Abstract
Purpose
Nonalcoholic fatty liver disease (NAFLD) is associated with various metabolic abnormalities that can increase the risk of an osteoporotic fracture. Across the few previous studies of the association between NAFLD and bone mineral density (BMD), the association was not consistent. We examined the association between BMD and NAFLD in generally healthy adults.
Methods
The subjects who visited the Seoul National University Hospital for health checkup between 2005 and 2015 were included. Men aged more than 40 and postmenopausal women were included. Lumbar spine and femoral neck (FN) BMD were measured using dual-energy X-ray absorptiometry. Liver ultrasonography was conducted to evaluate the extent of fatty changes. After excluding subjects with a secondary cause of liver disease such as heavy drinking or viral hepatitis, multivariable linear regression analysis adjusted for possible cofactors was performed to investigate the association between BMD and NAFLD.
Results
A total of 6634 subjects was included in this study (men:women = 3306:3328). Multivariate regression analysis revealed a significant negative association between FN BMD and NAFLD in men (β = −0.013, p = 0.029). However, there was a positive correlation between lumbar spine BMD and NAFLD in postmenopausal women (β = 0.022, p = 0.005).
Conclusions
Moderate or severe NAFLD exerted a detrimental effect on FN BMD in men. However, moderate or severe NAFLD had a positive effect on lumbar spine BMD in postmenopausal women. Potential sex-specific differences of the effect of NAFLD on BMD need to be elucidated further.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Nonalcoholic fatty liver disease (NAFLD) is one of the most common clinical disorders of the liver that can manifest as mild steatosis or nonalcoholic steatohepatitis and progress to end-stage liver disease with cirrhosis and hepatocellular carcinoma [1, 2]. Some studies indicated a possible association between NAFLD and clinical diseases, such as diabetes, cardiovascular disease, and chronic kidney disease [3–5]. Moreover, NAFLD is associated with central obesity, which is a component of metabolic syndrome (MetS) [6, 7]. These findings provide evidence that NAFLD is a hepatic manifestation of MetS, which is a cluster of risk factors for cardiovascular diseases, including central obesity, dyslipidemia, hypertension, and impaired glucose tolerance [8]. Recently, studies have determined that the risk of osteoporosis, characterized by decreased bone mineral density (BMD), is higher in subjects with MetS [9–12].
These associations have led to a concern about the relationship between NAFLD and osteoporosis. However, the association has not been consistent across studies [13–17]. In addition, the results of these studies might not be generalizable because of critical limitations, such as the small sample sizes [13, 14, 18–20], insufficient consideration of cofactors that could affect BMD (e.g., waist circumference, physical activity, inflammatory markers), and inclusion of a single sex [13, 14]. Moreover, as BMDs were not measured in multiple sites, the associations between NAFLD and BMDs of the femoral neck (FN) and lumbar spine could not be compared between studies [13]. Because most of these studies used ultrasonography to diagnose NAFLD, which does not provide information regarding the severity of liver steatosis, we evaluated the severity of fatty change in the present study using a four-point scale: normal (grade 0), mild (grade 1), moderate (grade 2), and severe (grade 3).
In this study, we aimed to investigate the association between NAFLD, with consideration of the level of steatosis, and lumbar spine and FN BMDs, using data from generally healthy adults and including various possible cofactors.
Methods
Subjects
In this study, 19,993 subjects who visited Seoul National University Hospital to undergo a health checkup, dual-energy X-ray absorptiometry (DXA), and abdominal ultrasonography between December 1, 2005, and March 31, 2015, were included. We initially chose to include adults aged >40 years. However, we considered that menopause is a major determinant of BMD [20, 22]. As a questionnaire for the assessment of menopause was not available for all women, we substituted being menopausal for age ≥55 years in defining subjects at the postmenopausal stage, by considering the trend of the ages at menopause in the general population [23, 24]. Finally, 3306 male and 3328 female subjects were included in this study (Fig. 1).
