Abstract
Aim
The study was aimed at investigating the influence of Vitexin on motor deficits and ataxia-like condition caused by Pb neurotoxicity in mice.
Materials and methods
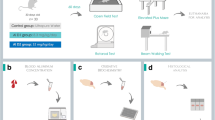
Twenty four adult male albino mice were divided into four groups of six animals. Group A (Control) was administered 0.2 ml of normal saline; Group B was administered with Pb acetate 100 mg/kg/b.wt./d for 14 days; Group C was administered Vitexin 1 mg/kg/b.wt./d for 14 days; and Group D was administered 100 mg/kg/b.wt./d of Pb acetate + 1 mg/kg/b.wt./d of Vitexin for 14 days. Footprint pattern and Hang wire tests were carried out, while the level of malondialdehyde (MDA) and superoxide dismutase (SOD) in the cerebellum were assayed. Furthermore, cerebellum sections were stained with Haematoxylin and Eosin, while Purkinje cells were counted.
Results
Pb treated group showed that the MDA level was significantly high while the SOD level was low when compared with other groups. Also, loss of Purkinje cells, poor gait, and motor coordination were observed. In Pb + Vitexin treated group, the SOD level was significantly high while the MDA level was low. Besides, there was a significant improvement in gait, and motor coordination in Pb + Vitexin treated group.
Conclusion
Pb neurotoxicity caused an increase in oxidative stress, loss of Purkinje cells, and ataxic-like symptoms. However, concurrent administration of Pb and Vitexin was able to neutralize oxidative stress and improve ataxic-like motor coordination.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The cerebellum is responsible for maintaining proper gait, motor coordination, and balance [1]. Recently, the cerebellum has been reported to be involved in the processing of signals for perception, cognition, and emotion [1,2,3,4,5]. Abnormalities of the cerebellum, either structural or functional, can be associated with conditions such as ataxia, tremor, dystonia, autism spectrum disorder, schizophrenia, and attention-deficit/hyperactivity disorder [1]. Cerebellar ataxia, therefore, is a condition that arises from a pure cerebellar disorder or the combination of cerebellar and extra cerebellar disorders [2, 4]. It also arises due to lesions that develop within the cerebellar circuit [6, 7]. Ataxia is characterized by an inability to coordinate balance, gait extremity, and eye movements. Dysfunction or degeneration of Purkinje cell (PC) is the most common ataxia symptoms discovered in animal models [8].
Some of the causes of cerebellar ataxia are multiple system atrophy (MSA), stroke, ethanol toxicity, drugs (including antiepileptic agents, lithium salts, antineoplastic, cyclosporine, metronidazole, cocaine, heroin). Other causes include infectious diseases and heavy metals toxicity such as Mercury, Lead, Manganese, and Aluminium [9,10,11,12,13].
One of the treatable causes of cerebellar ataxia is Pb toxicity [13]. Pb is a pollutant that exists everywhere and in different forms within the environment [14,15,16]. Human exposure to Pb is mainly through the ingestion of contaminated food or water; and inhalation of polluted air [14, 15, 17]. Regardless of age, Pb-induced neurotoxicity has various adverse consequences, particularly on the motor function of the body [17,18,19,20,21]. Pb administration in rats reportedly decreased motor function and superoxide dismutase (SOD) activity with increased malondialdehyde (MDA) levels [22]. The observation is in addition to alterations seen in the histological architecture of the cerebellar cortical layers due to Pb administration [22].
The fundamental mechanisms involved in lead-induced neurotoxicity are complex. However, oxidative stress, membrane bio-physics alterations, deregulation of cell signalling, and damage of neurotransmission have all been implicated in lead neurotoxicity [21]. Pb toxicity causes oxidative stress via excessive production of reactive oxygen species (ROS) and direct depletion of antioxidant reserves [20]. One of the resultant effects of oxidative stress is apoptosis [23, 24]. As a way of combating free radicals, oxidative stress, and Pb-induced toxicity, recent researches have focused on flavonoids. This is probably due to earlier studies that have shown that uptake of certain nutrients including, vitamins, and flavonoids can protect the body against environmental Pb [25]. Also, flavonoids have shown antioxidative activity, free radical scavenging capacity, hepatoprotective, anti-inflammatory, antiviral, anticancer, among other activities [26, 27]. According to emerging evidence, dietary flavonoids and their metabolites cross the blood–brain barrier and exert multiple neuropharmacological actions, which include modulating the innate architecture of the brain [28]. Amid the commonly known flavonoids is Vitexin [26, 29].
