Abstract
Exposure to drugs during pregnancy has the potential to harm offspring. Teratogenic effects are the most feared adverse outcomes in newborns; however, a wide spectrum of less known, usually reversible and often acute, neonatal adverse events can also occur due to drug intake by mothers during pregnancy, particularly in close proximity to delivery. This narrative review is aimed at the description of drugs and drug classes for which licit maternal use in the predelivery period has been associated with neonatal non-teratogenic disorders. For each drug class, epidemiology, clinical features, biological mechanism and management of these adverse reactions have been discussed in detail. Although these adverse reactions have been described mainly for substances used illicitly for recreational purposes, several prescription drugs have also been involved; these include mainly psychotropic medications such as opioids, antidepressants, antiepileptics and antipsychotics. These effects can be partly explained by withdrawal syndromes (defined also as ‘neonatal abstinence syndrome’) caused by the delivery-related discontinuation of the drug disposition from the mother to the fetus, with symptoms that may include feeding disorders, tremors, irritability, hypotonia/hypertonia, vomiting and persistent crying, occurring a few hours to 1 month after delivery. Otherwise, neonatal neurological and behavioral effects can also be caused by a residual pharmacological effect due to an accumulation of the drug in the blood and tissues of the newborn, with various symptoms related to the toxic effects of the specific drug class, usually developing a few hours after birth. With few exceptions, validated protocols for the assessment and management of withdrawal or residual pharmacological effects of these drugs in neonates are often lacking or incomplete. Spontaneous reporting of these adverse reactions seems limited, although it might represent a useful tool for improving our knowledge about drug-induced neonatal syndromes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Newborns exposed to psychotropic drugs during pregnancy may experience neonatal syndromes, including neonatal withdrawal symptoms and/or residual pharmacological effects. |
Psychotropic drugs most often reported with neonatal adaptation issues are opioids, antidepressants, antiepileptics (including barbiturates and benzodiazepines), and antipsychotics. |
1 Introduction
It is well known that exposure to pharmacologically-active substances during pregnancy has the potential to harm offspring. Teratogenic effects are definitely the most feared adverse outcomes in newborns [1]; however, a wide spectrum of less known, usually reversible, and often acute adverse events can also occur in newborns due to drug intake by mothers during pregnancy, particularly in close proximity to delivery. These effects have frequently been ascribed to withdrawal effects [2]. Indeed, the delivery determines a discontinuation of drug intake that the baby was receiving from the mother. In the traditional pharmacovigilance classification of adverse drug reactions, these events belong to the ‘E’ (end of use) category [3]. Alternatively, neonatal adverse effects may result from ‘residual’ activities of the drugs, particularly those endowed with a long half-life [type ‘A’ (augmented) adverse drug reactions] [3]. In these settings, the immaturity of metabolic functions in newborns is likely to play an important role [4]. Early identification of the origin of symptoms is of primary importance for the appropriate management of newborns. Indeed, in case of withdrawal, the newborn may benefit from a reintroduction of the discontinued drug or its safer alternative within the same drug class. By contrast, in case of residual toxicity, being exposed further to the withdrawn drug may have detrimental effects on the newborn [5].
Withdrawal symptoms have been extensively investigated for many years in drug-addicted pregnant women exposed to substance abuse. Nevertheless, some prescription drugs have also been reported to be associated with such events in neonates. Their clinical presentation is variable and usually includes several signs and symptoms, ranging from behavioral abnormalities to neurological impairments. For this reason, these effects are usually defined as a syndrome, which is sometimes designated as ‘neonatal abstinence syndrome’ [6], ‘neonatal withdrawal syndrome’ [7], ‘neonatal adaptation syndrome’ [8], or even ‘neonatal behavioral syndrome’ [9], depending on the putative mechanism. In the present review, we used the definition ‘neonatal abstinence syndrome’ (NAS), which is the most frequently employed term used to describe withdrawal symptoms, making a distinction from other kind of events, which can be more likely explained by residual pharmacological effects of the drug on the fetus or newborn.
Overall, based on the above background, this narrative review is aimed at the description of drugs and drug classes for which licit maternal use in the predelivery period has been associated with neonatal non-teratogenic disorders. These disturbances have been reviewed and described in detail on the basis of currently available evidence.
2 Methods
English-language literature indexed in MEDLINE was explored, without time limits, to 31 December 2015, using the terms ‘neonatal abstinence syndrome’, ‘neonatal withdrawal syndrome’, ‘neonatal behavioral syndrome’, and ‘neonatal adaptation syndrome’. Since there is no standard clinical definition for these syndromes, case reports dealing with neonatal behavioral and neurological alterations after exposure to any drug were used to generate clusters of symptoms suggestive of the syndromes. These clusters were then used as search terms to identify studies reporting the frequency of such neonatal outcomes [including single behavioral signs, poor neonatal adaptation, and admission to the neonatal intensive care unit (NICU)]. The reference lists of identified articles were examined carefully for additional pertinent publications.
For inclusion in the present review, meta-analyses, clinical trials, observational studies, case series and single case reports had to evaluate neonatal events consistent with a drug withdrawal or pharmacological residual effect consequent to prebirth exposure to any prescription drug. Studies addressing the neonatal effects of drugs used for recreational purposes during pregnancy, and articles focusing only on teratogenic effects (including abnormalities of physiological development occurring in utero, such as persistent pulmonary hypertension, alterations in fetal development, low birth weight, fetal hydantoin syndrome), congenital malformations, miscarriage, stillbirth, and abortion were excluded [10–12]. Abstracts presented at national and international meetings were also excluded.
3 Results
Drugs associated with neonatal non-teratogenic disorders belong to several psychotropic drug groups, and include opioids, antidepressants, antiepileptic drugs (AEDs) and antipsychotics. Notably, the lipophilic chemical nature of these drugs generally allows their placental disposition and/or excretion into breast milk, in accordance with the pharmacokinetics of each drug, thus explaining the variability of perinatal exposure and neonatal effects among drugs. Table 1 summarizes the main clinical patterns of these neonatal syndromes. Each drug class is discussed in detail in the following sections.
3.1 Opioids
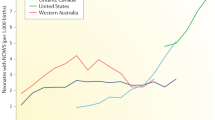
Epidemiology Opioids represent the most investigated drug class for their involvement in the occurrence of neonatal neurobehavioral symptoms, which is largely due to the illicit use of these drugs for recreational purposes since time immemorial. Opioid-associated NAS has been documented in Western countries since 1875, with the first case published in the US in 1892 [6]. In the US, it has been estimated that from 2000 to 2009, antepartum opioid use increased from 1.19 to 5.63 per 1000 live births [13]. Over the same period, the incidence of NAS increased from 7 to 27 cases per 1000 admissions to the NICU [14], and related hospitalization costs per infant with NAS increased from US$39,400 to US$53,400 [13]. Although most of the available evidence points towards the use of prescription opioids, and not illicit opioids, behind the increased NAS incidence, a clear relationship cannot be established [15–17]. In Canada, from 1992 to 2011, the incidence of opioid-related NAS increased 15-fold (from 0.28 to 4.29 per 1000 live births), and from 2006 to 2011 NAS could be ascribed to prescription opioids in 67 % of cases [15]. In the US, from 2008 to 2012, approximately one-third of fertile women were prescribed an opioid, and in Norway, 6 % of pregnant women filled at least one opioid prescription between 2004 and 2006 [16]. A study performed in Tennessee estimated that 63 % of NAS cases occurred in women receiving prescription opioids [17]. A large observational study (n = 290,605) performed in the Medicaid database indicated that the absolute risk of NAS due to prescription opioids, in the absence of other risk factors (history of opioid misuse or dependence, alcohol or other drug misuse, exposure to other psychotropic medications late in pregnancy, and smoking), was low (5.9 per 1000 deliveries) [18]; however, the risk increased with long-term use compared with short-term risk [relative risk (RR) 2.05, 95 % confidence interval (CI) 1.81–2.33], as well as for late pregnancy compared with early use (RR 1.24, 95 % CI 1.12–1.38), independently of additional risk factors [18]. Overall, 50–80 % of opioid-exposed infants required pharmacologic treatment for the management of NAS [6, 19, 20]. Preterm infants have been reported as being at lower risk of opioid withdrawal, with less severe and/or prolonged courses [21, 22].
Besides analgesic use, opioids are mainly prescribed for maintenance purposes in addicted women during pregnancy. The mainstay of this treatment is represented by tapering of methadone or buprenorphine [23]. Evidence in favor of buprenorphine use over methadone is growing due to more favorable neonatal brain growth patterns with buprenorphine [23]. Although evidence supporting the teratogenic effects of opioids is scarce [24–27], long-term use during pregnancy has been associated with brain development impairments [28, 29]. Furthermore, although the occurrence of NAS has been reported for both methadone and buprenorphine [30–36], it has been observed that, prenatally, buprenorphine-exposed neonates required significantly less morphine, shorter treatment duration, and shorter hospitalization compared with prenatally methadone-exposed neonates [19, 37]. Higher neurobehavioral score and less severe NAS have also been reported in newborns after in utero exposure to buprenorphine, compared with those exposed to methadone [38]. The relationship between methadone or buprenorphine dose and NAS severity is currently controversial, with some studies indicating an association and some not [39–45]. Other prescription opioids that have been associated with withdrawal syndrome include morphine [46], codeine [47–51], tramadol [52–56], propoxyphene [57–60], fentanyl [46, 61], and pentazocine [62–64].
Clinical features Besides individual genetic factors [65], the onset of withdrawal signs and the peak of symptom severity likely depend on opioid pharmacokinetics. For instance, prenatal exposure to morphine displays a shorter time to onset of newborn withdrawal (average 36 h), compared with methadone (average 60 h) [66]. NAS associated with buprenorphine generally starts after approximately 12–48 h and peaks at approximately 72–96 h [67]. For tramadol, the onset was reported within 35–48 h, with a peak in 3–7 days [52–54] and, for codeine, initial symptoms appear even after 2 h, with a peak within 24–48 h [47, 50]. Fentanyl-associated NAS was reported to develop within 24 h, with a peak at 72 h [46, 61], even when the drug was administered by transdermal devices [61].
Opioid-related NAS can develop with a range of different symptoms that involve critical regulatory functions of postnatal adaptation, ranging from neurologic hyperexcitability (insomnia, irritability, hypertonia, hyperreflexia, tremors, and seizures) to gastrointestinal symptoms (vomiting, diarrhea, feeding disturbances), and sympathetic/parasympathetic dysregulation (sweating, hyperthermia, tachypnea, and congestion) [68, 69]. Several scales and scores have been developed to assess NAS severity in opioid-exposed infants [70]. These are very heterogeneous and include, amongst others, the Neonatal Abstinence Syndrome Score, also known as the Finnegan score, which is the most used in the US [71] in its modified versions (see Table 2 for an example) [72]; Narcotic Withdrawal Score (Lipsitz Score) [73]; Neonatal Narcotic Withdrawal Index [74]; Neonatal Narcotic Withdrawal Inventory [75]; and the MOTHER NAS Scale (a modified version of the Finnegan scale) [19]. In newborns with NAS, these scores are estimated by caregivers every few hours. Based on their values, standard thresholds have been defined to establish the extent (e.g. dose) and duration (e.g. dose-titration scheduling for maintenance approaches) of pharmacological and non-pharmacological interventions [13].
Antenatal methadone exposure has also been reported to be associated with transient prolongation of QT interval in newborns, usually within the first 2 days of life [76]. This effect may partly explain the high rate of infant sudden death syndrome in newborns from mothers on maintenance with methadone, although the pathophysiology of this adverse outcome is likely to be multifactorial in nature [77]. In particular, this adverse effect has been ascribed to a direct toxicity after placental transfer of methadone, and not to a withdrawal syndrome [76].
Biological mechanisms The mechanism of opioid-induced NAS is complex and not fully understood. Opioids are small lipophilic molecules that can easily cross the placental barrier [20]. One of the most accepted theories suggests a pivotal role for a second messenger, cyclic adenosine monophosphate (cAMP), responsible for signal transduction in several cellular systems. The activation of opioid receptors strongly inhibits adenyl cyclase, thus preventing the synthesis of cAMP. After repeated opioid exposure, the cells attempt to compensate for the lack of cAMP by enhancing the expression of adenyl cyclase. When opioid intake is discontinued, the hyperexpressed adenyl cyclase is no longer inhibited, with consequent overproduction of cAMP. The latter leads to an excessive release of norepinephrine, which then binds to noradrenergic receptors, thus causing overactivation of the autonomic nervous system that becomes responsible for the onset of signs and symptoms associated with the withdrawal syndrome [78–81].
Management The management of opioid-induced NAS is also controversial. The most common approaches include non-pharmacological and pharmacological interventions [78, 82]. Among the non-pharmacological interventions, infant feeding methods are the most explored. In particular, the effect of feeding approach has been investigated in seven observational retrospective studies [83–89]. Although these studies are flawed by significant limitations and their results are not easily comparable [70], their findings suggest that, in infants with NAS, breastfeeding from mothers stable in methadone or buprenorphine maintenance (i.e. not using illicit opioids) is associated with an overall decrease in the need for pharmacological treatment (30 % reduction), a decrease in NAS scores, and a decreased duration of pharmacological therapy and hospitalization (3–19 days shorter) [70]. Notably, methadone excreted into maternal milk may theoretically provide an indirect maintenance treatment for babies with NAS. However, one study showed that methadone concentration in the blood of newborns breastfed by mothers on methadone maintenance is too low to explain a ‘pharmacological compensation’ of the delivery-induced drug withdrawal [90]. Thus, in this setting, the beneficial impact of breastfeeding on NAS symptoms likely results from the positive comfort associated with maternal contact [90]. Other non-pharmacologic approaches, for which lesser evidence of benefit in NAS is available, include rooming-in, bed type, infant position, and non-insertive acupuncture [70].
The pharmacological management of opioid-induced NAS may include a reintroduction of the discontinued drug (or an alternative safer opioid) or the use of symptomatic treatments. Orally administered morphine (morphine chloride, or even in the form of opium tincture, 0.3–1.0 mg/kg/day, administered every 3–4 h, titrated to effect and reduced every 24–48 h), or methadone (titrated in the range of 0.3–1.0 mg/kg/day, administered every 4–12 h and then weaned) are the most commonly used first-line medications, although there is no evidence on which drug is superior [70, 91]. Buprenorphine has also been investigated in recent studies, showing a decrease in treatment duration and reduced hospital stay compared with methadone [92] or opium solution [93]. Second lines of treatment include phenobarbital, clonidine and clonazepam [20, 78, 94, 95]. Notably, randomized clinical trials (RCTs) investigating the above pharmacological approaches are small, employed different assessment tools and protocols to escalate and wean medications, and adjusted for different covariates, and are therefore very difficult to compare. In RCTs, morphine was shown to be more beneficial than phenobarbitone (significantly shorter duration of treatment and reduced need for second-line treatment and NICU admission) [96], but less effective than opium tincture (n = 33; longer length of treatment and length of hospitalization) [97]. In another RCT, conducted on 25 infants with NAS, buprenorphine displayed a reduced length of hospital stay compared with neonatal opium solution [98]. Finally, the benefits of add-on therapies to first-line opioids, with clonidine and phenobarbital, have been investigated, showing a decrease in the duration of first-line therapy, with phenobarbital showing a shorter duration of treatment when directly compared with clonidine [95, 99, 100].
