Abstract
Purpose of Review
Children’s eating behaviors are critical determinants of their dietary intake and, hence, childhood growth. Nutritional interventions among families with young children are focused on parents as agents of change, with interventions increasingly targeting family routines as drivers of children’s eating and health outcomes. This review describes studies that have acted on family routines in the context of preschoolers’ eating and growth, summarizes their findings, and discusses the limitations of current approaches to studying family routines and the implications for future research.
Recent Findings
We found that food availability and parental offering of foods have been modified by several interventions and linked to positive changes in child outcomes. Parent interventions have had success in reducing controlling feeding practices and improving self-efficacy related to child feeding, but these have not been associated with long-term change in child outcomes.
Summary
We conclude that opportunities exist to strengthen the definition, operationalization, and measurement of family routine variables. Improvements in fidelity and process evaluation measures will be important for more efficacious intervention development and dissemination.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Children’s eating behaviors are an important driver of their dietary intake and, hence, childhood growth. Eating behaviors that develop in childhood can persist into adulthood and influence nutrition across the life course [1, 2]. Early childhood is therefore a critical window to shape life-long eating behaviors and dietary patterns. The preschool years represent a developmental period when children are learning about food through repeated exposure, acquiring food preferences, developing the necessary motor skills to self-feed, and learning to exert these preferences and skills [3]. Early childhood is a period of rapid eating development that is concomitantly challenging and frustrating for caregivers [4, 5].
Among preschool children in the developed world, difficult eating behaviors, such as food neophobia, food refusal, and selective eating, are common [6]. These types of eating behaviors predictably emerge between ages 2 and 5 years [7] and are associated with nutritional problems that are widespread among preschool children, such as inadequate fruit and vegetable intake and mixed associations with growth [8,9,10,11]. The preschool years are an opportune time to intervene on eating because children in this age group are increasingly autonomous in making choices about how much and what to eat, yet their adult caregivers still exert a high degree of control over the environment [12].
Extensive evidence supports that parents can shape children’s eating and growth [12], and thus, nutritional interventions among families with preschoolers are increasingly focused on parents as agents of change [13]. Numerous clinic-, center-, and community-based interventions in this population target outcomes such as parent knowledge of children’s nutritional requirements or parents repeatedly exposing their children to vegetables [14,15,16]. Findings from these studies are mixed; some show a positive intervention effect on children’s eating or growth, while many do not [17, 18]. The variability in effectiveness of interventions has been ascribed to their differing theoretical frameworks, differences in implementation and fidelity of the interventions, as well as wide variation in the outcomes assessed (and the rigor of these assessments) across interventions [19].
One novel and promising approach to improving children’s eating is to help parents to create and sustain family routines [20]. Routines previously have been conceptualized as “the activities we do each day from the time we wake up to the time we go to sleep again at night” [21]. Research in the fields of education and psychology has long shown that the structure, security, and stability provided by routines support the development of positive behaviors and academic achievement among children [22,23,24]. In general, caregiving routines can establish predictable environments which, in turn, support learning through experience and choice—key aspects for young children’s development [24]. In the study of developmental aspects of children’s eating behaviors, cross-sectional, qualitative, and longitudinal studies document a relationship between eating-related family routines and children’s nutrition outcomes [25,26,27,28,29,30]. Understanding the relations between family routines and children’s outcomes and identifying essential elements of routines and their relative impacts will be crucial for establishing effective interventions to improve children’s eating.
In recent years, a number of interventions have been designed to act on family routines as a way to promote healthy eating and growth among preschool children. No reviews to date have examined the types of family routines studied or the effectiveness of these interventions. The purpose of the current review is to describe the studies that have acted on family routines in the context of eating and growth among preschool children, to summarize their findings, and to discuss the limitations of current approaches to studying family routines and the implications for future research.
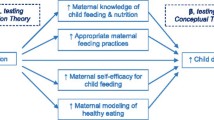
We define family routines as the way families behave and organize themselves to achieve their goals and specifically concentrate on the variables that shape family routines related to eating (see Fig. 1), as defined below:
-
1.
Home environment routines: We focused on food availability, defined as the presence of particular foods in the home.
-
2.
Parent feeding routines: We identified the behaviors and approaches used by parents to:
-
(a)
Feed their children (parent feeding practices and styles)
-
(b)
Model eating behaviors for their children such that, when observed by children, they generate and shape eating-related social norms for the family (role modeling)
-
(c)
Create structure related to food and eating (mealtime routines)
-
(d)
Determine how and when foods are offered to children (parental offerings of foods)
Last, we also included the construct of parental self-efficacy, defined as confidence in the ability to exercise control over one’s behaviors and to consistently enact those behaviors [31]. Self-efficacy is focal to Social Cognitive Theory (SCT)—a common theoretical framework for interventions aiming for behavior change. Bandura posited that self-efficacy is an essential component of “triadic reciprocality”: personal factors, behavior, and environmental influences which interact to produce behavior change [32]. We therefore conceptualized that self-efficacy would be an important element to include when considering the effectiveness of interventions aimed at family routines and their impacts on child eating and growth outcomes.
The primary questions addressed in this review are:
-
1.
What family routines have been studied in the context of nutritional interventions among preschool children?
-
2.
Were these studies effective at modifying family routines and, if so, do changes in family routines mediate the relationship between intervention impacts and child eating or growth?
-
3.
How can the limitations of current approaches to studying family routines in nutritional research be addressed to move the field forward and support optimal child eating and growth?
