Abstract
Study design
Retrospective.
Objectives
To assess final outcomes in patients with early-onset scoliosis (EOS) who underwent growth-preserving instrumentation (GPI).
Summary of background data
Various types of growth-preserving instrumentation (GPI) are frequently employed, but until recently had not been utilized long enough to assess final outcomes.
Methods
GPI “graduates” with multi-level congenital curves were identified. Graduation was defined as a final fusion or 5 years of follow-up without planned future surgeries. Outcomes included radiographic parameters and complications.
Results
26 patients were included. 11 had associated diagnoses; eight had fused ribs. 17 were treated with traditional growing rods, seven with vertically expandable prosthetic ribs, and two with Shilla procedures. The mean GPI spanned 12.3 levels including 10.7 motion segments, age at index surgery was 5.5 years, treatment spanned 7.5 years, and follow-up was 9.2 years. 24 patients underwent final fusion. Mean major curve decreased from 73° to 49° with index surgery (p < 0.01) and remained unchanged through a final follow-up. Final major curve was < 40° in 9 patients (35%), 40°–60° in 11 patients (42%), and > 60° in 6 patients (23%). None worsened throughout treatment. Mean T1–T12 height increased 2.4 cm with index surgery (p = 0.02) and 5.4 cm total (p < 0.01). T1–T12 height increased in all patients and was ultimately < 18 cm in 10 patients (38%), 18–22 cm in 10 patients (38%), and > 22 cm in 6 patients (23%). On average, there were 2.6 complications per patient, including 1.7 implant failures. 12 patients (46%) experienced ≥ 3 complications; four patients (15%) experienced none.
Conclusion
We observed successful prevention of deformity progression but substantial residual deformity among GPI graduates with multi-level congenital EOS. Most coronal curve correction was attained during GPI implantation; thoracic height improved throughout treatment. While some favorable results were found, treatment strategies allowing improved deformity correction would be valuable for this challenging population.
Level of evidence
Therapeutic-III.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The management of early-onset scoliosis (EOS) is notably complex, and within this heterogeneous group, patients with multi-level congenital anomalies are particularly challenging. While there is no accepted standard of care, growth-preserving instrumentation (GPI) is a common strategy for patients who are too skeletally immature for definitive spinal fusion. This category includes traditional growing rods (TGR) [1,2,3], vertically expandable prosthetic titanium ribs (VEPTR) [4, 5], guided growth procedures with screws (e.g. Shilla technique [6, 7]), guided growth procedures with sublaminar wires (e.g. Luque Trolley [8, 9]) and, most recently, magnetically controlled growing rods (MCGR) [10, 11]. However, treatment with GPI is notoriously fraught with complications [12, 13], carrying heavy financial and time burdens for patients, families and providers.
Recently, sufficient time has passed since the development of GPI to facilitate research of “graduates” [3, 14, 15]. Graduation typically culminates in definitive spinal fusion, though it remains controversial whether this final procedure is necessary [14, 16], and recent literature has suggested subsequent procedures are not uncommon [17]. While prior research has demonstrated the safety and efficacy of TGR in EOS patients with multi-level congenital etiologies [18], to our knowledge, no researchers have examined GPI graduates in this population. This study describes the characteristics and outcomes of patients with multi-level congenital scoliosis who have completed treatment with GPI. We hypothesized that GPI would successfully limit deformity progression but would not substantially correct existing deformity. We also hypothesized that initial coronal correction, as a proxy for curve flexibility, would predict final coronal correction and thoracic growth.
Materials and methods
We queried a prospective international multicenter EOS database founded in 1994 to identify “graduates” with congenital curves treated with GPI. Graduation was defined as having undergone definitive final fusion or cessation of treatment without planned future surgeries and at least 5 years of follow-up from GPI implantation. Pre-operative X-Rays were reviewed by two pediatric orthopedists, including the senior author, to confirm the presence of anomalies at multiple vertebral levels. Patients who had undergone GPI before entering the database were excluded. Patient who had previously undergone a short-segment fusion without GPI and still met all other inclusion criteria were eligible. GPI construct length was recorded on the basis of both total levels spanned and number of motion segments spanned; motion segments were defined as unfused levels within the construct (i.e., vertebral levels within short-segment fusions at the proximal anchors, distal anchors, centrally in Shilla procedures, and those from previous surgeries were not counted as motion segments).
