Abstract
Purpose
Alexithymia, a personality trait characterized by difficulties in emotional processing, has been associated with unhealthy behaviors and chronic medical conditions. This study aimed to further develop our understanding of this complex relationship by investigating whether alexithymia increases the risk of metabolic syndrome (MetS) in participants with obesity or overweight through the mediating role of binge eating (BE).
Methods
A consecutive sample of 238 treatment-seeking patients with obesity or overweight were recruited. Alexithymia (TAS-20), binge eating symptoms (BES), body mass index (BMI), and depression and anxiety symptoms (HADS) were concurrently assessed.
Results
Almost half of the participants met the criteria for MetS (44.12%). Compared to patients without MetS, those with MetS were older, had a longer duration of overweight, and had a higher BMI (p < 0.01). Individual with MetS also had higher HADS, BES, and TAS-20 scores, particularly difficulty identifying and describing feelings. The structural equation modeling (SEM) analysis revealed that BES levels exerted a significant direct effect on MetS (p < 0.01), and that TAS-20 levels exerted a significant direct effect on BES (p < 0.01), anxiety (p < 0.001) and depression (p < 0.001). Moreover, psychological distress (anxiety, p = 0.01, and depression, p = .05) indirectly affected MetS through the mediating effect of BES, and TAS-20 (p = 0.01) indirectly affected MetS through the mediating effect of HADS and BES. Finally, age had a significant direct effect on MetS (p < 0.001).
Conclusion
Our findings indicate that alexithymia is a concurrent causative factor to the development of MetS through the mediating role of BE and psychological distress.
Level of evidence
Level III, case–control analytic study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Globally, both obesity and metabolic syndrome (MetS) are growing public health problems [1]. The prevalence of both conditions has increased dramatically in industrialized countries over the past 30 years [2]. The prevalence of obesity doubled from 1975 (34 million men and 71 million women) to 2014 (266 million men and 375 million women) [3]. MetS is more common among individuals with obesity than normal weight individuals, with approximately 50% of women with obesity and nearly 60% of men with obesity experiencing MetS [4].
MetS is a combination of clinical criteria including abdominal obesity, metabolic abnormalities (high levels of glycaemia and blood pressure), and altered lipid metabolism (high levels of triglycerides and cholesterol) (see Methods 2.2.2 below), and is considered a major risk factor for cardiovascular disease [5]. MetS is highly prevalent among adults, ranging 7–34% in men and 5–22% in women [6], but can also affect children and adolescents. Its prevalence increases with age, with up to 44% of adults aged 40 and older presenting with MetS compared to 7% of younger adults aged 20–29 [7]. Furthermore, psychological distress is thought to increase the risk of MetS. Subjects with high psychological distress at baseline are more than twice as likely to develop MetS than those with low psychological distress. Pooled finding from cross-sectional studies show that anxiety and major depression are associated with an elevated risk of MetS (OR = 1.07, 95% CI 1.01–1.12 and OR = 1.82; 95% CI = 1.06–3.14, respectively) [8, 9]. Several of the identified causes and risk factors for obesity and MetS are related to unhealthy lifestyles, such as poor dietary patterns, sedentary lifestyle, and decreases or increases in sleep duration [10].
Binge eating (BE) is one behavior that has been identified as clinically relevant for the development of combined obesity and MetS [11,12,13]. BE involves the consumption of an unusually large amount of food within a discrete time period alongside a perceived inability to stop or control eating [14]. Recurrent BE episodes, at least once a week for three months, are a hallmark feature of binge eating disorder (BED). Other key features of BED include a lack of compensatory behaviors such as excessive exercise or vomiting, feeling depressed, embarrassed and disgusted with oneself after BE, and experiencing substantial distress regarding binge episodes [14]. BED has been associated with the severity of obesity [12], and general psychopathology, such as anger and impulsivity [15]. BED is typically managed with psychological and pharmacological interventions [16]. Compared with non-BE individuals with obesity, binge eaters with obesity engage in maladaptive eating behaviors and patterns that may place them at greater risk for MetS [17]. For example, hypercaloric food intake has been linked with more non-alcoholic fatty liver disease and elevated lipids in men and women with severe obesity [18]. A longitudinal study demonstrated that binge eaters were at greater risk for newly diagnosed MetS components, compared with non-binge eaters [11]. Despite the evidence for the co-occurrence of obesity with BE and MetS, little is known about the psychological characteristics of patients with obesity and MetS. In particular, it is still uninvestigated whether and how psychological characteristics are associated with different developmental trajectories of dieting, BE, and obesity problems.
Alexithymia is a personality dimension that has been associated with an increased incidence of numerous physical illnesses. The association between alexithymia and physical ill health is complex, alexithymia may modulate illness severity, pre-dispose an individual, be a consequence of the illness, or may involve a complex combination of all of these roles [19]. It is a multifaceted personality dimension composed of two higher‐order factors: a deficit of affect awareness [as difficulty identifying feelings [DIF] and difficulty describing feelings (DDF)] and operatory thinking (externally oriented thinking [EOT] and poor imaginal processes) [19]. These characteristics are thought to reflect deficits in the cognitive processing and regulation of emotions associated with anxiety and depression [20], and can affect health-related behaviors [21], such as dieting habits and physical activity [22]. Not surprisingly, alexithymia has been related to the clinical manifestation and maintenance of obesity [23] and a range of maladaptive eating patterns, including BE [24, 25]. Eating behaviors are known to be highly influenced by emotional regulation, providing a strong rationale for considering alexithymia as a potential predictor of obesity and BE [26]. Several neuroimaging studies have revealed that alexithymic traits are associated with activation in brain regions that subserve interoception and physiological monitoring [27, 28]. This is interesting in light of recent developments in the treatment of obesity. There is a growing literature demonstrating that mindfulness-based interventions, many of which stress increased attention to interoceptive information from the body, are an effective tool for promoting healthier eating behaviors [29].