3.2 Antidepressants
Epidemiology It has been estimated that 13.5 % of pregnant women present depressive disorders [101]. Depression may have a negative impact on pregnancy outcomes, including low birth weight and prematurity, irritation, agitation, lethargy, reduced attention, and relationship issues between mother and child, with consequent learning and behavioral problems during childhood [102, 103]; therefore, treatment with antidepressants is often recommended [101]. In Europe, 1–3 % of pregnant women take antidepressants [mainly selective serotonin reuptake inhibitors (SSRIs; including fluoxetine, paroxetine, sertraline, citalopram, escitalopram and fluvoxamine), and serotonin norepinephrine reuptake inhibitors (SNRIs; including venlafaxine and duloxetine) because of their effectiveness and safety], while in the US the rate is approximately 4–13 %. Overall, 25 % of women treated with antidepressants continue their treatment during pregnancy, and 0.5 % of women start treatment during pregnancy [104].
In 2004, the US FDA issued a class labeling change for SSRI and SNRI antidepressants, introducing a warning about the association of third-trimester exposure to antidepressants and signs and symptoms consistent with NAS [103]. Approximately 20–77 % of children exposed to SSRIs in utero have been estimated to develop symptoms of NAS [102], with paroxetine and fluoxetine having the higher incidence compared with other SSRIs [105–108]. The incidence of NAS in newborns exposed to tricyclic antidepressants (TCAs) in utero is approximately 20–50 % [102, 109]. NAS symptoms associated with SSRIs, SNRIs and TCAs are similar and include a variety of mild to moderate behavioral, autonomic and neurological signs, such as irritability, persistent crying, chills, tremors, restlessness, feeding difficulties, jaundice, vomiting, hypotonia, hypertonia, and sleep disorders [102, 110–124]. However, NAS may also rarely occur with severe symptoms requiring NICU management, such as respiratory distress syndrome and seizures [112–114, 123, 125–131]. Motor, respiratory, gastrointestinal, and metabolic dysfunctions, usually mild to moderate and self-limiting, occur in the majority of cases shortly after birth, within the first 24–72 h, and generally disappear within a few weeks. Residual pharmacological effects of antidepressants occur immediately after birth, and symptoms may depend on the specific antidepressant. Following exposure to TCAs, anticholinergic symptoms, such as urinary retention and constipation, can be observed [102]. For the SSRIs, symptoms are expected to be similar to those of a serotonergic syndrome in adults [102].
Several studies have attempted to estimate the NAS risk in babies exposed to antidepressants in utero. Late SSRI exposure is estimated to carry an overall risk ratio of 3.0 (95 % CI 2.0–4.4) for NAS compared with non-exposure or earlier exposure to SSRIs [101]. Grigoriadis et al. [132] found a significant increase in the risk of NAS as a result of exposure to antidepressants during pregnancy [odds ratio (OR) 5.7, 95 % CI 3.25–7.90], and signs such as respiratory distress (OR 2.20, 95 % CI 1.81–2.66) and tremors (OR 7.89, 95 % CI 3.33–18.73) [132]. In a study conducted on 997 infants whose mothers had used antidepressants during the latter part of their pregnancy, excess neonatal problems were observed more frequently after the use of TCAs than SSRIs. In particular, an increased risk was detected for respiratory distress (TCAs: OR 2.20, 95 % CI 1.44–3.35; SSRIs: OR 1.97, 95 % CI 1.38–2.83), neonatal hypoglycemia (TCAs: OR 2.07, 95 % CI 1.36–3.13; SSRIs: OR 1.35, 95 % CI 0.90–2.03), and neonatal seizures (TCAs: OR 6.8, 95 % CI 2.2–16.0; SSRIs: OR 3.6, 95 % CI 1.0–9.3), but not for neonatal jaundice (TCAs: OR 1.37, 95 % CI 0.88–2.12; SSRIs: OR 0.96, 95 % CI 0.63–1.46), after exposure to TCAs compared with SSRIs [129]. As far as SNRIs are concerned, late-pregnancy exposure to duloxetine can be associated with a low risk of NAS but its extent remains unclear [133]. Notably, the risk of NAS after exposure to venlafaxine seems to be comparable to the risk after exposure to SSRIs [102].
Clinical features The diagnosis of antidepressant-associated NAS is complicated by the lack of standard diagnostic criteria, the difficulty of discriminating between NAS and residual pharmacological effects, overlapping between the two clinical pictures, and the metabolic immaturity of newborns [102, 133–135]. For SSRIs/SNRIs, the main differences between NAS and residual pharmacological effects (usually consistent with a picture of serotonergic overstimulation) are likely in the time to event onset and the serum concentrations of the drug or serotonin metabolites [i.e. 5-hydroxyindoleacetic acid (5-HIAA)] in the umbilical cord. Indeed, in the case of residual serotonin toxicity, symptoms occur soon after delivery, and high concentrations of antidepressants can be detected in the umbilical cord serum [102]. By contrast, NAS symptoms occur within 24–72 h from labor [122, 136, 137], and 5-HIAA levels are low and the concentration inversely related with symptom severity [138]. The time to onset and duration of withdrawal symptoms or serotonergic overstimulation in exposed infants depend on the pharmacokinetics of the specific antidepressant [110]. The half-life of the antidepressant might influence the risk of NAS and serotonin toxicity, while the drug dose does not seem to be related to the occurrence or severity of NAS [102].
Commonly used scores for evaluating the severity of NAS (i.e. the Finnegan score) [72] have never been validated for antidepressants. In most cases, symptoms are non-specific and the diagnosis is carried out by excluding infectious problems, neurological diseases, intoxications, and metabolic dysfunctions (hypoglycemia, hypocalcemia, etc.) [102, 135, 139]. Maternal depression is an important confounding factor [134]. Oberlander et al. [140] showed that only neonatal respiratory distress was a symptom related to antidepressant withdrawal, while other neonatal symptoms, such as feeding problems, jaundice, and even convulsions, were found in both exposed and non-exposed infants from depressed mothers [140]. Moreover, pregnant women taking antidepressants are often exposed to other treatments with psychotropic drugs [113], such as benzodiazepines [131], which might contribute to the occurrence of neonatal adverse effects [107]. Children undergoing an NAS typically display normal cognitive abilities, but they may have a higher risk of developing social and behavioral abnormalities than children without NAS. Follow-up of these infants has been recommended [141].
Biological mechanisms Antidepressants are known to cross the placental barrier [142–144]. The mechanism of NAS associated with SSRIs is not fully understood and likely reflects a condition of withdrawal similar to that observed in adults [145]. Some authors have speculated about a temporary deficiency of synaptic serotonin occurring after abrupt withdrawal of an SSRI [146]. Indeed, during treatment, serotonin reuptake is blocked and therefore synaptic serotonin levels remain elevated. This circumstance could induce a downregulation of post-synaptic serotonin receptors (desensitization), which could remain in their relatively hypoactive condition for days to weeks [146]. At delivery, the blockade of serotonin reuptake is abruptly interrupted and serotonin synaptic levels are expected to rapidly decrease. This ‘serotonin shortage’, in concomitance with receptor desensitization, is thought to translate into a decrease of serotonin transmission, which can have significant consequences, not only on the serotonin system but also on the dopaminergic, noradrenergic and cholinergic neurotransmissions, owing to the modulating control exerted by serotonin on these pathways in the central nervous system (CNS). The alterations resulting from these neurotransmitter interplays may explain the development of NAS symptoms [105, 134, 146, 147]. TCA withdrawal has been brought back to a cholinergic and adrenergic theory [109]. The cholinergic theory is based on the fact that TCAs bind both peripheral and central muscarinic receptors, with blockade of cholinergic activity, and consequent upregulation of muscarinic receptors (which is an explanation for tolerance to cholinergic adverse effects). When TCAs are discontinued, the upregulation of muscarinic receptors promotes a condition of ‘cholinergic overdrive’ in some patients [134]. Notably, this mechanism has also been described for paroxetine, and this circumstance may provide an explanation for the higher frequency of NAS associated with paroxetine compared with other SSRIs [101].
The adrenergic theory holds that treatment with TCAs causes inhibition of norepinephrine reuptake, with an increase in the synaptic concentration of this mediator. Initially, this condition leads to a decrease in norepinephrine turnover and to a lowering of norepinephrine release mediated by the overactivation of presynaptic α2-adrenoceptors. However, with prolonged drug intake, a downregulation of presynaptic α2-adrenoceptors occurs, leading to a further increase in the synaptic accumulation of norepinephrine. Following abrupt discontinuation of TCA therapy, the synaptic levels of norepinephrine would be expected to decrease rapidly; however, owing to the desensitization of presynaptic α2-adrenoceptors, a significant facilitation of norepinephrine release is maintained for a certain period, with a subsequent temporary persistence of the activity of noradrenergic neurotransmission [134].
Management Most NAS cases are mild in nature, being characterized by short duration and self-limiting symptoms, and therefore they do not generally require treatment [148]. Medical management consists mainly of close monitoring of the newborn exposed to antidepressants in utero, at least in the first hours after delivery [149]. Should the syndrome develop fully, supportive care must be provided [101, 102, 106, 135, 150, 151]. Evolution of the clinical picture can be monitored using the Finnegan score; a score of 8 on a survey of more than three consecutive measurements is considered a serious NAS requiring medication or transfer to the NICU [102, 130, 135, 139]. Phenobarbital has shown a good safety profile in newborns and can be used to control irritability, stiffness, and seizures [102, 112, 135, 139, 151, 152]. Breastfeeding has been shown to reduce the severity and duration of NAS [102, 149]. Available evidence does not allow to exclude that, in mothers receiving SSRIs during lactation, this beneficial effect can be partly explained by the excretion of low amounts of these antidepressants into the maternal milk. In this way, drug exposure would not be abruptly interrupted by delivery. Therefore, some authors recommend breastfeeding as a preventive strategy for SSRI-induced NAS [102, 149, 153–155]. In this case, the differential diagnosis between SSRI/SNRI serotonin withdrawal and toxicity is a critical issue for clinical management [5, 136]. Indeed, in case of withdrawal, the newborn may benefit from being treated with an SSRI through lactation. In contrast, in case of serotonin toxicity, being exposed to an SSRI may have detrimental effects [5].
3.3 Antiepileptic Drugs
Epidemiology AEDs include a variety of drugs that are highly heterogeneous, both for mechanisms of action and indications. These drugs have been associated with the development of neonatal abnormalities related to drug exposure in utero, described as neonatal withdrawal symptoms or residual toxicities. In this section, neonatal syndromes related to maternal exposure to AEDs have been reviewed, with two subsections focusing on barbiturates and benzodiazepines since these two drug classes have been investigated both with other AEDs and separately as an individual drug class.
Epilepsy has been estimated to affect 0.3–1 % of pregnant women, and its treatment with AEDs should be aimed at carefully balancing the risk of seizures for both the mother and the baby [156] with the risk of teratogenic and other adverse effects in the newborn [157–162]. In a recent study performed on data from the Medication Exposure in Pregnancy Risk Evaluation Program (MEPREP) database, it was estimated that from 2001 to 2007 the use of AEDs during pregnancy increased, mainly owing to a fivefold increase in the use of newer AEDs. Older AEDs (i.e. benzodiazepines, valproic acid, carbamazepine and phenytoin) were the most commonly used drugs, with benzodiazepines being involved in over half of the exposed pregnancies. Among the newer AEDs, the most frequently used drugs were gabapentin, lamotrigine, topiramate, oxcarbazepine and levetiracetam. The most prevalent indications were psychiatric disorders, pain disorders and epilepsy [163]. Second-generation AEDs (e.g. lamotrigine) are progressively replacing first-generation AEDs (e.g. valproic acid) in pregnancy, both in monotherapy and polytherapy [164–166]. The trend towards an increased use of the newest AEDs in pregnant women is in line with the clinician concerns about the teratogenic risk associated with older compounds, such as valproic acid, phenytoin, phenobarbital, primidone, and carbamazepine. Newer AEDs appear to be safer in pregnancy compared with older AEDs, even though limited data makes it difficult to issue solid recommendations [163, 167, 168].
NAS has been described in newborns exposed prenatally to AEDs. Several small observational studies have attempted an estimation of the frequency of withdrawal syndrome in babies born from mothers exposed to AEDs during pregnancy. A frequent limitation of investigations attempting a comparison is the selection of non-epileptic mothers as the reference group, which does not allow to exclude that epilepsy may have a role in the occurrence and severity of symptoms. A prospective study (n = 123) estimated that the frequency of withdrawal-related jitteriness in babies with in utero exposure to phenytoin alone, valproic acid alone, or a combination of other AEDs (valproic acid, carbamazepine, phenytoin, phenobarbital, sulthiame, and primidone) was 18 versus 0 % in non-epileptic women [169]. Another study [170] evaluated the effects of in utero exposure to AEDs using apathy and hyperexcitability scores, and showed higher apathy scores for phenobarbital and phenytoin, and higher hyperexcitability scores for valproic acid, compared with a non-epileptic reference group. Dean et al. observed that 50 (20 %) of 255 newborns exposed to AEDs in utero experienced a withdrawal syndrome, with an RR of 7.45 (95 % CI 1.06–52.37), when compared with one case (3 %) over 38 non-exposed epileptic pregnancies [159]. Phenobarbital monotherapy was less likely to be associated with neonatal withdrawal symptoms (13 %), while polytherapy was most likely to be associated (30 %; p = 0.001). Neonatal withdrawal was significantly more frequent in newborns exposed to valproic acid monotherapy (24 %; p = 0.006) and phenytoin monotherapy (21 %; p = 0.018) than in the non-exposed group (3 %) [159]. A small study described 10 cases of NAS among 22 newborns exposed in utero to valproic acid as monotherapy or combined with carbamazepine [171]. A case-control study described four cases of NAS among 37 newborns exposed to valproic acid monotherapy or in combination with primidone, carbamazepine or lamotrigine compared with no cases in control groups (untreated epileptic women or healthy women) [157].
