Abstract
This study is an attempt to explore war-related trauma, its stressful effects, and the coping strategies of Saudi schoolchildren. The authors hypothesized that children exposed to war-related trauma will show higher levels of PTSD, and that those with higher levels of PTSD symptoms use more maladaptive coping strategies. The study describes the correlation between traumatic events and posttraumatic stress disorder (PTSD) as well as coping strategies. Five hundred twenty-seven intermediate and high school students, 12 to 18 years old, living in the conflict zone in southern Saudi Arabia completed three standardized self-reported scales: the War Zone Traumatic Events Checklist, the Child PTSD Symptom Scale, and the Children’s Coping Strategies Checklist. Each participating student was randomly chosen. Analysis was based on two groups: the high-PTSD symptoms group (182 children) and the low-PTSD symptoms group (345 children). The study was conducted between September 2020 and April 2022 while the war was ongoing as part of an ongoing larger study. Children exposed to war-related traumatic events exhibited greater prevalence rates for PTSD. The children reported high levels of PTSD symptoms and applied a variety of coping strategies to manage related stress. Participants rarely reported that psychological or educational interventions had been used to manage the war-related traumatic experiences and PTSD or to improve related coping styles. The results are discussed in the context of mental health services needed for children in the conflict zone. To bridge the gap between health care services and the needs of children with PTSD, and for better understanding and interventions, health professionals are invited to develop a biopsychosocial model that identifies the risks of PTSD related to exposure to war-related traumatic events in school-aged children and, hence, provide a multidisciplinary intervention program that educates, encourages, and supports teachers and parents in following medical recommendations and goals.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
War is a traumatic experience for all who are involved, but it can be especially devastating for children. War-related traumatic events can lead to a range of mental health problems (Catani, 2018). Mental and psychological consequences of war on children include increased rates of negative emotional states and mental disorders. Children who are exposed to war may witness or experience violence, death, destruction, and separation from loved ones. These experiences can have profound and lasting impact on children’s mental and emotional health and can increase their risk of developing mental disorders, both during and after the conflict (Attanayake et al., 2009). The infliction of war upon children should be considered a violation of their essential human rights, as it can affect their physical and psychological well-being and quality of life and have long-term consequences on their development (Bürgin et al., 2022).
One of the most common psychological problems that children exposed to war experience is posttraumatic stress disorder (PTSD), a mental health condition that can develop after a person experiences a traumatic event. PTSD is characterized by symptoms such as intrusive thoughts and memories of the trauma, nightmares, flashbacks, irritability, avoiding reminders of the trauma, and hyperarousal (increased alertness and anxiety) (Ressler et al., 2022). PTSD has been documented in children of all ages who have been exposed to war-related trauma: preschoolers (Feldman & Vengrober, 2011), school-aged children (Perkins et al., 2018), and adolescents (Martsenkovskyi et al., 2020), as well as in young adults (Llabre et al., 2015).
The relationship between PTSD and coping strategies is complex, bidirectional, and not inevitable. Some children who develop PTSD may use adaptive coping strategies and recover from the trauma. Conversely, children who use maladaptive coping strategies may be more likely to develop PTSD (Benuto et al., 2022). Further, children commonly use adaptive coping strategies to avoid showing PTSD symptoms (Pfefferbaum et al., 2014). Several studies have indicated that acceptance and psychological expression could buffer the psychological impact of PTSD in children and young adults (Kilmer & Gil-Rivas, 2010; Gil-Rivas et al., 2007). For example, negative coping strategies in children such as blaming, anger, avoidance, and social withdrawal have all been related to higher levels of PTSD (An et al., 2013; Pina et al., 2008). By contrast, a recent systematic review (Powell et al., 2021) showed that children who used adaptive coping strategies, such as seeking social support and positive cognitive restructuring, were less likely to develop PTSD symptoms after exposure to war trauma.
However, coping strategies are diverse across cultures and can be adapted individually to meet a cultural need and then provide children with their cultural coping mechanism (Kuehn, 2013). Often, this issue raises the question of how children’s coping strategies vary as a function of their sociocultural backgrounds (Xu et al., 2006). Therefore, understanding the involvement of cultural coping strategies among children living in conflict zones will help in developing a guideline for accurate assessment and better mental health promotion and interventions (Arega, 2023). Based on this, the present study is the first exploration of the impact of Yemen’s armed conflict on Saudi children in the Asir region.
The Asir region lies in the southwest of Saudi Arabia and has a population of approximately 2.5 million. It shares a border of armed conflict with the Saada Governorate of Yemen, the base camp and birthplace of the Houthi movement. The Houthi movement has conducted a campaign of attacks against civilians and civilian objects in Saudi Arabia since 2015. These attacks are part of the civil war in Yemen, where Saudi Arabia was involved and leading a military coalition supporting Yemen’s internationally recognized government. There have been several global condemnations of the Houthi militia attack on schools in Saudi Arabia’s Asir region (Saudi Gazette, 2022). Also, in August 2021, the Houthis fired a missile at a civilian airport in Abha, wounding eight civilians. The main Houthi manner of repeated attacks against civilians and critical infrastructures inside Saudi Arabia is via drones.
Aim and Hypotheses
This study investigates the relationship between PTSD and traumatic exposure and coping strategies. Two research hypotheses were addressed: (a) that children exposed to war-related trauma will show higher levels of PTSD and (b) that children with higher levels of PTSD symptoms use more maladaptive coping strategies.
Methods
The current study is part of a larger research project investigating the psychological consequences of Yemen’s armed conflict on children and the general population in southern Saudi Arabia. The study is funded by the Saudi Arabian National Center for Mental Health Promotion.
