Abstract
Background
Giant ovarian cysts are rarely described in the literature, owing to the availability of advanced imaging technologies in developed countries leading to early treatment. In resource limited areas patients may present late due to financial and social constraints.
Purpose
Through this case, we aim to discuss the importance of early diagnosis and appropriate management of giant benign tumours and highlight the management related issues.
Methods
We are reporting a rare case of a very large giant ovarian cystadenoma who presented to a tertiary care hospital with large abdominal mass of benign nature with poor functional status.
Results
She underwent laparotomy proceed debulking of an enormous cyst with 36 litres of mucinous fluid whose postoperative biopsy was reported as a borderline ovarian tumour. Her intraoperative management and fluid management was a challenge for the anaesthetist. She developed pulmonary embolism in her postoperative period requiring intensive care.
Conclusion
Through this case report, we would like to highlight the importance of a multidisciplinary team in managing such complex cases with perioperative morbidity. Early diagnosis and appropriate measure in time to handle complications are beneficial to these patients with good survival.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Tumours of the ovary presenting with diameters greater than 10 cm are referred to as giant ovarian cysts [1]. These tumours are rarely reported from high-income countries where there is good access to health care and advanced imaging technologies leading to early diagnosis of small or medium-sized tumours [2]. Giant cystadenomas are rare tumours that often are slow-growing and benign. Due to the nature of these tumours, in rare cases, they reach large dimensions leading to extreme discomfort and management challenges [3].
These tumours may be asymptomatic in early stages developing symptoms only after reaching huge dimensions, and consequently are diagnosed late [1]. Symptoms related to compression, or a visible abdominal mass are the most frequent presenting complaints [2].
The surgical management of these masses is associated with many life-threatening complications, which arise predominantly owing to sudden changes in blood volume distribution and body circulation predisposing them to pulmonary oedema. The complications include severe hypotension, increased venous return, cardiac failure, respiratory failure, and intestinal distention [2]. We report a case of a giant mucinous cystadenoma that presented to our tertiary care centre and had a rare yet life-threatening complication.
Case Report
A 48 years multiparous old lady, presented with slow onset, progressive abdominal distension over the last two years. It was associated with pain and breathlessness over the last two weeks. She did not have any bowel-related symptoms. She had regular menstrual cycles and had a history of 4 normal deliveries followed by tubal ligation she was a known diabetic on medications. On consulting with her local physician, she was advised surgery which she could not undergo due to social and financial issues. Her occupation involved long hours of sitting on the ground, which she could carry on in this position until the admission. Activities of daily life were impaired and she needed assistance.
Upon admission, her performance status was found to be ECOG 2. She was unable to lie down due to extreme lordosis caused by the enormous abdominal mass. Her resting pulse rate was 118 beats per minute, her blood pressure was 120/70 mmHg, and her BMI was 50 kg/m2 (weight-110 kg, Height 148 cm). She had bilateral pitting pedal oedema up to the knee with no calf tenderness or warmth. Breast examination revealed no abnormalities. She had equal air entry in her chest and normal cardiorespiratory and other systems. Chronic sitting position had caused hypertrophy of the buttock muscles.
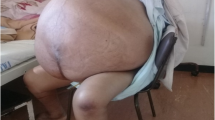
Examination of her abdomen revealed gross distention, with paeu d’orange edema of the abdominal. The abdomen was tense with fullness in the flanks, non-tender and uniformly distended(Figs. 1, 2) Vaginal examination revealed a large cystic mass filling the pouch of Douglas and pelvis going on to the abdomen. The uterus was not felt separately. Her blood tests showed low albumin levels at 2.2 g/dL with a total protein of 4.9 g/dL. Her blood revealed normal haematocrit with mildly elevated tumour markers the results of which are provided in Table 1. Further evaluation through an abdominal and pelvic CECT revealed the presence of a large, thin-walled, multiloculated cystic lesion extending from the pelvis to the epigastric region. The wall thickness of the lesion was measured at 2.6 mm with a septal thickness of 3 mm. This lesion caused displacement of the liver and diaphragm superiorly and bowel loops laterally and posteriorly (Fig. 3). The mass was compressing the aorta as well as the uterus and bladder resulting in mild bilateral hydronephrosis. Gross anterior abdominal wall oedema was noted. Her cardiac evaluation revealed a normal ECG and an ECHO which revealed mild tricuspid regurgitation and pulmonary hypertension. Deep vein thrombosis screening with colour Doppler was planned but not undertaken due to logistics of shifting the patient as she was unable to lie down flat or cooperate with the Doppler screening of her lower limbs.
