Abstract
The aim of the current investigation was to assess the ability GFJ to modulate the pharmacokinetic profile of paracetamol following single or repeated administrations of GFJ in Sprague–Dawley rats. Diclofenac and carbamazepine were both used as positive controls. Rats received single GFJ or single distilled water doses or pretreated with three doses of GFJ prior to test drug administration. Blood samples were collected, processed and analyzed using validated HPLC methods, and pharmacokinetic data were constructed for each group. Increase in the bioavailability of both diclofenac and carbamazepine following multiple GFJ ingestion was revealed. Conversely, the bioavailability of paracetamol was significantly reduced following multiple GFJ administration. The percentage of reduction in the C max and AUC of paracetamol were calculated as 31 and 51 %, respectively, compared to none-GFJ-treated control (P < 0.05). The T max was not essentially changed. In conclusion, frequent administration of GFJ was confirmed to modulate the pharmacokinetics of paracetamol in rats by reducing its bioavailability. Meanwhile, it may be advisable not to ingest large amounts of GFJ along with paracetamol to avoid a possible potential loss of the efficacy.
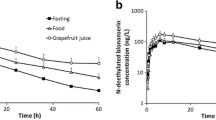
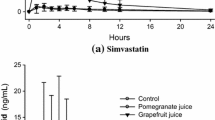
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Grapefruit (Citrus paradisi), particularly as juice (GFJ), is largely consumed by the general population. Through its inhibitory actions on the intestinal cytochrome P-450 (CYP) 3A4 system, GFJ can alter the bioavailability of many medications leading to serious consequences. The main reported action of grapefruit is increasing serum concentration of many drugs by inhibiting their pre-systemic (first-pass) metabolism in the intestine due to the presence of furanocoumarins in the juice (Paine et al. 2004). Such drug–food interaction has been reported in both white and colored (pink and red) grapefruit species that contains lower amounts of the furanocoumarin derivatives. Nevertheless, it was found that white and colored GFJ may be equipotent in producing drug interactions (Uesawa et al. 2008).
However, other reports indicated decreased plasma concentration of some drugs when ingested with GFJ. Among these are fexofenadine and talinolol (Dresser et al. 2002; Schwarz et al. 2005). This unusual interaction had been mainly attributed to the ability of GFJ to modulate the actions of efflux and uptake transport proteins that are present in the intestinal lumen (Hanley et al. 2011; Won et al. 2010). The most reported efflux protein affected by GFJ is the P-glycoprotein (P-gp) (Dahan and Amidon 2009). By inhibiting P-gp pumps, the efflux of drug molecules towards the intestinal lumen would be reduced, therefore, increasing their systemic concentrations and vise versa. However, definitive evidence supporting in vivo inhibition or activation of P-gp by GFJ is limited (Hanley et al. 2011; Deferme and Augustijns 2003). On the other hand, GFJ may also inhibit the organic anion-transporting peptide (OATP), which is a transmembrane sodium-ATP-independent transporter found in the intestinal mucosa and promotes uptake of drugs into the enterocytes (Bailey et al. 2007). The inhibition of OATP results in reduced blood levels of the drug substrate. This contradicts the actions of inhibition of CYP3A4 or P-gp by GFJ, which result in increased levels of circulating drugs.
Most of the previously reported drug–GFJ interactions focused mainly on prescription drugs with low therapeutic indices, extensive CYP first-pass metabolism or those with low systemic bioavailability thus, requiring high therapeutic doses. Conversely, GFJ interactions with many of over the counter (OTC) drugs are generally disregarded perhaps due to their wide margin of safety and large exposure. While GFJ interactions with some OTC drugs have been previously confirmed, such as a positive interaction with dextromethorphan or the negative interaction with caffeine (Maish et al. 1996; Strauch et al. 2009), interactions of GFJ with many other OTC drugs are still to be explored.
Paracetamol (acetaminophen, APAP) is a widely used OTC drug in both adult and pediatric practice. Due to its potent analgesic and antipyretic actions, it is often classified as a non-steroidal anti-inflammatory drug (NSAID), however, it lacks the other typical actions of NSAIDs such as antiplatelet activity and gastrotoxicity (Botting 2000). Glucuronidation and sulphation are recognized as major metabolic pathways of paracetamol while oxidation, mainly by CYP2E1, is considered a minor metabolic pathway (Bessems and Vermeulen 2001; Kim et al. 2011).
