Abstract
We reviewed the phenomenology of Post-Traumatic Stress Disorder (PTSD) and Traumatic Brain Injury (TBI), as well as the combined effects of PTSD + TBI comorbidity on functional outcomes. We also provide a series of research and treatment recommendations based on gaps in the literature with an emphasis on culture, interpersonal trauma, and treatment. Rates of PTSD + TBI are remarkably high. This comorbidity is especially common among combat-exposed military populations (with current estimates among Veterans returning from Afghanistan/Iraq at approximately 48%), as well as individuals who experience motor vehicle collisions (estimated base rate = 12%). These conditions often co-occur primarily because the events preceding the brain injury are both physically and psychologically traumatic. In many cases of PTSD + TBI, especially mild TBI, psychological factors largely account for accompanying functional outcomes (e.g., cognitive sequela, somatosensory health, quality of life, occupational functioning, social engagement). Overall, we suggest the importance of integrative teams in the early assessment, conceptualization, and treatment of PTSD + TBI. Psychological interventions and cognitive rehabilitation may synergistically improve psychological and functional outcomes for this patient population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Per the American Psychiatric Association’s (APA) Diagnostic and Statistical Manual for Mental Disorders (DSM-5-TR) [1], Posttraumatic Stress Disorder (PTSD) is a psychological condition that represents a constellation of psychiatric and cognitive symptoms (e.g., negative alterations to mood and cognition, distressing intrusions, augmented arousal responses, persistent avoidance behaviors) in response to experiencing a trauma. Trauma is defined as an exposure to actual or threatened death, serious injury, or sexual violence [1]. PTSD may arise from a variety of traumas (e.g., sexual assault, combat exposure) [1, 2]. Symptoms can be chronic [3] and often adversely affect functional outcomes across psychological, neurocognitive, medical/physical health, interpersonal/social, and adaptive domains [4]. A salient feature of PTSD is the high rate of comorbidity of other mental health conditions [1, 5, 6]. Such comorbidity is likely an artifact of symptom overlap [1, 6, 7], and may not represent unique syndromes/disorders. Risk of comorbidity may be a function of several variables such as trauma type, vocation, sex, and age of trauma exposure [8, 9].
Traumatic brain injury (TBI) has a high rate of co-occurrence with PTSD [1]. This comorbidity is especially common among combat-exposed military populations with current estimates among Veterans returning from Afghanistan/Iraq of 48% [1, 10, 11]. Elevated rates of PTSD + TBI (~ 12%) have also been documented among individuals who experience motor vehicle collisions (MVC) [12]. However, higher odds of PTSD in the setting of mild TBI (mTBI; see section titled “A Brief Primer on Traumatic Brain Injury: Mechanisms and Correlates” for clarification of TBIs) have been observed following blast injury (four-fold increase) compared to MVC (approximate two-fold increase) [12,13,14]. Extensive research links TBI with poor outcomes across psychiatric, physical, psychosocial, and neuropsychological health [15,16,17]. Like PTSD, TBI may arise from a multitude of events (e.g., physical assault, blast injury, MVC), all of which can lead to physical trauma to the head [18]. TBI and PTSD often co-occur (PTSD + TBI) primarily because the events preceding the brain injury are both physically and psychologically traumatic [13, 14, 19].
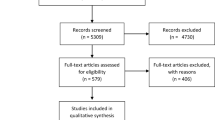
Despite the growing number of studies examining outcomes, diagnostic complications, and etiological factors in PTSD + TBI in the last decade, there is a paucity of qualitative and quantitative syntheses of this literature. A qualitative review by Vasterling et al. [20] addressed PTSD + TBI focusing on clinical considerations including clinical presentation, factors that can complicate recovery, and interventions (with emphasis on mTBI and pharmacotherapy) in civilian and military populations. Importantly, most studies have investigated PTSD + TBI in the context of military populations/combat-related traumas [10, 21, 22]. A search on the PsychINFO database for peer-reviewed publications in academic journals between years 2000 and 2023 containing phrases “Posttraumatic Stress Disorder” and “Traumatic Brain Injury,” excluding any articles containing terms “Military” and “Veteran” yielded a net total of n = 437 results. This same search barring exclusion criteria resulted in a markedly greater number of publications (n = 1,898).
In a separate vein, new evidence suggests that roughly 16% of civilian PTSD diagnoses include PTSD + TBI, largely due to MVCs [13]. Less is known about the potential roles non-combat trauma types (particularly sexual assault and contextual/sociocultural factors) play in PTSD + TBI. The aims of this narrative literature review were to (a) review phenomenology of PTSD and TBI (with emphasis on their unique effects on neuropsychiatric and neuropsychological functioning as well as cultural issues), (b) discuss the combined effects of PTSD + TBI on functional outcomes, (c) review treatment recommendations, and (d) examine specific gaps in the literature. We focused our qualitative review on peer-reviewed literature.
A Primer on Post-Traumatic Stress Disorder: Mechanisms and Correlates
PTSD is defined as a disorder of persistent nonrecovery following trauma exposure [3, 23]. PTSD symptom occurrence (within affected individuals) tends to decrease over time (e.g., from 80–94% two weeks after the event to 50% after three months) [24, 25]. Trauma is ubiquitous, with lifetime prevalence in U.S. national population = 89.7% [26]. While experience of trauma in any form is a probable lifetime event, not all who face a life-threatening trauma go on to develop enduring psychiatric complications such as PTSD. Using DSM-IV criteria, studies have reported lifetime prevalence of PTSD = 8.7–9.8% at age 75, in-line with that reported using DSM-5 criteria (8.3%) [1, 26, 27].
Accurate conceptualization of what constitutes a trauma is paramount to the accurate diagnosis of PTSD [1]. To this end, the DSM-5 operationalizes traumatic events in Criterion A of PTSD as follows: (1) must involve actual or perceived threat to personal safety, (2) are recognizable stressors that are expected to foment significant distress, (3) are different from normal experiences [28], (4) can be experienced indirectly or directly, and (5) if experienced indirectly, the individual must be close (e.g., friend, family member) of the involved person. Traumatic experience exists on multiple continuums, such as degree of severity and intimacy [3], and prior research suggests that PTSD rates may be a function of trauma type, and amount of trauma exposure [1, 29].
Cultural and Demographic Correlates
Numerous cultural and demographic factors (e.g., sex at birth, gender identity, sexual identity) are associated with trauma exposure and PTSD prevalence [1, 30, 31]. Although men are at higher risk of trauma across the lifespan, women are more likely to be exposed to interpersonal trauma, meet criteria for PTSD, and experience pathology for a longer duration [1, 32]. Differential rates of PTSD between sexes are likely related to the fact that as trauma is more personal (e.g., rape), risk of developing PTSD increases [33]. Similarly, non-heterosexual individuals demonstrate higher odds of having PTSD even when adjusting for race, gender, age, and PTSD risk factors (adjusted odds ratio = 1.7–3.7) [34]. The minority stress framework [35], a dominant theoretical model within the study of sexual identity development, suggests social discrimination and prejudices create internal and external stressors that exacerbate mental and physical health symptoms. Indeed, research suggests gender/sexual minorities may experience more severe mental health difficulties compared to cisgender/heterosexuals across multiple indicators [30, 31]. Therefore, both gender and sexual identity are important considerations when conceptualizing and diagnosing PTSD.
Other important factors to consider are racial identity, ethnicity, and socioeconomic status (SES) [1, 30, 31]. While literature shows that Persons of Color have greater risk of trauma exposure, SES moderates PTSD prevalence such that lower SES is associated with higher PTSD risk amongst Persons of Color [1, 36]. This may be explained in view of the diathesis-stress model where relative to White counterparts, Persons of Color are more likely be exposed to trauma. This risk is then compounded by low SES social contexts, which are associated with higher rates of violence and less access to care. Indeed, race is a putative correlate of SES. Conversely, studies found that PTSD is more common in developed/higher income countries, a phenomenon termed “the vulnerability paradox [37].” Many hypothesized explanations exist for this paradox such as lack of PTSD social education [38], underdiagnosis in economically developing areas of the world, and level of congruence of trauma with societal context (e.g., tragedies and violence being more common in poorer regions), and problematic assumptions (i.e., “the ecological fallacy”) [37].
Sociocultural factors also play a role in PTSD prevalence. Specifically, there is evidence that PTSD may be more common in individualistic than collectivistic cultures [39, 40]. For instance, in collectivistic cultures, holistic views of self-concept, and community orientation work to buffer resilience from traumatic events and engender acceptance. In individualistic Western cultures, people endorse less social support (i.e., a significant predictor of PTSD outcomes) compared to people in collectivistic cultures [41]. These data suggest that individual versus collective orientation may at least partly explain cross-national variations in PTSD rates. Manifestations of PTSD have also been shown to differ across cultures/countries [39, 40]. For example, de Jong and colleagues found that re-experiencing symptoms were the most prevalent PTSD feature in four war-stricken regions: Cambodia, Ethiopia, Algeria, and the Gaza Strip [42]. However, the least common symptoms among these four regions differed (i.e., hyperarousal for Cambodia and Ethiopia; avoidance behaviors for Algeria and Gaza) [42]. Lastly, growing literature has focused on the biopsychosocial intergenerational transmission of cultural trauma [39, 43]. That is, through epigenetic mechanisms, biologic changes in response to a cultural trauma may be transmitted from parents to their progeny. It remains unknown, whether epigenetic inheritance of cultural trauma is relevant to PTSD + TBI pathogenesis, pathophysiology, clinical presentation, and treatment factors in Persons of Color.
