Abstract
Objectives
To study the association of fluid overload with mortality and morbidity in critically-ill mechanically ventilated children.
Design
Prospective observational study.
Setting
Pediatric Intensive Care Unit (PICU) of a tertiary care hospital, New Delhi, India.
Participants
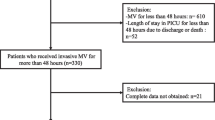
118 children (age 1 mo - 15 y) requiring mechanical ventilation.
Outcome measures
Primary: Association of fluid overload with mortality. Secondary: Association of fluid overload with oxygenation, organ dysfunction, duration of mechanical ventilation and PICU stay.
Results
Cumulative fluid overload of ≥15% was observed in 74 (62.7%) children. About 50% of these children reached cumulative fluid overload of ≥15% within the first 5 days of PICU stay. The mortality was 40.5% in those with ≥15% cumulative fluid compared to 34% in the rest [OR (95% CI): 1.02 (0.97, 1.07)]. On multivariate analysis, after adjusting for confounders, cumulative fluid overload ≥15% was associated with higher maximum PELOD (pediatric logistic organ dysfunction) score (Median: 21 vs. 12; P = 0.03), longer median duration of mechanical ventilation (10 vs. 4 d; P <0.0001) and PICU stay (13.5 vs. 6 d; P <0.0001). There was no significant association of fluid overload with oxygenation index (P=0.32).
Conclusion
There is no association of fluid overload with mortality. However, it is associated with poor organ function, longer duration of mechanical ventilation and PICU stay in critically-ill, mechanically ventilated children.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Duke T, Molyneux EM. Intravenous fluids for seriously ill children: Time to reconsider. Lancet. 2003;362:1320–3.
Schrier RW, Berl T, Anderson RJ. Osmotic and nonosmotic control of vasopressin release. Am J Physiol. 1979;236:F32132.
Schrier RW, Goldberg JP. The physiology of vasopressin release and the pathogenesis of impaired water excretion in adrenal, thyroid, and edematous disorders. Yale J Biol Med. 1980;53:525–41.
Briassoulis G, Venkataraman S, Thompson AE. Energy expenditure in critically ill children. Crit Care Med. 2000;28:1166–72.
Wiedemann HP. A perspective on the fluids and catheters treatment trial (FACTT). Fluid restriction is superior in acute lung injury and ARDS. Cleve Clin J Med. 2008;75:42–8.
Valentine SL, Sapru A, Higgerson RA, Spinella PC, Flori HR, Graham DA, et al. Fluid balance in critically ill children with acute lung injury. Crit Care Med. 2012;40:2883–9.
Leteurtre S, Duhamel A, Grandbastien B, Lacroix J, Leclerc F. Paediatric logistic organ dysfunction (PELOD) score. Lancet. 2006;367:897.
Holliday MA, Segar WE. The maintenance need for water in parenteral fluid therapy. Pediatrics. 1957;19:823–32.
Slater A, Shann F, Pearson G, Paediatric index of mortality (PIM) study group. PIM2: A revised version of the paediatric index of mortality. Intensive Care Med. 2003;29:278–85.
Flori HR, Church G, Liu KD, Gildengorin G, Matthay MA. Positive fluid balance is associated with higher mortality and prolonged mechanical ventilation in pediatric patients with acute lung injury. Crit Care Res Pract. 2011;2011:854142.
Michael M, Kuehnle I, Goldstein SL. Fluid overload and acute renal failure in pediatric stem cell transplant patients. Pediatr Nephrol. 2003;19:91–5.
Kennedy CE, Akcan Arikan A. Fluid overload and kidney injury score (FOKIS). Pediatr Crit Care Med. 2014;15:132.
Gillespie RS, Seidel K, Symons JM. Effect of fluid overload and dose of replacement fluid on survival in hemofiltration. Pediatr Nephrol Berl Ger. 2004;19:1394–9.
Sutherland SM, Zappitelli M, Alexander SR, Chua AN, Brophy PD, Bunchman TE, et al. Fluid overload and mortality in children receiving continuous renal replacement therapy: The prospective pediatric continuous renal replacement therapy registry. Am J Kidney Dis. 2010;55:316–25.
Foland JA, Fortenberry JD, Warshaw BL, Pettignano R, Merritt RK, Heard ML, et al. Fluid overload before continuous hemofiltration and survival in critically ill children: A retrospective analysis: Crit Care Med. 2004;32:1771–6.
Sinitsky L, Walls D, Nadel S, Inwald DP. Fluid overload at 48 hours is associated with respiratory morbidity but not mortality in a general PICU: Retrospective cohort study. Pediatr Crit Care Med. 2015;16:205–9.
Arikan AA, Zappitelli M, Goldstein SL, Naipaul A, Jefferson LS, Loftis LL. Fluid overload is associated with impaired oxygenation and morbidity in critically ill children. Pediatr Crit Care Med. 2012;13:253–8.
Maitland K, Kiguli S, Opoka RO, Engoru C, Olupot-Olupot P, Akech SO, et al. Mortality after fluid bolus in African children with severe infection. N Engl J Med. 2011;364:2483–95.
Benakatti G, Singhi S, Jayshree M, Bansal A. Conventional vs. restrictive maintenence fluid regimen in children with septic shock after initial resusitation. Pediatr Crit Care Med. 2014;15:30.
Sakka SG, Klein M, Reinhart K, Meier-Hellmann A. Prognostic value of extravascular lung water in critically ill patients. Chest. 2002;122:2080–6.
Malbrain MLNG, Marik PE, Witters I, Cordemans C, Kirkpatrick AW, Roberts DJ, et al. Fluid overload, deresuscitation, and outcomes in critically ill or injured patients: A systematic review with suggestions for clinical practice. Anestezjol Intensywna Ter. 2014;46:361–80.
Schuller D, Mitchell JP, Calandrino FS, Schuster DP. Fluid balance during pulmonary edema. Is fluid gain a marker or a cause of poor outcome? Chest. 1991;100:1068–75.
Kuzkov VV, Kirov MY, Sovershaev MA, Kuklin VN, Suborov EV, Waerhaug K, et al. Extravascular lung water determined with single transpulmonary thermodilution correlates with the severity of sepsis-induced acute lung injury. Crit Care Med. 2006;34:1647–53.
Morris C, Plumb J. Mobilising oedema in the oedematous critically ill patient with ARDS: Do we seek natriuresis not diuresis? J Intensive Care Soc. 2011;12:92–7.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Samaddar, S., Sankar, J., Kabra, S.K. et al. Association of Fluid Overload with Mortality in Critically-ill Mechanically Ventilated Children. Indian Pediatr 55, 957–961 (2018). https://doi.org/10.1007/s13312-018-1417-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-018-1417-y