Methods
Search Strategy
A search was conducted of two databases: Ovid Medline and Embase. The search strategy was designed to identify peer-reviewed articles that described home-based interventions, targeting family routines related to child eating, among families with preschool-aged children. The search was limited to human studies, in English, published between January 1, 2000, and July 15, 2016 (see Table 1). The age range was restricted to the category “Preschool Child: 1–6 years” in Embase and “Preschool Child (2 to 5 years)” in Ovid Medline. Observational, cross-sectional, and qualitative studies, as well as papers that were not an original research article, were excluded. Pilot and feasibility studies were excluded unless the study design was a randomized controlled trial. Methods papers that did not include any results and review papers were read to identify the types of family routines that have been evaluated and the tools used to measure those routines, and then excluded. Studies that were conducted in a developing country or focused solely on a special needs population (e.g., children with developmental delays) were excluded. Findings were categorized and reported by type of family routine: (1) home environment routines (including food availability) and (2) parent feeding routines (including feeding practices and styles, role modeling, mealtime routines, and parent offering of foods). Also considered was whether self-efficacy was measured as a central outcome or a mediator of other intervention outcomes. Studies that targeted any of the above family routines as part of the intervention, as well as studies that actually measured the above family routines at baseline and post-intervention, were included in the final list of publications for this review. For each publication, the following data were extracted and entered into a spreadsheet: year of publication, study population (sample size, age range, ethnicity, parent income or education level, urban or rural location, country), study design, intervention description, length of follow-up, outcomes, instruments, findings, author-reported limitations, the types of routines that were intervened on or measured, inclusion of the theoretical framework in intervention design and assessment, and fidelity and process evaluation measures. Studies in the spreadsheet were then grouped by the type of family routine they addressed and further sub-divided into studies that showed a positive intervention effect and those that did not. In four cases, the articles referred to other publications which reported other findings from the studies’ primary or secondary aims. These articles (n = 8) were then added to the list of studies, and the same information as above was extracted from each article.
Results
Summary of Included Studies
The search strategy yielded 1946 articles. The 26 original articles and 1 abstract that met the inclusion criteria are summarized in Table 2. The table includes the study design and population, intervention duration, assessment time points, family routines targeted by the intervention, and a brief description of the intervention methods. Also included in Table 2 are outcomes and how they were measured, findings, and author-reported limitations, use of theory in intervention design, measurement of implementation fidelity, and process evaluation. All of the studies evaluated an intervention, and all but two studies were randomized controlled trials. The majority of studies were conducted in the USA and Australia; the remaining studies were conducted in the UK, Canada, Denmark, and the Netherlands. Of the 26 studies, ten reported changes in body size or composition and 21 reported changes in dietary intake among children from pre- to post-intervention. Approximately one third of the interventions targeted a population at increased risk for poor nutritional outcomes. While many of the interventions targeted routines related to physical activity, sedentary behavior, or sleep, we limited the findings for this review to eating-related family routines. Intervention varied considerably in their intensities (from telephone to in-person contacts), and content was implemented via a variety of strategies which included group sessions, home visits, individual consultations, mailed interactive kits, telephone-based motivational interviewing, newsletters, print materials, and online modules. Almost all interventions targeted at least two family routines. Assessments of family routine and eating-related variables were undertaken using validated questionnaires, modified versions of validated questionnaires, or questions that were not yet validated and had been developed specifically for the study. Children’s weight status was primarily assessed using anthropometry. Length of follow-up in the studies ranged from immediately post-intervention to 2 years, with most studies conducting assessments at baseline and post-intervention only.
Home Environment Routines
Food Availability
Interventions that targeted food availability included in-person, online, and telephone-based education, along with print materials, to target the availability of fruits and vegetables, non-core or high-calorie foods, and/or nutritious snacks. All but one of these studies [35] were randomized controlled trials and used short surveys or single questions to assess food availability; only one study measured food availability by direct observation [49]. Six studies focused on increasing availability of foods that promote healthy eating and growth. The High 5 for Kids study showed that, compared to controls, intervention parents reported a significantly greater increase in the availability of eight different fruits and vegetables in the home (0.45 vs. 0.26 fruits and vegetables) [35]. The EMPOWER intervention had a similar effect on F/V availability in intervention, vs. control, families [38, 39••]. Among participants in the Kind, Assertive, Neutral, Dependable, and Open-Minded parenting (KAN-DO) study, there was a non-significant trend towards greater improvements in healthy food availability in the intervention vs. control arm [45]. The Learning about Activity and Understanding Nutrition for Child Health (LAUNCH) study documented short-term improvements in household F/V availability that were not sustained at the 12-month follow-up [49]. The Be Active, Eat Right study [53] had no impact on the availability of healthy foods in the household. The Healthy Habits study reported no intervention effects on F/V availability; however, availability mediated F/V intakes at the 12-month follow-up [57•].
Four studies focused on reducing availability of foods that are recommended to be eaten in limited amounts, or non-core foods. In the LAUNCH study, the authors reported significantly greater decreases in the number of high-calorie foods available in intervention, vs. control, households (−1.3 vs. −0.1 high-calorie foods) [49]. In the Miranos! Look at us! We are Healthy! study, parents in the home-based intervention group reported that their children consumed fewer sodas, candy, sugar-sweetened beverages, and sweets compared to children in the control conditions [47, 48]. The Be Active, Eat Right study had no impact on household availability of unhealthy foods [53]. Similarly, the Healthy Habits intervention targeted and measured non-core food availability, but no long-term effect of the intervention on non-core food availability was noted [57 •, 58 •, 59].
