Abstract
Background
Chronic wound infections are a serious global health concern affecting millions of people. One of the major challenges in treating biofilm-based wound infections is the presence of an extracellular polymeric substance (EPS) that limits the penetration of antimicrobial agents.
Area covered
This review focuses on conventional, current, and prospective anti-biofilm therapies for treating topical biofilm-based wound infections. Conventional strategies involving wound debridement, topical antibiotics, pH modulation, and surfactants have limited efficacy owing to the regrowth of bacteria, development of bacterial resistance, and difficulty in pH modulation. Improvements in anti-biofilm strategies involve current treatment modalities such as antimicrobial peptides, photodynamic substances, bacteriophages, quorum sensing inhibitors, nanoparticles, and hybrid hydrogels. Such strategies exhibit potent anti-biofilm effects upon topical application by targeting multiple mechanisms. However, the prospects of microbial resistance are still prevalent. Therefore, prospective strategies, such as Natural Deep Eutectic Solvents (NADES) and Clustered Regularly Interspaced Short Palindromic Repeats interfering system (CRISPRi), are required for effective anti-biofilm therapy of infected wounds.
Expert opinion
Strategies that completely eradicate biofilm-forming bacteria at wound sites can promote infection control and subsequent wound healing. Further developments in prospective strategies for topical anti-biofilm therapy for infected wounds are warranted. Our review provides valuable insights into the challenges and advancements in the treatment of biofilm-based wound infections, and highlights the need for ongoing research in this area.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A breach in the skin barrier function (following accidental injury, burns, metabolic dysfunction, or skin diseases) can lead to the formation of wounds (Kujath and Kujath 2010). Successful wound healing depends on a complex series of coordinated phenomena, including inflammation, proliferation, migration, and extracellular matrix remodeling, all of which occur at different stages (Eming et al. 2014; Hu et al. 2014). The failure of one or more of these underlying mechanisms can lead to persistent non-healing wounds, known as chronic wounds (Demidova-Rice et al. 2012). Venous and arterial diseases, diabetes, and microbial infections are among the primary aggravating conditions leading to the development of chronic wounds (Mustoe 2004).
From a microbiological perspective, the primary function of intact skin is to control the microbial population on its surface and prevent invasion and colonization of the underlying tissue (Bowler et al. 2001). A wound exposes the subcutaneous tissue, creating a warm, moist, and nutrient-rich environment that is favorable for microbial colonization and proliferation (Chang et al. 2020). Several factors can affect the abundance and variety of microorganisms in a wound, including the wound’s location and depth, the level of tissue perfusion, and antimicrobial efficacy of the host immune response (Bowler et al. 2001). Dermal infections, such as surgical site infections, burns, and non-healing diabetic foot ulcers, affect 9.1–26.1 million people worldwide (Thapa et al. 2020b).
A biofilm is an assemblage of microbial cells that are irreversibly attached to a surface and enclosed in a matrix of primarily polysaccharide material (Cook and Siraj 2017). The different stages of biofilm formation, including surface attachment, microcolony formation, biofilm maturation, dispersal, and detachment, are illustrated in Fig. 1. Biofilms are polymicrobial, and different genotypes are held together by extracellular polymeric substances (EPS) (Flemming et al. 2016). Wound colonization and subsequent infections can involve potentially pathogenic microorganisms, including Staphylococcus and Pseudomonas (Peters et al. 2012; Ruffin and Brochiero 2019). Biofilms present a significant obstacle to the healing of chronic wounds, as they offer substantial protection from host immunity and are often tolerant to antimicrobial agents, leading to delayed healing (Percival et al. 2015). Furthermore, the production of destructive enzymes and toxins by the biofilms can promote chronic inflammation and inhibit wound healing (Rajpaul 2015). In-vitro studies have reported that keratinocytes treated with conditioned media from S. aureus and P. aeruginosa inhibit cell proliferation, whereas conditioned media alone from S. aureus inhibit cell migration (Jeffery Marano et al. 2015). Moreover, low keratinocyte viability was evident following treatment with bacteria-conditioned media. Importantly, in vivo studies involving P. aeruginosa alone (Zhao et al. 2010) or in combination with S. aureus (a polymicrobial wound infection model) (Pastar et al. 2013) exhibited a decrease in the wound repair rate of cutaneous wounds in murine, rabbit, or porcine in vivo models (Brandenburg et al. 2015; Chaney et al. 2017; Karna et al. 2016; Mendes et al. 2013). Therefore, there are complex, proximate, and dynamic interactions between the chronic wound microenvironment and biofilm state that sustain each other, posing challenges for the effective treatment of chronically infected wounds. As a result, the continuous development of novel/improved antimicrobial strategies is required. This review focuses on the conventional, current, and prospective antimicrobial strategies for the treatment of topical biofilm-based wound infections.
Stages of biofilm formation. Initial biofilm attachment on biotic surfaces requires specific interactions between planktonic bacteria and the surface via specific anchoring proteins and pili. After successful attachment, planktonic bacteria form microcolonies in which the bacteria transform into a biofilm state via quorum-sensing and sRNA-based systems. Microcolonies gradually mature into a biofilm with a matrix comprising extracellular polymeric substances surrounded by host inflammatory materials and cells. Biofilms eventually form stalk-like structures, which disperse and detach to form new colonies or incorporate into existing biofilms. c-di-GMP cyclic-di-GMP; EPS extracellular polymeric substances; QS quorum-sensing molecules; sRNA small non-coding RNA. Reproduced with permission from (Wu et al. 2019)
Antimicrobial strategies for topical biofilm-based wound infections
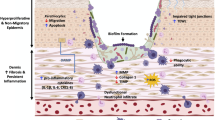
Biofilm eradication and infection control are crucial strategies to enhance wound healing in chronically infected wounds. However, biofilm infections are often unresponsive to several existing antimicrobial treatments owing to their complex physical and biological properties, multiple microbial genetic and molecular factors, and multi-species interactions (Wu et al. 2019). Therefore, targeting different stages of the biofilm life cycle is necessary to achieve improved therapeutic effects. Figure 2 describes potential treatment options for biofilm-based chronic wound infections at various stages of the biofilm life cycle (Koo et al. 2017). The initial adhesion of microorganisms to the wound site can be targeted by interrupting potential interactions between microorganisms and the wound surface through cell surface-associated adhesins, such as appendages, proteins, and EPS. The early stages of biofilm formation can be inhibited by targeting EPS production and cell division. The developed biofilms can be disrupted by physical removal, EPS matrix degradation, a pathogenic microenvironment (hypoxia or low pH), social interaction targeting, or elimination of dormant cells. Finally, EPS matrix remodeling or the activation of dispersal mechanisms can induce biofilm dispersion. An abundance of antimicrobial strategies (conventional, current, and prospective) can be used for biofilm eradication, as summarized in Table 1.
