Abstract
Introduction
Fixation of plateau posterolateral fracture (PLF) is challenging because the fracture site is mostly covered by vital neurovascular structures. We operated on 15 cases of PLF using a direct lateral approach. This study aims to report on clinical results.
Material and methods
Between 2017 and 2019, 15 cases of PLFs were fixed with a direct lateral approach and a tricortical autologous bone graft from the iliac crest. A depression of more than 2 mm was indicated for the surgical treatment. Clinical evaluation included Lysholm score, International Knee Documentation Committee Score (IKDC) score, and Tegner activity scale after two years follow-up.
Results
The last follow-up was at 24 months after the operation. The mean postoperative Tegner activity scale did not change significantly compared to before the injury (6.5 (6–7) vs. 7 (6–8, p = 0.5)). The postoperative IKDC and Lysholm scores improved significantly compared to before the operation (p < 0.001). The full range of motion was seen in all patients except one who was manipulated after three months.
Conclusions
Surgical treatment using a direct lateral approach is a safe procedure for PLFs that results in good, short-term clinical and radiologic outcomes without fibular osteotomy or compromising the important neurovascular structures.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The basic principle of treatment for a displaced tibial plateau fracture is the restoration of articular congruity, joint stability, and the original knee axis [7]. A recent study [10] has demonstrated a 44% incidence of the plateau posterolateral fracture (PLF), with 36% occurring in AO/OTA type B plateau fractures and 54% in type C. PLF is the result of compression of the tibia plateau with the femoral condyle, while the knee is flexed and the tibia is rotated internally [1].
The anterolateral approach is the most commonly used approach for the lateral tibia plateau fractures, however, direct visualization of PLF is often inadequate [6]. Isolated posterior approach is another suggestion for PLFs. The control of fracture reduction using the posterior approach is limited, especially in the more complex fractures [12]. Exposure of a tibial plateau posterolateral quadrant is challenging because of the ligamentous and neurovascular structures. Therefore, surgeons do not prefer a direct lateral approach to the treatment of the PLF [5].
The optimal approach for the treatment of a depressed PLF is still under debate. This study presents surgical details and clinical outcomes of fixation of depressed PLFs using a lateral approach and a tricortical autologous bone graft from the iliac crest.
Material and Methods
This study includes 15 patients with a depressed posterolateral tibial plateau fracture (PLF) who were treated between 2017 and 2019 by the senior author. Patients with a history of previous peroneal nerve injury or open surgery in the posterior compartment of the knee were excluded from the study. Approval was acquired from the local committee of ethics and research, and written informed consent was obtained from all participating patients before surgery. Radiological evaluations were performed using X-ray radiographs before surgery and two weeks, one and three months after surgery. Also, all patients were evaluated by CT scan with reconstruction before surgery.
There were three different types of PLF depending on fracture morphology and the defect size: (1) fractures of the dorsal proximal cortical rim of the tibia, (2) depression fracture of the posterolateral quadrant of the plateau tibia, and (3) shear fracture of the posterolateral quadrant. All patients were evaluated preoperatively and during the final follow-up using the Lysholm score, International Knee Documentation Committee (IKDC) score, and Tegner activity scale.
The surgical treatment was performed within 6 days (range 2–14 days) after trauma. The procedure was performed with the patient in the supine position with the leg hanging freely over the edge of the operating table to displace the common peroneal nerve posterior to the biceps muscle. An approximately 10-cm-long lateral skin incision was made. The incision started 3 cm above the joint line and followed distally along the fibula. Care must be taken so that the incision was not made too far dorsally to avoid scar contractions (Fig. 1a). After a direct incision of the fascia, the peroneal nerve was exposed at the posteromedial edge of the biceps femoris tendon. The nerve should be carefully dissected and gently mobilized during the operation (Fig. 1b). The peroneal nerve was not dissected entering the muscle because the muscle branches that lead off abnormally are easily damaged. The iliotibial band was retracted upward to explore the lateral collateral ligament (LCL). It may be necessary to cut the inferior attachment of the popliteomeniscal ligament that should be repaired after fixation. The visual control of the reduction was achieved using a lateral standard arthrotomy to the lateral tibia plateau.
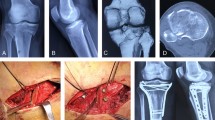
Depressed articular segments were elevated with a bone tamper through a small lateral rectangular cortical window under the fluoroscopic guidance. This window is safe regarding neurovascular anatomy and limited anteriorly with the LCL, posterosuperior with the popliteal tendon, and posteroinferiorly with the popliteofibular tendon (Fig. 2a). This reduction caused an approximately 10 mm defect below the articular surface posterior to the LCL. Screw osteosynthesis with optional bone graft was needed to fill this space. We used a tricortical autologous bone graft from the iliac crest that was fixed using two rafting screws inserting toward the posteromedial intact segment of the tibia (Fig. 2b). The posterolateral fragments were manipulated and reduced from the dorsal side with pointed reduction forceps. Finally, the wound was irrigated and the inferior popliteomeniscal ligament, the fascia, and the skin were sutured properly.
