Abstract
Renal cell carcinoma is among the leading causes of cancer-related death and was found to induce IL-10. We started by focusing on IL-10-secreting cells in tumor-infiltrating lymphocytes in renal cell carcinoma patients and observed that both CD3+ T cells and CD19+ B cells contributed to an elevated IL-10 expression. We then focused on IL-10-expressing B cells, and found that compared to non-IL-10-producing B cells, the IL-10-expressing B cells had significantly lower levels of CD19 and CD20 expression, a lack of IgM and IgD expression, while the level of CD27 was elevated. Moreover, culturing under unstimulated conditions resulted in higher antibody production by these IL-10-producing B cells than their peripheral blood counterparts, which strongly suggested that they are plasmablast-differentiating cells. Both IgA and IgG subtypes were found but IgA had a higher relative abundance in the tumor-infiltrating fraction. We then observed inverse correlations between the frequency of IL-10-producing B cells and pro-inflammatory cytokine-producing T cells and T cell proliferation. The expression of T cell exhaustion marker Tim-3, however, was upregulated in patients with high frequencies of IL-10-producing B cells. Moreover, supernatant from tumor B cells suppressed T cell inflammation. In addition, frequencies of IL-10-producing tumor-infiltrating B cells were inversely correlated with resected tumor size, and were higher in later stage tumors. Together, our data demonstrated that IL-10-producing B cells had plasmablast-differentiating phenotype, and could contribute to T cell immunosuppression in renal cell carcinoma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Renal cell carcinoma is among the top 10 leading causes of cancer-related deaths with a rising incidence worldwide [1–3]. Metastasis is present in one third of patients initially and will develop in another third within 10 years. Moreover, metastatic renal cell carcinoma is resistant to radiotherapy and systemic therapy, resulting in the extremely low 5-year survival rate of about 5 % in metastatic cancers [4, 5]. New mechanistic studies on the initiation, development and treatment of renal cell carcinoma are urgently needed. Although immunotherapies using tumor-specific T cells have been intensively investigated, their applications and efficacy are limited by a variety of tumor-mediated immunosuppression mechanisms [6, 7]. Tumor cells can escape immune surveillance by elevating FasL expression and downregulating Fas, which are involved in the killing of tumor-infiltrating lymphocytes (TILs) [8, 9]. Elevated levels of anti-inflammatory cytokines, including TGF-beta and IL-10, were discovered in freshly isolated tumor cells and were shown to mediate inhibition of tumor-eradicating immunity and escape from immune surveillance [8, 10–12]. Renal cell carcinoma in particular was found to induce IL-10 [13]. More studies are needed to examine the regulatory mechanisms in the tumor microenvironment.
Regulatory B cell (Breg) is an increasingly studied B cell subtype that was found to contribute to the suppression of anti-tumor immunity. Studies in murine models have found that unlike B cell knockout mice, wild-type mice were unable to reject and eliminate irradiated tumor cells due to a lack of robust IFN-gamma secretion by cytotoxic T cells and NK cells, an effect that is dependent on CD40-CD154 interaction [14, 15]. The presence of B cells was also found to correlate with increased regulatory T cell (Treg) expansion in wild-type mice that failed to inhibit tumor growth [16]. In other human diseases and animal models, Breg cells were found to mediate immune suppression through production of IL-10, an immunoregulatory cytokine that potentially suppresses T cell inflammation, promotes Treg cell expansion, and protects tissue integrity by preventing excessive inflammation [17, 18]. In the context of renal cancer initiation and progression, the participation of B cells is unclear, but several other kidney diseases involved aberrant B cell responses, including IgA nephropathy, acute kidney injury, and renal interstitial inflammation [19–21]. In addition, IgA and/or IgM depositions were found in tumors and glomeruli of renal cell carcinoma patients in several studies, with unknown implications on disease progression [22–24]. While these studies implicated a potential role of B cell participation in kidney cancer, no direct evidence is present on whether B cell-mediated inflammation and/or immune suppression have a role in renal cell carcinoma.
