Abstract
Official guidelines group together all cases of solitary hepatocellular carcinoma (HCC) without macroscopic vascular invasion, regardless of tumor size. Here, we examined whether this is justified based on overall survival (OS) after hepatic resection (HR). Patients with newly diagnosed solitary HCC treated by initial HR from January 2004 to October 2013 were classified into six groups based on tumor size (in 2-cm increments). Combining adjacent categories with similar OS led to three groups: ≤5 cm (n = 426), >5 and ≤8 cm (n = 229), and >8 cm (n = 202). Among all patients, median survival time was 62 months, and OS was 95 % at 1 year, 73 % at 3 years, and 54 % at 5 years. Patients in the ≤5 cm group showed significantly higher OS (P < 0.001) and lower tumor recurrence (P = 0.004) than those in the >5 and ≤8 cm group, who in turn showed significantly higher OS (P = 0.003) and lower tumor recurrence (P = 0.021) than those in the >8 cm group. Our results suggest that patients with solitary HCC should be subclassified based on tumor size for more accurate prognosis. We propose defining solitary HCC tumors >5 and ≤8 cm as “large” and tumors >8 cm as “huge”.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Hepatocellular carcinoma (HCC) is the third leading cause of cancer-related death worldwide [1], and it remains a diagnostic and treatment challenge for many surgeons despite improvements in screening and surgical techniques [2]. Hepatic resection (HR) is widely regarded as the first-line treatment for selected patients with HCC. Prognosis after HR depends on tumor stage, functional status of remnant liver, and general health.
Patients with similar hepatitis or cirrhosis status can present with tumors of quite different sizes. The latest version of the American Joint Committee on Cancer Tumor-Node-Metastasis staging system classifies as T1 all cases of solitary HCC without vascular invasion, regardless of size. The Barcelona Clinic Liver Cancer group recommends that all cases of solitary HCC >5 cm be grouped into the same stage [3, 4]. In general, HCC >5 cm is called big tumor [5] while ≥10 cm as huge tumor [6]. Size is not generally considered a factor in deciding whether a patient can undergo HR [5, 7], as long as the tumor has not metastasized or given rise to size-related symptoms. [3] Indeed, tumor size by itself is not contraindication for HR [5, 7].
This may not be consistent with the best available clinical evidence, since tumor size ranks together with tumor number, vascular invasion, and extrahepatic metastasis as a significant risk factor of poor prognosis in HCC patients [8, 9]. Multivariate analyses in large studies have shown tumor size >5 [10], >7 [11], >8 [12], and ≥10 cm [13, 14] to be independent predictors of death after HR. These findings call into question the appropriateness of classifying all cases of solitary HCC into the same prognostic group.
The present study examined whether patients with solitary HCC of different sizes differed significantly in long-term overall survival (OS) after HR, which would suggest the need for subclassification based on size.
Methods
Patients
This study was designed in accordance with the Declaration of Helsinki, and it was approved by the Affiliated Tumor Hospital of Guangxi Medical University. Medical records that had been entered prospectively into the central database of the Affiliated Tumor Hospital after admission were examined retrospectively to identify patients who underwent initial, potentially curative HR for primary solitary HCC between January 2004 and October 2013 at the Affiliated Tumor Hospital. Curative resection was defined as resection involving a tumor-free surgical margin, no residual tumor detected by imaging, and serum α-fetoprotein (AFP) levels that returned to normal within 1 month. Diagnosis of HCC was confirmed by postoperative pathological examination.
Patients were excluded from the study if they underwent palliative hepatectomy, if they had a mixed HCC-cholangiocarcinoma tumor, or if they presented with one or more of the following features: preoperative tumor rupture, macroscopic vascular invasion, and tumor metastasis to the lymph nodes and/or adjacent or distant organs. Patients who received preoperative transarterial chemoembolization or portal vein embolization were also excluded.
Study design
To examine possible subclassification of solitary HCC using an unbiased method as possible, we initially divided the patients into six groups based on tumor size: ≤2,>2 and ≤4, >4 and ≤6, >6 and ≤8, >8 and <10, and ≥10 cm. We planned to combine adjacent groups if they had similar OS.
