Abstract
Background
Latino men who have sex with men (LMSM) are disproportionally affected by HIV infections in the USA. The uptake rate of pre-exposure prophylaxis (PrEP) for HIV prevention has remained low among LMSM. Long-acting injectable PrEP (LAI-PrEP) may have the potential to improve structural, behavioral, and cognitive barriers to adherence. Given the potential benefits of LAI-PrEP and the limited data with this population, the aim of our study was to explore experiences and attitudes of LAI-PrEP among LMSM and identify implementation barriers compared to the standard oral presentation, align proposed implementation strategies, and propose outcomes to monitor and assess impact.
Methods
In this qualitative study, guided by the Consolidated Framework for Implementation Research, we explored health care providers perspectives on facilitators and barriers to LAI-PrEP implementation strategies for LMSM. Interviews were recorded, transcribed, and analyzed using thematic content analysis.
Results
Fear of immigration policies, ability to conceal PrEP medication, health insurance coverage, health information fatigue, lack of culturally adapted information, and provider’s lack of knowledge were among the main barriers to LAI-PrEP. Most providers discussed the need for adapted and/or tailored training materials for and suggested designing marketing materials and specific clinical recommendations for LAI-PrEP.
Conclusion
In order to ensure an effective adaptation process that encompasses local and national goals of HIV prevention, future interventions should be designed in a way that incorporates culturally relevant information for LMSM. This study provides an implementation research logic model to guide future studies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the United States, 1.2 million people are currently living with HIV, with the number of people living with a diagnosed HIV infection increased by 33% during 2009–18, from 797053 to 1023832 [1, 2]. Data from 2018 show that cisgender Latino men who have sex with men (LMSM) accounted for 26% of diagnoses despite accounting for only 18% of the US population [2]. Similarly, epidemiological data show that the annual number of LMSM newly diagnosed with HIV has increased by 7% between 2012 and 2016, and if current HIV diagnosis rates persist, about one in five LMSM will be diagnosed with HIV during their lifetime [3, 4]. Upon seroconversion, LMSM also experience disproportionately poorer clinical outcomes compared with White non-Hispanic MSM in the continuum of HIV care [4].
Since its approval in 2012, daily oral pre-exposure prophylaxis (DO-PrEP) has moved to the forefront of HIV prevention strategies and has been found to reduce likelihood of HIV acquisition by 99% with 60% effectiveness in real world trials [5,6,7,8]. Despite CDC guidelines recommending the widespread use of PrEP for HIV prevention, only 7600 Latinos out of a nearly 300,000 estimated Latinos who may have benefitted from PrEP filled a prescription for PrEP between 2015 and 2017 [9]. According to a recently published systematic review, LMSM face a myriad of barriers to access PrEP, including several factors ranging from individual level (e.g., acculturation, fear of medical treatment, and financial costs) to the community (e.g., geographical disparities in PrEP resources and provider willingness to work with Latinos), that limits engagement with PrEP [10].
Furthermore, low levels of PrEP among LMSM have been attributed to structural inequalities, such as state and federal restrictions to a range of social, medical, and legal rights [11,12,13,14]. Even when these barriers are overcome and LMSM are prescribed PrEP, there remain numerous challenges to sustained PrEP use and adherence, which has been attributed to various factors including, the logistical challenges of pill storage, forgetfulness, side effects, and social challenges, including fear of disclosure and experiences of rejection, judgement, and stigma [7, 14]. Moreover, compared with White non-Hispanic MSM, LMSM are more likely to report disruptions in routine as barriers to adherence [15] and challenges in their support networks, including partners, family members, health care workers, and friends [16]. Rates of DO-PrEP discontinuation have also been higher in LMSM, compared to White non-Hispanic and Black MSM, in several US-based observational studies [15, 17]. Indeed, according to a systematic review and meta-analysis that included 43,917 participants found that 41% of participants discontinued PrEP within 6 months, and there were greater rates of discontinuation among Latino and Black MSM [17].
Long-acting injectable PrEP (LAI-PrEP), formulations of antiretroviral medication administered periodically by injection, have the potential to overcome daily adherence challenges as well as the promise of PrEP/prevention in Ending the Epidemic (EHE) [18,19,20]. A randomized double-blind study demonstrated that LAI-PrEP was superior to DO-PrEP in preventing HIV infections among cisgender MSM and cisgender and transgender women, resulting in 66% (95% confidence interval 38–82%) reduction in HIV incidence [21]. LAI-PrEP in its current format will require healthcare provider-administered intragluteal injections every 2 months following two loading doses 4 weeks apart. Preference studies suggest that up to 70% of US MSM who currently or previously used DO-PrEP are interested in switching to LAI-PrEP [22] and that nearly 50% of MSM not using PrEP would prefer LAI-PrEP as an option [23, 24].
Despite broad recommendations and uptake in other populations, scant research has focused on LAI-PrEP use among LMSM. Because the majority of LAI-PrEP clinical trials and real-world data have occurred among non-Hispanic white MSM, barriers to LAI-PrEP among LMSM remain largely unexplored [25]. For LMSM, use of LAI-PrEP may be further complicated by cultural and structural issues such as medical mistrust [26], concerns regarding insurance and documentation status, and discomfort discussing their sex lives with their doctor or limited access to providers who speak in Spanish [27]. As such, we do not know how LMSM will respond to LAI-PrEP or characteristics of LMSM most likely to adhere to LAI-PrEP. It is also important to understand the challenges LAI-PrEP will impose on providers who work with LMSM. Recognizing these potential barriers can lead to the development and/or adaptation of effective implementation strategies as LAI-PrEP becomes widely available.