Biofilm development and anti-biofilm strategies. The microbial biofilm cycle could be classified into 4 phases: Initial attachment, Adhesion, Maturation, and Dispersal. The biofilm inhibitory and dispersal strategies are summarized as per the stages in biofilm development. (A) The initial attachment can be disrupted by interfering with the interactions between the surface and the microorganism either by surface remodeling or physical removal of the biofilms; (B) Adhesion can be inhibited by targeting biofilm EPS and cellular division; (C) Disruption of biofilms in proliferating and maturing phase may be accomplished either by physical removal or by damaging the EPS matrix primarily by affecting the formation of pathogenic microenvironments (such as hypoxia or low pH), and quorum sensing along with the eradication of persister cells. (D) Biofilm dispersal could be achieved by remodeling the EPS matrix or accelerating the dispersal mechanisms. Reproduced with permission from (Koo et al. 2017)
Wound debridement
Debridement involves the removal of necrotic tissue and foreign objects such as biofilms from a wound to promote healing via exposure to viable underlying tissues (Madhok et al. 2013). It helps to reduce bacterial burden within the wound, control inflammation, and promote the formation of granulation tissue (Sieggreen and Maklebust 1997). Wound debridement is one of the first key steps in the removal of biofilms. In chronic wounds, the body’s natural response to necrotic tissue is slow and time consuming. Therefore, a variety of wound debridement techniques can be employed in clinical practice, including enzymatic, conservative sharp and surgical, biodebridement, and mechanical techniques (Vowden and Vowden 1999a, b). Enzymatic debridement involves the use of enzymes, such as collagenase-based dressing, and is useful during the initial stages of wound management when other techniques are not feasible (Ramundo and Gray 2008). Conservative sharp and surgical debridement, which are currently the gold standard methods, are quick and effective techniques that require a skilled practitioner but are expensive (Bekara et al. 2018). Biodebridement, which involves the use of maggots, has become increasingly popular over the last decade. Larval therapy can be highly selective and rapid but often necessitates the use of other debridement methods following the initial larval application (Gottrup and Jørgensen 2011; Opletalová et al. 2012). Mechanical (wet or dry) debridement is also used; however, it damages healthy granulation tissue, and can be time consuming and painful (McCallon et al. 2015). Various factors, including the type, size, and location of the wound; the nature and volume of the exudate; cost-effectiveness; patient tolerance; and available expertise and equipment, can influence the method of technique. Complete debridement often requires the use of more than one type of debridement. In 2006, the concept of combined debridement was introduced, which involves the use of a combination of methods (e.g., combined sharp and hydrogel debridement, combined ultrasonic and surgical debridement, and combined ultrasonic and enzymatic debridement) to take advantage of complex wounds (Jiang et al. 2009). Although useful for removing biofilms from chronic wounds, debridement techniques can result in uneven and slow healing (caused by tissue removal) of wounds through repetitive processes. Therefore, a suitable combination of debridement techniques and other antimicrobial strategies (e.g., antibiotic or bacteriophage treatments) is required to achieve better therapeutic outcomes.
Antibiotics
Antibiotics are among the most widely used conventional strategies for treating chronically infected wounds. Topical and systemic antibiotics (with broad-spectrum activity) are widely used; however, chronically infected wounds often exhibit poor response to biofilms, which can further lead to the emergence of antibiotic-resistant strains (Hernandez 2006; Lipsky and Hoey 2009). Chronic wound biofilms are antibiotic-tolerant, which is partially attributed to the biofilm construct composed of an EPS matrix that is responsible for poor antibiotic penetration and enzymatic degradation (Høiby et al. 2010; Omar et al. 2017). Furthermore, intrinsic bacterial biofilm factors such as slower growth rates, reduced metabolic factors, and the formation of highly tolerant persister cells and small colony variants contribute to the development of resistance (Stewart 2002). Additionally, environmental factors such as increased oxidative stress, pH variation, and poor oxygenation can decrease the availability, distribution, and resulting efficacy of antibiotics in chronically infected wounds (Gupta et al. 2016; Percival et al. 2014). Examples of topical antibiotic regimens for cutaneous biofilm infections include mupirocin 2% ointment, metronidazole 0.8% gel, and silver sulfadiazine 1% cream (Ciofu et al. 2017). The therapeutic efficacy of these formulations is often limited by their short residence time, uncontrolled antibiotic delivery, and minimal effects on EPS dispersal. Therefore, suitable modifications of topical antibiotic formulations are required to effectively treat biofilm-based infections. For example, controlled release of antibiotics can enhance the treatment of biofilm-based wound infections. Furthermore, combining EPS-degrading agents (e.g., EPS-degrading enzyme) (Kaplan et al. 2018) with antibiotics in a suitable formulation can enhance the anti-biofilm therapeutic efficacy. A combination of antibiotics can be used to effectively kill biofilm cells by attacking the metabolically active layers (using antibiotics, such as ciprofloxacin, tobramycin, or -lactams) and cells with low metabolic activity (using antibiotics, such as colistin) (Pamp et al. 2008). Antibiotics can also be used to prevent the recurrence of infection following the application of other physical or chemical methods for EPS degradation and removal of biofilms from the wound site. Further modifications of antibiotic formulations and delivery are required to enhance their therapeutic efficacy as anti-biofilm agents.
Modulation of pH
The pH of the wound bed plays a critical role in the healing process of infected wounds, affecting collagen formation, matrix metalloproteinase (MMP) activity, angiogenesis, and immune cell function (Percival et al. 2014). Healthy skin has a slightly acidic pH (4.0–6.0) (Jones et al. 2015) whereas chronic wounds have an alkaline pH (7.15–8.9) that is attributed partly to bacterial proliferation by-products (Jones et al. 2015). This alkaline pH affects the microbial composition (e.g., promotes anaerobic bacterial growth because of low oxygen release) and density (e.g., increasing the density of biofilms by changing bacterial growth rate) (Percival et al. 2012) in infected wounds. Therefore, pH modulation may be a promising strategy for targeting wound biofilms to promote chronic wound healing. Acid treatment is a viable approach, with citric acid (Prabhu et al. 2014), acetic acid (Madhusudhan 2016), and boric acid (Kujath and Hügelschäffer 1987) being studied for their wound pH reduction and anti-biofilm activities. Lowering the wound bed pH can inhibit bacterial proliferation and reduce the toxicity of bacterial end-products, such as ammonia (Leveen et al. 1973). Acetic acid has been effective in both in vitro and clinical settings, particularly against P. aeruginosa biofilms (Nagoba et al. 2013); however, it poses a limitation for polymicrobial infections commonly present in chronic wounds.
Surfactants
Surfactants are surface-active agents that lower the surface tension between the liquid and surface, making molecules less likely to stick together. Surfactants play an essential role in wound care by interfering with the ability of microbes to adhere to the wound surface, thus reducing the risk of infection (Percival et al. 2017). Lowering the surface tension between the liquid (used to rinse wounds) and the surface (wound bed) results in liquid infiltration into the surface for the removal of debrided cells and microbes (Percival et al. 2019). One polymeric dressing containing surfactants showed its anti-biofilm effects, which led to the US-FDA approval for the removal of necrotic tissues around wounds (Das Ghatak et al. 2018). Such surfactant-loaded polymeric dressings prevent the biofilm formation by inhibiting aggregation and EPS matrix formation in P. aeruginosa and S. aureus. Furthermore, a synergistic effect was observed for the combination of antibiotics, resulting from EPS disruption by a surfactant polymer dressing, which converted biofilms into a more planktonic-like phenotype, which could then be cleared with antibiotics (Das Ghatak et al. 2018). Although reports on the use of surfactants as anti-biofilm agents are emerging, a safe and effective dressing or formulation is still required to cover a broad spectrum of biofilm-forming microorganisms.
