Abstract
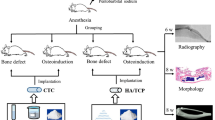
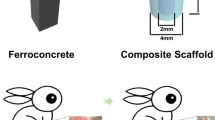
Although calcium sulfate bone cements possess favorable characteristics of excellent clinical handling and osteoconductivity, the rapid degradation and poor bioactivity limit their wide applications. This study reports a type of novel injectable and self-setting composite materials for bone defect repair. Magnesium substituted tricalcium phosphate nanoparticles (43.8±9.0 nm) and calcium sulfate hemihydrate micro-size particles (5–21 µm) were mixed with a polyvinyl alcohol solution with optimal compositions to obtain the composite materials, which showed reasonable initial setting time (11.7–19.2 min) and suitable compressed strength (2.28–6.33 MPa). By utilizing magnesium powder as a porogen, macro-pores (>100 µm) together with micro-pores were created in the final product after setting. In addition, MC3T3E1 cells extended well and exhibited numerous lamellipodia and long filopodia when cultured with the composite materials, indicating that they had no cytotoxicity. The in vivo results indicated that the injectable composite materials could achieve bone defect repair, when implanted in beagle femoral condyle defects for 10 months. Our results show that the new injectable composite materials are biocompatible and biodegradable, which possess great potential for bone defect repair.
摘要
硫酸钙骨水泥具有良好的骨传导性, 但降解速率快、 生物活性差的缺点限制了其临床应用. 本文将β-磷酸三钙纳米颗粒(粒径 43.8±9.0 nm)和半水硫酸钙颗粒(粒径5–21 μm)混合作为固相, 与液相聚乙烯醇溶液(5 wt.%)按优化重量比混匀, 制备了可注射自固化复合材料. 该材料具有合理的自固化时间(11.7–19.2 min)及适宜 的压缩强度(2.28–6.33 MPa). 同时, 利用镁颗粒作为成孔剂, 制备出大孔径(大于100 μm)的多孔支架. 体外细胞实验显示, MC3T3-E1细胞伸展良好, 表现出大量的板状伪足和伸展的丝状伪足, 表明该复合材料无细胞毒性. 将可注射复合材料植入比格犬股骨髁缺损区, 10个月后骨缺损愈合良好, 表明该材料具有良好的骨缺损修复潜力.
Article PDF
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
References
Bohner M. Resorbable biomaterials as bone graft substitutes. Mater Today, 2010, 13: 24–30
LeGeros RZ. Calcium phosphate-based osteoinductive materials. Chem Rev, 2008, 108: 4742–4753
Larsson S, Bauer TW. Use of injectable calcium phosphate cement for fracture fixation: A review. Clin Orthop Relat Res, 2002, 395: 23–32
Liu Y, Zheng Y, Hayes B. Degradable, absorbable or resorbable—what is the best grammatical modifier for an implant that is eventually absorbed by the body? Sci China Mater, 2017, 60: 377–391
Low KL, Tan SH, Zein SHS, et al. Calcium phosphate-based composites as injectable bone substitute materials: A review. J Biomed Mater Res, 2010, 94: 273
Hao F, Qin L, Liu J, et al. Assessment of calcium sulfate hemihydrate-tricalcium silicate composite for bone healing in a rabbit femoral condyle model. Mater Sci Eng-C, 2018, 88: 53–60
Moore WR, Graves SE, Bain GI. Synthetic bone graft substitutes. ANZ J Surg, 2001, 71: 354–361
Chow LC. Solubility of calcium phosphates. Monogl Oral Sci Basel Karger, 2001, 18: 94–111
Goto T, Kojima T, Iijima T, et al. Resorption of synthetic porous hydroxyapatite and replacement by newly formed bone. J Orthop Sci, 2001, 6: 444–447
Hibi A, Ishikawa T, Asano M, et al. A study of failed implantation of hydroxyapatite for benign bone tumor. Orthoped Surg, 1994, 45: 1423–1428
Bell WH. Resorption characteristics of bone and bone substitutes. Oral Surg Oral Med Oral Pathol, 1964, 17: 650–657
Wang ML, Massie J, Perry A, et al. A rat osteoporotic spine model for the evaluation of bioresorbable bone cements. Spine J, 2007, 7: 466–474
Masterman D. Ksp determination of calcium sulfate. J Chem Educ, 1987, 64: 408–409
Ferguson J, Athanasou N, Diefenbeck M, et al. Radiographic and histological analysis of a synthetic bone graft substitute eluting gentamicin in the treatment of chronic osteomyelitis. J Bone Jt Infect, 2019, 4: 76–84
