Abstract
This study was aimed to determine whether hypocalcemic analogs of active forms of vitamins D modulate expression of genes related to stem-like phenotype in colon cancer cell lines HT-29 and HCT-116 undergoing renewal after the treatment with 5-fluorouracil (5-FU). Both lines express vitamin D receptor, but differ in differentiation stage and vitamin D sensitivity. Cells that resisted the 5-FU exposure were treated with synthetic analog of 1,25-dihydroxyvitamin D2 (PRI-1906) and analogs of 1,25-dihydroxyvitamin D3 (PRI-2191 and PRI-2205). Proliferative activity was more profoundly affected by vitamin D analogs in HT-29/5-FU than in HCT-116/5-FU cells. In HT-29/5-FU cells, analogs PRI-1906 and PRI-2191 downregulated the expression of genes related to survival, re-growth, and invasiveness during renewal, while PRI-2205 increased expression of genes related to differentiation only. In HCT-116/5-FU cells, PRI-2191 decreased the expression of stemness- and angiogenesis-related genes, whereas PRI-1906 augmented their expression. The effects in HCT-116/5-FU cells were observed at higher concentrations of the analogs than those used for HT-29/5-FU cells. Out of the series of analogs studied, PRI-2191 might be used to counteract the renewal of both moderately and poorly differentiated cancer cells following conventional treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Colorectal cancer is the third most frequently diagnosed malignancy worldwide and the second cause of cancer-related deaths [1–4]. 5-Fluorouracil/leucovorin combined with oxaliplatin (FOLFOX) and irinotecan (FOLFIRI) chemotherapy regimens for colorectal carcinoma patients often fail to eradicate advanced tumor. It is assumed that cancer stem cells (CSC)/tumor-initiating cells (TIC) are relatively the most resistant ones to conventional treatment. A proportion of CSC/TIC with self-renewal ability and high potential of forming metastases may be increased among cells which resisted conventional chemotherapy [5–7]. New therapeutic strategies are to be developed to target both rapidly dividing differentiated cancer cells and CSC/TIC to prevent tumor recurrence initiated by CSC/TIC.
The experimental therapies developed so far in animal models combined cytoreductive treatment with the use of various natural dietary substances, such as retinoic acid, curcumin, sulforaphane, soy isoflavone, resveratrol, lycopene, piperine, and vitamin D [8–11], which modulate cell proliferation, migration, apoptosis, and differentiation by targeting self-renewal signaling pathways Wnt/β-catenin, Hedgehog, and Notch. These substances were used to sensitize tumor cells to chemotherapeutics and/or to induce tumor cell differentiation and inhibit self-renewal signaling [8, 12, 13].
Some clinical observations and experiments on animals strongly suggest that vitamin D might prevent cancer development [14, 15]. A protective role of vitamin D against cancer results from the increase of differentiation, the inhibition of proliferation, and the induction of apoptosis. A direct antitumor activity of calcitriol, the active form of vitamin D3, is observed at high hypercalcemic doses [16]. In the experimental settings, we and others have demonstrated that the combined treatment of cancer with vitamin D analogs and cytostatics was more effective than the treatment with cytostatics alone both in vitro [17–24] and in vivo [20–24], but some combined treatment schedules could lead to increased toxicity. It is a matter of debate whether vitamin D analogs should be administered prior or/and simultaneously with cytostatics to sensitize tumor cells to cytoreductive effects of cytostatics or sequentially to counteract tumor re-growth. Because of the antiproliferative effect of vitamin D, cancer cells rendered by vitamin D or analogs to the resting state may become more resistant to treatment with cytostatics targeting rapidly dividing cells. Vitamin D3 analogs prevent cancer cells from entering S-phase of the cell cycle by blocking the cell cycle at the G1/S transition [23, 24]. The simultaneous treatment of colon cancer cells with vitamin D analogs and cytostatic in vitro led to a decrease in the percentage of cell deaths [24]. We investigated whether low-calcemic synthetic analogs of vitamin D interfere with the renewal of colon cancer cells which resisted treatment with 5-FU. Since the anti-proliferative and pro-differentiating effects of vitamin D depend mostly on the differentiation status and the cancer cell type [25], we studied both moderately and poorly differentiated colon cancer cell lines.
Materials and methods
Drugs and analogs
5-Fluorouracil (5-FU, Ebewe Pharma, Vienna, Austria) solution was diluted in culture medium shortly before using, and added to cell culture at a concentration of 6 μg/ml (46 μM).
Analog PRI-1906 [(24E)-24a-homo-(1S)-1,25-dihydroxyvitamin D2] and analogs PRI- 2191 [(24R)-1,24-dihydroxyvitamin D3, tacalcitol) and PRI-2205, (5E,7E) isomer of calcipotriol, were synthesized at Pharmaceutical Research Institute, Warsaw, Poland [26, 27]. Samples of analogs, dried down in amber ampoules, were dissolved in ethanol (99,8 %) to obtain 200 μM stock solution. The solution was stored at −20 °C, and diluted in culture medium to working concentration, right before use.