Clinical features Symptoms of AED-related NAS are similar to those of opioid withdrawal. They usually occur during the first few hours after birth and up to 1 week after delivery, and may persist for weeks and months [172–175]. Symptoms may include irritability, jitteriness, abnormal tone, hypotonia, seizures, feeding disorders, hypoglycemia, apnoeic episodes and vomiting [12, 156, 159, 170, 176]. Hypotonia and feeding problems may depend on the sedative effect of AEDs [173]. Notably, withdrawal symptoms have been described as part of the ‘fetal anticonvulsant syndrome’, characterized also by malformations, developmental disorders and facial dysmorphism [12]. Valproic acid in monotherapy or polytherapy (in combination with phenytoin, carbamazepine, ethosuximide or primidone), oxcarbazepine and lamotrigine, used during pregnancy for the treatment of epilepsy, have been described in case reports as the suspected causative drugs for NAS [156, 173, 177, 178]. Withdrawal symptoms were also reported in infants born to women treated with gabapentin or baclofen during pregnancy for the management of neuropathic pain and paraplegia, respectively [174, 175, 179]. In late-preterm infants, withdrawal symptoms developed 1–3 days after birth and were preceded by bradycardia, difficulty in breathing, cyanosis, intercostal retractions, apnea, and hypotonia at birth [156, 177, 179].
Biological mechanisms Most AEDs cross the placenta by diffusion in substantial amounts [170]. For valproic acid and gabapentin, active transportation has been also described [172, 180–183]. Notably, for many newer generation AEDs, gestational pharmacokinetic data are still limited [180]. The occurrence of withdrawal symptoms in newborns of epileptic mothers has been correlated positively with the mean dose of valproic acid administered in the third trimester (daily dose ≥2 g) and the concentration of the free fraction of valproic acid in maternal plasma at delivery [171, 173]. Valproic acid concentrations at birth have been correlated with hyperexcitability in the newborn, while apathy was associated with high serum concentrations of unbound phenobarbital [170]. Jitteriness was related to phenytoin concentrations in maternal blood and cord blood [169]. Of note, these data are not conclusive since other studies failed to show any correlation between the drug dose or cord blood serum concentrations and the occurrence of withdrawal syndrome [159, 169]. Furthermore, deficient hepatic and renal elimination capacities in the neonate can result in a longer half-life of AEDs when compared with adults, such as in the case of valproic acid. By contrast, in utero exposures to phenytoin, carbamazepine and primidone have been shown to induce the fetal hepatic enzyme systems, resulting in drug elimination patterns similar to adults [172]. The presentation of signs and symptoms of NAS may sometimes be delayed, consistently with the elimination time of drug metabolites in the neonate. Alternatively, the delay can be explained by an increase in AED concentrations after delivery, likely due to their slow disposition from CNS and lipid stores [175, 177]. Indeed, the fetus can be considered as a ‘deep compartment’ filled up by these compounds during long-term therapy throughout pregnancy [172]. Accordingly, after delivery, AEDs (phenobarbital, primidone, valproic acid and benzodiazepines) have been found to persist in neonatal plasma for several days. This mechanism can explain some earlier neonatal events (direct toxicity), such as sedation, hypotonia, weak sucking, feeding problems and, later, neonatal withdrawal syndrome [173, 176, 184]. Signs of drug withdrawal in neonates can be monitored using the Finnegan scoring system [174, 177, 179], although other scoring systems have been used occasionally [170].
The mechanism underlying AED-induced NAS has not been fully understood yet, and is likely to differ across the various drugs. In adults, the γ-aminobutyric acid (GABA) system is known to play a pivotal role in the pathogenesis of withdrawal symptoms associated with benzodiazepines, barbiturates, gabapentin and baclofen [185, 186]. Prolonged use of baclofen also induces the inhibition of monoamine neurotransmitter systems, leading to upregulation of the dopamine and noradrenergic receptors. When baclofen is suddenly withdrawn, a disinhibition of the previously suppressed monoamine pathways occurs, with a consequent release of norepinephrine and dopamine onto upregulated receptors, leading to autonomic arousal (i.e. tachycardia, hypertension, agitation, restlessness), as well as delusions, hallucinations and delirium [186]. The administration of valproic acid in rats was related to increased levels of striatal met-enkephalin that might participate in the occurrence of valproic acid-induced abstinence behavior [187]. It has been suggested that withdrawal symptoms observed with carbamazepine are consistent with those of TCAs, likely due to chemical similarities [188]. Hypoglycemia is also one of the symptoms associated with AED withdrawal syndrome, a condition that is often associated with neonatal feeding issues. However, hypoglycemia may depend on residual toxicity of in utero exposure to valproic acid since this drug has been shown to decrease gluconeogenesis and impair glycogenolysis in newborns [156, 171].
Management A standard treatment of AED-induced NAS has not been defined. Symptoms can be mild and transient or severe, to such an extent as to require transfer to the NICU [156, 173, 177, 179]. Infants developing withdrawal symptoms after abrupt discontinuation of AEDs (valproic acid in mono- and polytherapy) have been treated with phenobarbital and diazepam (in case of repeated seizures) [171, 173], or the readministration of the drug responsible for withdrawal (gabapentin, baclofen) [174, 175, 179]. Some infants required enteral feeding or breast milk supplemented with formula milk, usually because of feeding problems caused by withdrawal symptoms [171, 179]. Among the preventive strategies, discontinuing AEDs during pregnancy is not usually an option since a recurrence of seizures in pregnant women is expected [159]. Monotherapy and the lowest drug dose may limit the risk of neonatal withdrawal [173]. Tapering down the dose of AEDs (i.e. gabapentin) slowly prior to delivery over a period of weeks to months can be useful in the minimization of NAS risk [12, 179].
3.3.1 Barbiturates
Epidemiology and clinical features For decades, barbiturates have been indicated for the treatment of several clinical conditions during pregnancy that, at least initially, included anxiety, sedation, prevention of hyperbilirubinemia in the newborn, pre-eclampsia and epilepsy [189, 190]. The management of epilepsy with barbiturates during pregnancy remains a controversial issue since in utero exposure to these drugs may result in newborn behavioral abnormalities, neurological impairments and/or NAS [190, 191].
Although abstinence syndrome is well-described in adults [192], barbiturate-related NAS is less well-documented and is often described by case reports and small case series published during the 1970s, when these compounds were more frequently prescribed by physicians for the management of epilepsy in pregnant women as well as for pre-eclampsia [170, 190, 191, 193, 194]. These early cases provide limited information, mainly due to diagnostic uncertainties related to the great variability of symptoms and the pioneering approach to NAS. In a retrospective study, performed in 15 infants born from mothers receiving barbiturates during pregnancy, Desmond et al. [190] reported that the syndrome develops with an early acute phase, characterized by symptoms such as persistent crying, tremors, sleeplessness, hiccups and mouthing, followed by a subacute phase, with symptoms such as hyperphagia, episodes of prolonged crying, irritability, hyperacusia and sweating [190]. Other symptoms reported in the literature include hypotonia, feeding accompanied by gagging, vomiting, jitteriness and seizures [193–195].
Although symptoms are similar to those observed in opioid-exposed infants, barbiturate withdrawal symptoms appear to have a later onset (median age 6 days, range 30 min–14 days) than opioid withdrawal symptoms (median age 6 h, range 10 min–2 days) [190, 194, 196]. This delay can be explained by the mechanism of tissue accumulation (described in the section dedicated to AEDs in general) and by the poor conjugating capacity of the neonate, as well as the poor glomerular and tubular function of immature kidneys [189–191]. The duration of symptoms can vary from 2 to 4 months (with a median of 3 months), although they may persist for up to 6 months [190]. Moreover, newborns receiving barbiturates (compared with opiates) are less frequently jaundiced, have better Apgar scores, and have no apparent residual injury following withdrawal [190, 194], as well as no autonomic and gastrointestinal distress [193].
Biological mechanisms Barbiturates can easily cross the placental barrier and can be detected at high concentrations in the serum and umbilical cord serum of newborns [191, 196–198]. A lower plasma protein binding (3–43 %) in newborns, compared with adults (51 %), could also explain the higher blood levels as compared with the mother [199]. Factors that may affect serum levels of phenobarbital in offspring include maternal dose, gestational age, neonatal weight and days of life, as well as the duration of prenatal exposure [191, 194]. The mechanism of barbiturate-induced NAS is not clear but is likely to be similar to that described in the section of this review dedicated to benzodiazepines, thus involving GABA neurotransmission [200].
Management Standard treatments for the management of barbiturate-associated NAS are not available. Phenobarbital has been shown to be effective in the management of the syndrome, even if an elevated rate of tolerance was reported. A daily dosage of phenobarbital 5–7 mg/kg/day in newborns affected by seizures or drug abstinence syndrome has been considered useful and safe for infants [199]. As far as preventive approaches are concerned, evidence and data obtained from studies conducted in infants from pregnant epileptic women confirmed the need to treat them with the minimum effective dose, in order to reduce the risk of withdrawal in infants, following placental disposition [191].
3.3.2 Benzodiazepines
Epidemiology Benzodiazepines are frequently used by women of reproductive age and pregnant women for a variety of indications, including anxiety, sleep disturbances, control of seizures and managing pre-eclampsia or eclampsia in the late phase of pregnancy [201–203]. It has been estimated that approximately 2–3 % of pregnant women use benzodiazepines [2, 102, 204, 205].
Despite the relatively frequent use of benzodiazepines during pregnancy, data on neonatal outcomes are still limited and the safety of these drugs in pregnancy, including their teratogenic potential, remains controversial [204, 206–210]. When benzodiazepines are administrated late in pregnancy, they are easily disposed into the fetus, where they have the potential to accumulate, causing two major neonatal syndromes: an NAS designated as ‘opiate-like withdrawal syndrome’ lasting several days, and ‘floppy infant syndrome’ (FIS), characterized by signs of poisoning within the first hours or days [206, 211]. At present, the actual prevalence of neonatal issues with benzodiazepines remains unknown since they can also be used as illicit drugs. Moreover, a small number of studies have examined newborns exposed prenatally to benzodiazepine monotherapy, and the pathophysiology of neonatal syndromes associated with benzodiazepines has been poorly described and understood [6, 208]. The neonatal consequences of benzodiazepine use at the end of pregnancy have been evaluated in an observational study performed by the Regional Pharmacovigilance Center of Tours (France) on 73 pregnancies recorded from 1998 to 2002 [212]. The most commonly used benzodiazepines were oxazepam, bromazepam, alprazolam, clonazepam and clorazepate. Indications included depression, anxiety, epilepsy, insomnia and psychiatric disorders. In this study, exposure to benzodiazepines was associated with adverse reactions in 51.5 % of newborns, comprising an ‘impregnation syndrome’ (characterized by hypotonia and hypoventilation) in 42 % and a withdrawal syndrome in 20 % of cases (tremors as the main symptom) [212]. Another study, performed to investigate infant and maternal characteristics of NAS in selected hospitals in Florida from 2010 to 2011, showed that benzodiazepines were the second most commonly reported drug class associated with NAS (40.5 %) [213]. Lastly, an analysis of the Swedish Medical Birth Register found that late exposure to benzodiazepines and benzodiazepine receptor agonists (zopiclone, zolpidem, zaleplon) is associated with a higher risk of respiratory problems (OR 2.21, 95 % CI 1.62–3.02) and low Apgar score (OR 2.20, 95 % CI 1.11–4.39). A trend towards an increased risk for signs of CNS disorders (e.g. seizures) was also detected but it was not statistically significant (OR 1.53, 95 % CI 0.42–3.92) [206]. Notably, some case series and studies conducted on specific benzodiazepines (diazepam, clonazepam, lorazepam, oxazepam, chlordiazepoxide, midazolam) did not show any neonatal toxicity or withdrawal syndromes in babies born from mothers who had taken benzodiazepines during pregnancy [214–221].
Clinical features Symptoms of NAS and FIS are largely similar and it can be difficult to distinguish between the two since they may occur in sequence and their symptoms can partly overlap [2, 102]. Signs and symptoms of these syndromes have been described in several case reports and case series of pregnant women exposed to benzodiazepines [203, 211, 216, 218, 222–242]. Symptoms of both NAS and FIS are also documented in dated observational studies [243–249].
NAS can hardly be recognized since it may start several days after delivery, up to 21 days in the case of chlordiazepoxide [235], and symptoms may last for up to 3–6 months [209, 250]. Time to onset and duration of symptoms correlates well with the pharmacokinetics and placental disposition of benzodiazepines and their accumulation in neonatal tissues [203]. NAS symptoms reported in case reports include tremors, irritability, hyperactivity, hypertonicity, tachypnea, vigorous sucking, poor weight gain, loose stools, and vomiting [203, 222, 224, 227, 229, 232–235, 239]. The benzodiazepines involved included diazepam (10–20 mg/day), chlordiazepoxide (20–30 mg/day), lorazepam (1 mg/day), alprazolam (1.5–8 mg/day), oxazepam and clobazam taken for the management of psychiatric disorders and anxiety throughout pregnancy or in the last 3–5 months [203, 222, 224, 227, 229, 232–235, 239]. Concomitant medications may have contributed to the occurrence of symptoms [224, 229]. Notably, in one case the infant died at 6 weeks of age following a withdrawal syndrome associated with in utero exposure to diazepam treated with phenobarbital for 28 days. Death was attributed to sudden infant death syndrome [229].
FIS usually occurs when the fetus is exposed to long-acting benzodiazepines on a long-term basis, or when benzodiazepines are administered shortly before delivery, leading to a newborn intoxication of variable severity and duration. FIS symptoms (hypotonia, inactivity, weak cry, lethargy, sucking difficulties, low Apgar score, hypothermia, apnea, cyanosis, hyperbilirubinemia, CNS depression) occurred mainly within the first hours after labor and lasted for up to 14 days [211, 216, 218, 223, 225, 226, 228, 230, 231, 236–238, 242]. Diazepam (10–30 mg intravenously or 6–25 mg/day) was the mostly reported drug, followed by nitrazepam (5–10 mg/day), lorazepam (7.5 mg/day), chlordiazepoxide (500 mg intravenously or 100 mg/day), clonazepam (0.75 mg/day) and flunitrazepam, taken late in pregnancy for the treatment of psychiatric disorders or during labor in the case of pre-eclampsia or premature labor [211, 216, 218, 223, 225, 226, 228, 230, 237, 242]. Only a few reports have described cases of neonatal apnea or mild depression associated with maternal exposure to clonazepam (5.5 mg/day) for the treatment of epilepsy [231, 238]. In some reports, we cannot exclude the contribution of other psychotropic medications to the occurrence of neonatal symptoms [211, 216, 218, 226, 228, 230].