Vitexin is a flavonoid that is extracted from many plants, including pearl millet, hawthorn, pigeon pea, mung bean, mosses, Passiflora, bamboo, mimosa, wheat leaves and chaste berry [29]. Vitexin has several pharmacological and biological roles such as antioxidative, anti-tumour, antiviral, anti-inflammatory, antibacterial, antihypertensive, anti-nociceptive, antispasmodic, anti-diabetic, antidepressant, neuroprotective and cognitive improving functions [30,31,32,33,34,35,36].
Despite broad studies on Vitexin, the literature on its effect on motor coordination and balance are scanty or not available in some cases. Also, the search for the best possible therapeutic control of oxidative stress caused by Pb toxicity is still on. It is because of these gaps in knowledge that the study was aimed at investigating the effect of Vitexin on ataxia-like condition caused by Pb neurotoxicity.
Results
Effect of Vitexin and lead acetate on motor coordination
The result from the hanging wire test (Fig. 1) shows no statistically significant difference in time that the animals took to fall from the wire when a comparison was made between the control group (82 ± 11) and all the experimental groups (52 ± 9.1; 72 ± 8.0; and 63 ± 10; P values 0.057; 0.48 and 0.22). Although both Vitexin (72 ± 8.0) and Pb + Vitexin (63 ± 10) treated groups had longer hanging time compared to Pb treated group (52 ± 9.1), the time was not significant (P = 0.12 and 0.42, respectively). Similarly, the hanging time between Vitexin and Pb + Vitexin treated groups (72 ± 8.0 vs. 63 ± 10; P = 0.42) was not statistically different when a comparison was made.
The representative footprint photograph (Fig. 2) shows a narrow-based stance with steady proximity forelimb (red colour) and hind limb footprints (blue colour) in the control group. In contrast, Pb treated group featured a wider overlap stance, small stride, and separated forelimb and hind limb prints. The footprint pattern in Pb + Vitexin treated group showed longer strides when compared with Pb treated group and the control group.
The footprint analysis of base width (Fig. 3) shows a significant decrease in forelimb base width (Fbw) of Pb treated group when compared with the control group (CV = 41.70%; P = 0.0045), Vitexin group (CV = 40.25%; P = 0.0002) and Pb + Vitexin group (CV = 17.97%; P = 0.01). Also, the Fbw significantly increases in Pb + Vitexin treated group when compared with the control group (CV = 20.1% P = 0.012). Furthermore, there was no statistically significant difference in Fbw when a comparison was made between the control group and the Vitexin group (CV = 6.37%; P = 0.22) as well as between the Vitexin group and Pb + Vitexin group (CV = 7.07%; P = 0.2).
Footprint analyses of the base width. Data expressed as mean ± SEM (n = 6 per group). Fbw Forelimb base width, Hbw Hind limb base width, α significant difference with control group, β significant difference with Pb group, γ significant difference with Vitexin group; δ significant difference with Pb + Vitexin group
The result on hind base width (Hbw) shows a significant increase in both Vitexin (CV = 19.1%; P = 0.03 and Pb + Vitexin (CV = 15.1%; P = 0.045) treated groups when compared with the control group. Similarly, Hbw also increases in both Vitexin and Pb + Vitexin treated groups when compared with the Pb treated group (CV = 17.8%; P = 0.01 and CV = 15.1%; P = 0.04, respectively). However, no statistically significant difference in Hbw was recorded between the control group and Pb group (CV = 8.3%; P = 0.19) as well as between Vitexin and Pb + Vitexin treated groups (CV = 6.3%; P = 0.28).
The result on stride length (Fig. 4) shows a significant decrease in forelimb stride length (Fls) when the comparison was made between Pb treated group and the control (CV = 45.1%; P = 0.0045) as well as Pb + Vitexin groups (CV = 15.9%; P = 0.041). There was also a significant decrease in Fls when the comparison was made between Pb + Vitexin treated group and the control group (CV = 15.7%; P = 0.048). Furthermore, Fls was not significantly different between the control group and Vitexin treated group (CV = 8.63%; P = 0.12).
