Abstract
Patients with lower limb amputation (LLA) are prone to greater physical demands. Retrospective studies reported 5 to 61% of ipsilateral or contralateral hip osteoarthritis after LLA. Total hip arthroplasty (THA) has proven effective in improving the quality of life of patients with hip osteoarthritis. Its incidence after ipsilateral LLA is reported to be 0.067%. There is little information on the technical aspects and results of this procedure in such patients. The objective of this study is to report a patient with bilateral LLA and ipsilateral hip arthritis treated with THA, highlighting the challenges of the surgical technique and the postoperative protocol. After Internal Review Board approval (IRB00010193), we present a 64-year-old male patient with bilateral infrapatellar amputation who underwent left THA where the surgical challenge lies in being able to perform an adequate osteotomy of the femoral neck, obtaining an adequate exposure of the femoral canal, and achieving a correct implant placement. Wide release of the psoas and gluteus maximus tendons was necessary to ease femoral preparation and intraoperative maneuverability of the lower extremity. Although THA is a common procedure, when performed in an unusual patient and in the absence of therapeutic guidelines or consensus when dealing with this association, an appropriate preoperative plan should be followed. This case provides a perioperative approach focused on the search for possible intraoperative scenarios that may occur in patients who will undergo a THA after LLA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients with lower limb amputation (LLA) are prone to increased physical demands. The level at which the LLA is executed is directly proportional to physiological oxygen consumption required to perform activities of daily living. [1, 2] Below-knee amputation (BKA) overloads the contralateral knee to such an extent that it may lead to articular degeneration [3], while it “unloads” the ipsilateral one; however, it is not clear whether BKA provides such joint “protection” for the ipsilateral or contralateral hip. [4, 5] Retrospective studies have reported a high prevalence of both ipsilateral and contralateral hip osteoarthritis after LLA, ranging from 5 to 61% without any superiority of either. [4, 6].
Increased ipsilateral hip degeneration could arise by over-compensation of the hip joint flexors, extensors, and external rotators due to the lack of ankle function while walking. [5] Total hip arthroplasty (THA) is a safe procedure and has been shown to be effective in improving quality of life of patients with hip osteoarthritis, and its incidence after ipsilateral LLA is 0.067% [7]. However, there is little information on the technical aspects and results of this procedure in such patients.
We report a case of a patient with LLA and ipsilateral hip arthritis treated with THA, highlighting the challenges of the surgical technique and the postoperative protocol. Secondarily, we aimed to review the literature on the outcomes of THA in LLA patients.
Case Report
A 64-year-old male patient, with a history of hypertension and body mass index of 30 kg/m2, underwent bilateral BKA at the age of 9, due to bilateral agenesis of the fibula. He required multiple additional soft tissue procedures for injuries secondary to the use of its transtibial lace exo-prosthesis and patellar tendon support. At the age of 39, he suffered a road accident where he presented a displaced left femoral neck fracture, treated by open reduction and internal fixation with 3 cannulated screws.
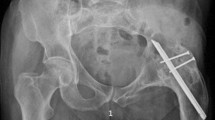
The patient was referred to our center in January 2020 with pain in the left hip of 3 years, associated with decreased range of motion of the hip and inability to perform activities of daily living. X-rays showed severe left hip osteoarthritis and the presence of osteosynthesis. A panoramic radiograph of both lower limbs showed bilateral infrapatellar amputation (Fig. 1). An uncemented THA was indicated (Fig. 2A), choosing metal-on-highly crosslinked polyethylene as bearing surface.
A Clinical photograph of the patient, standing on his exo-prosthesis with patellar tendon support. B Panoramic preoperative antero-posterior radiograph of the lower limbs that shows bilateral infrapatellar amputation and agenesis of both fibulas, severe left hip osteoarthritis, and the presence of osteosynthesis material
A Preoperative planning using an uncemented total hip arthroplasty template. B Clinical photograph of the surgical position and patient fixation to the stretcher. Right decubitus lateralis with one fixation post in the back and two in the front, holding the anterior–superior iliac crests to avoid a rolling movement during manipulation of the stump
The patient was operated under spinal anesthesia using a posterolateral approach. He was placed on the surgical table in right lateral decubitus, secured with a sacral post and two anterior posts at the level of the anterior–superior iliac spine to prevent rolling during lower limb stump manipulation (Fig. 2B). A protective silicone patch was placed over the grafted skin area of the stump.