Preoperative evaluation and treatment
Routine preoperative evaluation for HCC diagnosis included serum AFP assay, B ultrasound, abdomen and chest computed tomography, magnetic resonance imaging, and upper gastrointestinal endoscopy. Liver function was analyzed using a conventional test. Indocyanine green retention rate at 15 min was not determined for any patients.
All patients were initially evaluated for the possibility of HR unless the patient requested another treatment modality [14–16]. Indications for deciding whether to use HR to treat HCC have been described [15–17]. Anatomic HR was preferred to nonanatomical HR. Major hepatectomy was defined as resection of ≥3 segments; minor hepatectomy, as resection of ≤2 segments.
Follow-up and treatment for HCC recurrence
Follow-up for all patients began immediately after resection until death or March 2015. In principle, patients were followed up every 1–3 months during the first year after HR, and every 3–6 months thereafter. Follow-up visits comprised regular clinical examination, blood tests, and abdominal imaging. Serum AFP level and hepatitis B viral load were monitored before and after resection.
In patients found to have recurrent HCC, resection was repeated if judged feasible based on liver function and remnant liver volume [18]. If resection was not feasible, then transarterial chemoembolization, radiofrequency ablation, percutaneous ethanol injection, radiotherapy, or other palliative therapies were applied. Patients treated in our hospital after 2008 received postoperative antiviral therapy with nucleos(t)ide analogue if their serum contained ≥2000 IU/mL hepatitis B virus DNA [19].
Statistical analysis
The primary endpoint of this study was OS, which was calculated starting from the date of admission until death, last follow-up or March 2015, whichever occurred earliest. Data for categorical variables were expressed as number (%), and intergroup differences were compared using the chi-squared or Fisher’s exact tests (2-tailed) as appropriate. Continuous data were expressed as mean ± standard deviation (SD) or as median (range), and intergroup differences were compared using the t test or Mann-Whitney U test. Survival curves were estimated using the Kaplan-Meier method and compared using the log-rank test. Multivariate analysis to identify independent prognostic factors was carried out using a Cox proportional hazards model. A two-tailed P value < 0.05 was considered as the threshold of significance. All statistical analyses were performed using SPSS 19.0 (IBM, USA).
Results
Characteristics and perioperative outcomes of the entire study population
Of the 1613 patients with primary HCC admitted for the first time to our hospital and treated with initial, potentially curative HR during the nearly 10-year study period, 857 were included based on the inclusion and exclusion criteria (Table 1). Most were male (85.8 %), and their mean age was 49.0 years (SD 11.2). Most had hepatitis B virus (HBV) infection (777, 90.7 %) at the time of the study. Only 294 (34.3 %) had AFP levels ≥400 ng/mL. Most patients had Child-Pugh A liver function (95.0 %), and a substantial proportion had cirrhosis (70.9 %). Just over half of patients (59.4 %) had a complete tumor capsule. Mean tumor diameter was 6.3 cm (SD 3.6).
Only 94 patients (11.0 %) underwent major hepatectomy. Median blood loss was 250 mL, and 234 patients (27.3 %) experienced postoperative complications during follow-up. Three patients (0.4 %) died within 30 days after HR due to serious postoperative complications: one died due to sepsis, and the other two due to hepatic failure. Ten patients (1.2 %) died within 90 days after HR.
Overall survival of six initial groups based on tumor size
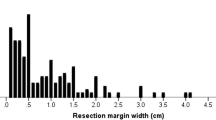
Among all 857 patients, median survival time was 62 months, and OS was 95 % at 1 year, 73 % at 3 years, and 54 % at 5 years. All patients were classified into one of six groups based on tumor size limits differing in 2-cm intervals. In general, OS decreased with increasing tumor diameter (Fig. 1). Median survival time (in months) across groups with the smallest to largest tumors was 62, 83, 64, 56, 43, and 45. OS was similar between the ≤2 cm group and >2 and ≤4 cm group at 1 year (98 vs. 97 %), 3 years (82 vs. 83 %), and 5 years (60 vs. 63 %) (P = 0.411; Fig. 2a). OS was significantly higher in the >2 and ≤4 cm group than in the >4 and ≤6 cm group at all three time points (P = 0.040; Fig. 2b), with the latter group showing rates of 97 % at 1 year, 75 % at 3 years, and 58 % at 5 years. OS in the >6 and ≤8 cm group (97, 75, and 58 %) was similar to that in the >4 and ≤6 cm group (P = 0.131; Fig. 2c) but greater than that in the >8 and <10 cm group (P = 0.060; Fig. 2d). OS was similar in the >8 and <10 cm group and in the ≥10 cm group (P = 0.816; Fig. 2e): 85 vs. 90 %, 55 vs. 56 %, and 39 vs. 41 %.