Given the potential benefits of LAI-PrEP and the limited data with this population [25], the primary aim of this study was to assess barriers and facilitators of LAI-PrEP among LMSM and to understand provider attitudes and concerns. Developing an understanding of the determinants that affect LAI-PrEP implementation is critical to ending the HIV epidemic, as this information can lead to the development of effective implementation strategies to increase LAI-PrEP use among LMSM. We organized the findings using the Updated Consolidated Framework for Implementation Research (CFIR) [28]. Innovation deliverers, high-level leaders, and implementation facilitators who work with LMSM and prescribe PrEP at a community health clinic were interviewed about the challenges with strategies implemented at their institution, with the goal of creating an implementation research logic model (IRLM) [29] to organize determinants which may require new or adapted interventions.
Method
The present study was approved by the Institutional Review Board (IRB) from Marquette University in partnership with a community health center in Wisconsin. This clinic was carefully chosen given their involvement with the Latino community, reporting serving approximately 43,00 patients, 86% being Latino and of those, 70% were primarily Spanish speaking in 2019. To participate in the interview, individuals must have been 21 years of age and have some form of clinical or community experience with Latinos and at least more than one year of experience. No other exclusionary criteria were applied. Between December 2020 and August 2021, the first author interviewed 18 providers, using non-random, purposive sampling to recruit providers with relevant work experiences. Each semi-structured interview lasted between 30 and 90 minutes. Guided by the tenets of inductive thematic analyses, it was expected that it would take 15–20 interviews to reach data saturation for individual interviews [30]. The 16th and 17th interview in this project corroborated the data from the previous interviews without presenting additional themes, suggesting saturation was achieved. This was determined using constant comparative methods [31]. Each community provider was interviewed once in English, Spanish, or a combination of both.
The in-depth interviews followed a semi-structured interview guide collectively developed by the research team and grounded in CFIR [32]. The interview guide included a series of questions and prompts to assess the multilevel (organizational- and consumer-level) aspects that need to be addressed for LAI-PrEP implementation. CFIR’s five main domains and multiple constructs used were intended to capture barriers to and facilitators of implementation. The domains we explored included innovation characteristics (e.g., relative advantage of LAI-PrEP over DO-PrEP, perceived adaptability of LAI-PrEP to meet the current local needs of Latinos, and potential complexity in the steps required to implement LAI-PrEP in their clinic) individual characteristics (e.g., knowledge and beliefs about the intervention and personal attributes such as motivation and capability to support LAI-PrEP), inner setting (e.g., capacity of the organization, the organizational implementation climate, and capacity for change), outer setting (e.g., patient needs and extent to which these needs are prioritized), and process (e.g., characterized by plans to ease implementation and engagement of community stakeholders). The interviews had open-ended questions reflecting patient, community, and healthcare providers’ perspectives and perceptions about LAI-PrEP implementation. Prior to data collection, we pretested the interview guides with the clinic managers who were not participating in the study.
Data Analysis
Data analysis followed a thematic analysis approach utilizing several grounded theory techniques, including inductive analysis, cross-case analysis, and analytical coding of textual data [33, 34]. In addition to the primary researcher, one peer debriefer, one auditor, and an independent coder were involved in coding and interpreting the data. During the open coding phase, the peer debriefer and primary researcher reviewed the audio recordings, and transcripts for salient categories of information until saturation were reached using constant comparative methods [31]. The initial codes evolved around the interview guide, each interview memo, and categories specific to each CFIR domain. For quality assurance, the primary researcher and an independent coder coded two separate transcripts with the codebook. Interrater reliability was high according to Cohen’s kappa statistic [35] for the coded text with an overall value of K = 0.84. Finally, themes were defined based on CFIR domains and clustering of code application.
Study Results
Participant Demographics
Between December 2020 and August 2021, eighteen interviews were conducted with 18 providers, including eight HIV/STI prevention outreach specialists (44.4%), two dieticians (11.1%), three primary care nurses (16.7%), three community social workers (16.7%), and two administrative providers (11.1%). There was variability in the years of experience of each provider in their current position (range 2–30 years). The sample was majority Hispanic/Latino (77.8%), followed by White (16.7%) and Bi-racial/Mixed-race (5.5%). In the sample, 61.1% were born in Mexico (n = 11), 22.2% were born in Puerto Rico (n = 4), and 16.7% were born in the continental U.S (n = 3). Additional provider demographics are provided in Table 1.
Innovation Characteristics
Many providers highlighted that LMSM could benefit from LAI antiretrovirals, given some of the practical benefits. They described LAI-PrEP as particularly beneficial because, even with social support, adherence to DO-PrEP could be challenging: “Many of them get distracted with work or you know a family incident happened and they can’t go to an appointment, and then, it's been two, three months since they’ve taken the pill” (Design). Compared to DO-PrEP, providers also expressed an injection would lessen the burden of having to conceal their medication at home (Relative Advantage). They noted that LMSM in their clinic have been hesitant to engage with DO-PrEP given their concern that their parents would see their medication and would out them. A smaller subset of providers also compared LAI-PrEP to forms of medication for birth control and suggested that LMSM may be more open to this format of medication.
