Abstract
Most patients with cancers died of distant metastasis. It is always difficult to find cancer metastasis in early time, let alone to prevent or cure it. Currently, oncologists place high hopes on circulating tumor cell (CTC), which, compared to current imaging methods, is found more sensitive for early metastasis. Recently, techniques for CTC enrichment and identification are developing quickly. However, there are great challenges in the clinical interpretation of CTC assessments. Increasing studies have shown the heterogeneity of CTCs, which may play different roles in cancer metastasis. Epithelial-mesenchymal transition is not only the main mechanism of the cancer cells invading the circulation system but also a distinguished characteristic of CTCs. Investigators are trying to differentiate specific subgroups of CTCs that are truly responsible for cancer metastasis. Here, we reviewed the current evidences on epithelial-mesenchymal transition of CTCs from perspectives of enrichment methods, biology, and its subgroups.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Distant metastasis accounts for almost 90 % of cancer-related deaths, and the details of cancer metastasis are largely unknown. Several hypotheses have been proposed to depict the basic process of cancer cell migration from primary site to ectopic organs [1]. Regardless of their differences, all models hypothesize the existence of circulating tumor cells (CTCs) and the intravasation of cancer cells from primary tumors. Epithelial-mesenchymal transition (EMT) has been widely accepted as the mechanism by which cancer cells acquire invasive capacity and migrate toward vessels by degrading extracellular matrix. Intra- and inter-patient heterogeneity of tumor cells has been found recently via single cancer cell RNA sequencing [2, 3] and immunological repertoire analysis [4, 5]. Some investigators believe that certain subgroups of cancer cells are highly invasive and are more contributable to metastases formation than others [6–8]. Phenotypes of CTCs have been explored from different perspectives such as EMT [9], apoptosis [10], and expressions of certain genes [11].
Among the multiple ways used by oncologists to identify phenotypes, epithelial and mesenchymal characteristics of cancer cells are one of the most frequently used classifications, particularly for tumors originating from epithelial cells. In these settings, EMT is considered as a pivotal step through which cancer cells invade into the circulation and form CTCs. A corresponding mesenchymal-epithelial transition (MET) is hypothesized to occur after extravasation of CTCs from the circulation. However, the detailed roles of EMT are still under debate since a cooperative model has opposed the hypothetical EMT-MET process [12]. Here, we review the current evidences on CTC-based metastasis from the perspective of CTC phenotypes in terms of their distribution, biological and clinical relevance, and their metastatic ability, particularly focusing on EMT.
Phenotype of cancer cells associated with metastasis
Calculating the number of CTCs in a patient’s body is difficult since most CTCs can only exist for several hours before they can be detected [13]. However, according to the current results of CTC capture technologies (all of which could capture only a part of CTC repertoire), a considerable number of CTCs is believed to exist in a patient’s circulation. It has been speculated that only 0.01 % of all CTCs are able to survive and form micrometastases in distant organs [14], which means that the majority of CTCs are “eliminated” in the circulation. While numerous studies have confirmed the prognostic value of CTC enumeration in breast [15], prostate [16], colorectal [17] and lung cancers [18], and cholangiocarcinoma [19], the phenotypes of CTCs and their implications in clinical practice are rarely reported.
The influence of cancer cell phenotype on metastasis exists in all stages of the metastatic cascade (well reviewed by Bonnomet et al. [20]). In the stage of CTC generation, induction of MET in the primary cancer reduced numbers of CTCs and lung metastases in an orthotropic mouse model of breast cancer [21]. In the circulation, the survival, viability, and invasive ability of CTCs determine the efficiency of extravasation. Epithelial cells tend to undergo apoptosis without detachment. Although cancer cells were believed to be resistant to anoikis [22], apoptosis of single CTC was relatively high in breast and lung cancers [10, 23, 24]. Intuitively, apoptotic CTCs are not likely to form metastases. Unfortunately, although nab-paclitaxel chemotherapy increased CTCs with apoptotic phenotype in patients with metastatic triple-negative breast cancer, it did not alter the proportion of apoptotic CTCs, nor there was correlation of apoptotic CTCs with clinical benefits [10]. Thus, there is little evidence that apoptotic phenotype of CTCs is associated with metastasis and prognosis.
Biology of cancer cells with distinct phenotypes
Expressions of certain crucial genes can lead to distinct biological behaviors of CTCs, which can be accordingly classified into different subgroups or phenotypes. Common phenotypes in CTC classification include epithelial/mesenchymal [25], cancer stem cell (CSC)/non-CSC [26], apoptotic/non-apoptotic [10], Her2-positive/-negative [27], and PD-L1-positive/-negative [28] phenotypes. Large/small size [8] and mono-/multi-nucleate [29] were also differentiated and studied in some institutes. Different phenotypes of CTCs, which have common traits as cancer cells, are all prone to survive in blood [9, 30] by resistance of anoikis [31], and are crucial for metastasis formation [32]. However, each phenotype of CTCs shows distinct capacity or specific characteristics of its own. For instance, Her2-positive tumor is more likely to be associated with presence of CTCs [33], suggesting that Her2-positive cancer cells are more invasive. Another example is that CTCs with large size from central venous blood are inclined to lodge in the lung and form metastases, while small-sized CTCs can easily pass through microvessels and can be detected in peripheral venous blood [34].
Among these phenotypes, EMT phenotype attracts the most attention. Epithelial cancer cells are stiffer and less invasive, while mesenchymal tumor cells or cancer cells undergoing EMT (EMT-CTCs, positive for mesenchymal markers with or without positivity for epithelial markers) are more invasive and easy to change their shapes. These characteristics were in accordance with massive changes of relevant gene expression such as genes of matrix metalloproteinase (MMP) and cytoskeleton proteins. Even though EMT-CTCs have been frequently observed, the exact mechanism by which EMT is induced in CTCs is largely unknown. Intuitively, inducers of EMT in CTCs are probably the same with those in common cancer cells. Animal experiments suggested that at least in hepatocellular carcinoma, hepatocyte growth factor (EGF) could induce EMT via c-Met overexpression [35]. Similar effect of EGF was noticed in breast cancer [36]. Moreover, studies in human breast cancer suggested that transforming growth factor-beta was another EMT inducer in CTCs [9, 36]. EMT-CTCs are believed to be responsible for metastasis formation via several mechanisms. New discoveries showed that MMPs expressed by EMT-CTCs could be induced by host stroma and facilitate CTC extravasation [37].
Up to date, there have been no standard methods or biomarkers for defining EMT status of CTCs. Cytokeratins (CKs) and vimentin are the most frequently used markers for epithelial and mesenchymal phenotypes. In addition, N-cadherin, Snail, Slug, Twist, and fibronectin were also adopted as mesenchymal markers by a few investigators [23, 36, 38, 39], while E-cadherin was the main representative for epithelial markers [23, 40]. More markers like plastin3 for EMT-CTC was identified [41]. More subgroups of CTCs will be identified if two or more markers are used for definition of EMT status since expressions of these markers is usually highly heterogeneous in CTCs [23, 36]. Therefore, caution should be taken when different results are interpreted.
Besides, biomarkers and methods for detection may both be important. Vimentin mRNA is exemplified to be an unsuitable marker [42], though vimentin itself is a well-accepted marker for mesenchymal phenotype. In addition, compared to epithelial cell adhesion molecule (EpCAM), CKs are more specific for detection of epithelial CTCs since vimentin-positive cells are often CK negative [26]. With the limited available data, a panel of markers may be more appropriate for definition of epithelial or mesenchymal phenotype.