Outcomes included radiographic parameters (coronal major curve, maximum global kyphosis, thoracic height measured from the T1 superior endplate to the T12 inferior endplate, coronal balance measured from a C7 plumb line to the central sacral vertical line, and sagittal balance measured from a C7 plumb line to the posterior corner of the S1 endplate), and complications. A 5° margin of error was accepted for Cobb technique measurements, and smaller differences were considered unchanged.
Statistical analysis
Groups were compared using Student’s t tests. Correlations were assessed using univariate linear regression and reported using Pearson’s coefficient. p < 0.05 was considered significant. Complications were defined at the treating surgeon’s discretion and grouped into five categories: implant failures, wound problems, medical issues, neurological deficits, and others.
Results
The database currently includes 2169 patients. 67 “graduates” with congenital scoliosis were identified. 12 were excluded because preoperative films were not available. 29 were excluded after a radiographic review showed their congenital anomalies were single-level rather than multi-level. Ultimately, 26 patients were included.
At index surgery, the mean age was 5.5 years (range 1.9–14.8 years). Mean follow-up was 9.2 years (range 1.9–17.7 years) with the mean treatment course spanning 7.3 years (range 1.8–14.1 years). Associated diagnoses, such as syndromes, were present in 11 patients, and 8 had fused ribs (Table 1). All patients were initially ambulatory; patient 7, who has Rett Syndrome, lost the ability to walk during the study. Three patients had previous spinal surgeries which were not considered part of the GPI treatment course: patient 6 had undergone hemivertebrectomy with in-situ fusion without instrumentation, patient 11 had undergone attempted surgery which was aborted before instrumentation due to loss of somatosensory evoked potentials, and patient 21 had undergone a limited fusion spanning several thoracic segments (further details were not available).
Mean preoperative major coronal curve magnitude was 73° (range 37°–128°) and mean global kyphosis was 45° (range 18°–74°). The majority of patients were treated with TGR and underwent a mean of 10.3 surgeries, including 7.5 lengthenings and 2.7 revisions (Table 2). Mean GPI spanned 12.3 segments (range 8–17 segments), including 10.7 motion segments (range 5–17segments). Six patients underwent some form of vertebral resection and four underwent thoracoplasty for fused ribs (Table 2). Final fusion was performed in 24 patients, and two concluded treatment with GPI left in place: 1 with spine-based TGR and 1 with a Shilla construct. Figures 1, 2 and 3 demonstrate representative radiographs of patients 9, 17, and 22, respectively.
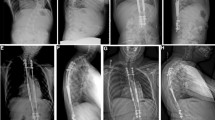
a PA and lateral preoperative standing radiograph of patient 9, a 3.3-year-old boy without associated diagnoses, demonstrating a 90° coronal curve, 13.5 cm T1-T12 height, 4.9 cm positive sagittal balance, and 2.3 cm coronal balance. b PA and lateral postoperative radiographs following placement of GPI at 3.6 years of age using a Shilla procedure from T2–L3 (13 levels, 9 motion segments due to fusion of T2–T3, T8–T10, and L2–L3) demonstrating a 21° coronal curve, 18.2 cm T1–T12 height, 1.4 cm positive sagittal balance, and 2.9 cm coronal balance. c PA and lateral standing radiographs at final follow-up (11.7 years of age) with instrumentation T2–L3 demonstrating a 38° coronal curve, 17.3 cm T1–T12 height, 2.5 cm positive sagittal balance, and 1.0 cm coronal balance
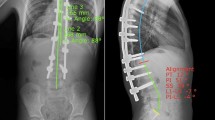
a PA and lateral preoperative standing radiographs of patient 17, a 5.4-year-old boy without associated diagnoses, demonstrating a 128° coronal curve, 9.7 cm T1–T12 height, 2.3 cm positive sagittal balance, and 1.5 cm coronal balance. b PA and lateral postoperative standing radiographs following placement of GPI at 5.4 years of age using spine-based TGR from T1–L3 (14 levels, 12 motion segments due to fusion of T1/T2 and L2/L3) demonstrating a 74° coronal major curve, 14.2 cm T1–T12 height, 1.2 cm negative sagittal balance, and 2.6 cm coronal balance. c PA and lateral standing radiographs after definitive fusion (11.3 years of age) with instrumentation C7–L2 demonstrating a 20° coronal major curve, 17.0 cm T1–T12 height, 0.3 cm positive sagittal balance, and 2.4 cm coronal balance
