Abstract
Background
Open reduction and internal fixation (ORIF) with transarticular screws to stabilize Lisfranc injuries may increase the risk of arthritis or affect outcomes. Joint-preserving fixation using staples, bridge plating, or Lisfranc screws avoids iatrogenic articular damage. This study analyzes functional outcomes and complications in Lisfranc-injury patients who underwent joint-preserving fixation.
Materials and Methods
We conducted a retrospective review of patients treated for Lisfranc injury at a Level 1 trauma center from July 2008 to October 2015. Patients over 18 years of age, with no concomitant procedures in the lower extremities, were included. Functional outcomes were evaluated through American Orthopaedic Foot and Ankle Society (AOFAS) scores.
Results
Fourteen patients met the inclusion criteria. The average followup time was 57 months (range 22-102 months). AOFAS scores averaged 80.4 (standard deviation [SD] 16) at the time of the latest followup, with time to return to regular activities averaging 34 weeks (SD 25 weeks). Five patients had their hardware removed, and two required subsequent fusion during the followup period. The single complication involved a screw backing out, with subsequent removal.
Conclusions
In this case series, joint-preserving fixation for Lisfranc injuries offered similar AOFAS scores as those reported for ORIF with transarticular screws but with a decreased rate of hardware removal and need for midfoot fusion.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lisfranc injuries are disruptions of the ligamentous or osseous structures of the tarsometatarsal (TMT) joints which, left untreated, can lead to chronic pain and functional loss due to arthritis, deformity, ligamentous instability, and soft-tissue injury [1].
Fixation using dorsal plates or staples preserves normal joint anatomy and articular surface [2, 3]. In biomechanical studies, extraarticular locking plates provide equally rigid fixation compared to transarticular screws [4, 5]. Clinical studies have shown that early outcomes are equivalent or improved with extraarticular fixation [6]. In the present study, we report our experience with joint-preserving fixation. We anticipate a decreased incidence of subsequent arthrodesis with joint-preserving fixation.
Materials and Methods
After obtaining institutional review board approval, a retrospective review was conducted of all patients over 18 years of age treated for a Lisfranc injury at a Level 1 trauma center from July 2008 to October 2015. Exclusion criteria included concomitant procedures in the lower extremities, revision Lisfranc open reduction and internal fixation (ORIF), or treatment with a cartilage-violating procedure (see below for definition) and primary arthrodesis. Joint-preserving fixation was defined as any type of fixation that does not cross the medial cuneiform, first metatarsal or middle cuneiform or second metatarsal joints. Therefore, a screw from the second metatarsal to the medial cuneiform, or Lisfranc screw, was considered joint-preserving fixation. We make this distinction because anatomically, the Lisfranc ligament is composed of plantar, dorsal, and interosseous components [7]. It follows that a screw placed through the ligamentous footprint of the interosseous portion of the Lisfranc ligament would not be violating any articular cartilage. This distinction has been used in prior studies as well [8, 9].
Eighteen patients were identified with Lisfranc injuries, of which 14 met the criteria for this study. Two were excluded as they underwent primary arthrodesis and two were excluded because their fixation violated the TMT joint. Patient demographics are depicted in Tables 1 and 2. The average age was 54.5 years (range 34-68 years), with an even distribution of males and females. Seven of the injuries were purely ligamentous, while the other seven involved a fracture. All but one of the Lisfranc injuries were Myerson type B2 injuries; the one exception was a Myerson type C injury. Ligamentous injuries were diagnosed by lack of fracture seen on X-ray, and laxity during stress examination under anesthesia or ligamentous disruption was seen on magnetic resonance imaging. Four of the patients were smokers and one was a well-controlled Type 2 diabetic without any stigmata of chronic diseases, such as peripheral neuropathy or retinopathy. Nine of the 14 patients were injured due to a low-energy mechanism, most commonly a fall from standing. Five occurred due to a high-energy mechanism, including fall from height, motor vehicle collision, or crush. There was one open injury. Hardware removal was only performed if symptomatic or if fusion was done.
Patients were then contacted for a phone survey. All patients contacted via telephone were available to respond to the survey, which asked patients to evaluate their postoperative levels of pain, functional limitations, footwear limitations, gait abnormality, walking surface, time to return to baseline function, and complications (including paresthesia, infections, hardware removal, and need for secondary surgery). Chart reviews provided information on further complications or additional surgeries. Foot alignment was evaluated via both patient self-assessment and review of most recent foot radiographs (typically 1 year after the date of surgery). Malalignment was defined as loss of longitudinal arch of the foot, defined as a downward Meary’s angle of over 15° [1].
