Abstract
The age-related resistance to thyroid hormones (THs) explains the paucity of symptoms and signs of hyperthyroidism in older adults and may partly explain the myriad of symptoms and signs of hypothyroidism in biochemically euthyroid older people. This review considers the available data on the mechanisms underlying TH resistance with aging and compares these physiologic changes with the changes observed in congenital TH resistance syndromes. Aging is associated with alterations in TH economy along with a host of changes in the responsiveness of various tissues to THs. The age-related resistance to THs can be attributed to decreased TH transport to tissues, decreased nuclear receptor occupancy, decreased activation of thyroxine to triiodothyronine, and alterations in TH responsive gene expression. Although an increase in serum TH levels is expected in syndromes of TH resistance, unchanged serum TH levels in the euthyroid elderly is the result of increased sensitivity to TH negative feedback with increased suppression of thyroid-stimulating hormone, decreased thyroidal sensitivity to thyroid-stimulating hormone, and decreased TH production and secretion. The current clinical evidence suggests that the age-related TH resistance is mostly an adaptive response of the aging organism. It is tempting to speculate that similar changes can occur prematurely in a group of younger people who present with signs and symptoms of hypothyroidism despite normal serum thyroid function tests.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The age-related resistance to thyroid hormones (THs) explains the paucity of symptoms and signs of hyperthyroidism in older adults and may explain the hypothyroid phenotype in euthyroid older people. |
TH resistance is the result of changes in TH economy and cellular biology. |
Similar changes may occur prematurely in a group of younger people who present with signs and symptoms of hypothyroidism despite normal serum TH levels. |
1 Introduction
Aging is associated with a host of hormonal changes [1]. Much of the change is regarded as an adaptive response of an organism attempting to conserve energy, shut down processes that are not essential for individual survival, and to minimize the risk of neoplastic disease [2]. One of the age-related changes in the hormonal milieu that is not widely appreciated is the reduced responsiveness of tissues to thyroid hormone (TH) action. This age-related resistance to TH may partly explain the myriad of symptoms and signs of hypothyroidism that older subjects exhibit despite normal plasma levels of TH [3, 4]. It can also account for the paucity of symptoms or signs of excess TH in patients with apathetic hyperthyroidism [5]. In extreme cases, a complete absence of any signs and symptoms of clinical hyperthyroidism may be found in some older patients with overt biochemical hyperthyroidism [5]. However, it is noteworthy that the signs and symptoms of hypothyroidism in older adults are generally not specific and may be related to concomitant diseases such as anemia and sarcopenia.
The interplay between the age-related changes in TH economy and TH action results in a unique syndrome that is distinct from the commonly recognized cases of congenital syndromes of TH resistance. These syndromes are characterized by reduced responsiveness of peripheral tissues to TH, and in most cases, they are the result of germline pathogenic variants in the TH receptor β gene [6]. The biochemical profile of these patients includes elevated plasma levels of TH with normal or mildly elevated plasma levels of thyroid-stimulating hormone (TSH) [6]. In contrast, age-related changes in TH responsiveness are associated with normal plasma levels of TH and TSH.
In this communication, the age-related changes in the TH economy and TH action are reviewed, and the distinctive features of TH resistance in aging are discussed. Relevant manuscripts were identified through a MEDLINE search on 1 April, 2019 of the English-language literature using the key phrase TH resistance and aging. The literature search was limited to core clinical journals that have accessible full texts.
2 Changes in Thyroid Hormone Economy
Several variables commonly found in older adults such as comorbidities, malnutrition, and polypharmacy are known to interfere with TH economy. However, even healthy older adults may have some changes in the TH economy. The changes attributable to aging per se occur at various levels of the hypothalamic-pituitary-thyroid gland axis [3, 4, 7]. There may be a reduction in the thyrotropin-releasing hormone level, as less thyrotropin-releasing hormone is released in vitro by hypothalamic tissue from older as compared with younger rats [8]. Furthermore, pituitary sensitivity to TH negative feedback may be increased [9,10,11]. In a study of 381 men, the steady-state serum free thyroxine (FT4) levels were correlated with the logarithm of serum TSH and the slope of the correlation was determined in 259 men over the age of 60 years (mean ± standard deviation 72.2 ± 8.6) and in 122 subjects aged younger than 60 (45.5 ± 9.4) years [10]. The slope of the curve in older men (− 0.038 ± 0.005) was somewhat lower than that in middle aged men (− 0.055 ± 0.008). However, this difference did not reach statistical significance [10]. These findings may be sex specific as there is a sex-specific response to TH with aging [11]. It is noteworthy that there is also sex- and age-related influences in the relationship between hypothyroidism and the lipid profile [12].
