Abstract
Purpose of review
Healthcare is a complex system where dynamic and unpredictable interactions of system components contribute to errors. In the design of a new healthcare facility, there is a need to increase levels of safety evaluation throughout all phases of hospital development as a means to manage risk. Simulation effectively represents the dynamics of care delivery in order to identify and remediate latent conditions in the built environment or work system prior to patient exposure.
Recent findings
Emerging literature suggests that the integration of human factor approaches with simulation-based activities has the potential to aid healthcare systems in achieving higher quality care. Simulation-based Hospital Design Testing (SbHDT) and Simulation-Based Clinical Systems Testing (SbCST) are applied in order to proactively identify latent conditions related to the built environment, work system, or care processes; ensure operational readiness; and ease transitioning healthcare systems by promoting preparedness.
Summary
Incorporation of simulation into the hospital development process places safety at the forefront of planning. By proactively identifying architectural or system weaknesses, corrective actions can be taken before harm occurs. This review discusses how simulation grounded in safety and architectural design concepts enhance safety evaluation during the development process.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In the last decade, there has been a major boom in the rates of hospital construction to create new or replace aging facilities and/or renovate existing ones to support population shifts [1]. Conflicting goals, limited resources, and the pressure to achieve more, faster, in a cost-effective manner challenges systems to consistently deliver high-quality care [2]. Healthcare-related errors are due to flaws in the system, barriers to optimal functioning, and deviations from prescribed work [3•, 4]. These flaws within the system, known as latent conditions [5,6,7,8,9], contribute to adverse events if not corrected [10]. As the relationship between the work environment and safety is becoming clear, it is necessary to increase levels of safety evaluation throughout all phases of hospital development as a means to reduce the risk [1].
Solutions to aid healthcare systems in managing risk involve the integration of human factor approaches with simulation-based activities [4]. While highly variable in approach, simulation is being utilized with increasing frequency in healthcare design, system development, and evaluation in order to proactively evaluate for latent conditions that can be corrected before harm occurs [11, 12•, 13].
The development of a new healthcare facility is a longitudinal endeavor which we describe in two distinct phases. In the early phase of hospital design, Simulation-based Hospital Design Testing (SbHDT) is conducted preconstruction during architectural planning to evaluate the built environment [14•]. In the postconstruction phase of development, Simulation-Based Clinical Systems Testing (SbCST) is conducted in situ in order to evaluate clinical systems and care processes prior to occupancy [15,16,17, 18•]. SbHDT and SbCST stress the built environment or work system for both routine and high-risk clinical scenarios. Facilitator-directed debriefing is used to conduct a risk analysis and identify latent conditions. Failure mode effect analysis (FMEA) is applied in order to score and prioritize each latent condition identified, thereby focusing efforts on devising solutions that mitigate latent conditions with the highest risk [14•, 15,16,17, 18•].
This review discusses how simulation is uniquely poised to bring together key safety and architectural design concepts to enhance the safety evaluation of a new healthcare facility (Fig. 1).
Safety and architectural concepts
High reliability
High reliability organizations (HROs) are organizations/industries, such as aviation, that operate in complex, high-hazard domains, for extended periods without serious accidents or catastrophic failures [19, 20]. HROs use systems thinking to evaluate and design for safety and are keenly aware that safety is an emergent, rather than a static, property [21]. These organizations maintain safety levels far better than those in healthcare.
Healthcare institutions are increasingly adapting and applying the lessons of HRO science to reach levels of quality and safety of the best high reliability organizations. In designing a new healthcare facility, proactive identification of latent conditions, fostering of safety culture and standardizing the process to reduce variation in care, builds the foundation for a resilient system that allows for challenges and disturbances without leading to system collapse [4].
Simulation integrates HRO concepts and promotes a culture of safety by directly engaging frontline staff and leaders to look at their work system through a lens that is focused on safety [4]. By involving frontline personnel in clinical simulations aimed at stressing systems to find potential threats to patient/provider safety and opportunities for improvement, it applies at least four key principles seen in HROs: (1) preoccupation with failure, (2) reluctance to simplify observations, (3) deference to expertise, and (4) sensitivity to frontline operations. With a focus on the future state, healthcare teams suspend disbelief as they envision future operational models and advancement in care technologies and processes. As a result, they open their minds to inevitable practice change and in comparison, to the current state, are able to identify issues of safety. This shift fosters a bottom-up catalyst to serve as a trigger to transform culture change in the new environment [4].