Participants
Participants selected for this study were students in both intermediate and high schools, aged 12 to 18 years (mean, 14.01 ± 0.88 years). Sample size selection was based on the hypothesis of a 20% (confidence interval [CI] = 15 − 25%) expected prevalence of PTSD in children. Accordingly, the sample comprised 527 intermediate and high school students in the Asir region in southern Saudi Arabia, representing the community of residents living near that zone of armed conflict.
The educational system in Saudi Arabia maintains separate schools for boys and girls. In all, 51 schools (23 for boys and 28 for girls), from three main cities in the Asir region: Abha, Khamis Mushayt, and Ahad Rafidah, were randomly selected for the study. Students were chosen from all three grades (1 to 3) of each intermediate and high school, and only the first 10 students (according to school records) were selected and included in the study.
Procedure
Studies suggest that people with high PTSD symptoms may use different coping strategies compared with people with low PTSD symptoms (Cénat et al., 2020; Thomassen et al., 2018) This could suggest that more PTSD symptoms means greater severity, leading to different coping strategies. For example, people with high PTSD symptoms may be more likely to use maladaptive coping strategies, such as self-harm and avoidance. Therefore, based on the level of PTSD symptoms (i.e., score on the PTSD Symptom Scale [CPSS-5-SR]), the participants were divided into high- and low-PTSD symptoms groups. Children with a score of 21 or higher were assigned to the high-PTSD symptoms group, while those with a score of 20 or lower were assigned to the low-PTSD symptoms group. Analysis was conducted using IBM SPSS Statistics (Version 22). All of the study scales were administered in a quiet place at the students’ schools and took around 15 to 20 min to complete. The study was approved by the institutional review board at Imam Mohammad Ibn Saud Islamic University (Approval Number: 312/2022) and was conducted between September 2020 and April 2022. Written informed consent and parental consent were obtained from all participants.
Instruments
The participating children completed three standardized self-reported scales: the War Zone Traumatic Events Checklist (El Hatw et al., 2015; Thabet et al., 2008), the Child PTSD Symptom Scale for DSM-5 (CPSS-5-SR) (Foa et al., 2018), and the Children’s Coping Strategies Checklist, revised version (CCSC-R1) (Ayers & Sandler, 1999). Because no validated Arabic versions of the instruments were available, all scales were adapted through forward and blind backward translation. The scales were sent to a panel of seven research experts—five academic staff in the Department of Psychology at King Khalid University, one psychiatrist, and one pediatrician—who commented on each scale’s appropriateness and acceptability. The experts all agreed that the scales were applicable within the Saudi environment. All of the scales were then tested in a pilot study involving 50 students, where comments reflecting participants’ difficulty in understanding instructions or items were made and the scales were modified accordingly.
The War Zone Traumatic Events Checklist
This scale describes the most common traumatic events that children could experience in the Saudi war zone due to Yemen’s armed conflict. The checklist was initially developed through a review of the local literature (El Hatw et al., 2015). Then checklist items were formulated through preliminary discussions with parents and an advisory panel including a psychiatrist, psychologists, and pediatricians. The final checklist consisted of 10 items covering the common traumatic events. According to the advisory panel’s recommendation, the checklist used a binary response scale (yes or no) to encourage a high response rate. The checklist is self-reported and requires less than 5 min to complete, and in this study it showed good internal consistency with a Cronbach’s α of 0.89.
The Child PTSD Symptom Scale
This is a 27-item, self-reported scale that evaluates the severity of PTSD symptoms related to a single identified traumatic event. The first part includes 20 items assessing DSM-5 PTSD symptoms experienced in the month prior to assessment. These 20 items cover all four DSM-5 PTSD symptom clusters (or subdimensions): intrusion, avoidance, changes in cognition and mood, and increased arousal and reactivity. The second part includes seven items assessing the impairment in daily functioning resulting from the endorsed symptoms. According to its results, a potential categorical diagnosis of PTSD can be achieved following the DSM-5 diagnostic criteria. The CPSS-5-SR is self-reported and requires minimal completion time (about 10 min). It has, therefore, been documented as a practical screening tool in schools, communities, and groups of children exposed to trauma. This is an efficient and valid measure of DSM-5 PTSD symptoms suitable for 8- to 18-year-old children (Foa et al., 2018). The items are rated on a five-point Likert scale to measure frequency and severity, from 0 (not at all) to 4 (almost always), while the seven items related to functioning are rated on a yes/no scale (Foa et al., 2018). Symptom severity based on the CPSS-5-SR score is as follows: 11 to 20, mild; 21 to 40, moderate; above 41, severe. The cutoff for recognizing possible PTSD in children in the current study was 21 on the full scale, which indicates moderate to severe symptoms and obtains the balance point between sensitivity and specificity (Silwal et al., 2021; Jiang et al., 2021; Foa et al., 2018). Cronbach’s alpha in our sample was 0.91.
The Children’s Coping Strategies Checklist
The Children’s Coping Strategies Checklist, revised version (CCSC-R1) was used in this study (Ayers & Sandler, 1999). It is a self-reported inventory for measuring coping strategies, comprising 54 items, suitable for children 9-years old and over. The scale has 13 subscales, which are divided into 5 dimensions: (1) problem-focused coping, (2) positive cognitive restructuring, (3) distraction coping strategies, (4) avoidance coping strategies, and (5) support-seeking strategies. The CCSC-R1 is answered using a four-point Likert scale (from 1, never, to 4, always). A high score on any subscale indicates high application of that coping strategy. For this study, Cronbach’s alpha for the whole scale was 0.93.
Results
According to their results on the CPSS-5-SR, 182 children (34.5%) were assigned to the high-PTSD symptoms group, and 345 children (65.5%) were assigned to the low-PTSD symptoms group.