Previously published studies mainly focused on the association of alexithymic features with single risk factors or components of MetS. The severity of alexithymia may contribute indirectly to MetS by influencing some of its components, such as T2D and cardiovascular risk [29, 30]. Given that alexithymia is thought to reflect deficits in mentalizing emotions, individuals with high levels of alexithymia may be more prone to experiencing psychological distress, anxiety, and depression [31,32,33,34]. Therefore, the relationship between alexithymia and MetS could be mediated through both BE and psychological distress. Moreover, to our knowledge, BE has not been considered as a co-variable in previous studies exploring the relationship between alexithymia and MetS. In this study, we aimed to explore the association between alexithymia and MetS by including maladaptive eating behavior and psychological distress as mediating factors. In particular, the aims of this study are: (a) to investigate whether patients with MetS have higher alexithymic traits, BE, depression, and anxiety than those without MetS, (b) to investigate whether patients with both MetS and BE have higher alexithymic traits than all other patients; and (c) to explore whether and to what extent psychological features (i.e., alexithymia, BE, depression, and anxiety) are associated with MetS. Based upon the previous literature, we expected that: (a) patients with MetS would exhibit more features of alexithymia, BE, depression, and anxiety than patients without MetS; (b) patients with both MetS and BE would have higher alexithymic traits than all other patients; and (c) psychological features (i.e., alexithymia, BE, depression, and anxiety) would be associated with MetS, and in particular alexithymia would indirectly affect MetS through the mediating role of BE, and depression and anxiety symptoms rather than directly.
Materials and methods
Participants
A sample of 297 treatment-seeking outpatients with obesity or overweight were consecutively enrolled at their first visit at the Obesity Centre at the University Clinical Hospital of Chieti (Italy). At intake subjects were first screened for medical conditions and their motivation to participate in the weight loss program. The weight loss program was characterized as an integrated approach including daily food intake monitoring, the promotion of a healthy lifestyle, behavioral modification of risk factors associated with eating behavior, and psychological counseling aimed at individual and interpersonal distress. To maximize the ecological validity of the sample, all adult outpatients from 18 to 70 years old with a Body Mass Index (BMI) ≥ 25 were invited to take part. Individuals were excluded if they self-reported a psychiatric or neurological disorder or the use of psychoactive substances in the past 10 years, were pregnant, were unable to complete the self-rating scales, or had documented or self-reported type 1 diabetes or any other endocrinological problem other than MetS.
All subjects provided written informed consent to take part in the study. The study was reviewed and approved by the Ethics Committee of University G.d'Annunzio—Chieti-Pescara and carried out in accordance with the World Medical Association Declaration of Helsinki and its subsequent revisions [35].
Measures
Socio-demographic and clinical characteristics
An ad hoc semi-structured interview was used to gather information on socio-demographic and clinical characteristics, such as age, gender, BMI, education level, marital status, and duration of overweight (years from the first dietary treatment), past and/or current psychopathological and neurologic symptoms, use of psychiatric medication, and experiences with psychotherapy. A BMI ≥ 30 was used as the cut-off for determining obesity and was analyzed as the ratio of weight in kilograms to the square of height in meters (kg/m2).
Clinical definition of MetS
In the present study, MetS was clinically defined using the NCEP–ATP III diagnostic criteria [36].
According to the polythetic NCEP–ATP III criteria [36], MetS is diagnosed when at least three of the following are satisfied: central obesity (defined as waist circumference ≥ 88 cm in females, and ≥ 102cmin males); triglycerides of 150 mg/dL or greater (1.7 mmol/L) or specific treatment for hypertriglyceridemia; HDL cholesterol less than 40 mg/dL (1.03 mmol/L) in males, and less than 50 mg/dL (1.29 mmol/L) in females or specific treatment for hypercholesterolemia; systolic blood pressure of 130 mm Hg or greater and/or diastolic blood pressure of ≥ 85 mm Hg or treatment for previously diagnosed hypertension; FPG of 100 mg/dL or greater (5.6 mmol/L) or previously diagnosed type 2 diabetes.
Binge eating (BE)
The Binge Eating Scale (BES) was used to assess the severity of BE behaviors [37]. The BES is a 16-item self-report questionnaire with scores ranging from 0 (no BE) to 46 (severe BE). Scores of ≥ 27 have typically served as the cut-off value for detecting the presence of severe BE, ≥ 18 for moderate BE, and ≤ 17 for minimal or no BE. For our sample, Cronbach’s α was 0.88.