Since paracetamol is acknowledged for its safety within therapeutic doses, high exposure, its convenient bioavailability and low CYP first-pass metabolism, it seems to be an insignificant candidate for drug–GFJ interaction investigations. Nevertheless, it has been previously demonstrated that GFJ can change the bioavailability of paracetamol in human saliva and surprisingly, by reducing the salivary levels of paracetamol when ingested with GFJ (Qinna et al. 2012). No other human in vivo interactions between GFJ and paracetamol have been clinically reported in the literature so far. Conversely, previous preclinical studies on rodents confirmed the presence of drug–food interaction between GFJ and paracetamol where the levels of paracetamol or its activity was concluded higher when ingested with GFJ (Dasgupta et al. 2008; Samojlik et al. 1999).
Therefore, the aim of the present study was to confirm the pharmacokinetic interaction between single and multiple doses of white GFJ with paracetamol in Sprague–Dawley rats. Diclofenac sodium (NSAID) and carbamazepine (anticonvulsant), both known to be metabolized by CYP3A4 in the gut wall and the liver (Garg et al. 1998; Zhu and Zhang 2012), were likewise investigated with paracetamol as positive controls.
2 Materials and methods
2.1 Drugs and chemicals
Sodium hydroxide and HPLC grade of methanol, acetonitrile and deionized water (HiPerSolv CHROMANORM®) were purchased from VWR International LLC, IL, USA. Perchloric acid, tert-Butyl methyl ether (Uvasol®) and 85 % phosphoric acid were purchased from Merck KGaA, Darmstadt, Germany. Triethylamine was obtained from Acros Organics, NJ, USA. Pharmaceutical grade of diclofenac sodium, paracetamol and metronidazole benzoate were kindly supplied by the Jordanian Pharmaceutical Manufacturing Co. Plc., Amman, Jordan. Mefenamic acid and carbamazepine were a kind gift from JOSWE Company, Amman, Jordan. Cefadroxil was kindly supplied by MidPharma Company, Amman, Jordan. Rat serum was freshly prepared and screened for interfering peaks prior to use.
2.2 Grapefruit juice preparation
White grapefruit ripe fruits cultivated in the Jordan Valley were purchased from a local market (Amman, Jordan). GFJ was fresh hand squeezed at the day of experimentation without any further treatment or additives and kept refrigerated at 4 °C until used.
2.3 Animal handling
Adult male Sprague–Dawley (SD) rats with an average weight of 220 ± 20 g were purchased from Yarmouk University (Irbid, Jordan) and accommodated at the University of Petra’s Animal House (Amman, Jordan) under controlled temperature (22–24 °C), humidity (55–65 %) and a 12-h light/dark photoperiod cycle and were offered standard pellet diet (Jordan Feed Co. Ltd, Amman, Jordan) and tap water ad libitum. All rats were acclimatized for 14 days before experimentation. All experiments were carried out in accordance with University of Petra’s institutional Guidelines on Animal Use that adopts the guidelines of the Federation of European Laboratory Animal Sciences Association (FELASA). The study protocol (Pharm6/13) was revised and approved (Approval number: 5, 28th Feb 2013) by the Ethical Committee of the Higher Research Council at the Faculty of Pharmacy and Medical Sciences, University of Petra (Amman, Jordan).
2.4 In vivo experimental design
For each experiment, rats were randomized into three groups (n = 10 rats/group). Fasting rats (12 h, water ad libitum) in the first and second groups were administered a single dose of distilled water or GFJ (10 ml/kg) 30 min prior the assigned drug administration. As for the third group, rats were administered multiple doses of GFJ (10 ml/kg) at 28 and 20 h then at 30 min prior drug administration to 12 h fasting rats.
All drugs were dissolved in distilled water and freshly prepared for each experiment. Rats received paracetamol (10 mg/kg), diclofenac sodium (2 mg/kg) or carbamazepine (30 mg/kg) using a stainless steel oral gavage needle (Harvard Apparatus, USA).
Blood samples were collected by pooling one drop of blood from each rat tail tip into a labeled Eppendorf tube just before drug administration (0 h) and at a specific time intervals (0.5, 1, 2, 3, 4, 6 h) post-drug administration. An extra blood sample at 8 h was collected for carbamazepine-treated rats due to its long half-life. Collected blood samples were allowed to clot at room temperature and centrifuged for 5 min at 6,000 rpm using a Hettich EBA 20 centrifuge, Tuttlingen, Germany. The serum was then collected and stored at −20 °C until analyzed.
