Abstract
Introduction
We previously reported several factors that cross-sectionally correlate with treatment satisfaction in Japanese patients with type 2 diabetes visiting diabetes clinics. The aim of this study is to identify factors associated with longitudinal changes in treatment satisfaction in patients with type 2 diabetes.
Methods
The study included 649 patients with type 2 diabetes treated with oral glucose-lowering agents who completed the first questionnaire in 2016. The collected data included scores from the Diabetes Treatment Satisfaction Questionnaire (DTSQ) and other parameters regarding diabetes treatment. We analyzed 1-year longitudinal changes in DTSQ scores and investigated factors associated with these changes.
Results
Univariate linear regression analyses showed that changes in body weight, adherence to diet therapy, adherence to exercise therapy, cost burden, motivation for treatment, regularity of mealtimes, and perceived hypoglycemia correlated with changes in DTSQ scores. On the basis of multiple linear regression analyses, a decrease in hypoglycemia (β ± SE = − 0.394 ± 0.134, p = 0.0034), cost burden (β ± SE = − 0.934 ± 0.389, p = 0.017), and an increase in treatment motivation (β ± SE = 1.621 ± 0.606, p = 0.0077) correlated with DTSQ score increases, suggesting that motivation for treatment had the strongest impact on score increases. Subgroup analyses revealed that an increase in motivation for treatment most significantly correlated with a DTSQ score increase in obese and poor glycemic control groups, regardless of age.
Conclusion
This is the first longitudinal study clarifying that an increase in motivation for treatment most strongly correlates with an increase in DTSQ score in patients with type 2 diabetes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Most previous studies about treatment satisfaction in patients with diabetes have been cross-sectional, and sufficient longitudinal studies have not been carried out. |
In this manuscript, we investigated factors associated with 1-year longitudinal changes in treatment satisfaction. |
This study showed that a decrease in hypoglycemia and cost burden and an increase in motivation for treatment correlate significantly with an increase in the Diabetes Treatment Satisfaction Questionnaire (DTSQ) score, and increased motivation for treatment had the strongest impact on increased treatment satisfaction especially in the obese group and poor glycemic control group, regardless of age. |
This is the first study assessing associations between longitudinal changes in DTSQ score and changes in each related factor for a large number of patients. |
Introduction
Patients with diabetes need to practice daily self-management, such as dietary control, exercise, and medication use. However, most patients feel burdened with this self-management, and their quality of life is likely to deteriorate [1]. One of the goals of diabetes treatment is to maintain the quality of life of patients at the same level as that of healthy people. Therefore, it is important to evaluate not only clinical outcomes but also patient-reported outcomes. Treatment satisfaction has often been used as an indicator of the quality of medical care for patients with diabetes [2].
Several studies have researched the factors associated with treatment satisfaction in patients with type 2 diabetes mellitus. High levels of glycosylated hemoglobin (HbA1c) [3] and diabetes complications [3, 4] reportedly correlate with lower treatment satisfaction. Our previous study using the Diabetes Treatment Satisfaction Questionnaire (DTSQ) and the study-specific questionnaire revealed that body mass index (BMI), adherence to diet therapy and medication use, motivation for treatment, and use of sodium-glucose cotransporter 2 inhibitor (SGLT2i) were positively associated with treatment satisfaction and that HbA1c, irregular diet schedule, cost burden, and perceived hypoglycemia were negatively associated with treatment satisfaction in patients with type 2 diabetes visiting diabetes clinics [5].
Most previous studies about treatment satisfaction in patients with diabetes have been cross-sectional, and sufficient longitudinal studies have not been carried out. Therefore, it is not fully elucidated which factors should be focused on in diabetes treatment to increase treatment satisfaction. In addition, it remains unclear whether factors associated with a change in treatment satisfaction differ according to various clinical backgrounds, among elderly or nonelderly, obese or nonobese, and under good or poor glycemic control groups. The aim of this study is to identify diabetes treatment factors which correlate with a 1-year longitudinal change in DTSQ score in patients with type 2 diabetes.
Methods
Subjects
We enrolled patients with type 2 diabetes, who attended the outpatient clinics of four diabetes clinics located in the urban districts of the western area of Japan (Hayashi Clinic, Watanabe Clinic, Nakata Clinic, and Ryoya Komatsu Clinic).