A more direct estimate of pituitary sensitivity to TH was observed by the pituitary response to thyroxine (T4) that is suppressed with exogenous iodide [13]. This study showed that the effectiveness of T4 in suppressing the TSH during hypothyroxinemia is increased in the elderly [13]. These changes could be partially attributed to either increased TH receptors in the pituitary, or more importantly, increased conversion of T4 to triiodothyronine (T3) through increased activity of 5′ deiodinase type 2, as has been previously observed in animal experiments [14, 15]. The central role of 5′ deiodinase type 2 in the TSH response to TH is supported by the observation that selective loss of this enzyme in mouse thyrotrophs blunts the thyrotropin response to hypothyroidism [16].
The neuroendocrine rhythm of TSH secretion is altered in older people with blunting of the nocturnal TSH peak and the circadian rises of TSH occurring 1–1.5 h earlier [17,18,19]. There is a resetting of the pituitary threshold of the TSH feedback suppression and the TSH nocturnal surge may be lost, suggesting hypothalamic dysfunction with age [19].
In aging rats, thyroid gland responsiveness to TSH can also be reduced [20]. In addition to reduced thyroidal secretion of TH, decreased T3 production also occurs in plasma secondary to decreased peripheral conversion of T4 to T3, as a result of a decreased T4 substrate and possibly secondary to reduced activity of 5′ deiodinase type 1 [14]. However, the reduced TH production with age in humans is mostly related to decreased serum TH clearance with a resultant increase in negative feedback inhibition of thyrotropin-releasing hormone and TSH [21]. In general, the serum levels of TH do not change with age as the decreased production of TH is counterbalanced with decreased clearance of TH [21]. However, in older people with frailty, high circulating FT4 levels are observed [22].
Although some studies have reported an age-dependent decline in serum free T3 (FT3) and an increase in reverse T3 (rT3) [23, 24], a more rigorously conducted study found a decreased level of serum FT3 only in centenarians [25]. Thus, the changes in FT3 and rT3 reported with age are probably a reflection of comorbidities or dietary changes that are common in people over the age of 80 years. It is noteworthy that more people in the older age groups may have serum TSH levels below the lower limit or above the higher limit of the reference range for younger people [26, 27]. It appears that the optimum serum TSH level that correlates best with longevity is somewhat higher than the currently accepted upper limit of the TSH reference range [28, 29].
Acute illness, inflammation, and poor nutrition (especially restriction of carbohydrates in the diet) cause a preferential conversion of T4 to rT3 through increased activity of deiodinase type 3 that has inner ring deiodinase activity and degrades T4 to rT3 and T3 to 3,3′-T2 [30]. The degree of peripheral thyroxine deiodination may also have a role in frailty, and long-term survival in hospitalized older patients [31]. Iodothyronine deiodinase types 2 and 3 that convert the prohormone T4 to its bioactive form T3 and degrade T4 to rT3 and T3 to 3,3′-T2, respectively, can locally modify TH bioactivity independent of serum TH levels [31]. Age-related changes of TH metabolism at the tissue level may also play an important role in TH metabolism and action.
3 Changes in Thyroid Hormone Action
Age-related changes in TH action are observed in various tissues including blood cells, thymocytes, and cardiac, renal, hepatic, and cerebral tissues (Table 1) [32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56]. Most of these changes are mediated through the nuclear receptors while some are non-nuclear receptor-mediated effects. The latter category include changes in human red blood cell Ca++ ATP-ase activity [34] and rat thymocyte membrane transport of glucose [36].
The basal levels and the response of the renal cortical Na+–K+–ATP-ase activity are reduced in aging rats [37]. A similar trend was observed in the activity of this enzyme in the liver [37]. Thyroid hormone responsiveness of some lipogenic enzymes such as malic enzyme, glucose-6 phosphate dehydrogenase, and free fatty acid synthase are reduced in aged rats [39, 40]. The responsiveness of apolipoprotein A1 gene to TH is also reduced with aging [41], and the age-related changes in the responsiveness of Spot 14, a gene product implicated in lipogenesis, is attributed to alterations of key transcription factors notably P-1 and PS-1 [42].
In the heart, there are age-related changes in TH effects on sarcoplasmic Ca2+ ATPase [43], β-myosin heavy chain [44, 45], glucose transporter 1 [46], and in the number of β-adrenergic receptors and the response of isoproterenol-stimulated adenylate cyclase activity [47, 48]. The inductive effects of T3 on epidermal growth factor in the submandibular glands is reduced with aging [49, 50]. This response is observed only in female mice. These observations highlight sex specificity of the age-related changes in TH action [49, 50].
