Abstract
Purpose
Antimicrobial resistance poses a major threat to human health globally and antibiotic overuse is a main driver of resistance. Antimicrobial stewardship (AMS) was developed to improve the rationale use of antibiotics. The Choosing Wisely campaign was initiated to ameliorate medical practice through avoidance of unnecessary diagnostic and therapeutic procedures. Our objective was to give an overview on the Choosing Wisely recommendations related to AMS practices from a selection of different countries in order to define future needs.
Methods
We evaluated the seven countries already analyzed for Choosing Wisely recommendations related to topics of infectious medicine before. Finally, we included five of the former countries (Australia/New Zealand, Canada, Italy, Switzerland, and USA) and Germany with easily accessible recommendations and selected those related to six categories of AMS as following: diagnostics, indication, choice of antiinfective drugs, dosing, application and duration of therapy.
Results
In total, 213 recommendations could be extracted related to AMS for the six countries and were matched to the chosen categories. Interestingly, no recommendations were found for the category “dosing.” Topics related to indication and diagnostics were most frequently found with 85 and 78 recommendations, respectively. Perioperative prophylaxis was a frequently addressed issue – both related to application, indication and duration. Avoiding antibiotic treatment of asymptomatic bacteriuria and upper respiratory tract infections were central topics of all countries.
Conclusion
AMS is an important strategy to fight increasing resistance and is frequently addressed by Choosing Wisely recommendations of different countries. Similar issues are considered important in the selected countries.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Antimicrobial resistance poses a major threat to human health globally and antibiotic overuse is a main driver of resistance [1, 2]. It is estimated that drug-resistant infections will increase dramatically in the coming decades without interventions [3]. WHO and other groups agree that a global action is necessary [4].
Antimicrobial stewardship (AMS) has been developed to improve the rationale use of antibiotics and guidelines related to its implementation have been published in several countries [5, 6].
The Choosing Wisely campaign – initiated in 2012 in the USA—was started to ameliorate medical practice through avoidance of unnecessary diagnostic and therapeutic procedures and has emerged nowadays in over 25 countries [7, 8]. Many multinational Choosing Wisely recommendations are related to the overuse of antibiotics and in Canada a campaign “Using antibiotics wisely” for the primary sector was implemented [9]. Nevertheless, a comprehensive review of Choosing Wisely recommendations related AMS strategies is missing.
Our objective was to give an overview on Choosing Wisely recommendations related to AMS practices of a selection of different medical societies and countries. Hereby, we adapted our search to the different AMS categories as described by the guidelines for AMS rounds, namely diagnostics, indication, application, duration, choice of drug and dosing [6].
Methods
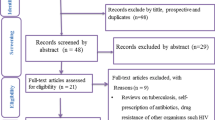
For this narrative review, it was decided to relate to the review written in 2015 [10]. The seven countries (Australia/New Zealand, Canada, Italy, Japan, The Netherlands, Switzerland and USA) evaluated in 2015 were chosen again. All Choosing Wisely recommendations of the seven countries and Germany were searched for those related to antimicrobial stewardship and a rational use of antiinfective agents. After the initial evaluation, however, Japan and the Netherlands had to be excluded as there were no clear recommendations to be found (Japan) or there was no collection of all recommendations which was easily accessible (Netherlands).
According to the German AWMF guideline antimicrobial stewardship, there are six categories for the rational use of antimicrobial agents during ward rounds: diagnostics, indication, choice of antiinfective drugs, dosing, application and duration of therapy [6]. We, therefore, sought to classify the international Choosing Wisely recommendations as well as the German recommendations according to these keywords.
Results
In total, 213 Choosing Wisely recommendations concerning AMS of the six countries could be listed for this review (see Tables 1, 2, 3, 4, and 5). They were derived from 85 different societies and associations from Australia/New Zealand, Canada, Germany, Italy, Switzerland and the USA. In each country, a substantial part of the recommendations was released by non-infectious diseases (non-ID) societies. Interestingly, Germany is the only country with recommendations made only by the internal medicine societies.