As with DO-PrEP, providers shared their concern for the cost of LAI-PrEP. Providers discussed that for many LMSM in their clinic, prevention for HIV is not a primary worry, and rather, many of them are more distressed about legal and/or financial burdens at home. Providers suggested LAI-PrEP might result in increased costs to the patient, given that many public/government health insurance programs do not cover LAI-PrEP. One provider stated the following:
They could be more worried about some potential additional bills associated with the costs. I think there might be some additional interest if people are able to get their injections from community stakeholders or covered publicly since it isn’t covered for a lot of people and because we already have a stronger relationship, and it may be cheaper than having to go to a hospital for example.
Further, respondents noted that the best practice guidelines most used for Wisconsin Providers, such as those posted by the Department of Health Services’ AIDS/HIV Program, have not yet issued LAI-PrEP recommendations (Evidence Base). Many providers expressed concerns that LAI-PrEP has not yet been properly evaluated for use among Latinos. They wanted to be reassured that LAI-PrEP would result in equivalent or improved outcomes to the current standard of care (DO-PrEP) before implementing it into their practice. Finally, as these recommendations are established, many providers suggested a need for accessible and trusted locations such as their community clinic or pharmacy for testing and injection administration. Most providers suggested that visits to their primary care provider or a larger hospital could be a potential barrier for many patients As such, providers favored recommendations for LAI-PrEP that would permit patients to see their provider of choice for administration (Adaptability). One provider noted the following for these practice guidelines:
We need more guidelines so that we can be more flexible and who can give the injections. Like, I work in case management, and we don't bill insurances and we meet with our clients for a very long time. They feel more comfortable with somebody who they've already established that rapport with. Doctor's visits are mostly limited to 15 to 30 minutes. So, then they don't get that opportunity as much with the providers to connect. So, I think there'd be a lot of benefits to community members being trained and shown how to properly administer the injectable. But we can’t do that until we have information that a system like that can work, and how much we can tailor it, you know.
Outer Setting
Providers described the outer setting in terms of the structural characteristics of the Latino population in the Midwest. One of the most prominent concerns was the environment in which LMSM are embedded within that may affect their engagement with HIV preventative care. Many providers commented that local support would heavily influence how much Latinos are willing to engage with LAI-PrEP, indicating that public approval or acceptance would be important. One such source, especially among Latinos in rural communities, is that of the church and/or religious center (e.g., “PrEP is not discussed at church, it is, an opportunity for us to introduce injection PrEP, so that we can work together and shape the conversation”) (Local Attitudes).
For the Outer Setting, providers also stressed broader concerns specific to local and national immigration policies. Several providers shared stories of some of their patients skipping clinic appointments due to fear of Immigration and Customs Enforcement (ICE) raids and deportation (Policies & Laws). One case manager explained that “we have a couple of clients that were here and then they were not because they heard of a raid and would not come back until much later”. Because of these stressors, many providers were concerned that Latinos would not return for their second or third dosage of PrEP and would be lost in care. Here, one provider discusses how immigration policies may affect LAI-PrEP:
I had a patient that withdrew from PrEP yesterday because they are going through the process of immigration and need to send their health history and they were worried that PrEP was going to be under health history and that immigration was going to assume that they have risky behavior essentially and that that was going to affect their, their immigration process. So, I could imagine how an injection might be even worse since it might be tracked more.
Finally, many providers discussed the ongoing effect of the COVID-19 pandemic on preventative care, stressing that many people are fatigued with health information (Local Conditions). They worried that LAI-PrEP would be seen by many as another vaccine or government enforced public health recommendation. These concerns then raised questions about how to re-engage with communities that are untrustful of medical care. As illustrated in the following quote, providers suspected that Latinos who saw the COVID-19 vaccine as ineffective might also be less likely to use/trust LAI-PrEP:
Since COVID, people do not want to come in or get more medication. People don’t want to hear about another injection or vaccine, especially since many of them complained about still getting COVID or having to miss more work because of side-effects. So, with PrEP injections, they would probably feel the same way, and not trust it. Like I got 3 COVID vaccines and still got COVID? And the same for HIV.
Inner Setting
Providers discussed current programs at their clinic that could be implemented to support LAI-PrEP awareness and uptake for Latinos. Some of the providers worried about their ability to discuss and find information in Spanish for LAI-PrEP (Available Resources). Some posited that standardized clinical guidelines for PrEP in Spanish are very poorly translated and are often too comprehensive for many of their patients to understand, though none of the providers reported familiarity with existing LAI-PrEP guidelines in Spanish. Further, in the event of more complex social cases, providers expressed that given their limited resources, LAI-PrEP might not be considered as essential service (Relative Priority). Many providers highlighted that since many of their resources are free to patients that they then have to prioritize programs that support people with HIV or with services that aid with shelter and documentation. Providers often drew on their own clinical experiences and emphasized that many of their clients need immediate support for essential care:
I think the demand for this [LAI-PrEP] is there, but it might not be the most important social need, so we as a group have to decide which services we support more, and that all of course has on impact on the things we can offer. I see that too in some of my work with my clients with HIV, and how they aren’t able to request the time necessary to take care of themselves. You must think about where they work and what benefits they have; do they have PPO [Preferred Provider Organization] to use to be able to get care? Are the clinics in those communities able to accommodate different work hours so that people do not have to take time off, that is another challenge, is being able to go to a clinic that is only open from 8-5.
