Abstract
A 64-year-old man visited the outpatient department of our hospital for the first time due to bilateral lower limb edema, which he noticed 1 week before the visit. Pain suddenly developed in the left lower limb while the patient was in the waiting room. Nephrotic syndrome was suspected based on blood and urine test results. Acute arterial thromboembolism in the left lower limb associated with hypercoagulation due to nephrotic syndrome was suspected, and a diagnosis was made using computed tomography angiography. Arterial thrombectomy was urgently performed, and the limb was salvaged without sequelae. Based on renal biopsy, minimal change nephrotic syndrome was diagnosed, and the patient underwent remission induction with steroid therapy. Heparin was drip infused and apixaban was orally administered to prevent recurrent thrombosis. Nephrotic syndrome in the acute phase is often complicated by thrombosis. Particularly, arterial thromboembolism requires prompt treatment, and prophylactic anticoagulation therapy needs to be considered.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients with nephrotic syndrome (NS) are likely to develop thromboembolism due to increased pro-thrombotic factors, decreased anti-thrombotic factors, and decreased activities of the fibrinolytic system. It can induce serious pathological conditions such as deep vein thrombosis of the lower limbs, renal vein thrombosis, and pulmonary embolism. Prompt diagnosis and treatment are required because not only venous thromboembolism (VTE) but also arterial thromboembolism (ATE) have been reported in rare cases [1]. We experienced a case of minimal change nephrotic syndrome (MCNS) diagnosed due to acute femoral thromboembolism and successfully salvaged limb. Here, we report the case along with a literature review.
Case report
A 64-year-old man with independent ADL visited our outpatient clinic for the first time with a chief complaint of bilateral lower limb edema, which he noticed 1 week before the visit. Pain suddenly developed in the left lower limb while the patient was in the waiting room. The waiting time was about 1 h. NS was diagnosed based on blood and urine test results. Acute arterial thromboembolism in the left lower limb associated with hypercoagulation due to NS was suspected.
The patient’s medical history included appendicitis at the age of 13; gastroesophageal reflux at the age of 50; and colonic diverticulitis at the age of 62. He neither smoked nor drank alcohol. He did not take any medications.
Physical findings on admission: Height 157 cm; body weight 65.5 kg (55 kg before edema developed); body temperature, 36.4 °C; blood pressure, 131/86 mmHg; pulse rate, 94 beats/min; percutaneous arterial oxygen saturation, 96% (room air); regular heart beat with no murmur; and clear breath sounds. An abdominal examination revealed flat, soft abdomen neither with tenderness nor with abnormal bowel sounds. Edema of bilateral lower limbs was present. Pain was present from the left groin to the periphery of the left lower limb. Cold feeling and hypoesthesia were present in the left foot. Left dorsalis pedis artery was not felt.
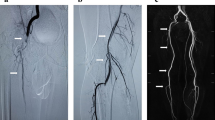
Laboratory data on admission (Table 1): A blood test showed hemoglobin level of 17.5 g/dL and hematocrit of 52.3%, showing hemoconcentration. The D-dimer level was 21.4 μg/mL, suggesting thrombosis. Fibrinogen level was high at 620 mg/dL, and antithrombin activity was low at 49%. Albumin level was low at 1.1 g/dL. Urinalysis showed protein urine of 12.28 g/gCr, indicating severe proteinuria. Plain chest radiography showed no pulmonary congestion or pleural effusion. Computed tomography angiography revealed filling defects in the distal common iliac artery and at the origin of the internal and external iliac arteries, suggesting thrombosis. The left internal iliac artery was occluded. Severe stenosis was noted in the left external iliac artery. The profunda femoris artery was occluded in the proximal femur (Fig. 1).
a Pelvic-computed tomography angiography revealed filling defects in the distal common iliac artery and at the origin of the internal and external iliac arteries, suggesting thrombosis. The left internal iliac artery was occluded. Severe stenosis was noted in the left external iliac artery. b Lower-extremity-computed tomography angiography revealed that the profunda femoris artery was occluded in the proximal femur
Clinical course (Fig. 2): The patient was urgently admitted to the hospital, and arterial thrombectomy was performed on the same day. The left common femoral artery was transversely incised, a balloon catheter for thrombectomy was inserted into the central and distal sides, and a large amount of thrombus was collected. The surgery was completed after intraoperative contrast imaging showing the periphery of the left lower limb was confirmed. Continuous drip infusion of heparin was then initiated to prevent thrombosis. On the second hospital day, treatment with prednisolone 55 mg/day (1 mg/kg/day) was started for NS. On the ninth hospital day, renal biopsy was performed, and diagnosis of MCNS was made (selectivity index = 0.05). On the 15th hospital day, ultrasonography was performed on the vessels of lower extremities, which showed no venous thrombosis. On the 16th hospital day, the prophylactic anticoagulant was switched from continuous drip infusion of heparin to oral administration of edoxaban 30 mg. The dose of prednisolone was tapered, and the patient was discharged from the hospital on the 38th hospital day. Serum albumin level of 3.7 g/dL and urinary protein of 0.17 g/gCr were confirmed on the 50th day from the initial visit. A reexamination of contrast-enhanced CT 3 months after the onset revealed that the stenosis of the left external iliac artery had disappeared, indicating that it was due to thrombus. Prednisolone was scheduled to be tapered while paying attention to recurrence of NS.
