Abstract
Purpose
This study aimed at testing the validity and reliability of the Emotional Overeating Questionnaire (EOQ) in a sample of Italian adults with obesity, overweight or normal weight.
Materials and methods
Participants were 314 Italian adults (72.6% females, aged 18–76 years) with obesity (27.4%), overweight (21.3%), or normal weight (51.3%), who completed the EOQ and measures of binge eating, mental well-being, and mindful eating. Retesting was performed 4 weeks later in a randomly selected subsample of 60 participants. Factor structure of the EOQ was estimated by confirmatory factor analysis (CFA). Reliability was tested with McDonald’s ω and ordinal α coefficients for internal consistency and Cohen’s weighted Kappa coefficient (Kw) for test–retest reliability.
Results
Based on CFA, the five negative emotional items formed one factor (EOQ-5) with good reliability (ω = 0.89; ordinal α = 0.88; Kw= 0.71), while the item referring to happiness was dropped. EOQ-5 scores were associated with higher binge eating, lower mental well-being, and lower mindful eating. A cut-off point of two identified individuals at risk for binge eating disorders with 75% sensitivity and 67% specificity. Negative emotional overeating was more frequent in women with obesity than women with normal weight and men with obesity.
Conclusions
EOQ-5 is a valid and reliable tool for measuring the frequency of emotional overeating at the Italian community-level.
Level of evidence
Level V, cross-sectional, descriptive study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Emotional eating is the tendency to overeat in response to emotions [1] and has predominately been characterized by negative emotions (e.g., anger, sadness, or boredom), although sometimes it also includes positive emotions [2]. Eating in response to negative emotions has been associated with increased consumption of high-fat and high-sugar foods, higher body mass index (BMI) [3], poor psychological well-being, and psychological symptoms and diseases such as eating disorders, anxiety, depression, obsessive–compulsive behaviors, and psychoticism [4,5,6,7,8]. There is also evidence that negative emotional eating is a stronger predictor of overeating than other eating behaviors such as restraint or disinhibition [9]. Therefore, emotional eating warrants clinical attention because of its association with eating disorders, but it may also represent a risk eating behavior in relation to obesity and overweight. Given that prevalence rates of overweight and obesity continue to be a leading public health concern worldwide [10], there is a need to investigate and understand behaviors, such as emotional overeating, that play a role in disordered eating and weight gain [11]. However, the frequency and correlates of emotional overeating in community samples have received considerably less attention than in clinical samples.
The Emotional Overeating Questionnaire (EOQ) [12] is a brief 6-item self-report that measures the frequency of overeating behavior in response to five negative (i.e., anxiety, sadness, loneliness, tiredness, and anger) and one positive emotion (i.e., happiness). Frequency refers to how many days, over the prior 28 days, the participant reports the occurrence of an episode of overeating defined as “eating an unusually large amount of food, given the circumstances” [12, p. 142]. Advantages of the EOQ compared with other existing tools are that it refers to overeating in response to emotions instead of just eating and assesses the frequency of overeating. Frequency is the gold-standard response set when examining eating pathology [13, 14], and the EOQ differs in this way from other measures that assess the desire to eat [15, 16], the tendency to eat [2], or how much one eats [17, 18] when feeling certain emotions. Finally, the EOQ brief 6-item length may reduce the respondent burden of long questionnaires and simplify administration.
The EOQ has been developed and validated in patients with binge eating disorder (BED) and BMI ≥ 25 showing good factorial validity as a one-factor measure and good reliability with Cronbach’s α = 0.85 and intra-class correlation coefficient (ICC) = 0.73 for the 1-week test–retest [12]. Convergent validity was found with measures of binge episodes, eating disorder symptomatology, and depressive symptoms [12] as well as with overeating in a sample bariatric surgery patients [19]. However, the 6-item EOQ showed a different structure across clinical and non-clinical samples. Indeed, in the original study of patients with BED [12], one factor emerged from explorative factor analysis (EFA) with all items of negative and positive emotional overeating loading on the factor. In a sample of female, normal weight university students [20], one factor was extracted from the five negative emotional items. The measure had good reliability (α = 0.81) and was positively associated with measures of disordered eating symptoms and loss of control over food intake. The item referring to happiness was excluded as its loading was under the threshold (< 0.40) established by the authors to retain an item within EFA.