Pairwise comparisons of overall survival curves between groups of patients with solitary HCC following hepatic resection, classified by tumor size. a ≤2 cm group vs. >2 and ≤4 cm group (P = 0.411). b >2 and ≤4 cm group vs. > 4 and ≤6 cm group (P = 0.040). c >4 and ≤6 cm group vs. > 6 and ≤8 cm group (P = 0.131). d >6 and ≤8 cm group vs. > 8 and <10 cm group (P = 0.060). e >8 and <10 cm group vs. ≥10 cm group (P = 0.816)
Redefinition of tumor size groups and their characteristics and perioperative outcomes
Based on similar OS, the ≤2 cm group was combined with the >2 and ≤4 cm group to form a new ≤4 cm category, and the >8 and <10 cm group was combined with the ≥10 cm group to form a new >8 cm category. Given the similar OS between the >4 and ≤6 cm group and the >6 and ≤8 cm group and the controversial cutoff of 5 cm as the boundary between “small” and “large” tumors [20–22], we reclassified patients into three new categories: ≤5 cm (n = 426), >5 and ≤8 cm (n = 229), and > 8 cm (n = 202). Comparison of clinical features among these three groups (Table 2) showed that increasing tumor size was associated with increasing platelet count, volume of blood loss, and rates of the following: AFP ≥ 400 ng/mL, major hepatectomy, postoperative complications, and 30- and 90-day mortality.
Overall survival of the three new groups
During follow-up until March 2015, 469 patients (54.7 %) experienced HCC recurrence, of which 372 (79.3 %) experienced intrahepatic recurrence. The rate of recurrence was significantly higher among patients in the >8 cm group (69.3 %) than among patients in the >5 and ≤8 cm group (58.1 %) or the ≤5 cm group (46.0 %; all P < 0.05). Patients in the >5 and ≤8 cm group experienced a significantly higher rate of recurrence than those in the ≤5 cm group (P = 0.004). Rates of any recurrence and of extrahepatic recurrence increased with tumor size (Table 3).
Median survival time (in months) was 76 in the ≤5 cm group, 56 in the >5 and ≤8 cm group, and 44 in the >8 cm group. OS was significantly higher among patients in the ≤5 cm group than among those in the >5 and ≤8 cm group (P < 0.001; Fig. 3) at all three time points: 97 vs. 95 % at 1 year, 81 vs. 72 % at 3 years, and 63 vs. 49 % at 5 years. OS was significantly higher in the >5 and ≤8 cm group than in the >8 cm group (P = 0.003; Fig. 3); OS in the latter group was 89 % at 1 year, 56 % at 3 years, and 40 % at 5 years.
Comparison of overall survival curves among three groups of patients with solitary HCC following hepatic resection. These groups were formed by combining adjacent groups in Fig. 1 that showed similar OS
Discussion
Numerous studies suggest that large tumor size is a significant risk factor of poor OS in patients with HCC after HR [10–15, 23], but some studies have not replicated these findings [2, 24, 25]. As a result, although some studies suggest that tumor size >5 cm is associated with significantly lower OS and higher tumor recurrence [10, 23], official guidelines still classify all cases of solitary HCC without macrovascular invasion in the same group, regardless of tumor size [4, 7]. In addition, the definition of so-called large (>5 cm) and huge (≥10 cm) HCC, which many clinicians use to guide treatment and management, remains controversial [20–22]. Here, we provide further evidence that tumor size is a significant predictor of OS and tumor recurrence, and that patients with solitary HCC should be subclassified according to tumor size (≤5, >5 and ≤8, and >8 cm). Our results suggest that large tumors should be defined as >5 cm and ≤8 cm and huge tumors as >8 cm.