Healthcare as a complex adaptive system
Healthcare is a complex adaptive system where each component of the system interacts and connects with each other in unpredictable and unplanned ways. In simplistic system modeling, it is assumed if individual system components are understood, then the entire system as a whole is fully realized. In this linear relationship, if each part is made to work better, then the whole system also functions at a higher quality [22]. Due to the complexity of healthcare delivery and the unpredictable ways that system components interact, this simple cause and effect assumption does not apply. In complex system modeling, a single system element is affected by and affects several other elements in a nonlinear interaction, so small changes have large downstream effects [22]. These complex, nonlinear, interactions of system components contribute to errors [23, 24]. The ability to effectively mitigate risk in the design process relies on systems engineering and the study of human factors to better understand the complexities of healthcare delivery [25, 26, 27•]. Simulation effectively demonstrates these dynamic interactions as teams interact and adapt to their environment and work system as they engage in patient care activities.
SEIPS 2.0
The Systems Engineering Initiative for Patient Safety (SEIPS) 2.0 provides a context to characterize these complex system interactions in a clear and concise manner, illustrating the impact that design or process changes have on the work system and patient safety [24]. SEIPS 2.0 describes five components of the work system: person, organization, technologies and tools, tasks, and environment [23, 24]. The work system (structure of an organization) affects how care is provided (process), which in turn impacts how safe care is delivered (outcome) [23, 24]. Feedback loops between system processes to the work system and outcomes to the work system represent opportunities for design and redesign. A failure in any component of the work system has the potential to impact outcomes and when designed well allows systems to function at a higher quality [23, 24]. In SbHDT latent conditions related to the environment are identified, while SbCST evaluates all 5 components of the work system (Table 1) [23, 24].
Evidence-based design
Evidence-based design (EBD) is the study of how the physical environment relates to healthcare outcomes [1, 26]. Rigorous EBD research describing how the built environment impacts patients and staff is applied by architects to influence architectural decisions. EBD encourages designers to create solutions that meet accepted EBD principles in order to reduce healthcare-associated conditions, improve staff job satisfaction, and minimize risk [28].
The Agency for Healthcare Research and Quality (AHRQ) and the Center for Health Design (CHD) describe evidence-based safe design principles (EbSDP) [25, 29]. These well-defined design considerations are known to impact healthcare outcomes and further expand the SEIPS 2.0 definition of the environmental system [23, 24]. SbHDT and SbCST anchored to evidence-based design utilize these principles to ensure that testing objectives are evidence based and can detect a wide range of latent conditions and system inefficiencies (Table 1). Scenarios are developed with pre-identified EbSDP objectives in mind, where each task in the scenario is linked to a design principle. Latent conditions related to design elements that do to meet accepted EBD principles are effectively discovered as participants interact with specific design elements in question.
Latent conditions
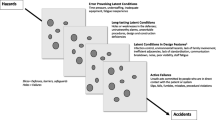
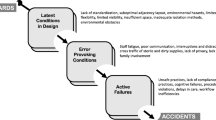
It is important to further understand how components of the healthcare system as described by SEIPS 2.0 relate to harm. The most recognized framework describing the relationship between system errors and healthcare design can be explained by Reason’s Swiss cheese model [6]. This model illustrates how defenses, barriers, and safeguards may be penetrated by an accident.
Latent conditions are flaws that remain hidden until they are revealed retrospectively as a chain of events that contribute to an error [5, 10]. Latent conditions may be error provoking, such as inadequate equipment, or a long-lasting weakness, such as a construction deficiency. An active failure is an error at the level of a frontline provider, where the effect is felt almost immediately [5]. When multiple “holes” align, safeguards may be penetrated, and harm may occur [6]. While unintended, decisions made by architects or system leaders introduce weaknesses into the architectural design or system despite exhaustive planning [5]. For example, lack of a standard location of mounted code blue buttons (long-standing weakness) requires that staff reorient themselves according to each room design (error-provoking condition). If staff cannot find the code blue button during an emergency (active failure), then there may be a delay in care resulting in patient harm (error). During simulation, implementation of care processes in its entirety provides a platform for teams to actively identify latent conditions. The potential impact of those latent conditions is further elucidated and explored during debriefings.