The reduction was achieved through a safe window regarding neurovascular anatomy that was limited anteriorly with the LCL (Thin arrow), posterosuperior with the popliteal tendon (Asterisk), and posteroinferiorly with the popliteofibular tendon (Thick arrow). a The graft was fixed using two rafting screws inserting toward the posteromedial intact segment of the tibia c
Similar physiotherapy and rehabilitation protocols were administered for all patients. One week after the operation, a continuous passive knee range of motion (ROM) was started changing to the active ROM after a week. The patients were non-weight-bearing for 6 weeks followed by partial weight-bearing. After 10 weeks the patients were allowed to have a full weight-bearing.
All statistical analyses were performed in the SPSS software (version 16). All values of parametric variables were presented as mean ± SD (standard deviation), while the values of all nonparametric variables were reported as median with range. A paired-samples t test was used to compare the parametric variables before and after surgery. A p value of less than 0.001 was chosen as the threshold for statistical significance.
Results
Between 2017 and 2019, 15 patients (3 females and 12 males) were included with a mean age of 33.4 (24–45) years. The injury causes included traffic accidents in 10 patients and falling from height in five patients. Five patients had isolated posterolateral fractures, three had both posterolateral and anterolateral fractures, and seven patients had concomitant posterolateral, anterolateral, and posteromedial fractures. The last follow-up was 24 months after the operation. Postoperative full range of motion in comparison to the contralateral knee was observed in 14 patients. One patient with a limited range of motion underwent manipulation after three months.
Tegner activity scale did not change significantly compared to before the injury (6.5 (6–7) vs. 7 (6–8), p = 0.5). The IKDC score was significantly improved from 46.4 ± 2 before the operation to 96 ± 2.4, postoperatively (p < 0.001). The preoperative Lysholm score was 45 ± 2.6 that improved significantly to 94 ± 2 (p < 0.001) (Fig. 3).
Tegner activity scale before the injury and after the operation. a International Knee Documentation Committee (IKDC) and Lysholm scores before and after the operation. b According to the radiographic findings, all participants experienced sufficient healing during the three months after surgery (Fig. 4)
According to the radiographic findings, all participants experienced sufficient healing during the three months after surgery (Fig. 4).
There was one superficial incision of the posteromedial approach in a case with concomitant posteromedial and posterolateral tibia plateau fracture. Apart from this, no other complications were observed in the patients during or within 3 months after the operation.
Discussion
This study underlines that the majority of depressed PLF can be directly reduced and fixated through a lateral approach with good clinical and radiological results (Fig. 5). The results of this study can be considered as a supplement to provide a guideline for the type and manner of surgical treatment for the depressed posterolateral corner of tibial plateau fracture.
An anatomic fracture reduction without intra-articular step-offs is an important goal in the treatment of tibial plateau fractures [9]. Solomon et al. [11] have shown that a displacement of posterolateral fragments of more than 5 mm is associated with poorer clinical results compared to anatomic-reduced fractures. Parkinnen et al [8] demonstrated that a depression greater than 2 mm developed more advanced osteoarthritis compared to patients with depression of 2 mm or less in lateral tibial plateau fractures.
While the anterolateral approach is the most commonly used approach for the lateral tibia plateau fractures [6] direct visualization of PLF is often inadequate. Anatomic reduction of the PLF can be achieved through an indirect method using the anterolateral approach. The isolated posterior approach is another suggestion for PLFs [2, 4, 12]. However, the control of fracture reduction under direct vision is limited, especially in the more complex fractures that require dissection of the common peroneal nerve and popliteal neurovascular structures. It is difficult to access the articular surface in this approach unless a posterolateral corner injury. Therefore, the damage to the soft tissue might be even higher with the isolated posterior approaches compared with our approach.
Tscherne and Lobenhoffer [13] proposed an extensive lateral approach with fibular osteotomy for PLFs. Their approach allows exposure of the posterolateral plateau, as well as the lateral and posterior flare of the proximal tibia. It facilitates anatomic reduction of the upper segment of PLF and even the fibular head. However, this approach may increase the risk of injury to the common peroneal nerve and proximal tibiofibular joint. The 50% of loss of reduction observed in this method can be attributed to the trauma to the posterolateral corner soft tissue caused by extended exposure and the associated reduced blood circulation in the fragments.
Frosch et al. [3] described a technique using a single skin incision with two deep dissection intervals for visualizing the joint surface via lateral arthrotomy and reduction and fixation with the help of a posterolateral approach. Although the method can provide relatively good exposure of the joint surface, like other posterolateral approaches, the risk of damage to the peroneal nerve and recurrent tibial or geniculate artery remains.
We presented a less invasive lateral approach as a method for direct anatomic reduction and internal fixation of PLFs. In this approach, we can fix concomitant anterolateral and posterolateral fragments with just one incision under direct vision without compromising the important neurovascular structures. The use of a tricortical autologous bone graft from the iliac crest helps to restorer the articular depression as well as the comminuted posterolateral cortex. Using only two parallel screws for osteosynthesis eliminates the need for additional surgery to remove the device.
