Abstract
Purpose
The false acetabulum lies more laterally and posteriorly compared with the true acetabulum. Spatial orientation of the pelvis is significantly altered in patients with neglected high hip dysplasia. There has been no study to investigate how pelvic or sagittal spinal alignment change after true acetabulum gains function with hip arthroplasty. The aim of this study was to investigate the effect of total hip arthroplasty with femoral shortening on spinopelvic parameters in patients with neglected high hip dysplasia.
Methods
Twenty patients with Crowe type 3 or 4 hip dysplasia, who underwent total hip arthroplasty with femoral shortening in our institution were evaluated preoperatively after completion of rehabilitation and return to their normal daily life. Sagittal alignment (sacral slope, pelvic incidence, global tilt, segmental lordosis, segmental kyphosis, GAP score) and coronal alignment angles (coronal tilt, Cobb angle) of patients were measured by two independent observers.
Results
Twenty patients underwent hip arthroplasty with femoral shortening followed up for a minimum of 12 months. We found higher preoperative global lordosis (68.7 ± 9.7) and sacral slope (52.1 ± 8.8) angles, but the pelvic incidences (57.9 ± 10.1) were in the normal range. No statistically significant difference in any sagittal spinopelvic parameters between pre- and postoperative measurements was detected. GAP scores also did not change significantly (p = 0.231). Coronal plane parameters (Cobb angle, coronal pelvic tilt) were the only parameters in which a statistical change was observed (p = 0.02, p = 0.05, respectively).
Conclusion
Lumbar lordosis and sacral slope values are outside standard ranges in patients with neglected dysplasia of the hip. The reconstruction of the distorted mechanics of the hip joint does not normalize sagittal pelvic and spine anatomy however improvements in coronal alignment were observed. Disease specific values of sagittal spinal alignment should be used in the treatment of lumbar degenerative problems in patients with neglected high hip dysplasia.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neglected hip dysplasia (NHD) is a challenging problem with distorted lumbopelvic anatomy and a broad spectrum of symptoms such as waddling gait, fatigue, low back and leg pain. The understanding of how important the sagittal spinal parameters are for a good clinical outcome in adult spine patients has led the physicians to consider how the distorted lumbopelvic anatomy affects the clinical outcomes of hip dysplasia patients [1]. Coronal and sagittal alignments of the spine in NHD patients display adaptive changes. Coronal alignment depends on which side the dysplasia is, how much limb length discrepancy the patient has and resultant magnitude of compensatory coronal tilt of the pelvis and spine. On the other hand, sagittal alignment is affected by a more posteriorly located hip joint (center of rotation) and increased lumbar lordosis and pelvic anteversion can be observed [2].
Spinal alignment has a direct effect on the orientation of the acetabulum in terms of inclination and version [3, 4]. This relation is distorted in Crowe 3–4 NHD patients as the true acetabulum is not functional. The true acetabulum lies far more medially and anteriorly than the false acetabulum in NHD patients. Total hip arthroplasty [5] surgery re-establishes the true acetabulum, changes the biomechanics of the lumbopelvic anatomy and recreates the relationship of the hip and spine.
The acetabulum, as a center of motion between the spine and lower extremity, is a direct influencer of the alignment of the spine. A decrease in the excessive pelvic anteversion and lumbar hyperlordosis might be observed after anatomic hip reconstruction surgery with a functional true acetabulum. In this study, we investigated normative spinal sagittal alignment in patients with Crowe 3–4 NHD and how spinal and pelvic parameters changed after THA surgery.