Failure mode and effect analysis
Simulation testing reveals several latent conditions. Ability to categorize and prioritize findings directs teams to focus corrective efforts on addressing latent conditions with the greatest risk of harm. FMEA is an established and widely used proactive risk assessment tool endorsed by AHRQ and Institute for Healthcare Improvement (IHI) [30,31,32]. It is used by multidisciplinary teams to seek out active and latent weaknesses in systems or processes, analyze causes, assess risk, and devise resolutions to remediate flaws [30, 31, 33].
Methodologically integrating simulation with FMEA allows for a robust description of each latent condition identified, the associated potential active failure, and possible solution. The utilization of an FMEA template ensures that a succinct report of all issues identified during simulation is documented. This makes simulation findings less daunting and provides direction for architects or system leaders who have to tackle the complex task of devising resolutions and alternatives to resolve latent conditions [14•, 18•].
Work-as-imagined versus work-as-done
In the planning of a new healthcare facility and evaluation of the work system, there is a practical need to “imagine” (work-as-imagined, WAI) how work would be conducted as part of the design, administrative, and operational planning [34]. It is impossible however, to precisely predict how work should be done, making work-as-imagined inadequate and even directly misleading [34]. Work-as-done (WAD), on the other hand, reflects actual care delivery and the realities of the work system. Ability to experience work-as-done illuminates how work is shaped by the environment and is necessary in order to identify hazards and make improvements [34].
Work-as-imagined is influenced by variation in perspectives, priorities, backgrounds, and experiences. In healthcare design and system development, work-as-imagined by architects and leadership often does not equate to work as performed by frontline staff. This gap impacts ability to effectively convey design intent, rationale for high-level system decisions, or clinical frontline needs. During architectural design or system planning, ineffective communication may steer decision making down a path that results in ineffective design or care processes that cannot be implemented as intended. By providing a shared experience, simulation bridges this gap in perceptions of varying stakeholders to more precisely illuminate how work is done. Here teams witness a course of events play out instead of having to imagine it or review it in hindsight [34].
Simulation-based Hospital Design Testing
SbHDT, implemented 5–7 years prior to facility opening, heavily focuses on assessing the safety of the physical environment where there is the potential to inform major design modifications that would be cost prohibitive and not feasible in an already built facility [35].
Collaboration between architects and clinical teams must occur early on in the design process to devise a design that meets the needs of all stakeholders. Effective collaboration is challenged by the fact that architects and clinicians see physical space through two distinct lenses. Architects are less familiar with intricacies related to patient care delivery [36•] while clinicians are unfamiliar with the role and impact of the built environment. The ability to effectively convey design intent and elicit useful feedback from clinicians is challenging as clinicians have a difficult time imaging how work would be conducted in a proposed space represented as two-dimensional drawings [27•, 34, 36•]. These traditional design evaluation methods are insufficient to predict the breadth of problems that arise when actually delivering patient care. Unleveled perception between clinical teams and architects can lead to less effective design decisions such as inefficient spatial layout that does not optimally support care activities or safe practices.
Simulations provide clinicians with an immersive opportunity to interact with the proposed architectural design and further evaluate room configurations, spatial requirements, equipment placement and accessibility, visibility, and staff experience [34]. Clinicians are able to provide the architect team with feedback, evaluate the impact of design decisions, test functionality and limitations of the environment, and evaluate design alternatives. For example, a simple mockup of inpatient room size may seem adequate. Yet, during simulations, pinch points and work disruptions are revealed as clinicians maneuver supplies and equipment throughout the room. Creative evidence-based design strategies require major architectural changes to radically alter the physical environment in order to resolve latent conditions and address environmental safety concerns. Changes to unit layout, moving walls, reducing the angle of corners, widening doors, and creation of pass-throughs can be accomplished a level of ease that would be impractical and cost-prohibitive postconstruction. Examples of latent conditions, potential active failures, and solutions identified during SbHDT can be found in Table 2.
