Abstract
The school food environment—including when and where children obtain food and the types of options available during the school day—plays an important role in children’s consumption patterns. Thus, childhood obesity prevention efforts often focus on altering the school food environment as a mechanism for improving student dietary intake. This review examines the role school food programs and policies play in improving children’s diet, weight, and health. Overall, research suggests that significant improvements have been made in school nutrition policies and programs. Due to the recent program changes made as a result of the 2010 Healthy, Hunger-Free Kids Act, an emphasis was placed on research conducted over the past decade and especially on the evaluation of foods and beverages served and sold since implementation of this national law. This review also examines remaining gaps in the literature and opportunities for further improvements in school food programs and policies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Childhood obesity is one of the most serious public health problems facing the USA, and there is an urgent need to find effective solutions. Efforts to prevent and reduce childhood obesity have the greatest effect when they take into account not only the individual but also the environment in which a person lives, learns, works, and plays. With children and adolescents consuming up to 50 % of their daily calories at school, the school food environment plays an important role in childhood obesity prevention [1]. This is particularly relevant for the more than 21.5 million school-age children from lower income households who receive free or reduced-price meals on a typical day [1]. An extensive review of the literature conducted by the 2015 Dietary Guidelines for Americans Advisory Committee found that school-based programs and policies can improve dietary intake and weight status of children [2]. Additionally, the US Department of Agriculture’s (USDA) updated nutrition standards for school meals, snacks, and beverages following the Healthy, Hunger-Free Kids Act (HHFKA) of 2010 ensure that the school food environment is an increasingly important focal point for ongoing efforts to improve children’s health and nutrition and prevent childhood obesity [3]. In this article, we explore various components of the school food environment and their capacity to positively influence children’s diet, weight, and overall health, with an emphasis on changes that have occurred from 2010 to present (Table 1).
School Meals: National School Lunch Program and School Breakfast Program
The National School Lunch Program (NSLP) and the School Breakfast Program (SBP) are the primary sources of foods and beverages provided by schools during the school day. The NSLP was established in 1946 and the SBP in 1966 in order to meet the needs of under-nourished children across the USA [4, 5]. Today, these programs are not only a primary source of nutritious meals for low-income children but they also play an important role in reducing the income and race or ethnicity-based disparities in diet quality and health outcomes. In 2014, 30.5 million children participated in the NSLP, 71.6 % of which received free or reduced-price lunch, and 13.64 million children participated in the SBP, 84.9 % of which received free or reduced-price breakfast [6, 7]. Given the marked difference between student participation in NSLP and SBP and the positive relationship between the SBP and academic outcomes, attendance, and dietary intake, recent efforts such as universal breakfast and breakfast in the classroom have focused on program expansion and outreach [8, 9].
Following the HHKFA, nutrition standards for the NSLP and SBP were updated for the first time in more than 15 years [10•]. These standards, which went into effect in 2012, were based on recommendations from the Institute of Medicine and primarily require schools to offer more servings and varieties of fruits and vegetables, more whole grains, and less saturated fat and sodium. Prior to 2012, meals provided by the NSLP and SBP were too high in sodium and saturated fat and low in important nutrients and food groups like fiber and whole grains [11]. Additionally, following HHFKA, schools were required to make free, potable water available to all students where meals are served [12]. Unfortunately, the guidance provided by USDA on this topic has primarily focused on lunch and only requires water to be served during breakfast when it is in the cafeteria, not in other locations [13]. Many consider this to be a significant loophole as breakfast in the classroom and universal breakfast options, such as grab-and-go, are becoming increasingly popular. Research has shown that replacing sugar-sweetened beverages with calorie-free beverages, such as water, may lead to decreased weight gain in children [14, 15]. Additionally, a plethora of research exists on the importance of adequate water consumption to children’s health and development, yet currently, over half of all children in the USA are inadequately hydrated [16].
Research has demonstrated significant improvements in the nutritional content of meals offered even after only 1 year of implementation [17•]. CDC data show that 94.4 % of schools nationwide are now offering whole grain foods every day at lunch, 79.4 % are offering two or more vegetables for lunch, and 78 % are providing two or more fruits for lunch [10•]. Further, in 2015, USDA reported that 97.1 % of school food authorities nationwide were meeting the updated school meal standards [18]. Along these lines, access to free water in schools has increased in California and nationally since implementation of the HHFKA provisions [19, 20]. These data suggests that there has been a significant improvement in the foods and beverages offered to children across the USA.
Student Acceptance and Consumption
Overall, it appears that student acceptance of the healthier offerings in school meals is improving. Initially, 53 % of elementary schools reported that children complained about the meal changes; however, after less than 1 year of implementation, 70 % of schools reported that children liked the lunches [21]. Among middle and high schools, trends were similar with initial pushback but improved acceptance over time [22]. There were significantly more complaints about the new meals at the high school level and in rural elementary schools, highlighting the need for increased training and technical assistance among these groups [21, 22].