Materials and methods
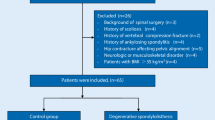
After obtaining institutional review board, a total number of 33 female patients diagnosed with Crowe 3 or 4 NHD were identified to have undergone THA with femoral shortening between the years from 2015 to 2019. Distance between inferior femoral head-neck junction and inter-teardrop line were divided into the pelvic height and the severity of proximal migration was determined according to Crowe classification on AP radiograph. Type 1–2 hip dislocations are referred as subluxation whereas type 3–4 dislocations as high hip dislocation and considered as advanced stage of the disease [6]. Patients who underwent a secondary surgical procedure such as debridement for surgical site infection, had non-union at the femoral osteotomy, loss of follow-up or incorrectly positioned acetabulum on radiographs were excluded from the study. Twenty female patients who met the inclusion criteria (4 bilateral, 16 unilateral) treated with THA with femoral shortening were evaluated radiographically with a minimum 1-year follow-up (mean 17.4 months, range 12–34). Prospectively collected full spine standing AP and lateral radiographs were evaluated retrospectively. All measurements were made by two independent observers under the supervision of two senior spine surgeons and the mean value was used for statistical evaluation. The Picture Archiving and Communicating System (PACS) (Centricity PACS-IW 3.7.3, GE Healthcare, Milwaukee, WI, USA) was used for all measurements.
Pre- and postoperative segmental lordosis (T12–L1, L1–L2, L2–L3, L3–L4, L4–L5, L5–S1), regional angulations (T2–T5, T5–T12, T10–T12, T10–L2, L4–S1), global lordosis (L1–S1), global kyphosis (T1–T12), global tilt, sacral slope (SS), Cobb angle, coronal pelvic tilt and preoperative spinosacral angle (SSA) were measured [7, 8] (Figs. 1, 2). Pre- and postoperative global alignment and proportion (GAP) Scores were calculated to evaluate the sagittal alignment of the spine more precisely [9]. We were not able to measure PI and PT preoperatively, because PI and PT are immeasurable in dislocated hip patients [10]. PI has a constant value in adults for every individual and it has a negligible positional change due to minimal range of motion of the sacroiliac joint between flexion and extension [11]. Thus, we accepted the postoperative measurements of PI after the anatomical reconstruction of the hip joint with THA. We used the postoperative values as reference values in other equations. Additionally, we used an equation that links PI with sacral slope (SS) and pelvic tilt [12]; PI = PT + SS to cross-check our postoperative measurements [13]. Preoperative spinosacral angle value also was used in a second equation that links global tilt with PI and SSA i to calculate the preoperative GAP score; GT = PI + 90 – SSA [9, 14].
a, b Pre- and postoperative segmental lordosis (T12–L1, L1–L2, L2–L3, L3–L4, L4–L5, L5–S1), segmental angulation (T2–T5, T5–T12, T10–T12, T10–L2, L4–S1), global lordosis (L1–S1), global kyphosis (T1–T12), spinosacral angle (SSA), global tilt and sacral slope (SS) were measured in a bilaterally operated patient
Statistical analysis was performed using Wilcoxon test to compare pre- and postoperative spinal and pelvic measurements. Intraclass correlation coefficient was also calculated to verify interobserver agreement. IBM SPSS Statistics v. 23.0 was used for statistical analysis.
Results
The mean age of the 20 patients was 51.6 (range 31–64) years. Interobserver agreement was moderate to high in all measurements (0.76–0.92). Pre- and postoperative values of coronal and sagittal measurements of the pelvis and spine are summarized at Table 1 for each patient. We found higher global lordosis (L1–S1: pre: 68.7 ± 9.7, post: 66.9 ± 8.7) and sacral slope (pre: 52.1 ± 8.6, post: 52.5 ± 7.3) in our patient group [15], but the increased lordosis and sacral slope did not return to normal values after surgery (p = 0.432 and p = 0.911, respectively). Postoperative pelvic incidences (57.9 ± 10.1) were in normal ranges in these patients [15, 16].
Lower segmental lordosis (L3–L4, L4–L5, L5–S1), regional angulation (T2–T5, T5–T12, T10–T12, T10–L2, L4–S1) and global kyphosis (T1–T12) were within normal ranges and upper segmental lordosis (L1–L2, L2–L3) values slightly above the normal ranges pre and postoperatively [8, 17]. We did not find any statistical significance between pre- and postoperative values of segmental lordosis, regional angulation, global lordosis (L1–S1), global kyphosis (T1–T12) and sacral slope (SS) (Table 2).