Phenotypes of captured CTCs
The technology for CTC isolation or capture has greatly improved over the past 15 years, giving us an opportunity to scrutinize CTCs. Current evidence clearly showed the inter- and intra-patient heterogeneity of phenotypes and oncogenic mutations of CTC [9, 43, 44]. The phenotypes of CTCs still largely depend on the methods used for CTC capture. EpCAM-based CTC capture, which is currently the most mature technology, mainly captures epithelial CTCs. However, several reports showed that EpCAM-based technology failed to detect CTCs in a considerable part (>30 %) of patients with metastatic cancer [9, 45]. Additionally, EpCAM-negative CTCs were identified, and EpCAM-positive CTCs account for roughly only a half of the total number of CTCs [7]. Although CellSearch®, the only US Food and Drug Administration (FDA)-approved facility for CTC capture, is no doubt a milestone of CTC capture, numerous methods using EpCAM-independent strategy have achieved a significantly higher yield [46, 47]. Simply by further detecting the waste discarded by CellSearch®, investigators doubled the incidence of CTCs found in patients and also the amount of CTCs in an individual patient [7]. Although surface marker-based technologies selectively capture CTCs, they are biased methods. Similarly, although isolation by size of epithelial tumor cells (ISET) platform can avoid differences in antigen expression, it actually selects CTCs according to their size and stiffness [8, 48]. From this point of view, all CTC capture methods are biased. But based on the perspectives of most investigators, we here define ISET platform as unbiased.
Since the extension of EMT can be different among CTCs, without a quantification method, it is difficult to determine the EMT status of CTCs among patients. In practice, although with slight difference, many investigators used a “ratio” of epithelial and mesenchymal markers (or the reciprocal) to demarcate CTC phenotypes [9, 49, 50]. The ratio has been confirmed to be directly associated with EMT [49]. Given the differences in their principles, it is not surprising that the results of EMT-CTC show a weak association between ISET platform and CellSearch®. A study focusing on this issue indicated that no significant correlation was found when comparing CellSieveTM (a microfiltration system using 7-μm pores) with CellSearch® [51].
Phenotypes of CTCs captured by surface marker-based technology
Surface marker-based technology isolated a subgroup of CTCs which expressed certain proteins such as EpCAM or Her2. These CTCs usually have similar characteristics although they are not homogeneous. The surface markers adopted can influence the results of CTC enumeration and phenotype in both isolation and detection steps. For instance, CK20 extensively improved the detection rate of CTCs after isolation using CellSearch® [52]. Based on EpCAM antibody, many methods have been developed for better efficacy and purity of CTC isolation. Given that the amount of EpCAM molecules on CTC surface influences antigen-antibody affinity in different velocity, a magnetic nanoparticle-mediated strategy was invented by the Canadian to isolate distinct subgroups of CTCs with high or low expression of EpCAM [43].
Phenotypes of CTCs captured by ISET platform
Generally, the yield of ISET platform is significantly higher (two to four times) than that of CellSearch® as the former is supposed to isolate both epithelial and mesenchymal CTCs [47, 53, 54]. Using ISET platform or similar methods, investigators could identify more EMT-CTCs, and the proportion of vimentin-positive CTCs could be as high as 80–100 % in most patients [29].
A pioneer study in lung cancer showed that all patients had EMT-CTCs, some patients had mesenchymal CTCs, but no patient had epithelial CTCs [55]. Wu et al. used a filtration method and tri-color RNA in situ hybridization (RNA-ISH) to investigate the EMT phenotype in 164 patients with six types of cancer. Approximately a half of samples contained CTCs with mixed epithelial/mesenchymal phenotype, and an equal proportion (27 %) of samples contained epithelial or mesenchymal CTCs [25]. These studies suggested a high proportion of EMT-CTCs in patients regardless of cancer types.
Phenotypes of CTCs captured by other strategies
CTCs isolated using a subtraction enrichment method from a non-small cell lung cancer (NSCLC) patient were found with vimentin expression via both immunofluorescence and iFISH, though EpCAM expression was much more frequent in patients with a variety of cancers using the same enrichment and detection platform. [56] Interestingly, CK18 was negative in most CTCs enriched using this EpCAM-independent technology from patients with lung and esophageal cancers [56]. Using reverse transcription polymerase chain reaction (RT-PCR) directly from collected blood samples, some investigators proved that the positive rate of intracellular markers (vimentin 45 %) was higher than that of surface markers (EpCAM 30 %, CK19 35 %), and the former was more significantly associated with disease stage. Particularly, vimentin rather than EpCAM or CK19 was extensively elevated in patients with stage IV breast cancer [57]. Biological behavior-based isolation was also used based on the logics that CTCs showing invasive potentials are more likely to form metastases. CAM-avid CTCs (Vitatex platform), which were believed to be highly invasive, were mainly mesenchymal and epithelial/mesenchymal phenotypes [46].
Phenotype of CTCs and its clinical implications
The clinical significance of CTC is generally acceptable but still under debate in some aspects. Early studies simply focused on qualitative analysis or enumeration of CTCs, and evidence has shown prognostic value of CTC enumeration in various types of cancers such as colorectal cancer, hepatocellular carcinoma, pancreatic cancer, breast cancer, lung cancer, prostate cancer, and head and neck squamous cell carcinoma [58–64]. However, the number of CTCs is highly different among the major types of cancers [65]. Many factors influence the quantity and clinical roles of CTCs. For instance, timing of CTC detection is important because CTC count can be extensively changed according to disease stage, treatment, and isolation methods. For example, some investigators demonstrated that presence of CTCs detected by CellSearch® in postoperative patients with colorectal cancer was infrequent and was not associated with patient survival or clinicopathological parameters [66], while others found that postoperative rather than preoperative CTCs were associated with clinicopathological parameters and prognosis as well in colorectal cancer [67]. This discrepancy suggests the complexity of clinical relevance of CTC.
It would be of great value to trace the sequential change of CTC count and phenotype during the whole process of treatment. CK-negative CTCs were correlated with metastatic tumor burden in a mouse model [68]. In human, limited data have shown that CTC count rapidly decreased in patients who had good responses to treatment, and mesenchymal CTCs seemed to be more relevant to recurrence and metastasis [9, 69]. The mutual change between epithelial and mesenchymal phenotypes provides another dimensional information about CTCs. A phenotype turnover of CTC from mesenchymal (CK negative) to epithelial (CK positive) was observed after systematic treatment in patients with non-metastatic breast cancer [36]. Nowadays, more and more studies have confirmed the roles of mesenchymal CTC and EMT-CTC in clinical practice [9, 25, 49]. Although some studies demonstrated that only the presence of EpCAM-positive CTCs was associated with poor prognosis [7], most studies claimed that mesenchymal CTCs which were often EpCAM-negative were more invasive and thus associated with metastasis [70, 71]. Actually, increasing studies have shown ambiguous or even negative results regarding the association between CTCs enumerated by CellSearch® and prognosis of patients [66, 72]. On the contrary, the incidence of mesenchymal CTCs in patients could be much higher than that of epithelial phenotype in a large trial of early stage breast cancer [69]. The proportion of mesenchymal CTCs was significantly correlated with tumor size and epidermal growth factor receptor expression in non-metastatic breast cancer [36]. In metastatic breast cancer, EMT-CTC was associated with tumor relapse after chemotherapy [38]. The ratio of mesenchymal CTCs was more significantly increased in metastatic cancer than in non-metastatic cancer as seen in many cancers [25, 50]. Consistently, Li’s group showed that a special antibody targeting cell-surface vimentin was efficient to capture EMT-CTC, which was significantly associated with adjuvant chemotherapy response [73]. A trial testing N-cadherin or O-cadherin as a biomarker of EMT-CTC in metastatic prostate and breast cancer patients is also being conducted (NCT02025413).
