Abstract
Purpose of Review
This systematic review evaluated existing evidence linking air pollution exposure in humans to major epigenetic mechanisms: DNA methylation, microRNAs, long noncoding RNAs, and chromatin regulation.
Recent Findings
Eighty-two manuscripts were eligible, most of which were observational (85%), conducted in adults (66%) and based on DNA methylation (79%).
Summary
Most observational studies, except panel, demonstrated modest effects of air pollution on the methylome. Panel and experimental studies revealed a relatively large number of significant methylome alterations, though based on smaller sample sizes. Particulate matter levels were positively associated in several studies with global or LINE-1 hypomethylation, a hallmark of several diseases, and with decondensed chromatin structure. Several air pollution species altered the DNA methylation clock, inducing accelerated biological aging. The causal nature of identified associations is not clear, however, especially that most originate from countries with low air pollution levels. Existing evidence, gaps, and perspectives are highlighted herein.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ambient air pollution is among the leading risk factors for mortality. Components such as airborne particles smaller than 2.5 μM in aerodynamic diameter (PM2.5) were estimated to cause 4.2 million deaths representing 7.6% of total global deaths in 2015 [1]. According to the World Health Organization (WHO), 92% of the population breathes air with unhealthy levels of pollutants [2]. Pollution is closely linked to climate changes, and future levels of air pollution will depend on emissions and global climate changes [3].
Since air pollution is a complex mixture, we still have little understanding of the individual contribution of its different components [4]. Components of air pollution include but are not limited to particulate matter (PM), ozone (O3), sulfur dioxide (SO2), nitrogen oxides (NOx), carbon monoxide (CO), benzene, black carbon, polycyclic aromatic hydrocarbons, and toxic metals. Because of their small size, airborne particles can be inhaled deeply into the lungs and deposited in the alveoli, and the smallest particles can directly reach the bloodstream [5]. Exposure to air pollution increases the risk for cardiovascular [6, 7] as well as respiratory diseases [8] and cancer [9]. In fact, air pollution has been classified by the International Agency for Research on Cancer as a group I carcinogen [10]. Besides this, evidence is mounting that exposure to air pollution is associated with neuro- and cognitive developmental alterations [11] in newborns [12] and children [13,14,15]. Oxidative stress, immune and inflammation responses, and mitochondrial changes are commonly considered as putative mechanisms underlying these health outcomes [7]. One of the mechanisms through which air pollution exposure can induce these biomolecular changes involves DNA damage and epigenetic alterations, which can influence health outcomes across life stages and possibly across generations [16, 17••, 18].
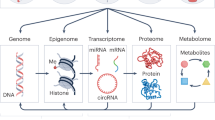
Epigenetics is the science of nongenetic mitotically heritable changes that result in variations in gene expression [19, 20]. Four major interacting systems ensure epigenetic control of gene expression: DNA methylation, histone modification, noncoding RNAs, and chromatin remodeling. These communicating mechanisms ensure the somatically heritable states of gene expression [21]. Epigenetic states display plasticity and are subjected to intrinsic (e.g., age, sex, genetic polymorphisms) and extrinsic (e.g., environmental exposures and dietary habits) influences [22].
Few reviews (all nonsystematic) are available on air pollution and epigenetics, and important novel technological developments in exposure assessment and in epigenome-wide association (EWAS) studies have become available since then. Accordingly, we provide a systematic review analyzing the existing evidence on the associations between air pollution and the major levels of human epigenetic control: DNA methylation, histone modifications, microRNA (miRNA), and long noncoding RNA (lncRNA) and chromatin regulation. We are only just beginning to understand the multitude of effects of air pollution on epigenetics, and this work could provide a timely guide into this rapidly evolving field.
Methods
This systematic review was conducted according to the STROBE guidelines [23]. The search strategy used to identify epidemiological studies examining the association between air pollution and epigenetic changes was made up of four stages, following the PRISMA statement guidelines [24], as depicted in Fig. 1.
In the first stage, articles were identified through a literature search. First, the search was performed through PubMed and Scopus engines without any time restriction and using the MeSH terms “air pollution” and “epigenomics” and the keywords: “particulate matter,” “ultrafine particle*,” “PM2.5,” “PM10,” “black carbon,” “elemental* carbon,” “nitrogen* dioxide*,” “nitrogen* oxide*,” “NOx,” “NO2,” “PAH” and “polycyclic aromatic hydrocarbon*,” “histon*,” “DNA methylation,” “DNA hydroxymethylation,” “non-coding RNA,” “miRNA,” “chromatin remodelling,” “chromatin,” “chip-on-chip,” and “chip seq.” Boolean operators were used to create every possible term combinations as reported in the Online Resource 1. The last search was run on the 6th September 2018.
The second stage consisted of the screening of all the papers identified. Two researchers (R.A. and M.P.) independently reviewed the relevance of the records through consultation of titles and abstracts (and in case uncertainty assessing the full texts).
In the third stage, the full text of the records was examined for eligibility. Eligibility criteria used were the following: (1) the paper is written in English, (2) the paper is an original article, (3) the paper deals with human species, (4) the paper deals with in vivo study, (5) the paper examines any epigenetics mechanism, and (6) the paper studies ambient air pollution as main exposure or the effects of air pollution through an experimental design.
In the fourth stage, selected studies were grouped according to epigenetics mechanisms under investigation and study population; the following information was extracted: authors, relevant country, study design and period, population size, age, and cohort from which data were derived, air pollution exposures examined, epigenetic markers analyzed along with the method of detection, confounders identified, main findings, and risk estimates.
For DNA methylation and hydroxymethylation, separate tables for adults and children are presented.
Results
We have analyzed existing evidence associating air pollution to the major levels of human epigenetic control (Fig. 1): DNA methylation (Tables 1, 2, and 3), noncoding RNAs (Table 4), and chromatin regulation (Table 4). Characteristics of the studies included in the review are summarized in Fig. 2.
DNA Methylation
DNA methylation was the most widely investigated epigenetic mechanism in response to air pollution (Fig. 2b). We have separated the results into those observed in children (Table 1) and those in adults (Tables 2 and 3). All studies among children were observational (cohort, cross-sectional, case-control, and longitudinal; Table 1), while adult studies were either observational (cohort, cross-sectional, case-control, longitudinal, and panel; Table 2) or experimental (crossover; Table 3).
In children (Table 1), EWAS studies in cohort or longitudinal studies showed little effect of perinatal air pollution exposure on the newborn’s blood epigenome (nos. 1–4). The few genes for which differential methylation did seem to relate to air pollution encompass EOGT and COLEC11 in response to PM and three mitochondria-related genes (LONP1, HIBADH, and SLC25A28) and ADOR2B in relation to NO2. Two other studies used an EWAS approach but in a cross-sectional design, comparing blood from individuals living in high- vs. low-polluted areas (nos. 5–6). The first (no. 5 in South Africa) showed no significant results but was based on a relatively small sample size (n = 21 newborns), while the second (no. 6 in Czech Republic) reported 9916 significant CpG sites, but half of its participants were asthmatics (which the study attempted to correct for). Both studies were conducted in countries with comparable air pollution burdens [20–30 μg/m3 of particles of less than 10 μM in aerodynamic diameter (PM10), according to WHO Global Urban Ambient Air Pollution 2016 Database http://www.who.int/phe/health_topics/outdoorair/databases/cities/en/]. All other studies were performed in countries that exhibit < 20 μg/m3 of PM10 and are considered relatively lowly polluted, with the exception of one study in Mexico (20 μg/m3 of PM10; no. 14), two in China (54 μg/m3 of PM10; nos. 10 and 15), and one in Iran (60 μg/m3 of PM10; no. 7). However, the Mexican and Chinese studies used targeted methylation approaches, among which long interspersed nucleotide elements (LINE-1 or L1) were used as a proxy for global methylation levels. The Mexican study did not find a significant association between L1 methylation and overall PM10, but a positive relationship was observed with one of the PM10 components, benzo[b]fluoranthene (no. 14). All other studies (including the Chinese) investigating the relationship between PM and L1 methylation reported a negative association (nos. 15 and 18), while ozone showed the opposite trend (no. 18). No association was found for Alu methylation with different air pollutants from a study in 11-year-old children (no. 18), while a positive association was observed with PM10 in placenta (no. 1). In contrast, global methylation was found always negatively associated with PAH, pyrene (no. 9) and PM (no. 8) levels, except from the Iranian study that found a positive association with PM (no. 7). Most of the studies investigated DNA modifications in relation to chronic exposure to air pollution, while only a few described effects of short-term exposure (nos. 1, 13, 14, 16, 20 and 23). Comparison of effects of short and chronic exposure to air pollution showed that the strength of associations was higher with chronic than recent exposure to air pollution (nos. 13, 20, and 22).