Cell lines
Human colon adenocarcinoma cell lines HT-29 (moderately differentiated cell line) and HCT-116 (poorly differentiated cell line) were purchased from DSMZ and ATCC, respectively. Both lines express vitamin D receptor (VDR). Cell lines were cultured in McCoy’s 5A medium (Lonza, Belgium) supplemented with glutamine, 10 % FBS and antibiotics at 37 °C and 5 % CO2.
Selection of cancer cells refractory to treatment with 5-FU
HT-29 or HCT-116 cells were seeded in 75-cm2 flasks (Nunclon) at a cell density of 1.7 × 106 cells/20-ml medium. After 4-h incubation, 5-FU at a final concentration of 6 μg/ml (46 μM) was added to cells attached to plastic. Cells were exposed to 5-FU for 24 h, and then culture medium was replaced with a fresh medium without 5-FU for the next 3 days. After the cytoreduction, cells resistant to a single treatment with 5-FU were collected using trypsin with EDTA (Trypsin-EDTA, Lonza). The collected cells denominated as HT-29/5-FU cells or HCT-116/5-FU cells were passaged to test their regrowth and clonogenicity without or in the presence of vitamin D analogs.
Cultures of cells preselected with 5-FU
HT-29/5-FU cells and HCT-116/5-FU cells were seeded in 75-cm2 flasks (Nunclon) at a cell density of 1.5 × 106 cells/20-ml medium without or with PRI-2191, PRI-2205, or PRI-1906. Fresh medium with or without vitamin D analogs was replaced after 2 days. On day 4 of culture, cells were harvested using trypsin with EDTA.
In the clonogenicity assay, 102/dish of chemonaive HT-29 or HCT-116 cells or 5 × 102/dish HT-29/5FU or HCT-116/5FU cells were plated in 35-mm diameter Petri dishes. Cells were cultured without or with PRI-2191, PRI-2205, or PRI-1906 for 10 days. The number of colonies was counted after fixing in methanol and staining with crystal violet. Colonies consisting of at least 20 cells were counted under a microscope at a 40-fold magnification.
Monolayer wound healing assay
To evaluate migration ability, monolayer wound healing assay for HT-29 and HCT-116 cells and also for the tumor cells preselected with 5-FU was performed. The cells were plated in Petri dishes. At the next day, the cells were confluent and two scratch wounds of approximately 400-μm width were made with pipet tip. The wounds were measured under inverted microscope. After treatment with vitamin D analogs for 24 h (chemonaive cells) or 48 h (pretreated cells), the wounds were measured again in the same marked site. The cell migration distance was determined by measuring the width of the wound divided by two and by subtracting this value from the initial half-width of the wound.
Antibodies and flow cytometry
AlexaFluor700-anti-CD44 and AlexaFluor647-anti-Ki-67 were purchased from BD Pharmingen (Franklin Lakes, NJ, USA) FITC-anti-EpCAM. PE-Cy7-anti-CXCR4 was purchased from BD Biosciences (San Jose, CA, USA). PE-anti-CD133/1 (AC133) was purchased from Miltenyi Biotec (Cologne, GE). Intracellular staining was performed using FoxP3 Staining Buffer Set (eBioscience) according to manufacturer’s protocol. Flow cytometry was performed using the FACSAriaIII, BD Biosciences. Data were analyzed using the FACSDiva software (BD Biosciences).
Gene expression analysis
Total RNA was extracted using TRIzol reagent according to manufacturer’s instruction. RNA quality was confirmed with NanoDrop ND-1000 spectrophotometer. Total RNA (1 μg) was reverse transcribed to complementary DNA (cDNA) using high-capacity cDNA reverse transcription kit (Life Technologies, Foster City, CA, USA). Next, the relative quantitation of genes expression was analyzed in triplicates by TaqMan Array and 7500 fast real-time PCR system (Life Technologies, Foster City, CA, USA). The comparative CT method was used with 18S rRNA serving as an endogenous control. The data output was expressed as a fold-change of expression levels. Fold-differences calculated using the ΔΔCT method are expressed as a range which is a result of incorporating the standard deviation of the ΔΔCT value into the fold-difference calculation.
Statistics
Statistical significance was evaluated with one-way ANOVA with Bonferroni multicomparison posttest correction using SPSS 14.0 (SPSS Inc). P values <0.05 were considered significant.
Results
Vitamin D analogs decrease clonogenicity of chemonaive HT-29 cells and HT-29 cells that survived treatment with 5-FU but do not affect clonogenicity of HCT-116 cells
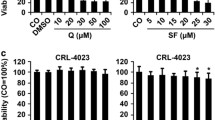
We evaluated the effect of vitamin D analogs on renewal of HT-29 and HCT-116 cells after the exposure to 5-FU in the clonogenicity assay. PRI-1906 was the most effective inhibitor of clone formation by chemonaive HT-29 cells, whereas among tested vitamin D analogs, PRI-2205 was the least effective inhibitor of clonogenicity (Fig. 1a). Vitamin D analogs tested at concentrations ranging from 2.5 to 1000 nM did not inhibit clone formation by chemonaive HCT-116 cells (Fig. 1b). Percentage of clonogenic cells decreased in HT-29 cells treated with 5-FU at a concentration of 6 μg/ml, in comparison to chemonaive HT-29 cells. Vitamin D analogs decreased further the number of clones formed by HT-29/5FU cells (Fig. 2a). Vitamin D analogs, even at concentration as high as 1000 nM, did not reduce clonogenicity of HCT-116/5-FU cells (Fig. 2b).