2.5 Instrumentation and chromatographic conditions
Drugs in serum samples were analyzed using a Merck-Hitachi high-performance liquid chromatography (HPLC) system (Merck-Hitachi, Japan) consisted of L-7100 LaChrom pump, L-7400 Lachrom UV detector, an L-7200 Lachrom autosampler and a D-7000 Interface. A Hypersil BDS C18 analytical column (Thermo Scientific, NJ, USA) with dimensions of 150 × 4.6 mm and a particle size of 5 μm was utilized for all investigated drugs. Cefadroxil, mefenamic acid and metronidazole benzoate were used as internal standards (IS) in analyzing paracetamol, diclofenac sodium and carbamazepine, respectively. The used chromatographic conditions for the investigated drugs are summarized in Table 1.
2.6 Preparation of calibration standards
All investigated drugs were dissolved initially in methanol at a concentration of 1,000 μg/ml (Stock A). The following dilutions were prepared by spiking Stock A in freshly separated rat serum: 0.25, 1.0, 3.0, 5.0, 10.0 and 20.0 μg/ml for paracetamol and 0.1, 0.2, 0.5, 1.0, 1.5 and 2.0 μg/ml for diclofenac sodium, respectively. For carbamazepine, 1.25 ml of Stock A was further diluted in 10 ml acetonitrile to obtain Stock B with a final drug concentration of 125 μg/ml. Stock B solution was used to spike rat serum at the following dilutions: 0.05, 0.10, 0.50, 1.00, 2.00, 3.00, and 5.00 μg/ml. All prepared samples were kept at 4–8 °C until injected in their corresponding HPLC system (Table 1). Calibration curves were constructed by plotting the peak area ratios (drug/IS) versus the concentrations of the drugs.
2.7 Sample preparation
For paracetamol test samples preparation, 20 μl of the internal standard (50 μg/ml of cefadroxil dissolved in methanol) was added to 100 μl of rat serum in a test tube, then 200 μl of 5 % perchloric acid was added to the mixture and vortex-mixed for 30 s then centrifuged for 10 min at 14,000 rpm (Sorvall centrifuge, model: SuperSpeed RC2–B, Thermo Fisher Scientific Inc., Waltham, MA, USA). The supernatant was injected into the HPLC column. Representative chromatograms of paracetamol analysis in processed serum samples obtained from GFJ-administered rats are shown in Fig. 1.
Representative HPLC chromatograms of analyzed Sprague–Dawley rat serum samples. The shown chromatograms represents a group treated with multiple doses of GFJ illustrating (a), a processed blank serum sample (b) a serum sample spiked with cefadroxil; the internal standard of paracetamol analysis and (c). A processed serum sample withdrawn 30 min post-paracetamol administration and spiked with the internal standard. Asterisk paracetamol glucuronide according to an in-house verification
For diclofenac sodium test samples preparation, 50 μl of the internal standard (3 μg/ml of mefenamic acid dissolved in methanol) was added to 100 μl of rat serum in a test tube, then 35 μl of 2.4 % perchloric acid was added and the mixture was vortex-mixed, then 6 ml of tert-Butyl methyl ether was added to the mixture and vortex-mixed for 30 s then centrifuged for 10 min. The upper layer was transferred to another tube contain 200 μl of 75 mM sodium hydroxide, vortex-mixed for 1 min then centrifuged for 6 min at 14,000 rpm. The lower layer was injected into the HPLC Column.
For the preparation of carbamazepine test samples, 300 μl of acetonitrile containing 7.5 μg/ml metronidazole benzoate was added to 200 μl of rat serum, the mixture was vortex-mixed for 30 s and centrifuged for 10 min at 14,000 rpm. The supernatant was injected into the HPLC column. Apart from the test samples, each analytical run consisted of the six calibration standards, duplicate quality control samples (at three concentration levels) and a drug-free serum sample that were randomly positioned in the HPLC autosampler.
2.8 Analytical methods validations
All analytical methods were developed and validated in-house. The validation of the analytical methods of paracetamol, diclofenac and carbamazepine in rats’ serum included specificity, linearity of response, accuracy, precision, Limit of Quantification (LOQ) validations and stability as detailed in Table 2. The validation data were generated from the seven points plotted standard curves, including LOQ samples, along with three different concentrations of quality control (QC) samples for each drug.