The subjects without high-sensitivity C-reactive protein (HSCRP) data were excluded. Those who did not answer questions about their current drinking and smoking statuses or physical activities were also excluded. In particular, those who did not provide a response for alcohol consumption were excluded, because NAFLD and non-NAFLD could not be distinguished in these subjects. Subjects with any evidence of chronic viral liver disease, cholestasis, cirrhosis, or malignancy were excluded. In addition, we decided to use the latest BMD results in the examinees who underwent repeated DXA.
Smoking habit was divided into two categories as follows: (1) current smoker and (2) nonsmoker or ex-smoker. Information on the type, amount, and frequency of alcohol consumption was collected. Based on the alcohol content of the beverages reported, the mean daily alcohol consumption was calculated and expressed in grams per week. Physical activity at leisure time was estimated using the short form of the International Physical Activity Questionnaire, by adding questions on the frequency and duration of moderate and vigorous activities and walking. The subjects were divided into either the exercise or nonexercise group. The exercise group included subjects who exercised moderately for >150 min/week or those who exercised intensively for >75 min/week [25].
This study was approved by the Seoul National University Hospital Institutional Review Board. It was designed as a retrospective, cross-sectional study, and data were obtained by reviewing hospital records.
Anthropometric measurements
Body mass index (BMI) was calculated by dividing weight by the square of height (kg/m2). Waist circumference (WC) was measured horizontally at the level of the umbilicus. Prior to measuring blood pressure (BP), the subjects were asked to rest for 5 min.
Serum biomarkers
After overnight fasting, serum was collected for measurement of biochemical markers, including total cholesterol (TC), triglyceride (TG), high-density lipoprotein (HDL), low-density lipoprotein (LDL), and fasting plasma glucose (FPG) levels. Alanine aminotransferase (ALT), aspartate aminotransferase (AST), and γ-glutamyltranspeptidase (γ-GTP) were measured using standard biochemical methods. Patients were divided into low-, moderate-, and high-risk groups according to HSCRP levels on the basis of the following cutoff points: >1, 1–3, and >3.0 mg/L, respectively. Glomerular filtration rate (GFR) was estimated using the Modification of Diet in Renal Disease (MDRD) formula: GFR = 186 × serum creatinine−1.154 × age−0.203 × 0.742 (for females). Using the chronic kidney function categorization of the US National Kidney Foundation, renal function was classified according to estimated GFR (eGFR) as follows: normal renal function (≥90 mL/min/1.73 m2), mild renal dysfunction (60–89.9 mL/min/1.73 m2), moderate renal dysfunction (30–59.9 mL/min/1.73 m2), severe renal dysfunction (15–29.9 mL/min/1.73 m2), and kidney failure (<15 mL/min/1.73 m2) [26].
Definition of MetS
MetS was defined according to the American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement (AHA/NHLBI) criteria for Asians [21]. For the diagnosis of MetS, three or more of the following criteria must be fulfilled: WC ≥90 cm in men and ≥80 cm in women, fasting TG ≥150 mg/dL or use of lipid-lowering medication, HDL <40 mg/dL in men and <50 mg/dL in women or use of medication, BP ≥130/85 mmHg or use of antihypertensive medication, and FPG ≥100 mg/dL or current use of anti-diabetes medication.
DXA for lumbar spine and FN BMDs
BMDs (g/cm2) at the lumbar spine and FN were measured using DXA (Lunar Prodigy Advance; General Electric Medical Systems, Milwaukee, WI, USA).
Liver ultrasonography and criteria for NAFLD
NAFLD was diagnosed based on ultrasonographic evidence of hepatic steatosis, such as a bright hepatic echo pattern, loss of intrahepatic architecture, and increased echo attenuation. According to ultrasonographic appearance, grades 0, 1, 2, and 3 indicated normal, mild, moderate, and severe changes, respectively. The subjects were divided into two groups as follows: group 1 included grades 0 (normal) and 1 (mild), and group 2 included grades 2 (moderate) and 3 (severe).