All of the studies reported here measured child eating, dietary intake, and/or anthropometric outcomes, and some produced a favorable effect. This included increases in fruit or vegetable intake [35, 38, 39 ••, 55, 57 •, 58 •], short-term decreases in non-core food intake [59], and greater decreases in BMI z-score [49] or body fatness [44] for children in the intervention groups.
Routines of Parent Feeding
Parenting Practices and Styles
Interventions focusing on feeding styles and practices included telephone-based and in-person health education, as well as print and computerized educational materials. Randomized controlled trials and one randomized nested cohort study assessed the effect of the interventions on feeding practices and styles, most often measured by the self-report measure, the Child Feeding Questionnaire [61], or items developed for the particular study. In KAN-DO, Østbye and colleagues evaluated the effect of a parenting intervention on feeding styles and practices and reported that instrumental and emotional feeding significantly decreased in intervention mothers [45]. A study conducted by Hart and colleagues [36] also evaluated changes in parent feeding practices following the Confident Body, Confident Child (CBCC) intervention to promote healthy eating and weight management. After controlling for baseline scores, significant differences in instrumental feeding (coercion or bribes), emotional feeding, and pushing to eat (most often termed pressure to eat) were noted between intervention parents and active and wait-list controls [36]. Harvey-Berino and Rourke assessed the effect of an obesity prevention plus parenting support intervention on parent feeding practices and showed that intervention mothers reported decreases in restrictive feeding practices over time [37]. Essery and colleagues similarly found that a mailed newsletter intervention was effective at reducing pressure to eat, but had no impact on other feeding practices [33], and Wyse and colleagues also reported significant differences in pressure to eat post-intervention, between treatment and control families, in the Healthy Habits study [57 •]. An evaluation of the Parents and Tots Together intervention by Walton et al. documented that, compared to controls, intervention parents used food as a reward significantly less frequently post-intervention; however, this finding was not sustained at 9-month follow-up [54, 62]. Lastly, the Mind, Exercise, Nutrition, Do It! (MEND 2–4) for families of preschoolers focused on parenting practices (e.g., managing fussy behaviors) but has not yet reported impacts on parenting practices.
Other studies reported no intervention effect on parent feeding styles or practices. Haire-Joshu et al. examined the effect of H5-KIDS (High 5 for Preschool Kids) on non-coercive feeding practices [35]. While the intervention was designed to promote the use of non-coercive feeding practices, the authors found that use of non-coercive feeding practices actually decreased among intervention parents. In a study among obese children with at least one overweight parent, Stark and colleagues reported that parents exposed to the LAUNCH intervention showed no change in restrictive feeding practices or pressure to eat over the course of the study [49]. However, the authors documented a significantly greater decrease in authoritative and permissive parenting styles among intervention vs. control parents.
Six of these eight studies measured child eating, dietary intake, and/or anthropometric outcomes. From pre- to post-intervention, six of the studies reported a significant and positive intervention effect, including decreases in child neophobia and improvements in satiety responsiveness [46 •], and increases in fruit and vegetable intake among children [57 •], although in the case of High 5 for Kids, only for normal-weight children and not for overweight children [35]. As underweight children did not comprise a large percentage of the sample, a specific determination could not be made for the effects on underweight children. Further, decreases in children’s energy intake [37] and in child BMIz [49] were also reported. It should be noted that only in the case of the Healthy Habits intervention [59] was change in parent child-feeding strategies specifically tested as a mediator of improvements in child outcomes. In Healthy Habits, parent-reported child-feeding strategies (restriction and coercive practices) were mediators of how the intervention influenced the consumption of non-core foods.
Role Modeling
The majority of studies that evaluated the effect of role modeling did so utilizing telephone-based or face-to-face interventions. Most of these interventions targeted and measured modeling of fruit and vegetable intake; two interventions targeted, but did not measure, role modeling [37, 48]. Typically, role modeling has been measured using a one- or two-item survey or by measuring the mother’s dietary intake with a dietary recall or the Food Behavior Checklist, which does not specifically measure the extent to which adults and children eat together [63]. Two studies, Healthy Habits and H5-KIDS, evaluated the number of times per week parents consumed fruits and vegetables in front of their children [35, 57 •]. The evaluation of H5-KIDS did not document a change in role modeling of consumption from pre- to post-intervention, though an increase in overall parent F/V consumption was reported. In Healthy Habits, neither role modeling nor parent intake of F/V was different between intervention and control groups at any point post-intervention [57 •, 58 •, 60]. The KAN-DO study reported an intervention effect for mothers’ fruit and vegetable intakes [45]. Two studies used intervention messages to promote positive role modeling related to eating, but did not report whether the intervention modified parental role modeling behaviors [37, 47, 59].
All seven of these studies measured dietary intake. Three interventions reported reductions in energy or non-core food intake [37, 42, 59], two interventions described increases in fruit and vegetable intake [35, 57 •], and one intervention found greater decreases in fruit and vegetable intake in the control group compared to the intervention group [42]. Two studies investigated the effects of parental role modeling as a mediator of child dietary intake, and one noted significant positive effects of role modeling on children’s F/V intake [42].