The effect of age on the TH responsiveness of the cerebral cortex is not well studied as there are only a few biomarkers of TH action in the brain of mature animals [51]. The TH responsiveness of β-adrenergic receptor activity in synaptosomal membranes and cerebral microvessels is reduced in aged rats [52, 53]. Cerebral glucose transporter 1 expression in response to TH is also altered in aging rats such that the 55-kDa moiety of glucose transporter 1 in hyperthyroid young rats is decreased while in aged rats it is increased [54]. Two markers of TH action in the brain, namely thyroid hormone responsive protein (THRP) and novel translational repressor (NAT-1), also show a significant reduction in TH responsiveness in senescent rats [55, 56].
The overall metabolic response of rats to TH is reduced with aging. The ethane exhalation following TH treatment, a function of metabolism and lipid peroxidation, is reduced in aging rats [57]. Thus, most of the changes with age show a decreased responsiveness to TH. One glaring exception is the effect of TH on body weight. Older rats lose more weight during experimental hyperthyroidism than younger rats [58]. Thus, differential weight loss was entirely the result of a decreased food intake in aging rats.
4 Mechanisms of Reduced Thyroid Hormone Responsiveness
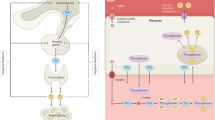
There are several alterations that can possibly explain the age-related resistance to TH (Fig. 1). These include decreased TH transport to the tissues, decreased nuclear receptor occupancy, decreased activation of thyroxin to T3, and alterations in TH responsive gene expression [4].
At steady-state conditions, T3 uptake by the liver, heart, and rectus abdominis muscle is reduced in aged rats [59]. In cerebral tissue, the blood–brain transport of T3 is also reduced with aging [60]. Transport of T3 across plasma membranes is a carrier-mediated process that has been shown to be reduced by 50% in the liver of old rats, leading to a decrease in the number of nuclear receptors occupied by T3, while receptor affinity for T3 (association constant) measured in vitro is unchanged [59]. However, a study of nuclear binding to TH in human mononuclear cells found that there is an age-related decline in nuclear binding of TH, while the association constant for T4 was increased and that of T3 was decreased [61].
Another important alteration with age that contributes to apparent TH resistance is changes in the tissue-specific deiodinase activity that would limit intracellular activation of T4 to T3. Aging is associated with an increase in the activity of 5′-deiodinase in the adenohypophysis, while 5′-deiodinase activity in the liver and thyroid gland is reduced [14]. However, the total conversion of T4–T3 in vivo is increased in older animals [62]. More importantly, there may be alterations in post-receptor processes that modulate gene expression. These could be related to alterations in transcription factors or secondary to structural changes of the gene such as altered methylation [4, 42]. In a seminal article, Visser et al. reported a significant common transcriptomic signature in livers from hypothyroid mice, DNA repair-deficient mice with severe or intermediate progeria, and naturally aged mice [63]. Induction of TH-inactivating deiodinase type 3 and a decrease of TH-activating deiodinase type 1 activities were observed in naturally aged animals, in mice with a progeria-like syndrome, and in wild-type mice exposed to a long-term sub-toxic dose of DNA-damaging agents [63]. In contrast, TH signaling in the muscle, heart, and brain was unaltered. These data highlight the importance of DNA damage as the underlying mechanism of suppression of TH signaling in specific organs in premature and normal aging. Diminished TH signaling may contribute to the protective metabolic response in aging [63].
5 Age-Related vs. Congenital Thyroid Hormone Resistance
One of the biochemical hallmarks of congenital TH resistance is increased FT4 and FT3 with normal or mildly elevated serum TSH levels [6, 64]. Although an increase in serum TH levels is expected in a syndrome characterized by resistance to TH action, unchanged serum TH levels in euthyroid elderly people may be secondary to confounding physiological changes with age, including increased sensitivity to TH negative feedback with increased suppression of TSH, decreased thyroidal sensitivity to TSH, and decreased TH production and secretion [4]. The combination of peripheral tissue resistance to TH action coupled by a lack of compensatory increase in plasma TH levels would potentially result in clinical or organ-specific hypothyroidism despite normal plasma TH levels. It is noteworthy that most of the evidence for age-related resistance to TH is derived from studies in animal models. Given the species specificity of TH actions, caution should be exercised when extrapolating the observations made in animal models to a clinical setting.
6 Is Thyroid Hormone Resistance in Aging Adaptive or Maladaptive?
An important area of uncertainty is the question whether supplementing euthyroid elderly patients with thyroxine would ameliorate some of the age-related changes that resemble hypothyroidism. The small number of clinical trials in older people with subclinical hypothyroidism and the observations made in older adults with subclinical hyperthyroidism suggest that age-related TH resistance is mostly an adaptive response of the aging organism.