There are several major concerns about elucidating the circulating epithelial lineage as CTCs in patients. Firstly, healthy people naturally have a small quantity of epithelial cells in the blood [46]. Secondly, sarcoma [74], pleural mesothelioma [75], and certain subtypes of cancers such as normal-like breast cancer [42] naturally have low expression of EpCAM or CKs, and epithelial CTCs are probably apoptotic [24]. Thirdly, EpCAM may be downregulated or translocated into nuclei, leading to reduced expression in the surface of CTCs [76]. Another critical one is that EMT is quite common in CTCs and can cause loss of EpCAM and CKs (affecting both isolation and detection process) [7, 77].
However, the conundrum is that EpCAM may be not a definite epithelial marker. Although inhibition of EpCAM was reported to be associated with loss of E-cadherin in vitro [78], EpCAM+/E-cadherin−, EpCAM+/CK−, and EpCAM−/CK+ CTCs were often detected in various cancers [79, 80]. Besides, by using EpCAM-based technology, investigators frequently acquired CTCs with mesenchymal phenotype and epithelial/mesenchymal biphenotype [26, 81]. This is related to the aforementioned question regarding the way to define epithelial and mesenchymal phenotypes in CTCs.
Knowing the high heterogeneity of CTCs in patients, oncologists have been searching for subtypes of CTCs responsible for metastasis. It is always difficult to identify a consistent subtype of CTCs associated with poor prognosis or treatment response [82]. Fortunately, some studies realized the importance of certain CTC subtypes such as mesenchymal CTC [25, 49], CTC clusters [6, 40], and small (and very small) nuclear CTCs [8]. These subtypes of CTCs may have biological properties, making them easier to form metastases in target organs. However, the metastatic priority of these subtypes of CTCs needs more evidence, and the mechanisms warrants further elucidation.
Even with such uncertainty, people believe that CTCs will be used for the next-generation cancer detection and act as a treatment monitor. CTC has now been used as an indicator in many clinical trials regarding cancer treatment and new drug development [83–86]. In addition, sequencing of CTCs is capable of profiling the whole genome-wide variation and also the specific mutations of the primary tumor [87, 88]. Nevertheless, capture of CTCs is promising to reduce tumor burden [89]. Although the dynamic variation of mutation status of CTCs needs further investigation, the consistency between CTC and primary tumor is inspiring and may provide clinicians a wonderful opportunity to examine the mutation status of critical genes feasibly and efficiently.
Difference of phenotypes of cancer cells within CTC clusters
CTC cluster was first identified in the 1960s; however, it is not until recently that the roles of CTC cluster in tumor metastasis have been emphasized. It was rare but convincing to see CTC clusters in microvessels of human lung by autopsy [90]. Currently, the most outstanding work regarding CTC cluster-mediated metastasis was done by Aceto and colleagues, who found that CTC clusters had much higher potential (∼40 times compared to single CTCs) of metastasis formation using a breast cancer mouse model [6]. In patients with cancer, reduction of CTC clusters was also remarkable after cancer treatment [9, 91], and recurrence of CTC clusters was associated with the relapse of tumor [9]. The incidences of CTC clusters found in patients’ peripheral blood ranged from 0 to >90 % in different studies [25, 27, 40, 46, 92–94], probably because of the different types of cancer, stages of the disease, and methods of detection. Several studies proved the survival advantage of CTC clusters [10, 23, 40], which may contribute to their highly metastatic potential. Notably, the incidence and number of CTC clusters in patients may not parallel the number of single CTC [46], suggesting that CTC cluster had its unique biological characteristics. Nevertheless, CTC clusters can also protect cancer cells from apoptosis. Cancer cells aggregating as clusters seldom undergo apoptosis [10, 23]. In addition, Geng et al. reported a positive feedback loop mediated by CTC cluster via pro-inflammatory cytokines to activate and maintain the adhesive phenotypic switch, resulting in a phenotype more capable of invading the endothelium [95].
Most CTC clusters consist of 2 to more than 100 of cancer cells with or without immune cells and platelets [9, 25, 29, 46, 89, 91]. The size of CTC cluster is critical for heterogeneity generation since it creates and maintains a special microenvironment within the cluster. For example, a two-layer spheroid with around 30 cells is sufficient to maintain a hypoxic environment in the inner layer of the cluster [40]. Cancer cells encounter distinctive microenvironments when they are located in the inner or outer layers of a cluster. These environmental parameters include oxygen, nutrients, blood shear force, cytokines, etc. The hypoxic microenvironment within a CTC cluster has been found [40]. Since hypoxia is a potent factor to induce EMT in nearly all types of cancers [96, 97], it is also reasonable that EMT can be induced or maintain within CTC clusters. Besides, cancer cells can undergo EMT by interacting with platelets integral to a CTC cluster [98].
The heterogeneity of EMT phenotype in CTC clusters has been confirmed in many types of cancers (Table 1). Using a size-based isolation technology and RNA-ISH detection method, Wu et al. identified 16 CTC clusters from three patients with metastatic liver cancer, nasopharyngeal cancer, and breast cancer, respectively, and all these clusters showed a mesenchymal phenotype [25]. Similarly, Yu and colleagues observed strong staining of mesenchymal markers and weak staining of epithelial markers via RNA-ISH in CTC clusters from a patient with breast cancer [9]. Consistently, using a flexible microspring array device, Harouaka et al. confirmed the higher proportion (nearly 90 %) of vimentin-positive cancer cells within clusters, although the proportion of the vimentin-positive cancer cell varied among clusters [29].
With the first device using label-free technology for CTC cluster capture, investigators from Harvard University reported the currently highest incidence (30–40 %) of CTC cluster in both epithelial and non-epithelial cancers [99]. In contrast, the previous herringbone-chip (HB-Chip) only identified CTC clusters in 15 % of patients with metastatic prostate and lung cancers [100]. Using EpCAM antibody, the CTC clusters isolated with the HB-Chip was found positive for CK7/8; unfortunately, the authors did not perform analysis on mesenchymal markers [100]. In another study on lung cancer, vimentin was found frequently expressed in CTC clusters, and E-cadherin was rarely seen [23]. Furthermore, an ex vivo study found that CTC clusters had more cells with mesenchymal phenotype during expansion, even though the epithelial cells and biphenotypic epithelial/mesenchymal cells persistently existed [91].
The next generation: phenotype-independent CTC capture and detection
The variation of results of CTC analysis based on different platforms can largely attribute to the technologies used for CTC isolation and detection. Having realized the shortcomings of the current methods, a plenty of novel technologies are under investigation. Generally, two strategies are adopted. The first one is still based on cell surface markers, using two or more antibodies (with at least one non-epithelial antibody) to isolate other subtypes of CTC in addition to EpCAM-positive CTC. The second one is based on physical, chemical, or other characteristics of cancer cells. In addition, nanomaterial technology has made high-throughput miniaturization and integration possible in CTC capture [101].
Surface marker-based technology
Following the scientific and commercial success of CellSearch®, improvements have been made on its basis. Numerous EpCAM-based devices have been developed [26, 43, 102], but they are still unable to fix the natural defect only by targeting this specific antigen. To remedy the loss of EMT-CTCs in epithelial tumor or MET-CTCs in mesenchymal tumor, combinatory antibodies such as anti-EpCAM and 84-1 (a monoclonal antibody against cell-surface vimentin) were used successfully to capture CTCs with both epithelial and mesenchymal phenotypes [74, 76]. Similarly, combination of melanoma cell adhesion molecule (MCAM) and EpCAM increased the detection rate of CTCs by 0.5–1-fold in patients with breast cancer undergoing neoadjuvant chemotherapy [103]. Combination of caveolin1 and EpCAM antibodies also led to a significantly higher recovery rate in breast and prostate cancers [39]. The captured EpCAM-negative CTCs were supposed to be EMT-CTCs captured by MCAM antibodies [103]. Barriere et al. suggested that it was imperative to use a combined strategy, for any surface marker-based technology, to target the epithelial, mesenchymal, and epithelial/mesenchymal biphenotypic CTCs [104].