The sociodemographic characteristics of the study population (Table 1) indicate that the time children spent in the war zone ranged from 5 to 7 years (SD = 1.4). Comparison of characteristics between the two groups was carried out using chi-square test, and the only significant difference found was between girls and boys in terms of the presence of PTSD symptoms. Girls were more likely to score a high level of PTSD symptoms than boys (χ2 = 5.45, p = .05; M = 26.09, SD = 2.15 for girls, M = 23.92, SD = 1.38 for boys). None of the children (0.0%) were reported to be receiving any kind of mental health services or support linked to the psychological consequences of war-related traumatic events.
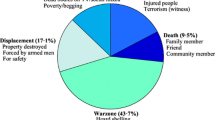
Children scored 7.0 (± 1.9) out of 10 items on the War Zone Traumatic Events Checklist assessing war-related traumatic event experiences (Table 2). There were significant differences between both groups (M = 8.6 ± 2.3; t = 3.73, p = .01). The most frequently experienced war-related traumatic events reported by the high-PTSD group were hearing anti-missiles (93%), leaving school/being absent due to shelling (83%), and witnessing the signs of shelling (77%). The most common war-related traumatic events reported by both groups were watching war-related traumatic events on television (83%) or other sources such as social media (93%), with no statistical significance between the two groups.
The children in our sample showed a variety of PTSD symptom clusters. As seen from the results in Table 3, there was a positive correlation between war-related traumatic experiences and the total score obtained on the CPSS-5-SR, the scores for subdimensions avoidance, changes in cognition and mood, and increased arousal and reactivity (p < .01), and the score for the subdimension intrusion (p < .05). This result indicates that a higher level of traumatic psychological experiences among the participants indicates a higher level of PTSD. There was no correlation between war-related traumatic experiences and the total score on the CCSC-R1 and its subdimensions except for avoidance coping strategies, which showed positive correlation (p < .05).
As seen in Table 4, children in the high-PTSD group used more problem-focused coping strategies, avoidance coping strategies, and distraction coping strategies, as well as more coping strategies overall compared with the low-PTSD group. There were statistically significant differences between the mean ranks of the two PTSD groups according to the CCSC-R1 in subdimensions problem-focused coping strategies (p < .05), avoidance coping strategies (p < .01), and distraction coping strategies (p < .001) as well as the total score (p < .01), with the high-PTSD symptoms group scoring higher.
Discussion
This investigation aimed to establish the association between war-related traumatic events, PTSD, and coping strategies in schoolchildren in the zone of conflict during a period of ongoing exposure to trauma (while the war was going on). The findings show that a significant percentage of intermediate and high school students in the Asir area, the border war zone of the Yemen armed conflict, showed moderate to high levels of PTSD symptoms based on the frequency of war-related traumatic experiences.
Except for gender, demographic characteristics did not explain the reason for the differences between the participants in level of PTSD. Girls in this study reported higher levels of PTSD than boys. This finding is consistent with the results of most previous studies carried out in various war zones (Yayan et al., 2020; El-Khodary & Samara, 2019; Solberg et al., 2020; Osokina et al., 2023). The vast majority of the sample in the present study (both high- and low-PTSD symptoms groups) had been exposed to at least two war-related traumatic events, and many of the remaining children had experienced more than one. These included witnessing the event, having auditory or visual experiences, experiencing drone attacks, and other direct experiences. Our results are broadly compatible with other results reported in the Middle-East including those by Alghamdi (2020) and Thabet et al. (2004).
As reported in previous studies (Thabet et al., 2008), the most common war-related traumatic experience was linked to reports on television or social media connected to Yemen’s armed conflict. However, there was no significant differences between the two groups. Children seem to be exposed to war scenes both on television and through social media, and it is common for Saudi families to spend a significant amount of time watching the news and other programs about Yemen’s armed conflict without understanding the negative effect of such programs on their children. Children everywhere are unable to protect themselves from the coverage and images of war. They can be indirectly and collectively affected by war experiences through television and social media. This means that they are constantly exposed to reminders of the war through television, news reports, social media posts, and conversations with others, which could conjure up several negative emotions in children, such as anxiety, fear, and stress (Bürgin et al., 2022). It could be beneficial to measure such exposure and consider its potential effects on children with PTSD as part of a prevention and management plan. In war zones, interventions should minimize the disruption happening to communities and families and involve parents in preventive or therapeutic programs for children whenever possible. Interventions should also address the negative and passive effects of the media’s coverage of war on children’s mental health (Thabet et al., 2009; Eltanamly et al., 2021).
Another traumatic event revealed in our results is experiencing drone attacks. As shown in previous studies (Hijazi et al., 2019) about the salient psychological effects of the traumatic experience related to drone attacks, depicting the pervasive emotion of the apprehension of anticipating attacks (Amnesty International, 2013; Walters, 2014), children at this age (i.e., intermediate and high school students) could be traumatized when they learn that attacks are drone-driven, because they know that drones are small and can be difficult to detect. Also, drones have been able to reach many populated areas, including schools, and not only military areas. It is not always clear whether the psychological consequences of drone strikes differ from those of other aerial strikes. And although there is a slight concern that drone attacks could boost anxiety and trauma, research is lacking in this area. Understanding how this occurs and how it could play a mediating role requires further investigation in the future.
On the other hand, the hypothesis that children exposed to war-related trauma would exhibit higher levels of PTSD was supported. Our sample, which represents the community of residents near the armed conflict zone, revealed a high level of PTSD and perhaps other psychological disorders. This result is consistent with those of other studies (Thabet et al., 2008; Kandemir et al., 2018; El-Khodary et al., 2020) documenting that when there is an increase in exposure to war-related traumatic events, there is an equal increase in PTSD and its subdimensions intrusion, avoidance, negative changes in cognition and mood, and increased arousal and reactivity; this highlights the urgent need for early psychological evaluation and support programs (El-Khodary et al., 2020).