She was posted for exploratory laparotomy and preoperatively counselling was done regarding the possible complications. At laparotomy, there was a huge abdominopelvic predominantly cystic mass filling the entire abdomen and pelvis reaching up to the xiphisternum with ascites of about 300 ml. The giant tumour containing 36 L of mucinous fluid with multiple septae and locules was removed and sent for frozen section which was reported as Benign Mucinous cystadenoma. The right tube and ovary were normal and the uterus was 14 weeks in size. The rest of the abdomen and appendix were normal on inspection at surgery. She underwent total abdominal hysterectomy with bilateral salpingo-oophorectomy with infra colic omentectomy under general anaesthesia. The estimated blood loss was 1500 ml, whereas the allowable blood loss for her was calculated as 975 ml she received a unit of albumin, two 5% dextrose solutions, two 0.9% saline and 2 units of packed cell transfusion intraoperatively. The patient was stable and transferred to the ward postoperatively. The patient was started on tri-ball therapy and compressive stockings along with intermittent compression by cuffed apparatus as part of routine post-op care on post-op day 2 she developed acute onset of chest pain and cough with a drop in saturation and laboured breathing. On examination, there was tachycardia and tachypnoea, whereas the blood gases done at that time were reported as normal with normal lactates and PF ratio with adequate oxygenation.
A pulmonologist’s opinion was sought and a further evaluation with a CECT Pulmonary Angiogram was done as per their advice which revealed both right and left pulmonary arteries and their branches showing hypodense filling defects suggestive of pulmonary embolism with subsegmental atelectasis in posterobasal segments of bilateral lower lobes (Fig. 4). She was transferred to surgical intensive care for expert care where she was transfused one unit of packed cell of blood for a drop in haemoglobin to 6. Her final histopathology report was confirmed as Borderline mucinous cystadenoma (Fig. 2a, b). The mass was biopsied at multiple sites. There was no evidence of stromal invasion in the multiple sections examined. There is no lymphovascular invasion, necrosis or any malignant mural nodules. Other peritoneal biopsies were not performed follow-up in the pulmonary outpatient clinic was advised after discharge. She was started on warfarin which was progressively increased to 6 mg once daily which was later switched to apixaban 5 mg once daily. She was asked to review in gynaecologic outpatient once every three months for the first year. She is presently on regular follow-up and doing well.
Discussion
Giant Mucinous tumours may be asymptomatic at early stages and develop symptoms only after reaching huge dimensions due to which they are usually diagnosed late [1]. Compressive symptoms or a visible abdominal mass are the most frequent presenting complaints [2]. Giant ovarian lesions are often associated with compressive symptoms and need debulking which includes high chances of post-operative morbidity [4, 5]. Optimal imaging, rapid growth (rarely) and abnormal mucin production can determine the giant evolution [2, 6]. As discussed by Hackethal A et al., even very huge intra-abdominal tumours that almost double a patient’s body weight could still be of benign origin [7]. The masses could even have normal or mildly elevated tumour markers with a loe risk of malignancy risk [8, 9]
The perioperative management of patients with giant ovarian tumours is associated with several risks and challenges. These may be dealt by a multidisciplinary approach, appropriate drainage methods, adequate anaesthesia and postoperative analgesia.
A multidisciplinary approach to preoperative planning is critical to achieve optimal intraoperative and postoperative outcomes in the management of patients with giant abdominal masses.
The potential risks of drainage of these masses intraop include a spill of the tumour and possible spread of ovarian cancer, as well as an elevated risk of abdominal infection, bleeding, and adhesions. Though evidence-based guidelines do not favour tumour puncturing and drainage, controlled drainage at 0.5–1 L/min seems to be safe where such large tumours are concerned, to improve surgical outcomes [10, 11]. In our case, as the imaging did not reveal any solid areas or suspicious foci we drained the ovarian cyst safely during surgery, with multiple punctures into locules.
Anaesthesia management in these cases is of vital importance. In particular, the respiratory and cardiovascular management of these patients is critical [12, 13]. The problems involving the circulatory system during the resection of giant ovarian tumours can be divided into the following aspects: supine hypotensive syndrome before the tumour is removed, induced by compression of the tumour; a rapid decrease in thoracic pressure and abdominal pressure after the removal of giant ovarian tumours causing hemodynamic collapse; intraoperatively bleeding can occur; and changes in intrathoracic pressure due to postural and intraoperative positive pressure ventilation which can also affect haemodynamic factors [12, 14]. A wedge at the right side of the trunk was used during the surgery of our patient till mass excision. The patient’s haemodynamic status was appropriately managed with fluids and blood.
Postoperative intestinal distension is probably due to a combination of sympathetic activity and diffusion of gases into the bowel lumen following decompression. Intestinal ileus has been reported in several cases [9]. The risk for intestinal distention may be reduced by the use of an abdominal binder and a nasogastric tube. Fortunately, our patient did not develop paralytic ileus.