Simulation-based clinical systems testing
SbCST conducted in situ, postconstruction, prior to occupancy, is implemented in order to identify latent conditions related to the system, care process, operational models [11], ensure operational readiness [37], and ease transitioning healthcare systems by promoting preparedness [13, 38, 39].
In this phase of planning, a significant amount of administrative and operational planning is centered around developing elements of the work system and efficient, safe care processes. This planning involves the conceptualization of work [26, 38]. However, the ability to predict all of the complexities that could actually occur when taking care of patients is impractical [11, 37, 40]. The potential for unintended consequences exists even when a system is developed with good intentions in mind [11]. Planning by system leaders may not be implemented as intended when performed by frontline staff. Barriers to implementation of processes as intended include time pressure, competing priorities, poor communication, or environmental barriers. These hindrances lead to the development of workarounds by frontline staff. Work-arounds are created to bypass these limitations that fail to comply with best practices or policy results in near misses, mistakes, cognitive failures, or procedural violations.
Simulation narrows the gap between high-level system priorities and the limitations that frontline staff face in achieving those goals. Latent conditions identified during SbCST are related to resources; personnel, medication, and equipment that are missing, malfunctioned, or unable to use, process/workflow; policies or procedures that do not work as anticipated, facility; limitations in the built environment not conducive to efficient and safe care, or clinical performance; gaps in knowledge, technical skills, or institutional processes [17]. Latent conditions with the highest potential to result in harm are opportunities for improvement that requires immediate attention and corrective action before facility opening. Accountability and oversight of change implementation are dependent on administrative, operational, and clinical leadership. Examples of latent conditions, potential active failures, and solutions identified in SbCST can be found in Table 2.
Summary
The ability to achieve seamless care delivery in a highly complex healthcare system is challenging given the diversity of tasks, patient care needs, and infinite combinations of care activities [24]. Human factors are consistently in play in healthcare and the complex ways in which humans interact with the work system make space utilization and process implementation unpredictable [17]. Opportunities for clinical teams to improve safety evaluation during architectural and system development of new healthcare facilities are at hand.
SbHDT and SbCST recreate the complexities of patient care delivery to evaluate the dynamic interaction of people with their environment helping to level and calibrate perception of patient care from varying perspectives essential to healthcare. SbHDT and SbCST are uniquely poised at the intersection of human factors, high reliability, and safety to be able to integrate these components into hospital development.
Simulation grounded in healthcare safety concepts and evidence-based design principles allows for a better understanding of work system complexity through the categorization of system elements as described by SEIP 2.0. EBD provides a background to better understand the role that the environment plays in impacting healthcare outcomes. EbSDPs expand on the SEIPS 2.0 definition of the environment, providing well-defined design elements that are the focus of pre-identified testing objectives. Anchoring simulations to EbSDP ensures that testing is able to detect a wide range of latent conditions. Theoretically, if elements of design are modified with the EbSDP in mind, there is a higher likelihood that risk will be mitigated prior to occupancy. Reason’s model provides the framework to understand how those latent conditions, once identified, can lead to potential harm. For clinical teams, methodologically integrating FMEA with simulation allows for a robust description of simulation findings and prioritization of threats, helping providing direction to address latent conditions with the highest risk.
linear evaluation of the work system by human factors and systems engineering analysis alone are insufficient to evaluate interactions of system components as one cannot fully understand space without using it. Therefore, it is impossible and impractical to assume that design teams, administrative, operational, or clinical planners are able to imagine all of the complexities of care delivery. Despite years and hundreds of hours of preparation and planning, the most obvious and simplest design or process flaws can be missed. Simulation provides an organized platform that more accurately represents work-as-done. Incorporation of simulation into the hospital design planning timeline facilitates countless design or system weaknesses to emerge at a time point that allows for course correction prior to delivering patient care. Continued application of simulation in the evaluation of hospital design has the ability to greatly impact how healthcare facilities are built and tested in the future.
Future directions
The ability to demonstrate the impact of design optimizations made in the preconstructed environment on the system once constructed and occupied with patients is yet to be determined. Research is needed to evaluate the impact of simulation testing on outcomes including cost avoidance associated with design and construction change orders, cost savings from mitigated risks, return on investment, impact on post-occupancy risk reduction, and long-term safety outcomes. Additionally, further research is needed to validate simulation as a methodology to identify and mitigate risk in the hospital design process.