Taken together, cultural context and identity impact PTSD symptom presentation, prevalence, and resilience. Serious consideration of these factors is critical to culturally competent assessment and treatment of PTSD. Hinton and Good’s seminal text highlights mounting critiques of applying the PTSD diagnosis, which was formulated in Western settings, to culturally and historically distinct (from Western convention) contexts [39]. For instance, there are diverse forms of distress in non-Western cultures, which are not fully appreciated by the DSM PTSD framework. Further, certain areas of the world represent settings of chronic insecurity, which challenges the meaningfulness of PTSD diagnosis in these contexts.
Psychological Models of PTSD
Early conceptual models of PTSD focused on disruption of memories. Brewin and colleagues [44] proposed a dual representation theory of PTSD to describe the ways in which traumatic memories are represented/encoded. Storage/consolidation was thought to occur in two fashions: verbally accessible memories (VAM) and situationally accessible memories (SAM). They also proposed two types of emotional responses to memories: primary emotions (i.e., responses conditioned during the trauma, such as fear) and secondary emotions (i.e., feelings that occur after trauma is processed, such as anger). According to this model, successful emotional processing of trauma requires activation of the VAM and SAM memory representational systems. Such activation is thought to promote resolution of schema conflicts and construction of new meaning through integration [3, 44].
Other prevailing models postulate experiential avoidance paradoxically functions to repress processing of trauma memories [45], thereby impeding meaningful change in trauma memory despite simultaneously experiencing trauma-intrusions [46]. Another theoretical consideration in conceptualizing PTSD relates to the existential consequences of trauma. Janoff-Bulman outlined major metaphysical assumptions that are damaged due to experiencing a trauma including personal invulnerability, the world as a meaningful and predictable place, and the self as good or worthy [47]. Further, experiencing trauma involving interpersonal violence challenges notions of safety and agency (i.e., control over the world) [47].
Concerning data-driven approaches, Cox et al. used factor analysis and latent construct modeling of associated psychological symptoms to develop the internalizing/externalizing model of PTSD [48]. Their analysis resulted in a model consisting of one internalizing and two externalizing dimensions [49]. Later work using cluster analysis confirmed model fit when applied to patterns of PTSD psychopathology [50]. The internalizing/externalizing model of PTSD has played important roles in explaining the high rate of comorbidity among people with PTSD and identifying subtypes within PTSD [3].
Physiological Models of PTSD
Central neurobiological models may be organized in their anatomical taxonomy, from microscopic substrates (e.g., intracellular neurotransmitters), to intermediate systems (e.g., the hypothalamic–pituitary–adrenal [HPA] axis), and finally macroscopic structures (e.g., brain regions) [3]. Neurotransmitters represent integral chemical substrates that facilitate chemotransduction among neurons. Notably, neurochemical alterations have been documented in PTSD across multiple neurotransmitters. In a sample of persons with PTSD, Vaiva and colleagues [51] found lower levels of plasma gamma-amino butyric acid, a common inhibitory neurotransmitter, which they interpreted as a marker of increased stress response. Conversely, literature has documented higher levels of serotonin (5H-T) and dopamine in individuals with PTSD, likely associated with hyperarousal, hypervigilance, panic/anxiety symptoms, negative alteration of mood, and intrusive memories [52]. Another important neurotransmitter involved in PTSD is norepinephrine, a central chemical messenger of the noradrenergic system amidst stress responses [3]. A systematic literature review found a consistent relation between noradrenergic system dysregulation and physiological (i.e., hyperarousal, startle response, increased pulse/blood pressure) and cognitive reexperiencing symptoms [53]. Relatedly, dysfunction of the noradrenergic system has been linked with heightened levels of baseline norepinephrine in the absence of imminent threat as seen in PTSD [54].
The HPA axis also plays a key role in the neurobiological model of PTSD. The HPA axis refers to a pathway involving three distinct, yet interrelated components (i.e., hypothalamus, pituitary gland, and adrenal glands) that work to coordinate the noradrenergic system in the stress response [3]. While under normal circumstances, stress activates the HPA axis and indirectly results in cortisol secretion, heterogenous forms of dysregulation have been observed in PTSD, likely an artifact of comorbid conditions among other reasons [54]. For example, hypocortisolism (i.e., low cortisol levels) and heightened levels of glucocorticoids has been observed in PTSD, presumably in relation to enhanced encoding of traumatic memories [55].
Broadly, multiple brain structures interact through passage of neurochemicals to give rise to PTSD phenomenology. Some of the studied neural substrates implicated in PTSD are the prefrontal cortex, hippocampus, and amygdala [3]. The former plays several key roles including executive control while the latter has functions related to arousal and generating emotional responses [56]. The prefrontal cortex and amygdala work in close unison through the frontolimbic neural circuit. Under normal circumstances, this neuronal system works to buffer immediate emotional reactions. Neuroimaging studies have documented hyperactivation/disinhibition in the amygdala, and subsequent inhibition of the prefrontal cortex, during exposure to stress in persons with PTSD [3, 57]. This pattern of activation is posited to contribute to physiological responses seen in PTSD [58].
Psychological, Neuropsychological, and Physical Health Correlates
Rates of comorbidity within PTSD are remarkably high. The base rate of comorbid mental health conditions among those with PTSD is 80% [1]. Prior research using a large outpatient psychiatric sample found that of “Axis I” disorders [27], PTSD demonstrated the highest lifetime prevalence of comorbidity. To this end, the entirety of their sample of persons with a primary diagnosis of PTSD (n = 82; 100%) met diagnostic criteria for at least one other mood disorder [59]. Conditions with notably high lifetime prevalence of comorbidity with PTSD were major depressive disorder (82%), panic disorder with agoraphobia (60%), generalized anxiety disorder (50%), social phobia (43%), substance use disorder (34%), and obsessive–compulsive disorder (24%) [59].
In addition to “Axis I” conditions, PTSD is associated with increased risk of personality (i.e., “Axis II”) disorders. An epidemiological study using data from the National Epidemiologic Survey on Alcohol and Related Conditions (n = 34,653) observed co-occurrence rates of PTSD and borderline personality disorder (BPD) ranging from 24.2% to 30.2%, depending on principal diagnosis [60]. Contemporary research attributes the concurrence of PTSD and BPD to interactive effects between genetic and environmental factors [61]. Studies have consistently demonstrated epigenetic changes in key stress-related systems (e.g., HPA) secondary to childhood traumas [62, 63]. Individuals with history of childhood trauma show a pattern of blunted HPA reactivity, marked with decreased neuroendocrine release of adrenocorticotropin and cortisol [64]. These stress hormones promote normal HPA function.
Neuropsychological Correlates
The pattern of neurocognitive deficits often observed in persons with PTSD include information processing speed, attention, learning and memory, and executive functioning [56, 65,66,67]. A meta-analysis of cognitive functioning in PTSD found largest effects for verbal learning (d = -0.62), processing speed (d = -0.59), attention/working memory (d = -0.50), and verbal memory (d = -0.46) [68]. A separate meta-analysis found similar results but indicated that memory and learning were the domains most consistently associated with PTSD pathology [69].
History of childhood sexual trauma moderates the relation between PTSD and cognitive functioning. To illustrate, Bremner and colleagues [70] found that women with history of childhood trauma showed pronounced deficits in verbal declarative memory compared to healthy controls, and even women with childhood trauma and no PTSD. A more recent study found children with sexual abuse history and PTSD symptoms demonstrated reduced ability to inhibit prepotent responding on the Stroop test [71]. Additional analyses indicated that the actual experience of sexual abuse was the most robust predictor of the observed cognitive changes [71]. In trauma-exposed children with a history of PTSD, a recent meta-analysis documented a wide range of neuropsychological deficits in domains of general intelligence (d = -0.88), language/verbal (d = -0.65), visuospatial (d = -0.53), information processing (d = -0.62), learning and memory (d = -0.67), and executive functioning (d = -0.52) [62]. Others have noted that cortical functions (e.g., language, visuomotor skills) are generally spared among children with PTSD [56].