As mentioned above, there is a significant correlation between war-related traumatic events and the CPSS-5-SR subdimensions, the greatest being with increased arousal and reactivity. This is likely because the data were collected while the war was still ongoing. During war, children may be more likely to show certain PTSD symptoms in order to reduce anxiety in the face of imminent danger (Allwood et al., 2002). However, the methodological issues in the current study, such as sample recruitment, sample age, and effect size might render the results conservative in estimating how war experiences affect PTSD symptoms in children.
Our study’s second hypothesis, that children with higher levels of PTSD symptoms use more maladaptive coping strategies, was partially supported. Children exposed to war-related traumatic experiences frequently adopt a variety of coping strategies (Ehntholt & Yule, 2006) that might influence symptom severity and morbidity (Pfefferbaum, 1997). Also, their coping skills can be either a protective or a risk factor for PTSD symptoms. Avoidant coping strategies, blame and anger, and social withdrawal have been shown to be risk factors for PTSD in children (Novo Navarro et al., 2018). The current results suggest that schoolchildren could adopt unhealthy coping strategies such as avoidant coping styles (including, for example, denial, wishful thinking, or emotional suppression) to disengage from stressful situations (Garcia et al., 2018). In fact, a recent study in Saudi Arabia by Alghamdi (2020) reported that children living in the southern border conflict zones failed to adopt some positive psychological strategies, such as problem-focused coping strategy, which was negatively associated with PTSD. Another study in the Middle-East showed that avoidant coping strategies in children, for example, are associated with maladaptive responses to traumatic experiences (Abdelaziz et al., 2013).
Consistent with previous research (Bartone & Homish, 2020; Fino et al., 2020), the current findings suggest that children may use a variety of coping strategies to deal with war-related traumatic experiences, and that the most common coping strategies are not always the most positive. Rather, children with high levels of PTSD symptoms tended to use maladaptive coping strategies, and this coping style was associated with an increase in mental health problems. This fits with previous studies that have suggested that more negative coping strategies is associated with higher levels of fear and anxiety (Ollendick et al., 2001). However, several studies reported that during stressful situations students could have helped themselves by adopting either negative or positive coping strategies (Babicka-Wirkus et al., 2021; Son et al., 2020).
Furthermore, cultural background could be responsible for which psychological responses are favored, albeit in different ways, and it could be considered among the most essential reasons for the differences in children’s coping strategies (Chun et al., 2006). The chosen coping strategies are particular interactions between the children and their cultures. The boundaries between well and sick, mainly in mental health, are far from clear, as they are explained according to cultural and social considerations (Engel, 1977). Cultural background here could be explained by several models, one is the collectivistic coping model, which highlights a culture’s impacts on the stress-coping process via collectivistic values and orientation (Yeh et al., 2006). Overall, collective coping behaviors are conceived from the community norms and values of a cultural group, and they involve a broad array of coping strategies ranging from those that are value-driven to others that are culturally conditioned or spirituality-oriented (Kuo, 2013).
The remarkable point the current findings reveal is that none of the children who were exposed to war-related traumatic events were previously identified as needing psychological help or support or referred for any mental health care. The results of previous similar studies reveal that children exposed to war-related traumatic events cannot regulate their emotions and that they could continue to experience mental health problems even many years after the war (Diab et al., 2019). A study in Lebanon found that children had psychological disorders such as posttraumatic stress, anxiety, and depression both immediately and one year after the armed conflicts (Karam et al., 2014). Five years after the military operation in Iraq, a regional study found that more than 85% of children exposed to war-related trauma still had PTSD (Ahmad et al., 2000).
Some studies suggest that the main barriers to mental health interventions for war-affected children are difficulties in priority setting and an insufficient mental health workforce (Vus et al., 2023). Other explanations could be related to lack of parental or caregiver awareness. Some parents may not be well-versed in mental health issues, which may limit their ability to monitor and understand their children’s subtle behavioral changes (Stormacq et al., 2019). However, community outreach efforts can overcome barriers to seeking mental health services like worrying about stigma and lack of awareness (Ahmed & Amer, 2013). Thus, cultural factors and the availability of mental health services must be accounted for as much as psychological and biological factors when analyzing coping strategies (Chun et al., 2006; Novita et al., 2019).
Developing a biopsychosocial model to assess children’s PTSD related to traumatic war events is essential. The biopsychosocial intervention was proposed as an essential change from the biomedical model in which health was the result of the absence of disease and illness, and treatment options were understood within a physiological concept (Engel, 1977). The model includes three main parts: the biological domain, such as the brain, genetics, and endocrine system; the psychological domain, which includes both emotional and cognitive processes and responses; and the social domain, which links perceptions of self to social settings (Black & Hoeft, 2015). This biopsychosocial model of mental health intervention may focus on emotion regulation, adjustment to new environments, and empowering children with effective problem-focused coping strategies.
Finally, while the sample was limited to children exposed to the war-related traumatic events of Yemen’s armed conflict on the Asir region, the current findings might justify the assumption that other children, in Jizan and Najran regions (also close to the conflict zone), could suffer from similar symptoms.
In contrast, on the other side of this war, children in Yemen might also be affected (more or less) by PTSD and its maladaptive coping strategies. A study among children in Yemen showed that approximately 80% experienced PTSD symptoms linked to exposure to war-related traumatic events (Al-Ammar, 2018). The suffering in the armed conflict zone falls on children on both the Saudi and the Yemeni sides. Therefore, it is important here to emphasize children’s rights, on both sides, and that every child has an inherent right to life that must be ensured, to the maximum extent possible, with high quality mental, physical, and psychological states.