Categorizing them according to their respective topic, most recommendations could be found for “indication” (n = 85, 40%) and “diagnostics” (n = 78, 37%). Issues that were addressed within the category “indication” by all six countries were avoiding antibiotic treatment in asymptomatic bacteriuria or upper respiratory infections with mostly viral origin. In addition, recommendations against antibiotics for mild-to-moderate sinusitis and against the treatment of microbiological results of superficial wound swaps were also frequently found.
Another central issue was the prophylactic use of antibiotics. In this respect, not only surgical prophylaxis was addressed but also antibiotic prophylaxis in neutropenic patients, travelers’ diarrhea, or acute burn injuries. Moreover, prophylactic use of antibiotics could also be categorized in “application” (when to give prophylactic substances if indicated) and “duration” (especially not to prolong surgical prophylaxis).
Results for “diagnostics” were much more diverse comparing the different countries. Avoiding urine cultures without symptoms of urinary tract infections was recommended most frequently within this category in four of the countries studied. This was followed by the recommendations not to test for C. difficile colitis in patients without diarrhea and not to obtain radiographic imaging in acute rhinosinusitis.
Much less recommendations were to be found for the other four categories. Worth mentioning for “choice of antiinfective drug” is the request to question anamnestic penicillin allergy and the cautious use of fluoroquinolones. Within “application” several countries recommend the oral use of antibiotics whenever possible. For the category “dosing”, no recommendations could be found which is interesting as the dosage of antibiotics is an important AMS topic. Consequently, there is no table for this category.
Overall, most of the recommendations advise against certain diagnostic or therapeutic measures (200/213, 94%) Germany keeps an exceptional position here: all positive recommendations listed for the review are from this country. In addition, recommendations within the six countries studied concentrate on similar fields and also gaps in recommendations are alike.
Discussion
In light of increasing bacterial resistance globally [1], we aimed to analyze the implementation of antimicrobial stewardship goals within the simple Choosing Wisely recommendations internationally. For this review, a substantial number of recommendations concerning AMS could be listed screening six countries.
For all countries and societies assessed, it can be stated that “indication” is central in AMS for both diagnostic measures and antiinfective therapy. For “diagnostics”, an important issue found in many recommendations is the “pretest” probability, i.e., what is the likelihood for an infection in the respective patient [11]. To truly understand the result of a test and properly diagnose a patient, we must use pretest probability. In interpreting microbiological results, it is frequently stressed that a differentiation has to be made between colonization and infection and that viral infections are not to be treated with antibiotics. These are important issues that can be found in many national and international guidelines concerning AMS or certain infections [5, 6, 12]. Repeating them in the simple Choosing Wisely recommendations seemed important for all countries included in this review.
A broad consensus could also be found concerning surgical prophylaxis. The incorrect timing, false indication and prolongation – shown to be associated with acute kidney failure and Clostridioides difficile infection but with no reduction in the incidence of surgical site infections, seems to be a problem in all countries studied [13, 14]. Despite increasing efforts in adjusting indication and duration of perioperative prophylaxis, there is still much misuse of antibiotics after surgical procedures. A fact which most likely reflects not only a lack of knowledge but also uncertainty and concern regarding the surgical outcome [15, 16]. Here another aspect of AMS is in demand: the psychological point which extends beyond simple recommendations. A rationale use of antibiotics often implies a behavioural change [17,18,19,20].
Surprisingly, no recommendations were found concerning “dosage” – a gap that should maybe lead to the creation of new recommendations. Reasons for this might be the difficulty of a dosage specification which is dependable on many variables (kidney function, body mass index and others). In addition, the dosage of antibiotic substances is also dependent on the microbiological resistance testing with e.g. pathogens tested as “increased dosage” [21]. With regard to the continuous application of β-lactam antibiotics, recommendations are probably missing as there is still a discussion about a gap of evidence for patient-centered endpoints [22, 23].