In this study, we first examined the intratumoral environment in freshly isolated renal tumors. Both intratumoral IL-10-secreting B cells and T cells were found, with elevated abundance in tumor compared to in autologous peripheral blood. Interestingly, comparing to non-IL-10-producing B cells, the IL-10-expressing B cells had significantly lower CD19 and CD20 and higher CD27 expression, did not present surface IgM and IgD, and were found to produce higher levels of IgA and IgG antibodies directly ex vivo, strongly suggesting a plasmablast differentiation. We then observed that the frequency of IL-10-producing B cells had a negative correlation with autologous T cell pro-inflammatory cytokine production and proliferation, and a positive correlation with Tim-3 expression in tumor-infiltrating T cells. Moreover, compared to that from circulating B cells, supernatant from tumor B cells directly suppressed T cell inflammation. In renal cell carcinoma patients, frequencies of IL-10-producing tumor-infiltrating B cells were positively correlated with resected tumor size and were higher in later stage tumors. Together, our data described a tumor-infiltrating population of IL-10-producing B cells that contained IgG and IgA-secreting cells and could contribute to immunosuppression in renal cell carcinoma.
Materials and methods
Clinical samples
Demographic and clinical patient information was summarized in Table 1. Exclusion criteria included use of chemotherapy, radiotherapy, or biological therapy one month prior to surgery, concurrent corticosteroids, or other immunosuppressive medications, hepatitis B infection, type II diabetes, and clinically significant autoimmune disease. Tumor tissues were obtained from renal cell carcinoma patients. Possible normal tissues attached to resected tumor were carefully separated and not included in the study. Peripheral blood specimen was collected from patients one day before surgery. Fresh tumor specimens were processed by sterile mechanical dissection, enzymatic digestion, and centrifuged through a sucrose gradient as described previously [25]. The resulting buffy coat layer was identified as tumor-infiltrating lymphocytes, washed and either used immediately or cryopreserved in −80 °C until use. Peripheral blood lymphocytes were obtained by Ficoll centrifugation and cryopreserved in −80 °C until use. The study was conducted according to the principles expressed in the Declaration of Helsinki. All protocols were approved by the Ethics Board of Changhai Hospital, Second Military Medical University and written informed consent was obtained from all patients.
Cell culture
Culture media were prepared as RPMI 1640 supplemented with 10 % fetal bovine serum, Pen Strep, and L-glutamine (Life Technologies), with additional stimulants in some cultures in an experiment-specific way. Cell culture condition was 37 °C 5 % CO2, unless otherwise specified.
Flow cytometry
All antibodies, including CD3, CD10, CD19, CD20, CD21, CD24, CD27, CD34, IgM, IgD, IFN-gamma, TNF-alpha, and IL-10, were purchased from BD and the manufacturer’s recommended concentrations were used. Isotype-matching antibodies were used as controls for gating. The general surface staining protocol included first washing cells in PBS supplemented with 2 % fetal bovine serum, adding surface antibodies and incubating for 30 min in 4 °C, and then washing cells twice and proceeding to flow cytometry analysis by BD LSRFortessa. For intracellular staining, cells were incubated in CytoFix/CytoPerm (BD) for 15 min in 4 °C, washed once with Perm/Wash (BD), and incubated with intracellular antibodies for 30 min in 4 °C. Cells were then washed twice and sent for flow cytometry analysis. For circulating lymphocytes, greater than 106 events were collected and analyzed. For tumor-infiltrating lymphocytes, greater than 105 events were collected and analyzed.
Cell isolation
Circulating or tumor-infiltrating B cells and T cells were negatively isolated using B cell or pan T isolation kits (Miltenyi) following the manufacturer’s protocol. Briefly, total peripheral blood mononuclear cells or tumor-infiltrating lymphocytes were treated with mouse-anti-human antibody cocktails that did not bind to B cells or T cells, followed by anti-mouse Ig magnetic beads. The non-B or non-T cells were then pulled away from the mixture by magnets, leaving B cells or T cells intact. The assays were repeated twice for improved purity.
ELISAs
Cells were cultured for 72 h at 5 × 104 cells per 100 μl of culture media in a round bottom 96-well plate. Plates were spun at 300g for 5 min and 75 μl of supernatant per well were carefully removed. IL-10 was measured by Human IL-10 ELISA Kit (Life Technologies) following the manufacturer’s instructions. Sensitivity was <3 pg/ml. For IgG and IgA detection, Human total IgG and IgA ELISA Kits (eBioscience) were used and the detection limit was 1.6 and 1.5 ng/ml, respectively.