Antimicrobial peptides (AMPs)
Antimicrobial peptides (AMPs) are short amphiphilic peptides comprising up to 100 amino acids that are present in the first line of defense in organisms (Thapa et al. 2020a). They are part of innate immunity and exert their antibacterial effects through different mechanisms, the most common of which is the formation of pores on the bacterial wall, resulting in leakage and cell death (Lei et al. 2019). Antimicrobial peptides have been studied for their potential roles in the effective treatment of infected wounds. In addition to their antibacterial effects, they also exert immunomodulatory effects, reduce inflammatory components, and induce epithelial cell migration and angiogenesis (Fig. 3) (Thapa et al. 2020a). Although various AMPs have been tested in clinical trials, only a few received market approval owing to their proteolytic instability, pH sensitivity, and high production costs (Dijksteel et al. 2021). Several studies have demonstrated therapeutic potential of different AMPs (innate defense regulator (IDR)-1018 (Mansour et al. 2015), LL37 (Duplantier and van Hoek 2013), DRGN-1 (Chung et al. 2017), and dermaseptin peptide 2 (DMS-PS2) (Song et al. 2020) ) for treating wound biofilms. Nonetheless, their clinical application is hampered due to the lack of an effective manner to prevent their degradation and to control their release, which calls the development of suitable formulation for AMPs to achieve anti-biofilm effects at infected wounds.
A schematic representation of the potential biological effects of AMPs on wound healing. Reproduced with permission from (Thapa et al. 2020a)
Photodynamic substances
Photodynamic substances, also known as photosensitizers (PS), produce cytotoxic reactive oxygen species (ROS) upon harmless visible light irradiation at a particular wavelength, which destroys bacterial biofilms in wounds (de Melo et al. 2013). Antimicrobial photodynamic therapy (aPDT) involves two steps: (1) application of PS to a confined wound area, either locally or systemically, and (2) illumination of the wounded area with a specific wavelength of light to excite the PS and to produce ROS in the presence of ambient molecular oxygen (Hu et al. 2018). Photosensitizers can either be completely sequestered by EPS or partially penetrate the EPS to contact microbial cells (Hu et al. 2018). The excessive ROS leads to oxidative damage to multiple non-specific targets, such as lipids, amino acids, and nucleic acid bases, resulting in cell death induced by damage to microbial proteins, DNA, and membranes (Cieplik et al. 2018). Potential PS for aPDT include acridine orange, tetrapyrrole macromolecules (e.g., porphyrins, chlorins, and synthetic phthalocyanines), non-tetrapyrrole dyes, and natural compounds (e.g., rose bengal, methylene blue, and toluidine blue) (Ghorbani et al. 2018). aPDT has multiple targets by which microbial cells are efficiently killed, and the matrix structure and EPS are weakened owing to the attack of numerous biomolecules (Melo et al. 2021). Nevertheless, the presence of EPS in biofilms and the requirement of a light source to activate PS are considered as downsides of aPDT-based wound treatment. It is typically considered challenging for PS to penetrate EPS in wound biofilms. A recent study showed that a nanoemulsion containing porphyrin exerted great antimicrobial photodynamic effects with a 6-log reduction of S. aureus in an infected ulcer mouse model, demonstrating its anti-biofilm effects that overcame the microbial mechanisms against PS uptake (Buzza et al. 2022). In addition, the electric charge of PS is an important criterion in the successful aPDT. Neutral or anionic PS are effective in eradiation of gram-positive bacteria, whereas they display poor efficacies against gram-negative bacteria due to the electro-repulsive forces between the bacteria’s additional asymmetric outer membrane and neutral or anionic PS (George et al. 2009; Sperandio et al. 2013). Such disadvantages could be overcome by cationic PS or conjugation of PS to positively charged entities such as polyethyleneimine (Sperandio et al. 2013). In summary, careful evaluations of the biofilm composition, i.e., whether it is gram-positive or gram-negative, could help to identify suitable PS (cationic, neutral, or anionic), enhancing the therapeutic outcome of aPDT.
Bacteriophages
Bacteriophages are viruses that are specifically designed to infect bacteria via bacterial cell surface receptor recognition and are considered an attractive alternative to combat antimicrobial resistance (O’Flaherty et al. 2009). Bacteriophages can be found abundantly in different environments ranging from soil to the human intestine (Abedon 2009). These viruses have shown effectiveness against a variety of Gram-positive (e.g., S. aureus and Enterococcus faecium) and Gram-negative bacteria (e.g., E. coli, P. aeruginosa, Klebsiella pneumoniae, Acinetobacter baumannii, Vibrio vulnificus, Salmonella spp) (Burrowes et al. 2011). Bacteriophages can be classified as either lytic or lysogenic. Lytic bacteriophages can lyse bacteria, whereas lysogenic bacteriophages are incorporated into bacterial DNA and do not induce bacterial lysis until they are reactivated at a later time, rendering them futile in treating infections (Abedon 2015; Hanlon 2007). Bacteriophages have gained considerable attention for the treatment of biofilms due to their bacteria-lysing abilities (O’Flaherty et al. 2009). Additionally, they can enzymatically degrade the extracellular matrix of the biofilm and spread within the biofilm using endolysins and depolymerases (Tait et al. 2002; Yilmaz et al. 2013). In fact, bacteria-specific phages decrease the areas of bacterial colonization, such as biofilms (Smith and Huggins 1982). The phage titer is proportional to the bactericidal effects and inhibition of the re-emergence of the pathogen (Sabouri Ghannad and Mohammadi 2012). Therefore, phage-mediated bactericidal effects suggest that they can manage wound colonization for safe and effective treatment (Hughes et al. 1998). Several preclinical animal studies have supported the treatment of clinical biofilm infections using bacteriophage therapy, wherein local phage treatment resulted in biofilm reduction (Mendes et al. 2013; Milho et al. 2019; Oliveira et al. 2018; Seth et al. 2013). However, the main concern regarding bacterial lysis by bacteriophages is the release of endotoxins into the wound, which can result in nonspecific and unrestrained activation of innate immunity and inflammatory responses, ultimately delaying wound healing. Other potential disadvantages of bacteriophage therapy include the failure of bacteriophage therapy owing to restrictive specificity, integration of phage DNA into the bacterial genome, and the development of bacterial resistance because of the alteration of bacterial cell surface receptors (Joerger 2003; Sabouri Ghannad and Mohammadi 2012). These disadvantages can be circumvented using a cocktail containing several phages in conjunction with a traditional antibiotic (Comeau et al. 2007). Local delivery of bacteriophages to biofilms in infected wounds is possible using different biopolymers, synthetic polymers, liposomal encapsulation, and inorganic materials (Rotman et al. 2020). Bacteriophage-loaded hydrogels are a potential formulation for effective local delivery to wounds for infection control and healing (Chang et al. 2021; Kim et al. 2021). A recent study reported the development of bacteriophage-loaded nanofibers for the wound treatment associated with P. aeruginosa and S. aureus (Kielholz et al. 2023). The researchers prepared bacteriophage-loaded nanofiber by electrospinning and showed its antimicrobial effects in the treatment of infected wounds.
