Abstract
Recent evidence suggests that dimethylfumarate (DMF), known as a highly potent anti-psoriatic agent, might have anti-tumorigenic properties in melanoma. It has recently been demonstrated that DMF inhibits melanoma proliferation by apoptosis and cell cycle inhibition and therefore inhibits melanoma metastasis. Nonetheless, the underlying mechanisms remain to be evaluated. To elucidate the effects of DMF on melanoma cell lines (A375, SK-Mel), we first performed cytotoxicity assays. No significant lactatedehydogenase (LDH) release could be found. In further analysis, we showed that DMF suppresses melanoma cell proliferation in a concentration-dependent manner. To examine whether these effects are conveyed by apoptotic mechanisms, we studied the amount of apoptotic nucleosomes and caspase 3/7 activity using ELISA analysis. Significant apoptosis was induced by DMF in both cell lines, and this could be paralleled with bcl-2 downregulation and PARP-1 cleavage. We also performed cell cycle analysis and found that DMF induced concentration-dependent arrests of G0/G1 as well as G2/M. To examine the underlying mechanisms of cell cycle arrest, we analyzed the expression profiles of important cell cycle regulator proteins such as p53, p21, cyclins A, B1, and D1, and CDKs 3, 4, and 6. Interestingly, DMF induced p53 and p21 yet inhibited cyclin B1 expression in a concentration-dependent manner. Other cell cycle regulators were not influenced by DMF. The knockdown of DMF induced p53 via siRNA led to significantly reduced apoptosis but had no influence on cell cycle arrest. We examined the adhesion of melanoma cells on lymphendothelial cells during DMF treatment and found a significant reduction in interaction. These data provide evidence that DMF inhibits melanoma proliferation by reinduction of important cell cycle inhibitors leading to a concentration-dependent G0/G1 or G2/M cell cycle arrest and induction of apoptosis via downregulation of bcl-2 and induction of p53 and PARP-1 cleavage. Hence, DMF might be an interesting agent in the treatment of melanoma and is worth further investigation in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Fumaric acid esters have been successfully used in the treatment of psoriasis for more than 40 years [1]. In 1994, a mixture of monomethylfumarate (MMF) and dimethylfumarate (DMF; Fumaderm®) was approved for the oral treatment of psoriasis. There are limited side effects that mainly consist of flush, mild lymphopenia, and gastrointestinal discomfort.
Recently, it became obvious that fumaric acid esters have anti-tumoral effects in various tumor entities [2, 3]. Loewe et al. demonstrated that DMF reduces melanoma metastasis in an SCID mouse model [4]. This was supported by Yamazoe et al., who showed that DMF reduces cell invasion and metastasis by inhibiting metalloproteases [5]. Additionally, Valero et al. demonstrated in an SCID mouse model that DMF reduced lymph node metastasis and lymphatic vessel density [6]. Thus, first evidence that DMF induces apoptosis and cell cycle inhibition in melanoma cells is provided. The underlying mechanisms of this action have yet to be determined.
In this study, we investigated the in vitro influence of DMF on melanoma cell proliferation and the underlying mechanisms of cell cycle regulation and apoptosis.
Material and methods
Reagents
Dimethylfumarate, TNF-α and Staurosporin were obtained from Sigma-Aldrich (Hamburg, Germany).
Cell culture
Human melanoma cell lines (A375 and SK-Mel) were purchased from ATCC (Manassas, USA). The cell lines were maintained in Dulbecco’s modified Eagle’s medium (DMEM; Invitrogen, Karlsruhe, Germany) supplemented with 10 % fetal calf serum (FCS, Greiner, Munich, Germany), 2 mM L-glutamine, 100 μg/ml streptomycin and 100 U/ml penicillin (Gibco/BRL, Karlsruhe, Germany) at 37 °C in an atmosphere of 5 % CO2 in air. The cell lines were grown to 80 % confluence before each passage using 0.25 % trypsin/EDTA solution (Invitrogen, Karlsruhe, Germany).