T cell proliferation and pro-inflammatory cytokine measurement
T cells were labeled with CFSE and cultured in normal culture media, supernatant from circulating B cells, or supernatant from tumor-infiltrating B cells for 5 days. Anti-human CD3 and anti-human CD28 monoclonal antibodies were added at 2.5 μg/ml in media. Twelve hours before the end of incubation, GolgiStop/GolgiPlug (BD) was added to the cell culture to retain secreted cytokine. Cells were then harvested and stained for flow cytometry analyses. B cell supernatant was obtained by culturing 105 purified circulating or tumor-infiltrating B cells per 1 ml culture media for 5 days in a 24-well plate, after which the cells were centrifuged at 300g for 5 min and the supernatant was carefully taken and stored at −80 °C.
Statistical analysis
All statistical analyses were performed in Prism 6 software (GraphPad). For comparison between two groups, unequal variances t tests were used. For comparisons between two different conditions in the same individual, paired t tests were used. Shapiro-Wilk normality test was used to confirm normal distribution. The Pearson correlation coefficient was calculated for correlation between two variables. Two-tailed P < 0.05 was considered statistically significant.
Results
IL-10-producing cells in resected tumor
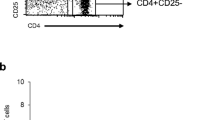
To examine the intratumoral environment, we obtained freshly resected tumors from renal cell carcinoma patients. The demographic and clinical characteristics of study subjects are summarized in Table 1. Flow cytometry analysis demonstrated that IL-10-producing cells were found in both T cell (CD3+) and B cell (CD19+) compartments of circulating lymphocytes and tumor-infiltrating lymphocytes (Fig. 1a, b). The relative distribution of IL-10+ cells in the T cell, B cell, or other (non-T non-B) cell compartments varied by patient (Fig. 1c, d), but the relative contribution of IL-10 by B cells was higher in the tumor-infiltrating fraction compared to the circulating fraction (Fig. 1e). We also examined the percentage of IL-10+ cells in total lymphocytes, T cells and B cells, and found that tumor-infiltrating lymphocytes had significantly upregulated IL-10+ cells compared to their peripheral blood counterparts (Fig. 1f). No significant correlation between the frequencies of peripheral blood IL-10+ cells and tumor-infiltrating IL-10+ cells were found, either in total lymphocytes (Fig. 1g) or in T cells and B cells (data not shown).
IL-10-producing cells were shifted toward the B cell fraction in the tumor compared to the blood. Blood lymphocytes or tumor-infiltrating lymphocytes were stained with anti-human CD3, CD19 on surface and with anti-human IL-10 intra-cellularly. Data were obtained by flow cytometry and were analyzed by unequal variances t tests and Pearson’s correlation. n.s. not significant. a, b First panel shows the gating of IL-10+ cells in lymphocytes. Second panel shows the expression of CD3/CD19 by IL-10+ cells (black dots) against all lymphocytes (gray dots). Numbers in the second panel indicate the percentage of all lymphocytes (gray dots) in each quadrant. c, d Distribution of IL-10+ cells in lymphocyte subsets that were CD3+ only, CD19+ only, or neither, representing T cell, B cell, or other cell subsets, respectively, in each individual. e Summary of the percentage of IL-10+ cells that were T cells, B cells or other, in all individuals in circulating compared to tumor-infiltrating lymphocytes. f Percentage of total lymphocytes, T cells, or B cells that were IL-10+ in the blood and tumor. g Correlation between blood lymphocytes and tumor lymphocytes in the frequencies of IL-10+ cells
ELISA experiments were performed on the supernatant from lymphocytes cultured ex vivo. Tumor-infiltrating lymphocytes secreted significantly higher IL-10 than their peripheral blood counterparts (Fig. 2a). Notably, circulating B cells from several patients had no detectable IL-10 production, while B cells isolated from tumor had detectable IL-10 secretion in all patients. Also, the relative contribution of IL-10 from B cells, as a ratio of IL-10 by B cells to IL-10 by T cells, is significantly elevated in tumor, compared to that in the peripheral blood (Fig. 2b).