Stride length in cm. Data expressed as mean ± SEM (n = 6 per group). Fls Forelimb stride length, Hls Hind limb stride length, α significant difference with control group, β significant difference with Pb group, γ significant difference with Vitexin group, δ significant difference with Pb + Vitexin group
Hind limb stride length (Hls) (Fig. 4) was significantly longer in the control group when compared with Pb treated group (CV = 32.9%; P = 0.031), Vitexin treated group (CV = 17.4%; P = 0.04), and Pb + Vitexin treated group (CV = 16.9%; P = 0.05). In addition to the result on Hls, no significant difference (P > 0.05) was observed when the comparison was made between Pb, Vitexin, and Pb + Vitexin treated groups (CV = 7.73%; P = 0.213).
The overlap length (as seen in Fig. 5) shows no statistically significant difference between the control group and all other groups (P > 0.05). Similarly, there was no statistically significant difference in overlap length when a comparison was made between Pb treated and Pb + Vitexin treated groups (0.43 ± 0.042 vs. 0.33 ± 0.061; P = 0.21). Furthermore, a comparison between Vitexin treated group and Pb + Vitexin treated group (0.38 ± 0.031 vs. 0.33 ± 0.061; P = 0.48) did not show a significant difference in overlap length.
Effect of Vitexin and lead acetate on oxidative stress markers
The malondialdehyde level (Fig. 6) in Pb treated group was significantly high when compared with the control group (1.7 ± 0.041 vs. 1.2 ± 0.015; P = 0.001). Similarly, when a comparison was made between Pb treated group and Vitexin (1.7 ± 0.041 vs. 1.3 ± 0.029; P = 0.001) as well as Pb + Vitexin, treated (1.7 ± 0.041 vs. 1.4 ± 0.0097; P = 0.001) groups, the MDA level was significantly high in Pb treated group. Furthermore, the MDA level in Pb + Vitexin was significantly higher (P < 0.05) than the control group when both were compared (1.4 ± 0.0097 vs. 1.2 ± 0.015; P = 0.046). In addition to the result of the MDA level (Fig. 6), no statistically significant difference (P > 0.05) was recorded when the control and Vitexin treated group was compared (1.2 ± 0.015 vs. 1.3 ± 0.029; P = 0.11). Similarly, the MDA level was not different (P > 0.05) between Vitexin treated group and Pb + Vitexin treated group (1.3 ± 0.029 vs. 1.4 ± 0.0097; P = 0.0578) when a comparison was made.
The level of superoxide dismutase (Fig. 7) in the Pb treated group was significantly lower than the control group (1.7 ± 0.036 vs. 2.5 ± 0.037; P = 0.009) as well as Vitexin treated group (1.7 ± 0.036 vs. 3.0 ± 0.16; P = 0.006). Similarly, there was a significant decrease (P < 0.01) in the level of SOD when Pb treated and Pb + Vitexin treated groups were compared (1.7 ± 0.036 vs. 2.3 ± 0.16; P = 0.0064). Furthermore, while the SOD level in Vitexin treated group was higher than the control group (3.0 ± 0.16 vs. 2.5 ± 0.037; P = 0.014). The SOD level in Pb + Vitexin treated group was not different from the control group (2.3 ± 0.16 vs. 2.5 ± 0.037; P = 0.39). Also, the level of SOD in the Pb + Vitexin treated group was significantly lower than the level seen in Vitexin treated group (2.3 ± 0.16 vs. 3.0 ± 0.16; P = 0.019).
Effect of Vitexin and lead acetate on the histology of cerebellum and Purkinje cells
The representative photomicrograph of H&E-stained sections of mice cerebellum at lower magnification (Fig. 8) did not show much cytoarchitectural difference between the groups; as all the groups appeared to have well-arranged molecular, granular and Purkinje cell layers at that magnification. However, at higher magnification (Fig. 9), the Purkinje cell layer in the Pb treated group appeared distorted with fewer cells when compared with the other groups. On the contrary, the Purkinje cell layer in Pb + Vitexin treated group appeared thick with numerous cells arranged in double layers. The Purkinje layer of the control and Vitexin treated group appeared similar.