2.9 Data analysis
Pharmacokinetic parameters for the measured serum drug concentrations were calculated by non-compartmental analysis (NCA) using Kinetica™ software version 5 (Thermo Fisher Scientific Inc., Waltham, MA, USA). The pharmacokinetics were characterized by maximum concentration in serum (C max), time to maximum serum concentration (T max) and AUC between zero time (pre-drug administration) and last sampling time post-dosing (AUC0–last). All data are expressed as mean ± SEM. Results were analyzed by two-tailed Student’s t test. The acceptable level of significance was established at P < 0.05.
3 Results
3.1 Method validations
Validation data of the presented HPLC methods are summarized in Table 2. The developed methods for analyzing paracetamol, diclofenac sodium and carbamazepine in rat serum showed convenient linearity in the tested concentration ranges. The precision and the accuracy of the used methods were satisfactory. The presented methods can be described as rapid, precise, sample-saving and considerably stable for analyzing rat serum samples of the three investigated drugs. Since all validations were performed on serum samples obtained from GFJ-untreated rats, selected serum samples obtained from GFJ-administered rats, post 30 min of GFJ intake, were also spiked with the drugs and their corresponding internal standards. It was observed that none of GFJ components was co-eluted with any of the spiked drugs.
3.2 Effect of GFJ ingestion on paracetamol pharmacokinetics
The mean serum concentration–time profiles of paracetamol following ingestion of single and multiple doses of GFJ compared to water-administered rats are illustrated in Fig. 2 while the key pharmacokinetic parameters of paracetamol–GFJ interactions are summarized in Table 3. The kinetic parameters of paracetamol following a single administration of GFJ were not altered compared to DW group (P > 0.05). However, significant reductions in the C max and AUC were obtained when rats were pre-administered multiple doses of GFJ (P < 0.05). The percentage of reduction in the C max and AUC were calculated as 31 and 51 %, respectively, compared to DW control group. The T max values were comparable in all groups without any noticeable shifting.
Paracetamol serum concentration versus time profiles. Rats were randomized into groups and pre-administered water (DW), a single dose of grapefruit juice (GFJ Single) or multiple doses of grapefruit juice (GFJ Multiple) prior paracetamol (10 mg/kg) oral administration. Each data point represents the mean ± SEM of five to six independent experiments
3.3 Effect of GFJ ingestion on diclofenac sodium pharmacokinetics
Results of pharmacokinetic interaction between GFJ and diclofenac sodium are illustrated in Fig. 3 and Table 3. Multiple GFJ administration propagated the serum concentration profile of diclofenac sodium where the AUC mean values were significantly increased compared to both single GFJ and DW groups (P < 0.05). However, the C max and T max were not changed following multiple GJF administration. On the other hand, no significant alterations were seen in the reported pharmacokinetic parameters of diclofenac sodium when rats were administered a single dose of GFJ (P > 0.05).
Diclofenac sodium serum concentration versus time profiles. Rats were randomized into groups and pre-administered water (DW), a single dose of grapefruit juice (GFJ Single) or multiple doses of grapefruit juice (GFJ Multiple) prior Diclofenac sodium (2 mg/kg) oral administration. Each data point represents the mean ± SEM of five to six independent experiments
3.4 Effect of GFJ ingestion on carbamazepine pharmacokinetics
Multiple GFJ administration to rats significantly increased the serum concentration of carbamazepine compared to single GFJ administration (Fig. 4). The calculated AUC of carbamazepine following multiple GFJ administration was nearly doubled compared to the other groups (P < 0.05). The C max was also increased in the case of multiple GFJ administration (P < 0.05) while a considerable shift in the T max was noticed but rather insignificantly (P > 0.05) due to the presence of high variation (Table 3).
Carbamazepine serum concentration versus time profiles. Rats were randomized into groups and pre-administered water (DW), a single dose of grapefruit juice (GFJ Single) or multiple doses of grapefruit juice (GFJ Multiple) prior carbamazepine (30 mg/kg) oral administration. Each data point represents the mean ± SEM of five to six independent experiments
4 Discussion
Many pharmacokinetic studies have demonstrated that GFJ can increase the bioavailability of drugs from an array of therapeutic classes as a result of irreversible inhibition of CYP3A4 by furanocoumarins present in the juice. However, due to the presence of multiple phytochemical components in GFJ, other mechanisms might be involved in reducing the bioavailability of some drugs when co-administered with GFJ. Most of these mechanisms, however, lack clinical evidence (Hanley et al. 2011).