IL-10 secretion is elevated in tumor B cells compared to blood B cells. Total lymphocytes, isolated T cells or B cells were cultured ex vivo for 72 h, at 5 × 104 cells per 100 μl of media. The concentration of IL-10 was measured by ELISA and analyzed by unequal variances t test. a Concentration of supernatant IL-10 in total lymphocyte, T cell and B cell cultures. b Relative IL-10 secretion by B cells, calculated by the amount of IL-10 in B cell culture divided by that in autologous T cell culture
Together, these data demonstrated that IL-10-expressing tumor-infiltrating T cells and B cells were present at higher frequencies in tumor than in peripheral blood. Interestingly, IL-10 secretion is more biased toward the B cell compartment in tumor compared to peripheral blood.
Phenotyping of IL-10-producing B cells in resected tumor
The role of regulatory T cells and T cell-mediated IL-10 secretion has been studied previously [25–27], while few data is available for the characterization of tumor-infiltrating B cells. Moreover, B cell-mediated suppression was seen to inhibit the induction of T cell-dependent anti-tumor immunity and autoimmunity through IL-10 secretion [28]. In humans, B cells that produce IL-10 and exhibited regulatory activity were found to be CD24hi CD38hi [30, 31], a phenotype previously associated with a group of immature-transitional B cells [32–34]. To allow further characterization and functional analysis, we examined the phenotype of IL-10-expressing B cells in tumor-infiltrating lymphocytes. We found that these B cells had lower CD19 and CD20 expression and higher CD27 expression than non-IL-10-expressing B cells, and were IgD-negative and IgM-negative. Unlike Breg cells in other studies, we did not find that these B cells were particularly high in CD24 and CD38 (Fig. 3a) [29, 30]. These features resembled antibody-producing plasmablasts. Overall, compared to IL-10− B cells, the phenotype of IL-10+ B cells in tumor is characterized by low CD19, CD20, CD38, IgD and IgM and high CD21 and CD27 (Fig. 3b), which resembled most closely to plasmablasts in surface marker expression.
IL-10-expressing B cells most closely resembled differentiating plasmablasts. Tumor-infiltrating cells were cultured with GolgiStop/GolgiPlug for 12 h, stained with surface antibodies, and then stained intra-cellularly with anti-IL-10 antibody. a Representative surface marker expression of IL-10+ B cells (black line) in comparison with IL-10− B cells (gray line and fill). Shown are gated on CD3−CD19+ B cells. b: Collection of surface phenotype in IL-10+ B cells compared to IL-10− B cells. N = 5. Mean fluorescence intensity (MFI) was shown
Antibody production by tumor-infiltrating B cells
Although IL-10 is primarily an immunosuppressive cytokine, in human B cells, IL-10 also promotes plasma cell differentiation [31, 32]. Secreted IgG and IgA were detected in the supernatant of tumor-infiltrating B cells without stimulation, and were present in higher concentration than that in the supernatant of autologous blood B cells (Fig. 4a). The relative concentration of IgA as a fraction of total adaptive antibodies (IgG + IgA), in particular, was significantly increased in tumor compared to blood (Fig. 4b), demonstrating a shift in secreted antibody isotype composition in tumor compared to peripheral blood.