Representative photomicrograph of H&E-stained section of mice cerebellum at higher magnification. Control control group, Pb lead treated group, Vitexin Vitexin treated group, Pb + Vitexin lead + Vitexin treated group. Purkinje cell layer (PCL) aligned between the molecular layer (ML), granule cell layer (GCL), blue arrows point to Purkinje cells. Scale bar = 45 μm
The number of Purkinje cells (PCs) counted (Fig. 10) was significantly fewer in Pb treated group when compared with the control group (P < 0.01), as well as Pb + Vitexin, treated group (P < 0.001). Furthermore, no statistically significant difference (P > 0.05) was recorded when the number of PCs was compared between the control and Vitexin treated and Pb + Vitexin treated groups.
Discussion
Cerebellar ataxia is caused by a disorder in the cerebellar and extra cerebellar structures [2, 4] in addition to other causes such as lesions that develop within the cerebellar circuit [6, 7]. In animal models such as mice, gait and motor coordination are tested using a footprint pattern test, Hang wire test, and beam walking [37, 38], among other tests.
The representative photomicrograph of H&E-stained sections of mice cerebellum in this study (Fig. 9) shows the Purkinje cell layer (PCL) in Pb treated group to be distorted with fewer cells when compared with other groups. Cell count also shows that Pb treated group had fewer Purkinje cells (PCs) in the PCL. This finding suggests that Pb administered may have caused distortion of PCL and degeneration of PCs, which in turn resulted in fewer cells seen in PCL. This result is probably due to a rapid increase in cell death as a result of increased oxidative stress brought about by Pb exposure. Histological data from earlier studies [17, 22, 39] indicated Pb exposure caused significant damage to neurons of the cerebellum. In this study, concurrent administration of Pb and Vitexin (Pb + Vitexin) shows better cytoarchitecture and the number of PCs counted when compared with only Pb administered group. This result suggests that Vitexin may have neutralized the potential toxic effect of Pb on PCs through its antioxidant activity, which in turn reduced the number of cells degenerated. Additionally, Vitexin may have protected the cerebellum from damage by suppression of neuroinflammatory processes and activation of adaptive cellular stress responses against oxidative stressors [28, 40].
Purkinje cells (PCs) constitute the middle layer of the cerebellum named the Purkinje cell layer (PCL). The PCL also comprises of interneurons known as candelabrum cells as well as specialized astrocytes termed Bergmann glia [3, 5]. Purkinje cells (PCs) receive climbing fibres and interneuron projections from the molecular layer and also contribute to relaying the main computations of the cerebellar cortex onto downstream nuclei [5]. Purkinje cells are the cornerstone of all cerebellar circuits. This was proven as defects in Purkinje cell morphology, and signalling prompted neurological motor conditions such as ataxic symptoms in animal models [5, 8].
The current data on footprint analysis show (Figs. 3, 4, 5) that Pb treated group generally displayed an abnormal pattern of base width, stride length, and overlap length when compared with the control group. In Pb + Vitexin treated group, the pattern of base width, stride length, and overlap length was similar to the pattern observed in the control group and better than Pb treated group. This result did not come as a surprise because, when many of the PCs in the Pb treated group degenerated, it was assumed that the PCs signalling would experience deficits, which in turn would affect motor activity leading to the abnormal gait pattern observed in Pb treated group. Moreover, an earlier report from a review article stated that deficits in Purkinje cells (PCs) signalling resulted in ataxia [8].
Reactive oxygen species (ROS) are transitory and highly reactive molecules that exist in equilibrium with a variety of antioxidant defences in cells [23]. At low levels, ROS are thought to be vital for the regulation of normal physiological functions, for example, cell cycle progression and proliferation, differentiation, migration, and cell death [23]. Excess cellular levels of ROS creates an imbalance with antioxidant defences in cells thereby causing damage to proteins, nucleic acids, lipids, membranes and organelles, which in turn lead to activation of cell death processes such as apoptosis [23, 24, 41].
Malondialdehyde (MDA) is one of the end products of lipid peroxidation and a widely recognized oxidative stress marker [41, 42]. In this study, the MDA level in Pb treated group was significantly higher than other groups, including the control. This observation suggests that the level of oxidative damage was higher in Pb treated group than in other groups. The observation further suggests that cell death processes are higher in this group, as revealed by the few Purkinje cells (PCs) observed in the histological data seen in this study. Earlier reports [22, 43, 44] also observed that Pb increases the level of tissue MDA. In contrast, Vitexin has been reported to reduce the MDA level significantly [45]. This could be the reason behind the reduced level of MDA observed in the Pb + Vitexin treated group.