Limitations
We identified multiple methodological limitations. We applied a quantitative method, which does not allow for the investigator to speak in depth with children adopting their own coping strategies or for the children to express their concerns about exposure to war-related traumatic events; therefore, a qualitative approach is recommended for future investigations. Other limitations relate to the translation and adaptation of all the assessment tools that were used for this study, the self-reported nature of the assessment tools in general, and the cross-sectional nature of the study. Funding should be viewed accordingly. However, the performance of the assessment tools used showed some evidence of convergent validity, and they can be used and retested in future Arabic studies. A further limitation is that our school-based sample may have excluded children with severe traumatic war experiences, limiting the generalizability of the findings to children who are not in school.
Lastly, it is worth mentioning that part of this study was carried out during the peak of the COVID-19 pandemic in Saudi Arabia, when the local community was influenced by the associated precautionary behaviors. Such behaviors could, on their own, act as a trigger for anxiety, PTSD, and other mental health issues. Hence, these results should be interpreted accordingly.
Conclusions
Exposure to war-related traumatic events poses a significant risk for developing PTSD in children, with potential long-term consequences for their mental health and well-being. Based on this, the establishment of psychosocial clinics for children experiencing war-related traumatic events in the southern conflict zone in Saudi Arabia should include comprehensive treatment and support, and should be oriented toward coping strategies (El Hatw et al., 2015). Prompt intervention plans should focus on providing essential psychosocial and emotional resources to help children obtain both inner security and external safety. Teachers and child care professionals must be trained in recognizing and helping PTSD-affected children at school. The current conflict crisis requires the establishment of guidelines, formulation of policies, and collective engagement of multidisciplinary mental health professionals to minimize harm to children exposed directly or indirectly to war and its consequences (Bürgin et al., 2022).
References
Abdelaziz, T., Abdulla, T., & Vostanis, P. (2013). Coping strategies of children and adolescents exposed to war conflict. Arabpsynet E Journal, 39(40), 289–295. https://refugeeresearch.net/wp-content/uploads/2017/06/Coping-strategies-of-children-and-adolescents-exposed-to-war-conflict.pdf.
Ahmad, A., Sofi, M. A., Sundelin-Wahlsten, V., & von Knorring, A. L. (2000). Posttraumatic stress disorder in children after the military operation Anfal in Iraqi Kurdistan. European Child & Adolescent Psychiatry, 9(4), 235–243. https://doi.org/10.1007/s007870070026.
Ahmed, S., & Amer, M. M. (Eds.). (2013). Counseling muslims: Handbook of mental health issues and interventions. Routledge.
Al-Ammar, F. (2018). Post-traumatic stress disorder among Yemeni children as a consequence of the ongoing war CARPO. https://carpo-bonn.org/wp-content/uploads/2018/03/10_carpo_brief_final.pdf.
Alghamdi, M. (2020). Resilience and trauma in the Southern Border conflict region of Saudi Arabia. Mediterranean Journal of Clinical Psychology, 8(2). https://doi.org/10.6092/2282-1619/mjcp-2386.
Allwood, M. A., Bell-Dolan, D., & Husain, S. A. (2002). Children’s trauma and adjustment reactions to violent and nonviolent war experiences. Journal of the American Academy of Child & Adolescent Psychiatry, 41(4), 450–457. https://doi.org/10.1097/00004583-200204000-00018.
Amnesty International. (21 (October, 2013). Will I be next? US drone strikes in Pakistan. https://www.amnestyusa.org/reports/willi-be-next-us-drone-strikes-in-pakistan/.
An, Y., Fu, F., Wu, X., Lin, C., & Zhang, Y. (2013). Longitudinal relationships between neuroticism, avoidant coping, and posttraumatic stress disorder symptoms in adolescents following the 2008 Wenchuan earthquake in China. Journal of Loss and Trauma, 18(6), 556–571. https://doi.org/10.1080/15325024.2012.719351.
Arega, N. T. (2023). March). Mental health and psychosocial support interventions for children affected by armed conflict in low-and middle-income countries: A systematic review. Child & Youth Care Forum, 52, 1431–1456. https://doi.org/10.1007/s10566-023-09741-0.
Attanayake, V., McKay, R., Joffres, M., Singh, S., Burkle, F. Jr., & Mills, E. (2009). Prevalence of mental disorders among children exposed to war: A systematic review of 7,920 children. Medicine Conflict and Survival, 25(1), 4–19. https://doi.org/10.1080/13623690802568913.
Ayers, T. A., & Sandler, I. N. (1999). Manual for the children’s coping strategies Checklist & the how I coped under pressure scale. Arizona State University. https://www.yumpu.com/en/document/read/12240213/manual-for-the-childrens-coping-strategies-checklist.
Babicka-Wirkus, A., Wirkus, L., Stasiak, K., & Kozłowski, P. (2021). University students’ strategies of coping with stress during the coronavirus pandemic: Data from Poland. PloS ONE, 16(7), e0255041. https://doi.org/10.1371/journal.pone.0255041.
Bartone, P. T., & Homish, G. G. (2020). Influence of hardiness, avoidance coping, and combat exposure on depression in returning war veterans: A moderated-mediation study. Journal of Affective Disorders, 265, 511–518. https://doi.org/10.1016/j.jad.2020.01.127.