Discussion
In this case, NS was found with acute femoral thromboembolism.
In some instances, thromboembolic disease is the initial presenting symptom, leading to the subsequent discovery of NS [2,3,4].
Patients with NS are susceptible to thrombus formation because of efflux of antithrombin and plasminogen into the urine, increased fibrinogen production in the liver, and increased viscosity due to blood concentration [5]. In this patient, antithrombin activity decreased to 49%, and fibrinogen level increased to 620 mg/dL when he visited the hospital, which normalized on the 27th hospital day after NS remission induction (antithrombin activity 129%, fibrinogen level 238 mg/dL, the D-dimer level 0.5 μg/mL).
In 2008, Mahmoodi et al. reported a cohort study on the incidence of VTE and ATE in 298 patients with NS [6]. The annual incidence of VTE and ATE was reported to be 1.02% and 1.48%, respectively, and the annual incidence of VTE and ATE combined was 2.50% during 10 years of the mean observation period. Particularly, the incidence during 6 months after the onset of NS was 9.85% for VTE (140 times higher than that in the general population) and 5.52% for ATE (50 times higher than that in the general population), and thrombosis occurred at a high rate.
Higher level of urine protein and serum albumin tended to be significantly associated with VTE (P = 0.03).
Conversely, neither degree of proteinuria nor serum albumin levels were related to ATE. Sex (male), age (≥ 35 years), hypertension, diabetes, smoking, prior ATE, and estimated glomerular filtration rate (≤ 30 mL/min/1.73 m2) were reported to predict ATE (P < 0.02).
The annual incidence of ATE by primary disease was 1.54% for focal glomerulosclerosis, 1.31% for membranous glomerulonephritis (MGN), 0.51% for membranoproliferative glomerulonephritis, and 0.3% for MCNS.
Fukunaga et al. reported a literature review of 17 cases of MCNS with artery thromboembolism. Most cases were reported in males, with marked hypoalbuminemia and severe urinary proteinuria. In addition, arterial embolism occurred regardless of the onset or recurrence of NS [5].
This patient developed ATE despite no risk factors related to ATE other than sex and age, suggesting the importance of preventing thrombosis in NS.
The 2012 Kidney Disease: Improving Global Outcomes (KDIGO) guidelines recommend prophylactic anticoagulation in idiopathic MGN only, but acknowledge that existing data are limited and of low quality [7].
According to the systematic review by Lin et al., the 2012 KDIGO guidelines suggest anticoagulation only for idiopathic MGN; however, available evidence suggests that perhaps anticoagulation can be considered in all patients with NS [8].
Most forms of NS appear to carry some clinically significant risk of thrombosis, and anticoagulation should be considered in the setting of hypoalbuminemia. The serum albumin threshold below which to commence anticoagulation is not clearly established, although most studies concur that the level is between 2 and 3 g/dL. This will need to be balanced with the patient’s risk of bleeding. If proceeding with anticoagulation, it should be commenced as soon as it is safe, as the risk of thrombosis has consistently been found to be highest in the first 6 months of diagnosis [6, 9, 10].
In the 2021 KDIGO guidelines, MGN carries a particularly high risk of thromboembolic events. In addition, prophylactic anticoagulation should be employed in patients with nephrotic syndrome when the risk of thromboembolism exceeds the estimated patient-specific risks of an anticoagulation induced serious bleeding event [11].
Unfortunately, there is little evidence available in the literature on the optimal prophylactic agent or its dosing, owing to a lack of randomized trials.
Factor Xa inhibitors are not systematically studied in patients with NS. Dosing in the general population is adjusted according to serum creatinine, creatinine clearance (estimated by Cockcroft-Gault equation), age, and weight. The effects of hypoalbuminemia on drug dosing have not been studied, and these drugs are heavily albumin-bound, which is likely to substantially affect their half-lives. Despite a few favorable case reports, the pharmacokinetic properties of these drugs require additional study for both safety and efficacy before they can be generally recommended in nephrotic patients [11].
The patient had acute femoral thromboembolism concurrent with NS; however, his limb was successfully salvaged by emergency thrombectomy.
In the cases of femoral artery thromboembolism concurrent with NS, some cases have been reported to result in leg amputation [12,13,14]. Meanwhile, other reports have revealed arterial obstruction at various sites, including pulmonary embolism [15, 16], cerebral infarction [13, 17,18,19,20,21], and superior mesenteric artery thrombosis [22].
In conclusion, patients with NS may concurrently develop ATE, resulting in a serious condition. Therefore, prophylactic anticoagulation therapy should be considered in patients at high risk of thromboembolism.
References
Evidence-Based Clinical Practice Guideline for Nephrotic Syndrome 2020. Tokyo-Igakusha. 2020: 43–44.