Preoperative GAP score calculation showed that 12 patients had proportioned alignment (total score: 0–2) and 8 patients had moderately disproportioned alignment (total score: 3–6). This distribution improved in favor of proportioned alignment in the postoperative group. 16 patients had proportioned alignment and 4 patients had moderately disproportioned alignment according to postoperative measurements. However, the postoperative changes in the GAP scores of the patients were not statistically significant (Table 2).
The only significant change was observed in the coronal alignment; mean Cobb angle and coronal pelvic tilt were decreased in the postoperative group, p = 0.02 and p = 0.05, respectively.
Discussion
Since the first description of the ‘hip-spine syndrome’ by Offerski and McNab in 1983, hip-related reasons were counted as one of the main causes of spine symptoms [1]. They classified hip-spine syndrome into simple, complex, primary and secondary subgroups and congenital hip dislocation was considered as a secondary hip-spine syndrome. Further investigations were made to evaluate the clinical and anatomical relationships of the hip and the spine and many researchers attributed importance to pelvic orientation as a fulcrum between the lower extremity and spine [18, 19]. The position of the pelvis is a direct influencer on both the spine and lower extremity, and has a critical role on human bipedalism [10, 13, 20]. It has been well known by spine surgeons that achieving an acceptable value of sagittal spinal parameters is of vital importance in spinal deformity patients. However, the importance of spinopelvic alignment in spinal deformity patients is a relatively new concept even in spinal surgery [4, 21,22,23].
Adaptive changes in spinopelvic alignment also occur in patients with hip osteoarthritis secondary to high hip dysplasia due to posterosuperiorly located center of motion (hip joint), increased lumbar lordosis, sacral slope and pelvic tilt [2]. Conversely, patients with only acetabular dysplasia without high hip dislocation do not develop a compensatory increase in sacral slope or lumbar lordosis [24, 25]. Nakamura et al. also reported a decrease in sacral slope and lumbar lordosis in primary coxarthrosis, whereas increase in these values were observed in secondary coxarthrosis in the same study [18]. These alterations in sagittal lumbopelvic anatomy can be explained by the concept of Dubousset [26], which hypothesizes the body’s tendency to maintain its posture with minimal effort in a ‘Cone of Economy’. It was explained with this theory how the human body maintains its bipedal posture on a foot-centered cone with minimal effort. Cervical and lumbar lordotic curves and pelvic orientation are the important constituents of spinopelvic anatomy and they are the major adaptations to maintain bipedalism with minimal effort. Dubousset mentioned the importance of the pelvis in sagittal spinopelvic alignment and spinal deformity. He also named the pelvis the ‘pelvic vertebra’ to emphasize its critical role as a transfer unit of body weight to the lower extremity [23, 26]. Upper segmental lordosis values (L1–L2, L2–L3) were slightly above the normal ranges according to some previously published studies, however the differences might be related to lack of number of our patient group [8, 17]. Regional angulation (T2–T5, T5–T12, T10–T12, T10–L2, L4–S1) values were within normal range in our patient group, but we have found an increased global lordosis (GL = L1–S1) in both pre- and postoperative measurements (GL: pre 68.7 ± 9.7, post 66.9 ± 8.7, respectively). A compensatory increase in sacral slope (SS) also followed the increase in lumber lordosis (SS: pre: 52.1 ± 8.6, post: 52.5 ± 7.3) as an adaptation to maintain posture with minimal effort. Increased GL and SS are consistent with the recent literature in NHD patients, as both are proportional and compensate for the posteriorly shifted sagittal gravity line of the spine [2].
