Abstract
Progressive multifocal leukoemcephalopathy (PML) is a fatal demyelinating disease caused by the human neurotropic JC virus (JCV). JCV infects the majority of the human population during childhood and establishes a latent/persistent life-long infection. The virus reactivates under immunosuppressive conditions by unknown mechanisms, resulting in productive infection of oligodendrocytes in the central nervous system (CNS). Given the fact that the natural occurrence of PML is strongly associated with immunosuppression, the functional and molecular interaction between glial cells and neuroimmune signaling mediated by soluble immune mediators is likely to play a major role in reactivation of JCV and the progression of the lytic viral life cycle leading to the development of PML. In order to explore the effect of soluble immune mediators secreted by peripheral blood mononuclear cells (PBMCs) on JCV transcription, primary human fetal glial (PHFG) cells were treated with conditioned media from PBMCs. We observed a strong suppression of JCV early as well as late gene transcription in cells treated with conditioned media from induced PBMCs. Using a variety of virological and molecular biological approaches, we demonstrate that immune mediators secreted by PBMCs induce the expression of SRSF1, a strong inhibitor of JCV gene expression, and inhibit the replication of JCV. Our results show that downregulation of SRSF1 in glial cells overcomes the suppression of JCV gene expression and its replication mediated by soluble immune mediators. These findings suggest the presence of a novel immune signaling pathway between glial cells and PBMCs that may control JCV gene expression during the course of viral reactivation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Replication of JC virus in glial cells causes the fatal demyelinating disease of the central nervous system, progressive multifocal leukoencephalopathy (PML), which is usually seen in immunocompromised patients (Ferenczy et al. 2012; Warnke et al. 2015; Carruthers and Berger 2014; Safak et al. 2005). PML is the only viral demyelinating disease of the human brain characterized by lytic infection of astrocytes and oligodendrocytes (Padgett et al. 1971; Eng et al. 2006; Berger and Khalili 2011). JCV infects the majority of the human population during childhood and establishes a life-long latent/persistent infection in healthy individuals (Weber 2008; Moens and Johannessen 2008). Between 3 and 5 % of HIV-infected individuals develop PML (Focosi et Al. 2010; Zheng et al. 2009; San-Andres et al. 2003). PML has also been diagnosed in patients with autoimmune diseases treated with immunomodulatory therapies, such as the monoclonal antibodies natalizumab and efalizumab, which bind to alpha-integrin molecules on the surface of B and T cells, respectively, and prevent their entry into the brain. Another example is rituximab which binds to the CD20 molecule on the surface of B cells, causing their depletion from peripheral circulation. PML was diagnosed in two multiple sclerosis patients and in one Crohn’s patient treated with Tysabri in 2005 (Sandborn et al. 2005; Langer-Gould et al. 2005; Kleinschmidt-DeMasters and Tyler 2005). As of March 5, 2015, there have been 541 confirmed PML cases (Biogen Idec), the majority of which have been observed in multiple sclerosis patients. PML has been detected in four plaque-psoriasis patients treated with efalizumab and in approximately 57 patients treated with Rituxan (rituximab) used in lymphoma patients and some rheumatoid arthritis patients (Carson et al. 2009). PML is highly fatal within 6–12 months (Brew et al. 2010). Currently, the only available option for PML patients is the restoration of the underlying immune impairment.
JC virus consists of a double-stranded, circular DNA genome with an icosahedral capsid. The bidirectional viral promoter separates the viral genome into early and late genes. The early JCV transcript encode for T antigen, small t antigen, and a series of T’ proteins generated by alternative splicing. T antigen plays a key role in JCV life cycle. T antigen can bind to its own promoter and act as a transcription factor to autoregulate early gene expression and activate the expression of the late viral transcript, which encodes the accessory protein, agnoprotein, and capsid proteins VP1, VP2, and VP3 (Lashgari et al. 1989). T antigen is expressed in the early phase of viral reactivation and is required for the initiation of the lytic viral life cycle.
The natural occurrence of PML is strongly associated with immunosuppression and limited inflammation is observed in the brain (Wüthrich et al. 2006). While evidence has suggested that cell-mediated immunity (i.e., T cell-mediated CTL response) could be the main mechanism controlling JC virus replication (Du Pasquier et al. 2004; Koralnik 2002), little is known about the immunobiology of JCV reactivation in glial cells and the role of immune, glial, and viral players in this regulation. As the natural occurrence of PML is strongly associated with immunosuppression, neuroimmune signaling mediated by soluble immune mediators are likely to play a major role in controlling JCV reactivation and the progression of the lytic viral life cycle leading to the development of PML. Here, we investigated the possible impact of soluble immune mediators secreted by activated immune cells on JCV gene expression as well as viral replication in primary human fetal glial (PHFG) cells. Our results have revealed that JCV transcription and DNA replication is tightly controlled by immune modulators secreted by peripheral blood mononuclear cells (PBMCs). Moreover, a series of virological and biochemical studies has suggested that serine arginine rich splicing factor 1 (SRSF1) is required for neuroimmune suppression of JCV replication. These results have established an important regulatory role of SRSF1 in neuroimmune suppression of JCV in glial cells.