Many providers also suggested the ways in which clinical care should transition from a “disease-based” approach to a “patient-centered” format that would allow for providers to understand and assess the physical and social environment in which their patients are embedded within (Culture; Recipient-Centeredness). According to informants, successful implementation of LAI-PrEP is dependent on whether clinics are able to also address care equally in a holistic way. That is, in addition to LAI-PrEP, are clinics able to assist their clients with navigating an unfamiliar health care system or provide resources for example to reduce fears related to accessing public services due to potential changes in public charge rules. One provider noted the following:
I think all medical interactions are issue based, following the disease model, where they see a doctor and something's treated, and then it's done and they either get better or are lost in treatment. And I think in order to shift that mindset, we need to approach it as open communication. For PrEP with a pill or injection, part of that mindset is how we approach it. So, if we approach it, as something that is part of their environment and their overall care, then great, we can get them on it, but we've also got a whole bunch of cool things, including support for housing or educational resources in Spanish. We want to encourage them to take advantage of everything, because if they don’t have a roof over their head, then it won’t work, and they won’t come back.
Characteristics of Individuals
“Individuals” in CFIR refers to those involved in the delivery of LAI-PrEP and includes both their perspective as implementors of the innovation and their account of innovation recipients and their characteristics. Providers cited a general lack of knowledge as a barrier that could impact not only their capacity to counsel patients on the risks, benefits, and alternatives to LAI-PrEP but also their motive to recommend LAI-PrEP (Innovation Deliverers; Capability and General Knowledge About & Attitudes Toward Innovation). Some stated that they had only received a cursory overview of LAI-PrEP during prior clinical trainings and requested for additional resources at the completion of the interview. Even for providers who felt more well-versed and were directly involved in HIV clinical care, discussing LAI-PrEP dosing posed another challenge. Respondents shared that unless they were very informed on the pragmatics of LAI-PrEP, then they would be unlikely to discuss this method as a form of prevention with their patients (Innovation Deliverers; Motivation).
Moreover, many providers voiced several perceived patient-level barriers for LAI-PrEP that are categorized as individual characteristics Respondents expressed that many patients would not have the educational background to understand how LAI-PrEP functions to prevent HIV (e.g., “With the injection, I can see how confused people would be, like is it going to wear off? Is there going to be a time where I won’t have the full protection?) (Innovation Deliverers; Capability and General Knowledge About & Attitudes Toward Innovation). Many providers also perceived patients to have low motivation to return for their second or third dose, stressing that some patients might believe that one dose is enough for some HIV protection (Innovation Recipients; Capability). Additionally, some providers were concerned that many of their patients with transient and/or migrant work would have less access to a provider for their dose (Innovation Recipients; Opportunity). These concerns were most related to providers’ perceptions of low patient knowledge:
The trick would be getting people to come back in time for the injections to work. Retention rates would be an issue because they wouldn’t understand how sensitive the timeline is for it to be effective. Because if someone comes for a dose and they miss the next dose, and then they come back for the next one, after that, they might not understand that because they missed the middle dose. They're starting over, right? So, like, if you didn't understand what was happening biologically, why would you think that because you missed this dose that you could, you couldn't just come back for the next one.
Process
Respondents provided suggestions for supporting implementation of LAI-PrEP for Latinos. Several cited the essential role of a Navigator or Community Advocate in promoting LAI-PrEP in communities, suggesting that it is necessary for familiar people to market LAI-PrEP to patients (Engaging Innovation Recipients). Others emphasized the importance of marketing, reference materials in Spanish, and tailored infographics to support implementation. Providers stressed the need for complementary interventions such as mobile applications and/or media campaigns for LAI-PrEP that have been developed for Latinos, rather than materials that were simply translated from English (Adaptation; Tailoring Strategies).
Implementation Research Logic Model
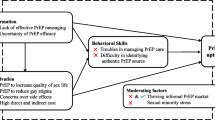
Through analyzing the information gained in the qualitative interviews with providers, our study team developed an IRLM [29] to guide implementation and evaluation of strategies to support LAI-PrEP uptake among LMSM. Within the model, we identify provider-proposed strategies for LAI-PrEP framed within the Expert Recommendations for Implementing Change (ERIC) [36]. With respect to implementation strategies (Fig. 1), most providers discussed the need for adapted and/or tailored training materials for LAI-PrEP. Further, providers suggested designing marketing materials and specific clinical recommendations for LAI-PrEP that requires additional implementation strategies to address the multilevel barriers to HIV prevention and care for Latino MSM (i.e., language barriers, stigma, and provider mistrust). The dearth of trainings and materials in Spanish for LAI-PrEP described by participants also reinforced the need for tailored education. Given some of the barriers that were discussed in the inner setting, many providers suggested that more technical assistance is needed to improve/assist with referrals, which would allow for consistent recruitment, integration, and retention. Indeed, providers noted how much of their time is used up in ensuring that patients are appropriately referred to, even within the same clinical system. Furthermore, providers attended to structural barriers within both the Inner and Outer settings, such as documentation status and clinical hours of operation, that need to be considered in selecting implementation strategies. Notably, providers discussed ways in which access to LAI-PrEP is dependent on providers having the interpersonal skills and education necessary to address political and/or social concerns. We hypothesize these strategies would increase key implementation outcomes including adoption and sustainment and result in clinical outcomes including an increased uptake of LAI-PrEP and overall lower HIV incidence among LMSM.