Available information on in vivo interactions between GFJ and paracetamol is limited. A previous finding showed that salivary levels of paracetamol in human were reduced following concurrent administration of GFJ (Qinna et al. 2012). The current research was initiated to confirm such an interaction preclinically in rats.
Therefore, validated rat serum sampling and analysis procedures were utilized to reveal any in vivo pharmacokinetic interactions that might occur in rats between paracetamol and GFJ compared to diclofenac sodium and carbamazepine.
In the current research, paracetamol bioavailability was confirmed to be reduced in rats after multiple GFJ consumption as evident by significant reductions in the C max and AUC by 31 and 51 %, respectively. On the other hand, a single dose of GFJ did not affect any of the tested parameters (Table 3). On the other hand, serum levels of diclofenac sodium and carbamazepine, both used as positive controls for GFJ-drug interactions, were significantly increased post-multiple GFJ ingestion in rats (P < 0.05). A single dose of GFJ was also found ineffective in modulating the pharmacokinetic parameters of both control drugs. It has been reported that concomitant administration of a single dose of GFJ is sufficient to produce considerable pharmacokinetic interactions with some drugs in human and rats (Boddu et al. 2009; Takanaga et al. 2000). This effect, however, can last for 72 h post-GFJ intake (Takanaga et al. 2000).
Since diclofenac and carbamazepine have been previously reported being highly metabolized by CYP450, the increase in their bioavailability following multiple GFJ ingestion was expected (Garg et al. 1998; Zhu and Zhang 2012). For example, in a pharmacokinetic interaction between diclofenac and GFJ in Wistar rats, it was found that plasma levels of diclofenac were elevated following repeated administration of GFJ (Cuciureanu et al. 2008). Moreover, it was found that GFJ can directly potentiate the anti-inflammatory action of diclofenac in rats (Mahgoub 2002) and can indirectly ameliorate diclofenac-induced intestinal toxicity in mice (Zhu and Zhang 2012); effects that have also been related to the inhibition of intestinal CYP450. On the other hand, it was reported in a clinical trial that human plasma concentration of carbamazepine was significantly increased when ingested concomitantly with GFJ compared to water (Garg et al. 1998).
As a relatively safe and widely investigated drug, the pharmacokinetic of paracetamol is well established (Prescott 1980). The absorption of paracetamol from human GIT is usually rapid in which the peak plasma concentration is attained within 30–60 min. Nonetheless, the absorption of paracetamol is somehow dependent on gastric emptying and, therefore, drugs that alter gastric emptying can change its pharmacokinetics (Toes et al. 2005). Paracetamol becomes distributed into most tissues of the body, and plasma protein binding is negligible at therapeutic doses (Kalantzi et al. 2006). Paracetamol is mainly metabolized in the liver, and to a less degree in the intestine and kidneys, which occurs by conjugation. These conjugates are eliminated mainly through urine. However, only small amount of paracetamol (about 1 %) is metabolized by CYP450 in an oxidative pathway forming N-acetyl-p-benzoquinone imine (NAPQI) which is later conjugated with glutathione and excreted (Bessems and Vermeulen 2001; Laine et al. 2009). Since NAPQI is a toxic metabolite, most research attempts were directed towards paracetamol’s overdose and liver toxicity. The main reported drug–food interaction of paracetamol, however, is with alcohol consumption that has been also linked to hepatotoxicity and CYP450 (Wolf et al. 2007; Prescott 2000).
Indeed, two scientific articles were found in the literature reporting the impact of ingesting GFJ with paracetamol. The first study was conducted by Samojlik and his colleagues in 1999 while investigating the analgesic effect of paracetamol on acetic acid-induced Writhing behavior in mice following single and multiple GFJ ingestion (Samojlik et al. 1999). Paracetamol was found to be active in reducing the irritant effect of acetic acid but only following chronic administration of GFJ. Unfortunately, this study was not supported by any pharmacokinetic data. The second study was presented, as a short communication, by Dasgupta et al. in 2008. The investigators confirmed a positive interaction between paracetamol and white GFJ in mice (n = 3) and illustrated that paracetamol serum levels were increased (Dasgupta et al. 2008). Unfortunately, the authors were only capable of calculating the half-life of paracetamol that did not differ between the GFJ treated and non-treated mice. Furthermore, by using only two sampling interval points at 1 and 2 h post-paracetamol administration, it was difficult to extract any other pharmacokinetic parameter of paracetamol from their presented preliminary data. Nonetheless, such previously reported positive interaction between paracetamol and GFJ in mice (Dasgupta et al. 2008; Samojlik et al. 1999) might suggest future comparative studies between mice and rats on such an interaction. Although similarity of drug metabolism between rodents and human do exist, it is currently a fact that rats are more resistant to paracetamol’s liver toxicity than mice (McGill et al. 2012). Therefore, extrapolation of results from rodents to humans has always been advised to be done with caution (Martignoni et al. 2006).