Tumor-infiltrating B cells secreted higher levels of antibodies than circulating B cells ex vivo. Purified B cells from blood or tumor were cultured ex vivo for 72 h, at 5 × 104 cells per 100 μl of media. IgG and IgA in the supernatant was measured by ELISA and then analyzed by paired t test. For control over potential contamination from antibodies in the serum, IgG and IgG ELISAs were also performed on autologous pure T cell cultures to be measured as the background level, which was already subtracted away in the presented data. a Antibody secretion in circulating B cells compared to tumor-infiltrating B cells. b Relative concentration of IgA, calculated as the concentration of IgA divided by the sum of the concentrations of IgG and IgA in each subject
Immunosuppressive function of tumor IL-10-producing B cells
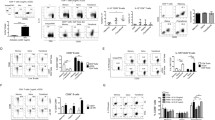
Next, we wondered whether these IL-10-producing B cells had an immunosuppressive function. Tumor-infiltrating cells were stimulated by anti-CD3/CD28. We found that the frequency of IL-10+ cells in tumor-infiltrating B cells is inversely correlated with the frequency of IFN-gamma- and TNF-alpha-producing tumor-infiltrating T cells, and proliferated T cells (CFSElo) after TCR stimulation (Fig. 5a). Interestingly, the T cell exhaustion marker Tim-3 is upregulated in patients with high frequencies of IL-10+ tumor-infiltrating B cells (Fig. 5b, c). This may reflect the possibility that some patients have a more anti-inflammatory intratumoral environment, resulting in higher IL-10-producing cells together with lower tumor T cell inflammation or that tumor B cells could directly suppress de novo T cell inflammation. To examine the latter possibility, and given that higher IL-10 production was observed in tumor B cells compared to blood B cells (Fig. 2), we obtained culture supernatant from purified peripheral blood B cells and that from tumor-infiltrating B cells. We then cultured autologous peripheral blood T cells with supernatant from the blood B cell culture or with supernatant from the tumor B cell culture. T cells cultured with tumor-infiltrating B cell supernatant had significantly reduced IFN-gamma production and T cell proliferation, compared to those cultured with blood B cell supernatant (Fig. 5d), demonstrating that soluble factors, from tumor-infiltrating B cell culture, possessed immunosuppressive function (see “Discussion”).
Increased frequencies of IL-10+ B cells in tumor-infiltrating cells were associated with suppressed pro-inflammatory cytokine expression by T cells and reduced T cell proliferation. a Correlations between the frequencies of IFN-gamma+, TNF-alpha+, or CFSElo tumor-infiltrating T cells and the frequencies of IL-10+ tumor-infiltrating B cells in each individual. Tumor-infiltrating cells were first stained CFSE and then cultured with anti-CD3/CD28 antibodies in normal culture media for 5 days. 12 h prior to end of culturing, GolgiStop/GolgiPlug was added to cells for cytokine retention. Cells were then stained by surface and intracellular antibodies, and processed by flow cytometry. Data were analyzed by Pearson’s Correlation. b Representative staining of Tim-3 on tumor-infiltrating T cells. c Correlation between the frequencies of Tim-3+ tumor-infiltrating T cells and the frequencies of IL-10+ tumor-infiltrating B cells in each individual. Data were analyzed by Pearson’s Correlation. d The frequencies of IFN-gamma+, TNF-alpha+, or CFSElo T cells when purified peripheral blood T cells were stimulated by anti-CD3/CD28 and cultured in supernatant obtained from purified blood B cells, or from purified tumor-infiltrating B cells. Normalized data were shown to account for individual differences and were analyzed by paired t test. 105 purified blood B cells or tumor B cells from each patient were cultured for 6 days in 1 ml of media. The supernatant were then collected and used for T cell cultures
Correlation with disease
T cell-mediated inflammation is thought to mediate anti-tumor immunity and can be utilized for potential cancer immunotherapies. Since the frequencies of IL-10-producing tumor-infiltrating B cells were inversely correlated with T cell pro-inflammatory cytokine production and proliferation, we then examined whether IL-10 production by B cells is associated with disease severity. We found that the frequency of IL-10-producing B cells was positively correlated with resected tumor size (Fig. 6a). Moreover, stage III + stage IV tumors contained significantly higher frequencies of IL-10-producing B cells than stage I + stage II tumors (Fig. 6b). This difference was not due to sex differences between the stage I and stage II group and the stage III + stage IV group, since no significant differences in the frequencies of tumor-infiltrating IL-10-producing B cells were observed between male patients and female patients (Fig. 6c).