Although subclinical hypothyroidism (normal FT4 and TSH < 10 and more than the upper limit of the normal reference range) in a younger population (younger than 65 years) may be associated with cardiovascular disease, stroke, and vascular dementia [65,66,67,68], in older people over the age of 75 years, there are no significant clinical sequelae of subclinical hypothyroidism [68,69,70,71,72,73] except possibly depression [74]. In a study of 559 Dutch individuals aged 85 through 89 years, subclinical or overt hypothyroidism was not associated with either depressive symptoms or impaired physical and cognitive function [72]. More importantly, mild TSH elevation in older adults aged 85 years or older was associated with longevity advantage [27, 72, 73], while higher levels of serum T4 were associated with increased mortality [72]. In another study of 403 independently living ambulatory men aged 73–94 years, low serum FT4 was associated with increased 4-year survival [28]. However, some studies do not support these observations. A meta-analysis of population-based prospective cohort studies found higher mortality rates associated with subclinical hypothyroidism for all age groups [65]. The contemporary data suggest that older people with low serum T3 levels may be subdivided into two groups: those with low serum FT4 and normal rT3, in whom a longer survival is expected, and those with mild non-thyroidal illness with high serum rT3 and FT4 [75].
There are several potential explanations for increased survival in older people with mild hypothyroidism. Overall reduced metabolic rate is associated with increased survival across species. Life-span extension with calorie restriction has been partly attributed to reduced metabolic rate, reduced oxidative load, reduced adrenergic tone, and down-regulation of thyroid function [76,77,78,79].
In contrast to the paucity of clinical sequelae of subclinical hypothyroidism in older adults, subclinical hyperthyroidism (low TSH especially < 0.10 mIU/L with normal FT4 and FT3) is associated with deleterious effects on the cardiovascular system, bone, and cognitive function [80,81,82,83,84,85,86]; three organ systems that undergo significant functional decline with age. In a study of 672 Italian subjects (age range 52–113 years), the investigators observed that the FT3 level and FT3/FT4 ratio decrease while FT4 and TSH increase in an age-dependent manner. In centenarians aged 105 years or older, a higher FT4 level and lower FT3/FT4 ratio are associated with an impaired functional status and an increased mortality [87]. However, there was large heterogeneity in thyroid function tests of centenarians that was related to different health, functional, and cognitive status [87].
Interventional trials with thyroxine supplementation in older patients with subclinical or mild hypothyroidism did not find any clinically and functionally beneficial outcomes [88]. In a double-blind, randomized, placebo-controlled trial involving 737 adults who were at least 65 years of age (mean age of 74.4 years) and who had FT4 levels within the reference range and thyrotropin levels of 4.60–19.99 mIU/L (mean of 6.40 ± 2.01 mIU/L), thyroxine supplementation did not improve the two primary outcomes, namely a change in the hypothyroid symptoms score and tiredness score on a thyroid-related quality-of-life questionnaire. Thyroid hormone therapy did not have any apparent benefits in older adults with subclinical hypothyroidism [88].
These observations taken together suggest that age-related TH resistance is adaptive. Whether it can become maladaptive in a subgroup of older people remains to be seen. The clinical impact of this adaptive or maladaptive change is not known. Studies of thyroid function in centenarians as a model of healthy aging would be helpful to elucidate possible TH-related adaptive mechanisms to attain longevity [89].
7 Future Directions of Research
The age-related change in TH responsiveness is the result of complex coordinated changes at multiple levels of TH economy and cellular biology. It is tempting to speculate that similar changes can occur prematurely in a group of younger people who present with signs and symptoms of hypothyroidism despite normal serum thyroid function tests. Progress in this area has been hampered by the lack of reliable and easily quantifiable tissue biomarkers of TH action. Future research should strive to identify such biomarkers, develop laboratory tools to measure cellular TH transport and deiodination capacity, elucidate the role of potential inhibitors of TH action such as thyronamines [90], and expand the armamentarium of tissue-specific analogs of TH [91].
References
Nowak FV, Mooradian AD. Endocrine function and dysfunction. In: Birren JE, editor. Encyclopedia of gerontology: age, aging, and the aged, vol. 1. 2nd ed. San Diego (CA): Elsevier Inc.; 2007. p. 480–93.
Mooradian AD. Biology of aging. In: Felsenthal G, Garrison SJ, Steinberg FU, editors. Rehabilitation of the aging and elderly patient. Baltimore (MD): Williams and Wilkins; 1994. p. 3–10.