Inclusion criteria: (1) Patients who had been treated with one or more oral glucose-lowering agents (OGLAs), and also had completed the first questionnaire from April to September 2016. (2) Patients who completed the second questionnaire from July 2017 to March 2018.
Exclusion criteria: (1) Patients who we could not follow up. (2) Patients whose second questionnaire lacked some data; as DTSQ total scores could not be calculated.
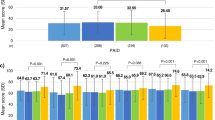
The number of patients who met inclusion criterion (1) was 754 (5); the number of those who met the inclusion criteria (1) and (2) was 680. Seventy-four patients were missing because we could not follow up with the entire sample. Furthermore, the number of patients who met exclusion criterion (2) was 31. Consequently, a total of 649 patients (277 at Watanabe Clinic, 150 at Nakata Clinic, 119 at Hayashi Clinic, and 103 at Ryoya Komatsu Clinic) participated in this study (Fig. 1). This study was approved by the Institutional Ethics Review Board of Osaka University Hospital and was carried out in accordance with the principles of the Declaration of Helsinki, and a signed consent form was obtained from each subject.
Questionnaires and Methods
We implemented the DTSQ [6], specifically the Japanese version [7], and a study-specific patient questionnaire designed to explore treatment adherence, diabetes complications, cost burden, social support, and lifestyle, including mealtime or work time irregularities (see Table S1 in the electronic supplementary material for details), which was used in our previous study [15]. Data on age, sex, BMI, HbA1c, duration of diabetes, and visit interval were collected from physician forms (see Table S2 in the electronic supplementary material for details). Information on adherence to diet therapy, exercise therapy, medication use, diabetes complications, cost burden, family support, and lifestyle was collected from the study-specific patient questionnaire (Table S1), which was also included in the same aforementioned study. The DTSQ is composed of eight items related to the current treatment of diabetes: (1) overall satisfaction, (2) perceived hyperglycemia, (3) perceived hypoglycemia, (4) convenience, (5) flexibility, (6) understanding of diabetes, (7) willingness to recommend current treatment to others, and (8) willingness to continue the current treatment. Each item is rated on a 7-point Likert scale, with a score ranging from 0 (very dissatisfied or never) to 6 (very satisfied or most of the time). All scores except items 2 and 3 were added to determine the DTSQ total score (range 0–36), representing the self-reported treatment satisfaction level of the patient. The average DTSQ score at the time of the previous study was 27.3, which suggested that the patients were considered to be a group with relatively high satisfaction level compared to the previously reported insulin-treated type 2 diabetes group [8]. The study-specific questionnaire answered by the patients consisted of items related to treatment adherence (questions 1–3), diabetes complications (questions 4–8), motivation for treatment (question 9), cost burden (question 10), social support (question 11), and lifestyle (questions 12–13); these were the same as the questions used previously. The physician-completed form was composed of clinical data on age, sex, anthropometric measurements, HbA1c, use of OGLAs, and the interval between visits. In addition, medical records were examined to determine whether the patients received nutrition education from nutritionists during the longitudinal period.
The study methods were the same as those described in our previous paper [5]. Briefly, each patient who completed the study-specific questionnaire and the Japanese version of the DTSQ was informed that the answers to the two questionnaires would not be viewed by the attending doctor. The doctor completed the physician form for the same patient and sent it to the Department of Diabetes Care Medicine, Graduate School of Medicine, Osaka University.
Statistical Analysis
Continuous data are presented as the mean ± standard deviation; categorical data are expressed as frequencies and percentages. The reported HbA1c value was based on the National Glycohemoglobin Standardization Program (NGSP). Associations between a change in DTSQ total score and various parameters were analyzed using multiple linear regression analysis. Subgroup analyses of associations were performed according to three clinical backgrounds: an elderly (≥ 65 years) or nonelderly (< 65 years) group, an obese (≥ 25 kg/m2) or non-obese (< 25 kg/m2) group, and a good (< 7%) or poor (≥ 7%) glycemic control group. Statistical analyses were performed using the statistical software EZR (Easy R) (R × 64 3.2.2) [9]. The significance level was set at p < 0.05.