Frequencies of IL-10+ cells in tumor-infiltrating B cells were correlated with disease progression. Pearson correlation test and unequal variances t test. a Correlation between the frequencies of IL-10+ cells in tumor-infiltrating B cells and the size of resected tumors. b The frequencies of IL-10+ tumor-infiltrating B cells in stages I + II patients, compared to that in stages III + IV patients. c The frequencies of IL-10+ tumor-infiltrating B cells in male vs. female patients
Discussion
In this study, we started by focusing on IL-10-producing cells in tumor-infiltrating lymphocytes, given that tumor-infiltrating lymphocyte responses had been associated with prognostic values and therapeutic values in various cancers [33]. Since IL-10 is one of the immunosuppressive cytokines that were induced in renal cell carcinoma and was found to contribute to continued tumor persistence [13, 34, 35], we first examined the IL-10 production by tumor-infiltrating lymphocytes. Both CD3+ T cells and CD19+ B cells were found to secrete IL-10, but interestingly, although T cells in general secreted higher levels of IL-10, both in peripheral blood and in tumors, IL-10 production by B cells was relatively increased in tumors, both in terms of the frequencies of IL-10+ cells by flow cytometry ex vivo and the concentration of secreted by ELISA in vitro. Surface marker examination suggested that these IL-10+ B cells possessed a plasmablast-like phenotype, and were negative for IgD and IgM. Moreover, tumor-infiltrating B cell cultures contained higher secreted IgG and IgA antibodies than autologous blood B cell cultures, suggesting higher plasmablast activity in tumor B cells. Negative correlations between the frequencies of IL-10+ cells in tumor-infiltrating B cells and the level of tumor-infiltrating T cell inflammation, in terms of IFN-gamma and TNF-alpha secretion and proliferation, were found. On the other hand, Tim-3 expression was upregulated in patients with higher frequencies of IL-10-producing tumor-infiltrating B cells. Moreover, supernatant from tumor-infiltrating B cell suppressed autologous blood T cell inflammation, demonstrating the existence of immunosuppressive activity in tumor-infiltrating B cell culture.
Overall, our experiments characterized a group of plasmablast-like B cells in renal cell carcinoma and demonstrated a potential in vivo immunosuppressive activity of these B cells. In a previous study, depletion of normal peripheral blood B cells with rituximab in metastatic renal cell carcinoma patients, in conjunction with IL-2 therapy, did not change IL-2-induced expansion of IFN-gamma-producing T cells in vitro [36]. This study by Aklilu et al., however, has a number of differences from our study. First, our population had low CD19 and CD20 expression, which may not be depleted by their anti-CD20 rituximab treatment. Second, the depletion of normal B cells in their study was confirmed in peripheral blood while the number of tumor-infiltrating plasmablast-like cells was unknown in these patients. Indeed, normal levels of circulating Ig after rituximab treatment was maintained over the course of their study (18 weeks), suggesting a preservation of plasma cells and/or plasmablasts. And third, the T cell stimulant was PMA + ionomycin in their study and anti-CD3/CD28 in ours, which signals through the TCR complex and may better represent physiological conditions.
Based on the evidence presented in this study, it is difficult to tell at this moment whether these plasmablast-like IL-10-producing cells were the same as canonical plasmablasts or represented a special subset of plasmablasts. During the preparation of this manuscript, Matsumoto et al. reported that murine CD138+CD44+ plasmablasts predominantly expressed IL-10 after experimental autoimmune encephalomyelitis (EAE) activation, and was shown to inhibit dendritic cell function to generate autoimmune T cells [37]. Here, we showed that the tumor-infiltrating B cell culture as a whole had IgG and IgA secretion ex vivo not requiring stimulation, suggesting that tumor B cells contained antibody-secreting plasmablasts. Interestingly, a relative increase in secreted IgA was observed in tumor B cell culture compared to that in blood. Whether these cells might contribute to IgA nephropathy in conjunction with renal cell carcinoma would require further examinations [22, 24, 38].
We also observed an association between higher frequencies of IL-10+ cells in tumor-infiltrating B cells and larger tumor size and disease stage. While it is likely that IL-10+ B cells could promote cancer development and/or inhibit anti-tumor immunity in vivo, we cannot rule out the possibility that larger tumors physically allowed more infiltrating IL-10+ B cells to enter and stay than smaller tumors, and later stage patients had larger tumor sizes in our study cohort (Table 1). One way to examine this possibility is to monitor tumor growth over time and associate IL-10-producing tumor-infiltrating cells with the rate of tumor progression. While this is clinically unfeasible and ethically not permissible, animal models may be employed in future studies.
References
Vogelzang NJ, Stadler WM. Kidney cancer. Lancet. 1998;352:1691–6.
Rini BI, Campbell SC, Escudier B. Renal cell carcinoma. Lancet. 2009;373:1119–32.
Wallen EM, Pruthi RS, Joyce GF, Wise M. Kidney cancer. J Urol. 2007;177:2006–18. discussion 2018–9.