After removing the osteosynthesis, the external rotators and capsule were simultaneously cut in an L-shaped fashion. After several failed attempts to dislocate the joint, an in situ femoral neck osteotomy was performed (Fig. 3A). Appropriate exposure of the acetabulum was made using a modified Hohmann retractor to move the femur anteriorly, and with two Charnley pins that were placed at the acetabular roof and at the ischium. Acetabular reaming was performed progressively, using a line-to-line technique. An uncemented Trident Stryker® (Stryker, Kalamazoo, MI, USA) cup of 60 mm diameter was implanted and augmented with a 30-mm screw. A highly crosslinked polyethylene liner with 36 mm internal diameter was used.
A Intraoperative photograph showing the in situ osteotomy of the femoral neck, protecting the sciatic nerve with a Hohmann retractor. B Intraoperative photograph during femoral preparation, shows the rasp positioning, with the optimal anteversion due to proper manipulation of the stump with one hand on the thigh and fulcrum in the body of the assistant obtaining a perpendicular position of the tibia with respect to the floor. C Intraoperative photograph during stem reduction, shows a Hohmann retractor placed on the anterior wall of the acetabulum applying a sliding force on the femur
The most complex technical difficulty in this surgery was femoral canal preparation, in which good exposure by releasing the gluteus maximus tendon insertion was required to obtain proper internal rotation, thus avoiding excessive torque force and preventing intraoperative fractures. Adequate femoral exposure was achieved without use of traction devices, but needing complete release of psoas and gluteus maximus tendons (Fig. 3B). Femoral canal preparation was made with progressive rasps up to size 5 (until intraoperative medial–lateral contact was noticed) with a neck of 132°, achieving good rotational stability. The reduction and stability test (8) were performed with a 36-mm head without the need to use any device to help maneuver the stump, other than a Hohmann retractor placed in the anterior wall of the acetabulum (Fig. 3C). The definitive uncemented Accolade II Stryker® (Stryker, Kalamazoo, MI, USA) No. 5 was implanted, with a 36-mm metal head. After wound closure, a postoperative antero-posterior pelvic x-ray was performed in the operating room (Fig. 4A).
The surgical procedure had a total duration of 41 min with 100 ml of blood loss, recorded from the aspiration receptacle. On the same day of surgery, the patient was encouraged to walk with the help of his previous exo-prosthesis attached to the stump, using a regular walker weight-bearing as tolerated. The day after surgery he was discharged home. The patient was provided with anti-dislocation guidelines such as avoiding adduction, internal rotation, and hip flexion above 90°, sleeping with a cushion between the knees, and sitting on chairs of at least 55 cm height and with support for both arms. Within 2 weeks of rehabilitation, he was encouraged to leave the walker and progressed to canes. After 3 months of follow-up, the patient was able to walk without any assistive device. He was able to return to his city of origin performing activities of daily living without restrictions at 2 years of follow-up (Fig. 4B).
Discussion
The reconstitution of hip biomechanics is a primary asset to determine the future success of a THA. This is even more challenging in patients with high functional demands and long-life expectancy [9], making implant selection an important part of treatment success [10]. In this sense, surgical exposure, maneuverability of the stump, and implant positioning are potential problems that a surgeon should anticipate in order to successfully perform a prosthetic replacement in the amputee patient.
The first surgical challenge of THA after a LLA is to perform an adequate osteotomy of the femoral neck. Second, obtaining adequate exposure is crucial for femoral preparation and to achieve a correct placement of the final implant. Third, adequate maneuverability of the limb stump is necessary at several surgical moments, including femoral head dislocation, femoral canal preparation, and reduction of both the trial and the final stem. However, it is not always possible to maneuver the stump using the knee and remnant tibia as a fulcrum, and this may result in insufficient traction.