Our data contradict the recommendations of the Barcelona Clinic Liver Cancer group to assign all cases of solitary HCC into a single stage [3, 4, 7]. We observed comparable 30- and 90-day mortality between patients with a solitary large (>5 and ≤8 cm) or huge tumor (>8 cm) and patients with a solitary small tumor (≤5 cm). These findings are consistent with other large studies suggesting that HR can be safe and effective in patients with solitary large or huge HCC [5, 6]. Therefore, we recommend HR as a safe and effective treatment for such patients, provided that liver functional reserve and residual remnant liver are sufficient [14, 15].
Previous work has associated remnant liver volume and reserve liver function with risk of liver failure after HR [26]. In fact, liver failure is the main cause of perioperative mortality [27]. Since patients with larger tumors are more likely to undergo major hepatectomy [28, 29], they are at higher risk of postoperative liver failure. Similarly, we found in the present work that patients with larger tumors were more likely to undergo major hepatectomy, lost greater volumes of blood, and experienced higher rates of perioperative mortality and postoperative complications. In contrast to trends in the literature, however, only 2 of 857 patients (0.2 %) died of liver failure within 30 days after HR, and rates of 30- and 90-day mortality were only 0.4 and 1.2 %. These results further emphasize the safety of HR in patients with large and huge tumors, consistent with a systematic review involving more than 15,000 patients [27].
Nearly all adjacent groups in our initial set of six showed similar OS, especially patients with a tumor ≤2 cm or a tumor >2 and ≤4 cm and patients with a tumor >8 and <10 cm or a tumor ≥10 cm. This may reflect the fact that our study population was consecutive, relatively large, and suitable for potentially curative HR. This raises the question of whether our findings can be generalized to patients with macroscopic vascular invasion or tumor metastasis before surgery. Further studies are also needed to determine whether our results are valid for patient populations with lower incidence of HBV infection.
Our analysis revealed similarities and discrepancies from the literature on what patient clinicopathologic characteristics are associated with poor OS. One study correlated low preoperative platelet count with poor OS [30]. In the present study, however, preoperative platelet counts were significantly higher among patients with larger tumor size. AFP is one of the most widely used tumor markers for detecting and monitoring HCC, and we found a positive correlation between AFP levels and tumor size, consistent with previous work [31, 32], including studies from our own group showing AFP ≥400 ng/mL to be an indicator of poor prognosis [13–16]. At the same time, our data do not support the positive correlations previously reported between tumor size and presence of cirrhosis, esophagogastric varices, or complete tumor capsule [2, 24]. Though the rate of HCC recurrence is increasing with the enlargement of tumor size, postoperative or adjuvant therapies may be useful to prolong OS [33, 34].
This study was designed to provide reliable conclusions in order to guide clinical practice. Similar studies in the literature [23, 35] focused on single pairwise comparisons between tumor size groups, such that the sample size for each comparison was the entire study population. In the present work, in contrast, we simultaneously compared several tumor size groups, such that the sample size of each comparison was smaller than the total population. In addition, we initially defined groups to span the entire range of observed tumor sizes, in 2-cm increments. Then we refined the groups based on OS analysis, and our groups spanned the controversial cutoff of 5 cm widely used to differentiate small and large HCC.
The present study provides strong evidence that tumor size correlates negatively with OS and positively with tumor recurrence among patients with solitary HCC. OS analysis suggests that these patients should be subclassified based on tumor size as follows: ≤5, >5 and ≤8, and >8 cm. Our results further support a growing literature demonstrating the safety and efficacy of HR for patients with large and even huge HCC tumors. These findings should be verified and extended in large, rigorously designed studies on patient populations of other ethnicities and disease backgrounds. In addition, the median follow-up period of further studies should be longer than 5 years because some included patients in this study were followed up for fewer than 5 years.
Abbreviations
- AFP:
-
α-fetoprotein
- HCC:
-
Hepatocellular carcinoma
- HR:
-
Hepatic resection
- OS:
-
Overall survival
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65(2):87–108.
Yang LY, Fang F, Ou DP, Wu W, Zeng ZJ, Wu F. Solitary large hepatocellular carcinoma: a specific subtype of hepatocellular carcinoma with good outcome after hepatic resection. Ann Surg. 2009;249(1):118–23.
