
R.M. Chandira, P. Pethappachetty, G. Rani Narayanan, D. Antony Samy, Design, optimization and evaluation of nanofibers containing NSAID for controlled drug delivery system. Asian J. Biol. Life Sci. (2022). https://doi.org/10.5530/ajbls.2022.11.52
S. Tang, Z. Zhao, G. Chen, Y. Su, L. Lu, B. Li, D. Liang, R. Jin, Fabrication of ampicillin/starch/polymer composite nanofibers with controlled drug release properties by electrospinning. J. Sol Gel Sci. Technol. 77, 594–603 (2016). https://doi.org/10.1007/s10971-015-3887-x
N.F. Theodoroula, C. Karavasili, M.C. Vlasiou, A. Primikyri, C. Nicolaou, A.V. Chatzikonstantinou, A.-T. Chatzitaki, C. Petrou, N. Bouropoulos, C.K. Zacharis et al., NGIWY-amide: a bioinspired ultrashort self-assembled peptide gelator for local drug delivery applications. Pharmaceutics 14, 133–134 (2022). https://doi.org/10.3390/pharmaceutics14010133
L.H. Nguyen, M. Gao, J. Lin, W. Wu, J. Wang, S.Y. Chew, Three-dimensional aligned nanofibers-hydrogel scaffold for controlled non-viral drug/gene delivery to direct axon regeneration in spinal cord injury treatment. Sci. Rep. 7, srep42212 (2017)
S. Song, Y. Zhao, X. Yuan, J. Zhang, β-Chitin nanofiber hydrogel as a scaffold to in situ fabricate monodispersed ultra-small silver nanoparticles. Colloids Surf. A Physicochem. Eng. Asp. 574, 36–43 (2019)
X. Liu, S. Song, J. Huang, H. Fu, X. Ning, Y. He, Z. Zhang, HBC-nanofiber hydrogel scaffolds with 3D printed internal microchannels for enhanced cartilage differentiation. J. Mater. Chem. B 8, 6115–6127 (2020)
J. Du, J. Liu, S. Yao, H.-Q. Mao, J. Peng, X. Sun, Z. Cao, Y. Yang, B. Xiao, Y. Wang et al., Prompt peripheral nerve regeneration induced by a hierarchically aligned fibrin nanofiber hydrogel. Acta Biomater. 55, 296–309 (2017)
G.J. Kim, K.O. Kim, Novel glucose-responsive of the transparent nanofiber hydrogel patches as a wearable biosensor via electrospinning. Sci. Rep. 10, 1–12 (2020)
S. Lohrasbi, E. Mirzaei, A. Karimizade, S. Takallu, A. Rezaei, Collagen/cellulose nanofiber hydrogel scaffold: physical, mechanical and cell biocompatibility properties. Cellulose 27, 927–940 (2019)
R. Jirkovec, A. Samkova, T. Kalous, J. Chaloupek, J. Chvojka, Preparation of a hydrogel nanofiber wound dressing. Nanomaterials 11, 2178 (2021)
X. Li, C. Zhang, A.E. Haggerty, J. Yan, M. Lan, M. Seu, M. Yang, M.M. Marlow, I. Maldonado-Lasunción, B. Cho et al., The effect of a nanofiber-hydrogel composite on neural tissue repair and regeneration in the contused spinal cord. Biomaterials 245, 119978 (2020)
F.A. Formica, E. Öztürk, S.C. Hess, W.J. Stark, K. Maniura-Weber, M. Rottmar, M. Zenobi-Wong, A bioinspired ultraporous nanofiber-hydrogel mimic of the cartilage extracellular matrix. Adv. Healthc. Mater. 5, 3129–3138 (2016)
A. Nishimura, T. Hayakawa, Y. Yamamoto, M. Hamori, K. Tabata, K. Seto, N. Shibata, Controlled release of insulin from self-assembling nanofiber hydrogel, PuraMatrix™: application for the subcutaneous injection in rats. Eur. J. Pharm. Sci. 45, 1–7 (2012)
M. Kawata, K. Azuma, H. Izawa, M. Morimoto, H. Saimoto, S. Ifuku, Biomineralization of calcium phosphate crystals on chitin nanofiber hydrogel for bone regeneration material. Carbohydr. Polym. 136, 964–969 (2016)