Along these lines, school food authorities and other stakeholders have expressed concern about whether or not there has been an increase in food waste following implementation of the updated standards. Several studies have measured plate waste in small subsets of schools and have shown mixed results [23, 24•, 25, 26]. Generally, these studies have found that food waste has not increased as a result of updated meal standards [23, 24•]. One study noted that observed food waste was high both pre and post implementation, suggesting that this is a long-standing issue and efforts are needed to improve consumption [23]. Another study found that food waste was lower post-implementation due to increases in vegetable consumption [24•]. Conversely, another study found that about 25 % of middle and high schools reported a little more waste and 16 % of middle and 20 % of high schools reported much more food waste after implementation [22].
Still, the research on selection and consumption following implementation of updated standards is promising, with some research showing that more students are selecting fruit, 100 % juice, other vegetables, whole grains, protein foods, milk, and fewer starchy vegetables [27]. Some research has also suggested that more low-income students are buying and consuming lunch post-implementation [21]. These findings are important given that low-income students are at increased risk for obesity.
Health and Weight Outcomes
Research suggests that the updated meal standards have and will continue to make meaningful contributions to obesity prevention by replacing consumption of energy-dense, nutrient-poor foods and beverages with healthier options. Significant associations have been found between several specific USDA meal components, specifically offering fruits or vegetables wherever food is sold in a school and not offering whole or 2 % milk, and a decreased odds of overweight and obesity among high school students [28]. Also, absence of sugar-sweetened beverages is associated with lower odds of overweight and obesity among Hispanic middle school students [28]. Research also suggests that the more components of the USDA meal standards that are successfully implemented by high schools, the lower the odds of overweight and obesity [28]. With regards to the water requirements, a recent study examining the effects of installing water jets in New York City schools also showed an association between a relatively low-cost water availability intervention and decreased student weight [29]. Additionally, an evaluation of guidelines similar to those required by USDA found reductions in calories consumed per student per year [30]. Further, research focused on state laws with standards similar to those now required by USDA suggests that more rigorous nutrition standards may be associated with more favorable weight status, especially among students receiving free and reduced-price meals as compared to students who do not participate in the NSLP [31]. These data highlight the importance of providing support to schools to ensure full implementation of the standards.
Ongoing Challenges
While the updated nutrition standards have generated some pushback, research generally suggests that they have resulted in measurable improvements in the school food environment and in children’s behaviors and intake. Yet, there are ongoing implementation challenges that need attention, such as the increased cost of serving healthier meals and the need for updated kitchen equipment and staff training. Several solutions to these challenges have been suggested by recent research (Table 2).
As part of the HHFKA, USDA provided schools meeting updated nutrition standards an additional 6 cents per lunch; no additional funds were provided for breakfast [3]. There is debate over whether this addition to the federal reimbursement rate is sufficient to provide the increased servings of fruits, vegetables, and whole grains required by updated standards. Analyses using varying methods have arrived at different estimates for the cost of serving healthier school meals, some showing 6 cents would be sufficient and some demonstrating 6 cents would leave a financial gap for schools to fill [32].
A recent nationwide survey of school nutrition staff found that the most commonly cited barriers to meeting updated nutrition standards were a lack of kitchen equipment or infrastructure and training and technical assistance [33, 34]. Nearly 90 % of schools reported that they needed one or more pieces of equipment to meet the standards [34]. Only 42 % of schools reported they had money in their budget for equipment, and of those, only about half felt the amount was sufficient [34]. Since 2009, USDA has allocated grant funding to provide equipment to schools, but more support will be needed as federal funding for kitchen equipment has largely been absent for the last 30 years [34, 35]. Further training and technical assistance are also needed for school nutrition staff on the updated nutrition standards, culinary skills, and professional standards [10•, 23, 33]. Only 37 % of schools have funding set aside for staff training, and few of these schools feel that funding is sufficient [33]. In 2015, USDA released a final rule that established minimum professional standards, hiring requirements, and continuing education requirements for individuals operating school meal programs [33]. These efforts will be important to ensuring effective implementation of USDA’s updated meal standards.
Finally, US studies suggest that providing and promoting appealing water in school cafeterias and providing cups can increase intake of water and decrease obesity [29, 36, 37]. However, more information and guidance is needed for schools on what qualifies as “effective” drinking water access. For example, research suggests that just having a traditional drinking fountain may not adequately increase intake in school cafeterias [38]. Examples of best practices include ensuring that the water source is safe and appealing to students, providing cups or reusable water bottles, and promoting water intake through signs or other activities [29, 36–38].
Competitive Foods and Beverages: Smart Snacks
While school meals are key components of the school food environment, there are a number of other foods and beverages available to students throughout the school day, such as those sold in a la carte lines, school stores, and vending machines. These foods and beverages make significant contributions to children’s consumption during the school day and may play an important role in obesity prevention efforts. Prior to the HHFKA, USDA termed these items competitive foods and beverages (CF); however, they are now more commonly referred to as Smart Snacks.
The HHFKA required USDA for the first time to establish minimum nutrition standards for CF. As a result, in 2014, the USDA Nutrition Standards for All Foods Sold in School, also known as the Smart Snacks nutrition standards, went into effect [39]. The Smart Snack standards limit the amount of calories, fat, sodium, and sugar found in CF and increase the servings of fruits, vegetables, and whole grains provided to children [39]. Prior to Smart Snacks, CF were readily available to students throughout the school day and generally contained higher than recommended amounts of fat, sugar, and sodium [40–42]. In 2012, a la carte foods were sold at lunch in 82 % of elementary schools, 95 % of middle schools, and 90 % of high schools across the country [43•]. Vending machines remain widely available in high schools but are much less common in elementary schools [43•]. Between 2008 and 2012, only 20 % of middle school and 17 % of high school students attended a school that did not offer candy and regular fat snacks. In comparison, fruits and vegetables were offered at only 25 % of middle schools and 16 % of high schools [44].