Mealtime Routines
A wide range of mealtime behaviors and routines were targeted and/or evaluated, including eating dinner together as a family, mealtime atmosphere, the frequency of television viewing during dinner, meal planning, preparing dinner at home, mealtime rules, and mealtime structure and rules. Some intervention studies specifically targeted mealtime routines and included their measurement while others included messaging and content related to mealtime routines but did not measure or assess change in mealtime behaviors as part of intervention effects. One of the most frequently studied family routines is eating dinner together as a family. Nine studies measured the frequency of family meals [34, 36, 43, 45, 47, 52, 53, 56, 59]. However, only one intervention, Health Exercise Nutrition for the Really Young (HENRY), reported a positive impact on the frequency of family meals [56].
The CBCC study assessed the atmosphere of family mealtimes, including whether mealtimes provided structure and social support, but atmosphere did not vary across intervention and control groups post-intervention [36]. The Healthy Start study assessed mealtime social climate (cozy vs. conflict-ridden mealtimes); the effects of the intervention on this variable were not reported [43]. Four studies evaluated the intervention effect on television usage during dinner. Three of the studies described a significant intervention effect on children eating a snack or dinner in front of the television or television viewing during family meals [36, 45, 56], while one study showed no effect [52]. The Healthy Habits intervention targeted television viewing during dinner; however, change in this variable was not evaluated from pre- to post-intervention [57 •].
A small number of studies also targeted meal planning [42, 52, 59] and preparing dinner at home [45, 52]. Three of the four studies did not measure change in these mealtime behaviors over time, while one reported no significant change from pre- to post-intervention [52].
The Be Active, Eat Right study [53], the Hassle Free Mealtimes/Triple P study [41], and the MEND 2–4 study [64] targeted rules and consistency related to mealtimes. van Grieken et al. showed that intervention, compared to control, families had more rules for healthy and unhealthy behaviors post-intervention [53]. Skouteris and colleagues included a workshop for parents about the importance of consistency related to mealtimes, but did not measure a corresponding variable, and therefore, it cannot be ascertained whether mealtime structure and rules were influenced by the intervention [46 •, 64]. Morawska and colleagues reported significant intervention effects but none related to mealtime practices and routines [41].
Eleven of the 13 articles in this content area reported measures of eating, dietary intake, and/or anthropometric outcomes among children, and five of the interventions resulted in significant changes from pre- to post-intervention. Changes included increases in fruit and vegetable intake [46 •, 56, 57 •], satiety responsiveness [46 •], and reductions in food neophobia [46 •], non-core food intake [59], and BMI [34]. One intervention found greater decreases in fruit and vegetable intake among control vs. intervention children [52]. No study reported a direct or mediational effect of mealtime routines on child outcomes.
Parental Offering of Foods
Five studies addressed both the availability of foods in the household as well as how and when parents offered foods to their children. Three studies showed that parental offering of fruits and vegetables was positively affected by the interventions [52, 57 •, 59], while another did not [55]. Both the Family Ties to Health [46 •] and the Healthy Habits [57 •, 59] interventions separately assessed the effects of F/V availability and parental offering of F/V to their children, though only the Healthy Habits study reported a significant association with children’s F/V intakes. Two studies evaluated or used intervention messages to target parental offering of fruits and vegetables, but the findings related to this variable have not yet been published [43, 52]. The Eat Well Play Hard study reported increases in parental offering of vegetables and low-fat milk, which was associated with small increases in vegetable intake, child-initiated vegetable snacking, as well as increased consumption of low-fat milk at home [55].
Self-efficacy
Studies evaluating the effect of in-person, online, telephone-based interventions that contained self-efficacy in the model included six randomized controlled trials and one cohort pre-test, post-test design. Self-efficacy was measured using several different surveys including the Child Adjustment and Parent Self-Efficacy scale, the Parental Self-Efficacy for Child Diet scale, the Parenting Self Agency Measure, and surveys developed specifically for studies. Positive intervention effects were reported for self-efficacy for handling emotional and behavioral behaviors (applied to mealtime) [41], preparing healthy meals and encouraging children to eat healthy foods before unhealthy ones [52], encouraging “good behavior,” and setting limits related to mealtimes [56]. However, other interventions were not successful with respect to influencing self-efficacy for recognizing the child’s satiety cues (measured by a single item developed for the study) [62], providing a healthy diet, and solving problems with their child’s eating habits [59].
Five of the six studies measured children’s dietary intake and/or anthropometric outcomes. No study reported significant associations between changes in parent self-efficacy and children’s intake of F/V or BMIz, and few examined self-efficacy as a mediator of intervention effects on child outcomes. While the Healthy Habits study reported a significant relation between parent self-efficacy and children’s consumption of non-core foods, the intervention did not impact significantly parent self-efficacy itself [59].
Discussion
We examined the evidence for effectiveness of interventions that have focused on creating and strengthening family routines designed to improve children’s eating behaviors, dietary intake, and growth. It should be noted that the majority of interventions included in this review used routines to augment children’s consumption of healthy foods and have done so in the context of obesity prevention or treatment (rather than the spectrum of child growth), though only half collected data related to children’s weight outcomes. We concentrated on childhood obesity because of its escalation globally over the last four decades [65] and because of the increase in funding mechanisms focused on preventing early childhood obesity during the time period specified in our search (2000–2016). We identified studies reporting on 18 interventions, most of which were randomized controlled trials and six of which reported on data collection periods that were a year or more post-intervention.
