Abstract
Purpose
Down-regulation of thyroid hormone receptor beta (THRβ) gene has been described in several human malignancies, including thyroid cancer. In this study, we analyzed THRβ mRNA expression in surgical specimens from a series of human papillary thyroid carcinomas (PTCs), characterized by their genotypic and clinical–biological features.
Methods
Thirty-six PTCs were divided into two groups according to the 2009 American Thyroid Association risk classification (17 low, 19 intermediate), and each group was divided into subgroups based on the presence or absence of the BRAFV600E mutation (21 BRAF mutated, 15 BRAF wild type). Gene expression was analyzed using fluidic cards containing probes and primers specific for the THRβ gene, as well as for genes of thyroperoxidase (TPO), sodium/iodide symporter (NIS), thyroglobulin (Tg) and thyroid stimulating hormone receptor (TSH-R) and for some miRNAs involved in thyroid neoplasia and targeting THRβ. The mRNA levels of each tumor tissue were compared with their correspondent normal counterpart.
Results
THRβ transcript was down-regulated in all PTCs examined. No significant differences were found between intermediate- vs low-risk PTCs patients, and BRAF-mutated vs BRAF wild-type groups. THRβ expression was directly correlated with NIS, TPO, Tg and TSH-R, and inversely correlated to miR-21, -146a, -181a and -221 expression.
Conclusions
Our results demonstrate that down-regulation of THRβ is a common feature of PTCs. While it is not associated with a more aggressive phenotype of PTC, it correlates with the reduction of all the markers of differentiation and is associated with overexpression of some miRNAs supposed to play a role in thyroid tumorigenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Thyroid hormone receptors (THRs) mediate the biological activities of the thyroid hormones in development, growth, differentiation and metabolism [1, 2]. Detection of alterations in the expression levels and/or integrity of THR genes in many neoplasms has made the analysis of these genes in human cancers an area of considerable interest. Several alterations have been described, including hypermethylation in breast cancer [3, 4], altered splicing in hepatocellular cancer [5] and loss of heterozygosity/deletions in breast, lung and melanoma cancer [2, 6–8], all resulting in reduced/lost expression of THR in tumor cells. Moreover, Martinez-Iglesias et al. have shown that THRβ1 re-expression in hepatocarcinoma and breast cancer cells was able to reduce tumor growth, enhancing expression of epithelial markers and diminishing that of the mesenchymal marker vimentin [9]. Gene mutations, small deletions and variations in the THR RNA and protein levels [10] have also been reported in thyroid cancers, in which a role of THRβ1 as potential suppressor of thyroid tumorigenesis has been proposed [11].
In the last years, miRNA expression profiling of human tumors has permitted to identify signatures associated with the diagnosis, staging, prognosis and response to treatment [12] and several studies have demonstrated that up-regulation of oncogenic miRNAs or down-regulation of miRNAs functioning as tumor suppressors is associated with carcinogenesis [13, 14]. Many groups have analyzed the expression of miRNAs in thyroid neoplasia and have shown an altered regulation of several miRNAs, proposing a role for some of them in papillary thyroid cancer (PTC) tumorigenesis [reviewed in 15, 16]. Noteworthy, a subset of miRNAs that are up-regulated in PTC tumors (miR-21, miR-146a, miR-181a and miR-221) has been described to target and to inhibit the expression of THRβ [17].
In this work, we have examined 36 PTCs, well characterized in their clinical–biological properties and genotypic alterations, to study THRβ expression and its correlation with the degree of aggressiveness, the presence of BRAF oncogene activating mutation and the expression of markers of thyrocyte differentiation thyroperoxidase (TPO), sodium/iodide symporter (NIS), thyroglobulin (Tg) and thyroid stimulating hormone receptor (TSH-R). Moreover, in the same tumors, we analyzed the expression levels of miRNAs targeting THRβ.