Materials and Methods
Ethics statement
Human PBMCs were isolated from buffy coats (obtained commercially, Biological Specimens, Inc.) in a study approved by the by the Temple University Institutional Review Board. Cultures of PHFG cells were prepared from human fetal brain tissue obtained from Advanced Bioscience Resources (Alameda, CA) under approval of the Temple University Institutional Review Board (IRB).
Cell lines and cultures
PHFG cells were cultured from fetal brain and provided by the Basic Science II Core Facility of the Temple P30 Comprehensive NeuroAIDS Center, Department of Neuroscience, Temple University Lewis Katz School of Medicine. Human PBMCs were isolated from the heparinized blood of buffy coats by Ficoll-Paque technique, induced with PMA and Ionomycin, and conditioned media from either uninduced or induced PBMCs were collected as described previously (De Simone et al. 2015). Conditioned media were supplemented into growth media (50 %) of PHFG cells transfected with reporter constructs or infected with JCV. SVG-A is a subclonal population of a human glial cell line which was established by transformation of human fetal glial cells with an origin-defective SV40 mutant (Major et al. 1985).
Stable cell lines
SVG-A cells (1 × 105 cells/35-mm tissue culture dish) were either cotransfected with pcDNA3.1 vector alone (Invitrogen) (1 μg/plate) and pLentiLox 3.7 vector alone (2 μg/plate) or with pcDNA3.1 vector alone (1 μg/plate) and pLentiLox 3.7-SRSF1-shRNA (Sariyer and Khalili 2011) (2 μg/plate) by Lipofectamine 2000 method according to manufacturer’s recommendations (Invitrogen). At 6 h posttransfection, cells were washed twice with phosphate-buffered saline (PBS) and re-fed with DMEM culture media containing 10 % FBS. After 24 h, cells from each 35-mm plate were trypsinized and re-plated onto three 100-mm plates. Cells were allowed to attach for 6 h, and then, the medium was replaced with DMEM containing 500 μg/ml G418 and 10 % FBS. The medium of the cells was replaced every 2–3 days until individual colonies formed. The single-cell colonies were selected based on GFP expression, screened for SRSF1 downregulation by Western blotting, expanded and frozen in liquid nitrogen.
Plasmid constructs
The luciferase reporter constructs pLuc-JCV-Early and pLuc-JCV-Late were made by blunt end cloning of the full-length Mad-1 NCCR into the SmaI site immediately upstream of the luciferase gene in the plasmid pGL3 (Promega, Madison, WI) as described previously (Wollebo et al. 2011). The luciferase reporter plasmid pLuc-SRSF1 (−1000) was made by cloning the −1000 to +49 promoter region of SRSF1 gene into pGL3 vector at BamH1 site. pLentilox3.7-SRSF1-shRNA was described previously (Sariyer and Khalili 2011). pBlue-Mad1 WT plasmid was described previously (Sariyer and Khalili 2011; De Simone et al. 2015).
Luciferase reporter assay
PHFG cells were plated in six-well tissue culture dishes and transiently transfected with the pLuc-JCV-Early, pLuc-JCV-Late, or pLuc-SRSF1-1000-bp reporter plasmids. At 48 h posttransfection, cells were extracted and lysed using reporter lysis buffer for the luciferase reporter system provided by the manufacturer (Promega). After cell lysis, luciferase activity of samples was determined through the use of luciferase assay reagent (LAR). The luciferase activities were then corrected for protein concentrations and normalized to the basal levels of transcription, allowing for determination of the fold change relative to control.
JCV infection
Infection of cells with JCV was performed as described previously (De Simone et al. 2015). Briefly, PHFG, SVG-A-GFP, or SVG-A-SRSF1-shRNA cells were plated in T75-cm tissue culture flask and were transfected with the full-length JCV Mad1 genomic DNA using Fugene6 transfection (Roche). At 8 days postinfection, infected cells were trypsinized and divided into two equal portions. One half portion of the cell pellet was used for the preparation of protein extracts for Western blot analysis, and the other half was used for viral genomic DNA preparation using the Qiaprep Spin Miniprep kit (Qiagen).