The effect of vitamin D analogs on the clonogenicity of chemonaive HT-29 cells (a) and chemonaive HCT-116 (b). For HCT-116 cell line, only data obtained at the highest used concentration (1000 nM) of vitamin D analogs are shown. The bar graphs indicate mean colony numbers ± standard deviation (SD). Cultures were set in n = 5 replicates, except for HT-29 cell control (n = 10). An asterisk indicates a significant difference between mean colony-forming cell numbers in cultures with vitamin D analog and in control, p < 0.05. Each of the experiments is a representative one out of three independent experiments
The effect of vitamin D analogs on the clonogenicity of HT-29/5-FU cells (a) and HCT-116/5FU cells (b). For HCT-116/5-FU cells, only data obtained at the highest used concentration (1000 nM) of vitamin D analogs are shown. The bar graphs indicate mean colony numbers ± SD. HT-29/5-FU cell cultures were plated in n = 5 replicates, and HCT-116/5-FU in n = 10 replicates. An asterisk indicates a significant difference between mean colony-forming cell numbers in cultures with vitamin D analog and in control, p < 0.05. Each of the experiments is a representative one out of three independent experiments
To evaluate migration/invasion potential of chemonaive and 5-FU-preselected colon cancer cell lines, the monolayer wound healing assay was performed. Vitamin D analogs had no effect on the migration of chemonaive or 5-FU-preselected HT-29 cells and HCT-116 cells after 24 or 48 h of observation (data not shown).
Vitamin D analogs decrease the proliferative activity of colon cancer cells during their renewal after the treatment with 5-FU and moderately modify the expression of CSC surface markers
Chemonaive HT-29 and HCT-116 cells expressed CD133, CXCR4, CD44, and EpCAM considered as cell surface markers of CSCs. Vitamin D analogs modified the expression of CSC markers in HT-29/5-FU cells undergoing renewal after treatment with 5-FU. CD133 expression level increased in HT-29/5-FU cells during 4-day renewal period after cell passage, but not in HT-29/5-FU cells exposed to vitamin D analogs (Fig. S1). CXCR4 and CD44 expression decreased in HT-29 cells following 5-FU treatment, and did not recover in HT-29/5-FU cells during 4-day culture after cell passage. Analogs PRI-1906 and PRI-2191 moderately promoted the re-expression of CD44 in HT-29/5-FU cells during the renewal period. Nonetheless, CD44 expression in HT-29/5-FU cells exposed to PRI-1906 or PRI-2191 did not recover to the level observed in chemonaive HT-29 cells. PRI-2205 did not promote the re-expression of CD44 in HT-29/5-FU cells.
PRI-1906, PRI-2191, and PRI-2205 decreased the proliferative potential of HT-29/5-FU cells during their renewal after treatment with 5-FU. The expression of intracellular proliferation marker Ki67 was substantially lower in HT-29/5-FU cells collected on day 3 after 5-FU removal from the culture as compared to chemonaive HT-29 cells, but recovered during a 4-day renewal period after cell passage (Fig. 3). Vitamin D analogs inhibited the recovery of Ki-67 expression in HT-29/5-FU cells during renewal after cell passage. The inhibitory effect of vitamin D analogs on the recovery of Ki-67 expression was observed in all HT-29/5-FU cell subsets identified depending on CD133 and CXCR4 expression level, except for a minor CD133−CXCR4+ cell subset. A proportion of cell subpopulations identified on the basis of CD133 and CXCR4 expression level in HT-29 cell population was changed after the exposure to 5-fluorouracil. CD133+CXCR4+cells prevailed among chemonaive HT-29 cells, whereas CD133+CXCR4− cells prevailed among HT-29/5-FU cells. A minor subpopulation of HT-29/5-FU cells identified as CD133−CXCR4+ cells highly expressed Ki-67. It suggested that this subpopulation might play an important role in the initiation of cancer re-growth after treatment with 5-FU.
The inhibitory effect of vitamin D analogs on Ki-67 expression in HT-29/5-FU cell subsets identified on a basis of CD133 and CXCR4 expression level. Flow cytometry plots shown in the upper row demonstrate analysis of CD133 expression versus CXCR4 expression in chemonaive HT-29 cells cultured for 4 days in medium only (HT-29 medium [4 days]), HT-29 cells treated with 5-FU for 1 day, and subsequently cultured without 5-FU for 3 days (HT-29 5-FU [1 day] medium [3 days]), HT-29/5-FU cells cultured after the passage for 4 days in medium (HT-29/5-FU medium [4 days]) or with 2.5 nM PRI-1906 (HT-29/5-FU PRI-1906 [4 days]) or 2.5 nM PRI-2191 (HT-29/5-FU PRI-2191 [4 days]) or 15 nM PRI-2205 (HT-29/5-FU PRI-2205 [4 days]). Ki-67 expression is shown in histogram overlays and separately for HT-29 cell subsets gated on a basis of CD133 and CXCR4 expression level
Vitamin D analogs at a concentration of 1 μM did not substantially modify CD133, CXCR4, CD44, or EpCAM expression level in HCT-116/5-FU cells during their renewal in 4-day culture after cell passage. PRI-1906 and PRI-2191 at a concentration of 1 μM decreased the proliferative capacity of HCT-116/5-FU cells during their renewal after the treatment with 5-FU, but CXCR4+ HCT-116/5-FU cells were less susceptible to the anti-proliferative effect of vitamin D analogs than CXCR4− HCT-116/5-FU cells. Ki-67 expression in CD133+CXCR4+ and in CD133−CXCR4+ HCT-116/5-FU cells was very high even after the treatment with vitamin D analogs (Fig. 4).