Benuto, L. T., Yang, Y., Bennett, N., & Lancaster, C. (2022). Distress tolerance and emotion regulation as potential mediators between secondary traumatic stress and maladaptive coping. Journal of Interpersonal Violence, 37(13–14), NP11557–NP11581. https://doi.org/10.1177/0886260520967136.
Black, J. M., & Hoeft, F. (2015). Utilizing biopsychosocial and strengths-based approaches within the field of child health: What we know and where we can grow. New Directions for Child and Adolescent Development, 2015(147), 13–20. https://doi.org/10.1002/cad.20089.
Bürgin, D., Anagnostopoulos, D., Vitiello, B., Sukale, T., Schmid, M., FegertJM, & Board and Policy Division of ESCAP. (2022). Impact of war and forced displacement on children’s mental health-multilevel, needs-oriented, and trauma-informed approaches. European Child & Adolescent Psychiatry, 31(6), 845–853. https://doi.org/10.1007/s00787-022-01974-z.
Catani, C. (2018). Mental health of children living in war zones: A risk and protection perspective. World Psychiatry, 17(1), 104–105. https://doi.org/10.1002/wps.20496.
Cénat, J. M., McIntee, S. E., & Blais-Rochette, C. (2020). Symptoms of posttraumatic stress disorder, depression, anxiety and other mental health problems following the 2010 earthquake in Haiti: A systematic review and meta-analysis. Journal of Affective Disorders, 273, 55–85. https://doi.org/10.1016/j.jad.2020.04.046.
Chun, C. A., Moos, R. H., & Cronkite, R. C. (2006). Culture: A fundamental context for the stress and coping paradigm. In P. T. P. Wong & L. C. J. Wong (Eds.), Handbook of multicultural perspectives on stress and coping (pp. 29–53). Spring Publications. https://doi.org/10.1007/0-387-26238-5_2.
Diab, M., Peltonen, K., Qouta, S. R., Palosaari, E., & Punamäki, R. L. (2019). Can functional emotion regulation protect children’s mental health from war trauma? A Palestinian study. International Journal of Psychology, 54(1), 42–52. https://doi.org/10.1002/ijop.12427.
Ehntholt, K. A., & Yule, W. (2006). Practitioner review: Assessment and treatment of refugee children and adolescents who have experienced war-related trauma. Journal of Child Psychology and Psychiatry, 47(12), 1197–1210. https://doi.org/10.1111/j.1469-7610.2006.01638.x.
El Hatw, M. M., Taher, E., El Hamidi, A. A., A., & Alturkait, F. A. (2015). The association of exposure to the 2009 south war with the physical, psychological, and family well-being of Saudi children. Saudi Medical Journal, 36(1), 73–81. https://doi.org/10.15537/smj.2015.1.9494.
El-Khodary, B., & Samara, M. (2019). The mediating role of trait emotional intelligence, prosocial behaviour, parental support and parental psychological control on the relationship between war trauma, and PTSD and depression. Journal of Research in Personality, 81, 246–256. https://doi.org/10.1016/j.jrp.2019.06.004.
El-Khodary, B., Samara, M., & Askew, C. (2020). Traumatic events and PTSD among Palestinian children and adolescents: The effect of demographic and socioeconomic factors. Frontiers in Psychiatry, 11, 4. https://doi.org/10.3389/fpsyt.2020.00004.
Eltanamly, H., Leijten, P., Jak, S., & Overbeek, G. (2021). Parenting in times of war: A meta-analysis and qualitative synthesis of war exposure, parenting, and child adjustment. Trauma. Violence & Abuse, 22(1), 147–160. https://doi.org/10.1177/1524838019833001.
Engel, G. L. (1977). The need for a new medical model: A challenge for biomedicine. Science, 196(4286), 129–136. https://www.urmc.rochester.edu/MediaLibraries/URMCMedia/medical-humanities/documents/Engle-Challenge-to-Biomedicine-Biopsychosicial-Model.pdf.
Feldman, R., & Vengrober, A. (2011). Posttraumatic stress disorder in infants and young children exposed to war-related trauma. Journal of the American Academy of Child & Adolescent Psychiatry, 50(7), 645–658. https://doi.org/10.1016/j.jaac.2011.03.001.
Fino, E., Mema, D., & Russo, P. M. (2020). War trauma exposed refugees and posttraumatic stress disorder: The moderating role of trait resilience. Journal of Psychosomatic Research, 129, 109905. https://doi.org/10.1016/j.jpsychores.2019.109905.
Foa, E. B., Asnaani, A., Zang, Y., Capaldi, S., & Yeh, R. (2018). Psychometrics of the child PTSD Symptom Scale for DSM-5 for trauma-exposed children and adolescents. Journal of Clinical Child & Adolescent Psychology, 47(1), 38–46. https://doi.org/10.1080/15374416.2017.1350962.
Garcia, F. E., Barraza-Pena, C. G., Wlodarczyk, A., Alvear-Carrasco, M., & Reyes-Reyes, A. (2018). Psychometric properties of the Brief-COPE for the evaluation of coping strategies in the Chilean population. Psicologia Reflexao E Critica, 31(1), 22. https://doi.org/10.1186/s41155-018-0102-3.
Gil-Rivas, V., Silver, R. C., Holman, E. A., McIntosh, D. N., & Poulin, M. (2007). Parental response and adolescent adjustment to the September 11, 2001 terrorist attacks. Journal of Traumatic Stress, 20(6), 1063–1068. https://doi.org/10.1002/jts.20277.
Hijazi, A. M., Ferguson, C. J., Ferraro, R., Hall, F., Hovee, H., M., & Wilcox, S. L. (2019). Psychological dimensions of drone warfare. Current Psychology, 38(5), 1285–1296. https://doi.org/10.1007/s12144-017-9684-7.