Biology behavior-based technology
CTCs with high invasive capacity or viability were more closely associated with metastasis, and they are particularly paid attention by some investigators. Methods for isolation of invasive or viable CTCs are being developed. Although with slight differences, these methods can generally exclude unwanted CTC using direct behavior assays [46, 105]. Matrigel invasive assays, which are often used for evaluation of capacity in cancer cells, provide natural selection for invasive CTCs. Encouragingly, the presence and enumeration of invasive CTCs detected using this method were found well correlated with metastasis in mouse models and also with disease stage in human patients [106]. Notably, invasive CTC is not equal to mesenchymal CTC or EMT-CTC because a high proportion of invasive CTCs did express CKs [106] or EpCAM [46].
Based on the hypothesis that E-selectin triggers rolling adhension of CTCs, which induce further extravasation, a device using selectin-mediated capture of viable CTCs has also been developed [107]. CTCs with high expression of E-selectin were prone to endothelial adhesion and metastasis formation. Theoretically, every step of tumor metastasis deserves to be elucidated via appropriate models and paralleled subgroups of CTCs [108].
Unbiased technology
ISET platform is currently the most advanced method for unbiased CTC capture. Myriad instruments based on biophysical properties have been reported [29, 109, 110]. Microfilter devices using nylon monofilament or mesh filter [111, 112], polycarbonate filter [113], parylene-C filter [29, 114], polydimethylsiloxane membrane filter [112], tapered-slit membrane filter [115], and two-layer 3D filter [116, 117] were reported to enrich CTCs. Notably, the tapered-slit filter and two-layer microfilters were particularly designed for CTC isolation because of their special structures to protect CTCs from deformation and fluid shear damage [115–117]. A more complicated design included resettable cell traps, which allowed adjustable aperture to prevent clogging [53]. This device had an amazing efficiency of CTC capture, leading to an increase of CTC count by ten times from the same volume of blood samples compared to CellSearch® [53]. Single-cell level in vivo synchrotron X-ray imaging of CTCs is also reported by using gold nanoparticles based on the special electrochemical properties of cancer cells [118]. Biochemical properties of cancer cells such as lactic acid and 5-aminolevulinic acid metabolisms were also used as label-free methods for detection of living CTCs regardless of epithelial or mesenchymal phenotype [47, 119].
Aptamer-based technology is also classified as unbiased method due to its empirical identification of cancer cells without understanding the in-depth mechanism. Both epithelial- and mesenchymal-phenotype CTCs could be captured using aptamer-based devices [120]. Aptamer associated with microporous nanomaterial can raise capture efficiency [120]; however, the microporous scaffold itself is able to capture CTCs as an immune cell-mediated and unbiased way [89].
Novel approaches taking advantage of recent advances in biomicroelectromechanical system and microfabrication are emerging. Acoustophoresis can successfully separate CTCs from white blood cells (WBCs), and the recovery rate by this simple method is as high as 90 % with a contamination rate of only 1–2 %. Optically-induced dielectrophoresis-mediated CTC separation is based on tumor size and electric properties, and is demonstrated to have acceptable recovery rate (∼80 %) and high purity (∼70 %) [121].
The human telomerase activity is upregulated to maintain a suitable length of telomere in cancer cells [122]. Several studies reported the feasibility to identify and capture CTCs from peripheral blood by a green fluorescent protein (GFP)-expressing adenoviral vector in which the telomerase promoter regulates GFP expression [87, 88, 123]. This method could capture CTCs regardless of tumor types and CTC phenotypes and exclude apoptotic CTCs whose telomerase activity was largely inhibited [122].
Subtraction enrichment strategy
Subtraction enrichment by eliminating blood cells via red blood cell lysis and WBC removal is also considered an unbiased strategy for heterogeneous CTC enrichment. CD45 antibody has been used to target and deplete WBCs from the blood of patients. Using various technologies, WBC depletion rate could be as high as 99.99 % [124, 125]. Since this strategy does not touch CTC itself, it is believed to be CTC friendly and can acquire intact CTC. High viability and proliferation ability were found using substraction enrichment strategies [126]. The recovery rate of cancer cells ranged from 50 to 100 %, with a mean of ∼60 % [50, 124]. However, due to the huge amount of WBCs in human blood, even a 99.99 % depletion rate still suggests contamination of thousands of WBCs; thus, the purity of enriched CTCs using subtraction enrichment strategy is usually low. A subsequent highly sensitive detection method is often needed. Taking the advantage of subtraction enrichment strategy, the enriched CTCs are more likely to be qualified for culture and culture-dependent analysis.
Combinatory strategy
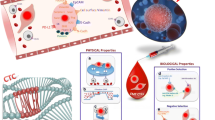
The processes of isolation and identification of CTCs are correlated but can also be independent. There is a variety of strategies using different combinations of current methods for isolation and identification of CTCs (Fig. 1), such as combination of filtration-based isolation and telomerase-based identification [127], anti-CD45 antibody-based negative selection and aptamer-based identification [128], CK-based immunomagnetic selection and miRNA-based identification [77], subtraction enrichment and immunostaining-fluorescence in situ hybridization (FISH) [56].
Novel strategies combining CTC isolation/capture, detection, and subsequent analysis. Generally, four strategies are used to isolate/capture CTCs, such as surface marker-based methods, cell size-based methods, negative selection methods, and other physical property-based methods (left panel). Similarly, at least four CTC detection strategies were introduced, basing on the assessment of cell surface marker, biochemical properties, biological characteristics, and genetic analysis (right panel). Notably, novel materials and microfluidic technologies are used to improve these methods for both enrichment and detection
Regarding isolation itself, platforms based on integrated methods were developed. The famous CTC-iChip, for example, combined three sequential microfluidic technologies including inertial focusing and magnetic separation. CTC-iChip is currently one of the most successful platforms that have been verified by many types of cancers. Notably, it can achieve both antigen-dependent and -independent sorting, making it widely applicable for different purposes [129]. Integrated devices such as combination of microfluidic system-based enrichment and antibody-based capture provide a fast processing speed as high as 10 ml/min. [130] Similarly, a two-stage microfluidic chip eluted WBCs first and could isolate heterogeneous CTCs both antigen positive and negative, such as EpCAM+/EpCAM− or Her2+/Her2− [131].
Future prospect
There is no doubt that CTCs will be used for the next-generation detection of tumors and will benefit more patients. However, current challenges including interpretation of the results limit its clinical practice. In particular, the phenotypic heterogeneity of CTCs related to the mechanisms of metastasis is believed to be the essence of CTC detection. While most types of phenotypes can be tumor-specific, EMT phenotype is common in all kinds of tumors. Decipherment of conundrums underlying EMT phenotype is deemed to make CTC detection accessible in clinics.
References
Krebs MG, Metcalf RL, Carter L, Brady G, Blackhall FH, Dive C. Molecular analysis of circulating tumour cells—biology and biomarkers. Nat Rev Clin Oncol. 2014;11(3):129–44.
Miyamoto DT, Zheng Y, Wittner BS, Lee RJ, Zhu H, Broderick KT, et al. RNA-Seq of single prostate CTCs implicates noncanonical Wnt signaling in antiandrogen resistance. Science. 2015;349(6254):1351–6.
Patel AP, Tirosh I, Trombetta JJ, Shalek AK, Gillespie SM, Wakimoto H, et al. Single-cell RNA-seq highlights intratumoral heterogeneity in primary glioblastoma. Science. 2014;344(6190):1396–401.
Bai X, Zhang Q, Wu S, Zhang X, Wang M, He F, et al. Characteristics of tumor infiltrating lymphocyte and circulating lymphocyte repertoires in pancreatic cancer by the sequencing of T cell receptors. Sci Rep. 2015;5:13664.
Robins HS, Ericson NG, Guenthoer J, O’Briant KC, Tewari M, Drescher CW, et al. Digital genomic quantification of tumor-infiltrating lymphocytes. Sci Transl Med. 2013;5(214), 214ra169.