Oiknine RF, Mooradian AD. Thyroid disorders. In: John Pathy MS, Sinclair AJ, Morley JE, editors. Principles and practice of geriatric medicine, vol. 2. 4th ed. Hoboken: Wiley; 2006. p. 1405–14.
Mooradian AD, Wong NCW. Age-related changes in thyroid hormone action. Eur J Endocrinol. 1994;131:451–61.
Mooradian AD. Asymptomatic hyperthyroidism in older adults: is it a distinct clinical and laboratory entity? Drugs Aging. 2008;25:371–80.
Concolino P, Costella A, Paragliola RM. Mutational landscape of resistance to thyroid hormone beta (RTHβ). Mol Diagn Ther. 2019;23:353–68.
Mooradian AD. Normal age-related changes in thyroid hormone economy. Clin Geriatr Med. 1995;11:159–69.
Pekary AE, Mirell CJ, Turner LF Jr, Walfish PG, Hershman JM. Hypothalamic secretion of thyrotropin releasing hormone declines in aging rats. J Endocrinol. 1987;114:271–7.
Lewis GF, Alessi CA, Imperial JG, Refetoff S. Low serum free thyroxine index in ambulating elderly is due to a resetting of the threshold of thyrotropin feedback suppression. J Clin Endocrinol Metab. 1991;73:843–9.
Friedman D, Reed RL, Mooradian AD. The prevalence of overmedication with levothyroxine in ambulatory elderly patients. Age. 1992;15:9–13.
Suzuki S, Nishio S, Takeda T, Komatsu M. Gender-specific regulation of response to thyroid hormone in aging. Thyroid Res. 2012;5:1.
Tognini S, Polini A, Pasqualetti G, Ursino S, Caraccio N, Ferdeghini M, et al. Age and gender substantially influence the relationship between thyroid status and the lipoprotein profile: results from a large cross-sectional study. Thyroid. 2012;22:1096–103.
Ordene KW, Pan C, Barzel US, Surks MI. Variable thyrotropin response to thyrotropin-releasing hormone after small decreases in plasma thyroid hormone concentrations in patients of advanced age. Metabolism. 1983;32:881–8.
Donda A, Lemarchand-Beraud T. Aging alters the activity of 5′-deiodinase in the adenohypophysis, thyroid gland, and liver of the male rat. Endocrinology. 1989;124:1305–9.
Donda A, Reymond MJ, Zurich MG, et al. Influence of sex and age on T3 receptors and T3 concentration in the pituitary gland of the rat: consequences on TSH secretion. Mol Cell Endocrinol. 1987;54:29–34.
Luongo C, Martin C, Vella K, et al. The selective loss of the type 2 iodothyronine deiodinase in mouse thyrotrophs increases basal TSH but blunts the thyrotropin response to hypothyroidism. Endocrinology. 2015;156:745–54.
van Coevorden A, Mockel J, Laurent E, Kerkhofs M, L’Hermite-Balériaux M, Decoster C, et al. Neuroendocrine rhythms and sleep in aging men. Am J Physiol. 1991;260:E651–61.
Barreca T, Franceschini R, Messina V, Bottaro L, Rolandi E. 24-Hour thyroid stimulating hormone secretory pattern in elderly men. Gerontology. 1985;31:119–23.
Monzani F, Del Guerra P, Caraccio N, Del Corso L, Casolaro A, Mariotti S, et al. Age-related modifications in the regulation of the hypothalamic-pituitary-thyroid axis. Horm Res. 1996;46:107–12.
Greeley GH Jr, Lipton MA, Kizer JS. Serum thyroxine, triiodothyronine, and TSH levels and TSH release after TRH in aging male and female rats. Endocr Res Commun. 1982–1983;9:169–77.
Gregerman RI, Gaffney GW, Shock NW, Crowder SE. Thyroxine turnover in euthyroid man with special reference to changes with age. J Clin Invest. 1962;41:2065–74.
Bano A, Chaker L, Schoufour J, et al. High circulating free thyroxine levels may increase the risk of frailty: the Rotterdam Study. J Clin Endocrinol Metab. 2018;103:328–35.
van den Beld AW, Visser TJ, Feelders RA, Grobbee DE, Lamberts SWJ. Thyroid hormone concentration, disease, physical function and mortality in elderly men. J Clin Endocrinol Metab. 2005;90:6403–9.
van Coevorden A, Laurent E, Decoster C, Kerkhofs M, Neve P, van Cauter E, et al. Decreased basal and stimulated thyrotropin secretion in healthy elderly men. J Clin Endocrinol Metab. 1989;69:177–85.