If we look from the point of view of arthroplasty, variations in pelvic orientation may cause unexpected clinical results in hip arthroplasty patients. Buckland et al. stated that unsatisfactory postoperative outcomes were obtained after spinal surgery in THA patients due to posteriorly tilted pelvis which caused altered acetabular anteversion and a higher risk for dislocation. They also suggested spinal corrective surgery before THA to avoid alignment changes of the acetabulum after spinal correction [27, 28]. However, prophylactic spinal surgery for a successful THA would be an aggressive approach for patients who have no spinal column-related symptoms and therefore are not candidates for spinal surgery. In our study, we hypothesized the opposite: changing the center of rotation of pelvis from false acetabulum to true acetabulum might affect spinopelvic alignment after patients returned to their daily lives (Figs. 3, 4). However, the postoperative mean values of GL and SS showed minimal decrease and we could not find any significant change (GL from 68.7 to 66.9, p = 0.432) (SS from 52.1 to 52.5, p = 0.911). We can conclude that the anatomy that has adapted to the NHD over the years did not change much, even if the center of gravity of the pelvis changed. Postoperative values of GL and SS were still above the normal values postoperatively, but pelvic incidence was within the normal range in postoperative measurements (PI: 57.9 ± 10.1) [15, 16, 29]. Although there are pelvic incidences with fewer mean values in some studies, as we mentioned in the methods section, the reliability of acetabular cup-centered PI measurement has not tested before and we think that the difference between our results and previously reported values might be resulted from this methodological differences [30,31,32].
An example for the adaptive decreases in global lordosis and sacral slope. Sagittal spinopelvic measurements pre and postoperatively. a. Preoperative increased global lordosis (93°) and sacral slope (63°). b. Postoperative measurement of pelvic tilt (− 3°), pelvic incidence (54°) and a slightly decreased sacral slope (58°) and global lordosis (76°). GL global lordosis (dashed line), SS sacral slope (dotted line), PI pelvic ıncidence, PT pelvic tilt
In addition to spinopelvic parameters, we also calculated the Global Alignment and Proportion (GAP) Score pre-and postoperatively for every patient. Yilgor et al. proposed this new scoring system based on PI, SS, lumbar lordosis, GT and age to predict mechanical complications after spinal surgery [9]. There are 3 categories according to scores gained from these parameters; proportioned (total score: 0–2), moderately disproportioned (total score: 3–6) and severely disproportioned (total score: ≥ 7). Here, we used it only to evaluate the sagittal balance of the spine more objectively instead of predicting complication risk of spinal surgery as in the original article. Although some patients seem to have better scores postoperatively and the number of the patients in the moderately disproportioned group decreased from 8 to 4 patients, the overall comparison of pre- and postoperative scores showed no significant change (p = 0.231).
The dislocated hip irreversibly changes the sagittal plane evolution of the spine and a distorted but self-balanced anatomy is established. We are in the opinion that it would be right for the spinal surgeons to consider this issue and not to bring the sagittal parameters into the normative range in NHD patients during any spinal reconstruction, to not disturb the self-balanced anatomy. These unchanged spinopelvic anatomical features of NHD patients also compelled us to think if NHD patients need to undergo spinal instrumentation before or after THA, disease specific values of sagittal spinopelvic parameters should be used during the reconstruction of the spine.
We observed statistically significant improvements only in coronal alignment of the spine and pelvis postoperatively, in terms of Cobb angle and coronal pelvic tilt (p = 0.02 and p = 0.05, respectively). We attributed this to decreased leg length discrepancy of lower extremity postoperatively, particularly in unilateral cases. This is consistent with the current literature [33].
Our study had some important limitations that might have affected our results. Our number of patients is low as we had to deal with a very special subgroup of patient that would meet following criteria: adult patient with neglected high hip dysplasia (Crowe 3 or 4) without any history of other orthopedic problems and a history of THA with femoral shortening and an anatomical reconstruction of the acetabulum. It is not easy to reach larger patient numbers in such a specific group. Short follow-up time was another limitation of our study, hence longer duration of time might have been needed to observe anatomical alignment changes radiographically. However, in our opinion, it is not realistic to expect that the unchanged alignment at least one year after the completion of rehabilitation will change in the longer term. The majority of our patients (% 80) underwent unilateral hip surgery; theoretically, bilateral NHD cases might have been affected more than unilateral cases as most of the unilateral patients have a normal hip joint on the contralateral side. We could not compare these two groups (unilateral vs bilateral) because of insufficient number of patients for statistics.