Alexithymia
The self-report 20-item Toronto Alexithymia Scale (TAS-20) was used to measure Alexithymia [38]. Each item is rated on a 5-point Likert scale, with total scores varying from 20 to 100. The TAS-20 consists of three subscales: the DIF, the DDF, and the EOT. The DIF subscale measures an individual’s capacity to identify feelings and discriminate them from bodily sensations. The DDF subscale evaluates an individual’s capacity to describe feelings to other people. The EOT subscale assesses the propensity of an individual to orientate their attention towards external over internal events. A score 61 or above is typically used as the cut-off for high alexithymic traits [39]. The scale is considered the standard measure for alexithymia because of its good psychometric properties including internal consistency, construct validity, and factor structure that have been demonstrated across the world [40]. For our sample, Cronbach's α was 0.83 for the total scale, 0.85 for the DIF, 0.70 for the DDF, and 0.56 for the EOT subscales.
Depressive and anxiety symptoms
Depressive and anxiety symptoms were measured using the Hospital Anxiety and Depression Scale (HADS) [41]. The HADS is a 14-item self-report scale that is broadly used to assess psychological distress in patients with medical health problems and contains two distinct 7-item subscales for depression (HADS-D) and anxiety (HADS-A). Items on each subscale are rated on 4-point Likert scales ranging from 0 (no symptom) to 3 (definite experience of symptoms). For each subscale, scores between 8 and 10 are classed as borderline cases and scores from 11 to 21 are considered as moderate to severe for symptoms of anxiety and depression. The HADS has been used in several medical settings, indicating good reliability and validity [42]. For our sample, Cronbach’s α for HADS-D was 0.78 and for HADS-A 0.81.
Statistical analysis
A 2-step strategy was used for data analysis.
First, Student’s t test or chi-square test (χ2) and an analysis of variance (ANOVA) were used to compare between-group differences in socio-demographic and clinical variables for patients with or without MetS and BE. The standardized mean difference was used as a measure of effect size. A standardized effect size (Cohen’s d) of 0.20–0.50 is considered small, 0.50–0.80 moderate, and > 0.80 large [43]. The Eta-squared (η2), a measure of effect size for ANOVA, was also used. A standardized effect size (η2) of 0.01–0.05 is considered small, 0.06–0.14 moderate, and > 0.14 large. Pearson’s correlation coefficient was used for the associations between socio-demographic, clinical and psychological variables.
Second, Structural Equation Modeling (SEM) was used to evaluate the direct, indirect and total effects of alexithymia on MetS through the mediating role of BE, depression and anxiety symptoms. SEM is a set of statistical techniques used to measure and analyze the relationships of observed and latent variables. It examines linear causal relationships among variables, while simultaneously accounting for measurement error. Latent variables or factors are considered to represent theoretical constructs that can be interpreted as latent traits or “true” variables underlying the measured items. Observable variables or factors are variables that can be observed and directly measured [44].
SEM, with a maximum likelihood estimation method, was used to evaluate the fit of the hypothesized model based on the following criteria: chi-squared (χ2) (p > 0.05), Root Mean Square Error of Approximation (RMSEA) close to 0.06 or less for a well-fitted model, Comparative Fit Index (CFI) near 0.90 or greater and Tucker–Lewis Index (TLI) near 0.90 or greater [45]. Missing data were replaced by way of multiple imputation algorithms. The structural components of the model included one exogenous latent trait (alexithymia), one endogenous observed factor (MetS), one latent mediated variable (BE), two continuous mediator variables (depression and anxiety symptoms), and one observed covariate (age). Hypotheses regarding the structural relationships among the constructs in the final model were evaluated using the magnitude of path coefficients (standardized coefficient) and their significance.
Results
Characteristics of the sample
Of the 297 recruited patients, 238 (80.1%) were enrolled. The main reason for not participating was a lack of time. Included patients were mostly females (69.33%) and with a median age of 48 years. Most of the participants had graduated from high or secondary school (73.95%) and were married (74.14%). According to the polythetic NCEP–ATPIII criteria (see Methods 2.2.2), MetS was present in 44.12% of the sample.
Between-group comparisons
MetS
Compared with No-MetS, patients with MetS had a higher BMI (d = 0.39), duration of overweight (d = 0.68), and older age (d = 0.74). No other sociodemographic differences were found between the two groups. BE behaviors, alexithymia, and psychological distress showed significant between-group differences, with effect sizes in the small range. In particular, patients with MetS reported significantly higher BES (d = 0.26), TAS-20 (d = 0.43), DIF (d = 0.39), and DDF (d = 0.34) scores than patients without MetS. Moreover, patients with MetS showed significantly higher depression and anxiety symptoms (d = 0.28) than patients without MetS (see Table1).
MetS + BE
Results from the one-way ANOVA showed significant differences between groups, with moderate-to-large effect sizes. Patients with MetS but without BE were older (η2 = 0.15) than the other 3 groups and had a higher BMI (η2 = 0.04) and a longer duration of overweight (η2 = 0.13) than patients without MetS and BE. Patients without MetS and BE exhibited significantly lower TAS-20 scores than the other groups (η2 = 0.09), particularly lower DIF (η2 = 0.09). Patients with both MetS and BE had significantly higher TAS-20 (0.09) and DIF (0.09) scores than patients without MetS and BE, had significantly higher depression score (η2 = 0.07) than groups without BE, and significantly higher anxiety score (η2 = 0.07) than patients without MetS and without BE. Patients without MetS and with BE had a significantly higher TAS-20 (η2 = 0.09), DIF (η2 = 0.09), DDF (η2 = 0.06), and anxiety (η2 = 0.07) than patients without MetS and without BE (see Table 2).
