Abstract
Background
Primary hyperparathyroidism is a common endocrine disease, and its incidence increases with age.
Aims
Our aim was to retrospectively evaluate the impact of age on patient outcomes following parathyroidectomy for primary hyperparathyroidism.
Methods
Two-hundred fifty-six consecutive patients undergoing parathyroidectomy with preoperative diagnosis of primary hyperparathyroidism were divided into three groups according to patient age: group A, ≤64 years; group B, 65–74 years; and group C, ≥75 years.
Results
Thyroid disease was associated with the hyperparathyroidism in 44 patients (28.2%) in group A, 34 (44.7%) in B, and 10 (41.7%) in C (p < 0.01). Minimally invasive parathyroidectomy was performed in 104 patients (66.7%) in group A, 35 (46.1%) in B, and 8 (33.3%) in C (p < 0.01). Conversion to bilateral exploration was carried out in five cases in group A (4.6%), three in B (8.3%), and two in C (20%). Multiglandular disease was observed in six patients (3.8%) in group A, seven (9.2%) in B, and five (20.8%) in C (p = 0.012). Mean postoperative stay was similar between groups; no major complications and no cases of mortality occurred.
Discussion
Multiglandular disease is more common in older patients than younger individuals, and minimally invasive approaches are less used in this patient group. Increased surgical risk and paucity of symptoms in these patients sometimes result in a delay in surgical treatment.
Conclusions
Parathyroidectomy is a safe and effective procedure to perform in elderly patients. Multiglandular disease was found to be more prevalent in older patients, but minimally invasive parathyroidectomy can be performed safely. Surgeons should consider parathyroidectomy in patients with primary hyperparathyroidism regardless of age.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary hyperparathyroidism (PHPT) is a common endocrine disease occurring in 0.2–1% of the population [1–3]. Women are affected two to three times more often than men [4]. The incidence increases with age, and it affects up to 2% of elderly individuals [1, 2, 5–7]. Surgery constitutes the most effective and only curative treatment for PHPT [2, 8]. Parathyroidectomy is expected to be curative in at least 95% of cases of sporadic PHPT [9].
Thanks to recent advancements in imaging and localization studies (which indicate where to start the procedure) and the more readily available rapid intraoperative parathyroid hormone assay (IOPTH) (which suggests when to stop the procedure), and minimally invasive parathyroidectomy has become more widely used [10–12]. Minimally invasive or ‘directed’ parathyroidectomy results in a smaller incision, less cervical dissection, and less postoperative discomfort [12].
Elderly patients with PHPT are often not referred for surgical intervention because of comorbidities that may increase the risk of perioperative complications [12]. Only about 25% of parathyroidectomies in the USA are performed in elderly patients [7, 13]. Symptoms may be difficult to distinguish from those associated with the general aging process [14]. For example, most elderly patients present some degree of bone disease and fatigue, and although these problems may also be caused by PHPT, they seem to be more often associated with neurological and psychiatric disorders [8, 15]. Kebebew et al. [16] found that 22% of their PHPT patients aged above 80 years referred for parathyroidectomy had experienced a delay of more than one year before referral, with a mean delay of 5 years. The reported morbidity and mortality rates associated with parathyroidectomy in elderly patients are as high as 10 and 4%, respectively [16].
Our aim was to retrospectively evaluate the impact of age on patient outcomes following parathyroidectomy for PHPT in a single endocrine surgery center.
Patients and methods
In this retrospective study, we reviewed the records of 256 consecutive patients with a preoperative diagnosis of PHPT who had undergone parathyroidectomy between 2003 and 2015 in the Department of Surgical Sciences, University of Cagliari, Italy. The recorded data comprised patient: age; sex; preoperative serum calcium and parathyroid hormone (PTH) levels; results of preoperative localization studies; surgical procedure; histopathological features; and postoperative complications. The patients underwent parathyroidectomy with unilateral or bilateral exploration. Causes for initial bilateral exploration included: other associated neck procedures; familial forms of PHP; or discordant or negative test results with very low PTH levels. All operations were performed by the same two experienced endocrine surgeons.
