Abstract
The growth of solid tumors requires angiogenesis to provide oxygen and nutrients and to support cell proliferation. The switch from an avascular to a vascular phenotype is typically related to acceleration of tumor growth. Anti-angiogenic therapy is becoming a very promising way for malignant tumors. Meanwhile, malignant tumor cells themselves were able to develop the formation of cell-lined vessels that contribute to tumor neovascularization and supply the nutrients and oxygen, which is called vasculogenic mimicry (VM). However, the molecular mechanism of VM remains unclear. The purpose of this study was to investigate the efficacy of the novel recombinant human endostatin (rh-Endo) protein combined with radiotherapy on human esophageal squamous cell carcinoma (ESCC) cell lines Eca-109 and TE13. Our results showed that rh-Endo combined with radiotherapy significantly inhibited the proliferation, migration, invasion, and VM of human esophageal cancer cells in a dose-dependent manner; however, it has no direct effect on apoptosis of carcinoma cells, which indicated that rh-Endo combined with radiotherapy significantly changed the microenvironment of esophageal carcinoma, and played an important role in preventing distant metastasis. Our findings suggested that rh-Endo inhibited the metastasis of esophageal cancer and the activation of AKT pathway, and the down-regulation of epithelial–mesenchymal transition (EMT) may be associated with such effect of rh-Endo. These results also supported the bright prospect of rh-Endo combined with radiotherapy for clinical applications in the future.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Esophageal cancer (EC) is the eighth most common cancer and the sixth most common cause of cancer-related death all over the world, and esophageal squamous cell carcinoma (ESCC) constitutes the major pathological type [1]. Though radiotherapy (RT) plays an important role in the local control of ESCC, the survival rate of patients with esophageal carcinoma still remains to be less than 20 %. The most probable reason is that the radiotherapy may not prevent the metastasis of the primary tumor, while the tumor’s metastasis causes the death [2]. Angiogenesis, or the formation of new capillaries from preexisting blood vessels, is involved in the pathogenesis of various diseases such as cancer, atherosclerosis, and diabetic retinopathy [3]. Several recent researches showed that anti-angiogenesis therapy may become one promising treatment of these diseases [4, 5]. Recombinant human endostatin (rh-Endo, under the trade name of Endostar), a fragment of collagen XVIII, was mainly found in the basement membrane around blood vessels. It has previously been applied to treat atherosclerosis and was also pushed into anti-cancer clinical trials [3, 6]. The rh-Endo has been approved by the China Food and Drug Administration since 2005 for the treatment of non-small-cell lung cancer (NSCLC) [7, 8]. In our previous study, we found that rh-Endo inhibits the development of cancer in mice xenotransplant model of esophageal squamous carcinoma. Nevertheless, the molecular mechanism still remains ambiguous.
VM involves the tube formation of tumor cells consisting of a type of mesenchymal cell, similar to epithelial–mesenchymal transition (EMT) [9]. EMT is the process by which differentiated epithelial cells changes from an epithelial cobblestone phenotype to an elongated fibroblastic phenotype [10], which results in the decreased expression of epithelial markers such as E-cadherin and the increased expression of mesenchymal markers such as Snail and N-cadherin [11]. Currently, EMT has been implicated in the processes that tumor cells metastasize to distant area and acquisition of therapeutic resistance [12]. Recent studies suggest that EMT plays a crucial role in the progress of cancer radioresistance [13]. In our study, we tried to find out the direct effect of rh-Endo combined with radiotherapy on the migration, invasion, and the tube formation of esophageal cancer, exploring the possible molecular mechanism. The bright prospects in application of this experiment were also revealed here.
Materials and methods
Reagents
Human recombinant endostatin (endostatin, also known as “rh-Endo”) was kindly provided by Simcere Pharmaceuticals (Nanjing, China).