Results
Characteristics of Study Participants
The characteristics of the study participants are listed in Table 1. The mean age of the subjects was 66, and the mean HbA1c was 6.9% (52 mmol/mol) at 1 year after starting the study. Regarding diabetic complications, the prevalence of each complication recognized by the patients was less than 10%. Almost all patients adhered to diabetic medication use (very good or good); however, only approximately two-thirds of the patients adhered to diet therapy, and only half adhered to exercise therapy. Most of the patients reported that their motivation for diabetes treatment was high, whereas the remaining 13% of the patients answered that it was medium or low. For lifestyle, 12% and 23% of the patients reported irregularity of mealtimes and working time, respectively. Most of the patients visited outpatient clinics once every 1 or 2 months. Regarding the cost burden for diabetes treatment, more than half of the patients reported that they felt economically burdened (high or medium). The use of OGLAs and other prescriptions are summarized in detail, as reported in the physician form, in Table 1. Dipeptidyl peptidase 4 inhibitors (DPP4is) were used by 68% of the patients, biguanide by 61%, and sodium-glucose cotransporter 2 inhibitors by 17%. The dosages of OGLAs are also listed.
Correlations of Change in DTSQ Total Score with Changes in Various Factors
The mean DTSQ total score was 27.7, with a change from the first administration of the questionnaire of 0.25 (Table 2). Univariate linear regression analysis to evaluate correlations of changes in DTSQ total scores with changes in various factors, as adjusted for the previous value of each factor and the previous DTSQ total scores, is shown in Table 3. Among the parameters, changes in body weight, adherence to diet therapy, adherence to exercise therapy, cost burden, motivation for treatment, regularity of mealtimes, and perceived hypoglycemia significantly correlated with changes in DTSQ total score. Conversely, initiation or cessation of each OGLA was not associated with a change in DTSQ total score.
Table 4 provides the results of multiple linear regression analyses, revealing correlations for a change in DTSQ total score and changes in various factors with significant associations with a change in DTSQ total score, which are shown in Table 3. Each factor was analyzed in three models: model 1—adjusted for the general factors such as age, sex, and the previous value of each factor and the previous DTSQ total scores, as we investigated the relationship between the changes of them; model 2—adjusted for the change in HbA1c, which was clinically supposed to have a relation with treatment satisfaction, in addition to the factors used in model 1; and model 3—adjusted for all other factors with significant associations with a change in DTSQ total score, which are shown in Table 3, in addition to the factors used in model 2. In overall analyses, the decrease in cost burden and perceived hypoglycemia and motivation for treatment correlated with an increase in DTSQ total score. Furthermore, adherence to diet therapy and regularity of mealtime tended to be related to an increase in DTSQ total score. According to the values of the standard partial regression coefficient, the increase in motivation for treatment (model 1, 2.327 ± 0.587; model 2, 2.343 ± 0.590; model 3, 1.621 ± 0.606) had the strongest impact on enhanced treatment satisfaction compared to the decrease in cost burden (model 1, − 1.310 ± 0.392; model 2, − 1.328 ± 0.395; model 3, − 0.934 ± 0.389) and the decrease in perceived hypoglycemia (model 1, − 0.427 ± 0.132; model 2, − 0.451 ± 0.134; model 3, − 0.394 ± 0.134). We also investigated the relationships between the change of treatment satisfaction and the duration of diabetes, the number of other drugs, and the presence or absence of malignancy and depression, all of which may be related to treatment satisfaction. However, we found no significant association.
Additionally, we evaluated the possible association of nutrition education during the longitudinal period with an increase in adherence to diet therapy or treatment satisfaction. The number of patients who received nutrition education from nutritionists one or more times was 179 at Watanabe Clinic, 33 at Nakata Clinic, 71 at Hayashi Clinic, and 74 at Ryoya Komatsu Clinic. Overall, receiving nutrition education had no association with an increase in adherence to diet therapy or increase in treatment satisfaction. Moreover, both DTSQ total scores and their longitudinal changes were not significantly different between groups that did or did not receive nutrition education.
Subgroups Analyses
Subgroup analyses were also performed according to three clinical backgrounds. In the elderly group, an increase in adherence to diet therapy and motivation for treatment correlated with an increase in DTSQ score, whereas an increase in HbA1c level or number of OGLAs correlated with a decrease in DTSQ score. In the nonelderly group, increased motivation for treatment correlated with increased DTSQ scores, but increased hypoglycemia correlated with decreased DTSQ scores (Table S3). In the obese group, increasing adherence to diet therapy or motivation for treatment correlated with increasing DTSQ score; in the nonobese group, an increase in cost burden and the use of sulfonylurea (SU) correlated with a decrease in DTSQ score (Table S3). In the poor glycemic control group, increased motivation for treatment correlated with increased DTSQ scores, and increased HbA1c, number of OGLAs, and hypoglycemia correlated with decreased DTSQ scores. In contrast, no factors were found to be associated with a change in DTSQ score in the good glycemic control group (Table S3). On the basis of the value of the standard partial regression coefficient, increased motivation for treatment had the strongest impact on the increase in treatment satisfaction in the obese and poor glycemic control groups, regardless of age.