Materials and methods
Patients and tissues
Thirty-six patients with sporadic PTCs have been enrolled at the University Hospital of Rome, Sapienza. For each patient, a sample of thyroid tumor tissue and contralateral non-tumor (normal) tissue were collected immediately after thyroidectomy, snap-frozen and stored in liquid nitrogen. All samples were reviewed by a single pathologist, who confirmed the diagnosis of PTC, identified the histological variant of the tumor and evaluated the percentage of tumor cells (all tumor tissues selected had a percentage of tumor cells higher than 60 %). Clinical data were collected by retrospective review of hospital charts, and tumors were staged according to the criteria of the AJCC/UICC TNM classification, 7th edition [18]. The 36 cases were risk-stratified on the basis of clinical and histological data in accordance with the 2009 American Thyroid Association (ATA) risk of recurrence staging system [19]. The study was approved by the local medical ethics committee and written informed consent was obtained from all patients whose tissues were analyzed.
Mutational analysis of BRAF
The mutational status of BRAF was analyzed by direct sequencing in cDNA samples of tumor tissues. The exon 15 of BRAF was amplified by PCR (Table S1) and the products sequenced with the BigDye Terminator version 3.1 Cycle Sequencing kit in an automated 3130xl analyzer (Life Technologies, Foster City, CA, USA). All PCR and sequencing reactions were repeated at least twice to confirm the presence of the mutation V600E.
RNA isolation from thyroid tissues and reverse transcription
Total RNA was extracted from tissue samples using Trizol reagent (Life Technologies) [20] according to the manufacturer’s instructions. RNA concentration was measured by a NanoDrop Spectrophotometer (Thermo Fisher Scientific, Inc., Waltham, MA, USA). First-strand cDNA synthesis was performed following the protocol provided with the High Capacity cDNA Reverse Transcription kit (Life Technologies), as previously described [21].
Gene expression analysis
In the screening step, mRNA levels of THRβ, NIS, TPO, Tg and TSH-R genes were assessed in thyroid tissues by real-time PCR using custom Taqman Low Density Arrays (TLDA, Life Technologies). Each TLDA was configured with specific predesigned assays (TaqMan Gene Expression Assays, Life Technologies) and four housekeeping genes (Glyceraldehyde-3-Phosphate Dehydrogenase; Beta-actin; Hypoxanthine Phosphoribosyltransferase 1 and Beta-2 microglobulin) were included to normalize RNA expression levels. The TaqMan arrays were set up as previously described [22] and all the PCR reactions were performed on a 7900 HT Fast Real-time PCR System (Life Technologies). Ct values were calculated with SDS 2.4 software (Life Technologies) and data analysis was carried out using RQ Manager 1.2.1 software (Life Technologies). Beta-actin was chosen as endogenous control because of its least variance among samples. Final results were determined by the comparative 2−ΔΔCt method and expressed as relative expression normalized to a calibrator sample.
miRNA expression analysis
TaqMan® Array Human MicroRNA Card Set v3.0 (Life Technologies) was used to evaluate the expression levels of miR-21, miR-146a, miR-181a and miR-221. Total RNA (500 ng) was reverse transcribed using high-capacity cDNA reverse transcription kit (Life Technologies) and MegaplexTM RT primer pool (Life Technologies). Real-time PCR was performed on a 7900 HT Fast Real-Time PCR System (Life Technologies). Ct values were calculated with SDS 2.4 software (Life Technologies) and data analysis was carried out using Expression Suite v1.0.3 (Life Technologies). U6 was chosen as endogenous control due to its least variance among samples. The relative level of miRNA expression was calculated by the comparative 2−ΔΔCt method using Expression Suite v1.0.3 (Life Technologies).
Statistical analysis
Statistical analysis was carried out using GraphPad Prism version 5.0 statistical software (GraphPad Software Inc., San Diego, CA, USA). Real-time PCR results are expressed as mean ± standard deviation (SD). Mann–Whitney test and Student’s t test were used to evaluate intergroup differences. Correlations between quantitative variables were analyzed by the Spearman rho rank correlation coefficient. p values lower than 0.05 were considered statistically significant.