Antibodies for phosphatase and tensin homolog deleted on chromosome ten (PTEN), Snail, GSK-3β, phosphorylated GSK-3β (p-GSK-3β), Akt, and phosphorylated Akt (p-Akt) were purchased from CST (Cell Signaling Technology, MA). E-cadherin antibodies were purchased from Abcam.
Cell lines and cell culture
ESCC cell lines ECA109 and TE13 were obtained from the Shanghai Institute of Cell Biology (Shanghai, China) and were maintained in Dulbecco’s modified eagle medium (DMEM) medium (Gibco, Life Technologies, Carlsbad, CA, USA) supplemented with 10 % fetal bovine serum (Hyclone, GE Healthcare, Little Chalfont, UK), 1 % penicillin/streptomycin (Invitrogen, Life Technologies). Cells were maintained in an incubator at 37 °C, in an atmosphere containing 5 % CO2.
Cell viability assay
A cell counting kit-8 (CCK-8) assay was used to measure the cell proliferation. Eca-109 and TE13 were seeded into 96-well plates at 5 × 103 cells/well for 24 h, then incubated with different concentrations of Rh-Endo (25, 50, 100, 200, 400, 600, and 800 μl). Then, a CCK8 cell proliferation and cytotoxicity assay kit (Obio Technology, Shanghai, China) was used after 24 h. The absorbance was measured at a wavelength of 490 nm.
Clonogenic survival assay
Esophageal cancer cells ECA109 and TE13 cells were seeded onto 6-well dishes. After overnight culture, cells were treated with 6-MV X-rays at doses of 0, 2, 4, 6, or 8 Gy at 4.5 Gy/min. The cells were then cultured in a 5 % CO2 incubator at 37 °C for 2 weeks. The colonies were fixed and stained with Giemsa dye to count the number of colonies (>50 cells/colony) under microscope.
Flow cytometric analysis
ECA109 and TE13 cells were plated in 6-well plates at a specific density. The cells were treated with rh-Endo (100 and 400 μg/ml) and exposed to X-rays (6 Gy). After 24 h, the cells were fixed in 2 % paraformaldehyde and stained with an Annexin V-FITC Apoptosis Kit (Keygene Biotechnology, Nanjing, China). The apoptotic cells were detected by flow cytometry with Cell-Quest software (BD Biosciences, San Jose, CA, USA).
Wound-healing migration assay
Tumor cells were seeded in 6-well plates and cultured until 60 % confluence; then, we treated each well with different concentrations of rh-Endo and different doses of IR. The confluent cell monolayer was scratched with a pipette tip to generate a vertical line across the middle of the wells. The spread of wound closure was observed after 0 and 24 h intervals and was photographed by a light microscope.
Transwell invasion assay
Invasion assays were performed in the transwell (Corning, MA, USA) chamber with 8-um pore size polycarbonate filters, which are coated with 2 mg/ml of basement membrane, and matrigel (Corning, MA, USA) was used. Five hundred microliters medium containing 20 % fetal bovine serum (FBS) were added to the bottom of the chambers as the chemotactic factor and then 1 × 105 tumor cells were seeded into the top chambers with 500 ul DMEM (without FBS). After that, we treated the top chambers with different concentrations of rh-Endo (100 and 400 μg/ml) or/and 6 Gy of IR, and then incubated for 24 h. The invasive cells were fixed with cold 4 % paraformaldehyde, stained with 0.1 % crystal violet for 15 min, and washed with PBS three times. The fixed cells were photographed under a light microscope (×100) from three random fields.
3D culture and tube formation assay
We used a 15-well μ-Slide (Ibidi, Germany) to conduct tube formation assay. Briefly, to promote cell adhesion, we filled the inner well with 10 μl liquid Matrigel and incubated them at 37 °C for 1 h. Forty microliters of cancer cell suspension (2 × 105/ml) was seeded into each upper well and incubated at 37 °C and 5 % CO2 as usual. The cultures were maintained in DMEM complemented with 10 % FBS and 0.1 % gentamicin sulfate. The cells then were retreated with altered concentrations of rh-Endo (0, 100, and 400 μg/ml) and different radiation doses (0 and 6 Gy). After 4 h, we photographed the tubular structure of cancer cells with an inverted microscope (OLYMPUS, Japan) at 100 magnification. We then counted the total tube length and the number of branch points in three random view fields each well using an Ibidi Quantitative Tube Formation Image Analysis-Wim tube system under a light microscope (×100).