Superoxide dismutase (SOD) is a first-line defence antioxidant enzymes that dismutate superoxide radicals into harmless molecules [46]. In this study, the level of SOD was significantly low in Pb treated group when compared with the control and other experimental groups (particularly Pb + Vitexin). This result suggests that Vitexin may have boosted the antioxidant enzyme defence of the cells to fight against excess cellular ROS generated as a result of Pb neurotoxicity. This, in turn, probably reduced cellular damage and apoptosis. This result could be the reason PCs count (Fig. 10) in Pb + Vitexin treated group was higher than the Pb treated group. Previous studies also observed an increase in the SOD level [22, 45, 47] and reduced cell deaths when Vitexin was administered [48].
Materials and methods
Chemicals and reagents
Vitexin extract, Pb acetate, malondialdehyde (MDA) test kit, and superoxide dismutase (SOD) test kit were purchased from Sigma-Aldrich (St Louis, MO, USA). Vitexin was dissolved in normal saline (NaCl, 0.9%).
Animals
Twenty four adult male albino mice weighing 19–20 g were procured from the Temidale animal husbandry centre, Ogbomosho. The animals were acclimatized for 14 days on a 12 h light/dark cycle in the animal holdings of Central Research Lab, University of Ilorin. The animals were provided with food and water ad libitum. The animals were maintained under the National Institutes of Health guide for the care and use of laboratory animals (NIH Publications, 8th edition). The experimental protocols involved in the study were approved by the University of Ilorin Ethical and Review Committee with approval number: UERC/ASN/2018/1257.
Animal grouping and administration
The animals were randomly divided into four groups of six animals. Group A which was also the control group was administered 0.2 ml normal saline for 14 days via oral gavage; Group B (Pb group) received oral gavage of Pb acetate 100 mg/kg/b.wt./d for 14 days; Group C (Vitexin group) received intraperitoneal injection of Vitexin 1 mg/kg/b.wt./d for 14 days; Group D (Pb + Vitexin group) received concurrent administration of 100 mg/kg/b.wt./d of Pb + 1 mg/kg/b.wt./d Vitexin for 14 days.
Hang wire test with two limbs
The test was carried out 4 days after the end of administration according to the modified method of Aartsma-Rus and van Putten [49]. The setup comprises of a 2 mm thick metallic wire that is 55 cm wide and secured between two vertical stands. The distance between the metallic wire and soft bedding underneath was 37 cm. In the test, the mouse was handled via the tail and allowed to grasp the 2 mm thick metallic wire with the two forepaws only. After that, timing with a stopwatch commenced until when the mouse fell off the wire. The record of hanging time was taken. The same process was repeated for all animals with each animal given a maximum of three trials before mean hanging time was calculated.
Footprint test
The technique used for the test was modified from protocols described by Carter et al. [37] and Meng et al. [50]. The test was carried out 5 days after the end of the administration. The apparatus for the test was an open-top runway with an enclosed cage that opens at both ends. The runway length was 60 cm long, and the width was 11 cm. Furthermore, the open-top runway was flanked by two walls (12 cm high) on each side. The mice were acclimatized to the test environment for 30 min. In other to obtain footprints, mice front and hind paws were coated with non-toxic red and blue inks, respectively, and were allowed to walk down the narrow runway that was covered with white paper (Fig. 2). Six mice from each group were used, and a total of three trials was performed on each mouse.
Once the footprints had dried, the following parameters were measured with the aid of a pencil and a measuring ruler: base width, overlap width, forelimb stride length, and hind limb stride length. The mean of each parameter was then calculated for each group.
Preparation of brain sample
Six days after the end of the administration, animals were anesthetized with an intraperitoneal injection of ketamine (50 mg/0.2 ml). The mice for histology were transcardially perfused with 4% paraformaldehyde (PFA) in phosphate buffer saline (PBS) solution. Excised cerebellar tissues were postfixed in 4% PFA for 24 h before transferring into a cold 20% sucrose solution. Tissue processing, as well as haematoxylin and eosin (H&E) staining procedures, was carried out according to the description of Bancroft and Gamble [51].