Similarly, in adult EWAS cohort studies (Table 2), few CpGs were significantly methylated (however, none could be replicated in different studies) in response to various air pollution components and based on blood as a surrogate tissue (nos. 1–11). Again, all these studies were conducted in relatively low-polluted countries (exhibiting < 20 μg/m3 of PM based on the WHO Global Urban Ambient Air Pollution 2016 Database). China was the only country identified in the literature (nos. 13, 14, 16, 17, 23, and 25–27) that had relatively high pollution levels, but only targeted DNA methylation (i.e., not EWAS) analyses have been performed in this population. Even though EWAS analyses in adult cohort studies have so far identified only a limited number of significant CpGs, one observation seems to be consistent across three EWAS studies addressing epigenetic aging and conducted in two different continents (represented by Germany and USA); this finding is that various air pollution components contribute to accelerated aging (nos. 5, 9, and 10) calculated from DNA methylation levels according to the Horvath and Hannum methods (using respectively 353 and 71 chronological age-correlated CpGs) [103, 104].
Similar to studies among children, in adults, global methylation estimated from EWAS approaches (nos. 12 and 15) was negatively associated with overall PM levels (Table 2). Similarly, a negative association was found between PM and L1 methylation levels, while no association was found for methylation of Alu elements (no. 32). Negative associations with global or L1 methylation were reported for NO2 (nos. 7 and 15), black carbon (nos. 22 and 32), and SO4 (no. 22) (Table 2). DNA methylation changes have been described for exposure durations to air pollutants ranging from only a few hours (no. 24) to several years. Longer-term exposures yielded more significant associations (no. 15). Two studies also investigated global hydroxymethylation levels in relation to PM but reported conflicting findings (no. 12 vs. 14).
As for the experimental studies (Table 3), all were conducted in adults and were crossover intervention trials in which the volunteers were sequentially exposed to particulate or diesel exhaust mixtures and to controlled exposures (filtered air). Similar to observations in the cohort studies, one experimental study found a negative association between PM and L1 methylation levels (no. 6), though another did not find any significant effect (no. 5). Exposure to fine concentrated ambient particles lowered Alu methylation but did not seem to have an effect on L1 (no. 7). Though the experimental studies conducted so far using an EWAS approach (nos. 1–4) are based on few subjects (n ≤ 36), they have identified several CpGs that are significantly altered by PM2.5 exposure (nos. 1 and 2) and a large number of CpGs that are differentially methylated in response to diesel exhaust (500 and 2827 CpGs in nos. 3 and 4, respectively).
Noncoding RNA (MiRNA and LncRNA)
Only 15 studies investigated the effect of air pollution on noncoding RNAs (ncRNAs) (Table 4), representing only 18% of the literature mined in this work (Fig. 2b). All these studies analyzed miRNAs except one that focused on lncRNAs (no. 15). Five studies had an experimental design (crossover; nos. 1, 6, and 8–10), while the remaining ten were observational studies (cohort and cross-sectional). Most of the studies investigated the effects of short-term exposure to air pollutants, while fewer focused on chronic exposures including the in utero time window (nos. 7, 11, and 15). All the studies examined adults, apart from two whose participants were newborns (no. 11) or school children (no. 13). Noncoding RNA was extracted from blood samples in ten reports, while lung tissue, bronchial brushing, sputum, saliva, and placenta samples were used in the remaining studies. Given the relatively small and diverse sample of publications available on ncRNAs and air pollution, it is difficult to currently draw generalizable conclusions. However, compared to DNA methylation, the ncRNA studies with observational and untargeted RNA approaches (RNA-seq or large panel of profiled ncRNAs) have been able to detect several significantly regulated ncRNAs in response to various air pollutants, even though their sample sizes were overall smaller (ranging between 22 and 1630 samples; median = 90; Table 3) relative to those reported with similar study designs on DNA methylation (ranging between 141 and 2956 samples, median = 839; Table 2). miR-21 was frequently reported to be associated with air pollution in different studies (Table 4).
Chromatin Regulation
Only two studies on chromatin modification related to environmental exposures were identified (Table 4). Both studies were carried out in China and used an observational design to investigate the association of personal (no. 17) and environmental PM (nos. 16 and 17) exposures on histone modifications in adult blood. One study characterized genome-wide profiles of histone H3 lysine 27 acetylation (H3K27ac) using chromatin immunoprecipitation sequencing but based on a small sample size (n = 4), while the other study measured candidate global histone H3 modifications (H3K9ac, H3K9me3, H3K27me3, and H3K36me3, with “me3” indicating trimethylation) via ELISA. Both studies showed that PM levels positively associate with a decondensed (i.e., active) chromatin structure around gene promoters, evidenced by increased H3K27ac (no. 16) or decreased H3K27me3 (no. 17) levels in those regions. Moreover, the PM2.5-associated differential H3K27ac markers were enriched in genes involved in immune cell activation (no. 16).
Discussion
We conducted a systematic review of the link between epigenetics and constituents of air pollution in humans. We identified 82 eligible manuscripts, among which 65 analyzed DNA methylation, 15 ncRNAs, and 2 chromatin modifications. In general, several studies profiling epigenome-wide associations as well as hypothesis-driven analyses show evidence that air pollution differentially affects epigenetic parameters at the genes that belong to various pathways including inflammation and immune system, DNA damage response, and cardiovascular and neurological functions. Because of their heritable but potentially reversible properties, epigenetic mechanisms have emerged as a promising biological explanation linking events and exposures across life to long-term health. Epigenetic alterations of stem cells in particular are believed to play a pivotal role in cell programming and may explain why exposures in early life can have effects that can be detectable later in life [105]. Since epigenetic changes can be mitotically heritable, distinct methylation patterns associated with air pollution could be considered as a memory of previous exposures that persist for decades [106]. One third of the studies identified in this work were performed in children or in newborns (Fig. 2a), with significant findings suggesting possible mechanisms underlying the developmental origin of health and disease (DOHaD) theory. Several novel CpG sites and mechanisms, which may create a molecular basis for the association between air pollution and health outcomes, have been detected (Tables 1, 2, 3, and 4), but more studies are needed to establish causality.
DNA Methylation
DNA methylation was the most widely investigated epigenetic mechanism among the screened studies. Though EWASs have proven to be powerful in identifying and replicating extensive exposure-associated epigenetic alterations, such as maternal tobacco smoke [107], results for particulate air pollution are still sparse and the magnitude of differential methylation detected is generally much lower compared to results found for smoking, which is also an airborne exposure. One reason likely lies in the fact that, apart from being a different type of exposure, air pollution levels are more prone to measurement error than smoking, and levels of exposure to air pollution are generally much lower than those related to direct and active inhalation of tobacco smoke. In particular, this work shows that most of the studies on air pollution are performed in countries with relatively low ambient levels of particulate air pollution.
Consistent evidence exists, however, in children and adults for a negative association between overall PM levels and global or L1 methylation, with less consistent findings regarding the methylation of Alu repetitive sequences. Methylation of repetitive elements represents almost 50% of global genomic methylation and has, therefore, been often used as proxy of global methylation [108]. However, the discrepancy identified in variations of L1 and Alu methylation in relation to air pollution is more in support to the emerging idea that each of these repetitive elements represents a distinct measure of dispersed methylation [109]. Global hypomethylation leads to genomic instability, which is a hallmark of several diseases, including cancer [110].