NAFLD was defined as definite hepatic steatosis on ultrasonography without a secondary cause including significant alcohol abuse (>210 g/week for men and >140 g/week for women) [26], any evidence of chronic viral liver disease, and other metabolic liver diseases. Liver ultrasonography was conducted with a 4-MHz probe and evaluated by board certified radiologists.
Statistical analysis
All analyses were performed using Stata version 14.0 (StataCorp., College Station, TX) For each baseline variable, according to sex, we performed the t test for continuous variables and the Chi-square test for categorical variables. To evaluate the association between NAFLD and BMD, factors with p values <0.05 in the univariate analysis were included in the subsequent linear regression analysis. First, unadjusted linear regression analyses were conducted to assess the association between each factor and the lumbar spine and FN BMDs. Then, multivariate linear regression analysis was conducted to assess the association between NAFLD and BMD after adjusting for the significant factors. Multiple regression analysis was performed with the mean lumbar spine and FN BMDs as dependent variables and two groups of NAFLD (groups 1 and 2) as the independent variables. Group 1 consisted of patients with a normal or mildly fatty liver on ultrasonography, and group 2 consisted of patients with advanced fatty liver on ultrasonography.
The analyses were adjusted for age, BMI, smoking status, alcohol consumption status, and ALT level, which were considered in light of the findings of previous studies (model 1). In addition, model 2 was adjusted for WC, HSCRP, and physical activity. Finally, model 3 was adjusted for diastolic blood pressure (DBP), FPG, HDL level, and MDRD-GFR, which were statistically significant variables in the univariate regression analysis. The BMD trend according to NAFLD was evaluated using the p values from the trend test.
Results
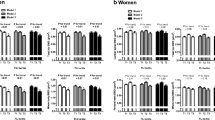
The general characteristics of the subjects are presented in Table 1. In both sexes, the NAFLD group had higher mean body weight, BMI, WC, SBP, DBP, FPG level, TC level, TG level, AST level, ALT level, and lumbar spine and FN BMDs than the non-NAFLD group (p < 0.05), but the non-NAFLD group had significantly higher HDL levels than the NAFLD group (p < 0.05, Table 1). Among the subjects, the men were younger and had significantly higher weight, height, BMI, WC, systolic blood pressure (SBP), DBP, TG level, FPG level, AST level, ALT level, γ-GTP level, and BMD in the lumbar spine and FN, but lower serum TC, HDL, and LDL levels and eGFR. Ultrasonographic results, serum HSCRP level, smoking and alcohol consumption statuses, and physical activity significantly differed between the men and women (Table S1).
The results of the univariate regression analyses are listed in Table S2. In both men and women, NAFLD was significantly correlated with lumbar spine BMD (β = 0.05; 95 % confidence interval [CI], 0.041–0.060; p < 0.001) and FN BMD (β coefficient = 0.03; 95 % CI, 0.020–0.032; p < 0.001). Age, body weight, height, BMI, WC, DBP, and FPG, TC, TG, γ-GTP, AST, and ALT levels were also associated with BMD.
Subgroup analyses according to both sex and severity of fatty liver were performed in group 1 (grades 0 and 1). BMD did not differ significantly between the patients with and without mild NAFLD (Table S3). However, among the patients with NAFLD in group 2 (moderate and severe steatosis), the men had lower FN BMDs (β = −0.013; 95 % CI, −0.024 to −0.001; p = 0.029), and the women had higher mean lumbar spine BMDs (β = 0.022; 95 % CI, 0.007–0.037; p = 0.005) than the patients in group 1 (Table 2). The result of the subgroup analysis performed for women who responded as being menopausal was consistent with the results of the analysis for the postmenopausal women (aged ≥55 years; Table S4).
Discussion
The results of the present analyses show a significant difference in the FN BMDs of men between groups 1 and 2 group after controlling for additional variables (β = −0.013, p = 0.029). In contrast, a positive correlation was found between lumbar spine BMD and NAFLD in postmenopausal women (β = 0.022, p = 0.005), which is not consistent with previous findings [13, 14].