Nonradioactive Southern blotting and DpnI assay
JCV genomic DNA purified from PHFG cells were first digested with DpnI and BamHI enzymes, run on 1 % agarose gel, and then transferred to nylon membranes. Replicated JCV DNA was visualized using a DIG-High Prime DNA Labeling and Detection Kit (Roche, USA) according to the manufacturer’s instructions. The whole Mad1 genome was linearized by BamH1 digestion, labeled with DIG, and used as a probe for hybridization of the membranes as described previously (De Simone et al. 2015).
Detection of viral particles in culture medium by Q-PCR
PHFA and SVGA subcell lines were infected with JCV Mad1 strain as described above. The growth media of the cells (containing viral particles) were collected at 8 days postinfections. The cellular debris in growth media was removed by centrifugation at 14,000 rpm for 10 min. The supernatants were collected and incubated at 95 °C for 10 min to inactivate the virus. Q-PCR analyses were performed to detect and quantify JCV copy numbers in growth media as described previously (Sariyer and Khalili 2011). All Q-PCR analyses were done by using the Lightcycler 480 (Roche). VP1 region of JCV was partially amplified by following primers: JCV Q-PCR-forward: 5′-AGTTGATGGGCAGCCTATGTA-3′ and JCV Q-PCR-reverse: 5′-TCATGTCTGGGTCCCCTGGA-3′. The probe for the Q-PCR was 5′-/HEX/CATGGA TGCTCAAGTAGAGGAGGTTAGAGTTT/3BHQ1/-3′.
Results
Conditioned media from activated immune cells suppress JC virus transcription
Given the fact that the natural occurrence of PML is strongly associated with immunosuppression, the functional and molecular interaction between JCV regulatory proteins and neuroimmune signaling mediated by soluble immune mediators is likely to play a major role in the reactivation of JCV and progression of the lytic viral life cycle leading to the development of PML. The first and essential step in viral reactivation is the potential induction of viral transcription for the expression of viral regulatory as well as structural proteins for the initiation of the viral life cycle. In order to investigate the possible role of neuroimmune signaling in JCV gene expression, we utilized an in vitro cell culture model of primary blood mononuclear cells (PBMCs) and PHFG cultures. Buffy coats were purchased from a vendor to isolate PBMCs. PBMCs were either induced with PMA and ionomycin or left uninduced in culture for 48 h as described in the Materials and methods. Conditioned media from uninduced and induced PBMCs were collected and supplemented into growth media of PHFG cells transfected with JCV reporter constructs. As the noncoding control regions of JCV are comprised of two independent promoters which drive the viral early and late transcripts, we examined the transcriptional activity of both early and late promoters. As shown in Fig. 1, PHFG cells treated with conditioned media from uninduced PBMCs showed a slight increase in late promoter activity and relatively no change in early promoter activity (compare lane 3 with lane 2). On the other hand, the activity of both early and late promoters was significantly reduced when the cells were treated with conditioned media from induced PBMCs (compare lane 4 with lane 2). These data suggest that soluble immune mediators secreted by activated immune cells inhibit JCV promoter activity in both early and late orientations.
Soluble immune mediators secreted by activated PBMCs inhibit JCV early and late gene transcription in PHFG cells. PBMCs were either induced or left uninduced in culture for 48 h as described in the Materials and methods. Conditioned media which contained soluble immune mediators secreted by PBMCs were collected and supplemented into growth media of PHFG cells transfected with JCV early and late reporter constructs. Relative luciferase activities were presented as bar graph. Experiments were carried out in triplicate. Images depict representative data
Soluble immune mediators inhibit JCV replication and induce SRSF1 expression in glial cells
To gain more insight into the immune-glial signaling mediated by soluble immune mediators secreted by activated immune cells, we investigated the effect of conditioned media from PBMCs on JCV replication in glial cells. PHFG cells were infected with the Mad1 strain of JCV and were treated with conditioned media from either uninduced or induced PBMCs at 2, 4, and 6 dpi. Low-molecular-weight viral DNA and whole-cell protein extracts were collected at 8 dpi and analyzed by DpnI/Southern blotting and Western blotting, respectively. The DpnI/Southern blotting assay allows the detection of newly replicated DNA but does not detect the nonreplicated bacterially produced transfected DNA based on ability of the DnpI enzyme to digest the transfected DNA due to differences in methylation. Interestingly, treatment of the cells with conditioned medium from induced but not from uninduced PBMCs caused a significant reduction in the levels of replicated genomic DNA (Fig. 2a, b, compare lanes 4 and 5). These data suggest that immune mediators secreted by activated PBMCs reduced JCV genomic replication. In parallel to the DNA samples, whole-cell protein extracts were also prepared from the same experiments and analyzed by Western blotting for the expression of T antigen and VP1 (Fig. 2c, d). Interestingly, conditioned medium from induced PBMCs showed a significant decrease in T antigen and a slight decrease in VP1 protein levels (compare lane 4 with lanes 2 and 3). We conclude that the observed suppression of viral DNA replication in Fig. 2a by conditioned media is possibly due, at least in part, to the decrease in T antigen and perhaps in VP1 protein levels rather than a direct suppressive impact on viral genomic replication. We have previously identified SRSF1 as a negative regulator of JCV gene expression in glial cells (Sariyer and Khalili 2011; Uleri et al. 2011; Uleri et al. 2013). We sought to analyze the effect of viral infection and soluble immune regulators secreted by activated immune cells on expression of SRSF1 in glial cells. Interestingly, treatment of JCV-infected cells with conditioned media from stimulated PBMCs caused a noticeable increase in the level of SRSF1 expression (Fig. 2c, d), suggesting a possible signaling mechanism between immune mediators secreted by activated PBMCs and SRSF1 in controlling JCV replication.