We examined family routines that included food availability (both healthy and non-core foods), parent feeding practices and styles, parent role modeling, mealtime routines (e.g., frequency of family meals), and parental offering of foods (primarily fruits and vegetables); we further explored whether self-efficacy played a role in the effectiveness of the interventions. A number of interventions reported positive impacts on both food availability and parent offering of foods, and both constructs were associated with increases in children’s intake of both healthy and unhealthy foods. Changes in food availability and offering of foods were the only constructs associated with small changes in child weight status across all interventions [44, 49]. One study reported positive effects of offering food to children, over and above those reported for having the food available in the home [57 •]. These findings align with Social Cognitive Theory which suggests that environmental and behavioral components interact (along with personal factors) to explain behavior change [32]. In this case, purchasing and making foods available is an initial step towards impacting children’s dietary intake, but making the foods salient and accessible by actively offering them to children may increase the impact of the environmental effects. However, none of the studies reported sustained effects on children’s food intake, suggesting that one-time interventions are insufficient to produce lasting changes in children’s dietary intake.
A number of studies reported intervention effects on parenting practices and styles, particularly the reduction of controlling and restrictive feeding practices [33, 36, 37, 45, 57 •, 58 •]. Several interventions referred to content related to improving mealtime atmosphere and structure, but results of this facet of the interventions were largely null [35, 49] or unreported. The existing child-feeding practices literature has principally focused upon the negative impact of controlling feeding practices on children’s eating and weight outcomes [66]. Instruments which measure feeding practices most often document use of negative strategies and are dependent upon parent self-report (e.g., [61]), which could lead to social desirability response bias and obscure true intervention effects. Alternatively, it may be that reduction in use of restrictive practices is not sufficient to improve children’s eating and that concurrently helping parents with supportive feeding practices, i.e., “catching parents doing something right,” could be useful to explore in addition to diminishing unproductive strategies.
Limited support was found for the effects of interventions on parental role modeling, and only one study found evidence of a linkage between changes in role modeling and child outcomes [42]. Role modeling was operationalized and measured inconsistently across interventions. In some, parent self-reports of consumption of foods were assumed to be a proxy for role modeling intake of those foods; in others, role modeling was specified as a process of consuming a food at a meal with their children. The extent to which role modeling was an active process (i.e., engaging with the child and drawing the child’s attention to the fact that the parent is eating that food) was, for the most part, undefined. Because of the lack of specificity in defining role modeling, its measurement was also highly variable and included quantifying foods consumed, frequency of family meals in which specific foods were consumed, and survey items which asked whether role modeling occurred. It did not, however, include any measurement of sibling impacts, which may also be important in considering role modeling. Given the variability in definition and measurement, the extent to which role modeling is an effective part of interventions cannot be determined.
Mealtime routines included a large range of examples and were most frequently operationalized as eating together as a family. Numerous observational studies have linked family meals to positive child outcomes, including nutritional, scholastic, and behavioral benefits [67]. Of the interventions reviewed here, only one resulted in improvements in the frequency of family meals [56]. Other dimensions of mealtime routines were, for the most part, not measured or reported as part of intervention impacts and none evaluated the relationship between changes in family meals and child outcomes.
Mixed results were reported for intervention impacts upon parental self-efficacy with positive impacts being reported for efficacy for preparing healthy meals, managing difficult mealtime behaviors, and setting limits related to mealtime and eating [41, 52, 56]. Self-efficacy is a central component of Social Cognitive Theory and, as a personal factor in this theoretical framework, interacts with both environmental and behavioral factors. However, an individual’s self-efficacy varies across behaviors; that is, high efficacy to make healthy food available does not necessarily confer the same level of efficacy on preparation and ability to eat together as a family. Therefore, the measurement of self-efficacy must parallel the goal and content of the intervention and the specific behaviors which are targeted for intervention. In the studies we examined, measurement of this construct ranged from general parenting agency to efficacy that was quite specific to the behavior and rarely was it examined in relation to changes in the target behavior, environment, or child outcome.
A strength of most of the studies was that they were randomized controlled trials and that some included longitudinal follow-up to ascertain the duration of intervention effects. The majority based their intervention design upon a theoretical framework, most often Social Cognitive Theory, and attempted to measure many components of the models. Some studies targeted or included diverse populations who are at risk for health disparities.
All studies have their shortcomings. Common limitations included (1) poor definition, and therefore inconsistent operationalization, of the routine constructs; (2) assessments with low specificity or limited evidence of psychometric performance; and (3) analytic methods that were not, in general, designed to test the effects of routines (either directly or in mediation models) on child outcomes. Very few studies collected or reported fidelity measures, and therefore, the ineffectiveness of the intervention, or the degree and rigor with which it was delivered, often could not be distinguished. Likewise, the presence and quality of process evaluation were often insufficient and not discussed in relation to intervention findings.
Implications for Future Research
Child eating behaviors, food intake, and weight outcome are influenced by a complex set of environmental and behavioral variables and therefore require multicomponent interventions to effect changes in their status. However, complex interventions are difficult to design, implement, and assess in a manner that allows for the estimation of effects of individual intervention components. Beyond the need for improvements in construct definition, operationalization, assessment, and increased sophistication of intervention analyses, the application of implementation science principles that include careful measurement of fidelity and processes of implementation will advance the delivery and efficacy of interventions [68]. These processes, when applied rigorously, help to determine dosage, reach, and quality of intervention delivery but also illuminate barriers to program implementation and opportunities for improvements in intervention effectiveness. Implementation science moves beyond outcome evaluation (i.e., results only) and progresses towards understanding the context and mechanisms related to intervention findings. It also provides opportunities for identifying adaptations that could improve effectiveness of the existing intervention, rather than necessarily leading to development of additional intervention programs. As demonstrated in the studies presented here, the inclusion of additional implementation techniques could greatly improve our understanding of intervention outcomes related to family routines, children’s eating, and growth outcomes.