Discussion
This study showed that a decrease in hypoglycemia and cost burden and an increase in motivation for treatment correlate significantly with a 1-year longitudinal increase in DTSQ score. In addition, increasing motivation for treatment had the strongest impact on increased treatment satisfaction, especially in the obese group and poor glycemic control group, regardless of age. This is the first study assessing associations between longitudinal changes in DTSQ scores and changes in each related factor for a large number of patients.
Motivation for treatment is associated with self-efficacy in patients with diabetes [10]. Self-efficacy reflects individuals’ belief in their capability to perform specific behaviors necessary to achieve their goals [11], and experience of successful actions is believed to be the most powerful way to increase self-efficacy [10]. Self-efficacy-focused education in these patients greatly improves dietary self-management behaviors and quality of life [12]. Hence, it is assumed that an increase in motivation for treatment might lead to an increase in treatment satisfaction, partly through an increase in self-efficacy. In addition, low self-efficacy is associated with poor glycemic control in patients with diabetes [13, 14] and with high BMI [15]. These are possible reasons why impacts of treatment motivation on DTSQ scores were observed, especially in those with obesity and poor glycemic control, perhaps through improvement in low self-efficacy. We think that the enhanced self-management of diabetes is associated with improved glycemic control and that clinicians can use standardized questionnaires to improve patients’ knowledge and self-efficacy regarding nutrition, physical activity, glucose self-monitoring, and the use of healthcare technology [16].
This study showed that a decrease in hypoglycemia might lead to an increase in treatment satisfaction, especially in nonelderly patients and those with poor glycemic control. These findings are in line with previous cross-sectional studies showing that hypoglycemia is negatively associated with treatment satisfaction [1, 17, 18]. Indeed, it has been reported that patients with diabetes without hypoglycemic episodes have a lower burden for medical treatment than patients with hypoglycemic episodes [19]. Additionally, several studies have shown that concern about hypoglycemia is associated with worse quality of life (QoL) [20]. Regarding the fact that hypoglycemia unexpectedly correlated with a change in satisfaction in nonelderly patients, it is possible that subjective symptoms of hypoglycemia are more likely to occur in that group than in elderly patients [21], which might lead to a significant effect on treatment satisfaction.
With respect to cost burden, patients with diabetes and more healthcare-related financial difficulties have a greater treatment burden [22], and economic status is a significant variable in predicting QoL of patients with chronic diseases, including diabetes [23]. Another report found that the use of a fixed combination of vildagliptin/metformin was associated with improved QoL, as measured by the DTSQ questionnaire, and was accompanied by a reduction in healthcare costs [24]. It is assumed that medical cost burden correlates with the QoL or treatment satisfaction of patients with diabetes, and subgroup analyses showed that an increase in cost burden correlated with a decrease in DTSQ score in nonobese patients. The reason why this correlation was observed only in nonobese patients is unclear. The average age of nonobese patients was 68.2, higher than the 62.7 years of obese patients, whereas cost burden was not a significant factor for the change in DTSQ score both in elderly and nonelderly patients. In addition, there were no significant differences between nonobese patients and obese patients in other clinical backgrounds. Some novel antidiabetic agents are much more expensive than many other antidiabetic agents, which might make a somewhat complicated association between cost burden and treatment satisfaction. The cost of novel antidiabetic therapies for patients with type 2 diabetes may be still a barrier for their wider use [25].
In this study, receiving nutrition education exhibited no relationship with an increase in adherence to diet therapy or in treatment satisfaction. It is highly possible that some of the patients who received nutrition education during the longitudinal period had already received it continuously at these urban diabetes clinics before the first questionnaire; therefore, the effect of nutrition education during this period on treatment satisfaction might be obscured. Nevertheless, in the group responding on the first questionnaire that their adherence to diet therapy was poor, receiving nutrition education tended to be related to an increase in adherence to diet therapy (the increase in adherence to diet therapy was 1.07 or 0.69 in those with or without nutrition education, respectively, p = 0.088). According to this result, there is a possibility that nutrition education focusing on patients with poor adherence to diet therapy might efficiently lead to an increase in adherence, resulting in enhanced treatment satisfaction in these patients.