Western blot analysis
The total proteins were extracted from the tumor cells using SDS Lysis Buffer (Keygen, Nanjing, China). The contents of proteins were measured by BCA assay (Keygen, Nanjing, China). Equal amounts of protein from each lysate were separated by SDS-PAGE (10 % acrylamide) and blotted to PVDF Western blotting membranes (Millipore). The membranes were blocked, probed overnight with primary antibodies against PTEN, Akt, p-Akt, GSK-3β, p-GSK-3, E-cadherin, Snail and glyceraldehyde 3-phosphate dehydrogenase (GAPDH, as loading control of total proteins). The immunoblotted proteins were visualized with the Chemidoc XRS imaging system (Quantity One Quantitation software; BioRad Laboratories, Hercules, CA, USA) using ECL reagents, after that measured by the public domain NIH Image J Program.
Data analysis
The mean ± standard deviation (SD) from triplicate assays was calculated, and the differences between treatment groups were determined using the ANOVA test. Statistical analysis was carried out by STATA 11.0 software (StataCorp, College Station, TX, USA) and Prism 5.0 software (GraphPad, La Jolla, CA, USA). P < 0.05 was considered to be statistically significant.
Results
rh-Endo does not improve radiosensitivity of ESCC in vitro
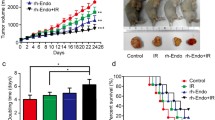
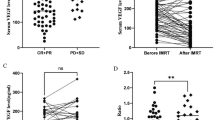
To explore whether rh-Endo affected ESCC cells directly and whether the improved radioresponse was due to radiation-induced tumor cell death, a CCK8 assay and flow cytometry assay were used. Although in CCK-8 assay, higher concentrations of rh-Endo (200 μg/ml and higher) exerted small inhibitory effects on the growth of ESCC cell lines, overall, there were no clear time- and dose-dependent effects (Fig. 1a). Flow cytometry assay revealed that rh-Endo combined with IR did not induce apoptosis of the ESCC cell lines ECA109 and TE13 in comparison with IR (Fig. 1c, d). The same conclusion was obtained in our previous clonogenic survival assay (Fig. 1b). These data suggested that the effect of rh-Endo combined with radiotherapy was not due to direct tumor-cell killing, which indicated it did not enhance the radiosensitivity in vitro [14].
rh-Endo does not improve the radioresponsiveness of ESCC in vivo. a rh-Endo did not inhibit the proliferation of ESCC cells in a dose-dependent manner, and the experimental concentrations for ESCC cells ECA109 and TE13 were 100 μg/ml (as the lower concentration) and 400 μg/ml (as the higher concentration), respectively. b, c Cell survival curve was established by clonogenic survival assay. The cells were treated with 100 or 400 μg/ml rh-Endo and the doses of 2, 4, 6, and 8 Gy irradiation as illustrated and harvested after incubation for 10–14 days; the result showed no statistical significance. d, e rh-Endo (100 and 400 μg/ml) did not enhanced irradiation-induced apoptosis of ECA109 cells and TE19 cells; the result also showed no statistical significance
Effect of irradiation on esophageal cancer cell migration, invasion and tube formation
The cells migration and invasion ability of irradiated esophageal cancer has been increased [15]. In our trait, we evaluated the migration and invasion ability of irradiated ECA109 and TE13 cells in vitro. Wound-healing assay showed that the irradiated cancer cells had significantly faster closure of wound area compared with non-irradiated cells (Fig. 2). Cell invasion of irradiated cancer cells was found to increase obviously, when compared with non-irradiated cells (Fig. 3). These results showed that the esophageal cancer cells migration and invasion ability were greatly increased after irradiation. Thus, irradiation may promote tumor metastasis, though radiation therapy itself had a strong anti-tumor effect in situ.