Zhang T, Zhou W, Jia Z, et al. Polydopamine-assisted functionalization of heparin and vancomycin onto microarc-oxidized 3D printed porous Ti6Al4V for improved hemocompatibility, osteogenic and anti-infection potencies. Sci China Mater, 2018, 61: 579–592
Gu X, Wang F, Xie X, et al. In vitro and in vivo studies on asextruded Mg-5.25wt.%Zn-0.6wt.%Ca alloy as biodegradable metal. Sci China Mater, 2018, 61: 619–628
Park JW, Kim YJ, Jang JH, et al. Osteoblast response to magnesium ion-incorporated nanoporous titanium oxide surfaces. Clin Oral ImPlants Res, 2010, 21: 1278–1287
Hung CC, Chaya A, Liu K, et al. The role of magnesium ions in bone regeneration involves the canonical Wnt signaling pathway. Acta Biomater, 2019, 98: 246–255
Zhang X, Zu H, Zhao D, et al. Ion channel functional protein kinase TRPM7 regulates Mg ions to promote the osteoinduction of human osteoblast via PI3K pathway: In vitro simulation of the bone-repairing effect of Mg-based alloy implant. Acta Biomater, 2017, 63: 369–382
Díaz-Tocados JM, Herencia C, Martínez-Moreno JM, et al. Magnesium chloride promotes osteogenesis through Notch signaling activation and expansion of mesenchymal stem cells. Sci Rep, 2017, 7: 7839
Tripp RA, Alvarez R, Anderson B, et al. Bioconjugated nanoparticle detection of respiratory syncytial virus infection. Int J NanoMed, 2007, 2: 117–124
Wang P, Zhao L, Liu J, et al. Bone tissue engineering via nano-structured calcium phosphate biomaterials and stem cells. Bone Res, 2014, 2: 14017
Zhou C, Xie P, Chen Y, et al. Synthesis, sintering and characterization of porous nano-structured CaP bioceramics prepared by a two-step sintering method. Ceramics Int, 2015, 41: 4696–4705
Fischer J, Prosenc MH, Wolff M, et al. Interference of magnesium corrosion with tetrazolium-based cytotoxicity assays. Acta Biomater, 2010, 6: 1813–1823
Matsunaga K, Kubota T, Toyoura K, et al. First-principles calculations of divalent substitution of Ca2+ in tricalcium phosphates. Acta Biomater, 2015, 23: 329–337
Polat S, Sayan P. Effects of tricarballylic acid on phase transformation of calcium sulfate hemihydrate to the dihydrate form. Cryst Res Technol, 2017, 52: 1600395
Liu X, Wang XM, Chen Z, et al. Injectable bone cement based on mineralized collagen. J Biomed Mater Res, 2010, 94B: 72–79
Laurencin CT, Ambrosio AMA, Borden MD, et al. Tissue engineering: orthopedic applications. Annu Rev Biomed Eng, 1999, 1: 19–46
Yu B, Han K, Ma H, et al. Treatment of tibial plateau fractures with high strength injectable calcium sulphate. Int Orthop (SICOT), 2009, 33: 1127–1133
Saleh AT, Ling LS, Hussain R. Injectable magnesium-doped brushite cement for controlled drug release application. J Mater Sci, 2016, 51: 7427–7439
Lewis G. Injectable bone cements for use in vertebroplasty and kyphoplasty: state-of-the-art review. J Biomed Mater Res, 2006, 76B: 456–468
Baino F, Fiume E. Mechanical characterization of 45S5 bioactive glass-derived scaffolds. Mater Lett, 2019, 245: 14–17
Li X, Niu Y, Guo H, et al. Preparation and osteogenic properties of magnesium calcium phosphate biocement scaffolds for bone regeneration. J Inst, 2013, 8: C07010
Zhang J, Liu W, Schnitzler V, et al. Calcium phosphate cements for bone substitution: Chemistry, handling and mechanical properties. Acta Biomater, 2014, 10: 1035–1049
Wagoner Johnson AJ, Herschler BA. A review of the mechanical behavior of CaP and CaP/polymer composites for applications in bone replacement and repair. Acta Biomater, 2011, 7: 16–30
Loh QL, Choong C. Three-dimensional scaffolds for tissue engineering applications: Role of porosity and pore size. Tissue Eng Part B-Rev, 2013, 19: 485–502