We can conclude that mild liver steatosis on ultrasonography does not affect BMD. However, advanced NAFLD was associated with BMD. Purnak et al. [18] showed that, although simple steatosis was not associated with decreased BMD, the presence of elevated serum ALT and HSCRP levels, which are indicators of nonalcoholic steatohepatitis, was associated with lower BMD.
Furthermore, although ultrasonography is an established technique for screening patients at risk of NAFLD, it has low accuracy and operator dependency in detecting mild steatosis but has acceptable sensitivity and specificity in detecting moderate-to-severe hepatic steatosis [22]. For patients without chronic liver disease, ultrasonography offers a reasonably accurate diagnosis of moderate-to-severe liver steatosis, with a reported sensitivity ranging from 81.8 to 100.0 % and a specificity as high as 98 % [22].
In our study, we found a negative association between NAFLD and FN BMD in men, consistent with previously reported results, but a positive association between NAFLD and lumbar spine BMD. Previous studies observed a sex-related difference in the association between NAFLD and BMD [14, 23, 24]. Potential explanations for this sex-related difference include features of age-related osteoporosis [25, 26], body fat deposition [27], a tendency to fall, and sex hormone levels.
In the present study, although NAFLD in women did not appear to have any effect on FN BMD, the results showed a positive correlation between NAFLD and lumbar spine BMD. According to the results of previous studies, central body fat distribution was associated with spinal BMD, but not with FN BMD [28, 29]. Saarelainen et al. [28] suggested that irrespective of the use of hormone replacement therapy (HRT), higher trunk fat mass is positively associated with spinal BMD but not with hip BMD in postmenopausal women. Kirchengast et al. [30] found that central or upper body fat distribution did not affect hip BMD. These findings suggest that upper body fat can hinder spinal bone loss and is mainly associated with higher lumbar spine BMD irrespective of HRT. In addition, the lumbar spine had a much higher relative proportion (60–95 %) of metabolically active and hormonally more sensitive trabecular bone than the FN (25 %) [31, 32].
Although many preceding studies have been conducted, the pathophysiological associations between NAFLD and BMD have not been completely clarified. However, identification of the molecular pathways and mechanisms that link these two disorders is of great importance because the development of preventive and pharmacological approaches for these disorders may be warranted [15].
The precise mechanisms that have been identified include insulin resistance and inflammation. Excess accumulation of adipose tissue in the liver increases the release of free fatty acids from adipocytes, which may be a main factor in the modulation of insulin sensitivity [33]. Insulin resistance and an inflammatory response are of critical importance for inducing NAFLD [34]. Prior studies indicate that insulin levels and/or insulin resistance is associated with BMD [35, 36]. Many factors promote inflammation, including the presence of pro-inflammatory cytokines, adipokines, mitochondrial dysfunction, oxidative stress, and subsequent lipid peroxidation. When accumulated in the mitochondria, free fatty acids and cholesterol are considered the “aggressive” lipids that lead to tumor necrosis factor alpha (TNF-α)-mediated liver damage and reactive oxygen species formation. These lipids could also exist in a nonsteatotic liver and act as early “inflammatory” hits that lead to NAFLD pathologies [37]. Furthermore, TNF-α increases the expression levels of genes that amplify osteoclastogenesis and decrease the expression levels of genes that are involved in bone formation [38]. In addition, recent evidence indicates that an elevated serum HSCRP level is an independent risk factor for NAFLD [34, 39], and the ALT level has been used as a marker of NAFLD [40]. Many previous studies showed that these pro-inflammatory chemokines and cytokines contribute to bone metabolism [14]. However, in the present study, the correlation analysis did not reveal a significant relationship between BMD and inflammatory markers such as HSCRP and ALT levels. Future studies are needed to clarify the underlying mechanism.
In this study, the associations observed differed from those demonstrated by previous research, likely because previous studies did not adjust for many of the confounding factors that were included in the present study and consisted of healthy old people who underwent health screening. While the sample size of most previous studies was relatively small, the present study had a large sample size of a generally healthy population with normal biochemical and metabolic profiles, which might allow for generalization to the Korean population.