The inhibitory effect of vitamin D analogs on Ki-67 expression in HCT-116/5-FU cell subsets identified by CD133 and CXCR4 expression level. Flow cytometry plots shown in the upper row demonstrate analysis of CD133 expression versus CXCR4 expression in chemonaive HCT-116 cells cultured for 4 days in medium only (HCT-116 medium [4 days]), HCT-116 cells treated with 5-FU for 1 day and subsequently cultured without 5-FU for 3 days (HCT-116 5-FU [1 day] medium [3 days]), HCT-116/5-FU cells cultured after the passage for 4 days in medium (HCT-116/5-FU medium [4 days]) or with 1 μM PRI-1906 (HCT-116/5-FU PRI-1906 [4 days]) or 1 μM PRI-2191 (HCT-116/5-FU PRI-2191 [4 days]). Ki-67 expression is shown in histogram overlays and separately for HCT-116 cell subsets gated on a basis of CD133 and CXCR4 expression level
The relative mRNA expression of CSC-related and EMT-related genes increases in colorectal cancer cells during their renewal following the exposure to 5-FU
Analysis of the relative messenger RNA (mRNA) expression showed that both colon adenocarcinoma-derived cell lines HT-29 and HCT-116 expressed genes linked to CSC-like phenotype and to epithelial-mesenchymal transition (EMT) process (Fig. 5). The expression of stem/progenitor cell genes ALCAM (CD166), EPHB2, and PTEN was markedly higher in HCT-116 cells than in HT-29 cells. Both cell lines similarly expressed CD44, EPCAM, EPHB4, NOTCH1, OCT3/4, PROM1 (CD133), and SOX2. The relative expression of colon tissue stem cell genes LGR5 and SHH, playing a substantial role in the maintenance and renewal of the colonic epithelium, and CXCR4 gene was markedly higher in HT-29 cells than in HT-116 cells. The expression of several genes (SNAI1, ZEB1, TGFB1, CTNNB1, FSCN1, BIRC5, HIF1A, VEGFB, NRP1) involved in EMT, invasion, or angiogenesis was higher in HCT-116 cells than in HT-29 cells, and the expression of other of such genes (i.e., TWIST1, SNAI2, VIM1, CDH2, MMP7, and NRP2) was detected in HCT-116 cells but not in HT-29 cells. The expression of genes KRT20, VIL1, CDH1 involved in cell differentiation and maintenance of the epithelial phenotype of colon cancer cells was higher in HT-29 cells than in HCT-116 cells. HT-29 cells expressed CSC/drug resistance genes ALDH1A1 and ABCG2, whereas HT-116 cells expressed ABCB1 and ABCG2, but did not express ALDH1A1.
The mRNA expression of numerous CSC-related and EMT-related genes increased highly in HT-29/5-FU cells undergoing renewal following treatment with 5-FU as compared to chemonaive HT-29 cells (Fig. 6). The expression of some CSC/EMT genes increased also in HCT-116/5-FU cells during renewal, although not as much as in HT-29/5-FU cells. The upregulation of CSC/EMT-related genes in HT-29/5-FU cells and in HCT-116/5-FU cells was observed on the third day after 5-FU removal from cultures, and also after additional 4 days of culture after cell passage.
CSC- and EMT-related genes are upregulated in HT-29/5-FU and HCT-116/5-FU on day 3 after 5-FU removal from the cultures and after next 4 days of culture after cell passage (day [3 + 4] after 5-FU). The graphs show fold change of mRNA expression level in HT-29/5-FU and HCT-116/5-FU in comparison to chemonaive HT-29 cells or chemonaive HCT-116 cells, respectively. Fold-differences calculated using the ΔΔCT method are expressed as a range which is a result of incorporating the standard deviation of the ΔΔCT value into the fold-difference calculation
PRI-1906 and PRI-2191 downregulate the expression of genes related to survival, re-growth, and invasiveness in HT-29/5-FU cells during renewal
We examined gene expression in 5-FU-preselected HT-29 colon cancer cells (HT-29/5-FU cells) cultured without or with vitamin D analogs (PRI-1906, PRI-2191, or PRI-2205) added to the cultures at a concentration of 10 nM during 4-day renewal following cell passage (Fig. 7). The inhibitory effect of PRI-1906 and PRI-2191 on the clonogenicity and proliferation of HT-29/5-FU cells was associated with downregulation of a wide range of genes involved in cell renewal process. PRI-1906 and PRI-2191 decreased the expression of a majority of genes related to stemness, EMT, angiogenesis, cell proliferation, and cell survival. The only CSC/SC-related genes upregulated in HT-29/5-FU cells treated with PRI-1906 were SHH1, CD44, LGR5, and SPP1. None of the CSC/SC-related genes was upregulated in HT-29/5-FU cells cultured with PRI-2191. The mRNA expression of PTEN, which is a critical negative regulator of the cell-survival signaling pathway initiated by PI3K was not affected by vitamin D analogs. PRI-1906 and PRI-2191 partially reversed the upregulation of some of CSC/EMT-related genes induced following the exposure of HT-29 cells to 5-FU. PRI-1906 and PRI-2191 decreased the expression of several pro-apoptotic genes, but also decreased the expression of anti-apoptotic gene BCL2. PRI-1906 and PRI-2191 down-regulated the expression of KRT20 and MUC1 related to colon cell differentiation.