rh-Endo combined with irradiation inhibits ESCC migration in a dose-dependent manner. Cell migration was measured by wound-healing migration assay. ESCC were treated with different concentrations of rh-Endo and different doses of IR as illustrated, and the migrated cells were quantified by manual counting after 0 and 24 h using a light microscope. Data are expressed as the mean ± S.E. (n = 3).*P < 0.05
rh-Endo combined with irradiation inhibits ESCC invasion in transwell invasion assay. ESCC were seeded in the top chamber of transwell and treated with different concentrations of rh-Endo and different doses of IR. The bottom chambers were filled with 500 ml DMEM with 20 % FBS. After 24 h, the invasive ESCC were stained and quantified by manual counting. Data are expressed as the mean ± S.E. (n = 3).*P < 0.05
Tube formation (called as VM formation) of esophageal cancer cell is a key step in the change of tumor microenvironment. Therefore, we evaluated the effects of the tube formation of cancer cells. The result was the same as wound-healing migration assay and invasion assay. The ability of tube formation was strongly increased in irradiated groups compared with non-irradiated (Fig. 4).
rh-Endo combined with irradiation inhibits VM formation of ESCC. HUVECs were seeded on a 15-well μ-Slide (Ibidi, Germany) at a density of 2 × 105 cells/well. After treated with different concentrations of rh-Endo and different doses of IR for 24 h, capillary tube structures were photographed (OLYMPUS, Japan), and the total tube length and the number of branch points in three random fields per well were counted. Representative capillary tube structures were shown. Data are expressed as the mean ± S.E. (n = 3).*P < 0.05
rh-Endo inhibits the migration and invasion of the non-irradiated and irradiated esophageal cancer cells
Wound-healing migration assays and transwell assays were used to further assess the effect of rh-Endo on the chemotactic motility of non-irradiated and irradiated cancer cells. rh-Endo significantly restricted the migration of cancer cells as presented in our wound-healing migration assays (Fig. 2). Meanwhile, in the invasive assays, only a few invasive cells were observed in the 400-μg/m rh-Endo-treated groups (Fig. 3). Therefore, we found that 100 and 400 μg/ml of rh-endo significantly inhibited the migration and invasion of cancer cells ECA109 and TE13 in both non-irradiated groups and 6-Gy-irradiated groups. The ratio was showed in the Fig. 4.
rh-Endo restricts the tube formation of the non-irradiated and irradiated esophageal cancer cells
VM formation is involved in cell migration and invasion, and the mechanism of which is analogous to that of endothelial cells [9, 16]. Thus, we used a well-established in vitro model of 3D culture to investigate tube formation of esophageal cancer cells similar to VM formation. Cancer cells were incubated with 10 μl liquid Matrigel, and capillary tube structures formed in the each group (as described in the materials and methods) at 4 h. We found the total tube length and branching points of tube formation were considerably restricted by rh-Endo both in non-irradiated and irradiated groups (Fig. 4), which revealed that rh-Endo restricts VM formation of the esophageal cancer cells with a dose-dependent relationship.