Conclusions
Some evidence was found for the potential to successfully intervene upon family routines, particularly home environment routines as well as some parent feeding routines. Interventions reported positive impacts on parental self-efficacy related to food preparation, managing children’s problem behaviors and, to some extent, for developing limits and structure for mealtimes. However, in very few cases were the impacts upon family routines tested for their relation to changes in intervention outcomes. Opportunities to advance the science related to family eating routines and child outcomes include the exploration of mediation and moderation analyses of existing studies, and the inclusion of these variables in the design of future studies to improve our understanding of intervention findings. The application of implementation science principles could speed the development and dissemination of effective programs.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Lytle LA, Seifert S, Greenstein J, McGovern P. How do children’s eating patterns and food choices change over time? Results from a cohort study. Am J Health Promot. 2000;14(4):222–8.
Mikkilä V, Räsänen L, Raitakari OT, et al. Major dietary patterns and cardiovascular risk factors from childhood to adulthood. The Cardiovascular Risk in Young Finns Study. Br J Nutr. 2007;98(1):218–25.
Nicklaus S. The role of food experiences during early childhood in food pleasure learning. Appetite. 2016;104:3–9.
Johnson SL, Goodell LS, Williams K, Power TG, Hughes SO. Getting my child to eat the right amount. Mothers’ considerations when deciding how much food to offer their child at a meal. Appetite. 2015;88:24–32.
Goodell LS, Johnson SL, Antono AC, Power TG, Hughes SO. Strategies low-income parents use to overcome their children’s food refusal. Mat Child Health J. 2016:1–9.
Carruth BR, Skinner J, Houck K, Moran J, Coletta F, Ott D. The phenomenon of “picky eater”: a behavioral marker in eating patterns of toddlers. J Am Coll Nutr. 1998;17(2):180–6.
Birch LL, Fisher JO. Development of eating behaviors among children and adolescents. Pediatrics. 1998;101(3 Pt 2):539–49.
Skinner JD, Carruth BR, Bounds W, Ziegler P, Reidy K. Do food-related experiences in the first 2 years of life predict dietary variety in school-aged children? J Nutr Educ Behav. 2002;34(6):310–5.
Nicklaus S, Boggio V, Chabanet C, Issanchou S. A prospective study of food variety seeking in childhood, adolescence and early adult life. Appetite. 2005;44(3):289–97.
Brown CL, Vander Schaaf EB, Cohen GM, Irby MB, Skelton JA. Association of picky eating and food neophobia with weight: a systematic review. Childhood Obesity. 2016;12(4):247–62.
Shim JE, Yoon JH, Kim K, Paik HY. Association between picky eating behaviors and growth in preschool children. Journal of Nutrition and Health. 2013;46(5):418–26.
Ventura AK, Birch LL. Does parenting affect children's eating and weight status? Int J Behav Nutr Phys Act. 2008;5:15.
Golan M, Weizman A. Familial approach to the treatment of childhood obesity: conceptual model. J Nutr Educ Behav. 2001;33(2):102–7.
Caton SJ, Ahern SM, Remy E, Nicklaus S, Blundell P, Hetherington MM. Repetition counts: repeated exposure increases intake of a novel vegetable in UK pre-school children compared to flavour–flavour and flavour–nutrient learning. Br J Nutr. 2013;109(11):2089–97.
Fildes A, van Jaarsveld CH, Wardle J, Cooke L. Parent-administered exposure to increase children's vegetable acceptance: a randomized controlled trial. J Acad Nutr Diet. 2014;114(6):881–8.
Johnson SL. Developmental and environmental influences on young children’s vegetable preferences and consumption. Adv Nutr: An Inter Rev J. 2016;7(1):220S–31S.
Collins C, Duncanson K, Burrows T. A systematic review investigating associations between parenting style and child feeding behaviours. J Human Nutr Diet. 2014;27(6):557–68.
Keller KL. The use of repeated exposure and associative conditioning to increase vegetable acceptance in children: explaining the variability across studies. J Acad Nutr Diet. 2014;114(8):1169–73.
Schlechter CR, Rosenkranz RR, Guagliano JM, Dzewaltowski DA. A systematic review of children's dietary interventions with parents as change agents: application of the RE-AIM framework. Prev Med. 2016;91:233–43.
Spagnola M, Fiese BH. Family routines and rituals: a context for development in the lives of young children. Infants Young Children. 2007;20(4):284–99.
Weisner T. The ecocultural family interview: new conceptualizations and uses for the study of illness. Padova: University of Padova Press; 2011.
Burchinal MR, Peisner-Feinberg E, Pianta R, Howes C. Development of academic skills from preschool through second grade: family and classroom predictors of developmental trajectories. J School Psychol. 2002;40(5):415–36.
Network NECCR. Relations between family predictors and child outcomes: are they weaker for children in child care? Dev Psychol. 1998;34(5):1119–28.
Shonkoff JP, Phillips DA. From neurons to neighborhoods: the science of early childhood development. Washington: National Academies Press; 2000.
Anderson SE, Whitaker RC. Household routines and obesity in US preschool-aged children. Pediatrics. 2010;125(3):420–8.