Bruix J, Gores GJ, Mazzaferro V. Hepatocellular carcinoma: clinical frontiers and perspectives. Gut. 2014;63(5):844–55.
Bruix J, Llovet JM. Prognostic prediction and treatment strategy in hepatocellular carcinoma. Hepatology. 2002;35(3):519–24.
Torzilli G, Belghiti J, Kokudo N, et al. A snapshot of the effective indications and results of surgery for hepatocellular carcinoma in tertiary referral centers: is it adherent to the EASL/AASLD recommendations?: an observational study of the HCC East-west study group. Ann Surg. 2013;257(5):929–37.
Chen XP, Qiu FZ, Wu ZD, Zhang BX. Chinese experience with hepatectomy for huge hepatocellular carcinoma. Br J Surg. 2004;91(3):322–6.
Zhong JH, Ke Y, Wang YY, Li LQ. Liver resection for patients with hepatocellular carcinoma and macrovascular invasion, multiple tumours, or portal hypertension. Gut. 2015;64(3):520–1.
European Association for Study of Liver, European Organisation for Research and Treatment of Cancer. EASL-EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol. 2012;56(4):908–43.
Yau T, Tang VY, Yao TJ, Fan ST, Lo CM, Poon RT. Development of Hong Kong liver cancer staging system with treatment stratification for patients with hepatocellular carcinoma. Gastroenterology. 2014;146(7):1691–700. e1693.
Vauthey JN, Lauwers GY, Esnaola NF, et al. Simplified staging for hepatocellular carcinoma. J Clin Oncol. 2002;20(6):1527–36.
Hsu CY, Hsia CY, Huang YH, et al. Comparison of surgical resection and transarterial chemoembolization for hepatocellular carcinoma beyond the Milan criteria: a propensity score analysis. Ann Surg Oncol. 2012;19(3):842–9.
Truant S, Boleslawski E, Duhamel A, et al. Tumor size of hepatocellular carcinoma in noncirrhotic liver: a controversial predictive factor for outcome after resection. Eur J Surg Oncol. 2012;38(12):1189–96.
Yuan BH, Yuan WP, Li RH, et al. Propensity score-based comparison of hepatic resection and transarterial chemoembolization for patients with advanced hepatocellular carcinoma. Tumour Biol. 2015. doi:10.1007/s13277-015-4091-x.
Zhong JH, You XM, Lu SD, et al. Historical comparison of overall survival after hepatic resection for patients with large and/or multinodular hepatocellular carcinoma. Medicine (Baltimore). 2015;94(35), e1426.
Zhong JH, Ke Y, Gong WF, et al. Hepatic resection associated with good survival for selected patients with intermediate and advanced-stage hepatocellular carcinoma. Ann Surg. 2014;260(2):329–40.
Zhong JH, Xiang BD, Gong WF, et al. Comparison of long-term survival of patients with BCLC stage B hepatocellular carcinoma after liver resection or transarterial chemoembolization. PLoS One. 2013;8(7), e68193.
Zhong JH, Ke Y, Wang YY, et al. Comparative efficacy of hepatic resection or transarterial chemoembolization for treating intermediate- and advanced-stage hepatocellular carcinoma. Chin J of Oncol Prev and Treat. 2014;6(12):363–70.
Xiang BD, Li LQ, Zhao YN, Liu JY, Yuan WP. Prognostic factors of patients with recurrent hepatocellular carcinoma after re-excision. Chin J Clin Oncol. 2010;37(17):994–7.
Ke Y, Ma L, You XM, et al. Antiviral therapy for hepatitis B virus-related hepatocellular carcinoma after radical hepatectomy. Cancer Biol Med. 2013;10(3):158–64.
Torzilli G, Belghiti J, Kokudo N, et al. Reply to letter: “a snapshot of the effective indications and results of surgery for hepatocellular carcinoma in tertiary referral centers: Is it adherent to the EASL/AASLD recommendations? an observational study of the HCC East-west study group”: when the study setting “ignores” the patients. Ann Surg. 2015;262(1):e30–1.
Bruix J, Fuster J. A snapshot of the effective indications and results of surgery for hepatocellular carcinoma in tertiary referral centers: is it adherent to the EASL/AASLD recommendations?: an observational study of the HCC East-west study group. Ann Surg. 2015;262(1), e30.