Studies have conceptualized cognitive deficits in PTSD in the context of psychological and neurobiological factors. For instance, Shin and colleagues found that experiential avoidance symptoms in PTSD predicted verbal memory functioning and subsequent severity of PTSD symptomology [72]. Evidence from neurochemistry, neurobiology, and neuroimaging literature has linked morphological and system-based abnormalities to cognitive changes seen in PTSD [3, 57, 58]. HPA axis dysregulation resulting in decreased cortisol and increased glucocorticoids is associated to neuronal damage to hippocampal gray matter and amygdala, brain regions associated with memory formation and emotional regulation, respectively [56]. Additionally, structural imaging studies in persons with PTSD have documented subcortical volumetric changes in relation with cognitive impairment [73]. Other neuroimaging studies in PTSD have observed involution in the anterior cingulate cortex and left insula, which subserve the limbic-prefrontal circuit and cognitive flexibility [74].
A Brief Primer on Traumatic Brain Injury: Mechanisms and Correlates
The Centers for Disease Control and Prevention defines TBI as an injury to the head caused by a bump, blow, or jolt that may or may not result in penetration to intracranial tissues, and causes disturbance (i.e., change) to normal brain function. It is estimated that 1.7 million individuals incur TBI-related injuries annually [75]. Rates of TBI are especially high among soldiers returning from recent conflicts (i.e., more than 30%) [18]. However, these figures may be inflated due to diagnostic complications relating to mild forms of TBI, which encompass the majority of civilian and military head injuries [16]. To illustrate, Faul and colleagues estimated that between 70 and 88% of TBIs among military populations are mild in nature [75]. Mechanisms are categorized as closed head injury or penetrating head injury. In response to TBI, a series of complex reactions may occur (e.g., primary = coup-contre-coup injury; secondary = physiological processes such as hypoxia or intracranial cerebral hypertension). As seen in PTSD, there is increasing evidence of disruption to neurotransmitter system functioning (particularly catecholaminergic) post-TBI [76].
In diagnosing TBI with conventional methods, severity is often graded as mild, moderate, or severe depending on multiple factors. These include observable changes in mentation, results from a structural imaging exam, Glasgow Coma Scale (GCS) scores, associated duration of loss of consciousness (LOC), and posttraumatic amnesia (PTA) [66]. Several classification systems of TBI severity have been advanced, the most rudimentary being type of physical trauma (i.e., whether there is penetrance of the cranium; open vs. closed head injury) [77]. Another popular way to grade brain injury severity considers the extent of initial mental status alteration/impairment using GCS score (most proximal to the injury; lower = more severe), time to follow commands (higher = more severe) as well as duration of LOC and PTA (higher = more severe) [77]. Under this convention, mTBI = GCS of 13–15, LOC of ≤ 30 min (or none), and PTA of < 60 min; moderate TBI = GCS of 9–12, LOC of 30 min to 24 h, and PTA of 1 to 24 h; and severe TBI = GCS of ≤ 8, LOC of > 24 h, and PTA of > 24 h [77]. The Mayo TBI Severity Classification System was developed to use the maximum amount of available data in determining severity, with the following classes: Symptomatic (Possible) TBI, Mild (Probable) TBI, and Moderate-Severe (Definite) TBI [78]. The Mayo System considers similar content as earlier approaches (e.g., GCS, LOC, PTA), but also takes into account broader neuro-physiological (i.e., intracerebral hematoma, subdural hematoma, epidural hematoma, cerebral contusion, hemorrhagic contusion, dura penetrated, subarachnoid hemorrhage, brainstem injury—the presence of any classified as Moderate-Severe TBI) and somatic (i.e., blurred vision, confusion/mental state changes, dazed, dizziness, focal neurologic symptoms, headache, nausea—all under the classification of Symptomatic TBI) features [78].
Like PTSD, neuropsychological sequelae associated with TBI include diminished processing speed, attention, working memory, memory, and executive functions [17]. Interestingly, while differential relations between trauma type and outcomes have been documented in TBI, literature has shown little evidence of TBI outcomes differing by mechanism (e.g., blast vs. non-blast injury) [18]. Neuropsychiatric and behavioral symptoms resulting after mTBI have been termed post-concussive symptoms [17]. Along with the neurocognitive deficits listed above, behavioral comorbidities include mood alterations (e.g., depression), personality disorders, and somatic features (e.g., fatigue, dizziness, sleep disturbance) [17].
A common phenomenon observed in TBI is decreasing insight/awareness (of deficits) as severity increases. Accordingly, the majority of neuropsychiatric and cognitive subjective complaints associated with TBI occur in mTBI [19]. In tandem with this finding, history of premorbid psychiatric problems is related with greater level of symptom complaints post-TBI [79]. Gil and colleagues found that subjects with less severe TBI were better able to recall events leading up to brain trauma, thereby increasing risk of subsequent PTSD diagnosis [65]. However, it is important to note that recall of traumatic event is not solely related to insight, as is the case for more severe TBIs. In these instances, extensive PTA is likely part of the clinical presentation, thereby hindering ability to recollect the trauma. Importantly, a burgeoning literature highlights racial/ethnic disparities across the spectrum of TBI-care (e.g., diagnosis, injury mechanism, post-injury adjustment, long-term outcomes) that are crucial to appreciate [80].
Comorbid Posttraumatic Stress Disorder and Traumatic Brain Injury
Indeed, there is high rate of comorbidity between PTSD and TBI (PTSD + TBI), likely partly due to considerable symptom overlap between these conditions [81, 82]. Alway and colleagues found that most cases of PTSD in TBI (66.7%), disease onset was delayed [83]. Frequency of PTSD was highest one-year post-injury, remained relatively stable two years post-injury, and diminished thereafter. Whereas experiential avoidance in stand-alone PTSD is a well-known predictor of poor outcome(s), Sofko et al. observed Veterans with both history of LOC and behavioral avoidance symptoms had worse psychological and quality of life outcomes [84]. This suggests LOC may function synergistically with behavioral avoidance. Al-Ozairi and colleagues reported similar findings, where shorter duration of PTA was a significant predictor of development of mental health conditions such as PTSD [85]. One possible explanation could the TBI-associated cognitive deficits disrupting the construction of lucid memories involving the traumatic event, thereby complicating the ability to sufficiently process negative trauma-related experiences [86, 87]. Furthermore, there is evidence to suggest that individuals who experience PTA after MVCs may reconstruct memories of the traumatic event that include negative self-attributions (e.g., guilt and shame) [13]. This phenomenon could partly explain the delayed onset of PTSD in patients with mTBI. Together, alterations to consciousness due to TBI may pose unique threats to adverse mental health outcomes and meaning making around the traumatic event.
In many cases of PTSD + TBI, especially mTBI, psychiatric factors may better explain cognitive and other functional (e.g., physical, social) outcomes compared to objective markers (e.g., performance on cognitive tests) [17]. For example, in a large (n = 2,525) U.S. Army sample following a 12-month tour in Iraq, PTSD and depression symptom severity accounted for the association between mTBI and postconcussive sequela (e.g., inattention, headaches) [86]. These findings were mirrored in a separate study examining neurocognitive test performance in a sample of Veterans with and without mTBI, such that PTSD symptoms explained all group differences [87]. Another cross-sectional study of Veterans with PTSD found that after adjusting for TBI, depression, education, and premorbid intellectual functioning, perceptions of cognitive problems mediated the association between PTSD and concurrent functional outcomes [88]. Larbig et al. observed 73% of their sample of patients with PTSD reported subjective cognitive decline in memory after experiencing a traumatic event that was associated with objective deficits in memory [89]. This suggests temporal precedence between PTSD and perceived memory deficits such that the latter is likely a consequence of trauma exposure rather than premorbid memory dysfunction. Conceptually, multiple studies have shown that PTSD symptomology in individuals with comorbid TBI amplifies severity of endorsement and perception of symptoms [16, 90, 91]. In a sample of children and adolescent MVC survivors with mTBI, persistent post-concussive symptoms were associated with PTSD symptoms rather than with comorbid PTSD + mTBI, emotional status predicted persistence in post-concussive symptoms six months post-MVC [92]. PTSD symptoms also predict worse functional outcomes as far as 24-months post-trauma in MVC survivors without TBI [93]. Together, these studies indicate psychiatric factors exacerbate post-concussive symptoms, predict adverse functional outcomes (thereby prolonging recovery), and highlight the importance of assessing psychological functioning and symptom validity in patients with comorbid PTSD + TBI.
Persons with comorbid PTSD + TBI show discernable neurobiological differences compared to their counterparts with only one condition. In their review, Kaplan and colleagues summarize pathophysiological overlap between TBI and PTSD including gray matter changes to the amygdala, hippocampus, and prefrontal cortex [94]. Their review also highlights unique signs of neuroinflammation, excitotoxicity, and oxidative damage (all of which lead to neuronal augmentation, damage, degeneration, and death) in those with PTSD + TBI [94]. Literature examining neuropsychological functioning in PTSD + TBI is somewhat sparse, likely due to controversy over symptom overlap between and complexity of these conditions [13]. Biopsychosocial alterations (e.g., neurotransmitter disruptions and psychosocial stressors) are often present in each condition, which raises questions of whether there are additive adverse outcomes in PTSD + TBI. Most literature in this area has focused on PTSD + mTBI [51,52,53, 76]. In a sample of MVC survivors with PTSD + TBI, Hickling and colleagues [95] reported deficits across all tasks that were speed dependent, as well as delayed verbal memory. Conversely, a more recent study reported no significant group differences in processing speed, executive functioning, or memory performance between Veterans with PTSD + mTBI and mTBI alone [22]. A review of cognitive functioning in comorbid PTSD + mTBI in Veteran samples showed a general profile consistent with the overlapping pattern of deficits between PTSD and TBI (i.e., mild to moderate impairment in attention, processing speed, and executive functions) [10].