Vitamin D analogs modify gene expression in HT-29/5-FU cells undergoing renewal. The graphs show the relative mRNA expression level in HT-29/5-FU exposed to vitamin D analog as compared to the level in HT-29/5-FU cultured in medium only for 4 days after cell passage. HT-29/5-FU cells were cultured with vitamin D analogs added at a concentration of 10 nM. Fold-differences calculated using the ΔΔCT method are expressed as a range which is a result of incorporating the standard deviation of the ΔΔCT value into the fold-difference calculation
In contrast to PRI-1906 and PRI-2191, PRI-2205 generally did not affect the expression of genes related to stemness, EMT, angiogenesis, cell proliferation, survival, and apoptosis in HT-29/5-FU cells, but increased the expression of anti-apoptotic gene BCL2 and genes related to differentiation of colonic epithelium. The mRNA expression of thymidine phosphorylase gene (TYMP) increased in HT-29/5-FU cells in the presence of each of vitamin D analogs tested.
Opposite effects of PRI-1906 and PRI-2191 on the expression of genes related to stemness and angiogenesis in HCT-116/5-FU cells during renewal
We compared gene expression in HCT-116/5-FU cells cultured for 4 days without or with PRI-1906 or PRI-2191 at a concentration of 1 μM (Fig. 8). PRI-1906 augmented expression of the majority of genes related to stemness and angiogenesis, whereas PRI-2191 decreased expression of such genes, except for SHH and NRP1. It suggested that PRI-2191 at a high concentration induced HCT-116/5-FU cell shift toward a more differentiated phenotype, whereas PRI-1906 reverted HCT-116/5-FU cells toward a less differentiated phenotype. PRI-1906 decreased the expression of some genes related to apoptosis. Both analogs: PRI-1906 or PRI-2191 augmented expression of CDH1 gene.
PRI-1906 and PRI-2191 differently modify gene expression in HCT-116/5-FU cells undergoing renewal. The graphs show the relative mRNA expression level in HCT-116/5-FU cells exposed to vitamin D analog as compared to the level in HCT-116/5-FU cultured in medium for 4 days after cell passage. HCT-116/5-FU cells were cultured with vitamin D analogs added at a concentration of 1 μM. Fold differences calculated using the ΔΔCT method are expressed as a range which is a result of incorporating the standard deviation of the ΔΔCT value into the fold-difference calculation
Discussion
The aim of this study was to examine whether vitamin D analogs decrease renewal capacity of colon cancer cells that resisted treatment with conventional chemotherapeutic 5-FU. It was reported previously that conventional chemotherapy preferentially spares CSC [28–33]. However, because of cancer cell plasticity, also heterogeneous cancer cells may acquire mesenchymal-like phenotype and stem-cell properties in response to chemotherapy [7, 34–37]. In our study, analysis of CSC- and EMT-related gene expression pattern indicated that a bulk of colon cancer cells that resisted the exposure to 5-FU acquired more features of a stem-like phenotype than the non-treated cancer cells. The phenotype shift toward stemness of 5-FU-selected cell population was much more pronounced in a moderately differentiated HT-29 cell line than in a poorly differentiated HCT-116 cell line. This observation indicated that more differentiated colon cancer cells display higher plasticity following the exposure to chemotherapeutic drug than undifferentiated colon cancer cells.
The regulatory effects of vitamin D analogs on the re-growth of colon cancer cell after treatment with 5-FU varied, depending on cell differentiation stage and sensitivity to vitamin D. Vitamin D analogs decreased clonogenicity and proliferation of HT-29 cell line and HT-29/5-FU cells even at relatively low doses. In contrast, vitamin D analogs at wide range of doses did not affect clonogenicity of HCT-116 cells and HCT-116/5-FU cells, although at a high dose partially inhibited proliferation of HCT-116/5-FU cells during their renewal. We observed a differential sensitivity of colon cancer cells to anti-proliferative activity of vitamin D analogs, depending on the expression of CXCR4 considered as a marker of cancer stem-like cells with high metastatic potential [38, 39]. Our data suggested that in both colon cancer cell lines, CXCR4+CD133− cancer cells initiated renewal after treatment with 5-FU, and this cell subpopulation was the least sensitive to anti-proliferative effects of vitamin D analogs.