Quorum sensing inhibitors
Quorum sensing is a communication system that allows neighboring bacterial cells to receive and send signal molecules (i.e., autoinducers) in a density-dependent manner (Brackman and Coenye 2015). This system plays a pivotal role in biofilm regulation via inter- and intra-species bacterial communication and genetic synchrony (Hentzer et al. 2003b). Therefore, the inhibition of quorum sensing has emerged as a significant innovation in the area of biofilm management (Hentzer et al. 2003a). Such inhibition can be achieved via the degradation of signaling molecules, inhibition of autoinducer synthesis, interference with signal binding, or inhibition of signal transduction cascades, resulting in dysregulated biofilm signaling and subsequent biofilm inhibition or dispersal (Brackman and Coenye 2015; Jiang et al. 2019). Combining these approaches may be necessary to overcome redundancy in bacterial communication and eradicate persisters (Hirakawa and Tomita 2013). Several promising candidates (e.g., furanone, C30, and HT61) have been identified as quorum-sensing inhibitors (Al-Bataineh et al. 2009; Baveja et al. 2004; Pan and Ren 2013). A quorum inhibitor, FS3, showed good efficacy and synergy when combined with daptomycin (Cirioni et al. 2013). Quorum-sensing inhibitors are effective in managing bacterial biofilms in wounds. However, their efficacy and safety in vivo must be substantiated. Furthermore, increasing evidence suggests the development of a resistant phenotype was initiated by quorum quenching (Gerdt and Blackwell 2014; Scutera et al. 2014), although the mechanism remains unclear. Hence, an appropriate quorum-sensing inhibitor should only be determined after identifying the bacterial species in the wound biofilm. Additionally, other agents, such as antibiotics, should be combined with quorum-sensing inhibitors to enhance the anti-biofilm effectiveness.
Nanoparticles
Emerging advances in nanoparticle-based therapies have provided new and promising opportunities for effectively treating wound infections associated with biofilms. Nanoparticles offer advantages such as cellular penetration, targeted delivery following surface modification, and localized delivery to infected wounds (Andrade et al. 2013). Nanoparticles exhibiting specific physical and chemical properties against biofilm wound infections have also been developed (Kim 2016). Different nanoparticles, such as organic (e.g., liposomes and polymeric nanoparticles), inorganic (e.g., graphene, carbon nanotubes, and mesoporous silica nanoparticles), and metal (e.g., silver and gold nanoparticles), can be used for either the delivery of anti-biofilm agents or for exhibiting intrinsic anti-biofilm activity (Darvishi et al. 2022). A schematic representation of the mechanisms of the different nanoparticle-based approaches for anti-biofilm activity is presented in Fig. 4. Further details on the design, synthesis, and mechanism of anti-biofilm activity can be obtained from recently published review articles (Darvishi et al. 2022; Dizaj et al. 2014). Despite the encouraging prospects for nanoparticle-based anti-biofilm treatment of infected wounds, only a few marketed nanoparticle-based drug delivery systems are available (Duncan and Gaspar 2011). It could be attributed to the complexity in characterization and analysis of nanoparticles. In addition, the limited target selectivity and instability of nanoparticle-based preparations could hinder the clinical successes of nanoparticle-based anti-biofilm therapeutics (Jones and Grainger 2009). Such unmet needs pose an opportunity to develop a new anti-biofilm therapeutic using nanotechnology.
A schematic representation of the mechanisms of action of various nanoparticle-based treatments for biofilm infections. Reproduced with permission from (Darvishi et al. 2022)
Hybrid hydrogels
Hydrogels are hydrophilic polymer networks that are capable of absorbing, swelling, and retaining large amounts of aqueous fluid (Peppas et al. 2000). They are well-suited for biological applications because of their high water content and permeability, tunable viscoelasticity, and structural similarity to the extracellular matrix (Wichterle and LÍM 1960). Hybrid hydrogels are chemically, morphologically, and functionally distinct building blocks composed of biologically active proteins, peptides, or nano-/microstructures interconnected by chemical or physical means (Palmese et al. 2019). These hybrid hydrogels have potential applications in the successful treatment of biofilms in wound infections. Gelatin hydrogels composed of genipin-cross-linked AgNPs exhibited effective antibacterial and anti-biofilm effects against S. aureus, Bacillus subtilis, P. aeruginosa, and E. coli (Katas et al. 2021). Melanin-loaded hybrid hydrogel was developed as wound patches (Cao et al. 2023). It exhibited photothermal antibacterial and antioxidant properties and provided a controlled release of proangiogenic-asiatic acid via liquid transformation of the hydrogel. We also developed a hybrid hydrogel composed of Pluronic F127, liposomes, and antimicrobial peptides exhibiting potent antibacterial and anti-biofilm effects against methicillin-resistant S. aureus wound infections (Thapa et al. 2021). The multiple antibacterial and anti-biofilm mechanisms of the hybrid hydrogel components effectively managed wound infections. However, potential toxicity and prevention of resistance development by the infecting bacteria should be taken into consideration.
Natural deep eutectic solvents (NADES)
In addition to water and lipids, natural deep eutectic solvents (NADES) are considered a third class of liquids in organisms and are composed of natural compounds such as amino acids, organic acids, sugars, tertiary amines, and polyols (Grønlien et al. 2020). They are a novel class of eutectics with unique potential as solubilizers of water-insoluble compounds, such as curcumin, for antimicrobial photodynamic therapy against bacteria (e.g., E. coli) (Wikene et al. 2015). Although this prospective strategy has potential as an antimicrobial agent in combination with a suitable photosensitizer for photodynamic therapy or as a carrier of an antimicrobial agent, it has some disadvantages, including the potential toxicity of acid-containing NADES (Wikene et al. 2017). Further research using NADES is required to explore their potential in prospective anti-biofilm therapy for infected wounds.
CRISPR interference (CRISPRi)
CRISPR interference (CRISPRi) is a new and prospective approach for quorum sensing inhibition in biofilm-forming bacteria. Several genes (e.g., luxS, fimH, mqsR, csrA, qseB, and motA) are involved in the quorum sensing mechanisms of E. coli (Zuberi et al. 2017a). CRISPRi is a gene perturbation technique used for inhibiting genes involved in quorum sensing (Zuberi et al. 2017b). This method reversibly and accurately alters gene expression by hindering transcriptional machinery through the lodging of inactive or dead Cas9 at a specific position (Qi et al. 2013). Although potent in vitro, the CRISPRi method is difficult to translate in vivo to treat wound infections. Further developments and rigorous research are warranted to explore the potential of CRISPRi in the anti-biofilm therapy of infected wounds.
Conclusions and future perspective
The treatment of topical biofilm-based wound infections is a major concern, as millions of people suffer from conditions such as diabetes that can lead to chronic wounds. Various anti-biofilm treatment options, including conventional and current strategies, have been utilized. Conventional strategies, such as wound debridement, antibiotics, pH modulation, and surfactants, are used as anti-biofilm measures. However, their use is limited owing to complications such as bacterial regrowth, limited antibiotic access to bacteria due to EPS, difficulty in pH alteration, and the development of resistant bacteria. Therefore, a combination of different strategies can be useful in synergistically combating the multiple mechanisms of microbial and biofilm wound infections for effective therapy. Furthermore, preclinical studies may hold interspecies differences likely to complicate the precise evaluation of antimicrobial strategies and their therapeutic effects, which requires more rigorous studies in the relevant animal models prior to clinical trials.