Human dermal lymphatic endothelial cells (DLEC) were purchased from AngioBio Co. (Heidelberg, Germany) and were cultured until the eight passage at 37 °C and 5 % CO2 in Endothelial Cell Growth Medium supplemented with 10 % human serum (Lonza, East Rutherford, NJ, USA).
Normal human skin fibroblasts were isolated from preputia. Cells were propagated in RPMI 1640 medium (Biochrom, Berlin, Germany) with 10 % FCS (PAA, Cölbe, Germany) and 1 % penicillin-streptomycin solution (Biochrom KG, Berlin, Germany) at 37 °C in a 5 % CO2-atmosphere. The medium was renewed twice a week. All procedures performed in studies involving human tissues were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Cell proliferation and cytotoxicity assay
The effect of DMF on cell proliferation was measured by quantifying BrdU via a cell proliferation immunoassay from Roche Diagnostics (Grenzach, Germany). Twenty-four hours after seeding, cells were serum-starved for 24 h and incubated with BrdU and DMF at the indicated concentrations for 24 h. The cytotoxic potential of DMF was determined using an LDH-based cytotoxicity detection kit from Roche. Twenty-four hours after seeding, the cells were incubated with DMF for 24 h at the indicated concentrations.
Apoptosis assay
The effect of DMF on apoptosis was analyzed using a Cell Death Detection ELISA PLUS-Kit and the Caspase 3/7 Assay from Roche Diagnostics (Grenzach, Germany). The assay was carried out according to the manufacturers’ instructions.
Tumor-lymphendothelial adhesion assay
The effect of DMF on tumor-lymphendothelial adhesion was analyzed using a commercial available CytoSelect Adhesion assay kit (Cell Biolabs, San Diego, USA).
Fluorescence-activated cell sorting analysis
Cells were incubated with 100 μM DMF and Ethanol as a control for 24 h after blocking the S-phase of the cell-cycle by treatment with serum depleted-medium for 24 h. The cells were fixed in ice-cold 70 % ethanol. Cells were incubated in PBS containing 40 g/mL RNase A for 30 min at 37 °C and resuspended in PBS containing 50 g/mL propidium iodide. Analysis of cell cycle was assessed by a BD FACScan Cytometer (Becton Dickinson, Franklin Lakes, NJ, USA).
Western blot analysis
Protein extracts were prepared as described previously [7]. Following SDS-PAGE and electroblotting, membranes were incubated with the following primary antibodies: anti-p21, anti-p53, CDC2, CDK2, CDK4, CDK6, cycline D1, cycline A1, cycline B1, bcl-2, cleaved PARP-1, bcl-XL, bax, bid, AIF and anti-tubulin (Cell Signaling, Danvers, MA, USA). Primary antibody application was followed by incubation with horseradish peroxidase-conjugated secondary antibodies (anti-mouse and anti-rabbit IgG, Amersham, Uppsala, Sweden; anti-goat, Dako, Glostrup, Denmark). Blots were developed using an enhanced chemiluminescence detection system (ECL) (Amersham) according to the manufacturer’s instructions.
Small interfering RNA
All small interfering RNA (siRNA) reagents including transfection reagents were obtained from Santa Cruz biotechnology (Dallas,Texas, USA). Cells were transfected with non-target siRNA (siRNA-A), used as negative control. P53 siRNA (pool of two target-specific siRNAs) was used to knockdown p53 expression in A375 cells. The experiments were carried out following the manufacturer’s standard procedures. Forty-eight hours after transfection, cells were left untreated (solvent only) or were treated with DMF (100 μM) for 24 h. Total protein was extracted, and western blot analysis was performed.
Statistical analysis
The data are expressed as the mean ± SEM from at least three independent experiments. Statistical analyses were performed using the Student’s t test or ANOVA where applicable *p < 0.05.