Between-variable associations
Multiple significant correlations in the moderate range (r = 0.30–0.50) were found among variables. Alexithymia was significantly associated with psychological distress and BE. In particular, the TAS-20 total and the DIF subscale correlated higher with HADS-D (r = 0.43 and r = 0.46, respectively) and at a lower level with HADS-A and BES scores (r = 0.30–0.35). The DDF subscale and BES also showed significant correlations with psychological distress within the same correlation range. The highest correlation coefficient occurred between age and the duration of overweight (r = 0.83) (see Table 3).
Structural equation modeling
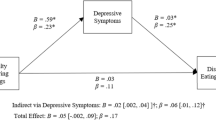
Figure 1 shows the path analysis and parameter estimates. All the observed variables were loaded on their corresponding latent constructs, supporting the validity of each latent construct, and standardized residuals were normally distributed. The parameter model estimates indicated that BE exerted a significant direct positive effect on MetS (β = 0.15), whereas there were no significant direct effects of HADS-A and HADS-D (β = 0.06 and β= 0.05, respectively). A significant direct effect of alexithymia was found on BE (β = 0.17), and depression (β = 0.50) and anxiety symptoms (β = 0.39). In addition, a significant direct effect of depression and anxiety symptoms (β = 0.17and β = 0.18, respectively) was found on BE. Finally, a significant direct effect of age as a covariate on MetS (β = 0.38), and a significant positive correlation between HADS-A and HADS-D were found (β = 0.37, p < 0.001). Put in more clinically bound words, results of SEM indicate that: (a) the higher the alexithymia level, the greater the increase of BE behaviors and psychological distress; (b) the higher the increase of psychological distress, the greater the increase of BE behaviors; and (c) the higher the BE behaviors, the greater the increase in MetS.
SEM showed positive and indirect effects of alexithymia (βindirect = 0.10, p = 0.01) on MetS through the mediation of BE behaviors and depression and anxiety symptoms. In addition, a positive and indirect effect of depression (βindirect = 0.02, p = 0.05) and anxiety symptoms (βindirect = 0.03, p = 0.01) was found on MetS through the mediation of BE behaviors (see Table 4). Finally, the total effect of alexithymia (β = 0.11, p = 0.01), BE (β = 0.14, p = 0.01), and age (β = 0.37, p = 0.001) on MetS was significant, but there were no significant total effects of psychological distress on MetS. The values of multiple fit indices indicated that the proposed model provided a good fit of the data, χ2(183) = 314.227, p < 0.001, TLI = 0.90, CFI = 0.91, CD = 0.90, and RMSEA = 0.05.
In sum, within our sample of patients with obesity or overweight, the SEM analysis showed that the relationship between alexithymia and MetS was not linear and direct but partially mediated by BE and psychological distress. In addition, age was found as a major factor influencing MetS.
Discussion
MetS is one of the major contributors to the epidemic of cardiovascular disorders in industrialized countries [7, 46, 47]. It should be noted that MetS is a heterogeneous label including hypertension, dyslipidemia, and hyperglycemia, which are all highly comorbid and correlated, although their pathophysiology does not necessarily overlap. One of the main utilities of the diagnostic label of MetS is to provide an opportunity to identify high-risk populations, such as individuals with obesity, and prevent the progression of some major causes of morbidity and mortality [48]. Several biomedical (e.g., insulin resistance, abdominal obesity, and increased activity of proinflammatory cytokines), lifestyle (e.g., smoking habits, lack of exercise, and disordered eating patterns), and psychiatric (e.g., mood, anxiety, schizophrenia, alcohol abuse, and personality disorders) risk factors for MetS have been identified [47, 48]. However, less is known about personality dimensions that may contribute to the development of MetS, particularly in high-risk populations, such as individuals with obesity or overweight. Alexithymia is considered a non-specific, trans-diagnostic construct associated with BE and obesity. The present study investigated whether alexithymia may constitute a potential risk factor for the development of MetS in outpatients with obesity or overweight, and whether a BE behavioral pattern and psychological distress may play a mediating role.
In our first hypothesis, we expected that patients with MetS would exhibit more features of alexithymia, BE, depression, and anxiety than non‐MetS obese patients. This hypothesis was fully confirmed. Patients with obesity or overweight and comorbid MetS had more alexithymic deficiencies (particularly difficulties in identifying and communicating their feelings), reported more behavioral patterns of BE, and were more psychologically distressed than those without MetS. These results are consistent with findings from previously published prospective studies on psychological factors and their co-occurrence with MetS and its components [28, 49]. For example, in a prospective population-based study, subjects with high psychological distress at baseline were more than twice as likely to develop MetS than those with low psychological distress, even after adjusting for sociodemographic variables, health behaviors, and C-reactive protein [50].