Biological mechanisms The onset of NAS and FIS, as well as their severity and duration, can be influenced by a number of factors: properties of the specific drug (plasma protein binding, ionization, lipophilicity, molecular weight, half-life, oral bioavailability), maternal treatment (dose, duration of exposure, time of last dose intake, comedication with other drugs), infant characteristics (fetal absorption and storage, postnatal tissue binding and release, metabolism and excretion), and underlying maternal/fetal conditions [102, 206, 229]. Neonatal complications following in utero exposure to benzodiazepines also seem to be related to the lipophilic nature of these drugs, which allows an easy crossing of the placental barrier [206, 225, 227, 237, 247, 251]. Placenta can also be considered as a ‘deep compartment’ where the drug and its metabolites accumulate and are eliminated slowly, in a similar situation to that generally described for AEDs in the previous section [227]. Oxazepam, lorazepam, nitrazepam and, in particular, flunitrazepam, appear to penetrate the human placenta more slowly than diazepam, but the clinical significance of this remains undetermined [214, 215, 251]. Long-acting benzodiazepines (i.e. diazepam, chlordiazepoxide, chlorazepate, flurazepam, prazepam, nitrazepam) exert sustained actions that often can produce a ‘hangover’ type of effect, with long-term treatments resulting in drug accumulation. Short-acting drugs (i.e. alprazolam, lorazepam, oxazepam, temazepam, lormetazepam) display relatively little residual effect but can induce withdrawal symptoms more commonly [203]. Due to immaturity, less total body fat, and differences in overall drug exposure, preterm infants may exhibit fewer signs of withdrawal than term infants. However, it is conceivable that drug metabolism can be delayed in the premature neonate with reduced enzymatic functions in the liver [215, 249]. The long half-life of some benzodiazepines and the immaturity of metabolic pathways in the newborn are not the only factors to be considered when explaining the persistence of neonatal symptoms for weeks after birth. Indeed, benzodiazepines can be easily metabolized by the neonate, and some benzodiazepines (i.e. diazepam and clorazepate) can be converted into active compounds with a longer half-life than those produced by maternal metabolism [211, 215, 229, 249].
Infants may develop NAS with the classical mechanism of abrupt benzodiazepine discontinuation after a passive addiction acquired during pregnancy [252]. The underlying mechanism seems to be related to the mechanism of action of benzodiazepines, and likely results from the modulation of GABA-A receptors. Indeed, benzodiazepines enhance the affinity of GABA-A receptors for GABA, resulting in an increment of chloride conductance, thus promoting a condition of CNS depression [2, 253].
The mechanism and significance of seizures associated with benzodiazepine withdrawal are unclear [20]. In adults, chronic therapy with benzodiazepines may lead to conformational changes in GABA-A receptors, with a decrease in receptor affinity resulting in decreased GABA activity. When benzodiazepines are withdrawn, the condition of decreased GABA receptor activity leads to reduced GABA inhibitory control on excitatory neurotransmitters, thus promoting a pro-excitatory status in the CNS [254]. Benzodiazepines with a short half-life, such as oxazepam and temazepam, do not usually elicit toxicity, but the risk of withdrawal is increased compared with benzodiazepines with a longer half-life [102]. The mechanism by which benzodiazepines can induce FIS is likely related to an enhancement of GABA actions on GABA-A receptors at limbic, thalamic, and hypothalamic levels, resulting in sedative, hypnotic, anxiolytic, anticonvulsant, and muscle relaxant effects [202]. Fetal benzodiazepine effects seem to be mediated by a central depression of cardiac and/or respiratory reflex centers [255]. High medication doses (i.e. diazepam >30 mg) [247] and benzodiazepines with a long half-life (i.e. nitrazepam and diazepam) were shown to have the highest risk owing to their accumulation in newborns [102].
Management The standard management of benzodiazepine-related neonatal syndromes (NAS and FIS) has not yet been defined, nor has a treatment protocol driven by an assessment tool [6]. The Finnegan score, used to assess the severity of withdrawal syndrome, can be useful for initiating, monitoring, and terminating treatments in neonates [2, 227, 248], and the Apgar score is useful for evaluating acute neonatal outcomes [248, 256]. The initial treatment option is commonly based on a supportive non-pharmacological intervention, and symptoms resolve spontaneously without sequelae [202, 223, 226]. Mechanical feeding and ventilation have been described for management of the most severe acute phases [230]. In the most severe situations, pharmacological treatment can be required [2]. There is general agreement that neonates can benefit from sedative pharmacotherapy [6]. Three cases of severe tremors, occurring in newborns after diazepam exposure in utero, were treated with phenobarbital [229]. Two case reports showed rapid, complete and sustained reversal of prolonged apnea and hypotonia induced by diazepam following treatment with flumazenil [211, 225].
Current information is insufficient to determine whether the potential benefits of benzodiazepine treatment in pregnant women overcome the risks for the fetus [202]. Bearing in mind the RR of drug exposure versus the potential impact of untreated psychiatric disorders [216], when necessary physicians should prescribe benzodiazepines that have more robust safety data, in monotherapy, at the lowest effective dose for the shortest period of time, dividing the daily dose into at least two doses and avoiding high single doses, multidrug regimens, and repeated and prolonged administration of benzodiazepines during pregnancy [202, 236]. If possible, use of the shorter-acting agents should be considered and their discontinuation should be performed, with doses tapered down well prior to delivery [202, 203].
3.4 Antipsychotics
Epidemiology and clinical features The prevalence of pregnancy in women with schizophrenic and other severe and persistent psychiatric disorders (SPPDs) has increased since the deinstitutionalization of mental hospitals and the consequent increased availability of sexual partners [257–259]. Moreover, the progressive reduction of the use of first-generation antipsychotics (FGAs), endowed with hyperprolactinemic effects that may exert a control on fertility, in favor of second-generation antipsychotics (SGAs), often lacking effects on fertility, are further increasing the frequency of pregnancy in patients with SPPD [260, 261].
Evidence regarding the impact of pregnancy on the course of schizophrenia is inconclusive. Women with a history of psychotic disorders may experience a worsening, rather than an improvement, of symptoms during pregnancy [262, 263]. As far as bipolar disorder is concerned, the issue of whether this disease worsens during pregnancy is controversial, with some studies showing worsening of the disease [264, 265] and other studies showing no consequences [266–270]. In this scenario, it is particularly important that the mental health of women with SPPDs is stable if they are about to become parents.
Antipsychotics are effective medications for psychotic and bipolar manic episodes, and their use is rising among pregnant women with bipolar disorder, schizophrenia, and unipolar depression, as well as other SPPDs [271–274]; however, reproductive safety data on these drugs are limited. Studies investigating the teratogenic potential of antipsychotic medications have shown a general increase in the risk of malformations associated with the overall drug class. This finding does not allow to exclude that the underlying disease or unidentified confounding factors may explain the increased risk [275]. Overall, the use of both SGAs and FGAs during late pregnancy has been associated with increased rates of neonatal complications (i.e. deficits in neuromotor performance, hypertonicity, tremors) compared with exposure to antidepressant and non-psychotropic drugs [276, 277].
In 2011, the US FDA issued a warning about neonatal extrapyramidal symptoms and possible medication withdrawal based on data from the Adverse Event Reporting System (AERS) [278]. Indeed, from 2008 to 2011, the AERS database identified 69 cases of neonatal extrapyramidal or withdrawal symptoms associated with several antipsychotic drugs. The reported symptoms included agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress and feeding disorder. Blood levels were not provided, making it impossible to determine whether the events resulted from NAS or residual pharmacological effects. The time to event onset ranged from delivery to 1 month after delivery. Symptoms varied in severity; some neonates recovered within a few hours or days without specific treatment, while others required NICU support and prolonged hospitalization [278].
A study of 142 live births recorded by the Australian National Register of Antipsychotic Medication in Pregnancy (NRAMP) described medication withdrawal symptoms in 15 % of babies. These newborns displayed at least two of the following symptoms: excessive high-pitched crying, pronounced Moro reflex, myoclonic jerks, intermittent bouts of sneezing and/or yawning, excessive drowsiness, tremors, pronounced irritability, difficulty feeding, vomiting, and loose stools [279]. Babies who experienced withdrawal symptoms had been exposed to higher doses of antipsychotics at 12 weeks’ gestation (4.4 vs. 2.7 mg/day), although this difference did not reach statistical significance (p = 0.162). Symptoms were prolonged in several babies, lasting up to 6–8 weeks [279].
Differences can be highlighted among individual antipsychotic drugs. Neonatal complications ranging from mild withdrawal reactions to seizures have been described for risperidone [280–283]. A case report described an episode of hyperbilirubinemia, thermoregulation, and feeding problems associated with in utero exposure to risperidone (4 mg/day), requiring hospitalization of the newborn for 6 weeks [282]. Neonatal alterations associated with late in utero exposure to haloperidol may include thermoregulation impairments, decreased muscle tone, tremor on stimulation, vomiting, and poor feeding [284]. In a study, neonatal symptoms were observed in 8 of 30 (27 %) olanzapine-exposed infants versus 1 of 51 (2 %) non-exposed controls. These symptoms included respiratory distress (two cases), hypotonia (one case), poor sucking or difficulty feeding (two cases), and unspecified withdrawal syndrome (three cases) [285]. For clozapine, reported neonatal complications include retinopathy, transient and severe neonatal hypoxemic encephalopathy, and FIS [226, 275, 286–294]. Two case reports described delayed extrapyramidal symptoms in infants following prenatal fluphenazine administration [295, 296]. One developed neurologic symptoms, such as choreoathetoid and dystonic movements of the upper limbs, jitteriness, and hypertonicity that began 3 weeks after birth and lasted for 9 months. The second case had extrapyramidal manifestations that began 4 weeks after delivery. Both infants responded to treatment with diphenhydramine hydrochloride. In these two cases, respiratory effects were not reported. Another case described an infant with severe rhinorrhea and upper respiratory distress 8 h after birth [297]. Over the next 48 h, nasal congestion, rhinorrhea, extrapyramidal movements and vomiting improved and the baby was discharged on day 3. Nasal congestion and rhinorrhea persisted for 3 months.
Biological mechanisms All psychotropic medications can diffuse readily to the fetus across the placenta due to their relatively small molecular size and lipophilic properties [298]. Fetal exposure to these drugs appears to vary according to the level of placental transfer. To quantify the placental permeability to antipsychotic medications, Newport et al. [299] conducted a prospective observational study in which maternal and umbilical cord plasma samples were collected at delivery from 50 women exposed to antipsychotics in pregnancy. The highest placental transfer ratio was observed for olanzapine (mean ratio ± standard deviation 72.1 ± 42.0 %), followed by haloperidol (65.5 ± 40.3 %), risperidone (49.2 ± 33.9 %) and quetiapine (23.8 ± 11.0 %). The mechanism underlying these effects is unclear. It has been suggested that withdrawal symptoms depend on a cholinergic rebound rather than a dopaminergic-blockade [300, 301]. However, we cannot rule out that at least part of the early symptoms is related to residual toxicity.
Management A standard treatment of neonatal complications associated with in utero exposure to antipsychotic medications is not available. In an analysis of 114 babies in the NRAMP database, those who were exclusively breastfed soon after delivery were less likely to experience withdrawal symptoms than those receiving exclusively artificial feeding [9 of 74 (12.2 %) vs. 11 of 40 (27.5 %); OR 2.74, 95 % CI 1.02–7.32] [302]. Mild symptoms may resolve spontaneously without treatments. The clinical management of the most severe cases is based on symptom control with sedative drugs, such as phenobarbital and benzodiazepines [278].
3.5 Other Drugs
In the medical literature, NAS or residual pharmacological effects due to drug exposure during pregnancy have been anecdotally described for clonidine (hypertension-related symptoms) [303], hydroxyzine (neurological symptoms) [304, 305], methyldopa (neonatal jitteriness) [306], pyridoxine (neonatal seizures) [307], and lithium (FIS) [102]; however, the evidence for these drugs is very limited and further studies are needed.
4 Conclusions
Several drugs prescribed during pregnancy can be associated with the development of neonatal abnormalities, resulting from delivery-related withdrawal symptoms or representing a direct harm of the drugs accumulated in the blood and tissues of newborns during the fetal period. These drugs are substantially used to treat CNS diseases, or are able to interfere with neurotransmission both in the brain and peripheral nervous system. These effects are mostly mild, even though severe reactions, rarely fatal in nature, may occur, and their early recognition and management can be helpful in reducing their clinical impact on newborns. Unfortunately, with the potential exception of opioids, validated protocols for the assessment and management of withdrawal or residual toxic effects of these drugs in neonates are often lacking and incomplete, and should be implemented in the future. Notably, the quality of available evidence is often limited, since neonatal adaptation issues have been investigated mainly in case reports and small observational studies. An additional limitation of these investigations stems from the circumstance that they evaluated pregnant women exposed to pharmacological treatments, compared with healthy pregnant women. Therefore, this design does not allow to exclude that the disease may play a role in the occurrence and severity of neonatal symptoms. Moreover, information about differences in the risk of neonatal syndromes across drugs belonging to different drug classes, or even the same drug class, are scarce. Overall, large studies aimed at identifying specific features (i.e. dose/effects relationship, placental function, impact on breastfeeding, and pharmacogenetics) of each drug should be performed, thus allowing the discrimination of the most appropriate and safer pharmacological approach, and also across the same therapeutic class. Spontaneous reporting of these adverse reactions seems limited, although it might represent a useful tool for improving our knowledge about drug-induced neonatal syndromes.
References
Friedman JM. ABCDXXX: The obscenity of postmarketing surveillance for teratogenic effects. Birth Defects Res Part A Clin Mol Teratol. 2012;94(8):670–6.
Kocherlakota P. Neonatal abstinence syndrome. Pediatrics. 2014;134(2):e547–61.
Edwards IR, Aronson JK. Adverse drug reactions: definitions, diagnosis, and management. Lancet. 2000;356(9237):1255–9.
Fabiano V, Mameli C, Zuccotti GV. Adverse drug reactions in newborns, infants and toddlers: pediatric pharmacovigilance between present and future. Expert Opinion Drug Saf. 2012;11(1):95–105.
Koren G. A new indication for therapeutic drug monitoring in the neonate. Ther Drug Monit. 2006;28(1):1.
Jones HE, Fielder A. Neonatal abstinence syndrome: Historical perspective, current focus, future directions. Prev Med. 2015;80:12–7.
Allegaert K, van den Anker JN. Neonatal withdrawal syndrome: reaching epidemic proportions across the globe. Arch Dis Child Fetal Neonatal Ed. 2016;101(1):2–3.
Koren G, Finkelstein Y, Matsui D, Berkovich M. Diagnosis and management of poor neonatal adaptation syndrome in newborns exposed in utero to selective seretonin/norepinephrine reuptake inhibitors. J Obstet Gynecol Can. 2009;31(4):348–50.
Jordan AE, Jackson GL, Deardorff D, Shivakumar G, McIntire DD, Dashe JS. Serotonin reuptake inhibitor use in pregnancy and the neonatal behavioral syndrome. J Matern Fetal Neonatal Med. 2008;21(10):745–51.
Belik J. Fetal and neonatal effects of maternal drug treatment for depression. Semin Perinatol. 2008;32(5):350–4.
Huang H, Coleman S, Bridge JA, Yonkers K, Katon W. A meta-analysis of the relationship between antidepressant use in pregnancy and the risk of preterm birth and low birth weight. Gen Hosp Psychiatry. 2014;36(1):13–8.
Greene CM, Goodman MH. Neonatal abstinence syndrome: strategies for care of the drug-exposed infant. Neonatal netw NN. 2003;22(4):15–25.