We found that during cancer cell renewal after the treatment with 5-FU, differential effects on gene expression pattern might be obtained in moderately and in poorly differentiated colon cancer cell lines by using synthetic analogs of active form of both, vitamins D2 and D3, modified in the aliphatic side chain. PRI-2191, a calcitriol analog that reduced proliferative activity of both moderately and poorly differentiated cancer cells during their renewal following treatment with 5-FU, induced changes in gene expression pattern toward the loss of stem-like phenotype. PRI-1906, a vitamin D2 analog, induced similar effects, but only in HT-29/5-FU cells. In HCT-116/5-FU cells, PRI-1906 decreased proliferation of HCT-116/5-FU cells during their renewal, but concomitantly increased the expression of CSC-related genes in these cells. Such a shift of cancer cell phenotype toward a more stem-like one could pose a risk of the increased tumorigenicity of mesenchymal-like colon cancer cells treated with PRI-1906 following 5-FU-based therapy. Therefore, PRI-2191 seems a safer candidate than PRI-1906 for targeting CSC-like cells initiating tumor recurrence after conventional chemotherapy.
PRI-1906 and PRI-2191 analogs highly increased SHH expression in HCT-116/5-FU cells during renewal. Hedgehog signaling is involved in constant renewing and differentiation of the colonic lining epithelium. It was reported [40] that poorly differentiated colon cancer cells are rather insensitive toward inhibition of Hh signal transduction by cyclopamine, in contrast to colon cancer cells with high differentiation status, such as HT-29, which depend on active Hh signaling. Data of this report supported assumption that a highly proliferative and dedifferentiated phenotype seems to be accompanied with a loss of active Hh signaling during oncogenesis of colon cancer. Our data showed that the two assessed vitamin D analogs reactivate SHH expression in poorly differentiated colon cancer cells.
We found that PRI-1906 and PRI-2191 decreased the expression of SNAI1 and SNAI2 in HT-29/5-FU cells during their renewal. It was reported that the transcription factor SNAIL represses VDR expression transcriptionally and post-transcriptionally in human colon cancer [12], which may lead to a loss of response to the antitumor effects of calcitriol and analogs in vitro and in vivo. A balance between VDR and SNAIL, ZEB1 expression is critical for E-cadherin expression, which influences cell fate during colon cancer progression [41]. Colon cancer patients with high levels of SNAIL are likely to be poor responders to therapy with vitamin D analogs. Thus, downregulation of SNAIL, and upregulation E-cadherin (encoded by CDH1 gene) in colon cancer cells by vitamin D analogs might promote mesenchymal-to-epithelial transition and increase the responsiveness to therapy with vitamin D analogs.
Thymidine phosphorylase overexpression has been associated with the promotion of tumorigenicity [42–45]. However, the increased TYMP expression induced by vitamin D analogs in colon cancer cells during renewal after treatment with 5-FU might favorably increase colon cancer response to 5-FU during the following cycle of treatment, since thymidine phosphorylase is an activating agent for pro-drugs of 5-FU [46–48].
In conclusion, our data suggest that select low-calcemic synthetic vitamin D analogs could be used to prevent cancer recurrence, if used sequentially after treatment with conventional chemotherapeutics to target colon cancer cell which acquired stem-like phenotype in response to chemotherapy. Out of series of vitamin D analogs studied, PRI-2191 might be useful both to decrease proliferative activity and to modulate the expression of stemness-related genes in moderately and in poorly differentiated colon cancer cells initiating cancer renewal after treatment with 5-FU.
References
GLOBOCAN 2008 website: globocan.iarc.fr. (12 July 2013, date last accessed).
Center MM, Jemal A, Ward E. International trends in colorectal cancer incidence rates. Cancer Epidemiol Biomarkers Prev. 2009;18:1688–94.
Bossetti C, Levi F, Rosato V, La Vecchia C, Bertuccio P, Lucchini F, et al. Recent trends in colorectal cancer mortality in Europe. Int J Cancer. 2011;129:180–91.
Siegel R, Ma J, Zou Z, Jemal A. Cancer Statistics 2014. CA Cancer J Clin. 2014;64:9–29.
Dallas NA, Xia L, Fan F, Gray MJ, Gaur P, van Buren G, et al. Chemoresistant colorectal cancer cells, the cancer stem cell phenotype, and increased sensitivity to insulin-like growth factor-I receptor inhibition. Cancer Res. 2009;69:11951–7.
Wang L, Guo H, Lin C, Yang L, Wang X. Enrichment and characterization of cancer stem like cells from a cervical cancer cell line. Mol Med Rep. 2014;9:2117–23.
Xu ZY, Tang JN, Xie HX, Du YA, Huang L, Yu PF, et al. 5-Fluorouracyl chemotherapy of gastric cancer generates residual cells with properties of cancer stem cells. Int J Biol Sci. 2015;11:284–94.
Danilenko M, Studzinski GP. Enhancement by other compounds of the anti-cancer activity of vitamin D(3) and its analogs. Exp Cell Res. 2004;298:339–58.
Kawasaki BT, Hurt EM, Mistree T, Farrar WL. Targeting cancer stem cells with phytochemicals. Mol Interv. 2008;8:174–84.