To the best of our knowledge, no study has evaluated the factor structure of the EOQ in a non-clinical sample of females and males of different age and educational attainment and various levels of BMI. Accordingly, the principal aim of this study was to investigate the factor structure of the EOQ by means of confirmatory factor analysis (CFA) in a community sample of both sexes with a wide range for age, education, and BMI. We also aimed at investigating the reliability and convergent/discriminant validity of the best fitting factor model and its associations with demographic characteristics and BMI levels.
The EOQ has been used in several studies of different samples in different countries, showing various associations with psychological, clinical or sociodemographic characteristics. High EOQ scores were associated with BED and with eating-disorder symptoms, such as eating concern, shape concern, and weight concern, in adults with overweight/obesity seeking treatment for weight loss in primary care (n = 129) [21]; with eating disorders in obese bariatric surgery candidates (n = 337) [22], and with under-estimation of obesity status in patient with class II obesity (n = 173) [23]. In patients with BED seeking treatment for obesity (n = 326) high EOQ scores were associated with difficulties with emotion regulation and depression [24]. In Veterans with obesity (n = 120) emotional eating was associated with post-traumatic stress disorder [25]. Finally, in a community sample (n = 330), EOQ scores were higher in participants with food addiction compared with those who were not [26].
Association with demographic variables showed that EOQ scores were generally unrelated to sex, age, and BMI, although a study of patients with BED and obesity [24] found an association with sex. In the literature of emotional eating in community samples, the effects of age and education were non-significant [7, 18], while women reported more frequent emotional eating behavior than men [9, 15, 18] and negative emotional eating was associated with higher BMI [5, 9, 15].
Based on the literature, the following hypotheses were postulated for this study: (1) emotional overeating would be positively associated with binge eating [21, 22] and the EOQ would demonstrate good sensitivity and specificity in identifying people at risk for BED, (2) emotional overeating would be negatively associated with mental well-being due to its positive association with depression [12, 24], (3) emotional overeating would be associated with mindless eating due to difficulties in recognizing internal cues of hunger and satiety as suggested by Bruch [27] and found in patients with BED and obesity [24], (4) emotional overeating would be more frequent in females than males [9, 15, 18, 24], and not related to age or education [7, 18], and (5) emotional overeating would be more frequent in participants with obesity or overweight than those of normal weight [5, 9, 15].
Method
Participants and procedure
A total of 392 volunteer adults responded to an advertisement on community services pages of three Italian cities asking to complete an online questionnaire for a research on eating behavior. Once the participant reached the online questionnaire initial page, a detailed description of the research was provided with the researchers’ names and e-mail addresses, information regarding the privacy and data treatment, and informed consent to participate that was given by clicking on the “yes, I consent to participate” button. Inclusion criteria were older than 18 years, native Italian-speaking, and not being diagnosed with any eating disorder. The final sample included 314 participants (80.1% of the initial sample); 78 questionnaires were excluded using listwise deletion due to 5–7% missing items in any of the considered variables, after observing that missingness was completely at random and the number of deleted cases did not dramatically affect the statistical power. No sociodemographic differences were found between who completed and who did not complete the questionnaire. Women were 72.6%; the age range was 18–76 years, Mage = 35.75, SD= 13.61; 51% had a bachelor’s degree or higher; BMI range was 18.51–66.10, MBMI = 27.13, SD= 8.11. Participants were classified into three categories based on the world health organization standards: 27.4% (n = 86) had obesity (BMI ≥ 30 kg/m2), 21.3% (n = 67) were of overweight (BMI 25–29.9 kg/m2), and 51.3% (n = 161) were of normal weight (BMI 18.5–24.9 kg/m2). It is noteworthy that, although all participants were self-selected volunteers, the prevalence of people with BMI ≥ 25 kg/m2 in this study (49%) was almost representative of the Italian population (49.8%) [28]. Among the final sample, 70 participants were randomly selected and invited to answer the EOQ again after 4 weeks via an online survey to assess test–retest reliability of the EOQ. Sixty participants completed the retest with a response rate of 85.7%.