Neck ultrasound (US) and MIBI scans were performed preoperatively. IOPTH determination was routinely used during surgery to confirm removal of all pathological glands; a test result was defined as positive when the PTH value 10′ after excision of the suspected pathological gland dropped by at least 50% of the preoperative value or when it was within range values (10–65 pg/ml). In the case of a negative test, a second PTH measurement was made 20′ after excision, and if the negative result was once again confirmed, bilateral exploration was performed. The STAT-IntraOperative-Intact-PTH chemiluminescence immune-assay semiautomated mobile system (Future Diagnostics, Wijchen, Netherlands) was used within the surgical suite complex for the intraoperative quantitative determination of PTH levels in EDTA plasma.
Patient demographics and postoperative complications were recorded, including: postoperative hematoma; recurrent laryngeal nerve injury; hypoparathyroidism; and wound infection. Hypoparathyroidism (defined as a PTH level < 10 pg/ml) was considered permanent if it lasted more than 6 months. Recurrent laryngeal nerve palsy was defined as vocal fold paralysis (assessed by postoperative fibrolaryngoscopy) and was considered permanent if it persisted for more than 6 months after surgery. Hyperparathyroidism was defined as persistent or recurrent (HPT) if high PTH blood levels were found within or after 6 months after surgery, respectively.
Follow-up consisted of neck US examination and the monitoring of serum calcium, phosphorus, and PTH.
Patients were divided into three groups: Those aged up to 64 years were included in group A; group B consisted of patients aged between 65 and 74 years; and group C consisted of patients aged 75 years or older.
The study was performed in accordance with the Declaration of Helsinki. Ethical approval for the study was obtained from the University of Cagliari institutional ethics committee. Informed consent was obtained from all patients for their inclusion in the study.
Statistical analysis
To assess factors influencing patient outcomes, analysis of variance (ANOVA) was used for continuous variables and the Chi-squared test was used for categorical data. A p value less than 0.05 was considered statistically significant.
Results
As reported in Table 1, 256 patients were included in the study; 156 (60.9%) in group A, 76 (29.7%) in group B, and 24 (9.4%) in group C. Women were more numerous than men in all age groups (Table 1). Mean preoperative calcemia was 11.5 ± 1.3 mg/dl in group A, 11.3 ± 1.3 in group B, and 10.8 ± 0.6 in group C; mean preoperative PTH levels were 285 ± 301 pg/mL, 324 ± 349, and 287 ± 182, respectively.
Thyroid disease was associated with PHPT in 44 patients (28.2%) in group A, in 34 patients (44.7%) in group B, and in 10 patients (41.7%) in group C (p < 0.01) (Table 1).
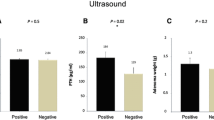
All patients had undergone preoperative US and MIBI scans. US sensitivity and positive predictive values (PPV) were 75.5 and 95.8%, respectively, in group A, 57.8 and 89.2% in group B, and 56.5 and 92.8% in group C. MIBI sensitivity and PPV were 93.5 and 92.8%, respectively, in group A, 89.2 and 87.7% in group B, and 70.6 and 85.7% in group C (Table 2).
All patients underwent parathyroidectomy. Minimally invasive focused parathyroidectomy was performed in 104 patients (66.7%) in group A, 35 (46.1%) in group B, and 8 (33.3%) in group C (p < 0.01) (Table 3). Initial bilateral exploration was performed as a result of associated thyroid disease in 44 cases in group A, in 34 cases in group B, and in 10 cases in group C, and because of the preoperative suspicion of multiglandular disease or a negative outcome of localization studies in 3 cases in group A, in 4 cases in group B, and in 4 cases in group C. Minimally invasive focused parathyroidectomy was converted to bilateral exploration following the results of IOPTH in five cases in group A (4.6%), in three cases in group B (8.3%), and in two cases in C (20%).
Mean postoperative stay was 2.3 ± 0.9 days for group A, 2.5 ± 0.9 days for group B, and 2.5 ± 0.6 days for group C (p = 0.15) (Table 3).