Li Y, Wicha MS, Schwartz SJ, Sun D. Implications of cancer stem cell theory for cancer chemoprevention by natural dietary compounds. J Nutr Biochem. 2011;22:799–806.
Nautiyal J, Kanwar SS, Yu Y, Majumdar APN. Combination of dasatinib and curcumin eliminates chemo-resistant colon cancer cells. J Mol Signal. 2011;6:7. doi:10.1186/1750-2187-6-7.
Palmer HG, Gonzalez-Sancho JM, Espada J, Berciano MT, Puig I, Baulida J, et al. Vitamin D3 promotes the differentiation of colon carcinoma cells by the induction of E-cadherin and the inhibition of beta-cadherin signaling. J Cell Biol. 2001;154:369–87.
Liu S, Dontu G, Wicha MS. Mammary stem cells, self-renewal pathways and carcinogenesis. Breast Cancer Res. 2005;7:86–95.
Krishnan AV, Trump DL, Johnson CS, Feldman D. The role of vitamin D in cancer prevention and treatment. Anticancer Res. 2006;26:2543–9.
Di Rosa M, Malaguarnera M, Zanghì A, Passaniti A, Malaguarnera L. Vitamin D3 insufficiency and colorectal cancer. Crit Rev Oncol Hematol. 2013;88:594–612.
Pełczyńska M, Wietrzyk J, Jaroszewicz I, Nevozhay D, Switalska M, Kutner A, et al. Correlation between VDR expression and antiproliferative activity of vitamin D. Anticancer Res. 2005;25:2235–40.
Ravid A, Rocker D, Machlenkin A, Rotem C, Hochman A, Kessler-Icekson G, et al. 1,25-dihydroxyvitamin D3 enhances the susceptibility of breast cancer cells to doxorubicin-induced oxidative damage. Cancer Res. 1999;59:862–7.
Cho YL, Christensen C, Saunders DE, Lawrence WD, Deppe G, Malviya VK, et al. Combined effects of 1,25-dihydroxyvitamin D3 and platinum drugs on the growth of MCF-7 cells. Cancer Res. 1991;51:2848–53.
Siwinska A, Opolski A, Chrobak A, Wietrzyk J, Wojdat E, Kutner A, et al. Potentiation of the antiproliferative effect in vitro of doxorubicin, cisplatin and genistein by new analogues of vitamin D. Anticancer Res. 2001;21:1925–9.
Hershberger PA, Yu WD, Modzelewski RA, Rueger RM, Johnson CS, Trump DL. Calcitriol (1, 25-dihydroxycholecalciferol) enhances paclitaxel antitumor activity in vitro and in vivo and accelerates paclitaxel-induced apoptosis. Clin Cancer Res. 2001;17:1043–51.
Wietrzyk J, Nevozhay D, Filip B, Milczarek M, Kutner A. The antitumor effect of lowered doses of cytostatics combined with new analogs of vitamin D in mice. Anticancer Res. 2007;27:3387–98.
Wietrzyk J, Nevozhay D, Milczarek M, Filip B, Kutner A. Toxicity and antitumor activity of the vitamin D analogs PRI-1906 and PRI-1907 in combined treatment with cyclophosphamide in a mouse mammary cancer model. Cancer Chemother Pharmacol. 2008;62:787–97.
Milczarek M, Rosińska S, Psurski M, Maciejewska M, Kutner A, Wietrzyk J. Combined colonic cancer treatment with Vitamin D analogs and irinitecan or oxaliplatin. Cancer Res. 2013;33:433–44.
Milczarek M, Filip-Psurska B, Swiętnicki W, Kutner A, Wietrzyk J. Vitamin D analogs combined with 5-fluorouracil in human HT-29 colon cancer treatment. Oncol Rep. 2014;32:491–504.
Deeb KK, Trump DL, Johnson CS. Vitamin D signalling pathways in cancer: potential for anticancer therapeutics. Nat Rev Cancer. 2007;7:684–700.
Baurska H, Marchwicka A, Klopot A, Kutner A, Marcinkowska E. Studies on the mechanisms of superagonistic pro-differentiating activities of side-chain modified analogs of vitamin D2. Oncol Rep. 2012;28:1110–6.
Gocek E, Kielbinski M, Wylob P, Kutner A, Marcinkowska E. Side-chain modified vitamin D analogs induce rapid accumulation of VDR in the cell nuclei proportionately to their differentiation-inducing potential. Steroids. 2008;73:1359–66.
Levina V, Marrangoni AM, DeMarco R, Gorelik E, Lokshin AE. Drug-selected human lung cancer stem cells: cytokine network, tumorigenic and metastatic properties. PLoS One. 2008;3:e3077. doi:10.1371/journal.pone.0003077.
Dylla SJ, Beviglia L, Park IK, Chartier C, Raval J, Ngan L, et al. Colorectal cancer stem cells are enriched in xenogeneic tumors following chemotherapy. PLoS One. 2008;18(3):e2428. doi:10.1371/journal.pone.0002428.
Li X, Lewis MT, Huang J, Gutierrez C, Osborne CK, Wu MF, et al. Intrinsic resistance of tumorigenic breast cancer cells to chemotherapy. J Natl Cancer Inst. 2008;100:672–9.