Measures
The EOQ [12] is a 6-item measure of the frequency, over the prior 28 days, of overeating in response to anxiety, sadness, loneliness, tiredness, anger, and happiness. Participants rate the frequency of overeating in response to each emotion on a 7-point scale (0 = no days, 1 = 1–5 days, 2 = 6–12 days, 3 = 13–15 days, 4 = 16–22 days, 5 = 23–27 days, and 6 = everyday). Responses to the six items are generally summed up to form a global emotional overeating score, with higher score indicating more frequent emotional overeating. For the purposes of this study, the EOQ was translated into Italian and backtranslated by two independent bilingual psychologists.
The binge eating scale (BES) [29], Italian version [30], is a 16-item measure of binge eating behavior that uses a 3- or 4-point response format. The questions are mainly based upon the amount of food consumed, the perceived control over eating behavior, and a feeling of guilt after overeating. Scores range from 0 to 46, with individuals scoring > 17 considered moderate to severe binge eaters and thus at risk for BED [29]. Cronbach’s α in our sample was 0.91.
The 5-item world health organization well-being index (WHO-5) is a widely used 5-item measure of subjective psychological well-being. It is a sensitive and specific screening tool for depression and has been applied successfully across a wide range of study fields [31]. In this study Cronbach’s α was 0.88.
The mindful eating questionnaire, Italian version (MEQ-20) [32] is a 20-item short form of the MEQ [33] developed to measure mindful eating. It is formed by two subscales: Recognition when being hungry or full and Awareness of how food affects the senses. In this study, Cronbach’s α was 0.76 for Recognition and 0.80 for Awareness.
Information was also collected on sex, age, educational level, and self-reported height and weight to calculate the BMI.
Data analyses
Skewness, kurtosis, mean and median values were preliminary calculated for each EOQ item. Descriptive statistics, including skewness and kurtosis, were also calculated for the summative score of all the psychological scales. At the item level, the EOQ was submitted to CFA to test for the original 6-item one-factor model [12] and an alternative one-factor model with only the five negative emotional items [20]. We used the robust unweighted least squares (RULS) method for ordinal-observed variables with polychoric correlations and asymptotic covariance matrices [34]. Goodness of fit was evaluated using the following criteria: ratio of the Satorra–Bentler scaled χ2 to its degrees of freedom (S-B χ2/df) ≤ 5 [35], standardized root mean-square residual (SRMR; cutoff < 0.08), non-normative (NNFI) and comparative (CFI) fit indices (cutoff ≥ 0.95) [36]. The Aikake Information Criterion (AIC) was also inspected, with lower values indicating a better fit [37]. Internal consistency was tested using McDonald’s ω and ordinal α, and 4-week test–retest reliability was tested with Cohen’s weighted Kappa coefficient to measure agreement in ordinal data with Kw > 0.60 good [38].
At the EOQ summative scale level, partial Spearman’s rank correlations (rs) with BES, WHO-5, and MEQ were calculated by BMI category controlling for the effect of sex, due to the non-normal distribution of the EOQ total score. Receiver Operating Characteristic (ROC) curve was calculated to estimate sensitivity and specificity of the EOQ score in relation to binge eating as measured with the BES using a cut-off > 17 [29].