Patrick SW, Schumacher RE, Benneyworth BD, Krans EE, McAllister JM, Davis MM. Neonatal abstinence syndrome and associated health care expenditures: United States, 2000–2009. JAMA. 2012;307(18):1934–40.
Tolia VN, Patrick SW, Bennett MM, Murthy K, Sousa J, Smith PB, et al. Increasing incidence of the neonatal abstinence syndrome in US neonatal ICUs. N Engl J Med. 2015;372(22):2118–26.
Turner SD, Gomes T, Camacho X, Yao Z, Guttmann A, Mamdani MM, et al. Neonatal opioid withdrawal and antenatal opioid prescribing. CMAJ Open. 2015;3(1):E55–61.
Engeland A, Bramness JG, Daltveit AK, Ronning M, Skurtveit S, Furu K. Prescription drug use among fathers and mothers before and during pregnancy. A population-based cohort study of 106,000 pregnancies in Norway 2004-2006. Br J Clin Pharmacol. 2008;65(5):653–60.
Warren MD, Miller AM, Traylor J, Bauer A, Patrick SW. Implementation of a statewide surveillance system for neonatal abstinence syndrome—Tennessee, 2013. MMWR Morb Mortal Wkly Rep. 2015;64(5):125–8.
Desai RJ, Huybrechts KF, Hernandez-Diaz S, Mogun H, Patorno E, Kaltenbach K, et al. Exposure to prescription opioid analgesics in utero and risk of neonatal abstinence syndrome: population based cohort study. BMJ (Clin Res ed). 2015;350:h2102.
Jones HE, Kaltenbach K, Heil SH, Stine SM, Coyle MG, Arria AM, et al. Neonatal abstinence syndrome after methadone or buprenorphine exposure. N Engl J Med. 2010;363(24):2320–31.
Hudak ML, Tan RC. Neonatal drug withdrawal. Pediatrics. 2012;129(2):e540–60.
Doberczak TM, Kandall SR, Wilets I. Neonatal opiate abstinence syndrome in term and preterm infants. J Pediatr. 1991;118(6):933–7.
Liu AJ, Jones MP, Murray H, Cook CM, Nanan R. Perinatal risk factors for the neonatal abstinence syndrome in infants born to women on methadone maintenance therapy. Aust N Z J Obstet Gynaecol. 2010;50(3):253–8.
Welle-Strand GK, Skurtveit S, Tanum L, Waal H, Bakstad B, Bjarko L, et al. Tapering from methadone or buprenorphine during pregnancy: maternal and neonatal outcomes in Norway 1996–2009. Eur Addict Res. 2015;21(5):253–61.
Yazdy MM, Mitchell AA, Tinker SC, Parker SE, Werler MM. Periconceptional use of opioids and the risk of neural tube defects. Obstet Gynecol. 2013;122(4):838–44.
Nasiraei-Moghadam S, Sahraei H, Bahadoran H, Sadooghi M, Salimi SH, Kaka GR, et al. Effects of maternal oral morphine consumption on neural tube development in Wistar rats. Brain Res Dev Brain Res. 2005;159(1):12–7.
Broussard CS, Rasmussen SA, Reefhuis J, Friedman JM, Jann MW, Riehle-Colarusso T et al. Maternal treatment with opioid analgesics and risk for birth defects. Am J Obstet Gynecol. 2011;204(4):314.e1–11.
Kivisto K, Tupola S, Kivitie-Kallio S. Prenatally buprenorphine-exposed children: health to 3 years of age. Eur J Pediatr. 2015;174(11):1525–33.
Fodor A, Timar J, Zelena D. Behavioral effects of perinatal opioid exposure. Life Sci. 2014;104(1–2):1–8.
Yuan Q, Rubic M, Seah J, Rae C, Wright IM, Kaltenbach K, et al. Do maternal opioids reduce neonatal regional brain volumes? A pilot study. J Perinatol. 2014;34(12):909–13.
Baglin S, Avenel S, Renaud C, Bavoux F, Francoual C, Badoual J. Withdrawal syndrome in a newborn infant born to an addicted mother receiving methadone [in French]. Arch Pediatr. 1995;2(7):702–3.
Dahan S, Elefant E, Girard I, Azcona B, Champion V, Mitanchez D. Neonatal seizures, buprenorphine abstinence syndrome, and substitutive treatment with morphine [in French]. Arch Pediatr. 2011;18(3):287–90.
Hagopian GS, Wolfe HM, Sokol RJ, Ager JW, Wardell JN, Cepeda EE. Neonatal outcome following methadone exposure in utero. J Matern Fetal Med. 1996;5(6):348–54.
Herve F, Quenum S. Buprenorphine (subutex) and neonatal withdrawal syndrome [in French]. Arch Pediatr. 1998;5(2):206–7.
Lacroix I, Berrebi A, Chaumerliac C, Lapeyre-Mestre M, Montastruc JL, Damase-Michel C. Buprenorphine in pregnant opioid-dependent women: first results of a prospective study. Addiction (Abingdon, England). 2004;99(2):209–14.
Liu WF, Singh K, Faisal M, Li S. Maternal methadone treatment and neonatal abstinence syndrome. Am J Perinatol. 2015;32(11):1078–86.
Maas U, Kattner E, Weingart-Jesse B, Schafer A, Obladen M. Infrequent neonatal opiate withdrawal following maternal methadone detoxification during pregnancy. J Perinat Med. 1990;18(2):111–8.
Gordon AL, Lopatko OV, Haslam RR, Stacey H, Pearson V, Woods A, et al. Ineffective morphine treatment regimen for the control of Neonatal Abstinence Syndrome in buprenorphine- and methadone-exposed infants. J Dev Orig Health Dis. 2012;3(4):262–70.
Coyle MG, Salisbury AL, Lester BM, Jones HE, Lin H, Graf-Rohrmeister K, et al. Neonatal neurobehavior effects following buprenorphine versus methadone exposure. Addiction (Abingdon, England). 2012;107(Suppl 1):63–73.
Berghella V, Lim PJ, Hill MK, Cherpes J, Chennat J, Kaltenbach K. Maternal methadone dose and neonatal withdrawal. Am J Obstet Gynecol. 2003;189(2):312–7.
Seligman NS, Almario CV, Hayes EJ, Dysart KC, Berghella V, Baxter JK. Relationship between maternal methadone dose at delivery and neonatal abstinence syndrome. J Pediatrics. 2010;157(3):428–33, 33.e1.
Cleary BJ, Donnelly J, Strawbridge J, Gallagher PJ, Fahey T, Clarke M et al. Methadone dose and neonatal abstinence syndrome-systematic review and meta-analysis. Addiction (Abingdon, England). 2010;105(12):2071–84.
O’Connor AB, O’Brien L, Alto WA. Maternal buprenorphine dose at delivery and its relationship to neonatal outcomes. Eur Addict Res. 2016;22(3):127–30.
Jones HE, Dengler E, Garrison A, O’Grady KE, Seashore C, Horton E, et al. Neonatal outcomes and their relationship to maternal buprenorphine dose during pregnancy. Drug Alcohol Depend. 2014;134:414–7.
Lejeune C, Simmat-Durand L, Gourarier L, Aubisson S. Prospective multicenter observational study of 260 infants born to 259 opiate-dependent mothers on methadone or high-dose buprenophine substitution. Drug Alcohol Depend. 2006;82(3):250–7.
McCarthy JJ, Leamon MH, Willits NH, Salo R. The effect of methadone dose regimen on neonatal abstinence syndrome. J Addict Med. 2015;9(2):105–10.
Sabatowski R, Radbruch L, Grond S, Gohring UJ. Treatment of severe low back pain with opioids during pregnancy in a patient with incomplete tetraplegia. Acta Anaesthesiol Scand. 2000;44(3):348–50.
Khan K, Chang J. Neonatal abstinence syndrome due to codeine. Arch Dis Child Fetal Neonatal Ed. 1997;76(1):F59–60.
Mangurten HH, Benawra R. Neonatal codeine withdrawal in infants of nonaddicted mothers. Pediatrics. 1980;65(1):159–60.
Van Leeuwen G, Guthrie R, Stange F. Narcotic withdrawal reaction in a newborn infant due to codeine. Pediatrics. 1965;36(4):635–6.
Nair V, Soraisham AS, Akierman A. Neonatal withdrawal syndrome due to maternal codeine use. Paediatr Child Health. 2012;17(5):e40–1.
Reynolds EW, Riel-Romero RM, Bada HS. Neonatal abstinence syndrome and cerebral infarction following maternal codeine use during pregnancy. Clin Pediatr. 2007;46(7):639–45.
Hartenstein S, Proquitte H, Bauer S, Bamberg C, Roehr CC. Neonatal abstinence syndrome (NAS) after intrauterine exposure to tramadol. J Perinat Med. 2010;38(6):695–6.
O’Mara K, Gal P, Davanzo C. Treatment of neonatal withdrawal with clonidine after long-term, high-dose maternal use of tramadol. Ann Pharmacother. 2010;44(7–8):1342–4.
Willaschek C, Wolter E, Buchhorn R. Tramadol withdrawal in a neonate after long-term analgesic treatment of the mother. Eur J Clin Pharmacol. 2009;65(4):429–30.
Meyer FP, Rimasch H, Blaha B, Banditt P. Tramadol withdrawal in a neonate. Eur J Clin Pharmacol. 1997;53(2):159–60.
de Wit D, Koomen-Botman I. Neonatal abstinence syndrome after maternal use of tramadol [in Dutch]. Ned Tijdschr Geneeskd. 2013;157(9):A5610.
Klein RB, Blatman S, Little GA. Probable neonatal propoxyphene withdrawal: a case report. Pediatrics. 1975;55(6):882–4.
Ente G, Mehra MC. Neonatal withdrawal from propoxyphene hydrochloride. N Y State J Med. 1978;78(13):2084–5.
Quillian WW 2nd, Dunn CA. Neonatal drug withdrawal from propoxyphene. JAMA. 1976;235(19):2128.
Tyson HK. Neonatal withdrawal symptoms associated with maternal use of propoxyphene hydrochloride (Darvon). J Pediatrics. 1974;85(5):684–5.
Regan J, Chambers F, Gorman W, MacSullivan R. Neonatal abstinence syndrome due to prolonged administration of fentanyl in pregnancy. BJOG Int J Obst Gynaecol. 2000;107(4):570–2.
Wu WH, Teng RJ, Shin HY. Neonatal pentazocine withdrawal syndrome—a case report of conservative treatment. Zhonghua yi Xue Za Zhi (Taipei). 1988;42(3):229–32.
Scanlon JW. Letter: pentazocine and neonatal withdrawal symptoms. J Pediatrics. 1974;85(5):735–6.
Goetz RL, Bain RV. Neonatal withdrawal symptoms associated with maternal use of pentazocine. J Pediatrics. 1974;84(6):887–8.
Wachman EM, Hayes MJ, Lester BM, Terrin N, Brown MS, Nielsen DA, et al. Epigenetic variation in the mu-opioid receptor gene in infants with neonatal abstinence syndrome. J Pediatr. 2014;165(3):472–8.
Ebner N, Rohrmeister K, Winklbaur B, Baewert A, Jagsch R, Peternell A, et al. Management of neonatal abstinence syndrome in neonates born to opioid maintained women. Drug Alcohol Depend. 2007;87(2–3):131–8.
Johnson RE, Jones HE, Fischer G. Use of buprenorphine in pregnancy: patient management and effects on the neonate. Drug Alcohol Depend. 2003;70(2 Suppl):S87–101.
Stover MW, Davis JM. Opioids in pregnancy and neonatal abstinence syndrome. Semin Perinatol. 2015;39(7):561–5.
Wolff K, Perez-Montejano R. Opioid neonatal abstinence syndrome: controversies and implications for practice. Current Drug Abuse Rev. 2014;7(1):44–58.
Bagley SM, Wachman EM, Holland E, Brogly SB. Review of the assessment and management of neonatal abstinence syndrome. Addict Sci Clin Pract. 2014;9(1):19.
Sarkar S, Donn SM. Management of neonatal abstinence syndrome in neonatal intensive care units: a national survey. J Perinatol. 2006;26(1):15–7.
Finnegan LP, Connaughton JF Jr, Kron RE, Emich JP. Neonatal abstinence syndrome: assessment and management. Addictive diseases. 1975;2(1–2):141–58.
Lipsitz PJ. A proposed narcotic withdrawal score for use with newborn infants. A pragmatic evaluation of its efficacy. Clin Pediatr. 1975;14(6):592–4.
Green M, Suffet F. The Neonatal Narcotic Withdrawal Index: a device for the improvement of care in the abstinence syndrome. Am J Drug Alcohol Abuse. 1981;8(2):203–13.
Zahorodny W, Rom C, Whitney W, Giddens S, Samuel M, Maichuk G, et al. The neonatal withdrawal inventory: a simplified score of newborn withdrawal. J Dev Behav Pediatr JDBP. 1998;19(2):89–93.
Parikh R, Hussain T, Holder G, Bhoyar A, Ewer AK. Maternal methadone therapy increases QTc interval in newborn infants. Arch Dis Child Fetal Neonatal Ed. 2011;96(2):F141–3.
Kandall SR, Gaines J, Habel L, Davidson G, Jessop D. Relationship of maternal substance abuse to subsequent sudden infant death syndrome in offspring. J Pediatr. 1993;123(1):120–6.
Bio LL, Siu A, Poon CY. Update on the pharmacologic management of neonatal abstinence syndrome. J Perinatol. 2011;31(11):692–701.
Bozarth MA. Physical dependence produced by central morphine infusions: an anatomical mapping study. Neurosci Biobehav Rev. 1994;18(3):373–83.
Maldonado R, Negus S, Koob GF. Precipitation of morphine withdrawal syndrome in rats by administration of mu-, delta- and kappa-selective opioid antagonists. Neuropharmacology. 1992;31(12):1231–41.
Przewlocki R. Opioid abuse and brain gene expression. Eur J Pharmacol. 2004;500(1–3):331–49.
Kraft WK, van den Anker JN. Pharmacologic management of the opioid neonatal abstinence syndrome. Pediatr Clin North Am. 2012;59(5):1147–65.
Wachman EM, Hayes MJ, Brown MS, Paul J, Harvey-Wilkes K, Terrin N, et al. Association of OPRM1 and COMT single-nucleotide polymorphisms with hospital length of stay and treatment of neonatal abstinence syndrome. JAMA. 2013;309(17):1821–7.
Abdel-Latif ME, Pinner J, Clews S, Cooke F, Lui K, Oei J. Effects of breast milk on the severity and outcome of neonatal abstinence syndrome among infants of drug-dependent mothers. Pediatrics. 2006;117(6):e1163–9.
McQueen KA, Murphy-Oikonen J, Gerlach K, Montelpare W. The impact of infant feeding method on neonatal abstinence scores of methadone-exposed infants. Adv Neonatal Care. 2011;11(4):282–90.