Results
DMF has no cytotoxic effects and inhibits melanoma cell proliferation
We examined the effect of DMF on cell proliferation and investigated its cytotoxicity using two melanoma cell lines, A375 and SK-Mel, revealing that it inhibited melanoma proliferation in a concentration-dependent manner, as determined by the BrdU assay (Fig. 1a, b). At 50 and 100 μM concentrations, DMF reduced melanoma cell proliferation by 52 and 62 % in A375 and by 55 and 61 % in SK-Mel, respectively. These results were not conveyed through cytotoxic effects because DMF did not significantly increase cytotoxicity (Fig. 1c, d).
a, b Proliferation assay for A375 and SK-Mel. Mean values from at least four independent experiments are shown as mean ± SD. c, d Cytotoxicity-assay for A375 and SK-Mel. Mean values from at least three independent experiments are shown as mean ± SD. e Proliferation assay of primary human fibroblasts. Mean values from at least four independent experiments are shown as mean ± SD. *p < 0.05: significant
To analyze whether a normal skin cell is influenced by DMF, we examined its effect on human primary fibroblasts extracted from human praeputia. Here, we could demonstrate that only the highest concentration of DMF (100 μM) suppressed the proliferation by 40 % (Fig. 1e). Therefore, DMF seems to differently affect melanoma cells and normal skin cells.
DMF induces G0/G1 and G2/M cell cycle arrest in a concentration-dependent manner
Results reported by Loewe et al. indicated that DMF could induce G2/M arrest [4]. Using the FACS analysis with propidium iodide-stained A375 and SK-Mel cells, we found that DMF treatment at a concentration of 50 μM increased the G0/G1 phase distribution from 48 to 62 % in A375 and from 67 to 81 % in SK-Mel, demonstrating G0/G1 cell cycle arrest (Fig. 2a, b). Increasing the concentration to 100 μM increased the G2/M phase distribution from 22 to 35 % in A375 and from 16 to 25 % in SK-Mel, demonstrating G2/M cell cycle arrest (Fig. 2a, b). This data shows that the specific cell cycle arrest phase was concentration-dependent. To determine the underlying mechanisms of cell cycle arrest, we examined the expression of important cell cycle regulators. As expected in G0/G1 and G2/M arrests, p21 levels increased in a concentration-dependent manner (Fig. 2c, see also supplementary Figure S1a,b). To determine whether inducing the cell cycle inhibitor p21 is regulated by p53, a major regulator of p21, we determined the expression of p53 after treatment with DMF using western blot analysis. Interestingly, we observed an increase in p53 protein expression in a concentration-dependent manner comparable to the induction of p21 protein expression (Fig. 2c; see also supplementary Figure S1c,d). Expression of cyclin B1, an important specific activator of the G2/M phase, was almost completely suppressed at the higher treatment concentration, possibly explaining the concentration-dependent G2/M cell cycle arrest (Fig. 2d; see also supplementary Figure 1g,h). The other cell cycle proteins did not change their expressions after DMF treatment.
a, b Analysis of cell cycle distribution by FACS using propidium iodide-stained melanoma cell lines A375 and SK-Mel. The figure shows the percentage of cells in G0/G1, S and G2/M phase. Data displayed are representative of at least three experiments that were performed revealing comparable results shown as mean ± SD. *p < 0.05: significant. c, d Representative western blot analyses of melanoma cell lines A375 and SK-Mel that were treated for 24 h with vehicle or DMF for varying concentrations as indicated. Comparable results were obtained from at least three independent experiments
DMF induces apoptosis via bcl-2 inhibition and PARP-1 cleavage
To rule out apoptotic mechanisms, we investigated the DMF-induced release of cytoplasmic histone-associated DNA fragments and caspase 3/7 activity. We found that DMF significantly induced apoptosis in both cell lines and that caspase 3/7 activity was increased in a concentration-dependent manner (Fig. 3a–d). To determine the underlying mechanisms of apoptosis, we examined the expression of various important apoptosis-associated proteins (Fig. 3e). We could then demonstrate that expression of the anti-apoptotic Bcl-2 protein was significantly suppressed, whereas bcl-XL, bax, bid, and AIF remained unchanged (Fig. 3e; see supplemental Fig. S1g,h). We also demonstrated a significant increase in cleaved PARP-1, an important aspect for its inactivation, and therefore a pro-apoptotic mechanism (Fig. 3e; see also supplemental Fig. S1e,f).