In conclusion, NHD changes the sagittal alignment of the spine and some of the sagittal parameters (GL, SS) are out of standard ranges in these patients. The reconstruction of distorted mechanics of the hip joint does not normalize the pelvic and sagittal spine anatomy although improvements in coronal alignment were observed. If this group of patients needs spinal reconstructive surgery before or after normalizing the hip joint with THA, disease-specific values of sagittal spinal alignment should be used as reference. Further studies with a larger patient population are needed to better delineate the possible effects of hip reconstruction on spinal sagittal alignment.
References
Offierski CM, MacNab I (1983) Hip-spine syndrome. Spine (Phila Pa 1976) 8(3):316–321
Matsuyama Y et al (2004) Hip-spine syndrome: total sagittal alignment of the spine and clinical symptoms in patients with bilateral congenital hip dislocation. Spine (Phila Pa 1976) 29(21):2432–2437
Lazennec JY, Brusson A, Rousseau MA (2011) Hip-spine relations and sagittal balance clinical consequences. Eur Spine J 20(Suppl 5):686–698
Ames CP et al (2012) Impact of spinopelvic alignment on decision making in deformity surgery in adults: a review. J Neurosurg Spine 16(6):547–564
Khan SQ et al (2007) Prognostic value of midregional pro-adrenomedullin in patients with acute myocardial infarction: the LAMP (leicester acute myocardial infarction peptide) study. J Am Coll Cardiol 49(14):1525–1532
Crowe JF, Mani VJ, Ranawat CS (1979) Total hip replacement in congenital dislocation and dysplasia of the hip. J Bone Joint Surg Am 61(1):15–23
Vaz G et al (2002) Sagittal morphology and equilibrium of pelvis and spine. Eur Spine J 11(1):80–87
Stagnara P et al (1982) Reciprocal angulation of vertebral bodies in a sagittal plane: approach to references for the evaluation of kyphosis and lordosis. Spine (Phila Pa 1976) 7(4):335–342
Yilgor C et al (2017) Global alignment and proportion (GAP) score: development and validation of a new method of analyzing spinopelvic alignment to predict mechanical complications after adult spinal deformity surgery. J Bone Joint Surg Am 99(19):1661–1672
Roussouly P, Pinheiro-Franco JL (2011) Biomechanical analysis of the spino-pelvic organization and adaptation in pathology. Eur Spine J 20(Suppl 5):609–618
Schroeder N et al (2018) Pelvic incidence changes between flexion and extension. Spine Deform 6(6):753–761
Lipton GE, Bowen JR (2005) A new modified technique of triple osteotomy of the innominate bone for acetabular dysplasia. Clin Orthop Relat Res 434:78–85
Schwab F et al (2010) Adult spinal deformity-postoperative standing imbalance: how much can you tolerate? An overview of key parameters in assessing alignment and planning corrective surgery. Spine (Phila Pa 1976) 35(25):2224–2231
Obeid I et al (2016) Global tilt: a single parameter incorporating spinal and pelvic sagittal parameters and least affected by patient positioning. Eur Spine J 25(11):3644–3649
Noshchenko A et al (2017) Spinopelvic parameters in asymptomatic subjects without spine disease and deformity: a systematic review with meta-analysis. Clin Spine Surg 30(9):392–403
Legaye J et al (1998) Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J 7(2):99–103
Gelb DE et al (1995) An analysis of sagittal spinal alignment in 100 asymptomatic middle and older aged volunteers. Spine (Phila Pa 1976) 20(12):1351–1358
Nakamura Y (1996) Hip-spine syndrome: tracing of coxarthropathy and the relationship between the lumbar and sacral angles. Sendai Red Cross Med J 5:73–76
Ivanov DV et al (2018) Biomechanics of compensatory mechanisms in spinal-pelvic complex. J Phys Conf Ser 991:012036
Le Huec JC et al (2011) Pelvic parameters: origin and significance. Eur Spine J 20(Suppl 5):564–571
Cheng I (2012) Commentary: spinopelvic parameters-how far have we come? Spine J 12(5):447–448