Conclusions
In the design of a healthcare facility, SbHDT and SbCST are applied to proactively identify latent conditions in the physical environment or work system. Simulation narrows the gap between work-as-imagined and work-as-done by facilitating a dialog that breaks down the degrees of separation between perception, intent, and actual clinical care delivery. Most importantly, simulation places safety at the forefront of planning to ensure the development of a facility that will better support productive processes, performance, safety, organizational health, and work satisfaction.
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance
Ulrich RS, Zimring C, Zhu X, DuBose J, Seo HB, Choi YS, et al. A review of the research literature on evidence-based healthcare design. HERD. 2008;1(3):61–125.
Provan D, Woods D, Dekker S, Rae A. Safety II professionals: how resilience engineering can transform safety practice. Reliab Eng Syst Saf. 2019;195:106740. https://doi.org/10.1016/j.ress.2019.106740.
Dube MM, Reid J, Kaba A, Cheng A, Eppich W, Grant V, et al. PEARLS for systems integration: a modified PEARLS framework for debriefing systems-focused simulations. Simul Healthc. 2019. https://doi.org/10.1097/SIH.0000000000000381. This study describes PEARLS, for systems integration, a conceptual framework and debriefing structure that is used during for debriefing simulations that are implemented to evaluate latent conditions within the work system.
Paige JT, Terry Fairbanks RJ, Gaba DM. Priorities related to improving healthcare safety through simulation. Simul Healthc. 2018;13(3S Suppl 1):S41–50. https://doi.org/10.1097/SIH.0000000000000295.
Joseph A, Rashid M. The architecture of safety: hospital design. Curr Opin Crit Care. 2007;13(6):714–9. https://doi.org/10.1097/MCC.0b013e3282f1be6e.
Reason J. Human error: models and management. West J Med. 2000;172(6):393–6.
Reiling J, Hughes RG, Murphy MR. The impact of facility design on patient safety. In: Hughes RG, editor. Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville: Advances in Patient Safety; 2008.
Wheeler DS, Geis G, Mack EH, LeMaster T, Patterson MD. High-reliability emergency response teams in the hospital: improving quality and safety using in situ simulation training. BMJ Qual Saf. 2013;22(6):507–14. https://doi.org/10.1136/bmjqs-2012-000931.
Weaver SJ, Lyons R, DiazGranados D, Rosen MA, Salas E, Oglesby J, et al. The anatomy of health care team training and the state of practice: a critical review. Acad Med. 2010;85(11):1746–60. https://doi.org/10.1097/ACM.0b013e3181f2e907.
Reiling J. Safe design of healthcare facilities. Qual Saf Health Care. 2006;15(Suppl 1):i34–40. https://doi.org/10.1136/qshc.2006.019422.
Geis GL, Pio B, Pendergrass TL, Moyer MR, Patterson MD. Simulation to assess the safety of new healthcare teams and new facilities. Simul Healthc. 2011;6(3):125–33. https://doi.org/10.1097/SIH.0b013e31820dff30.
• Torres-Landa S, Neylan C, Quinlan K, Klock C, Jefferson C, Williams NN, et al. Interprofessional simulations to inform perioperative facility planning and design. J Surg Educ. 2019;76(1):223–33. https://doi.org/10.1016/j.jsurg.2018.06.016. This study describes the role of simulation in evaluating a mockup of a proposed perioperative space. Based on participant feedback the perioperative design was modified resulting in increased satisfaction scores.
Villamaria FJ, Pliego JF, Wehbe-Janek H, Coker N, Rajab MH, Sibbitt S, et al. Using simulation to orient code blue teams to a new hospital facility. Simul Healthc. 2008;3(4):209–16. https://doi.org/10.1097/SIH.0b013e31818187f3.
Colman N, Edmond MB, Dalpiaz A, Walter S, Miller DC, Hebbar K. Designing for patient safety and efficiency: simulation-based Hospital Design Testing. HERD. 2020. https://doi.org/10.1177/1937586720921777. This study was a prospective investigation of Simulation-based Hospital Design Testing (SbHDT) in the schematic design planning phase for a 400-bed free standing children’s hospital. Results demonstrated a statistically significant reduction in risk through effective identification of latent conditions and validation of design changes.