Mariotti S, Barbesino G, Caturegli P, Bartalena L, Sansoni P, Fagnoni F, et al. Complex alteration of thyroid function in healthy centenarians. J Clin Endocrinol Metab. 1993;77:1130–4.
Surks MI, Hollowell JG. Age-specific distribution of serum thyrotropin and antithyroid antibodies in the US population: implications for the prevalence of subclinical hypothyroidism. J Clin Endocrinol Metab. 2007;92:4575–82.
Surks MI, Boucai L. Age- and race-based serum thyrotropin reference limits. J Clin Endocrinol Metab. 2010;95:496–502.
Atzmon G, Barzilai N, Hollowell JG, Surks MI, Gabriely I. Extreme longevity is associated with increased serum thyrotropin. J Clin Endocrinol Metab. 2009;94:1251–4.
Mooradian AD. Subclinical hypothyroidism in the elderly: to treat or not to treat? Am J Ther. 2011;18:477–86.
Peeters RP, Visser TJ. Metabolism of thyroid hormone. Endotext [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK285545/. Accessed 1 Sep 2019.
Pasqualetti G, Calsolaro V, Bernardini S, Linsalata G, Bigazzi R, Caraccio N, et al. Degree of peripheral thyroxin deiodination, frailty, and long-term survival in hospitalized older patients. J Clin Endocrinol Metab. 2018;103:1867–76.
Mooradian AD, Lieberman J. Age-related decrease in serum angiotensin converting enzyme activity: the role of thyroidal status and food intake. J Gerontol Biol Sci. 1990;45:B24–7.
Gambert SR. Effect of age on basal and 3,5,3′ triiodothyronine (T3) stimulated human mononuclear cell sodium-potassium adenosine-triphosphatase (Na+–K+ ATP’ase) activity. Horm Metab Res. 1986;18:649–50.
Davis PJ, Davis FB, Blas SD, Schoenl M, Edwards L. Donor age-dependent decline in response of human red cell Ca2+-ATPase activity to thyroid hormone in vitro. J Clin Endocrinol Metab. 1987;64:921–5.
Davis FB, Deziel MR, Van Liew JB, et al. Effects of caloric restriction and aging on erythrocyte membrane Ca2+-ATPase activity in specific pathogen free Fischer 344 rats. Metabolism. 1991;40:819–24.
Segal J, Troen BR. Effect of age on the 3,5,3′-tri-iodothyronine-induced increase in sugar uptake in rat thymocytes. J Endocrinol. 1986;110:511–5.
Gambert SR, Ingbar SH, Hagen EC. Interaction of age and thyroid hormone status on Na+–K+–ATPase in rat renal cortex and liver. Endocrinology. 1981;108:27–30.
Chehade J, Kim J, Pinnas JL, Mooradian AD. Age-related changes in the thyroid hormone effects on malondialdehyde modified proteins in the rat heart. Proc Soc Exp Biol Med. 1999;222:59–64.
Mooradian AD, Deebaj L, Wong NCW. Age-related alterations in the response of hepatic lipogenic enzymes to altered thyroid states in the rat. J Endocrinol. 1991;128:79–84.
Mooradian AD, Albert SG. The age-related changes in lipogenic enzymes: the role of dietary factors and thyroid hormone responsiveness. Mech Age Develop. 1999;108:139–49.
Mooradian AD, Wong NCW, Shah GN. Age-related changes in the responsiveness of apolipoprotein A1 to thyroid hormone. Am J Physiol. 1996;271:R1602–7.
Mooradian AD, Fox-Robichaud A, Meijer ME, Wong NCW. Relationship between transcription factors and S14 gene expression in response to thyroid hormone and age. Proc Soc Exp Biol Med. 1994;207:97–101.
Maciel LM, Polikar R, Rohrer D, Popovich BK, Dillmann WH. Age-induced decreases in the messenger RNA coding for the sarcoplasmic reticulum Ca2(+)-ATPase of the rat heart. Circ Res. 1990;67:230–4.
Effron MB, Bhatnager GM, Spurgeon HA, Ruano-Arroyo G, Lakatta EG. Changes in myosin isoenzymes, ATPase activity and contraction duration in rat cardiac muscle with aging can be modulated by thyroxine. Circ Res. 1987;60:238–45.
O’Neil L, Holbrook N, Lakatta EG. Progressive changes from young adult age to senescence in mRNA for rat cardiac myosin heavy chain. Cardioscience. 1992;2:1–5.
Mooradian AD, Chehade J, Kim J. Age-related changes in thyroid hormone effects on glucose transporter isoforms of rat heart. Life Sci. 1999;65:981–9.