Prior to Smart Snacks implementation, few schools met the requirements; therefore, these new USDA regulations have great potential to improve the school food environment and, as a result, children’s weight and health [44]. Because of the recency of the changes, there has been little research evaluating the Smart Snacks standards to date; however, there is a wealth of existing evidence on the effects of CF on children’s diets and health, and the role policies can play in improving the school food environment.
Availability and Consumption
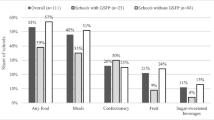
Research has consistently demonstrated that strong CF policies and programs have a significant influence on availability and in-school consumption of both healthy and unhealthy foods [45•, 46, 47]. For example, one study found that strong CF policies may be associated with reductions in the availability of sugar-sweetened beverages, as well as improvements in children’s reported consumption behaviors [47]. Studies have also found that state and district-level CF policies can exert a significant influence on improving the school food environment when compared to states without such policies [48]. Additionally, more rigorous CF policies have been associated with decreased consumption of sugar, fat, and calories and increased consumption of vegetables, fruits, and whole grains [48, 49].
Health and Weight Outcomes
The data examining CF policies and their influence on BMI and weight outcomes are limited. A recent systematic review of this topic found mixed results [45•]. One study demonstrated that CF policies were associated with reduced odds of overweight or obesity; another demonstrated that CF policies may be associated with a lower rate of increase of overweight among fifth graders, and two additional studies had mixed findings [50–53]. However, another national study of fifth grade students found no association between CF availability in schools and BMI [42]. Few of these studies used pretest/posttest study designs, with most using cross-sectional data to evaluate the impact of CF policies on the odds of overweight or obesity. Future research efforts should attempt to use longitudinal approaches to track the relationship between CF policies and BMI and weight outcomes. While studies examining the link between such policies and weight outcomes are limited in number, it is important to note that CF consumption can negatively influence children’s diet and health without significantly influencing their BMI [42].
While these examples may illustrate the potential impact of CF policies, they may not accurately reflect the true impact of Smart Snacks, as no existing state policies were fully aligned with the new USDA standards. Overall, this research suggests that CF exert a significant influence on the school food environment and that the Smart Snacks standards have the capacity to make significant, positive improvements in children’s diet, weight, and health.
Ongoing Challenges
While the Smart Snacks standards are a significant step to improving the CF offered in schools, there are several loopholes that should be addressed in future policy efforts. Fundraisers in schools are a common source of unhealthy foods and beverages [54]. Yet, the Smart Snacks standards allow for an exemption, whereby state agencies may determine an allowable number of fundraisers per year that can sell non-compliant items during the school day. There is wide variability among states in the number of exempted school fundraisers permitted, with some allowing as many as 90 exemptions per year. Moving forward, it will be important for state agencies to achieve a balance between students’ health and school financial needs.
Another issue that has recently emerged is that of “copy cat snacks.” Many manufacturers have reformulated food and beverage products to meet Smart Snack standards, and these healthier versions are sold directly to schools [55]. These products are designed to look like their less-healthy counterparts and are not commonly available in grocery stores. Moreover, brands advertise the less nutritious versions of the same products through various forms of media accessed by school-aged children. A recent report concluded that this will likely lead to confusion among consumers about the nutritional quality of snacks [55].
Concerns have also been raised regarding the cost implications of transitioning to Smart Snacks standards. However, recent research estimating the cost-effectiveness of several obesity prevention policies found that nutrition standards for foods sold outside of school meals were one of only a few policies that saved more in terms of future health care costs than they would cost to implement [56•]. Further, a growing body of research suggests that improving the nutritional quality of CF does not negatively impact school food service budgets over time [57] with some studies finding that CF policies may increase a la carte sales, participation in the NSLP and SBP, and average meal revenue [46, 47, 58, 59]. Overall, innovative policy and program solutions and research efforts will be required to overcome each of these challenges (Table 2).
Other Policies and Programs to Support a Healthy School Food Environment
There are a number of other policies and programs in place at the national, state, and local levels impacting the school food environment. In this section, we touch on four programs that have been shown to positively influence children’s diet: Farm to School, USDA Foods, the USDA Fresh Fruit and Vegetable Program, and Local School Wellness Policies. Several other programs such as afterschool meals and snacks and summer food service can also play an important role in student’s diets, especially for those children qualifying for free and reduced-price meals; however, as these programs typically occur outside of the school day and often at non-school building sites, they were outside the scope of this paper.