Conditioned media from PBMCs induces expression of SRSF1 and inhibits replication of JCV in PHFG cells. a DpnI/Sothern blot analysis of replicated JCV genome in PHFG cells. In lane 1, 5 ng Mad1 genome linearized by BamH1 digestion was loaded as positive control (input). In lane 2, DNA samples from uninfected cells were processed and loaded as negative control for the infection. b Band intensities of replicated viral DNA in a were quantified, and relative replication is shown as bar graph from three independent experiments. c Western blot analysis of the expression of JCV large T antigen, capsid protein VP1, and cellular SRSF1 in JCV-infected PHFG cells treated with conditioned media. Tubulin was probed as a loading control. d Band intensities of T antigen, VP1, and SRSF1 expression in c were quantified and are shown as a bar graph
SRSF1 transcription is induced by soluble immune mediators
To further define the neuroimmune induction of SRSF1 expression, we treated PHFG cells with conditioned media from either uninduced or induced PBMCs and analyzed SRSF1 expression by Western blotting. As shown in Fig. 3a, b, SRSF1 expression was increased approximately twofold when the cells were treated with conditioned media from induced but not from uninduced PBMCs in the absence of JCV infection. To gain more insight into the molecular mechanism of SRSF1 induction by immune mediators, the SRSF1 promoter region (−1000 to +49) was cloned into a firefly-luciferase reporter plasmid. PHFG cells were transfected with the SRSF1 reporter construct and treated with conditioned media from uninduced or induced PBMCs. Transcriptional activity of SRSF1 promoter was analyzed by luciferase assay as described in the Materials and methods. As shown in Fig. 3c, basal transcriptional activity of SRSF1 promoter was increased significantly (approximately twofold) when cells were treated with conditioned media from induced PBMCs (compare lane 4 with lane 2). These results suggest that SRSF1 expression in glial cells is possibly regulated by neuroimmune signaling mediated by soluble immune mediators.
SRSF1 transcription is induced by conditioned media from activated PBMCs. a Western blot analyses of SRSF1 expression in PHFG cells treated with conditioned media from PBMCs. b Band intensities of SRSF1 expression from studies presented in a were quantified and are shown as a bar graph. c Conditioned media containing soluble immune mediators secreted by PBMCs were collected and supplemented into growth media of PHFG cells transfected with SRSF1 reporter construct. Relative luciferase activities are presented as a bar graph. All experiments were carried out in triplicate. Images depict representative data
Neuroimmune suppression of JCV transcription is mediated by SRSF1
By using a variety of virological and molecular biological approaches, we have previously demonstrated that the alternative splicing factor, SRSF1, has the capacity to exert a negative effect on transcription of the JCV promoter in glial cells through direct association with a specific DNA sequence within the viral enhancer/promoter region (Sariyer and Khalili 2011; Uleri et al. 2013). Our results from PHFG cells treated with conditioned media from PBMCs suggested a possible regulatory role of immune conditioning in regulation of SRSF1 gene expression resulting in transcriptional suppression of JCV. Therefore, we sought to investigate the role of SRSF1 in neuroimmune suppression of JCV gene transcription in glial cells. PHFG cells were transiently transfected with the JCV early reporter construct along with a siRNA specific for SRSF1. As a control, cells were also transfected with a nontargeting control siRNA (NT-siRNA). As shown in Fig. 4a, cells transfected with NT-siRNA and treated with conditioned media from induced PBMCs showed a strong suppression in JCV transcriptional activity (lane 7). Interestingly, JCV promoter activity suppressed by conditioned media from induced PBMCs was completely restored and further activated by downregulation of SRSF1 using an SRSF1-specific siRNA (compare lane 8 with lane 7). These results suggest that neuroimmune suppression of JCV gene expression may be mediated by SRSF1 in glial cells.