a, b Analysis of apoptosis in melanoma cell lines A375 and SK-Mel. Mean values from at least four independent experiments are shown as mean ± SD. c, d Caspase 3/7 assay. Mean values from at least four independent experiments are shown as mean ± SD. *p < 0.05: significant. e Representative western blot analyses of melanoma cell lines A375 and SK-Mel that were treated for 24 h with vehicle or DMF for varying concentrations as indicated. Comparable results were obtained from at least three independent experiments
Knockdown of p53 reduces DMF dependent apoptosis significantly
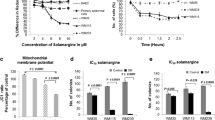
To analyze whether the knockdown of DMF-induced p53 expression influences apoptosis and the G2M cell cycle arrest we performed p53 siRNA experiments. Here, we could demonstrate that the knockdown of p53 significantly inhibits DMF-induced apoptosis. In contrast, p53 knockdown did not influence the amount of DMF-induced G2M cell cycle arrest (Fig. 4a–c).
a Representative western blot analyses of A375 cells that were incubated with siRNA against p53 or control siRNA and treated with DMF (at 100 μM) or solvent only as indicated for 24 h. Total cellular protein was separated by 10 % SDS-PAGE. p53 and α-tubulin protein as loading control were detected by enhanced chemiluminescence. Comparable results were obtained from three independent experiments.b Analysis of apoptosis in A375 after p53 knockdown. Mean values from at least four independent experiments are shown as mean ± SD. *p < 0.05: significant. c Analysis of cell cycle distribution by FACS using propidium iodide-stained A375 melanoma cells. The figure shows the percentage of cells in the G2/M phase after p53 knockdown. Data displayed are representative of at least three experiments that were performed revealing comparable results shown as mean ± SD. *p < 0.05: significant
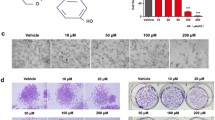
DMF inhibits melanoma-lymphendothelial cell adherence
In vivo, it could be demonstrated that DMF inhibits lymphogenic metastasis [6]. To determine whether DMF influences the interaction between lymphendothelial and melanoma cells, we performed adhesion assays (Fig. 5a, b) and found that it effectively inhibits the adherence of both A375 and SK-Mel melanoma cells on dermal lymphendothelial cells. This might be an important reason for reduced metastasis.
Discussion
In vivo DMF was found to have anti-tumorigenic as well as anti-lymphometastatic action in melanoma [4, 6]. The first analysis by Loewe et al. demonstrated that DMF induces apoptosis and G2/M cell cycle arrest in melanoma cell lines [4]. Unfortunately, the underlying mechanisms remained unclear.
In this study, we demonstrated that DMF inhibited the proliferation of melanoma cell lines via a concentration-dependent induction of G0/G1 and G2/M arrest in a p21-dependent manner. We also showed that it increased expression of the cell cycle inhibitor p21 and suppressed expression of the cell cycle inductor cyclin B1. In addition, we demonstrated that the expression of the tumor suppressor p53 is induced by DMF treatment. Knockdown of p53 reduces DMF-induced apoptosis but does not influence cell cycle arrest. We also revealed that DMF might induce apoptosis via suppression of Bcl-2 and increased PARP-1 cleavage. Furthermore, we demonstrated that it suppressed melanoma adherence on lymphendothelial cells.