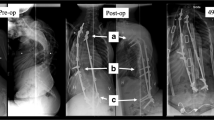
a PA and lateral preoperative standing radiographs of Patient 22, a 7.2-year-old boy with Trisomy 14, demonstrating a 76° coronal curve, 14.2 cm T1–T12 height, 2.2 cm positive sagittal balance, and 0.2 cm coronal balance. b PA and lateral postoperative standing radiographs following placement of GSI at 8.8 years of age using spine-based TGR from T2–L5 (15 levels, 12 motion segments due to fusion of T2–T4 and L4–L5) demonstrating a 44° coronal curve, 17.9 cm T1–T12 height, 3.5 cm positive sagittal balance, and 1.5 cm coronal balance. c PA and lateral standing radiographs at final follow-up (20.4 years of age) with instrumentation T2–L5 (T8–L4 instrumented and fused at the time of definitive fusion) demonstrating a 61° coronal major curve, 24.6 cm T1–T12 height, 2.2 cm negative sagittal balance, and 3.3 cm coronal balance
Over the course of treatment, 9 patients (35%) demonstrated coronal major curve correction ≤ 20%, 11 patients (42%) demonstrated correction between 20 and 50%, and 6 patients (23%) demonstrated correction > 50% (Table 3). At final follow-up, mean coronal major curve was < 40° in nine patients (35%), 40°–60° in 11 patients (42%), and > 60° in six patients (23%). 21 patients (81%) demonstrated a reduced coronal major curve at final follow-up, 5 (19%) remained within the 5° margin of measurement error, and none worsened. In the case of patient 16, the coronal major curve failed to improve because he was left uninstrumented due to a loss of neuromonitoring signals during final fusion. Overall, mean coronal major curve for the cohort decreased from 73° to 49° after GPI placement (p < 0.01), and this improvement was maintained until final follow-up (48°; p < 0.01) (Table 4).
Throughout the study period, thoracic height improved in all patients. Mean thoracic height increased during GPI implantation from 14.4 to 16.8 cm (p = 0.02) and then grew to 19.9 cm with final fusion (p < 0.01) (Table 4). At final follow-up, T1–T12 height was < 18 cm in ten patients (38%), 18-22 cm in ten patients (38%), and > 22 cm in six patients (23%).
Mean coronal and sagittal balance did not change during treatment (p = 0.91 and p = 0.66, respectively) (Table 4). Final coronal balance was < 2 cm in nine patients (35%), 2-4 cm in ten patients (38%), and > 4 cm in seven patients (27%). Final sagittal balance was < 2 cm in 13 patients (50%), 2-4 cm in eight patients (31%), and > 4 cm in five patients (19%). Of 24 patients with standing radiographs, 12 experienced improvements in coronal balance by a mean of 2.3 cm and 12 experienced worsened coronal balance by a mean of 2.2 cm. However, patient 19 experienced an increase of 11.6 cm; without this outlier, the mean increase was 1.3 cm. Of these 24 patients, sagittal balance worsened in nine patients by a mean of 2.7 cm and improved in 15 patients by a mean of 2.1 cm. Mean global kyphosis also remained unchanged after treatment (p = 0.68): it decreased from 45° to 36° after GPI placement (p = 0.03) before reverting to baseline by the final follow-up (Table 4).
Final correction of the coronal major curve was correlated with the correction attained during GPI implantation (r = 0.54, p = 0.004, Fig. 4). Correlation between the increase in thoracic height attained during GPI implantation and the final change in thoracic height demonstrated a trend that did not reach statistical significance (r = 0.38, p = 0.059). The coronal major curve correction attained subsequent to GPI placement was inversely related to the correction achieved during implantation (r = − 0.39, p = 0.047). Similarly, the increase in thoracic height subsequent to GPI placement was inversely related to the increase achieved during implantation (r = − 0.46, p = 0.017). No statistically significant correlations were detected between any of the following: initial coronal major curve correction and final change in thoracic height (r = 0.32, p = 0.11), initial coronal correction and change in thoracic height subsequent to implantation (r = 0.19, p = 0.35), age and final change in thoracic height (r = − 0.17, p = 0.41), age and final coronal correction (r = − 0.06, p = 0.76), number of motion segments spanned by GPI and final change in thoracic height (r = 0.21, p = 0.31), nor number of motion segments spanned by GPI and final coronal correction (r = 0.17, p = 0.41).