Distinguishing between acute TBI and post-traumatic stress (PTS) symptomatology is not difficult when the TBI is moderate to severe and symptoms may be attributed to longer periods of LOC, cranial fractures, and other signs of traumatic brain damage [20]. However, when dealing with mTBI, the distinction is more complex [20]. Many symptom complaints in persons with mTBI may be due to PTS or general psychological distress [21]. In the case of blast-injuries and other combat-related TBI’s, the event associated with the PTS and TBI symptoms is often either the same or temporally related [18]. Therefore, clinicians might consider an early screening, poly-treatment approach to intervene with PTSD + TBI [96].
Treatment Considerations for PTSD + TBI
Per an updated systematic review on PTSD treatment outcomes in patients with a history of TBI, cognitive behavioral interventions such as prolonged exposure (PE), and cognitive-processing therapy (CPT) evidenced favorable outcomes when clinicians also targeted cognitive deficits associated with TBI [97]. A recent RCT demonstrated the effectiveness of TBI-adapted CBT for patients with acquired brain injury (CBT-ABI) [96]. However, these adaptations may not be sufficiently tailored to PTSD + TBI comorbidity, and could be improved by focus on content adaptations as the majority of prior research addresses process adaptations. Gallagher et al. conducted a systematic review of treatment adjustments for cognitive impairment following TBI to identify clusters of recommendations based on the prior research framework [98, 99]. Using thematic analysis, five clusters were identified: therapeutic formulation and education specific to TBI, attention and concentration (i.e. shortening tasks, gradually increasing task duration, use of cues); communication (e.g., encourage clarifying questions, requests to slow down or repeat information), memory (e.g., using a diary or notebook for therapy tasks, cue recent events to facilitate recall), and executive functioning (e.g., planning events or interactions with patients, making lists) [99]. The most frequently reported adaptations were the use of memory aids and socializing patients to the CBT model, both of which are process rather than content adaptations. Content adaptations, such as increased psychoeducation about PTSD + TBI may amplify treatment effectiveness. However, more research is needed to examine the effectiveness of a broad range of interventions and the utility of specific content applications.
Psychological interventions for PTSD + TBI should also focus on appraisals of post-trauma cognitive functioning in addition to appraisals of the traumatic event, trauma coping self-efficacy, and negative self-appraisals. Samuelson et al. [88] found that perceptions of cognitive problems, but not objective performance, mediated the association between PTSD symptom severity and functional outcomes after adjusting for TBI severity. Further, negative self-appraisals, posttraumatic cognitions, and trauma coping self-efficacy may be mechanisms of the association between perception of cognitive problems and PTSD symptoms [100]. Additionally, Vasterling and colleagues [20] emphasize the importance of psychoeducation in targeting decreased inhibition, recklessness, and affect dysregulation, all of which may endanger the patient or reduce treatment adherence/engagement. Psychoeducation as an intervention aligns well with the robust literature highlighting the importance of the nocebo effect (i.e., negative patient expectations/beliefs about recovery dampening treatment effects) in TBI. Even a single session of psychoeducation reduces severity and duration of post-concussive syndrome symptoms) [101]. Given the nature of PTSD + TBI pathogenesis (i.e., often concurrently arising from the same event), future research should consider the nocebo effect when designing interventions.
Integrated models of care [13] in which clinical psychologists, neuropsychologists, and medical providers conduct joint assessments and intervention may improve functional and psychological outcomes by enhancing the effects of neurocognitive rehabilitation. Early assessment, interventions combining neurocognitive rehabilitation and evidence-based psychological techniques may also enhance treatment outcomes. To this end, a pilot study reported improvements in post-concussive symptoms, prospective memory, and to a lesser degree, psychiatric symptoms, in Veterans who underwent Cognitive Symptom Management and Rehabilitation Therapy (CogSMART), a compensatory cognitive training intervention that utilizes cognitive rehabilitation and psychoeducation approaches [102]. Lastly, as mTBI literature supports setting expectations for cognitive recovery is an important recovery variable.
Suicide Risk in mTBI and PTSD
A final treatment consideration for PTSD + TBI is the well-established elevated risk of suicide in this patient population. A recent systematic review and meta-analysis of 17 studies indicated a twofold higher risk of suicide among mTBI patients relative to healthy controls [103]. The two studies with a follow-up period reported that between 0.50 and 0.59% of people diagnosed with concussion or mTBI died by suicide within a median of four years of the injury [103]. A review of military and civilian studies on risk of suicide and TBI reported that comorbid depression and PTSD are significant post-TBI risk factors [104]. Additional factors serve as moderators or mediators of TBI and suicide risk such as substance misuse, female sex, and sleep disturbance [104]. TBI severity may impact the degree to which mental health factors explain elevated risk, though literature on this topic is sparse.
Indeed, most of the relevant reviews focus on the full spectrum of TBI severity rather than mTBI. Barnes and colleagues [105] compared suicide risk factors among a matched sample of OEF/OIF military personnel and Veterans with PTSD, as well as those with PTSD and history of mTBI. Differences between risk factors were minimal suggesting that PTSD symptom severity may account for most of the suicide risk elevation in this population. Another study identified a similar effect for depression symptom severity at 3 and 6-month follow-up [106]. Thus, the presence of mTBI alone may not elevate suicide risk above and beyond PTSD or depression symptom severity, indicating the critical need to assess patients with mTBI for psychiatric symptoms. Other mental health factors, such as substance use and insomnia may also elevate risk [106].
Given the elevated risk of suicide in PTSD + TBI, integrated care teams would benefit from implementing evidence-based practices for assessing and managing suicide risk in the context of PTSD treatment and cognitive rehabilitation. Considering the lack of evidence for standalone treatment packages for reducing suicidality in PTSD + TBI, as well as the multifaceted clinical needs of this population, treatment teams may benefit from using adjunctive interventions that either serve as a therapeutic framework or which can easily fit into a treatment plan largely focused on PTSD + TBI [107,108,109]. Specifically, the Collaborative Assessment and Management of Suicidality (CAMS) [110] is a therapeutic framework that both evaluates suicide risk and serves as a patient-centered treatment to help patients manage their SI. Other brief interventions may also be useful such as the Safety Planning Intervention (SPI) [111], the Hope Box intervention) [112], and means safety counseling (e.g., CALM) [113]. All such interventions can be easily integrated into a broader treatment plan targeting PTSD + TBI.
Overall, extant research on treatment considerations for PTSD + TBI is limited by the focus on adaptations of CBT rather than a broader range of interventions. Some research has identified treatment adaptations that are not beneficial for TBI (and perhaps by extension, PTSD + TBI). For example, in persons with TBI, early treatment in the acute phase [114] and more extensive treatment in the post-acute phase [115, 116] may be counterproductive. Nevertheless, past research has shown that “common factors” (e.g., therapeutic alliance) account for the most substantial portions of client outcomes regardless of intervention/presentation [117]. Indeed, there is growing evidence for compassion-focused, narrative, holistic, third-wave CBT, existential, and humanistic approaches to PTSD + TBI [86, 98, 118,119,120,121,122,123,124]. At this time, there is limited robust empirical evidence clarifying relative strengths and weaknesses among evidence-based treatments for PTSD + TBI.
Conclusions
PTSD and TBI are two distinct yet frequently co-occurring conditions. PTSD arises from adverse emotional reactions to experiencing a traumatic event which works to disrupt systems of meaning, self-concept, perception of others, and fundamental beliefs about the world. TBI occurs when external force(s) to the head result in observable cognitive changes, possible alterations in level of consciousness/orientation, and insults to brain matter. Injuries that result in TBI pathology are often in themselves perceived as traumatic by virtue of their nature and intensity. Traumatic events and head injuries alike occur in contexts, many of which literature shows are relevant.
Literature reviewed above provides a variety of explanations for high rates of comorbidity and symptom overlap between the two conditions. Symptom overlap exists in both psychological and cognitive respects. For instance, negative mood alterations and anxiety are common in both PTSD and TBI (i.e., neuropsychiatric post-concussive symptoms). Further, both conditions show a comparable constellation of cognitive deficits. Obfuscation of PTSD and TBI symptoms increases as severity approaches mTBI in comparison with moderate to severe TBI. Generally, cognitive features in severe forms of TBI are easily discernable from those of PTSD. Literature shows some clear differences between stand-alone TBI and (comorbid) PTSD + TBI. In the case of the latter, PTSD severity convincingly accounts for (and exacerbates) perceived cognitive and functional impairments in TBIs (especially mTBI). We present research and clinical recommendations based on gaps in the current literature reviewed here in Tables 1, 2. An inherent limitation of qualitative literature reviews is lack of formal quality and validity assessment of studies included. We attempted to balance this by focusing our narrative review on peer-reviewed literature.