G. Yang, Y. Yao, X. Wang, Comparative study of kerateine and keratose based composite nanofibers for biomedical applications. Mater. Sci. Eng. C 83, 1–8 (2018)
Z. Wu, S. Xie, Y. Kang, X. Shan, Q. Li, Z. Cai, Biocompatibility evaluation of a 3D-bioprinted alginate-GelMA-bacteria nanocellulose (BNC) scaffold laden with oriented-growth RSC96 cells. Mater. Sci. Eng. C 129, 112393 (2021)
K. Veerubhotla, Y. Lee, C.H. Lee, Parametric optimization of 3D printed hydrogel-based cardiovascular stent. Pharm. Res. 38, 1–16 (2021)
J. Yoo, J.H. Park, Y.W. Kwon, J.J. Chung, I.C. Choi, J.J. Nam, H.S. Lee, E.Y. Jeon, K. Lee, S.H. Kim et al., Augmented peripheral nerve regeneration through elastic nerve guidance conduits prepared using a porous PLCL membrane with a 3D printed collagen hydrogel. Biomater. Sci. 8, 6261–6271 (2020)
L. Huang, X. Du, S. Fan, G. Yang, H. Shao, D. Li, C. Cao, Y. Zhu, M. Zhu, Y. Zhang, Bacterial cellulose nanofibers promote stress and fidelity of 3D-printed silk-based hydrogel scaffold with hierarchical pores. Carbohydr. Polym. 221, 146–156 (2019)
R.E. Abouzeid, R. Khiari, A. Salama, M. Diab, D. Beneventi, A. Dufresne, In situ mineralization of nano-hydroxyapatite on bifunctional cellulose nanofiber/polyvinyl alcohol/sodium alginate hydrogel using 3D printing. Int. J. Biol. Macromol. 160, 538–547 (2020)
J. Guo, R. Zhang, L. Zhang, X. Cao, 4D printing of robust hydrogels consisted of agarose nanofibers and polyacrylamide. ACS Macro Lett. 7, 442–446 (2018)
S. Shin, J. Hyun, Rheological properties of cellulose nanofiber hydrogel for high-fidelity 3D printing. Carbohydr. Polym. 263, 117976 (2021)
B. Chu, J.-M. He, Z. Wang, L.-L. Liu, X.-L. Li, C.-X. Wu, C.-S. Chen, M. Tu, Proangiogenic peptide nanofiber hydrogel/3D printed scaffold for dermal regeneration. Chem. Eng. J. 424, 128146 (2020)
L. Huang, W. Yuan, Y. Hong, S. Fan, X. Yao, T. Ren, L. Song, G. Yang, Y. Zhang, 3D printed hydrogels with oxidized cellulose nanofibers and silk fibroin for the proliferation of lung epithelial stem cells. Cellulose 28, 241–257 (2021)
A. Serafin, C. Murphy, M.C. Rubio, M.N. Collins, Printable alginate/gelatin hydrogel reinforced with carbon nanofibers as electrically conductive scaffolds for tissue engineering. Mater. Sci. Eng. C 122, 111927 (2021)
M.A. Grimaudo, A. Concheiro, C. Alvarez-Lorenzo, Crosslinked hyaluronan electrospun nanofibers for ferulic acid ocular delivery. Pharmaceutics 12, 274 (2020)
P. Mehta, A.A. Al-Kinani, M.S. Arshad, M.-W. Chang, R.G. Alany, Z. Ahmad, Development and characterisation of electrospun timolol maleate-loaded polymeric contact lens coatings containing various permeation enhancers. Int. J. Pharm. 532, 408–420 (2017)
H. Li, G.R. Williams, J. Wu, H. Wang, X. Sun, L.-M. Zhu, Poly(N-isopropylacrylamide)/poly (l-lactic acid-co-ε-caprolactone) fibers loaded with ciprofloxacin as wound dressing materials. Mater. Sci. Eng. C 79, 245–254 (2017)
F. Ghahreman, D. Semnani, S.N. Khorasani, J. Varshosaz, S. Khalili, S. Mohammadi, E. Kaviannasab, Polycaprolactone-gelatin membranes in controlled drug delivery of 5-fluorouracil. Polym. Sci. Ser. A 62, 636–647 (2020)