Effects sizes of air pollution exposure on DNA methylation are generally between 2 and 10%. The respective associations are often highly significant in terms of nominal p values. Since false-positive or false-negative findings in individual studies may arise by chance or bias, many EWASs include a validation strategy, e.g., discovery-replication (albeit not always significant) or a meta-analytical approach in which several studies have been analyzed by consortia (Tables 1 and 2). A consortium approach is powerful but is dependent on the research question and on the availability and compatibility of exposures and outcomes. Generated results are more stable despite population heterogeneity, and consortium analyses typically require a standardized protocol. In the largest birth cohort epigenetics consortium (n > 29000), the Pregnancy and Childhood Epigenetics cohort (PACE) [111], a validation at later time points in life is also included. The EXPOsOMICS consortium, albeit smaller than PACE, focuses on air and water pollution measures and includes several cohorts in different life stages, land-use regression modeling (mostly based on the ESCAPE protocols), and personal exposure measurements [112]. Also, other groups fruitfully joined forces, such as the Normative Aging Study and KORA [53]. Although large consortia exist on exposure and epigenetics, the nested cohorts with available air pollution data remain limited, with the maximum sample size attained so far being 2956 (no. 6, Table 2). There are still opportunities to combine the present studies and build a consortium providing even larger statistical power and including different geographical locations with high- and low-exposure levels.
Another means to increase statistical power in air pollution-methylation associations is by reducing the dimension of the methylome into clusters of genomically proximal CpG sites exhibiting correlated methylation levels and termed as differentially methylated regions (DMRs). Only a few studies implemented DMRs in their studies. One example is a study on short-term and long-term exposures to high levels of CO, NO2, and PM2.5 that showed alterations in DMRs of FOXP3 and to a lower extent IL-10 [36]. Another study identified using a panel design a larger number of DMRs in 24 h personal monitoring relative to ambient exposure levels of each of PM2.5, soot and ultrafine particles [49••].
Noncoding RNA (miRNA and lncRNA)
The miRNAs that were most frequently identified via agnostic studies were hsa-miR-30 and hsa-miR-223 (in 4 studies), while hsa-miR-21, hsa-miR-146a, and hsa-miR-222 were the miRNAs most frequently identified via targeted studies (≥ 5 studies). Prominent associated pathways with these miRNAs are cancer [113, 114], hematopoiesis [115], heart disease [116, 117], inflammation, and immune system [118]. The first published study on miRNAs and air pollution was a crossover study on diesel exhaust exposure in 2013 and reported that miR-21 was significantly downregulated after exposure [94]. Hou and colleagues identified this miRNA in a nontargeted study in truck drivers, and four targeted studies (Table 1) also reported a significant association with particulate matter exposure [89]. miR-21 is frequently upregulated in tumors and plays a role in the development of heart diseases [119].
Only one study investigated lncRNAs and air pollution [100]. LncRNAs have emerged from obscurity to being recognized as a mechanism of genetic regulation. In cancer biology, the recent application of next-generation sequencing revealed a growing number of lncRNAs whose expression is associated with different cancer types. In addition, the field is moving from annotation of lncRNAs in various tumors toward understanding their importance in key cancer signaling networks [120, 121]. So far, no study has included epitranscriptomics, that is, all functionally relevant changes to the transcriptome that do not involve a change in the ribonucleotide sequence [122].
Chromatin Regulation
Two studies focused on chromatin remodeling by means of histone modifications. Specific modifications on histone proteins have been linked to chemical exposures such as nickel or arsenic [123] as well as oxidative stress [124] and inflammation [125]. The study of Zheng and colleagues identified in office workers that H3K9ac and H3K36me3 were associated with black carbon exposure [102]. These findings and their role in the pathway from exposure to disease should be further assessed in future studies.
Multiomics Integration
The identification of DNA methylation, ncRNA, and histone modification signals provides a better understanding of the health risks associated with air pollution such as cardiovascular disease and cancer. More (prospective) studies should, however, be performed to assess their causal role in air pollution-associated outcomes.
Different epigenetic layers can largely interact, and epigenetics may also exhibit reciprocal relations with other biological networks. However, only a few studies included more than one molecular layer of epigenetics or other omics, for example combining DNA methylation with gene expression [49••, 54], with inflammatory protein levels [7, 49••], or with genetic variation [27]. The contribution of different molecular levels to the effects of air pollution warrants further investigation.
Mitochondrial Epigenetics
Research on mitochondrial epigenetics especially DNA methylation is not as common nor as well understood as nuclear methylation. So far, two studies focused on mitochondrial DNA (mtDNA) methylation: (i) levels in the blood of boiler makers were negatively associated with PM2.5 exposure and modified the adverse relationships between PM2.5 exposure and heart rate variability outcomes [126]; and (ii) in a mother-newborn cohort, placental mtDNA methylation substantially mediated the association between PM2.5 exposure during gestation and mtDNA content in placental tissue, which could reflect signs of mitophagy and mitochondrial senescence [31]. Both studies proved that the mitochondrial methylome is subject to environmental influences and provide important indications to unravel the role of mtDNA methylation.
Individual Air Pollution Species
Currently, there is a paucity of knowledge about the contribution of individual air particulates. So far, evidence suggests different relative toxicities of PM species: one methylome-wide analysis performed on different sorts of PM2.5 in the Normative Aging Study identified a handful of CpG sites associated with Fe, Ni, and V [51], and a targeted study on repair genes and components of PM10 in a school showed significant CpG sites associated with acenaphthene, indeno[1,2,3-cd]pyrene, and pyrene [37]. Various studies observed distinct epigenetic alterations in response to different components of air pollution, including particle size and gases. An EWAS study of the European Prospective Investigation into Cancer and Nutrition (EPIC) on exposure to different particle sizes (PM10; coarse PM, subset of PM10 that is larger than 2.5 μm; and PM2.5), soot (absorbance of the PM2.5 filter), NOx, and NO2 described only limited similarity among the CpG sites that are differentially methylated in response to each exposure [54]. The Oxford street study, with an experimental crossover design, revealed different sets of miRNAs associated with each of NO2, ultrafine particles, PM2.5, PM10, and black carbon [86••]. A targeted study using pyrosequencing of DNA damage and P53 genes in the ENVIRONAGE cohort included residential PM2.5, black carbon, and NO2 exposures and also showed different epigenetic changes in response to these exposures [35].
Study Design
Most studies had an observational nature, having mainly cohort (42%) or cross-sectional designs (27%), while 12 studies incorporated an intervention. The Oxford street study previously demonstrated the adverse effect of traffic-related exposure to air pollution [127] but recently identified circulating miRNAs involved in the molecular processes of exposure-related diseases [86••]. An exciting result concerning preventative measures was also demonstrated via a human intervention trial demonstrating that acute ambient PM2.5-induced DNA methylation changes can be reversed by B-vitamin supplementation [80] as methyl donors. These intervention studies analyzed small sample sizes and low level of exposures and identified heterogeneous epigenetic signals in response to air pollution, thus, limiting the confidence that may be placed on their findings. In this regard, panel studies that allow investigation of repeated measures from the same individuals may be more advantageous to study the biological effect of air pollution, especially for short-term effects. Of note, among the five studies using a panel design, one performed a methylome-wide analysis and found an association between 24-h personal exposure to air pollution and DNA methylation both at single sites and regional clusters [49••].
Sample Type
The majority of studies have relied on blood or cord blood samples (74%) as surrogate tissues, while some included invasive tissues such as breast or the target tissue being lung. Tissue-/cell-type-specific profiles are particularly important in epigenetic studies because of the driver role epigenetics plays in tissue differentiation and lineage specializing. Caution is recommended in the interpretation of findings as associations of epigenetic profiles with air pollution might be explained by variations in the distribution of different cell types within the analyzed tissue. In this regard, recent advances in bioinformatics have helped correct for possible changes in cell subpopulations using DNA methylome-based deconvolution algorithms that rely on reference tissues (mostly peripheral, the Houseman algorithm [128]; and cord blood, the Bakulski algorithm [129]) and reference-free methods (a recent but rapidly developing field [130]). However, only half of the studies we reviewed in adults, and even less in children, adjusted findings for cell-type composition or proportion of leucocytes or neutrophils. In addition, changes in minor immune cell subtypes not covered by deconvolution algorithms may also bias DNA methylation analyses’ results [131]. Biological matrices that are noninvasive might serve as an excellent source for human samples but are currently underexplored, e.g., exposure-related epigenetic alterations have been recently found in placenta tissues [40, 132], saliva [98, 133], and blood spots [41].