rh-Endo combined with irradiation inhibits migration, invasion, and VM formation of ESCC by inhibiting EMT thought inactivation of AKT/GSK-3β signaling pathway in vitro
Vasculogenic mimicry (VM) is a very complex process, related to the EMT, and mediated by many signaling routes, including the PTEN/AKT/GSK-3β signaling pathway [17, 18]. It has been reported that expression of PTEN is decreased after irradiation, and anti-angiogenic treatment inhibited cell proliferation and migration via regulating of the expression of local AKT [19, 20]. Thus, Western blot assays were performed to detect the protein expression of PTEN, total AKT, p-AKt, GSK-3β, and p-GSK-3β, and we found that the negatively regulate protein of AKT signaling pathway PTEN was decreased after irradiation, leading to the increase of Snail and the decrease of E-cadherin (two of EMT makers). Meanwhile, the expression of p-AKt and p-GSK-3β was increased remarkably. Most interesting was that all of these trends reversed when adding rh-Endo into each treatment group (Fig. 5). These results were obtained in both ECA109 and TE13, which suggested that PTEN deficiency activates Akt/GSK-3β/Snail/E-cadherin pathway upon irradiation, resulting in the increasing of migration, invasion, and VM formation of ESCC. While rh-Endo could reverse this process, leading rh-Endo combined with irradiation to becoming a promising approach to inhibition of the esophageal cancer cells metastasis.
rh-Endo combined with irradiation inhibits EMT through inactivation of PTEN/AKT/GSK-3β signaling pathway in ESCC. a Western blot analysis showing that irradiation reduced the levels of PTEN and E-cadherin in ECA109 and TE13 cells and increased the levels of p-AKT and Snail, while the levels of AKT remained unchanged. b rh-Endo significantly increased the level of PTEN as well as E-cadherin and reduced the levels of p-AKT, p-GSK-3β, and Snail both in irradiated and non-irradiated groups. Meanwhile, the levels of PTEN and E-cadherin reduced and the levels of p-AKT, p-GSK-3β and Snail increased in irradiated groups compared with non-irradiated control groups (P < 0.05)
Discussion
Radiotherapy is a well-established treatment in esophageal cancer even at advanced stages. It provides survival benefits and the improvement in quality of life for esophageal cancer patients, but the 5-year survival and the locoregional control of the disease are still not optimistic. The mechanism underlying the failure of radiotherapy may be caused by the metastasis of cancer cells [1, 2]. That rh-Endo is used as an anti-angiogenic agent in advanced NSCLC is suggested according to NCCN guidelines (Chinese version), which inhibited the cancer-related neovascularization of NSCLC, leading it to play an important role in the comprehensive treatment of NSCLC [21]. Recently, clinical trials and retrospective studies have demonstrated anti-tumor effect of rh-Endo in many other advanced tumors, such as metastatic melanoma, head and neck cancer, breast cancer, and gastric cancer [22]. However, it required more study to prove whether rh-Endo can be utilized in esophageal cancer. In our study, we demonstrated that rh-Endo could significantly inhibit EMT via decreasing PTEN expression and suppressing of the AKT/GSK-3β activity. Depending on the literature, irradiation promoted EMT in esophageal cancer cells through PTEN deficiency-mediated AKT activation, which may result in cancer cell metastasis and poor prognosis [15]. Therefore, rh-Endo combining with radiotherapy possibly provides more survival benefits than radiotherapy alone.
In the year of 2010 and 2011, two independent studies by Wang et al. and Maniotis et al. showed that tumors do not merely rely on the blood vessels of their hosts for nourishment and can form tube of cancer cells to make their own vasculature [23, 24]. These findings explain why several treatments for cancer could not achieve the expected effect. It was not the first time that researchers suggested that cancer cells could form their own vessels. In 1999, Maniotis et al. reported a similar effect in melanoma cells, which they called vascular mimicry [24].In a recently study, Du et al. believed that hypoxia contributed to VM formation by inducing EMT [25]. Radiotherapy and anti-angiogenic therapy are all involved in the regulation of EMT [15, 26]. Our study partially revealed the relationship between irradiation, anti-angiogenic therapy, and EMT for the first time. Furthermore, we found that rh-Endo combined with irradiation cloud restrict VM formation of the non-irradiated and irradiated esophageal cancer cells via inhibiting the occurrence of EMT, which could provide a new sight for the comprehensive treatment of advanced esophageal cancer.