Scatterplot with regression line demonstrating the correlation between initial coronal major curve correction and final coronal major curve correction, each measured as percent change in coronal major curve angle from the preoperative deformity. Correlation coefficient (r) = 0.54, r2 = 0.29, p = 0.004, and the equation of the regression line is y = 0.73x + 0.092
Complications per patient ranged from 0 to 6 (Table 5). Mean number of complications was 2.7, including 1.7 implant failures and 0.5 wound problems (Table 6). Twelve patients (46%) experienced ≥ 3 complications and four patients (15%) experienced none. Three patients required reoperations following planned final fusion: patient 4 developed a pseudarthrosis, patient 6 developed a deep infection, and patient 18′s planned final fusion was aborted due to poor anchor fixation in the setting of severe osteopenia and completed one year later. Patient 19 developed respiratory failure with a large pleural effusion 2 days after final fusion which was treated with a chest tube and resolved 5 days later. Patient 16 was left uninstrumented due to neuromonitoring changes during final fusion as described above. No other complications occurred during or following final fusion.
Discussion
We evaluated the clinical courses, radiographic outcomes, and complications of 26 GPI graduates with EOS due to multi-level congenital anomalies. In this cohort, there was no progression of coronal curvature after GPI implantation, but there was a limited correction of the existing deformity. The coronal major curve did not worsen beyond the margin of measurement error in any patient, and thoracic height improved in all patients. However, at final follow-up, only 35% of patients attained a coronal major curve < 40°, and 23% demonstrated major curves > 60°. Similarly, 38% demonstrated final thoracic height < 18 cm, and only 23% attained thoracic height > 22 cm. The vast majority of curve correction was achieved during the index surgery, while thoracic height tended to improve during the index procedure as well as with subsequent treatment. Our results also support the hypothesis that initial coronal curve correction predicts final correction (r = 0.54, p = 0.004) but not the hypothesis that initial coronal correction predicts the ultimate change in thoracic height (r = 0.32, p = 0.11).
Only recently have GPI techniques been in use long enough to generate “graduation” results. Flynn et al. described the courses of 99 patients from the Growing Spine Study Group with various etiologies of EOS, focusing on treatment patterns [14]. The vast majority underwent final fusion but most spines had become “completely stiff” and achieved < 50% correction of residual coronal deformity during those procedures. More recently, Johnston et al. described the courses of 12 “graduates” of growth-sparing management with various etiologies [15]. The mean coronal major curve decreased from 88° to 47°, and the mean T1–T12 height increased from 13.3 to 22.3 cm. Their results compare favorably to this report. Importantly, Johnston et al. found that growth-sparing management maintained, but did not improve, pulmonary function as a percentage of normal. The Johnston et al. study included three congenital scoliosis patients out of 12 total subjects, and the Flynn et al. study included nine congenital patients out of 99 total subjects.
To our knowledge, the current study is the first to specifically examine GPI graduates with multi-level congenital anomalies. Campbell and Hell-Vocke studied a similar population in 2003. They examined thoracic growth among 21 congenital scoliosis patients with a unilateral bar and fused ribs treated with VEPTR and reported successful distraction, including 7.3% lengthening of congenital bars [19]. In 2013, Flynn et al. reported a multi-center analysis of congenital EOS patients treated with VEPTR [20]. Mean follow-up was 41 months, coronal major curve improved 9°, and thoracic height increased 3.4 cm. In the current study, we witnessed better correction of coronal curves and thoracic height: 25° and 5.4 cm mean improvement (it is an imperfect comparison as our growth occurred over a longer follow-up period). Dede et al. also reported VEPTR results in a cohort including a considerable number of congenital EOS patients (11 of 21) [4]. Their results were discouraging with a mean 1.8 cm gain in thoracic height over 11 lengthenings. The mean coronal major curve decreased from 80° to 67° with VEPTR placement and was maintained during treatment. However, outcomes from these studies are difficult to compare with our results as the former did not typically include graduation from surgical treatment.