Jiang, H., Jin, L., Qian, X., Xiong, X., La, X., Chen, W., Yang, X., Yang, F., Zhang, X., Abudukelimu, N., Li, X., Xie, Z., Zhu, X., Zhang, X., Zhang, L., Wang, L., Li, L., & Li, M. (2021). Maternal mental health status and approaches for accessing antenatal care information during the COVID-19 epidemic in China: Cross-sectional study. Journal of Medical Internet Research, 23(1), e18722. https://doi.org/10.2196/18722.
Kandemir, H., Karataş, H., Çeri, V., Solmaz, F., Kandemir, S. B., & Solmaz, A. (2018). Prevalence of war-related adverse events, depression and anxiety among Syrian refugee children settled in Turkey. European Child & Adolescent Psychiatry, 27(11), 1513–1517. https://doi.org/10.1007/s00787-018-1178-0.
Karam, E. G., Fayyad, J., Karam, A. N., Melhem, N., Mneimneh, Z., Dimassi, H., & Tabet, C. C. (2014). Outcome of depression and anxiety after war: A prospective epidemiologic study of children and adolescents. Journal of Traumatic Stress, 27(2), 192–199. https://doi.org/10.1002/jts.21895.
Kilmer, R. P., & Gil-Rivas, V. (2010). Exploring posttraumatic growth in children impacted by Hurricane Katrina: Correlates of the phenomenon and developmental considerations. Child Development, 81(4), 1211–1227. https://doi.org/10.1111/j.1467-8624.2010.01463.x.
Kuehn, P. D. (2013). Cultural coping strategies and their connection to grief therapy modalities for children: An investigation into current knowledge and practice [Master’s thesis, University of St. Thomas, Minnesota]. https://ir.stthomas.edu/cgi/viewcontent.cgi?article=1213&context=ssw_mstrp
Kuo, B. C. (2013). Collectivism and coping: Current theories, evidence, and measurements of collective coping. International Journal of Psychology, 48(3), 374–388. https://doi.org/10.1080/00207594.2011.640681.
Llabre, M. M., Hadi, F., La Greca, A. M., & Lai, B. S. (2015). Psychological distress in young adults exposed to war-related trauma in childhood. Journal of Clinical Child & Adolescent Psychology, 44(1), 169–180. https://doi.org/10.1080/15374416.2013.828295.
Martsenkovskyi, D., Napryeyenko, O., & Martsenkovsky, I. (2020). Depression in adolescents exposed to war trauma risk factors for development of depression in adolescents exposed to war trauma: Does PTSD matter? Global Psychiatry Archives, 3(2), 227–240. https://doi.org/10.52095/gpa.2020.1379.
Novita, S., Uyun, Q., Witruk, E., & Siregar, J. R. (2019). Children with dyslexia in different cultures: Investigation of anxiety and coping strategies of children with dyslexia in Indonesia and Germany. Annals of Dyslexia, 69(2), 204–218. https://doi.org/10.1007/s11881-019-00179-5.
Novo Navarro, P., Landin-Romero, R., Guardiola-Wanden-Berghe, R., Moreno-Alcázar, A., Valiente-Gómez, A., Lupo, W., García, F., Fernández, I., Pérez, V., & Amann, B. L. (2018). The EMDR therapy protocol, hypotheses of its mechanism of action and a systematic review of its efficacy in the treatment of post-traumatic stress disorder. Revista de Psiquiatría y Salud Mental (English Edition), 11(2), 101–114. https://doi.org/10.1016/j.rpsm.2015.12.002. 25 years of Eye Movement Desensitization and Reprocessing (EMDR).
Ollendick, T. H., Langley, A. K., Jones, R. T., & Kephart, C. (2001). Fear in children and adolescents: Relations with negative life events, attributional style, and avoidant coping. The Journal of Child Psychology and Psychiatry and Allied Disciplines, 42(8), 1029–1034. https://pubmed.ncbi.nlm.nih.gov/11806684/.
Osokina, O., Silwal, S., Bohdanova, T., Hodes, M., Sourander, A., & Skokauskas, N. (2023). Impact of the Russian invasion on mental health of adolescents in Ukraine. Journal of the American Academy of Child & Adolescent Psychiatry, 62(3), 335–343. https://doi.org/10.1016/j.jaac.2022.07.845.
Perkins, J. D., Ajeeb, M., Fadel, L., & Saleh, G. (2018). Mental health in Syrian children with a focus on post-traumatic stress: A cross-sectional study from Syrian schools. Social Psychiatry and Psychiatric Epidemiology, 53(11), 1231–1239. https://doi.org/10.1007/s00127-018-1573-3.
Pfefferbaum, B. (1997). Posttraumatic stress disorder in children: A review of the past 10 years. Journal of the American Academy of Child & Adolescent Psychiatry, 36(11), 1503–1511. https://doi.org/10.1016/S0890-8567(09)66558-8.
Pfefferbaum, B., Noffsinger, M. A., Wind, L. H., & Allen, J. R. (2014). Children’s coping in the context of disasters and terrorism. Journal of Loss and Trauma, ‘9(1), 78–97. https://doi.org/10.1080/15325024.2013.791797.
Pina, A. A., Villalta, I. K., Ortiz, C. D., Gottschall, A. C., Costa, N. M., & Weems, C. F. (2008). Social support, discrimination, and coping as predictors of posttraumatic stress reactions in youth survivors of Hurricane Katrina. Journal of Clinical Child & Adolescent Psychology, 37(3), 564–574. https://doi.org/10.1080/15374410802148228.
Powell, T., Wegmann, K. M., & Backode, E. (2021). Coping and post-traumatic stress in children and adolescents after an acute onset disaster: A systematic review. International Journal of Environmental Research and Public Health, 18(9), 4865. https://doi.org/10.3390/ijerph18094865.