Photomicrography and cell count
Stained sections were viewed under a light binocular microscope (Olympus, New Jersey, USA) attached to an amscope camera (MD500, CA, USA). Six visual fields of the Purkinje cell layer were photographed in each section and were used for cell counting with the aid of ImageJ 1.52r software (National Institute of Health, USA).
Biochemical assay
Cerebellar tissues (each 10% w/v) that were not fixed with PFA were washed with PBS and then homogenized with Teflon Potter–Elvehjem homogenizer on ice to prepare homogenate solution. The homogenate was centrifuged (13,000g, 5 min), and the supernatant was used for assessment of MDA and SOD levels. The levels of MDA and SOD were assessed according to the procedure on assay kits purchased from Sigma-Aldrich (St Louis, MO, USA).
Statistical analysis
All statistical analyses and graph fitting were performed using Graph Pad Prism version 5.0 for Windows. The significance of difference was determined using one-way ANOVA followed by Tukey’s posthoc test for all parameters except base width and stride length where two-way ANOVA (Bonferroni posthoc test) was used. All data in the text and figures were expressed as the mean ± standard error of the mean (SEM), with n representing the number of animals used in each experiment. Statistical significance was defined at the level of P < 0.05. The coefficient of variation (CV) expressed in percentage was used to reflect variability within groups in some of the parameters.
Conclusion
Pb neurotoxicity caused increase lipid peroxidation, loss of Purkinje cells, and ataxic-like symptoms characterized by poor gait and poor motor coordination. However, concurrent administration of Pb + Vitexin decreases lipid peroxidation level and increased antioxidant defences. These results suggest that Vitexin attenuates Pb-induced neurotoxicity via inhibition of oxidative stress and chelating activity. Also, no obvious ataxic-like symptoms were observed when Pb + Vitexin was concurrently administered.
References
Lackey EP, Heck DH, Sillitoe RV (2018) Recent advances in understanding the mechanisms of cerebellar granule cell development and function and their contribution to behavior. F1000Res 7:1142. https://doi.org/10.12688/f1000research.15021.1
Manto M, Marmolino D (2009) Cerebellar ataxias. Curr Opin Neurol 22(4):419–429
Miterko LN, Baker KB, Beckinghausen J, Bradnam LV, Cheng MY, Cooperrider J, Sillitoe RV (2019) Consensus paper: experimental neurostimulation of the cerebellum. Cerebellum. https://doi.org/10.1007/s12311-019-01041-5
Pandolfo M, Manto M (2013) Cerebellar and afferent ataxias. Continuum 19(5):1312–1343
Reeber SL, Otis TS, Sillitoe RV (2013) New roles for the cerebellum in health and disease. Front Syst Neurosci 7:83
Kelly G, Shanley J (2016) Rehabilitation of ataxic gait following cerebellar lesions: applying theory to practice. Physiother Theory Pract 32(6):430–437
Mochizuki H, Ugawa Y (2010) Cerebellar ataxic gait. Brain Nerve 62(11):1203–1210
Hoxha EB, Ilaria M, Maria C, Tempia F (2018) Purkinje cell signaling deficits in animal models of ataxia. Front Synaptic Neurosci 10:6
Alekseeva N, Mcgee J, Kelley RE, Maghzi AH, Gonzalez-Toledo E, Minaga A (2014) Toxic-metabolic, nutritional, and medicinal-induced disorders of the cerebellum. Neurol Clin 32(4):901–911
Jones TM, Shaw JD, Sullivan K, Zesiewicz TA (2014) Treatment of cerebellar ataxia. Neurodegener Dis Manag 4(5):379–392
Manto M (2012) Toxic agents causing cerebellar ataxias. Handb Clin Neurol 103:201–213
Manto M, Perrotta G (2018) Toxic-induced cerebellar syndrome: from the fetal period to the elderly. Handb Clin Neurol 155:333–352
Ramirez-Zamora A, Zeigler W, Desai N, Biller J (2015) Treatable causes of cerebellar ataxia. Mov Disord 30(5):614–623