Current anti-biofilm treatment options include antimicrobial peptides, photodynamic substances, bacteriophages, quorum-sensing inhibitors, nanoparticles, and hybrid hydrogels. Advancements in treatment modalities, based on intrinsic antimicrobial activity, light-induced ROS generation, controlled release, penetration of anti-biofilm agents into the EPS, and the combination of these anti-biofilm mechanisms within a single formulation, could enhance the potency of these current strategies in treating wound infections. Although promising, the development of resistance is still prevalent, limiting the effective treatment of chronic wounds. Furthermore, the commercialization of such anti-biofilm treatments is difficult owing to the complexity of treatment modalities, limited stability and modest efficacy, and cost. Rigorous characterization of the modalities, development of stable formulations, and innovative manufacturing process would aid in the clinical translation of new anti-biofilm treatments.
Nonetheless, several prospective strategies have emerged for the eradication of biofilm-forming bacteria at wounded sites. Especially, natural anti-biofilm strategies draw attentions due to their potential resistance against biofilm formation. It includes NADES and CRISPRi technologies. NADES, a natural substance, can act not only as an intrinsic antimicrobial agent but also as a carrier of PS, making itself suitable for combinational anti-biofilm therapy. CRISPRi technology could treat biofilm-forming bacteria selectively. A combination of CRISPRi with appropriate antibiotics could kill the bacteria more effectively at the wounded tissues. Further research on the utilization of NADES and CRISPRi will warrant their potentials for anti-biofilm therapy.
Future efforts for novel treatments for infected wounds require a focus on criteria such as (1) the development of new drugs and therapies, (2) prevention of bacterial resistance, and (3) protection of the natural host microbiome. Discovery of combinations of conventional, current, and prospective therapies will aid in the development of potent anti-biofilm therapies for wound infections. Although evolutionary mechanisms in humans and bacteria may lead to new resistance mechanisms, continuing research will help resolve it.
References
Abedon ST (2009) Phage evolution and ecology. Adv Appl Microbiol 67:1–45
Abedon ST (2015) Ecology of anti-biofilm agents II: bacteriophage exploitation and biocontrol of biofilm bacteria. Pharmaceuticals 8:559–589
Agrawal KS, Sarda AV, Shrotriya R, Bachhav M, Puri V, Nataraj G (2017) Acetic acid dressings: finding the holy grail for infected wound management. Indian J Plast Surg 50:273–280
Al-Bataineh SA, Luginbuehl R, Textor M, Yan M (2009) Covalent immobilization of antibacterial furanones via photochemical activation of perfluorophenylazide. Langmuir 25:7432–7437
Andrade F, Rafael D, Videira M, Ferreira D, Sosnik A, Sarmento B (2013) Nanotechnology and pulmonary delivery to overcome resistance in infectious diseases. Adv Drug Deliv Rev 65:1816–1827
Bayramov DF, Neff JA (2017) Beyond conventional antibiotics—new directions for combination products to combat biofilm. Adv Drug Deliv Rev 112:48–60
Baveja JK, Li G, Nordon RE, Hume EBH, Kumar N, Willcox MDP, Poole-Warren LA (2004) Biological performance of a novel synthetic furanone-based antimicrobial. Biomaterials 25:5013–5021
Benjamin KC, Stephen TA (2015) Bacteriophages and their enzymes in biofilm control. Curr Pharm Des 21:85–99
Bekara F, Vitse J, Fluieraru S, Masson R, Runz AD, Georgescu V, Bressy G, Labbé JL, Chaput B, Herlin C (2018) New techniques for wound management: a systematic review of their role in the management of chronic wounds. Arch Plast Surg 45:102–110
Bowler PG, Duerden BI, Armstrong DG (2001) Wound microbiology and associated approaches to wound management. Clin Microbiol Rev 14:244–269
Brackman G, Coenye T (2015) Quorum sensing inhibitors as anti-biofilm agents. Curr Pharm Des 21:5–11
Brooks BD, Brooks AE (2014) Therapeutic strategies to combat antibiotic resistance. Adv Drug Deliv Rev 78:14–27
Brandenburg KS, Calderon DF, Kierski PR, Brown AL, Shah NM, Abbott NL, Schurr MJ, Murphy CJ, McAnulty JF, Czuprynski CJ (2015) Inhibition of Pseudomonas aeruginosa biofilm formation on wound dressings. Wound Repair Regen 23:842–854
Burrowes B, Harper DR, Anderson J, McConville M, Enright MC (2011) Bacteriophage therapy: potential uses in the control of antibiotic-resistant pathogens. Expert Rev Anti Infect Ther 9:775–785
Buzza HH, Alves F, Tome AJB, Chen J, Kassab G, Bu J, Bagnato VS, Zheng G, Kurachi C (2022) Porphyrin nanoemulsion for antimicrobial photodynamic therapy: effective delivery to inactivate biofilm-related infections. Proc Natl Acad Sci USA 119(46):e2216239119
Cao X, Sun L, Xu D, Miao S, Li N, Zhao Y (2023) Melanin-integrated structural color hybrid hydrogels for wound healing. Adv Sci (Weinh). https://doi.org/10.1002/advs.202300902
Chaney SB, Ganesh K, Mathew-Steiner S, Stromberg P, Roy S, Sen CK, Wozniak DJ (2017) Histopathological comparisons of Staphylococcus aureus and Pseudomonas aeruginosa experimental infected porcine burn wounds. Wound Repair Regen 25:541–549
Chang RYK, Morales S, Okamoto Y, Chan H-K (2020) Topical application of bacteriophages for treatment of wound infections. Transl Res 220:153–166
Chang RYK, Okamoto Y, Morales S, Kutter E, Chan H-K (2021) Hydrogel formulations containing non-ionic polymers for topical delivery of bacteriophages. Int J Pharm 605:120850
Chung EMC, Dean SN, Propst CN, Bishop BM, van Hoek ML (2017) Komodo dragon-inspired synthetic peptide DRGN-1 promotes wound-healing of a mixed-biofilm infected wound. NPJ Biofilms Microbiomes 3:017–0017
Cieplik F, Deng D, Crielaard W, Buchalla W, Hellwig E, Al-Ahmad A, Maisch T (2018) Antimicrobial photodynamic therapy—what we know and what we don’t. Crit Rev in Microbiol 44:571–589
Ciofu O, Rojo-Molinero E, Macià MD, Oliver A (2017) Antibiotic treatment of biofilm infections. APMIS 125:304–319
Cirioni O, Mocchegiani F, Cacciatore I, Vecchiet J, Silvestri C, Baldassarre L, Ucciferri C, Orsetti E, Castelli P, Provinciali M, Vivarelli M, Fornasari E, Giacometti A (2013) Quorum sensing inhibitor FS3-coated vascular graft enhances daptomycin efficacy in a rat model of staphylococcal infection. Peptides 40:77–81