Zhong JH, Lu SD, Wang YY, Ma L, Li LQ. Intermediate-stage HCC—upfront resection can be feasible. Nat Rev Clin Oncol. 2015;12(5):295.
Hwang S, Lee YJ, Kim KH, et al. The impact of tumor size on long-term survival outcomes after resection of solitary hepatocellular carcinoma: single-institution experience with 2558 patients. J Gastrointest Surg. 2015;19(7):1281–90.
Cho YB, Lee KU, Lee HW, et al. Outcomes of hepatic resection for a single large hepatocellular carcinoma. World J Surg. 2007;31(4):795–801.
Jung YK, Jung CH, Seo YS, et al. BCLC stage B is a better designation for single large hepatocellular carcinoma than BCLC stage A. J Gastroenterol Hepatol. 2015. doi:10.1111/jgh.13152.
Truant S, Boleslawski E, Sergent G, et al. Liver function following extended hepatectomy can be accurately predicted using remnant liver volume to body weight ratio. World J Surg. 2015;39(5):1193–201.
Zhong JH, Rodriguez AC, Ke Y, Wang YY, Wang L, Li LQ. Hepatic resection as a safe and effective treatment for hepatocellular carcinoma involving a single large tumor, multiple tumors, or macrovascular invasion. Medicine (Baltimore). 2015;94(3), e396.
Poon RT, Fan ST, Wong J. Selection criteria for hepatic resection in patients with large hepatocellular carcinoma larger than 10 cm in diameter. J Am Coll Surg. 2002;194(5):592–602.
Hanazaki K, Kajikawa S, Shimozawa N, et al. Hepatic resection for large hepatocellular carcinoma. Am J Surg. 2001;181(4):347–53.
Pang Q, Qu K, Zhang JY, et al. The prognostic value of platelet count in patients with hepatocellular carcinoma: a systematic review and meta-analysis. Medicine (Baltimore). 2015;94(37), e1431.
An SL, Xiao T, Wang LM, et al. Prognostic significance of preoperative serum alpha-fetoprotein in hepatocellular carcinoma and correlation with clinicopathological factors: a single-center experience from China. Asian Pac J Cancer Prev. 2015;16(10):4421–7.
Hsu CY, Liu PH, Lee YH, et al. Using serum alpha-fetoprotein for prognostic prediction in patients with hepatocellular carcinoma: what is the most optimal cutoff? PLoS One. 2015;10(3), e0118825.
Zhong JH, Zhong QL, Li LQ, Li H. Adjuvant and chemopreventive therapies for resectable hepatocellular carcinoma: a literature review. Tumour Biol. 2014;35(10):9459–68.
Zhong JH, Ma L, Li LQ. Postoperative therapy options for hepatocellular carcinoma. Scand J Gastroenterol. 2014;49(6):649–61.
Zhang H, Yuan SX, Dai SY, et al. Tumor size does not independently affect long-term survival after curative resection of solitary hepatocellular carcinoma without macroscopic vascular invasion. World J Surg. 2014;38(4):947–57.
Acknowledgments
This work was supported by Guangxi Science and Technology Development Projects (14124003–4), a National Science and Technology Major Special Project (2012ZX10002010001009), a Guangxi University of Science and Technology Research Project (KY2015LX056), the Self-Raised Scientific Research Fund of the Ministry of Health of Guangxi Province (Z2015621, Z2015601, GZZC15-34, Z2014241), an Innovation Project of Guangxi Graduate Education (YCBZ2015030), and the Youth Science Foundation of Guangxi Medical University (GXMUYSF201302).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics Approval
This study was designed in accordance with the Declaration of Helsinki, and it was approved by the Affiliated Tumor Hospital of Guangxi Medical University.
Conflicts of interest
None
Additional information
Lei Liu, Qi-Shun Zhang and Ling-Hui Pan contributed equally to this work.
Rights and permissions
About this article
Cite this article
Liu, L., Zhang, QS., Pan, LH. et al. Subclassification of patients with solitary hepatocellular carcinoma based on post-hepatectomy survival: a large retrospective study. Tumor Biol. 37, 5327–5335 (2016). https://doi.org/10.1007/s13277-015-4387-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-4387-x