Aceto N, Bardia A, Miyamoto DT, Donaldson MC, Wittner BS, Spencer JA, et al. Circulating tumor cell clusters are oligoclonal precursors of breast cancer metastasis. Cell. 2014;158(5):1110–22.
Wit S, Dalum G, Lenferink AT, Tibbe AG, Hiltermann TJ, Groen HJ, et al. The detection of EpCAM(+) and EpCAM(−) circulating tumor cells. Sci Rep. 2015;5:12270.
Chen JF, Ho H, Lichterman J, Lu YT, Zhang Y, Garcia MA, et al. Posadas EM. Subclassification of prostate cancer circulating tumor cells by nuclear size reveals very small nuclear circulating tumor cells in patients with visceral metastases. Cancer. 2015;121(18):3240–51.
Yu M, Bardia A, Wittner BS, Stott SL, Smas ME, Ting DT, et al. Circulating breast tumor cells exhibit dynamic changes in epithelial and mesenchymal composition. Science. 2013;339(6119):580–4.
Paoletti C, Li Y, Muniz MC, Kidwell KM, Aung K, Thomas DG, et al. Translational breast cancer research C. Significance of circulating tumor cells in metastatic triple-negative breast cancer patients within a randomized, phase II trial: TBCRC 019. Clin Cancer Res. 2015;21(12):2771–9.
Wallwiener M, Hartkopf AD, Riethdorf S, Nees J, Sprick MR, Schonfisch B, et al. The impact of HER2 phenotype of circulating tumor cells in metastatic breast cancer: a retrospective study in 107 patients. BMC Cancer. 2015;15:403.
Tsuji T, Ibaragi S, Hu GF. Epithelial-mesenchymal transition and cell cooperativity in metastasis. Cancer Res. 2009;69(18):7135–9.
Meng S, Tripathy D, Frenkel EP, Shete S, Naftalis EZ, Huth JF, et al. Circulating tumor cells in patients with breast cancer dormancy. Clin Cancer Res. 2004;10(24):8152–62.
Luzzi KJ, MacDonald IC, Schmidt EE, Kerkvliet N, Morris VL, Chambers AF, et al. Multistep nature of metastatic inefficiency: dormancy of solitary cells after successful extravasation and limited survival of early micrometastases. Am J Pathol. 1998;153(3):865–73.
Giuliano M, Giordano A, Jackson S, Hess KR, De Giorgi U, Mego M, et al. Circulating tumor cells as prognostic and predictive markers in metastatic breast cancer patients receiving first-line systemic treatment. Breast Cancer Res. 2011;13(3):R67.
Scher HI, Heller G, Molina A, Attard G, Danila DC, Jia X, et al. Circulating tumor cell biomarker panel as an individual-level surrogate for survival in metastatic castration-resistant prostate cancer. J Clin Oncol. 2015;33(12):1348–55.
Cohen SJ, Punt CJ, Iannotti N, Saidman BH, Sabbath KD, Gabrail NY, et al. Prognostic significance of circulating tumor cells in patients with metastatic colorectal cancer. Ann Oncol. 2009;20(7):1223–9.
Krebs MG, Sloane R, Priest L, Lancashire L, Hou JM, Greystoke A, et al. Evaluation and prognostic significance of circulating tumor cells in patients with non-small-cell lung cancer. J Clin Oncol. 2011;29(12):1556–63.
Yang JD, Campion MB, Liu MC, Chaiteerakij R, Giama NH, Ahmed Mohammed H, et al. Circulating tumor cells are associated with poor overall survival in patients with cholangiocarcinoma. Hepatology. 2015.
Bonnomet A, Brysse A, Tachsidis A, Waltham M, Thompson EW, Polette M, et al. Epithelial-to-mesenchymal transitions and circulating tumor cells. J Mammary Gland Biol Neoplasia. 2010;15(2):261–73.
Javaid S, Zhang J, Smolen GA, Yu M, Wittner BS, Singh A, et al. MAPK7 regulates EMT features and modulates the generation of CTCs. Mol Cancer Res. 2015;13(5):934–43.
Liotta LA, Kohn E. Anoikis: cancer and the homeless cell. Nature. 2004;430(7003):973–4.
Hou JM, Krebs M, Ward T, Sloane R, Priest L, Hughes A, et al. Circulating tumor cells as a window on metastasis biology in lung cancer. Am J Pathol. 2011;178(3):989–96.
Mehes G, Witt A, Kubista E, Ambros PF. Circulating breast cancer cells are frequently apoptotic. Am J Pathol. 2001;159(1):17–20.
Wu S, Liu S, Liu Z, Huang J, Pu X, Li J, et al. Classification of circulating tumor cells by epithelial-mesenchymal transition markers. PLoS One. 2015;10(4), e0123976.
Raimondi C, Gradilone A, Naso G, Vincenzi B, Petracca A, Nicolazzo C, et al. Epithelial-mesenchymal transition and stemness features in circulating tumor cells from breast cancer patients. Breast Cancer Res Treat. 2011;130(2):449–55.
Agelaki S, Kalykaki A, Markomanolaki H, Papadaki MA, Kallergi G, Hatzidaki D, et al. Efficacy of Lapatinib in therapy-resistant HER2-positive circulating tumor cells in metastatic breast cancer. PLoS One. 2015;10(6), e0123683.
Mazel M, Jacot W, Pantel K, Bartkowiak K, Topart D, Cayrefourcq L, et al. Frequent expression of PD-L1 on circulating breast cancer cells. Mol Oncol. 2015;9(9):1773–82.
Harouaka RA, Zhou MD, Yeh YT, Khan WJ, Das A, Liu X, et al. Flexible micro spring array device for high-throughput enrichment of viable circulating tumor cells. Clin Chem. 2014;60(2):323–33.
Bednarz-Knoll N, Alix-Panabieres C, Pantel K. Plasticity of disseminating cancer cells in patients with epithelial malignancies. Cancer Metastasis Rev. 2012;31(3–4):673–87.
Frisch SM, Schaller M, Cieply B. Mechanisms that link the oncogenic epithelial-mesenchymal transition to suppression of anoikis. J Cell Sci. 2013;126(Pt 1):21–9.
Samatov TR, Tonevitsky AG, Schumacher U. Epithelial-mesenchymal transition: focus on metastatic cascade, alternative splicing, non-coding RNAs and modulating compounds. Mol Cancer. 2013;12(1):107.
Lv Q, Gong L, Zhang T, Ye J, Chai L, Ni C, et al. Prognostic value of circulating tumor cells in metastatic breast cancer: a systemic review and meta-analysis. Clin Transl Oncol. 2015.
Peeters DJ, Van den Eynden GG, van Dam PJ, Prove A, Benoy IH, van Dam PA, et al. Circulating tumour cells in the central and the peripheral venous compartment in patients with metastatic breast cancer. Br J Cancer. 2011;104(9):1472–7.
Ogunwobi OO, Puszyk W, Dong HJ, Liu C. Epigenetic upregulation of HGF and c-Met drives metastasis in hepatocellular carcinoma. PLoS One. 2013;8(5), e63765.
Serrano MJ, Ortega FG, Alvarez-Cubero MJ, Nadal R, Sanchez-Rovira P, Salido M, et al. EMT and EGFR in CTCs cytokeratin negative non-metastatic breast cancer. Oncotarget. 2014;5(17):7486–97.
Stamenkovic I. Matrix metalloproteinases in tumor invasion and metastasis. Semin Cancer Biol. 2000;10(6):415–33.
Mego M, Gao H, Lee BN, Cohen EN, Tin S, Giordano A, et al. Prognostic value of EMT-circulating tumor cells in metastatic breast cancer patients undergoing high-dose chemotherapy with autologous hematopoietic stem cell transplantation. J Cancer. 2012;3:369–80.