It is well known that a key step in EMT is down-regulation of E-cadherin. E-cadherin is regulated either by transcription factors, such as Snail-related zinc-finger transcriptional repressors (Snail and Slug), SIP-1/ZEB-2, Twist, or ubiquitylation-induced endocytosis. In our study, we found irradiation increased the expression of Snail and decreased the expression of E-cadherin at the protein level. Ectopic over expression of Snail also leads to the acquisition of increased resistance to apoptosis and cancer stem cell-like properties in various epithelial cells [27]. The activation of Snail may be one of mechanisms involved in the development of radioresistance in ESCC after radiotherapy. However, to our surprise, the expression of Snail was significantly decreased when combined with rh-Endo (the result was compared with irradiation alone group), which proved rh-Endo would promote the effect of radiotherapy though down-regulating the expression of Snail.
AKT pathway plays a central role in the three major radioresistance mechanisms, including intrinsic radioresistance, tumor-cell proliferation, and hypoxia. PTEN, as an inhibitor of AKT, is reported to associate with radiosensitivity [28]. Kim et al. found PTEN to be imperative for attenuation of invasion and EMT [29]. Covered together, the down-regulation of PTEN is linked with dephosphorylation of AKT and GSK-3β, and PTEN-dependent PI3K/Akt/GSK-3β signaling is necessary to up-regulate Snail and down-regulate E-cadherin for radiation-induced EMT in ESCC. In this study, we also found that rh-Endo could influence all the above process, including inhibiting the expression of PTEN, activated AKT/GSK3β pathway, decreased Snail, and increased E-cadherin. As a consequence, the EMT to develop in ESCC was inhibited by rh-Endo. This effect of rh-Endo may be a potential cellular and molecular mechanism for anti-angiogenic therapy and radiotherapy. It will have profound significance for future tumor-related comprehensive treatment.
The invasion and VM formation of esophageal cancer cells increased after irradiation. Meanwhile, rh-Endo could reverse this process. Regardless of the fact that we found the PTEN/AKT/GSK-3β signaling pathway involved, how the irradiated cancer cells sent messages to the cells surrounded remains to be further studied. Membrane-derived extracellular vesicles (EVs) (i.e., exosomes) are small vesicles with sizes ranging from 30 to 120 nm. Exosomes vary in cell type and mechanism of biogenesis [30]. Knowledge of secretome components that influence EMT including secreted proteins/peptides and exosomes has emerged. Exosomes mediate intercellular communication and direct integral facets of carcinogenesis that include EMT, invasion, migration, angiogenesis, and metastasis [31, 32]. In another research of ours, exosomes were extracted from irradiated esophageal cancer cells supernatant, then added these exosomes to non-irradiated cancer cells. To our great surprise, the ability of VM formation and invasion in ESCC were promoted compared with a control group, which indicated exosomes the irradiated cancer cells secreted were involved in the EMT caused by radiotherapy. How exosomes regulate the EMT after irradiation needs more experimental results to reveal.
In conclusion, this study provided in vitro evidence that rh-Endo combined with radiotherapy inhibited migration, invasion, and VM formation of ESCC, indicating that rh-Endo probably suppresses metastasis of esophageal cancer, though it did not enhance the radiosensitivity of ESCC directly. This phenomenon is associated with the up-regulation of expression of PTEN and E-cadherin, down-regulation of expression of p-AKT, p-GSK3β, and Snail. We will continually find the value of rh-Endo combined with radiotherapy on clinical application.
Abbreviations
- ESCC:
-
Esophageal squamous cell carcinoma
- RT:
-
Radiotherapy
- rh-Endo:
-
Recombinant human endostatin
- NSCLC:
-
Non-small-cell lung cancer
- EMT:
-
Epithelial–mesenchymal transition
- VM:
-
Vaculogenic mimicry
- DMSO:
-
Dimethyl sulfoxide
- DMEM:
-
Dulbecco’s modified eagle medium
- FITC:
-
Fluorescein isothiocyanate
- CCk-8:
-
Cell counting kit-8
- PTEN:
-
Phosphatase and tensin homolog deleted on chromosome ten
- Akt:
-
Protein kinase B PKB
- GSK-3β:
-
Glycogen synthase kinase 3β
- GAPDH:
-
Glyceraldehyde-3-phosphate dehydrogenase
References
Yu S, Yang CS, Li J, You W, Chen J, Cao Y, et al. Cancer prevention research in china. Cancer Prev Res (Phila). 2015;8:662–74.