Berge JM, Hoppmann C, Hanson C, Neumark-Sztainer D. Perspectives about family meals from single-headed and dual-headed households: a qualitative analysis. J Acad Nutr Diet. 2013;113(12):1632–9.
Brown R, Ogden J. Children’s eating attitudes and behaviour: a study of the modelling and control theories of parental influence. Health Educ Res. 2004;19(3):261–71.
Pearson N, Biddle SJ, Gorely T. Family correlates of fruit and vegetable consumption in children and adolescents: a systematic review. Public Health Nutr. 2009;12(2):267–83.
Rasmussen M, Krølner R, Klepp KI, et al. Determinants of fruit and vegetable consumption among children and adolescents: a review of the literature. Part I: quantitative studies. Int J Behav Nutr Phys Act. 2006;3:22.
Campbell K, Hesketh K, Silverii A, Abbott G. Maternal self-efficacy regarding children's eating and sedentary behaviours in the early years: associations with children's food intake and sedentary behaviours. Int J Pediatr Obes. 2010;5(6):501–8.
Bandura A. Human agency in social cognitive theory. Am Psychol. 1989;44(9):1175.
Bandura A. Social foundations of thought and action: a social cognitive perspective. Princeton-Hall: Englewood Cliffs; 1986.
Essery EV, DiMarco NM, Rich SS, Nichols DL. Mothers of preschoolers report using less pressure in child feeding situations following a newsletter intervention. J Nutr Educ Behav. 2008;40(2):110–5.
Haines J, McDonald J, O'Brien A, et al. Healthy habits, happy homes: randomized trial to improve household routines for obesity prevention among preschool-aged children. JAMA Pediatr. 2013;167(11):1072–9.
Haire-Joshu D, Elliott MB, Caito NM, et al. High 5 for Kids: the impact of a home visiting program on fruit and vegetable intake of parents and their preschool children. Prev Med. 2008;47(1):77–82.
Hart LM, Damiano SR, Paxton SJ. Confident body, confident child: a randomized controlled trial evaluation of a parenting resource for promoting healthy body image and eating patterns in 2- to 6-year old children. Int Eat Disorders. 2016;49(5):458–72.
Harvey-Berino J, Rourke J. Obesity prevention in preschool Native-American children: a pilot study using home visiting. Obes Res. 2003;11(5):606–11.
Knowlden A, Sharma M. One-year efficacy testing of Enabling Mothers to Prevent Pediatric Obesity Through Web-Based Education and Reciprocal Determinism (EMPOWER) randomized control trial. Health Educ Behav. 2016;43(1):94–106.
•• Knowlden AP, Sharma M, Cottrell RR, Wilson BR, Johnson ML. Impact evaluation of Enabling Mothers to Prevent Pediatric Obesity Through Web-Based Education and Reciprocal Determinism (EMPOWER) randomized control trial. Health Educ Behav. 2015;42(2):171–84. This study is one of the first inventions to target family routines using an Internet-based recruitment and intervention strategy, and one of the few to thoroughly assess measures of program fidelity.
Knowlden AP, Sharma M. Process evaluation of the Enabling Mothers to Prevent Pediatric Obesity Through Web-Based Learning and Reciprocal Determinism (EMPOWER) randomized controlled trial. Health Promot Pract. 2014;15(5):685–94.
Morawska A, Adamson M, Hinchliffe K, Adams T. Hassle Free Mealtimes Triple P: a randomised controlled trial of a brief parenting group for childhood mealtime difficulties. Behav Res Ther. 2014;53:1–9.
Natale RA, Messiah SE, Asfour L, Uhlhorn SB, Delamater A, Arheart KL. Role modeling as an early childhood obesity prevention strategy: effect of parents and teachers on preschool children's healthy lifestyle habits. J Dev Behav Pediatr. 2014;35(6):378–87.
Olsen NJ, Buch-Andersen T, Händel MN, et al. The Healthy Start project: a randomized, controlled intervention to prevent overweight among normal weight, preschool children at high risk of future overweight. BMC Public Health. 2012;12:590.
Olsen N, Rohde J, Heitmann B. The Healthy Start project: a randomized, controlled intervention to prevent overweight among normal weight, preschool children at high risk of future overweight. The Eur J Pub Health. 2015;25(suppl 3):ckv174. 067.
Østbye T, Krause KM, Stroo M, et al. Parent-focused change to prevent obesity in preschoolers: results from the KAN-DO study. Prev Med. 2012;55(3):188–95.
• Skouteris H, Hill B, McCabe M, Swinburn B, Busija L. A parent-based intervention to promote healthy eating and active behaviours in pre-school children: evaluation of the MEND 2-4 randomized controlled trial. Pediatr Obes. 2016;11(1):4–10. This study provides evidence that a theory-based intervention can elicit changes in food neophobia among preschool children.
Sosa ET, Parra-Medina D, He M, Trummer V, Yin Z. ¡Miranos! (Look at us! We are healthy!): home-based and parent peer-led childhood obesity prevention. Health Promot Pract. 2016;17(5):675–81.
Yin Z, Parra-Medina D, Cordova A, et al. Miranos! Look at us, we are healthy! An environmental approach to early childhood obesity prevention. Child Obesity. 2012;8(5):429–39.
Stark LJ, Clifford LM, Towner EK, Filigno SS, Zion C, Bolling C, Rausch J. A pilot randomized controlled trial of a behavioral family-based intervention with and without home visits to decrease obesity in preschoolers. 2014. J Pediatr Psychol.; 39(9):1001–12.