It is assumed that a change in HbA1c would be associated with a change in treatment satisfaction [1, 4], which was not shown when analyzing the total patient group in this study. The reason for this might be that their glycemic control was relatively good and that the longitudinal change in HbA1c was very small, namely 7.0% (53 mmol/mol) for the first questionnaire and 6.9% (52 mmol/mol) for the second questionnaire. However, subgroup analyses showed that a decrease in HbA1c in the elderly group and poor glycemic control group correlated with an increase in DTSQ score. Overall, the elderly and poor glycemic control groups had higher complication rates than the nonelderly and good glycemic control groups, respectively (average rates of complications including nephropathy, retinopathy, neuropathy, cardiovascular diseases, and diabetic foot were 7.2% in the elderly group vs 4.8% in the nonelderly group, 6.6% in the poor glycemic control group vs 5.8% in the good glycemic control group). In general, patients in the elderly or poor glycemic control group might have anxiety about the progression of complications and be more sensitive to HbA1c levels.
Subgroup analyses revealed other interesting results, whereby the use of SU in nonobese patients was negatively associated with an increase in satisfaction score. Although there was no relationship between the use of SU and perceived hypoglycemia in this study, it is possible that a decrease in SU dose or cessation of the use of SU leads to reduced concerns about hypoglycemia, resulting in an increase in treatment satisfaction.
The decrease in the number of OGLA tablets was significantly associated with increased DTSQ scores in the elderly group. It has been reported that elderly people with diabetes take more drugs than elderly people without diabetes [26], and elderly patients took more drugs than nonelderly patients also in this study (7.6 vs 6.4). If the total number of oral medications is large, elderly people are likely to feel a burden, such as taking time to take the medication; therefore, it is important to reduce the number of medications when treating elderly patients with diabetes [27].
We think that the findings from this study may have a greater importance during the current COVID-19 pandemic since proper management of diabetes must be a priority to reduce the burden of cardiometabolic complications and related mortality [28]. The experience we are collectively having during the pandemic should guide our future management of patients with diabetes in clinical practice.
This study has some limitations. We cannot discuss causal relationships, because this study is an observational study just examining the associations of the changes in each factor. We think that prospective interventional studies, which investigate whether increasing treatment motivation leads to an increase in treatment satisfaction, are needed in the future. It cannot be ruled out that the increase in treatment satisfaction resulted in the change in significant factors in an opposite manner. The patients enrolled in this study visited urban diabetes clinics, and glycemic control was relatively good. These patients might be expected to be well educated about diabetes. Therefore, the results of this study might not be applicable to patients with less education and poorer glycemic control. Though the average duration of diabetes was about 12 years, the glycemic control was relatively well maintained, and complication rates were relatively low. In addition, the enrolled patients used mainly OGLAs, so a significant change in treatment satisfaction could not be expected within 1 year. Finally, many factors evaluated by questionnaires are subjective, and there are missing data, so not all might be accurate. Nevertheless, we believe that it is important to improve not only clinical outcomes but also patient-reported outcomes, which may result in an improvement of the quality of life.
Conclusions
We found that a decrease in hypoglycemia and cost burden and an increase in motivation for treatment were significantly associated with an increase in satisfaction scores in this longitudinal study. Increased motivation for treatment had the strongest impact on increased treatment satisfaction, especially in the obese group and poor glycemic control group, regardless of age. This study also showed that factors associated with increased treatment satisfaction differ according to clinical background.
References
Saito I, Inami F, Ikebe T, et al. Impact of diabetes on health-related quality of life in a population study in Japan. Diabetes Res Clin Pract. 2006;73:51–7.
Redekop WK, Koopmanschap MA, Stolk RP, et al. Health-related quality of life and treatment satisfaction in Dutch patients with type 2 diabetes. Diabetes Care. 2002;25:458–63.
Boels AM, Vos RC, Hermans TGT, et al. What determines treatment satisfaction of patients with type 2 diabetes on insulin therapy? An observational study in eight European countries. BMJ Open. 2017;7:e016180.
Ozder A, Sekeroglu M, Eker HH, et al. Quality of life and satisfaction with treatment in subjects with type 2 diabetes: results from primary health care in Turkey. Int J Clin Exp Med. 2014;7:5715–22.