Transient hypoparathyroidism was reported in 10 cases (6.4%) in group A, in 14 cases (18.4%) in group B, and in 4 cases (16.7%) in group C (p = 0.013) (Table 3). Permanent hypoparathyroidism was reported in 2 (1.3%), 1 (1.3%), and 2 cases (8.3%), respectively (p = 0.06) (Table 3). Postoperative bleeding occurred in just a single patient, who belonged to group B. No recurrent laryngeal nerve injury, no other complications, and no cases of mortality occurred.
Persistent hyperparathyroidism occurred in three patients (1.9%) in group A, in two patients (2.6%) in group B, and in one patient (4.2%) in group C (Table 3).
Histopathological examination demonstrated single-gland disease vs. multigland disease in 150 (96.1%) versus 6 cases (3.8%), respectively, in group A, in 69 (90.8%) versus 7 cases (9.2%) in group B, and in 19 (79.2%) versus 5 cases (20.8%) in group C (p = 0.012) (Table 4).
IOPTH was performed in all patients; sensitivity, specificity, PPV, the negative predictive value (NPV), and accuracy values are reported in Table 5.
Discussion
An exact definition of the geriatric patient is not available in the medical literature. Various publications use different age definitions, e.g., 60, 65, 70, 75, or 80 years [1, 4, 5, 8, 9, 13, 15–19]. Here, we used as a minimum age limit of 65 years to refer to ‘older’ patients, and in addition we refer to patients aged over 75 years (i.e., group C) as ‘elderly.’
Primary hyperparathyroidism is a common endocrine disorder in the older population [20]. For example, one autopsy study reported the prevalence of parathyroid adenoma in the geriatric population to be 7% [21]. The incidence may actually be higher than this as the condition commonly goes undiagnosed in elderly patients as symptoms of PHPT, such as fatigue, neurological and psychological problems, bone demineralization and musculoskeletal pain, are often mistaken for those of general aging [12, 14, 21]. The present study does not confirm the data reported in the literature. Mean values of preoperative PTH were similar between our three age groups of ‘older’ patients, and there were no significant differences in reported symptoms. Perhaps this is a consequence of fact that our endocrinology is particularly focused on parathyroid diseases.
Multiglandular disease is significantly more common in older patients compared to younger patients with rates of 20–30% in older patients [5, 6, 21]. Uden et al. [22] showed that double adenoma was significantly more common in patients older than 60 years compared with younger patients (9.2% vs. 2.5%, respectively). Another study diagnosed hyperplasia in 27% of geriatric patients [21]. In a study by Kebebew et al. [16], 26% of octogenarians had multiglandular disease. Our study confirms the high rate of multiglandular disease in the elderly: The incidence of double adenomas was 0.6% in group A, 3.9% in group B, and 8.3% in group C (p = 0.03), and the incidence of multigland hyperplasia was 3.2, 5.3, and 12.5%, respectively, in the three groups (p = 0.13). Overall, the incidence of multiglandular disease was 3.8% in group A, 9.2% in group B, and 20.8% in group C (p = 0.012).
Parathyroidectomy remains the mainstay of PHPT management [4]. Cervical exploration for PHPT is successful in over 90% of cases, with very low morbidity and mortality rates [14]. The benefits of minimally invasive parathyroidectomy include: shorter operative times; shorter hospital lengths of stay; and lower overall costs sustained by the patients. It also alleviates the need for general anesthesia and is likely to result in smaller scars with less postoperative pain during recovery [2]. Elderly patients seem to be more suitable candidates for minimally invasive surgical approaches, with their associated smaller incisions, shorter operative times, and limited hospital stays compared with the more invasive operations typical of past decades [23]. Some authors have reported a significant increase in the proportion of elderly patients referred for parathyroidectomy since the introduction of mini-invasive parathyroidectomy [2, 5, 24].