Almost all recommendations listed here were negative ones, i.e., advising against a certain measure. This reflects the original idea of the Choosing Wisely campaign to rather avoid unnecessary interventions [8]. It also fits the AMS notion – given the current habit in antibiotic use, doing less is often the advice to clinicians in stewardship interventions [24]. Germany represents an exception with its “Klug entscheiden” initiative publishing negative and positive recommendations [25].
Another interesting point was the finding that recommendations of all six countries concerned similar topics. This is most likely due to the fact that six industrial countries were chosen with very similar socio-economic status and similar health care systems. Recommendations in low-income countries conceivably would have been different with health care problems which differ substantially to the ones seen in the countries chosen for the review. A specific guidance for setting up AMS in low- and middle-income countries is discussed [26].
This leads to a limitation of our review, the selection of the six countries. We had decided to concentrate on the countries which participated in the Choosing Wisely initiative from the beginning and were evaluated for the review published a few years ago [10]. However, in recent years many more countries began the establishment of Choosing Wisely recommendations. But an overview of all possible countries would have exceeded the scope of this study.
For the review, we did not address prophylaxis regarding central venous catheters or even more important urine catheters. This is an important AMS issue as well, but however represents a large overlap with clinical hygiene and was therefore left out.
Conclusions
AMS is an important strategy to combat increasing antibiotic resistance. The Choosing Wiselycampaign addresses multiple topics related to AMS and might be a helpful instrument to attract attention for improving the implementation of AMS.
This work is dedicated to the 50th anniversary of Infection.
Availability of data and materials
Not applicable.
References
Antimicrobial RC. Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. Lancet. 2022;399:629–55.
Bell BG, Schellevis F, Stobberingh E, Goossens H, Pringle M. A systematic review and meta-analysis of the effects of antibiotic consumption on antibiotic resistance. BMC Infect Dis. 2014;14:13.
Cassini A, Hogberg LD, Plachouras D, Quattrocchi A, Hoxha A, Simonsen GS, et al. Attributable deaths and disability-adjusted life-years caused by infections with antibiotic-resistant bacteria in the EU and the European economic area in 2015: a population-level modelling analysis. Lancet Infect Dis. 2019;19:56–66.
World Health Organisation. Global action plan on antimicrobial resistance. 2016. Available from: https://www.who.int/publications/i/item/9789241509763. Accessed 4 Feb 2023.
Barlam TF, Cosgrove SE, Abbo LM, MacDougall C, Schuetz AN, Septimus EJ, et al. Implementing an antibiotic stewardship program: guidelines by the infectious diseases society of America and the society for healthcare epidemiology of America. Clin Infect Dis. 2016;62:e51–77.
S3- Leitlinie Strategien zur Sicherung rationaler Antibiotika Anwendung im Krankenhaus. 2019. Available from: https://register.awmf.org/de/leitlinien/detail/092-001. Accessed 4 Feb 2023.
Morden NE, Colla CH, Sequist TD, Rosenthal MB. Choosing wisely–the politics and economics of labeling low-value services. N Engl J Med. 2014;370:589–92.
Wolfson D, Santa J, Slass L. Engaging physicians and consumers in conversations about treatment overuse and waste: a short history of the choosing wisely campaign. Acad Med. 2014;89:990–5.
Using Antibiotics Wisely. Available from: https://choosingwiselycanada.org/primary-care/antibiotics/. Accessed 4 Feb 2023.
Jung N, Lehmann C, Fatkenheuer G. The, “choosing wisely”: initiative in infectious diseases. Infection. 2016;44:283–90.
Fowkes FG. Containing the use of diagnostic tests. Br Med J (Clin Res Ed). 1985;290:488–90.