Akbarnia et al. described more favorable results in 13 non-congenital EOS patients managed with TGR: mean coronal major curve correction was 66% after final fusion, and T1-S1 height increased by 10.6 cm over a mean of 4.4 years [3]. This compares favorably to our findings: 39% coronal curve correction after final surgery and mean 9.6 cm T1-S1 growth over 7.5 years. Similarly, Kamaci et al. treated 12 patients with idiopathic EOS using TGRs and witnessed 66% correction of the coronal major curve [21]. They achieved 6 cm of T1-T12 growth over 6.5 years, even without final fusion, which compares favorably to the 5.5 cm change in T1–T12 height seen in our cohort over 7.5 years of treatment, including final fusion.
Still, while radiographic gains may be limited among congenital patients compared to other EOS populations, and while some cases of congenital scoliosis do not naturally progress, we suspect that the results observed here far exceed those of non-operative care. The natural history of severe congenital cases can entail thoracic insufficiency syndrome with respiratory dysfunction and mortality [22]. The primary implication of the limited deformity correction and high complication rate seen in this study is the need for improved treatment strategies in this challenging population. MCGR may reduce complications but is unlikely to significantly alter the deformity correction seen in this study. In select patients, more aggressive vertebral osteotomies with short-segment fusions may afford better correction and allow continued growth in the remainder of the spine. However, this approach needs future research to determine its benefits, safety, and optimal patient population.
Recent literature investigating complications after planned final fusion for EOS reported a 20% reoperation rate and 1.5 complications per patient [17]. We witnessed three reoperations (12.5%) and 5 total complications (20.8%) among 24 patients undergoing definitive fusions. However, the aforementioned study had longer mean follow-up after final fusion: 4.3 years versus 2.2 years in our population (including 10 patients with < 1-year follow-up after final fusion) [17].
This study also elucidates the typical course of deformity correction in this population by examining several correlations. We found that initial coronal curve correction (i.e., during GPI implantation) correlated with final correction. However, greater initial correction is inversely correlated with subsequent correction. In other words, more straightening during GPI placement means less can be expected later. Still, that greater initial correction ultimately translates into a straighter spine. We also observed a strong trend (likely limited by sample size) suggesting a similar pattern for thoracic height. We found that age was not correlated with ultimate coronal correction or change in thoracic height. We suspect this is the result of two opposing phenomena: while younger patients tend to have more flexible spines, patients requiring treatment at younger ages tend to have more severe deformities.
This study has several limitations. Congenital scoliosis patients comprise a heterogeneous population with large variations in deformity and risk of progression, so our results are not perfectly generalizable to other EOS patients with multi-level congenital anomalies. Similarly, patients were treated at varying ages and for varying durations per the treating physicians’ discretion as there cannot be a universal standard of care in this population. Moreover, this study included patients treated with various forms of GPI which limits generalizability; however, this was deemed an acceptable weakness because no form of GPI has been proven significantly more or less effective than the alternatives. Additionally, this study included some patients who had undergone previous surgery before GPI (though not prior GPI) or who underwent various concomitant procedures during GPI implantation such as three-column osteotomies. These factors further limit generalizability but were also deemed acceptable because, given the heterogenous nature of multi-level congenital scoliosis, these patients would still meet inclusion criteria regardless of whether these prior or concomitant procedures were performed.