Discussion
In identifying barriers and facilitators to LAI-PrEP implementation, we contribute to the growing implementation research literature examining determinants of LAI-PrEP. While others have identified barriers and facilitators of LAI-PrEP implementation for cisgender women [37], heterosexual men [38], MSM in the military regardless of race [39], and transgender women [40], few have examined determinants of LAI-PrEP for LMSM. Azhar et al. [25] identified determinants to participation in LAI-PrEP trials for cisgender MSM, transgender women, and gender-nonconforming people, including LMSM. However, determinants of trial participation may be very different based on the inner setting context, as well as innovation characteristics, as compared to uptake of and adherence to the innovation. To the best of our knowledge, one other paper examines perceived determinants of LAI-PrEP for LMSM; however, this study utilized qualitative methods with a small group of Black, Latino, and White non-Hispanic MSM [41]. Our study adds an identification of barriers for uptake and delivery through interviews with providers specifically for LMSM.
These barriers include perceived worries regarding the cost of LAI-PrEP. While data collection occurred prior to the approval of Apretude (cabrotegravir) for LAI-PrEP and its official release for public use, new information about costs of LAI-PrEP has been documented. Apretude’s price range is estimated to be nearly four-thousand dollars per injection, with two doses needed in the initial month and then one dose every other month (Sharfstein et al., 2022). While ViiV Healthcare, the manufacturer of Apretude, provides a cost-sharing program to assist patients in affording LAI-PrEP, this program is only available to those with insurance and in particular with insurance that covers at least part of the cost of Apretude [42]. As of 2022, Latinos had the highest uninsured rate of all racial/ethnic groups in the U.S. at 17.7% [43]. Thus, researchers, clinicians, and policy makers must develop strategies to mitigate or entirely cover the cost of LAI-PrEP to increase uptake and adherence for LMSM, including those who are undocumented.
Interview participants also spoke to the need to address structural and social determinants of health or those upstream factors that influence implementation and uptake of clinical innovations downstream for intersectionally marginalized populations. Factors, including educational attainment, immigration status, access to Spanish-speaking and/or Latino providers, and employment, among others, influence not only PrEP use [44], but LMSM’s everyday survival. Multilevel stigmas, including participant-mentioned anticipated stigma regarding familial, partner, or friend reactions to discovering one is on PrEP as well as stigma of discussing sex with a provider, continue to hinder efforts to increase uptake of even DO-PrEP [44, 45]. These structural and community-level barriers can be addressed through equity-focused behavioral interventions and structural interventions. The recent NIH request for applications to use implementation science to address social and structural determinants of health and improve HIV outcomes is one step in hopefully moving in this direction [46]. In addition to developing new interventions, researchers can use implementation science models and frameworks of innovation adaptation to develop racially and culturally tailored interventions and strategies for LMSM. For example, researchers can utilize Stirman, Baumann, and Miller’s (2019) FRAME-IS [47, 48]. This framework provides researchers a step-by-step process to modify interventions and document adaptations for future replication in practice and research [48]. Researchers can also look to previous adaptations of interventions to increase uptake and adherence for DO-PrEP to identify whether they will work as is or need modification to meet the unique determinants of LAI-PrEP implementation. One example includes “Proyecto Compadre,” a tailored, peer navigation intervention for LMSM, involving peer-led navigation, social media recruitment and dissemination, tailored educational material, and attention to stigma and medical mistrust [49].
Additionally, a critical analysis of the current evidence on culturally adapted interventions for Latinx communities is necessary. Growing demands from government bodies and funding agencies for more research to include Latinx in their data collection, intervention designs, or clinical trials do not necessarily reflect on studies that consider the nuances and particularities of such a diverse group [50]. Although Latinx is a group that shares a series of sociocultural similarities, its operationalization in a single category homogenizes peoples, ethnicities, cultures, and languages that do not fit into a single adaptation process [51]. The implementation of new EBIs needs to consider a critical stance on the cultural adaptation of these tools, as well as the inter-Latin variability between communities in different settings.
Finally, researchers can turn to health equity implementation frameworks to ensure that development, adaptation, and implementation of interventions and strategies to enhance LAI-PrEP implementation in LMSM populations attend to equity and community-engagement from the start. The health equity implementation framework is an adaptation of the Integrated-Promoting Action on Research Implementation in Health Services (i-PARIHS) framework, which incorporates attention to sociopolitical forces, economies, and improvements in health equity [52]. Prior to identification of barriers, researchers can use an approach like that of Allen et al. [53] who apply the Public Health Critical Race Praxis methodology [54] to CFIR to develop a race(ism) conscious adaptation of the framework. Novel theoretical frameworks like Critical “Street Race” Praxis are further ensuring attention to colorism and racism to capture within-group differences in analyses of health disparities for Latinos, through an application of Latino Critical Race Theory (LatCRT) to Public Health Critical Race Praxis [54].
There are several study limitations to consider. First, there is the potential for selection bias due to health care providers voluntary participation and results may have been different than those who opted not to be enrolled in our study. To reduce the likelihood of volunteer bias, the study team ensured anonymity of participants and offered flexible interview times including nights and weekends. Second, this qualitative study was conducted in a single health-focused clinic system with extensive HIV services; thus, results may not generalize to other settings.