Data Availability
Not applicable.
Code Availability
Not applicable.
References
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 5th ed. American Psychiatric Publishing, Inc.; 2013. https://doi.org/10.1176/appi.books.9780890425596.
Bradley R, Greene J, Russ E, Dutra L, Westen D. A multidimensional meta-analysis of psychotherapy for PTSD. Am J Psychiatry. 2005;162:214–27. https://doi.org/10.1176/APPI.AJP.162.2.214/ASSET/IMAGES/LARGE/N72T6.JPEG.
Resick PA, Monson CM, Rizvi SL. Posttraumatic stress disorder. In: Craighead WE, Miklowitz DJ, Craighead LW, editors. Psychopathology: History, diagnosis, and empirical foundations. 2nd ed. Wiley; 2013. pp. 244–284.
Tsai J, Shen J. Exploring the link between posttraumatic stress disorder and inflammation-related medical conditions: An epidemiological examination. Psychiatr Q. 2017;88:909–16. https://doi.org/10.1007/S11126-017-9508-9/TABLES/2.
Orme DR. Diagnosing PTSD: Lessons From Neuropsychology. APA. 2012;24:397–413. https://doi.org/10.1080/08995605.2012.695262.
Rosen GM, Lilienfeld SO. Posttraumatic stress disorder: An empirical evaluation of core assumptions. Clin Psychol Rev. 2008;28:837–68. https://doi.org/10.1016/J.CPR.2007.12.002.
Rosen GM, Spitzer RL, McHugh PR. Problems with the post-traumatic stress disorder diagnosis and its future in DSM-V. Br J Psychiatry. 2008;192:3–4. https://doi.org/10.1192/BJP.BP.107.043083.
Brewin CR, Andrews B, Valentine JD. Meta-analysis of risk factors for posttraumatic stress disorder in trauma-exposed adults. J Consult Clin Psychol. 2000;68:748–66. https://doi.org/10.1037/0022-006X.68.5.748.
Wanklyn SG, Belus JM, Pukay-Martin ND, Cyr KS, Girard TA, Monson CM. Trauma types as differential predictors of posttraumatic stress disorder (PTSD), major depressive disorder (MDD), and their comorbidity. Can J Behav Sci. 2016;48:296–305. https://doi.org/10.1037/CBS0000056.
Dolan S, Martindale S, Robinson J, Kimbrel NA, Meyer EC, Kruse MI, Morissette SB, Young KA, Gulliver SB. Neuropsychological sequelae of PTSD and TBI following war deployment among OEF/OIF veterans. Neuropsychol Rev. 2012;22:21–34. https://doi.org/10.1007/S11065-012-9190-5/TABLES/1.
Yurgil KA, Barkauskas DA, Vasterling JJ, Nievergelt CM, Larson GE, Schork NJ, Litz BT, Nash WP, Baker DG. Association between traumatic brain injury and risk of posttraumatic stress disorder in active-duty marines. JAMA Psychiat. 2014;71:149–57. https://doi.org/10.1001/JAMAPSYCHIATRY.2013.3080.
Bryant RA, Creamer M, O’Donnell M, Silove D, Clark CR, McFarlane AC. Post-traumatic amnesia and the nature of post-traumatic stress disorder after mild traumatic brain injury. J Int Neuropsychol Soc. 2009;15:862–7. https://doi.org/10.1017/S1355617709990671.
Bryant R. Post-traumatic stress disorder vs traumatic brain injury. Dialogues Clin. Neurosci. 2011;13:251–262. https://doi.org/10.31887/DCNS.2011.13.2/RBRYANT.
Loignon A, Ouellet MC, Belleville G. A systematic review and meta-analysis on PTSD following TBI among military/veteran and civilian populations. J Head Trauma Rehabil. 2020;35:E21–35. https://doi.org/10.1097/HTR.0000000000000514.
Brickell TA, Lange RT, French LM. Health-related quality of life within the first 5 years following military-related concurrent mild traumatic brain injury and polytrauma. Mil Med. 2014;179:827–38. https://doi.org/10.7205/MILMED-D-13-00506.
Nampiaparampil DE. Prevalence of Chronic Pain After Traumatic Brain Injury: A Systematic Review. JAMA. 2008;300:711–9. https://doi.org/10.1001/JAMA.300.6.711.
Riggio S, Wong M. Neurobehavioral sequelae of traumatic brain injury, Mt. Sinai J Med A J Transl Pers Med. 2009;76:163–172. https://doi.org/10.1002/MSJ.20097.
Belanger HG, Kretzmer T, Yoash-Gantz R, Pickett T, Tupler LA. Cognitive sequelae of blast-related versus other mechanisms of brain trauma. J Int Neuropsychol Soc. 2009;15:1–8. https://doi.org/10.1017/S1355617708090036.
Glaesser J, Neuner F, Lütgehetmann R, Schmidt R, Elbert T. Posttraumatic stress disorder in patients with traumatic brain injury. BMC Psychiatry. 2004;4:1–6. https://doi.org/10.1186/1471-244X-4-5/TABLES/2.
Vasterling JJ, Jacob SN, Rasmusson A. Traumatic brain injury and posttraumatic stress disorder: Conceptual, diagnostic, and therapeutic considerations in the context of co-occurrence. J Neuropsychiatry Clin Neurosci. 2017;30: 91–100. https://doi.org/10.1176/APPI.NEUROPSYCH.17090180.
Belanger HG, Kretzmer T, Vanderploeg RD, French LM. Symptom complaints following combat-related traumatic brain injury: Relationship to traumatic brain injury severity and posttraumatic stress disorder. J Int Neuropsychol Soc. 2010;16:194–9. https://doi.org/10.1017/S1355617709990841.
Gordon SN, Fitzpatrick PJ, Hilsabeck RC. No effect of PTSD and other psychiatric disorders on cognitive functioning in veterans with mild TBI. Clin Neuropsychol. 2011;25:337–47. https://doi.org/10.1080/13854046.2010.550634.
Steckler T, Risbrough V. Pharmacological treatment of PTSD – Established and new approaches. Neuropharmacology. 2012;62:617–27. https://doi.org/10.1016/J.NEUROPHARM.2011.06.012.
Rothbaum BO, Foa EB. Subtypes of posttraumatic stress disorder and duration of symptoms. In: Davidson JRT, Foa EB, editors. Posttraumatic stress disorder: DSM-IV and beyond. American Psychiatric Press; 1993. p. 23–35.
Norris FH. Epidemiology of trauma: Frequency and impact of different potentially traumatic events on different demographic groups. J Consult Clin Psychol. 1992;60:409–18. https://doi.org/10.1037/0022-006X.60.3.409.
Kilpatrick DG, Resnick HS, Milanak ME, Miller MW, Keyes KM, Friedman MJ. National estimates of exposure to traumatic events and PTSD prevalence using DSM-IV and DSM-5 criteria. J Trauma Stress. 2013;26:537–47. https://doi.org/10.1002/JTS.21848.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed., text revision. American Psychiatric Publishing, Inc.; 2000. https://doi.org/10.1176/APPI.BOOKS.9780890423349.
Breslau N, Kessler RC. The stressor criterion in DSM-IV posttraumatic stress disorder: An empirical investigation. Biol Psychiatry. 2001;50:699–704. https://doi.org/10.1016/S0006-3223(01)01167-2.
Galea S, Nandi A, Vlahov D. The epidemiology of post-traumatic stress disorder after disasters. Epidemiol Rev. 2005;27:78–91. https://doi.org/10.1093/EPIREV/MXI003.
Borgogna NC, McDermott RC, Aita SL, Kridel MM. Anxiety and depression across gender and sexual minorities: Implications for transgender, gender nonconforming, pansexual, demisexual, asexual, queer, and questioning individuals. Psychol Sex Orientat Gend Divers. 2019;6:54–63. https://doi.org/10.1037/SGD0000306.
Borgogna NC, Aita SL, Aita LJ. Minority stress in consensually non-monogamous individuals: Mental health implications. Sex Relation Ther. 2021. https://doi.org/10.1080/14681994.2021.1959545.
Olff M. Sex and gender differences in post-traumatic stress disorder: An update. Eur J Psychotraumatol. 2017;8:1351204. https://doi.org/10.1080/20008198.2017.1351204.
Kessler RC, Sonnega A, Bromet E, Hughes M, Nelson CB. Posttraumatic stress disorder in the national comorbidity survey. Arch Gen Psychiatry. 1995;52:1048–60. https://doi.org/10.1001/ARCHPSYC.1995.03950240066012.