Although some reports encourage the use of a Steinman pin anchored to the distal femur to obtain traction and ease in rotation [11, 12], the osteopenia present in the femoral condyles due to disuse may generate an area of weakness and predispose to femoral mid-shaft or distal fracture. In the eventuality of severe soft tissue contractures or heterotopic ossifications, a greater trochanteric osteotomy can be performed. In this case, the instruments for the trochanteric fixation should also be ready in the operating table. [13] In our case, an in situ femoral neck was enough to enable femoral canal preparation (Fig. 3A).
On the other hand, manipulation of the femur during femoral time is no less important since inadequate exposure of the canal could preclude periprosthetic fracture or femoral component malalignment. Prickett and Scanlon reported the latter complication in a patient with a BKA, in which case the placement of the patient’s exo-prosthesis had to be adjusted in internal rotation to amend the femoral component’s malpositioning.[14] In any case, this situation should be avoided, as it would increase the risk of dislocation and alter the kinematics of the gait. [15] One option to avoid such complication would be to place the anteriorly described Steinman or a periarticular clamp in the distal femur to obtain a lever arm for better rotational control. [16].
Additionally, any effort to dislocate the femoral head or rotate the stump during surgery is in vain if the patient is not “fixed” to the stretcher with appropriate supports. When a posterolateral approach is performed, the classic fixation is one post in the back and one in the front at the level of the pubis. This type of fixation has proven to be less effective controlling pelvic pitch and roll. In a prospective study, Gonzalez Della Valle et al. showed that the maximum pelvic roll and pitch detected during surgery averaged 17.62° (SD: 5.08) and 9.3° (SD: 3.39) respectively, using one anterior post and other posterior [17]. Pekmezci et al. presented a case of a patient with a through-knee amputation who underwent a THA, and suggested the use of a peg-board to improve patient positioning [10]. We prefer to use a 3-point fixation system, with one post in the back at the level of the sacrum and 2 in the front at the level of the anterior–superior iliac crests as shown in Fig. 2B.
Rapid rehabilitation plays a key role in LLA patients to avoid contractures and improve functional outcomes. A protocol focused on strengthening hip flexors and knee extensors is needed to avoid hip flexion contracture as much as possible. During the surgical procedure, tenotomies of the corresponding muscular groups should be added. [18].
There are few reports and case series focusing on clinical improvement in amputated patients with a THA (Table 1). The largest one was published in 2015 by Amanatullah et al. [7], where the authors presented 13 cases with a BKA due to peripheral vascular disease and/or diabetes mellitus, and treated with primary THA through an anterolateral approach in the vast majority. Four reports also suggested tips and tricks during the THA surgical technique when performed in a LLA patient [7, 10, 12, 15], but only one highlighted these tips when the amputation was below the knee [7].
We conclude that the approach of the patient with THA after LLA must be carried out with a meticulous preoperative plan. As it is a common procedure in an unusual patient, in the absence of therapeutic guidelines or consensus, this case provides a perioperative approach focused on the search for possible intraoperative scenarios that may occur in patients who will undergo a THA surgery after LLA.
Data Availability
Not applicable.
Code Availability
Not applicable.
References
Jeans KA, Browne RH, Karol LA. Effect of amputation level on energy expenditure during overground walking by children with an amputation. J Bone Joint Surg Am. 2011;93(1):49–56.
Herbert LM, Engsberg JR, Tedford KG, Grimston SK. A comparison of oxygen consumption during walking between children with and without below-knee amputations. Phys Ther. 1994;74(10):943–50.
Norvell DC, Czerniecki JM, Reiber GE, Maynard C, Pecoraro JA, Weiss NS. The prevalence of knee pain and symptomatic knee osteoarthritis among veteran traumatic amputees and. Arch Phys Med Rehabil. 2005;86(3):487–93.
Kulkarni J, Adams J, Thomas E, Silman A. Association between amputation, arthritis and osteopenia in British male war veterans with major lower limb amputations. Clin Rehabil. 1998;12(4):348–53.
Sadeghi H, Allard P, Duhaime PM. Muscle power compensatory mechanisms in belowknee amputee gait. Am J Phys Med Rehabil. 2001;80(1):25–32.
Burke MJ, Roman V, Wright V. Bone and joint changes in lower limb amputees. Ann Rheum Dis. 1978;37(3):252–4.