In this study, the decrease in paracetamol bioavailability seems not to be related to change in gastric emptying time since GFJ ingestion had been previously reported increasing blood concentrations of many drugs presumably by slowing down gastric emptying (Lilja et al. 1998; Odou et al. 2005). Furthermore, GFJ is acidic in nature and is unlikely to affect the absorption of the acidic paracetamol (pKa 9.5 at 25 °C) (Prescott 1980). Since the pre-hepatic metabolism of paracetamol is known to be minimal, mechanisms other than modulating intestinal CYP450 by GFJ might be involved in reducing paracetamol bioavailability. It was found that organic anion-transporting polypeptide (OATP) is expressed in both human liver and intestinal epithelial cells (Grandvuinet et al. 2012; Shitara et al. 2013). The reduction of bioavailability of some drugs was attributed to the decreased intestinal uptake by inhibiting this transporter protein following GFJ consumption. For example, Dresser and his colleagues expressed that reduced bioavailability of fexofenadine was possibly due to direct inhibition of intestinal uptake by intestinal OATP (Dresser et al. 2002, 2005). Later, the same group reported that naringin, a flavonoid present in GFJ, was a major selective inhibitor of OATP1A2 and decreased oral fexofenadine bioavailability clinically (Bailey et al. 2007). Recently, it was found that naringin and hesperidin are the major OATP2B1 inhibitors in GFJ and orange juice, respectively (Shirasaka et al. 2013a). In another study, however, Shirasaka and his colleagues also confirmed that apple juice and orange juice, to a lesser extent, induced a remarkable decrease in OATP2B1-mediated estrone-3-sulfate uptake in a concentration-dependent manner, whereas GFJ had no effect. The complexity of fruit juices interactions in vivo was accordingly concluded (Shirasaka et al. 2013b).
Although conflicting reports illustrated that GFJ can induce or inhibit both intestinal and hepatic P-gp efflux pumps, considerable evidence indicates that GFJ has minimal effect on P-gp that is dependable on the dose of GFJ (Hanley et al. 2011). Inline with our results, however, a previous study reported a reduction in diltiazem bioavailability in Wistar rats following repeated GFJ administrations and pointed out that a single dose exposure to GFJ showed no effect on P-gp, whereas multiple dose administration of GFJ resulted in increased levels of P-gp expression and decreased levels of OATP (Boddu et al. 2009).
5 Conclusions
Frequent administration of a large amount of white GFJ was confirmed to modulate the pharmacokinetics of paracetamol in Sprague–Dawley rats by reducing its bioavailability. The mechanism of such drug interaction is not defined so far. Due to the complexity and overlapping mechanisms of drug–GFJ interactions, correlation studies between in vivo and in vitro interactions of paracetamol with GFJ are warranted. Further investigations are also required to confirm and link the observed reduction of paracetamol bioavailability with its therapeutic effect. Meanwhile, it may be advisable not to ingest large amounts of GFJ along with paracetamol to avoid a possible potential loss of efficacy.