Thus, we in part confirmed the results of Loewe et al. that DMF inhibits melanoma cell line proliferation [4]. We found this inhibition after 24 h rather than 3 and 6 days, as reported by Loewe et al. and our cytotoxicity analysis excluded cytotoxic effects as the means to proliferation inhibition. Loewe et al. demonstrated G2/M arrest using 84 μM DMF [4]. We used 100 μM DMF and obtained similar results, but showed a G0/G1 cell cycle arrest using 50 μM DMF. We were additionally able to demonstrate the underlying mechanism of cell cycle arrest. We revealed a concentration-dependent increase in p21 expressions. Recently, DMF was shown to induce G0/G1 cell cycle arrest via induction of p21 in vascular smooth muscle cells [8]. The induction of p21 by DMF was demonstrated, up to now, only in vascular smooth muscle cells, pre-adipocytes, and lymphendothelial cells [8–10], and it seemed to be an important mechanism of regulation. Our data support this. Induction of G2/M cell cycle arrest by DMF was shown not only in melanoma cells but also in colon carcinoma cells [11]. We showed that cyclin B1, an important cell cycle activator at the G2/M boundary, was almost completely suppressed after treatment with 100 μM DMF. Kedinger et al. demonstrated that suppression of cyclin B1 in melanoma cells leads to effective inhibition of melanoma metastasis in a B16-F10 murine melanoma metastasis model [12]. Therefore, we postulate that the combination of cyclin B1 suppression and p21 induction induces G2/M arrest at higher DMF concentrations in melanoma cells, whereas the exclusive induction of p21 at lower concentrations induces G0/G1 arrest. Comparable results were demonstrated by Lee et al. in HT29 cells, where lower concentrations of cordycepin induced G2/M arrest, and higher concentrations induced G0/G1 arrest [13]. Miyanaga et al. showed that low docetaxel concentrations induced G0/G1 arrest, whereas higher concentrations induced G2/M arrest [14]. Therefore, cell cycle inhibition by DMF seems to be not only cell type-specific but also concentration-dependent when the blocked cell cycle boundary is involved. Loewe et al. demonstrated that DMF induces apoptosis in human melanoma cell lines, but failed to demonstrate the underlying mechanisms [4]. We could demonstrate that the DMF treatment led to inhibition of the anti-apoptotic protein bcl-2 and increased cleavage of PARP-1. Inhibition of bcl-2 is an important way to suppress melanoma cell proliferation [15]. Recently, Tsubaki et al. demonstrated that DMF induces apoptosis in hematopoetic tumor cells, in part via inhibition of bcl-XL expression, another protein of the bcl-group with anti-apoptotic effects [16]. In our melanoma cells, the expression of bcl-XL was unchanged. Our results are comparable to those obtained by Treumer et al., who demonstrated that DMF suppresses bcl-2 expression in human T cells and effectively induces apoptosis [17]. We additionally demonstrated a significant increase in PARP-1 cleavage, leading to its inactivation. This is an important pro-apoptotic mechanism. Inhibition of PARP-1 is a promising target of further anti-tumor strategies, and there are various studies under way to prove the efficacy of PARP-1 inhibitors in clinical practice [18]. Chevanne et al. demonstrated that inhibition of PARP-1 leads to sustainable growth impairment in melanoma cells [19]. Staibano et al. demonstrated that in melanomas of the head and neck, overexpression of PARP-1 is associated with more aggressive cell behavior [20]. We showed that DMF facilitates PARP-1 cleavage and is therefore a new PARP-1 inhibitor. Promising clinical phase II studies are underway in ovarian cancer using the PARP-1 inhibitor Olaparib, demonstrating anti-tumor activity [21, 22].