Kim YJ, Koo GB, Lee JY, Moon HS, Kim DG, Lee DG, et al. A microchip filter device incorporating slit arrays and 3-D flow for detection of circulating tumor cells using CAV1-EpCAM conjugated microbeads. Biomaterials. 2014;35(26):7501–10.
Denes V, Lakk M, Makarovskiy A, Jakso P, Szappanos S, Graf L, et al. Metastasis blood test by flow cytometry: in vivo cancer spheroids and the role of hypoxia. Int J Cancer. 2015;136(7):1528–36.
Yokobori T, Iinuma H, Shimamura T, Imoto S, Sugimachi K, Ishii H, et al. Plastin3 is a novel marker for circulating tumor cells undergoing the epithelial-mesenchymal transition and is associated with colorectal cancer prognosis. Cancer Res. 2013;73(7):2059–69.
Sieuwerts AM, Kraan J, Bolt J, van der Spoel P, Elstrodt F, Schutte M, et al. Anti-epithelial cell adhesion molecule antibodies and the detection of circulating normal-like breast tumor cells. J Natl Cancer Inst. 2009;101(1):61–6.
Mohamadi RM, Besant JD, Mepham A, Green B, Mahmoudian L, Gibbs T, et al. Nanoparticle-mediated binning and profiling of heterogeneous circulating tumor cell subpopulations. Angew Chem. 2015;54(1):139–43.
Schneck H, Blassl C, Meier-Stiegen F, Neves RP, Janni W, Fehm T, et al. Analysing the mutational status of PIK3CA in circulating tumor cells from metastatic breast cancer patients. Mol Oncol. 2013;7(5):976–86.
Wicha MS, Hayes DF. Circulating tumor cells: not all detected cells are bad and not all bad cells are detected. J Clin Oncol. 2011;29(12):1508–11.
Friedlander TW, Ngo VT, Dong H, Premasekharan G, Weinberg V, Doty S, et al. Detection and characterization of invasive circulating tumor cells derived from men with metastatic castration-resistant prostate cancer. Int J Cancer. 2014;134(10):2284–93.
Matsusaka S, Kozuka M, Takagi H, Ito H, Minowa S, Hirai M, et al. A novel detection strategy for living circulating tumor cells using 5-aminolevulinic acid. Cancer Lett. 2014;355(1):113–20.
Kojic N, Milosevic M, Petrovic D, Isailovic V, Sarioglu AF, Haber DA, et al. A computational study of circulating large tumor cells traversing microvessels. Comput Biol Med. 2015;63:187–95.
Polioudaki H, Agelaki S, Chiotaki R, Politaki E, Mavroudis D, Matikas A, et al. Variable expression levels of keratin and vimentin reveal differential EMT status of circulating tumor cells and correlation with clinical characteristics and outcome of patients with metastatic breast cancer. BMC Cancer. 2015;15:399.
Nel I, Baba HA, Ertle J, Weber F, Sitek B, Eisenacher M, et al. Individual profiling of circulating tumor cell composition and therapeutic outcome in patients with hepatocellular carcinoma. Transl Oncol. 2013;6(4):420–8.
Adams DL, Stefansson S, Haudenschild C, Martin SS, Charpentier M, Chumsri S, et al. Cytometric characterization of circulating tumor cells captured by microfiltration and their correlation to the cellsearch CTC test. Cytometry A. 2015;87(2):137–44.
Welinder C, Jansson B, Lindell G, Wenner J. Cytokeratin 20 improves the detection of circulating tumor cells in patients with colorectal cancer. Cancer Lett. 2015;358(1):43–6.
Qin X, Park S, Duffy SP, Matthews K, Ang RR, Todenhofer T, et al. Size and deformability based separation of circulating tumor cells from castrate resistant prostate cancer patients using resettable cell traps. Lab Chip. 2015;15(10):2278–86.
Kaifi JT, Kunkel M, Das A, Harouaka RA, Dicker DT, Li G, et al. Circulating tumor cell isolation during resection of colorectal cancer lung and liver metastases: a prospective trial with different detection techniques. Cancer Biol Ther. 2015;16(5):699–708.
Lecharpentier A, Vielh P, Perez-Moreno P, Planchard D, Soria JC, Farace F. Detection of circulating tumour cells with a hybrid (epithelial/mesenchymal) phenotype in patients with metastatic non-small cell lung cancer. Br J Cancer. 2011;105(9):1338–41.
Ge F, Zhang H, Wang DD, Li L, Lin PP. Enhanced detection and comprehensive in situ phenotypic characterization of circulating and disseminated heteroploid epithelial and glioma tumor cells. Oncotarget. 2015;6(29):27049–64.
Wang HY, Ahn S, Kim S, Park S, Jung D, Park S, et al. Detection of circulating tumor cell-specific markers in breast cancer patients using the quantitative RT-PCR assay. Int J Clin Oncol. 2015;20(5):878–90.
Lang JE, Scott JH, Wolf DM, Novak P, Punj V, Magbanua MJ, et al. Expression profiling of circulating tumor cells in metastatic breast cancer. Breast Cancer Res Treat. 2015;149(1):121–31.
Wang Z, Cui K, Xue Y, Tong F, Li S. Prognostic value of circulating tumor cells in patients with squamous cell carcinoma of the head and neck: a systematic review and meta-analysis. Med Oncol. 2015;32(5):164.
Fan JL, Yang YF, Yuan CH, Chen H, Wang FB. Circulating tumor cells for predicting the prognostic of patients with hepatocellular carcinoma: a meta analysis. Cell Physiol Biochem. 2015;37(2):629–40.
Han L, Chen W, Zhao Q. Prognostic value of circulating tumor cells in patients with pancreatic cancer: a meta-analysis. Tumour Biol. 2014;35(3):2473–80.
Ma XL, Xiao ZL, Liu L, Liu XX, Nie W, Li P, et al. Meta-analysis of circulating tumor cells as a prognostic marker in lung cancer. Asian Pac J Cancer Prev. 2012;13(4):1137–44.
Zhang L, Riethdorf S, Wu G, Wang T, Yang K, Peng G, et al. Meta-analysis of the prognostic value of circulating tumor cells in breast cancer. Clin Cancer Res. 2012;18(20):5701–10.
Wang FB, Yang XQ, Yang S, Wang BC, Feng MH, Tu JC. A higher number of circulating tumor cells (CTC) in peripheral blood indicates poor prognosis in prostate cancer patients--a meta-analysis. Asian Pac J Cancer Prev. 2011;12(10):2629–35.
Allard WJ, Matera J, Miller MC, Repollet M, Connelly MC, Rao C, et al. Tumor cells circulate in the peripheral blood of all major carcinomas but not in healthy subjects or patients with nonmalignant diseases. Clin Cancer Res. 2004;10(20):6897–904.
Sotelo MJ, Sastre J, Maestro ML, Veganzones S, Vieitez JM, Alonso V, et al. Role of circulating tumor cells as prognostic marker in resected stage III colorectal cancer. Ann Oncol. 2015;26(3):535–41.
Murray NP, Albarran V, Perez G, Villalon R, Ruiz A. Secondary circulating tumor cells (CTCs) but not primary CTCs are associated with the clinico-pathological parameters in Chilean patients with Colo-rectal cancer. Asian Pac J Cancer Prev. 2015;16(11):4745–9.
Pecot CV, Bischoff FZ, Mayer JA, Wong KL, Pham T, Bottsford-Miller J, et al. A novel platform for detection of CK+ and CK- CTCs. Cancer Discov. 2011;1(7):580–6.
Barriere G, Riouallon A, Renaudie J, Tartary M, Rigaud M. Mesenchymal characterization: alternative to simple CTC detection in two clinical trials. Anticancer Res. 2012;32(8):3363–9.