Conclusion
This research study suggests that the success of LAI-PrEP implementation will depend largely on public health efforts to address structural and social determinants of health or those upstream factors that influence implementation and uptake of clinical innovations downstream for LMSM. Through analyzing the information gained in the qualitative interviews with providers, our study team developed an IRLM to guide implementation and evaluation of strategies to support LAI-PrEP uptake among LMSM. Our findings are helpful in documenting the data gaps and implementation considerations for health care providers working with LMSM and other stakeholders, as they anticipate scale-up of LAI-PrEP in community clinics.
Data Availability
Data is not accessible to the public to minimize the risk of loss of confidentiality. Individuals who meet criteria for access to de-identified data should contact the Principal Investigator (juan.zapata@northwestern.edu) to facilitate data transfer.
References
Gant Z, Dailey A, Hu X, Johnson AS. HIV care outcomes among Hispanics or Latinos with diagnosed HIV infection—United States, 2015. Morbid Mortal Weekly Rep. 2017;66(40):1065.
Sullivan PS, Johnson AS, Pembleton ES, Stephenson R, Justice AC, Althoff KN, Bradley H, Castel AD, Oster AM, Rosenberg ES, Mayer KH. Epidemiology of HIV in the USA: epidemic burden, inequities, contexts, and responses. Lancet. 2021;397(10279):1095–106.
Hess KL, Hu X, Lansky A, Mermin J, Hall HI. Lifetime risk of a diagnosis of HIV infection in the United States. Ann Epidemiol. 2017;27(4):238–43.
Trujillo L, Chapin-Bardales J, German EJ, Kanny D, Wejnert C, Abrego M, Al-Tayyib A, Anderson B, Barak N, Bautista G, Bayang L. Trends in sexual risk behaviors among Hispanic/Latino men who have sex with men—19 urban areas, 2011–2017. Morbid Mortal Weekly Rep. 2019;68(40):873.
Crepaz N, Salabarría-Peña Y, Mullins MM, Gunn JK, Higa DH. Systematic review of social determinants of health associated with HIV testing among Hispanic/Latino gay, bisexual, and other men who have sex with men in the United States. AIDS Educ Prevent. 2023;35(1):36–S6.
Grulich AE, Guy R, Amin J, Jin F, Selvey C, Holden J, Schmidt HM, Zablotska I, Price K, Whittaker B, Chant K. Population-level effectiveness of rapid, targeted, high-coverage roll-out of HIV pre-exposure prophylaxis in men who have sex with men: the EPIC-NSW prospective cohort study. Lancet HIV. 2018;5(11):e629–37.
Mayer KH, Agwu A, Malebranche D. Barriers to the wider use of pre-exposure prophylaxis in the United States: a narrative review. Adv Therapy. 2020;37:1778–811.
Jourdain H, de Gage SB, Desplas D, Dray-Spira R. Real-world effectiveness of pre-exposure prophylaxis in men at high risk of HIV infection in France: a nested case-control study. Lancet Public Health. 2022;7(6):e529–36.
Kamitani E, Johnson WD, Wichser ME, Adebukola HA, Mullins MM, Sipe TA. Growth in proportion and disparities of HIV PrEP use among key populations identified in the United States national goals: systematic review & meta-analysis of published surveys. J Acq Immune Deficien Syndr (1999). 2020;84(4):379.
Zapata JP, de St AE, Rodriguez-Diaz CE, Malave-Rivera S. Using a structural-ecological model to facilitate adoption of preexposure prophylaxis among Latinx sexual minority men: a systematic literature review. J Latinx Psychol. 2022;10(3):169.
Doblecki-Lewis S, Liu A, Feaster D, Cohen SE, Cardenas G, Bacon O, Andrew E, Kolber MA. Healthcare access and PrEP continuation in San Francisco and Miami following the US PrEP demo project. J Acq Immune Deficien Syndr (1999). 2017;74(5):531.
Bonacci RA, Smith DK, Ojikutu BO. Toward greater pre-exposure prophylaxis equity: increasing provision and uptake for Black and Hispanic/Latino individuals in the US. Am J Prevent Med. 2021;61(5):S60–72.
Harkness A, Weinstein ER, Atuluru P, Mayo D, Vidal R, Rodríguez-Díaz CE, Safren SA. Latinx sexual minority men’s access to HIV and behavioral health services in South Florida during COVID-19: a qualitative study of barriers, facilitators, and innovations. J Assoc Nurses AIDS Care: JANAC. 2022;33(1):9.
Weinstein ER, Glynn TR, Simmons EM, Safren SA, Harkness A. Structural life instability and factors related to Latino sexual minority men’s intention to engage with biomedical HIV-prevention services. AIDS Behav. 2022;4:1–1.
Nieto O, Fehrenbacher AE, Cabral A, Landrian A, Brooks RA. Barriers and motivators to pre-exposure prophylaxis uptake among Black and Latina transgender women in Los Angeles: perspectives of current PrEP users. AIDS Care. 2021;33(2):244–52.
Flores DD, Meanley SP, Wood SM, Bauermeister JA. Family characteristics in sex communication and social support: implications for emerging adult men who have sex with men’s PrEP engagement. Arch Sexual Behav. 2020;49:2145–53.