O’Connor AB, Collett A, Alto WA, O’Brien LM. Breastfeeding rates and the relationship between breastfeeding and neonatal abstinence syndrome in women maintained on buprenorphine during pregnancy. J Midwifery Womens Health. 2013;58(4):383–8.
Welle-Strand GK, Skurtveit S, Jansson LM, Bakstad B, Bjarko L, Ravndal E. Breastfeeding reduces the need for withdrawal treatment in opioid-exposed infants. Acta paediatrica (Oslo, Norway: 1992). 2013;102(11):1060–6.
Dryden C, Young D, Hepburn M, Mactier H. Maternal methadone use in pregnancy: factors associated with the development of neonatal abstinence syndrome and implications for healthcare resources. BJOG Int J Obstet Gynaecol. 2009;116(5):665–71.
Pritham UA, Paul JA, Hayes MJ. Opioid dependency in pregnancy and length of stay for neonatal abstinence syndrome. J Obstet Gynecol Neonatal Nurs JOGNN/NAACOG. 2012;41(2):180–90.
Jansson LM, Choo R, Velez ML, Harrow C, Schroeder JR, Shakleya DM, et al. Methadone maintenance and breastfeeding in the neonatal period. Pediatrics. 2008;121(1):106–14.
Minozzi S, Amato L, Bellisario C, Ferri M, Davoli M. Maintenance agonist treatments for opiate-dependent pregnant women. Cochrane Database Syst Rev. 2013;12:CD006318.
Hall ES, Isemann BT, Wexelblatt SL, Meinzen-Derr J, Wiles JR, Harvey S, et al. A cohort comparison of buprenorphine versus methadone treatment for neonatal abstinence syndrome. J Pediatr. 2016;170(39–44):e1.
Kraft WK, Gibson E, Dysart K, Damle VS, Larusso JL, Greenspan JS, et al. Sublingual buprenorphine for treatment of neonatal abstinence syndrome: a randomized trial. Pediatrics. 2008;122(3):e601–7.
Jansson LM, Velez M, Harrow C. The opioid-exposed newborn: assessment and pharmacologic management. J Opioid Manag. 2009;5(1):47–55.
Surran B, Visintainer P, Chamberlain S, Kopcza K, Shah B, Singh R. Efficacy of clonidine versus phenobarbital in reducing neonatal morphine sulfate therapy days for neonatal abstinence syndrome. A prospective randomized clinical trial. J Perinatol. 2013;33(12):954–9.
Jackson L, Ting A, McKay S, Galea P, Skeoch C. A randomised controlled trial of morphine versus phenobarbitone for neonatal abstinence syndrome. Arch Dis Child Fetal Neonatal Ed. 2004;89(4):F300–4.
Langenfeld S, Birkenfeld L, Herkenrath P, Muller C, Hellmich M, Theisohn M. Therapy of the neonatal abstinence syndrome with tincture of opium or morphine drops. Drug Alcohol Depend. 2005;77(1):31–6.
Kraft WK, Dysart K, Greenspan JS, Gibson E, Kaltenbach K, Ehrlich ME. Revised dose schema of sublingual buprenorphine in the treatment of the neonatal opioid abstinence syndrome. Addiction (Abingdon, England). 2011;106(3):574–80.
Coyle MG, Ferguson A, Lagasse L, Oh W, Lester B. Diluted tincture of opium (DTO) and phenobarbital versus DTO alone for neonatal opiate withdrawal in term infants. J Pediatr. 2002;140(5):561–4.
Agthe AG, Kim GR, Mathias KB, Hendrix CW, Chavez-Valdez R, Jansson L, et al. Clonidine as an adjunct therapy to opioids for neonatal abstinence syndrome: a randomized, controlled trial. Pediatrics. 2009;123(5):e849–56.
Moses-Kolko EL, Bogen D, Perel J, Bregar A, Uhl K, Levin B, et al. Neonatal signs after late in utero exposure to serotonin reuptake inhibitors: literature review and implications for clinical applications. JAMA. 2005;293(19):2372–83.
Kieviet N, Dolman KM, Honig A. The use of psychotropic medication during pregnancy: how about the newborn? Neuropsychiatr Dis Treat. 2013;9:1257–66.
Payne JL, Meltzer-Brody S. Antidepressant use during pregnancy: current controversies and treatment strategies. Clin Obstet Gynecol. 2009;52(3):469–82.
Olivier JD, Akerud H, Kaihola H, Pawluski JL, Skalkidou A, Hogberg U, et al. The effects of maternal depression and maternal selective serotonin reuptake inhibitor exposure on offspring. Front Cell Neurosci. 2013;7:73.
Sanz EJ, De-las-Cuevas C, Kiuru A, Bate A, Edwards R. Selective serotonin reuptake inhibitors in pregnant women and neonatal withdrawal syndrome: a database analysis. Lancet. 2005;365(9458):482–7.
Thormahlen GM. Paroxetine use during pregnancy: is it safe? Ann Pharmacother. 2006;40(10):1834–7.
Oberlander TF, Misri S, Fitzgerald CE, Kostaras X, Rurak D, Riggs W. Pharmacologic factors associated with transient neonatal symptoms following prenatal psychotropic medication exposure. J Clin Psychiatry. 2004;65(2):230–7.
Stahl MM, Lindquist M, Pettersson M, Edwards IR, Sanderson JH, Taylor NF, et al. Withdrawal reactions with selective serotonin re-uptake inhibitors as reported to the WHO system. Eur J Clin Pharmacol. 1997;53(3–4):163–9.
ter Horst PG, van der Linde S, Smit JP, den Boon J, van Lingen RA, Jansman FG, et al. Clomipramine concentration and withdrawal symptoms in 10 neonates. Br J Clin Pharmacol. 2012;73(2):295–302.
Forsberg L, Naver L, Gustafsson LL, Wide K. Neonatal adaptation in infants prenatally exposed to antidepressants–clinical monitoring using Neonatal Abstinence Score. PLoS ONE. 2014;9(11):e111327.
Ansary A, Ibhanesebhor S, Manjunatha C. Myoclonic seizures in a preterm baby: is this a presentation of venlafaxine withdrawal? Singap Med J. 2014;55(4):e57–9.
Eyal R, Yaeger D. Poor neonatal adaptation after in utero exposure to duloxetine. Am J Psychiatry. 2008;165(5):651.
Abdy NA, Gerhart K. Duloxetine withdrawal syndrome in a newborn. Clin Pediatr. 2013;52(10):976–7.
Alehan F, Saygi S, Tarcan A, Gurakan B. Prolonged neonatal complications after in utero exposure to fluoxetine. J Matern Fetal Neonatal medicine. 2008;21(12):921–3.
Anbu AT, Theodore A. Fluoxetine withdrawal syndrome in the newborn. Indian Pediatr. 2006;43(1):66–9.
Bellantuono C, Bozzi F, Orsolini L. Safety of escitalopram in pregnancy: a case series. Neuropsychiatr Dis Treat. 2013;9:1333–7.
Boringa JB, de Jong GM, Touw DJ. Neonatal withdrawal symptoms following the use of clomipramine during pregnancy [in Dutch]. Ned Tijdschr Geneeskd. 1992;136(30):1473–5.
Costei AM, Kozer E, Ho T, Ito S, Koren G. Perinatal outcome following third trimester exposure to paroxetine. Arch Pediatr Adolesc Med. 2002;156(11):1129–32.
Davis RL, Rubanowice D, McPhillips H, Raebel MA, Andrade SE, Smith D, et al. Risks of congenital malformations and perinatal events among infants exposed to antidepressant medications during pregnancy. Pharmacoepidemiol Drug Saf. 2007;16(10):1086–94.
de Moor RA, Mourad L, ter Haar J, Egberts AC. Withdrawal symptoms in a neonate following exposure to venlafaxine during pregnancy [in Dutch]. Ned Tijdschr Geneeskd. 2003;147(28):1370–2.
Leibovitch L, Rymer-Haskel N, Schushan-Eisen I, Kuint J, Strauss T, Maayan-Metzger A. Short-term neonatal outcome among term infants after in utero exposure to serotonin reuptake inhibitors. Neonatology. 2013;104(1):65–70.
Levinson-Castiel R, Merlob P, Linder N, Sirota L, Klinger G. Neonatal abstinence syndrome after in utero exposure to selective serotonin reuptake inhibitors in term infants. Arch Pediatr Adolesc Med. 2006;160(2):173–6.
Nordeng H, Lindemann R, Perminov KV, Reikvam A. Neonatal withdrawal syndrome after in utero exposure to selective serotonin reuptake inhibitors. Acta paediatrica (Oslo, Norway: 1992). 2001;90(3):288–91.
Santos RP, Pergolizzi JJ. Transient neonatal jitteriness due to maternal use of sertraline (Zoloft). J Perinatol. 2004;24(6):392–4.
Cowe L, Lloyd DJ, Dawling S. Neonatal convulsions caused by withdrawal from maternal clomipramine. Br Med J (Clin Res Ed). 1982;284(6332):1837–8.
Haddad PM, Pal BR, Clarke P, Wieck A, Sridhiran S. Neonatal symptoms following maternal paroxetine treatment: serotonin toxicity or paroxetine discontinuation syndrome? J Psychopharmacol (Oxf Engl). 2005;19(5):554–7.
Pakalapati RK, Bolisetty S, Austin MP, Oei J. Neonatal seizures from in utero venlafaxine exposure. J Paediatr Child Health. 2006;42(11):737–8.
Pogliani L, Schneider L, Dilillo D, Penagini F, Zuccotti GV. Paroxetine and neonatal withdrawal syndrome. BMJ Case Rep. 2010;2010. pii:bcr1220092528. doi:10.1136/bcr.12.2009.2528.
Kallen B. Neonate characteristics after maternal use of antidepressants in late pregnancy. Arch Pediatr Adolesc Med. 2004;158(4):312–6.
Jaiswal S, Coombs RC, Isbister GK. Paroxetine withdrawal in a neonate with historical and laboratory confirmation. Eur J Pediatr. 2003;162(10):723–4.
Murray KL, Miller KM, Pearson DL. Neonatal withdrawal syndrome following in utero exposure to paroxetine, clonazepam and olanzapine. J Perinatol. 2007;27(8):517–8.
Grigoriadis S, VonderPorten EH, Mamisashvili L, Eady A, Tomlinson G, Dennis CL, et al. The effect of prenatal antidepressant exposure on neonatal adaptation: a systematic review and meta-analysis. J Clin Psychiatry. 2013;74(4):e309–20.
Andrade C. The safety of duloxetine during pregnancy and lactation. J Clin Psychiatry. 2014;75(12):e1423–7.
Ter Horst PG, Jansman FG, van Lingen RA, Smit P, Jong-van den Berg LT, Brouwers JR. Pharmacological aspects of neonatal antidepressant withdrawal. Obstet Gynecol Surv. 2008;63(4):267–79.
Klinger G, Merlob P. Selective serotonin reuptake inhibitor induced neonatal abstinence syndrome. Isr J Psychiatry Relat Sci. 2008;45(2):107–13.
Bot P, Semmekrot BA, van der Stappen J. Neonatal effects of exposure to selective serotonin reuptake inhibitors during pregnancy. Arch Dis Child Fetal Neonatal Ed. 2006;91(2):F153.
Eleftheriou G, Butera R, Cotti Cottini F, Bonati M, Farina M. Neonatal toxicity following maternal citalopram treatment. Fetal Pediatr Pathol. 2013;32(5):362–6.
Laine K, Heikkinen T, Ekblad U, Kero P. Effects of exposure to selective serotonin reuptake inhibitors during pregnancy on serotonergic symptoms in newborns and cord blood monoamine and prolactin concentrations. Arch Gen Psychiatry. 2003;60(7):720–6.
Koren G, Matsui D, Einarson A, Knoppert D, Steiner M. Is maternal use of selective serotonin reuptake inhibitors in the third trimester of pregnancy harmful to neonates? CMAJ. 2005;172(11):1457–9.
Oberlander TF, Warburton W, Misri S, Aghajanian J, Hertzman C. Neonatal outcomes after prenatal exposure to selective serotonin reuptake inhibitor antidepressants and maternal depression using population-based linked health data. Arch Gen Psychiatry. 2006;63(8):898–906.
Klinger G, Frankenthal D, Merlob P, Diamond G, Sirota L, Levinson-Castiel R, et al. Long-term outcome following selective serotonin reuptake inhibitor induced neonatal abstinence syndrome. J Perinatol. 2011;31(9):615–20.
Rampono J, Simmer K, Ilett KF, Hackett LP, Doherty DA, Elliot R, et al. Placental transfer of SSRI and SNRI antidepressants and effects on the neonate. Pharmacopsychiatry. 2009;42(3):95–100.
Rampono J, Proud S, Hackett LP, Kristensen JH, Ilett KF. A pilot study of newer antidepressant concentrations in cord and maternal serum and possible effects in the neonate. Int J Neuropsychopharmacol. 2004;7(3):329–34.
Heikkine T, Ekblad U, Laine K. Transplacental transfer of citalopram, fluoxetine and their primary demethylated metabolites in isolated perfused human placenta. BJOG Int J Obstetr Gynaecol. 2002;109(9):1003–8.
Coupland NJ, Bell CJ, Potokar JP. Serotonin reuptake inhibitor withdrawal. J Clin Psychopharmacol. 1996;16(5):356–62.
Warner CH, Bobo W, Warner C, Reid S, Rachal J. Antidepressant discontinuation syndrome. Am Fam Physician. 2006;74(3):449–56.
Warburton W, Hertzman C, Oberlander TF. A register study of the impact of stopping third trimester selective serotonin reuptake inhibitor exposure on neonatal health. Acta Psychiatr Scand. 2010;121(6):471–9.
Ferreira E, Carceller AM, Agogue C, Martin BZ, St-Andre M, Francoeur D, et al. Effects of selective serotonin reuptake inhibitors and venlafaxine during pregnancy in term and preterm neonates. Pediatrics. 2007;119(1):52–9.
Jefferies AL. Selective serotonin reuptake inhibitors in pregnancy and infant outcomes. Paediatr Child Health. 2011;16(9):562–3.
Tuccori M, Testi A, Antonioli L, Fornai M, Montagnani S, Ghisu N, et al. Safety concerns associated with the use of serotonin reuptake inhibitors and other serotonergic/noradrenergic antidepressants during pregnancy: a review. Clin Ther. 2009;31(Pt 1):1426–53.
Morris R, Matthes J. Serotonin syndrome in a breast-fed neonate. BMJ Case Rep. 2015;2015. pii:bcr2015209418. doi:10.1136/bcr-2015-209418.
Ahmed M, Parameshwaran A, Swamy P. Neonatal convulsions secondary to paroxetine withdrawal. J Pak Med Assoc. 2007;57(3):162.
Hendrick V, Stowe ZN, Altshuler LL, Mintz J, Hwang S, Hostetter A, et al. Fluoxetine and norfluoxetine concentrations in nursing infants and breast milk. Biol Psychiatry. 2001;50(10):775–82.