To analyze whether DMF dependent p53 expression increase is relevant concerning apoptosis and cell cycle arrest, we performed p53 knockdown experiments revealing that DMF-induced p53 increases apoptosis but does not influence G2M cell cycle arrest. P53 is an important regulator of apoptosis as well as the cell cycle [23]. Interestingly, suppression of DMF-induced p53 does not influence cell cycle arrest in our melanoma cell lines. This might be due because of the effective induction of the cell cycle inhibitor p21 and the suppression of cyclin B1.
Finally, we demonstrated that DMF suppresses adherence of both melanoma cell lines on primary dermal lymphendothelial cells. This action might be an additional anti-lymphometastatic action of DMF, and if it is, this strengthens the in vivo results of Valero et al., who demonstrated inhibition of lymphatic metastasis by DMF [6].
In summary, we have elucidated the underlying mechanisms of DMF-induced apoptosis and cell cycle inhibition in melanoma cell lines and have shown that lymph endothelial adherence in melanoma cells is reduced. Suppression of bcl-2 and inactivation of PARP-1 could demonstrate a significant increase in p21 and p53 expression and cyclin B1 suppression. These data now explain, in part, the anti-tumorigenic action of DMF in melanoma.
Abbreviations
- DMF:
-
Dimethylfumarate
- BrdU:
-
Bromodesoxyuridine
- LDH:
-
Lactatedehydrogenase
- DMSO:
-
Dimethylsulfoxide
- DLEC:
-
Dermal lymphatic endothelial cells
References
Schweckendiek W. Treatment of psoriasis vulgaris. Med Monatsschr. 1959;13(2):103–4.
Meissner M, Valesky EM, Kippenberger S, Kaufmann R. Dimethyl fumarate—only an anti-psoriatic medication? J Dtsch Dermatol Ges. 2012;10(11):793–801.
Arbiser JL. Fumarate esters as angiogenesis inhibitors: key to action in psoriasis? J Invest Dermatol. 2011;131(6):1189–91.
Loewe R, Valero T, Kremling S, Pratscher B, Kunstfeld R, Pehamberger H, et al. Dimethylfumarate impairs melanoma growth and metastasis. Cancer Res. 2006;66(24):11888–96.
Yamazoe Y, Tsubaki M, Matsuoka H, Satou T, Itoh T, Kusunoki T, et al. Dimethylfumarate inhibits tumor cell invasion and metastasis by suppressing the expression and activities of matrix metalloproteinases in melanoma cells. Cell Biol Int. 2009;33(10):1087–94.
Valero T, Steele S, Neumüller K, Bracher A, Niederleithner H, Pehamberger H, et al. Combination of dacarbazine and dimethylfumarate efficiently reduces melanoma lymph node metastasis. J Invest Dermatol. 2010;130(4):1087–94.
Meissner M, Doll M, Hrgovic I, et al. Suppression of VEGFR2 expression in human endothelial cells by dimethylfumarate treatment: evidence for anti-angiogenic action. J Invest Dermatol. 2011;131(6):1356–64.
CJ O, Park S, Kim JY, Kim HJ, Jeoung NH, Choi YK, et al. Dimethylfumarate attenuates restenosis after acute vascular injury by cell-specific and Nrf2-dependent mechanisms. Redox Biol. 2014;2:855–64.
Valesky EM, Hrgovic I, Doll M, Wang XF, Pinter A, Kleemann J, et al. Dimethylfumarate effectively inhibits lymphangiogenesis via p21 induction and G1 cell cycle arrest. Exp Dermatol. 2015. doi:10.1111/exd.12907.
Kang HJ, Seo HA, Go Y, CJ O, Jeoung NH, Park KG, et al. Dimethylfumarate suppresses adipogenic differentiation in 3T3-L1 preadipocytes through inhibition of STAT3 activity. PLoS One. 2013;8(4):e61411.
Odom RY, Dansby MY, Rollins-Hairston AM, Jackson KM, Kirlin WG. Phytochemical induction of cell cycle arrest by glutathione oxidation and reversal by N-acetylcysteine in human colon carcinoma cells. Nutr Cancer. 2009;61(3):332–9.