Boles RE, Scharf C, Filigno SS, Saelens BE, Stark LJ. Differences in home food and activity environments between obese and healthy weight families of preschool children. J Nutr Educ Behav. 2013;45(3):222–31.
Boles RE, Scharf C, Stark LJ. Developing a Treatment Program for Obesity in Preschool Age Children: Preliminary Data. Children’s Health Care.. 2010; 39(1):34.
Tabak RG, Tate DF, Stevens J, Siega-Riz AM, Ward DS. Family ties to health program: a randomized intervention to improve vegetable intake in children. J Nutr Educ Behav. 2012;44(2):166–71.
van Grieken A, Renders CM, Veldhuis L, Looman CW, Hirasing RA, Raat H. Promotion of a healthy lifestyle among 5-year-old overweight children: health behavior outcomes of the ‘Be active, eat right’ study. BMC Public Health. 2014;14:59.
Walton K, Filion AJ, Gross D, Morrongiello B, Darlington G, Randall Simpson J, Hou S, Haines J. Parents and Tots Together: Pilot randomized controlled trial of a family-based obesity prevention intervention in Canada. 2015; 106(8):e555–62.
Williams PA, Cates SC, Blitstein JL, et al. Nutrition-education program improves preschoolers’ at-home diet: a group randomized trial. J Acad Nutr Diet. 2014;114(7):1001–8.
Willis TA, George J, Hunt C, et al. Combating child obesity: impact of HENRY on parenting and family lifestyle. Pediatr Obes. 2014;9(5):339–50.
• Wyse R, Wolfenden L, Bisquera A. Characteristics of the home food environment that mediate immediate and sustained increases in child fruit and vegetable consumption: mediation analysis from the Healthy Habits cluster randomised controlled trial. Int J Behav Nutr Phys Act. 2015;12(1) This study provides evidence that parent intake and provision of fruits and vegetables mediate the effect of a telephone-based intervention on child fruit and vegetable intake.
• Wolfenden L, Wyse R, Campbell E, et al. Randomized controlled trial of a telephone-based intervention for child fruit and vegetable intake: long-term follow-up. The Am J Clin Nutr. 2014;99(3):543–50. This study assesses the long-term impact of a telephone-based intervention on children’s fruit and vegetable intake and shows that maintenance strategies are needed to sustain intervention effects beyond one year.
Fletcher A, Wolfenden L, Wyse R, Bowman J, McElduff P, Duncan S. A randomised controlled trial and mediation analysis of the ‘Healthy Habits’, telephone-based dietary intervention for preschool children. Int J Behav Nutr Phys Act. 2013;10:43.
Wyse R, Wolfenden L, Campbell E, et al. A cluster randomized controlled trial of a telephone-based parent intervention to increase preschoolers’ fruit and vegetable consumption. Am J Clin Nutr. 2012;96(1):102–10.
Birch LL, Fisher J, Grimm-Thomas K, Markey C, Sawyer R, Johnson SL. Confirmatory factor analysis of the Child Feeding Questionnaire: a measure of parental attitudes, beliefs and practices about child feeding and obesity proneness. Appetite. 2001;36(3):201–10.
Walton K, Filion AJ, Darlington G, Morrongiello B, Haines J. Parents and tots together: adaptation of a family-based obesity prevention intervention to the Canadian context. Can J Diab. 2015;39:S72–3.
Townsend MS, Sylva K, Martin A, Metz D, Wooten-Swanson P. Improving readability of an evaluation tool for low-income clinents using visual information processing theories. J Nutr Educ Behav. 2008;40:181–6.
Skouteris H, Edwards S, Rutherford L, Cutter-MacKenzie A, Huang T, O'Connor A. Promoting healthy eating, active play and sustainability consciousness in early childhood curricula, addressing the Ben10TM problem: a randomised control trial. BMC Public Health. 2014;14:548.
Ng M, Fleming T, Robinson M, et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2014;384(9945):766–81.
Bergmeier H, Skouteris H, Horwood S, Hooley M, Richardson B. Associations between child temperament, maternal feeding practices and child body mass index during the preschool years: a systematic review of the literature. Obes Rev. 2014;15(1):9–18.
Eisenberg ME, Olson RE, Neumark-Sztainer D, Story M, Bearinger LH. Correlations between family meals and psychosocial well-being among adolescents. Arch Pediatr Adolesc Med. 2004;158(8):792–6.
Northridge ME, Metcalf SS. Enhancing implementation science by applying best principles of systems science. Health Res Pol Sys. 2016;14(1):74.
Acknowledgments
This project is supported by the Agriculture and Food Research Initiative Grant no. 2015-68001-23240 from the USDA National Institute of Food and Agriculture, Childhood Obesity Prevention: Integrated Research, Education, and Extension to Prevent Childhood Obesity – A2101.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Traci A. Bekelman, Laura L. Bellows, and Susan L. Johnson declare they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Food Acceptance and Nutrition in Infants and Young Children
Rights and permissions
About this article
Cite this article
Bekelman, T.A., Bellows, L.L. & Johnson, S.L. Are Family Routines Modifiable Determinants of Preschool Children’s Eating, Dietary Intake, and Growth? A Review of Intervention Studies. Curr Nutr Rep 6, 171–189 (2017). https://doi.org/10.1007/s13668-017-0207-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13668-017-0207-9