Chen R, Hunt JA. Biomimetic materials processing for tissue-engineering processes. J Mater Chem, 2007, 17: 3974–3979
Karageorgiou V, Kaplan D. Porosity of 3D biomaterial scaffolds and osteogenesis. Biomaterials, 2005, 26: 5474–5491
Hulbert SF, Young FA, Mathews RS, et al. Potential of ceramic materials as permanently implantable skeletal prostheses. J Biomed Mater Res, 1970, 4: 433–456
Babaie E, Lin B, Bhaduri SB. A new method to produce macro-porous Mg-phosphate bone growth substitutes. Mater Sci Eng-C, 2017, 75: 602–609
Cui W, Song Q, Su H, et al. Synergistic effects of Mg-substitution and particle size of chicken eggshells on hydrothermal synthesis of biphasic calcium phosphate nanocrystals. J Mater Sci Technol, 2020, 36: 27–36
Xiao Y, Yin Q, Wang L, et al. Macro-porous calcium phosphate scaffold with collagen and growth factors for periodontal bone regeneration in dogs. Ceramics Int, 2015, 41: 995–1003
Orsini G, Ricci J, Scarano A, et al. Bone-defect healing with calcium-sulfate particles and cement: An experimental study in rabbit. J Biomed Mater Res, 2004, 68B: 199–208
Acknowledgements
This work was supported by the Key Research Program of Frontier Sciences (QYZDY-SSW-JSC031) from the Chinese Academy of Sciences (CAS), the Key Research and Development Program of Liaoning Province (201703031), Liaoning Science and Technology Project (20170540972) and Shenyang Key R&D and Technology Transfer Program (Z17-7-023).
Author information
Authors and Affiliations
Contributions
Author contributions Xu Q and Cao L prepared the injectable composite materials and conducted the material characterization. Liang J and Xue H designed and performed the animal experiments. Liu Y performed HE staining and analyzed the experimental data. Li X, Tian J and Zhang X conducted the experimental design and result analysis, and revised the manuscript. All authors contributed to the general discussion.
Corresponding authors
Ethics declarations
Conflict of interest The authors declare that they have no conflict of interest.
Additional information
Qian Xu received her master’s degree in materials physics and chemistry from the Northeastern University in 2016. She is currently a PhD student in materials physics and chemistry at the Northeastern University. Her research interest mainly focuses on the development of biomedical materials for orthopaedic applications.
Jiulong Liang received his MD degree in plastic surgery from the Second Military Medical University in 2010. He is currently the director of the Rehabilitation and Reconstruction Center at the General Hospital of the Northern Theater Command. His research interests include microsurgery and auricular reconstruction.
Xiaowu Li received his PhD degree from the Institute of Metal Research, Chinese Academy of Sciences in 1998. He is currently a professor and head of the Department of Materials Physics and Chemistry, School of Materials Science and Engineering, Northeastern University. His research interest mainly focuses on the mechanical behavior of materials including biomaterials.
Jing Tian received his MD degree from the Fourth Military Medical University in 2013. He is currently the deputy chief physician and associate professor in the Department of Orthopedics, the General Hospital of the Northern Theater Command. His research interests include traumatic and infectious bone defect repair.
Supplementary information
Rights and permissions
About this article
Cite this article
Xu, Q., Liang, J., Xue, H. et al. Novel injectable and self-setting composite materials for bone defect repair. Sci. China Mater. 63, 876–887 (2020). https://doi.org/10.1007/s40843-019-1233-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40843-019-1233-7