G. Kuang, Z. Zhang, S. Liu, D. Zhou, X. Lu, X. Jing, Y. Huang, Biphasic drug release from electrospun polyblend nanofibers for optimized local cancer treatment. Biomater. Sci. 6, 324–331 (2018)
Z. Li, R. Zeng, L. Yang, X. Ren, K.G. Maffucci, Y. Qu, Development and characterization of PCL electrospun membrane-coated Bletilla striata polysaccharide-based gastroretentive drug delivery system. AAPS PharmSciTech 21, 66 (2020)
L. Behbood, P. Moradipour, F. Moradi, E. Arkan, Mucoadhesive electrospun nanofibers of chitosan/gelatin containing vancomycin as a delivery system. J. Rep. Pharm. Sci. 6, 150 (2017)
M. Hadjianfar, D. Semnani, J. Varshosaz, Polycaprolactone/chitosan blend nanofibers loaded by 5-fluorouracil: an approach to anticancer drug delivery system. Polym. Adv. Technol. 29, 2972–2981 (2018)
A.C. Alavarse, F.W. de Oliveira Silva, J.T. Colque, V.M. da Silva, T. Prieto, E.C. Venancio, J.-J. Bonvent, Tetracycline hydrochloride-loaded electrospun nanofibers mats based on PVA and chitosan for wound dressing. Mater. Sci. Eng. C 77, 271–281 (2017)
E.A. Tawfik, D.Q.M. Craig, S.A. Barker, Dual drug-loaded coaxial nanofibers for the treatment of corneal abrasion. Int. J. Pharm. 581, 119296 (2020)
P. Yousefi, G. Dini, B. Movahedi, S. Vaezifar, M. Mehdikhani, Polycaprolactone/chitosan core/shell nanofibrous mat fabricated by electrospinning process as carrier for rosuvastatin drug. Polym. Bull. 79, 1627–1645 (2021)
E. Yan, J. Jiang, X. Yang, L. Fan, Y. Wang, Q. An, Z. Zhang, B. Lu, D. Wang, D. Zhang, pH-sensitive core-shell electrospun nanofibers based on polyvinyl alcohol/polycaprolactone as a potential drug delivery system for the chemotherapy against cervical cancer. J. Drug Deliv. Sci. Technol. 55, 101455 (2020)
M. Baghali, H. Ziyadi, R. Faridi-Majidi, Fabrication and characterization of core–shell TiO2-containing nanofibers of PCL-zein by coaxial electrospinning method as an erythromycin drug carrier. Polym. Bull 79, 1729–1749 (2022)
K.D. Miller, L. Nogueira, A.B. Mariotto et al., Cancer treatment and survivorship statistics, 2019. CA Cancer J Clin 69(5), 363–385 (2019)
T. Eren Boncu, A. Uskudar Guclu, M.F. Catma, A. Savaser, A. Gokce, N. Ozdemir, In vitro and in vivo evaluation of linezolid loaded electrospun PLGA and PLGA/PCL fiber mats for prophylaxis and treatment of MRSA induced prosthetic infections. Int. J. Pharm. 573, Article ID 118758 (2020)
H.R. Bakhsheshi-Rad, Z. Hadisi, A.F. Ismail et al., In vitro and in vivo evaluation of chitosan-alginate/gentamicin wound dressing nanofibrous with high antibacterial performance. Polym. Test. 82, Article ID 106298 (2020)
A. Faccendini, M. Ruggeri, D. Miele et al., Norfloxacin loaded electrospun scaffolds: montmorillonite nanocomposite vs. free drug. Pharmaceutics 12(4), 325 (2020)
M. Norouzi, S.M. Boroujeni, N. Omidvarkordshouli, M. Soleimani, Advances in skin regeneration: application of electrospun scaffolds. Adv. Healthcare Mater. 4(8), 1114–1133 (2015)
A.T. El-Serafi, I.T. El-Serafi, M. Elmasry, I. Steinvall, F. Sjoberg, Skin regeneration in three dimensions, current status, challenges and opportunities. Differentiation 96, 26–29 (2017)
F. Brako, R. Orogate, S. Mahalingam, B. Raimi-Abraham, D.Q.M. Craig, M. Edirisinghe, Mucoadhesion of progesterone-loaded drug delivery nanofiber constructs. ACS Appl. Mater. Interfaces 10(16), 13381–13389 (2018)