Conclusion
Over the last decade, considerable progress has been made in environmental epigenetics including the introduction of agnostic studies with accompanying technological advancements. Evidence that exposure to air pollution is linked to epigenetic changes has been provided by several studies; however, most of these biomarkers have not yet been validated and their role in the causal paradigm is not yet clear. An additional challenge would be the integration of multiple epigenetic layers in this rapidly evolving field, which we are just beginning to understand. The major findings and related future directions described above are summarized in Fig. 3. This work provides a timely guide into the existing evidence, the missing gaps, and possible next steps forward.
Summary of the major observations and findings derived from the review of the literature on the impact of air pollution on epigenetic mechanisms. For every finding, the corresponding possible next step is suggested. DMR: differentially methylated region; EWAS: epigenome-wide association study; ncRNA: noncoding RNA; lncRNA: long noncoding RNA; L1: LINE-1; PM: particulate matter; WHO: World Health Organization
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
Cohen AJ, Brauer M, Burnett R, Anderson HR, Frostad J, Estep K, et al. Estimates and 25-year trends of the global burden of disease attributable to ambient air pollution: an analysis of data from the Global Burden of Diseases Study 2015. Lancet. 2017;389(10082):1907–18. https://doi.org/10.1016/S0140-6736(17)30505-6.
WHO. WHO Global Urban Ambient Air Pollution 2016 Database http://www.who.int/phe/health_topics/outdoorair/databases/cities/en/. 2016.
Silva RA, West JJ, Lamarque J-F, Shindell DT, Collins WJ, Faluvegi G, et al. Future global mortality from changes in air pollution attributable to climate change. Nat Clim Chang. 2017;7(9):647–51. https://doi.org/10.1038/nclimate3354.
Forman HJ, Finch CE. A critical review of assays for hazardous components of air pollution. Free Radic Biol Med. 2018;117:202–17. https://doi.org/10.1016/j.freeradbiomed.2018.01.030.
Brook RD, Rajagopalan S, Pope CA 3rd, Brook JR, Bhatnagar A, Diez-Roux AV, et al. Particulate matter air pollution and cardiovascular disease: an update to the scientific statement from the American Heart Association. Circulation. 2010;121(21):2331–78. https://doi.org/10.1161/CIR.0b013e3181dbece1.
Nawrot TS, Perez L, Kunzli N, Munters E, Nemery B. Public health importance of triggers of myocardial infarction: a comparative risk assessment. Lancet. 2011;377(9767):732–40. https://doi.org/10.1016/S0140-6736(10)62296-9.
Fiorito G, Vlaanderen J, Polidoro S, Gulliver J, Galassi C, Ranzi A, et al. Oxidative stress and inflammation mediate the effect of air pollution on cardio- and cerebrovascular disease: a prospective study in nonsmokers. Environ Mol Mutagen. 2018;59(3):234–46. https://doi.org/10.1002/em.22153.
Hoek G, Krishnan RM, Beelen R, Peters A, Ostro B, Brunekreef B, et al. Long-term air pollution exposure and cardio- respiratory mortality: a review. Environ Health. 2013;12(1):43. https://doi.org/10.1186/1476-069X-12-43.
Hamra GB, Guha N, Cohen A, Laden F, Raaschou-Nielsen O, Samet JM, et al. Outdoor particulate matter exposure and lung cancer: a systematic review and meta-analysis. Environ Health Perspect. 2014;122(9):906–11. https://doi.org/10.1289/ehp.1408092.
Loomis D, Grosse Y, Lauby-Secretan B, El Ghissassi F, Bouvard V, Benbrahim-Tallaa L, et al. The carcinogenicity of outdoor air pollution. Lancet Oncol. 2013;14(13):1262–3.
Clifford A, Lang L, Chen R, Anstey KJ, Seaton A. Exposure to air pollution and cognitive functioning across the life course—a systematic literature review. Environ Res. 2016;147:383–98. https://doi.org/10.1016/j.envres.2016.01.018.
Saenen ND, Plusquin M, Bijnens E, Janssen BG, Gyselaers W, Cox B, et al. In utero fine particle air pollution and placental expression of genes in the brain-derived neurotrophic factor signaling pathway: an ENVIRONAGE birth cohort study. Environ Health Perspect. 2015;123(8):834–40. https://doi.org/10.1289/ehp.1408549.
Lanki T, Pekkanen J, Aalto P, Elosua R, Berglind N, D'Ippoliti D, et al. Associations of traffic related air pollutants with hospitalisation for first acute myocardial infarction: the HEAPSS study. Occup Environ Med. 2006;63(12):844–51. https://doi.org/10.1136/oem.2005.023911.
Harris MH, Gold DR, Rifas-Shiman SL, Melly SJ, Zanobetti A, Coull BA, et al. Prenatal and childhood traffic-related air pollution exposure and childhood executive function and behavior. Neurotoxicol Teratol. 2016;57:60–70. https://doi.org/10.1016/j.ntt.2016.06.008.
Saenen ND, Provost EB, Viaene MK, Vanpoucke C, Lefebvre W, Vrijens K, et al. Recent versus chronic exposure to particulate matter air pollution in association with neurobehavioral performance in a panel study of primary schoolchildren. Environ Int. 2016;95:112–9. https://doi.org/10.1016/j.envint.2016.07.014.
Goodson JM, Weldy CS, MacDonald JW, Liu Y, Bammler TK, Chien WM, et al. In utero exposure to diesel exhaust particulates is associated with an altered cardiac transcriptional response to transverse aortic constriction and altered DNA methylation. FASEB Journal. 2017;31(11):4935–45. https://doi.org/10.1096/fj.201700032R.
•• Plusquin M, Chadeau-Hyam M, Ghantous A, Alfano R, Bustamante M, Chatzi L, et al. DNA methylome marks of exposure to particulate matter at three time points in early life. Environ Sci Technol. 2018;52(9):5427–37. https://doi.org/10.1021/acs.est.7b06447 Using longitudinal measurements of blood DNA methylation from birth to adolescence provides evidence that residential PM10 exposure affects methylation of sites involved in neurological and cell division control mechanism.
Martens DS, Cox B, Janssen BG, Clemente DBP, Gasparrini A, Vanpoucke C, et al. Prenatal air pollution and newborns’ predisposition to accelerated biological aging. JAMA Pediatr. 2017;171(12):1160–7. https://doi.org/10.1001/jamapediatrics.2017.3024.
Waterland RA, Michels KB. Epigenetic epidemiology of the developmental origins hypothesis. Annu Rev Nutr. 2007;27:363–88. https://doi.org/10.1146/annurev.nutr.27.061406.093705.
Rakyan VK, Down TA, Balding DJ, Beck S. Epigenome-wide association studies for common human diseases. Nat Rev Genet. 2011;12(8):529–41. https://doi.org/10.1038/nrg3000.
Jones PA, Liang G. The human epigenome. In: Michels KB, editor. Epigentic epidemiology. 1 ed.: Springer, Dordrecht; 2012. p. 5–20.
Herceg Z, Ghantous A, Wild CP, Sklias A, Casati L, Duthie SJ, et al. Roadmap for investigating epigenome deregulation and environmental origins of cancer. Int J Cancer. 2018;142(5):874–82. https://doi.org/10.1002/ijc.31014.
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008;61(4):344–9. https://doi.org/10.1016/j.jclinepi.2007.11.008.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol. 2009;62(10):1006–12. https://doi.org/10.1016/j.jclinepi.2009.06.005.
Abraham E, Rousseaux S, Agier L, Giorgis-Allemand L, Tost J, Galineau J, et al. Pregnancy exposure to atmospheric pollution and meteorological conditions and placental DNA methylation. Environ Int. 2018;118:334–47. https://doi.org/10.1016/j.envint.2018.05.007.
Gruzieva O, Xu CJ, Breton CV, Annesi-Maesano I, Antó JM, Auffray C, et al. Epigenome-wide meta-analysis of methylation in children related to prenatal NO2 air pollution exposure. Environ Health Perspect. 2017;125(1):104–10. https://doi.org/10.1289/EHP36.
Breton CV, Gao L, Yao J, Siegmund KD, Lurmann F, Gilliland F. Particulate matter, the newborn methylome, and cardio-respiratory health outcomes in childhood. Environ Epigenetics. 2016;2(2):dvw005. https://doi.org/10.1093/eep/dvw005.