Results
Clinical and pathological features
We examined 36 tissues from patients with apparently sporadic PTC. They included 17 cases with a low risk of recurrence, and 19 with an intermediate risk based on the 2009 ATA risk stratification system. Table 1 summarizes the characteristics of study population at the time of the primary treatment, which consisted in total or near total thyroidectomy, with or without radioactive iodine remnant ablation. Among the low-risk patients and those at intermediate risk, 7 (41.1 %) and 14 (73.7 %), respectively, carry the BRAF V600E mutation (Fig. 1).
Expression of THRβ and correlation with thyroid-specific genes in PTCs
Analysis of mRNA showed that expression levels of THRβ were lower in tumor tissues than in the normal counterpart tissues (Normal tissues = 1 ± 0.536, Tumor tissues = 0.618 ± 0.434, p = 0.0021) (Fig. 2). By comparison of the subgroups, no significant deregulation was found between low-risk PTCs and intermediate-risk PTCs (Fig. 2), as well as between BRAF V600E PTCs and BRAF wild-type PTCs (Fig. 2). The expression of THRβ was then compared to mRNA levels of the thyroid-specific genes NIS, TPO, Tg and TSH-R. A statistically significant and direct correlation with THRβ levels was detected for all of the thyrocyte-specific genes examined (Table 2). In addition, as reported in Fig. 3, NIS mRNA levels showed the major significant reduction and TSH-R the minor. Moreover, expression levels of TPO were significantly lower in PTC with intermediate risk and in BRAF V600E PTCs (Table S2). No significant deregulation was found for NIS, Tg and TSH-R (Table S2).
Expression of THRβ in human PTCs. Expression levels of THRβ in tumor tissues are lower than corresponding normal. No significant differences were found between the PTCs at ATA intermediate risk vs low risk of recurrence, and BRAF V600E vs BRAF wild-type PTCs. Data represent the mean ± standard deviation. p value was obtained by Mann–Whitney test. **0.001 < p < 0.01. ns not significant
Expression of miRNAs in PTC tissues
Twenty-one PTC tissues of the present cohort were also analyzed for the expression level of a subset of miRNA previously predicted to target THRβ (miR-21, miR-146a, miR-181a and miR-221) [22]. Expression levels of miR-21, miR-181a and miR-221 resulted significantly higher in tumor tissues compared to normal tissues (Table S3). According to ATA risk and BRAF mutational status, no significant deregulation was found (Table S3).
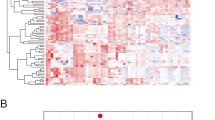
As reported in Fig. 4, a higher expression of miR-21, miR-146a, miR-181a and miR-221 was observed in almost all those tumor tissues displaying lower levels of THRβ. However, Spearman correlation of miRNA and THRβ data did not show a statistically significant association (data not shown). miRNA expression levels were then compared with those of thyroid-specific genes NIS, TPO, Tg and TSH-R. As shown in Fig. S1, a statistically significant and inverse correlation was found between expression levels of TG and both miR-21 and miR-146a, and between TPO and miR-21.
Discussion
In the last two decades, the incidence of thyroid cancer, the most common malignancy in the endocrine system, has greatly increased [23] and about 80 % of all cases are represented by PTCs. Although most of these tumors present a good prognosis (survival rates of 90–95 % at 5 years), there is a minority of patients unresponsive to treatment based on association of surgery and radioactive iodine. The loss of differentiation of the transformed cells, and in particular the reduction/loss of expression of functioning NIS protein represents a major cause of lack of responsiveness to radioiodine treatment in case of recurrent/metastatic disease [24–27]. Several genetic and epigenetic alterations are involved in the loss of differentiation of PTCs and the acquisition of more aggressive phenotype [28–31]. Thus, elucidating the molecular mechanisms that contribute to dedifferentiation and aggressiveness of PTCs may help to tailor diagnostic and therapeutic strategies and to propose novel targeted therapy approaches.