G.L. Perez-González, J.M. Cornejo-Bravo, R. Vera-Gráciano, E.S. Adan-López, L.J. Villarreal-Gómez, Development, characterization, and in vitro evaluation of adhesive fibrous mat for mucosal propranolol delivery. EPolymers 22(1), 58–68 (2022)
H.-W. Tong, X. Zhang, M. Wang, A new nanofiber fabrication technique based on coaxial electrospinning. Mater. Lett. 66(1), 257–260 (2012)
P. Gupta, G.L. Wilkes, Some investigations on the fiber formation by utilizing a side-by-side bicomponent electrospinning approach. Polymer 44(20), 6353–6359 (2003)
H. Na, P. Chen, S.-C. Wong, S. Hague, Q. Li, Fabrication of PVDF/PVA microtubules by coaxial electrospinning. Polymer 53(13), 2736–2743 (2012)
X. Li, Y. He, J. Hou, G. Yang, S. Zhou, A time-programmed release of dual drugs from an implantable trilayer structured fiber device for synergistic treatment of breast cancer. Small 16(9), Article ID 1902262 (2020)
B. Boddupalli, Z.K. Mohammed, R. Nath, D. Banji, Mucoadhesive drug delivery system: an overview. J. Adv. Pharm. Technol. Res. 1(4), 381–382 (2010)
L. Behbood, S. Karimi, E. Mirzaei, G. Mohammadi, M. Azami, E. Arkan, Mucoadhesive chitosan electrospun nanofibers containing tetracycline and triamcinolone as a drug delivery system. Fibers Polym. 19(7), 1454–1462 (2018)
C.L. He, Z.M. Huang, X.J. Han, Fabrication of drug-loaded electrospun aligned fibrous threads for suture applications. J. Biomed. Mater. Res. Part A 89, 80–95 (2009)
Z.M. Huang, C.L. He, A. Yang, Y. Zhang, X.J. Han, J. Yin, Q. Wu, Encapsulating drugs in biodegradable ultrafine fibers through co-axial electrospinning. J. Biomed. Mater. Res. Part A 77, 169–179 (2006)
G. Verreck, I. Chun, J. Rosenblatt, J. Peeters, A.V. Dijck, J. Mensch, M. Noppe, M.E. Brewster, Incorporation of drugs in an amorphous state into electrospun nanofibers composed of a water-insoluble, nonbiodegradable polymer. J. Control. Release 92, 349–360 (2003)
Y. Yang, T. Xia, W. Zhi, L. Wei, J. Weng, C. Zhang, X. Li, Promotion of skin regeneration in diabetic rats by electrospun core-sheath fibers loaded with basic fibroblast growth factor. Biomaterials 32, 4243–4254 (2011)
H.J. Lai, C.H. Kuan, H.C. Wu, J.C. Tsai, T.M. Chen, D.J. Hsieh, T.W. Wang, Tailored design of electrospun composite nanofibers with staged release of multiple angiogenic growth factors for chronic wound healing. Acta Biomater. 10, 4156–4166 (2014)
X. Sheng, L. Fan, C. He, K. Zhang, X. Mo, H. Wang, Vitamin E-loaded silk fibroin nanofibrous mats fabricated by green process for skin care application. Int. J. Biol. Macromol. 56, 49–56 (2013)
W.A. Sarhan, H.M. Azzazy, I.M. El-Sherbiny, Honey/chitosan nanofiber wound dressing enriched with Allium sativum and Cleome droserifolia: enhanced antimicrobial and wound healing activity. ACS Appl. Mater. Interfaces 8(10), 6379–6390 (2016)
T.T. Yuan, A.M.D. Foushee, M.C. Johnson, A.R. Jockheck-Clark, J.M. Stahl, Development of electrospun chitosan-polyethylene oxide/fibrinogen biocomposite for potential wound healing applications. Nanoscale Res. Lett. 13(1), 88 (2018)
N. Mahmoudi, A. Simchi, On the biological performance of graphene oxide-modified chitosan/polyvinylpyrrolidone nanocomposite membranes: in vitro and in vivo effects of graphene oxide. Mater. Sci. Eng., C 70, 121–131 (2017)