Goodrich JM, Reddy P, Naidoo RN, Asharam K, Batterman S, Dolinoy DC. Prenatal exposures and DNA methylation in newborns: a pilot study in Durban, South Africa. Environ Sci. 2016;18(7):908–17. https://doi.org/10.1039/c6em00074f.
Rossnerova A, Tulupova E, Tabashidze N, Schmuczerova J, Dostal M, Rossner Jr P et al. Factors affecting the 27K DNA methylation pattern in asthmatic and healthy children from locations with various environments. Mutation Research - Fundamental and Molecular Mechanisms of Mutagenesis. 2013;741–742:18–26. doi:https://doi.org/10.1016/j.mrfmmm.2013.02.003.
Maghbooli Z, Hossein-Nezhad A, Adabi E, Asadollah-Pour E, Sadeghi M, Mohammad-Nabi S, et al. Air pollution during pregnancy and placental adaptation in the levels of global DNA methylation. PLoS One. 2018;13(7):e0199772. https://doi.org/10.1371/journal.pone.0199772.
Janssen BG, Byun HM, Gyselaers W, Lefebvre W, Baccarelli AA, Nawrot TS. Placental mitochondrial methylation and exposure to airborne particulate matter in the early life environment: an ENVIRONAGE birth cohort study. Epigenetics. 2015;10(6):536–44. https://doi.org/10.1080/15592294.2015.1048412.
Herbstman JB, Tang D, Zhu D, Qu L, Sjodin A, Li Z, et al. Prenatal exposure to polycyclic aromatic hydrocarbons, benzo[a]pyrene-DNA adducts, and genomic DNA methylation in cord blood. Environ Health Perspect. 2012;120(5):733–8. https://doi.org/10.1289/ehp.1104056.
Li Y, Mu Z, Wang H, Liu J, Jiang F. The role of particulate matters on methylation of IFN-γ and IL-4 promoter genes in pediatric allergic rhinitis. Oncotarget. 2018;9(25):17406–19. https://doi.org/10.18632/oncotarget.24227.
Nawrot TS, Saenen ND, Schenk J, Janssen BG, Motta V, Tarantini L, et al. Placental circadian pathway methylation and in utero exposure to fine particle air pollution. Environ Int. 2018;114:231–41. https://doi.org/10.1016/j.envint.2018.02.034.
Neven KY, Saenen ND, Tarantini L, Janssen BG, Lefebvre W, Vanpoucke C, et al. Placental promoter methylation of DNA repair genes and prenatal exposure to particulate air pollution: an ENVIRONAGE cohort study. Lancet Planetary Health. 2018;2(4):e174–e83. https://doi.org/10.1016/s2542-5196(18)30049-4.
Prunicki M, Stell L, Dinakarpandian D, de Planell-Saguer M, Lucas RW, Hammond SK, et al. Exposure to NO2, CO, and PM2.5 is linked to regional DNA methylation differences in asthma. Clin Epigenetics. 2018;10:2. https://doi.org/10.1186/s13148-017-0433-4.
Alvarado-Cruz I, Sanchez-Guerra M, Hernandez-Cadena L, De Vizcaya-Ruiz A, Mugica V, Pelallo-Martinez NA, et al. Increased methylation of repetitive elements and DNA repair genes is associated with higher DNA oxidation in children in an urbanized, industrial environment. Mutat Res. 2017;813:27–36. https://doi.org/10.1016/j.mrgentox.2016.11.007.
Cai J, Zhao Y, Liu P, Xia B, Zhu Q, Wang X et al. Exposure to particulate air pollution during early pregnancy is associated with placental DNA methylation. Sci Total Environ. 2017;607–608:1103–8. doi:https://doi.org/10.1016/j.scitotenv.2017.07.029.
Lovinsky-Desir S, Jung KH, Jezioro JR, Torrone DZ, de Planell-Saguer M, Yan B, et al. Physical activity, black carbon exposure, and DNA methylation in the FOXP3 promoter. Clin Epigenetics. 2017;9(1):65. https://doi.org/10.1186/s13148-017-0364-0.
Saenen ND, Vrijens K, Janssen BG, Roels HA, Neven KY, Vanden Berghe W, et al. Lower placental leptin promoter methylation in association with fine particulate matter air pollution during pregnancy and placental nitrosative stress at birth in the ENVIRONAGE cohort. Environ Health Perspect. 2017;125(2):262–8. https://doi.org/10.1289/EHP38.
Breton CV, Yao J, Millstein J, Gao L, Siegmund KD, Mack W, et al. Prenatal air pollution exposures, DNA methyl transferase genotypes, and associations with newborn line1 and Alu methylation and childhood blood pressure and carotid intima-media thickness in the children’s health study. Environ Health Perspect. 2016;124(12):1905–12. https://doi.org/10.1289/EHP181.
Somineni HK, Zhang X, Biagini Myers JM, Kovacic MB, Ulm A, Jurcak N, et al. Ten-eleven translocation 1 (TET1) methylation is associated with childhood asthma and traffic-related air pollution. J Allergy Clin Immunol. 2016;137(3):797–805.e5. https://doi.org/10.1016/j.jaci.2015.10.021.
Hew KM, Walker AI, Kohli A, Garcia M, Syed A, McDonald-Hyman C, et al. Childhood exposure to ambient polycyclic aromatic hydrocarbons is linked to epigenetic modifications and impaired systemic immunity in T cells. Clin Exp Allergy. 2015;45(1):238–48. https://doi.org/10.1111/cea.12377.
Breton CV, Salam MT, Wang X, Byun HM, Siegmund KD, Gilliland FD. Particulate matter, DNA methylation in nitric oxide synthase, and childhood respiratory disease. Environ Health Perspect. 2012;120(9):1320–6. https://doi.org/10.1289/ehp.1104439.
Salam MT, Byun HM, Lurmann F, Breton CV, Wang X, Eckel SP, et al. Genetic and epigenetic variations in inducible nitric oxide synthase promoter, particulate pollution, and exhaled nitric oxide levels in children, J Allergy Clin Immunol. 2012;129(1):232–9.e7. https://doi.org/10.1016/j.jaci.2011.09.037.
Tang WY, Levin L, Talaska G, Cheung YY, Herbstman J, Tang D et al. Maternal exposure to polycyclic aromatic hydrocarbons and 5′-CpG methylation of interferon-γ in cord white blood cells. Environ Health Perspect 2012;120(8):1195–1200. doi:https://doi.org/10.1289/ehp.1103744.
Nadeau K, McDonald-Hyman C, Noth EM, Pratt B, Hammond SK, Balmes J, et al. Ambient air pollution impairs regulatory T-cell function in asthma. J Allergy Clin Immunol. 2010;126(4):845–52.e10. https://doi.org/10.1016/j.jaci.2010.08.008.
Perera F, Tang WY, Herbstman J, Tang D, Levin L, Miller R et al. Relation of DNA methylation of 5′-CpG island of ACSL3 to transplacental exposure to airborne polycyclic aromatic hydrocarbons and childhood asthma. PLoS One 2009;4(2):e4488. doi:https://doi.org/10.1371/journal.pone.0004488.
•• Mostafavi N, Vermeulen R, Ghantous A, Hoek G, Probst-Hensch N, Herceg Z, et al. Acute changes in DNA methylation in relation to 24h personal air pollution exposure measurements: a panel study in four European countries. Environ Int. 2018;120:11–21. https://doi.org/10.1016/j.envint.2018.07.026 Using panel design revealed an association between 24-hour personal exposure to air pollution and DNA-methylation both at single sites and regional clusters.
Lichtenfels AJFC, Van Der Plaat DA, De Jong K, Van Diemen CC, Postma DS, Nedeljkovic I, et al. Long-term air pollution exposure, genome-wide DNA methylation and lung function in the lifelines cohort study. Environ Health Perspect. 2018;126(2):027004. https://doi.org/10.1289/EHP2045.
Dai L, Mehta A, Mordukhovich I, Just AC, Shen J, Hou L, et al. Differential DNA methylation and PM2.5 species in a 450K epigenome-wide association study. Epigenetics. 2017;12(2):139–48. https://doi.org/10.1080/15592294.2016.1271853.
Nwanaji-Enwerem JC, Dai L, Colicino E, Oulhote Y, Di Q, Kloog I, et al. Associations between long-term exposure to PM2.5 component species and blood DNA methylation age in the elderly: the VA normative aging study. Environ Int. 2017;102:57–65. https://doi.org/10.1016/j.envint.2016.12.024.