Roberts AL, Rosario M, Corliss HL, Koenen KC, Austin SB. Elevated risk of posttraumatic stress in sexual minority youths: Mediation by childhood abuse and gender nonconformity. Am J Public Health. 2012;102:1587–93. https://doi.org/10.2105/AJPH.2011.300530.
Meyer IH. Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: Conceptual issues and research evidence. Psychol Bull. 2003;129:674–97. https://doi.org/10.1037/0033-2909.129.5.674.
Atwoli L, Stein DJ, Koenen KC, McLaughlin KA. Epidemiology of posttraumatic stress disorder: Prevalence, correlates and consequences. Curr Opin Psychiatry. 2015;28:307–11. https://doi.org/10.1097/YCO.0000000000000167.
McNally RJ. Resolving the vulnerability paradox in the cross-national prevalence of posttraumatic stress disorder. J Anxiety Disord. 2018;54:33–5. https://doi.org/10.1016/J.JANXDIS.2018.01.005.
Perrin M, Vandeleur CL, Castelao E, Rothen S, Glaus J, Vollenweider P, Preisig M. Determinants of the development of post-traumatic stress disorder, in the general population. Soc Psychiatry Psychiatr Epidemiol. 2014;49:447–57. https://doi.org/10.1007/S00127-013-0762-3/TABLES/4.
Hinton DE, Good BJ. Culture and PTSD: Trauma in global and historical perspective. University of Pennsylvania Press; 2016. https://doi.org/10.9783/9780812291469.
Jayawickreme N, Jayawickreme E, Foa EB. Using the individualism-collectivism construct to understand cultural differences in PTSD. In: Gow K, Celinski M, editors. Mass trauma: Impact and recovery issues. Nova Science Publishers; 2012. pp. 55–76.
Ozer EJ, Best SR, Lipsey TL, Weiss DS. Predictors of posttraumatic stress disorder and symptoms in adults: A meta-analysis. Psychol Bull. 2003;129:52–73. https://doi.org/10.1037/0033-2909.129.1.52.
De Jong JTVM, Komproe IH, Van Ommeren M, El Masri M, Araya M, Khaled N, Van De Put W, Somasundaram D. Lifetime events and posttraumatic stress disorder in 4 postconflict settings. JAMA. 2001;286:555–62. https://doi.org/10.1001/JAMA.286.5.555.
Lehrner A, Yehuda R. Cultural trauma and epigenetic inheritance. Dev Psychopathol. 2018;30:1763–77. https://doi.org/10.1017/S0954579418001153.
Brewin CR, Dalgleish T, Joseph S. A dual representation theory of posttraumatic stress disorder. Psychol Rev. 1996;103:670–86. https://doi.org/10.1037/0033-295X.103.4.670.
Hayes SC, Wilson KG, Gifford EV, Follette VM, Strosahl K. Experiential avoidance and behavioral disorders: A functional dimensional approach to diagnosis and treatment. J Consult Clin Psychol. 1996;64:1152–68. https://doi.org/10.1037/0022-006X.64.6.1152.
Ehlers A, Clark DM. A cognitive model of posttraumatic stress disorder. Behav Res Ther. 2000;38:319–45. https://doi.org/10.1016/S0005-7967(99)00123-0.
Janoff-Bulman R. Shattered assumptions: Towards a new psychology of trauma. Free Press; 1992.
Cox BJ, Clara IP, Enns MW. Posttraumatic stress disorder and the structure of common mental disorders. Depress Anxiety. 2002;15:168–71. https://doi.org/10.1002/DA.10052.
Miller MW, Greif JL, Smith AA. Multidimensional Personality Questionnaire profiles of veterans with traumatic combat exposure: externalizing and internalizing subtypes. Psychol Assess. 2003;15:205–15. https://doi.org/10.1037/1040-3590.15.2.205.
Miller MW, Kaloupek DG, Dillon AL, Keane TM. Externalizing and internalizing subtypes of combat-related PTSD: A replication and extension using the PSY-5 scales. J Abnorm Psychol. 2004;113:636–45. https://doi.org/10.1037/0021-843X.113.4.636.
Vaiva G, Thomas P, Ducrocq F, Fontaine M, Boss V, Devos P, Rascle C, Cottencin O, Brunet A, Laffargue P, Goudemand M. Low posttrauma GABA plasma levels as a predictive factor in the development of acute posttraumatic stress disorder. Biol Psychiatry. 2004;55:250–4. https://doi.org/10.1016/J.BIOPSYCH.2003.08.009.
Southwick SM, Paige S, Morgan CA, Bremner JD, Krystal JH, Charney DS. Neurotransmitter alterations in PTSD: Catecholamines and serotonin. Semin Clin Neuropsychiatry. 1999;4:242–8. https://doi.org/10.153/SCNP00400242.
O’Donnell T, Hegadoren KM, Coupland NC. Noradrenergic mechanisms in the pathophysiology of post-traumatic stress disorder. Neuropsychobiology. 2004;50:273–83. https://doi.org/10.1159/000080952.
Sherin JE, Nemeroff CB. Post-traumatic stress disorder: The neurobiological impact of psychological trauma. Dialogues Clin Neurosci. 2011;13:263–78.
de Quervain DJF, Margraf J. Glucocorticoids for the treatment of post-traumatic stress disorder and phobias: A novel therapeutic approach. Eur J Pharmacol. 2008;583:365–71. https://doi.org/10.1016/J.EJPHAR.2007.11.068.
Getz GE. Applied biological psychology. Springer; 2014. https://doi.org/10.1891/9780826109231.
Rauch SL, Whalen PJ, Shin LM, McInerney SC, MacKlin ML, Lasko NB, Orr SP, Pitman RK. Exaggerated amygdala response to masked facial stimuli in posttraumatic stress disorder: A functional MRI study. Biol Psychiatry. 2000;47:769–76. https://doi.org/10.1016/S0006-3223(00)00828-3.
Milad MR, Pitman RK, Ellis CB, Gold AL, Shin LM, Lasko NB, Zeidan MA, Handwerger K, Orr SP, Rauch SL. Neurobiological basis of failure to recall extinction memory in posttraumatic stress disorder. Biol Psychiatry. 2009;66:1075–82. https://doi.org/10.1016/J.BIOPSYCH.2009.06.026.
Brown TA, Campbell LA, Lehman CL, Grisham JR, Mancill RB. Current and lifetime comorbidity of the DSM-IV anxiety and mood disorders in a large clinical sample. J Abnorm Psychol. 2001;110:585–99. https://doi.org/10.1037/0021-843X.110.4.585.
Pagura J, Stein MB, Bolton JM, Cox BJ, Grant B, Sareen J. Comorbidity of borderline personality disorder and posttraumatic stress disorder in the U.S. population. J Psychiatr Res. 2010;44:1190–1198. https://doi.org/10.1016/J.JPSYCHIRES.2010.04.016.
Cattane N, Rossi R, Lanfredi M, Cattaneo A. Borderline personality disorder and childhood trauma: Exploring the affected biological systems and mechanisms. BMC Psychiatry. 2017;171:1–14. https://doi.org/10.1186/S12888-017-1383-2.
Malarbi S, Abu-Rayya HM, Muscara F, Stargatt R. Neuropsychological functioning of childhood trauma and post-traumatic stress disorder: A meta-analysis. Neurosci Biobehav Rev. 2017;72:68–86. https://doi.org/10.1016/J.NEUBIOREV.2016.11.004.
Maniam J, Antoniadis C, Morris MJ. Early-life stress, HPA axis adaptation, and mechanisms contributing to later health outcomes. Front Endocrinol (Lausanne). 2014;5:73. https://doi.org/10.3389/FENDO.2014.00073/BIBTEX.
Carpenter LL, Shattuck TT, Tyrka AR, Geracioti TD, Price LH. Effect of childhood physical abuse on cortisol stress response. Psychopharmacology. 2011;214:367–75. https://doi.org/10.1007/S00213-010-2007-4/TABLES/1.
Gil T, Calev A, Greenberg D, Kugelmass S, Lerer B. Cognitive functioning in post-traumatic stress disorder. J Trauma Stress. 1990;3:29–45. https://doi.org/10.1002/JTS.2490030104.
Sanders C, Ziegler A, Schmitter-Edgecombe M. Traumatic brain injury and the impact of secondary influences. In: Arnett PA, editor. Secondary influences on neuropsychological test performance: Research findings and practical applications. Oxford University Press; 2013. pp. 292–327.
Vasterling JJ, Constans JI, Brailey K, Sutker PB. Attention and memory dysfunction in posttraumatic stress disorder. Neuropsychology. 1998;12:125–33. https://doi.org/10.1037/0894-4105.12.1.125.
Scott JC, Matt GE, Wrocklage KM, Crnich C, Jordan J, Southwick SM, Krystal JH, Schweinsburg BC. Quantitative meta-analysis of neurocognitive functioning in posttraumatic stress disorder. Psychol Bull. 2015;141:105–40. https://doi.org/10.1037/A0038039.