The results of our retrospective study show that the minimally invasive approach is used less frequently in the most elderly patients compared with the younger population of older patients: Minimally invasive focused parathyroidectomy was performed in 66.7% of patients in group A, 46.1% in group B, and 33.3% in group C (p < 0.01). These results depend on different causes. An important element that comes to light from the results of our series is the frequent association of thyroid disease with PHPT in the elderly. This finding is not surprising given that Sardinia has a very high rate of thyroid disease, especially goiter and autoimmune thyroiditis. This fact, together with the advantages associated with treating potential thyroid disease in a single operation, is a reason for our frequent use of bilateral exploration of the neck in the elderly. Moreover, as previously reported in the literature [10, 25, 26], the co-presence of PHPT with thyroid disease results in a lower sensitivity of localization studies. In our study, US sensitivity was 75.5% in group A, 57.8% in group B, and 56.5% in group C, while MIBI sensitivity in the three groups was 93.5, 89.2, and 70.6%, respectively. A further element which has led to a higher use of bilateral exploration has been the previously reported high incidence of multiglandular disease.
According to Mekel [6], the rate of conversion to bilateral exploration in older patients was 32%, the cause usually being an insufficient decrease in IOPTH levels. Moreover, Irvin and Carneiro showed that by using IOPTH to determine single or multiglandular involvement 95% to 96% of patients with sporadic primary hyperparathyroidism can be successfully treated by excision of just a single gland [5]. In the present study, the rate of conversions was highest in the oldest patient group: 4.6% in group A, 8.3% in group B, and 20% in C. In these cases, it was again the insufficient reduction of IOPTH that led to the diagnosis of multiglandular disease. However, the routine use of IOPTH is a controversial matter [27–34], although it is our opinion that its use in the elderly is essential given the high incidence of multiglandular disease in these subjects. Indeed, this is confirmed by our results showing a high success rate of the surgical treatment. The rate of persistent hyperparathyroidism was not statistically different between the three groups.
Moreover, the increased surgical risk and paucity of symptoms in these patients sometimes result in a delay in surgical treatment [21]. Associated morbidities and old age are often given as reasons for deferring surgery and choosing conservative managements [14]. Elderly patients referred for surgical intervention tend to have more severe forms of the disease, indicating that they are being presented for surgical intervention at a later stage of the disease process [8, 15]. In the patient series studied by Shin and colleagues [12], the most elderly patients were referred for surgery at a later stage of their disease (once it had already progressed); the sole reason for which was age. In the study by Kebebew et al. [16], surgery in 22% of octogenarians and nonagenarians was delayed by more than 1 year.
Comorbidities are frequent in HTPT patients with more than two-thirds of cases also receiving treatment for hypertension and a high incidence of cardiovascular disease, dyspnea, and diabetes [1, 7, 19, 20, 35].
According to some studies, the rates of perioperative morbidity (4–10%) and mortality (0–4%) in elderly patients undergoing parathyroidectomy are similar to those of the general population [21, 24]. However, according to Thomas [7], the overall unadjusted complication rates of elderly patients aged 65 years or older were nearly double those of patients aged 45–64 years, and respiratory complications were three times more frequent. Elderly patients are more likely to have cardiac complications [4. 24]. On the contrary, Chen [15] found that elderly patients had similar complication rates compared with younger patients. In our study, there were no cases of mortality or any major general morbidities associated with parathyroidectomy, confirming that age alone is not a contraindication to surgery. We observed a higher incidence of transient hypoparathyroidism in the most elderly patients: 6.4% in group A, 18.4% in B, and 16.7% in C (p = 0.013), as well as permanent hypoparathyroidism: 1.3, 1.3, and 8.3%, respectively (p = 0.06).
Multiple studies have shown that parathyroidectomy is safe, effective, feasible, and beneficial in elderly patients [4, 6, 7, 12, 15]; although according to some studies elderly patients are more likely to spend more time in the recovery room and have longer overall hospital lengths of stay [4, 9, 24]. In the study by Thomas et al. [7], elderly patients experienced more complications in spite of shorter operation times and the average hospital length of stay was longer. In our study, all patients were operated under general anesthesia and no statistically significant difference in the mean hospital stay between the three groups of patients was observed.