SRSF1 is required for the transcriptional suppression of JCV by soluble immune mediators. a Conditioned media containing soluble immune mediators secreted by either induced or uninduced PBMCs were collected and supplemented into growth media of PHFG cells transiently transfected with a SRSF1 reporter construct and an siRNA specific for SRSF1 or a nontargeting control siRNA (NT-siRNA). Relative luciferase activities were determined and are presented as a bar graph. All experiments were carried out in triplicate. b PHFG cells were transfected either with an siRNA specific for SRSF1 or a nontargeting siRNA (NT-siRNA) in increasing concentrations. Whole-cell protein lysates were analyzed by Western blotting for the detection of SRSF1 expression. Tubulin was probed as loading control
Soluble immune mediators fail to suppress JCV replication in SVG-A subclones with downregulated SRSF1 expression
To investigate the involvement of SRSF1 in suppression of JCV replication by soluble immune mediators, we stably downregulated SRSF1 expression in SVG-A cells with a lentivirus construct encoding shRNA that specifically targets SRSF1 expression. SVG-A cells were transiently transfected with lentiviral constructs encoding either GFP alone or SRSF1-shRNA in addition to GFP in combination with a plasmid carrying a G418 resistance gene, and cells were grown for 2 to 3 weeks in G418-containing medium. Subclones of SVG-A were selected and analyzed for the downregulation of SRSF1. A representative SVG-A subclone with approximately 50 % downregulation of SRSF1 protein levels was characterized and is shown in Fig. 5a–c.
Generation of an SVG-A subclone with constitutive downregulation of SRSF1 expression. a SVG-A cells were transiently transfected with a lentiviral construct encoding either GFP alone or SRSF1-shRNA in addition to GFP in combination with a plasmid carrying the G418 resistance gene, and cells were grown for 2 to 3 weeks in G418 containing medium. Subclones of the SVG-A cells were selected as described in the Materials and methods. Phase contrast and GFP expression images of representative subclones are shown. b Western blot analysis of SRSF1 expression in SVG-A subclones are presented in a. Tubulin was probed as loading control. c Band intensities of SRSF1 expression in b were quantified and are shown as a bar graph
In the next series of experiments, we analyzed JCV infection and the impact of soluble immune mediators on JCV propagation in the SVG-A subclone presented in Fig. 5a. Cells were infected with the Mad1 strain of JCV as described in the Materials and methods and treated with conditioned media from either uninduced or induced PBMCs. Whole-cell protein lysates were collected at 10 dpi and analyzed by Western blotting for the detection of the major viral capsid protein, VP1. As shown in Fig. 6a, comparable levels of VP1 expression were detected in SVG-A cells with GFP expression (lane 2) and in cells with GFP and SRSF1-shRNA (lane 6). As expected, treatment of the control cells (SVG-A-GFP) with conditioned medium from induced but not from uninduced PBMCs showed a dramatic reduction in the levels of VP1 (compare lane 4 with lane 3), suggesting that soluble immune mediators secreted by activated PBMCs suppress JCV propagation in SVG-A cells. On the other hand, treatment of the SVG-A subclonal cells with downregulated levels of SRSF1 (SVG-A-GFP-SRSF1-shRNA) with conditioned media from induced PBMCs resulted in a comparable levels of VP1 expression with the cells treated with conditioned media from uninduced PBMCs (compare lanes 7 and 8). In parallel to cellular extracts, the growth media of the cells was also collected and subjected to Q-PCR for the detection of viral genomic DNA from the same infection studies presented in Fig. 6a. Consistent with VP1 expression, conditioned media from induced PBMCs caused a dramatic decrease in viral copy numbers in SVG-A-GFP cells (Fig. 6b). On the other hand, SVG-A-GFP + SRSF1-shRNA cells showed comparable levels of viral copies with control infections when treated with conditioned media from induced PBMCs. These results suggest that soluble immune mediators secreted by activated immune cells may require SRSF1 to suppress JCV propagation in glial cells.