Stone KHL, Reid J, Deutsch E. Systems integration, human factors, and simulation. In: Grant V, Cheng A, editors. Comprehensive Healthcare Simulation: Pediatrics Comprehensive Healthcare Simulation. Switzerland: Springer International Publishing; 2016.
Auerbach M, Stone K, Patterson M. The role of simulation in improving patient safety Comprehensive Healthcare Simulation. In: Grant V, Cheng A, editors. Comprehensive Healthcare Simulation: Pediatrics Comprehensive Healthcare Simulation. Switzerland: Springer International Publishing; 2016.
Colman N, Doughty C, Arnold J, Stone K, Reid J, Dalpiaz A, et al. Simulation-based clinical systems testing for healthcare spaces: from intake through implementation. Adv Simul (Lond). 2019;4:19. https://doi.org/10.1186/s41077-019-0108-7.
• Colman N, Stone K, Arnold J, Doughty C, Reid J, Younker S, et al. Prevent safety threats in new construction through integration of simulation and FMEA. Pediatr Qual Saf. 2019;4(4):e189. https://doi.org/10.1097/pq9.0000000000000189. This study discusses the integration of simulation and FMEA risk assessment in evaluating a new space for safety threats, workflow, and process inefficiencies in the post-construction environment, providing a framework for prioritizing issues with the greatest risk for harm.
Carroll JS, Rudolph JW. Design of high reliability organizations in health care. Qual Saf Health Care. 2006;15(Suppl 1):i4–9. https://doi.org/10.1136/qshc.2005.015867.
Weick KE, Sutcliffe KM. Managing the Unexpected: Sustained Performance in a Complex World. In: Jossey-Bass, editor. . 3rd ed. Hoboken: John Wiley & Sons Inc; 2015.
High Reliability. In Agency for Research Healthcare and Quality. 2019. https://psnet.ahrq.gov/primer/high-reliability. Accessed 16 May 2020.
Lipsitz LA. Understanding health care as a complex system: the foundation for unintended consequences. JAMA. 2012;308(3):243–4. https://doi.org/10.1001/jama.2012.7551.
Holden RJ, Carayon P, Gurses AP, Hoonakker P, Hundt AS, Ozok AA, et al. SEIPS 2.0: a human factors framework for studying and improving the work of healthcare professionals and patients. Ergonomics. 2013;56(11):1669–86. https://doi.org/10.1080/00140139.2013.838643.
Carayon P, Schoofs Hundt A, Karsh BT, Gurses AP, Alvarado CJ, Smith M, et al. Work system design for patient safety: the SEIPS model. Qual Saf Health Care. 2006;15(Suppl 1):i50–8. https://doi.org/10.1136/qshc.2005.015842.
Agency for Healthcare Research and Quality. Improve Patient Safety Through Simulation Research. Agency for Healthcare Research and Quality. 2018. https://www.ahrq.gov/research/findings/factsheets/errors-safety/simulproj11/index.html. Accessed 16 May 2020.
Joseph A, Quan X, Taylor E, Jelen M. Designing for Patient Safety: Developing Methods to Integrate Patient Safety Concerns in the Design Process. Center for Healthcare Design. 2012;Appendix V. 105–116. https://www.healthdesign.org/sites/default/files/chd416_ahrqreport_final.pdf
• Bayramzadeh S, Joseph A, Allison D, Shultz J, Abernathy J, Group ROS. Using an integrative mock-up simulation approach for evidence-based evaluation of operating room design prototypes. Appl Ergon. 2018;70:288–99. https://doi.org/10.1016/j.apergo.2018.03.011. This study described the process and tools used as part of a multidisciplinary collaborative approach to the design and evaluation of operating room prototypes. Key design changes were made based on end-user feedback, highlighting the role of participatory and iterative design.
Alfonsi E, Capolongo S, Buffoli M. Evidence based design and healthcare: an unconventional approach to hospital design. Ann Ig. 2014;26(2):137–43. https://doi.org/10.7416/ai.2014.1968.