For group differences we used ANOVA with Dunnett’s T3 for multiple comparisons. To control for Type I error Welch’s adjustment was used for independent groups with nonnormally distributed data and heterogeneous variances [39] (Levene statistic based on median was 4.17, p = 0.001).
Significance was set at p ≤ 0.05. Effect size according to Cohen was rs of 0.10 small, 0.30 medium, and 0.50 large; d of 0.20 small, 0.50 medium, and 0.80 large [40]. CFAs were performed with LISREL 8.80 and the other analyses with IBM-SPSS 25.
Results
Factor structure and reliability of the EOQ
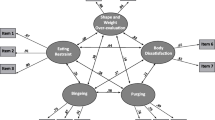
Preliminary analyses showed that all EOQ items had frequency distributions that were positively skewed (values between 1.44 and 1.81) and leptokurtic (values between 1.60 and 2.77). Median values were between 0 and 1 showing floor effects. Skewness, kurtosis, and the mean and median values for each EOQ item are reported in Table 1. The model fit of the 6-item one-factor EOQ was nonoptimal (S-B \(\chi_{9}^{2}\) = 57.27, p < 0.001; S-B χ2/df = 6.36; SRMR = 0.06; NNFI = 0.93; CFI = 0.96). The alternative 5-item one-factor model was tested, after removing the happiness item, which had a nonsignificant factor loading (λ = 0.09, p = 0.11) and small correlations with the other items (r = − 0.01 to 0.27). The fit was good (S-B \(\chi_{5}^{2}\) = 20.62, p < 0.001; S-B χ2/df = 4.12; SRMR = 0.03; NNFI = 0.97; CFI = 0.99), with all items loading highly on the latent factor (λ = 0.67–0.89, p < 0.001) and error variances in the 0.20–0.56 range (Fig. 1). The AIC-value (50.62) for the 5-item model was lower and thus better than that for the 6-item model (AIC = 93.27). The 5-item one-factor model had also a higher McDonald’s coefficient (ω = 0.89) compared to the 6-item one-factor model (ω = 0.84).
The sum of the five items (EOQ-5) formed an index of negative emotional overeating (scores range 0–35), while the happiness item was dropped. Internal consistency was optimal also with the ordinal α coefficient (α = 0.88), and test–retest reliability was good with Kw= 0.71.
In the EOQ-5, none of the participants returned a total score of zero, indicating that all of them had at least one episode of negative emotional overeating within the past 28 days. The frequency distribution of the EOQ-5 scale was moderately skewed and leptokurtic (Table 1).
Correlations with other measures and sensitivity/specificity
Preliminary analyses showed that the BES, the WHO-5, and the MEQ scales were close to normally distributed (Table 1). As shown in Table 2, controlling for the effect of sex, EOQ-5 was associated with BES among all BMI groups with significant and strong positive correlations. A BES cut-off > 17 identified 76 (24.2%) participants who were at risk for BED and 238 (75.8%) who were not. The median value of the EOQ-5 scale in the whole sample was 2 and a value > 2 provided the best compromise between sensitivity (75%) and specificity (67%) in discriminating participants who were at risk for BED from those who were not, based on the BES cut-off.
EOQ-5 significantly and negatively correlated with WHO-5 with large, medium, or small effect sizes among participants with obesity, overweight and normal weight, respectively.
Correlations were significant, negative and strong with MEQ-Recognition among participants with obesity, and moderate among both overweight and normal-weight participants. Correlations with MEQ-Awareness were small to negligible among all BMI groups.