Vrtovec T et al (2012) A review of methods for evaluating the quantitative parameters of sagittal pelvic alignment. Spine J 12(5):433–446
Dubousset J (1998) Importance de la vertèbre pelvienne dans l’équilibre rachidien. Application à la chirurgie de la colonne vertébrale chez l’enfant et l’adolescent. In: Villeneuve P (ed) Pied Équilibre et Rachis, Frison-Roche, Paris. pp. 141–149
Okuda T et al (2007) Stage-specific sagittal spinopelvic alignment changes in osteoarthritis of the hip secondary to developmental hip dysplasia. Spine (Phila Pa 1976) 32(26):E816–E819
Yoshimoto H et al (2005) Spinopelvic alignment in patients with osteoarthrosis of the hip: a radiographic comparison to patients with low back pain. Spine (Phila Pa 1976) 30(14):1650–1657
Dubousset J (1994) Three-dimensional analysis of the scoliotic deformity. In: Weinstein SL (ed) The pediatric spine: principles and practice. Raven Press, New York, pp 479–496
Buckland AJ et al (2019) Prevalence of sagittal spinal deformity among patients undergoing total hip arthroplasty. J Arthroplasty 35:160–165
Buckland AJ et al (2015) Acetabular anteversion changes due to spinal deformity correction: bridging the gap between hip and spine surgeons. J Bone Joint Surg Am 97(23):1913–1920
Iyer S et al (2016) Variations in sagittal alignment parameters based on age: a prospective study of asymptomatic volunteers using full-body radiographs. Spine (Phila Pa 1976) 41(23):1826–1836
Pesenti S et al (2018) The amount of proximal lumbar lordosis is related to pelvic incidence. Clin Orthop Relat Res 476(8):1603–1611
Zhu Z et al (2014) Sagittal alignment of spine and pelvis in asymptomatic adults: norms in Chinese populations. Spine (Phila Pa 1976) 39(1):E1–6
Hammerberg EM, Wood KB (2003) Sagittal profile of the elderly. J Spinal Disord Tech 16(1):44–50
Abe Y et al (2015) The impact of the leg-lengthening total hip arthroplasty on the coronal alignment of the spine. Scoliosis 10(Suppl 2):S4–S4
Funding
No funds were received in support of this work.
Author information
Authors and Affiliations
Contributions
Omur Caglar, Samet Isik, Mehmet Kaymakoglu, Halil Gokhan Demirkiran, Halil Gokhan Demirkiran, Bulent Atilla, Mazhar Tokgozoglu, Muharrem Yazici: Made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data. Omur Caglar, Samet Isik, Mehmet Kaymakoglu, Halil Gokhan Demirkiran, Halil Gokhan Demirkiran, Bulent Atilla, Mazhar Tokgozoglu, Muharrem Yazici: Drafted the work or revised it critically for important intellectual content; Omur Caglar, Samet Isik, Mehmet Kaymakoglu, Halil Gokhan Demirkiran, Halil Gokhan Demirkiran, Bulent Atilla, Mazhar Tokgozoglu, Muharrem Yazici: Approved the version to be published. Omur Caglar, Samet Isik, Mehmet Kaymakoglu, Halil Gokhan Demirkiran, Halil Gokhan Demirkiran, Bulent Atilla, Mazhar Tokgozoglu, Muharrem Yazici: Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. Omur Caglar: Attending surgeon. Samet Isik: Collecting data. Mehmet Kaymakoglu: Collecting data, Attending surgeon. Bulent Atilla: Attending surgeon. Mazhar Tokgozoglu: Attending Bulent Atilla surgeon. Muharrem Yazici.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
Ethical approval was obtained from Hacettepe University Faculty of Medicine.
Availability of data and material
We summerized our data as a table in the manucript.
Code availability
Not applicable.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Patients signed informed consent regarding publishing their data and photographs.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Caglar, O., Isik, S., Kaymakoglu, M. et al. Sagittal spinal alignment after total hip arthroplasty for neglected high hip dysplasia: does changing the distorted mechanics of the hip normalize spinal alignment?. Spine Deform 9, 221–229 (2021). https://doi.org/10.1007/s43390-020-00204-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-020-00204-3