•• Panni T, Mehta AJ, Schwartz JD, Baccarelli AA, Just AC, Wolf K, et al. Genome-wide analysis of DNA methylation and fine particulate matter air pollution in three study populations: KORA F3, KORA F4, and the Normative Aging Study. Environ Health Perspect. 2016;124(7):983–90. https://doi.org/10.1289/ehp.1509966 Combining evidence from three independent adult cohorts suggests novel plausible systemic pathways linking ambient PM exposure to adverse health effect through variations in DNA methylation.
Plusquin M, Guida F, Polidoro S, Vermeulen R, Raaschou-Nielsen O, Campanella G, et al. DNA methylation and exposure to ambient air pollution in two prospective cohorts. Environ Int. 2017;108:127–36. https://doi.org/10.1016/j.envint.2017.08.006.
Chi GC, Liu Y, MacDonald JW, Barr RG, Donohue KM, Hensley MD, et al. Long-term outdoor air pollution and DNA methylation in circulating monocytes: results from the multi-ethnic study of atherosclerosis (MESA). Environ Health. 2016;15(1):119. https://doi.org/10.1186/s12940-016-0202-4.
Nwanaji-Enwerem JC, Colicino E, Trevisi L, Kloog I, Just AC, Shen J et al. Long-term ambient particle exposures and blood DNA methylation age: findings from the VA normative aging study. Environ Epigenetics. 2016;2(2). doi:https://doi.org/10.1093/eep/dvw006.
Ward-Caviness CK, Nwanaji-Enwerem JC, Wolf K, Wahl S, Colicino E, Trevisi L, et al. Long-term exposure to air pollution is associated with biological aging. Oncotarget. 2016;7(46):74510–25. https://doi.org/10.18632/oncotarget.12903.
Carmona JJ, Sofer T, Hutchinson J, Cantone L, Coull B, Maity A, et al. Short-term airborne particulate matter exposure alters the epigenetic landscape of human genes associated with the mitogen-activated protein kinase network: a cross-sectional study. Environ Health. 2014;13(1):94. https://doi.org/10.1186/1476-069X-13-94.
De Nys S, Duca RC, Nawrot T, Hoet P, Van Meerbeek B, Van Landuyt KL, et al. Temporal variability of global DNA methylation and hydroxymethylation in buccal cells of healthy adults: association with air pollution. Environ Int. 2018;111:301–8. https://doi.org/10.1016/j.envint.2017.11.002.
Liu J, Xie K, Chen W, Zhu M, Shen W, Yuan J, et al. Genetic variants, PM2.5 exposure level and global DNA methylation level: a multi-center population-based study in Chinese. Toxicol Lett. 2017;269:77–82. https://doi.org/10.1016/j.toxlet.2017.02.003.
Sanchez-Guerra M, Zheng Y, Osorio-Yanez C, Zhong J, Chervona Y, Wang S, et al. Effects of particulate matter exposure on blood 5-hydroxymethylation: results from the Beijing truck driver air pollution study. Epigenetics. 2015;10(7):633–42. https://doi.org/10.1080/15592294.2015.1050174.
De Prins S, Koppen G, Jacobs G, Dons E, Van de Mieroop E, Nelen V, et al. Influence of ambient air pollution on global DNA methylation in healthy adults: a seasonal follow-up. Environ Int. 2013;59:418–24. https://doi.org/10.1016/j.envint.2013.07.007.
Wang C, Chen R, Shi M, Cai J, Shi J, Yang C, et al. Possible mediation by methylation in acute inflammation following personal exposure to fine particulate air pollution. Am J Epidemiol. 2018;187(3):484–93. https://doi.org/10.1093/aje/kwx277.
Wang C, Chen R, Cai J, Shi J, Yang C, Tse LA, et al. Personal exposure to fine particulate matter and blood pressure: a role of angiotensin converting enzyme and its DNA methylation. Environ Int. 2016;94:661–6. https://doi.org/10.1016/j.envint.2016.07.001.
Sofer T, Maity A, Coull B, Baccarelli A, Schwartz J, Lin X. Multivariate gene selection and testing in studying the exposure effects on a gene set. Stat Biosci. 2012;4(2):319–38. https://doi.org/10.1007/s12561-012-9072-7.
Peng C, Bind MAC, Colicino E, Kloog I, Byun HM, Cantone L, et al. Particulate air pollution and fasting blood glucose in nondiabetic individuals: associations and epigenetic mediation in the normative aging study, 2000-2011. Environ Health Perspect. 2016;124(11):1715–21. https://doi.org/10.1289/EHP183.
Ouyang B, Baxter CS, Lam HM, Yeramaneni S, Levin L, Haynes E, et al. Hypomethylation of dual specificity phosphatase 22 promoter correlates with duration of service in firefighters and is inducible by low-dose benzo[a]pyrene. J Occup Environ Med. 2012;54(7):774–80. https://doi.org/10.1097/JOM.0b013e31825296bc.
Madrigano J, Baccarelli A, Mittleman MA, Sparrow D, Spiro A, Vokonas PS, et al. Air pollution and DNA methylation: interaction by psychological factors in the VA normative aging study. Am J Epidemiol. 2012;176(3):224–32. https://doi.org/10.1093/aje/kwr523.
Madrigano J, Baccarelli A, Mittleman MA, Wright RO, Sparrow D, Vokonas PS, et al. Prolonged exposure to particulate pollution, genes associated with glutathione pathways, and DNA methylation in a cohort of older men. Environ Health Perspect. 2011;119(7):977–82. https://doi.org/10.1289/ehp.1002773.
Liu Y, Lan Q, Shen M, Jin J, Mumford J, Ren D, et al. Aberrant gene promoter methylation in sputum from individuals exposed to smoky coal emissions. Anticancer Res. 2008;28(4 B):2061–6.
Lepeule J, Bind MA, Baccarelli AA, Koutrakis P, Tarantini L, Litonjua A, et al. Epigenetic influences on associations between air pollutants and lung function in elderly men: the normative aging study. Environ Health Perspect. 2014;122(6):566–72. https://doi.org/10.1289/ehp.1206458.
Hou L, Zhang X, Zheng Y, Wang S, Dou C, Guo L, et al. Altered methylation in tandem repeat element and elemental component levels in inhalable air particles. Environ Mol Mutagen. 2014;55(3):256–65. https://doi.org/10.1002/em.21829.
Guo L, Byun HM, Zhong J, Motta V, Barupal J, Zheng Y, et al. Effects of short-term exposure to inhalable particulate matter on DNA methylation of tandem repeats. Environ Mol Mutagen. 2014;55(4):322–35. https://doi.org/10.1002/em.21838.
Chen R, Qiao L, Li H, Zhao Y, Zhang Y, Xu W, et al. Fine particulate matter constituents, nitric oxide synthase DNA methylation and exhaled nitric oxide. Environ Sci Technol. 2015;49(19):11859–65. https://doi.org/10.1021/acs.est.5b02527.
Cantone L, Iodice S, Tarantini L, Albetti B, Restelli I, Vigna L, et al. Particulate matter exposure is associated with inflammatory gene methylation in obese subjects. Environ Res. 2017;152:478–84. https://doi.org/10.1016/j.envres.2016.11.002.
Callahan CL, Bonner MR, Nie J, Han D, Wang Y, Tao MH, et al. Lifetime exposure to ambient air pollution and methylation of tumor suppressor genes in breast tumors. Environ Res. 2018;161:418–24. https://doi.org/10.1016/j.envres.2017.11.040.
Bind MA, Coull BA, Peters A, Baccarelli AA, Tarantini L, Cantone L, et al. Beyond the mean: quantile regression to explore the association of air pollution with gene-specific methylation in the Normative Aging Study. Environ Health Perspect. 2015;123(8):759–65. https://doi.org/10.1289/ehp.1307824.
Bind MA, Lepeule J, Zanobetti A, Gasparrini A, Baccarelli A, Coull BA, et al. Air pollution and gene-specific methylation in the Normative Aging Study: association, effect modification, and mediation analysis. Epigenetics. 2014;9(3):448–58. https://doi.org/10.4161/epi.27584.