Ahmed MB, Ahmed MI, Meki A, Abdraboh N (2013) Neurotoxic effect of lead on rats: relationship to apoptosis. Int J Health Sci 7(2):192–199
Liu F, Xue Z, Li N, Huang H, Ying Y, Li J, Li W (2014) Effects of lead exposure on the expression of amyloid beta and phosphorylated tau proteins in the C57BL/6 mouse hippocampus at different life stages. J Trace Elem Med Biol 28(2):227–232
Zhang L, Tu R, Wang Y, Hu Y, Li X, Cheng X, Huang H (2017) Early-life exposure to lead induces cognitive impairment in elder mice targeting SIRT1 phosphorylation and oxidative alterations. Front Physiol 8:446
Mahmoud YI, Sayed SS (2016) Effects of l-cysteine on lead acetate induced neurotoxicity in albino mice. Biotech Histochem 91(5):327–332
Mason LH, Harp JP, Han DY (2014) Pb neurotoxicity: neuropsychological effects of lead toxicity. Biomed Res Int 2014:840547
Reckziegel P, Dias VT, Benvegnu D, Boufleur N, Silva Barcelos RC, Segat HJ, Burger ME (2011) Locomotor damage and brain oxidative stress induced by lead exposure are attenuated by gallic acid treatment. Toxicol Lett 203(1):74–81
Sharma B, Singh S, Siddiqi NJ (2014) Biomedical implications of heavy metals induced imbalances in redox systems. Biomed Res Int 2014:640754
Sharma P, Chambial S, Shukla KK (2015) Lead and neurotoxicity. Indian J Clin Biochem 30(1):1–2
Abubakar K, Muhammad Mailafiya M, Danmaigoro A, Musa Chiroma S, Bin E, Rahim A, Abu Bakar MZ (2019) Curcumin attenuates lead-induced cerebellar toxicity in rats via chelating activity and inhibition of oxidative stress. Biomolecules 9:453
Redza-Dutordoir M, Averill-Bates DA (2016) Activation of apoptosis signaling pathways by reactive oxygen species. Biochim Biophys Acta (BBA) Mol Cell Res 1863(12):2977–2992
Ryter SW, Kim HP, Hoetzel A, Park JW, Nakahira K, Wang X, Choi AM (2007) Mechanisms of cell death in oxidative stress. Antioxid Redox Signal 9(1):49–89
Flora Gagan, Gupta Deepesh, Tiwari Archana (2012) Toxicity of lead: a review with recent updates. Interdiscip Toxicol 5(2):47–58
Shashank K, Abhay KP (2013) Chemistry and biological activities of flavonoids: an overview. Sci World J 2013:16
Panche AN, Diwan AD, Chandra SR (2016) Flavonoids: an overview. J Nutr Sci 5:e47
Muralidhara KG (2015) Dietary supplements as cognitive enhancers: the role of flavonoid-rich foods and their relevance in age-related neurodegeneration. In: Watson RR, Preedy VR (eds) Bioactive nutraceuticals and dietary supplements in neurological and brain disease. Academic Press, San Diego, pp 281–290
He M, Min JW, Kong WL, He XH, Li JX, Peng BW (2016) A review on the pharmacological effects of vitexin and isovitexin. Fitoterapia 115:74–85
Choi JS, Nurul Islam MD, Yousof Ali MD, Kim EJ, Kim YM, Jung HA (2014) Effects of C-glycosylation on anti-diabetic, anti-Alzheimer’s disease and anti-inflammatory potential of apigenin. Food Chem Toxicol 64:27–33
Hritcu L, Ionita R, Postu PA, Gupta GK, Turkez H, Lima T, De Sousa DP (2017) Antidepressant flavonoids and their relationship with oxidative stress. Oxid Med Cell Longev 2017:5762172
Lima LKF, Pereira SKS, Junior R, Santos F, Nascimento AS, Feitosa CM, Rai M (2018) A brief review on the neuroprotective mechanisms of vitexin. Biomed Res Int 2018:4785089
Nabavi SF, Khan H, D’onofrio G, Samec D, Shirooie S, Dehpour AR, Sobarzo-Sanchez E (2018) Apigenin as a neuroprotective agent: of mice and men. Pharmacol Res 128:359–365
Rosa S, Iara G, Rios-Santos F, Balogun SO, Martins DT (2016) Vitexin reduces neutrophil migration to inflammatory focus by down-regulating pro-inflammatory mediators via inhibition of p38, ERK1/2 and JNK pathway. Phytomedicine 23(1):9–17
Yang L, Yang ZM, Zhang N, Tian Z, Liu SB, Zhao MG (2014) Neuroprotective effects of vitexin by inhibition of NMDA receptors in primary cultures of mouse cerebral cortical neurons. Mol Cell Biochem 386(1–2):251–258