Zhang J, Li C, Xu J, Hu Z, Rutstein SE, Tucker JD, Ong JJ, Jiang Y, Geng W, Wright ST, Cohen MS. Discontinuation, suboptimal adherence, and reinitiation of oral HIV pre-exposure prophylaxis: a global systematic review and meta-analysis. Lancet HIV. 2022;9(4):e254–68.
Clement ME, Kofron R, Landovitz RJ. Long-acting injectable cabotegravir for the prevention of HIV infection. Curr Opin HIV and AIDS. 2020;15(1):19.
Parkin N, Gao F, Grebe E, Cutrell A, Das M, Donnell D, et al. Facilitating next‐generation pre‐exposure prophylaxis (PrEP) clinical trials using HIV recent infection assays: a consensus statement from the Forum HIV Prevention Trial Design Project. Clin Pharmacol Ther. 2022. https://doi.org/10.1002/cpt.2830.
Flexner C, Owen A, Siccardi M, Swindells S. Long-acting drugs and formulations for the treatment and prevention of HIV infection. Int J Antimicro Agents. 2021;57(1):106220.
Landovitz RJ, Donnell D, Clement ME, Hanscom B, Cottle L, Coelho L, Cabello R, Chariyalertsak S, Dunne EF, Frank I, Gallardo-Cartagena JA. Cabotegravir for HIV prevention in cisgender men and transgender women. New Eng J Med. 2021;385(7):595–608.
John SA, Whitfield TH, Rendina HJ, Parsons JT, Grov C. Will gay and bisexual men taking oral pre-exposure prophylaxis (PrEP) switch to long-acting injectable PrEP should it become available? AIDS Behav. 2018;22:1184–9.
Biello KB, Bazzi AR, Mimiaga MJ, Biancarelli DL, Edeza A, Salhaney P, Childs E, Drainoni ML. Perspectives on HIV pre-exposure prophylaxis (PrEP) utilization and related intervention needs among people who inject drugs. Harm Reduct J. 2018;15:1–2.
Greene GJ, Swann G, Fought AJ, Carballo-Diéguez A, Hope TJ, Kiser PF, Mustanski B, D’Aquila RT. Preferences for long-acting pre-exposure prophylaxis (PrEP), daily oral PrEP, or condoms for HIV prevention among US men who have sex with men. AIDS Behav. 2017;21:1336–49.
Azhar S, Tao X, Jokhakar V, Fisher CB. Barriers and facilitators to participation in long-acting injectable PrEP research trials for MSM, transgender women, and gender-nonconforming people of color. AIDS Educ Prevent. 2021;33(6):465–82.
Gelaude D, Denson D. “Why You Putting This Drug in Your Body to Fight off Something that You Don’t Have?” Perceptions about PrEP use among Black and Latino men who have sex with men in the US South. J Homosexual. 2023;70(5):900–16.
Cantos VD, Hagen K, Duarte AP, Escobar C, Batina I, Orozco H, Rodriguez J, Camacho-Gonzalez A, Siegler AJ. Development of a mobile app to increase the uptake of HIV pre-exposure prophylaxis among Latino sexual minority men: qualitative needs assessment. JMIR Form Res. 2023;8(7):e43844.
Damschroder LJ, Reardon CM, Opra Widerquist MA, Lowery J. Conceptualizing outcomes for use with the Consolidated Framework for Implementation Research (CFIR): the CFIR Outcomes Addendum. Implement Sci. 2022 ;17(1):1-0.
Smith JD, Li DH, Rafferty MR. The implementation research logic model: a method for planning, executing, reporting, and synthesizing implementation projects. Implement Sci. 2020;15:1–2.
Guest G, Namey E, Chen M. A simple method to assess and report thematic saturation in qualitative research. PloS One. 2020;15(5):e0232076.
Fram SM. The constant comparative analysis method outside of grounded theory. Qual Rep. 2013;18:1.
Keith RE, Crosson JC, O’Malley AS, Cromp D, Taylor EF. Using the Consolidated Framework for Implementation Research (CFIR) to produce actionable findings: a rapid-cycle evaluation approach to improving implementation. Implement Sci. 2017;12(1):1–2.
Ridder HG. Book Review: Qualitative data analysis. A methods sourcebook. Sage UK: London England: Sage publications; 2014.
Strauss A, Corbin JM. Grounded theory in practice. Sage; 1997.
McHugh ML. Interrater reliability: the kappa statistic. Biochem Med. 2012;22(3):276–82.
Powell BJ, Waltz TJ, Chinman MJ, Damschroder LJ, Smith JL, Matthieu MM, Proctor EK, Kirchner JE. A refined compilation of implementation strategies: results from the Expert Recommendations for Implementing Change (ERIC) project. Implement Sci. 2015;10(1):1–4.
Philbin MM, Parish C, Kinnard EN, Reed SE, Kerrigan D, Alcaide ML, Cohen MH, Sosanya O, Sheth AN, Adimora AA, Cocohoba J. Interest in long-acting injectable pre-exposure prophylaxis (LAI PrEP) among women in the women’s interagency HIV study (WIHS): a qualitative study across six cities in the United States. AIDS Behav. 2021;25:667–78.