Conditioned media from induced PBMCs fail to suppress JCV propagation in SVG-A subclones with constitutive expression of SRSF1-shRNA. a Western blot analysis of VP1 expression in SVG-A subclones infected with the JCV Mad1 strain. SVG-A subclones with constitutive expression of GFP or GFP + SRSF1-shRNA were infected with the JCV Mad1 strain and treated with conditioned media from either uninduced or induced PBMCs at 2, 5, and 8 dpi. Whole-cell protein lysates were collected at 10 dpi and analyzed by Western blotting for the detection of VP1 expression. Tubulin was probed as loading control. b Q-PCR analysis of viral DNA copies in growth media of SVG-A subclones infected with JCV. Growth media was collected in parallel to whole-cell protein extracts from the infections presented in a. JCV DNA copies in culture media were determined by Q-PCR as described in the Materials and methods
Discussion
There is little known about the immunobiology of JCV reactivation in glial cells and the role of immune, glial, and viral players in this regulation. Since the natural occurrence of PML is strongly associated with immunosuppression, neuroimmune interactions are likely to play a major role in controlling JCV reactivation and the progression of the lytic life cycle leading to the development of PML. Neuroimmune interaction is an extensive bidirectional communication taking place between nervous and immune system in both health and disease. Presumably the same molecules, cytokines/chemokines, neurotransmitters, and neurotropic factors are involved as mediators in both directions (Pacheco et al. 2012). Here, we investigated the effects of soluble immune mediators (cytokines/chemokines) secreted by activated PBMCs on JCV gene expression and replication. Our results suggest that JCV gene expression and viral replication is controlled by immune conditioning of glial cells by activated PBMCs. Moreover, we also showed that SRSF1, shown to be a strong inhibitor of JC virus gene expression (Uleri et al. 2013; Sariyer and Khalili 2011), is required for the immune mediated suppression of JCV replication.
Cell type-specific reactivation of JCV in glial cells is primarily regulated at the transcriptional level (White et al. 2009, 2015). In this respect, several transcription factors including YB-1, Purα, Egr-1, c-jun, NF1, and others have been identified based on their ability to modulate JCV promoter activities in glial cells (Chang et al. 1996; Safak et al. 2002; Ravichandran et al. 2006; Romagnoli et al. 2008). Of note, none of these regulators have been associated with JCV latency or have been shown to be involved in viral reactivation. One may speculate that the combination of ubiquitous negative and inducible positive glial specific factors may determine the level of viral gene expression during the process of viral reactivation. We previously identified an RNA splicing regulatory protein, SRSF1, ubiquitously expressed in all cell types, as a negative regulator of JCV gene transcription in glial cells (Sariyer and Khalili 2011). While SRSF1 plays a role in splicing viral transcripts, it has a profound impact on transcription of the viral genome and replication of JCV. Overexpression of SRSF1 suppresses JCV gene transcription in human glial cells. Accordingly, suppression of SRSF1 enhances the level of viral replication in glial cells. Here, we showed that soluble immune mediators secreted by activated PBMCs suppress JCV replication and induce SRSF1 protein levels in glial cells. Moreover, glial cells with low levels of SRSF1 expression failed to suppress JCV under neuroimmune conditioning, suggesting that SRSF1 is required for the neuroimmune suppression of JCV gene expression and perhaps for the maintenance of viral latency (see proposed model, Fig. 7). The exact role of SRSF1 in JCV latency and viral reactivation remains to be investigated.
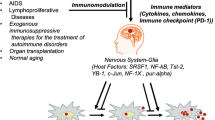
Proposed model of JC virus reactivation in glial cells. JC virus infects and establishes a latent infection in glial cells in immunocompetent individuals. During the latent phase, JCV remains relatively silent and viral gene expression is tightly controlled by SRSF1 whose expression is regulated by neuroimmune signaling mediated by soluble immune mediators. Alteration of the delicate balance between neuroimmune signaling and SRSF1 in immunocompromised individuals may result in expression of the JCV early genes and initial replication of the JCV genome causing viral reactivation. If immunomodulation persists, JCV may undergo productive replication and complete its lytic cycle leading to the development of PML
The key to understanding JCV reactivation will require teasing out the complex regulations that underlie the expression of viral genes and neuroimmune interactions that suppress or activate viral replication. JCV replicates only in human cells and investigation of the role of neuroimmune interactions in JCV reactivation and the development of PML has been severely hampered by the lack of a suitable animal model for JCV replication and reactivation studies. Because there is no suitable animal model for PML, we modelized human PBMCs and PHFG cells in a cell culture setting as the source of soluble immune mediators and glial cells in our JCV studies. Our results suggest that JCV gene transcription is under the negative control of soluble immune mediators which are composed of a combination of cytokines and chemokines expressed by activated PBMCs. Cytokine/chemokine arrays of supernatants from PBMCs upon induction with PMA/ionomycin have been shown to secrete robustly increased levels of IL2, Rantes, IFN-γ, IL-1β, IL-13, and IL-3 and a concomitant decrease in secretion of MCP-1, MDC, and MIG (De Simone et al. 2015). Future investigation of these cytokines individually or in combination in the suppression of JCV transcription and induction of SRSF1 gene expression is needed to further define the molecular pathways associated with neuroimmune regulation of JCV.