Schuitevoerder S, Rosen JW, Twamley EW, Ayers CR, Sones H, Lohr JB, Goetter EM, Fonzo GA, Holloway KJ, Thorp SR. A meta-analysis of cognitive functioning in older adults with PTSD. J Anxiety Disord. 2013;27:550–8. https://doi.org/10.1016/J.JANXDIS.2013.01.001.
Bremner JD, Vermetten E, Afzal N, Vythilingam M. Deficits in verbal declarative memory function in women with childhood sexual abuse-related posttraumatic stress disorder. J Nerv Ment Dis. 2004;192:643–9. https://doi.org/10.1097/01.NMD.0000142027.52893.C8.
Barrera M, Calderón L, Bell V. The cognitive impact of sexual abuse and PTSD in children: A neuropsychological study. J Child Sex Abus. 2013;22:625–638. https://doi.org/10.1080/10538712.2013.811141.
Shin KM, Chang HY, Cho SM, Kim NH, Kim KA, Chung YK. Avoidance symptoms and delayed verbal memory are associated with post-traumatic stress symptoms in female victims of sexual violence. J Affect Disord. 2015;184:145–8. https://doi.org/10.1016/J.JAD.2015.05.051.
O’Doherty DCM, Chitty KM, Saddiqui S, Bennett MR, Lagopoulos J. A systematic review and meta-analysis of magnetic resonance imaging measurement of structural volumes in posttraumatic stress disorder. Psychiatry Res Neuroimaging. 2015;232:1–33. https://doi.org/10.1016/J.PSCYCHRESNS.2015.01.002.
Meng L, Jiang J, Jin C, Liu J, Zhao Y, Wang W, Li K, Gong Q. Trauma-specific grey matter alterations in PTSD. Sci Rep. 2016;6:33748. https://doi.org/10.1038/srep33748.
Faul M, Xu L, Wald MM, Coronado V, Dellinger AM. Traumatic brain injury in the United States: National estimates of prevalence and incidence, 2002–2006. Inj Prev. 2010;16:A268–A268. https://doi.org/10.1136/IP.2010.029215.951.
Jenkins PO, Mehta MA, Sharp DJ. Catecholamines and cognition after traumatic brain injury. Brain. 2016;139:2345–71. https://doi.org/10.1093/BRAIN/AWW128.
Rao V, Lyketsos C. Neuropsychiatric sequelae of traumatic brain injury. Psychosomatics. 2000;41:95–103. https://doi.org/10.1176/APPI.PSY.41.2.95.
Malec JF, Brown AW, Leibson CL, Flaada JT, Mandrekar JN, Diehl NN, Perkins PK. The Mayo classification system for traumatic brain injury severity. J Neurotrauma. 2007;24:1417–1424. https://doi.org/10.1089/neu.2006.0245.
Kashluba S, Paniak C, Casey JE. Persistent symptoms associated with factors identified by the WHO task force on mild traumatic brain injury. Clin Neuropsychol. 2008;22:195–208. https://doi.org/10.1080/13854040701263655.
Saadi A, Bannon S, Watson E, Vranceanu AM. Racial and ethnic disparities associated with traumatic brain injury across the continuum of care: A narrative review and directions for future research. J Racial Ethn Heal Disparities. 2022;9:786–799. https://doi.org/10.1007/s40615-021-01017-4.
Helmick K, Guskiewicz K, Barth J, Cantu R, Kelly JP, McDonald C Eric, Flaherty C Stephen, Bazarian J, Bleiberg JD, Carter C Tony, Cooper M Jimmy, Drake AD, French LD, Grant L Gerald, Holland C Martin, Hunt R, Hurtado M Timothy, Jenkins C Donald, Johnson C Thomas, Kennedy JD, Labutta C Robert, Lopez C Mary, McCrea MD, Montgomery M Harold, Riechers M Ronald, Ritchie C Elspeth, Ruscio L Bruce, Schneider C Theresa, Schwab K, Tanner C William, Zitnay GD, Warden D. Defense and Veterans Brain Injury Center Working Group on the acute management of mild traumatic brain injury in military operational settings: Clinical practice guideline and recommendations. Washington, DC: Defense and Veteran Brain Injury Center; 2006. https://www.psychceu.com/brain_Basics/Brain_courses/clinical_practice_guideline_recommendations.pdf.
Vasterling JJ, Dikmen S. Mild traumatic brain injury and posttraumatic stress disorder: Clinical and conceptual complexities. J Int Neuropsychol Soc. 2012;18:390–3. https://doi.org/10.1017/S1355617712000367.
Alway Y, McKay A, Gould KR, Johnston L, Ponsford J. Factors associated with posttraumatic stress disorder following moderate to severe traumatic brain injury: A prospective study. Depress Anxiety. 2016;33:19–26. https://doi.org/10.1002/DA.22396.
Sofko CA, Currier JM, Hill BD, Drescher KD. History of loss of consciousness with mild traumatic brain injury affects PTSD symptom presentation in treatment-seeking Iraq/Afghanistan veterans. Brain Inj. 2016;30:1561–1569. https://doi.org/10.1080/02699052.2016.1199897.
Al-Ozairi A, McCullagh S, Feinstein A. Predicting posttraumatic stress symptoms following mild, moderate, and severe traumatic brain injury: The role of posttraumatic amnesia. J Head Trauma Rehabil. 2015;30:283–9. https://doi.org/10.1097/HTR.0000000000000043.
Holland JM, Lisman R, Currier JM. Mild traumatic brain injury, meaning made of trauma, and posttraumatic stress: A preliminary test of a novel hypothesis. Rehabil Psychol. 2013;58:280–6. https://doi.org/10.1037/A0033399.
Vasterling JJ, Verfaellie M, Sullivan KD. Mild traumatic brain injury and posttraumatic stress disorder in returning veterans: Perspectives from cognitive neuroscience. Clin Psychol Rev. 2009;29:674–84. https://doi.org/10.1016/J.CPR.2009.08.004.
Samuelson KW, Abadjian L, Jordan JT, Bartel A, Vasterling J, Seal K. The association between PTSD and functional outcome is mediated by perception of cognitive problems rather than objective neuropsychological test performance. J Trauma Stress. 2017;30:521–30. https://doi.org/10.1002/JTS.22223.
Larbig F, Jelinek L, Kellner M, Biesold K, Barre K, Moritz S. Subjective premorbid memory in posttraumatic stress disorder. Ger J Psych. 2008;11:149–52.
Brenner LA, Terrio H, Homaifar BY, Gutierrez PM, Staves PJ, Harwood JEF, Reeves D, Adler LE, Ivins BJ, Helmick K, Warden D. Neuropsychological test performance in soldiers with blast-related mild TBI. Neuropsychology. 2010;24:160–7. https://doi.org/10.1037/A0017966.
Geisser ME, Roth RS, Bachman JE, Eckert TA. The relationship between symptoms of post-traumatic stress disorder and pain, affective disturbance and disability among patients with accident and non-accident related pain. Pain. 1996;66:207–14. https://doi.org/10.1016/0304-3959(96)03038-2.
Segev S, Shorer M, Rassovsky Y, Peleg TP, Apter A, Fennig S. The contribution of posttraumatic stress disorder and mild traumatic brain injury to persistent post concussive symptoms following motor vehicle accidents. Neuropsychology. 2016;30:800–10. https://doi.org/10.1037/NEU0000299.
Kuhn E, Blanchard EB, Hickling EJ. Posttraumatic stress disorder and psychosocial functioning within two samples of MVA survivors. Behav Res Ther. 2003;41:1105–12. https://doi.org/10.1016/S0005-7967(03)00071-8.
Kaplan GB, Leite-Morris KA, Wang L, Rumbika KK, Heinrichs SC, Zeng X, Wu L, Arena DT, Teng YD. Pathophysiological bases of comorbidity: Traumatic brain injury and post-traumatic stress disorder. J Neurotrauma. 2018;35:210–25. https://doi.org/10.1089/NEU.2016.4953.
Hickling EJ, Gillen R, Blanchard EB, Buckley T, Taylor A. Traumatic brain injury and posttraumatic stress disorder: A preliminary investigation of neuropsychological test results in PTSD secondary to motor vehicle accidents. Brain Inj. 2009;12:265–74. https://doi.org/10.1080/026990598122566.
Brenner LA, Vanderploeg RD, Terrio H. Assessment and diagnosis of mild traumatic brain injury, posttraumatic stress disorder, and other polytrauma conditions: Burden of adversity hypothesis. Rehabil Psychol. 2009;54:239–46. https://doi.org/10.1037/A0016908.
Mikolić A, Polinder S, Retel Helmrich IRA, Haagsma JA, Cnossen MC. Treatment for posttraumatic stress disorder in patients with a history of traumatic brain injury: A systematic review. Clin Psychol Rev. 2019;73:101776. https://doi.org/10.1016/J.CPR.2019.101776.