S3 Leitlinie Epidemiologie, Diagnostik, Therapie, Prävention und Management unkomplizierter, bakterieller, ambulant erworbener Harnwegsinfektionen bei erwachsenen Patienten. 2017. Available from: https://register.awmf.org/de/leitlinien/detail/043-044. Accessed 4 Feb 2023.
Branch-Elliman W, O’Brien W, Strymish J, Itani K, Wyatt C, Gupta K. Association of duration and type of surgical prophylaxis with antimicrobial-associated adverse events. JAMA Surg. 2019;154:590–8.
de Jonge SW, Boldingh QJJ, Solomkin JS, Dellinger EP, Egger M, Salanti G, et al. Effect of postoperative continuation of antibiotic prophylaxis on the incidence of surgical site infection: a systematic review and meta-analysis. Lancet Infect Dis. 2020;20:1182–92.
Miranda D, Mermel LA, Dellinger EP. Perioperative antibiotic prophylaxis: surgeons as antimicrobial stewards. J Am Coll Surg. 2020;231:766–8.
Mazuski JE. Perioperative antibiotic prophylaxis: can we do better? J Am Coll Surg. 2020;231:768–9.
Pouly E, Coppry M, Rogues AM, Dumartin C. Systematic review of factors promoting behaviour change toward antibiotic use in hospitals. Clin Microbiol Infect. 2022;28:911–9.
Charani E, de Barra E, Rawson TM, Gill D, Gilchrist M, Naylor NR, et al. Antibiotic prescribing in general medical and surgical specialties: a prospective cohort study. Antimicrob Resist Infect Control. 2019;8:151.
Charani E, Ahmad R, Tarrant C, Birgand G, Leather A, Mendelson M, et al. Opportunities for system level improvement in antibiotic use across the surgical pathway. Int J Infect Dis. 2017;60:29–34.
Charani E, Ahmad R, Rawson TM, Castro-Sanchez E, Tarrant C, Holmes AH. The differences in antibiotic decision-making between acute surgical and acute medical teams: an ethnographic study of culture and team dynamics. Clin Infect Dis. 2019;69:12–20.
European Committee on Antimicrobial Susceptibility Testing. Clinical breakpoints and dosing of antibiotics. 2023. Available from: https://www.eucast.org/clinical_breakpoints. Accessed 4 Feb 2023.
Dulhunty JM, Roberts JA, Davis JS, Webb SA, Bellomo R, Gomersall C, et al. Continuous infusion of beta-lactam antibiotics in severe sepsis: a multicenter double-blind, randomized controlled trial. Clin Infect Dis. 2013;56:236–44.
Abdul-Aziz MH, Dulhunty JM, Bellomo R, Lipman J, Roberts JA. Continuous beta-lactam infusion in critically ill patients: the clinical evidence. Ann Intensiv Care. 2012;2:37.
Fathi A, Hennigs A, Addo MM. Less is more... in infectious diseases. Internist (Berl). 2021; 62(4): 373–8.
Klug entscheiden. Available from: https://www.klug-entscheiden.com/. Accessed 4 Feb 2023.
Cox JA, Vlieghe E, Mendelson M, Wertheim H, Ndegwa L, Villegas MV, et al. Antibiotic stewardship in low- and middle-income countries: the same but different? Clin Microbiol Infect. 2017;23:812–8.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
NJ and RD wrote the main manuscript text and LT prepared all tables. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
NJ has received lecture fees from Bayer, Gilead, Infectopharm, Labor Stein, Medacta and MSD and travel grants from Basilea, Correvio, Gilead, Novartis and Pfizer and grants from an observational study from Infectopharm. RD has received lecture fees from MSD and Andmore Media GmbH and fees for the advisory board from Eumedica. LT none.
Ethical approval
Not applicable.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jung, N., Tometten, L. & Draenert, R. Choosing Wisely internationally – helpful recommendations for antimicrobial stewardship!. Infection 51, 567–581 (2023). https://doi.org/10.1007/s15010-023-02005-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-023-02005-y