This study had some limitations. First, hepatic biopsy data were not available for our participants, and NAFLD was diagnosed according to the presence of hepatic steatosis on ultrasonography. However, although liver biopsy is the gold standard for confirming NAFLD, ultrasonographic examination is the most widely used modality to detect hepatic steatosis. Moreover, it has been suggested to have high sensitivity (89 %) and specificity (93 %) for the prediction of liver histology [41]. Second, bone metabolism could be influenced by many undetected confounding factors. Although the present study considered many additional factors that were not evaluated in previous studies, including physical activity, inflammatory markers, and eGFR, undetected confounding factors that contribute to osteoporosis such as the use of corticosteroids, calcium/vitamin D intake, and use of HRT could not be ruled out [42, 43]. Finally, owing to the cross-sectional nature of the present study, incidental correlations could not be completely excluded. Longitudinal studies are needed to clarify their precise interrelationships.
In conclusion, the results of this analysis showed a significant difference in BMD between patients with moderate or severe NAFLD and those with normal or mild NAFLD, after adjusting for possible confounding factors. Potential sex-specific differences in the effect of NAFLD on BMD need to be elucidated further, and additional studies are needed to clarify the correlation between NAFLD and BMD.
References
Bugianesi E, Leone N, Vanni E, Marchesini G, Brunello F, Carucci P, Musso A, De Paolis P, Capussotti L, Salizzoni M, Rizzetto M (2002) Expanding the natural history of nonalcoholic steatohepatitis: from cryptogenic cirrhosis to hepatocellular carcinoma. Gastroenterology 123:134–140
White DL, Kanwal F, El-Serag HB (2012) Association between nonalcoholic fatty liver disease and risk for hepatocellular cancer, based on systematic review. Clin Gastroenterol Hepatol 10(1342–1359):e2
Adams LA, Waters OR, Knuiman MW, Elliott RR, Olynyk JK (2009) NAFLD as a risk factor for the development of diabetes and the metabolic syndrome: an eleven-year follow-up study. Am J Gastroenterol 104:861–867
Zhang QQ, Lu LG (2015) Nonalcoholic fatty liver disease: dyslipidemia, risk for cardiovascular complications, and treatment strategy. J Clin Transl Hepatol 3:78–84
Orlic L, Mikolasevic I, Bagic Z, Racki S, Stimac D, Milic S (2014) Chronic kidney disease and nonalcoholic fatty liver disease-is there a link? Gastroenterol Res Pract 2014:847539
Lopez-Velazquez JA, Silva-Vidal KV, Ponciano-Rodriguez G, Chavez-Tapia NC, Arrese M, Uribe M, Mendez-Sanchez N (2014) The prevalence of nonalcoholic fatty liver disease in the Americas. Ann Hepatol 13:166–178
Carr DB, Utzschneider KM, Hull RL, Kodama K, Retzlaff BM, Brunzell JD, Shofer JB, Fish BE, Knopp RH, Kahn SE (2004) Intra-abdominal fat is a major determinant of the National Cholesterol Education Program Adult Treatment Panel III criteria for the metabolic syndrome. Diabetes 53:2087–2094
Lonardo A, Ballestri S, Marchesini G, Angulo P, Loria P (2015) Nonalcoholic fatty liver disease: a precursor of the metabolic syndrome. Dig Liver Dis 47:181–190
von Muhlen D, Safii S, Jassal SK, Svartberg J, Barrett-Connor E (2007) Associations between the metabolic syndrome and bone health in older men and women: the Rancho Bernardo Study. Osteoporos Int 18:1337–1344
Jeon YK, Lee JG, Kim SS, Kim BH, Kim SJ, Kim YK, Kim IJ (2011) Association between bone mineral density and metabolic syndrome in pre- and postmenopausal women. Endocr J 58:87–93