Block CK, West SE. Psychotherapeutic treatment of survivors of traumatic brain injury: Review of the literature and special considerations. Brain Inj. 2013;27:775–88. https://doi.org/10.3109/02699052.2013.775487.
Gallagher M, McLeod HJ, McMillan TM. A systematic review of recommended modifications of CBT for people with cognitive impairments following brain injury. Neuropsychol Rehabil. 2016;29:1–21. https://doi.org/10.1080/09602011.2016.1258367.
Samuelson KW, Bartel A, Valadez R, Jordan JT. PTSD symptoms and perception of cognitive problems: The roles of posttraumatic cognitions and trauma coping self-efficacy. Psychol Trauma. 2017;9:537–44. https://doi.org/10.1037/TRA0000210.
Vanderploeg RD, Belanger HG, Kaufmann PM. Nocebo effects and mild traumatic brain injury: Legal implications. Psychol Inj Law. 2014;7:245–54. https://doi.org/10.1007/s12207-014-9201-3.
Twamley EW, Jak AJ, Delis DC, Bondi MW, Lohr JB. Cognitive symptom management and rehabilitation therapy (CogSMART) for veterans with traumatic brain injury: Pilot randomized controlled trial. J Rehabil Res Dev. 2014;51:59–70. https://doi.org/10.1682/JRRD.2013.01.0020.
Fralick M, Sy E, Hassan A, Burke MJ, Mostofsky E, Karsies T. Association of concussion with the risk of suicide: A systematic review and meta-analysis. JAMA Neurol. 2019;76:144–51. https://doi.org/10.1001/JAMANEUROL.2018.3487.
McIntire KL, Crawford KM, Perrin PB, Sestak JL, Aman K, Walter LA, Page DB, Wen H, Randolph BO, Brunner RC, Novack TL, Niemeier JP. Factors increasing risk of suicide after traumatic brain injury: A state-of-the-science review of military and civilian studies. Brain Inj. 2021;35:151–63. https://doi.org/10.1080/02699052.2020.1861656.
Barnes SM, Walter KH, Chard KM. Does a history of mild traumatic brain injury increase suicide risk in veterans with PTSD? Rehabil Psychol. 2012;57:18–26. https://doi.org/10.1037/A0027007.
Campbell-Sills L, Jain S, Sun X, Fisher LB, Agtarap SD, DIkmen S, Nelson LD, Temkin N, McCrea M, Yuh E, Giacino JT, Manley GT, Stein MB. Risk factors for suicidal ideation following mild traumatic brain injury: A TRACK-TBI study. J Head Trauma Rehabil. 2021;36:E30–E39. https://doi.org/10.1097/HTR.0000000000000602.
Simpson GK, Tate RL, Whiting DL, Cotter RE. Suicide prevention after traumatic brain injury: A randomized controlled trial of a program for the psychological treatment of hopelessness. J Head Trauma Rehabil. 2011;26:290–300. https://doi.org/10.1097/HTR.0B013E3182225250.
Rapoport MJ, Chan F, Lanctot K, Herrmann N, McCullagh S, Feinstein A. An open-label study of citalopram for major depression following traumatic brain injury. J Psychopharmacol. 2008;22:860–4. https://doi.org/10.1177/0269881107083845.
Rees RJ, Bellon ML. Post concussion syndrome ebb and flow: Longitudinal effects and management. NeuroRehabilitation. 2007;22:229–42. https://doi.org/10.3233/NRE-2007-22309.
Jobes DA. Managing suicidal risk : A collaborative approach. 2nd ed. The Guilford Press; 2016.
Stanley B, Brown GK. Safety planning intervention: A brief intervention to mitigate suicide risk. Cogn Behav Pract. 2012;19:256–64. https://doi.org/10.1016/J.CBPRA.2011.01.001.
Bush NE, Smolenski DJ, Denneson LM, Williams HB, Thomas EK, Dobscha SK. A Virtual Hope Box: Randomized controlled trial of a smartphone app for emotional regulation and coping with distress. Psychiatr Serv. 2017;68:330–6. https://doi.org/10.1176/APPI.PS.201600283.
Sale E, Hendricks M, Weil V, Miller C, Perkins S, McCudden S. Counseling on Access to Lethal Means (CALM): An evaluation of a suicide prevention means restriction training program for mental health providers. Comm Ment Health J. 2018;54:293–301. https://doi.org/10.1007/S10597-017-0190-Z/FIGURES/4.
Ghaffar O, McCullagh S, Ouchterlony D, Feinstein A. Randomized treatment trial in mild traumatic brain injury. J Psychosom Res. 2006;61:153–60. https://doi.org/10.1016/j.jpsychores.2005.07.018.
Paniak C, Toller-Lobe G, Reynolds S, Melnyk A, Nagy J. A randomized trial of two treatments for mild traumatic brain injury: 1 year follow-up. Brain Inj. 2000;14:219–26. https://doi.org/10.1080/026990500120691.
Paniak C, Toller-Lobe G, Durand A, Nagy J. A randomized trial of two treatments for mild traumatic brain injury. Brain Inj. 1998;12:1011–23. https://doi.org/10.1080/026990598121927.
Wampold BE. How important are the common factors in psychotherapy? An update. World Psychiatry. 2015;14:270–7. https://doi.org/10.1002/WPS.20238.
Gómez-De-Regil L, Estrella-Castillo DF, Vega-Cauich J. Psychological intervention in traumatic brain injury patients. Behav Neurol. 2019;2019:6937832. https://doi.org/10.1155/2019/6937832.
Ashworth F. Soothing the injured brain with a compassionate mind: building the case for compassion focused therapy following acquired brain injury*. In Yeates G, Farrell G, editors. Eastern influences on neuropsychotherapy. Routledge. 2018; pp. 77–120. https://doi.org/10.4324/9780429466618-4.
Roche L. An acceptance and commitment therapy-based intervention for PTSD following traumatic brain injury: A case study. Brain Inj. 2019;34:290–7. https://doi.org/10.1080/02699052.2019.1683896.
Rauwenhoff J, Peeters F, Bol Y, Van Heugten C. The BrainACT study: Acceptance and commitment therapy for depressive and anxiety symptoms following acquired brain injury: Study protocol for a randomized controlled trial. Trials. 2019;20:773. https://doi.org/10.1186/S13063-019-3952-9/TABLES/2.
Hoge CW, McGurk D, Thomas JL, Cox AL, Engel CC, Castro CA. Mild traumatic brain injury in U.S. soldiers returning from Iraq. N Engl J Med. 2008;358:53–463. https://doi.org/10.1056/NEJMOA072972/SUPPL_FILE/NEJMOA072972-SA1.PDF.
Storzbach D, O’Neil ME, Roost SM, Kowalski H, Iverson GL, Binder LM, Fann JR, Huckans M. Comparing the neuropsychological test performance of operation enduring freedom/operation Iraqi freedom (OEF/OIF) veterans with and without blast exposure, mild traumatic brain injury, and posttraumatic stress symptoms. J Int Neuropsychol Soc. 2015;21:353–63. https://doi.org/10.1017/S1355617715000326.
Ponsford J, Lee NK, Wong D, Mckay A, Haines K, Downing M, Alway Y, Furtado C, O’donnell ML. Factors associated with response to adapted cognitive behavioral therapy for anxiety and depression following traumatic brain injury. J Head Trauma Rehabil. 2020;35:117–26. https://doi.org/10.1097/HTR.0000000000000510.
Bahraini NH, Simpson GK, Brenner LA, Hoffberg AS, Schneider AL. Suicidal ideation and behaviours after traumatic brain injury: A systematic review. Brain Impair. 2013;14:92–112. https://doi.org/10.1017/BRIMP.2013.11.
Author information
Authors and Affiliations
Contributions
SLA: Conceptualization, design, acquisition of literature, interpretation of literature, drafting and revising the article, and approval of final draft. KRS: Conceptualization, design, acquisition of literature, interpretation of literature, drafting and revising the article, and approval of final draft. SLI: Conceptualization, interpretation of literature, revising the article, and approval of final draft. NCB: Conceptualization, interpretation of literature, revising the article, and approval of final draft. GGM: Conceptualization, interpretation of literature, revision the article, and approval of final draft. SDH: Conceptualization, design, acquisition of literature, interpretation of literature, revising the article, and approval of final draft. BDH: Conceptualization, interpretation of literature, revising the article, and approval of final draft.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflicts of Interest/Competing Interests
Authors SLA, KRS, SLI, NCB, GGM, SDH, and BDH declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Medicine
Rights and permissions
About this article
Cite this article
Aita, S.L., Schuler, K.R., Isaak, S.L. et al. Posttraumatic Stress Disorder Complicated by Traumatic Brain Injury: A Narrative Review. SN Compr. Clin. Med. 5, 92 (2023). https://doi.org/10.1007/s42399-023-01431-1
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-023-01431-1