Hayashi I, Watanabe N, Nakata S, et al. Factors associated with treatment satisfaction in patients with type 2 diabetes mellitus using oral glucose-lowering agents: a cross-sectional study in urban districts in Japan. Endocr J. 2018;65:1001–9.
Bradley C. The Diabetes Treatment Satisfaction Questionnaire: DTSQ. In: Bradley C, editor. Handbook of Psychology and Diabetes: a guide to psychological measurement in diabetes research and practice. Chur: Harwood; 1994. p. 111–32.
Ishii H, Bradley C, Riazi A, et al. The Japanese version of the Diabetes Treatment Satisfaction Questionnaire (DTSQ): translation and clinical evaluation. J Clin Exp Med. 2000;192:809–14.
Ishii H, Nakajima H, Kamei N, et al. Comparison of patient-led and physician-led insulin titration in Japanese type 2 diabetes mellitus patients based on treatment distress, satisfaction, and self-efficacy: the COMMIT-patient study. Diabetes Ther. 2021;12(2):595–611.
Kanda Y. Investigation of the freely available easyto-use software ‘EZR’ for medical statistics. Bone Marrow Transplant. 2013;48:452–8.
Lakerveld J, Palmeria AL, van Duinkerken E, et al. Motivation: key to a healthy lifestyle in people with diabetes? Current and emerging knowledge and applications. Diabetic Med. 2020;37:464–72.
Jingjing Y, Haipeng W, Xiao Y, et al. The association between self-efficacy and self-management behaviors among Chinese patients with type 2 diabetes. PLoS ONE. 2019;14(11):e0224869.
Jiang X, Wang J, Lu Y, et al. Self-efficacy-focused education in persons with diabetes: a systematic review and meta-analysis. Psychol Res Behav Manag. 2019;12:67–79.
D’Souza MS, Karkada SN, Parahoo K, et al. Self-efficacy and self-care behaviours among adults with type 2 diabetes. Appl Nurs Res. 2017;36:25–32.
Cheng LJ, Wang W, Lim ST, et al. Factors associated with glycaemic control in patients with diabetes mellitus: a systematic literature review. J Clin Nurs. 2019;28:1433–50.
Ovaskainen ML, Tapanainen H, Laatikainen T, et al. Perceived health-related self-efficacy associated with BMI in adults in a population-based survey. Scand J Public Health. 2015;43:197–203.
Popoviciu MS, Marin VN, Vesa CM, et al. Correlations between diabetes mellitus self-care activities and glycaemic control in the adult population: a cross-sectional study. Healthcare. 2022;10:174.
Clare B, Eveline E, Pedro de Pablos-Velasco, et al. Predictors of quality of life and other patient-reported outcomes in the PANORAMA multinational study of people with type 2 diabetes. Diabetes Care. 2018;41:267–76.
Gordon J, Beresford-Hulme L, Bennett H, et al. Relationship between hypoglycaemia, body mass index and quality of life among patients with type 1 diabetes: observations from the DEPICT clinical trial programme. Diabetes Obes Metab. 2020;22:857–65.
Ishii H, Shin K, Tosaki T, et al. Correction to: Reproducibility and validity of a questionnaire measuring treatment burden on patients with type 2 diabetes: diabetic treatment burden questionnaire (DTBQ). Diabetes Ther. 2018;9:1719.
Sakane N, Kotani K, Tsuzaki K, et al. Fear of hypoglycemia and its determinants in insulin-treated patients with type 2 diabetes mellitus. J Diabetes Investig. 2015;6:567–70.
Bremer JP, Jauch-Chara K, Hallschmid M, et al. Hypoglycemia unawareness in older compared with middle-aged patients with type 2 diabetes. Diabetes Care. 2009;32:1513–7.
Rogers EA, Yost KJ, Rosedahl JK, et al. Validating the patient experience with treatment and self-management (PETS), a patient-reported measure of treatment burden, in people with diabetes. Patient Relat Outcome Meas. 2017;8:143–56.
Samiei Siboni F, Alimoradi Z, Atashi V, et al. Quality of life in different chronic diseases and its related factors. Int J Prev Med. 2019;10:65.
Genovese S, Tedeschi D. Effects of vildagliptin/metformin therapy on patient-reported outcomes: work productivity, patient satisfaction, and resource utilization. Adv Ther. 2013;30:152–64.