Baccarelli A, Wright RO, Bollati V, Tarantini L, Litonjua AA, Suh HH, et al. Rapid DNA methylation changes after exposure to traffic particles. Am J Respir Crit Care Med. 2009;179(7):572–8. https://doi.org/10.1164/rccm.200807-1097OC.
Zhong J, Karlsson O, Wang G, Li J, Guo Y, Lin X, et al. B vitamins attenuate the epigenetic effects of ambient fine particles in a pilot human intervention trial. Proc Natl Acad Sci U S A. 2017;114(13):3503–8. https://doi.org/10.1073/pnas.1618545114.
Clifford RL, Jones MJ, MacIsaac JL, McEwen LM, Goodman SJ, Mostafavi S, et al. Inhalation of diesel exhaust and allergen alters human bronchial epithelium DNA methylation. J Allergy Clin Immunol. 2017;139(1):112–21. https://doi.org/10.1016/j.jaci.2016.03.046.
Jiang R, Jones MJ, Sava F, Kobor MS, Carlsten C. Short-term diesel exhaust inhalation in a controlled human crossover study is associated with changes in DNA methylation of circulating mononuclear cells in asthmatics. Particle Fibre Toxicol. 2014;11(1):71. https://doi.org/10.1186/s12989-014-0071-3.
Tobaldini E, Bollati V, Prado M, Fiorelli EM, Pecis M, Bissolotti G, et al. Acute particulate matter affects cardiovascular autonomic modulation and IFN-Γ methylation in healthy volunteers. Environ Res. 2018;161:97–103. https://doi.org/10.1016/j.envres.2017.10.036.
Chen R, Meng X, Zhao A, Wang C, Yang C, Li H, et al. DNA hypomethylation and its mediation in the effects of fine particulate air pollution on cardiovascular biomarkers: a randomized crossover trial. Environ Int. 2016;94:614–9. https://doi.org/10.1016/j.envint.2016.06.026.
Bellavia A, Urch B, Speck M, Brook RD, Scott JA, Albetti B, et al. DNA hypomethylation, ambient particulate matter, and increased blood pressure: findings from controlled human exposure experiments. J Am Heart Assoc. 2013;2(3):e000212. https://doi.org/10.1161/JAHA.113.000212.
•• Krauskopf J, Caiment F, van Veldhoven K, Chadeau-Hyam M, Sinharay R, Chung KF, et al. The human circulating miRNome reflects multiple organ disease risks in association with short-term exposure to traffic-related air pollution. Environ Int. 2018;113:26–34. https://doi.org/10.1016/j.envint.2018.01.014 Proposes cmiRNA signature comprised of organ-enriched miRNAs as a highly specific candidate for biomarker-based health risk assessment allowing the early detection and prevention of TRAP-induced health outcomes.
Liu PF, Yan P, Zhao DH, Shi WF, Meng S, Liu Y, et al. The effect of environmental factors on the differential expression of miRNAs in patients with chronic obstructive pulmonary disease: a pilot clinical study. Int J Chronic Obstructive Pulmonary Dis. 2018;13:741–51. https://doi.org/10.2147/copd.S156865.
Pergoli L, Cantone L, Favero C, Angelici L, Iodice S, Pinatel E, et al. Extracellular vesicle-packaged miRNA release after short-term exposure to particulate matter is associated with increased coagulation. Particle and fibre toxicology. 2017;14(1):32. https://doi.org/10.1186/s12989-017-0214-4.
Hou L, Barupal J, Zhang W, Zheng Y, Liu L, Zhang X, et al. Particulate air pollution exposure and expression of viral and human microRNAs in blood: the Beijing Truck Driver Air Pollution Study. Environ Health Perspect. 2016;124(3):344–50. https://doi.org/10.1289/ehp.1408519.
Motta V, Favero C, Dioni L, Iodice S, Battaglia C, Angelici L, et al. MicroRNAs are associated with blood-pressure effects of exposure to particulate matter: results from a mediated moderation analysis. Environ Res. 2016;146:274–81. https://doi.org/10.1016/j.envres.2016.01.010.
Rider CF, Yamamoto M, Gunther OP, Hirota JA, Singh A, Tebbutt SJ, et al. Controlled diesel exhaust and allergen coexposure modulates microRNA and gene expression in humans: effects on inflammatory lung markers. J Allergy Clin Immunol. 2016;138(6):1690–700. https://doi.org/10.1016/j.jaci.2016.02.038.
Rodosthenous RS, Coull BA, Lu Q, Vokonas PS, Schwartz JD, Baccarelli AA. Ambient particulate matter and microRNAs in extracellular vesicles: a pilot study of older individuals. Particle Fibre Toxicol. 2016;13:13. https://doi.org/10.1186/s12989-016-0121-0.
Fry RC, Rager JE, Bauer R, Sebastian E, Peden DB, Jaspers I, et al. Air toxics and epigenetic effects: ozone altered microRNAs in the sputum of human subjects. Am J Physiol Lung Cell Mol Physiol. 2014;306(12):L1129–L37. https://doi.org/10.1152/ajplung.00348.2013.
Yamamoto M, Singh A, Sava F, Pui M, Tebbutt SJ, Carlsten C. MicroRNA expression in response to controlled exposure to diesel exhaust: attenuation by the antioxidant N-acetylcysteine in a randomized crossover study. Environ Health Perspect. 2013;121(6):670–5. https://doi.org/10.1289/ehp.1205963.
Chen R, Li H, Cai J, Wang C, Lin Z, Liu C, et al. Fine particulate air pollution and the expression of microRNAs and circulating cytokines relevant to inflammation, coagulation, and vasoconstriction. Environ Health Perspect. 2018;126(1):017007. https://doi.org/10.1289/EHP1447.
Tsamou M, Vrijens K, Madhloum N, Lefebvre W, Vanpoucke C, Nawrot TS. Air pollution-induced placental epigenetic alterations in early life: a candidate miRNA approach. Epigenetics. 2018:1–12. https://doi.org/10.1080/15592294.2016.1155012.
Louwies T, Vuegen C, Panis LI, Cox B, Vrijens K, Nawrot TS, et al. miRNA expression profiles and retinal blood vessel calibers are associated with short-term particulate matter air pollution exposure. Environ Res. 2016;147:24–31. https://doi.org/10.1016/j.envres.2016.01.027.
Vriens A, Nawrot TS, Saenen ND, Provost EB, Kicinski M, Lefebvre W, et al. Recent exposure to ultrafine particles in school children alters miR-222 expression in the extracellular fraction of saliva. Environ Health. 2016;15(1):80. https://doi.org/10.1186/s12940-016-0162-8.
Fossati S, Baccarelli A, Zanobetti A, Hoxha M, Vokonas PS, Wright RO, et al. Ambient particulate air pollution and microRNAs in elderly men. Epidemiology (Cambridge, Mass). 2014;25(1):68–78. https://doi.org/10.1097/EDE.0000000000000026.
Wei MM, Zhou YC, Wen ZS, Zhou B, Huang YC, Wang GZ, et al. Long non-coding RNA stabilizes the Y-box-binding protein 1 and regulates the epidermal growth factor receptor to promote lung carcinogenesis. Oncotarget. 2016;7(37):59556–71. https://doi.org/10.18632/oncotarget.10006.
Liu C, Xu J, Chen Y, Guo X, Zheng Y, Wang Q, et al. Characterization of genome-wide H3K27ac profiles reveals a distinct PM2.5-associated histone modification signature. Environ Health. 2015;14(1):65. https://doi.org/10.1186/s12940-015-0052-5.
Zheng Y, Sanchez-Guerra M, Zhang Z, Joyce BT, Zhong J, Kresovich JK, et al. Traffic-derived particulate matter exposure and histone H3 modification: a repeated measures study. Environ Res. 2017;153:112–9. https://doi.org/10.1016/j.envres.2016.11.015.
Horvath S. DNA methylation age of human tissues and cell types. Genome Biol. 2013;14(10):R115. https://doi.org/10.1186/gb-2013-14-10-r115.
Hannum G, Guinney J, Zhao L, Zhang L, Hughes G, Sadda S, et al. Genome-wide methylation profiles reveal quantitative views of human aging rates. Mol Cell. 2013;49(2):359–67. https://doi.org/10.1016/j.molcel.2012.10.016.