Zhu Q, Mao L, Liu C, Sun Y, Jiang B, Zhang W, Li J (2016) Antinociceptive effects of vitexin in a mouse model of postoperative pain. Sci Rep 6:19266
Carter RJ, Morton J, Dunnett SB (2001) Motor coordination and balance in rodents. Curr Protoc Neurosci 15:8–12
Carter M, Shieh JC (2010) Guide to research techniques in neuroscience. Elsevier, New York, pp 46–48
Barkur RR, Bairy LK (2016) Histological study on the hippocampus, amygdala, and cerebellum following low lead exposure during prenatal and postnatal brain development in rats. Toxicol Ind Health 32(6):1052–1063
Arredondo F, Echeverry C, Blasina F, Vaamonde L, Díaz M, Rivera F, Dajas F et al (2015) Flavones and flavonols in brain and disease: facts and pitfalls. In: Watson RR, Preedy VR (eds) Bioactive nutraceuticals and dietary supplements in neurological and brain disease. Academic Press, San Diego, pp 229–236
Ayala A, Mario F, Elles S (2014) Lipid peroxidation: production, metabolism, and signaling mechanisms of malondialdehyde and 4-hydroxy-2-nonenal. Oxid Med Cell Longev 2014:31
Tang Q, Su Y, Xian CJ (2019) Determining oxidative damage by lipid peroxidation assay in rat serum. Bio-protocol 9(12):e3263
Barkur RR, Bairy LK (2015) Assessment of oxidative stress in the hippocampus, cerebellum, and frontal cortex in rat pups exposed to lead (Pb) during specific periods of initial brain development. Biol Trace Elem Res 164(2):212–218
Xu J, Lian L, Wu C, Wang X, Fu W, Xu L (2008) Lead induces oxidative stress, DNA damage, and alteration of p53, Bax and Bcl-2 expressions in mice. Food Chem Toxicol 46(5):1488–1494
Nurdiana S, Goh YM, Hafandi A, Dom SM, Nur Syimal’ain A, Noor Syaffinaz NM, Ebrahimi M (2018) Improvement of spatial learning and memory, cortical gyrification patterns and brain oxidative stress markers in diabetic rats treated with Ficus deltoidea leaf extract and vitexin. J Tradit Complement Med 8(1):190–202
Ighodaro OM, Akinloye OA (2017) First-line defense antioxidants-superoxide dismutase (SOD), catalase (CAT), and glutathione peroxidase (GPX): their fundamental role in the entire antioxidant defense grid. Alex J Med 54(4):287–293
An F, Yang G, Tian J, Wang S (2012) Antioxidant effects of the orientin and vitexin in Trollius chinensis Bunge in d-galactose-aged mice. Neural Regen Res 7(33):2565–2575
Lyu Z, Cao J, Wang J, Lian H (2018) Protective effect of vitexin reduces sevoflurane-induced neuronal apoptosis through HIF-1α, VEGF, and p38 MAPK signaling pathway in vitro and newborn rats. Exp Ther Med 15(3):3117–3123
Aartsma-Rus A, Van Putten M (2014) Assessing functional performance in the mdx mouse model. J Vis Exp 85:e51303
Meng H, Larson SK, Gao R, Qiao X (2007) BDNF transgene improves ataxic and motor behaviors in stargazer mice. Brain Res 1160:47–57
Bancroft JD, Gamble M (2008) Theory and practice of histological techniques. Churchill Livingstone, London
Acknowledgements
The authors thank Mr. Leviticus Arietarhire and Dr. Emeka central research and diagnostic laboratory, Ilorin.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Nathaniel Ohiemi Amedu and Gabriel Olaiya Omotoso declare that they have no conflict of interest.
Ethical approval
The experimental protocols involved in the study were approved by the University of Ilorin Ethical and Review Committee with approval number: UERC/ASN/2018/1257.
Rights and permissions
About this article
Cite this article
Amedu, N.O., Omotoso, G.O. Influence of Vitexin on ataxia-like condition initiated by lead exposure in mice. Toxicol. Environ. Health Sci. 12, 305–313 (2020). https://doi.org/10.1007/s13530-020-00041-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13530-020-00041-x