Associations with demographic characteristics and BMI
The EOQ-5 was not significantly associated with age (rs= 0.05, p = 0.38) or education [Welch’s F(2145.79) = 0.59, p = 0.53]. ANOVAs were run for sex differences separately among each BMI category and for BMI differences separately among women and men using post hoc tests when appropriate. Table 3 shows descriptive statistics and main effects of sex and BMI in the subgroups. Women scored higher than men among participants with obesity (p = 0.04, Cohen’s d = 0.46) and with overweight (p = 0.02, Cohen’ d = 0.57), with almost medium effect sizes, while no sex differences were found among participants of normal weight. Among women, those with obesity scored higher than women of normal weight (p < 0.001, Cohen’s d = 0.72) with medium effect size, while women with overweight did not differ from both the other groups of women. Among men there were no differences in EOQ-5 according to BMI.
Discussion
In the present study we found the negative emotions of the 5-item EOQ to be a reliable single factor of emotional eating with adequate internal consistency and test–retest reliability. EOQ-5 scores were associated with higher binge eating, lower mental well-being, and lower mindful eating. A cut-off score of 2 identified individuals at risk for binge eating disorders with 75% sensitivity and 67% specificity. Negative emotional overeating was more frequent in women with obesity than women with normal weight and men with obesity.
The EOQ one-factor structure was consistent with a previous non-clinical female student sample [20], but unlike the original EOQ two-factor structure found in a clinical sample of patients with BED [12]. This may have been due to different emotional overeating patterns between patients with BED and non-clinical participants [41].
In our community sample, although participants who reported a diagnosis of eating disorder were excluded, overeating in response to negative emotions was associated with the habit of consuming a large amount of food and losing control over food intake, independent of sex and BMI. This result was in line with previous studies where emotional eating was associated with disordered eating behaviors such as binge eating [16, 21, 22, 42]. Emotional overeating might represent a risk eating behavior, as a cutoff score greater than two on the EOQ-5 scale identified people who might be at risk for BED in the present study.
In this study, negative emotional overeating was associated with poor perceived mental well-being and this association was the strongest among participants with obesity. This result was in line with previous studies of patients with BED [12, 24]. Finally, negative emotional overeating was associated with poor recognition of hunger and satiety. This might be explained by the difficulties in emotion regulation that characterize people who overeat in response to emotional cues instead of eating in response to hunger sensations [24, 27].
The EOQ-5 was not associated with age or education as has been reported in previous studies [7, 18]. Also consistent with non-clinical samples was that we found women to report more frequent emotional overeating behavior than men [9, 15, 18, 24]. In the literature, negative emotional eating was generally associated with higher BMI [5, 9, 15], while in our study EO was associated with higher BMI only among women.
In studies of patients with BED using the EOQ [12, 43], neither sex differences nor associations with BMI were found. This might indicate that within BED, other mechanisms than emotional overeating may play a role in weight regulation. However, in those studies, the constrained BMI range (all participants had a BMI ≥ 25) may have limited the observation of different emotional overeating frequencies according to BMI.
The present study has several limitations. First, it used a cross-sectional design that did not allow causal inferences. Second, it used a sample of convenience which limited the generalizability of findings. Indeed, women and more educated people were over-represented, as they are usually more likely to participate in surveys [44]. Third, BMI relied on self-reported height and weight and a large body of literature demonstrates that people systematically overestimate their height and underestimate their weight [e.g., 45, 46], although high correlations were also found between self-reported weight and height and objective measurements [46]. Finally, since the single item referring to happiness was discarded, future studies should develop a brief multi-item measure of the frequency of positive emotional overeating and investigate its relationship with the EOQ-5.
In conclusion, the results of our psychometric analyses support the use of the EOQ-5 as a brief, valid and reliable tool to measure the frequency of overeating behavior in response to negative emotions in Italian non-clinical adults. The findings of this study suggest that, in an adult community sample, emotional overeating in response to negative or positive emotions, as measured by the original EOQ [12], refers to two unrelated dimensions. Although the present study needs replication, it may help gain some insights into emotional overeating behavior, which might be a risk factor for overweight, obesity, BED, and reduced mental wellbeing.