Conclusions
Parathyroidectomy is safe, well tolerated, curative, beneficial, and effective in elderly patients. Multiglandular disease in PHPT was found to be more prevalent in older patients, but minimally invasive parathyroidectomy can also be performed safely in elderly patients with the adjunctive use of preoperative localization imaging and IOPTH. These results show that surgeons should consider parathyroidectomy in PHPT patients regardless of age.
Abbreviations
- PHPT:
-
Primary hyperparathyroidism
- IOPTH:
-
Intraoperative parathyroid hormone assay
- PTH:
-
Parathyroid hormone
- US:
-
Ultrasound
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
References
Egan KR, Adler JT, Olson JE et al (2007) Parathyroidectomy for primary hyperparathyroidism in octogenarians and nonagenarians: a risk-benefit analysis. J Surg Res 140:194–198
Pruhs ZM, Starling JR, Mack E, et al (2005) Changing trends for surgery in elderly patients with hyperparathyroidism at a single institution. J Surg Res 127:59–62
Siilin H, Lundgren E, Mallmin H et al (2011) Prevalence of primary hyperparathyroidism and impact on bone mineral density in elderly men: MrOs Sweden. World J Surg 35:1266–1272. doi:10.1007/s00268-011-1062-2
Young VN, Osborne KM, Fleming MM, et al (2009) Parathyroidectomy in the elderly population: does age really matter? Laryngoscope 120:247–252
Irvin GL, Carneiro DM (2001) “Limited” parathyroidectomy in geriatric patients. Ann Surg 233:612–616
Mekel M, Gilshtein H, Chapchay K, et al (2014) Parathyroid surgery in the elderly: should minimally invasive surgery be abandoned? Ann Surg Oncol 21:1369–1373
Thomas DC, Roman SA, Sosa JA (2011) Parathyroidectomy in the elderly: analysis of 7313 patients. J Surg Res 170:240–246
Bachar G, Gilat H, Mizrachi A, et al (2008) Comparison of perioperative management and outcome of parathyroidectomy between older and younger patients. Head Neck 30:1415–1421
Stechman MJ, Weisters M, Gleeson FV, et al (2009) Parathyroidectomy is safe and improves symptoms in elderly patients with primary hyperparathyroidism (PHPT). Clin Endocrinol 71:787–791
Boi F, Lombardo C, Cocco MC, et al (2013) Thyroid disease cause mismatch between MIBI scan and neck ultrasound in the diagnosis of hyperfunctioning parathyroids: usefulness of FNA-PTH assay. Eur J Endocrinol 168:49–58
Calò PG, Tatti A, Medas F, et al (2010) Nuove tecniche nella chirurgia delle paratiroidi. G Chir 31:322–324
Shin SH, Holmes H, Bao R, et al (2009) Outpatient minimally invasive parathyroidectomy is safe for elderly patients. J Am Coll Surg 208:1071–1076
Wu B, Haigh PI, Hwang R, et al (2010) Underutilization of parathyroidectomy in elderly patients with primary hyperparathyroidism. J Clin Endocrinol Metab 95:4324–4330
Roche NA, Young AE (2000) Role of surgery in mild primary hyperparathyroidism in the elderly. Br J Surg 87:1640–1649
Chen H, Parkerson S, Udelsman R (1998) Parathyroidectomy in the elderly: do the benefits outweigh the risks? World J Surg 22:531–535 (discussion 535–536)
Kebebew E, Duh QY, Clark OH (2003) Parathyroidectomy for primary hyperparathyroidism in octogenarians and nonagenarians. A plea for early surgical referral. Arch Surg 138:867–871
Agrusa A, Romano G, Frazzetta G et al (2014) Role and outcomes of laparoscopic cholecystectomy in the elderly. Int J Surg 12(Suppl 2):S37–S39
Calò PG, Medas F, Loi G et al (2014) Differentiated thyroid cancer in the elderly: our experience. Int J Surg 12(Suppl 2):S140–S143
Oltmann SC, Rajaei MH, Sippel RS et al (2014) Primary hyperparathyroidism across the ages: presentation and outcomes. J Surg Res 190:185–190
Dobrinja C, Silvestri M, De Manzini N (2012) Primary hyperparathyroidism in older people: surgical treatment with minimally invasive approaches and outcome. Int J Endocrinol 2012:539542