Motzer RJ, Hutson TE, McCann L, Deen K, Choueiri TK. Overall survival in renal-cell carcinoma with pazopanib versus sunitinib. N Engl J Med. 2014;370:1769–70.
Motzer RJ, Russo P. Systemic therapy for renal cell carcinoma. J Urol. 2000;163:408–17.
Finke J, Ferrone S, Frey A, Mufson A, Ochoa A. Where have all the T cells gone? Mechanisms of immune evasion by tumors. Immunol Today. 1999;158–60.
Wang RF, Zeng G, Johnston SF, Voo K, Ying H. T cell-mediated immune responses in melanoma: implications for immunotherapy. Crit Rev Oncol Hematol. 2002;1–11.
Kim R, Emi M, Tanabe K, Uchida Y, Toge T. The role of Fas ligand and transforming growth factor beta in tumor progression: molecular mechanisms of immune privilege via Fas-mediated apoptosis and potential targets for cancer therapy. Cancer. 2004;100:2281–91.
Rabinowich H, Reichert TE, Kashii Y, Gastman BR, Bell MC, Whiteside TL. Lymphocyte apoptosis induced by Fas ligand- expressing ovarian carcinoma cells. Implications for altered expression of T cell receptor in tumor-associated lymphocytes. J Clin Invest. 1998;101:2579–88.
Heckel MC, Wolfson A, Slachta CA, Schwarting R, Salgame P, Katsetos CD, et al. Human breast tumor cells express IL-10 and IL-12p40 transcripts and proteins, but do not produce IL-12p70. Cell Immunol. 2011;266:143–53.
Mumm JB, Emmerich J, Zhang X, Chan I, Wu L, Mauze S, et al. IL-10 Elicits IFNγ-dependent tumor immune surveillance. Cancer Cell. 2011;20:781–96.
Jovasevic VM, Gorelik L, Bluestone JA, Mokyr MB. Importance of IL-10 for CTLA-4-mediated inhibition of tumor-eradicating immunity. J Immunol. 2004;172:1449–54.
Ménétrier-Caux C, Bain C, Favrot MC, Duc A, Blay JY. Renal cell carcinoma induces interleukin 10 and prostaglandin E2 production by monocytes. Br J Cancer. 1999;79:119–30.
Inoue S, Leitner WW, Golding B, Scott D. Inhibitory effects of B cells on antitumor immunity. Cancer Res. 2006;66:7741–7.
Shah S, Divekar AA, Hilchey SP, Cho HM, Newman CL, Shin SU, et al. Increased rejection of primary tumors in mice lacking B cells: inhibition of anti-tumor CTL and TH1 cytokine responses by B cells. Int J Cancer. 2005;117:574–86.
Tadmor T, Zhang Y, Cho HM, Podack ER, Rosenblatt JD. The absence of B lymphocytes reduces the number and function of T-regulatory cells and enhances the anti-tumor response in a murine tumor model. Cancer Immunol Immunother. 2011;60:609–19.
Mauri C, Bosma A. Immune regulatory function of B cells. Annu Rev Immunol. 2012;30:221–41.
Ouyang W, Rutz S, Crellin NK, Valdez PA, Hymowitz SG. Regulation and functions of the IL-10 family of cytokines in inflammation and disease. Annu Rev Immunol. 2011;29:71–109.
Jang HR, Gandolfo MT, Ko GJ, Satpute SR, Racusen L, Rabb H. B cells limit repair after ischemic acute kidney injury. J Am Soc Nephrol. 2010;21:654–65.
Ascon DB, Lopez-Briones S, Liu M, Ascon M, Savransky V, Colvin RB, et al. Phenotypic and functional characterization of kidney-infiltrating lymphocytes in renal ischemia reperfusion injury. J Immunol Am Assoc Immunol. 2006;177:3380–7.
Heller F, Lindenmeyer MT, Cohen CD, Brandt U, Draganovici D, Fischereder M, et al. The contribution of B cells to renal interstitial inflammation. Am J Pathol. 2007;170:457–68.
Mimura I, Tojo A, Kinugasa S, Uozaki H, Fujita T. Renal cell carcinoma in association with IgA nephropathy in the elderly. Am J Med Sci. 2009;338:431–2.