In clinical contexts, the EOQ-5 could be used to test for improvements of eating behavior after treatments since emotional overeating is a learned behavior that can be modified with practice [3]. The associations found in this study between emotional overeating and mindful eating suggest that mindfulness-based eating interventions could effectively apply to emotional eaters, as it was found in 63% of the studies reviewed by O’Reilly et al. [47] as well as in a more recent study [48].
Data availability
The datasets generated and analysed during the current study are available from the corresponding author on reasonable request.
References
van Strien T, Ouwens MA (2007) Effects of distress, alexithymia and impulsivity on eating. Eat Behav 8:251–257. https://doi.org/10.1016/j.eatbeh.2006.06.004
Sultson H, Kukk K, Akkermann K (2017) Positive and negative emotional eating have different associations with overeating and binge eating: construction and validation of the positive-negative emotional eating scale. Appetite 116:423–430. https://doi.org/10.1016/j.appet.2017.05.035
Frayn M, Knäuper B (2018) Emotional eating and weight in adults: a review. Curr Psychol 37:924–933. https://doi.org/10.1007/s12144-017-9577-9
Lindeman M, Stark K (2001) Emotional eating and eating disorder psychopathology. Eat Disord 9:251–259. https://doi.org/10.1080/10640260127552
Konttinen H, Männistö S, Sarlio-Lähteenkorva S, Silventoinen K, Haukkala A (2010) Emotional eating, depressive symptoms and self-reported food consumption. A population-based study. Appetite 54:473–479. https://doi.org/10.1016/j.appet.2010.01.014
Poínhos R, Oliveira BM, Correia F (2018) Psychopathological correlates of eating behavior among Portuguese undergraduate students. Nutrition 48:33–39. https://doi.org/10.1016/j.nut.2017.10.009
Bourdier L, Orri M, Carre A et al (2018) Are emotionally driven and addictive-like eating behaviors the missing links between psychological distress and greater body weight? Appetite 120:536–546. https://doi.org/10.1016/j.appet.2017.10.013
Braden A, Musher-Eizenman D, Watford T, Emley E (2018) Eating when depressed, anxious, bored, or happy: are emotional eating types associated with unique psychological and physical health correlates? Appetite 125:410–417. https://doi.org/10.1016/j.appet.2018.02.022
Gibson EL (2012) The psychobiology of comfort eating: implications for neuropharmacological interventions. Behav Pharmacol 23:442–460. https://doi.org/10.1097/FBP.0b013e328357bd4e
Williams EP, Mesidor M, Winters K, Dubbert PM, Wyatt SB (2015) Overweight and obesity: prevalence, consequences, and causes of a growing public health problem. Curr Obes Rep 4:363–370. https://doi.org/10.1097/00000441-200604000-00002
Grace C (2011) A review of one-to-one dietetic obesity management in adults. J Hum Nutr Diet 24:13–22. https://doi.org/10.1111/j.1365-277X.2010.01137.x
Masheb RM, Grilo CM (2006) Emotional overeating and its associations with eating disorder psychopathology among overweight patients with binge eating disorder. Int J Eat Disord 39:141–146. https://doi.org/10.1002/eat.20221
Celio AA, Wilfley DE, Crow SJ, Mitchell J, Walsh BT (2004) A comparison of the binge eating scale, questionnaire for eating and weight patterns-revised, and eating disorder examination questionnaire with instructions with the eating disorder examination in the assessment of binge eating disorder and its symptoms. Int J Eat Disord 36:434–444. https://doi.org/10.1002/eat.20057
Fairburn CG, Cooper Z, O’Connor M (2014) The eating disorder examination, 17th ed. The centre for research on eating disorders at Oxford http://www.credo-oxford.com/pdfs/EDE_17.0D.pdf. Accessed 4 April 2019