Farm to School
Research has demonstrated that Farm to School (F2S) programs can play a role in the prevention of childhood obesity through increasing preferences for fruits and vegetables [60]. First emerging in the mid-1990s, F2S programs have grown rapidly over the past two decades [61, 62]. With this growth came national policy support and the inclusion of F2S provisions in the 2008 Farm Bill and the 2010 HHFKA [62]. The Farm Bill included a geographic preference provision, which permitted school food service directors to give preference to local vendors for the first time [63]. Similarly, the HHFKA encouraged participants in the NSLP and SBP to source some of their food from local or regional farmers [61] and established the USDA Farm to School grant program, which provides technical assistance to schools, as well as grants to develop or improve successful F2S programs [3]. To date, 221 F2S grants have been made by USDA [64]. Grantees primarily use these funds to buy healthy food, train staff, purchase equipment, deliver experiential education, and develop partnerships [64]. Data have also shown that schools with operational F2S programs report reduced plate waste, improved acceptance of healthier school meals, lower school meal program costs, and increased participation in the school meals program, among other benefits [65]. As such, F2S may be an important strategy for responding to concerns regarding cost and acceptance of updated school meal standards in addition to improving dietary intake and preventing obesity.
USDA Foods
USDA Foods, also called “entitlement” foods or commodities, provide an important opportunity for schools to offset some of the costs associated with the updated school meal nutrition standards [66, 67]. Schools participating in the NSLP or SBP are entitled to receive USDA Foods for each meal served. Research has shown that USDA foods comprised 20 % of all food served in school lunches and were the single largest ingredient in school meals [67]. Yet, many schools do not participate in the program or use their full entitlement [68]. Of the participating schools, approximately 82 % of entitlement dollars were spent on meat and cheese, whereas only 13 % of funds went to fruit, fruit juice, vegetables, and legumes [68]. Approximately 50 % of foods were externally processed to convert raw or bulk items into ready-to-use end products higher in added fat, sugar, and sodium [68].
The HHFKA directed USDA to analyze the quantity and quality of nutrition information available to schools on USDA Food Products and to submit a report to Congress, including recommendations to improve access to information [53]. USDA also agreed to develop model product specifications for external processing to minimize added sugar, fat, and sodium [3]. In 2011, USDA also made several improvements to the nutritional quality of products offered to schools, such as only providing canned fruits packed in extra light syrup or slightly sweetened fruit juice and reducing sodium content in a variety of foods [69].
Fresh Fruit and Vegetable Program
The USDA Fresh Fruit and Vegetable Program (FFVP) began in 2002 with the intent of increasing fruit and vegetable consumption among children in elementary schools, particularly those who are low income and at increased risk of overweight and obesity. Research has demonstrated that this program not only improves children’s attitudes about fruits and vegetables but also has a measurable, positive impact on consumption [70–73]. Students at schools participating in FFVP are more likely to report liking most fruits and trying new fruits and vegetables [73]. Additionally, they consumed about one third cup more of fruits and vegetables each day than students at non-participating schools, mostly in the form of raw fruits and vegetables [73]. Children at participating schools also had higher overall scores on the Healthy Eating Index and higher intakes of fruits and vegetables outside of school. Importantly, research has also demonstrated that the FFVP does not increase overall caloric intake, so the fruits and vegetables provided by the program may displace more calorie-dense, nutrient-poor foods in children’s diets [73]. Participating schools were also more likely to offer more nutrition education and have nutrition education messages posted throughout their school [73].
Local School Wellness Policies
As a result of the Child Nutrition and WIC Reauthorization Act of 2004, all local educational agencies were required to develop a Local School Wellness Policy (LSWP) to support healthy eating and physical activity in the school environment [74]. Research suggests that LSWPs may be associated with improved implementation of health-promoting practices in the school environment [75, 76] and increased consumption of healthier items among students [77]. However, research has also demonstrated that there may be room for improvement in LSWP development and implementation. Some studies have shown that school wellness policies prior to HHFKA may have been weakly worded and that schools may have been simply adopting standard wellness policy templates lacking strong nutrition standards [76, 78]. Further, geographic disparities in the strength and effectiveness of LSWPs may exist with rural schools particularly at risk [79, 80]. Some research has suggested that urban schools and schools with a higher percent of students on free and reduced-price lunch have higher quality wellness policies [75, 80].
The 2010 HHFKA strengthened the LSWP requirement by expanding the scope of wellness policies to promote health and prevent childhood obesity and increasing the accountability and transparency of policies [81]. USDA released a proposed rule in 2014, which establishes a framework for policy content, ensures stakeholder participation in policy development, and requires periodic compliance assessment and reporting on progress toward achieving the LSWP goals [81]. The proposed rule also requires each policy to include guidelines for the marketing of foods and beverages on the school campus during the school day consistent with nutrition standards for Smart Snacks [81].
Ongoing Challenges
Among these school food environment policies and programs, there are important gaps that should be addressed in future research, policy, and program efforts (Table 2). There is an ongoing need for technical assistance and training in many areas such as incorporating healthier USDA Foods into school meals, updating LWSPs and monitoring and evaluating their impact, and supporting F2S programs. Each of the above-mentioned programs play an important role in creating a healthy school food environment, and continued improvements through research and policy efforts are critical (Table 2).