Cheng CY, Quaife M, Eakle R, Cabrera Escobar MA, Vickerman P, Terris-Prestholt F. Determinants of heterosexual men’s demand for long-acting injectable pre-exposure prophylaxis (PrEP) for HIV in urban South Africa. BMC Public Health. 2019;19(1):1–9.
Gutierrez JI, Vlahov D, Dubov A, Altice FL. Preferences for long-acting and alternative modalities for PrEP among military men who have sex with men: segmentation results of an adaptive choice-based conjoint analysis study. J Urban Health. 2022;99(2):277–92.
Pedrana L, Magno L, Zucchi EM, da Silva LA, Ferraz D, Grangeiro A, Castellanos M, Brasil SA, Dourado I. Zero knowledge and high interest in the use of long-acting injectable pre-exposure prophylaxis (PrEP) among adolescent men who have sex with men and transgender women in two capital cities in Brazil. BMC Public Health. 2022;22(1):1.
Tran NK, Martinez O, Scheim AI, Goldstein ND, Welles SL. Perceived barriers to and facilitators of long-acting injectable HIV PrEP use among Black, Hispanic/Latino, and White gay, bisexual, and other men who have sex with men. AIDS Educ Prevent. 2022;34(5):365–78.
Prather C, Jeon C. Cabotegravir: The first long-acting injectable for HIV pre-exposure prophylaxis. Am J Health-Syst Pharm. 2022;79(21):1898–905.
Guilamo-Ramos V, Thimm-Kaiser M, Benzekri A, Chacón G, López OR, Scaccabarrozzi L, Rios E. The invisible US Hispanic/Latino HIV crisis: addressing gaps in the national response. Am J Public Health. 2020;110(1):27–31.
Caba AE, Rathus T, Burson E, Chan PA, Eaton LA, Watson RJ. Who is using PrEP on-demand? Factors associated with PrEP use modality among Black and Hispanic/Latino emerging adults. AIDS Behav. 2022;26(10):3411–21.
Watson RJ, Morgan E, Sherman J, Caba AE, Wheldon CW, Chan PA, Eaton LA. Pre-exposure prophylaxis (PrEP) use, anticipated PrEP stigma, and bisexual identity among a Black and Hispanic/Latino sexual and gender diverse sample. Behav Med. 2022;2:1–9.
Greenwood G, Gaist P, Namkung A, Rausch D. Methodological and measurement advances in social determinants of HIV: view from NIH. AIDS Behav. 2021;1:1–6.
Miller CJ, Barnett ML, Baumann AA, Gutner CA, Wiltsey-Stirman S. The FRAME-IS: a framework for documenting modifications to implementation strategies in healthcare. Implement Sci. 2021;16:1–2.
Wiltsey Stirman S, Baumann AA, Miller CJ. The FRAME: an expanded framework for reporting adaptations and modifications to evidence-based interventions. Implement Sci. 2019;14:1.
Tsuyuki K, Stockman JK, Stadnick NA, Moore V, Zhu H, Torres V, Cano R, Penninga K, Aldous JL. Proyecto compadre: using implementation science to tailor peer navigation for Latino men in the US–Mexico Border Region. JAIDS J Acq Immune Deficien Syndr. 2022;90(1):S98–104.
Barrera M Jr, Castro FG, Strycker LA, Toobert DJ. Cultural adaptations of behavioral health interventions: a progress report. J Consult Clin Psychol. 2013;81(2):196.
Licea R. Is “Latino” useful? Diversity, commonality, and politics. Sociol Compass. 2020;14(12):1–3.
Woodward EN, Matthieu MM, Uchendu US, Rogal S, Kirchner JE. The health equity implementation framework: proposal and preliminary study of hepatitis C virus treatment. Implement Sci. 2019;14:1–8.
Allen M, Wilhelm A, Ortega LE, Pergament S, Bates N, Cunningham B. Applying a race (ism)-conscious adaptation of the CFIR framework to understand implementation of a school-based equity-oriented intervention. Ethnic Dis. 2021;31(Suppl 1):375.
Vargas ED, Juarez M, Stone LC, Lopez N. Critical ‘street race’praxis: advancing the measurement of racial discrimination among diverse Latinx communities in the US. Cri Public Health. 2021;31(4):381–91.
Acknowledgements
The authors acknowledge the contributions of other members of the study’s advisory team, especially Drs. John Steven, Andrew Petroll, and Katherine Quinn. We wish to thank our staff and students at Sixteenth Street Clinic in Milwaukee, especially Jacob Stanley Yarbrough, Jose Salazar, and Pedro Perez. We also wish to thank our participants who volunteered their time.
Funding
The first author’s time was supported by a training grant from the National Institute of Mental Health (T32MH130325; PI: Newcomb).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to Participate
This study met Marquette University Institutional Review Board’s definition of “minimal risk” and a waiver of informed consent was granted. All participants agreed to participate after completion of a guided procedure using Qualtrics that described the study’s purpose, procedures, and other critical components, as well as a capacity-to-consent procedure.
Disclaimer
The content of this manuscript is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zapata, J.P., zamantakis, a. & Queiroz, A.A.F.L.N. Identification of Determinants and Implementation Strategies to Increase Long-Acting Injectable PrEP for HIV Prevention Among Latino Men Who Have Sex with Men (MSM). J. Racial and Ethnic Health Disparities 11, 2093–2102 (2024). https://doi.org/10.1007/s40615-023-01678-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-023-01678-3