Amanatullah DF, Trousdale RT, Sierra RJ. Total hip arthroplasty after lower extremity amputation. Orthopedics. 2015;38(5):e394-400. https://doi.org/10.3928/01477447-20150504-56.
Lucas DH, Scott RD. The Ranawat sign a specific maneuver to assess component positioning in total hip arthroplasty. J Orthop Techniques. 1994;2:59–61.
Gallart X, Riba J, Fernández-Valencia JA, Bori G, Muñoz-Mahamud E, Combalia A. Hip prostheses in young adults. Surface prostheses and short-stem prostheses. Rev Esp Cir Ortop Traumatol. 2018 Mar-Apr;62(2):142–152.
Pivec R, Johnson AJ, Mears SC, Mont MA. Hip arthroplasty. Lancet. 2012;380(9855):1768–77.
Pekmezci M, Nunley RM, Barrack RL. Technique for total hip arthroplasty in a patient with through-knee amputation. J Arthroplasty. 2010;25(4):659.
Leonard M, Nicholson P. Total hip arthroplasty in a patient with arthrogryphosis and an ipsilateral above knee amputation. Hip Int. 2010;20(4):559–61.
Sathappan SS, Wee J, Ginat D, Teicher M, Meere P, Di Cesare PE. Total hip arthroplasty in patients with aboveknee amputation: a case report. Am J Orthop. 2011;40:E17–9.
Prickett NM, Scanlon CJ. Total joint replacement in extremities with below-knee amputations. Phys Ther. 1976;56:925–7.
Yang L, Solomonidis SE, Spense WD, Paul JP. The influence of limb alignment on the gait of above-knee amputees. J Biomech. 1991;24:981–97.
Malagelada F, Coll Rivas M, Jiménez Obach A, Auleda J, Guirao L, Pleguezuelos E. Total hip replacement in an ipsilateral above-the-knee amputation: surgical technique, rehabilitation, and review of the literature. Int J Low Extrem Wounds. 2013;12(1):39–43. https://doi.org/10.1177/1534734613479380.
Gonzalez Della Valle A, Shanaghan K, Benson JR, Carroll K, Cross M, McLawhorn A, Sculco PK. Pelvic pitch and roll during total hip arthroplasty performed through a posterolateral approach. A potential source of error in free-hand cup positioning. Int Orthop. 2019 Aug;43(8):1823–1829. https://doi.org/10.1007/s00264-018-4141-2. Epub 2018 Sep 21. PMID: 30242516.
Salai M, Amit Y, Chechik A, Blankstein A, Dudkiewicz I. Total hip arthroplasty in patients with below-knee amputations. J Arthroplasty. 2000;15:999–1002.
Nejat EJ, Meyer A, Sánchez PM, Schaefer SH, Westrich GH. Total hip arthroplasty and rehabilitation in ambulatory lower extremity amputees–a case series. Iowa Orthop J. 2005;25:38–41.
Mak J, Solomon M, Faux S. Ipsilateral total hip arthroplasty in a dysvascular below-knee amputee for advanced hip osteoarthritis: a case report and review of the literature. Prosthet Orthot Int. 2008;32(2):155–9. https://doi.org/10.1080/03093640802015953 PMID: 18569883.
Author information
Authors and Affiliations
Contributions
Agustin Garcia-Mansilla: idea, redaction. Martín Buljubasich: redaction, review. Carlos Lucero: redaction. Gerardo Zanotti: review. Fernando Martín Comba: review. Francisco Piccaluga: idea, review. Pablo Ariel Slullitel: review, translation. Martín Alejandro Buttaro: idea, review, translation.
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Internal Review Board #IRB00010193.
Consent to Participate
Written consent was obtained from the patient included in the study.
Written Consent for Publication
The patient has given written permission for publication.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This Article Is Part of the Topical Collection On Surgery
Rights and permissions
About this article
Cite this article
Garcia-Mansilla, A., Buljubasich, M., Lucero, C. et al. Total Hip Replacement in a Patient with Bilateral Infrapatellar Amputation: Case Report, Literature Review, Tips and Tricks. SN Compr. Clin. Med. 4, 30 (2022). https://doi.org/10.1007/s42399-021-01095-9
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-021-01095-9