Conclusions
Childhood obesity continues to be one of the most pressing public health issues in the USA today. This paper summarizes recent research demonstrating the critical role that school food programs and policies play in improving children’s diet, weight, and health. The school food environment is particularly powerful because of its unique ability to reach children most at risk of overweight and obesity through programs such as the NSLP, SBP, and FFVP. While significant progress has been made in recent years to improve the quality of foods and beverages provided in schools, there is still work to be done to ensure effective implementation of policy changes (Table 2).
Successful implementation efforts should focus on improving the whole school food environment in order to have the greatest possible impact on children’s health and well-being. Evaluation research is needed to examine the effectiveness of school-based nutrition policy and program changes and to determine which strategies are the most cost-effective and have the greatest impact. Pilot feasibility studies also may be helpful to quickly identify promising novel school-based approaches to improve dietary intakes and weight status among children and adolescents. The majority of published research focuses on children in grades K-8, and more intervention studies are needed on adolescents in middle and high schools.
The evidence is clear that school food policies and programs have the capacity to significantly improve children’s dietary intake and reduce their risk of chronic disease. However, in order to achieve large-scale, sustainable prevention of childhood obesity, multi-component, multi-level interventions that include not only schools but also communities, homes, and food retail environments will be needed [2]. Policies should strive to support effective programs that increase availability, accessibility, and consumption of healthy foods, while reducing less healthy CF. The combination of economic incentives along with specific policies can increase the likelihood that individual approaches will be effective [2].
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Kids’ Safe and Healthful Foods Project. The State of School Nutrition [Internet]. 2014 Jan 28 [cited 2015 November 10] Available from: http://www.pewtrusts.org/en/about/news-room/opinion/2014/01/28/the-state-of-school-nutrition.
Scientific Report of the 2015 Dietary Guidelines Advisory Committee. United States Department of Agriculture and Department of Health and Human Services; 2014.
Public Law 111–296, the Healthy, Hunger-Free Kids Act of 2010, Dec. 13, 2010.
School Breakfast Program [Internet]. United States Department of Agriculture; 2013 [updated 2013 July 26; cited 2015 November 18]. Available from: http://www.fns.usda.gov/sbp/program-history.
National School Lunch Act [Internet]. United States Department of Agriculture; 2015 [updated 2015 August 26; cited 2015 November 11]. Available from: http://www.fns.usda.gov/nslp/history_5.
National School Lunch Program: Participation and Lunches Served [Internet]. United States Department of Agriculture; 2015 [updated 2015 November 06; cited 2015 November 15]. Available from: http://www.fns.usda.gov/sites/default/files/pd/slsummar.pdf.
School Breakfast Program Participation and Meals Served [Internet]. United States Department of Agriculture; 2015 [updated 2015 November 6; cited 2015 November 15]. Available from: http://www.fns.usda.gov/sites/default/files/pd/sbsummar.pdf.
Egner R, Oza-Frank R, Cunningham SA. The school breakfast program: a view of the present and preparing for the future-a commentary. J Sch Health. 2014;84(7):417–20.
Anzman-Frasca S, Djang HC, Halmo MM, Dolan PR, Economos CD. Estimating impacts of a breakfast in the classroom program on school outcomes. JAMA Pediat. 2015;169(1):71–7.
Merlo C, Brener N, Kann L, McManus T, Harris D, Mugavero K. School-level practices to increase availability of fruits, vegetables, and whole grains, and reduce sodium in school meals-United States 2000, 2006, and 2014. Morb Mortal Wkly Rep. 2015;64(33):905–8. This report provides nationally representative data from the School Health Policies and Practices Study both pre- and post-HHFKA implementation in elementary, middle, and high schools.
Crepinsek MK, Gordon AR, McKinney PM, Condon EM, Wilson A. Meals offered and served in US public schools: do they meet nutrient standards? J Am Diet Assoc. 2009;109(2 Suppl):S31–43.
Public Law 111–296, the Healthy, Hunger-Free Kids Act of 2010, Section 203, Dec. 13, 2010.
Long C. Child nutrition reauthorization 2010: water availability during national school lunch program meal service. Alexandria: United States Department of Agriculture; 2011.
de Ruyter JC, Olthof Mr Fau - Seidell JC, Seidell Jc Fau - Katan MB, Katan MB. A trial of sugar-free or sugar-sweetened beverages and body weight in children. (1533–4406 (Electronic)).
Pan A, Malik Vs, Hao T, Willett WC, Mozaffarian D, Hu FB. Changes in water and beverage intake and long-term weight changes: results from three prospective cohort studies. (1476–5497 (Electronic)).
Kenney EL, Long MW, Cradock AL, Gortmaker SL. Prevalence of inadequate hydration among US children and disparities by gender and race/ethnicity: National Health and Nutrition Examination Survey, 2009–2012. (1541–0048 (Electronic)).
Terry-McElrath YM, O’Malley PM, Johnston LD. Foods and beverages offered in US public secondary schools through the national school lunch program from 2011–2013: early evidence of improved nutrition and reduced disparities. Prev Med. 2015;78:52–8. This study provides nationally representative data on the trends in foods and beverages offered in middle and high schools pre- and post-HHFKA.
School Meals: School Meal Certification Data [Internet]. United States Department of Agriculture; 2015 [updated 2015 October 26; cited 2015 November 5]. Available from: http://www.fns.usda.gov/school-meals/school-meal-certification-data.