In conclusion, our results have revealed a novel neuroimmune signaling between SRSF1 and PBMCs mediated by soluble immune mediators (cytokines and chemokines) in the regulation of JCV gene expression, and provide a new avenue of research to understand the molecular mechanism of JCV reactivation in patients who are at risk of developing PML.
References
Berger JR, Khalili K (2011) The pathogenesis of progressive multifocal leucoencephalopathy. Discov Med 12(67):495–503
Brew BJ, Davies NW, Cinque P, Clifford DB, Nath A (2010) Progressive multifocal leukoencephalopathy and other forms of JC virus disease. Nat Rev Neurol 6(12):667–679
Carruthers RL, Berger J (2014) Progressive multifocal leukoencephalopathy and JC Virus-related disease in modern neurology practice. Mult Scler Relat Disord 3(4):419–430. doi:10.1016/j.msard.2014.01.005
Carson KR, Focosi D, Major EO, Petrini M, Richey EA, West DP, Bennett CL (2009) Monoclonal antibody-associated progressive multifocal leucoencephalopathy in patients treated with rituximab, natalizumab, and efalizumab: a review from the Research on Adverse Drug Events and Reports (RADAR) Project. Lancet Oncol 10(8):816–824
Chang CF, Gallia GL, Muralidharan V, Chen NN, Zoltick P, Johnson E, Khalili K (1996) Evidence that replication of human neurotropic JC virus DNA in glial cells is regulated by the sequence-specific single-stranded DNA-binding protein Pur alpha. J Virol 70(6):4150–4156
De Simone F, Sariyer R, Lopez Otalora Y, Craigie M, Gordon J, Sariyer IK (2015) IFN-gamma inhibits JC virus replication in glial cells by suppressing T-antigen expression. PLoS ONE 10(6), e0129694
Du Pasquier RA, Schmitz JE, Jean-Jacques J, Zheng Y, Gordon J, Khalili K, Letvin NL, Koralnik IJ (2004) Detection of JC virus-specific cytotoxic T lymphocytes in healthy individuals. J Virol 78:10206–10210
Eng PM, Turnbull BR, Cook SF, Davidson JE, Kurth T, Seeger JD (2006) Characteristics and antecedents of progressive multifocal leukoencephalopathy in an insured population. Neurology 67(5):884–886
Ferenczy MW, Marshall LJ, Nelson CD, Atwood WJ, Nath A, Khalili K, Major EO (2012) Molecular biology, epidemiology, and pathogenesis of progressive multifocal leukoencephalopathy, the JC virus-induced demyelinating disease of the human brain. Clin Microbiol Rev 25(3):471–506. doi:10.1128/CMR.05031-11
Focosi D, Marco T, Kast RE, Maggi F, Ceccherini-Nelli L, Petrini M (2010) Progressive multifocal leukoencephalopathy: what’s new? Neuroscientist 16(3):308–323
Kleinschmidt-DeMasters BK, Tyler KL (2005) Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis. N Engl J Med 353(4):369–374
Koralnik IJ (2002) Overview of the cellular immunity against JC virus in progressive multifocal leukoencephalopathy. J Neurovirol 8(Suppl 2):59–65
Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D (2005) Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 353(4):375–381
Lashgari MS, Tada H, Amini S, Khalili K (1989) Regulation of JCVL promoter function: transactivation of JCVL promoter by JCV and SV40 early proteins. Virology 170:292–295
Major EO, Miller AE, Mourrain P, Traub RG, de Widt E, Sever J (1985) Establishment of a line of human fetal glial cells that supports JC virus multiplication. Proc Natl Acad Sci U S A 82:1257–1261
Moens U, Johannessen M (2008) Human polyomaviruses and cancer: expanding repertoire. J Dtsch Dermatol Ges 6(9):704–708
Pacheco R, Contreras F, Prado (2012) Cells, molecules and mechanisms involved in the neuro-immune interaction. In: Gowder S (ed) Cell Interaction. ISBN 978-953-51-0792-7
Padgett BL, Zu Rhein GM, Walker DL, Echroade R, Dessel B (1971) Cultivation of papova-like virus from human brain with progressive multifocal leukoencephalopathy. Lancet 1:1257–1260
Ravichandran V, Sabath BF, Jensen PN, Houff SA, Major EO (2006) Interactions between c-Jun, nuclear factor 1, and JC virus promoter sequences: implications for viral tropism. J Virol 80(21):10506–10513
Romagnoli L, Sariyer IK, Tung J, Feliciano M, Sawaya BE, Del Valle L, Ferrante P, Khalili K, Safak M, White MK (2008) Early growth response-1 protein is induced by JC virus infection and binds and regulates the JC virus promoter. Virology 375(2):331–341
Safak M, Sadowska B, Barrucco R, Khalili K (2002) Functional interaction between JC virus late regulatory agnoprotein and cellular Y-box binding transcription factor, YB-1. J Virol 76(8):3828–3838