We were also susceptible to the usual limitations of retrospective research with occasionally limited data. For example, one patient’s earliest post-operative radiographs were 4.5 years after GPI implantation. In that time, he underwent nine lengthenings, so it was impossible to assess the correction gained during GPI implantation. Similarly, certain data was not consistently available in the database such as the extent of auto fusion at the time of definitive fusion. However, these occasions were rare, and the dataset was typically comprehensive and meticulous. Similarly, the radiographs we reviewed demonstrated varying quality, so in some cases it was difficult to definitively determine levels, define congenital anomalies, or measure angles. This issue was compounded by abnormal congenital anatomy. However, this limitation is inherent to the research topic, and low-quality radiographs were rare. Still, without definitively determining the extent of congenital fusions and auto fusions, it is not possible to ascertain whether thoracic height increased more than would be expected without GPI. Likewise, cross-sectional imaging was not routinely obtained in this study, so some aspects of growth could not be analyzed, such as the elongation of congenital fusions as described by Campbell and Hell-Vocke, which required baseline and follow-up computed tomography scans [19]. Another limitation is the lack of established criteria for “acceptable” outcomes in this population. To avoid overstating poor results, we included thresholds that would be universally considered unacceptable in the management of other forms of scoliosis. Additionally, given the rare nature of congenital multi-level EOS, we had a small sample size which limited power and prevented multivariate regressions. Finally, our analysis lacked a control group, though non-operative observation would be unethical in this population given the expected deformity progression and potential pulmonary compromise. Future studies in this area would benefit by including pulmonary function tests.
In conclusion, we studied 26 EOS patients with multi-level congenital anomalies who “graduated” from GPI management. There was no observed progression of coronal curvature after GPI implantation, but there was a limited correction of the existing deformity. The majority of coronal curve correction was attained during GPI implantation, whereas thoracic height continued to improve throughout treatment. While the natural history of complex congenital cases is highly variable, severe cases can have a very poor prognosis [22], so we view the absence of coronal progression after GPI implantation as an important outcome. However, the residual deformity and limited thoracic height attained in our cohort compare unfavorably to non-congenital EOS [3]. Therefore, when considering GPI, one must understand the goals of treatment and balance halting deformity progression with achieving deformity correction or gaining thoracic height in this complex population.
References
Bachabi M, McClung A, Pawelek JB et al (2018) Idiopathic early-onset scoliosis: growing rods versus vertically expandable prosthetic titanium ribs at 5-year follow-up. J Pediatr Orthop. https://doi.org/10.1097/BPO.0000000000001202
Thompson GH, Akbarnia BA, Campbell RM (2007) Growing rod techniques in early-onset scoliosis. J Pediatr Orthop 27(3):354–361. https://doi.org/10.1097/BPO.0b013e3180333eea
Akbarnia BA, Breakwell LM, Marks DS et al (2008) Dual growing rod technique followed for three to eleven years until final fusion: the effect of frequency of lengthening. Spine 33(9):984–990. https://doi.org/10.1097/BRS.0b013e31816c8b4e
Dede O, Motoyama EK, Yang CI et al (2014) Pulmonary and radiographic outcomes of VEPTR (Vertical Expandable Prosthetic Titanium Rib) treatment in early-onset scoliosis. J Bone Jt Surg Am 96(15):1295–1302. https://doi.org/10.2106/JBJS.M.01218
El-Hawary R, Kadhim M, Vitale M et al (2017) VEPTR Implantation to treat children with early-onset scoliosis without rib abnormalities: early results from a prospective multicenter study. J Pediatr Orthop 37(8):e599–e605. https://doi.org/10.1097/BPO.0000000000000943
Luhmann SJ, Smith JC, McClung A et al (2017) Radiographic outcomes of shilla growth guidance system and traditional growing rods through definitive treatment. Spine Deform 5(4):277–282. https://doi.org/10.1016/j.jspd.2017.01.011