Comeau AM, Tétart F, Trojet SN, Prère M-F, Krisch HM (2007) Phage-antibiotic synergy (PAS): beta-lactam and quinolone antibiotics stimulate virulent phage growth. PLoS ONE 2:e799–e799
Cook PP, Siraj DS (2017) Chapter 109—bacterial arthritis. In: Firestein GS, Budd RC, Gabriel SE, McInnes IB, O’Dell JR (eds) Kelley and Firestein’s textbook of rheumatology, 10th edn. Elsevier, Amsterdam, pp 1876–1890
Darvishi S, Tavakoli S, Kharaziha M, Girault HH, Kaminski CF, Mela I (2022) Advances in the sensing and treatment of wound biofilms. Angew Chem Int Ed 61:e202112218
Das Ghatak P, Mathew-Steiner SS, Pandey P, Roy S, Sen CK (2018) A surfactant polymer dressing potentiates antimicrobial efficacy in biofilm disruption. Sci Rep 8:873
de Melo WCMA, Avci P, de Oliveira MN, Gupta A, Vecchio D, Sadasivam M, Chandran R, Huang Y-Y, Yin R, Perussi LR, Tegos GP, Perussi JR, Dai T, Hamblin MR (2013) Photodynamic inactivation of biofilm: taking a lightly colored approach to stubborn infection. Expert Rev Anti Infect Ther 11:669–693
de Melo MA, de Cassia W, Celiešiūtė-Germanienė R, Šimonis P, Stirkė A (2021) Antimicrobial photodynamic therapy (aPDT) for biofilm treatments. Possible synergy between aPDT and pulsed electric fields. Virulence 12:2247–2272
Demidova-Rice TN, Hamblin MR, Herman IM (2012) Acute and impaired wound healing: pathophysiology and current methods for drug delivery, part 1: normal and chronic wounds: biology, causes, and approaches to care. Adv Skin Wound Care 25:304–314
Desjardins H, Guo L (2018) An overlooked but effective wound care methodology: hydromechanical therapy revisited. Plast Reconstr Surg—Global Open 6:e1883
Dijksteel GS, Ulrich MMW, Middelkoop E, Boekema BKHL (2021) Review: lessons learned from clinical trials using antimicrobial peptides (AMPs). Front Microbiol 12:616979
Dizaj SM, Lotfipour F, Barzegar-Jalali M, Zarrintan MH, Adibkia K (2014) Antimicrobial activity of the metals and metal oxide nanoparticles. Mater Sci Eng C Mater Biol Appl 44:278–284
Duncan R, Gaspar R (2011) Nanomedicine(s) under the microscope. Mol Pharm 8:2101–2141
Duplantier AJ, van Hoek ML (2013) The human cathelicidin antimicrobial peptide LL-37 as a potential treatment for polymicrobial infected wounds. Front Immunol 4:143–143
Eming SA, Martin P, Tomic-Canic M (2014) Wound repair and regeneration: mechanisms, signaling, and translation. Sci Transl Med 6(265):265sr6
Finnegan S, Percival SL (2015) Clinical and antibiofilm efficacy of antimicrobial hydrogels. Adv Wound Care (New Rochelle) 4:398–406
Flemming H-C, Wingender J, Szewzyk U, Steinberg P, Rice SA, Kjelleberg S (2016) Biofilms: an emergent form of bacterial life. Nat Rev Microbiol 14:563–575
George S, Hamblin MR, Kishen A (2009) Uptake pathways of anionic and cationic photosensitizers into bacteria. Photochem Photobiol Sci 8:788–795
Gerdt JP, Blackwell HE (2014) Competition studies confirm two major barriers that can preclude the spread of resistance to quorum-sensing inhibitors in bacteria. ACS Chem Biol 9:2291–2299
Ghorbani J, Rahban D, Aghamiri S, Teymouri A, Bahador A (2018) Photosensitizers in antibacterial photodynamic therapy: an overview. Laser Ther 27:293–302
Gilles B, Tom C (2015) Quorum sensing inhibitors as anti-biofilm agents. Curr Pharm Des 21:5–11
Gottrup F, Jørgensen B (2011) Maggot debridement: an alternative method for debridement. Eplasty 11:e33–e33
Grønlien KG, Pedersen ME, Tønnesen HH (2020) A natural deep eutectic solvent (NADES) as potential excipient in collagen-based products. Int J Biol Macromol 156:394–402
Gupta S, Laskar N, Kadouri DE (2016) Evaluating the effect of oxygen concentrations on antibiotic sensitivity, growth, and biofilm formation of human pathogens. Microbiol Insights 9:37–46
Hanlon GW (2007) Bacteriophages: an appraisal of their role in the treatment of bacterial infections. Int J Antimicrob Agents 30:118–128
Hentzer M, Eberl L, Nielsen J, Givskov M (2003a) Quorum sensing: a novel target for the treatment of biofilm infections. BioDrugs 17:241–250
Hentzer M, Wu H, Andersen JB, Riedel K, Rasmussen TB, Bagge N, Kumar N, Schembri MA, Song Z, Kristoffersen P, Manefield M, Costerton JW, Molin S, Eberl L, Steinberg P, Kjelleberg S, Høiby N, Givskov M (2003b) Attenuation of Pseudomonas aeruginosa virulence by quorum sensing inhibitors. EMBO J 22:3803–3815
Hernandez R (2006) The use of systemic antibiotics in the treatment of chronic wounds. Dermatol Ther 19:326–337
Hirakawa H, Tomita H (2013) Interference of bacterial cell-to-cell communication: a new concept of antimicrobial chemotherapy breaks antibiotic resistance. Front Microbiol 4:114
Høiby N, Bjarnsholt T, Givskov M, Molin S, Ciofu O (2010) Antibiotic resistance of bacterial biofilms. Int J Antimicrob Agents 35:322–332
Hu MS, Maan ZN, Wu J-C, Rennert RC, Hong WX, Lai TS, Cheung ATM, Walmsley GG, Chung MT, McArdle A, Longaker MT, Lorenz HP (2014) Tissue engineering and regenerative repair in wound healing. Ann Biomed Eng 42:1494–1507
Hu X, Huang Y-Y, Wang Y, Wang X, Hamblin MR (2018) Antimicrobial photodynamic therapy to control clinically relevant biofilm infections. Front Microbiol 9:1299–1299
Hughes KA, Sutherland IW, Jones MV (1998) Biofilm susceptibility to bacteriophage attack: the role of phage-borne polysaccharide depolymerase. Microbiology 144:3039–3047
Jeffery Marano R, Jane Wallace H, Wijeratne D, William Fear M, San Wong H, O’Handley R (2015) Secreted biofilm factors adversely affect cellular wound healing responses in vitro. Sci Rep 5:13296–13296
Jiang P, Zhang T, Feng Y, Yang R, Liang N (2009) Determination of plastic properties by instrumented spherical indentation: expanding cavity model and similarity solution approach. J Mater Res 24:1045–1053
Jiang Q, Chen J, Yang C, Yin Y, Yao K (2019) Quorum sensing: a prospective therapeutic target for bacterial diseases. Biomed Res Int 4:2015978
Joerger RD (2003) Alternatives to antibiotics: bacteriocins, antimicrobial peptides and bacteriophages. Poult Sci 82:640–647
Jones CF, Grainger DW (2009) In vitro assessments of nanomaterial toxicity. Adv Drug Deliv Rev 61:438–456
Jones EM, Cochrane CA, Percival SL (2015) The Effect of pH on the extracellular matrix and biofilms. Adv Wound Care (New Rochelle) 4:431–439
Kaplan JB, Mlynek KD, Hettiarachchi H, Alamneh YA, Biggemann L, Zurawski DV, Black CC, Bane CE, Kim RK, Granick MS (2018) Extracellular polymeric substance (EPS)-degrading enzymes reduce staphylococcal surface attachment and biocide resistance on pig skin in vivo. PLoS ONE 13:e0205526