Consistent with the literature, our patients showed a close link between alexithymia and psychological symptoms (i.e., anxiety, depression, BE). A substantial body of evidence indicates that alexithymia and affective symptoms largely overlap, and that it is difficult to disentangle the causative role played by either one of these overlapping factors [31]. A number of longitudinal studies have shown that across a variety of clinical and non-clinical samples that alexithymic traits are relatively stable overtime. However, there can be some fluctuation in these trait alongside changes in anxiety and depression symptoms, further highlighting the intricate relationship between these variables [51, 52]. In our study, the association between alexithymia and duration of overweight suggests that there may be a vicious cycle between emotional dysregulation, overtime persistence of the clinical condition, and BE behavior. This is also in line with our second hypothesis that patients with MetS and BE would have higher alexithymic traits than all other patients. Our results showed that patients with MetS and BE had significantly higher alexithymia and DIF scores than those without MetS and BE. These results are consistent with findings that difficulties with emotional dysregulation may lead to compensatory overeating and, in turn, failed weight-loss attempts, which may further exacerbate difficulties in down-regulating emotional arousal, a pattern that has been repeatedly evidenced in alexithymic patients engaging in substance use and eating disorders [53]. Consistently, a number of longitudinal studies have demonstrated that personality traits characterized by inadequate stress control can increase the risk of MetS [49, 50].
In our third hypothesis, alexithymia was expected to indirectly affect MetS through the mediating role of BE behaviors and psychological distress. As expected, SEM analysis revealed that alexithymia affected MetS through the mediating role of BE, and depression and anxiety symptoms. This finding is in line with the results of our previous study that have emphasized the effect of alexithymic features on the severity of BE behaviors in patients with obesity [25]. The present study showed that alexithymia was linked to BE both directly and through the mediating effect of psychological distress. Several mechanisms may explain how this pathway can increase the risk of MetS. In a model proposed by Goldbacher et al. [54], psychological factors may contribute to the pathogenesis of MetS via physiological as well as behavioral mediating pathways. Several studies confirm that alexithymia is related to physical [55] and psychological distress [56], and directly associated with hyperarousal, sympathetic over-activity [57], and altered immune responses [58]. It may represent a personality marker of stress sensitivity or a vulnerability marker of stress, facilitating both unhealthy behaviors and inflammatory processes [57]. As inflammation is a recently purported physiological mechanism linking psychological distress to the development of MetS [59], alexithymia may be seen as a predisposing factor to illness not only through lifestyle factors but also through shared physiological factors.
Limitations
There are several methodological limitations that require consideration when interpreting the findings of this study. First and foremost, a consecutive non‐probabilistic sampling method was used. Non-probabilistic recruitment can result in a biased sample that is not fully representative of the wider population. A probabilistic sampling procedure should, therefore, be utilized in future studies. Second, the cross‐sectional nature of the current study does not enable us to explore causal relationships between MetS, BE, and alexithymia. Prospective longitudinal studies should be used in the future to explore the timing and sequence of BE onset and various metabolic disruptions across the lifespan to tease apart these complex relationships. Third, alexithymia, psychological distress, and BE were only assessed using self-report scales. Self-reported scales require a considerable amount of personal insight and may be influenced by subjective biases and social desirability effects. Nonetheless, evidence indicates that the self-report TAS-20 is a valid and sound measure of alexithymia [60]. The integration of the TAS-20 within a multimethod assessment framework would be preferred, although more difficult in clinical settings [61]. Fourth, a number of potentially relevant factors were not controlled for, such as an objective measure or document of past psychopathology, lifetime and current psychiatric conditions, quality of life, sleep quality, social support, medical comorbidity, physical activity, dietary habits, and inflammation activity. Future investigations should take into account those factors as relevant moderating and mediating variables whose change overtime may influence the association of alexithymia and BE with MetS. Fifth, our patients were recruited in a secondary care center and seeking treatment for their clinical condition. Individuals with obesity or overweight actively seeking medical, dietary, and psychological help for their weight problem and eating behavior are likely to be more motivated to make behavioral changes and more aware of their psychological problems. Follow-up studies should investigate whether the role of alexithymia and BE is different in patients with obesity seeking treatment who completed the intervention program and those who are non-treatment seeking or dropped out.
Clinical implications and conclusions
With these limitations in mind, the present findings indicate that alexithymia, particularly the facets of difficulty identifying and describing feelings, and BE have a relevant role in explaining the development of MetS in individuals with obesity or overweight, which may have important clinical implications. Clinicians should consider binge eating behavioral patterns and alexithymic characteristics in the clinical management of patients with MetS because these psychological aspects may influence the clinical presentation of the overall syndrome or its separate components. In addition, both alexithymia and BE can be modified through specific psychological interventions as well as integrated multicomponent treatment programs [62]. Screening for alexithymia and BE may, therefore, help in planning individualized, tailored treatment for improving MetS and its consequences on health.
In conclusion, we aimed to further explore the complex association between alexithymia and MetS by evaluating the mediating role of binge eating behavior and psychological distress. Our findings suggest that MetS is associated with distinct emotional and behavioral characteristics that require appropriate attention in the clinical management of patients.
What is already known on this subject?
Overweight, obesity, and metabolic syndrome are an increasing global health challenge. Alexithymia has previously been associated with unhealthy behaviors and chronic medical conditions. Binge eating has not been considered as a co-variable in previous studies exploring the relationship of alexithymia with MetS. In this study, we aimed to explore the association between alexithymia and MetS by including maladaptive eating behavior and psychological distress as mediating factors.
What this study adds?