McCarthy RE, McCullough FL (2015) Shilla growth guidance for early-onset scoliosis: results after a minimum of five years of follow-up. J Bone Jt Surg Am 97(19):1578–1584. https://doi.org/10.2106/JBJS.N.01083
Luque ER (1976) Treatment of scoliosis without arthrodesis or external support preliminary report. Clin Orthop Relat Res 119:276
Ouellet J (2011) Surgical technique: modern Luqué trolley, a self-growing rod technique. Clin Orthop 469(5):1356–1367. https://doi.org/10.1007/s11999-011-1783-4
Akbarnia BA, Pawelek JB, Cheung KMC et al (2014) Traditional growing rods versus magnetically controlled growing rods for the surgical treatment of early-onset scoliosis: a case-matched 2-year study. Spine Deform 2(6):493–497. https://doi.org/10.1016/j.jspd.2014.09.050
Lebon J, Batailler C, Wargny M et al (2017) Magnetically controlled growing rod in early onset scoliosis: a 30-case multicenter study. Eur Spine J 26(6):1567–1576. https://doi.org/10.1007/s00586-016-4929-y
Bess S, Akbarnia BA, Thompson GH et al (2010) Complications of growing-rod treatment for early-onset scoliosis: analysis of one hundred and forty patients. J Bone Jt Surg Am 92(15):2533–2543. https://doi.org/10.2106/JBJS.I.01471
Sankar WN, Acevedo DC, Skaggs DL (2010) Comparison of complications among growing spinal implants. Spine 35(23):2091–2096. https://doi.org/10.1097/BRS.0b013e3181c6edd7
Flynn JM, Tomlinson LA, Pawelek J et al (2013) Growing-rod graduates: lessons learned from ninety-nine patients who completed lengthening. J Bone Jt Surg Am 95(19):1745–1750. https://doi.org/10.2106/JBJS.L.01386
Johnston CE, Tran D-P, McClung A (2017) Functional and radiographic outcomes following growth-sparing management of early-onset scoliosis. J Bone Jt Surg Am 99(12):1036–1042. https://doi.org/10.2106/JBJS.16.00796
Jain A, Sponseller PD, Flynn JM et al (2016) Avoidance of “Final” surgical fusion after growing-rod treatment for early-onset scoliosis. J Bone Jt Surg Am 98(13):1073–1078. https://doi.org/10.2106/JBJS.15.01241
Poe-Kochert C, Shannon C, Pawelek JB et al (2016) Final fusion after growing-rod treatment for early onset scoliosis: Is it really final? J Bone Jt Surg Am 98(22):1913–1917. https://doi.org/10.2106/JBJS.15.01334
Elsebai HB, Yazici M, Thompson GH et al (2011) Safety and efficacy of growing rod technique for pediatric congenital spinal deformities. J Pediatr Orthop 31(1):1–5. https://doi.org/10.1097/BPO.0b013e318202c1f0
Campbell RM, Hell-Vocke AK (2003) Growth of the thoracic spine in congenital scoliosis after expansion thoracoplasty. J Bone Jt Surg Am. 85-A(3):409–420
Flynn JM, Emans JB, Smith JT et al (2013) VEPTR to treat nonsyndromic congenital scoliosis: a multicenter, mid-term follow-up study. J Pediatr Orthop 33(7):679–684. https://doi.org/10.1097/BPO.0b013e31829d55a2
Kamaci S, Demirkiran G, Ismayilov V, Olgun ZD, Yazici M (2014) The effect of dual growing rod instrumentation on the apical vertebral rotation in early-onset idiopathic scoliosis. J Pediatr Orthop 34(6):607–612. https://doi.org/10.1097/BPO.0000000000000169
Ramírez N, Cornier AS, Campbell RM, Carlo S, Arroyo S, Romeu J (2007) Natural history of thoracic insufficiency syndrome: a spondylothoracic dysplasia perspective. J Bone Jt Surg Am 89(12):2663–2675. https://doi.org/10.2106/JBJS.F.01085
Funding
No funding was received for this work.
Author information
Authors and Affiliations
Consortia
Contributions
Design: RCC, BY, AM, CB, NN, DL, GHT, OBA, PDS, SAS, JOS, JP, GMM, BA, Growing Spine Study Group. Data Acquisition, analysis and/or interpretation of work : RCC, BY, AM, CB, NN, DL, GHT, OBA, PDS, SAS, JOS, JP, GMM, BA, Growing Spine Study Group. Manuscript drafting and/or critically revising: RCC, BY, AM, CB, NN, DL, GHT, OBA, PDS, SAS, JOS, JP, GMM, BA, Growing Spine Study Group. Final approval: RCC, BY, AM, CB, NN, DL, GHT, OBA, PDS, SAS, JOS, JP, GMM, BA, Growing Spine Study Group.
Corresponding author
Ethics declarations
Ethical approval
IRB approval was obtained for this study.
Rights and permissions
About this article
Cite this article
Clement, R.C., Yaszay, B., McClung, A. et al. Growth-preserving instrumentation in early-onset scoliosis patients with multi-level congenital anomalies. Spine Deform 8, 1117–1130 (2020). https://doi.org/10.1007/s43390-020-00124-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-020-00124-2