D’Journo XB, Thomas PA. Current management of esophageal cancer. J Thorac Dis. 2014;6 Suppl 2:S253–64.
Jain RK. Normalizing tumor vasculature with anti-angiogenic therapy: a new paradigm for combination therapy. Nat Med. 2001;7:987–9.
Carmeliet P, Jain RK. Angiogenesis in cancer and other diseases. Nature. 2000;407:249–57.
Behl T, Kaur I, Goel H, Kotwani A. Significance of the antiangiogenic mechanisms of thalidomide in the therapy of diabetic retinopathy. Vascul Pharmacol 2015.
Salza R, Oudart JB, Ramont L, Maquart FX, Bakchine S, Thoannes H, et al. Endostatin level in cerebrospinal fluid of patients with Alzheimer’s disease. J Alzheimers Dis. 2015;44:1253–61.
Al-Rawi S, Meehan-Andrews T, Bradley C, Al-Rawi J. Novel benzoxazines as inhibitors of angiogenesis. Investig New Drugs. 2015;33:45–52.
Xu X, Mao W, Chen Q, Zhuang Q, Wang L, Dai J, et al. Endostar, a modified recombinant human endostatin, suppresses angiogenesis through inhibition of Wnt/beta-catenin signaling pathway. PLoS One. 2014;9:e107463.
Sun T, Zhao N, Zhao XL, Gu Q, Zhang SW, Che N, et al. Expression and functional significance of Twist1 in hepatocellular carcinoma: its role in vasculogenic mimicry. Hepatology. 2010;51:545–56.
Kong D, Li Y, Wang Z, Sarkar FH. Cancer stem cells and epithelial-to-mesenchymal transition (EMT)-phenotypic cells: are they cousins or twins? Cancers (Basel). 2011;3:716–29.
Kalluri R, Weinberg RA. The basics of epithelial-mesenchymal transition. J Clin Invest. 2009;119:1420–8.
Polyak K, Weinberg RA. Transitions between epithelial and mesenchymal states: acquisition of malignant and stem cell traits. Nat Rev Cancer. 2009;9:265–73.
Hassan H, Greve B, Pavao MS, Kiesel L, Ibrahim SA, Gotte M. Syndecan-1 modulates beta-integrin-dependent and interleukin-6-dependent functions in breast cancer cell adhesion, migration, and resistance to irradiation. FEBS J. 2013;280:2216–27.
Meng MB, Jiang XD, Deng L, Na FF, He JZ, Xue JX, et al. Enhanced radioresponse with a novel recombinant human endostatin protein via tumor vasculature remodeling: experimental and clinical evidence. Radiother Oncol. 2013;106:130–7.
He E, Pan F, Li G, Li J. Fractionated ionizing radiation promotes epithelial-mesenchymal transition in human esophageal cancer cells through PTEN deficiency-mediated akt activation. PLoS One. 2015;10:e126149.
Ricci-Vitiani L, Pallini R, Biffoni M, Todaro M, Invernici G, Cenci T, et al. Tumour vascularization via endothelial differentiation of glioblastoma stem-like cells. Nature. 2010;468:824–8.
Dejana E. The role of wnt signaling in physiological and pathological angiogenesis. Circ Res. 2010;107:943–52.
Otrock ZK, Mahfouz RA, Makarem JA, Shamseddine AI. Understanding the biology of angiogenesis: review of the most important molecular mechanisms. Blood Cells Mol Dis. 2007;39:212–20.