Binge eating and psychological distress mediate the relationship between alexithymia and MetS. Our findings suggest that MetS is associated with distinct emotional and behavioral characteristics that require appropriate attention in the clinical management of patients.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Arcelus J, Mitchell AJ, Wales J, Nielsen S (2011) Mortality rates in patients with anorexia nervosa and other eating disorders: a meta-analysis of 36 studies. Arch Gen Psychiatry 68(7):724–731. https://doi.org/10.1001/archgenpsychiatry.2011.74
van Vliet-Ostaptchouk JV, Nuotio ML, Slagter SN, Doiron D, Fischer K, Foco A et al (2014) The prevalence of metabolic syndrome and metabolically healthy obesity in Europe: a collaborative analysis of ten large cohort studies. BMC EndocrDisord. 14(1):9. https://doi.org/10.1186/1472-6823-14-9
NCD Risk Factor Collaboration (2016) Trends in adult body-mass index in 200 countries from 1975 to 2014: a pooled analysis of 1698 population-based measurement studies with 19· 2 million participants. Lancet 387(10026):1377–1396. https://doi.org/10.1016/S0140-6736(16)30054-X
Park YW, Zhu S, Palaniappan L, Heshka S, Carnethon MR, Heymsfield SB (2003) The metabolic syndrome: prevalence and associated risk factor findings in the US population from the Third National Health and Nutrition Examination Survey, 1988–1994. Arch Intern Med 163(4):427–436. https://doi.org/10.1001/archinte.163.4.427
McNeill AM, Rosamond WD, Girman CJ, Golden SH, Schmidt MI, East HE et al (2005) The metabolic syndrome and 11-year risk of incident cardiovascular disease in the atherosclerosis risk in communities study. Diabetes Care 28(2):385–390. https://doi.org/10.2337/diacare.28.2.385
Balkau B, Charles MA, Drivsholm T, Borch-Johnsen K, Wareham N, Yudkin JS et al (2002) Frequency of the WHO metabolic syndrome in European cohorts, and an alternative definition of an insulin resistance syndrome. Diabetes Metab 28(5):364
Weihe P, Weihrauch-Blüher S (2019) Metabolic syndrome in children and adolescents: diagnostic criteria. Ther Opt Perspect Curr Obes Rep. https://doi.org/10.1007/s13679-019-00357-x
Goldbacher EM, Bromberger J, Matthews KA (2009) Lifetime history of major depression predicts the development of the metabolic syndrome in middle-aged women. Psychosom Med 71(3):266
Tang F, Wang G, Lian Y (2017) Association between anxiety and metabolic syndrome: a systematic review and meta-analysis of epidemiological studies. Psychoneuroendocrinology 77:112–121. https://doi.org/10.1016/j.psyneuen.2016.11.025
Hruby A, Hu FB (2015) The epidemiology of obesity: a big picture. Pharmacoeconomics 33(7):673–689. https://doi.org/10.1007/s40273-014-0243-x
Bulik CM, Sullivan PF, Kendler KS (2002) Medical and psychiatric morbidity in obese women with and without binge eating. Int J Eat Disord 32:72–78. https://doi.org/10.1002/eat.10072
Grilo CM, White MA, Barnes RD, Masheb RM (2012) Psychiatric disorder co-morbidity and correlates in an ethnically diverse sample of obese patients with binge eating disorder in primary care settings. Compr Psychiatry. https://doi.org/10.1016/j.comppsych.2012.07.012
Hudson JI, Hiripi E, Pope HG, Kessler RC (2007) The prevalence and correlates of eating disorders in the NCS Replication. Biol Psychiatry 61:348–358. https://doi.org/10.1016/j.biopsych.2006.03.040
American Psychiatric Association [APA] (2013) Diagnostic and statistical manual of mental disorders (DSM-5®). American Psychiatric Publication, Philadelphia
Amianto F, Siccardi S, Abbate-Daga G, Marech L, Barosio M, Fassino S (2012) Does anger mediate between personality and eating symptoms in bulimia nervosa? Psychiatry Res 200(2–3):502–512
Amianto F, Ottone L, Daga GA, Fassino S (2015) Binge-eating disorder diagnosis and treatment: a recap in front of DSM-5. BMC psychiatry 15(1):70
Hudson JI, Lalonde JK, Coit CE, Tsuang MT, McElroy SL, Crow SJ et al (2010) Longitudinal study of the diagnosis of components of the metabolic syndrome in individuals with binge-eating disorder. Am J Clin Nutr 91(6):1568–1573
Kovalic AJ, Cholankeril G, Satapathy SK (2019) Nonalcoholic fatty liver disease and alcoholic liver disease: metabolic diseases with systemic manifestations. Transl Gastroenterol Hepatol. https://doi.org/10.1007/s13300-019-00693-0
Luminet O, Bagby RM, Taylor GJ (2018) Alexithymia: advances in research, theory, and clinical practice. Cambridge University Press, Cambridge. https://doi.org/10.1017/9781108241595
Honkalampi K, Koivumaa-Honkanen H, Lehto SM, Hintikka J, Haatainen K, Rissanen T, Viinamäki H (2010) Is alexithymia a risk factor for major depression, personality disorder, or alcohol use disorders? A prospective population-based study. J Psychosom Res 68(3):269–273. https://doi.org/10.1016/j.jpsychores.2009.05.010
Porcelli P, Taylor GJ (2018) Alexithymia and physical illness: a psychosomatic approach. In: Luminet O, Bagby RM, Taylor GJ (eds) Alexithymia: advances in research, theory, and clinical practice. Cambridge University Press, Cambridge. https://doi.org/10.1017/9781108241595