References
Bailey DG, Dresser GK, Leake BF, Kim RB (2007) Naringin is a major and selective clinical inhibitor of organic anion-transporting polypeptide 1A2 (OATP1A2) in grapefruit juice. Clin Pharmacol Ther 81:495–502
Bessems JG, Vermeulen NP (2001) Paracetamol (acetaminophen)-induced toxicity: molecular and biochemical mechanisms, analogues and protective approaches. Crit Rev Toxicol 31:55–138
Boddu SP, Yamsani MR, Potharaju S, Veeraraghavan S, Rajak S, Kuma SV, Avery BA, Repka MA, Varanasi VS (2009) Influence of grapefruit juice on the pharmacokinetics of diltiazem in Wistar rats upon single and multiple dosage regimens. Pharmazie 64:525–531
Botting RM (2000) Mechanism of action of acetaminophen: is there a cyclooxygenase 3? Clin Infect Dis 31(Suppl 5):S202–S210
Cuciureanu R, Cuciureanu, M, Vlase, L, Muntean, D (2008) Pharmacokinetic interaction between grapefruit juice and diclofenac. In: Proceedings of Congress of Federation of European Pharmacological Societies; Manchester, UK. http://www.pa2online.org/abstract/abstract.jsp?abid=28989. Accessed 20 Feb 2014
Dahan A, Amidon GL (2009) Grapefruit juice and its constituents augment colchicine intestinal absorption: potential hazardous interaction and the role of p-glycoprotein. Pharm Res 26:883–892
Dasgupta A, Reyes MA, Risin SA, Actor JK (2008) Interaction of white and pink grapefruit juice with acetaminophen (paracetamol) in vivo in mice. J Med Food 11:795–798
Deferme S, Augustijns P (2003) The effect of food components on the absorption of P-gp substrates: a review. J Pharm Pharmacol 55:153–162
Dresser GK, Bailey DG, Leake BF, Schwarz UI, Dawson PA, Freeman DJ, Kim RB (2002) Fruit juices inhibit organic anion transporting polypeptide-mediated drug uptake to decrease the oral availability of fexofenadine. Clin Pharmacol Ther 71:11–20
Dresser GK, Kim RB, Bailey DG (2005) Effect of grapefruit juice volume on the reduction of fexofenadine bioavailability: possible role of organic anion transporting polypeptides. Clin Pharmacol Ther 77:170–177
Garg SK, Kumar N, Bhargava VK, Prabhakar SK (1998) Effect of grapefruit juice on carbamazepine bioavailability in patients with epilepsy. Clin Pharmacol Ther 64:286–288
Grandvuinet AS, Vestergaard HT, Rapin N, Steffansen B (2012) Intestinal transporters for endogenic and pharmaceutical organic anions: the challenges of deriving in vitro kinetic parameters for the prediction of clinically relevant drug-drug interactions. J Pharm Pharmacol 64:1523–1548
Hanley MJ, Cancalon P, Widmer WW, Greenblatt DJ (2011) The effect of grapefruit juice on drug disposition. Expert Opin Drug Metab Toxicol 7:267–286
Kalantzi L, Reppas C, Dressman JB, Amidon GL, Junginger HE, Midha KK, Shah VP, Stavchansky SA, Barends DM (2006) Biowaiver monographs for immediate release solid oral dosage forms: acetaminophen (paracetamol). J Pharm Sci 95:4–14
Kim DW, Tan EY, Jin Y, Park S, Hayes M, Demirhan E, Schran H, Wang Y (2011) Effects of imatinib mesylate on the pharmacokinetics of paracetamol (acetaminophen) in Korean patients with chronic myelogenous leukaemia. Br J Clin Pharmacol 71:199–206
Laine JE, Auriola S, Pasanen M, Juvonen RO (2009) Acetaminophen bioactivation by human cytochrome P450 enzymes and animal microsomes. Xenobiotica 39:11–21
Lilja JJ, Kivisto KT, Backman JT, Lamberg TS, Neuvonen PJ (1998) Grapefruit juice substantially increases plasma concentrations of buspirone. Clin Pharmacol Ther 64:655–660
Mahgoub AA (2002) Grapefruit juice potentiates the anti-inflammatory effects of diclofenac on the carrageenan-induced rat’s paw oedema. Pharmacol Res 45:1–4
Maish WA, Hampton EM, Whitsett TL, Shepard JD, Lovallo WR (1996) Influence of grapefruit juice on caffeine pharmacokinetics and pharmacodynamics. Pharmacotherapy 16:1046–1052
Martignoni M, Groothuis GM, de Kanter R (2006) Species differences between mouse, rat, dog, monkey and human CYP-mediated drug metabolism, inhibition and induction. Expert Opin Drug Metab Toxicol 2:875–894