Hwang DK, Choi HJ (2010) The relationship between low bone mass and metabolic syndrome in Korean women. Osteoporos Int 21:425–431
Kim H, Oh HJ, Choi H, Choi WH, Lim SK, Kim JG (2013) The association between bone mineral density and metabolic syndrome: a Korean population-based study. J Bone Miner Metab 31:571–578
Moon SS, Lee YS, Kim SW (2012) Association of nonalcoholic fatty liver disease with low bone mass in postmenopausal women. Endocrine 42:423–429
Cui R, Sheng H, Rui XF, Cheng XY, Sheng CJ, Wang JY, Qu S (2013) Low bone mineral density in Chinese adults with nonalcoholic fatty liver disease. Int J Endocrinol 2013:396545
Targher G, Lonardo A, Rossini M (2015) Nonalcoholic fatty liver disease and decreased bone mineral density: is there a link? J Endocrinol Invest 38:817–825
Upala S, Sanguankeo A, Jaruvongvanich V (2015) Association between nonalcoholic fatty liver disease and bone mineral density: a systematic review and meta-analysis. J Endocrinol Invest 38:931–932
Bhatt SP, Nigam P, Misra A, Guleria R, Qadar Pasha MA (2013) Independent associations of low 25 hydroxy vitamin D and high parathyroid hormonal levels with nonalcoholic fatty liver disease in Asian Indians residing in north India. Atherosclerosis 230:157–163
Purnak T, Beyazit Y, Ozaslan E, Efe C, Hayretci M (2012) The evaluation of bone mineral density in patients with nonalcoholic fatty liver disease. Wien Klin Wochenschr 124:526–531
Pirgon O, Bilgin H, Tolu I, Odabas D (2011) Correlation of insulin sensitivity with bone mineral status in obese adolescents with nonalcoholic fatty liver disease. Clin Endocrinol (Oxf) 75:189–195
Campos RM, de Piano A, da Silva PL, Carnier J, Sanches PL, Corqosinho FC, Masquio DC, Lazaretti-Castro M, Oyama LM, Nascimento CM, Tock L, de Mello MT, Tufik S, Damaso AR (2012) The role of pro/anti-inflammatory adipokines on bone metabolism in NAFLD obese adolescents: effects of long-term interdisciplinary therapy. Endocrine 42:146–156
Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA, Gordon DJ, Krauss RM, Savage PJ, Smith SC, Spertus JA, Costa F (2005) Diagnosis and management of the metabolic syndrome: an American heart association/national heart, lung, and blood institute scientific statement. Circulation 112:2735–2752
Lee SS, Park SH (2014) Radiologic evaluation of nonalcoholic fatty liver disease. World J Gastroenterol 20:7392–7402
Li M, Xu Y, Xu M, Ma L, Wang T, Liu Y, Dai M, Chen Y, Lu J, Liu J, Bi Y, Ning G (2012) Association between nonalcoholic fatty liver disease (NAFLD) and osteoporotic fracture in middle-aged and elderly Chinese. J Clin Endocrinol Metab 97:2033–2038
Xia MF, Lin HD, Yan HM, Bian H, Chang XX, Zhang LS, He WY, Gao X (2016) The association of liver fat content and serum alanine aminotransferase with bone mineral density in middle-aged and elderly Chinese men and postmenopausal women. J Transl Med 14:11
Foger-Samwald U, Patsch JM, Schamall D, Alaghebandan A, Deutschmann J, Salem S, Mousavi M, Pietschmann P (2014) Molecular evidence of osteoblast dysfunction in elderly men with osteoporotic hip fractures. Exp Gerontol 57:114–121
Oursler MJ, Osdoby P, Pyfferoen J, Riggs BL, Spelsberg TC (1991) Avian osteoclasts as estrogen target cells. Proc Natl Acad Sci U S A 88:6613–6617
Franklin RM, Ploutz-Snyder L, Kanaley JA (2009) Longitudinal changes in abdominal fat distribution with menopause. Metabolism 58:311–315
Saarelainen J, Honkanen R, Kroger H, Tuppurainen M, Jurvelin JS, Niskanen L (2011) Body fat distribution is associated with lumbar spine bone density independently of body weight in postmenopausal women. Maturitas 69:86–90