Recent investigations showed that alterations causing a marked impairment of the THR expression and function can influence the process of thyroid tumorigenesis [10, 32]. By analyzing the expression of THRβ in 17 PTCs, Kim et al. observed a significant reduction of its mRNA expression levels in cancer tissues [10]. A functional role of THRβ was further supported by in vitro data in which reactivation of the silenced THRβ expression delayed thyroid tumor progression [10]. Moreover, Zhu et al. have demonstrated in a mouse model of metastatic follicular thyroid cancer that functional loss of THRβ and THRα gene promoted the development of thyroid carcinomas and metastasis, suggesting that THRs could function as a tumor suppressor in this experimental model [11]. In our study, analysis of THRβ expression was performed in a wider cohort of PTCs. In all 36 tumors examined, the transcript was down-regulated compared with the corresponding normal tissue. However, such as NIS, Tg and TSH-R, we did not find significant differences of THRβ mRNA levels by comparing the groups in terms of tumor extent and risk of having structural persistent/recurrent disease based on the 2009 ATA risk stratification staging system [19]. Thus, the reduced expression of THRβ may not be considered as a marker of aggressiveness, at least in this cohort of PTCs. This finding is also strengthened by the absence of significant differences in THRβ expression levels between the subgroups of tumors presenting the BRAF V600E mutation or not. BRAF V600E is the most common genetic alteration found in PTCs [33] and is associated with a reduced expression of the genes involved in iodide metabolism [34], the presence of worrisome clinicopathologic features, and a significantly higher risk of recurrence than BRAF wild-type tumors [30, 35].
In this series of PTCs, analysis of expression levels of thyroid-specific genes, which confirmed our previous finding regarding the presence of the lowest levels of NIS and the close to normal levels of TSH-R [21], revealed that THRβ expression was directly correlated with all the genes examined, suggesting for the loss of THR intra-thyroidal expression the behavior as a marker of differentiation.
It is now well established that disregulation of the profile of miRNAs expression occurs in a variety of malignancies, where they are emerging as oncogenes or tumor suppressor genes [12–14]. There are many reports about the expression of miRNAs in thyroid tumors [reviewed in 15, 16]. Interestingly, up-regulation of miR-21, miR-181a, miR-146a, and miR-221 has been described as an important mechanism of silencing of THRβ [17]. In our study, we found the upregulation of miR-21, miR-181a, miR-146a and miR-221 in all tumor tissues displaying low levels of THRβ. Although the correlation did not reach a statistical significance, the general trend confirms the results of Jazdzewski [17], suggesting that an up-regulation of these miRNAs might be responsible for the down-regulation of THRβ in PTCs. As for other thyroid-specific genes, a statistically significant and inverse correlation was found between expression levels of Tg and both miR-21 and miR-146a, and also between TPO and miR-21.
In conclusion, our findings demonstrate that a reduction of THRβ gene expression is a common feature of PTCs even if not associated with a more aggressive phenotype of the tumors. Moreover, it is directly correlated with the reduction of all the markers of differentiation and associated with overexpression of some miRNAs supposed to play a role in thyroid tumorigenesis. Overall, our results suggest that THRβ could represent an additional thyroid differentiation marker.