Ressler, K. J., Berretta, S., Bolshakov, V. Y., Rosso, I. M., Meloni, E. G., Rauch, S. L., & Carlezon, W. A. Jr. (2022). Post-traumatic stress disorder: Clinical and translational neuroscience from cells to circuits. Nature Reviews Neurology, 18(5), 273–288. https://doi.org/10.1038/s41582-022-00635-8.
Saudi Gazette (2021, June 14). US leads global condemnation of Houthi drone attack on Asir school. Saudi Gazette. https://saudigazette.com.sa/article/607772.
Silwal, S., Chudal, R., Dybdahl, R., Sillanmäki, L., Lien, L., & Sourander, A. (2021). Post-traumatic stress and depressive symptoms among adolescents after the 2015 earthquake in Nepal: A longitudinal study. Child Psychiatry & Human Development, 1–10. https://doi.org/10.1007/s10578-021-01136-3.
Solberg, Ø., Nissen, A., Vaez, M., Cauley, P., Eriksson, A. K., & Saboonchi, F. (2020). Children at risk: A nation-wide, cross-sectional study examining post-traumatic stress symptoms in refugee minors from Syria, Iraq and Afghanistan resettled in Sweden between 2014 and 2018. Conflict and Health, 14(1), 1–12. https://doi.org/10.1186/s13031-020-00311-y.
Son, C., Hegde, S., Smith, A., Wang, X., & Sasangohar, F. (2020). Effects of COVID-19 on college students’ mental health in the United States: Interview survey study. Journal of Medical Internet Research, 22(9), e21279. https://doi.org/10.2196/21279.
Stormacq, C., Van den Broucke, S., & Wosinski, J. (2019). Does health literacy mediate the relationship between socioeconomic status and health disparities? Integrative review. Health Promotion International, 34(5), e1–e17. https://doi.org/10.1093/heapro/day062.
Thabet, A. A. M., Abed, Y., & Vostanis, P. (2004). Comorbidity of PTSD and depression among refugee children during war conflict. Journal of Child Psychology and Psychiatry, 45(3), 533–542. https://doi.org/10.1111/j.1469-7610.2004.00243.x.
Thabet, A. A., Tawahina, A. A., El Sarraj, E., & Vostanis, P. (2008). Exposure to war trauma and PTSD among parents and children in the Gaza strip. European Child & Adolescent Psychiatry, 17(4), 191–199. https://doi.org/10.1007/s00787-007-0653-9.
Thabet, A. A., Ibraheem, A. N., Shivram, R., Winter, E. A., & Vostanis, P. (2009). Parenting support and PTSD in children of a war zone. International Journal of Social Psychiatry, 55(3), 226–237. https://doi.org/10.1177/0020764008096100.
Thomassen, Å. G., Hystad, S. W., Johnsen, B. H., Johnsen, G. E., & Bartone, P. T. (2018). The effect of hardiness on PTSD symptoms: A prospective mediational approach. Military Psychology, 30(2), 142–151. https://doi.org/10.1080/08995605.2018.1425065.
Vus, V., Shipley, K., & Lühmann, T. (2023). Mapping and identifying barriers and facilitators to mental health and psychosocial support interventions for war-affected children. Polski Merkuriusz Lekarski, 51(1), 64–73. https://doi.org/10.36740/Merkur202301110.
Walters, W. (2014). Drone strikes, dingpolitik and beyond: Furthering the debate on materiality and security. Security Dialogue, 45(2), 101–118. https://doi.org/10.1177/0967010613519162.
Xu, Y., Farver, J. M., Chang, L., Yu, L., & Zhang, Z. (2006). Culture, family contexts, and children’s coping strategies in peer interactions. In X. Chen, D. French, & B. Schneider (Eds.), Peer relationships in cultural context (pp. 264–280). Cambridge University Press. https://doi.org/10.1017/CBO9780511499739.012.
Yayan, E. H., Düken, M. E., Özdemir, A. A., & Çelebioğlu, A. (2020). Mental health problems of Syrian refugee children: Post-traumatic stress, depression and anxiety. Journal of Pediatric Nursing, 51, e27–e32. https://doi.org/10.1016/j.pedn.2019.06.012.
Yeh, C. J., Arora, A. K., & Wu, K. A. (2006). A new theoretical model of collectivistic coping. In P. T. P. Wong & L. C. J. Wong (Eds.), Handbook of multicultural perspectives on stress and coping (pp. 55–72). Springer. https://doi.org/10.1007/0-387-26238-5_3.
Acknowledgements
The authors thank all participants and parents for their interest and willingness to contribute to the study. We extend our heartfelt appreciation to all the teachers and school professionals who helped us recruit participants. Finally, we are delighted to acknowledge the invaluable contribution of the Saudi National Center for Mental Health Promotion in funding this project.
Funding
This research was funded by the National Center for Mental Health Promotion, Saudi Arabia (https://ncmh.org.sa).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics, Approval, and Consent to Participate
The Research Ethics Committee at Imam Mohammad Ibn Saud Islamic University (Approval Number: 312/2022). Verbal informed consent was obtained from all participants prior to the interviews.
Competing Interests
The authors declare that they have no competing conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alqahtani, M.M.J., Al-Loghbi, A.S., AlSalehi, S.M. et al. Coping Mechanisms and Posttraumatic Stress Exhibited by Children in Areas of Yemen’s Armed Conflict in Southern Saudi Arabia. Journ Child Adol Trauma 17, 723–733 (2024). https://doi.org/10.1007/s40653-024-00630-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40653-024-00630-9