Karna SLR, D’Arpa P, Chen T, Qian L-W, Fourcaudot AB, Yamane K, Chen P, Abercrombie JJ, You T, Leung KP (2016) RNA-seq transcriptomic responses of full-thickness dermal excision wounds to Pseudomonas aeruginosa acute and biofilm infection. PLoS ONE 11:e0165312
Katas H, Mohd Akhmar MA, Suleman Ismail Abdalla S (2021) Biosynthesized silver nanoparticles loaded in gelatine hydrogel for a natural antibacterial and anti-biofilm wound dressing. J Bioact Compat Polym 36:111–123
Kielholz T, Rohde F, Jung N, Windbergs M (2023) Bacteriophage-loaded functional nanofibers for treatment of P. aeruginosa and S. aureus wound infections. Sci Rep 13:8330
Kim M-H (2016) Nanoparticle-based therapies for wound biofilm infection: Opportunities and challenges. IEEE Trans Nanobiosci 15:294–304
Kim HY, Chang RYK, Morales S, Chan H-K (2021) Bacteriophage-delivering hydrogels: current progress in combating antibiotic resistant bacterial infection. Antibiot (Basel) 10:130
Koo H, Allan RN, Howlin RP, Stoodley P, Hall-Stoodley L (2017) Targeting microbial biofilms: current and prospective therapeutic strategies. Nat Rev Microbiol 15:740–755
Kujath P, Hügelschäffer C (1987) Pseudomonas aeruginosa: pathogenicity, prevention and therapeutic approaches. Zentralbl Chir 112:558–563
Kujath P, Kujath C (2010) Complicated skin, skin structure and soft tissue infections: are we threatened by multi-resistant pathogens? Eur J Med Res 15:544–553
Lei J, Sun L, Huang S, Zhu C, Li P, He J, Mackey V, Coy DH, He Q (2019) The antimicrobial peptides and their potential clinical applications. Am J Transl Res 11:3919–3931
Leveen HH, Falk G, Borek B, Diaz C, Lynfield Y, Wynkoop BJ, Mabunda GA, Rubricius JL, Christoudias GC (1973) Chemical acidification of wounds. An adjuvant to healing and the unfavorable action of alkalinity and ammonia. Ann Surg 178:745–753
Lipsky BA, Hoey C (2009) Topical antimicrobial therapy for treating chronic wounds. Clin Infect Dis 49:1541–1549
Liu W-L, Jiang Y-L, Wang Y-Q, Li Y-X, Liu Y-X (2017) Combined debridement in chronic wounds: a literature review. Chin Nurs Res 4:5–8
Madhok BM, Vowden K, Vowden P (2013) New techniques for wound debridement. Int Wound J 10:247–251
Madhusudhan V (2016) Efficacy of 1% acetic acid in the treatment of chronic wounds infected with Pseudomonas aeruginosa: prospective randomised controlled clinical trial. Int Wound J 13:1129–1136
Mansour SC, de la Fuente-Núñez C, Hancock REW (2015) Peptide IDR-1018: modulating the immune system and targeting bacterial biofilms to treat antibiotic-resistant bacterial infections. J Pept Sci 21:323–329
McCallon SK, Weir D, Lantis JC (2015) Optimizing wound bed preparation with collagenase enzymatic debridement. J Am Coll Clin Wound Spec 6:14–23
Mendes JJ, Leandro C, Corte-Real S, Barbosa R, Cavaco-Silva P, Melo-Cristino J, Górski A, Garcia M (2013) Wound healing potential of topical bacteriophage therapy on diabetic cutaneous wounds. Wound Repair Regen 21:595–603
Milho C, Andrade M, Vilas Boas D, Alves D, Sillankorva S (2019) Antimicrobial assessment of phage therapy using a porcine model of biofilm infection. Int J Pharm 557:112–123
Mustoe T (2004) Understanding chronic wounds: a unifying hypothesis on their pathogenesis and implications for therapy. Am J Surg 187:S65–S70
Nagoba BS, Selkar SP, Wadher BJ, Gandhi RC (2013) Acetic acid treatment of pseudomonal wound infections—a review. J Infect Public Health 6:410–415
O’Flaherty S, Ross RP, Coffey A (2009) Bacteriophage and their lysins for elimination of infectious bacteria. FEMS Microbiol Rev 33:801–819
Olivares E, Badel-Berchoux S, Provot C, Prévost G, Bernardi T, Jehl F (2020) Clinical impact of antibiotics for the treatment of Pseudomonas aeruginosa biofilm infections. Front Microbiol 10:2894
Oliveira A, Sousa JC, Silva AC, Melo LDR, Sillankorva S (2018) Chestnut honey and bacteriophage application to control Pseudomonas aeruginosa and Escherichia coli biofilms: evaluation in an ex vivo wound model. Front Microbiol 9:1725
Omar A, Wright JB, Schultz G, Burrell R, Nadworny P (2017) Microbial biofilms and chronic wounds. Microorganisms 5:9
Opletalová K, Blaizot X, Mourgeon B, Chêne Y, Creveuil C, Combemale P, Laplaud A-L, Sohyer-Lebreuilly I, Dompmartin A (2012) Maggot therapy for wound debridement: a randomized multicenter trial. Arch Dermatol 148:432–438
Palmese LL, Thapa RK, Sullivan MO, Kiick KL (2019) Hybrid hydrogels for biomedical applications. Curr Opin Chem Eng 24:143–157
Pamp SJ, Gjermansen M, Johansen HK, Tolker-Nielsen T (2008) Tolerance to the antimicrobial peptide colistin in Pseudomonas aeruginosa biofilms is linked to metabolically active cells, and depends on the pmr and mexAB-oprM genes. Mol Microbiol 68:223–240
Pan J, Ren D (2013) Structural effects on persister control by brominated furanones. Bioorg Med Chem Lett 23:6559–6562
Pastar I, Nusbaum AG, Gil J, Patel SB, Chen J, Valdes J, Stojadinovic O, Plano LR, Tomic-Canic M, Davis SC (2013) Interactions of methicillin resistant Staphylococcus aureus USA300 and Pseudomonas aeruginosa in polymicrobial wound infection. PLoS ONE 8:e56846
Peppas NA, Bures P, Leobandung W, Ichikawa H (2000) Hydrogels in pharmaceutical formulations. Eur J Pharm Biopharm 50:27–46
Percival SL, Hill KE, Williams DW, Hooper SJ, Thomas DW, Costerton JW (2012) A review of the scientific evidence for biofilms in wounds. Wound Repair Regen 20:647–657
Percival SL, McCarty SM, Lipsky B (2015) Biofilms and wounds: an overview of the evidence. Adv Wound Care (New Rochelle) 4:373–381
Percival SL, McCarty S, Hunt JA, Woods EJ (2014) The effects of pH on wound healing, biofilms, and antimicrobial efficacy. Wound Repair Regen 22:174–186
Percival SL, Mayer D, Kirsner RS, Schultz G, Weir D, Roy S, Alavi A, Romanelli M (2019) Surfactants: role in biofilm management and cellular behaviour. Int Wound J 16:753–760
Percival SL, Mayer D, Malone M, Swanson T, Gibson D, Schultz G (2017) Surfactants and their role in wound cleansing and biofilm management. J Wound Care 26:680–690
Peters BM, Jabra-Rizk MA, O’May GA, Costerton JW, Shirtliff ME (2012) Polymicrobial interactions: impact on pathogenesis and human disease. Clin Microbiol Rev 25:193–213
Pletzer D, Coleman SR, Hancock REW (2016) Anti-biofilm peptides as a new weapon in antimicrobial warfare. Curr Opin Microbiol 33:35–40