Patient room design checklist and evaluation tool. In The Center for Health Design. 2015. https://www.healthdesign.org/patient-room-design-checklist-and-evaluation-tool. Accessed 26 April 2016.
Davis S, Riley W, Gurses AP, Miller K, Hansen H. Failure modes and effects analysis based on in situ simulations: a methodology to improve understanding of risks and failures. In: Henriksen K, Battles JB, Keyes MA, Grady ML, editors. Advances in Patient Safety: New Directions and Alternative Approaches (Vol 3: Performance and Tools). Rockville: Advances in Patient Safety; 2008.
Thornton E, Brook OR, Mendiratta-Lala M, Hallett DT, Kruskal JB. Application of failure mode and effect analysis in a radiology department. Radiographics. 2011;31(1):281–93. https://doi.org/10.1148/rg.311105018.
Institute for Healthcare Improvement. Failure Mode and Effect Analysis Tool. Institute for Healthcare Improvement. 2017. http://www.ihi.org/resources/Pages/Tools/FailureModesandEffectsAnalysisTool.aspx. Accessed 12 Sept 2018.
DeRosier J, Stalhandske E, Bagian JP, Nudell T. Using health care failure mode and effect analysis: the VA National Center for patient safety’s prospective risk analysis system. Jt Comm J Qual Improv. 2002;28(5):248–6709.
Health Quality Council of Alberta. Simulation-Based Mock-up Evaluation Framework. Calgary Alberta, Canada. 2016.
Taylor E, Hignett S, Joseph A. The environment of safe care: considering building design as one facet of safety. Int Symp Hum Fact Ergon Healthc Care: Adv Cause. 2014;3:123–7.
• Wingler D, Machry H, Bayramzadeh S, Joseph A, Allison D. Comparing the effectiveness of four different design media in communicating desired performance outcomes with clinical end users. HERD. 2019;12(2):87–99. https://doi.org/10.1177/1937586718796626. This study compared effectiveness of four different design communication media in conveying structural and functional information to clinical end users. Results demonstrated that more immersive media such as mockups increased understanding of proposed design.
Ventre KM, Barry JS, Davis D, Baiamonte VL, Wentworth AC, Pietras M, et al. Using in situ simulation to evaluate operational readiness of a children’s hospital-based obstetrics unit. Simul Healthc. 2014;9(2):102–11. https://doi.org/10.1097/SIH.0000000000000005.
Bender J, Shields R, Kennally K. Testing with simulation before a big move at Women & Infants Hospital. Med Health R I. 2010;93(5):1459-50.
Francoeur C, Shea S, Ruddy M, Fontela P, Bhanji F, Razack S, et al. It takes a village to move a hospital: simulation improves intensive care team preparedness for a move to a new site. Hosp Pediatr. 2018;8(3):148–56. https://doi.org/10.1542/hpeds.2017-0112.
Hollnagel E. Prologue: Why do our expectations of how work should be done never correspond exactly to how work is done? In: Braithwaite J, Wears R, Hollnagel E, editors. Resiliant Health Care III: Reconciling work-as-imagined and work-as-done. Boca Raton: CRC Press, Taylor & Francis Group; 2017.
Acknowledgments
We acknowledge members of the simulation centers at Children’s Healthcare of Atlanta who has diligently worked to deliver SbHDT and SbCST. The simulation community’s knowledge sharing, sharing of success, and failures have played a role in the completion of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors are familiar with submission instructions and are responsible for the content of the manuscript. NC performed background research; conceptualized the manuscript; prepared the article, modified, and revised the tools included in this manuscript; and approved the final version as submitted. KH oversaw the concept and design of this innovation, reviewed, and revised the article, and approved the article as submitted. AD reviewed and revised the article and approved the article as submitted.
Corresponding author
Ethics declarations
Conflict of Interest
Nora Colman declares that she has no conflict of interest. Ashley Dalpiaz declares that she has no conflict of interest. Kiran B. Hebbar declares that he has no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Patient Safety
Rights and permissions
About this article
Cite this article
Colman, N., Dalpiaz, A. & Hebbar, K.B. Simulation Enhances Safety Evaluation in the Design of New Healthcare Facilities. Curr Treat Options Peds 6, 214–225 (2020). https://doi.org/10.1007/s40746-020-00202-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40746-020-00202-7