Jung IL, Kang HJ, Kim KC, Kim IG. PTEN/pAkt/p53 signaling pathway correlates with the radioresponse of non-small cell lung cancer. Int J Mol Med. 2010;25:517–23.
Bai X, Li X, Tian J, Zhou Z. Antiangiogenic treatment diminishes renal injury and dysfunction via regulation of local AKT in early experimental diabetes. PLoS One. 2014;9:e96117.
Kim ES, Herbst RS. Angiogenesis inhibitors in lung cancer. Curr Oncol Rep. 2002;4:325–33.
Cui C, Mao L, Chi Z, Si L, Sheng X, Kong Y, et al. A phase II, randomized, double-blind, placebo-controlled multicenter trial of Endostar in patients with metastatic melanoma. Mol Ther. 2013;21:1456–63.
Wang R, Chadalavada K, Wilshire J, Kowalik U, Hovinga KE, Geber A, et al. Glioblastoma stem-like cells give rise to tumour endothelium. Nature. 2010;468:829–33.
Maniotis AJ, Folberg R, Hess A, Seftor EA, Gardner LM, Pe’Er J, et al. Vascular channel formation by human melanoma cells in vivo and in vitro: vasculogenic mimicry. Am J Pathol. 1999;155:739–52.
Du J, Sun B, Zhao X, Gu Q, Dong X, Mo J, et al. Hypoxia promotes vasculogenic mimicry formation by inducing epithelial-mesenchymal transition in ovarian carcinoma. Gynecol Oncol. 2014;133:575–83.
Welch-Reardon KM, Wu N, Hughes CC. A role for partial endothelial-mesenchymal transitions in angiogenesis? Arterioscler Thromb Vasc Biol. 2015;35:303–8.
Fan F, Samuel S, Evans KW, Lu J, Xia L, Zhou Y, et al. Overexpression of snail induces epithelial-mesenchymal transition and a cancer stem cell-like phenotype in human colorectal cancer cells. Cancer Med. 2012;1:5–16.
Keniry M, Parsons R. The role of PTEN signaling perturbations in cancer and in targeted therapy. Oncogene. 2008;27:5477–85.
Kim J, Kang HS, Lee YJ, Lee HJ, Yun J, Shin JH, et al. EGR1-dependent PTEN upregulation by 2-benzoyloxycinnamaldehyde attenuates cell invasion and EMT in colon cancer. Cancer Lett. 2014;349:35–44.
Roma-Rodrigues C, Fernandes AR, Baptista PV. Exosome in tumour microenvironment: Overview of the crosstalk between normal and cancer cells. Biomed Res Int. 2014;2014:179486.
Tickner JA, Urquhart AJ, Stephenson SA, Richard DJ, O’Byrne KJ. Functions and therapeutic roles of exosomes in cancer. Front Oncol. 2014;4:127.
Greening DW, Gopal SK, Mathias RA, Liu L, Sheng J, Zhu HJ, et al. Emerging roles of exosomes during epithelial-mesenchymal transition and cancer progression. Semin Cell Dev Biol. 2015;40:60–71.
Acknowledgments
This work was supported by the Natural Science Foundation of China (No. 81272504, No. 81472809), Innovation Team [No. LJ201123 (EH11)], A Project Funded by the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD) (JX10231801), grants from Key Academic Discipline of Jiangsu Province “Medical Aspects of Specific Environments”, Research and Innovation Project for College Graduates of Jiangsu Province (KYLX_0955). The methods were carried out in accordance with the approved guidelines.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Additional information
Xiaochen Chen, Hao Zhang and Hongcheng Zhu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Chen, X., Zhang, H., Zhu, H. et al. Endostatin combined with radiotherapy suppresses vasculogenic mimicry formation through inhibition of epithelial–mesenchymal transition in esophageal cancer. Tumor Biol. 37, 4679–4688 (2016). https://doi.org/10.1007/s13277-015-4284-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-4284-3