Cardio-Metabolic Academy Europe East, Banach M, Gaita D, et al. Adoption of the ADA/EASD guidelines in 10 Eastern and Southern European countries: physician survey and good clinical practice recommendations from an international expert panel. Diabetes Res Clin Pract. 2021;172:108535.
Strehblow C, Smeikal M, Fasching P, et al. Polypharmacy and excessive polypharmacy in octogenarians and older acutely hospitalized patients. Wien Klin Wochenschr. 2014;126:195–200.
Abdelhafiz AH, Sinclair AJ. Deintensification of hypoglycaemic medications-use of a systematic review approach to highlight safety concerns in older people with type 2 diabetes. J Diabetes Compl. 2018;32:444–50.
Stoian AP, Banerjee Y, Rizvi AA, et al. Diabetes and the COVID-19 pandemic: how insights from recent experience might guide future management. Metab Syndr Relat Disord. 2020;18:173–5.
Acknowledgements
We thank Prof. Ishii for allowing us to use the Japanese version of the DTSQ. We would like to acknowledge Prof. Clare Bradley and Health Psychology Research Limited as the owners of the DTSQ questionnaire, and to thank them for permitting its use in this study.
Funding
This work was supported in part by JSPS KAKENHI (Grant No. 16K09237), the journal’s Rapid Service Fee was funded by the authors.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship of this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Authorship Contributions
S.M. collected the data and wrote the manuscript. N.W., S.N., I.H. and R.K. recruited all the patients and contributed to the discussion. Y.F., S.F., C.I., M.Y.B., T.K., A.T. and M.T. contributed to the discussion. H.I. conceived the study design and contributed to the discussion. J.K. and I.S. contributed to the discussion and reviewed/edited the manuscript. J.K. is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Disclosure
Mitsuyoshi Takahara, Hiromi Iwahashi and Junji Kozawa are staff members of the endowed chair (Department of Diabetes Care Medicine) established by funds from Mitsubishi Tanabe Pharma Co.; AstraZeneca; Nippon Boehringer Ingelheim Co.; Taisho Pharmaceutical Co.; Ono Pharmaceutical Co.; MSD; Novo Nordisk Pharma Ltd., and Keiseikai Hospital. Yukari Fujita is a member of the endowed chair (Department of Community Medicine) established by funds from Rinku General Medical Center. Iichiro Shimomura has received lecture fees from MSD; Ono Pharmaceutical Co.; Kowa Pharmaceutical Co. Ltd.; Sanofi; Sanwa Kagaku Kenkyusho Co.; Takeda Pharmaceutical Co.; Eli Lilly Japan and Novo Nordisk Pharma Ltd. and has received research funds from Astellas Pharma, Inc.; MSD; Ono Pharmaceutical Co.; Kyowa Kirin Co.; Kowa Company, Ltd.; Sanofi; Daiichi Sankyo Co.; Takeda Pharmaceutical Co.; Mitsubishi Tanabe Pharma Co.; Teijin Pharma Ltd.; Nippon Boehringer Ingelheim Co., Ltd; Novartis Pharmaceuticals Corp.; Novo Nordisk Pharma Ltd.; Taisho Pharmaceutical Co.; Sumitomo Dainippon Pharma Co.; Takeda Pharmaceutical Co.; Mitsubishi Tanabe Pharma Co.; Midori Health Care Center; Uehara Memorial Foundation; MSD Life Science Foundation; Soiken, Inc.; Japan Foundation for Applied Enzymology and The Japan Diabetes Society. Saori Motoda, Nobuaki Watanabe, Shinsuke Nakata, Isao Hayashi, Ryoya Komatsu, Chisaki Ishibashi, Shingo Fujita, Megu Y Baden, Takekazu Kimura, Ayumi Tokunaga and Kenji Fukui have nothing to declare.
Compliance with Ethics Guidelines
This study was approved by the Institutional Ethics Review Board of Osaka University Hospital and was carried out in accordance with the principles of the Declaration of Helsinki, and a signed consent form was obtained from each subject.
Data Availability
The datasets generated and/or analyzed during this study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Motoda, S., Watanabe, N., Nakata, S. et al. Motivation for Treatment Correlating Most Strongly with an Increase in Satisfaction with Type 2 Diabetes Treatment. Diabetes Ther 13, 709–721 (2022). https://doi.org/10.1007/s13300-022-01235-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-022-01235-x