van Strien T, Frijters JE, Bergers GP, Defares PB (1986) The dutch eating behavior questionnaire (DEBQ) for assessment of restrained, emotional, and external eating behavior. Int J Eat Disord 5:295–315. https://doi.org/10.1002/1098-108X(198602)5:2%3c295:AID-EAT2260050209%3e3.0.CO;2-T
Arnow B, Kenardy J, Agras WS (1995) The emotional eating scale: the development of a measure to assess coping with negative affect by eating. Int J Eat Disord 18:79–90. https://doi.org/10.1002/1098-108X(199507)18:1%3c79:AID-EAT2260180109%3e3.0.CO;2-V
Geliebter A, Aversa A (2003) Emotional eating in overweight, normal weight, and underweight individuals. Eat Behav 3:341–347. https://doi.org/10.1016/S1471-0153(02)00100-9
Meule A, Reichenberger J, Blechert J (2018) Development and preliminary validation of the salzburg emotional eating scale. Front Psychol 9:88. https://doi.org/10.1016/j.appet.2017.10.003
Weineland S, Alfonsson S, Dahl J, Ghaderi A (2012) Development and validation of a new questionnaire measuring eating disordered behaviours post bariatric surgery. Clin Obesity 2:160–167. https://doi.org/10.1111/cob.12005
Constant A, Gautier Y, Coquery N et al (2018) Emotional overeating is common and negatively associated with alcohol use in normal-weight female university students. Appetite 129:186–191. https://doi.org/10.1016/j.appet.2018.07.012
Wiedemann AA, Ivezaj V, Barnes RD (2018) Characterizing emotional overeating among patients with and without binge-eating disorder in primary care. Gen Hosp Psychiatry 55:38–43. https://doi.org/10.1016/j.genhosppsych.2018.09.003
Hrabosky JI, White MA, Masheb RM et al (2008) Psychometric evaluation of the eating disorder examination-questionnaire for bariatric surgery candidates. Obesity 16:763–769. https://doi.org/10.1038/oby.2008.3
Jones M, Grilo CM, Masheb RM, White MA (2010) Psychological and behavioral correlates of excess weight: misperception of obese status among persons with Class II obesity. Int J Eat Disord 43:628–632. https://doi.org/10.1002/eat.20746
Gianini LM, White MA, Masheb RM (2013) Eating pathology, emotion regulation, and emotional overeating in obese adults with binge eating disorder. Eat Behav 14:309–313. https://doi.org/10.1016/j.eatbeh.2013.05.008
Dorflinger LM, Masheb RM (2018) PTSD is associated with emotional eating among veterans seeking treatment for overweight/obesity. Eat Behav 31:8–11. https://doi.org/10.1016/j.beh.2018.07.005
Brunault P, Courtois R, Gearhardt AN et al (2017) Validation of the French version of the DSM-5 Yale food addiction scale in a nonclinical sample. Canadian J Psychiatry 62:199–210. https://doi.org/10.1177/0706743716673320
Bruch H (1961) Social and emotional factors in diet changes. J Am Dent Assoc 63:461–465. https://doi.org/10.14219/jada.archive.1961.0243
Ng M, Fleming T, Robinson M et al (2014) Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 384:766–781. https://doi.org/10.1016/S0140-6736(14)60460-8
Gormally J, Black S, Daston S, Rardin D (1982) The assessment of binge eating severity among obese persons. Addict Behav 7:47–55. https://doi.org/10.1016/0306-4603(82)90024-7
Imperatori C, Innamorati M, Lamis DA et al (2016) Factor structure of the Binge Eating Scale in a large sample of obese and overweight patients attending low energy diet therapy. Eur Eat Disorders Rev 24:174–178. https://doi.org/10.1002/erv.2384
Topp CW, Østergaard SD, Søndergaard S, Bech P (2015) The WHO-5 well-being index: a systematic review of the literature. Psychother Psychosom 84:167–176. https://doi.org/10.1159/000376585