Prins GS, Calderon-Gierszal EL, Hu WY. Stem cells as hormone targets that lead to increased cancer susceptibility. Endocrinology. 2015;156(10):3451–7. https://doi.org/10.1210/en.2015-1357.
Vineis P, Chatziioannou A, Cunliffe VT, Flanagan JM, Hanson M, Kirsch-Volders M, et al. Epigenetic memory in response to environmental stressors. FASEB Journal. 2017;31(6):2241–51. https://doi.org/10.1096/fj.201601059RR.
Joubert BR, Felix JF, Yousefi P, Bakulski KM, Just AC, Breton C, et al. DNA methylation in newborns and maternal smoking in pregnancy: genome-wide consortium meta-analysis. Am J Hum Genet. 2016;98(4):680–96. https://doi.org/10.1016/j.ajhg.2016.02.019.
Yang AS, Estecio MR, Doshi K, Kondo Y, Tajara EH, Issa JP. A simple method for estimating global DNA methylation using bisulfite PCR of repetitive DNA elements. Nucleic Acids Res. 2004;32(3):e38. https://doi.org/10.1093/nar/gnh032.
Price EM, Cotton AM, Penaherrera MS, McFadden DE, Kobor MS, Robinson W. Different measures of “genome-wide” DNA methylation exhibit unique properties in placental and somatic tissues. Epigenetics. 2012;7(6):652–63. https://doi.org/10.4161/epi.20221.
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144(5):646–74. https://doi.org/10.1016/j.cell.2011.02.013.
Felix JF, Joubert BR, Baccarelli AA, Sharp GC, Almqvist C, Annesi-Maesano I, et al. Cohort profile: pregnancy and childhood epigenetics (PACE) consortium. Int J Epidemiol. 2018;47(1):22–3u. https://doi.org/10.1093/ije/dyx190.
Vineis P, Chadeau-Hyam M, Gmuender H, Gulliver J, Herceg Z, Kleinjans J, et al. The exposome in practice: design of the EXPOsOMICS project. Int J Hyg Environ Health. 2017;220(2 Pt A):142–51. https://doi.org/10.1016/j.ijheh.2016.08.001.
Yang SJ, Yang SY, Wang DD, Chen X, Shen HY, Zhang XH, et al. The miR-30 family: versatile players in breast cancer. Tumour Biol. 2017;39(3):1010428317692204. https://doi.org/10.1177/1010428317692204.
Qu K, Lin T, Pang Q, Liu T, Wang Z, Tai M, et al. Extracellular miRNA-21 as a novel biomarker in glioma: evidence from meta-analysis, clinical validation and experimental investigations. Oncotarget. 2016;7(23):33994–4010. https://doi.org/10.18632/oncotarget.9188.
Sweeney CL, Teng R, Wang H, Merling RK, Lee J, Choi U, et al. Molecular analysis of neutrophil differentiation from human induced pluripotent stem cells delineates the kinetics of key regulators of hematopoiesis. Stem Cells. 2016;34(6):1513–26. https://doi.org/10.1002/stem.2332.
Paterson MR, Kriegel AJ. MiR-146a/b: a family with shared seeds and different roots. Physiol Genomics. 2017;49(4):243–52. https://doi.org/10.1152/physiolgenomics.00133.2016.
Ding S, Huang H, Xu Y, Zhu H, Zhong C. MiR-222 in cardiovascular diseases: physiology and pathology. Biomed Res Int. 2017;2017:4962426. https://doi.org/10.1155/2017/4962426.
Testa U, Pelosi E, Castelli G, Labbaye C. miR-146 and miR-155: two key modulators of immune response and tumor development. Noncoding RNA. 2017;3(3). doi:https://doi.org/10.3390/ncrna3030022.
Thum T, Gross C, Fiedler J, Fischer T, Kissler S, Bussen M, et al. MicroRNA-21 contributes to myocardial disease by stimulating MAP kinase signalling in fibroblasts. Nature. 2008;456(7224):980–4. https://doi.org/10.1038/nature07511.
Huarte M. The emerging role of lncRNAs in cancer. Nat Med. 2015;21(11):1253–61. https://doi.org/10.1038/nm.3981.
Bartonicek N, Maag JL, Dinger ME. Long noncoding RNAs in cancer: mechanisms of action and technological advancements. Mol Cancer. 2016;15(1):43. https://doi.org/10.1186/s12943-016-0530-6.
Jantsch MF, Quattrone A, O'Connell M, Helm M, Frye M, Macias-Gonzales M, et al. Positioning Europe for the EPITRANSCRIPTOMICS challenge. RNA Biol. 2018:1–3. https://doi.org/10.1080/15476286.2018.1460996.
Baccarelli A, Bollati V. Epigenetics and environmental chemicals. Curr Opin Pediatr. 2009;21(2):243–51. https://doi.org/10.1097/MOP.0b013e32832925cc.
Chervona Y, Costa M. The control of histone methylation and gene expression by oxidative stress, hypoxia, and metals. Free Radic Biol Med. 2012;53(5):1041–7. https://doi.org/10.1016/j.freeradbiomed.2012.07.020.
Bayarsaihan D. Epigenetic mechanisms in inflammation. J Dent Res. 2011;90(1):9–17. https://doi.org/10.1177/0022034510378683.
Byun HM, Colicino E, Trevisi L, Fan T, Christiani DC, Baccarelli AA. Effects of air pollution and blood mitochondrial DNA methylation on markers of heart rate variability. J Am Heart Assoc. 2016;5(4). https://doi.org/10.1161/JAHA.116.003218.
McCreanor J, Cullinan P, Nieuwenhuijsen MJ, Stewart-Evans J, Malliarou E, Jarup L, et al. Respiratory effects of exposure to diesel traffic in persons with asthma. N Engl J Med. 2007;357(23):2348–58. https://doi.org/10.1056/NEJMoa071535.
Houseman EA, Accomando WP, Koestler DC, Christensen BC, Marsit CJ, Nelson HH, et al. DNA methylation arrays as surrogate measures of cell mixture distribution. BMC Bioinformatics. 2012;13:86. https://doi.org/10.1186/1471-2105-13-86.
Bakulski KM, Feinberg JI, Andrews SV, Yang J, Brown S, McKenney SL, et al. DNA methylation of cord blood cell types: applications for mixed cell birth studies. Epigenetics. 2016;11(5):354–62. https://doi.org/10.1080/15592294.2016.1161875.
Houseman EA, Kile ML, Christiani DC, Ince TA, Kelsey KT, Marsit CJ. Reference-free deconvolution of DNA methylation data and mediation by cell composition effects. BMC Bioinformatics. 2016;17:259. https://doi.org/10.1186/s12859-016-1140-4.
Bauer M, Linsel G, Fink B, Offenberg K, Hahn AM, Sack U, et al. A varying T cell subtype explains apparent tobacco smoking induced single CpG hypomethylation in whole blood. Clin Epigenetics. 2015;7(1):81. https://doi.org/10.1186/s13148-015-0113-1.
Green BB, Karagas MR, Punshon T, Jackson BP, Robbins DJ, Houseman EA, et al. Epigenome-wide assessment of DNA methylation in the placenta and arsenic exposure in the New Hampshire Birth Cohort Study (USA). Environ Health Perspect. 2016;124(8):1253–60. https://doi.org/10.1289/ehp.1510437.
Langie SA, Szarc Vel Szic K, Declerck K, Traen S, Koppen G, Van Camp G, et al. Whole-genome saliva and blood DNA methylation profiling in individuals with a respiratory allergy. PLoS One. 2016;11(3):e0151109. https://doi.org/10.1371/journal.pone.0151109.
Funding
Support for this work was provided by the project EXPOSOMICS, grant agreement 308610-FP7 European Commission, and by the Plan Cancer-Eva-Inserm research grant.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
Rossella Alfano has a PhD fellowship from Bijzonder Onderzoeksfonds (BOF) Hasselt University.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Environmental Epigenetics
Electronic supplementary material
ESM 1
(DOCX 105 kb)
Rights and permissions
About this article
Cite this article
Alfano, R., Herceg, Z., Nawrot, T.S. et al. The Impact of Air Pollution on Our Epigenome: How Far Is the Evidence? (A Systematic Review). Curr Envir Health Rpt 5, 544–578 (2018). https://doi.org/10.1007/s40572-018-0218-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-018-0218-8