Pulmonary embolism (PE) is a rare but serious and many a time fatal complication that could occur after surgery due to the sudden re-expansion of a chronically collapsed lung along with a long-standing compression on the deep veins in the pelvis. Unfortunately, this serious complication though rare did occur in our patient where she developed tachypnoea on the second postoperative day and was diagnosed to have pulmonary embolism on an angiogram. She was treated in surgical intensive care for a short period, stabilized and continued anticoagulants for an extended period.
Conclusion
Mucinous cystadenomas can grow to massive sizes, and provide a huge surgical challenge. A multidisciplinary approach is essential to know the operability and in anticipating postoperative complications. There are potential problems associated with the removal of giant ovarian tumours including operative and postoperative complications of cardiovascular dysfunction or ventilator inadequacy. Furthermore, understanding the possibility of complications and being prepared to handle them can lead to better outcomes in such rare cases.
Data Availability
Not applicable.
References
Yeika EV, Efie DT, Tolefac PN, Fomengia JN. Giant ovarian cyst masquerading as a massive ascites: a case report. BMC Res Notes. 2017;10(1):749.
Pilone V, Tramontano S, Picarelli P, Monda A, Romano M, Renzulli M, Cutolo C. Giant mucinous ovarian borderline tumor. A good lesson from an asymptomatic case. Int J Surg Case Rep. 2018;50:25–7. https://doi.org/10.1016/j.ijscr.2018.07.016.
Levine DA, Dizon DS, Yashar CM, et al. Handbook for principles and practice of gynecologic oncology. 2nd ed. Philadelphia: Lippincott Williams & Wilkins; 2015.
Brown J, Frumovitz M. Mucinous tumors of the ovary: current thoughts on diagnosis and management. Curr Oncol Rep. 2014;16(6):389.
Frumovitz M, Schmeler KM, Malpica A, Sood AK, Gershenson DM. Unmasking the complexities of mucinous ovarian carcinoma. Gynecol Oncol. 2010;117(3):491–6.
Zurawski VR Jr, Orjaseter H, Andersen A, Jellum E. Elevated serum CA 125 levels prior to diagnosis of ovarian neoplasia: relevance for early detection of ovarian cancer. Int J Cancer. 1988;42(5):677–80.
Hackethal A, Brueggmann D, Turovets M, Bassaly B, Stein A, Gerber EL, et al. Removal of enormous bilateral mucinous cystadenomas of the ovaries with abdominal plastic reconstruction. Arch Gynecol Obstet. 2009;279(1):65–7.
Deligeoroglou E, Eleftheriades M, Shiadoes V, Botsis D, Hasiakos D, Kontoravdis A, et al. Ovarian masses during adolescence: clinical, ultrasonographic and pathologic findings, serum tumor markers and endocrinological profile. Gynecol Endocrinol. 2004;19(1):1–8.
Nolen B, Velikokhatnaya L, Marrangoni A, De Geest K, Lomakin A, Bast RC, Lokshin A. Serum biomarker panels for the discrimination of benign from malignant cases in patients with an adnexal mass. Gynecol Oncol. 2010;117(3):440–5. https://doi.org/10.1016/j.ygyno.2010.02.005.
Tingulstad S, Hagen B, Skjeldestad FE, Onsrud M, Kiserud T, Halvorsen T, et al. Evaluation of a risk of malignancy index based on serum CA125, ultrasound findings and menopausal status in the pre-operative diagnosis of pelvic masses. Br J Obstet Gynaecol. 1996;103(8):826–31.
Güraslan H, Yaşar L, Ekin M, Kaya C, Cengiz H, Gonenc M. A successful management of a giant mucinous ovarian tumor with intraoperative controlled fluid aspiration. Eur J Gynaecol Oncol. 2015;36(5):615–7.
Leibman AJ, Kruse B, McSweeney MB. Transvaginal sonography: comparison with transabdominal sonography in the diagnosis of pelvic masses. AJR Am J Roentgenol. 1988;151(1):89–92.
Bennet P, Williamson C, editors. Basic science in obstetrics and gynaecology. 4th ed. Edinburgh: Churchill Livingstone; 2010.
University of Wisconsin Comprehensive Cancer Center Gynecologic Oncology Program. Preparing for surgery for an ovarian mass. https://www.uwhealth.org/healthfacts/gyn-onc/5666.pdf. Accessed 21 Dec 2018
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Consent for Publication
Written informed consent was obtained from the patient’s next of kin to publish this case report and any accompanying images.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sindhu, N.R., John, A.E., Punneshetty, S. et al. Giant Borderline Mucinous Cystadenoma: Hazards of Surgical Debulking. Indian J Gynecol Oncolog 22, 104 (2024). https://doi.org/10.1007/s40944-024-00868-z
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40944-024-00868-z