McGill MR, Williams CD, Xie Y, Ramachandran A, Jaeschke H (2012) Acetaminophen-induced liver injury in rats and mice: comparison of protein adducts, mitochondrial dysfunction, and oxidative stress in the mechanism of toxicity. Toxicol Appl Pharmacol 264:387–394
Odou P, Ferrari N, Barthelemy C, Brique S, Lhermitte M, Vincent A, Libersa C, Robert H (2005) Grapefruit juice-nifedipine interaction: possible involvement of several mechanisms. J Clin Pharm Ther 30:153–158
Paine MF, Criss AB, Watkins PB (2004) Two major grapefruit juice components differ in intestinal CYP3A4 inhibition kinetic and binding properties. Drug Metab Dispos 32:1146–1153
Prescott LF (1980) Kinetics and metabolism of paracetamol and phenacetin. Br J Clin Pharmacol 10(Suppl 2):291S–298S
Prescott LF (2000) Paracetamol, alcohol and the liver. Br J Clin Pharmacol 49:291–301
Qinna NA, Mallah EM, Arafat TA, Idkaidek NM (2012) Effect of licorice and grapefruit juice on paracetamol pharmacokinetics in human saliva. Int J Pharm Pharm Sci 4:158–162
Samojlik I, Raskovic A, Dakovic-Svajcer K, Mikov M, Jakovljevic V (1999) The effect of paracetamol on peritoneal reflex after single and multiple grapefruit ingestion. Exp Toxicol Pathol 51:418–420
Schwarz UI, Seemann D, Oertel R, Miehlke S, Kuhlisch E, Fromm MF, Kim RB, Bailey DG, Kirch W (2005) Grapefruit juice ingestion significantly reduces talinolol bioavailability. Clin Pharmacol Ther 77:291–301
Shirasaka Y, Shichiri M, Mori T, Nakanishi T, Tamai I (2013a) Major active components in grapefruit, orange, and apple juices responsible for OATP2B1-mediated drug interactions. J Pharm Sci 102:3418–3426
Shirasaka Y, Shichiri M, Murata Y, Mori T, Nakanishi T, Tamai I (2013b) Long-lasting inhibitory effect of apple and orange juices, but not grapefruit juice, on OATP2B1-mediated drug absorption. Drug Metab Dispos 41:615–621
Shitara Y, Maeda K, Ikejiri K, Yoshida K, Horie T, Sugiyama Y (2013) Clinical significance of organic anion transporting polypeptides (OATPs) in drug disposition: their roles in hepatic clearance and intestinal absorption. Biopharm Drug Dispos 34:45–78
Strauch K, Lutz U, Bittner N, Lutz WK (2009) Dose-response relationship for the pharmacokinetic interaction of grapefruit juice with dextromethorphan investigated by human urinary metabolite profiles. Food Chem Toxicol 47:1928–1935
Takanaga H, Ohnishi A, Murakami H, Matsuo H, Higuchi S, Urae A, Irie S, Furuie H, Matsukuma K, Kimura M, Kawano K, Orii Y, Tanaka T, Sawada Y (2000) Relationship between time after intake of grapefruit juice and the effect on pharmacokinetics and pharmacodynamics of nisoldipine in healthy subjects. Clin Pharmacol Ther 67:201–214
Toes MJ, Jones AL, Prescott L (2005) Drug interactions with paracetamol. Am J Ther 12:56–66
Uesawa Y, Abe M, Mohri K (2008) White and colored grapefruit juice produce similar pharmacokinetic interactions. Pharmazie 63:598–600
Wolf KK, Wood SG, Allard JL, Hunt JA, Gorman N, Walton-Strong BW, Szakacs JG, Duan SX, Hao Q, Court MH, von Moltke LL, Greenblatt DJ, Kostrubsky V, Jeffery EH, Wrighton SA, Gonzalez FJ, Sinclair PR, Sinclair JF (2007) Role of CYP3A and CYP2E1 in alcohol-mediated increases in acetaminophen hepatotoxicity: comparison of wild-type and Cyp2e1(−/−) mice. Drug Metab Dispos 35:1223–1231
Won CS, Oberlies NH, Paine MF (2010) Influence of dietary substances on intestinal drug metabolism and transport. Curr Drug Metab 11:778–792
Zhu Y, Zhang QY (2012) Role of intestinal cytochrome p450 enzymes in diclofenac-induced toxicity in the small intestine. J Pharmacol Exp Ther 343:362–370
Acknowledgments
This work was funded by the Deanship of Scientific Research, University of Petra, Amman, Jordan.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qinna, N.A., Ismail, O.A., Alhussainy, T.M. et al. Evidence of reduced oral bioavailability of paracetamol in rats following multiple ingestion of grapefruit juice. Eur J Drug Metab Pharmacokinet 41, 187–195 (2016). https://doi.org/10.1007/s13318-014-0251-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13318-014-0251-4