Considering the results of this study, one should pay attention to its limitations. First, this study is not a comparison between the technique used in this study with other techniques, so despite the good results of this study, it is not possible to accurately infer the superiority of this method over other methods. Second, the small sample size may affect the results of this study, although the fracture type studied is not a common type of tibia plateau fracture. A long-term analysis including a control group with higher sample size is necessary. Therefore, we are continuing to recruit consecutive patients with this type of injury.
Conclusion
We offered a less invasive with better exposure and direct reduction of the fracture fragments in PLFs. The advantages of the presented lateral approach include a direct vision for anatomic reduction, the ability to dispense with fibular osteotomy, and the preservation of soft tissue around the posterolateral corner of the tibia plateau.
Data availability
The data that support the findings of this study are available from the corresponding author [MS], upon reasonable request.
References
Bernholt, D. L., DePhillipo, N. N., Grantham, W. J., et al. (2020). Morphologic variants of posterolateral tibial plateau impaction fractures in the setting of primary anterior cruciate ligament tear. American Journal of Sports Medicine, 48(2), 318–325.
Berwin, J. T., Donovan, R. L., Riddick, A., & Kelly, M. B. (2020). The “FCR” approach to the knee for the management of posterior tibial plateau fractures. Journal of Orthopaedic Trauma, 34(6), e221–e224.
Frosch, K.-H., Balcarek, P., Walde, T., & Stürmer, K. M. (2010). A new posterolateral approach without fibula osteotomy for the treatment of tibial plateau fractures. Journal of Orthopaedic Trauma, 24(8), 515–520.
He, X., Ye, P., Hu, Y., et al. (2013). A posterior inverted L-shaped approach for the treatment of posterior bicondylar tibial plateau fractures. Archives of Orthopaedic and Trauma Surgery, 133(1), 23–28.
Heidari, N., Lidder, S., Grechenig, W., Tesch, N. P., & Weinberg, A. M. (2013). The risk of injury to the anterior tibial artery in the posterolateral approach to the tibia plateau: a cadaver study. Journal of Orthopaedic Trauma, 27(4), 221–225.
Kandemir, U., & Maclean, J. (2014). Surgical approaches for tibial plateau fractures. The Journal of Knee Surgery, 27(01), 021–030.
Marsh, J. L., Buckwalter, J., Gelberman, R., et al. (2002). Articular fractures: does an anatomic reduction really change the result? JBJS, 84(7), 1259–1271.
Parkkinen, M., Madanat, R., Mustonen, A., Koskinen, S., Paavola, M., & Lindahl, J. (2014). Factors predicting the development of early osteoarthritis following lateral tibial plateau fractures: mid-term clinical and radiographic outcomes of 73 operatively treated patients. Scand J Surg, 103(4), 256–262.
Singleton, N., Sahakian, V., & Muir, D. (2017). Outcome after tibial plateau fracture: how important is restoration of articular congruity? Journal of Orthopaedic Trauma, 31(3), 158–163.
Sohn, H.-S., Yoon, Y.-C., Cho, J.-W., Cho, W.-T., Oh, C.-W., & Oh, J.-K. (2015). Incidence and fracture morphology of posterolateral fragments in lateral and bicondylar tibial plateau fractures. Journal of Orthopaedic Trauma, 29(2), 91–97.
Solomon, L. B., Stevenson, A. W., Lee, Y. C., Baird, R. P., & Howie, D. W. (2013). Posterolateral and anterolateral approaches to unicondylar posterolateral tibial plateau fractures: a comparative study. Injury, 44(11), 1561–1568.
Tao, J., Hang, D.-h, Wang, Q.-g, Gao, W., Zhu, L.-b, & Wu, X.-f. (2008). The posterolateral shearing tibial plateau fracture: Treatment and results via a modified posterolateral approach. The Knee, 15(6), 473–479.
Tscherne, H., & Lobenhoffer, P. (1993). Tibial plateau fractures: management and expected results. Clin Orthop Related Res., 292, 87–100.
Funding
No funds, grants, or other support was received.
Author information
Authors and Affiliations
Contributions
RN designed the study and was the main surgeon of the patients. He carried out the postoperative visits and drafted the manuscript. SSJ and KA helped Dr. Noktehsanj during surgery and postoperative visits and helped to draft the manuscript and revised the study design. MM carried out data acquisition and analysis and interpretation of data. MMS, SK, and BS revised the manuscript critically for important intellectual content and has given the final approval of the version to be publish.
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethical Approval
Ethical approval was waived by the local Ethics Committee of Shahid Beheshti University of Medical Sciences in view of the retrospective nature of the study and all the procedures being performed were part of the routine care.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Noktehsanj, R., Movahedinia, M., Jousheghan, S.S. et al. Clinical Outcomes of Fixation of Depressed Posterolateral Tibial Plateau Fractures Using a Direct Lateral Approach. JOIO 57, 466–471 (2023). https://doi.org/10.1007/s43465-023-00825-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-023-00825-6