Boyce PM, Hackett LP, Ilett KF. Duloxetine transfer across the placenta during pregnancy and into milk during lactation. Arch Womens Mental Health. 2011;14(2):169–72.
Briggs GG, Ambrose PJ, Ilett KF, Hackett LP, Nageotte MP, Padilla G. Use of duloxetine in pregnancy and lactation. Ann Pharmacother. 2009;43(11):1898–902.
Coban D, Kurtoglu S, Akin MA, Akcakus M, Gunes T. Neonatal episodic hypoglycemia: a finding of valproic acid withdrawal. J Clin Res Pediatr Endocrinol. 2010;2(2):92–4.
Burja S, Rakovec-Felser Z, Treiber M, Hajdinjak D, Gajsek-Marchetti M. The frequency of neonatal morbidity after exposure to antiepileptic drugs in utero: a retrospective population-based study. Wien Klin Wochenschr. 2006;118(Suppl 2):12–6.
Dean JC, Moore SJ, Turnpenny PD. Developing diagnostic criteria for the fetal anticonvulsant syndromes. Seizure. 2000;9(3):233–4.
Dean JC, Hailey H, Moore SJ, Lloyd DJ, Turnpenny PD, Little J. Long term health and neurodevelopment in children exposed to antiepileptic drugs before birth. J Med Genet. 2002;39(4):251–9.
Borthen I, Eide MG, Veiby G, Daltveit AK, Gilhus NE. Complications during pregnancy in women with epilepsy: population-based cohort study. BJOG Int J Obstetr Gynaecol. 2009;116(13):1736–42.
Brosh K, Matok I, Sheiner E, Koren G, Wiznitzer A, Gorodischer R et al. Teratogenic determinants of first-trimester exposure to antiepileptic medications. J Popul Ther Clin Pharmacol. 2011;18:e89–98.
Bech BH, Kjaersgaard MI, Pedersen HS, Howards PP, Sorensen MJ, Olsen J, et al. Use of antiepileptic drugs during pregnancy and risk of spontaneous abortion and stillbirth: population based cohort study. BMJ (Clin Research Ed). 2014;349:g5159.
Bobo WV, Davis RL, Toh S, Li DK, Andrade SE, Cheetham TC, et al. Trends in the use of antiepileptic drugs among pregnant women in the US, 2001–2007: a medication exposure in pregnancy risk evaluation program study. Paediatr Perinat Epidemiol. 2012;26(6):578–88.
Wen X, Meador KJ, Hartzema A. Antiepileptic drug use by pregnant women enrolled in Florida Medicaid. Neurology. 2015;84(9):944–50.
Utilization of antiepileptic drugs during pregnancy: comparative patterns in 38 countries based on data from the EURAP registry. Epilepsia. 2009;50(10):2305–9.
Vajda FJ, Hollingworth S, Graham J, Hitchcock AA, O’Brien TJ, Lander CM, et al. Changing patterns of antiepileptic drug use in pregnant Australian women. Acta Neurol Scand. 2010;121(2):89–93.
Meador KJ. Effects of in utero antiepileptic drug exposure. Epilepsy Curr Am Epilepsy Soc. 2008;8(6):143–7.
Crawford P. Best practice guidelines for the management of women with epilepsy. Epilepsia. 2005;46(Suppl 9):117–24.
D’Souza SW, Robertson IG, Donnai D, Mawer G. Fetal phenytoin exposure, hypoplastic nails, and jitteriness. Arch Dis Child. 1991;66(3):320–4.
Koch S, Jager-Roman E, Losche G, Nau H, Rating D, Helge H. Antiepileptic drug treatment in pregnancy: drug side effects in the neonate and neurological outcome. Acta paediatrica (Oslo, Norway: 1992). 1996;85(6):739–46.
Ebbesen F, Joergensen A, Hoseth E, Kaad PH, Moeller M, Holsteen V, et al. Neonatal hypoglycaemia and withdrawal symptoms after exposure in utero to valproate. Arch Dis Child Fetal Neonatal Ed. 2000;83(2):F124–9.
Nau H, Rating D, Koch S, Hauser I, Helge H. Valproic acid and its metabolites: placental transfer, neonatal pharmacokinetics, transfer via mother’s milk and clinical status in neonates of epileptic mothers. J Pharmacol Exp Ther. 1981;219(3):768–77.
Thisted E, Ebbesen F. Malformations, withdrawal manifestations, and hypoglycaemia after exposure to valproate in utero. Arch Dis Child. 1993;69(3 Spec No):288–91.
Duncan SD, Devlin LA. Use of baclofen for withdrawal in a preterm infant. J Perinatol. 2013;33(4):327–8.
Ratnayaka BD, Dhaliwal H, Watkin S. Drug points: Neonatal convulsions after withdrawal of baclofen. BMJ (Clin Res Ed). 2001;323(7304):85.
Koch S, Gopfert-Geyer I, Jager-Roman E, Jakob S, Huth H, Hartmann A, et al. Anti-epileptic agents during pregnancy. A prospective study on the course of pregnancy, malformations and child development [in German]. Dtsch Med Wochenschr. 1983;108(7):250–7.
Rolnitsky A, Merlob P, Klinger G. In utero oxcarbazepine and a withdrawal syndrome, anomalies, and hyponatremia. Pediatr Neurol. 2013;48(6):466–8.
Vieker S, Thiel M, Langler A. Neonatal seizures caused by lamotrigin withdrawal? [in German]. Z Geburtshilfe Neonatol. 2009;213(2):62–3.
Carrasco M, Rao SC, Bearer CF, Sundararajan S. Neonatal gabapentin withdrawal syndrome. Pediatr Neurol. 2015;53(5):445–7.
Tomson T. Gender aspects of pharmacokinetics of new and old AEDs: pregnancy and breast-feeding. Ther Drug Monit. 2005;27(6):718–21.
Ishizaki T, Yokochi K, Chiba K, Tabuchi T, Wagatsuma T. Placental transfer of anticonvulsants (phenobarbital, phenytoin, valproic acid) and the elimination from neonates. Pediatr Pharmacol (N Y NY). 1981;1(4):291–303.
Semczuk-Sikora A, Czuczwar S, Semczuk A, Kwasniewska A, Semczuk M. Valproic acid transfer across human placental cotyledon during dual perfusion in vitro. Ann Agric Environ Med AAEM. 2010;17(1):153–7.
Ohman I, Vitols S, Tomson T. Pharmacokinetics of gabapentin during delivery, in the neonatal period, and lactation: does a fetal accumulation occur during pregnancy? Epilepsia. 2005;46(10):1621–4.
Kuhnz W, Koch S, Helge H, Nau H. Primidone and phenobarbital during lactation period in epileptic women: total and free drug serum levels in the nursed infants and their effects on neonatal behavior. Dev Pharmacol Ther. 1988;11(3):147–54.
Tran KT, Hranicky D, Lark T, Jacob N. Gabapentin withdrawal syndrome in the presence of a taper. Bipolar Disord. 2005;7(3):302–4.
Leo RJ, Baer D. Delirium associated with baclofen withdrawal: a review of common presentations and management strategies. Psychosomatics. 2005;46(6):503–7.
Asai M, Talavera E, Massarini A, Zubieta M, Vindrola O. Valproic acid-induced rapid changes of met-enkephalin levels in rat brain. Probable association with abstinence behavior and anticonvulsant activity. Neuropeptides. 1994;27(3):203–10.
Duncan JS, Shorvon SD, Trimble MR. Discontinuation of phenytoin, carbamazepine, and valproate in patients with active epilepsy. Epilepsia. 1990;31(3):324–33.
Jalling B, Boreus LO, Kallberg N, Agurell S. Disappearance from the newborn of circulating prenatally administered phenobarbital. Eur J Clin Pharmacol. 1973;6(4):234–8.
Desmond MM, Schwanecke RP, Wilson GS, Yasunaga S, Burgdorff I. Maternal barbiturate utilization and neonatal withdrawal symptomatology. J Pediatr. 1972;80(2):190–7.
Zuppa AA, Carducci C, Scorrano A, Antichi E, Catenazzi P, Piras A, et al. Infants born to mothers under phenobarbital treatment: correlation between serum levels and clinical features of neonates. Eur J Obstet Gynecol Reprod Biol. 2011;159(1):53–6.
Zhang LL, Zeng LN, Li YP. Side effects of phenobarbital in epilepsy: a systematic review. Epileptic Disord Int Epilepsy J Videotape. 2011;13(4):349–65.
Bleyer WA, Marshall RE. Barbiturate withdrawal syndrome in a passively addicted infant. JAMA. 1972;221(2):185–6.
Blumenthal I, Lindsay S. Neonatal barbiturate withdrawal. Postgrad Med J. 1977;53(617):157–8.
Erith MJ. Letter: Withdrawal symptoms in newborn infants of epileptic mothers. Br Med J. 1975;3(5974):40.
Neonatal behaviour and maternal barbiturates. Br Med J. 1972;4(5832):63–4.
Ploman L, Persson BH. On the transfer of barbiturates to the human foetus and their accumulation in some of its vital organs. J Obstetr Gynaecol Br Emp. 1957;64(5):706–11.
Melchior JC, Svensmark O, Trolle D. Placental transfer of phenobarbitone in epileptic women, and elimination in newborns. Lancet. 1967;2(7521):860–1.
Davanzo R, Dal Bo S, Bua J, Copertino M, Zanelli E, Matarazzo L. Antiepileptic drugs and breastfeeding. Ital J Pediatr. 2013;39:50.
Bidlack JM, Morris HH 3rd. Phenobarbital withdrawal seizures may occur over several weeks before remitting: human data and hypothetical mechanism. Seizure. 2009;18(1):79–81.
Bergman U, Rosa FW, Baum C, Wiholm BE, Faich GA. Effects of exposure to benzodiazepine during fetal life. Lancet. 1992;340(8821):694–6.
Iqbal MM, Sobhan T, Ryals T. Effects of commonly used benzodiazepines on the fetus, the neonate, and the nursing infant. Psychiatric Serv (Wash, DC). 2002;53(1):39–49.
McElhatton PR. The effects of benzodiazepine use during pregnancy and lactation. Reprod Toxicol (Elmsford, NY). 1994;8(6):461–75.
Addis A, Dolovich LR, Einarson TR, Koren G. Can we use anxiolytics during pregnancy without anxiety? Can Fam Physician Med Fam Can. 2000;46:549–51.
Lendoiro E, Gonzalez-Colmenero E, Concheiro-Guisan A, de Castro A, Cruz A, Lopez-Rivadulla M, et al. Maternal hair analysis for the detection of illicit drugs, medicines, and alcohol exposure during pregnancy. Ther Drug Monit. 2013;35(3):296–304.
Wikner BN, Stiller CO, Bergman U, Asker C, Kallen B. Use of benzodiazepines and benzodiazepine receptor agonists during pregnancy: neonatal outcome and congenital malformations. Pharmacoepidemiol Drug Saf. 2007;16(11):1203–10.
McGrath C, Buist A, Norman TR. Treatment of anxiety during pregnancy: effects of psychotropic drug treatment on the developing fetus. Drug Saf. 1999;20(2):171–86.
Uzun S, Kozumplik O, Jakovljevic M, Sedic B. Side effects of treatment with benzodiazepines. Psychiatr Danub. 2010;22(1):90–3.
ACOG Practice Bulletin. Clinical management guidelines for obstetrician-gynecologists number 92, April 2008 (replaces practice bulletin number 87, November 2007). Use of psychiatric medications during pregnancy and lactation. Obstet Gynecol. 2008;111(4):1001–20.
Dolovich LR, Addis A, Vaillancourt JM, Power JD, Koren G, Einarson TR. Benzodiazepine use in pregnancy and major malformations or oral cleft: meta-analysis of cohort and case-control studies. BMJ (Clin Res Ed). 1998;317(7162):839–43.
Richard P, Autret E, Bardol J, Soyez C, Barbier P, Jonville AP, et al. The use of flumazenil in a neonate. J Toxicol Clin Toxicol. 1991;29(1):137–40.
Swortfiguer D, Cissoko H, Giraudeau B, Jonville-Bera AP, Bensouda L, Autret-Leca E. Neonatal consequences of benzodiazepines used during the last month of pregnancy [in French]. Arch Pediatr. 2005;12(9):1327–31.
Lind JN, Petersen EE, Lederer PA, Phillips-Bell GS, Perrine CG, Li R, et al. Infant and maternal characteristics in neonatal abstinence syndrome–selected hospitals in Florida, 2010–2011. MMWR Morb Mortal Wkly Rep. 2015;64(8):213–6.
Drury KA, Spalding E, Donaldson D, Rutherford D. Floppy-infant syndrome: Is oxazepam the answer? Lancet. 1977;2(8048):1126–7.
McBride RJ, Dundee JW, Moore J, Toner W, Howard PJ. A study of the plasma concentrations of lorazepam in mother and neonate. Br J Anaesth. 1979;51(10):971–8.
Weinstock L, Cohen LS, Bailey JW, Blatman R, Rosenbaum JF. Obstetrical and neonatal outcome following clonazepam use during pregnancy: a case series. Psychother Psychosom. 2001;70(3):158–62.
Decancq HG Jr, Bosco JR, Townsend EH Jr. Chlordiazepoxide in labor. Its effect on the newborn infant. J Pediatrics. 1965;67(5):836–40.
Haram K. “Floppy infant syndrome” and maternal diazepam. Lancet. 1977;2(8038):612–3.
Crawford JS. Premedication for elective Caesarean section. Anaesthesia. 1979;34(9):892–7.
Gitsch E, Philipp K, Schonbauer M. Intranatal administration of midazolam (author’s transl). Z Geburtshilfe Perinatol. 1982;186(1):46–9.
Shader RI. Is there anything new on the use of psychotropic drugs during pregnancy? J Clin Psychopharmacol. 1994;14(6):438.
Barry WS. St Clair SM. Exposure to benzodiazepines in utero. Lancet. 1987;1(8547):1436–7.
Bitnun S. Possible effect of chlordiazepoxide on the fetus. Can Med Assoc J. 1969;100(7):351.
Bellantuono C, Orsolini L, Bozzi F. The safety profile of escitalopram in pregnancy and breastfeeding [in Italian]. Riv Psichiatr. 2013;48(6):407–14.
Cone AM, Nadel S, Sweeney B. Flumazenil reverses diazepam-induced neonatal apnoea and hypotonia. Eur J Pediatr. 1993;152(5):458–9.
Di Michele V, Ramenghi L, Sabatino G. Clozapine and lorazepam administration in pregnancy. Eur Psychiatry J Assoc Eur Psychiatr. 1996;11(4):214.
Garcia-Algar O, Lopez-Vilchez MA, Martin I, Mur A, Pellegrini M, Pacifici R et al. Confirmation of gestational exposure to alprazolam by analysis of biological matrices in a newborn with neonatal sepsis. Clin Toxicol (Phila, Pa). 2007;45(3):295–8.