Clementi C, Casu G, Gremigni P (2017) An abbreviated version of the Mindful Eating Questionnaire. J Nutr Educ Behav 49:352–356. https://doi.org/10.1016/j.jneb.2017.01.016
Framson C, Kristal AR, Schenk JM et al (2009) Development and validation of the mindful eating questionnaire. J Am Diet Assoc 109:1439–1444. https://doi.org/10.1016/j.jada.2009.05.006
Morata-Ramírez MA, Holgado-Tello FP (2013) Construct validity of Likert scales through confirmatory factor analysis: a simulation study comparing different methods of estimation based on Pearson and polychoric correlations. Int J Soc Sci Stud 1:54–61. https://doi.org/10.11114/ijsss.v1i1.27
Wheaton B, Muthen B, Alwin DF, Summers GF (1977) Assessing reliability and stability in panel models. Sociol Methodol 8:84–136. https://doi.org/10.2307/270754
Hu L, Bentler PM (1999) Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Modeling 6:1–55. https://doi.org/10.1080/10705519909540118
Kline R (2011) Principles and practice of structural equation modeling, 3rd edn. Guilford, New York
Altman DG (1991) Practical statistics for medical research, 1st edn. Chapman & Hall, London
Cribbie RA, Wilcox RR, Bewell C, Keselman HJ (2007) Tests for treatment group equality when data are nonnormal and heteroscedastic. J Mod Appl Stat Methods 6:117–132. https://doi.org/10.22237/jmasm/1177992660
Cohen J (1992) A power primer. Psychol Bull 112:155–159 (PMID:19565683)
Nolan LJ, Halperin LB, Geliebter A (2010) Emotional appetite questionnaire. construct validity and relationship with BMI. Appetite 54:314–319. https://doi.org/10.1016/j.appet.2009.12.004
Duarte C, Pinto-Gouveia J (2015) Returning to emotional eating: the emotional eating scale psychometric properties and associations with body image flexibility and binge eating. Eat Weight Disord 20:497–504. https://doi.org/10.1007/s40519-015-0186-z
Udo T, McKee SA, White MA et al (2013) Sex differences in biopsychosocial correlates of binge eating disorder: a study of treatment-seeking obese adults in primary care setting. Gen Hosp Psychiatry 35:587–591. https://doi.org/10.1016/j.genhosppsych.2013.07.010
Angus VC, Entwistle VA, Emslie MJ, Walker KA, Andrew JE (2003) The requirement for prior consent to participate on survey response rates: a population-based survey in Grampian. BMC Health Serv Res 3:21. https://doi.org/10.1186/1472-6963-3-21
Niedhammer I, Bugel I, Bonenfant S, Goldberg M, Leclerc A (2000) Validity of self-reported weight and height in the French GAZEL cohort. Int J Obesity 24:1111–1118. https://doi.org/10.1038/sj.ijo.0801375
Kuczmarski MF, Kuczmarski RJ, Najjar M (2001) Effects of age on validity of self-reported height, weight, and body mass index: findings from the Third National Health and Nutrition Examination Survey, 1988–1994. J Am Diet Assoc 101:28–34. https://doi.org/10.1016/S0002-8223(01)00008-6
O’Reilly GA, Cook L, Spruijt-Metz D, Black DS (2014) Mindfulness-based interventions for obesity-related eating behaviours: a literature review. Obes Rev 15:453–461. https://doi.org/10.1111/obr.12156
Lattimore P (2019) Mindfulness-based emotional eating awareness training: taking the emotional out of eating. Eat Weight Disord St. https://doi.org/10.1007/s40519-019-00667-y
Funding
No funds were received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the University of Bologna Bioethical Committee, which approved the study protocol, and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Casu, G., Gremigni, P. & Masheb, R.M. Emotional overeating questionnaire: a validation study in Italian adults with obesity, overweight or normal weight. Eat Weight Disord 25, 1747–1754 (2020). https://doi.org/10.1007/s40519-019-00821-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-019-00821-6