Patel AI, Hecht K, Hampton KE, Grumbach JM, Braff-Guajardo E, Brindis CD. Tapping into water: key considerations for achieving excellence in school drinking water access. (1541–0048 (Electronic)).
Hood NE, Turner L, Colabianchi N, Chaloupka FJ, Johnston LD. Availability of drinking water in US public school cafeterias. (2212–2672 (Print)).
Turner L, Chaloupka FJ. Perceived reactions of elementary school students to changes in school lunches after implementation of the United States Department of Agriculture’s new meals standards: minimal backlash, but rural and socioeconomic disparities exist. Child Obes. 2014;10(4):349–56.
Terry-McElrath YM, Colabianchi, N, O’Malley PM, Johnston LD. First year of USDA school lunch meal standards: findings from US secondary schools. (Youth, Education, & Society Occasional Paper No. 7); 2014. Ann Arbor, MI: Institute for Social Research, 10 pp. Cohen Impact.
Cohen JF, Richardson S, Parker E, Catalano PJ, Rimm EB. Impact of the new U.S. Department of Agriculture school meal standards on food selection, consumption, and waste. Am J Prev Med. 2014;46(4):388–94.
Schwartz MB, Henderson KE, Read M, Danna N, Ickovics JR. New school meal regulations increase fruit consumption and do not increase total plate waste. Child Obes. 2015;11(3):242–7. This study uses strong methods to measure food consumption and plate waste both before and after policy changes resulting from the HHFKA.
Byker CJ, Farris AR, Marcenelle M, Davis GC, Serrano EL. Food waste in a school nutrition program after implementation of new lunch program guidelines. J Nutr Educ Behav. 2014;46(5):406–11.
Gase LN, McCarthy WJ, Robles B, Kuo T. Student receptivity to new school meal offerings: assessing fruit and vegetable waste among middle school students in the Los Angeles Unified School District. Prev Med. 2014;67 Suppl 1:S28–33.
Cullen KW, Chen TA, Dave JM. Changes in foods selected and consumed after implementation of the new National School Lunch Program meal patterns in southeast Texas. Prevent Med Rep. 2015;2:440–3.
Terry-McElrath YM, O’Malley PM, Johnston LD. Potential impact of national school nutritional environment policies: cross-sectional associations with US secondary student overweight/obesity, 2008–2012. JAMA Pediat. 2015;169(1):78–85.
Schwartz AE, Leardo M, Aneja S, Elbel B. Effect of a school-based water intervention on child body mass index and obesity. 2168–6211 (Electronic)).
Cummings PL, Welch SB, Mason M, Burbage L, Kwon S, Kuo T. Nutrient content of school meals before and after implementation of nutrition recommendations in five school districts across two U.S. counties. Prev Med. 2014;67 Suppl 1:S21–7.
Taber DR, Chriqui JF, Powell L, Chaloupka FJ. Association between state laws governing school meal nutrition content and student weight status: implications for new USDA school meal standards. JAMA Pediat. 2013;167(6):513–9.
Newman, C. The food costs of healthier school lunches. Agr Resource Econ Rev. 2012; 41(1):12–28.
Kids’ Safe and Healthful Foods Project. Serving healthy school meals: staff development and training needs. Washington: The Pew Charitable Trusts; 2015.
Kids’ Safe and Healthful Foods Project. Serving healthy school meals: U.S. schools need updated kitchen equipment. Washington: The Pew Charitable Trusts; 2015.
USDA Awards Grants to Support Schools Serving Healthier Meals and Snacks [Internet]. United States Department of Agriculture; 2015 [updated 2015 March 06; cited 2015 October 30]. Available from: http://www.usda.gov/wps/portal/usda/usdahome?contentidonly=true&contentid=2015/03/0058.xml.
Patel AI, Bogart LM, Elliott MN, Lamb S, Uyeda KE, Hawes-Dawson J, Klein DJ, et al. Increasing the availability and consumption of drinking water in middle schools: a pilot study. (1545–1151 (Electronic)).
Kenney EL, Gortmaker SL, Carter JE, Howe MC, Reiner JF, Cradock AL. Grab a cup, fill it up! An intervention to promote the convenience of drinking water and increase student water consumption during school lunch. (1541–0048 (Electronic)).
Patel AI, Chandran K, Hampton KE, Hecht K, Grumbach JM, Kimura AT, Braff-Guajardo E, et al. Observations of drinking water access in school food service areas before implementation of federal and state school water policy, California, 2011. (1545–1151 (Electronic)).
U.S. Department of Agriculture, “National School Lunch Program and School Breakfast Program: Nutrition Standards for All Foods Sold in School as Required by the Healthy, Hunger-Free Kids act of 2010; Interim Final Rule,” 7 C.F.R. 210, 220.
O’Toole TP, Anderson S, Miller C, Guthrie J. Nutrition services and foods and beverages available at school: results from the School Health Policies and Programs Study 2006. J Sch Health. 2007;77(8):500–21.
Johnston LD, O’Malley PM, Terry-McElrath YM, Colabianchi N. School policies and practices to improve health and prevent obesity: national secondary school results:school years 2006–07 through 2010–11. Volume 3. Bridging the Gap Program, Survey Research Center, Institute for Social Research, Ann Arbor MI; 2013.