Biertho L, Chu C, Inabnet WB (2003) Image-directed parathyroidectomy under local anaesthesia in the elderly. Br J Surg 90:738–742
Udén P, Chan A, Duh QY et al (1992) Primary hyperparathyroidism in younger and older patients: symptoms and outcome of surgery. World J Surg 16:791–797 (discussion 798)
Politz D, Norman J (2007) Hyperparathyroidism in patients over 80: clinical characteristics and their ability to undergo outpatient parathyroidectomy. Thyroid 17:333–339
Morris LF, Zelada J, Wu B et al (2010) Parathyroid surgery in the elderly. Oncologist 15:1273–1284
Calò PG, Pisano G, Loi G et al (2013) Surgery for primary hyperparathyroidism in patients with preoperatively negative sestamibi scan and discordant imaging studies: the usefulness of intraoperative parathyroid hormone monitoring. Clin Med Insights Endocrinol Diabetes 6:63–67
Medas F, Erdas E, Longheu A et al (2016) Retrospective evaluation of the pre- and postoperative factors influencing the sensitivity of localization studies in primary hyperparathyroidism. Int J Surg 25:82–87
Baldini E, Tuccilli C, Prinzi N et al (2015) Deregulated expression of Aurora kinases is not a prognostic biomarker in papillary thyroid cancer patients. PLoS ONE 10:e0121514. doi:10.1371/journal.pone.0121514
Calò PG, Pisano G, Loi G et al (2013) Intraoperative parathyroid hormone assay during focused parathyroidectomy: the importance of 20 minutes measurement. BMC Surg 13:36
Calò PG, Pisano G, Medas F et al (2014) Total thyroidectomy without prophylactic central neck dissection in clinically node-negative papillary thyroid cancer: is it an adequate treatment? World J Surg Oncol 12:152. doi:10.1186/1477-7819-12-152
Calò PG, Pisano G, Tatti A et al (2012) Intraoperative parathyroid hormone assay during focused parathyroidectomy for primary hyperparathyroidism: is it really mandatory? Minerva Chir 67:337–342
Cantisani V, Grazhdani H, Ricci P et al (2014) Q-elastosonography of solid thyroid nodules: assessment of diagnostic efficacy and interobserver variability in a large patient cohort. Eur Radiol 24:143–150
Catania A, Sorrenti S, Falvo L et al (2002) Validity and limits of intraoperative rapid parathyroid hormone assay in primary hyperparathyroidism treated by traditional and mini-invasive surgery. Int Surg 87:226–232
Gervasi R, Orlando G, Lerose MA et al (2012) Thyroid surgery in geriatric patients: a literature review. BMC Surg 12(Suppl 1):S16. doi:10.1186/1471-2482-12-S1-S16
Lombardi CP, Raffaelli M, Traini E et al (2008) Intraoperative PTH monitoring during parathyroidectomy: the need for stricter criteria to detect multiglandular disease. Langenbecks Arch Surg 393:639–645
Fui SL, Bonnichon P, Bonni N et al (2016) Hyperparathyroidism in octogenarian: a plea for ambulatory minimally invasive surgery under local anesthesia. Ann Endocrinol 77:600–605
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors listed have contributed sufficiently to the project to be included as authors, and to the best of our knowledge, no conflicts of interest, financial or other, exist.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Human and animal rights statement
The article does not contain any experiments involving animals.
Informed consent
Informed consent was obtained from all participants included in the study.
Rights and permissions
About this article
Cite this article
Calò, P.G., Medas, F., Loi, G. et al. Parathyroidectomy for primary hyperparathyroidism in the elderly: experience of a single endocrine surgery center. Aging Clin Exp Res 29 (Suppl 1), 15–21 (2017). https://doi.org/10.1007/s40520-016-0666-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-016-0666-7