Safak M, Major E, Khalili K (2005) Human polyomavirus, JC virus, and progressive multifocal encephalopathy. In: Howard IG, Gendelman E, Everall IP, Lipton SA, Swindells S (eds) The neurology of AIDS. Oxford University Press, New York, pp 461–474
San-Andres FJ, Rubio R, Castilla J, Pulido F, Palao G, de Pedro I, Costa JR, del Palacio A (2003) Incidence of acquired immunodeficiency syndrome- associated opportunistic diseases and the effect of treatment on a cohort of 1115 patients infected with human immunodeficiency virus, 1989–1997. Clin Infect Dis 36(9):1177–1185
Sandborn WJ, Colombel JF, Enns R, Feagan BG, Hanauer SB, Lawrance IC, Panaccione R, Sanders M, Schreiber S, Targan S, van Deventer S, Goldblum R, Despain D, Hogge GS, Rutgeerts P (2005) Natalizumab induction and maintenance therapy for Crohn’s disease. International Efficacy of Natalizumab as Active Crohn’s Therapy (ENACT-1) Trial Group; Evaluation of Natalizumab as Continuous Therapy (ENACT-2) Trial Group. N Engl J Med 353(4):375–381
Sariyer IK, Khalili K (2011) Regulation of human neurotropic polyomavirus, JCV, by alternative splicing factor, SF2/ASF, in glial cells. PLoS ONE 6(1), e14630
Uleri E, Beltrami S, Gordon J, Dolei A, Sariyer IK (2011) Extinction of tumor antigen expression by SF2/ASF in JCV transformed cells. Genes Cancer 2(7):728–736
Uleri E, Regan P, Patel PK, Sariyer IK (2013) SF2/ASF binding region within JC virus NCCR limits early gene transcription in glial cells. Virol J 10(1):147
Warnke C, Olsson T, Hartung HP (2015) PML: The dark side of immunotherapy in multiple sclerosis. Trends Pharmacol Sci
Weber T (2008) Progressive multifocal leukoencephalopathy. Neurol Clin 26(2008):833–854
White MK, Safak M, Khalili K (2009) Regulation of gene expression in primate polyomaviruses. J Virol 83(21):10846–10856
White MK, Gordon J, Berger JR, Khalili K (2015) Animal models for progressive multifocal leukoencephalopathy. J Cell Physiol 230(12):2869–2874
Wollebo HS, Safak M, Del Valle L, Khalili K, White MK (2011) Role for tumor necrosis factor-alpha in JC virus reactivation and progressive multifocal leukoencephalopathy. J Neurovirol 233(1–2):46–53
Wüthrich C, Kesari S, Kim WK, Williams K, Gelman R, Elmeric D, De Girolami U, Joseph JT, Hedley-Whyte T, Koralnik IJ (2006) Characterization of lymphocytic infiltrates in progressive multifocal leukoencephalopathy: co-localization of CD8(+) T cells with JCV-infected glial cells. J Neurovirol 12(2):116–128
Zheng HC, Yan L, Cui L, Guan YF, Takano Y (2009) Mapping the history and current situation of research on John Cunningham virus—a bibliometric analysis. BMC Infect Dis 9:28
Acknowledgments
The authors thank the past and present members of the Department of Neuroscience and Center for Neurovirology for sharing their ideas and reagents, particularly Dr. Kamel Khalili. Research reported in this publication was supported by the National Institute of Allergy and Infectious Diseases of the National Institutes of Health under award numbers R01AI101192 and R21NS081447. This study utilized services offered by core facilities of the Basic Science II Core Facility of the Temple P30 Comprehensive NeuroAIDS Center, Department of Neuroscience (CNAC NIMH Grant Number P30MH092177) at the Lewis Katz School of Medicine at Temple University School. The funding organizations played no role in the design of the study, in the collection, analysis, and interpretation of the data, or in the decision to submit this manuscript for publication. This work was partially presented at the 12th International Symposium on NeuroVirology meeting October 29–November 2, 2013, Washington DC, USA.
Author contributions
Conceived and designed the experiments: IKS. Performed the experiments: RS and FIDS. Analyzed the data: IKS and JG. Contributed reagents/materials/analysis tools: IKS and JG. Wrote the paper: IKS.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
RS and FIDS contributed equally to this work.
Rights and permissions
About this article
Cite this article
Sariyer, R., De-Simone, F.I., Gordon, J. et al. Immune suppression of JC virus gene expression is mediated by SRSF1. J. Neurovirol. 22, 597–606 (2016). https://doi.org/10.1007/s13365-016-0432-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13365-016-0432-9