Datar A, Nicosia N. Junk Food in Schools and Childhood Obesity. J Pol Anal Manag: J Assoc Pub Pol Anal Manag. 2012;31(2):312–37.
Fox MK, Condon E. School nutrition dietary assessment study IV. Alexandria, VA: United States Department of Agriculture; 2012. Available at: http://www.fns.usda.gov/sites/default/files/SNDA-IV_Findings_0.pdf. This study summarizes the findings from the most recent School Nutrition Dietary Assessment Study (SNDA), which used a nationally represenatitve sample to measure the nutrient content of meals served and the availability of competitive foods and beverages. This study is the most recent version of the SNDA series and therefore is a useful source for determining progress over time.
Bridging the Gap. Will the USDA’s school food standards make a difference in childhood obesity? Ann Arbor, MI; 2014.
Chriqui JF, Pickel M, Story M. Influence of school competitive food and beverage policies on obesity, consumption, and availability: a systematic review. JAMA Pediat. 2014;168(3):279–86. This study is a recent systematic review of the effects of competitive food and beverage policies on various outcomes. This review was conducted prior to Smart Snacks implementation.
Long MW, Henderson KE, Schwartz MB. Evaluating the impact of a Connecticut program to reduce availability of unhealthy competitive food in schools. J Sch Health. 2010;80(10):478–86.
Woodward-Lopez G, Gosliner W, Samuels SE, Craypo L, Kao J, Crawford PB. Lessons learned from evaluations of California’s statewide school nutrition standards. Am J Public Health. 2010;100(11):2137–45.
Taber DR, Chriqui JF, Chaloupka FJ. Differences in nutrient intake associated with state laws regarding fat, sugar, and caloric content of competitive foods. Arch Pediatr Adolesc Med. 2012;166(5):452–8.
Alaimo K, Oleksyk SC, Drzal NB, Golzynski DL, Lucarelli JF, Wen Y, et al. Effects of changes in lunch-time competitive foods, nutrition practices, and nutrition policies on low-income middle-school children’s diets. Child Obes. 2013;9(6):509–23.
Coffield JE, Metos JM, Utz RL, Waitzman NJ. A multivariate analysis of federally mandated school wellness policies on adolescent obesity. J Adoles Health Offic Pub Soc Adoles Med. 2011;49(4):363–70.
Riis J, Grason H, Strobino D, Ahmed S, Minkovitz C. State school policies and youth obesity. Matern Child Health J. 2012;16 Suppl 1:S111–8.
Sanchez-Vaznaugh EV, Sanchez BN, Baek J, Crawford PB. ‘Competitive’ food and beverage policies: are they influencing childhood overweight trends? Health Affairs (Project Hope). 2010;29(3):436–46.
Taber DR, Chriqui JF, Perna FM, Powell LM, Chaloupka FJ. Weight status among adolescents in States that govern competitive food nutrition content. Pediatrics. 2012;130(3):437–44.
Fox MK, Gordon A, Nogales R, Wilson A. Availability and consumption of competitive foods in US public schools. J Am Diet Assoc. 2009;109(2 Suppl):S57–66.
Harris JL, Schwartz MB, Shehan C, Hyary M, Appel J, Haraghey K, et al. Snack FACTS 2015: evaluating snack food nutrition and marketing to youth. UConn Rudd Center for Food Policy & Obesity; November 2015. Available at: http://www.uconnruddcenter.org/files/Pdfs/SnackFACTS_2015_Fulldraft02.pdf.
Gortmaker SL, Wang YC, Long MW, Giles CM, Ward ZJ, Barrett JL, et al. Three interventions that reduce childhood obesity are projected to save more than they cost to implement. Health Affairs (Project Hope). 2015;34(11):1932–9. This is a recent study evaluating the cost-effectiveness of various childhood obesity intervnetions and highlights the effectivess of competitive food and beverage policies. This study is unique because there are not many existing cost-effectiveness analyses of childhood obesity interventions.
Dr. Robert C., Atkins V. Center for weight and health. Dollars and sense: the financial impact of selling healthier school foods. Berkeley, CA; 2007. http://cwh.berkeley.edu/sites/default/files/primary_pdfs/Dollars_and_Sense_FINAL_3.07.pdf.
Peart T, Kao J, Crawford PB, Samuels SE, Craypo L, Woodward-Lopez G. Does competitive food and beverage legislation hurt meal participation or revenues in high schools? Child Obes. 2012;8(4):339–46.
Nollen NL, Kimminau KS, Nazir N. Demographic and financial characteristics of school districts with low and high a la Carte sales in rural Kansas Public Schools. J Am Diet Assoc. 2011;111(6):879–83.
Joshi A, Ratcliffe MM. Causal pathways linking Farm to School to childhood obesity prevention. Child Obes. 2012;8(4):305–14.
Nicholson L, Turner L, Schneider L, Chriqui J, Chaloupka F. State farm-to-school laws influence the availability of fruits and vegetables in school lunches at US public elementary schools. J Sch Health. 2014;84(5):310–6.
Feenstra G, Ohmart J. The evolution of the school food and farm to school movement in the United States: connecting childhood health, farms, and communities. Child Obes. 2012;8(4):280–9.