Prabhu V, Prasadi S, Pawar V, Shivani A, Gore A (2014) Does wound pH modulation with 3% citric acid solution dressing help in wound healing: a pilot study. Saudi Surg J 2:38–46
Qayyum S, Khan AU (2016) Nanoparticles vs. biofilms: a battle against another paradigm of antibiotic resistance. MedChemComm 7:1479–1498
Qi LS, Larson MH, Gilbert LA, Doudna JA, Weissman JS, Arkin AP, Lim WA (2013) Repurposing CRISPR as an RNA-guided platform for sequence-specific control of gene expression. Cell 152:1173–1183
Rajpaul K (2015) Biofilm in wound care. Br J Community Nurs 20:S6–S11
Ramasamy M, Lee J (2016) Recent nanotechnology approaches for prevention and treatment of biofilm-associated infections on medical devices. Biomed Res Int 2016:1851242
Ramundo J, Gray M (2008) Enzymatic wound debridement. J Wound Ostomy Cont Nurs 35:273–280
Rémy B, Mion S, Plener L, Elias M, Chabrière E, Daudé D (2018) Interference in bacterial quorum sensing: a biopharmaceutical perspective. Front Pharmacol 9:203
Rotman SG, Sumrall E, Ziadlou R, Grijpma DW, Richards RG, Eglin D, Moriarty TF (2020) Local bacteriophage delivery for treatment and prevention of bacterial infections. Front Microbiol 11:538060
Ruffin M, Brochiero E (2019) Repair process impairment by Pseudomonas aeruginosa in epithelial tissues: major features and potential therapeutic avenues. Front Cell Infect Microbiol 9:182
Sabouri Ghannad M, Mohammadi A (2012) Bacteriophage: time to re-evaluate the potential of phage therapy as a promising agent to control multidrug-resistant bacteria. Iran J Basic Med Sci 15:693–701
Scutera S, Zucca M, Savoia D (2014) Novel approaches for the design and discovery of quorum-sensing inhibitors. Expert Opin Drug Discov 9:353–366
Seth AK, Geringer MR, Nguyen KT, Agnew SP, Dumanian Z, Galiano RD, Leung KP, Mustoe TA, Hong SJ (2013) Bacteriophage therapy for Staphylococcus aureus biofilm-infected wounds: a new approach to chronic wound care. Plast Reconstr Surg 131:225–234
Sharma D, Misba L, Khan AU (2019) Antibiotics versus biofilm: an emerging battleground in microbial communities. Antimicrob Resist Infect Control 8:76
Sieggreen MY, Maklebust J (1997) Debridement: choices and challenges. Adv Wound Care 10:32–37
Silva LPd, Reis RL, Correlo VM, Marques AP (2019) Hydrogel-based strategies to advance therapies for chronic skin wounds. Annu Rev Biomed Eng 21:145–169
Smith HW, Huggins MB (1982) Successful treatment of experimental Escherichia coli infections in mice using phage: its general superiority over antibiotics. J Gen Microbiol 128:307–318
Song X, Pan H, Wang H, Liao X, Sun D, Xu K, Chen T, Zhang X, Wu M, Wu D, Gao Y (2020) Identification of new dermaseptins with self-assembly tendency: membrane disruption, biofilm eradication, and infected wound healing efficacy. Acta Biomater 109:208–219
Sperandio FF, Huang Y-Y, Hamblin MR (2013) Antimicrobial photodynamic therapy to kill gram-negative bacteria. Recent Pat Antiinfect Drug Discov 8:108–120
Stewart PS (2002) Mechanisms of antibiotic resistance in bacterial biofilms. Int J Med Microbiol 292:107–113
Tait K, Skillman LC, Sutherland IW (2002) The efficacy of bacteriophage as a method of biofilm eradication. Biofouling 18:305–311
Thapa RK, Diep DB, Tønnesen HH (2020a) Topical antimicrobial peptide formulations for wound healing: current developments and future prospects. Acta Biomater 103:52–67
Thapa RK, Kiick KL, Sullivan MO (2020b) Encapsulation of collagen mimetic peptide-tethered vancomycin liposomes in collagen-based scaffolds for infection control in wounds. Acta Biomater 103:115–128
Thapa RK, Winther-Larsen HC, Ovchinnikov K, Carlsen H, Diep DB, Tønnesen HH (2021) Hybrid hydrogels for bacteriocin delivery to infected wounds. Eur J Pharm Sci 166:105990
Vowden KR, Vowden P (1999a) a0 wound debridement, part 1: non-sharp techniques. J Wound Care 8:237–240
Vowden KR, Vowden P (1999b) Wound debridement, part 2: sharp techniques. J Wound Care 8:291–294
Wichterle O, LÍM D (1960) Hydrophilic gels for biological use. Nature 185:117–118
Wikene KO, Bruzell E, Tønnesen HH (2015) Characterization and antimicrobial phototoxicity of curcumin dissolved in natural deep eutectic solvents. Eur J Pharm Sci 80:26–32
Wikene KO, Rukke HV, Bruzell E, Tønnesen HH (2017) Investigation of the antimicrobial effect of natural deep eutectic solvents (NADES) as solvents in antimicrobial photodynamic therapy. J Photochem Photobiol B Biol 171:27–33
Wu Y-K, Cheng N-C, Cheng C-M (2019) Biofilms in chronic wounds: pathogenesis and diagnosis. Trends Biotechnol 37:505–517
Yang Q, Larose C, Della Porta AC, Schultz GS, Gibson DJ (2017) A surfactant-based wound dressing can reduce bacterial biofilms in a porcine skin explant model. Int Wound J 14:408–413
Yilmaz C, Colak M, Yilmaz BC, Ersoz G, Kutateladze M, Gozlugol M (2013) Bacteriophage therapy in implant-related infections: an experimental study. J Bone Joint Surg Am 95:117–125
Yin R, Dai T, Avci P, Jorge AES, de Melo WCMA, Vecchio D, Huang Y-Y, Gupta A, Hamblin MR (2013) Light based anti-infectives: ultraviolet C irradiation, photodynamic therapy, blue light, and beyond. Curr Opin Pharmacol 13:731–762
Zazo H, Colino CI, Lanao JM (2016) Current applications of nanoparticles in infectious diseases. J Control Release 224:86–102
Zhao G, Hochwalt PC, Usui ML, Underwood RA, Singh PK, James GA, Stewart PS, Fleckman P, Olerud JE (2010) Delayed wound healing in diabetic (db/db) mice with Pseudomonas aeruginosa biofilm challenge: a model for the study of chronic wounds. Wound Repair Regen 18:467–477
Zuberi A, Ahmad N, Khan AU (2017a) CRISPRi induced suppression of fimbriae gene (fimH) of a uropathogenic Escherichia coli: an approach to inhibit microbial biofilms. Front Immunol 8:1552
Zuberi A, Misba L, Khan AU (2017b) CRISPR interference (CRISPRi) inhibition of luxS gene expression in E. coli: an approach to inhibit biofilm. Front Cell Infect Microbiol 7:214
Acknowledgements
This work was supported by the 2023 Yeungnam University Research Grant.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors (Raj Kumar Thapa, Jong Oh Kim, and Jeonghwan Kim) declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human and animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Thapa, R.K., Kim, J.O. & Kim, J. Antimicrobial strategies for topical biofilm-based wound infections: past, present, and future. J. Pharm. Investig. 53, 627–641 (2023). https://doi.org/10.1007/s40005-023-00628-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40005-023-00628-9