References
Cheng SY (2000) Multiple mechanisms for regulation of the transcriptional activity of thyroid hormone receptors. Rev Endocr Metab Disord 1:9–18
Kim WG, Cheng SY (2013) Thyroid hormone receptors and cancer. Biochim Biophys Acta 1830:3928–3936
Li Z, Meng ZH, Chandrasekaran R, Kuo WL, Collins CC, Gray JW, Diarkee SH (2002) Biallelic inactivation of the thyroid hormone receptor β1 gene in early stage breast cancer. Cancer Res 62:1939–1943
Ling Y, Xu X, Hao J, Ling X, Du X, Liu X, Zhao X (2010) Aberrant methylation of the THRB gene in tissue and plasma of breast cancer patients. Cancer Genet Cytogenet 196:140–145
Lin KH, Shieh HY, Chen SL, Hsu HC (1999) Expression of mutant thyroid hormone nuclear receptors in human hepatocellular carcinoma cells. Mol Carcinog 26:53–61
Futreal PA, Cochran C, Marks JR, Iglehart JD, Zimmerman W, Barret JC, Wiseman RW (1994) Mutation analysis of the THRA1 gene in breast cancer: deletion/fusion of the gene to a novel sequence on 17q in the BT474 cell line. Cancer Res 54:1791–1794
Dobrovic A, Houle B, Belouchi A, Bradley WE (1988) erbA-related genes coding for DNA-binding hormone receptors localized to chromosome 3p21-3p25 and deleted in small cell lung carcinoma. Cancer Res 48:682–685
Sisley K, Kurtis D, Rennie IG, Rees RC (1993) Loss of heterozygosity of the thyroid hormone receptor β in posterior uveal melanoma. Melanoma Res 3:457–461
Martinez-Iglesias O, Garcia-Silva S, Tenbaum SP, Regadera J, Larcher F, Paramio JM, Vennström B, Aranda A (2009) Thyroid hormone receptor β1 acts as a potent suppressor of tumor invasiveness and metastasis. Cancer Res 69(2):501–509
Kim WG, Zhu X, Kim DW, Zhang L, Kebebew E, Cheng SY (2013) Reactivation of the silenced thyroid hormone receptor β gene expression delays thyroid tumor progression. Endocrinology 154:25–35
Zhu XG, Zhao L, Willingham MC, Cheng SY (2010) Thyroid hormone receptors are tumor suppressors in a mouse model of metastatic follicular thyroid carcinoma. Oncogene 29:1909–1919
Lu J, Getz G, Miska EA, Alvarez-Saavedra E, Lamb J, Peck D, Sweet-Cordero A, Ebert BL, Mak RH, Fernando AA, Dowing JR, Jacks T, Horvitz HR, Golub TR (2005) MicroRNA expression profiles classify human cancers. Nature 435:834–838
Adams BD, Kasinski AL, Slack FJ (2014) Aberrant regulation and function of microRNAs in cancer. Curr Biol 24(16):R762–R776
Hayes J, Peruzzi PP, Lawler S (2014) MicroRNAs in cancer: biomarkers, functions and therapy. Trends Mol Med 20(8):460–469
Pallante P, Battista S, Pierantoni GM, Fusco A (2014) Deregulation of microRNA expression in thyroid neoplasias. Nat Rev Endocrinol 10:88–101
Dettmer MS, Perren A, Moch H, Komminoth P, Nikiforov YE, Nikiforova MN (2014) MicroRNA profile of poorly differentiated thyroid carcinomas–new diagnostic and prognostic insights. J Mol Endocrinol 52:181–189
Jazdzewski K, Boguslawska J, Jendrzejewski J, Liyanarachchi S, Pachucki J, Wardyn KA, Nauman A, De la Chapelle A (2011) Thyroid hormone receptor β (THRB) is a major target gene for microRNAs deregulated in papillary thyroid carcinoma (PTC). J Clin Endocrinol Metab 96:E546–E553
Edge SB, Compton CC (2010) The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol 17:1471–1474
Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, Mazzaferri EL, McIver B, Pacini F, Schlumberger M, Sherman SI, Steward DL, Tuttle RM (2009) Revised American thyroid association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
Sponziello M, Bruno R, Durante C, D’Agostino M, Corradino R, Giannasio P, Ciociola E, Ferretti E, Maranghi M, Verrienti A, De Toma G, Filetti S, Russo D (2011) Growth factor receptors gene expression and Akt phosphorylation in benign human thyroid nodules are unaffected by chronic thyrotropin suppression. Horm Metab Res 43:22–25
D’Agostino M, Sponziello M, Puppin C, Celano M, Maggisano V, Baldan F, Biffoni M, Bulotta S, Durante C, Filetti S, Damante G, Russo D (2014) Different expression of TSH receptor and NIS genes in thyroid cancer: role of epigenetics. J Mol Endocrinol 52:121–131