Geographic Preference Option for the Procurement of Unprocessed Agricultural Products in Child Nutrition Programs; Final Rule,” 7 C.F.R., 210, 215, 220, 225, 226.
Benson M, Russel M, Kane E. USDA Farm to School Grant Program FY 2013-FY 2015 summary of awards. Alexandria: United States Department of Agriculture; 2015.
The Farm to School Census [Internet]. United States Department of Agriculture; 2015 [cited 2015 October 28]. Available from: https://farmtoschoolcensus.fns.usda.gov.
Peterson C. A rotten deal for schools? An assessment of states’ success with the National School Lunch Program’s in-kind benefit. Food Pol. 2011;36:588–96.
Woodward-Lopez G, Kao J, Kiesel K, Lewis Miller M, Boyle M, Drago-Ferguson S, et al. Is scratch-cooking a cost-effective way to prepare healthy school meals with US Department of Agriculture foods? J Acad Nutr Diet. 2014;114(9):1349–58.
Hecht K, Samuels S, Sharp M, et al. The federal child nutrition commodity program: a report on nutritional quality. Oakland: California Food Policy Advocates; 2008.
United States Department of Agriculture. USDA foods: healthy choices for our schools [Internet]. 2011 [updated 2011 May; cited 2011 Oct 20]. Available from: http://www.fns.usda.gov/sites/default/files/8_USDAFHCFUS.pdf.
Jamelske E, Bica LA, McCarty DJ, Meinen A. Preliminary findings from an evaluation of the USDA Fresh Fruit and Vegetable Program in Wisconsin schools. WMJ Offic Pub State Med Soc Wiscon. 2008;107(5):225–30.
Ohri-Vachaspati P, Turner L, Chaloupka FJ. Fresh fruit and vegetable program participation in elementary schools in the United States and availability of fruits and vegetables in school lunch meals. J Acad Nutr Diet. 2012;112(6):921–6.
Davis EM, Cullen KW, Watson KB, Konarik M, Radcliffe J. A fresh fruit and vegetable program improves high school students’ consumption of fresh produce. J Am Diet Assoc. 2009;109(7):1227–31.
Bartlett S, Olsho L, Klerman J, et al. Evaluation of the Fresh Fruit and Vegetable Program (FFVP): final evaluation report. Alexandria: United States Department of Agriculture Food and Nutrition Service; 2013.
Team Nutrition: Local School Wellness Policy [Internet]. United States Department of Agriculture; 2015 [updated 2015 September 01; cited 2015 October 20]. Available from: http://www.fns.usda.gov/tn/local-school-wellness-policy.
Schwartz MB, Henderson KE, Falbe J, Novak SA, Wharton CM, Long MW, et al. Strength and comprehensiveness of district school wellness policies predict policy implementation at the school level. J Sch Health. 2012;82(6):262–7.
Belansky ES, Cutforth N, Delong E, Litt J, Gilbert L, Scarbro S, et al. Early effects of the federally mandated local wellness policy on school nutrition environments appear modest in Colorado’s rural, low-income elementary schools. J Am Diet Assoc. 2010;110(11):1712–7.
Nanney MS, MacLehose R, Kubik MY, Davey CS, Coombes B, Nelson TF. Recommended school policies are associated with student sugary drink and fruit and vegetable intake. Prev Med. 2014;62:179–81.
Lucarelli JF, Alaimo K, Belansky ES, Mang E, Miles R, Kelleher DK, et al. Little association between wellness policies and school-reported nutrition practices. Health Promot Pract. 2015;16(2):193–201.
Nanney MS, Davey CS, Kubik MY. Rural disparities in the distribution of policies that support healthy eating in US secondary schools. J Acad Nutr Diet. 2013;113(8):1062–8.
Caspi CE, Davey C, Nelson TF, Larson N, Kubik MY, Coombes B, et al. Disparities persist in nutrition policies and practices in Minnesota secondary schools. J Acad Nutr Diet. 2015;115(3):419–25.e3.
U.S. Department of Agriculture, “Local School Wellness Policy Implementation Under the Healthy, Hunger-Free Kids Act of 2010; Proposed Rule,” 7 C.F.R. 210, 220; Federal register, vol. 79, No.38 pg.10693.
United States Department of Agriculture. School meals: healthy hunger-free kids act [Internet]. 2014 [updated 2014 Mar 03; cite 2015 Nov 25]. Available from: http://www.fns.usda.gov/school-meals/healthy-hunger-free-kids-act.
Patel AI, Hampton KE. Encouraging consumption of water in school and child care settings: access, challenges, and strategies for improvement. Am J Public Health. 2011;101(8):1370–9.
Smith S, Wleklinski D, Roth SL, Tragoudas U. Does school size affect interest for purchasing local foods in the midwest? Child Obes. 2013;9(2):150–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Emily Welker, Megan Lott, and Mary Story declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Obesity Prevention
Rights and permissions
About this article
Cite this article
Welker, E., Lott, M. & Story, M. The School Food Environment and Obesity Prevention: Progress Over the Last Decade. Curr Obes Rep 5, 145–155 (2016). https://doi.org/10.1007/s13679-016-0204-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13679-016-0204-0