Corven CB, Khalaf A, Courville P, Sibert L, Gobet F, Joly P. Renal chromophobe cell carcinoma and paraneoplastic linear IgA bullous dermatosis. J Urol Elsevier. 2003;169:270–1.
Magyarlaki T, Kiss B, Buzogány I, Fazekas A, Sükösd F, Nagy J. Renal cell carcinoma and paraneoplastic IgA nephropathy. Nephron Karger Publ. 1999;82:127–30.
Siddiqui SA, Frigola X, Bonne-Annee S, Mercader M, Kuntz SM, Krambeck AE, et al. Tumor-infiltrating Foxp3-CD4+CD25+ T cells predict poor survival in renal cell carcinoma. Clin Cancer Res. 2007;13:2075–81.
Curiel TJ. Tregs and rethinking cancer immunotherapy. J Clin Invest Am Soc Clin Investig. 2007;117:1167–74.
Desar IME, Jacobs JHFM, Hulsbergen-vandeKaa CA, Oyen WJG, Mulders PFA, van der Graaf WTA, et al. Sorafenib reduces the percentage of tumour infiltrating regulatory T cells in renal cell carcinoma patients. Int J Cancer. 2011;129:507–12.
Qin Z, Richter G, Schuler T, Ibe S, Cao X, Blankenstein T. B cells inhibit induction of T cell-dependent tumor immunity. Nat Med. 1998;4:627–30.
Yanaba K, Bouaziz J-D, Haas KM, Poe JC, Fujimoto M, Tedder TF. A regulatory B cell subset with a unique CD1dhiCD5+ phenotype controls T cell-dependent inflammatory responses. Immunity. 2008;28:639–50.
Blair PA, Noreña LY, Flores-Borja F, Rawlings DJ, Isenberg DA, Ehrenstein MR, et al. CD19+ CD24hi CD38hi B cells exhibit regulatory capacity in healthy individuals but are functionally impaired in systemic Lupus Erythematosus patients. Immunity. 2010;32:129–40.
Arpin C, Dechanet J, Van Kooten C, Merville P, Grouard G, Briere F, et al. Generation of memory B cells and plasma cells in vitro. Science (80-.). 1995;720–2.
Crotty S. Follicular helper CD4 T cells (TFH). Annu Rev Immunol. 2011;29:621–63.
Gooden MJM, de Bock GH, Leffers N, Daemen T, Nijman HW. The prognostic influence of tumour-infiltrating lymphocytes in cancer: a systematic review with meta-analysis. Br J Cancer Cancer Res UK. 2011;105:93–103.
Sato T, Terai M, Tamura Y, Alexeev V, Mastrangelo MJ, Selvan SR. Interleukin 10 in the tumor microenvironment: a target for anticancer immunotherapy. Immunol Res. 2011;51:170–82.
Ruffell B, Chang-Strachan D, Chan V, Rosenbusch A, Ho CMT, Pryer N, et al. Macrophage IL-10 blocks CD8+ T cell-dependent responses to chemotherapy by suppressing IL-12 expression in intratumoral dendritic cells. Cancer Cell Elsevier. 2014;26:623–37.
Aklilu M, Stadler WM, Markiewicz M, Vogelzang NJ, Mahowald M, Johnson M, et al. Depletion of normal B cells with rituximab as an adjunct to IL-2 therapy for renal cell carcinoma and melanoma. Ann Oncol. 2004;15:1109–14.
Matsumoto M, Baba A, Yokota T, Nishikawa H, Ohkawa Y, Kayama H, et al. Interleukin-10-producing plasmablasts exert regulatory function in autoimmune inflammation. Immun Elsevier Inc. 2014;41:1040–51.
Sessa A, Volpi A, Tetta C, Meroni M, Torri Tarelli L, Battini G, et al. IgA mesangial nephropathy associated with renal cell carcinoma. Appl Pathol. 1989;7:188–91.
Acknowledgments
This work is supported by the National Natural Science Foundation of China (No.: 81202019).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflicts of interests
None
Additional information
Chen Cai and Jin Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Cai, C., Zhang, J., Li, M. et al. Interleukin 10-expressing B cells inhibit tumor-infiltrating T cell function and correlate with T cell Tim-3 expression in renal cell carcinoma. Tumor Biol. 37, 8209–8218 (2016). https://doi.org/10.1007/s13277-015-4687-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-4687-1