Mooradian AD, Scarpace PJ. The response of isoproterenol-stimulated adenylate cyclase activity after administration of l-triiodothyronine is reduced in aged rats. Horm Metab Res. 1989;21:638–9.
Scarpace PJ, Abrass IB. Thyroid hormone regulation of beta-adrenergic receptor number in aging rats. Endocrinology. 1981;108:1276–8.
Gresik EW, Wenk-Salamone K, Onetti-Muda A, Gubits RM, Shaw PA. Effect of advanced age on the induction by androgen or thyroid hormone of epidermal growth factor and epidermal growth factor mRNA in the submandibular glands of C57BL/6 male mice. Mech Ageing Dev. 1986;34:175–89.
Gresik EW, Maruyama S. Inductive effects of triiodothyronine or dihydrotestosterone on EGF in the submandibular glands of young, middle-aged, and old C57BL/6NNia female mice. J Gerontol. 1987;42:491–6.
Haas MJ, Mreyoud A, Fishman M, Mooradian AD. Microarray analysis of thyroid hormone-induced changes in mRNA expression in the adult rat brain. Neurosci Lett. 2004;365:14–8.
Mooradian AD, Scarpace PJ. β-Adrenergic receptor activity of cerebral microvessels is reduced in aged rats. Neurochem Res. 1991;16:447–51.
Mooradian AD, Scarpace PJ. 3,5,3′-l-triiodothyronine regulation of B-adrenergic receptor density and adenylyl cyclase activity in synaptosomal membranes of aged rats. Neurosci Lett. 1993;161:101–4.
Mooradian AD, Girgis WE, Shah GN. Thyroid hormone-induced GLUT-1 expression in rat cerebral tissue: effect of age. Brain Res. 1997;747:144–6.
Shah GN, Li J, Mooradian AD. Novel translational repressor (NAT-1) expression is modified by thyroid state and age in brain and liver. Eur J Endocrinol. 1999;139:649–53.
Mooradian AD, Li J, Shah GN. Age-related changes in thyroid hormone responsiveness protein (THRP) expression in cerebral tissue of rats. Brain Res. 1998;793:302–4.
Mooradian AD, Habib MP, Dickerson F, Yetskievych T. The effect of age on l-3,5,3′, triiodothyronine induced ethane exhalation. J Appl Physiol. 1994;77:160–4.
Mooradian AD. Age-related differences in body weight loss in response to altered thyroidal status. Exp Gerontol. 1990;25:29–35.
Mooradian AD. The hepatic transcellular transport of 3,5,3′-triiodothyronine is reduced in aged rats. Biochim Biophys Acta. 1990;1054:1–7.
Mooradian AD. Blood–brain transport of triiodothyronine is reduced in aged rats. Mech Ageing Dev. 1990;52:141–7.
Kvetny J. Nuclear thyroxine and triiodothronine binding in mononuclear cells in dependence of age. Horm Metab Res. 1985;17:35–8.
Jang M, DiStefano JJ 3rd. Some quantitative changes in iodothyronine distribution and metabolism in mild obesity and aging. Endocrinology. 1985;116:457–68.
Visser WE, Bombardieri CR, Zevenbergen C, et al. Tissue-specific suppression of thyroid hormone signaling in various mouse models of aging. PLoS One. 2016;11(3):e0149941.
Onigata K, Szinnai G. Resistance to thyroid hormone. Endocr Dev. 2014;26:118–29.
Ochs N, Auer R, Bauer DC, et al. Meta-analysis: subclinical thyroid dysfunction and the risk for coronary heart disease and mortality. Ann Intern Med. 2008;148:832–45.
Forti P, Olivelli V, Rietti E, Maltoni B, Pirazzoli G, Gatti R, et al. Serum thyroid-stimulating hormone as a predictor of cognitive impairment in an elderly cohort. Gerontology. 2012;58:41–9.
Winkler A, Weimar C, Jöckel KH, Erbel R, Dragano N, Broecker-Preuss M, et al. Thyroid-stimulating hormone and mild cognitive impairment: results of the Heinz Nixdorf recall study. J Alzheimers Dis. 2016;49:797–807.
Chaker L, Baumgartner C, den Elzen WP, et al. Subclinical hypothyroidism and the risk of stroke events and fatal stroke: an individual participant data analysis. J Clin Endocrinol Metab. 2015;100:2181–91.
Razvi S, Shakoor A, Vanderpump M, et al. The influence of age on the relationship between subclinical hypothyroidism and ischemic heart disease: a metaanalysis. J Clin Endocrinol Metab. 2008;93:2998–3007.