Khanna A. Undiagnosed and unsuspected nephrotic syndrome in a young adult presenting as submassive pulmonary embolism. Chest. 2016;149:A506.
Qureshi M, Alabi F, Christian F, Romero C. The forgotten urinalysis: an integral part of unmasking thrombophilia. J Community Hosp Intern Med Perspect. 2019;9:40–4.
Pallavi R, Sunggeun L, Baumstein D, Mendoza RC, Chaudhariet A. Stroke in a young woman as a presenting manifestation of membranous nephropathy. Am J Ther. 2016;23:e950–4.
Fukunaga S, Matsumoto K, Tanno Y, Sudo K, Uehara G, Miyasato H, Tsuboi N, Ogura M, Yokoo T. A case of right femoral artery thromboembolism in steroid-dependent nephrotic syndrome. Nihon Jinzo Gakkai Shi. 2016;58:604–9.
Mahmoodi BK, ten Kate MK, Waanders F, Veeger NJ, Brouwer JL, Vogt L, et al. High absolute risks and predictors of venous and arterial thromboembolic events in patients with nephrotic syndrome: results from a large retrospective cohort study. Circulation. 2008;117:224–30.
Kidney Disease: Improving Global Outcomes (KDIGO) Glomerulonephritis Work Group. KDIGO clinical practice guideline for glomerulonephritis. Kidney Int Suppl. 2012;2:139.
Lin R, McDonald G, Jolly T, Batten A, Chacko B. A systematic review of prophylactic anticoagulation in nephrotic syndrome. Kidney Int Rep. 2019;5:435–47.
Harza M, Ismail G, Mitroi G, Gherghiceanu M, Preda A, Mircescu G, et al. Histological diagnosis and risk of renal vein thrombosis, and other thrombotic complications in primitive nephrotic syndrome. Rom J Morphol Embryol. 2013;54:555–60.
Zou PM, Li H, Cai JF, Chen ZJ, Li C, Xu P, et al. A cohort study of incidences and risk factors for thromboembolic events in patients with idiopathic membranous nephropathy. Chin Med Sci J. 2018;33:91–9.
Kidney Disease: Improving Global Outcomes (KDIGO) Glomerulonephritis Work Group. KDIGO clinical practice guideline for glomerulonephritis. Kidney Int. 2021;100:S36–8.
Togashi T, Shimosato Y, Saida K, Miyake N, Nakamura T, Ito S. Childhood nephrotic syndrome complicated by catastrophic multiple arterial thrombosis requiring bilateral above-knee amputation. Front Pediatr. 2020;8:107.
Nagalla VK, Raju SB, Ramesh Bura NR. Arterial thrombosis associated with factor v leiden mutation in a child with nephrotic syndrome. Indian J Nephrol. 2021;31:187–9.
Cameron JS, Ogg CS, Ellis FG, Salmon MA. Femoral arterial thrombosis in nephrotic syndrome. Arch Dis Child. 1971;46:215–6.
Mohamed HN, Bashir AM, Mohamed YG. Multiple venous and pulmonary artery thrombosis as a presenting complaint of nephrotic syndrome-case report and challenges in management. Vasc Health Risk Manag. 2022;18:589–93.
Ruggeri P, Lo Bello F, Nucera F, Gaeta M, Monaco F, Caramori G, et al. Hereditary hyperhomocysteinemia associated with nephrotic syndrome complicated by artery thrombosis and chronic thromboembolic pulmonary hypertension: a case report. Monaldi Arch Chest Dis. 2017;87:880.
Kara A, Gurgoze MK, Serin HM, Aydin M. Cerebral arterial thrombosis in a child with nephrotic syndrome. Niger J Clin Pract. 2018;21:945–8.
Sasaki Y, Raita Y, Uehara G, Higa Y, Miyasato H. Carotid thromboembolism associated with nephrotic syndrome treated with dabigatran. Case Rep Nephrol Urol. 2014;4:42–52.
Brahmbhatt BK, Mathew A, Rajesh R, Kurian G, Unni VN. Brachiocephalic artery thrombosis in adult nephrotic syndrome. Indian J Nephrol. 2011;21:204–7.
Song KS, Won DI, Lee AN, Kim CH, Kim JS. A case of nephrotic syndrome associated with protein S deficiency and cerebral thrombosis. J Korean Med Sci. 1994;9:347–50.
Pandian JD, Sarada C, Elizabeth J, Visweswaran RK. Fulminant cerebral infarction in a patient with nephrotic syndrome. Neurol India. 2000;48:179–81.
Kim HJ, Park CH, Kang CM, Park HC, Kim CY, Cho YS. Arterial thrombosis associated with nephrotic syndrome–a case report and review (adult cases in the English literature). J Korean Med Sci. 1993;8:230–4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
Not applicable.
Consent for publication
Informed consent was obtained from participants included in the article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Tokoyoda, T., Inagaki, T., Aoki, Y. et al. Minimal change nephrotic syndrome diagnosed with acute femoral thromboembolism and successfully salvaged limb: a case report. CEN Case Rep 12, 357–361 (2023). https://doi.org/10.1007/s13730-023-00774-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13730-023-00774-x