Zillikens MC, Uitterlinden AG, van Leeuwen JP, Berends AL, Henneman P, van Dijk KW, Oostra BA, van Duijn CM, Pols HA, Rivadeneira F (2010) The role of body mass index, insulin, and adiponectin in the relation between fat distribution and bone mineral density. Calcif Tissue Int 86:116–125
Kirchengast S, Peterson B, Hauser G, Knogler W (2001) Body composition characteristics are associated with the bone density of the proximal femur end in middle- and old-aged women and men. Maturitas 39:133–145
Riggs BL, Wahner HW, Seeman E, Offord KP, Dunn WL, Mazess RB, Johnson KA, Melton LJ 3rd (1982) Changes in bone mineral density of the proximal femur and spine with aging. Differences between the postmenopausal and senile osteoporosis syndromes. J Clin Invest 70:716–723
Wells G, Tugwell P, Shea B, Guyatt G, Peterson J, Zytaruk N, Robinson V, Henry D, O’Connell D, cranney A, Osteoporosis Methodology Group and The Osteoporosis Research Advisory Group (2002) Meta-analyses of therapies for postmenopausal osteoporosis. V. Meta-analysis of the efficacy of hormone replacement therapy in treating and preventing osteoporosis in postmenopausal women. Endocr Rev 23:529–539
Perseghin G, Ghosh S, Gerow K, Shulman GI (1997) Metabolic defects in lean nondiabetic offspring of NIDDM parents: a cross-sectional study. Diabetes 46:1001–1009
Park SH, Kim BI, Yun JW, Kim JW, Park DI, Cho YK, Sung IK, Park CY, Sohn CI, Jeon WK, Kim H, Rhee EJ, Lee WY, Kim SW (2004) Insulin resistance and C-reactive protein as independent risk factors for non-alcoholic fatty liver disease in non-obese Asian men. J Gastroenterol Hepatol 19:694–698
Reid IR, Evans MC, Cooper GJ, Ames RW, Stapleton J (1993) Circulating insulin levels are related to bone density in normal postmenopausal women. Am J Physiol 265:E655–E659
Stolk RP, Van Daele PL, Pols HA, Burger H, Hofman A, Birkenhager JC, Lamberts SW, Grobbee DE (1996) Hyperinsulinemia and bone mineral density in an elderly population: the Rotterdam Study. Bone 18:545–549
Tilg H, Moschen AR (2010) Evolution of inflammation in nonalcoholic fatty liver disease: the multiple parallel hits hypothesis. Hepatology 52:1836–1846
Nanes MS (2003) Tumor necrosis factor-alpha: molecular and cellular mechanisms in skeletal pathology. Gene 321:1–15
Kogiso T, Moriyoshi Y, Shimizu S, Nagahara H, Shiratori K (2009) High-sensitivity C-reactive protein as a serum predictor of nonalcoholic fatty liver disease based on the Akaike Information Criterion scoring system in the general Japanese population. J Gastroenterol 44:313–321
Schindhelm RK, Diamant M, Dekker JM, Tushuizen ME, Teerlink T, Heine RJ (2006) Alanine aminotransferase as a marker of non-alcoholic fatty liver disease in relation to type 2 diabetes mellitus and cardiovascular disease. Diabetes Metab Res Rev 22:437–443
Joseph AE, Saverymuttu SH, Al-Sam S, Cook MG, Maxwell JD (1991) Comparison of liver histology with ultrasonography in assessing diffuse parenchymal liver disease. Clin Radiol 43:26–31
Reid IR (2015) Effects of vitamin D supplements on bone density. J Endocrinol Invest 38:91–94
Romagnoli E, Carnevale V, Biondi P, Minisola S (2014) Vitamin D supplementation: when and how? J Endocrinol Invest 37:603–607
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants (that were performed by any of the authors of this article) were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
No informed consent.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lee, S.H., Yun, J.M., Kim, S.H. et al. Association between bone mineral density and nonalcoholic fatty liver disease in Korean adults. J Endocrinol Invest 39, 1329–1336 (2016). https://doi.org/10.1007/s40618-016-0528-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-016-0528-3