Helmets KF, Mente A (1999) Alexithymia and health behaviors in healthy male volunteers. J Psychosom Res 47:635–645. https://doi.org/10.1016/S0022-3999(99)00067-7
Da Ros A, Vinai P, Gentile N, Forza G, Cardetti S (2011) Evaluation of alexithymia and depression in severe obese patients not affected by eating disorders. Eat Weight Disord 16(1):24–29. https://doi.org/10.1007/BF03327517
Westwood H, Kerr-Gaffney J, Stahl D, Tchanturia K (2017) Alexithymia in eating disorders: Systematic review and metaanalyses of studies using the Toronto Alexithymia Scale. J Psychosom Res 99:66–81. https://doi.org/10.1016/j.jpsychores.2017.06.007
Conti C, Di Francesco G, Lanzara R, Severo M, Fumagalli L, Guagnano MT, Porcelli P (2019) Alexithymia and binge eating in obese outpatients who are starting a weight- loss program: a structural equation analysis. Eur Eat Disorders Rev. https://doi.org/10.1002/erv.2696
Prefit AB, Cândea DM, Szentagotai-Tătar A (2019) Emotion regulation across eating pathology: a meta-analysis. Appetite. https://doi.org/10.1016/j.appet.2019.104438
Haase L, May AC, Falahpour M, Isakovic S, Simmons AN, Hickman SD et al (2015) A pilot study investigating changes in neural processing after mindfulness training in elite athletes. Front BehavNeurosci 9:229. https://doi.org/10.3389/fnbeh.2015.00229
Lemche E, Surguladze SA, Giampietro VP, Brammer MJ, Williams SCR, Sierra M, David AS, Phillips ML (2013) Interoceptive–reflective regions differentiate alexithymia traits in depersonalization disorder. Psychiat Res-Neuroim 214(1):66–72. https://doi.org/10.1016/j.pscychresns.2013.05.006
O'Reilly GA, Cook L, Spruijt-Metz D, Black DS (2014) Mindfulness-based interventions for obesity-related eating behaviours: a literature review. Obes Rev 15:453–461. https://doi.org/10.1111/obr.12156
Karukivi M, Jula A, Hutri-Kähönen N, Juonala M, Raitakari O (2016) Is alexithymia associated with metabolic syndrome? A study in a healthy adult population. Psychiatry Res 236:58–63. https://doi.org/10.1016/j.psychres.2015.12.034
Li S, Zhang B, Guo Y, Zhang J (2015) The association between alexithymia as assessed by the 20-item Toronto Alexithymia Scale and depression: a meta-analysis. Psychiatry Res 227(1):1–9. https://doi.org/10.1016/j.psychres.2015.02.006
Kojima M (2012) Alexithymia as a prognostic risk factor for health problems: a brief review of epidemiological studies. Biopsychosoc Med 6(1):21. https://doi.org/10.1186/1751-0759-6-21
Taylor GJ, Bagby RM (2004) New trends in alexithymia research. Psychother Psychosom 73(2):68–77
Taylor GJ (2000) Recent developments in alexithymia theory and research. Can J Psychiatry 45(2):134–142
World Medical Association (2013) World Medical Association declaration of Helsinki ethical principles for medical research involving human subjects. J Am Med Assoc 310(20):2191–2194. https://doi.org/10.1001/jama.2013.281053
Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA et al (2005) Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute scientific statement. Circulation 112:2735–2752. https://doi.org/10.1161/CIRCULATIONAHA.105.169404
Gormally J, Black S, Daston S, Rardin D (1982) The assessment of binge eating severity among obese persons. Addict Behav 7(1):47–55. https://doi.org/10.1016/0306-4603(82)90024-7
Bagby RM, Parker JD, Taylor GJ (1994) The twenty-item Toronto Alexithymia Scale—I. Item selection and cross-validation of the factor structure. J Psychosom Res 38(1):23–32. https://doi.org/10.1016/0022-3999(94)90005-1
Taylor GJ, Bagby RM, Parker JDA (1997) Disorders of affect regulation. Alexithymia in medical and psychiatric illness. Cambridge University Press, Cambridge
Parker JD, Taylor GJ, Bagby RM (2003) The 20-Item Toronto Alexithymia Scale: III. Reliability and factorial validity in a community population. J Psychosom Res 55(3):269–275. https://doi.org/10.1016/S0022-3999(02)00578-0
Zigmond AS, Snaith RP (1983) The Hospital Anxiety and Depression Scale. Acta Psychiatry Scand 67(6):361–370. https://doi.org/10.1111/j.1600-0447.1983.tb09716.x
Norton S, Cosco T, Doyle F, Done J, Sacker A (2013) The Hospital Anxiety and Depression Scale: A meta- confirmatory factor analysis. J Psychosom Res 74:74–81. https://doi.org/10.1016/j.jpsychores.2012.10.010
Cohen J (1988) Statistical power for the behavioral sciences, 2nd edn. Erlbaum, Hillsdale
Bollen KA (2002) Latent variables in psychology and social sciences. Annu Rev Psychol 53:605–634. https://doi.org/10.1146/annurev.psych.53.100901.135239
Schumacker RE, Lomax RG (1996) A Beginner's guide to structural equation modeling. Mahwah, New Jersey
Ford ES, Giles WH, Dietz WH (2002) Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey. JAMA 287:356–359. https://doi.org/10.1001/jama.287.3.356
Sherling DH, Perumareddi P, Hennekens CH (2017) Metabolic syndrome. J Cardiovasc Pharmacol Ther 22:365–367. https://doi.org/10.1177/1074248416686187