Ma S, Lee TK, Zheng BJ, Chan KW, Guan XY. CD133+ HCC cancer stem cells confer chemoresistance by preferential expression of the Akt/PKB survival pathway. Oncogene. 2008;27:1749–58.
Fabrizi E, Martino S, Pelacchi F, Ricci-Vitani L. Therapeutic implications of colon cancer stem cells. World J Gastroenterol. 2010;16:2387–3877.
Abubaker K, Latifi A, Luwor R, Nazaretian S, Zhu H, Quinn MA, et al. Short-term single treatment of chemotherapy results in the enrichment of ovarian cancer stem cell-like cells leading to an increased tumor burden. Mol Cancer. 2013;12:24.
Latifi A, Abubaker K, Castrechini N, Ward AC, Liongue C, Dobill F, et al. Cisplatin treatment of primary and metastatic epithelial ovarian carcinomas generates residual cells with mesenchymal stem cell-like profile. J Cell Biochem. 2011;112:2850–64.
Hu X, Ghisolfi L, Keates AC, Zhang J, Xiang S, Lee DK, et al. Induction of cancer cell stemness by chemotherapy. Cell Cycle. 2012;11:2691–8.
Kim Y, Joo KM, Jin J, Nam DH. Cancer stem cells and their mechanism of chemo-radiation resistance. Review. Int J Stem Cells. 2009;2:109–14.
Horst G, Bos L, Pluijm G. Epithelial plasticity, cancer stem cells, and the tumor-supportive stroma in bladder carcinoma. Mol Cancer Res. 2012;10:995–1009.
Zhang SS, Han ZP, Jing YY, Tao SF, Li TJ, Wang H, et al. CD133 + CXCR4+ colon cancer cells exhibit metastatic potential and predict poor prognosis of patients. BMC Med. 2012;10:85. doi:10.1186/1741-7015-10-85.
Sarvaiya PJ, Guo D, Ulasov I, Gabikian P, Lesniak MS. Chemokines in tumor progression and metastasis. Oncotarget. 2013;4:2171–85.
Alinger B, Kiesslich T, Datz C, Aberger F, Strasser F, Berr F, et al. Hedgehog signaling is involved in differentiation of normal colonic tissue rather than in tumor proliferation. Virchows Arch. 2009;454:369–79.
Peña C, García JM, García V, Silva J, Domínguez G, Rodríguez R, et al. The expression levels of the transcriptional regulators p300 and CtBP modulate the correlations between SNAIL, ZEB1, E-cadherin and vitamin D receptor in human colon carcinomas. Int J Cancer. 2006;119:2098–104.
Takebayashi Y, Yamada K, Miyadera K, Sumizawa T, Furukawa T, Kinoshita F, et al. The activity and expression of thymidine phosphorylase in human solid tumors. Eur J Cancer. 1996;32A:1227–32.
Saeki T, Tanada M, Takashima S, Saeki M, Takiyama W, Nishimoto N, et al. Correlation between expression of platelet-derived endothelial cell growth factor (thymidine phosphorylase) and microvessel density in early-stage human colon carcinomas. Jpn J Clin Oncol. 1997;27:227–30.
Toi M, Atiqur Rahman M, Bando H, Chow LW. Thymidine phosphorylase (platelet-derived endothelial-cell growth factor) in cancer biology and treatment. Lancet Oncol. 2005;6:158–66.
Mitselou A, Ioachim E, Skoufi U, Tsironis C, Tsimogiannis KE, Skoufi C, et al. Predictive role of thymidine phosphorylase expression in patients with colorectal cancer and its association with angiogenesis-related proteins and extracellular matrix components. In Vivo. 2012;26:1057–67.
Ackland SP, Peters GJ. Thymidine phosphorylase: its role in sensitivity and resistance to anticancer drugs. Drug Resist Updat. 1999;2:205–14.
Hirano Y, Takayama T, Kageyama S, Ushiyama T, Suzuki K, Fujita K. Thymidine phosphorylase and dihydropyrimidine dehydrogenase in renal cell carcinoma: relationship between hisological parameters and chemosensitivity to 5-fluorouracil. Eur Urol. 2003;43:45–51.
Nishina T, Hyodo I, Miyaike J, Inaba T, Suzuki S, Shiratori Y. The ratio of thymidine phosphorylase to dihydropyrimidine dehydrogenase in tumour tissues of patients with metastatic gastric cancer is predictive of the clinical response to 5-deoxy-5-fluorouridine. Eur J Cancer. 2004;40:1566–71.
Acknowledgments
This work was supported by a grant from National Science Centre, Poland (N N402 139738) for J.M.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Electronic supplementary material
Below is the link to the electronic supplementary material.
Fig. S1
(PPTX 371 kb)
Rights and permissions
About this article
Cite this article
Kotlarz, A., Przybyszewska, M., Swoboda, P. et al. Differential interference of vitamin D analogs PRI-1906, PRI-2191, and PRI-2205 with the renewal of human colon cancer cells refractory to treatment with 5-fluorouracil. Tumor Biol. 37, 4699–4709 (2016). https://doi.org/10.1007/s13277-015-4311-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-4311-4