Pasqualetti G, Pagano G, Rengo G, Ferrara N, Monzani F. Subclinical hypothyroidism and cognitive impairment: systematic review and meta-analysis. J Clin Endocrinol Metab. 2015;100:4240–8.
Ojala AK, Schalin-Jäntti C, Pitkälä KH, Tilvis RS, Strandberg TE. Serum thyroid-stimulating hormone and cognition in older people. Age Ageing. 2016;45:155–7.
Gussekloo J, van Exel E, de Craen AJ, et al. Thyroid status, disability and cognitive function, and survival in old age. JAMA. 2004;292:2591–9.
Cappola AR, Fried LP, Arnold AM, et al. Thyroid status, cardiovascular risk, and mortality in older adults. JAMA. 2006;295:1033–41.
Chueire VB, Romaldini JH, Ward LS. Subclinical hypothyroidism increases the risk for depression in the elderly. Arch Gerontol Geriatr. 2007;44:21–8.
Mariotti S. Thyroid function and aging: do serum 3,5,3′-triiodothyronine and thyroid-stimulating hormone concentrations give the Janus response? J Clin Endocrinol Metab. 2005;90:6735–7.
Mobbs CV, Bray GA, Atkinson RL, et al. Neuroendocrine and pharmacological manipulations to assess how caloric restriction increases life span. J Gerontol. 2001;56A:34–44.
Blanc S, Schoeller D, Kemnitz J, et al. Energy expenditure of rhesus monkeys subjected to 11 years of dietary restriction. J Clin Endocrinol Metab. 2003;88:16–23.
Ooka H, Shinkai T. Effects of chronic hyperthyroidism on the lifespan of the rat. Mech Ageing Dev. 1986;33:275–82.
Speakman JR, Selman C, McLaren JS, et al. Living fast, dying when? The link between aging and energetics. J Nutr. 2002;132(Suppl. 2):S1538–97.
Rieben C, Segna D, da Costa BR, et al. Subclinical thyroid dysfunction and the risk of cognitive decline: a meta-analysis of prospective cohort studies. J Clin Endocrinol Metab. 2016;101:4945–54.
Aubert CE, Bauer DC, da Costa BR, et al. The association between subclinical thyroid dysfunction and dementia: the Health, Aging and Body Composition (Health ABC) Study. Clin Endocrinol (Oxf). 2017;87:617–26.
Gan EH, Pearce SH. Clinical review: the thyroid in mind: cognitive function and low thyrotropin in older people. J Clin Endocrinol Metab. 2012;97:3438–49.
Annerbo S, Lökk J. A clinical review of the association of thyroid stimulating hormone and cognitive impairment. ISRN Endocrinol. 2013;2013:856017.
Moon JH, Park YJ, Kim TH, et al. Lower-but-normal serum TSH level is associated with the development or progression of cognitive impairment in elderly: Korean Longitudinal Study on Health and Aging (KLoSHA). J Clin Endocrinol Metab. 2014;99:424–32.
Delitala AP. Subclinical hyperthyroidism and the cardiovascular disease. Horm Metab Res. 2017;49:723–31.
Williams GR, Bassett JHD. Thyroid diseases and bone health. J Endocrinol Invest. 2018;41:99–109.
Ostan R, Monti D, Mari D, et al. Heterogeneity of thyroid function and impact of peripheral thyroxine deiodination in centenarians and semi-supercentenarians: association with functional status and mortality. J Gerontol A Biol Sci Med Sci. 2019;16(74):802–10.
Stott DJ, Rodondi N, Kearney PM, et al. Thyroid hormone therapy for older adults with subclinical hypothyroidism. N Engl J Med. 2017;376:2534–44.
Franceschi C, Ostan R, Mariotti S, Monti D, Vitale G. The aging thyroid: a reappraisal within the geroscience integrated perspective. Endocr Rev. 2019;40:1250–70.
Piehl S, Hoefig CS, Scanlan TS, Köhrle J. Thyronamines: past, present, and future. Endocr Rev. 2011;32:64–80.
Groeneweg S, Peeters RP, Visser TJ, Visser WE. Therapeutic applications of thyroid hormone analogues in resistance to thyroid hormone (RTH) syndromes. Mol Cell Endocrinol. 2017;458:82–90.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for the preparation of this article.
Conflict of interest
Arshag D. Mooradian has no conflicts of interest that are directly relevant to the content of this article.
Rights and permissions
About this article
Cite this article
Mooradian, A.D. Age-Related Resistance to Thyroid Hormone Action. Drugs Aging 36, 1007–1014 (2019). https://doi.org/10.1007/s40266-019-00711-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-019-00711-7