Surgical technique
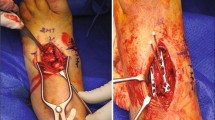
All of the surgeries were performed by the same foot and ankle surgeon. Initially, a stress radiograph was performed to evaluate TMT and intercuneiform stability. Incision was made longitudinally between the first and second metatarsal. Soft tissue dissection to the bone was performed with care to avoid neurovascular structures. Plate and screw placement was based on preoperative films, clinical evaluation, and intraoperative fluoroscopic views. A reduction clamp was placed between the base of the second metatarsal and the medial cuneiform, and a guidewire was introduced percutaneously from the second metatarsal into the medial cuneiform. Once satisfied with reduction and guidewire placement, a lateral incision was made over the wire, and a Lisfranc screw was inserted [9]. A bridge plate or staple was then placed dorsally over the first TMT joint. If laxity was appreciated in the second TMT joint, a second bridge plate or staple was placed [Figure 1] [10]. Patients were kept nonweight-bearing for 6 total weeks after which protected weight-bearing as tolerated in a removable boot was progressively allowed over the next 6 weeks.
Results
The average American Orthopaedic Foot and Ankle Society (AOFAS) midfoot score at the time of the phone survey was 80.4 (standard deviation 16). Followup occurred 57 months postoperatively, on average (range 22-102 months). The summary of results is presented in Table 3. The most common reason for lower postoperative AOFAS scores was mild-to-moderate pain with activities. Average patient-reported time to return to baseline function was 34 weeks. Five patients underwent subsequent hardware removal due to symptomatic hardware or residual pain, and two of these patients underwent subsequent arthrodesis for persistent pain. One hardware complication was encountered in which a screw backed out, requiring surgical removal. No episodes of numbness or complex regional pain syndrome were recorded in the chart or reported by the patients. No deep or soft-tissue infections occurred in the present case series.
Reviewing a subgroup of smokers, postoperative AOFAS scores were better in the nonsmokers compared to smokers (87.4 vs. 64.3, P = 0.009). Both patients who underwent subsequent arthrodesis, and three of the five patients who needed hardware removal, were smokers. Evaluating the mechanism of injury, no difference in AOFAS was seen between high- and low-energy mechanisms (78.3 vs. 79.4, P = 0.74).
All patients in our study had a good reduction based on <2 mm displacement and no malalignment on anteroposterior and lateral radiographs of the foot. Four patients experienced loss of reduction, two of whom went on to arthrodesis. In addition, three of the four patients collectively had the lowest postoperative AOFAS scores. The other patient eventually needed a hardware removal for pain and had evidence of radiographic arthritis within a year, but final AOFAS score was 88.
Ligamentous injuries trended toward better AOFAS scores compared to osseous injuries, although not statistically significant (86.6 vs. 74.7, P = 0.18) [Table 2].
Two patients had recent radiographs, one 6 years and the other 7 years out from their index operation [example radiographs of one of the patients is shown in Figure 2]. These patients were asymptomatic and had followup for other issues. Joint spaces were preserved in both of these patients. Broken screws were present in both patients but were asymptomatic and the hardware had not moved.
Discussion
Lisfranc injuries are rare and often missed; up to 20% on the first presentation [11]. Early anatomic reduction with rigid fixation greatly improves outcomes and reduces posttraumatic arthritis [11]. ORIF is a common method, using transarticular screws placed across the TMT joints and a screw from the second metatarsal into the medial cuneiform. However, even with operative fixation, 13% will develop arthrosis and symptoms requiring arthrodesis [12, 13]; cadaveric studies have shown that transarticular screws result in direct damage of 3%-4% of the total joint surface, which does not account for damage caused by heat-induced necrosis or errant drill attempts [4, 5, 14]. Some authors advocate for primary arthrodesis to decrease the rate of reoperation [15]; however, the potential negative impact on normal foot function in athletic populations, as well as increasing forces on adjacent joints, is a disadvantage [16].
Although there are several reports on joint preserving fixation for Lisfranc injuries, our study has some of the longest follow up [2, 6, 8, 9, 17,18,19,20]. Table 4 shows a selected literature review of other studies using different fixation methods [6]. Compared to other reports, we had higher rates of secondary arthrodesis, but this may have been due to our limited sample size or longer followup times. Smoking and loss of reduction were the risk factors for lower AOFAS score or conversion to arthrodesis. Our rate of hardware removal was lower than other studies, and this may have been because we also included staples in terms of dorsal fixation [17, 18]. Table 4 shows a selected literature review of the outcomes of dorsal plating and transarticular fixation for Lisfranc injuries.
We did not see a trend toward decreased AOFAS scores with longer followup. Our two cases requiring an arthrodesis both had their fusions within a year from surgery, slightly earlier than the time required for other studies [12, 13]. Furthermore, both of these cases had a delayed loss of reduction postoperatively. This suggests that quality and preservation of reduction are of high importance in the outcome.