Aktas B, Tewes M, Fehm T, Hauch S, Kimmig R, Kasimir-Bauer S. Stem cell and epithelial-mesenchymal transition markers are frequently overexpressed in circulating tumor cells of metastatic breast cancer patients. Breast Cancer Res. 2009;11(4):R46.
Crespo M, van Dalum G, Ferraldeschi R, Zafeiriou Z, Sideris S, Lorente D, et al. Androgen receptor expression in circulating tumour cells from castration-resistant prostate cancer patients treated with novel endocrine agents. Br J Cancer. 2015;112(7):1166–74.
Juan O, Vidal J, Gisbert R, Munoz J, Macia S, Gomez-Codina J. Prognostic significance of circulating tumor cells in advanced non-small cell lung cancer patients treated with docetaxel and gemcitabine. Clin Transl Oncol. 2014;16(7):637–43.
Satelli A, Mitra A, Brownlee Z, Xia X, Bellister S, Overman MJ, et al. Epithelial-mesenchymal transitioned circulating tumor cells capture for detecting tumor progression. Clin Cancer Res. 2015;21(4):899–906.
Nicolazzo C, Gradilone A. Significance of circulating tumor cells in soft tissue sarcoma. Anal Cell Pathol. 2015;2015:697395.
Raphael J, Massard C, Gong IY, Farace F, Margery J, Billiot F, et al. Detection of circulating tumour cells in peripheral blood of patients with malignant pleural mesothelioma. Cancer Biomark. 2015;15(2):151–6.
Satelli A, Brownlee Z, Mitra A, Meng QH, Li S. Circulating tumor cell enumeration with a combination of epithelial cell adhesion molecule- and cell-surface vimentin-based methods for monitoring breast cancer therapeutic response. Clin Chem. 2015;61(1):259–66.
Ortega FG, Lorente JA, Garcia Puche JL, Ruiz MP, Sanchez-Martin RM, de Miguel-Perez D, et al. miRNA in situ hybridization in circulating tumor cells—MishCTC. Sci Rep. 2015;5:9207.
Ni J, Cozzi P, Hao J, Beretov J, Chang L, Duan W, et al. Epithelial cell adhesion molecule (EpCAM) is associated with prostate cancer metastasis and chemo/radioresistance via the PI3K/Akt/mTOR signaling pathway. Int J Biochem Cell Biol. 2013;45(12):2736–48.
Pal SK, He M, Wilson T, Liu X, Zhang K, Carmichael C, et al. Detection and phenotyping of circulating tumor cells in high-risk localized prostate cancer. Clin Genitourin Cancer. 2015;13(2):130–6.
Liu Z, Fusi A, Klopocki E, Schmittel A, Tinhofer I, Nonnenmacher A, et al. Negative enrichment by immunomagnetic nanobeads for unbiased characterization of circulating tumor cells from peripheral blood of cancer patients. J Transl Med. 2011;9:70.
Sun YF, Xu Y, Yang XR, Guo W, Zhang X, Qiu SJ, et al. Circulating stem cell-like epithelial cell adhesion molecule-positive tumor cells indicate poor prognosis of hepatocellular carcinoma after curative resection. Hepatology. 2013;57(4):1458–68.
Bitting RL, Healy P, Halabi S, George DJ, Goodin M, Armstrong AJ. Clinical phenotypes associated with circulating tumor cell enumeration in metastatic castration-resistant prostate cancer. Urol Oncol. 2015;33(3), 110.e1-9.
Eigl BJ, North S, Winquist E, Finch D, Wood L, Sridhar SS, et al. A phase II study of the HDAC inhibitor SB939 in patients with castration resistant prostate cancer: NCIC clinical trials group study IND195. Investig New Drugs. 2015;33(4):969–76.
Gonzalez-Angulo AM, Lei X, Alvarez RH, Green MC, Murray JL, Valero V, et al. Phase II randomized study of ixabepilone versus observation in patients with significant residual disease after neoadjuvant systemic therapy for HER2-negative breast cancer. Clin Breast Cancer. 2015;15(5):325–31.
Pierga JY, Petit T, Levy C, Ferrero JM, Campone M, Gligorov J, et al. Pathological response and circulating tumor cell count identifies treated HER2+ inflammatory breast cancer patients with excellent prognosis: BEVERLY-2 survival data. Clin Cancer Res. 2015;21(6):1298–304.
Yap TA, Olmos D, Brunetto AT, Tunariu N, Barriuso J, Riisnaes R, et al. Phase I trial of a selective c-MET inhibitor ARQ 197 incorporating proof of mechanism pharmacodynamic studies. J Clin Oncol. 2011;29(10):1271–9.
Shigeyasu K, Tazawa H, Hashimoto Y, Mori Y, Nishizaki M, Kishimoto H, et al. Fluorescence virus-guided capturing system of human colorectal circulating tumour cells for non-invasive companion diagnostics. Gut. 2015;64(4):627–35.
Xu MJ, Cooke M, Steinmetz D, Karakousis G, Saxena D, Bartlett E, et al. A novel approach for the detection and genetic analysis of live melanoma circulating tumor cells. PLoS One. 2015;10(3), e0123376.
Azarin SM, Yi J, Gower RM, Aguado BA, Sullivan ME, Goodman AG, et al. In vivo capture and label-free detection of early metastatic cells. Nat Commun. 2015;6:8094.
Peeters DJ, Brouwer A, Van den Eynden GG, Rutten A, Onstenk W, Sieuwerts AM, et al. Circulating tumour cells and lung microvascular tumour cell retention in patients with metastatic breast and cervical cancer. Cancer Lett. 2015;356(2 Pt B):872–9.
Khoo BL, Lee SC, Kumar P, Tan TZ, Warkiani ME, Ow SG, et al. Short-term expansion of breast circulating cancer cells predicts response to anti-cancer therapy. Oncotarget. 2015;6(17):15578–93.
Cho EH, Wendel M, Luttgen M, Yoshioka C, Marrinucci D, Lazar D, et al. Characterization of circulating tumor cell aggregates identified in patients with epithelial tumors. Phys Biol. 2012;9(1):016001.
Mascalchi M, Falchini M, Maddau C, Salvianti F, Nistri M, Bertelli E, et al. Prevalence and number of circulating tumour cells and microemboli at diagnosis of advanced NSCLC. J Cancer Res Clin Oncol. 2015.
Molnar B, Ladanyi A, Tanko L, Sreter L, Tulassay Z. Circulating tumor cell clusters in the peripheral blood of colorectal cancer patients. Clin Cancer Res. 2001;7(12):4080–5.
Geng Y, Chandrasekaran S, Hsu JW, Gidwani M, Hughes AD, King MR. Phenotypic switch in blood: effects of pro-inflammatory cytokines on breast cancer cell aggregation and adhesion. PLoS One. 2013;8(1), e54959.
Zhang Q, Bai X, Chen W, Ma T, Hu Q, Liang C, et al. Wnt/beta-catenin signaling enhances hypoxia-induced epithelial-mesenchymal transition in hepatocellular carcinoma via crosstalk with hif-1alpha signaling. Carcinogenesis. 2013;34(5):962–73.
De Craene B, Berx G. Regulatory networks defining EMT during cancer initiation and progression. Nat Rev Cancer. 2013;13(2):97–110.
Labelle M, Begum S, Hynes RO. Direct signaling between platelets and cancer cells induces an epithelial-mesenchymal-like transition and promotes metastasis. Cancer Cell. 2011;20(5):576–90.
Sarioglu AF, Aceto N, Kojic N, Donaldson MC, Zeinali M, Hamza B, et al. A microfluidic device for label-free, physical capture of circulating tumor cell clusters. Nat Methods. 2015;12(7):685–91.