Gillberg C. “Floppy infant syndrome” and maternal diazepam. Lancet. 1977;2(8031):244.
Rementeria JL, Bhatt K. Withdrawal symptoms in neonates from intrauterine exposure to diazepam. J Pediatrics. 1977;90(1):123–6.
Speight AN. Floppy-infant syndrome and maternal diazepam and/or nitrazepam. Lancet. 1977;2(8043):878.
Fisher JB, Edgren BE, Mammel MC, Coleman JM. Neonatal apnea associated with maternal clonazepam therapy: a case report. Obstet Gynecol. 1985;66(3 Suppl):34s–5s.
Rane A, Sundwall A, Tomson G. Oxazepam withdrawal in the neonatal period [in Swedish]. Lakartidningen. 1979;76(48):4416–7.
Mazzi E. Possible neonatal diazepam withdrawal: a case report. Am J Obstet Gynecol. 1977;129(5):586–7.
Backes CR, Cordero L. Withdrawal symptoms in the neonate from presumptive intrauterine exposure to diazepam: report of case. J Am Osteopath Assoc. 1980;79(9):584–5.
Athinarayanan P, Pierog SH, Nigam SK, Glass L. Chloriazepoxide withdrawal in the neonate. Am J Obstet Gynecol. 1976;124(2):212–3.
Gonzalez de Dios J, Moya-Benavent M, Carratala-Marco F. “Floppy infant” syndrome in twins secondary to the use of benzodiazepines during pregnancy [in Spanish]. Rev Neurol. 1999;29(2):121–3.
Stirrat GM, Edington PT, Berry DJ. Letter: transplacental passage of chlordiazepoxide. Br Med J. 1974;2(5921):729.
Kriel RL, Cloyd J. Clonazepam and pregnancy. Ann Neurol. 1982;11(5):544.
Anderson PO, McGuire GG. Neonatal alprazolam withdrawal–possible effects of breast feeding. DICP Ann Pharmacother. 1989;23(7–8):614.
Shannon RW, Fraser GP, Aitken RG, Harper JR. Diazepam in preeclamptic toxaemia with special reference to its effect on the newborn infant. Br J Clin Pract. 1972;26(6):271–5.
Woods DL, Malan AF. Side-effects of maternal diazepam on the newborn infant. S Afr Med J. 1978;54(16):636.
Bavoux F, Lanfranchi C, Olive G, Asensi D, Dulac O, Francoual C, et al. Adverse effects on newborns from intra uterine exposure to benzodiazepines and other psychotropic agents (author’s transl). Therapie. 1981;36(3):305–12.
Flowers CE, Rudolph AJ, Desmond MM. Diazepam (valium) as an adjunct in obstetric analgesia. Obstet Gynecol. 1969;34(1):68–81.
Nisbet R, Boulas SH, Kantor HI. Diazepam (valium) during labor. Obstet Gynecol. 1967;29(5):726–9.
McCarthy GT, O’Connell B, Robinson AE. Blood levels of diazepam in infants of two mothers given large doses of diazepam during labour. J Obstetr Gynaecol Br Commonw. 1973;80(4):349–52.
Owen JR, Irani SF, Blair AW. Effect of diazepam administered to mothers during labour on temperature regulation of neonate. Arch Dis Child. 1972;47(251):107–10.
Cree JE, Meyer J, Hailey DM. Diazepam in labour: its metabolism and effect on the clinical condition and thermogenesis of the newborn. Br Med J. 1973;4(5887):251–5.
McAuley DM, O’Neill MP, Moore J, Dundee JW. Lorazepam premedication for labour. Br J Obstet Gynaecol. 1982;89(2):149–54.
Whitelaw AG, Cummings AJ, McFadyen IR. Effect of maternal lorazepam on the neonate. Br Med J (Clin Res Ed). 1981;282(6270):1106–8.
Neonatal drug withdrawal. American Academy of Pediatrics Committee on drugs. Pediatrics. 1998;101(6):1079–88.
Kanto JH. Use of benzodiazepines during pregnancy, labour and lactation, with particular reference to pharmacokinetic considerations. Drugs. 1982;23(5):354–80.
Weintraub Z, Bental Y, Olivan A, Rotschild A. Neonatal withdrawal syndrome and behavioral effects produced by maternal drug use. Addict Biol. 1998;3(2):159–70.
Potokar J, Coupland N, Wilson S, Rich A, Nutt D. Assessment of GABA(A)benzodiazepine receptor (GBzR) sensitivity in patients on benzodiazepines. Psychopharmacology. 1999;146(2):180–4.
Marriott S, Tyrer P. Benzodiazepine dependence. Avoidance and withdrawal. Drug Saf. 1993;9(2):93–103.
Stahl MM, Saldeen P, Vinge E. Reversal of fetal benzodiazepine intoxication using flumazenil. Br J Obstet Gynaecol. 1993;100(2):185–8.
Schmidt B, Kirpalani H, Rosenbaum P, Cadman D. Strengths and limitations of the Apgar score: a critical appraisal. J Clin Epidemiol. 1988;41(9):843–50.
Odegard O. Fertility of psychiatric first admissions in Norway 1936–1975. Acta Psychiatr Scand. 1980;62(3):212–20.
Miller WH Jr, Bloom JD, Resnick MP. Prenatal care for pregnant chronic mentally ill patients. Hosp Community Psychiatry. 1992;43(9):942–3.
Castle DJ, McGrath J, Kulkarni J. Reproductive, preconceptual and antenatal needs of women with schizophrenia. Women and Schizophrenia. Cambridge: Cambridge University Press; 2000.
Taylor D, Paton C, Kapur S. Prescribing guidelines in psychiatry. 11th ed. CornWall: Wiley; 2012.
Torre DL, Falorni A. Pharmacological causes of hyperprolactinemia. Ther Clin Risk Manag. 2007;3(5):929–51.
McNeil TF, Kaij L, Malmquist-Larsson A. Women with nonorganic psychosis: pregnancy’s effect on mental health during pregnancy. Acta Psychiatr Scand. 1984;70(2):140–8.
Coverdale JH, Turbott SH, Roberts H. Family planning needs and STD risk behaviours of female psychiatric out-patients. Br J Psychiatry J Mental Sci. 1997;171:69–72.
Burt VK, Rasgon N. Special considerations in treating bipolar disorder in women. Bipolar Disord. 2004;6(1):2–13.
Swann AC. Special needs of women with bipolar disorder. Intellyst Medical Communication International Congress on Women’s Mental Health; 17–20 March 2004; Washington, DC; 2004. p. 4–18.
Grof P, Robbins W, Alda M, Berghoefer A, Vojtechovsky M, Nilsson A, et al. Protective effect of pregnancy in women with lithium-responsive bipolar disorder. J Affect Disord. 2000;61(1–2):31–9.
Kendell RE, Chalmers JC, Platz C. Epidemiology of puerperal psychoses. Br J Psychiatry J Mental Sci. 1987;150:662–73.
Pugh TF, Jerath BK, Schmidt WM, Reed RB. Rates of mental disease related to childbearing. N Engl J Med. 1963;268:1224–8.
Videbech P, Gouliaev G. First admission with puerperal psychosis: 7–14 years of follow-up. Acta Psychiatr Scand. 1995;91(3):167–73.
Freeman MP, Smith KW, Freeman SA, McElroy SL, Kmetz GE, Wright R, et al. The impact of reproductive events on the course of bipolar disorder in women. J Clin Psychiatry. 2002;63(4):284–7.
Gentile S. Atypical antipsychotics for the treatment of bipolar disorder: more shadows than lights. CNS drugs. 2007;21(5):367–87.
Epstein RA, Bobo WV, Shelton RC, Arbogast PG, Morrow JA, Wang W, et al. Increasing use of atypical antipsychotics and anticonvulsants during pregnancy. Pharmacoepidemiol Drug Saf. 2013;22(7):794–801.
Einarson A, Boskovic R. Use and safety of antipsychotic drugs during pregnancy. J Psychiatr Pract. 2009;15(3):183–92.
Gentile S. Antipsychotic therapy during early and late pregnancy. A systematic review. Schizophr Bull. 2010;36(3):518–44.
Reis M, Kallen B. Maternal use of antipsychotics in early pregnancy and delivery outcome. J Clin Psychopharmacol. 2008;28(3):279–88.
Johnson KC, LaPrairie JL, Brennan PA, Stowe ZN, Newport DJ. Prenatal antipsychotic exposure and neuromotor performance during infancy. Arch Gen Psychiatry. 2012;69(8):787–94.
Auerbach JG, Hans SL, Marcus J, Maeir S. Maternal psychotropic medication and neonatal behavior. Neurotoxicol Teratol. 1992;14(6):399–406.
http://www.fda.gov/Drugs/DrugSafety/ucm243903.htm. Accessed 8 June 2016.
Kulkarni J, Worsley R, Gilbert H, Gavrilidis E, Van Rheenen TE, Wang W, et al. A prospective cohort study of antipsychotic medications in pregnancy: the first 147 pregnancies and 100 one year old babies. PLoS ONE. 2014;9(5):e94788.
McKenna K, Koren G, Tetelbaum M, Wilton L, Shakir S, Diav-Citrin O et al. Pregnancy outcome of women using atypical antipsychotic drugs: a prospective comparative study. J Clin Psychiatry. 2005;66(4):444–9 (quiz 546).
Kim SW, Kim KM, Kim JM, Shin IS, Shin HY, Yang SJ, et al. Use of long-acting injectable risperidone before and throughout pregnancy in schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry. 2007;31(2):543–5.
McCauley-Elsom K, Kulkarni J. Managing psychosis in pregnancy. Aust N Z J Psychiatry. 2007;41(3):289–92.
Coppola D, Russo LJ, Kwarta RF Jr, Varughese R, Schmider J. Evaluating the postmarketing experience of risperidone use during pregnancy: pregnancy and neonatal outcomes. Drug Saf. 2007;30(3):247–64.
Nako Y, Tachibana A, Fujiu T, Tomomasa T, Morikawa A. Neonatal thrombocytosis resulting from the maternal use of non-narcotic antischizophrenic drugs during pregnancy. Arch Dis Child Fetal Neonatal Ed. 2001;84(3):F198–200.
Gilad O, Merlob P, Stahl B, Klinger G. Outcome of infants exposed to olanzapine during breastfeeding. Breastfeed Med. 2011;6(2):55–8.
Bazire S. Psychotropic drug directory. Salisbury: Fivepin Limited; 2005:239.
Dev VJKP. Adverse event profile and safety of clozapine. Rev Contemp Pharmacother. 1995;6:197–208.
Vavrusova LKM. Clozapine administration during pregnancy [in Czechoslovakian]. Ceska Slov Psychiatr. 1998;94:282–5.
Mendhekar DN, Sharma JB, Srivastava PK, War L. Clozapine and pregnancy. J Clin Psychiatry. 2003;64(7):850.
Karakula H, Szajer K, Rpila B, Grzywa A, Chuchra M. Clozapine and pregnancy—a case history. Pharmacopsychiatry. 2004;37(6):303–4.
Stoner SC, Sommi RW Jr, Marken PA, Anya I, Vaughn J. Clozapine use in two full-term pregnancies. J Clin Psychiatry. 1997;58(8):364–5.
Yogev Y, Ben-Haroush A, Kaplan B. Maternal clozapine treatment and decreased fetal heart rate variability. Int J Gynaecol Obstet. 2002;79(3):259–60.
Biswasl PN, Wilton LV, Pearcel GL, Freemantle S, Shakir SA. The pharmacovigilance of olanzapine: results of a post-marketing surveillance study on 8858 patients in England. J Psychopharmacol (Oxf, Engl). 2001;15(4):265–71.
Goldstein DJ, Corbin LA, Fung MC. Olanzapine-exposed pregnancies and lactation: early experience. J Clin Psychopharmacol. 2000;20(4):399–403.
O’Connor M, Johnson GH, James DI. Intrauterine effect of phenothiazines. Med J Aust. 1981;1(8):416–7.
Cleary MF. Fluphenazine decanoate during pregnancy. Am J Psychiatry. 1977;134(7):815–6.
Nath SP, Miller DA, Muraskas JK. Severe rhinorrhea and respiratory distress in a neonate exposed to fluphenazine hydrochloride prenatally. Ann Pharmacother. 1996;30(1):35–7.
Iqbal MM, Aneja A, Rahman A, Megna J, Freemont W, Shiplo M, et al. The potential risks of commonly prescribed antipsychotics: during pregnancy and lactation. Psychiatry. 2005;2(8):36–44.
Newport DJ, Calamaras MR, DeVane CL, Donovan J, Beach AJ, Winn S, et al. Atypical antipsychotic administration during late pregnancy: placental passage and obstetrical outcomes. Am J Psychiatry. 2007;164(8):1214–20.
Gardos G, Cole JO, Tarsy D. Withdrawal syndromes associated with antipsychotic drugs. The American journal of psychiatry. 1978;135(11):1321–4.
Luchins DJ, Freed WJ, Wyatt RJ. The role of cholinergic supersensitivity in the medical symptoms associated with withdrawal of antipsychotic drugs. Am J Psychiatry. 1980;137(11):1395–8.
Worsley R, Gilbert H, Gavrilidis E, Naughton B, Kulkarni J. Breastfeeding and psychotropic medications. Lancet. 2013;381(9870):905.
Boutroy MJ, Gisonna CR, Legagneur M. Clonidine: placental transfer and neonatal adaption. Early Human Dev. 1988;17(2–3):275–86.
Prenner BM. Neonatal withdrawal syndrome associated with hydroxyzine hydrochloride. Am J Dis Child (1960). 1977;131(5):529–30.
Serreau R, Komiha M, Blanc F, Guillot F, Jacqz-Aigrain E. Neonatal seizures associated with maternal hydroxyzine hydrochloride in late pregnancy. Reprod Toxicol (Elmsford, NY). 2005;20(4):573–4.
Shimohira M, Iwakawa Y, Kohyama J. Rapid-eye-movement sleep in jittery infants. Early Human Dev. 2002;66(1):25–31.
South M. Neonatal seizures after use of pyridoxine in pregnancy. Lancet. 1999;353(9168):1940–1.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were used to assist in the preparation of this article.
Conflict of interest
Irma Convertino, Alice Capogrosso Sansone, Alessandra Marino, Maria Teresa Galiulo, Stefania Mantarro, Luca Antonioli, Matteo Fornai, Corrado Blandizzi and Marco Tuccori have no conflicts of interest that are directly relevant to the content of this review.
Rights and permissions
About this article
Cite this article
Convertino, I., Sansone, A.C., Marino, A. et al. Neonatal Adaptation Issues After Maternal Exposure to Prescription Drugs: Withdrawal Syndromes and Residual Pharmacological Effects. Drug Saf 39, 903–924 (2016). https://doi.org/10.1007/s40264-016-0435-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-016-0435-8