There are several limitations to the present study. These include a low sample size as well as a mixture of both fixation types and injury types in our sample. Our study is also bound by the same limitations as all studies involving retrospective reviews. All patients were contacted via telephone for a followup. Subsequently, these patients may be subject to recall bias.
Conclusions
We suggest that extraarticular fixation may be another viable option in the treatment of Lisfranc injuries. Patients had significant improvement in their AOFAS scores with minimal complications.
References
Myerson MS, Fisher RT, Burgess AR, Kenzora JE. Fracture dislocations of the tarsometatarsal joints: End results correlated with pathology and treatment. Foot Ankle 1986;6:225-42.
Stern RE, Assal M. Dorsal multiple plating without routine transarticular screws for fixation of Lisfranc injury. Orthopedics 2014;37:815-9.
Holmes GB. Staple fixation of Lisfranc injuries: A new description of a new technique and early clinical results. Tech Foot Ankle Surg 2013;12:196-200.
Alberta FG, Aronow MS, Barrero M, Diaz-Doran V, Sullivan RJ, Adams DJ. Ligamentous Lisfranc joint injuries: A biomechanical comparison of dorsal plate and transarticular screw fixation. Foot Ankle Int 2005;26:462-73.
Gaines RJ, Wright G, Stewart J. Injury to the tarsometatarsal joint complex during fixation of Lisfranc fracture dislocations: An anatomic study. J Trauma 2009;66:1125-8.
Hu SJ, Chang SM, Li XH, Yu GR. Outcome comparison of Lisfranc injuries treated through dorsal plate fixation versus screw fixation. Acta Ortop Bras 2014;22:315-20.
Johnson A, Hill K, Ward J, Ficke J. Anatomy of the Lisfranc ligament. Foot Ankle Spec 2008;1:19-23.
Lau S, Guest C, Hall M, Tacey M, Joseph S, Oppy A. Functional outcomes post lisfranc injury-transarticular screws, dorsal bridge plating or combination treatment? J Orthop Trauma 2017;31:447-52.
Aronow MS. Joint preserving techniques for Lisfranc injury. Tech Orthop 2011;26:43-9.
Panchbhavi VK. Orientation of the “Lisfranc screw”. J Orthop and internal fixation. A prospective, randomized study. J Bone Trauma 2012;26:e221-4.
Seybold JD, Coetzee JC. Lisfranc injuries: When to observe, fix, or fuse. Clin Sports Med 2015;34:705-23.
Kuo RS, Tejwani NC, Digiovanni CW, Holt SK, Benirschke SK, Hansen ST Jr., et al. Outcome after open reduction and internal fixation of Lisfranc joint injuries. J Bone Joint Surg Am 2000;82-A:1609-18.
Mulier T, Reynders P, Dereymaeker G, Broos P. Severe Lisfrancs injuries: Primary arthrodesis or ORIF? Foot Ankle Int 2002;23:902-5.
Ebramzadeh E, Knutsen AR, Sangiorgio SN, Brambila M, Harris TG. Biomechanical comparison of syndesmotic injury fixation methods using a cadaveric model. Foot Ankle Int 2013;34:1710-7.
Ly TV, Coetzee JC. Treatment of primarily ligamentous Lisfranc joint injuries: Primary arthrodesis compared with open reduction and internal fixation. A prospective, randomized study. J Bone Joint Surg Am 2006;88:514-20.
Panchbhavi VK. Controversies. Tech Foot Ankle Surg 2012;11:155.
van Koperen PJ, de Jong VM, Luitse JS, Schepers T. Functional outcomes after temporary bridging with locking plates in Lisfranc injuries. J Foot Ankle Surg 2016;55:922-6.
Del Vecchio JJ, Ghioldi M, Raimondi N, De Elias M. Minimally invasive medial plating of low-energy Lisfranc injuries: Preliminary experience with five cases. Adv Orthop 2016;2016:4861260.
Kestner CJ. Open reduction and fixation of unstable Lisfranc injuries using dorsal plates. Tech Foot Ankle Surg 2015;14:181-7.
Qiao Y, Li J, Shen H, Bao H, Jiang M, Liu Y, et al. Comparison of Arthrodesis and Non-fusion to Treat Lisfranc Injuries. Orthop Surg 2017;9:62-8.
Acknowledgments
We would like to thank Sean Bender, MD, for his assistance with the investigation and data curation.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patients have given their consent for their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
Vinod Panchbhavi is a consultant for Stryker Orthopaedics as well as an editor for Lippincott Williams and Wilkins Publishing.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Scofield, H.O., Lam, K.C., Stautberg, E.F. et al. Outcomes of Lisfranc Injuries Treated with Joint-Preserving Fixation. JOIO 54, 594–598 (2020). https://doi.org/10.1007/s43465-020-00070-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-020-00070-1