Sponziello M, Lavarone E, Pegolo E, Di Loreto C, Puppin C, Russo MA, Bruno R, Filetti S, Durante C, Russo D, Di Cristofano A, Damante G (2013) Molecular differences between human thyroid follicular adenoma and carcinoma revealed by analysis of a murine model of thyroid cancer. Endocrinology 154:3043–3053
Davies L, Welch HG (2014) Current thyroid cancer trends in the United States. JAMA Otolaryngol Head Neck Surg 140:317–322
Arturi F, Russo D, Giuffrida D, Schlumberger M, Filetti S (2000) Sodium-iodide symporter (NIS) gene expression in lymph-node metastases of papillary thyroid carcinomas. Eur J Endocrinol 143:623–627
Arturi F, Russo D, Bidart JM, Scarpelli D, Schlumberger M, Filetti S (2001) Expression pattern of the pendrin and sodium/iodide symporter genes in human thyroid carcinoma cell lines and human thyroid tumors. Eur J Endocrinol 145:129–135
Kogai T, Brent GA (2012) The sodium iodide symporter (NIS): regulation and approaches to targeting for cancer therapeutics. Pharmacol Ther 135:355–370
Schlumberger M, Lacroix L, Russo D, Filetti S, Bidart JM (2007) Defects in iodide metabolism in thyroid cancer and implications for the follow-up and treatment of patients. Nat Clin Pract Endocrinol Metab 3:260–269
Fagin JA, Mitsiades N (2008) Molecular pathology of thyroid cancer: diagnostic and clinical implications. Best Pract Res Clin Endocrinol Metab 22:955–969
Russo D, Damante G, Puxeddu E, Durante C, Filetti S (2011) Epigenetics of thyroid cancer and novel therapeutic targets. J Mol Endocrinol 46:R73–R81
Xing M (2013) Molecular pathogenesis and mechanisms of thyroid cancer. Nat Rev Cancer 13:184–199
Galrão AL, Sodré AK, Camargo RY, Friguglietti CU, Kulcsar MA, Lima EU, Medeiros-Neto G, Rubio IG (2013) Methylation levels of sodium-iodide symporter (NIS) promoter in benign and malignant thyroid tumors with reduced NIS expression. Endocrine 43:225–229
Puzianowska-Kuznicka M, Krystyniak A, Madej A, Cheng SY, Nauman J (2002) Functionally impaired TR mutants are present in thyroid papillary cancer. J Clin Endocrinol Metab 87(3):1120–1128
Ciampi R, Nikiforov YE (2005) Alterations of the BRAF gene in thyroid tumors. Endocr Pathol 16:163–172
Durante C, Puxeddu E, Ferretti E, Morisi R, Moretti S, Bruno R, Barbi F, Avenia N, Scipioni A, Verrienti A, Tosi E, Cavaliere A, Gulino A, Filetti S, Russo D (2007) BRAF mutations in papillary thyroid carcinomas inhibit genes involved in iodine metabolism. J Clin Endocrinol Metab 92(7):2840–2843
Puxeddu E, Durante C, Avenia N, Filetti S, Russo D (2008) Clinical implication of BRAF mutation in thyroid carcinoma. Trends Endocrinol Metab 19:138–145
Acknowledgments
This study was supported by the Fondazione Umberto Di Mario and by Banca d’Italia.
Conflict of interest
The authors declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
The authors declare that informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
F. Rosignolo and V. Maggisano equally contributed to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
40618_2015_309_MOESM1_ESM.ppt
Fig. S1 Correlation between miRNAs and thyroid-specific genes in human PTCs mRNA levels of TPO are significantly and inversely correlated to expression levels of miR-21 (a). mRNA levels of TG are significantly and inversely correlated to expression levels of miR-21 (b) and miR-146a (c). Correlations between miRNAs and thyroid-specific genes were analyzed by the Spearman rho rank correlation coefficient. Supplementary material 1 (PPT 248 kb)
Rights and permissions
About this article
Cite this article
Rosignolo, F., Maggisano, V., Sponziello, M. et al. Reduced expression of THRβ in papillary thyroid carcinomas: relationship with BRAF mutation, aggressiveness and miR expression. J Endocrinol Invest 38, 1283–1289 (2015). https://doi.org/10.1007/s40618-015-0309-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-015-0309-4