S. Gomes, G. Rodrigues, G. Martins, C. Henriques, J.C. Silva, Evaluation of nanofibrous scaffolds obtained from blends of chitosan, gelatin and polycaprolactone for skin tissue engineering. Int. J. Biol. Macromol. 102, 1174–1185 (2017)
T. Sultana, J. Amirian, C. Park, S.J. Lee, B.-T. Lee, Preparation and characterization of polycaprolactone-polyethylene glycol methyl ether and polycaprolactone-chitosan electrospun mats potential for vascular tissue engineering. J. Biomater. Appl. 32(5), 648–662 (2017)
R. Shen, W. Xu, Y. Xue, L. Chen, H. Ye, E. Zhong, Y. Yan, The use of chitosan/PLA nano-fibers by emulsion electrospinning for periodontal tissue engineering. Artif. Cells Nanomed. Biotechnol. 46(supp2), 419–430 (2018)
J. Jalvandi, M. White, Y. Gao, Y.B. Truong, R. Padhye, I.L. Kyratzis, Polyvinyl alcohol composite nanofibers containing conjugated levofloxacin-chitosan for controlled drug release. Mater. Sci. Eng. C 73, 440–446 (2017)
B. Darbasizadeh, H. Motasadizadeh, B. Foroughi-Nia, H. Farhadnejad, Tripolyphosphate-crosslinked chitosan/poly(ethyleneoxide) electrospun nanofi-brous mats as a floating gastro-retentive delivery system for ranitidine hydrochloride. J. Pharm. Biomed. Anal. 153, 63–75 (2018)
M. Radmansouri, E. Bahmani, E. Sarikhani, K. Rahmani, F. Sharifianjazi, M. Irani, Doxorubicin hydrochloride—loaded electrospun chitosan/cobalt ferrite/Ti-tanium oxide nanofibers for hyperthermic tumor cell treatment and controlled drug release. Int. J. Biol. Macromol. 116, 378–384 (2018)
A. Fakharmanesh, H. Tavanai, T. Khayamian, M. Morshed, Controlled release of doxorubicin embedded in carboxy methyl chitosan nanofibers. J. Text. Inst. 109(2), 178–185 (2018)
S. Samadi, M. Moradkhani, H. Beheshti, M. Irani, M. Aliabadi, Fabrication ofchitosan/poly(lactic acid)/graphene oxide/TiO2 composite nanofibrous scaffolds for sustained delivery of doxorubicin and treatment of lung cancer. Int. J. Biol. Macromol. 110, 416–424 (2018)
M. Irani, M. Mohamad, G. Sadeghi, I.A. Haririan, novel biocompatible drug delivery system of chitosan/temozolomide nanoparticles loaded PCL-PU nanofibers for sustained delivery of temozolomide. Int. J. Biol. Macromol. 97, 744–751 (2017)
Y. Fazli, Z. Shariatinia, Controlled release of cefazolin sodium antibiotic drug from electrospun chitosan-polyethylene oxide nanofibrous mats. Mater. Sci. Eng. C 71, 641–652 (2017)
Y. He, Y. Jin, X. Wang, S. Yao, Y. Li, Q. Wu, H. Liu, An antimicrobial peptide-loaded gelatin/chitosan nanofibrous membrane fabricated by sequential layer-by-layer electrospinning and electrospraying techniques. Nanomaterials (Basel, Switzerland) 8(5), 327 (2018)
Acknowledgements
The authors B.K and R.N. thank RUSA 2.0 for the funding of this research work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest in this research work.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Naveenkumar, R., Senthilvelan, S. & Karthikeyan, B. A Review on the Recent Developments in Electrospinned Nanofibers for Drug Delivery. Biomedical Materials & Devices 2, 342–364 (2024). https://doi.org/10.1007/s44174-023-00121-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s44174-023-00121-9