Kedinger V, Meulle A, Zounib O, Bonnet ME, Gossart JB, Benoit E, et al. Sticky siRNAs targeting survivin and cyclin B1 exert an antitumoral effect on melanoma subcutaneous xenografts and lung metastases. BMC Cancer. 2013;13:338.
Lee SY, Debnath T, Kim SK, Lim BO. Anti-cancer effect and apoptosis induction of cordycepin through DR3 pathway in the human colonic cancer cell HT-29. Food Chem Toxicol. 2013;60:439–47.
Miyanaga S, Ninomiya I, Tsukada T, Okamoto K, Harada S, Nakanuma S, et al. Concentration-dependent radiosensitizing effect of docetaxel in esophageal squamous cell carcinoma cells. Int J Oncol. 2016;48(2):517–24.
Chipuk JE. BCL-2 proteins: melanoma lives on the edge. Oncoscience. 2015;2(9):729–30.
Tsubaki M, Komai M, Fujimoto S, Itoh T, Imano M, Sakamoto K, et al. Activation of NF-κB by the RANKL/RANK system up-regulates snail and twist expressions and induces epithelial-to-mesenchymal transition in mammary tumor cell lines. J Exp Clin Cancer Res. 2013;32:62.
Treumer F, Zhu K, Gläser R, Mrowietz U. Dimethylfumarate is a potent inducer of apoptosis in human T cells. J Invest Dermatol. 2003;121(6):1383–8.
Anwar M, Aslam HM, Anwar S. PARP inhibitors. Hered Cancer Clin Pract. 2015;13(1):4.
Chevanne M, Zampieri M, Caldini R, Rizzo A, Ciccarone F, Catizone A, et al. Inhibition of PARP activity by PJ-34 leads to growth impairment and cell death associated with aberrant mitotic pattern and nucleolar actin accumulation in M14 melanoma cell line. J Cell Physiol. 2010;222(2):401–10.
Staibano S, Pepe S, Lo Muzio L, Somma P, Mascolo M, Argenziano G, et al. Poly(adenosine diphosphate-ribose) polymerase 1 expression in malignant melanomas from photoexposed areas of the head and neck region. Hum Pathol. 2005;36(7):724–31.
van der Noll R, Marchetti S, Steeghs N, Beijnen JH, Mergui-Roelvink MW, Harms E, et al. Long-term safety and anti-tumour activity of olaparib monotherapy after combination with carboplatin and paclitaxel in patients with advanced breast, ovarian or fallopian tube cancer. Br J Cancer. 2015;113(3):396–402.
Oza AM, Cibula D, Benzaquen AO, Poole C, Mathijssen RH, Sonke GS, et al. Olaparib combined with chemotherapy for recurrent platinum-sensitive ovarian cancer: a randomised phase 2 trial. Lancet Oncol. 2015;16(1):87–97.
Yu J, Zhang L. The transcriptional targets of p53 in apoptosis control. Biochem Biophys Res Commun. 2005;331(3):851–8.
Acknowledgments
The work was sponsored by the Brigitte und Dr. Konstanze Wegener-Stiftung (M.M.); Dr. Kurt & Eva Herrmann Stipendium, 2013 (I.K.); Nachlässe Maria Christine Held und Erika Hecker (E.V.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Irina Kaluzki and Igor Hrgovic contributed equally.
Electronic supplementary material
ESM 1
(PDF 113 kb)
Rights and permissions
About this article
Cite this article
Kaluzki, I., Hrgovic, I., Hailemariam-Jahn, T. et al. Dimethylfumarate inhibits melanoma cell proliferation via p21 and p53 induction and bcl-2 and cyclin B1 downregulation. Tumor Biol. 37, 13627–13635 (2016). https://doi.org/10.1007/s13277-016-5285-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-016-5285-6