Stott SL, Hsu CH, Tsukrov DI, Yu M, Miyamoto DT, Waltman BA, et al. Isolation of circulating tumor cells using a microvortex-generating herringbone-chip. Proc Natl Acad Sci U S A. 2010;107(43):18392–7.
Yoon HJ, Kozminsky M, Nagrath S. Emerging role of nanomaterials in circulating tumor cell isolation and analysis. ACS Nano. 2014;8(3):1995–2017.
Kim S, Han SI, Park MJ, Jeon CW, Joo YD, Choi IH, et al. Circulating tumor cell microseparator based on lateral magnetophoresis and immunomagnetic nanobeads. Anal Chem. 2013;85(5):2779–86.
Onstenk W, Kraan J, Mostert B, Timmermans MM, Charehbili A, Smit VT, et al. Improved circulating tumor cell detection by a combined EpCAM and MCAM cell search enrichment approach in patients with breast cancer undergoing neoadjuvant chemotherapy. Mol Cancer Ther. 2015;14(3):821–7.
Barriere G, Tartary M, Rigaud M. Epithelial mesenchymal transition: a new insight into the detection of circulating tumor cells. ISRN Oncol. 2012;2012:382010.
Pearl ML, Dong H, Tulley S, Zhao Q, Golightly M, Zucker S, et al. Treatment monitoring of patients with epithelial ovarian cancer using invasive circulating tumor cells (iCTCs). Gynecol Oncol. 2015;137(2):229–38.
Wang H, Hara Y, Liu X, Reuben JM, Xie Y, Xu H, et al. Detection and enumeration of circulating tumor cells based on their invasive property. Oncotarget. 2015;6(29):27304–11.
Mitchell MJ, Castellanos CA, King MR. Immobilized surfactant-nanotube complexes support selectin-mediated capture of viable circulating tumor cells in the absence of capture antibodies. J Biomed Mater Res A. 2015;103(10):3407–18.
Alix-Panabieres C, Pantel K. Challenges in circulating tumour cell research. Nat Rev Cancer. 2014;14(9):623–31.
Low WS, Wan Abas WA. Benchtop technologies for circulating tumor cells separation based on biophysical properties. BioMed Res Int. 2015;2015:239362.
Harouaka RA, Nisic M, Zheng SY. Circulating tumor cell enrichment based on physical properties. J Lab Autom. 2013;18(6):455–68.
Rye PD, Hoifodt HK, Overli GE, Fodstad O. Immunobead filtration: a novel approach for the isolation and propagation of tumor cells. Am J Pathol. 1997;150(1):99–106.
Fan X, Jia C, Yang J, Li G, Mao H, Jin Q, et al. A microfluidic chip integrated with a high-density PDMS-based microfiltration membrane for rapid isolation and detection of circulating tumor cells. Biosens Bioelectron. 2015;71:380–6.
Vona G, Sabile A, Louha M, Sitruk V, Romana S, Schutze K, et al. Isolation by size of epithelial tumor cells: a new method for the immunomorphological and molecular characterization of circulatingtumor cells. Am J Pathol. 2000;156(1):57–63.
Zheng S, Lin H, Liu JQ, Balic M, Datar R, Cote RJ, et al. Membrane microfilter device for selective capture, electrolysis and genomic analysis of human circulating tumor cells. J Chromatogr A. 2007;1162(2):154–61.
Kang YT, Doh I, Cho YH. Tapered-slit membrane filters for high-throughput viable circulating tumor cell isolation. Biomed Microdevices. 2015;17(2):45.
Zheng S, Lin HK, Lu B, Williams A, Datar R, Cote RJ, et al. 3D microfilter device for viable circulating tumor cell (CTC) enrichment from blood. Biomed Microdevices. 2011;13(1):203–13.
Lee SW, Hyun KA, Kim SI, Kang JY, Jung HI. Continuous enrichment of circulating tumor cells using a microfluidic lateral flow filtration chip. J Chromatogr A. 2015;1377:100–5.
Jung SY, Ahn S, Seo E, Lee SJ. Detection of circulating tumor cells via an X-ray imaging technique. J Synchrotron Radiat. 2013;20(Pt 2):324–31.
Chiu TK, Lei KF, Hsieh CH, Hsiao HB, Wang HM, Wu MH. Development of a microfluidic-based optical sensing device for label-free detection of circulating tumor cells (CTCs) through their lactic acid metabolism. Sensors. 2015;15(3):6789–806.
Viraka Nellore BP, Kanchanapally R, Pramanik A, Sinha SS, Chavva SR, Hamme 2nd A, et al. Aptamer-conjugated graphene oxide membranes for highly efficient capture and accurate identification of multiple types of circulating tumor cells. Bioconjug Chem. 2015;26(2):235–42.
Huang SB, Wu MH, Lin YH, Hsieh CH, Yang CL, Lin HC, et al. High-purity and label-free isolation of circulating tumor cells (CTCs) in a microfluidic platform by using optically-induced-dielectrophoretic (ODEP) force. Lab Chip. 2013;13(7):1371–83.
Shay JW, Zou Y, Hiyama E, Wright WE. Telomerase and cancer. Hum Mol Genet. 2001;10(7):677–85.
Dorsey JF, Kao GD, MacArthur KM, Ju M, Steinmetz D, Wileyto EP, et al. Tracking viable circulating tumor cells (CTCs) in the peripheral blood of non-small cell lung cancer (NSCLC) patients undergoing definitive radiation therapy: pilot study results. Cancer. 2015;121(1):139–49.
Dieguez L, Winter MA, Pocock KJ, Bremmell KE, Thierry B. Efficient microfluidic negative enrichment of circulating tumor cells in blood using roughened PDMS. Analyst. 2015;140(10):3565–72.
Hyun KA, Lee TY, Jung HI. Negative enrichment of circulating tumor cells using a geometrically activated surface interaction chip. Anal Chem. 2013;85(9):4439–45.
Lu Y, Liang H, Yu T, Xie J, Chen S, Dong H, et al. Isolation and characterization of living circulating tumor cells in patients by immunomagnetic negative enrichment coupled with flow cytometry. Cancer. 2015;121(17):3036–45.
Ma Y, Hao S, Wang S, Zhao Y, Lim B, Lei M, et al. A combinatory strategy for detection of live CTCs using microfiltration and a new telomerase-selective adenovirus. Mol Cancer Ther. 2015;14(3):835–43.
Zhang J, Li S, Liu F, Zhou L, Shao N, Zhao X. SELEX aptamer used as a probe to detect circulating tumor cells in peripheral blood of pancreatic cancer patients. PLoS One. 2015;10(3), e0121920.
Ozkumur E, Shah AM, Ciciliano JC, Emmink BL, Miyamoto DT, Brachtel E, et al. Inertial focusing for tumor antigen-dependent and -independent sorting of rare circulating tumor cells. Sci Transl Med. 2013;5(179), 179ra147.
Liu Z, Zhang W, Huang F, Feng H, Shu W, Xu X, et al. High throughput capture of circulating tumor cells using an integrated microfluidic system. Biosens Bioelectron. 2013;47:113–9.
Hyun KA, Lee TY, Lee SH, Jung HI. Two-stage microfluidic chip for selective isolation of circulating tumor cells (CTCs). Biosens Bioelectron. 2015;67:86–92.
Acknowledgments
This work was financially supported by the National Natural Science Foundation of China (No. 81401954) and the Medical Science & Technology Program of Zhejiang Province, China (2015KYA114). We appreciate Dr. Ziduo Li from ANZAC Research Institute, University of Sydney, Australia for help of search and full-text paper acquisition.
Author contributions
Hong Y and Zhang Q wrote the manuscript. Both authors approved the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Hong, Y., Zhang, Q. Phenotype of circulating tumor cell: face-off between epithelial and mesenchymal masks. Tumor Biol. 37, 5663–5674 (2016). https://doi.org/10.1007/s13277-016-4796-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-016-4796-5