Aguilar M, Bhuket T, Torres S, Liu B, Wong RJ (2015) Prevalence of the metabolic syndrome in the United States, 2003–2012. JAMA 313(19):1973–1974. https://doi.org/10.1001/jama2015.4260.3
Bergmann N, Gyntelberg F, Faber J (2014) The appraisal of chronic stress and the development of the metabolic syndrome: a systematic review of prospective cohort studies. Endocr Connect 3(2):R55–R80. https://doi.org/10.1530/EC-14-0031
Puustinen PJ, Koponen H, Kautiainen H, Mantyselka P, Vanhala M (2011) Psychological distress predicts the development of the metabolic syndrome: a prospective population-based study. Psychosom Med 73:158–165. https://doi.org/10.1097/PSY.0b013e3182037315
Santor DA, Bagby RM, Joffe RT (1997) Evaluating stability and change in personality and depression. J Pers Soc Psychol 73:1354–1362. https://doi.org/10.1037/0022-3514.73.6.1354
Porcelli P, Tulipani C, Di Micco C, Spedicato MR, Todarello O, Maiello E (2011) Temporal stability of alexithymia in cancer patients following a psychological intervention. J Clin Psychol 67:1177–1187. https://doi.org/10.1002/jclp.20839
Morie KP, Ridout N (2018) Alexithymia and maladaptive regulatory behaviors in substance use disorders and eating disorders. In: Luminet O, Bagby RM, Taylor GJ (eds) Alexithymia: advances in research, theory, and clinical practice. Cambridge University Press, Cambridge. https://doi.org/10.1017/9781108241595
Goldbacher EM, Bromberger J, Matthews KA (2009) Lifetime history of major depression predicts the development of the metabolic syndrome in middle-aged women. Psychosom Med 71:266–272
Sepede G, Racciatti D, Gorgoretti V, Nacci M, Pizzigallo E, Onofrj M et al (2011) Psychophysical distress and alexithymic traits in chronic fatigue syndrome with and without comorbid depression. Int J Immunopath Pharmacol 24(4):1017–1025. https://doi.org/10.1177/039463201102400419
Bardosa F, Mota C, Patricio P, Alcantara C, Ferreira C, Barbosa A (2011) The relationship between alexithymia and physiological factors in systemic lupus erythematosus. Compr Psychiatry 53:754–762. https://doi.org/10.1016/j.comppsych.2010.11.004
Declercq F, Vanhaule S, Deheergher J (2010) Alexithymia and posttraumatic stress: subscales and symptom clusters. J Clin Psychol 66:1079–1089. https://doi.org/10.1002/jclp.20715
Honkalampi K, Lehto S, Koivumaa-Honkanen H, Hintikka J, Niskanen L, Valkonen-Korhonen M, Viinamäki H (2011) Alexithymia and tissue inflammation. Psychother Psychosom 80:359–364. https://doi.org/10.1159/000327583
Goldstein BI, Kemp DE, Soczynska JK, Mc-Intyre RS (2009) Inflammation and phenomenology, pathophysiology, comorbidity, and treatment of bipolar disorder: a systematic review of the literature. J Clin Psychiatry 70:1078–1090
Bagby RM, Parker JDA, Taylor GJ (2020) Twenty-five years with the 20-item Toronto Alexithymia Scale. J Psychosom Res. https://doi.org/10.1016/j.jpsychores.2020.109940
Taylor GJ, Bagby RM, Parker JDA (2016) What’s in the name ‘alexithymia’? A commentary on “Affective agnosia: Expansion of the alexithymia construct and a new opportunity to integrate and extend Freud’s legacy”. Neurosci Biol Behav Rev 68:1006–1020. https://doi.org/10.1016/j.neubiorev.2016.05.025
Nightingale BA, Cassin SE (2019) Disordered eating among individuals with excess weight: a review of recent research. Curr Obes Rep 8:112–127. https://doi.org/10.1007/s13679-019-00333-5
Funding
Open access funding provided by Università degli Studi G. D'Annunzio Chieti Pescara within the CRUI-CARE Agreement. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. KR is supported by the Health Foundation Scaling Up programme.
Author information
Authors and Affiliations
Contributions
All authors participated in the concept and writing of this manuscript. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any competing interests (financial and non-financial) that could be construed as a potential conflict of interest.
Ethical approval
The study was reviewed and approved by the Ethics Committee of University G.d'Annunzio—Chieti-Pescara and carried out in accordance with the World Medical Association Declaration of Helsinki and its subsequent revisions.
Informed consent
All patients provided their written informed consent to participate in this study.
Consent for publication
The publication of the research is approved by all authors and tacitly or explicitly by the responsible authorities where the work was carried out.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The article is part of the Topical Collection on Personality and Eating and Weight Disorders.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Conti, C., Di Francesco, G., Severo, M. et al. Alexithymia and metabolic syndrome: the mediating role of binge eating. Eat Weight Disord 26, 1813–1823 (2021). https://doi.org/10.1007/s40519-020-00964-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-020-00964-x